Abstract
Background
Social determinants of health (SDoH) are increasingly recognized as crucial factors affecting the well-being of pediatric chronic kidney disease (CKD) patients. This study explores the impact of SDoH on the quality of life (QoL) of children with CKD in Saudi Arabia.
Methods
This observational, descriptive, cross-sectional study included 50 participants with CKD stages three to five, as well as children with end-stage renal disease (ESRD) undergoing peritoneal dialysis (PD) or hemodialysis (HD) in Riyadh, Saudi Arabia. Data were collected from children and their caregivers using a validated Arabic-adapted version of the Pediatric Quality of Life Inventory (PedsQL) 3.0 and an SDoH survey.
Results
The study revealed that access to education significantly affects pediatric QoL (H/Z score 2.825; P-value 0.005), and the lack of dietary recommendations was identified as a critical factor (H/Z score 1.441; P-value 0.029). ESRD patients on PD from larger families reported better QoL, whereas lower family income was associated with reduced QoL in PD patients (P-value 0.048). Compared to those in earlier stages of CKD, ESRD patients showed lower QoL (H/Z score 2.154; P-value 0.031).
Conclusion
Our study provides initial insights into the relationship between SDoH and the QoL of children with CKD in Saudi Arabia. It calls for a comprehensive approach that includes these determinants in care strategies to improve patient outcomes and QoL.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12882-024-03710-y.
Keywords: Social determinant of health, Chronic kidney disease, End stage renal disease
Background
Social determinants of health (SDoH) are the social and economic factors that influence health outcomes, including income, education, and access to healthcare. They have gained increasing recognition in recent years, particularly in the context of pediatric healthcare and the role of healthcare providers in addressing them [1]. They have been recognized by the World Health Organization and the Centers for Disease Control and Prevention (CDC) [2]. Although SDoH impacts all humans globally, they have a more pronounced effect on children [3]. Recently, the American Academy of Pediatrics endorsed screening children for SDoH at different settings [4].
SDoH have a profound influence on children with chronic kidney disease (CKD), significantly shaping disease awareness, progression, and outcomes [5]. Factors such as socioeconomic status, education, race, and gender are intricately linked with patient awareness of CKD, underscoring their pivotal role in the health disparities associated with the condition [6]. However, the intersectionality of SDoH and pediatric CKD has not been extensively explored in the Middle East, particularly in Saudi Arabia.
Evaluating quality of life (QoL) is essential for gauging their overall health and functionality. Research emphasizes the importance of health-related quality of life (QoL) surveys in assessing various QoL dimensions in young CKD sufferers. These surveys reveal deficiencies in the physical, emotional, social, and educational domains in these children [7]. QoL is also recognized as a critical marker for tracking the health and function of children with end-stage renal disease (ESRD) [8]. Issues such as fatigue, depressive symptoms, and behavioral disorders are linked to lower QoL in these patients [9].
SDoH plays a crucial role in influencing the quality of life (QoL) outcomes for children and youths with chronic diseases [10]. Specifically, children and adolescents with CKD tend to experience a lower QoL compared to their healthy peers [11]. This disparity can be exacerbated by inequities in care [12]. Inequity itself is a clear example of SDoH [13]. Even before the concept of SDoH was widely recognized, many pediatric practitioners were aware of the significant impact of CKD and its treatment regimen on the QoL of children and youths [14]. Exploring the intersectionality of SDoH, CKD, and QoL can aid in understanding this complex relationship, thereby improving the care for children with CKD both within and beyond the clinical setting.
To the best of our knowledge, no research has been conducted to investigate the impact of SDoH on the QoL in children with CKD in the Middle East, including Saudi Arabia. Our objective is to examine the impact of SDoH on the QoL of children with CKD. The findings of this study can help tailor pediatric care for children with CKD based on their SDoH to enhance their QoL. Additionally, it can shed light on how to improve equity and reduce health disparities for many children with CKD in Saudi Arabia.
Methods
Study design and setting
This observational, descriptive, cross-sectional study was conducted at a single tertiary care center in Riyadh, Saudi Arabia. The cross-sectional study design aimed to capture demographic, geographical, and clinical diversity to accurately reflect the broader population of children suffering from CKD. The study aimed to explore the association between certain SDoH and the QoL of children with CKD. The investigated SDoH included family income, transportation, food security, education, and housing stability. These were selected based on a literature review and the opinions of Saudi pediatric nephrology experts [15]. To assess QoL, a validated Arabic version of the PedsQL 3.0, tailored for each child’s age, was used.
