Abstract
Background
Previous studies have shown that overall sleep quality among Chinese nurses is relatively low, with a sleep disorder prevalence rate of approximately 66.4%. Against the backdrop of healthcare reforms, China has been striving to improve the mental health and sleep quality of nurses. Stress mindset can influence how individuals respond to stress, but there is limited research on how stress mindset affects nurses’ sleep quality. This study aims to explore the impact of stress mindset on sleep quality among nurses, as well as the mediating roles of stress overload and anxiety in this relationship.
Methods
The study was conducted online using a questionnaire from February 18 to February 22, 2024. It utilized the Stress Mindset Measure (SMM), the Stress Overload Scale-Short (SOS-S), the Generalized Anxiety Disorder 7-item scale (GAD-7), and the Pittsburgh Sleep Quality Index (PSQI) to survey 441 nurses in three regions of China: Chongqing, Hunan, and Shandong (M = 34.39, SD = 7.82, 95.7% female). A chain mediation model was employed to examine the mediating roles of stress overload and anxiety in the relationship between stress mindset and sleep quality.
Results
The participants’ average sleep quality score was 7.18 ± 3.47. Nurses’ stress mindset was significantly negatively correlated with both stress overload and anxiety, and significantly positively correlated with sleep quality. Stress overload was significantly positively correlated with anxiety and significantly negatively correlated with sleep quality. Anxiety was also significantly negatively correlated with sleep quality. The direct effect of nurses’ stress mindset on sleep quality was significant (effect size = -0.10, 95% CI: -0.19 to -0.01), as were the indirect effects through stress overload (effect size = -0.05, 95% CI: -0.11 to -0.01) and anxiety (effect size = -0.09, 95% CI: -0.13 to -0.05), along with their chain mediation effect (effect size = -0.10, 95% CI: -0.14 to -0.06).
Conclusion
Our study demonstrates that a higher level of nurses’ stress mindset is associated with better sleep quality, with stress overload and anxiety mediating this relationship. A positive stress mindset helps nurses cope more effectively with professional challenges and reduces anxiety, leading to improved sleep quality. Healthcare institutions should therefore prioritize fostering positive stress mindsets in nurses, encouraging regular psychological training and workshops to support the development of effective coping strategies.
Keywords: Nurses, Stress mindset, Sleep quality, Stress overload, Anxiety
Introduction
The demand for healthcare is unlimited, but healthcare resources are limited. With the rapid aging of China’s population, the need for high-quality nursing care and full-life-cycle services continues to grow. According to the 2022 Statistical Bulletin on the Development of Health and Health Undertakings in China, the total number of healthcare personnel is 14.41 million, with nurses outnumbering doctors at a ratio of 1.17:1 [1]. Consequently, Chinese nurses are facing increasing work pressure and challenges [2]. As the cornerstone of healthcare development, nurses often work under high pressure, intensity, and risk. The continuity of nursing care in medical institutions requires them to frequently adjust their work and sleep schedules to meet job demands [3]. Therefore, shift work is particularly common among nurses [4]. Shift work is one of the leading causes of circadian rhythm disruption, resulting in significant changes in sleep patterns and biological functions. This disruption affects both mental and physical health and negatively impacts work performance [5]. Irregular shift patterns and increased workloads make nurses a vulnerable group susceptible to poor sleep quality [6]. Many nurses experience sleep issues such as insomnia, frequent dreams, and difficulty maintaining sleep. These sleep disturbances not only affect their daily lives and work efficiency but may also trigger a range of physical and mental illnesses [7].
Sleep quality, anxiety, and high levels of stress are interconnected in a bidirectional relationship. Stress reflects the dynamic interaction between an individual and their environment, evaluated as the balance between perceived demands and available resources [8]. When an individual perceives that environmental demands exceed their adaptive capacity, psychological stress occurs [9]. This stress results from the interaction of external environmental factors and internal psychological perceptions, constituting what is termed “stress overload” [10]. When demands overwhelm resources, normal functioning deteriorates, increasing vulnerability to illness [11]. Nurses are particularly exposed to significant work-related stress due to shift work and long hours, often leading to sleep deprivation and disorders [12]. Sleep deprivation can impair cognitive functions, negatively affecting decision-making, attention, and increasing the risk of medical errors, ultimately compromising patient safety [13]. Prolonged sleep deprivation can dysregulate the hypothalamic-pituitary-adrenal (HPA) axis, raising cortisol levels and triggering anxiety and depression [14]. This physiological response contributes to fatigue, burnout, and chronic health issues such as cardiovascular disease [15]. These adverse effects can create a negative feedback loop, worsening stress and further disrupting sleep quality [16].
Adopting a positive stress mindset may mitigate these negative effects by altering individuals’ perceptions of stress and enhancing their coping strategies [17]. Stress mindset refers to the belief that stress can lead to either positive or negative outcomes [17]. Specifically, individuals can have a stress-is-enhancing mindset, believing that stress leads to benefits such as improved work efficiency, better health, and personal growth, or a stress-is-debilitating mindset, viewing stress as harmful and resulting in reduced efficiency and poorer health. This mindset significantly affects cognitive, emotional, and physiological stress responses, shaping how individuals interpret and emotionally react to stressful situations [18]. The critical factor is not the amount of stress a person experiences, but how they perceive and respond to it [19]. A positive stress mindset encourages individuals to see stress as a challenge rather than a threat, which can reduce physiological stress responses and improve mental health [20]. This shift in perspective is linked to reduced anxiety and depression, greater resilience, and better sleep quality [21]. By fostering a positive stress mindset, interventions may help break the negative cycle of stress and sleep disturbances, ultimately improving both nurses’ health and the quality of care they provide [22].
In the high-intensity and high-pressure work environment of Chinese nurses, ensuring adequate sleep is challenging. This lack of sufficient sleep negatively affects both their work and personal lives, posing risks to both the nurses and their patients. Therefore, mitigating the impact of work-related stress on nurses’ physical and mental health and improving their sleep quality is of critical importance. While much research has explored the effects of stress on sleep quality, fewer studies have focused on how stress mindset influences sleep quality through stress overload and anxiety, particularly in the nursing population. Nurses with a stress-enhancing mindset are more likely to perceive stress as an opportunity for growth and development, potentially reducing their levels of stress overload [17, 21]. Lower stress overload, in turn, may reduce the occurrence of negative emotions such as anxiety [10, 11]. However, this process is shaped by individual factors such as coping strategies, social support, and personality traits [23]. Anxiety is known to be associated with a decline in sleep quality [24], but sleep quality is also influenced by a variety of factors, including physical health, sleep hygiene habits, and environmental conditions [25]. Therefore, the relationship between stress mindset and sleep quality is complex, involving multiple interrelated variables. Understanding how stress mindset, stress overload, anxiety, and sleep quality interact requires a multifaceted approach.
For nurses, stress mindset may affect sleep quality through the mediating roles of stress overload and anxiety, as well as through their chain mediation. This relationship is particularly significant for nurses, who face intense work-related stress, frequent night shifts, and rotating schedules [26]. These occupational characteristics make them especially vulnerable to high levels of stress overload and anxiety [27]. Additionally, the high demands of responsibility and emotional engagement in nursing further exacerbate the negative effects of stress and anxiety on sleep quality [28, 29]. Studying this chain mediation relationship is crucial for nurses, as it may offer targeted strategies to improve their mental health and sleep quality.
