Abstract
Objective
Currently, there is no established guideline on whether to opt for percutaneous endoscopic lumbar discectomy (PELD) or traditional transforaminal lumbar interbody fusion (TLIF) surgery based on specific types of lumbar disc herniation (LDH). Based on the Michigan State University (MSU) classification system, this study conducted a medium‐ to long‐term follow‐up analysis of two surgical methods over 5 years for the first time, aiming to provide empirical evidence to assist in making more informed decisions before surgery for LDH treatment.
Methods
This was a retrospective study that included 273 patients with single‐level LDH who underwent PELD or TLIF treatment at our hospital between January 1, 2016, and December 31, 2018. Detailed metrics included preoperative and postoperative visual analogue scale (VAS) scores and Oswestry disability index (ODI) at 1‐day, 1‐week, 1‐year, and 5‐year follow‐ups. Complications, recurrences, and 5‐year postoperative modified MacNab criteria scores were also recorded. Statistical methods included independent sample t‐tests, repeated measures analysis of variance (ANOVA), and χ 2 tests.
Results
Classified into seven groups according to the MSU classification, it was found that there was an improvement in the VAS and ODI scores at four postoperative follow‐ups (p < 0.001). PELD showed better results than TLIF in reducing pain and improving the ODI scores in the classifications of 3B, 2B, and 2C (p < 0.05). TLIF demonstrated consistent superiority over PELD in 2A, 2AB, 3A, and 3AB classifications (p < 0.05). The total recurrence rate in the PELD group (11.05%) within 5 years after surgery was higher (p < 0.05) than that in the TLIF group (3.96%). These were mainly concentrated in the 2A, 2AB, 3A, and 3AB types. Moreover, the rate of excellent and good outcomes in the PELD was higher than in the TLIF but no significant difference (χ 2 = 1.0568, p = 0.5895).
Conclusion
This study suggests that PELD and TLIF may relieve LDH, but have advantages under different MSU classifications. The MSU classification has specific guiding significance and could aid in the surgical selection of PELD or TLIF to achieve optimal treatment outcomes for patients with lumbar disc herniation.
Keywords: Lumbar disc herniation, MSU classification, PELD, Retrospective study, TLIF
Based on our study's visual analogue scale (VAS) and Oswestry disability index (ODI) data, most people are more suitable to undergo percutaneous endoscopic lumbar discectomy (PELD) surgery than traditional transforaminal lumbar interbody fusion (TLIF) surgery. Traditional open TLIF surgery may not be suitable for people who require high spinal mobility and who want to return to everyday life in a short period. Therefore, based on comprehensive consideration of clinical efficacy and surgical recurrence rate, our study shows that PELD surgery is recommended for patients with type 2B, 2C, and 3B. For patients with types 2A, 2AB, 3A, and 3AB, TLIF surgery is recommended. However, it is necessary to reduce strenuous activities and heavy physical labor postoperatively to prevent complications such as screw loosening and adjacent segment disease.

Introduction
Lumbar disc herniation (LDH) is a major cause of low back pain, with most lumbar herniations occurring at the L4‐L5 or L5‐S1 levels. 1 This prevalent and disabling condition results in annual costs exceeding $100 billion in the United States alone. 2 Surgical intervention should be considered for symptomatic LDH refractory to conservative treatment. Percutaneous endoscopic lumbar discectomy (PELD) is characterized by a small incision and rapid recovery. It is the most common minimally invasive technique for the treatment of lumbar disc herniation. 3 It has gained widespread acceptance in clinical practice and is well‐regarded by numerous spine surgeons and patients. However, the limited visual field and anatomy may increase the difficulty of surgery, and some patients may be at risk of recurrence. 4 , 5 , 6 As a result, for those who fear recurrence, cannot remove the nucleus pulposus under PELD vision, or have mild instability, transforaminal lumbar interbody fusion (TLIF) becomes a vital alternative. TLIF is a spinal surgery that treats conditions such as disc herniation and spondylolisthesis 7 , 8 and involves the posterior insertion of fusion devices and bone graft materials between the vertebrae to promote spinal stability and fusion. Although TLIF surgery is effective, it still carries surgical risks such as infection, hematoma, screw loosening or breakage, and cage subsidence. It may require an extended recovery period, primarily until complete spinal fusion is achieved. 6 However, there is currently no established guidance on whether to opt for PELD or traditional TLIF surgery based on the specific types of LDH.
The Michigan State University (MSU) classification, proposed in 2010, effectively evaluates LDH. It utilizes a T2 axial magnetic resonance imaging (MRI) section as the reference plane (Figure 1). It uses a single inner facet line as a reference point to measure disc herniation at the maximum extrusion level. Specifically, using the inner line of the articular process, the end of the maximum protrusion distance was divided into levels 1–3 from top to bottom. Next, three points, A, B, and C, were placed along the in‐plane line and divided into four equal quarters, and vertical lines were drawn through each end to create the left, right, and left and right central quadrants. Among them, zone A is considered the central type. Zone C is the area from the medial edge of any facet joint to the lateral quadrant, and is regarded as the intervertebral foramen level. 9 Currently, in clinical practice, personalized treatment strategies for patients with LDH remain limited, especially considering the complex social and psychological factors of patients. Moreover, the MSU classification has been used to evaluate the clinical efficacy of different types of LDH for ozone injection into intervertebral discs. 10 We conducted a retrospective comparative analysis using the traditional minimally invasive and open surgery techniques, PELD and TLIF, combined with the MSU classification for the first time. First, we explored this classification system (Figure 2), then evaluated the clinical efficacy and recurrence rates of the two surgical methods under this system. Finally, we hoped that this classification system provided a clear framework for communication, provide a reasonable basis for the selection of surgical methods, promotes consistency in clinical decision‐making, and provided a scientific basis for creating personalized treatment plans for patients, thereby improving treatment outcomes and advancing clinical research. 11
FIGURE 1.
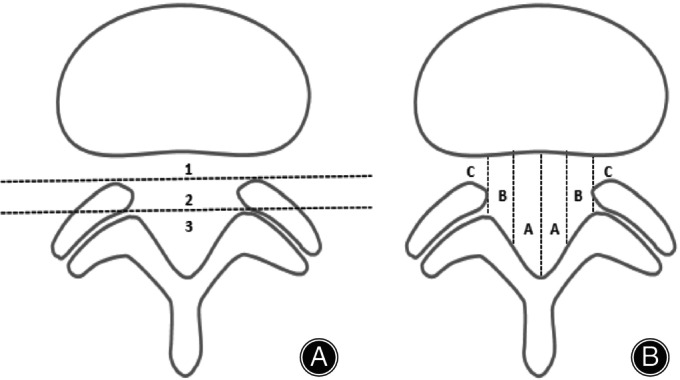
Grading and zoning according to the Michigan State University (MSU) classification system. (A) Lines denoting the grading of disc herniation are drawn along the horizontal axis. Grades 1 to 3 signify an increasing impact on nerve compression. (B) Lines indicating the zoning of disc herniation are drawn along the vertical axis. Lesions in Zone‐B and Zone‐C are considered to have a more significant impact.