Participant selection
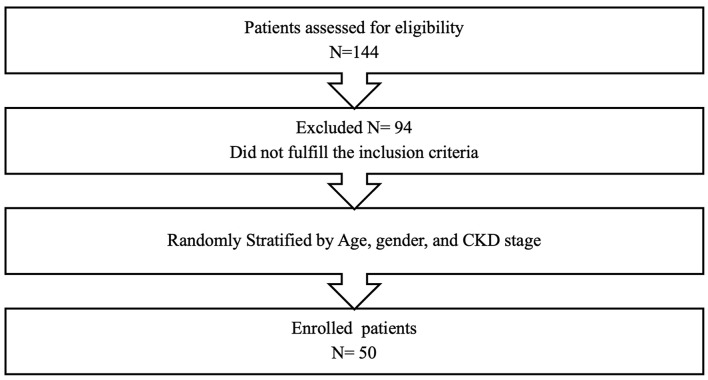
Patients were randomly selected from the CKD clinic at King Fahad Medical City in Riyadh, Saudi Arabia. The inclusion criteria were an age range of 2 to 18 years and a confirmed diagnosis of CKD at stages three, four, or five. Children with end-stage renal disease (ESRD) undergoing peritoneal dialysis (PD) or hemodialysis (HD) were also included. Another criterion was the ability of caregivers to give consent and for children older than 7 years to provide assent. The study excluded patients with comorbid conditions other than CKD. All patients were listed in an Excel sheet, and those in odd-numbered rows were selected for participation. Participants were classified into five different groups (CKD stage 3, CKD stage 4, CKD stage 5, ESRD on PD, and ESRD on HD), with groups matched by age (Fig. 1).
Fig. 1.
Flowchart of patient selection
Patients demographics and clinical data
Patient demographics, including age, sex, education level, parents’ marital status, and parents’ employment status, were collected from chart reviews. Clinical and laboratory data, such as serum creatinine, height, and weight, were also recorded. To estimate the glomerular filtration rate (eGFR), the Modified Schwartz formula [16] was used, and CKD staging was based on the criteria established by the Kidney Disease Outcomes Quality Initiative and the Kidney Disease Improving Global Outcomes (KDIGO) [17].
SDoH and QoL data collection
QoL and SDoH assessments were conducted using electronic surveys. Both surveys were self-administered, and parents completed them privately and anonymously to preserve their dignity. For parents who were illiterate or semi-literate, one of the investigators assisted in completing the surveys without collecting any identifying information.
The first survey examined SDoH through 11 questions, divided into multiple domains: education, food security, healthcare access, housing stability, transportation, and family income (supplementary material). The second survey used a validated Arabic version of PedsQL 3.0 tailored for each child’s age [18, 19]. PedsQL survey was completed by both children and their parents according to their respective age.
Social determinants of health
The socio-economic characteristics of the study participants were assessed by a parental survey consisting of 11 questions that encompassed six distinct domains. The initial category examined was the size of the family, which assessed the number of individuals residing in the household. The categories included 1–2 members, 3–4 members, or more than four people. The survey also inquired about the residence type, namely, if it was owned or rented and whether it was a house, apartment, or another sort of structure. The study also inquired about the child’s living arrangement, namely whether they resided with both parents or only one. The parents’ marital status was recorded, with possibilities including separated, divorced, both alive or deceased. Another component examined the family’s healthcare accessibility, taking into account their proximity to medical facilities and the child’s principal way of transportation to these services. The last aspect examined was the family’s financial situation, which was evaluated by inquiring about their monthly income based on the criteria established by the General Authority for Statistics for Saudi Revenue [20].
Statistical analysis
Descriptive statistics were summarized using numbers, percentages, means, and standard deviations whenever appropriate. The association between QoL and SDoH was analyzed using the Mann–Whitney U test as well as the Kruskal–Wallis H test. Normality tests were conducted using the Shapiro–Wilk test and the Kolmogorov–Smirnov test. The children’s QoL scores followed a non-normal distribution. Therefore, non-parametric tests were applied. A P-value of < 0.05 was considered statistically significant. Furthermore, the relationship between CKD stage and sociodemographic variables was analyzed using the Fisher’s Exact test. Data analyses were conducted using Statistical Packages for Social Sciences (SPSS) version 26. Armonk, NY: IBM Corporation.
Results
Study participants
We enrolled 50 children at different stages of CKD to assess various SDoH in relation to their QoL. The study included 9 children on hemodialysis, 10 children on PD, 11 children with CKD stage 5, 10 children with CKD stage 4, and 10 children with CKD stage 3. The ages of the participants varied, but the most common age group was school-aged children, with 32% being between 8 and 12 years old. Gender distribution among all participants was 56% (28/50) for males and 44% (22/50) for females. The median (IQR) age for participants was 9 [5–12] years.
SDoH of children with CKD
Just over half of the participants were living in the same city as the pediatric CKD clinic in Riyadh, 56% (28/50). More than two-thirds of the participants came from large families; 66% (33/50) had five or more family members. 48% (24/50) of the participants had stable housing. A vast majority of the children (88%, 44/50) lived with both parents in a stable nuclear family, while another 14% (7/50) had separated parents. Access to healthcare was relatively high, with 64% (32/50) of participants indicating that a hospital was in close proximity. Transportation appeared to be convenient; 86% (43/50) of the families owned a reliable mode of transportation for accessing care (Table 1).
Table 1.