This study employs the Stress Mindset Scale, Stress Overload Scale, Generalized Anxiety Disorder Scale, and Pittsburgh Sleep Quality Index to examine how Chinese nurses’ stress mindset influences sleep quality, with stress overload and anxiety serving as chain mediators in this relationship. The following hypotheses are proposed: Hypothesis 1: Nurses’ stress mindset positively predicts sleep quality, indicating that a higher stress mindset correlates with better sleep quality. Hypothesis 2: Stress overload mediates the relationship between nurses’ stress mindset and sleep quality. Hypothesis 3: Anxiety mediates the relationship between nurses’ stress mindset and sleep quality. Hypothesis 4: Stress overload and anxiety jointly mediate the relationship between nurses’ stress mindset and sleep quality in a chain mediation model.
Methods
Sample and data collection
To improve the generalizability of the findings, this study included nurse samples from various regions of China, specifically from the western, central, and eastern areas. This approach ensured sample diversity and enhanced the representativeness of the results, providing a more robust data foundation for subsequent analysis. A convenience sampling method was used, with online questionnaire links distributed to nurse work groups in 12 hospitals across the three regions, allowing interested nurses to participate by clicking the link. This web-based cross-sectional study took place from February 18 to February 22, 2024. The questionnaire was hosted on an online data collection platform, beginning with an informed consent form that participants could review before deciding whether to participate. To ensure data accuracy and completeness, all questions were mandatory, and each IP address was restricted to one submission to prevent duplicates.
The sample size for this study was determined by the rule that it should be 5 to 10 times the number of variables [30]. The study included 22 dimensions for statistical analysis: 10 from the general information questionnaire, 2 from the stress mindset scale, 7 from the Pittsburgh Sleep Quality Index, 1 from the Generalized Anxiety Scale, and 2 from the Stress Overload Scale. To account for potential errors from the convenience sampling method and possible sample loss, a 20% increase in the sample size was recommended, resulting in a required sample size between 138 and 275. In total, 496 questionnaires were collected for the study. Invalid questionnaires were excluded based on completion time (responses completed in less than two minutes were excluded, as the estimated completion time was about three minutes) and response consistency (reverse-scored items were used to verify accuracy). After excluding 55 invalid questionnaires, 441 valid responses remained, resulting in an effective rate of 88.9%.
Measurement instruments
This study gathered data using a combination of the General Information Questionnaire, the Stress Mindset Measure, the Pittsburgh Sleep Quality Index, the Generalized Anxiety Disorder Scale, and the Stress Overload Scale-Short.
General information questionnaire
The general information questionnaire, designed by the researchers, collected data on gender, age, marital status, number of children, highest education level, department, years of work in the current department, professional title, salary, and work shift patterns.
Stress mindset measure (SMM)
The Stress Mindset Measure [29] was used to assess nurses’ stress mindsets. This questionnaire consists of two parts: “stress-is-enhancing mindset” and “stress-is-debilitating mindset”. An example item for the stress-is-enhancing mindset is, “Experiencing stress can improve my health and vitality,” whereas an example item for the stress-is-debilitating mindset is, “The effects of stress are negative and should be avoided.” The scale includes 8 items, scored on a 5-point Likert scale (0 = strongly disagree, 4 = strongly agree). Items 1, 3, 5, and 7 are reverse scored, while items 2, 4, 6, and 8 are positively scored. The average score is calculated to indicate the individual’s stress mindset level, with higher scores representing a stronger stress-is-enhancing mindset. The Chinese version of the scale has been validated among healthcare professionals [31], and the Cronbach’s α coefficient for the Stress Mindset Measure in this study was 0.83.
Pittsburgh sleep quality index (PSQI)
The Pittsburgh Sleep Quality Index [32] was used to assess participants’ sleep quality over the past month. The PSQI includes 18 self-reported items encompassing seven components: sleep quality, sleep latency, sleep duration, sleep efficiency, sleep disturbances, use of sleep medication, and daytime dysfunction. Each component is scored from 0 to 3, with the total PSQI score ranging from 0 to 21, where higher scores indicate poorer sleep quality. A PSQI score greater than 5 differentiates poor sleepers from healthy controls with a sensitivity of 98% and a specificity of 55%, indicating primary sleep disorders [33]. The Chinese version of the PSQI has demonstrated good reliability and validity in Chinese populations [34]. The Cronbach’s α coefficient for the PSQI in this study was 0.93.
Generalized anxiety disorder 7-item scale (GAD-7)
The GAD-7 [35] is commonly used to identify generalized anxiety disorder and assess the severity of its symptoms over the past two weeks. The scale includes 7 items, each scored on a 4-point Likert scale (0 = not at all, 3 = nearly every day), with total scores ranging from 0 to 21. Scores of 0–4 indicate no anxiety, 5–9 indicate mild anxiety, 10–14 indicate moderate anxiety, and 15–21 indicate severe anxiety. The Chinese version of the GAD-7 has been widely used among Chinese populations [36]. The Cronbach’s α coefficient for the GAD-7 in this study was 0.95.
Stress overload scale-short (SOS-S)
The SOS-S [37] was used to assess participants’ stress overload over the past week. The scale includes 10 items divided into two dimensions: Event Load (EL) and Personal Vulnerability (PV). An example item for the EL subscale is, “In the past week, have you felt like you were carrying a heavy burden?” and an example item for the PV subscale is, “In the past week, have you felt like nothing was going right?” The scale uses a 5-point Likert scale (1 = not at all, 5 = very much), with the average scores of EL and PV reflecting the stress overload level. Higher scores indicate higher stress overload. The Chinese version of the SOS-S has been validated in Chinese populations with good psychometric properties [38]. The Cronbach’s α coefficient for the SOS-S in this study was 0.93.
Statistical methods
SPSS 26.0 was used to conduct common method bias testing, descriptive statistical analysis of demographic variables, as well as independent samples t-tests and one-way ANOVA to analyze the relationships between demographic variables and sleep quality. Additionally, correlation analyses were performed to examine the relationships between stress mindset, stress overload, anxiety, and sleep quality, and one-way ANOVA was conducted across the three regions of Chongqing, Hunan, and Shandong. After standardizing all variables, model 6 from Hayes’ PROCESS v3.5 was applied to assess the mediating roles of stress overload and anxiety in the relationship between stress mindset and sleep quality, with stress mindset as the independent variable, sleep quality as the dependent variable, and stress overload and anxiety as mediating variables. The Bootstrap method was employed with 5,000 resamples to test the mediating effects and calculate 95% confidence intervals. An effect was considered significant if the confidence interval did not include zero.
Ethics approval
This study received approval from the Ethics Committee of Southwest University (No. H24118), and participants were required to sign an informed consent form prior to the survey. The research procedures complied with the ethical standards of the Declaration of Helsinki.
Results
Demographic characteristics
Among the 441 nurses surveyed, 422 were female (95.7%) and 19 were male (4.3%). The majority of participants (80.7%) were between 20 and 40 years old. Geographically, 200 participants (45.4%) were from Chongqing, 82 (18.6%) were from Hunan, and 159 (36.0%) were from Shandong. Most participants were married (72.1%) and held a bachelor’s degree (78.2%). In terms of professional titles, 15.6% were nurses, 28.8% were nursing specialists, and 43.8% were head nurses. Regarding work experience in their department, 57.6% had worked for 0–10 years, and 34.0% had 11–20 years of experience. Additionally, 48.1% worked only day shifts, while 39.9% were engaged in a three-shift rotation (Table 1).
