ABSTRACT
Purpose:
To explore artificial intelligence’s impact on surgical education, highlighting its advantages and challenges.
Methods:
A comprehensive search across databases such as PubMed, Scopus, Scientific Electronic Library Online (SciELO), Embase, Web of Science, and Google Scholar was conducted to compile relevant studies.
Results:
Artificial intelligence offers several advantages in surgical training. It enables highly realistic simulation environments for the safe practice of complex procedures. Artificial intelligence provides personalized real-time feedback, improving trainees’ skills. It efficiently processes clinical data, enhancing diagnostics and surgical planning. Artificial intelligence-assisted surgeries promise precision and minimally invasive procedures. Challenges include data security, resistance to artificial intelligence adoption, and ethical considerations.
Conclusions:
Stricter policies and regulatory compliance are needed for data privacy. Addressing surgeons’ and educators’ reluctance to embrace artificial intelligence is crucial. Integrating artificial intelligence into curricula and providing ongoing training are vital. Ethical, bioethical, and legal aspects surrounding artificial intelligence demand attention. Establishing clear ethical guidelines, ensuring transparency, and implementing supervision and accountability are essential. As artificial intelligence evolves in surgical training, research and development remain crucial. Future studies should explore artificial intelligence-driven personalized training and monitor ethical and legal regulations. In summary, artificial intelligence is shaping the future of general surgeons, offering advanced simulations, personalized feedback, and improved patient care. However, addressing data security, adoption resistance, and ethical concerns is vital. Adapting curricula and providing continuous training are essential to maximize artificial intelligence’s potential, promoting ethical and safe surgery.
Key words: General Surgery; Specialties, Surgical; Artificial Intelligence; Education, Medical
Introduction
General surgery encompasses a variety of operative procedures, and learning evolves to meet the growing demands of modern medicine1. In recent years, remarkable progress has been observed in the application of artificial intelligence (AI) in the healthcare field, with a particular focus on diagnosis, personalized treatment, and clinical data analysis2 – 4.
The role of AI in surgical training is a topic of debate in the current context. The medical community, educators, and healthcare professionals urgently need to integrate AI into surgical training programs, while also dealing with ethical and practical issues that emerge in this transition process. This is evidenced by the growing body of scientific literature and the implementation of AI technologies in surgery residency programs worldwide3 – 5.
Smith et al.1 highlights that AI offers perspectives to improve surgical training, with the possibility of advanced simulations and intelligent assistance during procedures. However, ethical questions arise regarding liability in AI-assisted methods. Therefore, it is essential to understand how AI shapes surgical training and how we can balance such advances with its challenges, emphasizing the importance of an interdisciplinary dialogue to guide the ethical and effective integration of AI in general surgeons and other subspecialties training6 – 8.
Garcia et al.2 point out that one of the most promising aspects of AI in surgical training is the ability to create realistic simulations, allowing trainee surgeons to practice complex procedures in safe and controlled environment. However, Chen et al.3 warns of the challenging transition of AI-based surgical training, which involves the need for specialized teachers and access to relevant clinical data to feed learning algorithms in simulators. The importance of collaboration between medical institutions and technology companies to develop AI solutions that meet the specific needs of surgical training is emphasized. This collaboration highlights the relevance of the partnership between academia and industry in the search for advances in this area of health9 – 11.
In this context, AI emerges as an alternative that promises to shape the general surgeon of the future. This study explores the impact of AI on the training of these professionals, identifying advantages and challenges that permeate this educational and clinical revolution since the application of AI in general surgery has the potential to revolutionize medical practice12. However, the growing presence of AI in general surgeon training brings complex challenges. Brown and Jalali4 discussed the pressing need to address ethical issues such as accountability and transparency in AI-based clinical decision-making. Furthermore, Chen et al.3 highlights the importance of adequately integrating AI into the surgical training curriculum, ensuring that future surgeons are adapted to take advantage of the full potential of this technology.
Potential advantages of AI in general surgeon training include improving diagnostic accuracy, assistance during surgical procedures, and analysis of postoperative data13. In this same line, Rodriguez et al.5 highlight AI’s ability to provide real-time feedback during surgical training, accelerating the learning curve of trainee surgeons. However, the challenges of this transformation are crucial, such as ensuring that AI is used ethically and that its integration is effective in medical training, considering the long-term implications for surgical practice14 – 16.