Demographic characteristics and SDoH of the study participants (n = 50)
| Study variables | N (%) |
|---|---|
| Child Age (Years) | |
| • 2–4 | 12 (24.0%) |
| • 5–7 | 10 (20.0%) |
| • 8–12 | 16 (32.0%) |
| • 13–16 | 12 (24.0%) |
| Child gender | |
| • Male | 28 (56.0%) |
| • Female | 22 (44.0%) |
| Residence city | |
| • Urban | 28 (56.0%) |
| • Rural | 22 (44.0%) |
| Family Size (No. of Members) | |
| • 1–2 | 02 (04.0%) |
| • 3–4 | 15 (30.0%) |
| • ≥ 5 | 33 (66.0%) |
| Housing | |
| • Owned a house | 24 (48.0%) |
| • Rented house | 10 (20.0%) |
| • Owned apartment | 03 (06.0%) |
| • Rented apartment | 13 (26.0%) |
| Child living situation | |
| • Family (mother and father) | 44 (88.0%) |
| • Mother | 05 (10.0%) |
| • Father | 01 (02.0%) |
| Parental marital status | |
| • Living together | 43 (86.0%) |
| • Separated | 07 (14.0%) |
| Distance to Nearest Hospital | |
| • In the same city of residence | 32 (64.0%) |
| • Outside the city of residence | 18 (36.0%) |
| Transportation type | |
| • Personal vehicle | 43 (86.0%) |
| • Public transportation | 03 (06.0%) |
| • Airplane | 04 (08.0%) |
| Family monthly income (SAR) | |
| • Low (5000) | 14 (28.0%) |
| • Middle (5,000–10,000) | 25 (50.0%) |
| • Upper-middle (10,001–20,000) | 08 (16.0%) |
| • High (> 20,000) | 03 (06.0%) |
| Caregivers (Mother) education | |
| • Illiterate /Uneducated | 07 (14.0%) |
| • Middle school or lower | 11 (22.0%) |
|
• High school • Collage or higher |
11 (22.0%) 21 (42.0%) |
| Availability of education for the child | |
| • Unavailable | 10 (20.0%) |
| • Available | 33 (66.0%) |
| • Difficult to find | 07 (14.0%) |
| Availability of diet recommended by nephrology team | |
| • Unavailable | 02 (04.0%) |
| • Available | 40 (80.0%) |
| • Difficult to find | 08 (16.0%) |
| CKD stage | |
| • Stage 3 | 10 (20.0%) |
| • Stage 4 | 10 (20.0%) |
| • Stage 5 | 11 (22.0%) |
| • HD | 09 (18.0%) |
| • PD | 10 (20.0%) |
Most primary caregivers were well-educated, with 42% (21/50) of mothers having higher education. Schooling and education were available to only 66% of children with CKD. Access to a specialized renal diet was high, reaching 80% of participants.
QoL of children with CKD in Saudi Arabia
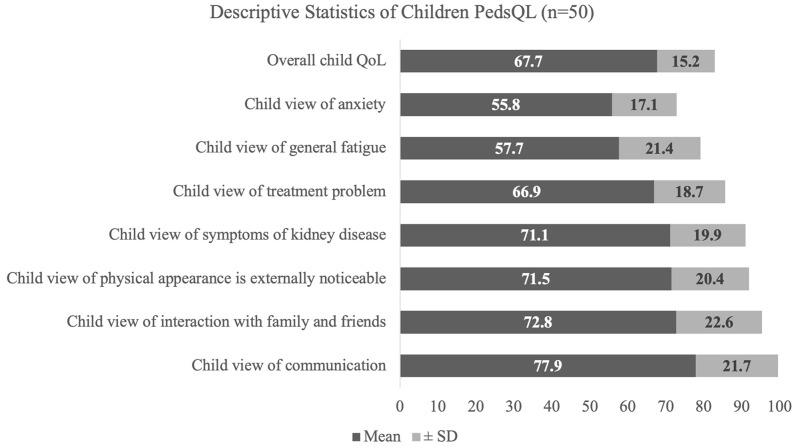
The highest ratings of QoL for children with CKD in Saudi Arabia were observed in the communication domain (mean score: 77.9). This was followed by the interaction with family and friends domain (mean score: 72.8), and then the physical appearance domain (mean score: 71.5). The overall mean QoL score for the children was 67.7 (SD 15.2) (Fig. 2).
Fig. 2.
Parents and children report anxiety and children’s view of fatigue, followed by their view of treatment problems as the most influencing factors of the QoL in children with CKD in Saudi Arabia
Intersectionality of SDoH and QoL of children with CKD in Saudi Arabia
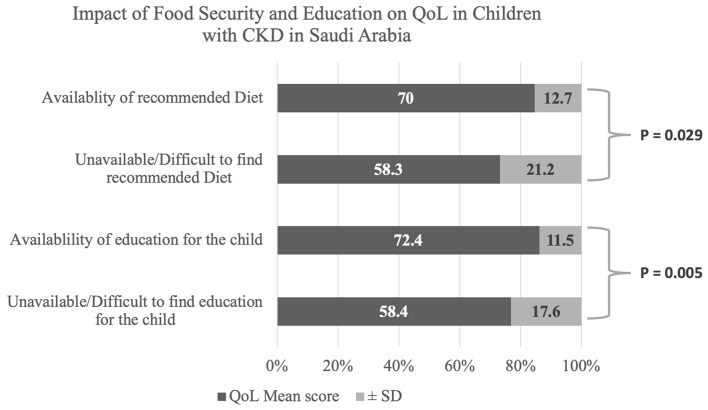
Analyzing the association between children’s QoL scores and SDoH revealed a positive correlation between higher QoL and the ability to attend school for a proper education (Z = 2.825; p = 0.005). Similar patterns were observed with the security of a specialized renal diet (Z = 1.441; p = 0.029) (Fig. 3). On the other hand, we observed a negative correlation between children’s QoL and advanced stages of CKD, especially ESRD (H = 2.154; p = 0.031). Interestingly, in children with ESRD on PD, higher QoL scores were associated with larger family sizes (Z = 2.009; p = 0.045), higher income (H = 6.093; p = 0.048), and access to school (Z = 2.158; p = 0.031) [21] (Table 2).
