Abstract
This study aimed to investigate the change in diet quality in addition to dietary adherence to the planetary health diet during night shifts in healthcare workers. This observational follow-up study involved 450 healthcare workers working night shifts (327 females, 123 males). A survey form requesting sociodemographic information (gender, age, marital status), job title, sleeping duration during the night shift, 24 h dietary records for pre-night-shift, during night shift, and post-night-shift, and anthropometric measurements (body weight and height) was applied. The scores of the Planetary Health Diet Index (PHDI) and the Healthy Eating Index 2020 (HEI-2020) were calculated according to the dietary records. The total HEI-2020 and PHDI scores decreased significantly (p < 0.05) during the night shift (44.0 ± 8.8 and 48.3 ± 13.2, respectively) compared to pre-night-shift (46.1 ± 9.2 and 51.9 ± 13.4, respectively) and increased post-night-shift (44.7 ± 9.9 and 50.6 ± 14.9, respectively), with no statistically significant difference between pre- and post-night-shift. There was a significant main effect of night shift working on total PHDI (F(896, 2) = 8.208, p < 0.001, ηp2 = 0.018) and HEI-2020 scores (F(894, 2) = 6.277, p = 0.002, ηp2 = 0.014). Despite healthcare workers’ knowledge of health factors, night shifts lead to poor dietary choices. To improve diet quality and sustainability, it is crucial to enhance access to healthy food options in their work environment.
Keywords: healthcare workers, sustainable nutrition, diet quality, night shift
1. Introduction
Healthcare workers make up one-third of shift workers, while nurses represent the largest group [1]. Shift work schedules are required for individuals to access healthcare services 24 h a day. Almost a quarter of healthcare workers regularly work night shifts [2]. The well-being of healthcare professionals directly affects the health of the patients who need their care. Although practices related to the safety and health of patients come to the fore in healthcare institutions, the safety and health of healthcare professionals should also be supported at the same rate. A natural connection has been reported between the healthcare professional workforce and basic self-care activities (e.g., physical activity, diet quality). In healthcare workers who experience high levels of stress and fatigue, sleep quantity/quality, diet quality, and physical activity cannot reach the desired levels, and this may threaten health [3,4].
Although health professionals have advanced health knowledge, they have difficulty in implementing health-promoting behaviors recommended at the national/international level. The main reasons for this are long working hours and shift work (especially night shift work). These harmful working conditions increase the risk of physiological and psychological disorders. Shift work mainly changes the diet undesirably [5]. When working the night shift, food intake differs from day to night. Night shift workers have a higher meal frequency and lower diet quality than day shift workers [6,7]. As a first step to ensuring the implementation of targeted wellness strategies, it is critical to determine changes in nutrition as well as sleep and physical activity assessments under extended hours and night shift working conditions. The average diet quality of nurses working night shifts is low. Nurses working the night shift need resources to support diet quality to reduce the adverse effects caused by working conditions [8]. Additionally, fatty and salty foods were found to be negatively associated with diet quality in female nurses working night shifts [2]. Attention is drawn to the importance of intervention studies on meal timing and diet quality of healthcare workers working shifts [9].
Global changes in nutrition are associated with intensive production methods that contribute to environmental degradation (greenhouse gas emissions, land use change, land degradation, water pollution, etc.) while causing an increase in non-communicable chronic diseases. The Planetary Health Diet Index (PHDI) was developed to measure compliance with dietary evidence established by the EAT-Lancet Commission. It has been reported that nutritional adequacy in terms of vitamins, fiber, and minerals will be increased by changing diets according to EAT-Lancet recommendations. The need for policy action to support healthier and more-sustainable diets worldwide has been highlighted [10]. It is thought that evaluating the compliance of healthcare professionals, who are pioneers in protecting and improving public health, with the planetary health diet and revealing the current situation will contribute to filling the gap in the literature.
To our knowledge, no study has been found that evaluates the differences in healthcare workers’ diet quality and planetary health diet compliance by following up throughout the periods of pre-night-shift, during, and post-night-shift. Therefore, this study aimed to investigate the change in diet quality and dietary adherence to the planetary health diet during night shifts in healthcare workers.
2. Materials and Methods
2.1. Participants and Study Design
This study was conducted as a prospective observational follow-up study with the voluntary participation of 450 nurses, doctors, emergency medical technicians, and ambulance care technicians working in private, university, and state hospitals and private health institutions in Ankara, the capital of Turkey. The study was conducted between June 2023 and January 2024. Criteria for inclusion of healthcare professionals in the study were: being between the ages of 20 and 40 years, not having a disease that affects food consumption (situations that limit the consumption of various foods, such as lactose intolerance and celiac), not being a vegetarian or vegan, not being on a weight loss diet, not having any food allergies, not being pregnant or breastfeeding, and working shifts for at least a year. Individuals (n = 22) who started working the day shift instead of the night shift, who did not provide 24 h dietary records, or who lost communication during the study period were excluded from the study.
Healthcare workers’ shift working patterns were 24 h a day, from 08:00 a.m. to 08:00 a.m. the next day. The data obtained in this period were evaluated as “during night shift” in this article. The working schedule of healthcare professionals was 24 h work/24–48 h off. In the article, the day before the 24 h working day was expressed as the “pre-night-shift” (off day). The day after a 24 h working day was defined as the “post-night-shift” (off day). The healthcare workers were followed up for three days: pre-night-shift, during night shift, and post-night-shift.
Ethical approval was obtained from the Ethical Committee of Gazi University (Date: 16 April 2024, No: 2023-851-07). In addition, written informed consent was obtained from the participants in the study. This research was carried out following the Declaration of Helsinki.
2.2. Data Collection Tools
In this study, a survey form requesting sociodemographic information (gender, age, marital status), job title, sleeping duration during the night shift, and 24 h dietary records pre-night-shift, during night shift and post-night-shift was applied by the researchers via a face-to-face interview method. The participants’ body weight and height were measured using a BC 532 Innerscan scale (Tanita Corporation, Tokyo, Japan) and stadiometer, respectively. Body mass index (BMI) was calculated as body weight in kilograms divided by the square of the height in meters (kg/m2) and categorized [11].
The researchers conducted a nutritional assessment by collecting 24 h dietary records from all participants for three days including “pre-”, “during” and “post-night-shift”. Participants were instructed to log everything they consumed, including foods, beverages, sauces, and condiments. In addition, the mealtimes were recorded, and information was obtained about which meal they consumed that food in. The healthcare workers prepared and brought in the meals they consumed during the night shift from home or obtained them from places such as canteens and cafeterias at work. Individuals self-declared the ingredients of the meals they prepared while keeping 24 h dietary records. However, the ingredients that went into the ready-made meals they purchased from places such as canteens and cafeterias were obtained through the Standard Food Recipes book [12]. The collected data were then analyzed for total energy and nutrient intake using the BeBiS program, version 7.2.