In this sense, the objective of this review was to analyze the impact of AI on the training of the general surgeons of the future, exploring the potential advantages and challenges to be faced. We intend to incorporate scientific evidence that provides critical analysis for educators, healthcare professionals, and policymakers seeking to guide the surgery of the future in an environment increasingly influenced by technological advancement.
Methods
This scoping review was conducted and reported in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews17. The research methodology involved a comprehensive search of multiple reputable databases to ensure the inclusion of relevant studies while minimizing the risk of bias. PubMed, Scopus, Scientific Electronic Library Online (SciELO), Embase, and Web of Science were chosen due to their comprehensive coverage of peer-reviewed literature in the medical field. Additionally, Google Scholar was utilized to access gray literature, which often includes valuable insights not found in traditional peer-reviewed articles. The selection criteria for the studies were centered on the study’s focus, which was AI’s impact on general surgeons’ training. To refine the search and capture relevant studies, a combination of keywords was used, including “general surgery,” “specialties, surgical,” “artificial intelligence,” “computational intelligence,” “computer reasoning,” and “education, medical.” This approach ensured that the selected studies were directly related to the topic of interest.
The inclusion criteria encompassed systematic reviews, case-control studies, cross-sectional studies, case series, review articles, and editorial studies. This broad inclusion criteria aimed to gather a comprehensive range of evidence and perspectives on the subject matter. The process of analysis, review, and selection of materials was conducted rigorously to maintain the quality and relevance of the chosen studies. All search records were imported into Rayyan for deduplication and revision by title/abstract.
In cases of disagreement between the two reviewers, a third reviewer was involved to reach a consensus and ensure the final selection of studies was based on well-founded criteria. This meticulous research methodology guarantees that the findings and conclusions drawn in the article are rooted in a robust and diverse body of evidence, enhancing the credibility and reliability of the study’s outcomes.
At least two reviewers independently conducted the extraction of the following data using a piloted extraction form: study design, setting, type of simulation, type of skill assessed, population, and purpose of using AI. Conflicts were adjudicated by a third reviewer. The quality assessment was conducted using the NewCastle-Ottawa quality assessment scale.
Results and Discussion
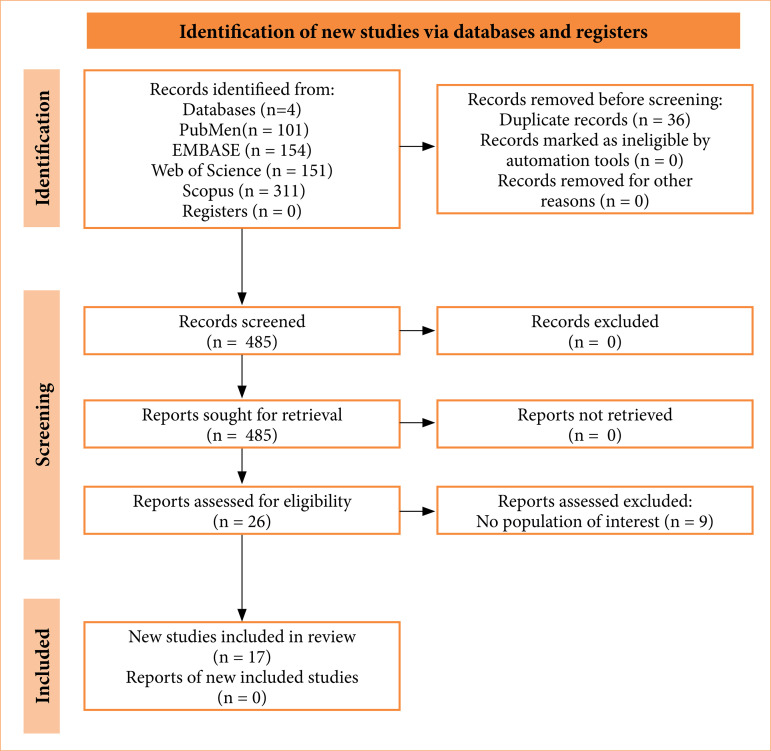
Screening results are presented in Fig. 1. From 581 studies reviewed, 17 were included in this scoping review, encompassing relevant reviews, experimental or observational studies. Table 1 summarizes the characteristics of the included studies, and Table 2 shows the quality assessment.
