Abstract
Video Abstract
OBJECTIVE
We sought to determine whether clonidine, a non-opioid α−2-adrenergic agonist, would effectively treat neonatal opioid withdrawal syndrome (NOWS).
METHODS
This was an intention-to-treat randomized clinical trial. Enrollment criteria included prenatal opioid exposure, age ≤7 days, gestational age ≥35 weeks, no other medical condition, and need for pharmacotherapy. Primary outcomes were length of treatment and neurobehavioral performance.
RESULTS
A total of 1107 patients were screened for enrollment (645 ineligible, 91 parents or staff unavailable, 216 declined, 155 consented). Of 155 infants, 120 required treatment and were randomized to receive oral clonidine (n = 60) at 1 µg/kg/dose or morphine (n = 60), 0.06 mg/kg/dose, every 3 hours. Infants with no improvement had their doses increased by 25% of the initial dose every 12 to 24 hours. Those without improvement by the fourth dose increase, received adjunct therapy. Length of treatment did not differ between morphine and clonidine, with median (95% confidence interval [CI]) days, respectively, of 15 (13–17) and 17 (15–19), P = .48. More clonidine-treated infants (45%) needed adjunct therapy versus 10% in the morphine group, adjusted odds ratio (95% CI) = 8.85 (2.87–27.31). After treatment completion, the NICU Network Neurobehavioral Scales summary scores did not differ between clonidine-treated and morphine-treated infants.
CONCLUSIONS
Length of pharmacologic treatment and final neurobehavioral performance were not significantly different between the clonidine- and morphine-treated groups. Clonidine appears to be an effective non-opioid medication to treat NOWS. Future studies are needed to determine the optimal clonidine dosage for a quicker response and obviation of adjunct therapy.
What’s Known on This Subject:
Morphine is a commonly used treatment of neonatal opioid withdrawal syndrome (NOWS) despite concerns about its adverse effects on the developing brain. Clonidine, a non-opiate α−2 adrenergic agonist, is reported to be effective as an adjunct therapy in NOWS treatment.
What This Study Adds:
Clonidine, as a non-opiate single-drug treatment for NOWS, is not significantly different from morphine regarding the duration of treatment and infant neurobehavioral outcomes post-treatment. Clonidine appears to be an effective non-opioid medication for NOWS therapy.
The opioid epidemic in the United States has resulted in increasing overdose deaths,1 maternal death,2 and neonatal abstinence syndrome (NAS),3 which is associated with short-term and long-term consequences.4,5 From 2010 to 2017, NAS rates increased from 4.0/1000 to 7.3/1000 hospital births; rates varied across states from 1.3/1000 to 53.5/1000 births by region,3,6 urbanicity,7 or county.8,9 These increased NAS rates were related to prenatal opioid exposure with or without other substances, lately referred to as neonatal opioid withdrawal syndrome (NOWS). In utero exposure occurs from opioid misuse or as prescribed for chronic pain relief or medication for opioid use disorder (MOUD). NOWS has been associated with increased health care costs4,10,11 from the prolonged length of hospital stay (LOS) related to the length of treatment (LOT).10
The reported adverse effects of in utero opioid exposure on the developing brain include hydrocephaly,12,13 neonatal stroke,14 small head size,15–23 decreased brain cell number,24 postnatal head growth deceleration,25,26 reduced brain volumes,27 and associated long-term cognitive deficits and behavioral problems.28,29 Despite the detrimental effects of in utero opioid exposure, the opiate morphine remains a common first-line drug for NOWS treatment,30–32 resulting in additional weeks to months of exposing the developing brain to opioids.33–35
Prolonged opioid exposure results in the activation of opioid receptors in the locus coeruleus, in which clusters of noradrenergic cells are collocated.36,37 Chronic opioid supply inhibits noradrenergic cells; the discontinuation of opioid exposure increases noradrenergic activity.38 Clonidine inhibits noradrenaline release, resulting in decreased noradrenergic activity and opioid withdrawal manifestations.39,40 Clonidine is a reported effective single-drug therapy in a small number of babies with NOWS41–43 and as an adjunct therapy.44–46 In preclinical studies, clonidine has advantages over morphine; it stabilizes breathing and temperature control that is disrupted by morphine,47 decreases ketamine-induced apoptosis and brain injury in hypoxic-ischemic brain damage,48 suppresses cytokines, and downregulates opioid receptor expression in neonatal mononuclear cells.49
In our previous study, clonidine, compared with morphine for NAS treatment, was associated with shorter LOT and improved neurobehavioral performance.50 This supported evaluating a non-opioid drug as an alternative to treat NOWS. We sought to determine if the non-opioid α−2 adrenergic agonist, clonidine, would effectively treat NOWS.
Methods
This study (https://clinicaltrials.gov/ct2/show/NCT03396588) had approval from the institutional review board (IRB) and a certificate of confidentiality from the National Institute on Drug Abuse. Parent(s) gave informed consent for study participation. This study was an intention-to-treat, double-blind trial, with treatment randomized between clonidine and morphine, carried out at the Kentucky Children’s Hospital. Primary outcomes included LOT and post-treatment neurobehavioral status, which is a reported predictor of childhood outcomes.51
Research nurses screened all admissions for prenatal substance exposure at the well-baby nursery and the NICU. Enrollment criteria included (1) gestational age ≥35 weeks, (2) any prenatal opioid exposure with or without other substances from the mother reporting opioid use or positive toxicology results, (3) ≤7 days postnatal age, (4) not unlikely to survive, (5) no medical condition other than NOWS, (6) no seizures, (7) no prenatal cocaine exposure, (8) meets treatment criteria for NOWS, and (9) informed consent. Prenatal cocaine exposure was excluded because tone abnormalities have been attributed to cocaine central nervous system effects rather than drug withdrawal.52,53
All infants had non-pharmacological intervention (swaddling, low noise, and lighting environment, rooming in, infant massage, etc).54–56 Throughout the hospital stay, infants were monitored using the Finnegan Neonatal Abstinence Scoring System.55 The Finnegan Neonatal Abstinence Scoring System scores (FS) guided the initiation and monitoring of treatment, allowing for comparison with other treatment studies.45,57,58 Clonidine or morphine was started when an infant had 3 consecutive FSs ≥8 or 2 consecutive FSs ≥12 with the evaluation and approval of the attending physician. Treatment assignment was obtained through the Investigational Drug Service of the Center for Clinical and Translational Science. Clinical pharmacists prepared and dispensed the study drug, with clonidine and morphine having identical appearances. Block randomization allowed for balanced enrollment in each treatment arm. Families, providers, and research staff were masked to the treatment assignment. Our initial drug dosage (clonidine, 1 µg/kg/dose or morphine, 60 µg/kg/dose) approximated our previous study’s receiver operating characteristics that provided the best control of signs50 and was given every 3 hours concomitant with the infant’s feeding schedule. The initial clonidine dose was within the range given in other studies42–46 and supported by published population pharmacokinetics.59
The dose for either drug was increased by 25% of the initial dose every 12 to 24 hours until FSs were consistently <8, to a maximum of 2 μg/kg/dose for clonidine and 120 µg/kg/dose for morphine. The maximum clonidine dose of 16 μg/kg/day was slightly higher than reported by Agthe et al45 but within the dose range reported by O’Mara et al.60
After 24 to 48 hours of stabilization, dose weaning began by 10% of the maximum dose every 24 hours. When FSs increased during weaning, the dose was increased to the previous dose; weaning resumed after 24 to 48 hours. If no improvement was noted at the maximum dose, phenobarbital was added at a loading dose of 10 mg/kg and maintenance dose of 2.5 mg/kg q 12 hours.61 Some attending physicians preferred clonidine or morphine as an adjunct. Thus, infants were allowed to receive either morphine or clonidine as the secondary drug, which the infant was not randomly assigned to receive. Masking was maintained. After stabilization after the addition of the adjunct drug, the primary (first) drug was weaned daily by 10% of the maximum dose. After discontinuation of the primary drug, adjunct drug weaning followed. After 48 hours of observation without medication, infants were discharged. Infants on phenobarbital were discharged with a weaning schedule over 3 weeks.
