Abstract
Background
The implementation of evidence-based practices (EBPs) in healthcare is of critical importance, and nursing leadership plays a significant role in this process; however, there is a lack of validated instruments to measure the effectiveness of implementation leadership for EBPs. This study aims to evaluate the validity and reliability of the Turkish version of the Implementation Leadership Scale (ILS) within the context of nursing.
Methods
Data were obtained through a cross-sectional study. The original ILS was first translated into Turkish and then back into English. The scale was administered to 343 nurses working in a training and research hospital in Türkiye. Content validity was assessed with input from 10 experts. The data set was randomly divided into two subsamples to evaluate the construct validity of the ILS. Exploratory factor analyse (EFA) was conducted in sub-sample 1 (n = 172) and Confirmatory factor analyse (CFA) was conducted in sub-sample 2 (n = 171). Reliability was assessed using Cronbach’s alpha values, test-retest reliability, item-total statistics, and split-half reliability.
Results
The content validity index was calculated to be 0.96, indicating high validity. EFA revealed that the scale consists of four factors with eigenvalues greater than 1, and these factors together explained a high proportion of the total variance (77.10%). Confirmatory factor analysis results (χ2 / df = 1.29; CFI = 0.98; GFI = 0.94; AGFI = 0.91; NFI = 0.94; RMSEA = 0.04) confirmed that the Turkish version of the ILS maintains the original four-factor structure (Proactive, Knowledgeable, Supportive, and Perseverant leadership). Cronbach’s alpha values (0.80–0.88) and intraclass correlation coefficients (ICC) (0.78–0.86) were found to be high. Item-total correlations (0.38–0.63) and the Spearman-Brown coefficient (0.75) were above acceptable levels.
Conclusion
The findings suggest that the Turkish version of the ILS is a valid and reliable tool for assessing implementation leadership in evidence-based practice (EBP) among nurses. This version of the ILS could contribute to further research on implementation leadership in Türkiye, international comparisons of EBP leadership, and the development of EBP practices.
Keywords: Evidence-based practice, Implementation leadership, Validity, Reliability, Nurses, Türkiye
Introduction
Evidence-Based Practice (EBP) has become increasingly popular worldwide and has prioritized enhancing quality and improving population health [1, 2]. In healthcare, EBP is widely accepted due to factors such as the vast amount of scientific information, new technologies, an aging population, and rising patient expectations. EBP is suggested to lead to more effective healthcare delivery, increased patient satisfaction, and reduced costs, while also potentially improving clinicians’ work-life aspects. Consequently, the implementation of EBP is of global interest as it promotes quality clinical practice and optimal patient outcomes [3, 4].
EBP involves the conscious, explicit, and judicious use of the best available evidence when making decisions about patient care [5]. It is a problem-solving approach that combines the best evidence from well-designed studies with clinical expertise and patient preferences to achieve optimal outcomes in care delivery [2]. The two main steps in evidence-based practice are: first, translating fundamental scientific knowledge into clinical practice, and second, implementing evidence-based practices that have been proven effective into routine health services and policies within local settings [6]. Leadership is considered a critical factor in organizational change and is frequently identified as a key component in the implementation of organizational changes and innovations [7–9].
Leaders can influence the capacity to promote change and innovation either positively or negatively, and therefore play a crucial role in facilitating an innovative climate and fostering positive attitudes towards EBP [10]. In EBP implementations, leaders have critical roles in providing support, solving problems, adapting EBP, and offering guidance [7]. Effective leadership has been noted to be essential for successful organizational changes, creating a favorable climate for implementation, fostering more positive attitudes towards EBP, and improving patient outcomes such as satisfaction and quality of life [11]. Additionally, leaders play a critical role in facilitating implementation by fulfilling management responsibilities such as planning, organizing, and supervising to ease the process of change [12].
Implementing change in healthcare is a complex and challenging task [5]. Nursing leadership is a critical factor in creating conducive environments for the successful implementation of EBP. Nurses are healthcare professionals who interact with patients more frequently and for longer periods. Therefore, equipping clinical nurses with the ability and opportunities to implement EBP is of utmost importance [2]. Nurse managers play a significant role in overcoming implementation barriers, providing support, and creating appropriate work environments [13]. Nurse managers act as a “link” between executive leadership and frontline clinicians, and they can promote EBP within healthcare organizations. They are responsible for overseeing their units, which includes staff management, budget maintenance, ensuring high-quality nursing practices, quality improvement, and promoting patient safety. Consequently, the facilitation of EBP integration and the creation of an EBP-friendly unit climate are heavily influenced by nurse managers’ leadership [1]. In the nursing context, leadership creates an environment that impacts nurses’ ability to enhance the quality of nursing care [14]. Nurse managers play a vital role throughout the EBP implementation process as they can influence the organizational climate for EBP, the degree of collaboration among team members, and the attitudes of nursing staff towards EBP [4].
Transformational and reward-based leadership theories, along with the full-range leadership model, are among the leadership models most commonly associated with EBP [7, 15, 16]. In particular, the full-range leadership model has frequently been used as a conceptual framework to explore the relationships between leadership and organizational performance. Leadership impacts multiple factors in the organizational context, including culture, communication, networks, and resources, and is key to creating an environment conducive to the implementation of EBP [17]. Transformational leadership emphasizes visionary leadership and directs followers to achieve optimal outcomes through inspiration and motivation. In contrast, reward-based leadership focuses on “transactions” between the leader and followers, incentivizing through rewards and penalties [15]. However, there is ongoing debate about whether these leadership theories are sufficient to understand specific outcomes, such as EBP success. For leadership to be effective in EBP, managers must focus their actions on EBP and demonstrate domain-specific leadership [18].
The leadership style towards EBP is described by the concept of “Implementation Leadership” (IL). IL has emerged as a critical type of leadership necessary for the successful implementation of EBP [19]. IL is defined as a multidimensional influence process involving the activities and behaviors of unit-level managers and supervisors who enable clinical staff to utilize evidence in clinical decision-making processes and impact personnel, the environment, and organizational infrastructure [20]. The implementation of EBP in healthcare institutions is of paramount importance and requires effective leadership. However, there is a lack of adequate assessment tools to measure how well employees evaluate their leaders’ success in implementing EBP. This highlights the need for valid and widely used scales for EBP [21].