Fig. 3.
Special diet access impacted the QoL of children with CKD and their access to school and proper education
Table 2.
Role of SDoH on influencing children with CKD QoL in Saudi Arabia (n = 50)
| Factor | Child QoL Score (100) Mean ± SD |
H/Z-test; P-value |
|---|---|---|
| Age group a | ||
| • 5–7 years | 69.5 ± 11.7 |
0.803; 0.669 |
| • 8–12 years | 68.2 ± 20.9 | |
| • 13–16 years | 65.2 ± 17.7 | |
| Child gender b | ||
| • Male | 68.7 ± 16.9 |
1.417; 0.156 |
| • Female | 66.4 ± 13.0 | |
| Residence city b | ||
| • Urban | 66.7 ± 14.1 |
0.138; 0.890 |
| • Rural | 68.9 ± 16.8 | |
| Number of family members b | ||
| • < 5 | 64.5 ± 18.1 |
1.371; 0.170 |
| • ≥ 5 | 69.3 ± 13.6 | |
| Child residency b | ||
| • House stability | 70.9 ± 10.4 |
1.245; 0.213 |
| • House instability | 63.9 ± 19.0 | |
| Parental marital status b | ||
| • Living together | 69.5 ± 12.5 |
0.816; 0.414 |
| • Separated | 56.7 ± 25.1 | |
| Nearest hospital b | ||
| • In the same city of residence | 68.5 ± 11.5 |
0.081; 0.935 |
| • Outside city of residence | 66.1 ± 20.6 | |
| Family monthly income (SAR) a | ||
| • < 5000 | 62.3 ± 19.7 |
3.081; 0.214 |
| • 5,000–10,000 | 68.2 ± 13.0 | |
| • > 10,000 | 73.4 ± 12.2 | |
| Mother education b | ||
| • High school or below | 68.2 ± 15.5 |
0.396; 0.692 |
| • Higher education | 66.9 ± 15.3 | |
| Father education b | ||
| • High school or below | 71.2 ± 14.5 |
1.833; 0.067 |
| • Higher education | 63.6 ± 15.4 | |
| Availability of education for the child b | ||
| • Unavailable/Difficult to find | 58.4 ± 17.6 |
2.825; 0.005 ** |
| • Available | 72.4 ± 11.5 | |
| Availability of diet | ||
| • Unavailable/Difficult to find | 58.3 ± 21.2 |
1.441; 0.029 ** |
| • Available | 70.0 ± 12.7 | |
| CKD stages b | ||
| • Stage 3–5 | 71.6 ± 12.9 |
2.154; 0.031 ** |
| • ESRD | 61.2 ± 16.7 | |
a P-value has been calculated using Kruskal Wallis H-test
b P-value has been calculated using Mann Whitney Z-test
** Significant at p<0.05 level
Discussion
Our study provides the first insights into exploring the relationship between SDoH and the QoL of children with CKD in Saudi Arabia. In fact, it is the first study to explore such a relationship in the Middle East at large. Understanding the complex relationship between SDoH and QoL can assist in tailoring care and interventions to match the resources and living conditions of each child and their family. This approach marks a step forward toward personalized medicine and has the potential to improve the QoL of children with CKD in Saudi Arabia and the broader region.
Populations with poor SDoH are disproportionately affected by CKD and ESRD, highlighting the importance for primary care providers to prioritize education and screening in their interventions [22]. Specifically, low socioeconomic status and limited access to healthcare contribute to disparities and worsen the impact of genetic or biological predispositions [23]. These findings are particularly relevant in pediatric CKD, where the influence of SDoH on disease onset and progression warrants further investigation.
Access to school and proper education were major determinants of QoL for children with CKD in our study. This finding is similar to that of Narva et al. [24]. Additionally, Lopez-Vargas et al. documented the positive impact of education on CKD management in children [25]. School is not just a place for learning; it is also a place for socialization and emotional support [26]. The COVID-19 pandemic provided a clear example of the impact that the inability to attend school has on children’s learning abilities and neurodevelopment [27]. Even without concerns about neurodevelopment, access to schools and education are basic human rights and should be available to all children. Despite efforts by the Saudi Ministry of Education to include children with CKD in public schools, many parents hesitate to send their children to school, especially those in advanced stages of the disease. Future efforts should focus on empowering parents to facilitate their children’s full attendance at school.
The importance of having social support was evident in achieving a higher QoL among large families in our findings. Furthermore, children identified communication and relationships as the most valuable aspects for their QoL [28, 29]. Psychosocial and financial support for families were reported in the literature as major determinants of QoL. The impact of family income was highlighted among children with ESRD on PD in our findings.