Data Collection
Drug use during pregnancy was obtained through maternal interviews by research staff, who also abstracted medical records for demographic information, including race and ethnicity, maternal pregnancy history, drug use, MOUD, delivery information, FSs, dose changes, duration of treatment, and drug effects, conditions, complications for reporting to the IRB and Drug Safety Monitoring Board (DSMB) of the Center for Clinical and Translational Science. Data entry and management were conducted by using Research Electronic Data Capture tools (REDCap 11.4.2 - 2021 Vanderbilt University).62,63
Neurobehavior Assessment
The NICU Network Neurobehavioral Scale (NNNS)64,65 requires eliciting responses from a sleep or quiet state to crying (behavioral state 6). Infants with severe withdrawal are typically unable to complete the assessment. Therefore, after withdrawal signs improved and dose weaning began, trained and certified research nurses, who were blinded to treatment assignment, performed the initial assessment; this was repeated at treatment completion. The NNNS assesses neurologic, behavioral, and stress/abstinence components from the Brazelton Scale66 and Finnegan’s work,67 yielding 13 summary scores:65 habituation, attention, handling, quality of movement, regulation, non-optimal reflexes, asymmetry total/reflexes, stress/abstinence, arousal, hypertonicity, hypotonicity, excitability, and lethargy.
Statistical Methods
When designing this study, we anticipated recruiting ∼200 infants. Assuming 20% attrition (80 infants in each treatment group), there would be at least 80% power to detect a difference with an effect size of at least 0.45 when using a 2-sided test with a 5% significance level. This effect size was exceeded for some outcomes in the pilot data.50 An interim analysis was conducted in 2020 for the DSMB. At that time, 94 subjects had been randomly assigned. The study was allowed to continue.
Based on Consolidated Standards of Reporting Trials (CONSORT) standards, baseline demographic variables were summarized for morphine and clonidine treatment.68,69 Frequencies (%) are presented for categorical variables and either mean (SD) or median (min, max) for continuous variables. For outcome results, we present 95% confidence intervals (CIs).
A log-rank test was used to compare treatment arms regarding LOT and LOS.70 To use data from infants withdrawn from the study, the time of withdrawal was specified as the censoring time. Cox proportional hazards regression modeling was used in a follow-up analysis using treatment and selected risk factors associated with NOWS severity (birth weight, gestational age, gender, cesarean delivery, maternal psychiatric disorder, inborn status, MOUD, other opioid, and non-opioid substance use).32,51,71–74 Because smoking was highly prevalent and alcohol use was infrequent, they were not included in the model. In post hoc analyses, a negative binomial regression was used to model LOT for 115 infants, excluding those withdrawn from the study. Empirical SE estimates were employed to ensure valid inference.
Treatment arms were compared regarding the need for adjunct medication using frequencies (%) and χ2 tests. Of 5 infants withdrawn, only 1 received adjunct medication; the other 4 were observed for <2 days. Utilizing data from all 120 infants, we assumed that the 4 infants did not require adjunct treatment. We also removed these 4 infants in a follow-up analysis. The remaining 116 infants were used to fit a logistic regression model, from which adjusted odds ratios were derived.
Wilcoxon rank tests were used to compare treatment groups regarding the timing between initial and final NNNS assessments and the NNNS scores (initial, final, and change). P values were adjusted using the false discovery rate method because of multiple comparisons across 13 summary scores.75
Intention-to-treat analyses used all available data based on treatment assignment. All tests were 2-sided, with a statistical significance of P <.05. Analyses were conducted in SAS v9.4 (SAS Institute Inc 2013. SAS/ACCESS® 9.4 Interface to ADABAS: Reference. Cary, NC: SAS Institute Inc.).
Results
The enrollment period started in December 2017 and ended in February 2022, at funding completion. In 2020 and 2021, coronavirus disease 2019 restrictions over face-to-face encounters with subjects resulted in decreased enrollment. Enrollment continued through phone consent and follow-up post-discharge through virtual visits.
The CONSORT diagram is in Fig 1. Infants with prenatal substance exposure (n = 1107) were assessed for eligibility. There were 155 whose parents gave consent, but 35 did not meet the treatment criteria. The remaining 120 infants were randomly assigned to receive clonidine (n = 60) or morphine (n = 60). Five infants were withdrawn from the study (clonidine [n = 2] and morphine [n = 3]). Four of 5 infants were withdrawn after 1 to 2 days of treatment; 1 randomly assigned to receive clonidine was withdrawn after 10 days of treatment because of abnormal chromosome results.
FIGURE 1.
CONSORT flow diagram showing the number of participants screened for eligibility who were consented for enrollment, enrolled, received allocation, were excluded or withdrawn from participation after the intervention initiated and the reasons, and included in the outcome analysis.
Table 1 reveals characteristics of mothers and infants by treatment with no post hoc comparison, per the CONSORT statement.68,69 A total of 52 (87%) and 49 (82%) mothers in the clonidine and morphine groups, respectively, were receiving MOUD. Despite this, the use of other substances was prevalent (Table 2) based on maternal self-report and toxicology results.
TABLE 1.
Characteristics of Mothers and Infants Enrolled in the Study by Treatment Assignment
| Maternal Characteristics | Clonidine (n = 60) | Morphine (n = 60) | All (n = 120) | Infant Characteristics | Clonidine (n = 60) | Morphine (n = 60) | All (n = 120) |
|---|---|---|---|---|---|---|---|
| n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | ||
| Age, y, mean (SD) | 29.3 (4.8) | 29.5 (4.3) | 29.4 (4.5) | Gest age, wk, mean (SD) | 38.7 (1.2) | 38.3 (1.3) | 38.5 (1.3) |
| Race and ethnicitya | Race and ethnicitya | ||||||
| Non-Hispanic white | 53 (88) | 50 (83) | 103 (86) | ||||
| Non-Hispanic Black | 0 (0) | 0 (0) | 0 (0) | ||||
| Non-Hispanic white | 57 (95) | 59 (98) | 116 (97) | Non-Hispanic multiracial | 6 (10) | 6 (10) | 12 (10) |
| Non-Hispanic Black | 1 (2) | 0 (0) | 1 (1) | Non-Hispanic American Indian | 1 (2) | 0 (0) | 1 (1) |
| Non-Hispanic multiracial | 1 (2) | 1 (2) | 2 (2) | Hispanic white | 0 (0) | 2 (3) | 2 (2) |
| Non-Hispanic American Indian | 1 (2) | 0 (0) | 1 (1) | Hispanic multiracial | 0 (0) | 2 (3) | 2 (2) |
| Insurance | Preterm <37 wk | 3 (5) | 4 (7) | 7 (6) | |||
| Medicaid | 58 (97) | 59 (98) | 117 (98) | ||||
| Private | 2 (3) | 1 (2) | 3 (2) | ||||
| Rural | 42 (70) | 46 (77) | 88 (73) | Males | 37 (62) | 30 (50) | 67 (56) |
| Limited or no prenatal care | 23 (38) | 24 (40) | 47 (39) | Inbornb | 27 (45) | 27 (45) | 54 (45) |
| Hospitalization, this pregnancy before delivery | 9 (15) | 12 (20) | 21 (18) | Birth weight, mean (SD) g | 3144 (497) | 3037 (496) | 3091 (497) |
| Gravida, median (min, max) | 4 (1,10) | 3 (1,10) | 4 (1, 10) | Birth head circ, mean (SD) cm | 33.9 (1.7) | 33.6 (1.6) | 33.7 (1.6) |
| Para, median (min, max) | 3 (1, 7) | 3 (1, 9) | 3 (1, 9) | Birth length, mean (SD) cm | 48.1 (2.4) | 48.3 (2.1) | 48.2 (2.2) |
| Hypertension | 9 (15) | 7 (12) | 16 (13) | 1 min Apgar median (min, max) | 8 (1, 9) | 8 (4, 9) | 8 (1, 9) |
| Diabetes | 3 (5) | 6 (10) | 9 (8) | 5 min Apgar median (min, max) | 9 (5,10) | 9 (7, 10) | 9 (5, 10) |
| Hepatitis C positive | 26 (43) | 34 (57) | 60 (50) | Intrauterine growth restriction | 6 (10) | 7 (12) | 13 (11) |
| Hypothyroid | 3 (5) | 10 (17) | 13 (11) | Cesarean section birth | 31 (52) | 29 (48) | 60 (50) |
| Psych/emotional illness | 23 (38) | 19 (32) | 42 (35) | Not breastfed | 40 (67) | 35 (58) | 75 (63) |
| MOUD | 52 (87) | 49 (82) | 101 (84) | Post-natal age at treatment start, mean (SD) d | 2.7 (1.3) | 2.5 (1.2) | 2.6 (1.3) |
| Buprenorphine | 26 (50) | 30 (61) | 56 (55) | ||||
| Buprenorphine/naloxone | 21 (40) | 16 (33) | 37 (37) | ||||
| Methadone | 5 (10) | 3 (6) | 8 (8) | ||||
| Tobacco | 51 (85) | 52 (87) | 103 (86) | ||||
| Alcohol | 0 (0) | 3 (5) | 3 (3) | ||||
a Race and ethnicity were derived from review of electronic medical records.
