Abstract
Background
Emergency departments (EDs) have had to cope with various pandemics, such as HIN1, Ebola and the currently ongoing COVID-19. This study aimed to determine the elements of the new norm that has introduced changes into healthcare systems, particularly EDs, during the COVID-19 pandemic and to obtain consensus from the experts, the Emergency physicians in EDs across Malaysia. No previous study has been conducted on this topic.
Methods
This study used the fuzzy Delphi method (FDM) to acquire expert consensus. There were two phases in this study. The first involved extracting the elements to be assessed by the selected experts from a literature review. Three major domains were considered: infrastructure, governance and human resources. A total of 35 items were identified and divided into the three domains. In the second phase, the selected items were sent to a group of 15 ED physicians, who were asked to rate the items on a Likert-type scale. The data were then analysed using FDM.
Results
A total of 35 items were identified as possible new norms from a literature search for the three domains (governance, infrastructure and human resources). The first step of the FDM analysis showed that 9 out of the 35 items did not fulfil the initial requirement of the FDM, since the threshold value (d) must be lower than 0.2 (d </ 0.2). In meeting the second condition for the FDM, 25 out of the 35 items had an expert consensus of > 75%. Regarding the third requirement for FDM, only 1 out of the 35 items did not meet the criteria of an average fuzzy number (A value) of > 0.5. Finally, 25 items fulfilled all three requirements of FDM, so these were retained and the remaining 10 items were discarded.
Conclusion
The FDM used in this study had identified 25 items achieved the required level of agreement by the chosen experts. The results of this study can be used to guide EDs in Malaysia to utilise the new norms items in mitigating major outbreak affecting the ED services.
Keywords: new norms, emergency departments, COVID-19, pandemic, Fuzzy Delphi
Introduction
COVID-19 is a global infectious disease, with its first outbreak reported in Wuhan, China. COVID-19 infection has caused millions of deaths worldwide, leading the World Health Organization (WHO) to declare a pandemic. The rapid spread of the pandemic is a ramification of human movement and global communication. To date, COVID-19 has remained active, costing the world in various ways, including human lives, the economy, travel and healthcare capacity (1).
The COVID-19 pandemic has impacted and exposed the limitations of healthcare systems, especially in their management and delivery of treatment. In particular, it has challenged the global healthcare system’s capacity to prepare for and respond to infectious diseases. The success of healthcare systems in managing the pandemic has largely depended on their organisation, coordination and governance. Therefore, the lessons learned during the COVID-19 pandemic can strengthen healthcare systems’ preparedness to respond and combat emerging infectious diseases in the future. Coping with the pandemic has affected and changed existing healthcare systems worldwide, particularly in terms of their infrastructure, governance and human resources (2). Changes made during the COVID-19 pandemic have been maintained as preventive measures and control strategies to contain the constantly evolving pandemic disease.
During the COVID-19 pandemic, the new norms practiced can be major glitches faced by emergency department (ED) employees (3). The elements of the new norm mainly impacted EDs and involved screening, containing and alerting the nation about infectious diseases. Attempts to prevent the transmission of the disease before it became a pandemic were made. EDs have experienced various outbreaks, such as SARS, H1N1 and COVID-19; therefore, EDs should maintain the changes they have adopted to establish well-prepared systems for coping with future outbreaks (4). This study aimed to determine the elements of the new norm that has introduced changes into the healthcare system, particularly in EDs, during the COVID-19 pandemic. It also aimed to obtain consensus from experts, namely, emergency physicians from across Malaysia, by using the fuzzy Delphi method (FDM). FDM was selected because it is significantly less taxing to the experts in comparison to the traditional Delphi method (DM). Additionally, FDM utilises a more objective quantitative analysis than traditional DM (5, 6). To date, no previous study has explored this topic.
Methods
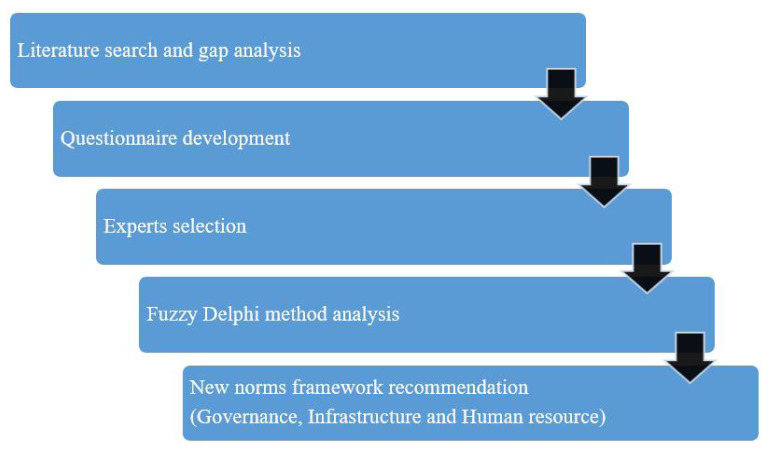
FDM was used in this study to effectively acquire expert consensus (Figure 1). This study has two phases as follows:
Figure 1.
Flow chart of study
Phase 1
Phase 1 involved identifying domains and elements to be assessed and validated by selected experts from a literature review. The domains were selected based on the investigator’s clinical experience at a study centre and after interviewing an experienced emergency physician on the floor. Three major domains were identified: i) infrastructure, ii) governance and iii) human resources. Governance describes the process through which an administration or organisation can consolidate its workflow management by implementing standards, rules and guidelines to achieve objectives simultaneously. Infrastructure refers to treatment facilities. In the COVID-19 context, the designated space includes severe acute respiratory distress isolation rooms, fever centres, negative-pressure airborne isolation rooms and spaces for managing critical and non-critical cases for people under investigation and COVID-19-positive patients. Lastly, human resources include the management of healthcare staff and in the context of this study, they include those working in EDs in Malaysia during the COVID-19 pandemic. FDM elements of assessment are identified based on a rapid review and evidence-based information obtained from sources such as Google Scholar, PubMed Central and the Cochrane Library. Thirty-five items were identified and divided according to their domains. They were sent to Scribendi for English academic editing. The items were then given to a group of three emergency physicians for review and validation based on the research objectives and questions. These emergency physicians were selected based on their expertise and clinical experience. The criteria for selecting an expert for inclusion in the study were as follows:
The emergency physicians were working in the ED of Hospital Universiti Sains Malaysia.
The emergency physicians had more than 10 years of working experience in their respective specialties.
The emergency physicians had experience in managing cases of COVID-19 and severe acute respiratory infection.