FIGURE 2.
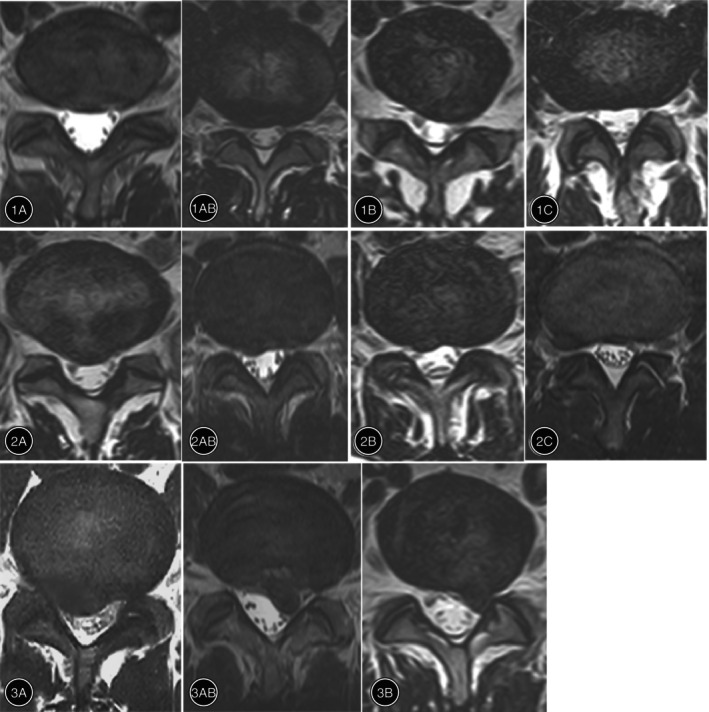
Michigan State University (MSU) classification in clinical practice. 1–3 are the grades of the MSU classification, with the severity of the hernia increasing sequentially. (A–C) represent different protrusion regions.
Materials and Methods
Patients' Characteristics
This study included 273 patients with single‐level LDH who underwent surgery at our hospital between January 2016 and December 2018. Among them, 172 underwent PELD, and 101 underwent TLIF. The same highly experienced spine surgeon performed all the procedures. The inclusion criteria for patients in this study were as follows: (i) clinical symptoms of back pain; (ii) single‐level disc herniation with symptoms confirmed by magnetic resonance imaging; (iii) underwent PELD or TLIF surgery; (iv) ineffective conservative treatment for more than 6 months; and (v) a minimum follow‐up period of 5 years. The exclusion criteria were: (i) spinal canal stenosis, lumbar spondylolisthesis, severe instability, or severe intervertebral space collapse; (ii) severe cardiac, pulmonary, or cerebral diseases, coagulopathy, or intolerance to surgery; and (iii) a history of lumbar surgery, fracture, infection, or tumor. This study was approved by the Ethics Committee of the Affiliated Hospital of Traditional Chinese Medicine, Southwest Medical University. Informed consent was obtained from all participants (BY2024015).
Surgical Operation
The procedure for PELD surgery is as follows. After the anesthesia takes effect, the puncture needle is inserted into the shoulder of the superior articular process, followed by the gradual insertion of a soft tissue dilator along the guide wire, and the protruding nucleus pulposus is excised using an intervertebral foramen endoscope (Figure 3). In case of a high iliac crest, foraminoplasty is used to treat L5‐S1 disc herniation.
FIGURE 3.
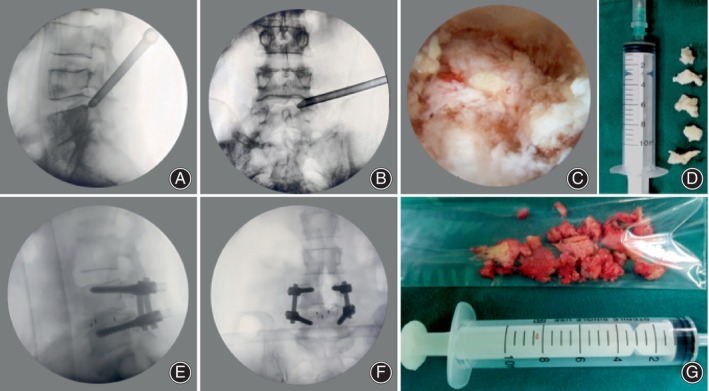
Illustrated cases. (A–D) Intraoperative fluoroscopy of the surgical area in percutaneous endoscopic lumbar discectomy (PELD) operation and the removed nucleus pulposus. (E–G) Intraoperative fluoroscopy of the traditional transforaminal lumbar interbody fusion (TLIF) surgical area and the removed nucleus pulposus.
The operating procedure for traditional TLIF is as follows. An incision is made along the posterior midline over the lumbar spine, followed by detachment of the paraspinal muscles from the spinous processes, laminae, facet capsules, and transverse processes. The implantation of the pedicle screws is then completed. Inferior facetectomy is carried out, followed by resectioning of the superior facet, discectomy, cage implantation, and bone grafting (Figure 3).
Clinical Evaluation
Detailed metrics included preoperative and postoperative visual analogue scale (VAS) 12 scores and the Oswestry disability index (ODI) 13 at the 1‐day, 1‐week, 1‐year, and 5‐year follow‐ups. The 5‐year postoperative modified MacNab 14 criteria scores were also recorded.
Visual Analogue Scale
The VAS is used to evaluate the degree of pain using a ruler that provides a range of scores from 0 to 10, where 0 indicates no pain, and 10 represents unbearable pain. A higher score indicates greater pain intensity.
Oswestry Disability Index
The ODI is a measure used to evaluate spinal disorders and to assess patient progression in clinical practice. Scores of 0%–20% are considered mild dysfunction, 21%–40% are considered moderate dysfunction, 41%–60% are considered severe dysfunction, and 61%–80% are considered disability. Patients with scores of 81%–100% are either long‐term bedridden or exaggerating the impact of pain on their lives.
Modified MacNab Criteria
A typical version of the modified MacNab criteria scale is as follows. Excellent: no pain, no restriction of mobility, return to routine work, and level of activity. Good: occasional nonradicular pain, relief of presenting symptoms, able to return to modified work. Fair: some improvement in functional capacity, still handicapped, and/or unemployed. Poor: continued objective symptoms of root involvement and additional operative intervention required at the index level, irrespective of the length of postoperative follow‐up.