b Birth at the hospital study site versus those transferred in to study site from another birth facility.
TABLE 2.
Exposures to Other Substances (Opioid and Non-Opioids) by Treatment Groups From Maternal Self-Report or Toxicology Results Compared With Exposures Based Only on Toxicology Results
| Clonidine (n = 60) | Morphine (n = 60) | |||
|---|---|---|---|---|
| Opioids | Maternal Report or Toxicology, n (%) | Toxicology Only, n (%) | Maternal Report or Toxicology, n (%) | Toxicology Only, n (%) |
| Codeine | 3 (5) | 2 (3) | 3 (5) | 2 (3) |
| Hydrocodone | 8 (13) | 1 (2) | 5 (8) | 0 (0) |
| Hydromorphone | 5 (8) | 4 (7) | 2 (3) | 0 (0) |
| Morphine | 8 (13) | 4 (7) | 6 (10) | 6 (10) |
| Heroin | 14 (23) | 3 (5) | 10 (17) | 1 (2) |
| Oxycodone | 9 (15) | 3 (5) | 11 (18) | 6 (10) |
| Methadone* | 3(5)* | 2 (3)* | 1 (2)* | 1 (2)* |
| Fentanyl | 14 (23) | 7 (12) | 12 (20) | 7 (12) |
| Buprenorphine* | 5 (8)* | 4 (7)* | 7 (12)* | 3 (3)* |
| Tramadol | 3 (5) | 2 (3) | 3 (5) | 3 (5) |
| Non-opioids | ||||
| Tobacco** | 51 (85) | ** | 52 (87) | ** |
| Alcohol | 0 (0) | 0 (0) | 3 (5) | 1 (2) |
| Amphetamines/ methamphetamine | 19 (32) | 11 (18) | 15 (25) | 10 (17) |
| Benzodiazepines | 8 (13) | 5 (8) | 5 (8) | 2 (3) |
| Cannabinoids | 23 (38) | 14 (23) | 9 (15) | 3 (5) |
| Gabapentin** | 12 (20) | ** | 12 (20) | ** |
| Phencyclidine | 0 (0) | 0 (0) | 0 (0) | 0 (0) |
| Barbiturates | 1 (2) | 1 (2) | 2 (3) | 1 (2) |
| SSRI (selective serotonin reuptake inhibitor)** | 10 (17) | ** | 10 (17) | ** |
* Only included are exposures other than MOUD.
** Toxicology test not performed.
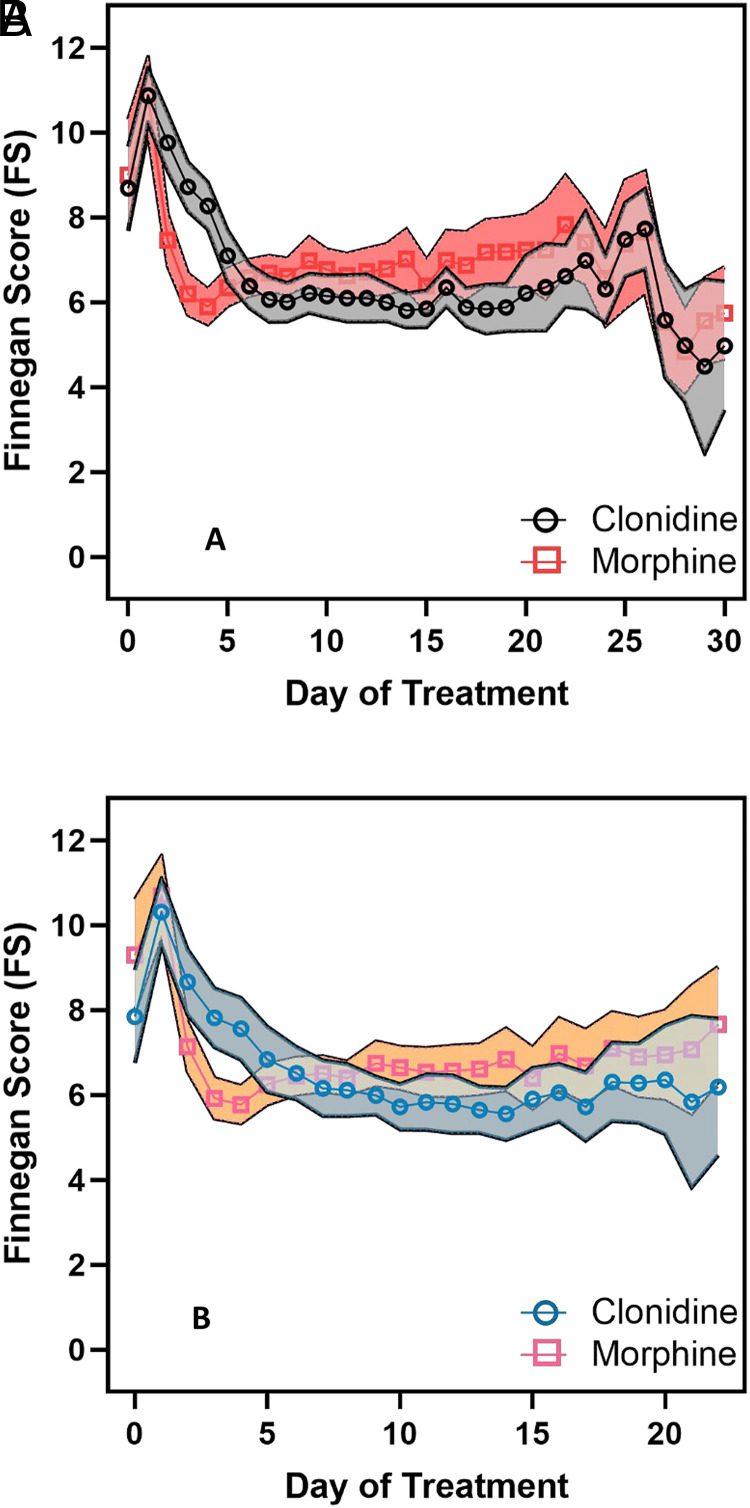
Before treatment, the median (95% CI) of the maximum FS was similar in clonidine- and morphine-treated infants (14.5 [14.1–15.6] and 14 [13.9–15.5], respectively). FS decreased subsequently. By the third day of treatment, the maximum FS was significantly lower (P < .001) in the morphine-treated group, with a median (95% CI) of 8.0 (7.3–8.6) versus 11.5 (11.0–12.5) in the clonidine group. In Fig 2A–B, there are similar patterns of mean FS (95% CI) over time for the treatment groups and subgroups with monotherapy. Mean FS scores were similar at treatment initiation, with a more pronounced drop by the second day of treatment with morphine treatment. After 6 days, the mean daily scores of the clonidine group trended lower than the morphine group, although the CIs overlapped.
