BACKGROUND
Fournier's gangrene is an aggressive condition caused by polymicrobial infection, in which infected gangrene spreads rapidly along the fascial planes of the perineum and genitalia (Figure 1). 1,2 It requires immediate and radical debridement of all necrotic tissue with concurrent broad-spectrum antibiotic cover. 2,3 Frequent relook procedures involving further debridement are often required, resulting in an extensive wound that can be challenging to manage. 4,5
Figure 1 .

Initial presentation of Fournier's gangrene of the scrotum and perineum
TECHNIQUE
All infected, necrotic tissue is debrided until viable tissue is reached (Figure 2). A vacuum-assisted closure (VAC) sponge is placed over the wound and secured at the wound edge with staples. A window is cut in the sponge to accommodate the anal opening. Similarly, a coordinating window is cut in the overlying plastic adhesive. A Foley catheter is placed into the anal canal. A stoma bag is placed over the anal opening (with the other end of the Foley catheter placed inside the bag). The drainage tubing is placed and connected to the canister (Figure 3).
Figure 2 .
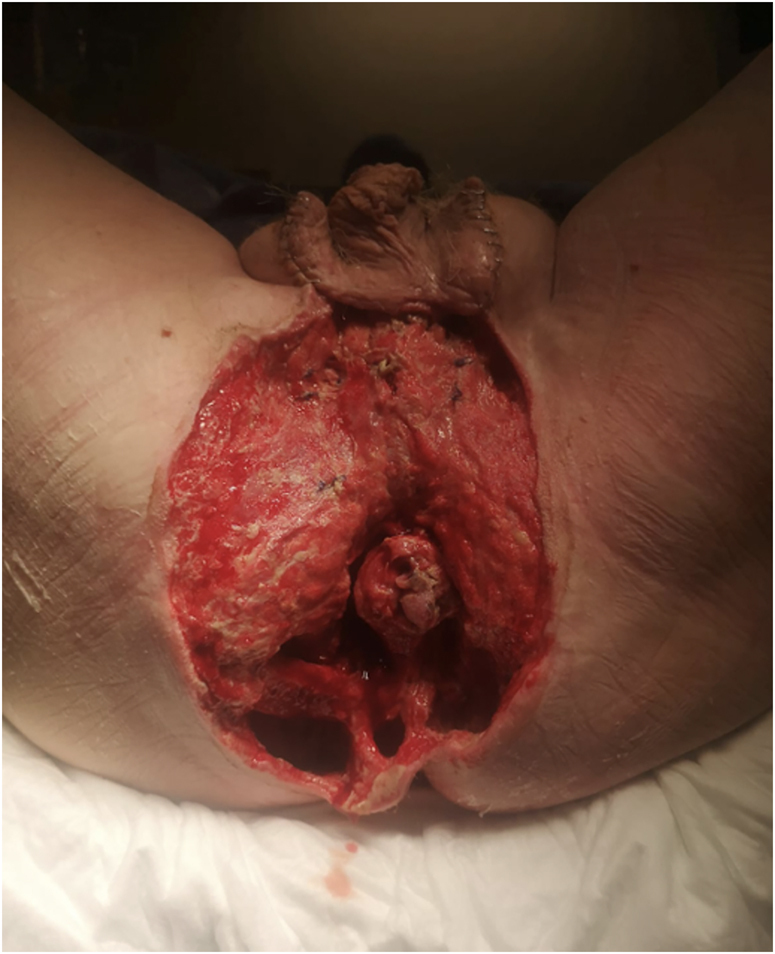
Debridement of necrotic tissue back to viable tissue (note testicles temporarily relocated into inguinal pouch)
Figure 3 .
Placement of black vacuum-assisted closure foam over debrided area with insertion of a Foley catheter into the anal canal and overlying stoma bag in situ
DISCUSSION
Negative-pressure wound therapy with faecal diversion is commonly used in the management of Fournier's gangrene. 5 The technical details that distinguish this technique from other methods of management are: (i) placement of a Foley catheter into the anal canal; and (ii) placement of a stoma bag over the protruding end of the Foley catheter. This acts as a vent, maintaining the VAC seal while enabling the continuous collection of secretions from the anal canal. This reduces congestion of the sponge with secretions while maintaining negative pressure, which aids in clean and effective wound healing, tissue granulation and neovascularisation.
References
- 1. Kuzaka B, Wróblewska MM, Borkowski Tet al. Fournier’s gangrene: clinical presentation of 13 cases. Med Sci Monit 2018; 24 : 548–555. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Chernyadyev SA, Ufimtseva MA, Vishnevskaya IFet al. Fournier’s gangrene: literature review and clinical cases. Urol Int 2018; 101 : 91–97. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Oguz A, Gümüş M, Turkoglu Aet al. Fournier’s gangrene: a summary of 10 years of clinical experience. Int Surg 2015; 100 : 934–941. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Singh A, Ahmed K, Aydin Aet al. Fournier’s gangrene. A clinical review. Arch Ital Urol Androl 2016; 88 : 157–164. [DOI] [PubMed] [Google Scholar]
- 5. Zhang N, Yu X, Zhang K, Liu T. A retrospective case series of Fournier’s gangrene: necrotizing fasciitis in perineum and perianal region. BMC Surg 2020; 20 : 259. [DOI] [PMC free article] [PubMed] [Google Scholar]