Statistical Analysis
All data were analyzed using SPSS software (version 28.0, SPSS Inc., Chicago, IL, USA), and continuous variables were expressed as mean ± standard deviation. Independent‐sample t‐tests were used to compare the age, follow‐up time, and perioperative outcomes. Repeated measures analysis of variance (ANOVA) were utilized for VAS and ODI data, with Bonferroni correction applied for multiple comparisons. Chi‐square tests were used for categorical data, such as sex, disc location, disc level, complications, and recurrence rates. Statistical significance was defined as p < 0.05 or p < 0.001 in our study.
Results
Preoperative Data of the Patients
We conducted a minimum 5‐year follow‐up for 273 patients, with a mean follow‐up period of 5.65 ± 0.23 months. No significant differences were observed in baseline demographic characteristics, including age, sex, operative segment, disc location, and sensory dysfunction, except for motor deficits. The clinical and demographic profiles of patients in both groups are summarized (Table 1).
TABLE 1.
Preoperative data of PELD and TLIF groups.
| Operations | Age | Sex | Disc location | Disc level | Sensory deficits | Motor deficits | Follow‐up time | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| (years) | M | F | 2A | 2AB | 2B | 2C | 3A | 3AB | 3B | L3/4 | L4/5 | L5/S1 | (years) | |||
| PELD n = 172 | 51.3 ± 13.7 | 97 | 75 | 23 | 1 | 39 | 16 | 30 | 20 | 33 | 6 | 89 | 77 | 117 | 96 | 5.6 ± 0.3 |
| TLIF n = 101 | 50.8 ± 9.9 | 57 | 44 | 19 | 9 | 17 | 9 | 20 | 8 | 19 | 3 | 52 | 46 | 79 | 83 | 5.7 ± 0.2 |
| p | 0.6439 | 1.0000 | 0.6910 | 0.9469 | 0.0710 | <0.05 | 0.5490 | |||||||||
Note: Data of age and follow‐up time were mean ± standard deviation.
Abbreviations: F, female; M, male; PELD, percutaneous endoscopic lumbar discectomy; TLIF, transforaminal lumbar interbody fusion.
Perioperative Observational Index, Complications, and Recurrence
Compared with the TLIF group, the PELD group had significantly shorter surgery times, less intraoperative bleeding, and shorter postoperative hospital stay (p < 0.05) (Table 2). Thirteen complications occurred in the PELD group (7.56%) and six complications occurred in the TLIF group (5.94%) (p = 0.6140). In the TLIF group, three patients developed an epidural hematoma and were cured after hematoma drainage. Three patients in the TLIF group developed fever 1 day postoperatively, which improved after bed rest and physical cooling. In the PELD group, nine patients complained of poor lower limb sensation, which improved after treatment with neurotrophic drugs. During surgery in the PELD group, four cases of epidural hematoma occurred, which were cured after hematoma drainage. The total recurrence rate in the PELD group (11.05%) within 5 years after surgery was significantly higher (p < 0.05) than that in the TLIF group (3.96%). Patients with recurrence of PELD complained of low back pain, and re‐examination MRI showed that the intervertebral disc at the surgical level had re‐herniated. The numbers of recurrence cases in the PELD group in the 2A, 2AB, 2B, and 2C classifications were five, four, one, and one, respectively. The numbers of recurrence cases in the PELD group according to the 3A, 3AB, and 3B classifications were four, three, and one, respectively. In the TLIF group, there was one case of recurrence according to the 2A, 3A, 3AB, and 3B classifications (Table 3). Patients with TLIF recurrence also complained of low back pain; however, no disc herniation at the surgical level was observed on follow‐up MRI.
TABLE 2.
Perioperative outcomes (mean ± standard deviation).
| Operations | Operation time (minutes) | Intraoperative hemorrhage (mL) | Postoperative hospitalization (days) |
|---|---|---|---|
| PELD n = 172 | 54.3 ± 5.5 | 16.5 ± 10.3 | 3.0 ± 0.4 |
| TLIF n = 101 | 123.5 ± 20.6 | 197.3 ± 94.8 | 6.0 ± 0.5 |
| p | <0.05 | <0.05 | <0.05 |
Abbreviations: PELD, percutaneous endoscopic lumbar discectomy; TLIF, transforaminal lumbar interbody fusion.
TABLE 3.
Perioperative complications and recurrence.
| Grade | Complication, n (%) | Recurrence, n (%) | ||
|---|---|---|---|---|
| PELD | TLIF | PELD | TLIF | |
| 2A | 2 (1.16) | 1 (0.99) | 5 (2.90) | 0 (0) |
| 2AB | 3 (1.74) | 0 (0) | 4 (2.32) | 0 (0) |
| 2B | 2 (1.16) | 1 (0.99) | 1 (0.58) | 1 (0.99) |
| 2C | 2 (1.16) | 1 (0.99) | 1 (0.58) | 0 (0) |
| 3A | 1 (0.58) | 1 (0.99) | 4 (2.32) | 1 (0.99) |
| 3AB | 1 (0.58) | 1 (0.99) | 3 (1.74) | 1 (0.99) |
| 3B | 2 (1.16) | 1 (0.99) | 1 (0.58) | 1 (0.99) |
| p | 0.6140 | <0.05 | ||
Abbreviations: PELD, percutaneous endoscopic lumbar discectomy; TLIF, transforaminal lumbar interbody fusion.
Clinical Evaluation
Visual Analog Scale
There was no significant difference in the preoperative VAS scores among all LDH types (p > 0.05). Moreover, they significantly improved after undergoing PELD or TLIF (p < 0.001). The relevant VAS data are presented in Table 4 and Figure 4. Compared to the TLIF group, the VAS scores at 1 day and 1 week after PELD were significantly lower in all groups (p < 0.05). In the 2A classification, there was no significant difference in the VAS scores between the two groups during the 1‐year follow‐up after surgery (F = 0.844, p = 0.364). However, at the last follow‐up at in the 5th year, the VAS score of the PELD group (2.65 ± 1.90) was significantly higher (p < 0.05) than that of the TLIF group (0.89 ± 0.88). Similarly, in the 2AB classification, there was no significant difference in the VAS scores between the PELD and TLIF groups at the 1‐year follow‐up after surgery (F = 1.351, p = 0.260). The VAS score of the PELD group (2.55 ± 2.02) 5 years after surgery was significantly higher (p < 0.05) than that of the TLIF group (0.78 ± 1.09). In the 2B classification, the VAS score in the PELD group (0.74 ± 0.75) was significantly lower (p < 0.05) than that in the TLIF group (1.76 ± 0.83) at 1 year after surgery. However, the two groups showed no significant difference in the VAS scores at 5 years after surgery (F = 2.550, p = 0.116). According to the 2C classification, the VAS scores at all follow‐up visits in the PELD group were significantly lower (p < 0.05) than those in the TLIF group. In the 3A classification, there was no significant difference in the VAS scores between the two groups during the 1‐year follow‐up after surgery (F = 0.006, p = 0.938). However, at the last follow‐up in the 5th year, the VAS score of the PELD group (2.07 ± 1.82) was significantly higher (p < 0.05) than that of the TLIF group (0.85 ± 0.67). Similarly, in the 3AB classification, there was no significant difference in the VAS scores between the two groups during the 1‐year follow‐up after surgery (F = 1.582, p = 0.220). However, at the last follow‐up in the 5th year, the VAS score of the PELD group (2.00 ± 1.38) was significantly higher (p < 0.05) than that of the TLIF group (0.75 ± 0.71). In the 3B classification, there was no significant difference in the VAS scores between the two groups at 1 and 5 years after surgery (F = 1.332/0.466, p = 0.254/0.498).