2.3. Instruments to Evaluate Diet Quality and Sustainability
The United States Department of Agriculture (USDA) developed the Healthy Eating Index (HEI) in 1995 based on the American Dietary Guidelines [13]. This index was updated in 2005, 2010, and 2015. The components and standards of the HEI-2015 remained unchanged in the HEI-2020. The HEI-2020 retains the same 13 components and scoring standards as the HEI-2015, despite being renamed to reflect its alignment with the 2020–2025 Dietary Guidelines for Americans.
The HEI-2020, utilized in this study, includes 13 components: nine that should be consumed in adequate amounts and four that should be consumed in moderation. The nine desired components are total fruit, whole fruit, total vegetables, green leafy vegetables and fresh legumes, whole grains, dairy products, protein foods, seafood and plant-based proteins, and fatty acids. The four components to be limited are refined grains, sodium, added sugars, and saturated fats. Each component in the index is scored between 0 and 5 or 0 and 10, with low scores indicating poor nutrition and high scores indicating good nutrition [14].
The Planetary Health Diet Index (PHDI) was created by Cacau et al. (2021) based on the dietary recommendations from the EAT-Lancet Commission [15]. The index scores range from 10 to 5 points per component, with a total possible score of 0–150. Sixteen diet components are assessed using food records. The components and their maximum points are: red meat (10 points), nuts and peanuts (10 points), legumes (10 points), chicken and its substitutes (10 points), fish and seafood (10 points), eggs (10 points), fruit (10 points), vegetables (10 points), the ratio of dark green leafy vegetables to other vegetables (5 points), the ratio of red vegetables to other vegetables (5 points), whole grains (10 points), milk and its products (10 points), unsaturated fats (10 points), animal fats (10 points), and added sugars (10 points).
2.4. Physical Activity Assessment
Healthcare workers’ physical activity adequacies were evaluated using the Brief Physical Activity Assessment Tool developed by Marshall et al. (2005) [16]. The assessment includes two questions: one about the frequency and duration of vigorous-intensity physical activity, and the other about the frequency and duration of moderate-intensity activities (including walking) performed in a typical week. A scoring algorithm combines the responses to these questions to determine if individuals are classified as “adequately active”.
2.5. Statistical Analysis
Continuous variables were presented as the arithmetic mean with standard deviation, while categorical variables were shown as percentages. The HEI-2020 and PHDI total scores were categorized according to descriptive characteristics, including gender, age group, BMI group, marital status, job title, sleeping status during the night shift, and physical activity adequacy, and the changes between pre-, during and post-night-shift were compared using repeated-measures ANOVA (Table 1). If there was a significant difference in the repeated-measures ANOVA test, Tukey’s post-hoc test was used for pairwise comparisons of the parameters. Changes in the HEI-2020 and PHDI total scores and subcomponent scores between pre-, during, and post-night-shift were compared using repeated-measures ANOVA (Table 2). Tukey’s post-hoc test was used for pairwise comparisons of the parameters. The effects of individuals’ night shift changes (pre-, during, and post-) and, the interactions of the night shift changes with gender, age groups, BMI groups, marital status, branch of work, sleeping status during the night shift, and physical activity on the total PHDI and HEI-2020 scores were analyzed using two-way between-subjects ANOVA (Table 3). The results were interpreted with 95% confidence. Statistical analysis was conducted using IBM SPSS Statistics version 28.0.1.0, with significance determined at p < 0.05.
Table 1.
Descriptive characteristics of the health workers.
| Variables | Percentages n (%) |
Total PHDI Score (Mean ± SD) | Total HEI-2020 Score (Mean ± SD) | ||||
|---|---|---|---|---|---|---|---|
| Pre-Night-Shift | During Night Shift | Post-Night-Shift | Pre-Night-Shift | During Night Shift | Post-Night-Shift | ||
| Gender | |||||||
| Female | 327 (72.7) | 51.9 ± 13.4 a | 48.2 ± 13.8 b | 50.8 ± 14.9 a | 46.6 ± 9.4 a | 43.8 ± 8.8 b | 44.6 ± 10.2 b |
| F = 10,730.176; p < 0.001; η2 = 0.971 | F = 8034.557; p < 0.001; η2 = 0.985 | ||||||
| Male | 123 (27.3) | 51.9 ± 13.3 a | 48.8 ± 11.7 b | 50.8 ± 14.9 a,b | 44.7 ± 8.4 | 44.6 ± 8.6 | 45.0 ± 8.9 |
| F = 5049.914; p < 0.001; η2 = 0.976 | F = 18,506.432; p = 0.170; η2 = 0.014 | ||||||
| Age group (years) | |||||||
| 20–25 | 122 (27.1) | 49.3 ± 14.1 a | 45.5 ± 12.9 b | 46.2 ± 14.5 a,b | 45.6 ± 9.6 a | 43.4 ± 8.4 b | 42.7 ± 9.9 b |
| F = 3830.169; p < 0.001; η2 = 0.969 | F = 6830.632; p < 0.001; η2 = 0.983 | ||||||
| 26–30 | 188 (41.8) | 52.5 ± 13.2 a | 49.7 ± 13.1 b | 51.7 ± 14.9 a,b | 45.9 ± 9.1 a,b | 44.4 ± 8.6 b | 46.1 ± 9.9 a |
| F = 6845.947; p < 0.001; η2 = 0.973 | F = 10,859.282; p < 0.001; η2 = 0.983 | ||||||