The investigator discussed and reviewed all 35 items with the experts individually. Certain elements required modification for content and wording, whereas others must be eliminated or exchanged with other elements for valid reasons as provided by the experts. Finally, the 35 items were modified and prepared in Google Forms. Additional questions inquired about information such as the number of isolation rooms, bed status and current practices.
Phase 2
Phase 2 of the study involved 15 experts as guided by the FDM, requiring 10–15 respondents. The study was conducted over 3 months, from September 2021 to November 2021. The 15 experts were selected based on their experience in their respective specialties. The criteria for selecting an expert for this phase of this study included the following:
Emergency physicians working in Malaysia, with more than 5 years of experience in their respective specialties
Emergency physicians involved in the Ministry of Health Malaysia and Hospital Universiti Sains Malaysia
Emergency physicians with experience managing COVID-19 and severe acute respiratory infection cases
Emergency physicians who perform scholarly work on COVID-19 management and outbreaks
The items were distributed to the 15 emergency physicians from across Malaysia through Google Forms link via a text messaging platform, namely, WhatsApp or Telegram. Experts eligible according to the criteria were included and all consented to participate voluntarily. They were asked to assess and declare their level of agreement with the 35 items. These items were the ‘new norms’ introduced as changes in EDs in Malaysia during the COVID-19 pandemic. The participants were given 1 week to respond with an evaluation of the items. Table 1 illustrates the agreement level of seven levels of linguistic variables (Likert scoring) and the fuzzy scale. The fuzzy rating scale was introduced to cope with the imprecision of human thought and experience in measuring attitudes in many fields of study.
Table 1.
Level of agreement and fuzzy scale (7 points)
| Linguistic variables | Fuzzy scale |
|---|---|
| Not at all important | (0.0, 0.0, 0.1) |
| Low important | (0.0, 0.1, 0.3) |
| Slightly important | (0.1, 0.3, 0.5) |
| Somewhat important | (0.3, 0.5, 0.7) |
| Moderately important | (0.5, 0.7, 0.9) |
| Very important | (0.7, 0.9, 1.0) |
| Extremely important | (0.9, 1.0, 1.0) |
The linguistic variables of agreement in the Likert scale format were performed by each expert for each item. Then, these variables were translated into fuzzy number data and analysed in Microsoft Excel FDM software, version 2.0 using FDM as the data analysis technique.
Fuzzy Delphi Method Implementation Steps
Step 1: Selection of Experts
In the selection of experts, satisfactory results can be obtained from small panels of 10–15 individuals from a homogenous group of experts (7).
The definition of expert will vary depending on the context and field of interest to which FDM will be applied. Being an expert in a particular field entails the acquisition of experience, special skills and knowledge of that particular subject. In this context, the selection of experts was as described above.
Step 2: Conversion of Linguistic Variables into Triangular Fuzzy Numbers
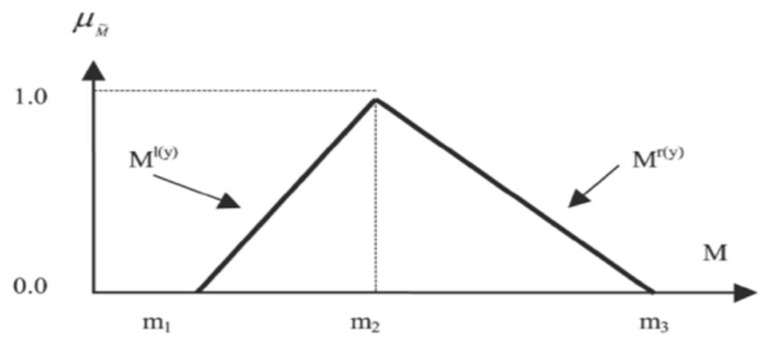
The next step involves converting all the linguistic variables into triangular fuzzy numbers. A triangular fuzzy number represents the values of m1, m2 and m3 indicating the minimum, reasonable and maximum values, respectively. Figure 2 illustrates the m1, m2 and m3 values for a triangular fuzzy number. A triangular fuzzy number is used to convert a fuzzy scale (which is similar to a Likert scale). Then, a fuzzy scale is used to convert linguistic variables into fuzzy numbers.
Figure 2.
Triangular fuzzy number
Step 3: Identifying the Value of Threshold d
The next step involves identifying the value of threshold d. The threshold value is particularly important in the process of identifying the agreement level among the experts. To obtain expert agreement on each item, d must not exceed 0.2 (d < 0.2) (8). If d is less than 0.2 (d < 0.2), then all the experts have reached an agreement on an item. Otherwise, a second round should be conducted to consider whether the item is needed or not. This condition is the first requirement that needs to be met for FDM.
The threshold value (d) was calculated as follows:
| (Equation 1) |
Step 4: Determining Experts’ Agreement Level
The second requirement for the FDM involves determining whether the experts’ agreement is greater than or equal to 75% for each item (9). If the percentage of experts’ agreement is greater than or equal to 75% for an item, then that item can be assumed to achieve expert agreement. The percentage of expert agreement can be calculated by using the following formula:
| (Equation 2) |
Step 5: Consensus of Experts for Receiving an Item
The third criterion required for FDM is the α-cut. If α-cut is greater than or equal to 0.5 (10) then the item will be accepted as it shows the consensus of experts on receiving the item. The calculation and determination of the fuzzy values are determined as follows:
| (Equation 3) |
If A is more than the α-cut value of 0.5, then the item will be accepted as it shows the consensus of the expert on retaining the item.
Step 6: Ranking an Item
This step ranks the items into sub-phases. The ranking steps are determined by selecting an item based on its defuzzification value obtained from experts’ agreement. The item with the most important ranking in the model has the highest value.
Results
Thirty-five items were identified for the new norms from a literature search of all three domains (governance, infrastructure and human resources) (Table 2). All the items were initially scored based on linguistic variables (Likert scale scoring) and these scores were converted into fuzzy numbers. The fuzzy numbers were recorded, and average m1, m2 and m3 values were calculated. The higher the fuzzy number value, the higher the level of agreement. The value of the threshold d was obtained by Equation 1. Nine of the 35 items did not meet the first requirement for FDM as the threshold value d must be less than 0.2 (d < 0.2).
Table 2.