Table 1.
Analysis of sleep quality among nurses with different demographic characteristics (N = 441)
| Characteristics | N | % | PSQI (M ± SD) |
t/F | p-value |
|---|---|---|---|---|---|
| Gender | 0.72 | 0.90a | |||
| Male | 19 | 4.3% | 7.74 ± 3.36 | ||
| Female | 422 | 95.7% | 7.15 ± 3.48 | ||
| Age | 0.93 | 0.58b | |||
| 20-40years | 356 | 80.7% | 7.13 ± 3.50 | ||
| 41-60years | 85 | 19.3% | 7.38 ± 3.43 | ||
| Region | 1.11 | 0.33b | |||
| Chongqing | 200 | 45.4% | 7.17 ± 3.34 | ||
| Hunan | 82 | 18.6% | 7.65 ± 3.43 | ||
| Shandong | 159 | 36.0% | 6.94 ± 3.65 | ||
| Marital Status | 2.54 | 0.56b | |||
| Single | 104 | 23.6% | 7.25 ± 3.48 | ||
| Married | 318 | 72.1% | 7.15 ± 3.46 | ||
| Divorced | 14 | 3.2% | 5.86 ± 3.33 | ||
| Other | 5 | 1.1% | 10.80 ± 1.79 | ||
| Education Level | 0.77 | 0.54b | |||
| High School/ Technical School | 8 | 1.8% | 7.13 ± 2.10 | ||
| Associate Degree | 77 | 17.5% | 6.81 ± 3.73 | ||
| Bachelor’s Degree | 345 | 78.2% | 7.26 ± 3.45 | ||
| Master’s Degree | 9 | 2.0% | 6.67 ± 3.04 | ||
| Doctorate | 2 | 0.5% | 10.50 ± 2.12 | ||
| Professional Title | 1.90 | 0.09b | |||
| Nurse | 69 | 15.6% | 6.30 ± 2.90 | ||
| Nurse Practitioner | 127 | 28.8% | 7.55 ± 3.83 | ||
| Nurse-in-charge | 193 | 43.8% | 7.42 ± 3.34 | ||
| Associate Chief Nurse | 33 | 7.5% | 6.42 ± 3.26 | ||
| Chief Nurse | 7 | 1.6% | 5.86 ± 3.98 | ||
| Other | 12 | 2.7% | 7.08 ± 4.17 | ||
| Years of Service | 0.83 | 0.74b | |||
| 0-10years | 254 | 57.6% | 7.20 ± 3.57 | ||
| 11-20years | 150 | 34.0% | 6.89 ± 3.27 | ||
| 21-31years | 31 | 7.0% | 8.52 ± 3.47 | ||
| 31-40years | 6 | 1.4% | 6.50 ± 3.02 | ||
| Shift System | 0.66 | 0.58b | |||
| Day Shift Only | 212 | 48.1% | 7.05 ± 3.31 | ||
| Night Shift Only | 2 | 0.4% | 8.50 ± 3.54 | ||
|
Two-shift System (12-hour work schedule) |
51 | 11.6% | 6.82 ± 3.36 | ||
|
Three-shift System (8-hour work schedule) |
176 | 39.9% | 7.42 ± 3.69 |
ap-value of independent samples t-test
bp-value of one-way analysis of variance (ANOVA)
Correlation between sleep quality and demographic characteristics
Based on the results of independent samples t-tests and one-way ANOVA, no statistically significant differences in sleep quality (the dependent variable) were observed across various demographic characteristics (Table 1). As a result, these demographic factors have a minimal influence on the mediation model and do not need to be included as covariates.
Common method bias
This study utilized self-reported questionnaires, which may introduce common method bias. To mitigate this, reverse scoring and anonymous responses were incorporated into the survey process. Harman’s single-factor test was conducted to assess the presence of common method bias. The results identified nine factors with eigenvalues greater than 1, with the first factor explaining 33.4% of the variance, which is below the critical threshold of 40%. This suggests that common method bias is not a significant concern in this study.
Descriptive statistics and correlation analysis of stress mindset, stress overload, anxiety, and sleep quality
A correlation analysis was conducted on the four variables: stress mindset, stress overload, anxiety, and sleep quality. The results showed that the overall PSQI score among Chinese nurses was poor (7.18 ± 3.47), with 293 nurses (66.4% of the sample) experiencing sleep disorders (PSQI > 5). Stress mindset was significantly negatively correlated with stress overload (r = -0.45, p < 0.001) and anxiety (r = -0.46, p < 0.001), while being significantly positively correlated with sleep quality (r = -0.34, p < 0.001). Additionally, stress overload was significantly positively correlated with anxiety (r = 0.63, p < 0.001) and significantly negatively correlated with sleep quality (r = 0.42, p < 0.001). Anxiety also had a significant negative correlation with sleep quality (r = 0.53, p < 0.001), where higher PSQI scores indicate poorer sleep quality (Table 2).
Table 2.
Descriptive statistics and correlation analysis results of study variables
| Variable | M ± SD | Stress mindset | Stress overload | Anxiety | PSQI |
|---|---|---|---|---|---|
| r | r | r | r | ||
| Stress Mindset | 1.86 ± 0.81 | — | |||
| Stress Overload | 2.43 ± 0.97 | -0.45*** | — | ||
| Anxiety | 5.27 ± 5.11 | -0.46*** | 0.63*** | — | |
| PSQI | 7.18 ± 3.47 | -0.34*** | 0.42*** | 0.53*** | — |
N = 441, *p < 0.05, **p < 0.01, ***p < 0.001, M = Mean, SD = Standard Deviation
One-way ANOVA of nurses in Chongqing, Shandong and Hunan
When comparing the stress mindset, stress overload, anxiety, and sleep quality of nurses from Chongqing, Shandong, and Hunan, it was found that nurses in Chongqing reported the highest levels of stress mindset (M ± SD = 1.91 ± 0.83) and stress overload (M ± SD = 2.46 ± 1.00). Nurses in Shandong had the highest anxiety levels (M ± SD = 5.77 ± 5.54), while nurses in Hunan exhibited the poorest sleep quality (M ± SD = 7.65 ± 3.43). However, according to the results of the one-way ANOVA, no statistically significant differences were observed in stress mindset, stress overload, anxiety, or sleep quality among nurses across these three regions (Table 3).
Table 3.