Aarons et al. (2014) developed the Implementation Leadership Scale (ILS) in alignment with effective and pragmatic measurement recommendations, emphasizing brevity, reliability, and validity [10]. The ILS is a psychometric tool designed to assess strategic leadership demonstrated by leaders in the implementation of EBP. It consists of 12 items and four subdimensions: (1) proactive leadership, (2) knowledgeable leadership, (3) supportive leadership, and (4) perseverant leadership. Proactive leadership refers to the leader’s ability to anticipate and address challenges related to EBP. Knowledgeable leadership assesses the leader’s understanding of the EBP being implemented and their ability to effectively respond to staff questions. Supportive leadership involves the leader’s support for, recognition of, and endorsement of staff efforts to use and learn EBP. Finally, perseverant leadership measures the leader’s consistency, determination, and responsiveness to challenges and issues in EBP implementation [10, 22].
Initially developed in English, the ILS has been translated into German [17], Norwegian [21], Greek [3], Japanese [4], and Chinese [23], with its validity and reliability confirmed in these languages. The ILS has been validated with clinicians in mental health clinics, counselors in alcohol and drug treatment agencies, and social workers and other health professionals in child welfare services, establishing it as an effective and practical scale for capturing leadership behaviors in EBP implementation [23]. However, there has been no study on the validity and reliability of the Turkish version of the scale. This study aims to investigate the validity and reliability of the Turkish version of the ILS in the context of nursing. A valid and reliable measurement tool is essential for understanding and evaluating the impact of nursing leadership on EBP. The availability of a validated Turkish scale could facilitate further research on EBP in Türkiye and contribute to the improvement of EBP practices.
Method
Participants and procedure
The study is a cross-sectional study. The study was conducted on nurses working in a training and research hospital in Türkiye. Permission to conduct the study was obtained from the authors who developed the ILS. The study was conducted between April 15 and June 15, 2024. In validity and reliability studies, it is generally recommended that the sample size be at least ten times the number of items in the scale [24, 25]. In this study, 500 questionnaires were distributed and 343 nurses voluntarily participated in the study (Response rate: 68.6%).
Data collection tool
Implementation Leadership Scale (ILS)
The ILS consists of four dimensions: proactive leadership, knowledgeable leadership, supportive leadership, and determined leadership. Each dimension includes three items, making a total of 12 items. The items are rated on a 5-point Likert scale (0 = Not at all, 1 = Slight extent, 2 = Moderate extent, 3 = Great extent, 4 = Very great extent). For each subscale, the score is calculated by averaging the item scores assigned to that specific subscale. The scale has two versions: The staff version is designed for employees to evaluate their supervisors/managers, while the supervisor version is for supervisors or managers to evaluate themselves. Both versions contain the same items and same factors, differing only in their references. In the supervisor version, items begin with “I,” while in the staff version, they begin with " name of supervisor” [10]. The scale items are presented in Table 2.
Table 2.
Implementation leadership scale, subscales and item statistics
| Subsample 1 (n = 172) | Subsample 2 (n = 171) | Total Sample (n = 343) | |||||||
|---|---|---|---|---|---|---|---|---|---|
| ILS items, subscales and total | Mean ± SD | EFA Factor Loadings | h2* | Mean ± SD | DFA Factor Loadings | Mean ± SD | |||
| Factor 1 | Factor 2 | Factor 3 | Factor 4 | ||||||
| Proactive leadership | 2.56 ± 0.65 | 2.64 ± 0.64 | 0.57 | 2.60 ± 0.65 | |||||
| 1. Develops a plan to facilitate EBP implementation | 2.57 ± 0.75 | 0.30 | 0.09 | 0.24 | 0.77 | 0.75 | 2.68 ± 0.72 | 0.87 | 2.63 ± 0.74 |
| 2. Minimizes obstacles to implementation of EBP | 2.63 ± 0.77 | 0.35 | 0.11 | 0.21 | 0.75 | 0.73 | 2.71 ± 0.76 | 0.74 | 2.67 ± 0.76 |
| 3. Establishes clear standards for implementation of EBP | 2.48 ± 0.83 | 0.01 | 0.13 | 0.05 | 0.82 | 0.69 | 2.53 ± 0.78 | 0.72 | 2.50 ± 0.81 |
| Knowledgeable leadership | 2.73 ± 0.89 | 2.88 ± 0.84 | 0.62 | 2.81 ± 0.87 | |||||
| 4. Is knowledgeable about EBP | 2.72 ± 0.99 | 0.34 | 0.82 | 0.15 | 0.09 | 0.82 | 2.88 ± 0.98 | 0.87 | 2.80 ± 0.99 |
| 5. Is able to answer staff questions about EBP | 2.76 ± 1.02 | 0.09 | 0.87 | 0.16 | 0.21 | 0.83 | 2.90 ± 1.01 | 0.80 | 2.83 ± 1.02 |
| 6. Knows what he/she is taking about when it comes to EBP | 2.71 ± 0.97 | 0.18 | 0.85 | 0.22 | 0.06 | 0.81 | 2.87 ± 0.90 | 0.75 | 2.79 ± 0.94 |
| Supportive leadership | 2.97 ± 0.84 | 2.98 ± 0.76 | 0.71 | 2.97 ± 0.80 | |||||
| 7. Recognizes and appreciates employee efforts | 3.05 ± 1.03 | 0.86 | 0.16 | 0.20 | 0.21 | 0.84 | 2.96 ± 0.86 | 0.84 | 3.00 ± 0.94 |
| 8. Supports employee efforts to learn more about EBP | 3.01 ± 1.01 | 0.83 | 0.20 | 0.16 | 0.20 | 0.79 | 3.05 ± 0.93 | 0.83 | 3.03 ± 0.97 |
| 9. Supports employee efforts to use EBP | 2.85 ± 0.84 | 0.74 | 0.21 | 0.20 | 0.12 | 0.64 | 2.92 ± 0.82 | 0.77 | 2.88 ± 0.83 |
| Perseverant leadership | 2.61 ± 0.73 | 2.77 ± 0.74 | 0.70 | 2.69 ± 0.74 | |||||
| 10. Perseveres through the ups and downs of implementing | 2.71 ± 0.81 | 0.23 | 0.17 | 0.84 | 0.17 | 0.81 | 2.78 ± 0.82 | 0.89 | 2.75 ± 0.82 |
| 11. Carries on through the challenges of implementing EBP | 2.56 ± 0.85 | 0.18 | 0.14 | 0.85 | 0.08 | 0.78 | 2.74 ± 0.86 | 0.83 | 2.65 ± 0.86 |
| 12. Addresses critical issues about implementation of EBP | 2.58 ± 0.83 | 0.15 | 0.24 | 0.80 | 0.22 | 0.76 | 2.79 ± 0.84 | 0.75 | 2.68 ± 0.84 |
| Implementation leadership scale total | 2.72 ± 0.60 | 2.82 ± 0.54 | 2.77 ± 0.57 | ||||||
| Eigenvalues | 5.39 | 1.49 | 1.27 | 1.11 | |||||
| Variance (%) | 44.91 | 12.39 | 10.60 | 9.21 | |||||
| Cumulative (%) | 44.91 | 57.29 | 67.89 | 77.10 | |||||
*Common Variance
The Turkish translation and adaptation process of the implementation leadership scale (ILS)
The translation process for the ILS followed the standard guidelines for cross-cultural adaptation as recommended by Sousa & Rojjanasrirat [26] and Yu et al. [27], taking their suggestions into account, and was carried out in the following steps: The ILS was translated from its original English language into Turkish by two independent translators fluent in both languages. The author and two nursing academics in a panel meeting assessed the translations. These nursing academics who were familiar with the terminology had worked on EBP, and thus ensuring clarity and contextual relevance of the translation. The combined Turkish translation was then back-translated into English by two professional translators independent of the initial translators. The back-translation was compared with the original text to identify inconsistencies. In the Turkish version, “supervisor” was replaced with “manager” to reflect the Turkish context, because in Türkiye “supervisor” is usually used for nurses who manage night shifts. A pilot study was conducted with 10 volunteer nurses. During the implementation, participants were asked to evaluate the clarity of the scale items. Once it was determined that the scale items were clear and that there were no inconsistencies between the original and final Turkish translations, the Turkish translation was accepted. In order to assess the appropriateness of the scale items, content validity was evaluated by ten experts and then the psychometric properties of the scale were tested.