Initial items obtained from the literature review before FDM analysis
| Domain | New norm element/item description (NN) |
|---|---|
|
| |
| Governance (G) | |
| NNG-1 | Usage of proper personal protective equipment (PPE) is compulsory during the triaging process. |
| NNG-2 | The creation of a screening process (questionnaire) to aid in clinical triaging of COVID-19 and facilitating zone disposition based on PPE requirements. |
| NNG-3a | Conducting a questionnaire-based self-reporting screening process of COVID-19 on patients and family members or caretakers before they enter the ED. |
| NNG-3b | Screening patients and family members or caretakers before they enter the ED using COVID-19 rapid test kits (RTK). |
| NNG-3c | Screening patients and family members or caretakers before they enter the ED using a questionnaire-based self-reporting and COVID-19 RTK. |
| NNG-4 | Screening for COVID-19 symptoms and measuring temperature of all visitors at the ED entrance. |
| NNG-5 | Healthcare workers performing aerosol-generating procedures (such as intubation) must use an aerosol box to minimise the spread of COVID-19. |
| NNG-6 | Standard PPE worn by healthcare workers when attending to patients without COVID-19. |
| NNG-7a | PPE: A facial shield or eye protection (goggles), a surgical mask and gloves The standard PPE for aerosol-generating procedures (such as intubation) includes a powered air-purifying respirator (PAPR), N95 mask, boot covers and gloves. |
| NNG-7b | The standard PPE for aerosol-generating procedures (such as intubation) includes a disposable isolation gown suit (coveralls suit), a face shield, an N95 mask, boot covers, and gloves. |
| NNG-8 | A standard intubation checklist for suspected and confirmed patients with COVID-19. |
| NNG-9 | Using an isolation pod (ISOPOD) to transfer suspected and confirmed patients with COVID-19. |
| NNG-10 | Developing teleconsultation helpline services at the ED to facilitate the screening and triaging process of suspected, probable or confirmed patients with COVID-19. |
| NNG-11 | A computerised system or manual clerking sheet template with the checklist method to augment the speed and efficiency of management. |
| NNG-12 | Establishing standard operational protocols or guidelines on training and clinical management of COVID-19 and updating it promptly. |
| NNG-13 | Developing a guideline for the ED on COVID-19 preparedness and response strategy at the hospital level. |
|
| |
| Infrastructure (I) | |
|
| |
| NNI-14a | Designated negative pressure system cabins or tents for fever centre/acute respiratory influenza-like illness outside of the ED. |
| NNI-14b | Designated cabins or tents without a negative pressure system for fever centre/acute respiratory influenza-like illness outside of the ED. |
| NNI-15 | Restructuring a respiratory and non-respiratory zone within the ED with separate access and exit points. |
| NNI-16a | Establishing a negative pressure isolation room for suspected, probable or confirmed COVID-19 cases with separate access and exit points. |
| NNI-16b | Establishing an isolation room without a negative pressure system for suspected, probable or confirmed COVID-19 cases with separate access and exit points. |
| NNI-17 | Establishing a separate resuscitation area for non-COVID-19 cases with separate access and exit points. |
| NNI-18 | A designated PPE donning/doffing area in the ED. |
| NNI-19 | A designated portable X-ray room in the ED. |
| NNI-20 | The isolation area should have dedicated washrooms, hand-washing stations and trash bins. |
| NNI-21 | Creating predetermined transport routes to transfer patients with COVID-19 to minimise exposure. |
| NNI-22 | During access block, establish an observation ward for suspected, probable, or confirmed COVID-19 and non-COVID-19 cases. |
|
| |
| Human resources (HR) | |
|
| |
| NNHR-23 | Setting up a COVID-19 team and rotating the team occasionally to minimise the risk of COVID-19 transmission. |
| NNHR-24 | Interdepartmental recruitment of a COVID-19 team within the hospital to manage suspected, probable, or confirmed patients with COVID-19 in the ED. |
| NNHR-25 | Frequent training of healthcare workers on performing nasopharyngeal swabs, donning and doffing PPE. |
| NNHR-26 | To ensure safety, high-risk healthcare workers (workers with pre-existing comorbidities and pregnancy) should work in a non-COVID-19 zone. |
| NNHR-27 | Active surveillance of COVID-19 risk in emergency healthcare workers upon arrival at work. |
| NNHR-28 | Active mental health surveillance on emergency healthcare workers during the pandemic. |
| NNHR-29 | Providing hospital scrubs to all healthcare workers working in the respiratory zone. |
| NNHR-30 | The ED team conducts close contact tracing of suspected or confirmed COVID-19 cases among healthcare workers. |
In the second requirement for FDM, 20 of the 35 items had an expert consensus of > 75%. For the third requirement, only one item did not meet the criterion for an average fuzzy number (A value) of > 0.5. Finally, in this study, only 25 items met all three requirements of FDM and were therefore retained, whereas the remaining 10 items were discarded. The final step was defuzzification performed during the data analysis using the FDM technique. The defuzzification step determines the ranking of each item. Supplementary Table 1 summarises all three domains after analysing the findings of FDM for the new norm elements in the EDs in Malaysia during the COVID-19 pandemic. Approximately 30% (n = 5), 18% (n = 2) and 25% (n = 2) of the items were finally discarded for governance, infrastructure and human resource domains, respectively. Supplementary Table 2 shows the detailed descriptions of each item and their ranking of acceptance based on the FDM criteria (Supplementary Tables 1 and 2 files)
Discussion
This study obtains experts’ consensus on the findings of the new norm items in EDs in Malaysia during the COVID-19 pandemic. The findings of this study showed that the retained items should form the new norms in EDs during the COVID-19 pandemic as these items have all obtained expert consensus. The retained items can be used to develop guidelines as the FDM findings involved all experts’ opinions. Certain experts have the authority to develop protocols in the field, whereas others are more experienced and knowledgeable.
In the area of governance, this study obtained expert consensus on 11 items to be retained, with the remaining five to be discarded. Among the top three rankings of the retained items, the experts have reached an agreement to establish ED guidelines for COVID-19 preparedness and response strategy to be applied at the hospital level. This study also found that the operational planning and development of emergency response protocols will better prepare EDs for the pandemic and any future outbreaks (11). A pandemic crisis such as COVID-19 requires a preparedness plan to manage disasters in the short and long term (12). Furthermore, the top-ranked item includes the use of standard personal protective equipment (PPE) for aerosol-generating procedures (such as intubation). The PPE should include a disposable isolation gown suit, a face shield, an N95 mask, boot covers and gloves. Although a powered air-purifying respirator provides greater protection than the standard PPE, the standard PPE for aerosol-generating procedures is top-ranked by experts due to several reasons, such as the availability of the device and cost-effectiveness. According to the Centers for Disease Control and Prevent, respirators with N95 filters or higher are used for all aerosol-generating procedures, consistent with the study’s findings (13). The third-ranked item involves establishing standard operational procedures for the training and clinical management of COVID-19 and updating them regularly. Based on expert consensus, the discarded elements include the use of an aerosol box to minimise the spread of COVID-19 when performing aerosol-generating procedures (such as intubation) and an isolation pod to transfer COVID-19 patients and the development of a teleconsultation helpline service. Evidence for the effectiveness of the aerosol box or any barriers is currently insufficient and suggests that they may bring additional risks (14). However, teleconsultation has gained significant visibility in many countries, particularly in Western countries. Currently, it has been used in previous epidemics, such as Ebola and SARS. Teleconsultation aims to prevent disease transmission, reduce patient volume and load, and provide psychosocial support services. Thus, health authorities in several countries have already implemented telemedicine user guidelines to provide support during the pandemic (15). Implementing teleconsultation would be helpful in the clinical setting, particularly during the pandemic (16). Based on this study, we should consider adopting teleconsultation in EDs.