One-way ANOVA of nurses in Chongqing, Hunan, and Shandong
| M ± SD | F | p-value | ||
|---|---|---|---|---|
| Stress Mindset | Chongqing | 1.91 ± 0.83 | 1.14 | 0.32 |
| Shandong | 1.78 ± 0.84 | |||
| Hunan | 1.89 ± 0.67 | |||
| Stress Overload | Chongqing | 2.46 ± 1.00 | 0.16 | 0.86 |
| Shandong | 2.42 ± 0.96 | |||
| Hunan | 2.39 ± 0.91 | |||
| Anxiety | Chongqing | 5.12 ± 5.00 | 1.39 | 0.25 |
| Shandong | 5.77 ± 5.54 | |||
| Hunan | 4.70 ± 4.43 | |||
| PSQI | Chongqing | 7.17 ± 3.34 | 1.11 | 0.33 |
| Shandong | 6.94 ± 3.65 | |||
| Hunan | 7.65 ± 3.43 |
Chain mediation effect analysis of stress overload and anxiety on the relationship between stress mindset and sleep quality
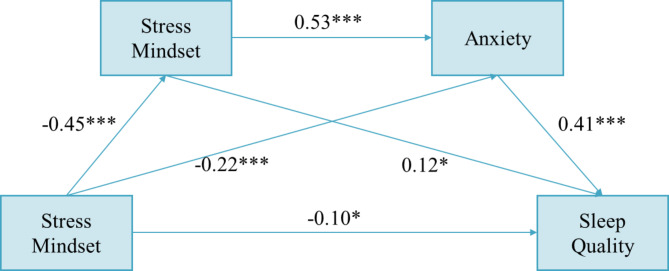
The results showed that a stress mindset positively predicted sleep quality (effect size=-0.10, P < 0.05). Furthermore, it negatively predicted both stress overload (effect size=-0.45, P < 0.001) and anxiety (effect size=-0.22, P < 0.001). In addition, stress overload significantly and positively predicted anxiety (effect size = 0.53, P < 0.001) while negatively predicting sleep quality (effect size = 0.12, P < 0.05). Moreover, anxiety itself negatively predicted sleep quality (effect size = 0.41, P < 0.001) (Fig. 1).
Fig. 1.
Results of the serial mediation analysis. The values shown are the standardized coefficients. *p < 0.05, **p < 0.01, ***p < 0.001
In this mediation model, there are four pathways through which stress mindset predicts sleep quality. Stress mindset directly positively predicted sleep quality (effect size=-0.10, 95% CI: -0.19~-0.01. When stress overload was introduced as a mediator between stress mindset and sleep quality, stress mindset also positively predicted sleep quality (effect size=-0.05, 95% CI: -0.11~-0.01. When anxiety was introduced as a mediator between stress mindset and sleep quality, stress mindset continued to positively predict sleep quality (effect size=-0.09, 95% CI: -0.13~-0.05). When both stress overload and anxiety were introduced as mediators, stress mindset still positively predicted sleep quality (effect size=-0.10, 95% CI: -0.14~-0.06). Thus, the overall effect of stress mindset on sleep quality was significant, and both stress overload and anxiety had significant simple and chain mediation effects in the relationship between stress mindset and sleep quality. The direct effect accounted for 29.4% of the total effect, while the total indirect effect accounted for 70.6% (Table 4).
Table 4.
Direct and indirect effects of stress mindset on sleep quality, with stress overload and anxiety serving as mediators
| Effect value | Boot SE | Boot LLCI | Boot ULCI | Effect size | |
|---|---|---|---|---|---|
| Total effect | -0.34 | 0.04 | -0.43 | -0.25 | 100% |
| Direct effect | -0.10 | 0.05 | -0.19 | -0.01 | 29.4% |
| Total indirect effect | -0.24 | 0.03 | -0.30 | -0.19 | 70.6% |
|
Stress mindset → stress overload → sleep quality |
-0.05 | 0.03 | -0.11 | -0.01 | 14.7% |
| Stress mindset → anxiety → sleep quality | -0.09 | 0.02 | -0.13 | -0.05 | 26.5% |
| Stress mindset → stress overload → anxiety → sleep quality | -0.10 | 0.02 | -0.14 | -0.06 | 29.4% |
Discussion
This study aims to assess the relationship between stress mindset and sleep quality while exploring the mediating roles of stress overload and anxiety. First, we evaluated whether nurses’ stress mindset can positively predict their sleep quality—that is, whether nurses with a higher stress mindset are more likely to have better sleep quality. Next, we examined whether stress overload and anxiety act as mediators in the relationship between stress mindset and sleep quality, indicating that stress mindset may influence sleep quality by reducing stress overload or anxiety. Finally, we investigated whether stress overload and anxiety together form a chain mediation effect between stress mindset and sleep quality, providing further insight into the underlying mechanisms through which stress mindset affects sleep quality.
The current status of nurses’ sleep quality and the relationship between stress mindset, stress overload, anxiety, and sleep quality
The study results indicate that nurses generally experience poor sleep quality, with a prevalence of sleep disorders at 66.4%, which is higher than that of the general population [39–41]. These findings are consistent with previous research that has also reported a high prevalence of sleep disorders among nurses. For instance, a study found that 64.8% of clinical nurses in general hospitals in China suffer from sleep disorders [42]; another study noted that nurses have significantly poorer sleep quality compared to the general population [43]. The poor sleep quality among nurses may be related to the high demands and stressful work environment they face in hospitals. As frontline healthcare providers, nurses are responsible for continuous patient monitoring and direct care, often requiring high-intensity work where mistakes are not tolerated [44]. Compared to other healthcare professionals, nurses more frequently undertake 24-hour shifts, including night shifts and rotating schedules, which are more likely to disrupt their circadian rhythms [45]. This disruption is associated with sleep disorders and decreased sleep quality, a situation particularly prominent among nurses [46].
Our analysis further revealed significant correlations among stress mindset, stress overload, anxiety, and sleep quality within the nurse population. Specifically, a nurse’s stress mindset is significantly negatively correlated with stress overload and anxiety, and significantly positively correlated with sleep quality. Additionally, stress overload is positively correlated with anxiety and negatively correlated with sleep quality, while anxiety is negatively correlated with sleep quality. Individuals with poor sleep quality may develop maladaptive cognitive patterns, such as excessive worry and rumination about sleep, which can exacerbate symptoms of anxiety and depression [47]. These psychological factors are associated with the worsening of sleep disorders, forming a bidirectional relationship between sleep disturbances and mental health issues [48]. Moreover, stress and negative emotions may activate the physiological arousal system, including the hypothalamic-pituitary-adrenal (HPA) axis, potentially further disrupting sleep patterns [14]. The interaction among cognitive, emotional, and physiological factors often leads to a vicious cycle concerning sleep quality.
Studies have shown that anxiety is closely related to poor sleep quality [49], and individuals with generalized anxiety disorder often experience worse sleep quality [50]. High levels of stress are also associated with poor sleep and increased anxiety, with significant correlations observed among job stress, sleep quality, and anxiety in nurses [51, 52]. Various forms of sleep deprivation—whether total sleep deprivation, partial sleep deprivation (e.g., limiting sleep to 4–5 h per night), or sleep fragmentation (frequent sleep interruptions despite adequate total sleep time)—have been shown to be associated with reduced positive emotions, increased symptoms of anxiety and depression, and impaired emotional regulation [53]. Furthermore, individuals with a “stress-is-enhancing” mindset tend to report lower perceived stress [21] and anxiety [17], more positive emotions [17], and better job performance [54]. While previous studies have explored the relationships among stress, anxiety, and sleep quality, this study delves deeper into the role of stress mindset, providing evidence of its interrelation with sleep, emotions, and stress.
The impact of stress mindset on sleep quality and the mediating role of stress overload and anxiety
Our research significantly contributes to the understanding of how stress mindset, stress overload, anxiety, and sleep quality interrelate. This study investigated the associations between nurses’ stress mindset and their sleep quality, focusing on the mediating roles of stress overload and anxiety. The results indicate that nurses with a stress-enhancing mindset tend to have lower levels of stress overload and anxiety, as well as better sleep quality [17]. Conversely, nurses with a stress-debilitating mindset are more likely to report higher stress overload and anxiety, along with poorer sleep quality [21]. This study introduces a new perspective on the relationships among nurses’ stress mindset, emotional well-being, and sleep, enriching the theoretical foundation for stress management.