Data analysis
The data were analyzed using SPSS 21 (Statistical Package for the Social Sciences) and AMOS statistical software. To evaluate the validity of the scale, both content and construct validity were assessed. Content validity was determined by calculating the content validity ratio (CVR) and content validity index (CVI). Exploratory factor analysis (EFA) and confirmatory factor analysis (CFA) were performed to test construct validity. It is recommended that EFA and CFA be conducted on different samples [28]. Therefore, the data set was randomly divided into two subsamples. EFA was conducted in sub-sample 1 (n = 172) and CFA was conducted in sub-sample 2 (n = 171). Reliability of the scale was assessed using Cronbach’s alpha values, intraclass correlation coefficients (ICC), item-total statistics, and the Spearman-Brown coefficient. Reliability analyses (cronbach’s alpha, item-total statistics, split half reliability) were tested both in the total sample and in the subsamples. Skewness and kurtosis values were calculated to assess the normality assumption of the data. In the total sample, kurtosis values ranged from − 0.68 to 0.03, and skewness values ranged from − 0.52 to 0.22. In subsample 1, kurtosis values ranged from − 0.69 to 0.08, and skewness values ranged from − 0.53 to 0.04. In subsample 2, kurtosis values ranged from − 0.66 to 0.45, and skewness values ranged from − 0.47 to 0.31. Kurtosis and skewness values between − 1 and + 1 are assumed to meet the normality assumption [25]. Additionally, the multivariate normality of the data was evaluated in the CFA using a critical value for multivariate kurtosis of 6.22. A multivariate kurtosis value less than 8 suggests that the assumption of multivariate normality is satisfied [29]. Descriptive statistics (mean, standard deviation, frequency, percentage) were used to describe the participants’ characteristics and to analyze the scale and item scores.
Results
Participant characteristics and descriptive statistics
Of the 343 nurses who participated in the study, the majority (86.6%) were female. The average age of participants was approximately 29 years. The average duration of professional experience was around 7 years, while the average time spent working at the hospital was about 4.5 years. More than half of the participants held a bachelor’s degree. Over half of the nurses worked in surgical and internal medicine units (Table 1).
Table 1.
Professional and demographic characteristics of participants (n = 343)
| n | % | Mean ± SD | Min-Max | |||
|---|---|---|---|---|---|---|
| Gender | Female | 297 | 86.6 | |||
| Male | 46 | 13.4 | ||||
| Education | High School | 53 | 15.5 | |||
| Associate Degree | 78 | 22.7 | ||||
| Bachelor’s Degree | 183 | 53.6 | ||||
| Graduate Degree | 29 | 8.2 | ||||
| Unit | Internal Medicine Units | 107 | 31.2 | |||
| Surgical Units | 75 | 21.9 | ||||
| Intensive Care Units | 45 | 13.1 | ||||
| Operating Room | 47 | 13.7 | ||||
| Emergency Department | 69 | 20.1 | ||||
| Age | 28.51 ± 5.42 | 21–49 | ||||
| Years of Service in the Profession | 6.66 ± 5.41 | 1–31 | ||||
| Years of Service in the Hospital | 4.51 ± 3.80 | 1–21 | ||||
When the mean scores of the scale were analyzed, it was determined that the overall mean score of the scale was 2.77 ± 0.57, the dimension with the highest score was supportive leadership (2.97 ± 0.80), and the dimension with the lowest score was proactive leadership (2.60 ± 0.65) (Table 2).
Validity
Content validity
In this study, the opinions of 10 experts were consulted. The expert panel comprised five academicians and five nurse managers. Among the academicians, three of them held the title of associate professor, while two of them were assistant professors and they have conducted research on EBP and leadership. While three of the academicians work in the department of nursing, two of them work in the department of health management. Additionally, among the experts there are five executive nurses with at least a master’s degree education level. These nurse managers are employed in training and research hospitals and familiar to EBP. The experts evaluated each item as “necessary,” “necessary but insufficient,” or “unnecessary.” For each item, the content validity ratio (CVR) was calculated. CVR was determined using the formula CVR = [N/(E/2)] − 1, where N represents the number of experts who rated the item as “necessary” and E represents the total number of experts. The content validity index (CVI) for the scale was calculated by averaging the CVR values across all items. For an assessment by 10 experts, the CVR value should exceed 0.62, and the CVI value should be greater than 0.67 [30]. In this study, the CVR for the items was found to be between 0.80 and 1.00. The CVI was calculated as 0.96, indicating a very high level of content validity.