Eleven items for infrastructure were initially extracted from the literature search. Following the FDM analysis, nine items were retained, whereas two were not accepted by the expert consensus. The items retained include designating respiratory and non-respiratory zones in EDs with separate entrance and exit points, an isolation room with or without negative pressure for COVID-19 patients with separate entrance and exit points, PPE donning/doffing area in EDs, predetermined transport routes to transfer COVID-19 patients to minimise exposure, and other elements as stated in Supplementary Table 1. Some of the emergency physicians stated that their EDs had a minimum of 1–5 isolation rooms without negative pressure or a bay with a minimum 5–60-bed capacity. For the negative-pressure isolation rooms, a minimum of 1–5 rooms were required with a 1–12-bed capacity. Most EDS in Malaysia are not equipped with negative-pressure isolation rooms due to their high cost. Building negative-pressure isolation rooms is one of the ideal ways of controlling the spread of infectious respiratory diseases to prevent the transmission of airborne infections (17). In Middle Eastern countries, health ministries have mandated certain hospitals to designate a separate respiratory zone after the 2012 Middle East respiratory syndrome coronavirus (MERS-CoV) outbreak to prevent mixing infected patients (18, 19). In the future, hospitals with more treatment spaces designated for infectious diseases in the ED should be built. For the discarded elements, cabins or tents with and without a negative-pressure system for fever centre/acute respiratory influenza-like illnesses designated outside of EDs were unfavourable among the experts. The lack of treatment spaces in EDs leads to restructuring and reconverting other available spaces into COVID-19 treatment areas. In other places, patients are triaged and screened based on presenting complaints and risk stratification of COVID-19 into the respiratory and non-respiratory zones (20).
The human resources group had eight items: three were discarded and the remaining five were retained. After the defuzzification step, the top three priority items were regular training of healthcare workers on performing nasopharyngeal swabs and PPE donning/doffing, providing hospital scrubs to all healthcare workers in the respiratory zone, and conducting close contact tracing by the ED team of suspected and confirmed COVID-19 cases among its healthcare workers. Nasopharyngeal or oropharyngeal swabs remain the gold standard for diagnosing COVID-19, and improper techniques for collecting COVID-19 samples can lead to false-negative COVID-19 results. Therefore, training sessions in swabbing techniques improve sampling techniques, knowledge and confidence (21). PPE training is essential to protecting healthcare workers, especially during pandemics. A recent study investigated whether the frequent use of incorrect steps when donning and doffing PPE was a risk for contamination. It revealed that suboptimal training and education are significant contributing factors (22). Another recent study showed that contamination while removing PPE is significant. Hence, preventive measures, such as intensive and repeated training, interactive audio-visuals, and the assistance of trained personnel during donning and doffing, should be conducted frequently (23). Providing hospital scrubs to all healthcare workers in the respiratory zone can prevent disease transmission among them (24). The other retained items for the human resource management domain are interdepartmental recruitment and rotation. They will solve the issues of work scheduling, redeployment and staff shortages. Frequent training programmes and strict standard operating procedures on the use of PPE will ensure adherence to infection control and staff safety. Health surveillance mechanisms must be established to monitor and ensure mental and physical well-being throughout the pandemic.
Different healthcare systems may have different priorities for the items to be included, depending on local settings or as suited to their particular needs. Each ED must respond in various ways depending on the features of infectious diseases and the surge of cases. At the early stage, whether a variant can be super-spreading in a short period, such as the COVID-19 pandemic, cannot be determined. The implications of this pandemic have introduced drastic changes to EDs. The changes made during the COVID-19 pandemic have been maintained as preventive measures and control strategies to contain the constantly evolving pandemic disease.
Thus, FDM can be used to develop guidelines, standard protocols and optimal workflows by achieving consensus among experts. FDM is also advantageous because it ranks items, indicating the relative importance of the selected elements, whereas unfit elements are discarded based on expert consensus. Therefore, one may select the best items suited for one’s needs based on the ranking priority as one size may not fit all. Selecting experts who have had significant experience with the intervention approach and having a balanced number of experts with a similar job scope will help to improve the validity of these findings. FDM has been, and will continue to be, an important data collection methodology with various applications and uses for people who aim to gather expert information on a particular subject (25). Expert opinions and involvement in various dimensions positively impact the formation of guidelines.
Limitation of Study
A weakness in the FDM includes the constant reminders needed before the experts can provide their responses. At the same time, the experts’ views may have been limited to their perspectives and experience and thus may not have represented the views of the entire fraternity. In addition, no comments were given by the experts to explain their low scale scores for certain elements as FDM is based on the Likert-type scale scoring without any request to explain the reason for the answer.
Conclusion
The impact of COVID-19 has led to the introduction of extraordinarily new norms and has reshaped our daily workflow; no one can predict how long a pandemic will last. The current standards of practice, which were previously rare, are being adapted well. The findings of this study are based on the expert consensus. Twenty-five items within the domains of governance, infrastructure and human resource management were accepted by expert consensus and met all three requirements of FDM. The three domains cover strict adherence to infection control and screening mechanisms. The experts also agreed that ensuring staff well-being during outbreaks is a crucial item that was retained within the domain of human resource management. Hence, this consensus would provide helpful guidelines for implementation in EDs when managing the COVID-19 pandemic or other newly emerging infectious diseases.
Acknowledgements
The authors would like to express sincere gratitude to all the Emergency Physicians in Malaysia involved in this study for their support and assistance in this research.
Appendix
Supplementary Table 1.
