Abstract
Background
Fertility is one of the three main components which determines the size, structure, and composition of a population, and fertility preferences are important measures for forecasting fertility levels of a population. Therefore, this study aims to assess the impacts of the inequalities in the utilization of key maternal health services on fertility preference among high parity women in four selected regions (i.e., Afar, Beninshangul-Gumuz, Gambella and Somali) of Ethiopia.
Methods
The study used data collected for the 2016 Ethiopian Demographic and Health Surveys (EDHS) survey. It includes a total of 977 high parity women (104 urban and 873 rural) residing in the four regions of the study. Bivariate logistic regression was used to select the potential variables by using a cut off p-value < 0.2 and then the multivariable logistic regression analyses were performed to assess the association between the selected explanatory variables (i.e., control and exposure variables) and the outcome variable (i.e. fertility preference). Further, the study employed a Population Attributable Fractions (PAFs) to examine the population level impacts of the inequalities in maternal and child health service variables on fertility preference.
Results
The results showed that religion, household wealth index, place of delivery and contraceptive use were significantly associated with fertility preference. The results of the PAFs analysis indicated that contraceptive use had the biggest impact (80%), meaning that non-use of contraceptive increased fertility preference among women in the four regions. Similarly, out of health facility delivery increased fertility preference by 37%.
Conclusion
The study findings underscore the critical factors influencing women’s fertility preferences in the studied regions. Low utilization of maternal health services had an impact on fertility preference, accounting for more than half of the observed variations in fertility preferences. To address this issue, targeted interventions are recommended: enhancing access to maternal health services, strengthening fertility control programs, promoting the benefits of using these services, and actively addressing inequalities.
Keywords: ANC, Decomposition, Ethiopia, Fertility preference, Inequality, Place of delivery, PNC, PAF
Background
Maternal health is the health of women during pregnancy, childbirth, and in the post-partum period [1].Maternal health has been becoming a global concern because the lives of millions of women in reproductive age can be saved through maternal health care services [2, 3]. The key maternal health services include antenatal care (ANC), delivery care, postnatal care (PNC) and family planning (contraceptive) services. Recent studies indicated that nearly all pregnant women in developed countries who have low fertility, experience greater access to the key maternal health care services like ANC and delivery care. Contrary to this, women in low- and middle-income countries (LMICs) have high fertility and poor utilization of maternal health services [3–5].
Antenatal care (ANC) is also used by health providers as an opportunity to promote the use of skilled attendance at birth, the exciting family planning options, healthy life style changes, benefit for optimal pregnancy spacing, and benefit of child limiting [6, 7].Health facility delivery also another opportunity to provide information after delivery including the exciting family planning options and providing counseling about birth spacing. Countries with high rates of female contraceptive use typically have lower fertility rates [8]. Further, the studies also show that contraceptive utilization has an impact on fertility behavior [9].
Fertility is one of the three main components which determine the size, structure, and composition of a population. In three decades, the global fertility rate dropped from 3.2 live births per woman in 1990 to 2.3 in the year 2021. In similar manner, the Sub-Saharan Africa Total Fertility Rate (TFR) dropped from 6.3 births per woman in 1990 to 4.6 in 2021 [5]. Among all regions in the world, the Sub-Sharan Africa is well known for its highest fertility level [5]. Fertility preferences are important measures for forecasting fertility, calculating levels of unwanted or mistimed birth, and assessing unmet need for contraceptives [10].
Ethiopia is one of the Sub-Saharan Africa countries experiencing a fast population growth and has the highest fertility rate in the region [5, 11]. The TFR of Ethiopia in 1990 was 6.9 birth per-women which declined to 4.3 children per woman in the year 2019 [11]. In Ethiopia, there is a huge spatial variation in TFR by place of residence (such as regional and rural-urban differentials). For instance, the total fertility rate (TFR) in Somali region was 6.4 children per woman, a region known for the highest TFR [11].
Despite pro-poor health policies in Ethiopia, maternal, neonatal, and child health services utilization remains a challenge. The study done by Alem, and colleagues assessed inequality in the utilization of various maternal and child health services. Findings revealed that maternal health services were low and unevenly distributed, favoring better-off women particularly skilled birth attendance. In contrast, preventive child health services were evenly distributed. Ethiopia aims for universal and equitable use of health services. The other studies done by Alem et al., examined the association between household wealth, and maternal education with the utilization of maternal and child health services. The results indicated that higher household wealth was linked to an increased likelihood of skilled birth assistance during delivery and full child immunization. Furthermore, women’s education demonstrated a positive association solely with skilled birth assistance during delivery. Educated women were more likely to receive skilled attendance during childbirth, particularly within more wealthy households. Alem et al., also done a qualitative exploratory study which highlighted inequality in MCH service utilization. Education played a significant role; educated individuals were more likely to seek timely care. Addressing educational disparities is crucial for improving maternal and child health services. These studies emphasize the need for targeted interventions to bridge gaps in health service utilization, especially among vulnerable populations in Ethiopia [12–14].
According to the 2016 Ethiopian Demographic and Health Survey (EDHS) report, 36.7% of currently married women in Ethiopia either desire no more children or have undergone sterilization at the national level. In the study regions, we find that the proportions of mothers who wanted no more children were as follows: 12.4% in Afar, 7.9% in Somali, 35.1% in Benishangul-Gumuz, and 30.7% in Gambella [15].
Several socio-demographic characteristics affect fertility preference such as age, marital status, income, household wealth, employment, educational level, parity, place of residence (urban-rural), region, religion, and number of children ever born, partners preference, sex preference for children [10, 16, 17]. Inequalities in the utilization of health services are among the most critical public health concerns in low-income economies. Despite modest progress in service utilization, significant inequality persists both within and between countries (WHO, 2010). Studies also indicated the existence of inequalities among various population groups (such as rural vs. urban, educated vs. less educated…etc.) in the utilization of maternal health services in Ethiopia [18, 19].
