Summary
Background
Migrant women who are pregnant or postpartum and their infants are often at increased risk of poorer perinatal outcomes compared to host country populations. This review aimed to identify public health, policy, and clinical interventions to improve maternity care for migrant women and their infants in high-income countries (HICs).
Methods
In this systematic review we searched EMBASE, EMCARE, MEDLINE and PsycINFO, CENTRAL, Scopus, CINAHL Plus, Web of Science, and grey literature from inception to 13th March 2024, with no language or date restrictions (PROSPERO: CRD42022380678). Interventional and observational studies assessing the effectiveness of any intervention to improve perinatal care for migrant women and their infants in HICs delivered in the pregnancy, peripartum, or postpartum period (up to one year after birth) were included. Quantitative outcomes were extracted. Qualitative studies were excluded. The main outcomes of interest were preterm birth, birthweight, and appointment attendance. Quantitative synthesis was conducted using Harvest plots and binomial exact calculations.
Findings
15,689 records were retrieved, 29 studies comprising data from 16,763,837 women were included. 22 studies (75.9%) included multiple interventions. Five interventions had strong evidence of effectiveness. Two clinical interventions: 100.0% of studies including specialist multidisciplinary teams improved one or more of the main outcomes of interest, namely preterm birth, birthweight, and appointment attendance (95% confidence interval 73.5–100.0%; p < 0.001); and 90.9% of studies including specialist in-person interpreting improved one or more of the main outcomes of interest (58.7–100.0%; p = 0.012). Three public health or policy interventions: 100.0% of social welfare interventions (75.3%–100.0%; p < 0.001) improved one or more of the main outcomes of interest; 100.0% of maternal education interventions (71.5–100.0%. p < 0.001), and 83.3% of studies assessing access to free healthcare (51.6–97.9%; p = 0.039).
Interpretation
The findings suggest that multicomponent interventions comprising multidisciplinary teams, in-person interpreting, maternal education, and social welfare support can improve perinatal outcomes for migrant women and their infants. Removing financial barriers to care may improve perinatal outcomes and be cost saving to healthcare systems. However, these findings should be interpreted with caution given that most included studies were of poor quality and that sensitivity analysis restricting to interventional studies only did not demonstrate any effect on the main outcomes of interest.
Funding
KS is supported by a National Institute for Health Research (NIHR) Doctoral Fellowship (NIHR302577). HRJ is supported by an NIHR Advanced Fellowship (NIHR303183). HRJ is supported by NIHR Applied Research Collaboration (ARC) South London. MM is supported by a Medical Research Council Clinical Research Training Fellowship (Grant number MR/W01498X/1). GF is supported by a Nuffield Department of Population Health Clinical Research Fellowship. MK is an NIHR Senior Investigator (NIHR303806). The views expressed are those of the authors and not necessarily those of the NIHR or the Department of Health and Social Care.
Keywords: Public health, Obstetrics, Paediatrics, Health policy
Research in context.
Evidence before this study
Women who are migrants and who are pregnant or postpartum may be at higher risk of poorer perinatal outcomes because of pre-migration, transit, and post-migration stressors, and this can have longer-term impacts on their health and the health of their children. In preparing for this review, a rapid literature search including the key terms “migrant”, “intervention”, “maternity care”, “high-income” and “systematic review” was conducted for papers published on MEDLINE and PubMed from inception until 13th March 2024. Three systematic reviews were retrieved, none of which identified public health or policy interventions and all of which highlighted the need for further research amongst a more diverse range of HICs.
Added value of this study
Findings from our review suggest perinatal care for underserved migrant women and their infants in HICs could be delivered by multidisciplinary teams with access to specialist in-person interpreters, alongside maternal education programmes. There was good evidence for the effectiveness of group antenatal care, mental health support, and continuity of care through a known midwife, a small team of midwives, or multi-disciplinary professionals alongside social welfare support such as housing, immigration, social welfare, food banks, and free clothing/baby equipment support embedded within clinical services. Wider public health interventions such as these are crucial to achieving the UN’s Sustainable Development Goal of access to Universal Health Coverage for all by 2030 which includes financial risk protection and access to quality essential health-care services for all regardless of migration background.
Implications of all the available evidence
The findings highlight the importance of policy and public health interventions alongside equitable clinical care for pregnant migrant women and their infants in HICs. Recognising that the evidence from this review suggests that access to free maternity care for migrant women in HICs can improve outcomes and be cost saving to national and regional healthcare systems, policymakers should consider prioritising this approach to financing maternity care for migrant women. Overall, there is a need for further research exploring the effectiveness of public health and policy interventions in this field, as well as the effectiveness of interventions offering extended postpartum care, infant feeding support, mental health support, and doula services.
Introduction
Approximately 2.3 percent of the world’s population lives outside their country of nationality.1 This constitutes approximately 281 million international migrants and 89 million forced migrants, and this has been increasing in past decades.1 Rates of migration to high-income countries (HICs) have also been increasing, particularly to the United States (US) and Europe.1 In the US, migrant women represent approximately 14% of the total female population.2 In England and Wales, one in three women giving birth is from a migrant background.3 The majority of international migrants move voluntarily for economic or family reasons, but approximately one third are forced to move due to climate change, conflict, or persecution.1
Migrants giving birth in a host country can have difficulty accessing maternity care, and may face significant barriers in maternity services.4, 5, 6 This includes discrimination, poverty, social isolation, lack of knowledge about services, and language barriers.4, 5, 6 Forced migrant women experience additional challenges including war trauma, perilous journeys, and limited access to free healthcare.5,7,8 The evidence surrounding perinatal outcomes for migrant women and their infants is conflicting8, 9, 10, 11, 12, 13, 14; some studies have demonstrated as good or better perinatal outcomes for migrant communities compared to host populations, but others have demonstrated poorer outcomes. A systematic review by Gagnon et al. of studies published between 1995 and 2008 demonstrated a lower or similar prevalence of preterm birth and low birthweight amongst migrants compared to women born in high-income host countries.11 A meta-analysis distinguishing between region of origin demonstrated migrants moving from lower income countries had poorer perinatal outcomes compared to those from higher income countries. Heslehurst et al. conducted a systematic review of systematic reviews and found that globally asylum seekers and refugees had poorer perinatal outcomes compared to host country populations, but they did not assess outcomes in high-income host countries separately.9 These outcomes can have an adverse effect on the immediate and longer term health of the mother and child.8,13,15
Most HICs provide some level of maternity care for migrant women, but services are rarely tailored to their needs and some charge women for maternity care.7,16, 17, 18 In the US, migrant women who cannot afford to pay for care may be eligible for Medicaid or Refugee Medical Assistance (RMA), but many low-income and undocumented (persons who do not fulfil the administrative requirements established by the country of destination to enter, stay, or exercise an economic activity) migrant women are not offered free care and have to pay out-of-pocket if they cannot afford private medical insurance.19,20 In the UK, refugees and asylum seekers are offered free maternity care, but undocumented migrants are charged 150% of NHS care costs.21,22 Across Europe, refugees and asylum seekers are usually offered free maternity care, but undocumented migrants often pay out-of-pocket.23 Three reviews have explored interventions to improve outcomes for pregnant migrant women and their infants in HICs, but all focused on clinical interventions and none focused on policy or public health interventions.16,17,24 All included interventions which were qualitatively evaluated, and found that migrant women valued peer support and holistic care. One identified six quantitatively evaluated interventions which were mostly from the US, but they were of weak to moderate quality and focused only on clinical care.17 All reviews highlighted the need for further research in this area, particularly amongst a more diverse range of HICs.
This systematic review aimed to update the literature through identifying existing interventions that aim to improve perinatal outcomes for migrant women and infants in HICs and determine their effectiveness through quantitative synthesis. Unlike previous reviews which focused only on clinical maternity care and synthesised qualitative outcomes, this review sought to also include interventions addressing the wider determinants of health including policy and public health interventions and focused on quantitative synthesis. In addition, there has been a large increase in literature in this field in the past several years, and no recent systematic reviews exist. The primary objective was to determine what interventions exist to improve perinatal outcomes for migrant women in HICs. The secondary objective was to explore the effectiveness of these interventions by exploring the impact on perinatal outcomes. In this review, the perinatal period is defined as the antenatal, intrapartum, and postpartum period (up to one year after birth). The perinatal outcomes of interest were decided with mothers with lived experience of migration and maternity care in the UK, alongside references to World Health Organisation (WHO) measures of quality in maternity care.25
Methods
Public involvement and equality statement
Our authorship team includes mothers living in the UK with lived experience of migration and maternity care in the UK from a range of backgrounds. These women helped design the research question, analyse, and interpret these data to maximise relevance and contextual insight. Together we decided to include an assessment of the involvement of migrant women in the design and or the delivery of the interventions. The terms ‘pregnant women’ and ‘mothers’ will be used throughout this review, but the authors recognise not everyone who is pregnant or giving birth will identify as a woman or a mother.