The results indicate that stress mindset is positively associated with nurses’ sleep quality, with nurses who adopt a stress-enhancing mindset experiencing better sleep, supporting Hypothesis 1. Interestingly, these findings diverge from previous studies conducted on college students [55]. This variation may be related to the heightened work stress [56], more frequent shift work [4], and higher levels of psychological distress [57] that nurses face, which contribute to a greater prevalence of sleep disorders compared to the general population and college students. Although sleep issues are common in other high-stress professions [58], the unique demands and responsibilities of nurses—such as direct patient care, high-stakes decision-making, and emotional labor—may amplify the association between stress mindset and sleep quality in this particular group [59]. This phenomenon may be explained by the influence of sleep-related beliefs on sleep quality [60]. Specifically, an individual’s beliefs and attitudes towards sleep can influence how they address sleep problems. People with negative sleep beliefs often experience heightened anxiety and worry about their sleep difficulties, which in turn is associated with increased physiological arousal and worsened insomnia symptoms [60]. Similarly, stress mindset, as a personal belief, can significantly influence how individuals perceive stress. It shifts the perception from viewing stress as harmful to seeing it as beneficial [61]. This shift toward a positive stress mindset may be associated with reduced anxiety and negative emotions when encountering stress, potentially lowering physiological arousal [61, 62]. Due to reduced arousal and psychological stress, nurses with a stress-enhancing mindset may experience better sleep quality. Thus, stress mindset may be associated with better sleep quality by influencing sleep-related beliefs and modulating responses to stress.
Consistent with Hypothesis 2, stress overload was found to mediate the relationship between nurses’ stress mindset and sleep quality. In other words, a nurse’s stress mindset may be associated with their levels of stress overload, which in turn may be related to their sleep quality. This finding expands on existing research by suggesting a potential connection among stress mindset, stress overload and sleep quality. As healthcare demands increase and the population ages, hospitals place greater demands on nurses, leading to heightened work-related stress and challenges. According to the Job Demands-Resources Model, when job demands surpass available resources, employees are more likely to experience stress and burnout [63]. In nursing, factors such as high workload, shift work, emotional labor, and staff shortages, combined with subjective stress perceptions like patient expectations and high-risk duties, collectively contribute to significant stress overload [64]. Previous research has shown that stress overload among nurses is closely linked to poor sleep quality, anxiety, and depression [65]. Social cognitive theory also suggests that behavior is influenced by the interaction of external environmental and internal personal factors [66]. In nursing, internal factors such as coping strategies, self-efficacy, and stress mindset may influence how nurses perceive and respond to work-related stress, thereby affecting their mental health and job performance [67]. This study utilized the Stress Overload Scale to assess nurses’ stress levels, considering both objective environmental factors and subjective psychological stress. Nurses with a stress-enhancing mindset are more likely to adopt active coping strategies when facing stress [17], which is associated with lower perceived stress levels. Lower perceived stress may, in turn, be associated with better sleep quality among nurses [68]. From a physiological perspective, stress triggers the release of cortisol, and dysregulated cortisol levels are closely associated with sleep disorders [69]. Research suggests that stress mindset may influence physiological responses, including the regulation of cortisol levels. Individuals with a stress-is-enhancing mindset exhibited more adaptive cortisol responses when facing stress [17]. This indicates that a stress-enhancing mindset may help regulate physiological arousal states, promoting appropriate cortisol levels. This may be related to enhanced nurse performance and reduced negative health impacts, potentially improving their sleep quality.
The study also found that anxiety mediates the relationship between nurses’ stress mindset and sleep quality, supporting Hypothesis 3. More specifically, nurses with a positive cognitive appraisal of stress tend to report lower levels of anxiety, which is associated with better sleep quality. Those with a stress-enhancing mindset are more likely to view stress as beneficial, believing it can enhance their performance, work efficiency, and overall health. This outlook is related to reduced anxiety and improved sleep quality [70]. In contrast, nurses with a stress-debilitating mindset are more inclined to avoid anxiety-inducing situations, which may limit their ability to manage anxiety effectively, and is associated with heightened baseline anxiety levels and increased sensitivity to anxiety. Nurses who adopt a stress-enhancing mindset are generally more prepared to face challenges and gain experience in managing stress-related anxiety. Viewing stress as part of life may reduce its perceived threat [71], potentially promoting better stress management, lowering anxiety [72], and is associated with better sleep quality.
The study also found that stress overload and anxiety jointly mediate the relationship between nurses’ stress mindset and sleep quality, supporting Hypothesis 4. Specifically, stress mindset is associated with nurses’ stress levels, which in turn are related to their anxiety and sleep quality. While prior studies have primarily examined the relationships between stress, anxiety, and sleep quality independently, this research integrates these variables into a single model, revealing their interconnectedness. By focusing on nurses—a high-stress occupational group—this study examines the model within this population, providing new insights into their mental health and sleep issues. The self-fulfilling prophecy effect [73], suggests that individuals’ expectations influence their behavior, eventually leading those expectations to materialize. Nurses with a stress-enhancing mindset are more likely to believe in their ability to overcome challenges, adopt proactive coping strategies, and have higher self-efficacy and performance, which are associated with lower stress levels. Additionally, the Pygmalion effect [74] indicates that others’ positive expectations can enhance an individual’s confidence and performance. Nurses with a stress-enhancing mindset not only believe in their abilities but also report better performance, which is associated with lower perceived stress. Higher stress levels are closely related to mental health, often correlating with heightened anxiety [75]; higher stress overload in nurses may increase their likelihood of experiencing anxiety. Anxiety, in turn, is associated with poorer sleep quality and may be related to sleep disorders and structural alterations in sleep [76, 77]. Nurses with a stress-enhancing mindset tend to experience lower stress overload, which is associated with reduced anxiety and improved sleep quality, supporting the potential for a chain mediation effect. Compared to previous studies, this research highlights the chain mediation roles of stress overload and anxiety between nurses’ stress mindset and sleep quality, offering a deeper understanding of the mechanisms through which stress mindset affects sleep quality. These findings provide valuable insights into strategies to reduce nurses’ stress overload and anxiety and improve sleep quality, revealing the potential direct and indirect effects of stress mindsets on nurses’ sleep quality.
Limitations and future directions
While this study offers valuable and innovative insights, several limitations should be acknowledged. First, although nurses from various departments and with different shift schedules were included, the study did not fully account for their distinct differences. For example, nurses in intensive care units or obstetrics might experience more severe sleep disturbances due to frequent night shifts, which could disrupt their circadian rhythms. Future research should consider categorizing nurses by department and shift schedules to better assess how different work environments affect sleep quality and to inform more targeted interventions. Second, the cross-sectional design of this study only captures associations between nurses’ stress mindset and sleep quality at one point in time, preventing the determination of causal relationships. To address this, future studies should employ longitudinal or cross-lagged designs to explore the long-term effects of stress mindset on sleep quality and uncover the underlying mechanisms, offering more robust causal insights. Third, the study utilized convenience sampling from a limited geographic area, which may limit the generalizability of the findings. Future research should aim to expand the geographic scope, increase the sample size, and use random sampling methods to enhance the generalizability of the results. Finally, although this research focused on nurses, high stress levels and poor sleep quality are prevalent across various healthcare professions. Future studies could extend the investigation to other healthcare workers to examine whether similar mediating effects occur, thereby providing broader evidence for stress management and sleep improvement strategies in the healthcare sector.