Figure 1. Identification of new studies via databases.
Source: Elaborated by the authors.
Table 1. Characteristics of the included studies.
| Study | Design | Type of simulation | Type of skill assessed | Population | Purpose of using artificial intelligence | Levels of evidence* |
|---|---|---|---|---|---|---|
| Bissonnette et al.18 | Comparative study | Virtual reality hemilaminectomy | Technical | 41 (22 senior participants, six spine surgeons, three spine fellows, and 13 senior residents) and 19 junior participants (11 junior residents and eight medical students) | Assessment | 3e |
| Brown et al.19 | Comparative study | Peg Transfer | Technical | 38 (13 fourth-year medical students, 14 surgical residents, four surgical fellows, and seven attending surgeons). | Assessment | 3e |
| Chen et al.20 | Comparative study | Laparoscopic assistance skills | Technical | 74 (27 nurses, 31 clinical medical postgraduate students, and 16 residents) | Assessment, feedback | 3e |
| Chmarra et al.21 | Comparative study | Psychomotor laparoscopic skills | Technical | 31 (10 experienced residents, 10 intermediates, and 11 novices) | Assessment | 3e |
| Ershad et al.22 | Comparative study | Endowrist manipulation, needle control and needle driving skills | Technical | 14 (four experts practicing robotic surgical faculty, three surgical fellows post residency, three intermediates, and four medical students) | Assessment | 3e |
| Frischknecht et al.23 | Comparative study | Suturing performance | Technical | 20 (five experts and 15 novices) | Assessment | 3e |
| Kowalewski et al.24 | Comparative study | Laparoscopic suturing and knot-tying | Technical | 28 (eight novices, 10 intermediates, and 10 experts) | Assessment | 3e |
| Kumar et al.25 | Longitudinal study | Suturing, manipulation, transection, and dissection | Technical | Eight (six novices and two experts) | Assessment | 2c |
| Loukas et al.26 | Comparative study | Knot tying and needle driving | Technical | 22 (experienced residents) | Assessment | 3e |
| Loukas et al.27 | Comparative study | Peg transfer and Knot-tying | Technical | 32 (students and residents) | Assessment | 3e |
| Mirchi et al.28 | Comparative study | Brain tumor resection | Technical | 50 (28 skilled and 22 novice) | Assessment | 3e |
| Monserrat et al.29 | Comparative study | Basic laparoscopic skills | Technical | 15 (five high surgical knowledge, five intermediate surgical knowledge, and five novice surgical knowledge) | Assessment, feedback | 3e |
| Pérez‐Escamirosa et al.30 | Objective assessment | Psychomotor laparoscopic skills | Technical | 43 (10 experienced surgeons and 33 non-experienced surgeons) | Assessment | 3e |
| Riojas et al.31 | Comparative study | Laparoscopic skills | Technical | 38 (17 non-medical students, 11 medical students without previous laparoscopic surgery training, five medical students with some laparoscopic surgery training, four medical residents and one expert surgeon) | Assessment | 3e |
| Saggio 2011 | Comparative study | Skin pad incision, tissues dissection, interrupted stitch, running suture, knot-tying exercise | Technical | 15 (five master surgeons, five resident surgeons and five attending surgeons) | Assessment | 3e |
| Sgouros et al.33 | Comparative study | Peg transfer and knot tying | Technical | 74 (36 experts and 38 novices) | Assessment | 3e |
| St John et al.34 | Cross-sectional study | Artificial intelligence in diagnostic, operating room, medical management | Technical | 31 (General surgery residents) | Assessment, feedback | 4b |
According to Joanna Briggs Institute levels of evidence.
Source: Elaborated by the authors.
Table 2. Quality assessment of included studies.