FIGURE 2.
Trajectories of the Finnegan scores, mean, and 95% CI over the course of treatment of all infants in the treatment groups (Fig 2A) and for those who only received a single drug therapy and no adjunct medication (Fig 2B). The means and 95% CIs are descriptive and conditional on subjects still being treated on the given day.
Duration of Treatment
The LOT did not differ significantly between treatments (P = .48); the medians (95% CI) were 17 (15–19) and 15 (13–17) days, respectively, for the clonidine and morphine groups. Neither was there a significant difference in LOS between clonidine and morphine groups, with medians (95% CI) of 22 (20–24) and 19 (17–21) days, respectively (P = .30). In those receiving a single therapy, the LOT was similar for clonidine and morphine subgroups, with medians (95% CI) of 14 (12–16) days and 14 (12–17) days, respectively (P = .59). The mean (SD) total morphine dose per patient in the clonidine arm was 5.5 (13.2) mg and 9.1 (19.8) mg in the morphine arm. The clonidine-treated infants who also received morphine had a mean (SD) of 27.7 (16.0) mg total morphine dose per patient; the morphine treatment duration was longer, starting a few days from clonidine initiation and weaning beginning only after clonidine discontinuation.
In an unadjusted model, the hazard ratio (HR) for clonidine to morphine was estimated to be 0.88 (95% CI: [0.61–1.28], P = .50). In the adjusted model (Table 3), the results were similar, (HR = 0.82, 95% CI: [0.55–1.23], P = .33). A heavier birth weight was associated a with longer LOT (HR = 0.95, 95% CI: [0.91–0.99], P = .01). Exposure to any other opioids predicted a shorter LOT, but not significantly when exposures were only based on toxicology results.
TABLE 3.
Adjusted Results From Cox Proportional Hazards Regression Model and Logistic Regression Model Based on Exposures
| Adjusted Results Predicting LOT Cox Proportional Hazards Regression Model | Adjusted Results Predicting Adjunct Therapy Logistic Regression Model | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Variables | Substance Exposure All Sourcesa | Substance Exposure Toxicologyb | Variables | Substance Exposure All Sourcesa | Substance Exposure Toxicologyb | ||||
| HR (95% CI) | P | HR (95% CI) | P | Odds Ratio (95% CI) | P | Odds Ratio (95% CI) | P | ||
| Treatment group |
.33 |
.58 |
Treatment group |
<.001 |
<.001 |
||||
| Clonidine | 0.82 (0.55–1.23) | 0.90 (0.61–1.32) | Clonidine | 8.85 (2.87–27.31) | 8.22 (2.72–24.91) | ||||
| Morphine | Reference | Reference | Morphine | Reference | Reference | ||||
| Gestational age, wk | 0.92 (0.75–1.12) | .41 | 0.97 (0.79–1.18) | .75 | Gestational age, wk | 1.20 (0.74–1.96) | .46 | 1.21 (0.74–1.99) | .45 |
| Birth Weight, 100 g | 0.95 (0.91–0.99) | .01 | 0.95 (0.91–0.99) | .01 | Birth Weight, 100 g | 1.17 (1.04–1.31) | .007 | 1.17 (1.04–1.31) | .007 |
| Sex |
.85 |
.95 |
Sex | .27 |
.24 |
||||
| Female | 1.04 (0.70–1.56) | 1.01 (0.67–1.54) | Female | 1.81 (0.63–5.24) | 1.88 (0.65–5.44) | ||||
| Male | Reference | Reference | Male | Reference | Reference | ||||
| Cesarean delivery | 1.46 (0.98–2.17) | .06 | 1.27 (0.84–1.92) | .26 | Cesarean delivery | 0.86 (0.31–2.36) | .76 | 1.02 (0.37–2.82) | .98 |
| Inborn | 0.72 (0.45–1.13) | .15 | 0.96 (0.62–1.49) | .87 | Inborn | 1.19 (0.38–3.75) | .77 | 0.89 (0.28–2.81) | .84 |
| Psych disorder | 0.96 (0.62–1.50) | .85 | 1.00 (0.65–1.54) | .99 | Psych disorder | 0.45 (0.14–1.49) | .19 | 0.48, (0.15–1.51) | .21 |
| MOUD | 1.44 (0.76–2.74) | .27 | 0.88 (0.43–1.79) | .72 | MOUD | 1.31 (0.24–7.17) | .76 | 2.96 (0.47–18.65) | .25 |
| Any other opioid use | 2.66 (1.60–4.40) | <.001 | 1.16 (0.64–2.09) | .62 | Any other opioid use | 0.76 (0.22–2.65) | .67 | 1.95 (0.49–7.77) | .35 |
| Any non-opioid substance usec | 0.88 (0.58–1.35) | .57 | 1.00 (0.63–1.58) | 1.00 | Any non-opioid substance usec | 1.73 (0.55–5.42) | .35 | 1.73 (0.57–5.24) | .33 |
a The sources of substance use were derived from maternal report or urine toxicology, or infant urine or meconium toxicology results.
b The sources of substance use were derived only from toxicology results.
c Selective serotonin reuptake inhibitor (SSRI) and Gabapentin were included in the model although they were not tested but prescribed.
When excluding infants who were withdrawn from the study, the results were similar (Supplemental Table 5). The unadjusted negative binomial model showed an estimated mean duration of treatment of clonidine to be 18.8 days and 18.0 days for morphine, corresponding to a ratio of 1.05 (95% CI: 0.87–1.26).
Need for Adjunct Medication
More clonidine-treated infants required adjunct therapy than the morphine-treated infants, as follows: 27/60 (45%) and 6/60 (10%), respectively (P <.001). The results were similar when excluding the withdrawn subjects (P <.001). The adjusted odds for adjunct therapy were higher for clonidine (odds ratio = 8.85, 95% CI: [2.87–27.31], P <.001; Table 3). No other factor except heavier birth weight was associated with adjunct therapy (odds ratio = 1.17, 95% CI [1.04–1.31]).
Neurobehavioral Outcome Measures
For the clonidine group (n = 56), the median (min, max) interval between treatment initiation and the initial NNNS examination was 5 (1–16) days (1 outlier), which is significantly longer compared with 3 (1–9) days in the morphine-treated (n = 57) group (P <.001). For a post hoc comparison of subgroups, clonidine only (n = 31) and morphine only (n = 51), the median (min, max) intervals, respectively, were 3 (1–8) days and 3 (1–9) days (P = .52).
The interval between treatment initiation and the final NNNS examination did not differ significantly between treatment groups; for clonidine (n = 54), the median (min, max) was 16.5 (8–48) days, and for morphine (n = 51), it was 15 (7–50) days (P = .24). For monotherapy subgroups, clonidine (n = 32) and morphine (n = 45), the intervals were 14 (8–24) and 14 (7–32), respectively, and P = .94.
