Abstract
Background
Preterm birth (PTB) is the most stubborn cause of neonatal morbidity and mortality globally. Social determinants are one of the predictors of health disparities and conflicting when regarding the etiology of PTB. The current study objected to investigate the impact of the factors especially from socioeconomic aspects and provided a snapshot of the indicators of PTB in Kazakhstan.
Material and methods
A multi-center hospital-based cohort study was conducted on 3,000 singleton pregnant women in Kazakhstan to investigate whether socioeconomic status (SES) influences PTB in Kazakhstan. The study involved clinical data collection and structured questionnaires covering socioeconomic status, health behaviors, and obstetric history, with a final sample of 2,235 women successfully followed through to delivery. The social, demographic, and other health-related determinants for preterm birth were analyzed using bivariate and multivariate statistical methods. The associations between factors and PTB were evaluated by chi-squared tests in bivariate analysis. Independent variables with p < 0.1 in the bivariate analysis were included in a logistic regression model.
Result
History of PTB in previous pregnancies, maternal body mass index, housing stability, history of teen pregnancy, parity and general health status of mother were associated with PTB in bivariate analysis. In the logistic regression model, variabls significantly associated with PTB included a history of previous preterm birth, history of teen pregnancy, lower pre-gestational body mass index, primiparity and poorer maternal general health status. Additionally, the significance of the variables varied among the different subtypes of PTB heterogeneity. Women who were divorced, widowed and separated (OR = 5.1; 95% CI: 1.9–13.7) and those who pregnant for first time (OR = 3.8; 95% CI: 1.9–7.7), those with gestational diabetes (OR = 5.2; 95% CI: 1.7–16.3) had increased risk of extremely and very preterm birth, respectively. Women with a low body mass index (OR = 2.3; 95% CI: 1.3–3.9) and those with a history of teen pregnancy (OR = 0.4; 95% CI: 0.2–0.7) had increased risk of moderate to late preterm.
Conclusion
These results contribute to a better understanding of PTB predictors in Kazakhstan and highlight the need for comprehensive maternal care strategies to improve pregnancy outcomes.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12884-024-06984-0.
Keywords: Preterm birth, Socioeconomic status, Risk factors
Introduction
Preterm birth (PTB), accompanied by significant long-term health implications, is the most common adverse pregnancy outcome and remains one of the most stubborn research problems in obstetrics and gynecology in the world [1]. The estimated global prevalence of PTB in 2020 was approximately 9.9%. In Central Asia, the rate was slightly lower, at about 7.9% [2]. Despite advancements in medical care, the rates of PTB have not significantly declined, which contributes to ongoing high levels of neonatal mortality and morbidity in most of the countries [1, 2].
Socioeconomic inequalities are one of the predictors of health disparities, largely due to factors such as inadequate nutrition, unstable housing, financial stress, and limited access to healthcare [3–5]. Studies reported PTB has been linked to socioeconomic factors, even the presence of a universal healthcare system, indicating that these associations may not be solely due to the type of prenatal care provided [6, 7]. Lower social class, limited education, unstable marital status, poverty, unemployment, poor living conditions, maternal mental health issues, and minimal contact with neighbors have all been linked to pregnancy complications resulting in PTB among other populations [6–8].
Kazakhstan, one of the Central Asian countries, reports approximately 400 000 infant deliveries annually, with a preterm birth rate of 5% [9]. According to WHO statistics, Kazakhstan has a relatively low rate of PTB, placing it among the least affected nations in the world [2]. However, the Infant mortality rate in Kazakhstan was 8.7 deaths per 1000 live births in 2022, with prematurity contributing to around 1% of these cases [10, 11]. Since PTBs account for a significant proportion of infant deaths in Kazakhstan [10], identifying their determinants or associated factors is essential for reducing infant mortality. Moreover, significant regional disparities in infant mortality rates persist despite an overall decrease in the national average, according to the Statistics Committee of the Ministry of National Economy of Kazakhstan [10]. Additionally, there is limited research on how SES affects birth outcomes in Kazakhstan [12]. Therefore, it is difficult to determine how much the results of similar studies can be applied to Kazakhstan due to differences in the country's socioeconomic and healthcare structures. In Kazakhstan, the public health system provides antenatal service and obstetric care to all pregnant women with national welfare, regardless of socioeconomic status or location. This approach has led to high antenatal care coverage, achieving 99.2% [13]. A comprehensive evaluation of the determinants influencing the current population is crucial for implementing effective preventive strategies, especially regarding PTB. The current study objected to investigate the impact of the factors especially from socioeconomic aspects and provided a snapshot of the indicators of PTB in Kazakhstan.