The 2019 Ethiopian Mini Demographic and Health Survey, though conducted in relatively smaller sample size, indicates the key maternal health services utilization in Ethiopia was very low. i.e., the percentage of ANC utilization with the recommended 4+ visits was 43%, women’s delivered in a health facility was 47.5%, women’s who attended a postnatal checkup during the first 2 days after their birth were 33.8% and 41.4% of women were found as users of any one method of contraceptive [20]. Further, there is also a regional inequality in the utilization of the key maternal health services in Ethiopia. For those regions included in this study; the key maternal health services utilization was reported as; ANC service utilization (at least four times during pregnancy) was 28.3% in Afar, 23% in Somali, 31.8% in Gambella and 55.9% in Benishangul Gumuz. This indicates except Benishangul Gumuz all of the remining three regions had a lower utilization of ANC service in reference to the national average (43%) [20].
The percentage of the health facility delivery was 28.3% in Afar, 23% in Somali, 63.7% in Benishangul Gumuz and 70.3% Gambela, indicating that the health facility delivery in Afar and Somali regions were lower than the national average. The prevalence of postnatal checkup during the first 2 days after birth was 23% in Afar, 10.3% in Somali, 45% in Benishangul Gumuz, and 55% in Gambella. This suggests that Gambella and Benishangul Gumuz had a higher utilization of the PNC service compared to the other study regions and with the national average (33.8%). However, the current contraceptive use ratees in all of the study regions were lower than the national average 41.4%) i.e., only 12.7% in Afar, 3.4% in Somali, 38.5% in Benishangul Gumuz and 33.8% in Gambella were using any one of the contraceptive methods [20].
Ethiopia needs to provide effective health interventions to reduce fertility level and achieve the Sustainable Development Goals by 2030. It is important to understand how inequalities in receiving maternal health services affect fertility preferences at the population level. However, little attention has been paid to the impact of inequalities in maternal health service on fertility preference in the four study regions, where women have lower access to services and higher fertility levels. Previous studies on this topic have mainly focused on estimating prevalence, determinants, and geographical variation [21–24].
Therefor our study fills the gap in the research on the population level attribution of maternal services to fertility preferences in four selected regions of Ethiopia. Moreover, the study has a methodological contribution/relevance by using Population Attributable Fractions (PAF) to measure inequalities and population level impacts of service utilization, which are rarely used in large scale data. In addition, understanding the fertility preferences among women with high parity contributes to improved reproductive health outcomes. By informing targeted interventions, promoting reproductive autonomy, and bridging the gap between expressed desires and contraceptive practices, we empower individual decision-making. Therefore, the study aims to assess the impacts of inequalities in the utilization of key maternal health services on fertility preference among high parity women in the study regions (Afar, Benishangul Gumuz, Gambella and Somali regions of Ethiopia). The study warrants primarily to answer the question “How much is the proportional reduction in fertility preference attributable to Maternal health service utilization in the four regions of Ethiopia”.
Methods
The study setting
Ethiopia is a federal democratic republic country composed of eleven national regional states and two chartered administrative cities. Among them, the four regional states of Ethiopia (Afar, Beninshangul-Gumuz, Gambella and Somali) signify a considerable part of the country’s most underdeveloped parts. According to the Ethiopian Statistics Service (ESS) projection, the size of the Ethiopia population by July 2022 was 123.4 million, of which, those residing in the four regions comprised 2.51 million in Somali, 2.03 million in Afar, 1.22 million in Benishangul-Gumuz and 508 thousands in Gambella [25].
The aforementioned-four regions of Ethiopia are known by relatively new administrations which needs further support to align their capacity to the standards required and practiced by those relatively developed regional states and chartered administrative cities of the country. Further, those four regions have a common characteristics that includes; relatively slow underlying pace of development in several sectors including the development of the basic infrastructures, long-standing disputes which are commonly shaped by several factors including their being peripheral in location, the existence of inequities in levels of development across all regions, the volatility and influx of refugees from bordering countries, all situated in a areas where Ethiopia shares a country border with its neighboring countries, they are prone and commonly encounters unforeseen natural phenomena’s like recurrent drought and flooding, having multiple ethnic groups, weak governance, and limited social services [26–28].
Data source and sampling
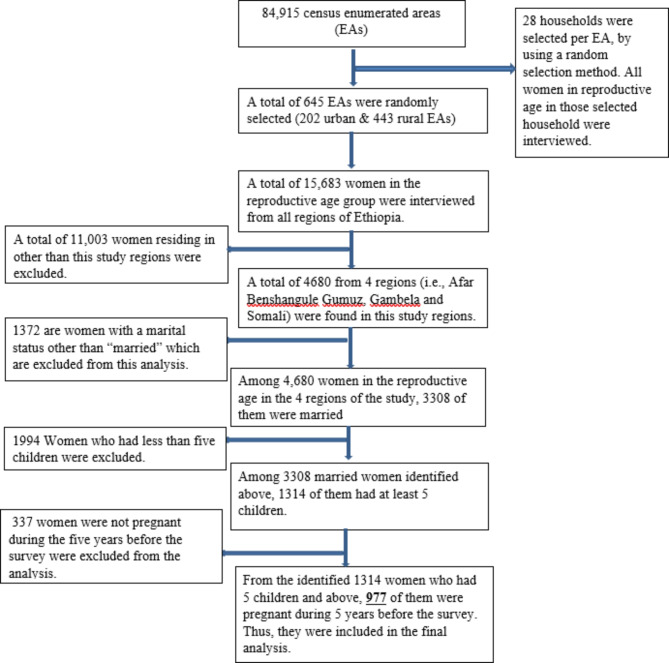
This study utilized a secondary data collected for 2016 Ethiopia Demographic and Health Surveys (EDHS). The EDHS is a nationally representative data that provides up-to-date estimates of key demographic and health indicators for Ethiopia. Among other things; the EDHS data also includes information on maternal health services, fertility, knowledge and utilization of contraception… etc. The EDHS employed a two-stage stratified sampling technique i.e., a total of 645 Enumeration Areas (EAs) were selected in the first stage and a fixed 28 households per EA were selected in the second stage. The main criteria of selecting the respondent was “All women in the age group 15 to 49 years who permanently lived or visitors and who stayed the night before the survey and were available during the survey”. Further, five different DHS Program’s standard questionnaires were adopted and used during EDHS. Therefore, the current study only included married women with at least five births during the five years prior to the survey. It was determined that 977 women (aged 15 to 49) in total (104 from urban and 873 from rural) met the eligible criteria for the analysis. Figure 1 shows the detail of the selection processes of the respondents for this study.