The initial, final, and change in the NNNS summary scores of the treatment groups are shown in Table 4. The results are similar when comparing monotherapy subgroups (Supplemental Table 6). At the initial testing, clonidine-treated babies scored worse on arousal, hypertonicity, and stress abstinence. However, between the initial and final assessments, with the duration being similar between groups, the clonidine-treated infants showed significant improvement (less handing, excitability, stress abstinence, and improved arousal and regulation); thus, after treatment completion, clonidine-treated infants did as well as those who were morphine-treated regarding neurobehavioral performance.
TABLE 4.
Comparison of the NNNS Summary Scores Between Treatment Groups*
| NNNS Summary Scores | Clonidine | Morphine | Adjusted P Value Between Treatment | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Initial | Final | Change | Initial | Final | Change | Initial | Final | Change | |
| Habituation | n = 20, 7.5 (6.0 to 8.3) | n = 23, 8.0 (6.0 to 9.0) | n = 9, 0.5 (−1.0 to 1.0) | n = 33, 7.0 (5.7 to 8.0) | n = 23, 8.0 (7.5 to 8.7) | n = 15, 0.3 (−1.0 to 1.0) | .71 | .92 | .77 |
| Attention | n = 35, 4.4 (3.3 to 5.3) | n = 48, 5.1 (4.1 to 6.2) | n = 31, 1.0 (−0.1 to 2.0) | n = 42, 4.3 (3.7 to 5.1) | n = 41, 5.3 (4.7 to 5.7) | n = 31, 0.6 (0.2 to 1.6) | .91 | .92 | .42 |
| Handling | n = 39, 0.6 (0.3 to 0.9) | n = 48, 0.5 (0.4 to 0.8) | n = 35, −0.1 (−0.4 to 0.1) | n = 44, 0.6 (0.4 to 0.8) | n = 46, 0.6 (0.4 to 0.9) | n = 37, 0.1 (0.0 to 0.4) | .91 | .44 | .01 |
| Quality of movement | n = 56, 4.5 (4.0 to 5.1) | n = 53, 5.0 (4.2 to 5.2) | n = 52, 0.1 (−0.3 to 0.8) | n = 57, 4.8 (4.5 to 5.0) | n = 51, 4.7 (4.3 to 5.2) | n = 51, 0.0 (−0.5 to 0.5) | .47 | .61 | .42 |
| Regulation | n = 56, 5.1 (4.3 to 5.6) | n = 53, 5.4 (4.9 to 5.9) | n = 52, 0.5 (−0.5 to 1.3) | n = 56, 5.4 (4.9 to 5.8) | n = 51, 5.2 (4.6 to 5.6) | n = 50, −0.2 (−0.8 to 0.2) | .15 | .44 | .01 |
| Non-optimal reflexes | n = 56, 5.0 (4.0 to 6.0) | n = 54, 4.0 (3.0 to 5.0) | n = 52, −1.0 (−2.5 to 1.0) | n = 57, 5.0 (3.0 to 6.0) | n = 51, 4.0 (2.0 to 4.0) | n = 51, −1.0 (−2.0 to 1.0) | .36 | .59 | .77 |
| Asymmetry total/reflexes | n = 56, 0.0 (0.0 to 0.0) | n = 54, 0.0 (0.0 to 0.0) | n = 52, 0.0 (0.0 to 0.0) | n = 57, 0.0 (0.0 to 0.0) | n = 51, 0.0 (0.0 to 0.0) | n = 51, 0.0 (0.0 to 0.0) | .99 | .69 | .51 |
| Arousal | n = 56, 4.0 (3.7 to 4.3) | n = 53, 3.9 (3.4 to 4.1) | n = 52, −0.1 (−0.6 to 0.3) | n = 57, 3.7 (3.3 to 4.1) | n = 51, 3.9 (3.7 to 4.1) | n = 51, 0.4 (0.0 to 0.7) | .04 | .44 | .004 |
| Hypertonia | n = 56, 1.0 (0.0 to 2.0) | n = 54, 0.0 (0.0 to 0.0) | n = 52, −1.0 (−2.0 to 0.0) | n = 57, 0.0 (0.0 to 1.0) | n = 51, 0.0 (0.0 to 0.0) | n = 51, 0.0 (−1.0 to 0.0) | .04 | .92 | .06 |
| Hypotonia | n = 56, 0.0 (0.0 to 0.0) | n = 54, 0.0 (0.0 to 1.0) | n = 52, 0.0 (0.0 to 0.5) | n = 57, 0.0 (0.0 to 0.0) | n = 51, 0.0 (0.0 to 0.0) | n = 51, 0.0 (0.0 to 0.0) | .91 | .69 | .42 |
| Excitability | n = 56, 4.0 (2.0 to 6.0) | n = 53, 3.0 (1.0 to 4.0) | n = 52, −1.0 (−3.0 to 1.0) | n = 57, 3.0 (2.0 to 4.0) | n = 51, 3.0 (1.0 to 5.0) | n = 51, 1.0 (−1.0 to 3.0) | .15 | .44 | .01 |
| Lethargy | n = 56, 6.0 (4.0 to 8.5) | n = 54, 5.0 (4.0 to 7.0) | n = 52, 0.0 (−3.0 to 1.0) | n = 57, 6.0 (5.0 to 8.0) | n = 51, 4.0 (3.0 to 6.0) | n = 51, −2.0 (−4.0 to 1.0) | .91 | .59 | .42 |
| Stress abstinence | n = 56, 0.2 (0.1 to 0.2) | n = 53, 0.1 (0.1 to 0.2) | n = 52, 0.0 (−0.1 to 0.0) | n = 57, 0.1 (0.1 to 0.2) | n = 51, 0.1 (0.1 to 0.2) | n = 51, 0.0 (0.0 to 0.1) | .02 | .59 | .004 |
* A comparison is shown between treatment groups at the initial administration and at the end of treatment and the change in summary scores from the initial and final assessments. Sample sizes, median, and 25th and 75th percentiles are reported. The false discovery method was used to adjust P values for multiple testing. Each item administered is dependent on infant’s behavioral state (eg, habituation is elicited during sleep state), and thus, the varying n for each item.
Monitoring of Adverse Effects
Conditions monitored and reported to both the DSMB and IRB are in Supplemental Table 7. These conditions were rare and may not be related to treatment.
Discussion
In this randomized trial comparing the clonidine and morphine treatment of NOWS, we found no significant differences in LOT and LOS. However, nearly one-half of the infants treated with clonidine received adjunct therapy. The FS decreased with the initiation of treatment, but the decrease in scores in clonidine-treated babies lagged behind that of morphine-treated infants by 1 to 2 days, resulting in the initiation of adjunct therapy. Initially, clonidine-treated infants had worse neurobehavioral performance scores but were no longer different from morphine-treated infants at treatment completion within similar intervals between the initial and final assessments.
The lack of difference in LOT between groups is notable, considering a larger proportion of clonidine-treated babies receiving adjunct therapy and adjustment for multiple factors. We were able to successfully provide an opioid-sparing medication-assisted treatment regimen to a cohort of infants with significant NOWS. This use of non-opioids may be extended for conditions other than NOWS, such as for the relief of chronic pain or in postoperative states.