| 31–40 | 140 (31.1) | 53.4 ± 12.8 a | 48.9 ± 13.5 b | 52.9 ± 14.5 a | 46.7 ± 8.8 a | 44.1 ± 9.4 b | 44.7 ± 9.6 b |
| F = 5937.575; p < 0.001; η2 = 0.977 | F = 9026.722; p < 0.001; η2 = 0.985 | ||||||
| BMI (kg/m2) | |||||||
| Normal weight | 288 (64.0) | 51.5 ± 13.3 a | 48.4 ± 13.3 b | 51.2 ± 15.4 a | 46.3 ± 9.5 a | 44.5 ± 8.5 b | 45.2 ± 9.9 a |
| F = 4.642; p = 0.010; η2 = 0.016 | F = 3.407; p = 0.034; η2 = 0.012 | ||||||
| Overweight | 135 (30.0) | 51.7 ± 13.2 a | 47.8 ± 13.5 b | 49.4 ± 13.9 b | 45.1 ± 8.4 a | 43.4 ± 9.2 b | 43.7 ± 9.8 b |
| F = 3.057; p = 0.049; η2 = 0.022 | F = 1.549; p = 0.011; η2 = 0.011 | ||||||
| Obese | 27 (6.0) | 56.8 ± 13.7 | 50.5 ± 11.6 | 50.4 ± 13.7 | 48.8 ± 8.8 | 43.8 ± 9.3 | 45.5 ± 10.1 |
| F = 2.631; p = 0.082; η2 = 0.092 | F = 2.147; p = 0.127; η2 = 0.076 | ||||||
| Marital status | |||||||
| Married | 200 (44.4) | 53.1 ± 12.8 a | 49.4 ± 12.9 b | 51.7 ± 14.6 a,b | 46.7 ± 8.6 a | 44.6 ± 9.2 b | 45.6 ± 9.7 a,b |
| F = 8042.590; p < 0.001; η2 = 0.976 | F = 13,786.891; p < 0.001; η2 = 0.986 | ||||||
| Single | 250 (55.6) | 50.9 ± 13.8 a | 47.5 ± 13.5 b | 49.7 ± 15.1 b | 45.6 ± 9.6 a | 43.6 ± 8.4 b | 44.1 ± 9.9 a,b |
| F = 7959.767; p < 0.001; η2 = 0.970 | F = 13,266.537; p < 0.001; η2 = 0.982 | ||||||
| Job title | |||||||
| Nurse | 267 (59.3) | 50.2 ± 13.5 a | 46.6 ± 12.9 b | 49.1 ± 15.6 b | 46.5 ± 9.0 a | 44.7 ± 8.6 b | 44.6 ± 10.3 b |
| F = 8425.803; p < 0.001; η2 = 0.969 | F = 14,954.402; p < 0.001; η2 = 0.983 | ||||||
| Doctor | 36 (8.0) | 50.5 ± 13.2 a | 46.3 ± 12.9 b | 52.6 ± 14 a | 45.6 ± 9.6 a | 44.9 ± 7.7 b | 48.9 ± 9.6 a |
| F = 1694.439; p < 0.001; η2 = 0.980 | F = 2088.182; p < 0.001; η2 = 0.984 | ||||||
| Emergency medical technician | 100 (22.2) | 54.5 ± 12.8 a | 49.7 ± 12.4 b | 51.6 ± 12.4 a,b | 45.4 ± 9.4 a | 42.1 ± 8.4 b | 44.1 ± 9.4 a,b |
| F = 4620.098; p < 0.001; η2 = 0.979 | F = 7232.001; p < 0.001; η2 = 0.987 | ||||||
| Ambulance care technician | 47 (10.4) | 57.0 ± 12.1 | 56.5 ± 14.2 | 55.6 ± 14.7 | 45.7 ± 9.2 | 43.8 ± 10.5 | 43.9 ± 7.9 |
| F = 2685.913; p = 0.881; η2 = 0.003 | F = 2789.670; p = 0.489; η2 = 0.015 | ||||||
| Sleeping during night shift | |||||||
| Not sleeping | 118 (26.2) | 47.1 ± 11.9 a | 43.9 ± 13.4 b | 46.3 ± 13.3 a,b | 44.9 ± 8.6 a | 42.8 ± 7.6 b | 43.4 ± 9.3 a,b |
| F = 4145.019; p < 0.001; η2 = 0.973 | F = 8357.545; p < 0.001; η2 = 0.986 | ||||||
| 0–2 h sleep | 332 (73.8) | 53.6 ± 13.4 a | 49.9 ± 13.4 b | 52.1 ± 15.1 a | 46.5 ± 9.3 a | 44.5 ± 9.1 b | 45.2 ± 10.1 a,b |
| F = 13,167.330; p < 0.001; η2 = 0.975 | F = 18,804.628; p < 0.001; η2 = 0.983 | ||||||
| Physical activity status | |||||||
| Inadequate | 170 (37.8) | 48.9 ± 13.1 a | 45.8 ± 12.5 b | 48.1 ± 15.3 a,b | 46.7 ± 8.8 | 45.7 ± 8.4 | 45.1 ± 9.9 |
| F = 10,383.005; p < 0.001; η2 = 0.974 | F = 9883.626; p = 0.189; η2 = 0.010 | ||||||
| Adequate | 280 (62.2) | 53.7 ± 13.2 a | 49.9 ± 13.5 b | 52.1 ± 14.4 a | 45.7 ± 9.3 a | 43.0 ± 8.9 b | 44.5 ± 9.9 a,b |
| F = 6230.596; p < 0.001; η2 = 0.974 | F = 16,912.648; p < 0.001; η2 = 0.984 | ||||||
a,b represent the statistically significant differences among the line groups at p < 0.05. BMI: body mass index; HEI: Healthy Eating Index; SD: standard deviation; PHDI: Planetary Health Diet Index.
Table 2.
Diet quality and sustainable nutrition trends of health workers pre-, during and post-night-shifts according to the HEI-2020 and PHDI.
| Indices and Their Components | F | p | η2 | |||
|---|---|---|---|---|---|---|
| HEI-2020 score | 46.1 ± 9.2 a | 44.0 ± 8.8 b | 44.7 ± 9.9 a | 6.277 | 0.002 | 0.014 |
| HEI-2020 components scores [] | ||||||
| Whole grains | 0.8 ± 2.5 a | 0.5 ± 1.9 b | 0.7 ± 2.3 b | 3.633 | 0.027 | 0.008 |
| Refined grains | 7.6 ± 2.9 | 7.2 ± 2.9 | 7.3 ± 3.3 | 2.676 | 0.069 | 0.006 |
| Seafood and plant proteins | 4.9 ± 0.7 a | 4.9 ± 0.5 a | 4.8 ± 0.9 b | 5.626 | 0.006 | 0.012 |
| Sodium | 9.4 ± 1.9 a | 6.7 ± 1.3 b | 9.4 ± 1.9 a | 4.428 | 0.014 | 0.010 |
| Dairy | 3.2 ± 2.1 | 3.1 ± 2.0 | 3.4 ± 2.7 | 1.895 | 0.153 | 0.004 |
| Greens and beans | 3.5 ± 1.7 a | 3.5 ± 1.6 a | 3.2 ± 1.8 b | 5.796 | 0.003 | 0.013 |
| Total vegetable | 3.2 ± 1.5 | 3.2 ± 1.4 | 3.1 ± 1.6 | 0.348 | 0.706 | 0.001 |
| Whole fruit | 3.5 ± 1.9 a | 2.1 ± 1.7 b | 2.4 ± 2.0 a | 6.568 | 0.001 | 0.014 |
| Total fruit | 1.7 ± 1.6 a | 1.3 ± 1.2 b | 1.7 ± 1.7 a | 10.502 | <0.001 | 0.023 |
| Added sugar | 4.9 ± 4.6 a | 4.1 ± 4.5 b | 4.6 ± 4.7 a | 4.662 | 0.010 | 0.010 |
| MUFA/PUFA ratio | 0.1 ± 0.6 b | 0.1 ± 0.5 b | 0.2 ± 1.3 a | 5.001 | 0.014 | 0.011 |
| Saturated fatty acids | 0.0 ± 0.0 | 0.0 ± 0.0 | 0.1 ± 0.4 | 1.000 | 0.318 | 0.002 |
| PHDI score [] | 51.9 ± 13.4 a | 48.3 ± 13.2 b | 50.6 ± 14.9 a | 8.208 | <0.001 | 0.018 |
| PHDI components scores [] | ||||||
| Red meat | 1.5 ± 3.5 a | 0.6 ± 2.3 b | 2.3 ± 4.1 c | 27.081 | <0.001 | 0.057 |
| Nuts and peanuts | 5.3 ± 4.2 a | 5.6 ± 4.2 a | 4.7 ± 4.4 b | 5.163 | 0.006 | 0.011 |
| Legumes | 3.2 ± 3.8 b | 3.5 ± 3.8 a | 2.7 ± 3.8 b | 4.332 | 0.013 | 0.010 |
| Chicken and substitutes | 7.7 ± 4.2 a | 6.6 ± 4.7 b | 8.0 ± 3.9 a | 13.943 | <0.001 | 0.030 |
| Fish and seafood | 0.0 ± 0.0 | 0.0 ± 0.0 | 0.1 ± 0.1 | 0.640 | 0.491 | 0.001 |