Summary of all three domains after Fuzzy Delphi analysis findings for the new norm elements in ED in Malaysia during the COVID-19 pandemic
| No. | Items/Elements | Threshold value, D < 0.2 | Percentage of expert consensus, % | Average of fuzzy numbers (A value) | Ranking | Verdict |
|---|---|---|---|---|---|---|
| Domain: Governance | ||||||
| 1 | NNG-1 | 0.094 | 93.3% | 0.909 | 6 | Retained |
| 2 | NNG-2 | 0.111 | 86.7% | 0.911 | 5 | Retained |
| 3 | NNG-3a | 0.138 | 93.3% | 0.898 | 9 | Retained |
| 4 | NNG-3b | 0.425 | 33.33% | 0.613 | 15 | Discarded |
| 5 | NNG-3c | 0.383 | 40.00% | 0.638 | 14 | Discarded |
| 6 | NNG-4 | 0.094 | 93.33% | 0.909 | 6 | Retained |
| 7 | NNG-5 | 0.377 | 40.00% | 0.371 | 16 | Discarded |
| 8 | NNG-6 | 0.068 | 100.00% | 0.933 | 3 | Retained |
| 9 | NNG-7a | 0.252 | 86.67% | 0.818 | 11 | Retained |
| 10 | NNG-7b | 0.060 | 100.00% | 0.940 | 1 | Retained |
| 11 | NNG-8 | 0.094 | 93.33% | 0.909 | 6 | Retained |
| 12 | NNG-9 | 0.402 | 46.67% | 0.642 | 13 | Discarded |
| 13 | NNG-10 | 0.290 | 60.00% | 0.742 | 12 | Discarded |
| 14 | NNG-11 | 0.094 | 100.00% | 0.878 | 10 | Retained |
| 15 | NNG-12 | 0.068 | 100.00% | 0.933 | 3 | Retained |
| 16 | NNG-13 | 0.060 | 100.00% | 0.940 | 1 | Retained |
| DOMAIN: INFRASTRUCTURE | ||||||
| 1 | NNI-14a | 0.321 | 53.3% | 0.738 | 10 | Discarded |
| 2 | NNI-14b | 0.410 | 40.0% | 0.716 | 11 | Discarded |
| 3 | NNI-15 | 0.116 | 93.3% | 0.909 | 4 | Retained |
| 4 | NNI-16a | 0.155 | 93.33% | 0.873 | 6 | Retained |
| 5 | NNI-16b | 0.186 | 93.33% | 0.829 | 9 | Retained |
| 6 | NNI-17 | 0.244 | 86.67% | 0.842 | 8 | Retained |
| 7 | NNI-18 | 0.089 | 93.33% | 0.922 | 1 | Retained |
| 8 | NNI-19 | 0.183 | 93.33% | 0.860 | 7 | Retained |
| 9 | NNI-20 | 0.076 | 100.00% | 0.920 | 2 | Retained |
| 10 | NNI-21 | 0.076 | 100.00% | 0.913 | 3 | Retained |
| 11 | NNI-22 | 0.131 | 93.33% | 0.878 | 5 | Retained |
| DOMAIN: HUMAN RESOURCE | ||||||
| 1 | NNHR-23 | 0.409 | 20.0% | 0.647 | 8 | Discarded |
| 2 | NNHR-24 | 0.291 | 66.7% | 0.704 | 6 | Discarded |
| 3 | NNHR-25 | 0.087 | 100.0% | 0.896 | 1 | Retained |
| 4 | NNHR-26 | 0.373 | 40.00% | 0.662 | 7 | Discarded |
| 5 | NNHR-27 | 0.197 | 93.33% | 0.842 | 4 | Retained |
| 6 | NNHR-28 | 0.145 | 93.33% | 0.829 | 5 | Retained |
| 7 | NNHR-29 | 0.173 | 93.33% | 0.878 | 2 | Retained |
| 8 | NNHR-30 | 0.119 | 93.33% | 0.864 | 3 | Retained |
Notes: Threshold value (d) < 0.2 (three decimal points is accepted); Percentage expert consensus agreement > 75%; Average fuzzy value (A value ) > 0.5; All three must be fulfilled for the elements to be retained
Supplementary Table 2.
Summary of all three domains after Fuzzy Delphi analysis findings for the new norm elements in ED in Malaysia during the COVID-19 pandemic
| Domain | New norm element/item description (NN) | Verdict | Ranking |
|---|---|---|---|
|
| |||
| Governance (G) | |||
| NNG-1 | Usage of proper Personal Protective Equipment (PPE) is compulsory during the triaging process. | Retained | 6 |
| NNG-2 | The creation of a screening process (questionnaire) to aid in clinical triaging of COVID-19 and facilitating zone disposition based on PPE requirements. | Retained | 5 |
| NNG-3a | Conducting a questionnaire-based self-reporting screening process of COVID-19 on patients and family members or caretakers before they enter the emergency department (ED). | Retained | 9 |
| NNG-3b | Screening patients and family members or caretakers before they enter the ED using COVID-19 rapid test kits (RTK). | Discarded | 15 |
| NNG-3c | Screening patients and family members or caretakers before they enter the ED using a questionnaire-based self-reporting and COVID-19 rapid test kits (RTK). | Discarded | 14 |
| NNG-4 | Screening for COVID-19 symptoms and measuring the temperature of all visitors at the ED entrance. | Retained | 6 |
| NNG-5 | Healthcare workers performing aerosol-generating procedures (such as intubation) must use an aerosol box to minimise the spread of COVID-19. | Discarded | 16 |
| NNG-6 | Standard PPE worn by healthcare workers when attending to patients without COVID -19. PPE: A facial shield or eye protection (goggles), a surgical mask and gloves. | Retained | 3 |
| NNG-7a | The standard PPE for aerosol-generating procedures (such as intubation) includes a powered air-purifying respirator (PAPR), N95 mask, boot covers, and gloves. | Retained | 11 |
| NNG-7b | The standard PPE for aerosol-generating procedures (such as intubation) includes a disposable isolation gown suit (coveralls suit), a face shield, an N95 mask, boot covers, and gloves. | Retained | 1 |
| NNG-8 | A standard intubation checklist for suspected and confirmed patients with COVID-19. | Retained | 6 |
| NNG-9 | Using an isolation pod (ISOPOD) to transfer suspected and confirmed patients with COVID-19. | Discarded | 13 |
| NNG-10 | Developing teleconsultation helpline services at the ED to facilitate the screening and triaging process of suspected, probable, or confirmed patients with COVID-19. | Discarded | 12 |
| NNG-11 | A computerised system or manual clerking sheet template with the checklist method augments the speed and efficiency of management. | Retained | 10 |
| NNG-12 | Establishing standard operational protocols or guidelines on training and clinical management of COVID-19 and updating it promptly. | Retained | 3 |
| NNG-13 | Developing a guideline for the ED on COVID-19 preparedness and response strategy at the hospital level. | Retained | 1 |
|
| |||
| Infrastructure | |||
|
| |||
| NNI-14a | Designated negative pressure system cabins or tents for fever centre/acute respiratory influenza-like illness outside of the ED. | Discarded | 10 |
| NNI-14b | Designated cabins or tents without a negative pressure system for fever centre/acute respiratory influenza-like illness outside of the ED. | Discarded | 11 |