Fig. 1.
Schematic presentation of the sampling procedure
Outcome variables
The outcome variable of the study is fertility preference. The information on fertility preference was collected in the Demographic and Health Surveys by asking married women whether they want more children or not. The responses included “have another”, “undecided”, “no-more”, “sterilized (respondent or partner)”, “declared fecund” and “never had sex”. For the purposes of this study, we re-classified responses into a dichotomous response as 0 = no which includes responses of those married women’s that includes “no-more”, “sterilized (respondent or partner)”, “declared fecund” and “never had sex” and 1 = yes (have preference) which includes “have another” and “undecided” [29, 30]. Ethiopia has a very high total fertility rate (4.3 births per woman) [11]. High fertility is define as having five or more children by a women over her reproductive period [31]. In addition, the study also denoted high fertility in reference to the national average. Therefore, this study included women with high fertility, who reported having five and more children during the survey period.
Exposure and control variables
The main exposure variables we wanted to measure the impacts on the outcome variable were the key maternal health service utilization variables (ANC, place of delivery, PNC, and contraception utilization). Socio demographic variables were used as a control variables, i.e. they were used as confounding variables in the analysis so that examining the net effects of the MHS variables is possible.Table 1 summarizes the list and description of exposure and control variables included in the study.
Table 1.
Description of exposure and control variables
| Exposure variables | ||
| Name of variables | Variable Description | Coding |
| ANC | Health care during pregnancy 5 years before the survey. | 1. < 4 |
| 2. > = 4 | ||
| Place of delivery | Births by place of delivery 5 years before the survey. | 1. Out of Health facility |
| 2. Health facility | ||
| PNC | Care given to the women after delivery 5 years before the survey. | 1. No |
| 2. Yes | ||
| Current use of contraceptive | Use of any medicines, devices, or surgery to prevent pregnancy. | 1. Not Using |
| 2. Using | ||
| Control variables | ||
| Name of variables | Variable Description | Coding |
| Women age | Age in completed years. | 1. 15–19 |
| 2. 20–34 | ||
| 3. 35–49. | ||
| Husband/partner education level /women educational level | Women or men aged 15–49 by highest level of schooling attended or completed. | 1.No education |
| 2.Primary education, | ||
| 3. Secondary & above | ||
| Residence | Place of residence is the type of place where the respondent resides. | 1.Urban |
| 2. Rural | ||
| Household size | The number of persons in a household. | 1.<=5, |
| 2.>6 | ||
| Work status | Women/husband employed in the 12 months before the survey. | 1.Not working |
| 2. working | ||
| Women autonomy on their own-health care | Women’s ability and freedom to make independent decisions about their medical care. | 1. No(women with her husband / her husband/ others) |
| 2- Yes (by her own ) | ||
| Wealth Index | Composite measure of a household’s cumulative living standard measured by ownership of key assets. | 1.Poorest |
| 2. Poorer | ||
| 3.Midle | ||
| 4.Richer | ||
| 5.Richest | ||
| Religion | Religion could be based on self-identification, affiliation, beliefs, practices, or other indicators of religious involvement of the respondent. | 1. Muslim |
| 2. orthodox, | ||
| 3. protestant | ||
| 4. Other | ||
| Husband desire for more children | Husband wants to have more kids. | 1. want more |
| 2. others |
Statistical analysis
For data cleaning and analysis, a statistical software called Stata v-17 [32] and SPSS v-25 [33] were used. The analysis of this study followed four steps: univariate (descriptive), bivariate and multivariable logistic regression, and computation of Population Attributable Fractions (PAFs) analysis. Bivariate logistic regression was used to select the potential variables by using a cut off p-values < 0.2 and then the multivariable logistic regression analyses were performed to assess the association between the main exposure variables and the outcome variable (i.e. fertility preference), controlling for the possible effects of the confounding variables.
To check possible multicollinearity among the independent variables, the study used Variable Inflation Factor (VIF) and those which showed a VIF values > 2.5 were excluded from further analysis. In this regard, the preliminary analysis result indicated that there was significant multicollinearity among region, religion, husband age and women age variables. Therefore, the study excluded two potential predictors (women age and region) from the logistic regression analysis. For multivariable logistic regression analysis, a p-value < 0.05 with 95% confidence interval were used to declare statistical significant associations. To select the best fitting model, we used the Akaike Information Criterion (AIC) and Bayesian Information Criterion (BIC). Further, we applied regression-based Population Attributable Fractions (PAFs) which is considered as a reliable method in measuring population level impacts of interventions or risk factors [34].
PAF works under four major assumptions. It primarily assumes causality, which is a causal relationship between a specific exposure (such as a risk factor) and a disease or adverse condition. It implies that the exposure contributes to the occurrence of the desired outcome Second; PAF assumes that other risk factors are unaffected when estimating the fraction of cases attributable to a specific exposure. Multiple risk factors often interact, and their effects may not be independent. Ignoring shared causal responsibility or multicausality can lead to misinterpretations of PAFs. The third assumption is realistic intervention which indicates PAF provides insights into the potential impact of reducing exposure to a risk factor. It assumes that interventions are feasible and can realistically reduce exposure. In summary, PAF informs research priorities and guides public policies by quantifying the proportion of disease burden attributable to specific risk factors [35].
Greenland and Drescher [36] introduced the methods of obtaining Attributable Fractions directly from logistic regression analysis. In this study, we adopted the steps identified by Simon Ruckinger et al. (2009) to calculate the PAF of the risk factor of interest [34].
Step I
The risk factor must be coded dichotomously. It is ‘removed’ from the population by classifying all individuals as unexposed, irrespective of their real status.
Step II
The predicted probabilities for each-individual estimated by using this modified dataset with the below formula:
 |
Where α is the estimate for the intercept of the logistic regression model, β represents the parameter vector for the covariates included in the model, and xi representing the observations of the covariates for everyone, however, with the ‘removed’ covariate set to zero for all individuals.
Step III
The sum of all predicted probabilities is the adjusted number of cases of the fertility preference that would be expected if the risk factor was absent in the population.
Step IV
The PAF is finally calculated by subtracting these expected cases from the observed cases and dividing by the observed cases.