| Eggs | 0.4 ± 1.5 a | 0.9 ± 2.4 b | 2.9 ± 3.7 a | 106.921 | <0.001 | 0.192 |
| Fruits | 6.9 ± 3.7 | 6.4 ± 3.6 | 6.4 ± 3.9 | 2.4560 | 0.086 | 0.005 |
| Vegetables | 6.7 ± 2.5 a | 8.7 ± 2.5 a | 8.3 ± 3.0 b | 3.469 | 0.033 | 0.008 |
| DGV/total ratio | 0.5 ± 0.3 | 0.4 ± 0.3 | 0.4 ± 0.3 | 0.056 | 0.944 | 0.000 |
| ReV/total ratio | 0.8 ± 0.3 a | 0.9 ± 0.3 b | 0.8 ± 0.4 b | 6.928 | 0.001 | 0.015 |
| Whole cereals | 0.7 ± 1.8 a | 0.4 ± 0.3 b | 0.6 ± 0.3 a,b | 3.633 | 0.027 | 0.008 |
| Tubers and potatoes | 0.3 ± 0.1 | 0.4 ± 0.1 | 0.5 ± 0.8 | 1.907 | 0.150 | 0.004 |
| Dairy | 2.7 ± 0.3 a | 2.9 ± 0.4 a | 2.3 ± 0.3 b | 4.613 | 0.010 | 0.010 |
| Vegetable oils | 3.9 ± 0.6 a | 3.2 ± 0.7 b | 3.1 ± 0.4 b | 6.853 | 0.001 | 0.015 |
| Animal fats | 5.1 ± 0.9 a | 4.6 ± 0.4 b | 5.7 ± 0.9 c | 7.822 | 0.001 | 0.017 |
| Added sugar | 4.3 ± 0.6 a | 3.4 ± 0.4 b | 4.1 ± 0.6 a | 5.706 | 0.003 | 0.013 |
a,b,c represent the statistically significant differences among the line groups at p < 0.05. DGV: dark green vegetables; HEI: Healthy Eating Index; MUFA: mono unsaturated fatty acids; SD: standard deviation; PHDI: Planetary Health Diet Index; PUFA: polyunsaturated fatty acids; ReV: red vegetables.
Table 3.
Healthy Eating Index 2020 and Planetary Health Diet Index total score differences according to interactions of the night shift working with descriptive variables.
| Variables | SS | df | MS | F | p | ηp2 |
|---|---|---|---|---|---|---|
| PHDI total scores | ||||||
| Night shift working | 2933.499 | 2 | 1466.750 | 8.208 | <0.001 | 0.018 |
| Night shift working * Gender | 16.190 | 2 | 8.095 | 0.045 | 0.956 | 0.000 |
| Night shift working * Age group | 513.499 | 4 | 128.375 | 0.717 | 0.580 | 0.003 |
| Night shift working * BMI group | 581.021 | 4 | 145.255 | 0.812 | 0.517 | 0.004 |
| Night shift working * Marital status | 5.662 | 2 | 2.831 | 0.016 | 0.984 | 0.000 |
| Night shift working * Job title | 777.763 | 6 | 129.627 | 0.724 | 0.630 | 0.005 |
| Night shift working * Sleeping | 20.722 | 2 | 10.361 | 0.058 | 0.944 | 0.000 |
| Night shift working * Physical activity | 33.696 | 2 | 16.848 | 0.094 | 0.910 | 0.000 |
| HEI-2020 total scores | ||||||
| Night shift working | 975.849 | 2 | 487.924 | 6.277 | 0.002 | 0.014 |
| Night shift working * Gender | 342.720 | 2 | 171.360 | 2.210 | 0.110 | 0.005 |
| Night shift working * Age group | 425.992 | 4 | 106.498 | 1.372 | 0.242 | 0.006 |
| Night shift working * BMI group | 142.162 | 4 | 35.541 | 0.456 | 0.768 | 0.002 |
| Night shift working * Marital status | 14.640 | 2 | 7.320 | 0.094 | 0.910 | 0.000 |
| Night shift working * Job title | 604.204 | 6 | 100.701 | 1.298 | 0.255 | 0.009 |
| Night shift working * Sleeping | 6.188 | 2 | 3.094 | 0.040 | 0.961 | 0.000 |
| Night shift working * Physical activity | 236.282 | 2 | 118.141 | 1.522 | 0.219 | 0.003 |
BMI: body mass index; HEI: Healthy Eating Index; MS: mean square; SS: sum of squares; PHDI: Planetary Health Diet Index. The * symbol shows the combined interactions of the night shift changes with gender, age group, BMI group, marital status, branch of work, sleeping statues, respectively.
3. Results
The descriptive characteristics of the participants and the total PHDI and total HEI-2020 scores pre-, during and post-night-shift, categorized according to these characteristics, are shown in Table 1. It has been shown that total PHDI scores in females were lowest during the night shift (48.2 ± 13.8; p < 0.001). Total HEI-2020 scores in females were found to be significantly lower during and post-night-shift than pre-night-shift (43.8 ± 8.8; 44.6 ± 10.2; 46.6 ± 9.4, respectively; p < 0.001). There was no significant change in total HEI-2020 scores in men according to shift patterns (p > 0.05). However, it was determined that total PHDI scores in males decreased significantly during and post-night-shift (48.8 ± 11.7 and 50.8 ± 14.9, respectively) compared to pre-night-shift (51.9 ± 13.3; p < 0.001). It has been shown that the total PHDI and total HEI-2020 scores of healthcare workers according to their age groups decreased significantly during the night shift compared to pre-night-shift. Total PHDI and total HEI-2020 scores of individuals decreased during the night shift in normal-body-weight and overweight groups, and there was still a significant difference post-night-shift compared to pre-night-shift, that is, there was no increase in total PHDI and HEI-2020 scores after the shift. Similarly, it was determined that total HEI-2020 and PHDI scores decreased significantly during the night shift in single and married individuals compared to pre-night-shift (p < 0.001). When looked at according to the professions of healthcare workers, it has been shown that both total HEI-2020 and total PHDI scores decrease significantly during the night shift in nurses, doctors, and emergency medical technicians, except for ambulance maintenance technicians (p < 0.001). A decrease in total HEI-2020 and PHDI scores was detected in individuals who did not sleep during the night shift and those who slept for 2 h during the night shift, while a similar decrease was observed in those who did sufficient physical activity (p < 0.001).