Search strategy and selection criteria
The protocol was registered with PROSPERO (CRD42022380678) in December 2022, peer-reviewed, and published in August 2023.26 Studies of migrant women who were pregnant or up to one year postpartum were eligible for inclusion.27 Studies of women aged over fifteen years (usual age of consent for medical treatment), living in a high-income country (HIC) (defined as being in the World Bank high-income economy category), and who were born outside their host country were included, i.e., first-generation migrants.27,28 Studies in which fewer than 90% of participants were first generation migrants, i.e., not born in the host country, were excluded to maximise the relevance of the findings to the most underserved groups of migrant women. Eligible interventions were any hospital- or community-based initiatives offered in the antenatal, perinatal, or postnatal period (up to one year postpartum) that aimed to improve any maternal or infant outcomes. The comparison group was usual care if data were available. If no comparison group was given, studies were included and assessed as beneficial or not based on before and after comparisons.
The main outcomes of interest were decided based on the literature and input from our stakeholders and service users; these were rates of preterm birth, birthweight, and number of antenatal or postnatal appointments attended. These are also key measures of maternity care quality according to the WHO.25 However, as per Cochrane systematic review guidance, any outcomes were recorded and synthesised.29 Observational, quasi-experimental, and experimental intervention studies with quantitative outcomes were included. Abstracts, non-empirical research, opinion, or editorial pieces were excluded, but all were assessed to determine if any relevant studies were cited. If duplicate reports or publications of the same data were retrieved, the less recent version was excluded. Studies with only qualitative outcomes were excluded given that these studies have been extensively reviewed previously.16,17,24 Interventions that were not specifically designed or adapted for migrant women or their infants in the perinatal period were excluded to ensure data are focused on interventions that could have direct impact on outcomes for migrant women and their infants. Inclusion and exclusion criteria are summarised in Table 1.
Table 1.
Inclusion and exclusion criteria.
| Inclusion Criteria | Exclusion Criteria |
|---|---|
| Observational, quasi-experimental, and experimental intervention studies | Qualitative outcome assessments only |
| Quantitative outcome measures | Abstracts, non-empirical research, opinion, or editorial pieces |
| Interventions designed to be delivered in pregnancy, intrapartum, or postpartum (up to one year after birth) | Interventions not specifically designed or adapted for migrant women or their infants in the perinatal period |
| Studies including women aged over fifteen years (usual age of consent for medical treatment) | Studies in which fewer than 90% of participants were first generation migrants, i.e., not born in host country |
| Intervention delivered in a high-income country | |
| Any hospital- or community-based initiatives |
EMBASE, EMCARE, MEDLINE, PsycInfo, CENTRAL, Scopus, CINAHL Plus, and Web of Science were searched for studies published from inception up until 13th March 2024 (Appendix 1). Grey literature sources including Google Scholar and trial registries were searched up until 28th January 2023. The first 150 results from the following sources were searched: Google Scholar, WHO International Clinical Trials Registry Platform, Clinicaltrials.gov, the WHO Website, and the UN Refugee Agency website. The Boolean operators ‘AND’ and ‘OR’ were employed to combine the descriptors, where appropriate. No date or language restrictions were applied. Forward and backward citation searching was employed on all included articles, and the reference lists of all included articles were searched. If studies were published in a language other than English, a member of the research team fluent in that language assessed it for likely relevance and extracted the data, if appropriate. The article was translated using Google Translate™ and a second reviewer reviewed its relevance and extracted the data, if appropriate. If none of the research team were fluent in the language, papers were assessed by two reviewers using Google Translate™. EndNote™ was used to collect and manage the studies retrieved.30 Covidence™ was used for deduplication and study selection.31
Screening and data extraction
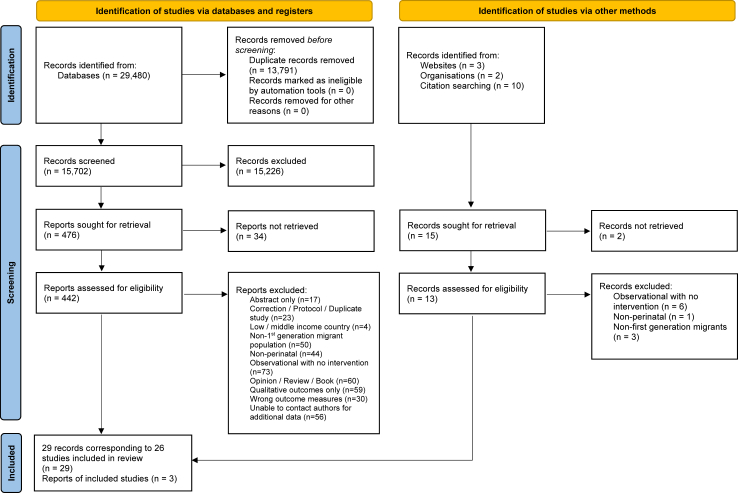
Two independent reviewers (KS and SE/GF/MMC/NSC/HRJ/KO/RA/MA) screened the abstracts and full texts for relevance. Full texts were assessed for eligibility using a checklist of the inclusion and exclusion criteria. All excluded articles from the full text screening were recorded with reason for exclusion noted. Disagreements between reviewers were discussed and agreement sought from a third reviewer if necessary. If data were not accessible from the paper, the authors were contacted. All extracted data were recorded on the piloted data extraction form by two separate reviewers and cross-checked. A flowchart summarises the selection process (Fig. 1). Study characteristics are summarised in Appendix 2.
Fig. 1.
Preferred reporting items for systematic reviews and meta-analysis (PRISMA) flow diagram.
Deviations from the protocol
The authors originally planned to include only interventional studies in this review. However, following the full literature search it became clear that there were several observational studies of interventions which could provide valuable insights into effective interventions in this area. Thus, it was decided that both observational and interventional studies would be included, and that the findings for interventional studies would be presented separately.
Quality assessment and risk of bias
Two independent reviewers (KS and SE/GF/MMC/NSC/HRJ) performed critical appraisal, and this was cross-checked. The Quality Assessment Tool for Quantitative Studies was used to assess rigor for each included study and confidence in the strength of evidence (Appendix 3).32 This tool was chosen as it was developed and validated to assess both observational and interventional studies and shows reliability and validity. We expected to identify many non-randomised studies of interventions. These studies have a high risk of time-related bias such as when prevalent users of an intervention rather than incident users are included in analyses and compared to non-users; this is known as lead time bias.29 We mitigated this by including an assessment of time-related bias using the Risk of Bias in Non-Randomised Studies (ROBINS-I) tool (Appendix 3).33 Publication bias was not assessed given the lack of standardised outcome data.
Data synthesis
Narrative synthesis was conducted according to Cochrane guidance and included creation of categories of interventions with input from the research team and experts by experience.34 A meta-analysis was planned if sufficient studies reported data on the same outcomes in a format that could be meaningfully combined into estimates of pooled odds ratios or risk ratios. Due to heterogeneity of outcome measures, meta-analysis was not possible, and we therefore followed Cochrane guidance to create a Harvest Plot.34 A Harvest Plot is a visual supermatrix summarising vote counting by categorising studies as having a beneficial effect or no effect in each outcome category. Each bar represents a single study and is annotated with the reference number. Bar height indicates study quality: strong (tallest), moderate (medium), weak (shortest). Following the Cochrane guidance, for the main outcomes of interest (preterm birth, birthweight, and appointment attendance) an intervention is counted as beneficial if there is evidence of benefit in each outcome separately. For analyses including all outcomes presented in the studies, a study is counted as beneficial if one or more of the outcomes in each outcome group showed evidence of benefit. Vote counting is recommended when there are inconsistent effect measures across studies. Traditional vote counting methods using statistical significance, magnitude of effect, or subjective rules have been shown to be misleading.34 In accordance with Cochrane guidance, we calculated the proportion of beneficial studies using the binomial exact calculation, i.e., using raw numbers and not relying on statistical tests. We analysed the number of studies showing improvement in the outcomes of interest compared to the number of total outcomes reported per intervention category. Sensitivity analysis according to study quality, method of recruitment, and service user involvement was conducted. Statistical analyses were conducted using R Studio.35 This strength of evidence assessment was based on the amount of evidence available, visual inspection of the Harvest Plot, the binomial exact calculation, and risk of bias assessment. This systematic review is reported in accordance with the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) guidelines.