Material and methods
This multi-center hospital-based cohort study was conducted among a sample of 3000 Kazakh singleton pregnant women who consented to the study. The minimal required sample size was calculated. The data were collected from three large Reproductive and Perinatal Center in Atyrau, Aktobe and in Kyzylorda regions in Southern and Western Kazakhstan. More than 99% of pregnant women in Kazakhstan registered in local health centers [13]. The health facilities provide free maternal and child care for pregnant women. We collect the study participants from September 2022 to April 2024. During this period, 2235 women were followed up successfully, giving a 75% response rate for the research. Our research team explained the aims and process of the research to the participants using the informing sheet, the benefits of participation, the confidentiality of personal information and the voluntary nature of participation were informed. Those who signed consent answered a questionnaire. Before applying the questionnaire to the study sample, a trained researcher fluent in Kazakh and Russian conducted a pilot survey among 30 pregnant visitors at the Aktobe Reproductive and Perinatal Center to improve clarity.
A structured questionnaire and medical report of the pregnant women were used to explore the potential factors related to preterm birth regardless of whether spontaneous or induced, including the mother’s socio-demographic, anthropometric characteristics, obstetric and medical history during and before pregnancy. Gestational weeks at labor and type of delivery were obtained after delivery ( attached in supplementary file). Data on socio economic status such as household size and income, main working member of the family, workload, social welfare status, educational level, marital and employment status, main speaking language, accommodation, medical insurance, self evaluation of general health status and the father of the child.
The project supervisor obtained permissions from the hospital authorities to use medical records of involved patients. The author who analyzed the data did not have access to personal data.
Births that occurred prior to the 37th week of gestation were classified as PTB. Subgroups of preterm birth classified according to gestational age, as extremely preterm (EPTB) with less than 28 weeks gestation, very preterm (VPTB) with 28 to less than 32 weeks gestation, moderate to late preterm (MLPTB) with 32 to less than 37 weeks gestation, recognizing that the timing of a preterm birth significantly affects both risks and outcomes for the infant.
All the data were inserted into SPSS software and analysis was conducted, including the frequency of distribution. Chi-square test were used to establish associations between categorical variables and PTB and its subtypes. Independent associations between PTB and potential predictors were studied using a multinomial logistic regression model. Crude and adjusted odds ratios (OR) were calculated with 95% confidence intervals (CI). Multivariable analysis was performed only on variables associated with the outcome in crude analysis at the level of significance below 0.1. The analyses were repeated separately for the subgroups of PTB.
Result
Among the 2235 pregnant women in the study, 280 (12.5%) cases of singleton preterm birth (PTB) were reported. Of these PTB cases, 39(14%) were classified as EPTB, 41(15%) as VPTB, and 200 (71%) as MLPTB, representing 1.7%,1.8% and 8.9% of total sample, respectively. The mean age of the sample was 29.5 (SD = 5.9) years with no difference between term and preterm mothers (p = 0.66). Regarding the overall sample characteristics, 98% from ethnic Kazakh, 88% had a higher education(more than 12 years), and 63% had occupations. None reported smoking and consuming alcohol during pregnancy.