Conclusion
This study employed a chain mediation model to investigate the relationship between nurses’ stress mindset and sleep quality, with stress overload and anxiety serving as mediating variables. The results indicate that a stress-is-enhancing mindset is associated with reduced stress overload and anxiety, which are, in turn, linked to better sleep quality. These findings underscore the significant influence that stress mindset has on nurses’ stress overload, anxiety, and sleep quality. In nursing practice, interventions aimed at fostering a stress-enhancing mindset may help alleviate stress overload and anxiety, thereby potentially improving nurses’ sleep quality.
Acknowledgements
The researchers would like to thank the nurses from the following hospitals who participated in the survey: The First Affiliated Hospital of Chongqing Medical University, The Second Affiliated Hospital of Chongqing Medical University, The Children’s Hospital of Chongqing Medical University, The University-Town Hospital of Chongqing Medical University, The Dazu Hospital of Chongqing Medical University, The Yongchuan Hospital of Chongqing Medical University, The First Affiliated Hospital of Army Medical University, The Second Affiliated Hospital of Army Medical University, Chongqing Jiulongpo Traditional Chinese Medicine Hospital, Chongqing West District Hospital, Rencheng District Maternal and Child Health Hospital of Jining, Shandong, The Nanhua Hospital Affiliated to University of South China. Thank you for your support and contributions.
Abbreviations
- GAD
Generalized Anxiety Disorder
- PSQI
Pittsburgh Sleep Quality Index
- SMM
Stress Mindset Measure
- SOS-S
Stress Overload Scale-Short
Author contributions
YW conceptualized the research idea, conducted a literature review, data collection, data extraction, and data analysis, obtained informed consent from participants, and wrote the manuscript. TY contributed to the study’s conception and design. JL was responsible for data analysis and methodology. ZS, JG, XP, and QL reviewed and edited the manuscript. All authors read and approved the final manuscript.
Funding
This project was jointly supported by the Humanities and Social Sciences Research Programme of Chongqing Municipal Education Commission, China (22SKDJ043), Chongqing Social Science Planning Project, China (2023PY13), Fundamental Research Funds for the Central Universities (SWU2009106).
Data availability
No datasets were generated or analysed during the current study.
Declarations
Ethical approval
The present study was approved by Institutional Review Board of Faculty of Psychology, Southwest University (No. H24118). The authors of this article, while observing the rules and provisions of ethical regulations, including the Helsinki Declaration and obtaining informed consent from the participants and full assurance of the confidentiality of the collected information and complete freedom to participate in the study as well as leaving the study, conducted the present study.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Footnotes
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.National Health Commission of the People’s Republic of China. Statistical bulletin on the development of health care in China; 2022.
- 2.Zhou Y, Wang Y, Huang M, et al. Psychological stress and psychological support of Chinese nurses during severe public health events. BMC Psychiatry. 2022;22(1):800. 10.1186/s12888-022-04451-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Liao Y, Wei W, Fang S, et al. Work immersion and perceived stress among clinical nurses: a latent profile analysis and moderated mediation analysis. BMC Nurs. 2023;22(1):346. 10.1186/s12912-023-01467-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Imes CC, Barthel NJ, Chasens ER, et al. Shift work organization on nurse injuries: a scoping review. Int J Nurs Stud. 2023;138:104395. 10.1016/j.ijnurstu.2022.104395. [DOI] [PubMed] [Google Scholar]
- 5.Kecklund G, Axelsson J. Health consequences of shift work and insufficient sleep. BMJ. 2016;355:i5210. 10.1136/bmj.i5210. [DOI] [PubMed] [Google Scholar]
- 6.Zhang Y, Murphy J, Lammers-van Der Holst HM, Barger LK, Lai Y, Duffy JF. Interventions to improve the sleep of nurses: a systematic review. Res Nurs Health. 2023;46:462–84. 10.1002/nur.22337. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Hale L, Troxel W, Buysse DJ. Sleep Health: An Opportunity for Public Health To Address Health Equity. Annu Rev Public Health. 2020;41:81–99. 10.1146/annurev-publhealth-040119-094412. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Lazarus RS. Psychological stress and the coping process. Am J Psychol. 1966;83(4).
- 9.Cohen S, Kessler RC, Gordon LU. Measuring stress: a guide for health and social scientists. Oxford University Press; 1995.
- 10.Amirkhan JH. Stress overload: a new approach to the assessment of stress. Am J Community Psychol. 2012;49(1–2):55–71. 10.1007/s10464-011-9438-x. [DOI] [PubMed] [Google Scholar]
- 11.Amirkhan JH. Stress overload in the spread of coronavirus. Anxiety Stress Coping. 2021;34(2):121–9. 10.1080/10615806.2020.1824271. [DOI] [PubMed] [Google Scholar]
- 12.Geiger-Brown J, Rogers VE, Trinkoff AM, Kane RL, Bausell RB, Scharf SM. Sleep, sleepiness, fatigue, and performance of 12-hour-shift nurses. Chronobiol Int. 2012;29(2):211–9. 10.3109/07420528.2011.645752. [DOI] [PubMed] [Google Scholar]
- 13.Lockley SW, Cronin JW, Evans EE, et al. Effect of reducing interns’ weekly work hours on sleep and attentional failures. N Engl J Med. 2004;351(18):1829–37. 10.1056/NEJMoa041404. [DOI] [PubMed] [Google Scholar]
- 14.Meerlo P, Sgoifo A, Suchecki D. Restricted and disrupted sleep: effects on autonomic function, neuroendocrine stress systems, and stress responsivity. Sleep Med Rev. 2008;12(3):197–210. 10.1016/j.smrv.2007.07.007. [DOI] [PubMed] [Google Scholar]
- 15.Puttonen S, Härmä M, Hublin C. Shift work and cardiovascular disease—pathways from circadian stress to morbidity. Scand J Work Environ Health. 2010;36(2):96–108. 10.5271/sjweh.2894. [DOI] [PubMed] [Google Scholar]
- 16.Åkerstedt T. Psychosocial stress and impaired sleep. Scand J Work Environ Health. 2006;32(6):493–501. 10.5271/sjweh.1054. [PubMed] [Google Scholar]
- 17.Crum AJ, Salovey P, Achor S. Rethinking stress: the role of mindsets in determining the stress response. J Pers Soc Psychol. 2013;104(4):716–33. 10.1037/a0031201. [DOI] [PubMed] [Google Scholar]
- 18.Chen WB, Zhang N. Stress mindset predicts depression symptoms in college students during the COVID-19 pandemic lockdown: the mediating role of positive and negative emotions. Chin J Health Psychol. 2023;31(08):1239–43. [Google Scholar]