Furthermore, the relationship between SDoH and QoL appeared to be stage-specific. It is not surprising that children with CKD stages 3–5 had higher QoL scores than those with ESRD on PD or HD. Our data are consistent with Krishnan et al. [30]. Additionally, Pagels et al. found that QoL scores were higher in CKD stages 3–5 compared to those in dialysis patients [31]. A similar finding was noted in previously published literature, showing that children on PD self-reported a significantly higher QoL than those on hemodialysis [32]. Furthermore, previous research consistently showed that the QoL of individuals with CKD is significantly impacted by the severity of the disease [33, 34]. This could suggest that families with greater disease severity may benefit from increased healthcare support to improve their children’s QoL.
Our study showed that children rated the communication domain as most satisfying in the Pediatric Quality of Life Inventory (PedsQL). This indicates that effective communication can significantly improve their QoL as they often struggle to express their symptoms and emotions to healthcare providers, ask questions about their treatment, and discuss their condition with peers and family. Ineffective communication can lead to isolation and hinder their emotional and social development. Effective communication within the family unit and with healthcare providers appears to be a critical component of perceived QoL, possibly acting as a buffer against the stressors associated with managing a chronic condition. The communication skills of Saudi pediatric healthcare providers were perceived as suboptimal by many Saudi families, according to the literature [35, 36]. Improving the communication skills of pediatric providers can enhance CKD outcomes, adherence to medication, and children’s QoL [37, 38]. This underscores the need to enhance the communication skills of the next generation of Saudi pediatricians and pediatric nephrologists. Fortunately, Saudi pediatric residency trainees are required to complete formal communication skills training that takes into account Saudi Arabia’s cultural sensitivities [39]. To address these issues, targeted communication training can help these children articulate their needs more effectively. Supportive counseling can assist in managing communication-related anxieties, and family education programs can empower relatives better to support the child’s emotional and communicative needs. These strategies collectively aim to bolster the child’s confidence and overall well-being.
On the other hand, children rated the anxiety domain as least satisfied in the Pediatric Quality of Life Inventory (PedsQL). Children with CKD often face communication difficulties and heightened anxiety, which significantly impact their quality of life. They may feel isolated due to misunderstandings about their condition, preventing them from participating in everyday activities. Concerns about treatment efficacy, potential surgeries, and chronic health issues heighten their anxiety. To address these challenges, strategies such as Educational Support to inform peers, teachers, and family about CKD can create a supportive environment [40]. Psychological Counseling offers regular sessions to help manage anxiety and feelings of isolation. Social Inclusion Efforts organize activities that accommodate the child’s limitations, maintaining social connections [41]. Communication Workshops teach effective communication techniques to children and their families [41, 42]. Regular Medical Reviews with healthcare providers clarify treatment plans and reduce uncertainties, all aiming to improve the emotional and social well-being of children with CKD, helping them lead more fulfilling lives despite their medical challenges [43].
Our findings are consistent with existing literature that reliably shows children with CKD have a lower QoL [44]. This reduced QoL is influenced by various SDoH, including schooling, food security, and family size. Conversely, many other SDoH did not impact the QoL of children with CKD in Saudi Arabia. Family income, parental marital status, and healthcare proximity did not affect the QoL of the study’s participants. This contrasts with prior research in other settings that linked parental education, occupation, marital status, income, and health insurance coverage to a lower QoL in children with chronic diseases such as CKD [45]. This underscores the importance of understanding local resources and the cultural sensitivity of SDoH to accurately measure their impact on QoL in any given geographic area. Conversely, our findings cannot be generalized to other locations due to the variability in the impact of different SDoH on the QoL of children with CKD.
In the context of children with ESRD on PD, larger family sizes and higher family incomes were correlated with an improved QoL in these children. Contrary to our findings, multiple studies collectively suggest that larger family sizes may not necessarily lead to an improved QoL in children with CKD in general [46–48]. However, having a larger family size was found to be protective against stress and emotional dysregulation [49]. PD is administered at home and can be a source of stress for many caregivers. The presence of more individuals to assist with setting up PD, facilitated by either a larger family size or higher income, might explain our findings.
Despite its strengths, the study has inherent limitations. It was conducted in a single center in the capital city, and its cross-sectional nature prevents the inference of causal relationships. Being based on self-reported data makes this study subject to recall bias. Parent reports are inherently biased by recall and perceptions as well as some parents might be influenced by their own perceptions. However, it is the first study in the region to assess the relationship between QoL and SDoH of children with CKD. It can serve as a foundation for future studies involving multiple centers and longitudinal designs.
Conclusions
This study provides insights into the intersectionality of SDoH and QoL of children with chronic illnesses in Saudi Arabia, using CKD as an example. Children with CKD identified communication as the most significant domain of their QoL, which can be enhanced at no additional cost through current communication skills training. SDoH significantly influenced the QoL of children with CKD in Saudi Arabia, with certain factors having a more pronounced impact than others. Schooling and proper education emerged as the primary determinants of a higher QoL for children with CKD, followed by food security related to a specialized diet. However, the influence of certain SDoH was stage-specific. Family size and income were found to improve the QoL of children with ESRD on PD only. This information can assist in tailoring care for families choosing between PD and HD based on family size and income. Barriers to HD, such as transportation, did not appear to be significant determinants of QoL for children with CKD in Saudi Arabia. Further research is needed to guide practitioners in Saudi Arabia on how to choose between PD and HD for children with ESRD, taking into account their SDoH.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Acknowledgements
The authors would like to thank the Research Center at King Fahad Medical City for their valuable support in conducting this study.