In bivariate analysis, the following variables include history of PTB, history of teen pregnancy, gravida, pre pregnancy BMI, housing condition and self reported general health status of mother were significantly associated with PTB. Apart from history of PTB and self reported general health, variables associated with EPTB include marital status. Gestational diabetes, parity and place of healthcare were associated with VPTB, while pre gestational BMI and history of teen pregnancy were associated with MLPTB (Table 1).
Table 1.
Distribution of demographics, maternal socioeconomic and health status and obstetric history between Term and Preterm groups
| Variables | Term (n = 1955) | preterm (n = 280) |
P | EPTB (n = 39) |
P | VPTB (n = 41) |
P | MLPTB (n = 200) |
P |
|---|---|---|---|---|---|---|---|---|---|
| Age, years | |||||||||
| < 20 | 91 (4.7) | 17 (6.1) | 0.2 | 3 (7.7) | 0.3 | 2 (4.9) | 0.5 | 12 (6.0) | 0.7 |
| 20–24 | 475 (24.3) | 73 (26.1) | 8 (20.5) | 13 (31.7) | 52 (26.0) | ||||
| 25–29 | 593 (30.3) | 71 (25.4) | 7 (17.9) | 8 (19.5) | 56 (28.0) | ||||
| 30–34 | 454 (23.2) | 59 (21.1) | 11 (28.2) | 8 (19.5) | 40 (20.0) | ||||
| > 35 | 342 (17.5) | 60(21.4) | 10 (25.6) | 10 (24.4) | 40 (20.0) | ||||
| Pre-pregnancy weight | |||||||||
| Obese/overweight | 898 (45.9) | 123 (43.9) | 0.002 | 16 (41) | 0.8 | 14 (34.1) | 0.1 | 93 (46.5) | 0.002 |
| Normal weight | 952 (48.7) | 127 (45.4) | 21 (53.8) | 22 (53.7) | 84 (42.0) | ||||
| Underweight | 105 (5.4) | 30 (10.7) | 2 (5.1) | 5 (12.2) | 23 (11.5) | ||||
| Gravida | |||||||||
| Primigravida | 312 (16) | 59 (21) | 0.03 | 4 (10.3) | 0.28 | 26 (63.4) | 0.001 | 40 (20.0) | 0.18 |
| Multigravida | 1643(84) | 221(79) | 35 (89.7) | 15 (36.6) | 160 (80.0) | ||||
| Age at First Childbirth | |||||||||
| < 20 | 310 (15.9) | 51 (18.2) | < 0.001 | 10 (25.6) | 0.20 | 2 (4.9) | 0.02 | 39 (19.5) | < 0.001 |
| 20–25 | 1270 (65.0) | 151 (53.9) | 23 (59.0) | 26 (63.4) | 102 (51.0) | ||||
| 26–30 | 279 (14.3) | 48 (17.1) | 6 (15.4) | 7 (17.1) | 35 (17.5) | ||||
| > 30 | 96 (4.9) | 30 (10.7) | 0 | 6 (14.6) | 24 (12.0) | ||||
| Maternal and obstetrical complications | |||||||||
| Miscarage | |||||||||
| Yes | 379 (19.4) | 61 (21.8) | 0.35 | 10 (25.6) | 0.35 | 5 (12.2) | 0.22 | 46 (23.0) | 0.22 |
| No | 1576 (80.6) | 219 (78.2) | 29 (74.4) | 36 (87.8) | 1564 (77.0) | ||||
| Abortion | |||||||||
| Yes | 184 (9.4) | 27 (9.6) | 0.90 | 5 (12.8) | 0.48 | 3 (7.3) | 0.64 | 19 (9.5) | 0.98 |
| No | 1771 (90.6) | 253 (90.4) | 34 (87.2) | 38 (92.7) | 181 (90.5) | ||||
| Gestational diabet | |||||||||
| Yes | 48 (2.5) | 11 (3.9) | 0.15 | 0 | 0.30 | 4 (9.8) | 0.004 | 7 (3.5) | 0.43 |
| No | 1907 (97.5) | 269 (96.1) | 39 (100) | 37 (90.2) | 193 (96.5) | ||||
| Preeclampsia | |||||||||
| Yes | 162 (8.3) | 18 (6.4) | 0.29 | 1 (2.6) | 0.20 | 1 (2.4) | 0.18 | 16 (8.0) | 0.98 |
| No | 1793 (91.7) | 262 (93.6) | 38 (97.4) | 40 (97.6) | 184 (92.0) | ||||
| History of preterm | |||||||||
| Yes | 263 (13.5) | 127 (45.4) | < 0.001 | 17 (43.6) | < 0.001 | 15 (36.6) | 0.001 | 95 (47.5) | < 0.001 |
| No | 1692 (86.5) | 153 (54.6) | 22 (56.4) | 26 (63.4) | 105 (52.5) | ||||
| Self reported general health status of mother | |||||||||
| Poor | 85 (4.3) | 29 (10.4) | < 0.001 | 7 (17.9) | 0.001 | 4 (9.8) | 0.01 | 18 (9.0) | 0.01 |
| Fair | 376 (19.3) | 77 (27.5) | 12 (30.8) | 16 (39.0) | 49 (24.5) | ||||
| Good | 1008 (51.6) | 113 (40.4) | 16 (41.0) | 14 (34.1) | 83 (41.5) | ||||
| Very good | 282 (14.4) | 29(10.4) | 2 (5.1) | 3 (7.3) | 24 (12.0) | ||||
| Excellent | 204 (10.4) | 32 (11.4) | 2 (5.1) | 4 (9.8) | 26 (13.0) | ||||
| Mother reported general health status of father | |||||||||
| Poor | 42 (2.1) | 9 (3.2) | 0.16 | 1 (2.6) | 0.16 | 1 (2.4) | 0.11 | 7 (3.5) | 0.27 |