The change in the mean and standard deviation values of the HEI-2020 and PHDI subcomponents of healthcare workers pre-, during and post-night-shift is shown in Table 2. It was revealed that the total HEI-2020 scores of individuals decreased significantly during the night shift (44.0 ± 8.8) compared to pre-night-shift (46.1 ± 9.2; p = 0.002) and increased post-night-shift (44.7 ± 9.9), with no statistically significant difference between pre- and post-night-shift. The change observed in subcomponent scores during the night shift compared to the pre-night-shift was similarly demonstrated in the sodium (p = 0.014), whole fruit (p = 0.001), total fruit (p < 0.001), and added sugar (p = 0.010) subcomponents. It was revealed that the total PHDI scores of individuals decreased significantly during the night shift (48.3 ± 13.2) compared to pre-night-shift (51.9 ± 13.4; p < 0.001) and increased post-night-shift (50.6 ± 14.9), with no statistically significant difference between pre- and post-night-shifts. The change observed in subcomponent scores during the night shift compared to the pre-night-shift was similarly demonstrated in the chicken and substitutes (p < 0.001), vegetable oils (p = 0.001), animal fats (p = 0.001), whole cereals (p = 0.027), and added sugar (p = 0.003) subcomponents. However, it was found that individuals’ legumes (p = 0.013), eggs (p < 0.001), and dairy (p = 0.010) PHDI subcomponent scores increased significantly during the night shift compared to pre-night-shift and decreased again post-night-shift.
The effects of individuals’ night shift changes (pre-, during, and post-night-shift) and the interactions of the night shift changes with gender, age group, BMI group, marital status, branch of work, sleeping status during the night shift, and physical activity on the total PHDI and HEI-2020 scores are shown in Table 3. There was a significant main effect of night shift working on total PHDI (F(896, 2) = 8.208, p < 0.001, ηp2 = 0.018) and HEI-2020 scores (F(894, 2) = 6.277, p = 0.002, ηp2 = 0.014). In contrast, there was no significant main effect of night-shift-working interactions with gender, age group, BMI group, marital status, branch of work, sleeping status during the night shift, and physical activity on total PHDI and HEI-2020 scores (p > 0.05).
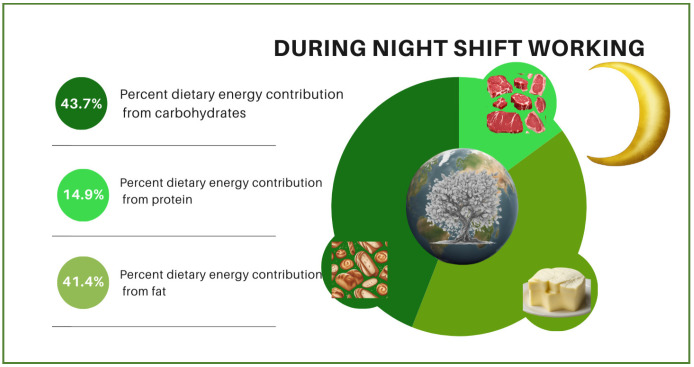
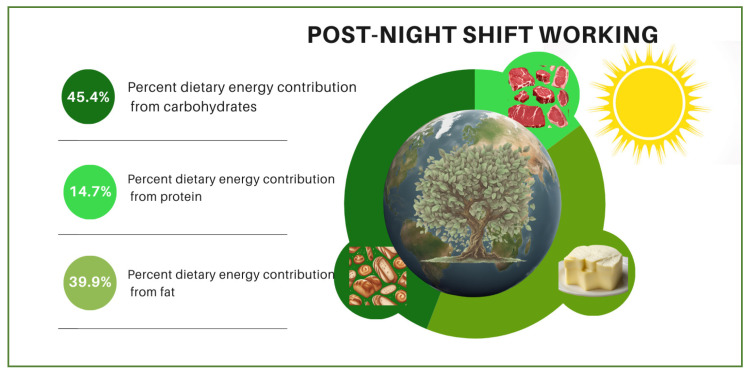
The changes in contributions of individuals’ dietary macronutrients to their dietary energy, diet quality, and diet sustainability according to whether they were pre-, during, or post-night-shift are visualized in Figure 1, Figure 2 and Figure 3. In the figures, the night shift sequence is expressed with moonlight while pre- and post-night-shift are expressed with sunlight. The size of the world map symbolizes diet quality. It is stated that the larger the world map (pre-night-shift), the higher the diet quality. Meanwhile, the smallest world map diameter indicates the lowest diet quality (during night shift) and the medium-sized world map (post-night-shift) indicates a higher diet quality than the lowest diet quality. According to the difference among the shift periods, it is symbolized that as the diameter of the world map decreases, the quality of the diet also decreases. The vibrant shades of green color on tree leaves vary depending on their dietary sustainability. The most vibrant shade of green indicates the highest diet sustainability (pre-night-shift), while paler green indicates lower diet sustainability (post-night-shift), and the palest green indicates the lowest diet sustainability (during night shift). Moreover, the proportional distributions of green colors and the world map diameter are shown for illustrative purposes only, not mathematical purposes. No significant change was observed in the contribution of individuals’ dietary protein intake to dietary energy according to whether they were pre-, during, or post-night-shifts. While the contribution of individuals’ dietary carbohydrate intake to dietary energy decreased significantly during the night shift (43.7%; p < 0.001) compared to pre-night-shift (44.4%), it increased significantly post-night-shift (45.4%; p = 0.047) and reached a level where there was no statistical difference compared with pre-night-shift (p = 0.156). While the contribution of individuals’ dietary fat intake to dietary energy increased significantly during the night shift (41.4%; p = 0.008) compared to pre-night-shift (40.7%), it decreased post-night-shift (39.9%; p < 0.001) and reached a level where there was no statistical difference compared with before the shift (p = 0.253).
Figure 1.
The contributions of individuals’ dietary macronutrients to their dietary energy, diet quality, and diet sustainability pre-night-shift.
Figure 2.
The contributions of individuals’ dietary macronutrients to their dietary energy, diet quality, and diet sustainability while working the night shift.
Figure 3.
The contributions of individuals’ dietary macronutrients to their dietary energy, diet quality, and diet sustainability post-night-shift.
4. Discussion
In this observational follow-up study conducted on healthcare workers working night shifts, it was shown that both the diet sustainability and diet quality of individuals decreased significantly during night shift working compared to before and increased again after the night shift. This change occurred regardless of the healthcare professionals’ job title, age, ability to sleep during shifts, and physical activity status.
It has been shown that the circadian rhythm disruption experienced by healthcare professionals as a result of working night shifts causes many negative health consequences, such as impaired glucose tolerance [17], decreased insulin sensitivity [18,19], obesity [20], cardiometabolic diseases [21], and cancer [22]. It was found that the health problems seen in individuals were not only caused by circadian disruptions as a result of changes in the sleep–wake cycle, but night shifts can also cause diseases by changing eating habits in an unhealthy way [20,23,24,25,26]. In order to intervene in changing eating habits during a night shift, it is necessary first to reveal the changes. In this study, which examined the diet quality and diet sustainability of the night shift in healthcare workers, a group with basic knowledge about health protection, it was shown that there were negative changes in nutritional status during the night shift. Participants’ diet quality measured using HEI-2020 and dietary sustainability measured using PHDI were found to be significantly lower during the night shift compared to pre- and post-night-shift. Similarly, it has been revealed that individuals working night shifts frequently choose unhealthy snacks as a strategy to stay awake during their shifts, and these snacks are often high in fat, sodium, and added sugar [23,27,28]. In this study, it was shown that the index scores of individuals according to their saturated fatty acid intake were low pre-, during, and post-night-shift, without any significant differences among them. Additionally, individuals’ diet quality scores from added sugar intake were shown to significantly decrease during night shifts (4.9 ± 4.6, 4.1 ± 4.5, 4.6 ± 4.7, pre-, during, and post-night-shift, respectively; p = 0.010), supporting previous studies.