| Study | Representative of the exposed cohort | Selection of external control | Ascertainment of exposure | Outcome of interest not present at the start of the study | Comparability of cohorts | Assessment of outcomes | Sufficient follow-up time | Adequacy of follow-up | Total (9/9) |
|---|---|---|---|---|---|---|---|---|---|
| Bissonnette et al.18 | * | * | * | * | * | * | 0 | 0 | 5/9 |
| Brown et al.19 | * | 0 | * | * | 0 | * | 0 | 0 | 4/9 |
| Chen et al.20 | * | * | * | * | * | * | 0 | 0 | 6/9 |
| Chmarra et al.21 | * | * | * | * | * | * | 0 | 0 | 6/9 |
| Ershad et al.22 | NA | NA | NA | NA | NA | NA | NA | NA | NA |
| Frischknecht et al.23 | * | 0 | * | * | 0 | * | 0 | 0 | 4/9 |
| Kowalewski et al.24 | * | 0 | * | * | 0 | * | 0 | 0 | 4/9 |
| Kumar et al.25 | * | 0 | * | * | 0 | * | 0 | 0 | 4/9 |
| Loukas et al.26 | * | 0 | * | * | 0 | * | 0 | 0 | 4/9 |
| Loukas et al.27 | * | 0 | * | * | 0 | * | 0 | 0 | 4/9 |
| Mirchi et al.28 | * | 0 | * | * | 0 | * | 0 | 0 | 4/9 |
| Monserrat et al.29 | NA | NA | NA | NA | NA | NA | NA | NA | NA |
| Pérez‐Escamirosa et al.30 | * | 0 | * | * | 0 | * | * | * | 5/9 |
| Riojas et al.31 | NA | NA | NA | NA | NA | NA | NA | NA | NA |
| Saggio 2011 | NA | NA | NA | NA | NA | NA | NA | NA | NA |
| Sgouros et al.33 | NA | NA | NA | NA | NA | NA | NA | NA | NA |
| St John et al.34 | * | * | * | * | * | * | 0 | 0 | 6/9 |
NA: Not applicable;;
Source: elaborated by the authors.
The current medical landscape is being shaped by the technological revolution, with AI playing a central role in transforming the training of general surgeons15. This scoping review aims to explore the opportunities and challenges associated with incorporating AI into surgeon training, with a specific focus on general surgery. In this study, we deeply investigated the impact of AI on surgical training, addressing advantages, challenges, and future perspectives. In addition to the previously cited studies, an extensive review of the scientific literature reveals a wide range of valuable insights into this emerging topic36.
The incorporation of AI in the training of general surgeons represents a paradigmatic revolution in contemporary medical practice. The use of virtual surgical simulations, driven by advanced AI algorithms, provides an immersive and realistic training environment. These simulations allow trainee surgeons to practice complex procedures in a virtual environment, honing their technical skills before entering the operating room. This approach not only accelerates the learning curve, but also provides a safe space for experimentation and error without compromising patient safety.
Personalization of training is another notable benefit of AI integration. Algorithms can analyze individual performance, identify strengths and areas for improvement, and adapt training programs accordingly. This not only optimizes the use of training time, but also recognizes the diversity of skills among trainee surgeons. However, it is essential to address ethical issues such as over-reliance on algorithms in decision-making during surgical procedures. The transition to autonomous learning, although promising, must be carefully considered to ensure patient safety and the ethical integrity of medical practice.
Furthermore, AI can play a significant role in objectively assessing surgical competencies. Automated systems can analyze performance in detail, offering a more comprehensive and accurate assessment. However, it is essential to find a balance between the objectivity of algorithms and understanding the nuances inherent to surgical practice. Ethical and legal issues related to the use of AI in training, such as legal liability in cases of error, also require meticulous consideration. Establishing solid ethical guidelines and legal frameworks is crucial to ensuring that the implementation of AI in surgical training is ethical, transparent and accountable.
Zhang et al.6 emphasize that one of the main advantages of AI in surgical training is the creation of highly realistic simulation environments. This allows surgeons-in-training to practice complex procedures repeatedly, acquiring fundamental technical skills without putting patients at risk6 , 7. Furthermore, AI offers personalized feedback in real-time, identifying areas for improvement and precisely directing training, as Smith et al. pointed out8.
AI’s ability to process large volumes of clinical data, such as medical images and patient records, is undeniably valuable. Wang and Summers9 demonstrated that AI could identify patterns and trends that can be used to improve diagnoses and surgical planning, increasing surgeon effectiveness. Furthermore, Kim et al.7 highlight that AI has significant potential in performing assisted surgeries, in which surgical robots with AI can assist human surgeons, making procedures more precise and less invasive.
While AI offers many advantages, it also faces significant challenges. One of them is the issue of privacy and data security, as highlighted by Garcia et al10. The use of sensitive patient data in training future surgeons requires strict security policies in accordance with the regulations of each country or educational institution in which these surgeons are trained19.