A high proportion of clonidine-treated infants needing adjunct therapy is a concern. However, this could be addressed by adjusting the dosing schedule. On the basis of our pilot trial results of conservatively starting clonidine dosing at 0.5 µg/kg,50 published data,76 and a plan to monitor possible adverse events, we started clonidine at 1 µg/kg. Considering that the estimated half-life of clonidine in a neonate is 14 hours,59 compared with 6.5 hours77,78 for morphine, it is reasonable to assume that the maximum pharmacologic effects would be near the time of achieving steady-state, which is typically 5-fold the agent’s half-life, or ∼70 hours for clonidine and ∼32 hours for morphine. This is consistent with the lag in the decrease of FS by 1 to 2 days with clonidine treatment. Conversely, the subsequent trend of lower mean FS with clonidine treatment probably reflects achieving a steady state. This delayed onset of efficacy for clonidine likely necessitated dose escalations and adjunct medication. We are currently examining our pharmacokinetics data to optimize the dosing regimen with clonidine to shorten the time to steady state.
The worse neurobehavioral performance of the clonidine-treated infants compared to the morphine group on the initial assessment may be explained by the delayed or lesser effectiveness of the clonidine response or not having a designated specific time point for the initial assessment. The improvement in neurobehavioral performance with clonidine treatment is reassuring; neurobehavioral functioning is reported to predict early childhood outcomes in drug-exposed infants.51 Long-term follow-up is needed to understand the implications of NOWS and its various treatment modalities.
This study was not powered to show equivalence or non-inferiority. Having this limitation, the lack of significant difference may reflect a type II hypothesis testing error, which would become less probable with a larger sample size. The coronavirus disease 2019 pandemic impacted our plans to enroll a larger sample and add another study site. Nonetheless, the number of infants randomly assigned in our study was similar to that of other multicenter treatment trials.58,79 Being a single study site limits the generalizability of findings. However, we provide information on infants from rural areas. Some mothers did not room in with their babies, and many did not initiate breastfeeding; these affect non-pharmacological care and LOS.80,81 Although a high proportion of mothers were on MOUD, the use of other substances was common. Polypharmacy may also influence NOWS treatment.82 Ascertaining the effects of polydrug use will require a larger number of participants.
In summary, in a randomized trial, the length of pharmacologic treatment and the final assessment of neurobehavioral performance were not significantly different between the clonidine- and morphine-treated groups. Future studies are needed to investigate the optimal dose and frequency of clonidine administration for improved efficacy and the decreased need for adjunctive therapy in NOWS.
Supplementary Material
Acknowledgments
We thank the following for their contribution to the completion of this research: Gail L. Camp, Heather Collins, Susan DeGraff, Caitlin Dunworth, Karen Garlitz, Pui Man (Julia) Ho, Carrie Hobbs, Jamie Horn, Seth Larkin, Alisa McKinney-Whitlock, Leanne Pollard, Brandon Schanbacher, Ashley Stratton, and Amanda Wilburn. We also thank anonymous peer reviewers for their comments, which informed the revision of this work.
Glossary
- CI
confidence interval
- CONSORT
Consolidated Standards of Reporting Trials
- DSMB
Drug Safety Monitoring Board
- FS
Finnegan Neonatal Abstinence Scoring System score
- HR
hazard ratio
- IRB
institutional review board
- LOS
length of stay
- LOT
length of treatment
- MOUD
medication for opioid use disorder
- NAS
neonatal abstinence syndrome
- NOWS
neonatal opioid withdrawal syndrome
- NNNS
NICU network neurobehavioral scale
Footnotes
Drs Bada, Westgate, Sithisarn, Yolton, Charnigo, Pourcyrous, Tang, Gibson, Shearer-Miller, Giannone, and Leggas substantially contributed to the conception or design of the work, analysis or interpretation of the data, and drafting or critically revising this manuscript for intellectual content; and all authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
This trial has been registered at www.clinicaltrials.gov (identifier NCT03396588).
COMPANION PAPER: A companion to this article can be found online at www.pediatrics.org/cgi/doi/10.1542/peds.2024-068359.
Deidentified individual participant data will not be made available for sharing based on participant institutional review board consent.
FUNDING: Funded by the National Institutes of Health (NIH). Supported by National Institute on Drug Abuse (R01 DA043519) and the NIH (NIH/NCATS UL1TR001998 and UL1TR000445). The NIH had no role in the design and conduct of the study.
CONFLICT OF INTEREST DISCLOSURES: The authors have indicated they have no potential conflicts of interest relevant to this article to disclose.
References
- 1.Spencer MR, Minino AM, Warner M. Drug overdose deaths in the United States, 2001–2021. NCHS Data Brief. 2022;(457):1–8 [PubMed] [Google Scholar]
- 2.Gemmill A, Berger BO, Crane MA, et al. Mortality rates among U.S. women of reproductive age, 1999–2019. Am J Prev Med. 2022;62(4):548–557 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Hirai AH, Ko JY, Owens PL, et al. Neonatal abstinence syndrome and maternal opioid-related diagnoses in the US, 2010–2017. JAMA. 2021;325(2):146–155 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Ko JY, Yoon J, Tong VT, et al. Maternal opioid exposure, neonatal abstinence syndrome, and infant healthcare utilization: a retrospective cohort analysis. Drug Alcohol Depend. 2021;223:108704. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Larson JJ, Graham DL, Singer LT, et al. Cognitive and behavioral impact on children exposed to opioids during pregnancy. Pediatrics. 2019;144(2):e20190514. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Umer A, Lilly C, Hamilton C, et al. Disparities in neonatal abstinence syndrome and health insurance status: a statewide study using non-claims real-time surveillance data. Paediatr Perinat Epidemiol. 2021;35(3):330–338 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Villapiano NL, Winkelman TN, Kozhimannil KB, et al. Rural and urban differences in neonatal abstinence syndrome and maternal opioid use, 2004 to 2013. JAMA Pediatr. 2017;171(2):194–196 [DOI] [PubMed] [Google Scholar]
- 8.Patrick SW, Faherty LJ, Dick AW, et al. Association among county-level economic factors, clinician supply, metropolitan or rural location, and neonatal abstinence syndrome. JAMA. 2019;321(4):385–393 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.KCHFS. Neonatal abstinence syndrome in Kentucky: annual report on 2021 Public Health Neonatal Abstinence Syndrome (NAS) Reporting Registry. Available at: https://www.chfs.ky.gov/agencies/dph/dmch/Documents/NASReport.pdf. Published 2021. Accessed April 2, 2023
- 10.Patrick SW, Schumacher RE, Benneyworth BD, et al. Neonatal abstinence syndrome and associated health care expenditures: United States, 2000–2009. JAMA. 2012;307(18):1934–1940 [DOI] [PubMed] [Google Scholar]
- 11.Corr TE, Xing X, Liu G. Longitudinal health care utilization of Medicaid-insured children with a history of neonatal abstinence syndrome. J Pediatr. 2021;233:82–89.e1 [DOI] [PubMed] [Google Scholar]