In addition, when it was investigated as to how the effects of a night shift on the decrease in diet quality would change when combined with these sociodemographic data, it was shown that the night shift did not show its effects on diet quality by interacting with these sociodemographic descriptors, and that the night shift was the main influencing factor (F(894, 2) = 6.277, p = 0.002, ηp2 = 0.014, Table 3). Similar to this study, it has been revealed that food intake or eating habits change in an “unhealthy” direction [20,24,25,26,27,28,29,30,31] along the same lines as in this study conducted in healthcare workers. However, studies investigating diet quality in night shift workers are quite limited [8]. The evaluation of the HEI-2020 score and its subcomponents, which allow for comparison of the nutritional status of individuals with more objective criteria, has contributed an essential finding to the literature.
Sustainable nutrition, the importance of which has become more evident with the rapid depletion of natural resources, will be an inevitable strategy of this age, not only because of its low environmental impacts and protection of the ecosystem and biodiversity but also because it is a nutritionally adequate and healthy nutrition model [32]. This should also be recommended for night shift workers. In this way, the health of these individuals in the at-risk group working the night shift will be protected while natural resources will also be protected. Sustainable nutrition models, which will become an inevitable proposal of the age by consensus, are characterized by prominently featuring substantial quantities of plant-based foods, including vegetables, fruits, seeds, nuts, legumes, and whole grains, while incorporating only moderate-to-minimal amounts of animal-based products, such as meat, poultry, seafood, eggs, and dairy [15,32,33,34,35]. Considering the foods included in sustainable nutrition recommendations, it appears that they meet the dietary approaches recommended to improve health in individuals working night shifts. Therefore, the implementation of sustainable nutrition approaches in individuals working night shifts reduces the intake of saturated fatty acids and added sugars, which are included in unhealthy eating tendencies in this group [20,23,24,25,26], while increasing the intake of fiber, unsaturated fatty acids, fruits, and vegetables. The supporting data in this study demonstrate that sustainable diet quality decreased when healthcare workers switched to night shifts. During the night shift, healthcare workers’ sustainable diet quality scores of red meat (0.6 ± 2.3), chicken and substitutes (6.6 ± 4.7), and animal fats (4.6 ± 0.4) decreased significantly (p < 0.05) compared to pre-night-shift (1.5 ± 3.5, 7.7 ± 4.2, 5.1 ± 0.9, respectively), meaning their consumption of these foods increased significantly. The significant decrease in the consumption of these foods post-night-shift (p < 0.05), that is, the increase in the PHDI subscores (2.3 ± 4.1, 8.0 ± 3.9, 5.7 ± 0.9, respectively), strengthens the hypothesis that the changes occur only during the night shift (Table 2). Similarly, studies have shown that meat consumption increases during the night shift, and that individuals tend to eat meals containing high saturated fat, sodium, red meat, and chicken, and especially “fast” foods [29,36,37].
Studies have shown that females tend to have a higher sustainable diet quality than males and are more prone to plant-based foods [38,39,40]. For these reasons, in this study, the sustainable diet quality of females increased faster than males’ post-night-shift. It is thought that the effect of the increase in sustainable diet quality after the night shift depending on the sleeping state during the night shift is also related to the effect of sleep duration on the feeling of hunger. In individuals with less sleep time, the feeling of hunger increases, and as a result, the tendency to foods with poorer nutritional value including “fast” food increases. Studies supporting this interpretation have shown that the feeling of hunger, which causes unhealthy eating choices, is affected by sleep duration [8,41,42]. It has been shown that decreasing sleep duration affects hunger and satiety levels through the mechanism of changing plasma ghrelin and leptin levels, which are hormones that regulate appetite [8,41,42]. The increase in sustainable diet quality after a night shift in individuals with a normal body weight and adequate physical activity level has been interpreted as being related to the fact that the diet choices of individuals who make healthy lifestyle choices may also be healthy. However, when it was investigated as to how the effects of the night shift on the decrease in sustainable diet quality (total PHDI score) would change when combined with these sociodemographic data, it was shown that the night shift did not show its effects on sustainable diet quality by interacting with these sociodemographic descriptors, and that the night shift was the main influencing factor on sustainable diet quality (F(894, 2) = 6.277, p = 0.002, ηp2 = 0.014, Table 3).
One of the strengths of this study is that it evaluated night shift workers’ nutritional status by following a large sample before, during, and after the night shift. In addition, this study, in which the diet quality of the participants was calculated according to HEI-2020, has another strength due to the limited number of studies in the literature that have observed changes in diet quality by following night shift workers. Another of its strengths is that it is the first study to investigate the implementation of sustainable nutrition, which will inevitably become a healthy nutrition strategy for every individual due to today’s conditions, including night shift workers. The first limitation of this study is that since the study was conducted only in healthcare workers, the results cannot be generalized to all night shift workers. Secondly, there are limitations in generalizing the findings of the study because the factors affecting individuals’ eating habits and food preferences vary across countries and even geographical regions within the same country. Thirdly, considering that the stress experienced by healthcare workers during night shifts may affect their eating behavior, it will be important to include this parameter in future studies. Lastly, healthcare workers may encounter many emergencies during the night shift. Experiencing these emergencies may also affect individuals’ food consumption. However, in this study, no evaluation was made regarding the emergency situations encountered by healthcare workers working on night shifts, and it is recommended that future studies include this evaluation and exclude from the study periods when unusual emergencies (long surgeries, etc.) occur.
5. Conclusions
Compared to before the night shift, both the diet quality and diet sustainability of healthcare workers decreased during the night shift, without any differences according to gender, age group, BMI group, marital status, job title, and napping during the night shift. The significant increase in diet quality and diet sustainability scores again after the night shift supports the finding that the night shift is an important factor affecting these two parameters. It is thought that sustainable nutrition, which is a solution-oriented proposal of the age with its health benefits and strengths such as the protection of natural resources and low environmental impact, will be inevitable to be implemented day by day in health professionals working night shifts.
The fact that these negative dietary changes occur during the night shift, even among healthcare workers who have basic knowledge about the factors affecting the protection and promotion of health, reveals that further steps are needed than just providing information on the subject. The first of these should be to increase the chance of accessing healthy alternatives by evaluating the environment in which healthcare workers access food sources. Other suggestions include organizing break times at work by encouraging healthy eating and ensuring that workplace cafeterias and vending machines contain healthy alternatives. Ensuring that not only healthcare professionals but also managers are informed about sustainable nutrition will make it easier to accelerate the steps to be taken. Finally, it is also valuable to evaluate the nutritional knowledge levels of healthcare professionals in future studies and correlate them with diet quality and sustainable nutritional quality, and to develop suggestions for updates to be made in the undergraduate education curriculum of healthcare professionals based on the results of the research.