Construct validity
Exploratory factor analysis
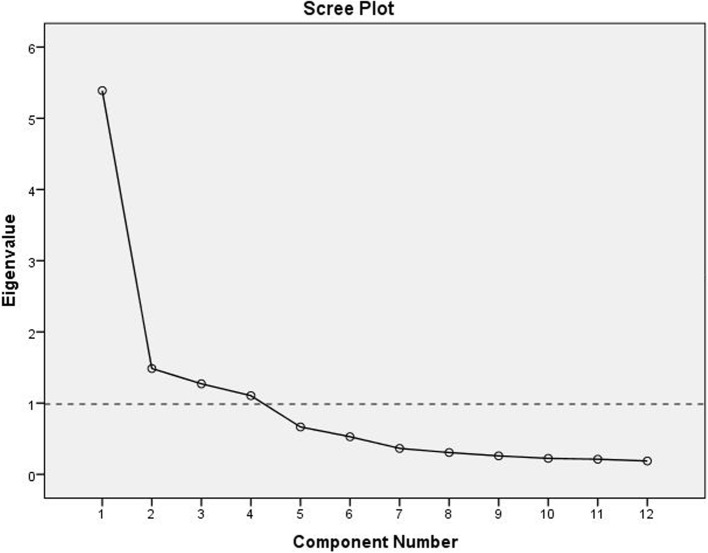
For EFA, the Kaiser-Meyer-Olkin (KMO) measure and Bartlett’s test of sphericity were first conducted. A KMO value greater than 0.60 and a significant Bartlett’s test indicate that the dataset is suitable for factor analysis and that the data structure is factorable [31, 32]. In this study, the KMO value was 0.83, and Bartlett’s test yielded significant results (χ² = 11143.67; df = 67; p < 0.01). The EFA used the principal component method of factor extraction with varimax rotation. The analysis revealed that the scale items loaded onto four factors with eigenvalues greater than 1. The scree plot showed that factors after the fourth one had eigenvalues below 1, with eigenvalues being close to each other and the slope becoming more horizontal (Fig. 1). The contribution of each factor to the total variance was 44.91% for the first factor, 12.39% for the second, 10.60% for the third, and 9.21% for the fourth. Together, the four factors explained 77.10% of the total variance. The factor loadings of the items ranged from 0.74 to 0.87. The communalities of the items ranged from 0.64 to 0.84 (Table 2). Since the communalities greater than 0.50 are considered sufficient for the items to be included in the scale [32], the scale items were deemed to have high communalities.
Fig. 1.
Scree plot of the factor analysis of the Turkish version of the ILS
Confirmatory factor analysis
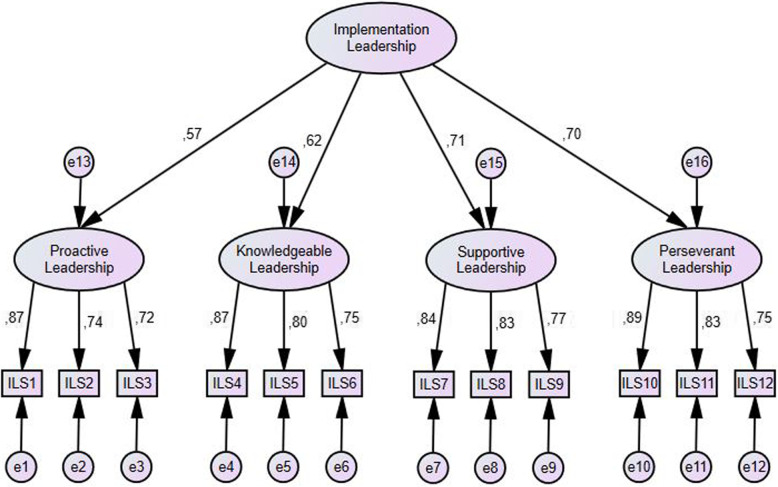
CFA was conducted as it allowed for the validation of the factor structure of the ILS and confirmed the hypothesized relationships between the observed variables and their latent constructs. The first- and second-order estimates in the CFA analysis provide important insights into the structural relationships among the latent variables measured by the ILS. While the first-order estimates reflect the direct relationships between individual items and related factors, the second-order estimates indicate the higher-order structures to which these factors contribute, thus providing a comprehensive understanding of the dimensions underlying practice leadership. In the CFA, the standardized factor loadings for the first-order factors ranged from 0.72 to 0.89, and for the second-order factors, they ranged from 0.57 to 0.71. All factor loadings were found to be statistically significant (p < 0.01) (Fig. 2). The model fit indices were as follows: chi-square/df (χ²/df) = 1.29, Root Mean Square Error of Approximation (RMSEA) = 0.04, Comparative Fit Index (CFI) = 0.98, Goodness of Fit Index (GFI) = 0.94, Adjusted Goodness of Fit Index (AGFI) = 0.91, and Normed Fit Index (NFI) = 0.94 (Table 3). The NFI and GFI values were deemed to be at acceptable levels of fit, while the χ²/df, RMSEA, CFI, and GFI AGFI values were considered to indicate a good level of fit [33].
Fig. 2.
Second-order confirmatory factor analysis and factor loadings of Turkish version of ILS (all factor loadings are standardized and statistically significant, p < 0.01)
Table 3.
Fit indices of the model (n = 171)
| Fit indices | Good fit* | Acceptable fit* | Model | Fit status |
|---|---|---|---|---|
| χ2/df | 0 ≤ χ2/df ≤ 2 | 2 < χ2/df ≤ 3 | 64.61/50 = 1.29 | Good fit |
| RMSEA | 0 ≤ RMSEA ≤ 0.05 | 0.05 < RMSEA ≤ 0.08 | 0.04 | Good fit |
| CFI | 0.97 ≤ CFI ≤ 1 | 0.95 < CFI ≤ 0.97 | 0.98 | Good fit |
| GFI | 0.95 ≤ GFI ≤ 1 | 0.90 < GFI ≤ 0.95 | 0.94 | Acceptable fit |
| AGFI | 0.90 ≤ AGFI ≤ 1 | 0.85 < AGFI ≤ 0.90 | 0.91 | Good fit |
| NFI | 0.95 ≤ NFI ≤ 1 | 0.90 < NFI ≤ 0.94 | 0.94 | Acceptable fit |
*Criteria for fit indices were taken from Yılmaz and Varol (2015)
Reliability
Cronbach’s alpha
The Cronbach’s alpha coefficient for the ILS total was 0.88 in the total sample. The Cronbach’s alpha values for the subdimensions ranged from 0.80 to 0.86. In subsample 1, the Cronbach’s alpha coefficient for the ILS was 0.89, in subsample 2, it was 0.86. (Table 4). These values indicate high internal consistency for both the total scale and its subdimensions [34].
Table 4.