- 12.Ostrea EM, Chavez CJ. Perinatal problems (excluding neonatal withdrawal) in maternal drug addiction: a study of 830 cases. J Pediatr. 1979;94(2):292–295 [DOI] [PubMed] [Google Scholar]
- 13.Heinonen OP, Slone D, Shapiro S. Birth Defects and Drugs in Pregnancy. Publishing Science Group; 1977 [Google Scholar]
- 14.Reynolds EW, Riel-Romero RMS, Bada HS. Neonatal abstinence syndrome and cerebral infarction following maternal codeine use during pregnancy. Clin Pediatr (Phila). 2007;46(7):639–645 [DOI] [PubMed] [Google Scholar]
- 15.Doberczak TM, Kandall SR, Friedmann P. Relationship between maternal methadone dosage, maternal-neonatal methadone levels, and neonatal withdrawal. Obstet Gynecol. 1993;81(6):936–940 [PubMed] [Google Scholar]
- 16.Chasnoff IJ, Hatcher R, Burns WJ. Polydrug- and methadone-addicted newborns: a continuum of impairment? Pediatrics. 1982;70(2):210–213 [PubMed] [Google Scholar]
- 17.Kaltenbach K, Finnegan LP. Perinatal and developmental outcome of infants exposed to methadone in-utero. Neurotoxicol Teratol. 1987;9(4):311–313 [DOI] [PubMed] [Google Scholar]
- 18.Lifschitz MH, Wilson GS, Smith EO, et al. Factors affecting head growth and intellectual function in children of drug addicts. Pediatrics. 1985;75(2):269–274 [PubMed] [Google Scholar]
- 19.Wilson GS, Desmond MM, Verniaud WM. Early development of infants of heroin-addicted mothers. Am J Dis Child. 1973;126(4):457–462 [DOI] [PubMed] [Google Scholar]
- 20.Wilson GS, Desmond MM, Wait RB. Follow-up of methadone-treated and untreated narcotic-dependent women and their infants: health, developmental, and social implications. J Pediatr. 1981;98(5):716–722 [DOI] [PubMed] [Google Scholar]
- 21.Towers CV, Hyatt BW, Visconti KC, et al. Neonatal head circumference in newborns with neonatal abstinence syndrome. Pediatrics. 2019;143(1):e20180541. [DOI] [PubMed] [Google Scholar]
- 22.Hudak ML, Makker K. Fetal opioid exposure and smaller birth head circumference: cause for concern? Pediatrics. 2019;143(1):e20183376. [DOI] [PubMed] [Google Scholar]
- 23.Cutler AJ, Cox DF, Gabrielson SMB, et al. Association of medication-assisted treatment and short- acting opioids with newborn head circumference and birth weight. J Perinatol. 2023;43(3):277–282 [DOI] [PubMed] [Google Scholar]
- 24.Naeye RL, Blanc W, Leblanc W, et al. Fetal complications of maternal heroin addiction: abnormal growth, infections, and episodes of stress. J Pediatr. 1973;83(6):1055–1061 [DOI] [PubMed] [Google Scholar]
- 25.Johnson H, Diano A, Rosen T. 24-month neurobehavioral follow up of methadone-maintained mothers. Inf Behav Dev. 1984;7:115–123 [Google Scholar]
- 26.Hans SL. Developmental consequences of prenatal exposure to methadone. Ann N Y Acad Sci. 1989;562:195–207 [DOI] [PubMed] [Google Scholar]
- 27.Walhovd KB, Moe V, Slinning K, et al. Volumetric cerebral characteristics of children exposed to opiates and other substances in utero. Neuroimage. 2007;36(4):1331–1344 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Bada HS, Das A, Bauer CR, et al. Impact of prenatal cocaine exposure on child behavior problems through school age. Pediatrics. 2007;119(2):e348–e359 [DOI] [PubMed] [Google Scholar]
- 29.Miller JS, Anderson JG. Factors in children with a history of neonatal abstinence syndrome at 10 years of age: evidence from the maternal lifestyle study. J Spec Pediatr Nurs. 2022;27(1):e12358. [DOI] [PubMed] [Google Scholar]
- 30.Osborn DA, Jeffery HE, Cole MJ. Opiate treatment for opiate withdrawal in newborn infants. Cochrane Database Syst Rev. 2010;(10):CD002059. [DOI] [PubMed] [Google Scholar]
- 31.Patrick SW, Barfield WD, Poindexter BB; Committee on Fetus and Newborn, Committee on Substance Use and Prevention. Neonatal opioid withdrawal syndrome. Pediatrics. 2020;146(5):e2020029074. [DOI] [PubMed] [Google Scholar]
- 32.Reddy UM, Davis JM, Ren Z, et al. ; Opioid Use in Pregnancy, Neonatal Abstinence Syndrome, and Childhood Outcomes Workshop Invited Speakers. Opioid use in pregnancy, neonatal abstinence syndrome, and childhood outcomes: executive summary of a joint workshop by the Eunice Kennedy Shriver National Institute of Child Health and Human Development, American College of Obstetricians and Gynecologists, American Academy of Pediatrics, Society for Maternal-Fetal Medicine, Centers for Disease Control and Prevention, and the March of Dimes Foundation. Obstet Gynecol. 2017;130(1):10–28 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Byerley EM, Mohamed MW, Grindeland CJ, et al. Neonatal abstinence syndrome practices in the United States. J Pediatr Pharmacol Ther. 2021;26(6):577–583 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Maalouf FI, Cooper WO, Slaughter JC, et al. Outpatient pharmacotherapy for neonatal abstinence syndrome. J Pediatr. 2018;199:151–157.e1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Clemans-Cope L, Holla N, Lee HC, et al. Neonatal abstinence syndrome management in California birth hospitals: results of a statewide survey. J Perinatol. 2020;40(3):463–472 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Beitner DB, Duman RS, Nestler EJ. A novel action of morphine in the rat locus coeruleus: persistent decrease in adenylate cyclase. Mol Pharmacol. 1989;35(5):559–564 [PubMed] [Google Scholar]
- 37.Duman RS, Tallman JF, Nestler EJ. Acute and chronic opiate-regulation of adenylate cyclase in brain: specific effects in locus coeruleus. J Pharmacol Exp Ther. 1988;246(3):1033–1039 [PubMed] [Google Scholar]
- 38.Rasmussen K, Beitner-Johnson DB, Krystal JH, et al. Opiate withdrawal and the rat locus coeruleus: behavioral, electrophysiological, and biochemical correlates. J Neurosci. 1990;10(7):2308–2317 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Nestler EJ, Terwilliger R, Beitner D. Regulation by chronic clonidine of adenylate cyclase and cyclic AMP-dependent protein kinase in the rat locus coeruleus. Life Sci. 1989;45(12):1073–1080 [DOI] [PubMed] [Google Scholar]
- 40.Aghajanian GK. Tolerance of locus coeruleus neurones to morphine and suppression of withdrawal response by clonidine. Nature. 1978;276(5684):186–188 [DOI] [PubMed] [Google Scholar]
- 41.Hoder EL, Leckman JF, Ehrenkranz R, et al. Clonidine in neonatal narcotic-abstinence syndrome. N Engl J Med. 1981;305(21):1284. [DOI] [PubMed] [Google Scholar]
- 42.Hoder EL, Leckman JF, Poulsen J, et al. Clonidine treatment of neonatal narcotic abstinence syndrome. Psychiatry Res. 1984;13(3):243–251 [DOI] [PubMed] [Google Scholar]
- 43.Leikin JB, Mackendrick WP, Maloney GE, et al. Use of clonidine in the prevention and management of neonatal abstinence syndrome. Clin Toxicol (Phila). 2009;47(6):551–555 [DOI] [PubMed] [Google Scholar]
- 44.Esmaeili A, Keinhorst AK, Schuster T, et al. Treatment of neonatal abstinence syndrome with clonidine and chloral hydrate. Acta Paediatr. 2010;99(2):209–214 [DOI] [PubMed] [Google Scholar]
- 45.Agthe AG, Kim GR, Mathias KB, et al. Clonidine as an adjunct therapy to opioids for neonatal abstinence syndrome: a randomized, controlled trial. Pediatrics. 2009;123(5):e849–e856 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Surran B, Visintainer P, Chamberlain S, et al. Efficacy of clonidine versus phenobarbital in reducing neonatal morphine sulfate therapy days for neonatal abstinence syndrome. A prospective randomized clinical trial. J Perinatol. 2013;33(12):954–959 [DOI] [PubMed] [Google Scholar]
- 47.Kesavan K, Ezell T, Bierman A, et al. Breathing and temperature control disrupted by morphine and stabilized by clonidine in neonatal rats. Respir Physiol Neurobiol. 2014;201:93–100 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Ponten E, Viberg H, Gordh T, et al. Clonidine abolishes the adverse effects on apoptosis and behaviour after neonatal ketamine exposure in mice. Acta Anaesthesiol Scand. 2012;56(8):1058–1065 [DOI] [PubMed] [Google Scholar]