TABLE 4.
Low back VAS outcomes of PELD and TLIF groups (mean ± standard deviation).
| Grade | Preoperative | Post 1 day | Post 1 week | Post 1 year | Post 5 years | F | p | |
|---|---|---|---|---|---|---|---|---|
| 2A | PELD | 6.64 ± 0.79 | 2.70 ± 0.70 a | 1.35 ± 0.78 a | 0.74 ± 0.62 a | 2.65 ± 1.90 a | 262.535 | <0.001 |
| TLIF | 7.16 ± 0.83 | 3.95 ± 0.78 a | 2.00 ± 0.67 a | 0.95 ± 0.85 a | 0.89 ± 0.88 a | 200.781 | <0.001 | |
| F | 3.246 | 29.889 | 8.343 | 0.844 | 13.821 | |||
| p | 0.079 | <0.05 | <0.05 | 0.364 | <0.05 | |||
| 2AB | PELD | 7.18 ± 1.08 | 2.55 ± 0.82 a | 1.18 ± 0.87 a | 0.91 ± 0.54 a | 2.55 ± 2.02 a | 207.060 | <0.001 |
| TLIF | 7.16 ± 0.83 | 3.89 ± 0.78 a | 2.11 ± 0.60 a | 1.22 ± 0.67 a | 0.78 ± 1.09 a | 182.423 | <0.001 | |
| F | 1.536 | 13.844 | 7.311 | 1.351 | 5.537 | |||
| p | 0.231 | <0.05 | <0.05 | 0.260 | <0.05 | |||
| 2B | PELD | 7.18 ± 1.12 | 2.10 ± 0.85 a | 1.49 ± 0.76 a | 0.74 ± 0.75 a | 0.69 ± 0.95 a | 633.051 | <0.001 |
| TLIF | 7.65 ± 0.83 | 4.12 ± 0.99 a | 2.24 ± 0.90 a | 1.76 ± 0.83 a | 1.18 ± 1.24 a | 197.327 | <0.001 | |
| F | 2.513 | 59.879 | 10.281 | 28.796 | 2.550 | |||
| p | 0.119 | <0.05 | <0.05 | <0.05 | 0.116 | |||
| 2C | PELD | 6.81 ± 1.01 | 1.69 ± 0.87 a | 0.63 ± 0.62 a | 0.73 ± 0.88 a | 0.69 ± 0.79 a | 344.509 | <0.001 |
| TLIF | 7.44 ± 0.88 | 3.56 ± 0.88 a | 1.89 ± 0.60 a | 2.11 ± 1.17 a | 1.56 ± 0.53 a | 119.280 | <0.001 | |
| F | 2.561 | 26.179 | 24.497 | 12.026 | 22.358 | |||
| p | 0.123 | <0.05 | <0.05 | <0.05 | <0.05 | |||
| 3A | PELD | 7.34 ± 0.86 | 2.13 ± 0.78 a | 0.77 ± 0.77 a | 0.97 ± 0.73 a | 2.07 ± 1.82 a | 611.865 | <0.001 |
| TLIF | 7.86 ± 0.87 | 4.10 ± 0.91 a | 2.20 ± 0.70 a | 0.95 ± 0.76 a | 0.85 ± 0.67 a | 318.795 | <0.001 | |
| F | 4.114 | 66.969 | 44.543 | 0.006 | 8.166 | |||
| p | 0.048 | <0.05 | <0.05 | 0.938 | <0.05 | |||
| 3AB | PELD | 7.68 ± 0.67 | 2.35 ± 0.49 a | 0.85 ± 0.75 a | 1.45 ± 0.61 a | 2.00 ± 1.38 a | 644.394 | <0.001 |
| TLIF | 7.88 ± 0.64 | 5.00 ± 0.93 a | 2.63 ± 0.74 a | 1.75 ± 0.46 a | 0.75 ± 0.71 a | 145.427 | <0.001 | |
| F | 0.411 | 98.895 | 32.450 | 1.582 | 27.495 | |||
| p | 0.527 | <0.05 | <0.05 | 0.220 | <0.05 | |||
| 3B | PELD | 7.66 ± 0.79 | 2.18 ± 0.64 a | 0.82 ± 0.73 a | 1.15 ± 0.97 a | 0.67 ± 0.69 a | 535.651 | <0.001 |
| TLIF | 7.37 ± 0.46 | 4.32 ± 0.75 a | 2.42 ± 0.77 a | 1.47 ± 0.96 a | 0.84 ± 1.17 a | 211.014 | <0.001 | |
| F | 2.258 | 119.292 | 56.241 | 1.332 | 0.466 | |||
| p | 0.139 | <0.05 | <0.05 | 0.254 | 0.498 |
Abbreviations: PELD, percutaneous endoscopic lumbar discectomy; Post, post‐operation; TLIF, transforaminal lumbar interbody fusion; VAS, visual analog scale.
After Bonferroni correction, the difference is statistically significant.
FIGURE 4.
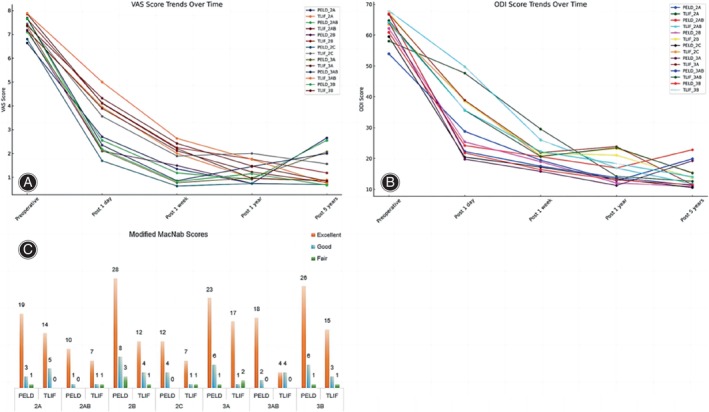
Statistical data graph of two groups before and after surgery under Michigan State University (MSU) classification. (A) VAS statistics of percutaneous endoscopic lumbar discectomy (PELD) groups and traditional transforaminal lumbar interbody fusion (TLIF) groups at each classification. (B) Oswestry disability index (ODI) statistics of PELD groups and TLIF groups at each classification. (C) Modified MacNab Scores of two groups at each classification.