| NNI-15 | Restructuring a respiratory and non-respiratory zone within the ED with separate access and exit points. | Retained | 4 |
| NNI-16a | Establishing a negative pressure isolation room for suspected, probable, or confirmed COVID-19 cases with separate access and exit points. | Retained | 6 |
| NNI-16b | Establishing an isolation room without a negative pressure system for suspected, probable, or confirmed COVID-19 cases with separate access and exit points. | Retained | 9 |
| NNI-17 | Establishing a separate resuscitation area for non-COVID-19 cases with separate access and exit points. | Retained | 8 |
| NNI-18 | A designated PPE donning/ doffing area in the ED | Retained | 1 |
| NNI-19 | A designated portable X-ray room in the ED. | Retained | 7 |
| NNI-20 | The isolation area should have dedicated washrooms, hand-washing stations, and trash bins. | Retained | 2 |
| NNI-21 | Creating predetermined transport routes to transfer patients with COVID-19 to minimise exposure. | Retained | 3 |
| NNI-22 | During access block, establish an observation ward for suspected, probable, or confirmed COVID-19 and non-COVID-19 cases. | Retained | 5 |
|
| |||
| Human resources (HR) | |||
|
| |||
| NNHR-23 | Setting up a COVID-19 team and rotating the team occasionally to minimise the risk of COVID-19 transmission. | Discarded | 8 |
| NNHR-24 | Interdepartmental recruitment of a COVID-19 team within the hospital to manage suspected, probable, or confirmed patients with COVID-19 in the ED. | Discarded | 6 |
| NNHR-25 | Frequent training of healthcare workers on performing nasopharyngeal swabs, donning and doffing PPE. | Retained | 1 |
| NNHR-26 | To ensure safety, high-risk healthcare workers (workers with pre-existing comorbidities and pregnancy) should work in a non-COVID-19 zone. | Discarded | 7 |
| NNHR-27 | Active surveillance of COVID-19 risk in emergency healthcare workers upon arrival at work. | Retained | 4 |
| NNHR-28 | Active mental health surveillance on emergency healthcare workers during the pandemic. | Retained | 5 |
| NNHR-29 | Providing hospital scrubs to all healthcare workers working in the respiratory zone. | Retained | 2 |
| NNHR-30 | The ED team conducts close contact tracing of suspected or confirmed COVID-19 cases among healthcare workers. | Retained | 3 |
Footnotes
Ethics of Study: All the authors effort and process of conduct of the study complied with international and local rules and guidelines of research work ethics based on Helsinki Declaration.
Conflict of Interest: None.
Funds: None.
Authors’ Contributions: Conception and design: JRS, NHNAR
Analysis and interpretation of the data: JRS
Drafting of the article: NHNAR
Critical revision of the article for important intellectual content: NHNAR
Final approval of the article: NHNAR
Provision of study materials or patients: JRS
Statistical expertise: JRS
Administrative, technical or logistic support: NHNAR
Collection and assembly of data: JRS
References
- 1.Shrestha N, Shad MY, Ulvi O, Khan MH, Karamehic-Muratovic A, Nguyen USD, et al. The impact of COVID-19 on globalization. One Health. 2020;11:100180. doi: 10.1016/j.onehlt.2020.100180. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Legido-Quigley H, Mateos-García JT, Campos VR, Gea Sánchez M, Muntaner C, McKee M. The resilience of the Spanish health system against the COVID-19 pandemic. Lancet Public Health. 2020;5(5):e251–e252. doi: 10.1016/S2468-2667(20)30060-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Sutherland K, Chessman J, Zhao J, Sara G, Shetty A, Smith S, et al. Impact of COVID-19 on healthcare activity in NSW, Australia. Public Health Res Pract. 2020;30(4):3042030. doi: 10.17061/phrp3042030. [DOI] [PubMed] [Google Scholar]
- 4.Nadarajan GD, Omar E, Abella BS, Hoe PS, Do Shin S, Ma MHM, et al. A conceptual framework for ED design in a pandemic. Scand J Trauma Resusc Emerg Med. 2020;28(1):1–13. doi: 10.1186/s13049-020-00809-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Lin GSS, Chin YJ, Chong RS, Baharin F, Syed Saadun Tarek Wafa SWW, Dziaruddin N. Expert consensus on relevant topics for undergraduate paediatric dental curriculum using the fuzzy Delphi method: a new direction for Malaysian dental education. BMC Oral Health. 2023;23(1):452. doi: 10.1186/s12903-023-03130-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Sulaiman HF, Ismail R, Mohd Yusoff H, Anuar N, Mohd Jamil MR, Daud F. Validation of occupational zoonotic disease questionnaire using fuzzy Delphi method. J Agromedicine. 2020;25(2):166–172. doi: 10.1080/1059924X.2019.1666763. [DOI] [PubMed] [Google Scholar]
- 7.Chu HC, Hwang GJ. A Delphi-based approach to developing expert systems with the cooperation of multiple experts. Expert Syst Appl. 2008;34(4):2826–2840. doi: 10.1016/j.eswa.2007.05.034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Cheng CH, Lin Y. Evaluating the best main battle tank using fuzzy decision theory with linguistic criteria evaluation. Eur J Oper Res. 2002;142(1):174–186. doi: 10.1016/S0377-2217(01)00280-6. [DOI] [Google Scholar]
- 9.Bodjanova S. Median alpha-levels of a fuzzy number. Fuzzy Sets Syst. 2006;157(7):879–891. doi: 10.1016/j.fss.2005.10.015. [DOI] [Google Scholar]
- 10.Whiteside T, Kane E, Aljohani B, Alsamman M, Pourmand A. Redesigning ED operations amidst a viral pandemic. Am J Emerg Med. 2020;38(7):1448–1453. doi: 10.1016/j.ajem.2020.04.032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Schreyer KE, Daniel A, King LL, Blome A, DeAngelis M, Stauffer K, et al. ED management of the COVID-19 pandemic. J Emerg Med. 2020;59(6):946–951. doi: 10.1016/j.jemermed.2020.07.022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Centers for Disease Control and Prevention. Interim infection prevention and control recommendations for healthcare personnel during the coronavirus disease 2019 (COVID-19) pandemic [Internet] 2022. [Retrieved 17 January 2023] Available at: https://www.cdc.gov/coronavirus/2019.