| Fair | 239 (12.2) | 45 (16.1) | 9 (23.1) | 11 (26.8) | 25 (12.5) | ||||
| Good | 954 (48.8) | 123 (43.6) | 21 (53.8) | 17 (41.5) | 85 (42.5) | ||||
| Very good | 419 (21.4) | 56(20.4) | 5 (12.8) | 7 (17.1) | 44 (22.0) | ||||
| Excellent | 301 (15.4) | 47 (16.8) | 3 (7.7) | 5 (12.2) | 39 (19.5) | ||||
| Marital status | |||||||||
| Marid | 1896 (97.0) | 268 (95.7) | 0.26 | 33 (84.6) | < 0.001 | 41 (100) | 0.23 | 194 (97.0) | 0.81 |
| Divorced, widowed, separated | 59 (3.0) | 12 (4.3) | 6 (15.4) | 0 | 6(3.0) | ||||
| Housing stability | |||||||||
| Homeless or housing with parents | 172 (8.8) | 24 (8.6) | 0.02 | 3 (7.7) | 0.66 | 2 (4.7) | 0.21 | 19 (9.5) | 0.11 |
| Owned | 422 (21.6) | 41 (14.6) | 6 (15.4) | 5 (11.6) | 30 (15.0) | ||||
| Rent or loan | 1361 (69.6) | 215 (76.8) | 30 (76.9) | 34 (83.7) | 151 (75.5) | ||||
| Education | |||||||||
| uncompleted school | 243 (12.4) | 32 (11.4) | 0.32 | 8 (20.5) | 0.29 | 7 (17.1) | 0.64 | 17 (8.5) | 0.07 |
| completed school or technical College | 477 (24.4) | 80 (28.6) | 9(23.1) | 10 (24.4) | 61 (30.5) | ||||
| University or higher | 1235 (63.2) | 168 (60.0) | 22 (56.4) | 24 (58.5) | 122 (61.0) | ||||
| Employment | |||||||||
| Jobless | 187 (9.6) | 30 (10.7) | 0.89 | 0 | 0.05 | 8 (19.5) | 0.07 | 22 (11.4) | 0.74 |
| Housewife | 545 (27.9) | 73 (26.1) | 17 (43.6) | 6 (14.6) | 50 (25.0) | ||||
| Employee | 1140 (58.3) | 165 (58.9) | 21 (53.8) | 26 (63.4) | 118 (58.4) | ||||
| Student | 83 (4.2) | 12 (4.3) | 1 (2.6) | 1 (2.4) | 10 (5.0) | ||||
| Income | |||||||||
| ≤ 2 minimum wages | 567 (29.0) | 87 (31.1) | 0.57 | 15 (38.5) | 0.44 | 15(36.6) | 0.48 | 57 (28.5) | 0.51 |
| 2–5 minimum wages | 1132 (57.9) | 162 (57.9) | 20 (51.3) | 20 (51.5) | 122 (61.0) | ||||
| ≥ 6 minimum wages | 256 (13.1) | 31 (11.1) | 4 (10.3) | 6 (14.6) | 21 (10.5) | ||||
| Main breadwinner of family | |||||||||
| Husband | 1463 (74.8) | 197 (70.4) | 0.34 | 23 (59) | 0.16 | 28 (69.8) | 0.81 | 146 (73.0) | 0.92 |
| Wife | 245 (12.5) | 41 (14.6) | 8 (19.5) | 8 (18.6) | 25 (12.5) | ||||
| Both husband and wife | 75 (3.8) | 13 (4.6) | 3 (2.4) | 1 (2.3) | 9 (10.2) | ||||
| Other member | 172 (8.8) | 29 (10.4) | 5 (12.8) | 4 (9.3) | 20(10.0) | ||||
| Working load of husband | |||||||||
| Jobless | 217 (11.1) | 41 (14.6) | 0.22 | 5(12.8) | 0.93 | 7 (17.1) | 0.25 | 29 (14.5) | 0.23 |
| Part time | 467 (23.9) | 56 (20.0) | 8 (20.5) | 9 (21.9) | 39 (19.5) | ||||
| Full time | 647 (33.1) | 90 (32.1) | 12 (30.8) | 17 (41.5) | 61 (30.5) | ||||
| Full time plus part time | 624 (31.9) | 93 (33.2) | 14(35.9) | 8 (19.5) | 71 (35.5) | ||||
| Social support from government | |||||||||
| With | 516 (26.4) | 67 (23.9) | 0.38 | 11 (28.2) | 0.76 | 14 (34.1) | 0.24 | 42 (20.8) | 0.08 |
| Without | 1439 (73.6) | 213 (76.1) | 28 (71.8) | 27 (65.9) | 158 (79.2) | ||||
| Main place for health care | |||||||||
| Government hospital | 1282 (65.6) | 174 (62.1) | 0.39 | 25(64.1) | 0.89 | 24 (55.8) | < 0.001 | 125 (62.5) | 0.48 |
| Private practice | 601 (30.8) | 92 (32.9) | 13 (33.3) | 10 (24.4) | 69 (34.5) | ||||
| Both | 71 (3.6) | 14 (5.0) | 1 (2.6) | 7 (17.1) | 6 (3.0) | ||||
EPTB(gestation < 28 week):Extremely preterm birth
VPTB (28 ≤ gestation < 32 week):Very preterm birth
MLPB (32 ≤ gestation < 37 week):Moderate to late preterm birth
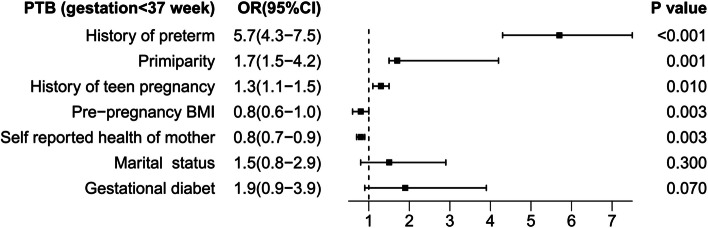
In multivariable analysis, women with a history of previous preterm birth were six times more likely to have PTB compared to women who had never experienced PTB. Moreover, the other determinants of PTB included history of teen pregnancy, pre-gestational BMI (OR = 0.8; 95% CI: 0.6–1.0), primigravida (OR = 1.7; 95% CI: 1.5–4.2) and maternal general health status (OR = 0.8; 95% CI: 0.7–0.9), shown in Fig. 1.
Fig. 1.