Cronbach’s alpha values and item-total statistics
| Subsample 1 (n = 172) | Subsample 2 (n = 171) | Total Sample (n = 343) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ILS items, subscales and total | α* | Corrected item-total correlation | Squared multiple correlation | α* if item deleted | α* | Corrected item-total correlation | Squared multiple correlation | α* if item deleted | α* | Corrected item-total correlation | Squared multiple correlation | α* if item deleted |
| Proactive leadership | 0.78 | 0.82 | 0.80 | |||||||||
| 1 | 0.59 | 0.59 | 0.88 | 0.53 | 0.56 | 0.85 | 0.56 | 0.56 | 0.87 | |||
| 2 | 0.59 | 0.60 | 0.88 | 0.48 | 0.49 | 0.85 | 0.54 | 0.54 | 0.87 | |||
| 3 | 0.37 | 0.37 | 0.89 | 0.39 | 0.48 | 0.86 | 0.38 | 0.40 | 0.88 | |||
| Knowledgeable leadership | 0.88 | 0.84 | 0.86 | |||||||||
| 4 | 0.64 | 0.69 | 0.87 | 0.56 | 0.61 | 0.85 | 0.61 | 0.65 | 0.86 | |||
| 5 | 0.58 | 0.62 | 0.88 | 0.58 | 0.57 | 0.85 | 0.58 | 0.58 | 0.87 | |||
| 6 | 0.60 | 0.66 | 0.88 | 0.48 | 0.51 | 0.85 | 0.55 | 0.58 | 0.87 | |||
| Supportive leadership | 0.85 | 0.85 | 0.85 | |||||||||
| 7 | 0.66 | 0.67 | 0.87 | 0.58 | 0.61 | 0.85 | 0.62 | 0.62 | 0.86 | |||
| 8 | 0.64 | 0.62 | 0.87 | 0.55 | 0.60 | 0.85 | 0.60 | 0.60 | 0.86 | |||
| 9 | 0.59 | 0.46 | 0.88 | 0.60 | 0.52 | 0.85 | 0.59 | 0.48 | 0.86 | |||
| Perseverant leadership | 0.86 | 0.86 | 0.86 | |||||||||
| 10 | 0.63 | 0.64 | 0.87 | 0.62 | 0.63 | 0.85 | 0.63 | 0.62 | 0.86 | |||
| 11 | 0.54 | 0.56 | 0.88 | 0.57 | 0.60 | 0.85 | 0.56 | 0.57 | 0.87 | |||
| 12 | 0.62 | 0.57 | 0.87 | 0.54 | 0.51 | 0.85 | 0.59 | 0.54 | 0.86 | |||
| ILS total | 0.89 | 0.86 | 0.88 | |||||||||
*Cronbach’s alpha
Item-total statistics
The high and positive correlations between the scale items and the total scale score further indicate that the items measure a similar construct and that the scale has high internal consistency. Item-total correlations are expected to be greater than 0.30 [31]. In this study, item-total correlations in the total sample ranged from 0.38 to 0.63. In subsample 1 and subsample 2, these values ranged from 0.37 to 0.66 and 0.39 to 0.62, respectively and were statistically significant (p < 0.01). (Table 4).
Split-Half reliability
Split-half reliability was assessed using the Spearman-Brown coefficient [35]. For this, the scale items were randomly divided into two equal halves. In the total sample, the Spearman-Brown coefficient in this study was found to be 0.75. For subsample 1, this value was 0.79, and for subsample 2, it was 0.70.
Test-retest reliability (ICC)
To evaluate test-retest reliability, surveys were re-administered to 62 nurses, who were reachable, after an interval of 2–4 weeks (Alpar, 2014; Büyüköztürk, 2013). Intraclass correlation coefficients (ICCs) were calculated. ICCs between 0.60 and 0.75 are considered “good,” while values above 0.75 are deemed “excellent” [36]. In this study, the ICC for the total scale score was 0.86, and the ICCs for the subdimensions ranged from 0.78 to 0.86, indicating high reliability (Table 5).
Table 5.
Intraclass correlation coefficients (n = 62)
| ILS items, subscales and total | ICC | 95% CI (lower–upper bound) |
|---|---|---|
| Proactive leadership | 0.84 | 0.70–0.91 |
| 1 | 0.81 | 0.65–0.89 |
| 2 | 0.72 | 0.50–0.85 |
| 3 | 0.85 | 0.72–0.92 |
| Knowledgeable leadership | 0.86 | 0.74–0.92 |
| 4 | 0.84 | 0.71–0.92 |
| 5 | 0.78 | 0.60–0.88 |
| 6 | 0.82 | 0.68–0.91 |
| Supportive leadership | 0.78 | 0.59–0.88 |
| 7 | 0.83 | 0.69–0.91 |
| 8 | 0.70 | 0.43–0.83 |
| 9 | 0.68 | 0.40–0.82 |
| Perseverant leadership | 0.86 | 0.74–0.93 |
| 10 | 0.80 | 0.62–0.89 |
| 11 | 0.62 | 0.29–0.79 |
| 12 | 0.73 | 0.49–0.85 |
| Implementation leadership scale total | 0.86 | 0.74–0.92 |
Discussion
This study involved the translation of the ILS into Turkish and assessed its validity and reliability among nurses. To assess the content validity of the scale, the CVI was calculated and a high value was obtained [30]. This indicates that there was significant agreement among the experts regarding the validity of the items [37]. EFA and CFA were conducted on different samples to examine the factor structure of the scale. EFA revealed that the scale consists of four factors with eigenvalues greater than 1, and these factors together explained a high proportion of the total variance. A high total variance indicates that the factor structure of the scale is strong and the factors represent practice leadership well enough [31]. CFA revealed that χ²/df, RMSEA, CFI and AGFI were at good fit levels. The good fit of these indices indicates that the model is appropriately structured for the data set and accurately reflects the expected relationships between the factors. NFI and AGFI were found to be at acceptable fit levels. The acceptable levels of these indices indicate that the model provides an adequate fit in general, but there may be space for some improvements [33]. EFA and CFA findings indicate that the Turkish version of the ILS exhibits a well-structured four-factor model. This validation of the four-factor structure is consistent with previous studies [3–5, 10, 17, 21, 38].
Cronbach’s alpha, a widely used measure of internal consistency [39]. In this study, both the overall Cronbach’s alpha value of the ILS and the Cronbach’s alpha values of the subscales of the scale were found to be high. It can be said that this finding is consistent with the findings of previous studies. In the studies conducted by Mandrou et al. [3], Saiki et al. [4], and Hu et al. [5], the overall Coronbach alpha values of ILS were found to be 0.94, 0.97, and 0.93, respectively. Item-total correlations are used as an indicator of internal consistency [31]. The item-total correlation values obtained in this study exceeded the expected threshold. To further assess the reliability of the ILS, test-retest reliability was also evaluated. In this study, both the total score and the subdimensions ICC values were found to be quite high [36]. Similarly, Saiki et al. (2023) found high ICC values in their study with nurses [4]. Additionally, the Spearman-Brown coefficient was examined to test the reliability of the ILS. A Spearman-Brown coefficient above 0.70 is considered sufficient [3]. In this study, the Spearman-Brown coefficient exceeded this threshold, indicating that the scale demonstrates satisfactory split-half reliability.