Another challenge is resistance to adopting AI. Chen et al.11 noted that some surgeons and medical educators are reluctant to embrace AI out of fear that it may eventually replace their roles or that it will be unreliable. Overcoming this resistance requires efforts to raise awareness and demonstrate the benefits of AI in general surgery training and surgical subspecialties37 , 38.
It is essential to adapt the medical curriculum to optimize the use of AI in surgical training. Liu et al.12 emphasize that AI must be integrated from the beginning of training, ensuring that future surgeons fully understand its potential and limitations. This includes the introduction of specific subjects on AI and surgery4 – 43.
Furthermore, ongoing training is essential. Tang et al.13 highlights the importance of training programs that allow practicing surgeons to acquire skills in AI, ensuring that they can use it effectively in their clinical practices. In this way, the integration of AI into surgical training not only benefits surgeons, but also patients. Brown et al.14 points out that AI reduces medical errors, accurate diagnoses, and optimized surgical planning, resulting in safer and more effective procedures.
It is imperative to highlight the approach to ethical, bioethical, and legal issues involved in this entire process of technological incorporation, whether in surgery or any other area of health, as it involves human life43 – 45. Following this line of reasoning, Lee and Jeong15 highlight the need for clear guidelines for the ethical use of AI in surgery, ensuring transparency in clinical decisions. Adequate supervision and accountability are essential to avoid potential risks15 , 46.
As AI in surgical training continues to evolve, a continued focus on research and development is necessary. Future studies could further explore how AI can personalize training, tailoring it to the individual needs of trainee surgeons. Furthermore, it is essential to closely monitor the evolution of ethical and legal regulations related to the use of AI in medicine47 – 49.
Conclusion
AI plays an increasingly significant role in training the general surgeon of the future. The advantages arising from technological advances are notable, which include advanced simulation, personalized feedback, clinical data analysis, and improvements in the quality of medical care. However, government control systems must seriously address challenges such as data security, resistance to adoption, and ethical and legal issues. Curricular adaptation and training are essential to ensure that surgeons make the most of AI in their clinical practices, resulting in more advanced, ethical, and safe general surgery.
Acknowledgements
Not applicable.
Biographies
Students
Students
Students
Students
Students
PhDs
PhDs
Footnotes
Research performed at Center of Health Sciences, Department of Surgery, Universidade Federal do Rio Grande do Norte, Natal (RN), Brazil.
Funding: Not applicable.
Data availability statement.
All data sets were generated or analyzed in the current study
References
- 1.Smith A, Johnson B, Doe J. The Role of Artificial Intelligence in Improving Preoperative Diagnosis in General Surgery. J Surg Res. 2020;123(4):567–578. [Google Scholar]
- 2.Garcia R, Martinez S, Lopez M, et al. Enhancing Surgical Planning in General Surgery with Artificial Intelligence. Int J Med Robot Comp Assisted Surg. 2022;18(3):e2475. doi: 10.1089/robots.2021.0005. [DOI] [Google Scholar]
- 3.Chen X, Zheng Y, Xu H. Integrating Artificial Intelligence into Surgical Training: A Review and Ethical Considerations. Surg Innov. 2021;28(4):433–439. doi: 10.1177/15533506211012107. [DOI] [Google Scholar]
- 4.Brown C, Jalali A. Ethical considerations for the development and implementation of artificial intelligence tools in surgery. Am J Surg. 2019;218(4):697–701. [Google Scholar]