- 13.Sorbello M, Rosenblatt W, Hofmeyr R, Greif R, Urdaneta F. Aerosol boxes and barrier enclosures for airway management in COVID-19 patients: a scoping review and narrative synthesis. British J Anaesth. 2020;125(6):880–894. doi: 10.1016/j.bja.2020.08.038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Baudier P, Kondrateva G, Ammi C, Chang V, Schiavone F. Patients’ perceptions of teleconsultation during COVID-19: a cross-national study. Technol Forecast Soc Change. 2021;163:120510. doi: 10.1016/j.techfore.2020.120510. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Thong HK, Wong DKC, Gendeh HS, Saim L, Athar PPBSH, Saim A. Perception of telemedicine among medical practitioners in Malaysia during COVID-19. J Med Life. 2021;14(4):468. doi: 10.25122/jml-2020-0119. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Kim H, Kim D, Paul C, Lee CK. The spatial allocation of hospitals with negative pressure isolation rooms in Korea: are we prepared for new outbreaks? Int J Health Policy Manage. 2020;9(11):475. doi: 10.34172/ijhpm.2020.118. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.AlAssaf W. Challenges in pandemic disaster preparedness: experience of a Saudi academic medical center. Disaster Med Public Health Prep. 2022;16(1):285–289. doi: 10.1017/dmp.2020.268. [DOI] [PubMed] [Google Scholar]
- 18.Yaffee AQ, Peacock E, Seitz R, Hughes G, Haun P, Ross M, et al. 2020. Preparedness, adaptation, and innovation: approach to the COVID-19 pandemic at a decentralized, quaternary care emergency department. West J Emerg Med. 2020;21(6):63–70. doi: 10.5811/westjem.2020.8.48624. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Cook TM, El-Boghdadly K, McGuire B, McNarry AF, Patel A, Higgs A. Consensus guidelines for managing the airway in patients with COVID-19: guidelines from the Difficult Airway Society, the Association of Anaesthetists the Intensive Care Society, the Faculty of Intensive Care Medicine and the Royal College of Anaesthetists. Anaesthesia. 2020;75(6):785–799. doi: 10.1111/anae.15054. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Abud BT, Hajnas NM, Redleaf M, Kerolus JL, Lee V. Assessing the impact of a training initiative for nasopharyngeal and oropharyngeal swabbing for COVID-19 testing. OTO Open. 2020;4(3):2473974X20953094. doi: 10.1177/2473974X20953094. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.John A, Tomas ME, Cadnum JL, Mana TS, Jencson A, Shaikh A, et al. Are health care personnel trained in correct use of personal protective equipment? Am J Infect Control. 2016;44(7):840–842. doi: 10.1016/j.ajic.2016.03.031. [DOI] [PubMed] [Google Scholar]
- 22.Lim SM, Cha WC, Chae MK, Jo IJ. Contamination during doffing of personal protective equipment by healthcare providers. Clin Exp Emerg Med. 2015;2(3):162. doi: 10.15441/ceem.15.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Quah LJJ, Tan BKK, Fua TP, Wee CPJ, Lim CS, Nadarajan G, et al. Reorganising the ED to manage the COVID-19 outbreak. Int J Emerg Med. 2020;13(1):1–11. doi: 10.1186/s12245-020-00294-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Habibi A, Jahantigh FF, Sarafrazi A. Fuzzy Delphi technique for forecasting and screening items. Asian J Res Business Econ Manage. 2015;5:130–143. doi: 10.5958/2249-7307.2015.00036.5. [DOI] [Google Scholar]
- 25.Gardashova L. Application of operational approaches to solving decision making problem using Z-numbers. Appl Math. 2014;5:1323–1334. doi: 10.4236/am.2014.59125. [DOI] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplementary Table 1.
Summary of all three domains after Fuzzy Delphi analysis findings for the new norm elements in ED in Malaysia during the COVID-19 pandemic
| No. | Items/Elements | Threshold value, D < 0.2 | Percentage of expert consensus, % | Average of fuzzy numbers (A value) | Ranking | Verdict |
|---|---|---|---|---|---|---|
| Domain: Governance | ||||||
| 1 | NNG-1 | 0.094 | 93.3% | 0.909 | 6 | Retained |
| 2 | NNG-2 | 0.111 | 86.7% | 0.911 | 5 | Retained |
| 3 | NNG-3a | 0.138 | 93.3% | 0.898 | 9 | Retained |
| 4 | NNG-3b | 0.425 | 33.33% | 0.613 | 15 | Discarded |
| 5 | NNG-3c | 0.383 | 40.00% | 0.638 | 14 | Discarded |
| 6 | NNG-4 | 0.094 | 93.33% | 0.909 | 6 | Retained |
| 7 | NNG-5 | 0.377 | 40.00% | 0.371 | 16 | Discarded |
| 8 | NNG-6 | 0.068 | 100.00% | 0.933 | 3 | Retained |
| 9 | NNG-7a | 0.252 | 86.67% | 0.818 | 11 | Retained |
| 10 | NNG-7b | 0.060 | 100.00% | 0.940 | 1 | Retained |
| 11 | NNG-8 | 0.094 | 93.33% | 0.909 | 6 | Retained |
| 12 | NNG-9 | 0.402 | 46.67% | 0.642 | 13 | Discarded |
| 13 | NNG-10 | 0.290 | 60.00% | 0.742 | 12 | Discarded |
| 14 | NNG-11 | 0.094 | 100.00% | 0.878 | 10 | Retained |
| 15 | NNG-12 | 0.068 | 100.00% | 0.933 | 3 | Retained |
| 16 | NNG-13 | 0.060 | 100.00% | 0.940 | 1 | Retained |
| DOMAIN: INFRASTRUCTURE | ||||||
| 1 | NNI-14a | 0.321 | 53.3% | 0.738 | 10 | Discarded |
| 2 | NNI-14b | 0.410 | 40.0% | 0.716 | 11 | Discarded |
| 3 | NNI-15 | 0.116 | 93.3% | 0.909 | 4 | Retained |
| 4 | NNI-16a | 0.155 | 93.33% | 0.873 | 6 | Retained |
| 5 | NNI-16b | 0.186 | 93.33% | 0.829 | 9 | Retained |
| 6 | NNI-17 | 0.244 | 86.67% | 0.842 | 8 | Retained |
| 7 | NNI-18 | 0.089 | 93.33% | 0.922 | 1 | Retained |
| 8 | NNI-19 | 0.183 | 93.33% | 0.860 | 7 | Retained |
| 9 | NNI-20 | 0.076 | 100.00% | 0.920 | 2 | Retained |
| 10 | NNI-21 | 0.076 | 100.00% | 0.913 | 3 | Retained |
| 11 | NNI-22 | 0.131 | 93.33% | 0.878 | 5 | Retained |
| DOMAIN: HUMAN RESOURCE | ||||||
| 1 | NNHR-23 | 0.409 | 20.0% | 0.647 | 8 | Discarded |
| 2 | NNHR-24 | 0.291 | 66.7% | 0.704 | 6 | Discarded |
| 3 | NNHR-25 | 0.087 | 100.0% | 0.896 | 1 | Retained |
| 4 | NNHR-26 | 0.373 | 40.00% | 0.662 | 7 | Discarded |
| 5 | NNHR-27 | 0.197 | 93.33% | 0.842 | 4 | Retained |
| 6 | NNHR-28 | 0.145 | 93.33% | 0.829 | 5 | Retained |
| 7 | NNHR-29 | 0.173 | 93.33% | 0.878 | 2 | Retained |
| 8 | NNHR-30 | 0.119 | 93.33% | 0.864 | 3 | Retained |
Notes: Threshold value (d) < 0.2 (three decimal points is accepted); Percentage expert consensus agreement > 75%; Average fuzzy value (A value ) > 0.5; All three must be fulfilled for the elements to be retained
Supplementary Table 2.