Further, employing a combination of Population Attributable Fractions (PAFs) and multivariable logistic regression to measure inequality in maternal health services (MHS) utilization is believed to add up to the robustness of the findings. PAFs quantify the proportion of health outcomes attributable to specific risk factors, indirectly revealing inequality across different population groups. Meanwhile, multivariable logistic regression models consider multiple risk factors simultaneously, adjusting for confounders and showing how these factors impact distinct subgroups. By estimating PAFs directly from logistic regression results, we gain context-specific insights into risk factor impacts within specific populations, informing targeted interventions and addressing health inequalities.
Results
Back ground characteristics of respondent
Table 2 summarizes the characteristics of the 977 respondent drawn from the four regions (Afar, Benishangul Gumuz, Gambella and Somali). Most respondents were residing in the rural areas (89.4%) and the remaining 10.6% of them resided in urban areas. Most of the respondents of the study (47.6%) were in the age group 24–34 years. Majority (88.4%) of women had no education. Most of the women were living in poorest households (70%). About 75% of the respondents were Muslim and 74% were not working during the survey period.
Table 2.
Background characteristics of women with high parity in four regions of Ethiopia (n = 977)
| Characteristics | Number | Percent |
|---|---|---|
| Region | ||
| Afar | 236 | 24.2 |
| Somali | 388 | 39.7 |
| Benishangul Gumuz | 225 | 23.0 |
| Gambela | 128 | 13.1 |
| Type of place of residence | ||
| Rural | 873 | 89.4 |
| Urban | 104 | 10.6 |
| Women age | ||
| <=24 | 106 | 10.8 |
| 25–34 | 465 | 47.6 |
| >34 | 406 | 41.6 |
| Education level | ||
| No education | 864 | 88.4 |
| Primary | 93 | 9.5 |
| Secondary and above | 20 | 2.0 |
| Household wealth status | ||
| Poorest | 684 | 70.0 |
| Poorer | 103 | 10.5 |
| Middle | 56 | 5.7 |
| Richer | 66 | 6.8 |
| Richest | 68 | 7.0 |
| Religion | ||
| Muslim | 737 | 75.4 |
| Orthodox | 66 | 6.8 |
| Protestant | 138 | 14.1 |
| Others | 36 | 3.7 |
| Work status | ||
| No | 723 | 74.0 |
| Yes | 254 | 26.0 |
| Total | 977 | 100 |
Bivariate relationship between socio demographic variables and fertility preference
Table 3 presents the results of the chi-square analysis and the percentage distribution of fertility preferences of married women in the four regions of Ethiopia by the selected characteristics and key maternal health service variables. The results revealed that women who resided in all of the age groups had a higher proportion of fertility preference, and also a gradual decline in fertility preference also observed when we go from the early to late reproductive age groups, i.e., 92.9% of those women who were in the age of 24 years and less, 81.3% from the main childbearing ages, and 67.2% of women whose age is greater than and equal to 34 years had fertility preference. The proportion of fertility preference was higher among those in no education category compared to women with primary, secondary, and above education status, respectively. Larger proportion (82%) of women from Muslim religion had higher fertility preference.
Table 3.
Result of bivariate relationship between socioeconomic variables, key maternal health service and fertility preference(N = 977)
| Characteristics | Fertility preference | χ2(P value ) | |
|---|---|---|---|
| No Number and % |
Yes Number and % |
||
| Women age | |||
| <=24 | 1(7.1) | 13(92.9) | < 0.001 |
| 24–34 | 92(18.7) | 401(81.3) | |
| >=34 | 154(32.8) | 316(67.2) | |
| Women Education Level | |||
| No education | 200(23.1) | 664(76.9) | < 0.001 |
| Primary | 39(41.9) | 54(58.1) | |
| Secondary and above | 8 ( 40.0) | 12(60.0) | |
| Religion | |||
| Muslim | 131(17.8) | 606(82.2) | < 0.001 |
| Orthodox | 42(63.6) | 24(36.4) | |
| Protestant | 59(42.8) | 79(57.2) | |
| Others | 15(41.7) | 21(58.3) | |
| Region | |||
| Afar | 33(14.0) | 203(86.0) | < 0.001 |
| Somali | 44(11.3) | 344(88.7) | |
| Benishangul Gumuz | 120(53.3) | 10546.7) | |
| Gambela | 50(39.1) | 78(60.9) | |
| Type of place of residence | |||
| Rural | 220(25.2) | 653(74.8) | 0.47 |
| Urban | 27(26.0) | 77(74.0) | |
| Work status | |||
| No | 159(22.0) | 564(78.0) | < 0.001 |
| Yes | 88(34.6) | 166(65.4) | |
| Women autonomy on their health care | |||
| No | 186(24.3) | 581(75.7) | 0.09 |
| Yes (by hear own ) | 61(29.0) | 149(71.0) | |
| Husband age | |||
| <=34 | 20(18.9) | 86(81.1) | 0.02 |
| 35–44 | 106(22.8) | 359(77.2) | |
| > 45 | 121(29.9) | 285(70.2) | |
| Husband education | |||
| No education | 151(21.3) | 559(78.7) | < 0.001 |
| Primary | 60(35.5) | 108(64.3) | |
| Secondary and above | 36(36.4) | 63(63.6) | |
| Wealth index | |||
| Poorest | 129(18.9) | 555(81.1) | < 0.001 |
| Poorer | 34(33.0) | 69(67.7) | |
| Middle | 26(46.45) | 30(53.6) | |
| Richer | 34(51.5) | 32(48.5) | |
| Richest | 24(35.3) | 64.7) | |
| Household size | |||
| <=5 | 20(20.4) | 78(79.6) | 0.24 |
| >=6 | 227(25.8) | 652(74.2) | |
| Husband desire for more children | |||
| want more children | 85(23.4) | 278(76.6) | 0.32 |
| others | 161(26.3) | 452(73.7) | |
| ANC | |||
| < 4 | 182(22.3) | 633(77.7) | < 0.001 |
| >=4 | 65(40.1) | 97(59.9) | |
| Place of delivery | |||
| Out of health facility | 186(22.7) | 633(77.3) | < 0.001 |
| At health Facility | 61(38.6) | 97(61.4) | |
| PNC | |||
| No | 214(24.4) | 662(75.6) | 0.07 |
| Yes | 21.9) | 68(67.3) | |
| Current contraceptive use | |||
| Not using | 197(21.6) | 714(78.4) | < 0.001 |
| Using | 50(75.8) | 16(24.2) | |
| Total | 247 | 730 | |
Further, the result in Table 3 also showed women’s fertility preferences based on the key maternal health services (ANC, place of delivery, PNC, and current contraceptive use). About 78% of women who attended ANC services below the recommended 4 visits, 77.3% of women who delivered out of health facilities, and 78.4% of women who did not use any contraceptives had a higher proportion of fertility preference.