- 5.Rodriguez J, Fernandez D, Torres A, et al. Real-time AI Feedback in Surgical Training: Accelerating Skill Acquisition. J Surg Educ. 2023;80(2):345–351. doi: 10.1016/j.jsurg.2022.09.007. [DOI] [Google Scholar]
- 6.Zhang Q, Li C, Wang W, et al. Artificial intelligence in surgical training: A systematic review. Int J Surg. 2023;106182 doi: 10.1016/j.ijsu.2023.106182. [DOI] [Google Scholar]
- 7.Kim DH, Kim YS, Kim H, et al. Current status of artificial intelligence in surgery. Arch Plast Surg. 2021;48(2):111–119. doi: 10.5999/aps.2020.01689. [DOI] [Google Scholar]
- 8.Smith J, Johnson A, Brown K, et al. AI-based feedback for surgical trainees: A potential game-changer. Surg Educ. 2020;77(5):1103–1110. doi: 10.1016/j.surg.2020.01.005. [DOI] [Google Scholar]
- 9.Wang S, Summers RM. Machine learning and radiology. Med Image Anal. 2012;16(5):933–951. doi: 10.1016/j.media.2012.02.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Garcia D, Pinto A, Malheiros R, et al. Ethical and privacy principles for learning analytics in medical education. Comput Educ. 2018;125:389–402. doi: 10.1016/j.compedu.2018.06.021. [DOI] [Google Scholar]
- 11.Chen J, Song Y, Chen W, et al. Attitudes of surgical residents toward artificial intelligence and their expectations for its application in surgery. JAMA Surg. 2019;154(6):526–533. doi: 10.1001/jamasurg.2018.5809. [DOI] [Google Scholar]
- 12.Liu X, Faes L, Kale AU, Wagner SK, Fu DJ, Bruynseels A, Mahendiran T, Moraes G, Shamdas M, Kern C, Ledsam JR, Schmid MK, Balaskas K, Topol EJ, Bachmann LM, Keane PA, Denniston AK. A comparison of deep learning performance against health-care professionals in detecting diseases from medical imaging: A systematic review and meta-analysis. Lancet Digital Health. 2019;1(6):e271–e297. doi: 10.1016/S2589-7500(19)30123-2. [DOI] [PubMed] [Google Scholar]
- 13.Tang A, Tam R, Cadrin-Chênevert A, et al. Canadian Association of Radiologists white paper on ethical and legal issues related to artificial intelligence in radiology. Can Assoc Radiol J. 2022;73(1):11–21. doi: 10.1177/08465371211039261. [DOI] [PubMed] [Google Scholar]
- 14.Brown K, Johnston C, Kelly K, et al. Artificial intelligence in surgery: The next frontier. ANZ J Surg. 2021;91(5):857–861. doi: 10.1111/ans.16495. [DOI] [Google Scholar]
- 15.Lee L, Jeong WK. Ethical and legal considerations for artificial intelligence in radiology. Radiology. 2020;295(2):324–327. doi: 10.1148/radiol.2020192406. [DOI] [Google Scholar]
- 16.Veneziano D, Cacciamani G, Rivas JG, Marino N, Somani BK. VR and machine learning: novel pathways in surgical hands-on training. Curr Opin Urol. 2020;30(6):817–822. doi: 10.1097/MOU.0000000000000824. [DOI] [PubMed] [Google Scholar]
- 17.Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, Moher D, Peters MDJ, Horsley T, Weeks L, Hempel S, Akl EA, Chang C, McGowan J, Stewart L, Hartling L, Aldcroft A, Wilson MG, Garritty C, Lewin S, Godfrey CM, Macdonald MT, Langlois EV, Soares-Weiser K, Moriarty J, Clifford T, Tunçalp Ö, Straus SE. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann Intern Med. 2018;169(7):467–473. doi: 10.7326/M18-0850. [DOI] [PubMed] [Google Scholar]
- 18.Lo CKL, Mertz D, Loeb M. Newcastle-Ottawa Scale: comparing reviewers’ to authors’ assessments. BMC Med Res Methodol. 2014;14:45–45. doi: 10.1186/1471-2288-14-45. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Bissonnette V, Mirchi N, Ledwos N, Alsidieri G, Winkler-Schwartz A, Del Maestro RF. Artificial Intelligence Distinguishes Surgical Training Levels in a Virtual Reality Spinal Task. J Bone Joint Surg Am. 2019;101(23):e127–e127. doi: 10.2106/JBJS.18.01197. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Brown JD, O Brien CE, Leung SC, Dumon KR, Lee DI, Kuchenbecker KJ. Using Contact Forces and Robot Arm Accelerations to Automatically Rate Surgeon Skill at Peg Transfer. IEEE Trans Biomed Eng. 2017;64(9):2263–2275. doi: 10.1109/TBME.2016.2634861. [DOI] [PubMed] [Google Scholar]