Adjusted odds ratios of associated variables and PTB
There was no significant association between pre-gestational BMI with EPTB and VPTB, while maternal general health status and parity were not significant contributors to MLPTB. Moreover, women who divorced, widowed and separated had five times increased risk of EPTB. Women who pregnant for first time and had gestational diabetes had four and five times increased risk of VPTB, respectively. Women with low BMI and those with a history of teen pregnancy had two times increased risk of MLPTB, shown in Table 2.
Table 2.
Association between maternal determinants and PTB subgroups
| EPTB (gestation < 28 week) | |||
| Variables | Adjusted OR | 95% CI | P |
| History of preterm | 4.4 | 2.2–8.5 | 0 < 0.001 |
| Self reported health of mother | 0.6 | 0.4–0.8 | 0.001 |
| Marital status | 5.1 | 1.9–13.7 | 0.001 |
| VPTB (28 ≤ gestation < 32 week) | |||
| Variables | Adjusted OR | 95% CI | P |
| History of preterm | 4.5 | 2.3–9.0 | 0.001 |
| Primiparity | 3.8 | 1.9–7.7 | 0.001 |
| History of teen pregnancy | 0.1 | 0.02–0.7 | 0.02 |
| Self reported health of mother | 0.7 | 0.5–0.9 | 0.02 |
| Gestational diabet | 5.2 | 1.7–16.3 | 0.005 |
| MLPB (32 ≤ gestation < 37 week) | |||
| Variables | Adjusted OR | 95% CI | P |
| History of preterm | 6.1 | 4.5–8.4 | 0 < 0.001 |
| Pre-pregnancy weight | 2.3 | 1.3–3.9 | 0.003 |
| History of teen pregnancy | 0.4 | 0.2–0.7 | 0.003 |
EPTB(gestation < 28 week):Extremely preterm birth
VPTB (28 ≤ gestation < 32 week):Very preterm birth
MLPB (32 ≤ gestation < 37 week):Moderate to late preterm birth
Discussion
The current study investigated the impact of the factors reported in international studies, especially from socioeconomic aspects and provided a snapshot of the indicators of PTB in Kazakhstan. Kazakhstan is one of the Central Asian countries with 400 000 deliveries annually [9]. The representativeness of the result is evident, given the minimal selection bias, as the concerned reproductive and prenatal hospitals in our study capture over 90% of PTB cases in the regions [14]. Moreover, the main PTB -affecting factors found in our study align with the findings of international evidence that a history of PTB remains the most significant predictor along with several maternal characteristics [15–17]. In addition, we identified marital status as a risk factor for EPTB and gestational diabetes for VPTB. Studies highlights that the diversity of factors contributed to the various subtypes of PTB, which was consistent with our findings [18]. Research has shown that the likelihood of PTB is greater among primiparas compared to multiparas [19]. The findings consistently indicated in our study that the primiparas had a 1.7 times higher risk of experiencing PTB, a 3.8 times higher risk of experiencing VPTB. At the same time, we observed an increased risk of having a preterm birth especially MLPTB among mothers with lower BMI. The result aligns with those of previous study [20]. Our study, consistent with the similar studies emphasizes the necessity of a multifaceted approach to prenatal care that goes beyond socioeconomic status to include a focus on obstetric history, age-related risks, and lifestyle factors that contribute to the well-being of both mother and child [21].
The conflicting results across studies highlight the intricate association between SES and PTB [22, 23]. While most highlighted indicators of SES such as maternal education and income [24] were not main determinants in our sample, which is consistent with the findings of the study conducted in Canadian pregnant sample [25]. A possible explanation for the weaker association between PTB and socioeconomic status (SES), especially maternal education, compared to neighboring countries like Iran [23], is Kazakhstan’s relatively well-developed public healthcare system, which provides universal access to maternity services [13]. Through this system, prenatal care, childbirth services, and postpartum care are available at little or no cost, helping to reduce disparities in healthcare access. Additionally, Kazakhstan has a high education rate, with literacy levels close to 100%. The high baseline educational attainment and broad healthcare coverage may reduce the variability in maternal health outcomes related to education and lessen its impact on PTB rates [3].
The results of the study revealed that mothers who owned their houses had reduced odds of experiencing a preterm birth compared to those living in small housing with a lot of children or living in rented or loaned residence. These findings may be explained by the fact that home ownership which reflects more excellent financial stability or reduced stress levels may play a protective role against PTB [4, 26]. Despite the variability in its definition, housing instability is widely recognized as having a significant impact on a large segment of the younger population in Kazakhstan, while purchasing a house requires more than ten years’ worth of income, excluding daily living expenses [27]. Evaluation of housing instability regarding PTB is necessary because it reflects socioeconomic inequalities that disproportionately affect the reproductive-age women [26, 28]. Kazakhstan has implemented several housing programs to address housing instability. These programs aim to boost housing construction, improve housing affordability, and provide targeted support for various socioeconomic groups. The targeted policies should expand to support the socially vulnerable groups, including low-income families and multi-child families along with accessible prenatal care.