Oswestry Disability Index
There was no significant difference in the preoperative ODI among all the LDH types (p > 0.05). Moreover, they significantly improved after undergoing PELD or TLIF (p < 0.001). The relevant ODI data statistics are presented in Table 5 and Figure 4. Compared with the TLIF group, the ODI scores at 1 day and 1 week after PELD were significantly reduced in all groups (p < 0.05). In the 2A classification, there was no significant difference in the ODI scores 1 year after surgery between the PELD and TLIF groups (F = 0.725, p = 0.400). However, the ODI scores 5 years after surgery in the PELD group (16.78 ± 5.45) were significantly higher (p < 0.05) than those in the TLIF group (12.58 ± 4.17). Similar to the 2A classification, in the 2AB classification, there was no significant difference in the ODI scores 1 year after surgery between the PELD and TLIF groups (F = 0.000, p = 0.995). However, the ODI scores 5 years after surgery in the PELD group (22.82 ± 11.44) were significantly higher (p < 0.05) than those in the TLIF group (11.78 ± 8.29). However, in the 2B classification, the ODI score 1 year after surgery in the PELD group (12.03 ± 5.27) was significantly lower (p < 0.05) than that in the TLIF group (21.06 ± 6.86). There was no significant difference in the ODI scores between the two groups at the 5‐year follow‐up (F = 1.659, p = 0.203). Similarly, in the 2C classification, the ODI score 1 year after surgery in the PELD group (13.38 ± 5.06) was significantly lower (p < 0.05) than that in the TLIF group (23.22 ± 11.78). In the follow‐up ODI score after 5 years, the PELD group (10.56 ± 3.69) was also significantly lower (p < 0.05) than the TLIF group (15.44 ± 7.62). In the 3A classification, the ODI score 1 year after surgery in the PELD group (11.23 ± 4.72) was significantly lower (p < 0.05) than that in the TLIF group (23.85 ± 7.76). However, the ODI score 5 years after surgery in the PELD group (19.23 ± 11.26) was significantly higher (p < 0.05) than that in the TLIF group (11.50 ± 5.01). In the 3AB classification, the ODI score 1 year after surgery in the PELD group (13.80 ± 4.41) was significantly lower (p < 0.05) than that in the TLIF group (23.50 ± 5.73). There was no significant difference in the ODI scores between the two groups at 5 years after surgery (F = 2.248, p = 0.146). In the 3B classification, the ODI score 1 year after surgery in the PELD group (13.00 ± 4.97) was significantly lower (p < 0.05) than that in the TLIF group (18.32 ± 8.38). There was no significant difference in the ODI scores between the two groups 5 years after surgery (F = 1.198, p = 0.279).
TABLE 5.
Clinical ODI outcomes of PELD and TLIF groups (mean ± standard deviation).
| Grade | Preoperative | Post 1 day | Post 1 week | Post 1 year | Post 5 years | F | p | |
|---|---|---|---|---|---|---|---|---|
| 2A | PELD | 53.95 ± 10.84 | 28.78 ± 6.90 a | 19.43 ± 4.88 a | 12.78 ± 4.54 a | 16.78 ± 5.45 a | 103.354 | <0.001 |
| TLIF | 58.05 ± 8.32 | 47.68 ± 6.51 a | 29.53 ± 7.28 a | 14.21 ± 6.31 a | 12.58 ± 4.17 a | 108.753 | <0.001 | |
| F | 1.186 | 82.150 | 28.708 | 0.725 | 5.698 | |||
| p | 0.285 | <0.05 | <0.05 | 0.400 | <0.05 | |||
| 2AB | PELD | 60.9 ± 12.57 | 24.18 ± 4.67 | 20.55 ± 3.75 | 16.91 ± 5.17 | 22.82 ± 11.44 a | 104.813 | <0.001 |
| TLIF | 67.89 ± 4.86 | 49.78 ± 5.49 a | 26.00 ± 5.15 a | 16.89 ± 8.07 a | 11.78 ± 8.29 a | 227.744 | <0.001 | |
| F | 1.295 | 127.124 | 7.515 | 0.000 | 26.713 | |||
| p | 0.323 | <0.05 | <0.05 | 0.995 | <0.05 | |||
| 2B | PELD | 62.18 ± 10.16 | 25.38 ± 5.77 a | 18.95 ± 4.38 a | 12.03 ± 5.27 a | 10.87 ± 6.66 a | 321.463 | <0.001 |
| TLIF | 67.29 ± 5.59 | 38.47 ± 3.99 a | 21.65 ± 3.00 a | 21.06 ± 6.86 a | 13.71 ± 9.39 a | 131.141 | <0.001 | |
| F | 3.742 | 71.956 | 5.340 | 28.855 | 1.659 | |||
| p | 0.058 | <0.05 | <0.05 | <0.05 | 0.203 | |||
| 2C | PELD | 59.53 ± 9.21 | 20.44 ± 4.29 a | 17.19 ± 4.00 a | 13.38 ± 5.06 a | 10.56 ± 3.69 a | 168.462 | <0.001 |
| TLIF | 63.56 ± 7.31 | 38.88 ± 4.79 a | 20.78 ± 3.38 a | 23.22 ± 11.78 a | 15.44 ± 7.62 a | 94.026 | <0.001 | |
| F | 1.348 | 103.252 | 5.144 | 6.460 | 4.726 | |||
| p | 0.258 | <0.05 | <0.05 | <0.05 | <0.05 | |||
| 3A | PELD | 64.14 ± 5.41 | 19.77 ± 4.76 a | 15.80 ± 3.14 a | 11.23 ± 4.72 a | 19.23 ± 11.26 a | 1073.253 | <0.001 |
| TLIF | 66.86 ± 3.87 | 38.90 ± 5.20 a | 21.90 ± 2.98 a | 23.85 ± 7.76 a | 11.50 ± 5.01 a | 403.695 | <0.001 | |
| F | 2.783 | 176.136 | 50.962 | 51.167 | 8.296 | |||
| p | 0.102 | <0.05 | <0.05 | <0.05 | <0.05 | |||
| 3AB | PELD | 66.74 ± 5.88 | 22.25 ± 3.42 a | 17.50 ± 3.35 a | 13.80 ± 4.41 a | 11.25 ± 5.14 a | 423.025 | <0.001 |
| TLIF | 64.75 ± 5.26 | 35.63 ± 5.53 a | 20.63 ± 2.67 a | 23.50 ± 5.73 a | 15.25 ± 8.91 a | 102.277 | <0.001 | |
| F | 0.799 | 61.011 | 5.519 | 23.330 | 2.248 | |||
| p | 0.380 | <0.05 | <0.05 | <0.05 | 0.146 | |||
| 3B | PELD | 66.94 ± 5.42 | 21.79 ± 3.34 a | 16.36 ± 4.02 a | 13.00 ± 4.97 a | 11.45 ± 5.18 a | 680.405 | <0.001 |
| TLIF | 64.16 ± 4.00 | 35.68 ± 7.74 a | 22.21 ± 2.99 a | 18.32 ± 8.38 a | 14.05 ± 11.87 a | 283.523 | <0.001 | |
| F | 2.888 | 81.095 | 30.363 | 8.286 | 1.198 | |||
| p | 0.095 | <0.05 | <0.05 | <0.05 | 0.279 |
Abbreviations: ODI, Oswestry Disability Index; PELD, percutaneous endoscopic lumbar discectomy; TLIF, transforaminal lumbar interbody fusion; Post, post‐operation.