Multivariable logistic regression model for investigating the impact of key maternal health service on fertility preference
Table 4 shows that religion, household wealth status, place of delivery, and current contraceptive use have a significant association with fertility preference in the four study regions. The results reveal that women who delivered at health facilities had 41% lower odds of fertility preference (AOR: 0.59; 95% CI: 0.04 to 0.36; P < 0.05) than women who delivered out of health facilities. Moreover, the results in Table 4 show that women who are currently using contraceptives had 71% lower odds of fertility preference (AOR: 0.19; 95% CI: 0.00 to 0.10; P < 0.05) than women who are not using contraceptives.
Table 4.
Multivariable binary logistic regression analysis for examining the effects of key maternal health services on fertility preference in four regions of Ethiopia (N = 977)
| Variables | Model1 (Control variables only) |
Model 2 (Control and exposure variables) |
||||||
|---|---|---|---|---|---|---|---|---|
| AOR | P value | 95%CI | AOR | P value | 95%CI | |||
| Women education level | ||||||||
| Not educated RC | ||||||||
| Primary | 0.73 | 0.23 | 0.44 | 1.22 | 0.75 | 0.28 | 0.44 | 1.28 |
| Secondary and above | 1.03 | 0.95 | 0.36 | 2.96 | 0.96 | 0.94 | 0.33 | 2.84 |
| Religion | ||||||||
| Muslim RC | ||||||||
| Orthodox | 0.16 | 0.00 | 0.09 | 0.28 | 0.19 | 0.00 | 0.11 | 0.36 |
| protestant | 0.33 | 0.00 | 0.22 | 0.52 | 0.34 | 0.00 | 0.21 | 0.53 |
| Others | 0.28 | 0.00 | 0.14 | 0.56 | 0.31 | 0.00 | 0.15 | 0.64 |
| Women autonomy on their own health care | ||||||||
| No RC | ||||||||
| Yes | 0.75 | 0.13 | 0.52 | 1.08 | 0.72 | 0.09 | 0.49 | 1.05 |
| Working status | ||||||||
| No RC | ||||||||
| Yes | 0.88 | 0.47 | 0.62 | 1.25 | 0.92 | 0.66 | 0.64 | 1.33 |
| Husband education level | ||||||||
| Not educated RC | ||||||||
| Primary | 0.93 | 0.73 | 0.61 | 1.42 | 1.06 | 0.79 | 0.68 | 1.66 |
| Secondary and above | 0.89 | 0.68 | 0.51 | 1.55 | 0.99 | 0.96 | 0.55 | 1.75 |
| Wealth index combined | ||||||||
| Poorest RC | ||||||||
| Poorer | 0.49 | 0.00 | 0.30 | 0.80 | 0.68 | 0.14 | 0.40 | 1.14 |
| Middle | 0.31 | 0.00 | 0.17 | 0.56 | 0.44 | 0.01 | 0.23 | 0.85 |
| Richer | 0.33 | 0.00 | 0.18 | 0.58 | 0.50 | 0.03 | 0.27 | 0.95 |
| Richest | 0.49 | 0.02 | 0.27 | 0.89 | 0.76 | 0.42 | 0.39 | 1.48 |
| ANC | ||||||||
| < 4 RC | ||||||||
| >=4 | 0.76 | 0.23 | 0.48 | 1.19 | ||||
| Place of delivery | ||||||||
| Out of health facility RC | ||||||||
| At health Facility | 0.59 | 0.04 | 0.36 | 0.98 | ||||
| PNC | ||||||||
| No | ||||||||
| Yes | 1.20 | 0.55 | 0.66 | 2.17 | ||||
| Current contraceptive use | ||||||||
| Not using RC | ||||||||
| Using | 0.19 | 0.00 | 0.10 | 0.35 | ||||
| AIC | 997.85 | 969.03 | ||||||
| BIC | 1066.23 | 1056.95 | ||||||
RC = Reference category
Population attributable fraction (PAFs) for selected risk factor of fertility preference
The results displayed in Table 5 shows the Population-Attributed Fractions (PAFs), which is an impact measurement of an individual risk factor at the population level. Due to the small proportion of non-fertility preferences among women residing in those four regions of the study, the PAFs were computed only for women who had fertility preferences. The estimated adjusted PAFs indicate that current contraceptive use contributed the biggest proportion (80%) of impacts. This is interpreted as the proportion of fertility preference among women residing in the four regions that could have been reduced at the population level if the exposure (the non-use of contraceptives) had been removed. Similarly, 38% of the fertility preferences of women in the four regions of Ethiopia can be reduced if in the women residing in the poor households were removed. Further, 37% of the fertility preferences of women can also be reduced if the exposure to non-health facility delivery was removed. Moreover, the other socio-demographic factors, including religion and type of place of residence, were also important risk factors whose combined impact at the population level is close to 64%. The combined population-level impacts of all the significant risk factors amounted to 219%.
Table 5.