- 19.Park D, Yu A, Metz SE, Tsukayama E, Crum AJ, Duckworth AL. Beliefs about stress attenuate the relation among adverse life events, perceived distress, and self-control. Child Dev. 2018;89(6):2059–69. 10.1111/cdev.12946. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Jamieson JP, Mendes WB, Blackstock E, Schmader T. Turning the knots in your stomach into bows: reappraising arousal improves performance on the GRE. J Exp Soc Psychol. 2010;46(1):208–12. 10.1016/j.jesp.2009.08.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Keech JJ, Hagger MS, O’Callaghan FV, Hamilton K. The influence of university students’ stress mindsets on health and performance outcomes. Ann Behav Med. 2018;52(12):1046–59. 10.1093/abm/kay008. [DOI] [PubMed] [Google Scholar]
- 22.Zhang Y, Zhang C, Han XR, Li W, Wang YL. Determinants of compassion satisfaction, compassion fatigue and burnout in nursing: a correlative meta-analysis. Med (Baltim). 2018;97(26). 10.1097/MD.0000000000011086. [DOI] [PMC free article] [PubMed]
- 23.Connor-Smith JK, Flachsbart C. Relations between personality and coping: a meta-analysis. J Pers Soc Psychol. 2007;93(6):1080–107. 10.1037/0022-3514.93.6.1080. [DOI] [PubMed] [Google Scholar]
- 24.Cox RC, Olatunji BO. A systematic review of sleep disturbance in anxiety and related disorders. J Anxiety Disord. 2016;37:104–29. 10.1016/j.janxdis.2015.12.001. [DOI] [PubMed] [Google Scholar]
- 25.Grandner MA, Patel NP, Gehrman PR, Perlis ML, Pack AI. Problems associated with short sleep: bridging the gap between laboratory and epidemiological studies. Sleep Med Rev. 2010;14(4):239–47. 10.1016/j.smrv.2009.08.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Li L, Ruan H, Yuan W, Wang Z. Associations of occupational stress, sleep duration and sleep quality with cardiovascular diseases among coal miners in Xinjiang, China: a cross-sectional study. BMJ Open. 2020;10(8). 10.1136/bmjopen-2019-036087. [DOI] [PMC free article] [PubMed]
- 27.García-Iglesias JJ, Rodríguez-Muñoz A, Agudo-Tabuenca A, et al. Relationship between job demand and burnout in nurses: does it depend on work engagement? J Nurs Manag. 2020;28(4):852–9. 10.1111/jonm.13011. [Google Scholar]
- 28.Ramin C, Devore EE, Wang W, et al. Night shift work at specific age ranges and chronic disease risk factors. Occup Environ Med. 2015;72(2):100–7. 10.1136/oemed-2014-102292. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Flo E, Pallesen S, Magerøy N, et al. Shift work disorder in nurses—assessment, prevalence and related health problems. PLoS ONE. 2012;7(4). 10.1371/journal.pone.0033981. [DOI] [PMC free article] [PubMed]
- 30.Wolf EJ, Harrington KM, Clark SL, Miller MW. Sample size requirements for structural equation models: an evaluation of Power, Bias, and Solution Propriety. Educ Psychol Meas. 2013;73:913–34. 10.1177/0013164413495237. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Zhang N, Bai B, Zhu J. Stress mindset, proactive coping behavior, and posttraumatic growth among health care professionals during the COVID-19 pandemic. Psychol Trauma. 2023;15(3):515–23. 10.1037/tra0001377. [DOI] [PubMed] [Google Scholar]
- 32.Buysse DJ, Reynolds CF 3rd, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989;28(2):193–213. 10.1016/0165-1781(89)90047-4. [DOI] [PubMed] [Google Scholar]
- 33.Tsai PS, Wang SY, Wang MY, et al. Psychometric evaluation of the Chinese version of the Pittsburgh Sleep Quality Index (CPSQI) in primary insomnia and control subjects. Qual Life Res. 2005;14(8):1943–52. 10.1007/s11136-005-4346-x. [DOI] [PubMed] [Google Scholar]
- 34.Liu XC, Tang MQ, Hu L, Wang AZ, Wu HX, Zhao GF, et al. Reliability and validity of Pittsburgh sleep quality index. Chin J Psychiatry. 1996;29(02):103–7. [Google Scholar]
- 35.Spitzer RL, Kroenke K, Williams JB, Löwe B. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166(10):1092–7. 10.1001/archinte.166.10.1092. [DOI] [PubMed] [Google Scholar]
- 36.He Xiaoyan L, Chunbo Q. Jie Reliability and validity of generalized anxiety scale in general hospital [J]. Shanghai Psychiatry. 2010;22(04):200–3.
- 37.Amirkhan JH. A brief stress Diagnostic Tool: the short stress overload scale. Assessment. 2018;25(8):1001–13. 10.1177/1073191116673173. [DOI] [PubMed] [Google Scholar]
- 38.Duan W, Mu W. Validation of a Chinese version of the stress overload scale-short and its use as a screening tool for mental health status. Qual Life Res. 2018;27(2):411–21. 10.1007/s11136-017-1721-3. [DOI] [PubMed] [Google Scholar]
- 39.Wang L, Qin P, Zhao Y, et al. Prevalence and risk factors of poor sleep quality among Inner Mongolia Medical University students: a cross-sectional survey. Psychiatry Res. 2016;244:243–8. 10.1016/j.psychres.2016.04.011. [DOI] [PubMed] [Google Scholar]
- 40.Li RH, Wing YK, Ho SC, Fong SY. Gender differences in insomnia - a study in the Hong Kong Chinese population. J Psychosom Res. 2002;53(1):601-609. 10.1016/s0022-3999(02)00437-3. [DOI] [PubMed]
- 41.Cho HS, Kim YW, Park HW, et al. The relationship between depressive symptoms among female workers and job stress and sleep quality. Ann Occup Environ Med. 2013;25(1):12. 10.1186/2052-4374-25-12. Published 2013 Jul 22. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Dong H, Zhang Q, Sun Z, Sang F, Xu Y. Sleep disturbances among Chinese clinical nurses in general hospitals and its influencing factors. BMC Psychiatry. 2017;17(1):241. 10.1186/s12888-017-1402-3. Published 2017 Jul 3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Lu L, Lok KI, Zhang Q, et al. Sleep disturbance and its association with quality of life among psychiatric nurses in China. PeerJ. 2021;9:e10659. 10.7717/peerj.10659. Published 2021 Feb 17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Chen J, Li H, Qiu X, et al. Job stress and performance among nursing staff in a hospital: the mediating effect of emotional intelligence. Int J Nurs Sci. 2019;6(2):150–5. 10.1016/j.ijnss.2018.12.001. [Google Scholar]
- 45.Booker LA, Magee M, Rajaratnam SMW, Sletten TL. Individual vulnerability to insomnia, excessive sleepiness and shift work disorder amongst healthcare shift workers. A systematic review. Sleep Med Rev. 2018;41:220–33. 10.1016/j.smrv.2018.03.005. [DOI] [PubMed] [Google Scholar]
- 46.Rosa D, Terzoni S, Dellafiore F, Destrebecq A. Systematic review of shift work and nurses’ health. Occup Med (Lond). 2019;69(4):237–43. 10.1093/occmed/kqz063. [DOI] [PubMed] [Google Scholar]
- 47.Espie CA, Broomfield NM, MacMahon K, Macphee LM, Taylor LM. The attention-intention-effort pathway in the development of psychophysiologic insomnia: a theoretical review. Sleep Med Rev. 2006;10(4):215–45. 10.1016/j.smrv.2006.03.002. [DOI] [PubMed] [Google Scholar]