Overall, the findings suggest that the Turkish version of the ILS is a valid and reliable tool for assessing implementation leadership behavior among nurses. The ILS has demonstrated successful psychometric properties across various professions and languages. The Chinese [23], Greek [3], and Japanese [4] versions of the ILS have been tested among nurses and similarly confirmed to be valid and reliable for evaluating implementation leadership behavior. Additionally, the Norwegian version [21] has been validated among therapists in mental health clinics, the German version [17] among primary care physicians, and the English versions among mental health clinic staff [9, 10] and child health service workers [7].
ILS assesses the degree to which a leader is proactive, knowledgeable, supportive, and perseverant regarding evidence-based practice [10]. Previous studies have shown that effective leadership is an important factor in developing healthcare workers’ attitudes toward EBP. For instance this, a study conducted by Anne Li et al. [40] indicated that leadership is a factor influencing the implementation of EBP. In a study by Harvey et al. [41], it was stated that a combination of managerial and facilitative leadership roles is needed to ensure and strengthen the implementation of EBP in nursing and midwifery. Additionally, a study by Bianchi et al. [42] highlighted that nurse managers play a particularly effective role in implementing EBP by fostering a supportive culture and environment. Measurement tools assessing transformational leadership or general leadership have predominantly been used to evaluate the relationships between leadership and EBP [7, 15, 16]. There is a need for a measurement tool that specifically evaluates EBP leadership to highlight the significant impacts of leadership on EBP and to gain a better understanding of its effects. It can be said that the ILS may serve as a valuable tool in addressing this need.
EBP’s in healthcare are often associated with the quality of patient care and patient outcomes. A systematic review conducted by Connor et al. [43] indicated that the findings demonstrate EBP’s ability to improve patient outcomes. A study by Ramírez-Morera et al. [44] reported slight quality improvements in patient outcomes and healthcare processes due to evidence-based clinical practice guidelines. Research by Clarke et al. [45] expressed that nurses value evidence-based practices and believe they are crucial for standardizing patient care. Additionally, a study by Moreno-Poyato et al. [46] noted that a higher level of evidence-based practices, particularly concerning nurses’ attitudes and knowledge, positively enhances the therapeutic nurse-patient relationship in mental health settings. Therefore, it can be stated that the development of EBP applications in healthcare positively impacts patient outcomes. Consequently, the promotion of EBP by leadership [41, 42] highlights the importance of leadership in EBP initiatives.
When the EBP literature in Türkiye was examined, a significant gap was identified in studies examining the relationship between EBP and leadership. Similarly, Üner and Baykal [47] emphasized that there is not enough research focusing on the role of management in EBP implementation in Türkiye. In addition, Doğan & Bağcı [48], Menekli & Korkmaz [49], and Şadi Şen & Yurt [50] reported that nurses’ attitudes towards evidence-based practice should be improved. Karataş Baran et al. [51] found that 59% of nurse participants did not grasp the concept of evidence-based nursing practice. In addition, Ongün et al. [52] determined that the primary obstacle to the implementation of EBP was inappropriate work environments. As a result, it can be suggested that studies should be conducted to increase the development of EBPs in Türkiye. Implementation leadership is recognized as a crucial factor in promoting EBP [10, 23]. However, there is a need for valid and reliable tools to conduct experimental studies in this area. The ILS, being both a valid and reliable measurement tool and relatively brief, facilitates its application. The Turkish version of the ILS can be utilized in studies on EBP in Türkiye and may contribute to promoting evidence-based practices.
Limitations
This study was conducted with nurses and focused solely on the validity and reliability of the staff version of the ILS. Future research is recommended to assess the validity and reliability of the supervisor version of the ILS with nurse managers. One of the limitation of this study is the potential for variation or bias in the psychometric examination and the generalization of the study results. Additionally, as the study was carried out in a training and research hospital, the findings may not be generalizable to other types of hospitals (e.g., private hospitals) or other professional groups (e.g., doctors). The study was designed as a cross-sectional research, meaning that responses are based on participants’ subjective evaluations and the results may vary over time.
Conclusion
Turkish version of the ILS is a valid and reliable tool for assessing implementation leadership (proactive, knowledgeable, supportive and perseverant leadership) in EBP among nurses. It can be said that there is a gap in the Turkish literature on implementation leadership. The Turkish version of the ILS may contribute to further studies on implementation leadership among nurses in and emphasize the role of practice leadership in EBPs. In the future, it is recommended to conduct studies on the validity and reliability of the ILS on other nurse groups, in different professional groups and in different institutions.
Acknowledgements
The author thanks all participants who voluntarily contributed to this study.
Authors’ contributions
This paper is a single-authored paper and done by the single author. A.Y., conceptualized and designed the study, completed data acquisition, interpreted the data, drafted the manuscript, and supervised the study. The author critically revised and approved the final version of the manuscript.
Funding
No funding was received for conducting this study.
Availability of data and materials
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Declarations
Ethics approval and consent to participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Ethical approval was obtained from the approved by the Batman University Ethics Committee (date: 31.01.2024; decision no: 2024/01–02). Informed consent: Consent was obtained from all participants included in the study.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Shuman CJ, Liu X, Aebersold ML, Tschannen D, Banaszak-Holl J, Titler MG. Associations among unit leadership and unit climates for implementation in acute care: a cross-sectional study. Implement Sci. 2018;13:62. 10.1186/s13012-018-0753-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Zhang YP, Liu WH, Yan YT, Porr C, Zhang Y, Wei HH. Psychometric testing of the evidence-based practice nursing Leadership Scale and the Work Environment Scale after Cross-cultural Adaptation in Mainland China. Eval Heal Prof. 2019;42:328–43. 10.1177/0163278718801439. [DOI] [PubMed] [Google Scholar]
- 3.Mandrou E, Tsounis A, Sarafis P. Validity and reliability of the Greek version of implementation Leadership Scale (ILS). BMC Psychol. 2020;8:1–7. 10.1186/s40359-020-00413-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Saiki M, Tomotaki A, Fukahori H, Yamamoto T, Nishigaki M, Matsuoka C et al. Reliability and Validity of the Japanese Version of the Implementation Leadership Scale for Nurse Managers and Staff Nurses: A Cross-Sectional Study. J Nurs Manag. 2023;2023. 10.1155/2023/4080434.