Population Attributable Fraction (PAFs) for selected risk factor of fertility preference in four region of Ethiopia ( N = 977)
| Risk factor | AOR | P value | (95%CI) | PAF % | |
|---|---|---|---|---|---|
| Women age ( < = 24 years age) | 0.98 | 0.39 | -1.25 | 3.22 | 1 |
| Women education (no education) | 0.25 | 0.31 | -0.24 | 0.74 | 20 |
| Religion (Muslim) | 1.23 | 0.00 | 0.86 | 1.60 | 59 |
| Type of place of residence (Rural) | -0.70 | 0.02 | -1.28 | -0.12 | 5 |
| Women currently working (not working) | 0.02 | 0.93 | -0.36 | 0.39 | 1 |
| Women autonomy on their own health care (decision made by her husband/ others) | 0.32 | 0.11 | -0.07 | 0.72 | 22 |
| Husband age ( < = 34 years age) | 0.31 | 0.32 | -0.30 | 0.91 | 3 |
| Husband education (no education) | -0.03 | 0.90 | -0.42 | 0.37 | -2 |
| Wealth index (poorest) | 0.68 | 0.00 | 0.29 | 1.08 | 38 |
| Family size ( < = 5) | 0.13 | 0.63 | -0.40 | 0.67 | 1 |
| Husband desire for more children (want more) | -0.06 | 0.72 | -0.40 | 0.28 | -2 |
| ANC (< 4) | 0.32 | 0.15 | -0.12 | 0.77 | 24 |
| Place of delivery (out of health facility) | 0.56 | 0.02 | 0.08 | 1.04 | 37 |
| PNC (no) | -0.21 | 0.49 | -0.81 | 0.39 | -21 |
| Current contraceptive use (not using) | 1.72 | 0.00 | 1.08 | 2.36 | 80 |
| Total for only significant variables | 219 | ||||
| Total for all variables | 266 | ||||
Discussion
This study has primarily aimed to determine the impacts of the inequalities in utilization of key maternal health services on fertility preference among high-parity women in four regions of Ethiopia (Afar, Benishangul Gumuz, Gambella, and Somali regions). The study employed both the conventional regression analysis and PAF analysis to understand the role of the exposure variables on women’s fertility preference. The first level of analysis, showed the existence of a significant association between a range of predictors (both exposure and control variables) and the dependent variable (fertility preference). The second level of analysis using PAF documented the impacts of the inequalities in the key exposure variables on the outcome variable.
Among the background characteristics used in this study, religion and wealth index were found to have significant associations with fertility preference. i.e., non-Muslim women had a lower desire to have more children compared to Muslim women. This finding is consistent with the results of previous study conducted among two Muslim communities in Kenya and in Ghana, both of which reported that Muslim women prefer red to have more children compared to Christians. The reason reported was that the respondents strongly believed that children are blessing of God [16–37].
This study also found that women who had better wealth status had lower fertility preferences compared to those living in the poorest (lowest) wealth category. This finding is in line with the results of some previous studies which indicated that higher socioeconomic status is associated with lower fertility preferences [16, 39, 40]. The possible explanations for this finding may correspond to the fact that women in the lowest wealth quintile have a greater desire to have more children as most of them believe in the utility of children as old age security i.e., it is a customary practice/expectation that most children will support their family when they grow older. In addition, in most developing countries like Ethiopia, women from the poorest families may not get the opportunity to go to school or they are poorly educated which may, by itself, hinder them from having good knowledge of family planning or reproductive [40, 41].
The contraceptive use and place of delivery had significant associations with fertility preferences. This finding is consistent with other previous studies which indicated that women who use contraception have a lower preference to have more children than those who are not using a contraceptive [39, 40]. Tessema et al. (2020) and Tessema & Tamirat, (2020) reported place of delivery as a key determinant of fertility preference of women in Ethiopia. The possible reason for such association could be skilled health professionals usually provide counseling service on FP choices and birth interval or spacing between births [22, 23]. Furthermore, those women may have a more negative subjective birth experience and an emergency operative mode of delivery (instrumental vaginal delivery or emergency cesarean delivery) which may also related to a change in fertility intentions in their postpartum period i.e., desiring fewer children and/or increasing desired inter-pregnancy interval [42].
Further, the study also analyzed the risk factors or population level impacts using the PAFs analysis. The findings confirmed that the three socioeconomic variables (religion, type of place of residence and wealth index) and the two key maternal health service (place of delivery and current contraceptive use) posed significant impacts on women’s fertility preference. The PAF result in this study exceeded 100%, suggesting that some of the women had multiple risk factors that affected their fertility preference. These risk factors with fertility preference could be prevented by different methods, and the prevention cases of these women could be counted more than once [43].
The combined PAFs of the two main maternal health services (place of delivery and current contraceptive use) in this study were 117%. This means that more than half of the women’s fertility preferences in this study could have been prevented by removing the risk factors (i.e., ensuring access to those nonusers of the services). The other half could also be prevented by addressing the risk factors identified from the socioeconomic variables. As previous studies indicated, the PAF results for a specific population may not be fitting or consistent to the PAF results done in other populations, since there might be a varying prevalence of risk factors [34]. This makes comparison of PAF results across different population.
This study has several strengths, such as the use of a nationally representative dataset that helps to make sound generalizations of the findings. It also has a methodological contribution/ relevance as it addressed population-level impacts of service utilization using Population Attributable Fractions (PAF), which is rarely reported by previous studies. Thus, the findings of the study can serve as one of the few references for similar studies in the future. However, this study also has some limitations. First, the study used a cross-sectional design that limits the inference of causality. Second, some of the responses might have been affected by recall bias, as the respondents might have difficulty remembering events that occurred in the last five years before the survey. Moreover, EDHS did not collect information related to some key socio-cultural variables which play important role in fertility preference. For this reason, the analysis did not account for some variables (such as norms and values, social influences or other family members’ perspectives, especially the husband’s, ) which may have a significant impact on reproductive decisions. The measurement of fertility preferences is based on what currently married women reported which can be changed over time.
Conclusion and implications
This study investigated the factors influencing fertility preferences among high-parity women in four regions of Ethiopia. The finding reveals that maternal health service utilization (such as place of delivery and contraceptive use) and socioeconomic conditions (such as religion, type of residence, and wealth index) significantly impacted fertility preferences. Interestingly, inadequate utilization of essential maternal health services (nonuse of institutional delivery and contraception) accounted for half of the conventional risk factors for fertility preferences.
To address these disparities, we recommend enhancing access to maternal health services through proactive measures, strengthening existing fertility control programs, and engaging religious leaders. Collaborating with religious institutions can promote safe deliveries, adoption of family planning, and overall well-being of women and their children. Additionally, localizing maternal services through implementing mobile clinics, community health workers, and outreach programs is essential. Empowering local leaders to champion maternal health will bridge gaps and ensure equitable access for women in remote areas.
Acknowledgements
The Ethiopian Statistical Authority and ICF International have been acknowledged for granting the authors permission to conduct study using their DHS data.