Other predictors reported in similar studies, including advanced or younger maternal age, multiple pregnancies, obesity, smoking and preeclampsia, are failed to be observed in the study [29]. Moreover, the distinct predictors associated with extremely preterm birth (EPTB), very preterm birth (VPTB), and moderate-to-late preterm birth (MLPTB) found in our study confirm that preterm birth is a multifaceted syndrome with diverse etiologies and phenotypes, each displaying unique characteristics [20, 30]. This heterogeneity highlights the complexity of preterm birth and underscores the need to differentiate between the various types to understand their specific underlying mechanisms better. Observing these predictors in the study could be due to various reasons, including sample size limitations, differences in population characteristics, or variations in data collection methods [8]. Additionally, it's possible that the population under study had lower exposure to these risk factors or that these factors were underreported or not sufficiently captured in the data.
The limitations of the study include the reliance on self-reported data for some variables, such as general health status and lifestyle factors, which introduces the possibility of recall bias and social desirability bias. Such inaccuracies can obscure the true relationship between variables and health outcome. For example, when determining social variables, participants may overreport income levels or education attainment if they feel these answers reflect positively on them, or they may downplay certain difficulties, such as financial stress, due to social stigma. This could lead to inaccurate or inflated responses, obscuring the true relationship between these socioeconomic factors and health outcomes like preterm birth. Additionally, using data from only three specific setting with 98% of Kazakh ethnicity may only partially capture the national characteristics of PTB in Kazakhstan. Future nationwide studies should address these limitations by incorporating more precise measures of SES and health behaviors and exploring the potential mediating effects of other factors, such as stress and medical support, on the relationship between SES and birth outcomes.
Conclusion
In conclusion, this study fills an essential gap in the existing literature, as limited studies have investigated the association between SES and preterm birth among the Kazakh population. Although SES does not affect the factor of preterm birth statistically, its possible interaction with other determinants of health suggests that addressing disparities in living conditions remains an essential component of public health interventions aimed at improving the outcome. Moreover, other factors such as previous preterm, parity, and first childbirth age affect various levels of prematurity, providing valuable insights into the multifaceted nature of preterm birth. Moreover, since there have been limited studies in this field, our study can provide foundational information for future studies.
Supplementary Information
Authors’ contributions
All authors fulfill the authorship criteria through participating in designing the study, data collection, data analysis, drafting the manuscript and making substantial contribution to its contents in subsequent versions.
Funding
The research funded by the project named “Gene-infection interaction in spontaneous preterm birth” by the Ministry of Science and Higher Education of the Republic of Kazakhstan (AP14972889) and “Clinical, Genomic and Environmental Variable Approach to Preterm birth” by the Ministry of Science and Higher Education of the Republic of Kazakhstan (AP14869249).
Data availability
The data sets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Ethics approval and consent to participate
Ethical approval was obtained from the Al-Farabi Kazakh national university Ethical Committee (IRB-A308). The study performed in accordance with the Declaration of Helsinki.
Written informed consent was obtained form all the participants.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Romero R, Espinoza J, Kusanovic JP, Gotsch F, Hassan S, Erez O, Chaiworapongsa T, Mazor M. The preterm parturition syndrome. BJOG. 2006;113 Suppl 3(Suppl 3):17–42. 10.1111/j.1471-0528.2006.01120.x. Erratum in: BJOG. 2008 Apr;115(5):674–5. PMID: 17206962; PMCID: PMC7062298. [DOI] [PMC free article] [PubMed]