- 5.Hu J, Gifford W, Ruan H, Harrison D, Li Q, Ehrhart MG, et al. Validating the implementation Leadership Scale in Chinese nursing context: a cross-sectional study. Nurs Open. 2021;8:3420–9. 10.1002/nop2.888. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Carlson MA, Morris S, Day F, Dadich A, Ryan A, Fradgley EA, et al. Psychometric properties of leadership scales for health professionals: a systematic review. Implement Sci. 2021;16. 10.1186/s13012-021-01141-z. [DOI] [PMC free article] [PubMed]
- 7.Finn NK, Torres EM, Ehrhart MG, Roesch SC, Aarons GA. Cross-validation of the implementation Leadership Scale (ILS) in child Welfare Service organizations. Child Maltreat. 2016;21:250–5. 10.1177/1077559516638768. [DOI] [PubMed] [Google Scholar]
- 8.Mosson R, Von Thiele Schwarz U, Hasson H, Lundmark R, Richter A. How do iLead? Validation of a scale measuring active and passive implementation leadership in Swedish healthcare. BMJ Open. 2018;8:1–11. 10.1136/bmjopen-2018-021992. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Torres EM, Ehrhart MG, Beidas RS, Farahnak LR, Finn NK, Aarons GA. Validation of the implementation Leadership Scale (ILS) with supervisors’ self-ratings. Community Ment Health J. 2018;54:49–53. 10.1007/s10597-017-0114-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Aarons GA, Ehrhart MG, Farahnak LR. The implementation leadership scale (ILS): development of a brief measure of unit level implementation leadership. Implement Sci. 2014;9:1–10. 10.1186/1748-5908-9-45. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Egeland KM, Skar AMS, Endsjø M, Laukvik EH, Bækkelund H, Babaii A, et al. Testing the leadership and organizational change for implementation (LOCI) intervention in Norwegian mental health clinics: a stepped-wedge cluster randomized design study protocol. Implement Sci. 2019;14:1–12. 10.1186/s13012-019-0873-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Guerrero EG, Padwa H, Fenwick K, Harris LM, Aarons GA. Identifying and ranking implicit leadership strategies to promote evidence-based practice implementation in addiction health services. Implement Sci. 2016;11:1–13. 10.1186/s13012-016-0438-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Clavijo-Chamorro MZ, Romero-Zarallo G, Gómez-Luque A, López-Espuela F, Sanz-Martos S, López-Medina IM. Leadership as a facilitator of evidence implementation by nurse managers: a metasynthesis. West J Nurs Res. 2022;44:567–81. 10.1177/01939459211004905. [DOI] [PubMed] [Google Scholar]
- 14.Kim HO, Lee I, Lee BS. Nursing leaders’ perceptions of the state of nursing leadership and the need for nursing leadership education reform: a qualitative content analysis from South Korea. J Nurs Manag. 2022;30:2216–26. 10.1111/jonm.13596. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Cheng L, Feng S, Hu Y, Broome ME. Leadership practices of nurse managers for implementing evidence-based nursing in China. J Nurs Manag. 2018;26:671–8. 10.1111/jonm.12594. [DOI] [PubMed] [Google Scholar]
- 16.Holmberg R, Fridell M, Arnesson P, Bäckvall M. Leadership and implementation of evidence-based practices. Leadersh Heal Serv. 2008;21:168–84. 10.1108/17511870810893001. [Google Scholar]
- 17.Söling S, Pfaff H, Karbach U, Ansmann L, Köberlein-Neu J, Kellermann-Mühlhoff P, et al. How is leadership behavior associated with organization-related variables? Translation and psychometric evaluation of the implementation leadership scale in German primary healthcare. BMC Health Serv Res. 2022;22:1–13. 10.1186/s12913-022-08434-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Richter A, von Thiele Schwarz U, Lornudd C, Lundmark R, Mosson R, Hasson H. iLead-a transformational leadership intervention to train healthcare managers’ implementation leadership. Implement Sci. 2016;11:1–13. 10.1186/s13012-016-0475-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Castiglione SA. Implementation leadership: a concept analysis. J Nurs Manag. 2020;28:94–101. 10.1111/jonm.12899. [DOI] [PubMed] [Google Scholar]
- 20.Gifford W, Graham ID, Ehrhart MG, Davies BL, Aarons GA. Ottawa model of implementation leadership and implementation leadership scale: mapping concepts for developing and evaluating theory-based leadership interventions. J Healthc Leadersh. 2017;9:15–23. 10.2147/JHL.S125558. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Braathu N, Laukvik EH, Egeland KM, Skar AMS. Validation of the Norwegian versions of the implementation Leadership Scale (ILS) and Multifactor Leadership Questionnaire (MLQ) in a mental health care setting. BMC Psychol. 2022;10:1–11. 10.1186/s40359-022-00725-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Aarons GA, Ehrhart MG, Torres EM, Finn NK, Roesch SC. Validation of the implementation Leadership Scale (ILS) in Substance use Disorder Treatment organizations. J Subst Abuse Treat. 2016;68:31–5. 10.1016/j.jsat.2016.05.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Hu J, Gifford W, Ruan H, Harrison D, Li Q, Ehrhart MG, et al. Translation and linguistic validation of the implementation leadership scale in Chinese nursing context. J Nurs Manag. 2019;27:1030–8. 10.1111/jonm.12768. [DOI] [PubMed] [Google Scholar]
- 24.Büyüköztürk Ş. Factor analysis: Basic concepts and using to Development Scale. Educ Adm Theory Pract. 2002;32:470–83. [Google Scholar]
- 25.Gürbüz S. AMOS Ile yapısal eşitlik modellemesi [Structural equation modeling with AMOS]. Ankara: Seçkin Yayıncılık; 2019. [Google Scholar]
- 26.Sousa VD, Rojjanasrirat W. Translation, adaptation and validation of instruments or scales for use in cross-cultural health care research: A clear and user-friendly guideline. J Eval Clin Pract. 2011;17:268–274. 10.1111/j.1365-2753.2010.01434.x2011;17:268–74. [DOI] [PubMed]
- 27.Yu DSF, Lee DTF, Woo J. Issues and challenges of instrument translation. West J Nurs Res. 2004;26:307–20. 10.1177/0193945903260554. [DOI] [PubMed] [Google Scholar]
- 28.Worthington RL, Whittaker TA. Scale Development Research: a content analysis and recommendations for best practices. Couns Psychol. 2006;34:806–38. 10.1177/0011000006288. [Google Scholar]
- 29.Klein RB. Principles and pracitce of structural equation modeling. The Guilford Press.
- 30.Alpar R. Uygulamalı İstatistik ve Geçerlilik-Güvenirlik: SPSS’de Çözümleme Adımları İle Birlikte, [Applied Statistics and Validity-Reliability: With Analysis Steps in SPSS]. 3rd edition. Ankara: Detay Yayıncılık; 2014.