Abbreviations
- AIC
Akaike information criterion
- ANC
Antenatal Care
- AOR
Adjusted Odd Ratio
- BIC
Bayesian information criterion
- CI
Confidence Interval
- CSA
Central Statistics Agency
- EA
Enumeration Area
- EDHS
Ethiopian Demographic and Health Survey
- MHS
Maternal Health service
- PNC
Post natal care
- VIF
Variance inflation Factor
- WHO
World Health Organization
Author contributions
TS was involved in the study conceptualization, designing, analyzing, and interpreting the data, drafting, and final writing of this manuscript. NR provided the necessary guidance during the draft preparation, reviewing and revising the paper. Both authors read and approved the final manuscript.
Funding
This manuscript is not funded by any funding agency in the public, commercial, or non-governmental organizations.
Data availability
Secondary data from ICF International’s DHS programme (https://dhsprogram.com/data/new-user-registration.cfm). was used for this publication. The data is accessible.
Declarations
Ethics approval and consent to participate
The 2016 EDHS (https://dhsprogram.com/methodology/Protecting-the-Privacy-of-DHS-Survey-Respondents.cfm) follows the required ethical approval procedure and their received participant consent during the data collection. We used publicly accessible secondary data from the 2016 EDHS for this manuscript, and we asked ICF International’s DHS programme for permission to download and use the raw data as well. We were granted this permission through their platform at https://dhsprogram.com/data/new-user-registration.cfm.
Consent for publication
Not applicable.
Computing interests
The authors declare that they have no competing interests.
Footnotes
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.World Health Organization. Maternal health [Internet]. WHO Geneva. 2023.[cited 2023 June]. https://www.who.int/health-topics/maternal-health#tab=tab_1
- 2.World Health Organization (WHO). Maternal mortality [Internet]. WHO Geneva. 2023. [cited 2023 June]. https://www.who.int/news-room/fact-sheets/detail/maternal-mortality Maternal.
- 3.Yaya S, Ghose B. Global Inequality in Maternal Health Care Service utilization: implications for Sustainable Development Goals. Heal Equity. 2019;3(1):145–54. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Shaw D, Guise JM, Shah N, Gemzell-Danielsson K, Joseph KS, Levy B et al. Drivers of maternity care in high-income countries: can health systems support woman-centred care? Lancet [Internet]. 2016;388(10057):2282–95. 10.1016/S0140-6736(16)31527-6 [DOI] [PubMed]
- 5.Department of Economic and Social Affairs PD. World Population Prospects 2022 [Internet]. United Nation. 2022. 1–54 p. [cited 2023 July]. www.un.org/development/desa/pd/
- 6.Begum N, Rahman M, Rahman MM, Nayan SK, Zinia SN, Khan SZ. Utilization of antenatal care services in a selected rural area in Bangladesh. North Int Med Coll J. 2015;6(1):25–8. [Google Scholar]
- 7.World HEalth Organization(WHO). WHO recommendations on antenatal care for a positive pregnancy experuence [Internet]. Geneva: WHO Press. 2016. [cited 2023 June]. https://apps.who.int/iris/rest/bitstreams/1064182/retrieve [PubMed]
- 8.United Nations. World Fertility and Family Planning 2020: Highlights [Internet]. 2020. [cited 2023 June]. https://www.un.org/development/desa/pd/sites/www.un.org.development.desa.pd/files/files/documents/2020/Jan/un_2020_worldfertilityfamilyplanning_highlights.pdf
- 9.Hasan A, Singh MK, Khan AA. Fertility behaviour and contraceptive use in urban slums of district Gorakhpur. Int J Community Med Public Heal. 2017;4(12):4702. [Google Scholar]
- 10.Sennott C, Yeatman S. Stability and Change in Fertility preferences among Young women in Malawi. Int Perspect Sex Reprod Health. 2012;38(01):034–42. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Misganaw A, Naghavi M, Walker A, Mirkuzie AH, Giref AZ, Berheto TM, et al. Progress in health among regions of Ethiopia, 1990–2019: a subnational country analysis for the global burden of Disease Study 2019. Lancet. 2022;399(10332):1322–35. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Wuneh AD, Medhanyie AA, Bezabih AM, Persson LÅ, Schellenberg J, Okwaraji YB. Wealth-based equity in maternal, neonatal, and child health services utilization: a cross-sectional study from Ethiopia. Int J Equity Health. 2019;18(1):1–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Wuneh AD, Bezabih AM, Okwaraji YB, Persson LÅ, Medhanyie AA. Wealth and Education Inequities in Maternal and Child Health Services Utilization in Rural Ethiopia. Int J Environ Res Public Health. 2022;19(9). [DOI] [PMC free article] [PubMed]
- 14.Wuneh AD, Bezabih AM, Persson LÅ, Okwaraji YB, Medhanyie AA, If IW, Educated IW. Call the ambulance and give birth at the Health Facility—A qualitative exploratory study of inequities in the utilization of maternal, newborn, and Child Health Services in Northern Ethiopia. Int J Environ Res Public Health. 2022;19(18). [DOI] [PMC free article] [PubMed]
- 15.Ethiopia Central Statstics Agency(CSA)[Ethiopia] and, Ethiopia Demographic ICF. and Health Survey 2016: Final Report [Internet]. CSA. Addis Ababa, Ethiopia,and Rockville, Maryland, USA; 2017. [cited 2023 July]. https://dhsprogram.com/pubs/pdf/FR328/FR328.pdf
- 16.Ahinkorah BO, Seidu AA, Armah-Ansah EK, Ameyaw EK, Budu E, Yaya S. Socio-economic and demographic factors associated with fertility preferences among women of reproductive age in Ghana: evidence from the 2014 demographic and Health Survey. Reprod Health [Internet]. 2021;18(1):1–10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Rai P, Paudel IS, Ghimire A, Pokharel PK, Rijal R, Niraula SR. Effect of gender preference on fertility: cross-sectional study among women of Tharu community from rural area of eastern region of Nepal. Reprod Health. 2014;11(1):2–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Chaka EE. Inequalities in the Utilization of Maternal Health Services by Key indicators in Ethiopia. J Heal Med Nurs. 2017;39:96–103. [Google Scholar]