- 48.Baglioni C, Spiegelhalder K, Lombardo C, Riemann D. Sleep and emotions: a focus on insomnia. Sleep Med Rev. 2010;14(4):227–38. 10.1016/j.smrv.2009.10.007. [DOI] [PubMed] [Google Scholar]
- 49.Chen X, Liu P, Lei GF, Tong L, Wang H, Zhang XQ. Sleep quality and the depression-anxiety-stress state of Frontline nurses who perform nucleic acid Sample Collection during COVID-19: a cross-sectional study. Psychol Res Behav Manag. 2021;14:1889–900. 10.2147/PRBM.S338495. Published 2021 Nov 26. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Brenes GA, Miller ME, Stanley MA, Williamson JD, Knudson M, McCall WV. Insomnia in older adults with generalized anxiety disorder. Am J Geriatr Psychiatry. 2009;17(6):465–72. 10.1097/jgp.0b013e3181987747. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Deng X, Liu X, Fang R. Evaluation of the correlation between job stress and sleep quality in community nurses. Med (Baltim). 2020;99(4):e18822. 10.1097/MD.0000000000018822. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.D’emeh WM, Yacoub MI, Shahwan BS. Work-related stress and anxiety among Frontline nurses during the COVID-19 pandemic: a cross-sectional study. J Psychosoc Nurs Ment Health Serv. 2021;59(8):31–42. 10.3928/02793695-20210322-02. [DOI] [PubMed] [Google Scholar]
- 53.Palmer CA, Bower JL, Cho KW et al. Sleep loss and emotion: a systematic review and meta-analysis of over 50 years of experimental research. Psychol Bull. 10.1037/bul0000410 [DOI] [PubMed]
- 54.Smith EN, Young MD, Crum AJ. Stress, mindsets, and Success in Navy SEALs Special Warfare Training. Front Psychol. 2020;10:2962. 10.3389/fpsyg.2019.02962. Published 2020 Jan 15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Goyer JP, Akinola M, Grunberg R, Crum AJ. Thriving under pressure: the effects of stress-related wise interventions on affect, sleep, and exam performance for college students from disadvantaged backgrounds. Emotion. 2022;22(8):1755–72. 10.1037/emo0001026. [DOI] [PubMed] [Google Scholar]
- 56.Shen Y, Jian W, Zhu Q, Li W, Shang W, Yao L. Nurse staffing in large general hospitals in China: an observational study. Hum Resour Health. 2020;18(1):3. 10.1186/s12960-020-0446-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Murali KP, Brody AA, Stimpfel AW, Nurses. Psychological distress, and Burnout: is there an app for that? Ann Am Thorac Soc. 2023;20(10):1404–5. 10.1513/AnnalsATS.202307-629ED. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Linton SJ, Kecklund G, Franklin KA, et al. The effect of the work environment on future sleep disturbances: a systematic review. Sleep Med Rev. 2015;23:10–9. 10.1016/j.smrv.2014.10.010. [DOI] [PubMed] [Google Scholar]
- 59.Garcia CL, Abreu LC, Ramos JLS, et al. Influence of Burnout on Patient Safety: systematic review and Meta-analysis. Med (Kaunas). 2019;55(9):553. 10.3390/medicina55090553. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Jansson M, Linton SJ. Psychological mechanisms in the maintenance of insomnia: arousal, distress, and sleep-related beliefs. Behav Res Ther. 2007;45(3):511–21. 10.1016/j.brat.2006.04.003. [DOI] [PubMed] [Google Scholar]
- 61.Crum AJ, Jamieson JP, Akinola M. Optimizing stress: an integrated intervention for regulating stress responses. Emotion. 2020;20(1):120–5. 10.1037/emo0000670 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Jamieson JP, Mendes WB, Nock MK. Improving acute stress responses: the power of reappraisal. Curr Dir Psychol Sci. 2013;22(1):51–6. 10.1177/0963721412461500. [Google Scholar]
- 63.Demerouti E, Bakker AB, Nachreiner F, Schaufeli WB. The job demands-resources model of burnout. J Appl Psychol. 2001;86(3):499–512. [PubMed] [Google Scholar]
- 64.Heinen MM, van Achterberg T, Schwendimann R, et al. Nurses’ intention to leave their profession: a cross sectional observational study in 10 European countries. Int J Nurs Stud. 2013;50(2):174–84. 10.1016/j.ijnurstu.2012.09.019. [DOI] [PubMed] [Google Scholar]
- 65.Zhang Y, Punnett L, Nannini A. Work-family conflict, sleep, and mental health of nursing assistants working in nursing homes. Workplace Health Saf. 2017;65(7):295–303. 10.1177/2165079916671121. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Bandura A. Self-efficacy: toward a unifying theory of behavioral change. Psychol Rev. 1977;84(2):191–215. 10.1037/0033-295X.84.2.191. [DOI] [PubMed] [Google Scholar]
- 67.Schwarzer R, Hallum S. Perceived teacher self-efficacy as a predictor of job stress and burnout: mediation analyses. Appl Psychol. 2008;57:152–71. 10.1111/j.1464-0597.2008.00359.x. [Google Scholar]
- 68.Slavish DC, Dietch JR, Kane HS, et al. Daily stress and sleep associations vary by work schedule: a between- and within-person analysis in nurses. J Sleep Res. 2022;31(3):e13506. 10.1111/jsr.13506. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Schmidt ME, Semik J, Habermann N, Wiskemann J, Ulrich CM, Steindorf K. Cancer-related fatigue shows a stable association with diurnal cortisol dysregulation in breast cancer patients. Brain Behav Immun. 2016;52:98–105. 10.1016/j.bbi.2015.10.005. [DOI] [PubMed] [Google Scholar]
- 70.Crum AJ, Akinola M, Martin A, Fath S. The role of stress mindset in shaping cognitive, emotional, and physiological responses to challenging and threatening stress. Anxiety Stress Coping. 2017;30(4):379–95. 10.1080/10615806.2016.1275585. [DOI] [PubMed] [Google Scholar]
- 71.Crum A, Lyddy C. De-stressing stress: the power of mindsets and the art of stressing mindfully. Wiley Blackwell Handb Mindfulness. 2014;948–63. 10.1002/9781118294895.ch49.
- 72.Alker L, Radstaak M. Distress tolerance as a mediator of the relation between stress mindset and anxiety. ASEAN J Psychiatry. 2024;25(2):1–12. [Google Scholar]
- 73.Merton RK. The self-fulfilling prophecy. Antioch Rev. 1948;8(2):193–210. 10.2307/4609267. [Google Scholar]
- 74.Babad EY, Inbar J, Rosenthal R, Pygmalion. Galatea, and the Golem: investigations of biased and unbiased teachers. J Educ Psychol. 1982;74(4):459–74. 10.1037/0022-0663.74.4.459. [Google Scholar]
- 75.Fawzy M, Hamed SA. Prevalence of psychological stress, depression and anxiety among medical students in Egypt. Psychiatry Res. 2017;255:186–94. 10.1016/j.psychres.2017.05.027. [DOI] [PubMed] [Google Scholar]
- 76.Johnson EO, Roth T, Breslau N. The association of insomnia with anxiety disorders and depression: exploration of the direction of risk. J Psychiatr Res. 2006;40(8):700–8. 10.1016/j.jpsychires.2006.07.008. [DOI] [PubMed] [Google Scholar]
- 77.Horváth A, Montana X, Lanquart JP, et al. Effects of state and trait anxiety on sleep structure: a polysomnographic study in 1083 subjects. Psychiatry Res. 2016;244:279–83. 10.1016/j.psychres.2016.03.001. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
No datasets were generated or analysed during the current study.