- 49.Chavez-Valdez R, Kovell L, Ahlawat R, et al. Opioids and clonidine modulate cytokine production and opioid receptor expression in neonatal immune cells. J Perinatol. 2013;33(5):374–382 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Bada HS, Sithisarn T, Gibson J, et al. Morphine versus clonidine for neonatal abstinence syndrome. Pediatrics. 2015;135(2):e383–e391 [DOI] [PubMed] [Google Scholar]
- 51.Liu J, Bann C, Lester B, et al. Neonatal neurobehavior predicts medical and behavioral outcome. Pediatrics. 2010;125(1):e90–e98 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Chiriboga CA, Vibbert M, Malouf R, et al. Neurologic correlates of fetal cocaine exposure: transient hypertonia of infancy and early childhood. Pediatrics. 1995;96(6):1070–1077 [PubMed] [Google Scholar]
- 53.Chiriboga CA, Kuhn L, Wasserman GA. Prenatal cocaine exposures and dose-related cocaine effects on infant tone and behavior. Neurotoxicol Teratol. 2007;29(3):323–330 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Finnegan LP, MacNew BA. Care of the addicted infant. Am J Nurs. 1974;74(4):685–693 [PubMed] [Google Scholar]
- 55.Finnegan LP, Connaughton JF Jr., Kron RE, et al. Neonatal abstinence syndrome: assessment and management. Addict Dis. 1975;2(1-2):141–158 [PubMed] [Google Scholar]
- 56.Velez M, Jansson LM. The opioid dependent mother and newborn dyad: non-pharmacologic care. J Addict Med. 2008;2(3):113–120 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Kraft WK, Gibson E, Dysart K, et al. Sublingual buprenorphine for treatment of neonatal abstinence syndrome: a randomized trial. Pediatrics. 2008;122(3):e601–e607 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Davis JM, Shenberger J, Terrin N, et al. Comparison of safety and efficacy of methadone versus morphine for treatment of neonatal abstinence syndrome: a randomized clinical trial. JAMA Pediatr. 2018;172(8):741–748 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Xie HG, Cao YJ, Gauda EB, et al. Clonidine clearance matures rapidly during the early postnatal period: a population pharmacokinetic analysis in newborns with neonatal abstinence syndrome. J Clin Pharmacol. 2011;51(4):502–511 [DOI] [PubMed] [Google Scholar]
- 60.O’Mara K, Gal P, Davanzo C. Treatment of neonatal withdrawal with clonidine after long-term, high-dose maternal use of tramadol. Ann Pharmacother. 2010;44(7-8):1342–1344 [DOI] [PubMed] [Google Scholar]
- 61.Finnegan LP, Michael H, Leifer B, et al. An evaluation of neonatal abstinence treatment modalities. NIDA Res Monogr. 1984;49:282–288 [PubMed] [Google Scholar]
- 62.Harris PA, Taylor R, Minor BL, et al. ; REDCap Consortium. The REDCap consortium: building an international community of software platform partners. J Biomed Inform. 2019;95:103208. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Harris PA, Taylor R, Thielke R, et al. Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42(2):377–381 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Lester BM, Tronick EZ, Brazelton TB. The neonatal intensive care unit network neurobehavioral scale procedures. Pediatrics. 2004;113(Suppl 2):641–667 [PubMed] [Google Scholar]
- 65.Lester BM, Tronick EZ, LaGasse L, et al. Summary statistics of neonatal intensive care unit network neurobehavioral scale scores from the maternal lifestyle study: a quasinormative sample. Pediatrics. 2004;113(Suppl 2):668–675 [PubMed] [Google Scholar]
- 66.Brazelton T. Neonatal Behavioral Assessment Scale. : JB Lippincott; 1984 [Google Scholar]
- 67.Finnegan LP. Neonatal abstinence syndrome: assessment and pharmocotherapy. In: Rubatelli F, Granati B, eds. Neonatal Therapy: An Update. Elsevier Science Publishers B.V.(Biomedical Division); 1986:122–146 [Google Scholar]
- 68.Altman DG, Schulz KF, Moher D, et al. ; CONSORT Group (Consolidated Standards of Reporting Trials). The revised CONSORT statement for reporting randomized trials: explanation and elaboration. Ann Intern Med. 2001;134(8):663–694 [DOI] [PubMed] [Google Scholar]
- 69.de Boer MR, Waterlander WE, Kuijper LD, et al. Testing for baseline differences in randomized controlled trials: an unhealthy research behavior that is hard to eradicate. Int J Behav Nutr Phys Act. 2015;12:4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Klein JPaM ML. Survival Analysis: Techniques for Censored and Truncated Data. Springer-Verlag; 1997 [Google Scholar]
- 71.Kocherlakota P. Neonatal abstinence syndrome. Pediatrics. 2014;134(2):e547–e561 [DOI] [PubMed] [Google Scholar]
- 72.Kelty EA, Cumming CN, Preen DB. Contribution of pharmaceutical drugs of dependence to the incidence of neonatal abstinence syndrome in Western Australia between 2003 and 2018. Pharmacotherapy. 2022;42(5):405–410 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Devlin LA, Hu Z, Ounpraseuth S, et al. ; Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network and the NIH Environmental influences on Child Health Outcomes (ECHO) Program Institutional Development Awards States Pediatric Clinical Trials Network. The influence of mediators on the relationship between antenatal opioid agonist exposure and the severity of neonatal opioid withdrawal syndrome. Matern Child Health J. 2023;27(6):1030–1042 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Merhar SL, Ounpraseuth S, Devlin LA, et al. ; Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network and the NIH Environmental Influences on Child Health Outcomes (ECHO) Program Institutional Development Awards States Pediatric Clinical Trials Network. Phenobarbital and clonidine as secondary medications for neonatal opioid withdrawal syndrome. Pediatrics. 2021;147(3):e2020017830. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Benjamini Y, Hochberg Y. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J Royal Statistical Society, Series B (Methodological). 1995;57(1):289–300 [Google Scholar]
- 76.Arenas-Lopez S, Riphagen S, Tibby SM, et al. Use of oral clonidine for sedation in ventilated paediatric intensive care patients. Intensive Care Med. 2004;30(8):1625–1629 [DOI] [PubMed] [Google Scholar]
- 77.Kart T, Christrup LL, Rasmussen M. Recommended use of morphine in neonates, infants and children based on a literature review: Part 1–Pharmacokinetics. Paediatr Anaesth. 1997;7(1):5–11 [DOI] [PubMed] [Google Scholar]
- 78.Tang F, Ng CM, Bada HS, et al. Clinical pharmacology and dosing regimen optimization of neonatal opioid withdrawal syndrome treatments. Clin Transl Sci. 2021;14(4):1231–1249 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Peltz G, Jansson LM, Adeniyi-Jones S, et al. Ondansetron to reduce neonatal opioid withdrawal severity a randomized clinical trial. J Perinatol. 2023;43(3):271–276 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.MacMillan KDL, Rendon CP, Verma K, et al. Association of rooming-in with outcomes for neonatal abstinence syndrome: a systematic review and meta-analysis. JAMA Pediatr. 2018;172(4):345–351 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Welle-Strand GK, Skurtveit S, Jansson LM, et al. Breastfeeding reduces the need for withdrawal treatment in opioid-exposed infants. Acta Paediatr. 2013;102(11):1060–1066 [DOI] [PubMed] [Google Scholar]
- 82.Wachman EM, Warden AH, Thomas Z, et al. Impact of psychiatric medication co-exposure on neonatal abstinence syndrome severity. Drug Alcohol Depend. 2018;192:45–50 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.