Abbreviations
- SDoH
Social determinants of health
- CKD
Chronic kidney disease
- QoL
Quality of life
- ESRD
End stage renal disease
- PD
Peritoneal dialysis
- HD
Hemodialysis
Author contributions
All Authors have met authorship requirements. See below for each author’s contribution: S.A, Y.A, O.A designed the study. T.A, H.A, S.H.A, A.A, performed the data collection. S.A, Y.A, O.A, drafted the manuscript. S.A, Y.A, Substantial contributions to drafting the article, revising it, and final approval of the version to be published. All authors have read and agreed to the published version of the manuscript.
Funding
This study was supported by funding from the Saudi National Institutes of Health (NIH) grant number (353838662).
Data availability
All of the data generated and analyzed during the current study are available from the corresponding author upon reasonable request.
Declarations
Ethics approval and consent to participate
Prior to commencing the study, we obtained IRB approval from the Institutional Review Board of King Fahad Medical City (IRB number FWA00018774), ensuring the anonymity of participants and the confidentiality of data. We reminded patients that their clinical care would not be affected if they chose not to participate in this study and allowed them to withdraw their data before data analysis. Informed consent was obtained from all study participants, including legal representatives for illiterate and minor participants. This research was performed in accordance with relevant national guidelines and regulations. All data were stored without patient identifiers and were accessible only to the research investigators for research purposes.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Footnotes
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Magnan S. Social Determinants of Health 101 for Health Care: five plus five. NAM Perspect. 2017;7(10). [DOI] [PMC free article] [PubMed]
- 2.Marmot M. Global action on social determinants of health. Bull World Health Organ. 2011;89(10):702. 10.2471/BLT.11.094862 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Sokol R, Austin A, Chandler C, Byrum E, Bousquette J, Lancaster C et al. Screening Children for Social Determinants of Health: a systematic review. Pediatrics. 2019;144(4). [DOI] [PMC free article] [PubMed]
- 4.Hunt A. Development of a Screening Tool for Social Determinants of Health at a federally qualified Health Center. Pediatrics. 2021;147(3MeetingAbstract):40. 10.1542/peds.147.3MA1.40 [DOI] [Google Scholar]
- 5.Brown J, Elliott R. Social Determinants of Health: understanding the basics and their impact on chronic kidney disease. Nephrol Nurs Journal: J Am Nephrol Nurses Association. 2021;48(2). [PubMed]
- 6.Iroegbu C, Lewis L, Matura LA. An integrative review: chronic kidney disease awareness and the social determinants of health inequities. J Adv Nurs. 2022;78(4):918–28. 10.1111/jan.15107 [DOI] [PubMed] [Google Scholar]
- 7.Chaichana U, Jantongsree M, Chantaratin S, Sumboonnanonda A, Pattaragarn A, Supavekin S et al. Quality of life in children at different stages of chronic kidney disease in a Developing Country2024. [DOI] [PMC free article] [PubMed]
- 8.Lai WM. Quality of life in children with end-stage renal disease: does treatment modality matter? Perit Dial Int. 2009;29(Suppl 2):S190–1. 10.1177/089686080902902S38 [DOI] [PubMed] [Google Scholar]
- 9.Marciano RC, Soares CM, Diniz JS, Lima EM, Silva JM, Canhestro MR, et al. Behavioral disorders and low quality of life in children and adolescents with chronic kidney disease. Pediatr Nephrol. 2011;26(2):281–90. 10.1007/s00467-010-1683-y [DOI] [PubMed] [Google Scholar]
- 10.Lupini F, Rubinstein TB, Mackey ER, Sule S. Behavioral health outcomes and social determinants of health in children with diabetes and juvenile arthritis. Res Sq. 2023.
- 11.Gerson AC, Wentz A, Abraham AG, Mendley SR, Hooper SR, Butler RW, et al. Health-related quality of life of children with mild to moderate chronic kidney disease. Pediatrics. 2010;125(2):e349–57. 10.1542/peds.2009-0085 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Lombardi C, Glosser L, Knauss H, Norwood T, Berry J, Ekwenna O. Impact of Social Determinants of Health on Chronic Kidney Disease: A Review of Disparities in Renal Transplantation. Translation: The University of Toledo Journal of Medical Sciences. 2021;9(1).