Author Contributions
Conceptualization, S.N.-V. and H.M.; data curation, S.N.-V.; formal analysis, H.M.; investigation, S.N.-V. and H.M.; methodology, S.N.-V. and H.M.; project administration, S.N.-V.; resources, H.M. and S.N.-V.; software, H.M.; supervision, H.M. and S.N.-V.; validation, H.M.; visualization, H.M.; writing, H.M. and S.N.-V. All authors have read and agreed to the published version of the manuscript.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki and approved by the Ethics Committee of Gazi University of Ankara/Turkey (Date: 16 April 2024, No: 2023-851-07).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data presented in this study are available on request from the corresponding author (handeyilmaz@gazi.edu.tr) due to fact that it is intended to be shared only with researchers working in this field.
Conflicts of Interest
The authors declare no conflicts of interest.
Funding Statement
This research received no external funding.
Footnotes
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content.
References
- 1.Labor Force Statistics from the Current Population Survey Work Schedules (Flexible and Shift Schedules) [(accessed on 8 June 2024)];2018 Available online: https://www.bls.gov/cps/lfcharacteristics.htm#schedules.
- 2.Rijk M.G., Vries H.H.M., Mars M., Feskens E.J.M., Boesveldt S. Dietary taste patterns and diet quality of female nurses around the night shift. Eur. J. Nutr. 2024;63:513–524. doi: 10.1007/s00394-023-03283-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Berent D., Skoneczny M., Macander M., Wojnar M. The association among health behaviors, shift work and chronic morbidity: A cross-sectional study on nurses working in full-time positions. J. Public Health Res. 2022;11:2099. doi: 10.4081/jphr.2021.2099. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Mazurek Melnyk B., Pavan Hsieh A., Tan A., Teall A.M., Weberg D., Jun J., Gawlik K., Hoying J. Associations among nurses’ mental/physical health, lifestyle behaviors, shift length, and workplace wellness support during COVID-19: Important implications for health care systems. Nurs. Adm. Q. 2022;46:5–18. doi: 10.1097/NAQ.0000000000000499. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Shaw E., Dorrian J., Coates A.M., Leung G.K.W., Davis R., Rosbotham E., Warnock R., Huggins C.E., Bonham M.P. Temporal pattern of eating in night shift workers. Chronobiol. Int. 2019;36:1613.e52. doi: 10.1080/07420528.2019.1660358. [DOI] [PubMed] [Google Scholar]
- 6.Flanagan A., Lowson E., Arber S., Griffin B.A., Skene D.J. Dietary patterns of nurses on rotational shifts are marked by redistribution of energy into the nightshift. Nutrients. 2020;12:1053. doi: 10.3390/nu12041053. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Pepłońska B., Nowak P., Trafalska E. The association between night shift work and nutrition patterns among nurses: A literature review. Medycyna Pracy. 2019;70:363–376. doi: 10.13075/mp.5893.00816. [DOI] [PubMed] [Google Scholar]
- 8.Rangel T.L., Bindler T.S.R., Roney J.K., Penders R.A., Faulkner R., Miller L., Sperry M., James L., Wilson M.L. Exercise, diet, and sleep habits of nurses working full-time during the COVID-19 pandemic: An observational study. Appl. Nurs. Res. 2023;69:151665. doi: 10.1016/j.apnr.2022.151665. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Farías R., Sepúlveda A., Chamorro R. Impact of shift work on the eating pattern, physical activity and daytime sleepiness among chilean healthcare workers. Saf. Health Work. 2020;11:367–371. doi: 10.1016/j.shaw.2020.07.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Frank S.M., Jaacks L.M., Adair L.S., Avery C.L., Meyer K., Rose D., Taillie L.S. Adherence to the Planetary Health Diet Index and correlation with nutrients of public health concern: An analysis of NHANES 2003–2018. Am. J. Clin. Nutr. 2024;119:384–392. doi: 10.1016/j.ajcnut.2023.10.018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.World Health Organization (WHO) Fact Sheets. A Healthy Lifestyle-WHO Recommendations. 2010. [(accessed on 8 June 2024)]. Available online: https://www.who.int/europe/news-room/fact-sheets/item/a-healthy-lifestyle---who-recommendations.
- 12.Merdol T.K. Standart Yemek Tarifeleri. 1st ed. Hatipoğlu Yayınevi; Ankara, Türkiye: 2011. pp. 10–200. [Google Scholar]
- 13.Kennedy E.T., Ohls J., Carlson S., Fleming K. The Healthy Eating Index: Design and applications. J. Am. Diet. Assoc. 1995;95:1103–1108. doi: 10.1016/S0002-8223(95)00300-2. [DOI] [PubMed] [Google Scholar]
- 14.Krebs-Smith S.M., Pannucci T.E., Subar A.F., Kirkpatrick S.I., Lerman J.L., Tooze J.A., Wilson M.M., Reedy J. Update of the Healthy Eating Index: HEI-2015. J. Acad. Nutr. Diet. 2018;118:1591–1602. doi: 10.1016/j.jand.2018.05.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Cacau L.T., Carli E., de Carvalho A.M., Lotufo P.A., Moreno L.A., Bensenor I.M., Marchioni D.M. Development and validation of an index based on EAT-Lancet recommendations: The planetary health diet index. Nutrients. 2021;13:1698. doi: 10.3390/nu13051698. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Marshall A.L., Smith B.J., Bauman A.E., Kaur S. Reliability and validity of a brief physical activity assessment for use by family doctors. Br. J. Sports Med. 2005;39:294–297. doi: 10.1136/bjsm.2004.013771. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Suyoto P.S.T., de Rijk M.G., de Vries J.H., Feskens E.J.M. The effect of meal glycemic index and meal frequency on glycemic control and variability in female nurses working night shifts: A two-arm randomized cross-over trial. J. Nutr. 2024;154:69–78. doi: 10.1016/j.tjnut.2023.11.025. [DOI] [PubMed] [Google Scholar]
- 18.Chellappa S.L., Qian J., Vujovic N., Morris C.J., Nedeltcheva A., Nguyen H., Rahman N., Heng S.W., Kelly L., Kerlin-Monteiro K., et al. Daytime eating prevents internal circadian misalignment and glucose intolerance in night work. Sci. Adv. 2022;7:eabg9910. doi: 10.1126/sciadv.abg9910. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Augustin L.S.A., Kendall C.W.C., Jenkins D.J.A., Willett W.C., Astrup A., Barclay A.W., Björck I., Brand-Miller J.C., Brighenti F., Buyken A.E., et al. Glycemic index, glycemic load and glycemic response: An International Scientific Consensus Summit from the International Carbohydrate Quality Consortium (ICQC) Nutr. Metab. Cardiovasc. Dis. 2015;25:795–815. doi: 10.1016/j.numecd.2015.05.005. [DOI] [PubMed] [Google Scholar]