Role of the funders
The funders had no role in study design, data collection, data analysis, data interpretation, or writing of the report.
Results
The search retrieved 29,495 records, of which 15,689 abstracts were screened after duplicates were removed. 442 full texts were reviewed, and 29 studies were included comprising data from 16,763,837 women (Fig. 1) (Appendix 2).36, 37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53, 54, 55, 56, 57, 58, 59, 60, 61, 62, 63, 64 Studies were published between 1986 and 2023. 19 studies (66%) were published since 2015. 112 studies included mixed migrant populations, e.g., first- and second-generation migrant women. We contacted all these authors asking for disaggregated data for first generation migrants only (as per our inclusion criteria). 55 (49%) replied, and 22 (20%) were able to provide disaggregated data for first generation migrants. Characteristics of included studies are presented in Table 2. According to the Quality Assessment Tool for Quantitative Studies Tool,32 17 studies (59%) were of weak quality, 9 (31%) moderate, and 3 (10%) strong. 5 studies (17%) were at low risk of time-related bias assessed using the Risk of Bias in Non-Randomised Studies (ROBINS-I) Tool,33 15 (52%) at moderate risk, 7 (24%) at serious risk, and 2 (7%) did not provide enough information to make an assessment.
Table 2.
Characteristics and references of included studies, full study details are provided in Appendix 2 N = 29 studies.
| Characteristic | n (%)a |
|---|---|
| Study design: | |
| Randomised Controlled Trial41,43,46,47 | 4 (13.8%) |
| Cluster Randomised Controlled Trial39 | 1 (3.4%) |
| Controlled Clinical Trial36,44,45,55 | 4 (13.8%) |
| Cohort analytic (difference-in-difference)42 | 1 (3.4%) |
| Cohort (one group pre + post)40 | 1 (3.4%) |
| Quasi-experimental trial (1 intervention and 1 historical control group)37 | 1 (3.4%) |
| Interrupted time series analysis54 | 1 (3.4%) |
| Retrospective Cohort Study38,48, 49, 50,52,53,56, 57, 58,60,62, 63, 64 | 14 (48.3%) |
| Economic model59,61 | 2 (6.9%) |
| Country: | |
| US41,43,47,49,50,52,57,58,60, 61, 62, 63, 64 | 13 (44.8%) |
| Australia45,51,53,54,56 | 5 (17.2%) |
| Sweden37,38,46 | 3 (10.3%) |
| Canada42,48 | 2 (6.9%) |
| UK44,55 | 2 (6.9%) |
| Denmark39 | 1 (3.4%) |
| Japan40 | 1 (3.4%) |
| South Korea36 | 1 (3.4%) |
| Multi-country59 | 1 (3.4%) |
| Multi-component intervention: | |
| Yes36, 37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53, 54,56,57,65 | 22 (75.9%) |
| No58, 59, 60, 61, 62, 63, 64 | 7 (24.1%) |
| Perinatal period: | |
| Antenatal37,39,44,45,48,51, 52, 53, 54,56,59,61, 62, 63, 64 | 15 (51.7%) |
| Intrapartum38,46,57 | 3 (10.3%) |
| Postpartum36,42,55 | 3 (10.3%) |
| Antenatal/Intrapartum58 | 1 (3.4%) |
| Perinatal Period40,41,43,47,49,50,60 | 7 (24.1%) |
| Service user involvement in design/delivery: | |
| No service user involvement40,44,45,48,49,52,53,56,58, 59, 60, 61, 62, 63, 64 | 15 (51.7%) |
| Co-designed37,39,54 | 3 (10.3%) |
| Co-delivered36,38,41,46,47 | 5 (17.2%) |
| Co-designed and Co-Delivered42,43,50,51,55,57 | 6 (20.7%) |
| Intervention categories:a | |
| Maternity care interventions | |
| Specialist in-person interpreting18,20,23,27,31,32,36,39 | 13 (15.7%) |
| Trained peer/shared culture worker36,38,41, 42, 43,46,47,50,51,55,57 | 11 (13.3%) |
| Specialist multidisciplinary team48, 49, 50, 51,53,54,56 | 7 (8.4%) |
| Group antenatal care37,51,54,56 | 4 (4.8%) |
| Continuity of midwifery care37,53,56,57 | 4 (4.8%) |
| Mental health support36,48,53,56 | 4 (4.8%) |
| Extended postpartum support36,41,47,56 | 4 (4.8%) |
| Birth doula38,46,57 | 3 (3.6%) |
| Infant feeding support41,42,52 | 3 (3.6%) |
| Public health or policy interventions | |
| Education materials/classes for mothers36,39,40,43, 44, 45,49,51,52,55,56 | 11 (12.9%) |
| Social welfare assistance48, 49, 50,52,53,55,56 | 7 (8.4%) |
| Free healthcare58, 59, 60, 61,63,64 | 6 (7.2%) |
| Social/peer support40,41,43,47 | 4 (4.8%) |
| Staff education/process reform39,54 | 2 (2.4%) |
| Immigration law reforms62 | 1 (1.2%) |
| Mobile perinatal care49 | 1 (1.2%) |
| Outcome categories:a | |
| Main outcomes | |
| Antenatal/postnatal appointment attendance37,47, 48, 49, 50, 51, 52,54,56,58,60,64 | 12 (36.4%) |
| Birthweight37,44,48,49,52,56,58, 59, 60,63,64 | 11 (33.3%) |
| Preterm birth48,49,52,53,56,58,60,62, 63, 64 | 10 (30.3%) |
| All outcomes | |
| Any perinatal outcome38,39,44,46,48,49,52,53,55, 56, 57, 58, 59, 60,62, 63, 64,b | 17 (31.5%) |
| Care satisfaction/engagement37,40,46,50,52,54,56,58,60,64,c | 10 (18.5%) |
| Adequacy of care47, 48, 49,51,54,58,60,d | 7 (13.0%) |
| Mental health/wellbeing36,37,40,43,46,47,51 | 7 (13.0%) |
| Breastfeeding outcomes41,42,45,47,53,56 | 6 (11.1%) |
| Infant health outcomes44,47,50,61,62 | 5 (9.3%) |
| Cost-effectiveness59,61 | 2 (3.7%) |
Proportions will not total 100% if studies appear in more than one intervention or outcome category.
Any maternal or neonatal (up to 28 days old) health outcome: rates of miscarriage, stillbirth, small/large for gestational age, preeclampsia, preterm birth, induction of labour, birthweight, postpartum haemorrhage, mode of delivery, Apgar∗ score, critical care admission, maternal/neonatal death.
Subjective maternal assessment of quality and satisfaction with maternity care received, e.g., through a validated questionnaire; number of antenatal or postnatal appointments attended.
An assessment of the sufficiency of the maternity care received including gestational age at booking and adherence to national/international maternity care guidelines.
Sixteen types of intervention were identified; these were further classified into ‘Maternity Care Interventions’ defined as interventions that focused on maternity care delivery in hospital or in the community, and ‘Public Health or Policy Interventions’ defined as policy and public health interventions focused on the broader determinants of health. Operational definitions of intervention categories are presented in Table 3.
Table 3.