- 2.Ohuma EO, Moller AB, Bradley E, Chakwera S, Hussain-Alkhateeb L, Lewin A, Okwaraji YB, Mahanani WR, Johansson EW, Lavin T, Fernandez DE, Domínguez GG, de Costa A, Cresswell JA, Krasevec J, Lawn JE, Blencowe H, Requejo J, Moran AC. National, regional, and global estimates of preterm birth in 2020, with trends from 2010: a systematic analysis. Lancet. 2023;402(10409):1261–71. https://doi.org/10.1016/S0140-6736(23)00878-4. Erratum.In:Lancet.2024;403(10427):618. 10.1016/S0140-6736(24)00267-8. (PMID: 37805217). [DOI] [PubMed]
- 3.National Academies of Sciences, Engineering, and Medicine; National Academy of Medicine; Committee on the Future of Nursing 2020–2030; Flaubert JL, Le Menestrel S, Williams DR, et al., editors. The Future of Nursing 2020–2030: Charting a Path to Achieve Health Equity. Washington (DC): National Academies Press (US); 2021 May 11. 2, Social Determinants of Health and Health Equity. Available from: https://www.ncbi.nlm.nih.gov/books/NBK573923/. [PubMed]
- 4.Robinson K, Sherman ADF, Ogunwole S, Meggett J, Sharps P. Social Determinant of Housing Instability and Adverse Pregnancy Outcomes: A Scoping Review. J Perinat Neonatal Nurs. 2022;36(2):118–130. 10.1097/JPN.0000000000000648. PMID: 35476765. [DOI] [PubMed]
- 5.Nunes BP, Thumé E, Tomasi E, Duro SM, Facchini LA. Socioeconomic inequalities in the access to and quality of health care services. Rev Saude Publica. 2014;48(6):968–76. 10.1590/S0034-8910.2014048005388.PMID:26039400;PMCID:PMC4285826. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Kim MK, Lee SM, Bae SH, Kim HJ, Lim NG, Yoon SJ, Lee JY, Jo MW. Socioeconomic status can affect pregnancy outcomes and complications, even with a universal healthcare system. Int J Equity Health. 2018Jan 5;17(1):2. 10.1186/s12939-017-0715-7.PMID:29304810;PMCID:PMC5756361. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Maher GM, Ward LJ, Hernandez L, Kublickas M, Duvekot JJ, McCarthy FP, Khashan AS, Kublickiene K. Association between socioeconomic status with pregnancy and neonatal outcomes: An international multicenter cohort. Acta Obstet Gynecol Scand. 2023;102(11):1459–1468. 10.1111/aogs.14659. Epub 2023 Aug 21. PMID: 37602747; PMCID: PMC10577636. [DOI] [PMC free article] [PubMed]
- 8.Thoma ME, Drew LB, Hirai AH, Kim TY, Fenelon A, Shenassa ED. Black-White Disparities in Preterm Birth: Geographic, Social, and Health Determinants. Am J Prev Med. 2019;57(5):675–86. 10.1016/j.amepre.2019.07.007. (Epub 2019 Sep 25 PMID: 31561920). [DOI] [PubMed] [Google Scholar]
- 9.Sakko Y, Turesheva A, Gaipov A, Aimagambetova G, Ukybassova T, Marat A, Kaldygulova L, Amanzholkyzy A, Nogay A, Khamidullina Z, Mussenov Y, Almawi WY, Atageldiyeva K. Epidemiology of spontaneous pregnancy loss in Kazakhstan: A national population-based cohort analysis during 2014–2019 using the national electronic healthcare system. Acta Obstet Gynecol Scand. 2023;102(12):1682–1693. 10.1111/aogs.14669. Epub 2023 Sep 4. PMID: 37667510; PMCID: PMC10619606. [DOI] [PMC free article] [PubMed]
- 10.Yerdessov N, Zhamantayev O, Bolatova Z, Nukeshtayeva K, Kayupova G, Turmukhambetova A. Infant Mortality Trends and Determinants in Kazakhstan. Children (Basel). 2023May 24;10(6):923. 10.3390/children10060923.PMID:37371155;PMCID:PMC10297167. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Sabyrdilda Zh, Kosherbayeva L, Qumar A, Abikulova A, Akhmentzhan A. Situational Analysis of Maternal and Infant Mortality in Kazakhstan, 21 March 2024, PREPRINT (Version 1) available at Research Square. 10.21203/rs.3.rs-4091410/v1.
- 12.Oralkhan Zh, Sarsenova L, Kopbayeva M, Tastambek K, Grjibovski AM, Berdalinova A, Balmagambetova A, Zhurabekova G. Maternal correlates of spontaneous preterm birth in Kazakhstan: a matched case-control study. Ekologiya cheloveka (Human Ecology). 2023;30(12):901–8. 10.17816/humeco629001. [Google Scholar]
- 13.Multiple Indicator Cluster Survey (MICS) in the Republic of Kazakhstan 2010–2011. Monitoring the Situation of Children and Women; Statistics Committee of the Ministry of National Economy of the Republic of Kazakhstan: Astana, 2012.
- 14.International trade administration Kazakhstan – country commercial guide. Accessed January 2, 2023. https://www.trade.gov/country‐commercial‐guides/kazakhstan‐healthcare.