- 19.Gebre E, Worku A, Bukola F. Inequities in maternal health services utilization in Ethiopia 2000–2016: magnitude, trends, and determinants. Reprod Health. 2018;15(1):1–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Ethiopian public Health Institiute, ICF. Ethiopia Mini Demographic and Health Survey [Internet]. Addis Ababa. 2019. [cited 2023 June]. https://dhsprogram.com/pubs/pdf/FR363/FR363.pdf
- 21.Muluneh MW, Moyehodie YA. Determinants of desire for more children among women in Ethiopia. BMC Womens Health [Internet]. 2021;21(1):1–7. 10.1186/s12905-021-01563-3 [DOI] [PMC free article] [PubMed]
- 22.Tessema ZT, Tamirat KS. Determinants of high-risk fertility behavior among reproductive-age women in Ethiopia using the recent Ethiopian Demographic Health Survey: a multilevel analysis. Trop Med Health. 2020;48(1):1–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Tessema ZT, Azanaw MM, Bukayaw YA, Gelaye KA. Geographical variation in determinants of high-risk fertility behavior among reproductive age women in Ethiopia using the 2016 demographic and health survey: a geographically weighted regression analysis. Arch Public Heal. 2020;78(1):1–12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Tsegaye Negash B. Fertility intention among married women in Ethiopia: a multilevel analysis of Ethiopian demographic health survey 2016. Contracept Reprod Med [Internet]. 2023;8(1):1–10. 10.1186/s40834-022-00201-z [DOI] [PMC free article] [PubMed]
- 25.Ethiopian Central Statastics Agency. Population Projection [Internet]. Addis Ababa. 2022. [cited 2023 June]. http://www.statsethiopia.gov.et/population-projection/
- 26.Unicef. Context analysis Summery:Ethiopia [Internet]. 2015. [cited 2023 June] https://www.edu-links.org/sites/default/files/media/file/UNICEF 2015 PBEA-Conflict-Analysis_Ethiopia_201504.pdf.
- 27.United Nations. Strengthening Emerging Regional States Governance & Capacity Building [Internet]. United Nation. 2013. [cited 2023 July]. https://info.undp.org/docs/pdc/Documents/ETH/UNDP Ethiopia Fast Facts - Developing Regional States – 2013-12-04.pdf.
- 28.Berger DN, Bulanin N, García-Alix L, Jensen MW, Leth S, Ena Alvarado Madsen DM et al. The Indigenous World 2023 [Internet]. 37th ed. Mamo D, editor. (IWGIA; 2023. 1–721 p. www.nickpurserdesign.com
- 29.Bankole A, Biddlecom AE, Dzekedzeke K. Women’s and men’s fertility preferences and contraceptive behaviors by HIV status in 10 sub-saharan African countries. AIDS Educ Prev. 2011;23(4):313–28. [DOI] [PubMed] [Google Scholar]
- 30.Feyisetan B, Casterline JB. Fertility preferences and contraceptive change. Developing Ctries. 2000;26(3):100–9. [Google Scholar]
- 31.World Bank. Determinants and Consequences of High Fertility [Internet]. Determinants and Consequences of High Fertility. 2010. [cited 2023 July]. https://documents1.worldbank.org/curated/en/389381468147851589/pdf/630690WP0P10870nants0pub08023010web.pdf
- 32.StataCorp TX. StataCorp LLC; 2021. [cited 2023 June] https://downloads.digitaltrends.com/stata/windows
- 33.IBM Corp. IBM SPSS Statistics for Windows (Version 25.0) [Computer software] [Internet]. IBM Corp. 2017. [cited 2023 July]. https://www.scirp.org/%28S%28351jmbntvnsjt1aadkposzje%29%29/reference/referencespapers.aspx?referenceid=2757659
- 34.Rückinger S, Von Kries R, Toschke AM. An illustration of and programs estimating attributable fractions in large scale surveys considering multiple risk factors. BMC Med Res Methodol. 2009;9(1):1–6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Khosravi A, Nazemipour M, Shinozaki T, Mansournia MA. Population attributable fraction in textbooks: Time to revise. Glob Epidemiol [Internet]. 2021;3(August):100062. 10.1016/j.gloepi.2021.100062 [DOI] [PMC free article] [PubMed]
- 36.Greenland S, Drescher K. Maximum likelihood estimation of the attributable fraction from logistic models. Biometrics. 1993;49(3):865. [PubMed] [Google Scholar]
- 37.Abdi B, Okal J, Serour G, Temmerman M. Children are a blessing from God- A qualitative study exploring the socio-cultural factors influencing contraceptive use in two muslim communities in Kenya. Reprod Health. 2020;17(1):1–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Ahinkorah BO, Seidu AA, Armah-Ansah EK, Budu E, Ameyaw EK, Agbaglo E, et al. Drivers of desire for more children among childbearing women in sub-saharan Africa: implications for fertility control. BMC Pregnancy Childbirth. 2020;20(1):1–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Matthew AKPAO. Modeling the Determinants of Fertility among Women of Childbearing Age in Nigeria: Analysis Using Generalized Linear Modeling Approach. Int J Humanit Soc Sci [Internet]. 2012;2(18). https://www.researchgate.net/publication/327208425%0Awww.ijhssnet.com
- 40.Teshale AB, Worku MG, Tesema GA. Fertility decision and its associated factors in Sub-Saharan Africa: a multilevel multinomial logistic regression analysis. BMC Womens Health [Internet]. 2022;22(1):1–11. 10.1186/s12905-022-01920-w [DOI] [PMC free article] [PubMed]
- 41.Atake EH, Gnakou Ali P. Women’s empowerment and fertility preferences in high fertility countries in Sub-saharan Africa. BMC Womens Health. 2019;19(1):1–14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Preis H, Tovim S, Mor P, Grisaru-Granovsky S, Samueloff A, Benyamini Y. Fertility intentions and the way they change following birth-a prospective longitudinal study. BMC Pregnancy Childbirth. 2020;20(1):1–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Rowe AK, Powell KE, Flanders WD. Why population attributable fractions can sum to more than one. Am J Prev Med. 2004;26(3):243–9. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
Secondary data from ICF International’s DHS programme (https://dhsprogram.com/data/new-user-registration.cfm). was used for this publication. The data is accessible.