Operational definitions and examples of intervention categories.
| Intervention category | Operational definition | Examples from included studies |
|---|---|---|
| (1) Maternity care interventions | ||
| Specialist multidisciplinary team | Maternity care system that has been specifically tailored to the needs of migrant women including specialist multidisciplinary staff and clinical care. | Specialist multi-disciplinary migrant antenatal care team including clinicians, social workers, interpreters, psychologists.38,54 |
| Trained peer/shared culture worker | A migrant woman with experience of giving birth in the host country i.e., a service user who is trained to provide perinatal support, or someone from the same migration or cultural background who is specifically trained to work with migrant women during maternity care. | Somali-speaking doula supporting newly arrived Somali women during birth.58 Immigrant mothers living in Korea trained to visit new immigrant mothers at home for up to three months postpartum.37 |
| Specialist in-person interpreting | A specialist interpreter who is available on-site to interpret in all clinical encounters. This interpreter is experienced in working in a medical context with women from a migrant background. | Qualified specialist interpreters present for all antenatal classes.51 A community based doula who spoke the same language as the migrant mother they cared for.47 |
| Group antenatal care | Antenatal care delivered to migrant women alongside other migrant women in a group setting. | A group pregnancy care and information model for migrant mothers.52 A multiagency group antenatal care model involving interpreters, clinicians, and social welfare support workers.55 |
| Continuity of midwifery care | A known midwife or small team of midwives whom the woman can make a relationship with throughout pregnancy. Sometimes this extends to delivery and postpartum. | A known midwife throughout the antenatal care period.38 A dedicated midwife and back-up known midwifery team for antenatal, intrapartum, and postnatal care; this includes 24/7 h telephone support from the main midwife.57 |
| Extended postpartum support | Additional care and visiting in the postpartum period, i.e., care that extends beyond the standard 28 days postpartum. | Postpartum nursing home visiting for 3 months37; postpartum trained peer home visiting for 6 months.48 |
| Birth doulas | A person who supports migrant women through labour, and sometimes also before and after birth. | Bilingual community-based doula39; Somali-speaking doula supporting newly arrived Somali women during birth.58 |
| Postnatal infant feeding support | Postnatal support with infant feeding including breastfeeding, formula, and weaning advice. | Chinese language infant feeding hotline43; support from a lactation professional up to 6 months postpartum.42 |
| Mental health support | Any form of formal psychological support provided to women in the perinatal period, i.e., provision of care by a trained mental health professional. | Psychologists present at a specialist antenatal refugee health clinic.49 |
| (2) Public health or policy interventions | ||
| Social welfare assistance | Support with wider issues relating to the social determinants of health including housing, immigration, social welfare benefits, food banks, and free clothing/baby equipment. | Free baby clothing and equipment51; free food supplements.53 |
| Education materials/classes for mothers | Classes or educational information given to pregnant women or new mothers. | Group antenatal educational classes37; maternal health educational leaflets40; conversation cards and lessons to support conversations with clinicians during birth41; video and discussion session46; maternal and infant oral health education through home visits and telephone calls.56 |
| Free healthcare | No or low-cost access to maternity care for all migrant women. | Expanded access to MEDICAIDb for all migrants, included those who are undocumenteda,59; free antenatal care to undocumented migrants.60,a |
| Immigration law reform | Changes in the immigration system that make it easier (or more difficult) to prosecute or deport undocumented migrants.a | Legal reform to increase police funding for immigration enforcement including prosecutions and deportations of undocumented migrants.63,a |
| Social/peer support | Opportunities to create social networks between migrant women; trained peers working to support other migrant women in the perinatal period, including helping them to navigate a new healthcare system. | Establishing a social network group for migrant women in the perinatal period41; cultural bridging and support with navigating the host country system.54 |
| Staff education/process reform | Education programmes for maternity care staff; reform of the maternity care system in a hospital or regionally. | Training session for midwives on intercultural communication40; reformed data collection system to help tailor care for migrant women.55 |
| Mobile perinatal care van | An outreach healthcare van that travels to areas with high proportions of migrant women to signpost women to maternity healthcare providers and provide support with accessing social and welfare support e.g., food banks, immigration advice. Some may also offer some antenatal or postnatal care check-ups. | A mobile van delivering basic perinatal care and welfare support in neighbourhoods with a high proportion of Latina migrants.50 |
Undocumented migrants: persons who do not fulfil the administrative requirements established by the country of destination to enter, stay, or exercise an economic activity. This includes those who have been unsuccessful in asylum applications, those who have continued their residence in a country after their permit or other means of stay expired, or those who have entered a country irregularly.
MEDICAID: a public insurance program that provides health coverage to low-income individuals in the United States. It is jointly funded by the central government and individual states. Each state operates its own Medicaid program within national guidelines.
As per Cochrane guidance, all outcomes reported in included studies were recorded and categorised. We identified seven main outcome categories: any perinatal outcome, any infant health outcome, breastfeeding outcomes, adequacy of care, care satisfaction/engagement, mental health/wellbeing, and cost-effectiveness. Operational definitions and examples of outcome categories are presented in Table 4.
Table 4.
Operational definitions and examples of outcome categories.
| Outcome category | Operational definition | Examples from included studies |
|---|---|---|
| Perinatal outcomes | Any maternal or neonatal (up to 28 days old) health outcome: rates of miscarriage, stillbirth, small/large for gestational age, preeclampsia, preterm birth, induction of labour, birthweight, postpartum haemorrhage, mode of delivery, Apgara score, critical care admission, maternal/neonatal death. | Apgar scores for newborns39; A composite perinatal mortality/morbidity outcome: stillbirths, neonatal deaths, Apgara score, umbilical arterial pH, admissions to a neonatal intensive care unit >48 h, and NICU admissions for mechanical ventilation40; overall Caesarean section rates.58 |
| Adequacy of care | An assessment of the sufficiency of the maternity care received including gestational age at booking and adherence to national/international maternity care guidelines. | Proportion of women attending 5 or more antenatal care visits57; proportion of women receiving antenatal care before 13 weeks gestation.48 |
| Mental health/wellbeing | Improvement in mental health and wellbeing as measured by a peer-reviewed validated screening tool or clinical interview. | Maternal depression measured using mean EPDSb score37; maternal anxiety measured STAIc score and validated cut-off.41 |
| Breastfeeding outcomes | Any measure of breastfeeding uptake or engagement including breastfeeding initiation and duration, breastfeeding on discharge from birth hospital, exclusive breastfeeding postpartum. | Exclusive breastfeeding at discharge from hospital (feeding at the breast, and/or expressed breast milk)57; exclusive breastfeeding rate at 2 months postpartum43; exclusive breastfeeding continuation at 6 months postpartum.46 |
| Care satisfaction/engagement | Subjective maternal assessment of quality and satisfaction with maternity care received, e.g., through a validated questionnaire; number of antenatal or postnatal appointments attended. | Number of missed clinic appointments51; women’s overall ratings of labour care as measured by a single item question taken from the MFMCQ (Migrant Friendly Maternity Care Questionnaire).47 |
| Infant health outcomes | Any health outcome relating to the infant from 28 days old to 1 year old. | Infant deaths (>27 days old and up to one year)62; infant put to sleep on back48; childhood vaccination status at 1 year old.45 |
| Cost-effectiveness | The degree to which something is effective or useful in relation to its cost, i.e., a measure of how responsibly money is spent to achieve the desired results. | Cost-effectiveness analysis (QALYsd at a willingness-to pay threshold of $100,000)62; saving to the healthcare system.60 |
Apgar score: a standardised tool to describe the condition of the newborn infant immediately after birth.
The Edinburgh Postnatal Depression Scale (EPDS) is a peer-reviewed and validated screening questionnaire to assess for perinatal depression.
State Trait Anxiety Inventory (STAI) is a peer-reviewed and validated screening questionnaire to assess for anxiety (not exclusively used in the peripartum period).
Quality Adjusted Life Year (QALY) is a measure of disease burden, including both the quality and the quantity of life lived.
Amongst all included studies, five intervention groups had the strongest evidence of effectiveness on preterm birth, birthweight, and appointment attendance following the binomial exact calculation. Two were maternity care interventions: specialist multidisciplinary teams and specialist in-person interpreting; and three were public health or policy interventions: social welfare assistance, free healthcare, and education materials/classes for mothers (Table 5). Three other interventions had relatively strong evidence of effectiveness: group antenatal care, mental health support; and continuity of midwifery care (Table 5). When restricting to only interventional studies (n = 4), none showed a greater proportion of positive outcomes than would have been expected by chance (Table 6). None of the included interventions identified were harmful.
Table 5.