After Bonferroni correction, the difference was statistically significant.
Modified MacNab Criteria
In the 2A classification, 22 patients (95.7%) in the PELD groups obtained excellent or good prognoses, and 19 patients (100%) in the TLIF groups obtained excellent or good prognoses. In the 2AB classification, 11 patients (100%) in the PELD group obtained excellent or good prognoses, and eight patients (88.9%) in the TLIF group obtained excellent or good prognoses. In the 2B classification, 36 patients (92.3%) in the PELD group obtained excellent or good prognoses, and 16 patients (84.2%) in the TLIF group obtained excellent or good prognoses. In the 2C classification, 16 patients (100%) in the PELD group obtained excellent or good prognoses, and eight patients (88.9%) in the TLIF group obtained excellent or good prognoses. In the 3A classification, 29 patients (96.7%) in the PELD group obtained excellent or good prognoses, and 18 patients (90%) in the TLIF group obtained excellent or good prognoses. In the 3AB classification, 20 patients (100%) in the PELD group obtained excellent or good prognoses, and eight patients (100%) in the TLIF group obtained excellent or good prognoses. In the 3B classification, 32 patients (97.0%) in the PELD groups obtained excellent or good prognoses, and 18 patients (94.7%) in the TLIF groups obtained excellent or good prognoses. However, no significant differences were observed (χ 2 = 1.0568, p = 0.5895) (Figure 4).
Discussion
MSU Classification Plays a Crucial Role in the Choice between PELD and TLIF
The MSU classification is a scoring system based on MRI findings. It categorizes LDH into different types based on the extent and location of the herniated disc, providing a reference for clinical doctors in choosing surgical approaches. 8 Due to advancements in endoscopic surgical technology over the past decades, PELD has emerged as a routine, minimally invasive method for LDH treatment, acclaimed for its lesser impact on back muscles and bones, less surgical bleeding, shorter hospital stay durations, and expedited recovery periods. 5 , 15 Moreover, the surgical approach in PELD allows for preserving spinal mobility, a significant consideration for many patients, especially those younger or with active lifestyles. 16 , 17 Despite its benefits, PELD is a non‐fusion surgery, which increases the risk of complications (such as neurological symptoms, hematoma, etc.) and recurrent LDH. 18 In contrast, the traditional TLIF technique, introduced in 1982, effectively treats LDH by removing the damaged disc and using a cage and bone grafting for fusion, thus restoring spinal stability and relieving symptoms. 19 , 20 Traditional TLIF is believed to offer higher fusion success rates, lower recurrence rates, better removal of the nucleus pulposus, and improved vertebral stability. 21 , 22 , 23 However, TLIF surgery has drawbacks, including increased intraoperative injury, an extended recovery period, and a higher risk of potential complications such as infection, hematoma, screw loosening or breakage, and cage subsidence. 24 Notably, no comparison of the clinical efficacy of PELD and traditional TLIF surgical strategies based on LDH classification has been reported. Therefore, the selection of a safe and effective surgical plan for patients with different types of LDH is of paramount importance. Utilizing the MSU classification system in this decision‐making process allows for a more tailored approach that considers the specific characteristics and severity of disc herniation. This optimization aimed to enhance surgical treatment strategies for different LDH types, improve clinical efficacy, and reduce the risk of potential complications. Therefore, this study aimed to compare the efficacies of PELD and TLIF in treating lumbar disc herniation in a 5‐year retrospective follow‐up study based on the MSU classification system.
Clinical Efficacy between PELD and TLIF under MSU Classification
The perioperative data in our study showed that the PELD group experienced less blood loss during surgery, shorter operation times, and faster postoperative recovery than the TLIF group. These are consistent with findings from previous studies. 25 , 26 On the one hand, the clinical data of our study showed that PELD demonstrated superior VAS and ODI compared to TLIF in the 1‐day and 1‐week postoperative periods, likely due to the minimally invasive and less disruptive nature for muscle tissue and bone structure. However, these differences could affect the duration of disability and psychological health of patients, as well as their compliance with and trust in their physicians, which may lead to certain misunderstandings and inducements of the final recovery effect. Moreover, the data indicated that in types 2B and 2C (i.e., lateral and far lateral), PELD showed better 1‐ and 5‐year VAS and ODI outcomes than TLIF. Even in type 3B, the data on ODI showed that at the 1‐ and 5‐year follow‐ups, the ODI in the PELD group was significantly lower than that in the TLIF group. This is likely due to the transforaminal approach in PELD, which provides a better surgical field of view for lateral and foraminal‐level lateral protrusions under minimally invasive conditions. Moreover, according to the modified MacNab standard, the PELD group had excellent and reasonable rates, which were higher than those of the TLIF group.
On the other hand, clinical data of our study showed that in the types 2A and 2AB, the VAS scores at 5‐year follow‐up after TLIF surgery were significantly lower than those in the PELD groups, with a statistically significant difference. Moreover, significant differences were observed between Types 3A and 3AB. There were several reasons for this finding. Zone A is defined as the central type and zone AB lies between the central and lateral types. When grade 2 and 3 disc herniations occur in either of the two more constrained areas (zones A and AB), there is usually minimal impact on the spinal nerve. During TLIF, the diseased intervertebral disc is removed by avoiding damaging the spinal canal and exposing the surgical field.