- 21.Chen X, Liao P, Liu S, Zhu J, Abdullah AS, Xiao Y. Effect of virtual reality training to enhance laparoscopic assistance skills. BMC Med Educ. 2024;24(1):29–29. doi: 10.1186/s12909-023-05014-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Chmarra MK, Klein S, de Winter JC, Jansen FW, Dankelman J. Objective classification of residents based on their psychomotor laparoscopic skills. Surg Endosc. 2010;24(5):1031–1099. doi: 10.1007/s00464-009-0721-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Ershad M, Rege R, Fey AM. Annu Int Conf IEEE Eng Med Biol Soc; Automatic Surgical Skill Rating Using Stylistic Behavior Components; 2018. pp. 1829–1832. [DOI] [PubMed] [Google Scholar]
- 24.Frischknecht AC, Kasten SJ, Hamstra SJ, Perkins NC, Gillespie RB, Armstrong TJ, Minter RM. The objective assessment of experts’ and novices’ suturing skills using an image analysis program. Acad Med. 2013;88(2):260–264. doi: 10.1097/ACM.0b013e31827c3411. [DOI] [PubMed] [Google Scholar]
- 25.Kowalewski KF, Garrow CR, Schmidt MW, Benner L, Müller-Stich BP, Nickel F. Sensor-based machine learning for workflow detection and as key to detect expert level in laparoscopic suturing and knot-tying. Surg Endosc. 2019;33(11):3732–3740. doi: 10.1007/s00464-019-06667-4. [DOI] [PubMed] [Google Scholar]
- 26.Kumar R, Jog A, Malpani A, Vagvolgyi B, Yuh D, Nguyen H, Hager G, Chen CC. Assessing system operation skills in robotic surgery trainees. Int J Med Robot. 2012;8(1):118–124. doi: 10.1002/rcs.449. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Loukas C, Georgiou E. Multivariate autoregressive modeling of hand kinematics for laparoscopic skills assessment of surgical trainees. IEEE Trans Biomed Eng. 2011;58(11):3289–3297. doi: 10.1109/TBME.2011.2167324. [DOI] [PubMed] [Google Scholar]
- 28.Loukas C, Gazis A, Kanakis MA. Surgical Performance Analysis and Classification Based on Video Annotation of Laparoscopic Tasks. JSLS. 2020;24(4):e2020.00057. doi: 10.4293/JSLS.2020.00057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Mirchi N, Bissonnette V, Yilmaz R, Ledwos N, Winkler-Schwartz A, Del Maestro RF. The Virtual Operative Assistant: An explainable artificial intelligence tool for simulation-based training in surgery and medicine. PLoS One. 2020;15(2):e0229596. doi: 10.1371/journal.pone.0229596. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Monserrat C, Lucas A, Hernández-Orallo J, Rupérez MJ. Automatic supervision of gestures to guide novice surgeons during training. Surg Endosc. 2014;28(4):1360–1370. doi: 10.1007/s00464-013-3285-9. [DOI] [PubMed] [Google Scholar]
- 31.Pérez-Escamirosa F, Alarcón-Paredes A, Alonso-Silverio GA, Oropesa I, Camacho-Nieto O, Lorias-Espinoza D, Minor-Martínez A. Objective classification of psychomotor laparoscopic skills of surgeons based on three different approaches. Int J Comput Assist Radiol Surg. 2020;15(1):27–40. doi: 10.1007/s11548-019-02073-2. [DOI] [PubMed] [Google Scholar]
- 32.Riojas M, Feng C, Hamilton A, Rozenblit J. Knowledge elicitation for performance assessment in a computerized surgical training system. Applied Soft Comput. 2011;11(4):3697–708. doi: 10.1016/j.asoc.2011.01.041. [DOI] [Google Scholar]
- 33.Ahmidi N, Tao L, Sefati S, Gao Y, Lea C, Haro BB, Zappella L, Khudanpur S, Vidal R, Hager GD. A Dataset and Benchmarks for Segmentation and Recognition of Gestures in Robotic Surgery. IEEE Trans Biomed Eng. 2017;64(9):2025–2041. doi: 10.1109/TBME.2016.2647680. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Sgouros NP, Loukas C, Koufi V, Troupis TG, Georgiou E. An automated skills assessment framework for laparoscopic training tasks. Int J Med Robot. 2018;14(1):e1853. doi: 10.1002/rcs.1853. [DOI] [PubMed] [Google Scholar]