Effectiveness of intervention categories across the main outcomes measures (preterm birth, birthweight, and antenatal and postnatal appointment attendance).
| Studies offering an intervention | Beneficial main outcomes/total main outcomes | Proportion of beneficial outcomes (%) | 95% CI of the proportion of beneficial outcomes | p-value |
|---|---|---|---|---|
| (1) Maternity care interventions | ||||
| Specialist multidisciplinary team | 12/12 | 100.0% | 73.5–100.0% | <0.001a |
| Specialist in-person interpreting | 10/11 | 90.9% | 58.7–100.0% | 0.012a |
| Group antenatal care | 7/7 | 100.0% | 59.0–100.0% | 0.016a |
| Mental health support | 7/7 | 100.0% | 59.0–100.0% | 0.016a |
| Continuity of midwifery care | 6/6 | 100.0% | 54.1–100.0% | 0.031a |
| Trained peer/shared culture worker | 2/3 | 66.7% | 9.4–99.2% | 1.000 |
| (2) Public health or policy interventions | ||||
| Social welfare assistance | 13/13 | 100.0% | 75.3%–100.0% | <0.001a |
| Maternal education | 11/11 | 100.0% | 71.5–100.0% | <0.001a |
| Free healthcare | 10/12 | 83.3% | 51.6–97.9% | 0.039a |
| Mobile perinatal care | 3/3 | 100.0% | 29.2–100.0% | 0.25 |
| Immigration law reforms | 1/1 | 100.0% | 2.5%–100.0% | 1.000 |
| Staff education/process reform | 1/1 | 100.0% | 2.5%–100.0% | 1.000 |
| Social/peer support | 0/1 | 0.0% | 0.0%–97.5% | 1.000 |
CI: Confidence Interval.
Significant at p < 0.05 level.
Table 6.
Effectiveness of intervention categories across the main outcomes measures (preterm birth, birthweight, and antenatal and postnatal appointment attendance) restricting to only interventional studies.
| Intervention | Beneficial outcomes/total outcomes | Proportion of beneficial outcomes (%) | 95% CI of the proportion of beneficial outcomes | p-value |
|---|---|---|---|---|
| (1) Maternity care interventions | ||||
| Specialist multidisciplinary team | 1/1 | 100.0% | 2.5%–100.0% | 1.000 |
| Specialist in-person interpreting | 3/4 | 75.0% | 19.4–99.4% | 0.625 |
| Group antenatal care | 2/2 | 100.0% | 15.8–100.0% | 0.500 |
| Mental health support | N/A | N/A | N/A | N/A |
| Continuity of midwifery care | 2/2 | 100.0% | 15.8–100.0% | 0.500 |
| Trained peer/shared culture worker | 0/1 | 0.0% | 0.0%–97.5% | 1.000 |
| (2) Public health or policy interventions | ||||
| Social welfare assistance | N/A | N/A | N/A | N/A |
| Free healthcare | N/A | N/A | N/A | N/A |
| Maternal education | 2/2 | 100.0% | 15.8–100.0% | 0.500 |
| Mobile perinatal care | N/A | N/A | N/A | N/A |
| Immigration law reforms | N/A | N/A | N/A | N/A |
| Staff education/process reform | N/A | N/A | N/A | N/A |
| Social/peer support | 1/1 | 100.0% | 2.5%–100.0% | 1.000 |
CI: Confidence Interval.
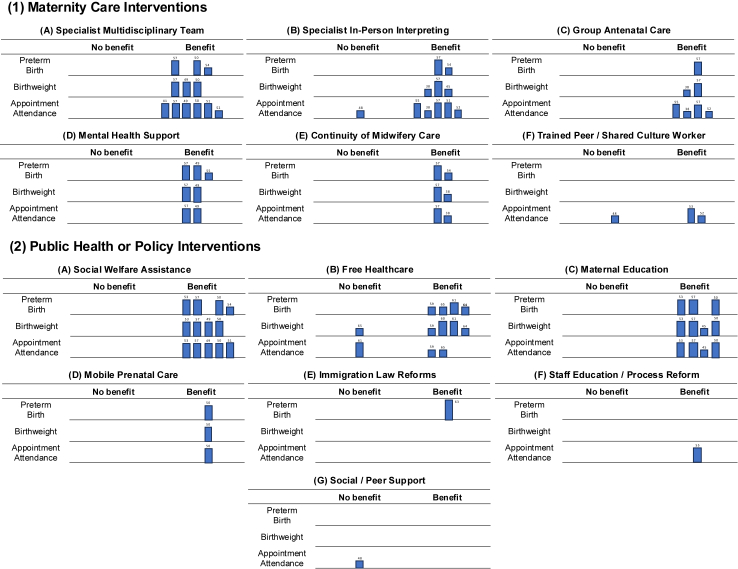
Binomial exact calculations for any outcomes are presented in Appendix 4. Three interventions showed evidence of benefit for any reported outcome measure, namely, specialist in-person interpreting, trained peer/shared culture worker, and free healthcare. When restricting to only interventional studies (n = 12), none showed a greater proportion of beneficial outcomes than would be expected by chance (Appendix 5), Fig. 2 presents the data for the main outcomes of interest: preterm birth, birthweight, and appointment attendance amongst all included studies. Appendix 6 presents the data for the main outcomes of interest for interventional studies only. Data for all outcomes from all included studies is presented in Appendix 7. Appendix 8 presents the data for all outcomes for interventional studies only. A full narrative synthesis of the findings for all interventions is presented in Appendix 9.
Fig. 2.
Evidence for effectiveness of (1) Maternity Care Interventions and (2) Public Health or Policy Interventions for migrant women by main outcome category – preterm birth, birthweight, appointment attendance. This harvest plot is a ‘supermatrix’ presenting thirteen interventions, and three outcomes. Each bar represents a single study and is annotated with the reference number. Bar height indicates study quality: strong (tallest), moderate (medium), weak (shortest). Preterm birth was defined as infants born alive before 37 weeks of pregnancy are completed. Birthweight was defined as the body weight of an infant at birth. Appointment attendance was defined as the number of antenatal and/or postnatal appointments a woman attended.
Most studies identified in this review (75.9%) were multicomponent, meaning various interventions were delivered as part of one programme. The most common intervention was specialist in-person interpreting which was defined as a specialist interpreter experienced in working in a medical context with women from a migrant background and available on-site to interpret in clinical encounters. This approach demonstrated strong evidence of improvement in the main outcomes of interest. Multidisciplinary teams also showed strong evidence of benefit and typically included midwives, physicians, social workers, interpreters, and psychologists. All offered antenatal care, and approximately half continued into the postnatal period. Seven studies embedded social welfare assistance into their clinical care, and in all cases there was very strong evidence of improvement in the main outcomes of interest. Examples of social welfare support included offering free baby clothing and supplies, free healthy food for mothers and infants, or providing referrals to social welfare services such as housing and employment support. Maternal education programmes were very common, and our findings suggest they improved the main outcomes. Examples included participation in a national programme aimed to educate mothers on healthy nutrition; exercise education and support; and education on birth and infant care. Finally, there was strong evidence that free maternity healthcare improved the main outcomes of interest and was cost-saving to national and regional healthcare systems. One was an economic model assessing the impact of including undocumented migrants in national free antenatal care programmes in Europe, and four explored the impact of expansion of free prenatal care (MEDICAID) for low-income women in the US.
Sensitivity analysis was carried out by restricting the binomial tests to strong and moderate quality studies only (n = 11 studies). This found that specialist multidisciplinary teams, mental health support, social welfare assistance, and maternal education showed a greater proportion of positive outcomes than would have been expected by chance (Appendix 10). When restricting the analysis to studies that involved service users in the design or delivery of the intervention, none showed a greater proportion of positive outcomes than would have been expected by chance (Appendix 10). Sensitivity analyses were also conducted for all outcomes (Appendix 1).
Discussion
We identified 29 studies comprising interventions which aimed to improve maternity care for migrant women in HICs. Most studies were multi-component interventions, approximately 40% of studies were interventional, and almost two thirds of studies were of weak quality. Clinical interventions with the strongest evidence of benefit on birthweight, preterm birth rates, and perinatal appointment attendance were specialist multidisciplinary teams and specialist in-person interpreting. There is also good evidence to suggest group antenatal care, mental health support, and continuity of midwifery care can improve outcomes for migrant women. Policy and public health interventions with the strongest evidence of benefit were social welfare assistance, free healthcare, and maternal education. Although only seven studies assessed social welfare support, there was very strong evidence of this improving perinatal outcomes amongst migrant women and their infants. Approximately half of studies involved migrant women in intervention design or delivery, and only a third co-designed interventions from the outset with migrant women. A sensitivity analysis including only studies who involved service users in the design or delivery of the intervention found no greater proportion of positive outcomes than would have been expected by chance, but this finding is limited by the lack of studies available.