Summary of all three domains after Fuzzy Delphi analysis findings for the new norm elements in ED in Malaysia during the COVID-19 pandemic
| Domain | New norm element/item description (NN) | Verdict | Ranking |
|---|---|---|---|
|
| |||
| Governance (G) | |||
| NNG-1 | Usage of proper Personal Protective Equipment (PPE) is compulsory during the triaging process. | Retained | 6 |
| NNG-2 | The creation of a screening process (questionnaire) to aid in clinical triaging of COVID-19 and facilitating zone disposition based on PPE requirements. | Retained | 5 |
| NNG-3a | Conducting a questionnaire-based self-reporting screening process of COVID-19 on patients and family members or caretakers before they enter the emergency department (ED). | Retained | 9 |
| NNG-3b | Screening patients and family members or caretakers before they enter the ED using COVID-19 rapid test kits (RTK). | Discarded | 15 |
| NNG-3c | Screening patients and family members or caretakers before they enter the ED using a questionnaire-based self-reporting and COVID-19 rapid test kits (RTK). | Discarded | 14 |
| NNG-4 | Screening for COVID-19 symptoms and measuring the temperature of all visitors at the ED entrance. | Retained | 6 |
| NNG-5 | Healthcare workers performing aerosol-generating procedures (such as intubation) must use an aerosol box to minimise the spread of COVID-19. | Discarded | 16 |
| NNG-6 | Standard PPE worn by healthcare workers when attending to patients without COVID -19. PPE: A facial shield or eye protection (goggles), a surgical mask and gloves. | Retained | 3 |
| NNG-7a | The standard PPE for aerosol-generating procedures (such as intubation) includes a powered air-purifying respirator (PAPR), N95 mask, boot covers, and gloves. | Retained | 11 |
| NNG-7b | The standard PPE for aerosol-generating procedures (such as intubation) includes a disposable isolation gown suit (coveralls suit), a face shield, an N95 mask, boot covers, and gloves. | Retained | 1 |
| NNG-8 | A standard intubation checklist for suspected and confirmed patients with COVID-19. | Retained | 6 |
| NNG-9 | Using an isolation pod (ISOPOD) to transfer suspected and confirmed patients with COVID-19. | Discarded | 13 |
| NNG-10 | Developing teleconsultation helpline services at the ED to facilitate the screening and triaging process of suspected, probable, or confirmed patients with COVID-19. | Discarded | 12 |
| NNG-11 | A computerised system or manual clerking sheet template with the checklist method augments the speed and efficiency of management. | Retained | 10 |
| NNG-12 | Establishing standard operational protocols or guidelines on training and clinical management of COVID-19 and updating it promptly. | Retained | 3 |
| NNG-13 | Developing a guideline for the ED on COVID-19 preparedness and response strategy at the hospital level. | Retained | 1 |
|
| |||
| Infrastructure | |||
|
| |||
| NNI-14a | Designated negative pressure system cabins or tents for fever centre/acute respiratory influenza-like illness outside of the ED. | Discarded | 10 |
| NNI-14b | Designated cabins or tents without a negative pressure system for fever centre/acute respiratory influenza-like illness outside of the ED. | Discarded | 11 |
| NNI-15 | Restructuring a respiratory and non-respiratory zone within the ED with separate access and exit points. | Retained | 4 |
| NNI-16a | Establishing a negative pressure isolation room for suspected, probable, or confirmed COVID-19 cases with separate access and exit points. | Retained | 6 |
| NNI-16b | Establishing an isolation room without a negative pressure system for suspected, probable, or confirmed COVID-19 cases with separate access and exit points. | Retained | 9 |
| NNI-17 | Establishing a separate resuscitation area for non-COVID-19 cases with separate access and exit points. | Retained | 8 |
| NNI-18 | A designated PPE donning/ doffing area in the ED | Retained | 1 |
| NNI-19 | A designated portable X-ray room in the ED. | Retained | 7 |
| NNI-20 | The isolation area should have dedicated washrooms, hand-washing stations, and trash bins. | Retained | 2 |
| NNI-21 | Creating predetermined transport routes to transfer patients with COVID-19 to minimise exposure. | Retained | 3 |
| NNI-22 | During access block, establish an observation ward for suspected, probable, or confirmed COVID-19 and non-COVID-19 cases. | Retained | 5 |
|
| |||
| Human resources (HR) | |||
|
| |||
| NNHR-23 | Setting up a COVID-19 team and rotating the team occasionally to minimise the risk of COVID-19 transmission. | Discarded | 8 |
| NNHR-24 | Interdepartmental recruitment of a COVID-19 team within the hospital to manage suspected, probable, or confirmed patients with COVID-19 in the ED. | Discarded | 6 |
| NNHR-25 | Frequent training of healthcare workers on performing nasopharyngeal swabs, donning and doffing PPE. | Retained | 1 |
| NNHR-26 | To ensure safety, high-risk healthcare workers (workers with pre-existing comorbidities and pregnancy) should work in a non-COVID-19 zone. | Discarded | 7 |
| NNHR-27 | Active surveillance of COVID-19 risk in emergency healthcare workers upon arrival at work. | Retained | 4 |
| NNHR-28 | Active mental health surveillance on emergency healthcare workers during the pandemic. | Retained | 5 |
| NNHR-29 | Providing hospital scrubs to all healthcare workers working in the respiratory zone. | Retained | 2 |
| NNHR-30 | The ED team conducts close contact tracing of suspected or confirmed COVID-19 cases among healthcare workers. | Retained | 3 |