In contrast, PELD may not remove the protruding nucleus pulposus in front of the spinal canal. However, in the Grade 3A, 3AB, and 3B types, the ODI scores 5 years post‐surgery for the TLIF group were significantly higher than those for the PELD group, with the difference being statistically significant. This may be due to scar tissue and internal fixation, which limits the patient's lumbar mobility. This could also explain why many patients with LDH are now less inclined to undergo TLIF. Although traditional open TLIF surgery is associated with a more extended recovery period and tremendous postoperative pain, appropriate postoperative management and rehabilitation programs can effectively address these issues and accelerate the patient's return to normal daily activities. 27 , 28 Therefore, based on the above clinical evaluation, PELD has advantages over TLIF in MSU classifications 3B, 2B, and 2C. TLIF also has advantages over PELD in MSU classifications 2A, 2AB, 3A, and 3AB.
Recurrence Rate between PELD and TLIF under MSU Classification
Because PELD is minimally invasive and patients recover quickly, most patients return to work and life earlier, making it more likely to cause LDH recurrence. The recurrence rate data from our study showed that the recurrence rate in the PELD group after 5 years was significantly higher (p < 0.05) than that in the TLIF group and was mainly in the 2A, 2AB, 3A, and 3AB classifications. There may be several reasons for postoperative recurrence of PELD in zones A and AB (central and paracentral types). First, owing to the enormous break in the annulus fibrosus after the nucleus pulposus is removed, the nucleus pulposus inside the intervertebral disc is more likely to be squeezed out of the break, causing LDH. Second, because of the protruding giant nucleus pulposus, resection of the nucleus pulposus results in hollowing out of the intervertebral disc, leading to insufficient support. Later, the nucleus pulposus inside the intervertebral disc is extruded, leading to the eventual recurrence of LDH. Third, because the protruding nucleus pulposus of zones A and AB is close to the dura mater (ventral side) and compresses the dura mater or nerves, a herniated nucleus pulposus may not be directly found under PELD vision. It is necessary to perform internal indirect decompression from the normal annulus fibrosus surface into the intervertebral disc, and then find and remove the original herniated nucleus pulposus. The nucleus pulposus inside the intervertebral disc may protrude from these two breaches, causing LDH recurrence. Fourth, when treating the herniated nucleus pulposus close to the dura mater (ventral side) in zones A and AB, heat conduction occurs when the disc surface is cauterized for annuloplasty, causing dural sac rupture and nerve injury. At this time, the formation of the annulus fibrosus is not perfect, and it is more likely to cause the nucleus pulposus to protrude again from the breach, resulting in the recurrence of LDH. Thus, based on the recurrence rate data, we do not recommend PELD for patients with types 2A, 2AB, 3A, and 3AB, but rather TLIF.
Surgical Selection Based on MSU Classification
Our study's VAS and ODI data showed that most patients were more suitable for PELD than TLIF. Traditional open TLIF may not be suitable for patients who require high spinal mobility and want to return to everyday life in a short period. Therefore, based on a comprehensive consideration of the clinical efficacy and surgical recurrence rate, our study shows that PELD surgery is recommended for patients with types 2B, 2C, and 3B. TLIF is recommended for patients with types 2A, 2AB, 3A, and 3AB. However, it is necessary to reduce strenuous activities and heavy physical labor postoperatively to prevent complications, such as screw loosening and adjacent segment disease.
Strengths and Limitations
This study is the first to study the clinical efficacy of PELD and TLIF surgery through MSU classification, providing certain insights for clinicians to treat this type of LDH and providing a scientific basis for patients to develop personalized treatment plans. But there are some limitations that must be acknowledged. First, we comprehensively sorted the imaging data and found that grade 1 herniations were treated with physical and drug treatments. Therefore, grade 1 herniations were not included in this study. Second, the clinical results are preliminary and needs to be verified in future larger‐scale randomized controlled trials.
Conclusion
Based on our findings, both PELD and TLIF may relieve LDH. MSU classification has specific guiding significance. It can be used for the surgical selection of PELD and TLIF to obtain the best treatment results in patients with lumbar disc herniation. However, further prospective studies exploring all spinal surgical modalities and guiding clinical decision making are essential.
Conflict of Interest Statement
The authors report no conflicts of interest.
Ethics Statement
This study was conducted in accordance with the principles of the Declaration of Helsinki. This study was approved by the Ethics Committee of the Southwest Medical University (BY2024015).
Author Contributions
Hongtao Li, Changming Xiao, and Hongyu Pan are co‐first authors who contributed equally to this study. The study was designed by Hongtao Li. Data collection was conducted by Hongtao Li, Changming Xiao, and Hongyu Pan. Data interpretation was carried out by Haomiao Yang, Haozhong Wang, and Yang Lei. Literature search was performed by all authors. Funding support was provided by Sen Li. Finally, all authors have read and approved the final manuscript.
Funding Information
This study was supported by the Nanjing Drum Tower Hospital Talent Introduction Research Initiation Fund (grant no. RC2023‐040).
Hongtao Li, Changming Xiao, and Hongyu Pan are co‐first authors who contributed equally to this study. All the authors have read and approved the final manuscript.