Only four studies (14%) assessed mental health support despite data to suggest migrant women are at significantly higher risk of perinatal mental illness when compared to host populations.8 The postnatal period is increasingly recognised as an important time for maternal and infant support, but only four studies (14%) explored interventions during this time.66 Economic analyses are key to political decision-making on healthcare interventions, but just two (7%) studies included a cost-effectiveness analysis.59,67 One was an economic model assessing the impact of including undocumented migrants in national free antenatal care programmes in three European countries.59 The model demonstrated that providing free access to antenatal care services to undocumented migrants would be cost saving in Germany, Greece and Sweden. Another explored the expansion of free antenatal care programmes to undocumented migrants in the US.64 It demonstrated that centrally-funded free antenatal care was cost-effective and increased uptake of antenatal care appointments. No studies focused specifically on maternal health indicators e.g., maternal mortality, intensive care admission, preeclampsia, anaemia, or intrapartum blood loss. This represents a significant gap in evidence and should be the focus of future studies.
There are few systematic reviews in this area. Balaam et al. conducted a systematic review in 2020 which aimed to identify perinatal social support interventions for women and new mothers in Europe.16 Sixteen studies were included and findings were qualitatively synthesised; women valued community-based holistic peer support interventions. We identified four quantitatively assessed interventions offering peer support and found weak evidence of their effectiveness, but this finding was limited by a lack of eligible studies. The NIHR commissioned a systematic review to explore interventions to improve maternity care for migrant women in the UK in 2017.24 The review only included UK studies and identified four interventions. Two included peer support but none were robustly evaluated, making it difficult to draw conclusions on their effectiveness. We have expanded the literature to look across HICs and have identified strong evidence of benefit for several interventions. We have also systematically assessed the involvement of service users in interventions development. Rogers et al. completed a scoping review of models of maternity and postpartum care in HICs in 2019 and identified 17 studies.17 Of these, just six had quantitative outcomes and were primarily from the US and of weak or moderate quality, and did not address the wider determinants of health. Following a more extensive search of the literature, we have identified significantly more studies with quantitative outcomes and also identified policy and public health interventions which could improve outcomes for migrant women in HICs.
The strengths of this review include rigorous methodology in accordance with the Cochrane Handbook of Systematic Reviews. Unlike most previous reviews, we included interventions addressing wider determinants of health including public health and policy interventions. We have demonstrated that there is a growing body of evidence from across HICs, recognising that two thirds of included studies were published since 2015. Unlike previous reviews, we narrowed our eligibility criteria to only include studies where greater than ninety percent of participants were first generation migrants, i.e., not born in the host country. This ensures our findings are directly relevant to the migrant women who often face the biggest challenges in accessing maternity care.4 We searched databases and the grey literature and had no language or date restrictions. Service users were involved throughout including in conception, analysis, and interpretation which ensures our findings are directly relevant to migrant women.
The findings are limited by the lack of high-quality interventional evidence available; approximately half of the studies were retrospective, and only 14% (n = 4) were RCTs. Owing to heterogenous outcome measures we were unable to assess publication bias formally. However, the inclusion of grey literature may have reduced this bias, as negative outcomes are less likely to be published in academic publications. In addition, several included studies report no benefit suggesting publication bias may be minimal. Over half of included studies did not involve service users in intervention design or delivery, meaning it was difficult to formally assess the effectiveness of involving service users in this process. Additionally, studies often included mixed populations of migrants including economic migrants, refugees, asylum seekers, and undocumented migrants, which makes it difficult to determine the impact on these heterogenous groups.68 In terms of quality, 59% (n = 17) of included studies were of weak quality, 31% (n = 9) moderate, and only 10% (n = 3) strong. The quality assessment tool used has been shown to have good inter-rater agreement, but may score studies higher than other tools.69 Almost half of the studies identified were from the US and predominantly conducted amongst Latina migrants which limits the generalisability of the findings. Thus, the findings should be interpreted with caution and the impact of the country of implementation as well as the background of the migrant women involved should be considered. Both are key mediators of effectiveness, particularly with the complex interventions we identified. We only included quantitative studies which limits our understanding of why interventions were successful or not, and their acceptability to participants. The use of vote counting based on raw numbers to assess benefit should be interpreted with caution as a small numerical benefit in an outcome may have little clinical significance.
Given that most included studies were of poor quality and that sensitivity analysis restricting to interventional studies only did not demonstrate any effect on the main outcomes of interest, we have chosen not to present conclusions. Only half of studies involved service users in intervention design or planning, despite increasing evidence to suggest that interventions created with or involving service users are more effective and more acceptable to patients.70 Overall, there is a need for further research exploring the effectiveness of public health and policy interventions in this field, as well as the effectiveness of interventions offering extended postpartum care, infant feeding support, mental health support, and doula services. The evaluation of all interventions should include an assessment of the impact on maternal mental and physical health. All efforts to improve care and public health or policy interventions must place migrant women at the centre of planning, delivery, and evaluation to ensure evidence is effectively translated into practice.
Contributors
KS, SE, KO, MA, RA, GF, WH, SL, RA, MK, FS contributed to the conception of the review. KS, SE, KO, MA, RA, GF, WH, SL, RA, MK, FS contributed to the methods. KS, SE, GF, KO, MA, RA, NSC, HRJ, MM, MMC contributed to the data curation and verification. KS and RA contributed to the statistical analysis. RA, MK, FS, SL provided supervision. All authors contributed to the data interpretation and review and editing. All authors had full access to all the data in the study and had final responsibility for the decision to submit for publication.
Data sharing statement
All data relating to this publication, including full search strategies, will be made publicly available in the appendices on publication and can be used without permission from the authors.
Declaration of interests
SL is a fellow of Pathway, a UK charity which provides and advocates for health interventions for inclusion health populations, including migrants. The authors declared no conflicts of interest.
Acknowledgements
We would like to thank the women who are part of our wider Expert by Experience (Service User) Panel who helped shape, inform, and interpret the findings of this review.
Footnotes
Supplementary data related to this article can be found at https://doi.org/10.1016/j.eclinm.2024.102938.