- 13.Brandt EJ. Social determinants of racial health inequities. Lancet Public Health. 2023;8(6):e396–7. 10.1016/S2468-2667(23)00100-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Kerklaan J, Hannan E, Baumgart A, Manera KE, Ju A, McCulloch M, et al. Patient- and parent proxy-reported outcome measures for life participation in children with chronic kidney disease: a systematic review. Nephrol Dial Transpl. 2020;35(11):1924–37. 10.1093/ndt/gfaa132 [DOI] [PubMed] [Google Scholar]
- 15.Sereni F, Edefonti A, Lepore M, Agostoni C, Sandoval Diaz M, Silva Galan Y, et al. Social and economic determinants of pediatric health inequalities: the model of chronic kidney disease. Pediatr Res. 2016;79(1–2):159–68. 10.1038/pr.2015.194 [DOI] [PubMed] [Google Scholar]
- 16.Schwartz GJ, Work DF. Measurement and estimation of GFR in children and adolescents. Clin J Am Soc Nephrol. 2009;4(11):1832–43. 10.2215/CJN.01640309 [DOI] [PubMed] [Google Scholar]
- 17.Inker LA, Astor BC, Fox CH, Isakova T, Lash JP, Peralta CA, et al. KDOQI US commentary on the 2012 KDIGO clinical practice guideline for the evaluation and management of CKD. Am J Kidney Dis. 2014;63(5):713–35. 10.1053/j.ajkd.2014.01.416 [DOI] [PubMed] [Google Scholar]
- 18.Goldstein SL, Rosburg NM, Warady BA, Seikaly M, McDonald R, Limbers C, et al. Pediatric end stage renal disease health-related quality of life differs by modality: a PedsQL ESRD analysis. Pediatr Nephrol. 2009;24(8):1553–60. 10.1007/s00467-009-1174-1 [DOI] [PubMed] [Google Scholar]
- 19.Goldstein SL, Graham N, Warady BA, Seikaly M, McDonald R, Burwinkle TM, et al. Measuring health-related quality of life in children with ESRD: performance of the generic and ESRD-specific instrument of the Pediatric Quality of Life Inventory (PedsQL). Am J Kidney Dis. 2008;51(2):285–97. 10.1053/j.ajkd.2007.09.021 [DOI] [PubMed] [Google Scholar]
- 20.Statistics GAf. average Monthly Wage (Salary) of Employed Persons (15 years and above) By Age categories, Sex & Nationality 2019 [ https://www.stats.gov.sa/en/6326
- 21.Dharnidharka VR, Sullivan EK, Stablein DM, Tejani AH, Harmon WE, North American Pediatric Renal Transplant Cooperative S. Risk factors for posttransplant lymphoproliferative disorder (PTLD) in pediatric kidney transplantation: a report of the North American Pediatric Renal Transplant Cooperative Study (NAPRTCS). Transplantation. 2001;71(8):1065–8. 10.1097/00007890-200104270-00010 [DOI] [PubMed] [Google Scholar]
- 22.Quinones J, Hammad Z. Social Determinants of Health and chronic kidney disease. Cureus. 2020;12(9):e10266. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Garcia-Garcia G, Jha V. CKD in disadvantaged populations. J Bras Nefrol. 2015;37(1):14–8. 10.5935/0101-2800.20150003 [DOI] [PubMed] [Google Scholar]
- 24.Narva AS, Norton JM, Boulware LE. Educating patients about CKD: the path to self-management and patient-centered care. Clin J Am Soc Nephrology: CJASN. 2016;11 4:694–703. 10.2215/CJN.07680715 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Lopez-Vargas PA, Tong A, Howell M, Craig JC. Educational interventions for patients with CKD: a systematic review. Am J Kidney Dis. 2016;68(3):353–70. 10.1053/j.ajkd.2016.01.022 [DOI] [PubMed] [Google Scholar]
- 26.Thummler R, Engel EM, Bartz J. Strengthening emotional development and emotion regulation in Childhood-As a Key Task in Early Childhood Education. Int J Environ Res Public Health. 2022;19(7). [DOI] [PMC free article] [PubMed]
- 27.Colvin MKM, Reesman J, Glen T. The impact of COVID-19 related educational disruption on children and adolescents: an interim data summary and commentary on ten considerations for neuropsychological practice. Clin Neuropsychol. 2022;36(1):45–71. 10.1080/13854046.2021.1970230 [DOI] [PubMed] [Google Scholar]
- 28.Watson AR. Psychosocial support for children and families requiring renal replacement therapy. Pediatr Nephrol. 2014;29(7):1169–74. 10.1007/s00467-013-2582-9 [DOI] [PubMed] [Google Scholar]
- 29.Medway M, Tong A, Craig JC, Kim S, Mackie F, McTaggart S, et al. Parental perspectives on the financial impact of caring for a child with CKD. Am J Kidney Dis. 2015;65(3):384–93. 10.1053/j.ajkd.2014.07.019 [DOI] [PubMed] [Google Scholar]
- 30.Krishnan A, Teixeira-Pinto A, Lim WH, Howard K, Chapman JR, Castells A, et al. Health-Related Quality of Life in people across the Spectrum of CKD. Kidney Int Rep. 2020;5(12):2264–74. 10.1016/j.ekir.2020.09.028 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Pagels AA, Söderkvist BK, Medin C, Hylander B, Heiwe S. Health-related quality of life in different stages of chronic kidney disease and at initiation of dialysis treatment. Health Qual Life Outcomes. 2012;10:71. 10.1186/1477-7525-10-71 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Park KS, Hwang YJ, Cho MH, Ko CW, Ha IS, Kang HG, et al. Quality of life in children with end-stage renal disease based on a PedsQL ESRD module. Pediatr Nephrol. 2012;27(12):2293–300. 10.1007/s00467-012-2262-1 [DOI] [PubMed] [Google Scholar]