References
- 1. Zhang AS, Xu A, Ansari K, Hardacker K, Anderson G, Alsoof D, et al. Lumbar disc herniation: diagnosis and management. Am J Med. 2023;136(7):645–651. 10.1016/j.amjmed.2023.03.024 [DOI] [PubMed] [Google Scholar]
- 2. Al Qaraghli MI, De Jesus O. Lumbar disc herniation. StatPearls. Treasure Island, FL: StatPearls Publishing; 2023. [PubMed] [Google Scholar]
- 3. Lew SM, Mehalic TF, Fagone KL. Transforaminal percutaneous endoscopic discectomy in the treatment of far‐lateral and foraminal lumbar disc herniations. J Neurosurg. 2001;94(2 Suppl):216–220. 10.3171/spi.2001.94.2.0216 [DOI] [PubMed] [Google Scholar]
- 4. Kang TW, Park SY, Oh H, Lee SH, Park JH, Suh SW. Risk of reoperation and infection after percutaneous endoscopic lumbar discectomy and open lumbar discectomy: a nationwide population‐based study. Bone Joint J. 2021;103‐B(8):1392–1399. 10.1302/0301-620X.103B8.BJJ-2020-2541.R2 [DOI] [PubMed] [Google Scholar]
- 5. Mooney J, Laskay N, Erickson N, Salehani A, Mahavadi A, Ilyas A, et al. General vs local anesthesia for percutaneous endoscopic lumbar discectomy (PELD): a systematic review and meta‐analysis. Global Spine J. 2023;13(6):1671–1688. 10.1177/21925682221147868 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Li Z, Tang J, Hou S, Ren D, Li L, Lu X, et al. Four‐year follow‐up results of transforaminal lumbar interbody fusion as revision surgery for recurrent lumbar disc herniation after conventional discectomy. J Clin Neurosci. 2015;22(2):331–337. [DOI] [PubMed] [Google Scholar]
- 7. Sousa JM, Ribeiro H, Silva JL, Nogueira P, Consciência JG. Clinical outcomes, complications and fusion rates in endoscopic assisted intraforaminal lumbar interbody fusion (iLIF) versus minimally invasive transforaminal lumbar interbody fusion (MI‐TLIF): systematic review and meta‐analysis. Sci Rep. 2022;12(1):2101. 10.1038/s41598-022-05988-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Patel J, Kundnani V, Raut S, Meena M, Ruparel S. Perioperative complications of minimally invasive transforaminal lumbar interbody fusion (MI‐TLIF): 10 years of experience with MI‐TLIF. Global Spine J. 2021;11(5):733–739. 10.1177/2192568220941460 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Mysliwiec LW, Cholewicki J, Winkelpleck MD, Eis GP. MSU classification for herniated lumbar discs on MRI: toward developing objective criteria for surgical selection. Eur Spine J. 2010;19(7):1087–1093. 10.1007/s00586-009-1274-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Hosseini B, Taheri M, Sheibani K. Comparing the results of intradiscal ozone injection to treat different types of intervertebral disc herniation based on MSU classification. Interv Neuroradiol. 2019;25(1):111–116. 10.1177/1591019918800458 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Kaliya‐Perumal AK, Luo CA, Yeh YC, Tsai YF, Chen MJW, Tsai TT. Reliability of the Michigan State University (MSU) classification of lumbar disc herniation. Acta Ortop Bras. 2018;26(6):411–414. 10.1590/1413-785220182606201444 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Faiz KW. VAS–visual analog scale. Tidsskr nor Laegeforen. 2014;134(3):323. 10.4045/tidsskr.13.1145 [DOI] [PubMed] [Google Scholar]
- 13. Fairbank JC, Pynsent PB. The oswestry disability index. Spine (Phila Pa 1976). 2000;25(22):2940–2952; discussion 2952. 10.1097/00007632-200011150-00017 [DOI] [PubMed] [Google Scholar]
- 14. Wang H, Yuan H, Yu H, Li C, Zhou Y, Xiang L. Percutaneous endoscopic lumbar discectomy using a double‐cannula guide tube for large lumbar disc herniation. Orthop Surg. 2022;14(7):1385–1394. 10.1111/os.13313 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Mayer HM, Brock M. Percutaneous endoscopic lumbar discectomy (PELD). Neurosurg Rev. 1993;16(2):115–120. 10.1007/BF00258242 [DOI] [PubMed] [Google Scholar]
- 16. Li H, Jiang C, Mu X, Lan W, Zhou Y, Li C. Comparison of MED and PELD in the treatment of adolescent lumbar disc herniation: a 5‐year retrospective follow‐up. World Neurosurg. 2018;112:e255–e260. 10.1016/j.wneu.2018.01.030 [DOI] [PubMed] [Google Scholar]
- 17. Li B, Wang TH, Huang Y, Fan YM, Yu H, Li AQ, et al. Correlation between disc imaging observations and clinical efficacy after percutaneous endoscopic lumbar discectomy: a 1‐year follow‐up study. Orthop Surg. 2024;16:851–863. 10.1111/os.14013 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Luo M, Wang Z, Zhou B, Yang G, Shi Y, Chen J, et al. Risk factors for lumbar disc herniation recurrence after percutaneous endoscopic lumbar discectomy: a meta‐analysis of 58 cohort studies. Neurosurg Rev. 2023;46(1):159. 10.1007/s10143-023-02041-0 [DOI] [PubMed] [Google Scholar]
- 19. Prabhu MC, Jacob KC, Patel MR, Pawlowski H, Vanjani NN, Singh K. History and evolution of the minimally invasive transforaminal lumbar interbody fusion. Neurospine. 2022;19(3):479–491. 10.14245/ns.2244122.061 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Harms J, Rolinger H. A one‐stager procedure in operative treatment of spondylolistheses: dorsal traction‐reposition and anterior fusion (author's transl). Z Orthop Ihre Grenzgeb. 1982;120(3):343–347. 10.1055/s-2008-1051624 [DOI] [PubMed] [Google Scholar]
- 21. Ge DH, Stekas ND, Varlotta CG, Fischer CR, Petrizzo A, Protopsaltis TS, et al. Comparative analysis of two transforaminal lumbar interbody fusion techniques: open TLIF versus Wiltse MIS TLIF. Spine (Phila Pa 1976). 2019;44(9):E555–E560. 10.1097/BRS.0000000000002903 [DOI] [PubMed] [Google Scholar]
- 22. Lin CH, Huang YH, Lien FC, Wu CY, Chao LY. Percutaneous endoscopic lumbar discectomy versus open lumbar microdiscectomy for treating lumbar disc herniation: using the survival analysis. Tzu Chi Med J. 2023;35(3):237–241. 10.4103/tcmj.tcmj_262_22 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Li YW, Wang HJ, Wang YS, Cui W, Zhou P, Li C. Comparison of percutaneous endoscopic lumbar discectomy versus transforaminal lumbar interbody fusion in treating upper lumbar disc herniation. Zhonghua Yi Xue za Zhi. 2018;98(2):113–116. [DOI] [PubMed] [Google Scholar]
- 24. Hammad A, Wirries A, Ardeshiri A, Nikiforov O, Geiger F. Open versus minimally invasive TLIF: literature review and meta‐analysis. J Orthop Surg Res. 2019;14(1):229. 10.1186/s13018-019-1266-y [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Xue J, Song Y, Liu H, Liu L, Li T, Gong Q. Minimally invasive versus open transforaminal lumbar interbody fusion for single segmental lumbar disc herniation: a meta‐analysis. J Back Musculoskelet Rehabil. 2021;35:505–516. 10.3233/BMR-210004 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Cao J, Huang W, Wu T, Jia JY, Cheng X. Percutaneous endoscopic lumbar discectomy for lumbar disc herniation as day surgery‐short‐term clinical results of 235 consecutive cases. Medicine (Baltimore). 2019;98(49):e18064. 10.1097/MD.0000000000018064 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Dave BR, Marathe N, Mayi S, Degulmadi D, Rai RR, Patil S, et al. Does conventional open TLIF cause more muscle injury when compared to minimally invasive TLIF?‐a prospective single center analysis. Global Spine J. 2024;14(1):93–100. 10.1177/21925682221095467 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Wong AP, Smith ZA, Stadler JA, Hu XY, Yan JZ, Li XF, et al. Minimally invasive transforaminal lumbar interbody fusion (MI‐TLIF): surgical technique, long‐term 4‐year prospective outcomes, and complications compared with an open TLIF cohort. Neurosurg Clin N Am. 2014;25(2):279–304. 10.1016/j.nec.2013.12.007 [DOI] [PubMed] [Google Scholar]