Appendix A. Supplementary data
References
- 1.International Organization for Migration World migration report 2022. https://www.iom.int/wmr/interactive
- 2.Batalova J., Batalova J. 2020. Immigrant women and girls in the United States.https://www.migrationpolicy.org/article/immigrant-women-and-girls-united-states 2020-03-03. [Google Scholar]
- 3.Office for National Statistics Births by parents' country of birth, England and Wales. ONS. https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/livebirths/bulletins/parentscountryofbirthenglandandwales/2019
- 4.Haith-Cooper M., Bradshaw G. Meeting the health and social care needs of pregnant asylum seekers; midwifery students' perspectives: Part 3; “The pregnant woman within the global context”; an inclusive model for midwifery education to address the needs of asylum. Nurse Educ Today. 2013;33(9):1045–1050. doi: 10.1016/j.nedt.2012.04.016. [DOI] [PubMed] [Google Scholar]
- 5.Fair F., Raben L., Watson H., Vivilaki V., Muijsenbergh Mvd, Soltani H. Migrant women's experiences of pregnancy, childbirth and maternity care in European countries: a systematic review. PLoS One. 2020;15(2) doi: 10.1371/journal.pone.0228378. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Almeida L.M., Caldas J., Ayres-De-Campos D., Salcedo-Barrientos D., Dias S. Maternal healthcare in migrants: a systematic review. Review. Matern Child Health J. 2013;17(8):1346–1354. doi: 10.1007/s10995-012-1149-x. [DOI] [PubMed] [Google Scholar]
- 7.World Health Organization Regional Office for Europe . 2018. Improving the health care of pregnant refugee and migrant women and newborn children.https://www.euro.who.int/__data/assets/pdf_file/0003/388362/tc-mother-eng.pdf [Google Scholar]
- 8.Stevenson K., Fellmeth G., Edwards S., et al. The global burden of perinatal common mental health disorders and substance use among migrant women: a systematic review and meta-analysis. Lancet Public Health. 2023 Mar 2023;8(3):e203–e216. doi: 10.1016/S2468-2667(22)00342-5. [DOI] [PubMed] [Google Scholar]
- 9.Heslehurst N., Brown H., Pemu A., Coleman H., Rankin J. Perinatal health outcomes and care among asylum seekers and refugees: a systematic review of systematic reviews. Article. BMC Med. 2018;16(1):89. doi: 10.1186/s12916-018-1064-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.David M., Pachaly J., Vetter K. Perinatal outcome in Berlin (Germany) among immigrants from Turkey. Arch Gynecol Obstet. 2006;274(5):271–278. doi: 10.1007/s00404-006-0182-7. [DOI] [PubMed] [Google Scholar]
- 11.Gagnon A.J., Zimbeck M., Zeitlin J., et al. Migration to western industrialised countries and perinatal health: a systematic review. Soc Sci Med. 2009;69(6):934–946. doi: 10.1016/j.socscimed.2009.06.027. [DOI] [PubMed] [Google Scholar]
- 12.Väisänen H., Remes H., Martikainenc P. Perinatal health among migrant women: a longitudinal register study in Finland 2000-17. SSM Popul Health. 2022;20 doi: 10.1016/j.ssmph.2022.101298. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Eslier M., Azria E., Chatzistergiou K., Stewart Z., Dechartres A., Deneux-Tharaux C. Association between migration and severe maternal outcomes in high-income countries: systematic review and meta-analysis. PLoS Med. 2023;20(6) doi: 10.1371/journal.pmed.1004257. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.David M., Borde T., Brenne S., et al. Obstetric care quality indicators and outcomes based on the degree of acculturation of immigrants-results from a cross-sectional study in Berlin. Arch Gynecol Obstet. 2018;297(2):313–322. doi: 10.1007/s00404-017-4574-7. [DOI] [PubMed] [Google Scholar]
- 15.Barker D.J.P. Developmental origins of chronic disease. Article. Publ Health. 2012;126(3):185–189. doi: 10.1016/j.puhe.2011.11.014. [DOI] [PubMed] [Google Scholar]
- 16.Balaam M.-C., Kingdon C., Haith-Cooper M. A systematic review of perinatal social support interventions for asylum-seeking and refugee women residing in Europe. ReviewPaper. J Immigr Minority Health. 2021-07-17 2021;24(3):741–758. doi: 10.1007/s10903-021-01242-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Rogers H.J., Hogan L., Coates D., Homer C.S.E., Henry A. Responding to the health needs of women from migrant and refugee backgrounds-Models of maternity and postpartum care in high-income countries: a systematic scoping review. Health Soc Care Community. 2020;28(5):1343–1365. doi: 10.1111/hsc.12950. [DOI] [PubMed] [Google Scholar]
- 18.Shaw D., Guise J., Shah N., et al. Drivers of maternity care in high-income countries: can health systems support woman-centred care? Lancet. 2016;388(10057):2282–2295. doi: 10.1016/S0140-6736(16)31527-6. [DOI] [PubMed] [Google Scholar]
- 19.Yeo S., Park Y., McClelland E., et al. A scoping review of maternal health among resettled refugee women in the United States. Front Public Health. 2023;11 doi: 10.3389/fpubh.2023.1157098. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Tarraf W., Jensen G., Li Y., Toseef M., Mahmoudi E., Gonzalez H. Changes in insurance coverage and healthcare use among immigrants and US-born adults following the affordable care act. J Racial Ethn Health Disparities. 2021;8(3):363–374. doi: 10.1007/s40615-020-00790-y. [DOI] [PubMed] [Google Scholar]
- 21.Maternity Action NHS Charging and how pregnant women are affected. https://maternityaction.org.uk/campaigns/nhscharging/campaign-toolkit-2/about-nhs-charging-and-how-pregnant-women-are-affected/
- 22.Department of Health & Social Care NHS cost recovery - overseas visitors: guidance for NHS service providers on charging overseas visitors in England. DHSC. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1186860/nhs-cost-recovery-overseas-visitors_september2023.pdf
- 23.Pařízková A., Clausen J.A., Balaam M.-C., et al. Inclusiveness of access policies to maternity care for migrant women across Europe: a policy review. Matern Child Health J. 2023;28(3):470–480. doi: 10.1007/s10995-023-03785-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Higginbottom G.M.A., Evans C., Hussain B., Morgan M., Bharj K.K., Eldridge J. Experience of and access to maternity care in the UK by immigrant women: a narrative synthesis systematic review. BMJ Open. 2019;9(12) doi: 10.1136/bmjopen-2019-029478. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Tunçalp Ӧ., Were W., MacLennan C., et al. Quality of care for pregnant women and newborns-the WHO vision. BJOG An Int J Obstet Gynaecol. 2015;122(8):1045–1049. doi: 10.1111/1471-0528.13451. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Stevenson K., Ogunlana K., Edwards S., et al. Interventions to improve perinatal outcomes among migrant women in high-income countries: a systematic review protocol. BMJ Open. 2023;13(8) doi: 10.1136/bmjopen-2023-072090. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.The World Bank World Bank Country and Lending Groups. https://datahelpdesk.worldbank.org/knowledgebase/articles/906519
- 28.NHS Consent to treatment - children and young people. @nhsuk. https://www.nhs.uk/conditions/consent-to-treatment/children/ Updated 20 Oct 201.
- 29.Cochrane Collaboration Training . Cochrane Handbook for Systematic Reviews of Interventions. 2023. Assessing risk of bias in a non-randomized study. chap 25. [Google Scholar]
- 30.EndNote. Version 20. Clarivate; 2013. [Google Scholar]
- 31.Covidence systematic review software. Veritas Health Innovation; 2021. [Google Scholar]
- 32.Effective Public Healthcare Panacea Project Quality Assessment Tool for Quantitative Studies. https://www.ephpp.ca/quality-assessment-tool-for-quantitative-studies/
- 33.Sterne J., Hernán M., Reeves B., et al. ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ. 2016;355 doi: 10.1136/bmj.i4919. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Cochrane Collaboration Training . 2022. Cochrane Handbook for Systematic Reviews of Interventions. [Google Scholar]
- 35.RStudio. 2020. http://www.rstudio.com/ [Google Scholar]
- 36.Bang K.S., Huh B.Y., Kwon M.K. The effect of a postpartum nursing intervention program for immigrant mothers. Child Health Nurs Res. 2014;20(1):11–19. [Google Scholar]
- 37.Ahrne M., Byrskog U., Essén B., Andersson E., Small R., E S. 2023. Group antenatal care compared with standard antenatal care for Somali-Swedish women: a historically controlled evaluation of the Hooyo Project. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Byrskog U., Small R., Schytt E. Community-based bilingual doulas for migrant women in labour and birth - findings from a Swedish register-based cohort study. BMC Pregnancy Childbirth. 2020;20(1):721. doi: 10.1186/s12884-020-03412-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Damsted Rasmussen T., Villadsen S., Hansen A., et al. Effectiveness evaluation of an antenatal care intervention addressing disparities to improve perinatal outcomes in Denmark: a nationwide register-based analysis of a cluster randomized controlled trial (MAMAACT) BJOG An Int J Obstet Gynaecol. 2023 doi: 10.1111/1471-0528.17404. [DOI] [PubMed] [Google Scholar]