- 33.Mujais SK, Story K, Brouillette J, Takano T, Soroka S, Franek C, et al. Health-related quality of life in CKD patients: correlates and evolution over time. Clin J Am Soc Nephrol. 2009;4(8):1293–301. 10.2215/CJN.05541008 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Tong A, Wong G, McTaggart S, Henning P, Mackie F, Carroll RP, et al. Quality of life of young adults and adolescents with chronic kidney disease. J Pediatr. 2013;163(4):1179–85. e5. 10.1016/j.jpeds.2013.04.066 [DOI] [PubMed] [Google Scholar]
- 35.Alnasser YS, Bin Nafisah HM, Almubarak ZA, Aleisa LA, El Sarrag AI, Babiker AM. Communication skills between physicians’ insights and parents’ perceptions in a teaching hospital in KSA. J Taibah Univ Med Sci. 2017;12(1):34–40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Zolaly MA. Satisfaction of parents of paediatric patients with physicians’ communication skills in Almadinah Almunawwarah, Kingdom of Saudi Arabia. J Taibah Univ Med Sci. 2012;7(1):29–34. [Google Scholar]
- 37.Glenn TW, Riekert KA, Roter D, Eakin MN, Pruette CS, Brady TM, et al. Engagement and Affective Communication during Pediatric Nephrology Clinic visits: associations with Medication Adherence. Patient Educ Couns. 2021;104(3):578–84. 10.1016/j.pec.2020.08.039 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Gutman T, Hanson CS, Bernays S, Craig JC, Sinha A, Dart A, et al. Child and parental perspectives on communication and decision making in Pediatric CKD: a Focus Group Study. Am J Kidney Dis. 2018;72(4):547–59. 10.1053/j.ajkd.2018.05.005 [DOI] [PubMed] [Google Scholar]
- 39.Alnasser YS, Alabdali AF, Alshabri RI, Albatati SM. Practice of general pediatrics in Saudi Arabia: current status, challenges, and opportunities. BMC Pediatr. 2022;22(1):621. 10.1186/s12887-022-03648-w [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Love S, Harrison TG, Fox DE, Donald M, Hemmelgarn BR, Elliott MJ. Healthcare Provider perspectives on integrating peer support in non-dialysis-dependent chronic kidney Disease Care: a mixed methods study. BMC Nephrol. 2022;23(1). [DOI] [PMC free article] [PubMed]
- 41.Buyan N, Türkmen M, Bilge İ, Baskın E, Haberal M, Bilginer Y, et al. Quality of life in children with chronic kidney disease (with child and parent assessments). Pediatr Nephrol. 2010;25(8):1487–96. 10.1007/s00467-010-1486-1 [DOI] [PubMed] [Google Scholar]
- 42.Boulware LE, Hill-Briggs F, Kraus ES, Melancon JK, Falcone B, Ephraim PL, et al. Effectiveness of Educational and Social Worker interventions to activate patients’ discussion and pursuit of preemptive living donor kidney transplantation: a Randomized Controlled Trial. Am J Kidney Dis. 2013;61(3):476–86. 10.1053/j.ajkd.2012.08.039 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Kogon AJ, Harshman LA. Chronic kidney disease: treatment of comorbidities I (Nutrition, Growth, neurocognitive function, and Mineral Bone Disease). Curr Treat Options Pediatr. 2019;5(2):78–92. 10.1007/s40746-019-00152-9 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Dotis J, Pavlaki A, Printza N, Stabouli S, Antoniou S, Gkogka C, et al. Quality of life in children with chronic kidney disease. Pediatr Nephrol. 2016;31(12):2309–16. 10.1007/s00467-016-3457-7 [DOI] [PubMed] [Google Scholar]
- 45.Didsbury MS, Kim S, Medway MM, Tong A, McTaggart SJ, Walker AM, et al. Socio-economic status and quality of life in children with chronic disease: a systematic review. J Paediatr Child Health. 2016;52(12):1062–9. [DOI] [PubMed]
- 46.Kilis-Pstrusinska K, Medynska A, Chmielewska IB, Grenda R, Kluska-Jozwiak A, Leszczynska B, et al. Perception of health-related quality of life in children with chronic kidney disease by the patients and their caregivers: multicentre national study results. Qual Life Res. 2013;22(10):2889–97. 10.1007/s11136-013-0416-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.McKenna AM, Keating LE, Vigneux A, Stevens SE, Williams A, Geary DF. Quality of life in children with chronic kidney disease-patient and caregiver assessments. Nephrology, dialysis, transplantation: official publication of the European Dialysis and Transplant Association -. Eur Ren Association. 2006;21 7:1899–905. [DOI] [PubMed] [Google Scholar]
- 48.Goldstein SL, Graham N, Burwinkle T, Warady B, Farrah R, Varni JW. Health-related quality of life in pediatric patients with ESRD. Pediatr Nephrol. 2006;21(6):846–50. 10.1007/s00467-006-0081-y [DOI] [PubMed] [Google Scholar]
- 49.Taanila A, Ebeling H, Kotimaa A, Moilanen I, Jarvelin MR. Is a large family a protective factor against behavioural and emotional problems at the age of 8 years? Acta Paediatr. 2004;93(4):508–17. 10.1111/apa.2004.93.4.508 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
All of the data generated and analyzed during the current study are available from the corresponding author upon reasonable request.