- 15.Institute of Medicine (US) Committee on Understanding Premature Birth and Assuring Healthy Outcomes; Behrman RE, Butler AS, editors. Preterm Birth: Causes, Consequences, and Prevention. Washington (DC): National Academies Press (US); 2007. 10, Mortality and Acute Complications in Preterm Infants. Available from: https://www.ncbi.nlm.nih.gov/books/NBK11385/. [PubMed]
- 16.Ville Y, Rozenberg P. Predictors of preterm birth. Best Pract Res Clin Obstet Gynaecol. 2018Oct;52:23–32. 10.1016/j.bpobgyn.2018.05.002. (Epub 2018 Jul 7 PMID: 30309793). [DOI] [PubMed] [Google Scholar]
- 17.Suff N, Xu VX, Dalla Valle G, Carter J, Brennecke S, Shennan A. Prior term delivery increases risk of subsequent recurrent preterm birth: An unexpected finding. Aust N Z J Obstet Gynaecol. 2022;62(4):500–505. 10.1111/ajo.13504. Epub 2022 Feb 27. PMID: 35220589; PMCID: PMC9543374. [DOI] [PMC free article] [PubMed]
- 18.Ji X, Wu C, Chen M, Wu L, Li T, Miao Z, Lv Y, Ding H. Analysis of risk factors related to extremely and very preterm birth: a retrospective study. BMC Pregnancy Childbirth. 2022;22(1):818. 10.1186/s12884-022-05119-7.PMID:36335328;PMCID:PMC9636775. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Koullali B, van Zijl MD, Kazemier BM, Oudijk MA, Mol BWJ, Pajkrt E, Ravelli ACJ. The association between parity and spontaneous preterm birth: a population based study. BMC Pregnancy Childbirth. 2020Apr 21;20(1):233. 10.1186/s12884-020-02940-w.PMID:32316915;PMCID:PMC7175552. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Girsen AI, Mayo JA, Carmichael SL, Phibbs CS, Shachar BZ, Stevenson DK, Lyell DJ, Shaw GM, Gould JB; March of Dimes Prematurity Research Center at Stanford University School of Medicine. Women's prepregnancy underweight as a risk factor for preterm birth: a retrospective study. BJOG. 2016;123(12):2001–2007. 10.1111/1471-0528.14027. Epub 2016 May 13. PMID: 27172996; PMCID: PMC5069076. [DOI] [PMC free article] [PubMed]
- 21.Tamura N, Hanaoka T, Ito K, Araki A, Miyashita C, Ito S, Minakami H, Cho K, Endo T, Sengoku K, Ogasawara K, Kishi R. Different Risk Factors for Very Low Birth Weight, Term-Small-for-Gestational-Age, or Preterm Birth in Japan. Int J Environ Res Public Health. 2018;15(2):369. 10.3390/ijerph15020369.PMID:29466290;PMCID:PMC5858438. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Vieira ACF, Alves CMC, Rodrigues VP, Ribeiro CCC, Gomes-Filho IS, Lopes FF. Oral, systemic and socioeconomic factors associated with preterm birth. Women Birth. 2019;32(1):e12–6. 10.1016/j.wombi.2018.02.007. (Epub 2018 Mar 16 PMID: 29551483). [DOI] [PubMed] [Google Scholar]
- 23.Dolatian M, Sharifi N, Mahmoodi Z. Relationship of socioeconomic status, psychosocial factors, and food insecurity with preterm labor: A longitudinal study. Int J Reprod Biomed. 2018;16(9):563–570. PMID: 30643863; PMCID: PMC6312711. [PMC free article] [PubMed]
- 24.Bushnik T, Yang S, Kaufman JS, Kramer MS, Wilkins R. Socioeconomic disparities in small-for-gestational-age birth and preterm birth. Health Rep. 2017;28(11):3–10 (PMID: 29140535). [PubMed] [Google Scholar]
- 25.Campbell EE, Gilliland J, Dworatzek PDN, De Vrijer B, Penava D, Seabrook JA. Socioeconomic status and adverse birth outcomes: a population-based canadian sample. J Biosoc Sci. 2018;50(1):102–13. 10.1017/S0021932017000062. (Epub 2017 Mar 8 PMID: 28270256). [DOI] [PubMed] [Google Scholar]
- 26.Zielenbach M, Ekpe E, Oot A, Yeh C, Yee LM. Association of Antenatal Housing Instability with Perinatal Care Utilization and Outcomes. J Womens Health (Larchmt). 2024;33(1):90–97. 10.1089/jwh.2023.0002. Epub 2023 Nov 1. PMID: 37944106; PMCID: PMC10794825. [DOI] [PMC free article] [PubMed]
- 27.Mukayev D, Shalbolova U, Tanaś, J. Housing affordability analysis in Kazakhstan based on D-HAQ model. Journal of International Studies. 2022;15(4):28–42. 10.14254/2071-8330.2022/15-4/2. [Google Scholar]
- 28.Pantell MS, Baer RJ, Torres JM, Felder JN, Gomez AM, Chambers BD, Dunn J, Parikh NI, Pacheco-Werner T, Rogers EE, Feuer SK, Ryckman KK, Novak NL, Tabb KM, Fuchs J, Rand L, Jelliffe-Pawlowski LL. Associations between unstable housing, obstetric outcomes, and perinatal health care utilization. Am J Obstet Gynecol MFM. 2019;1(4):100053. 10.1016/j.ajogmf.2019.100053. Epub 2019 Oct 16. PMID: 33345843. [DOI] [PubMed]
- 29.Mitrogiannis I, Evangelou E, Efthymiou A, Kanavos T, Birbas E, Makrydimas G, Papatheodorou S. Risk factors for preterm birth: an umbrella review of meta-analyses of observational studies. BMC Med. 202321(1):494. 10.1186/s12916-023-03171-4.PMID:38093369;PMCID:PMC10720103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Räisänen S, Gissler M, Saari J, Kramer M, Heinonen S. Contribution of risk factors to extremely, very and moderately preterm births - register-based analysis of 1,390,742 singleton births. PLoS One. 2013;8(4):e60660. 10.1371/journal.pone.0060660. Epub 2013 Apr 5. PMID: 23577142; PMCID: PMC3618176. [DOI] [PMC free article] [PubMed]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The data sets used and/or analyzed during the current study are available from the corresponding author on reasonable request.