- 40.Jin Q., Mori E., Sakajo A. Nursing intervention for preventing postpartum depressive symptoms among Chinese women in Japan. Jpn J Nurs Sci. 2020;17(4) doi: 10.1111/jjns.12336. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Linares A.M., Cartagena D., Rayens M.K. Las dos cosas versus exclusive breastfeeding: a culturally and linguistically exploratory intervention study in hispanic mothers living in Kentucky. J Pediatr Health Care. 2019;33(6):e46–e56. doi: 10.1016/j.pedhc.2019.07.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Janssen P.A., Livingstone V.H., Chang B., Klein M.C. Development and evaluation of a Chinese-language newborn feeding hotline: a prospective cohort study. BMC Pregnancy Childbirth. 2009;9:3. doi: 10.1186/1471-2393-9-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Kieffer E., Caldwell C., Welmerink D., Welch K., Sinco B., Guzmán J. Effect of the healthy MOMs lifestyle intervention on reducing depressive symptoms among pregnant Latinas. Am J Community Psychol. 2013;51(1–2) doi: 10.1007/s10464-012-9523-9. [DOI] [PubMed] [Google Scholar]
- 44.McEnery G., Rao K.P.S. The effectiveness of antenatal education of Pakistani and Indian women living in this country. Child Care Health Dev. 1986;12(6):385–399. doi: 10.1111/j.1365-2214.1986.tb00516.x. [DOI] [PubMed] [Google Scholar]
- 45.Rossiter J.C. The effect of a culture-specific education program to promote breastfeeding among Vietnamese women in Sydney. Int J Nurs Stud. 1994;31(4):369–379. doi: 10.1016/0020-7489(94)90077-9. [DOI] [PubMed] [Google Scholar]
- 46.Schytt E., Wahlberg A., Eltayb A., Tsekhmestruk N., Small R., Lindgren H. Community-based bilingual doula support during labour and birth to improve migrant women's intrapartum care experiences and emotional well-being-Findings from a randomised controlled trial in Stockholm, Sweden [ NCT03461640] PLoS One. 2022;17(11) doi: 10.1371/journal.pone.0277533. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Lutenbacher M., Elkins T., Dietrich M.S., Riggs A. The efficacy of using peer mentors to improve maternal and infant health outcomes in hispanic families: findings from a randomized clinical trial. Matern Child Health J. 2018;22(Suppl 1):92–104. doi: 10.1007/s10995-018-2532-z. https://www.ncbi.nlm.nih.gov/pubmed/30136069 Erratum in: Matern Child Health J. 2018 Aug 22;:; PMID: 30136069. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Malebranche M., Norrie E., Hao S., et al. Antenatal care utilization and obstetric and newborn outcomes among pregnant refugees attending a specialized refugee clinic. J Immigr Minor Health. 2020;22(3):467–475. doi: 10.1007/s10903-019-00961-y. [DOI] [PubMed] [Google Scholar]
- 49.O'Connell E., Zhang G., Leguen F., Prince J. Impact of a mobile van on prenatal care utilization and birth outcomes in Miami-Dade County. Matern Child Health J. 2010;14(4):528–534. doi: 10.1007/s10995-009-0496-8. [DOI] [PubMed] [Google Scholar]
- 50.Reavy K., Hobbs J., Hereford M., Crosby K. A new clinic model for refugee health care: adaptation of cultural safety. Rural Rem Health. 2012;12:1826. [PubMed] [Google Scholar]
- 51.Riggs E., Yelland J., Szwarc J., Muyeen S., Dawson W., Brown S. Improving access, equty and health literacy: group pregnancy care and information for refugee background women. J Paediatr Child Health. 2017;53(2):116. [Google Scholar]
- 52.Sana H. Birth outcomes of immigrant and native-born Hispanic women: role of prenatal care utilization and participation in the Women, Infants and Children (WIC) program. Diss Abstr Int B Sci Eng. 2016;77 (2-B(E)):No-Specified. [Google Scholar]
- 53.Stapleton H., Murphy R., Correa-Velez I., Steel M., Kildea S. Women from refugee backgrounds and their experiences of attending a specialist antenatal clinic. Narratives from an Australian setting. Women Birth. 2013;26(4):260–266. doi: 10.1016/j.wombi.2013.07.004. [DOI] [PubMed] [Google Scholar]
- 54.Yelland J., Mensah F., Riggs E., et al. Evaluation of systems reform in public hospitals, Victoria, Australia, to improve access to antenatal care for women of refugee background: an interrupted time series design. PLoS Med. 2020;17(7) doi: 10.1371/journal.pmed.1003089. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Yuan S. Evaluating an oral health education intervention in Chinese undocumented migrant mothers of infants in Northern Ireland. Dent J. 2019;7(1):8. doi: 10.3390/dj7010008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Dube M., Gao Y., Steel M., Bromley A., Ireland S., Kildea S. Effect of an Australian community-based caseload midwifery group practice service on maternal and neonatal outcomes for women from a refugee background. Women Birth. 2022;36(3):e353–e360. doi: 10.1016/j.wombi.2022.10.004. [DOI] [PubMed] [Google Scholar]
- 57.Dundek L.H. Establishment of a Somali doula program at a large metropolitan hospital. J Perinat Neonatal Nurs. 2006;20(2):128–137. doi: 10.1097/00005237-200604000-00006. [DOI] [PubMed] [Google Scholar]
- 58.Drewry J., Sen B., Wingate M., Bronstein J., Foster E., Kotelchuck M. The impact of the State Children’s Health Insurance Program’s unborn child ruling expansions on foreign-born Latina prenatal care and birth outcomes, 2000-2007. Matern Child Health J. 2015;19(7):1464–1471. doi: 10.1007/s10995-014-1650-5. [DOI] [PubMed] [Google Scholar]
- 59.European Union Agency for Fundamental Rights . The case of migrants in an irregular situation. 2015. Cost of exclusion from healthcare.https://www.europarl.europa.eu/cmsdata/226730/Session_1_-_FRA_Cost_of_exclusion_from_healthcare.pdf [Google Scholar]
- 60.Korenbrot C.C., Dudley R.A., Greene J.D. Changes in births to foreign-born women after welfare and immigration policy reforms in California. Matern Child Health J. 2000;4(4):241–250. doi: 10.1023/a:1026695605457. [DOI] [PubMed] [Google Scholar]
- 61.Rodriguez M.I., Swartz J.J., Lawrence D., Caughey A.B. Extending delivery coverage to include prenatal care for low-income, immigrant women is a cost-effective strategy. Wom Health Issues. 2020;30(4):240–247. doi: 10.1016/j.whi.2020.02.004. [DOI] [PubMed] [Google Scholar]
- 62.Stanhope K.K., Suglia S.F., Hogue C.J.R., Leon J.S., Comeau D.L., Kramer M.R. Spatial variation in very preterm birth to hispanic women across the United States: the role of intensified immigration enforcement. Ethn Dis. 2021;31(1):333–344. doi: 10.18865/ed.31.S1.333. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Welder E., Powers J., Walter A.C., Bedell D., Shen W.W. Providing prenatal care for patients with limited medical insurance coverage. J Community Health. 2022;47(6):974–980. doi: 10.1007/s10900-022-01133-0. [DOI] [PubMed] [Google Scholar]
- 64.Wherry L.R., Fabi R., Schickedanz A., Saloner B. State and federal coverage for pregnant immigrants: prenatal care increased, No change detected for infant health. Health Affairs. 2017;36(4):607–615. doi: 10.1377/hlthaff.2016.1198. [DOI] [PubMed] [Google Scholar]
- 65.Yuan S.-Y., Freeman R. Can social support in the guise of an oral health education intervention promote mother-infant bonding in Chinese immigrant mothers and their infants? Health Educ J. 2011;70(1):57–66. doi: 10.1177/0017896910366186. [DOI] [Google Scholar]
- 66.Finlayson K., Crossland N., Bonet M., Downe S. What matters to women in the postnatal period: a meta-synthesis of qualitative studies. PLoS One. 2020;15(4) doi: 10.1371/journal.pone.0231415. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Hoomans T., Severens J.L. Economic evaluation of implementation strategies in health care. EditorialNotes. Implement Sci. 2014;9(1):1–6. doi: 10.1186/s13012-014-0168-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Royal College of Obstetricians & Gynaecologists . 2022. Equitable access to maternity care for refugee, asylum seeking and undocumented migrant women.https://www.rcog.org.uk/about-us/campaigning-and-opinions/position-statements/position-statement-equitable-access-to-maternity-care-for-refugee-asylum-seeking-and-undocumented-migrant-women/ [Google Scholar]
- 69.Armijo-Olivo S., Stiles C., Hagen N., Biondo P., Cummings G. Assessment of study quality for systematic reviews: a comparison of the Cochrane collaboration risk of bias tool and the effective public health practice project quality assessment tool: methodological research. J Eval Clin Pract. 2012;18(1):12–18. doi: 10.1111/j.1365-2753.2010.01516.x. [DOI] [PubMed] [Google Scholar]
- 70.Bombard Y., Baker G.R., Orlando E., et al. Engaging patients to improve quality of care: a systematic review. Implement Sci. 2018;13(1):1–22. doi: 10.1186/s13012-018-0784-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.