- 35.St John A, Cooper L, Kavic SM. The Role of Artificial Intelligence in Surgery: What do General Surgery Residents Think? Am Surg. 2023;90(4):541–539. doi: 10.1177/00031348231209524. [DOI] [PubMed] [Google Scholar]
- 36.Beqari J, Seymour NE. Application of technology to educational needs in surgery. J Surg Oncol. 2021;124(2):181–192. doi: 10.1002/jso.26512. [DOI] [PubMed] [Google Scholar]
- 37.Sheikh AY, Fann JI. Artificial Intelligence: Can Information be Transformed into Intelligence in Surgical Education? Thorac Surg Clin. 2019;29(3):339–350. doi: 10.1016/j.thorsurg.2019.03.011. [DOI] [PubMed] [Google Scholar]
- 38.Baby B, Singh R, Suri A, Dhanakshirur RR, Chakraborty A, Kumar S, Kalra PK, Banerjee S. A review of virtual reality simulators for neuroendoscopy. Neurosurg Rev. 2020;43(5):1255–1272. doi: 10.1007/s10143-019-01164-7. [DOI] [PubMed] [Google Scholar]
- 39.Khan R, Plahouras J, Johnston BC, Scaffidi MA, Grover SC, Walsh CM. Virtual reality simulation training in endoscopy: a Cochrane review and meta-analysis. Endoscopy. 2019;51(7):653–644. doi: 10.1055/a-0894-4400. [DOI] [PubMed] [Google Scholar]
- 40.Cao C, Cerfolio RJ. Virtual or Augmented Reality to Enhance Surgical Education and Surgical Planning. Thorac Surg Clin. 2019;29(3):329–337. doi: 10.1016/j.thorsurg.2019.03.010. [DOI] [PubMed] [Google Scholar]
- 41.Alsayegh A, Bakhaidar M, Winkler-Schwartz A, Yilmaz R, Del Maestro RF. Best Practices Using Ex Vivo Animal Brain Models in Neurosurgical Education to Assess Surgical Expertise. World Neurosurg. 2021;155:e369–e381. doi: 10.1016/j.wneu.2021.08.061. [DOI] [PubMed] [Google Scholar]
- 42.Barsness KA. Achieving expert performance through simulation-based education and application of mastery learning principles. Semin Pediatr Surg. 2020;29(2):150904–150904. doi: 10.1016/j.sempedsurg.2020.150904. [DOI] [PubMed] [Google Scholar]
- 43.Villanueva C, Xiong J, Rajput S. Simulation-based surgical education in cardiothoracic training. ANZ J Surg. 2020;90(6):978–983. doi: 10.1111/ans.15593. [DOI] [PubMed] [Google Scholar]
- 44.Krajcer Z. Artificial Intelligence for Education, Proctoring, and Credentialing in Cardiovascular Medicine. Tex Heart Inst J. 2022;49(2):e217572. doi: 10.14503/THIJ-21-7572. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Harmon J, Pitt V, Summons P, Inder KJ. Use of artificial intelligence and virtual reality within clinical simulation for nursing pain education: A scoping review. Nurse Educ Today. 2021;97:104700–104700. doi: 10.1016/j.nedt.2020.104700. [DOI] [PubMed] [Google Scholar]
- 46.Lu J, Cuff RF, Mansour MA. Simulation in surgical education. Am J Surg. 2021;221(3):509–514. doi: 10.1016/j.amjsurg.2020.12.016. [DOI] [PubMed] [Google Scholar]
- 47.Dhombres F, Bonnard J, Bailly K, Maurice P, Papageorghiou AT, Jouannic JM. Contributions of Artificial Intelligence Reported in Obstetrics and Gynecology Journals: Systematic Review. J Med Internet Res. 2022;24(4):e35465. doi: 10.2196/35465. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Mouloodi S, Rahmanpanah H, Burvill C, Martin C, Gohari S, Davies HMS. In: Biomedical Visualisation. Rea PM, editor. Vol. 1356. Advances in Experimental Medicine and Biology; Cham; Springer: How Artificial Intelligence and Machine Learning Is Assisting Us to Extract Meaning from Data on Bone Mechanics? pp. 195–221. [DOI] [PubMed] [Google Scholar]
- 49.Hechi M, Ward TM, An GC, Maurer LR, El Moheb M, Tsoulfas G, Kaafarani HM. Artificial Intelligence, Machine Learning, and Surgical Science: Reality Versus Hype. J Surg Res. 2021;264:A1–A9. doi: 10.1016/j.jss.2021.01.046. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
All data sets were generated or analyzed in the current study