- 20.Heath G., Dorrian J., Coates A. Associations between shift type, sleep, mood, and diet in a group of shift working nurses. Scand. J. Work Environ. Health. 2019;45:402–412. doi: 10.5271/sjweh.3803. [DOI] [PubMed] [Google Scholar]
- 21.Hannemann J., Laing A., Middleton B., Schwedhelm E., Marx N., Federici M., Kastner M., Skene D.J., Böger R. Effect of oral melatonin treatment on insulin resistance and diurnal blood pressure variability in night shift workers. A double-blind, randomized, placebo-controlled study. Pharmacol. Res. 2024;199:107011. doi: 10.1016/j.phrs.2023.107011. [DOI] [PubMed] [Google Scholar]
- 22.Moon J., Holzhausen E.A., Mun Y. Risk of prostate cancer with increasing years of night shift work: A two-stage dose-response meta-analysis with duration of night shift work as exposure dose. Heliyon. 2024;10:e29080. doi: 10.1016/j.heliyon.2024.e29080. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Habib Rodrigues G., de Sousa Duarte A., Garrido A.L.F., Santana P.T., Pellegrino P., Nogueira L.F.R., Crispim C.A., Cipolla-Neto J., de Castro Moreno C.R., Marqueze E.C. A putative association between food intake, meal timing and sleep parameters among overweight nursing professionals working night shifts. Sleep Epidemiol. 2022;2:100040. doi: 10.1016/j.sleepe.2022.100040. [DOI] [Google Scholar]
- 24.Chen Y., Lauren S., Chang B.P., Shechter A. Objective food intake in night and day shift workers: A laboratory study. Clocks Sleep. 2019;1:42–49. doi: 10.3390/clockssleep1010005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Kosmadopoulos A., Kervezee L., Boudreau P., Gonzales-Aste F., Vujovic N., Scheer F.A.J.L., Boivin D.B. Effects of shift work on the eating behavior of police officers on patrol. Nutrients. 2020;12:999. doi: 10.3390/nu12040999. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Jansen E.C., Stern D., Monge A., O’Brien L.M., Lajous M., Peterson K.E., López-Ridaura R. Healthier dietary patterns are associated with better sleep quality among mid-life Mexican women. J. Clin. Sleep Med. 2020;16:1321–1330. doi: 10.5664/jcsm.8506. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Crispim C.A., Zalcman I., Dáttilo M., Padilha H.G., Tufik S., de Mello M.T. Relação entre sono e obesidade: Uma revisão da literature. Arq. Bras. Endocrinol. Metab. 2007;51:1041–1049. doi: 10.1590/S0004-27302007000700004. [DOI] [PubMed] [Google Scholar]
- 28.Schiavo-Cardozo D., Lima M.M.O., Parej J.C., Geloneze B. Appetite-regulating hormones from the upper gut: Disrupted control of xenin and ghrelin in night workers. Clin. Endocrinol. 2013;79:807–811. doi: 10.1111/cen.12114. [DOI] [PubMed] [Google Scholar]
- 29.Balieiro L.C., Rossato L.T., Waterhouse J., Paim S.L., Mota M.C., Crispim C.A. Nutritional status and eating habits of bus drivers during the day and night. Chronobiol. Int. 2014;31:1123–1129. doi: 10.3109/07420528.2014.957299. [DOI] [PubMed] [Google Scholar]
- 30.De Freitas E.S., Canuto R., Henn R.L., Olinto B.A., Macagnan J.B.A., Pattussi M.P., Busnello F.M., Olinto M.T.A. Alteração no comportamento alimentar de trabalhadores de turnos de um frigorífico do sul do Brasil. Ciência Saúde Coletiva. 2015;20:2401–2410. doi: 10.1590/1413-81232015208.18642014. [DOI] [PubMed] [Google Scholar]
- 31.Mota M.C., De-Souza D.A., Crispim C.A. Dietary patterns, metabolic markers and subjective sleep measures in resident physicians. Chronobiol. Int. 2013;30:1032–1041. doi: 10.3109/07420528.2013.796966. [DOI] [PubMed] [Google Scholar]
- 32.Food and Agriculture Organization Bioversity International. Sustainable Diets and Biodiversity: Directions and Solutions for Policy, Research and Action. [(accessed on 27 June 2024)]. Available online: http://www.fao.org/3/i3004e/i3004e.pdf.
- 33.Fardet A., Rock E. How to protect both health and food system sustainability? A holistic ‘global health’-based approach via the 3V rule proposal. Public Health Nutr. 2020;23:3028–3044. doi: 10.1017/S136898002000227X. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Steenson S., Buttriss J.L. The challenges of defining a healthy and ‘sustainable’ diet. Nutr. Bull. 2020;45:206–222. doi: 10.1111/nbu.12439. [DOI] [Google Scholar]
- 35.Meltzer H.M., Brantsaeter A.L., Trolle E., Eneroth H., Fogelholm M., Ydersbond T.A., Birgisdottir B.E. Environmental sustainability perspectives of the nordic diet. Nutrients. 2019;11:2248. doi: 10.3390/nu11092248. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Chaves D.B.R., Costa A.G.S., Oliveira A.R.S., Olivera T.C., Araujo T.L., Lopes M.V.O. Risk factors to high blood pressure: Inquiry with bus drivers and collectors. Rev. Enferm. 2008;16:370–376. [Google Scholar]
- 37.Cavagioni L.C. Master’s Thesis. Nursing School, University of São Paulo; São Paulo, Brazil: 2008. Cardiovascular Risk Profile Observed in Professional Truck Drivers Who Work on Highway BR116 within the Area of the State of São Paulo—Régis Bittencourt. [Google Scholar]
- 38.Seffen A.E., Dohle S. What motivates German consumers to reduce their meat consumption? Identifying relevant beliefs. Appetite. 2023;187:106593. doi: 10.1016/j.appet.2023.106593. [DOI] [PubMed] [Google Scholar]
- 39.Tobler C., Visschers V.H.M., Siegrist M. Eating green Consumers’ willingness to adopt ecological food consumption behaviors. Appetite. 2011;57:674–682. doi: 10.1016/j.appet.2011.08.010. [DOI] [PubMed] [Google Scholar]
- 40.Judge M., Wilson M.S. A dual-process motivational model of attitudes towards vegetarians and vegans. Eur. J. Soc. Psychol. 2019;49:169–178. doi: 10.1002/ejsp.2386. [DOI] [Google Scholar]
- 41.McHill A.W., Hull J.T., Klerman E.B. Chronic circadian disruption and sleep restriction influence subjective hunger, appetite, and food preference. Nutrients. 2022;14:1800. doi: 10.3390/nu14091800. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Spiegel K., Tasali E., Penev P., Van Cauter E. Brief communication: Sleep curtailment in healthy young men is associated with decreased leptin levels, elevated ghrelin levels, and increased hunger and appetite. Ann. Intern. Med. 2004;141:846–850. doi: 10.7326/0003-4819-141-11-200412070-00008. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The data presented in this study are available on request from the corresponding author (handeyilmaz@gazi.edu.tr) due to fact that it is intended to be shared only with researchers working in this field.