- 31.Büyüköztürk Ş. Sosyal bilimlerde veri analizi el kitabı [Handbook of data analysis in social sciences]. 18th edition. Ankara: Pegem Akademi; 2013.
- 32.Kalaycı Ş. SPSS uygulamalı çok değişkenli istatistik teknikleri [Multivariate statistical techniques with SPSS]. 5th edition. Ankara: Asil Yayın Dağıtım; 2010.
- 33.Yılmaz V, Varol S. Hazır yazılımlar ile yapısal eşitlik modellemesi: AMOS, EQS, LISREL [Structural equation modeling with ready-made software: AMOS, EQS, LISREL]. Dumlupınar. Univ J Soc Sci. 2015;151:10–7. [Google Scholar]
- 34.Özdamar K. Paket programlar ile istatistiksel veri analizi (cilt 1) [Statistical data analysis with package programs]. Ankara: Nisan Kitabevi; 2013. [Google Scholar]
- 35.Alpar R. Uygulamalı çok değişkenli istatistiksel yöntemler [Applied multivariate statistical methods]. 4th edition. Ankara: Detay Yayıncılık; 2013.
- 36.Günal A, Pekçetin S, Demirtürk F, Şenol H, Håkansson C, Wagman P. Validity and reliability of the Turkish Occupational Balance Questionnaire (OBQ11-T). Scand J Occup Ther. 2020;27:493–9. 10.1080/11038128.2019.1673479. [DOI] [PubMed] [Google Scholar]
- 37.Beckstead JW. Content validity is naught. Int J Nurs Stud. 2009;46:1274–83. 10.1016/j.ijnurstu.2009.04.014. [DOI] [PubMed] [Google Scholar]
- 38.Shuman CJ, Ehrhart MG, Torres EM, Veliz P, Kath LM, VanAntwerp K, et al. EBP implementation Leadership of Frontline Nurse managers: validation of the implementation Leadership Scale in Acute Care. Worldviews Evidence-Based Nurs. 2020;17:82–91. 10.1111/wvn.12402. [DOI] [PubMed] [Google Scholar]
- 39.Dilekçi Ü, Sezgin Nartgün Ş. Adaptation of teachers’ perceived adaptive performance scale to Turkish culture: validity-reliability and descriptive analysis. Hacettepe Egit Derg. 2020;35:448–65. 10.16986/HUJE.2019052615. [Google Scholar]
- 40.Anne Li S, Jeffs L, Barwick M, Stevens B. Organizational contextual features that influence the implementation of evidence-based practices across healthcare settings: a systematic integrative review. Syst Rev. 2018;7:1–19. 10.1186/s13643-018-0734-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Harvey G, Kelly J, Kitson A, Thornton K, Owen V. Leadership for evidence-based practice—enforcing or enabling implementation? Collegian. 2020;27:57–62. 10.1016/j.colegn.2019.04.004. [Google Scholar]
- 42.Bianchi M, Bagnasco A, Bressan V, Barisone M, Timmins F, Rossi S, et al. A review of the role of nurse leadership in promoting and sustaining evidence-based practice. J Nurs Manag. 2018;26:918–32. 10.1111/jonm.12638. [DOI] [PubMed] [Google Scholar]
- 43.Connor L, Dean J, McNett M, Tydings DM, Shrout A, Gorsuch PF, et al. Evidence-based practice improves patient outcomes and healthcare system return on investment: findings from a scoping review. Worldviews Evidence-Based Nurs. 2023;20:6–15. 10.1111/wvn.12621. [DOI] [PubMed] [Google Scholar]
- 44.Ramírez-Morera A, Tristán M, Salazar-Vargas J, Rivera-Chavarría AL. Effects of evidence-based clinical practice guidelines for breast cancer in health care quality improvements. A second systematic review. F1000Research. 2022;11:1–19. 10.12688/f1000research.126126.2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Clarke V, Lehane E, Mulcahy H, Cotter P. Nurse practitioners’ implementation of evidence-based practice into Routine Care: a scoping review. Worldviews Evidence-Based Nurs. 2021;18:180–9. 10.1111/wvn.12510. [DOI] [PubMed] [Google Scholar]
- 46.Moreno-Poyato AR, Casanova-Garrigos G, Roldán-Merino JF, Rodríguez-Nogueira Ó. Examining the association between evidence-based practice and the nurse-patient therapeutic relationship in mental health units: a cross-sectional study. J Adv Nurs. 2021;77:1762–71. 10.1111/jan.14715. [DOI] [PubMed] [Google Scholar]
- 47.Üner Z, Baykal Ü. Kanıta dayalı hemşirelik yönetimi [Evidence-based nursing management]. Fenerbahçe Üniversitesi Sağlık Bilim Derg. 2024;4:439–46. 10.56061/fbujohs.1434021. [Google Scholar]
- 48.Doğan R, Bağcı N. Karaciğer Nakli hemşirelerinin kanıta dayalı hemşireliğe yönelik tutumlarının incelenmesi [Investigation of the attitudes of liver transplant nurses towards evidence-based nursing]. Perspect Palliat Home Care. 2023;1:26–34. 10.29228/pphcjournal.66324. [Google Scholar]
- 49.Menekli T, Korkmaz M. Dâhiliye hemşirelerinin kanıta dayalı hemşireliğe yönelik tutumları. Intern Med Nurses’ Attitudes towards Evidence-Based Nurs. 2021;14:38–47. 10.46483/deuhfed.782131. [Google Scholar]
- 50.Sadi Sen E, Yurt S. Hemşirelerin kanıta dayalı uygulamalara yönelik tutumlarının belirlenmesi. [Determining the attitudes of nurses towards evidence-based practices]. Dokuz Eylül Üniversitesi Hemşirelik Fakültesi Elektron Derg. 2021;14:102–7. 10.46483/deuhfed.737729. [Google Scholar]
- 51.Karataş Baran G, Atasoy S, Şahin S. Hemşirelerin kanıta dayalı hemşirelik uygulamalarına yönelik farkındalık ve tutumlarının değerlendirilmesi [Evaluation of nurses’ awareness and attitudes towards evidence-based nursing practice]. Celal Bayar Üniversitesi Sağlık Bilim Enstitüsü Derg. 2020;7:352–9. 10.34087/cbusbed.699410. [Google Scholar]
- 52.Ongün P, Ayoğlu T, Öztürk Kandemir D, Akyüz N. Evidence-based practices and Research results of Surgical Unit Manager nurses using obstacles and proposals: descriptive research. Turkiye Klin J Nurs Sci. 2022;14:35–42. 10.5336/nurses.2021-83187. [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.