Abstract
Background
As Point-of-Care Ultrasound (POCUS) education is increasingly incorporated in undergraduate medical education (UME), evaluation of the effectiveness of various ultrasound-related curricula is a developing field. The Extended Focused Assessment with Sonography (EFAST) is a POCUS exam widely used in emergency medicine. This project examines third-year osteopathic medical (OMS III) students’ perceptions of the impact of a focused introduction to EFAST training curriculum on their performance ability and utilization of EFAST during third-year clinical rotations. Furthermore, we assessed student perceptions of barriers to the use of POCUS during third-year clinical rotations.
Methods
The introduction to EFAST curriculum was developed using competency-based backward design and was delivered in July 2022 to incoming OMS III students. The curriculum involved didactics, hands-on ultrasound practice with standardized patients, and a comprehensive OSCE assessment, where students performed the EFAST exam. In July/August 2023, curriculum participants were anonymously surveyed regarding the effectiveness of the EFAST curriculum and perceived barriers to EFAST and POCUS utilization during their third-year clerkships. Descriptive and thematic analyses were performed on quantitative and qualitative data.
Results
Twenty-one of 69 (30.4%) participants responded to the survey, with 17 (24.6%) participants completing the entire survey. Respondents reported increased knowledge and confidence in performing and interpreting EFAST, with 82.4% indicating increased likelihood of performing EFAST and POCUS in general. 76.4% performed EFAST at least once during third-year clerkships, with 11.8% performing it 15 times or more. Students reported valuing the safe simulated learning environment of the EFAST training, and identified lack of patients with indications for EFAST, time constraints, lack of ultrasound machine availability and clinician comfort level as barriers to EFAST utilization.
Conclusions
This study presents the implementation of a focused EFAST curriculum developed through competency-based deliberate backward design based on professional guidelines and the anticipated educational needs of our institution and community. Student perceptions provided valuable insight into access and barriers to EFAST and POCUS use in subsequent clinical clerkships, indicating student perception of POCUS curriculum effectiveness may provide insight to continual curriculum improvement.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12909-024-06513-9.
Keywords: Point-of-care ultrasound, Undergraduate medical education, Extended focused assessment with sonography for trauma, Curriculum design
Background
The importance of proficiency in the clinical use of point-of-care ultrasound (POCUS) by physicians in many specialties has become increasingly recognized [1]. As a focused ultrasound exam performed at the patient’s bedside by the treating clinician, POCUS provides immediate diagnostic information, allowing clinicians to make timely decisions regarding patient care [2]. POCUS education is being incorporated into undergraduate medical education (UME), but with great variation between the curricula implemented by different medical schools [2–4]. The study of effectiveness of different content and formats of ultrasound-related curriculum in UME is a developing field [5, 6].
Studies have indicated participation in focused POCUS training sessions increases medical students’ performance on ultrasound skills assessments and increases their confidence in their ability to perform ultrasound. While many of these studies have assessed these outcomes directly upon completion of the POCUS training [7], fewer studies have examined medical students’ perception of the impact of POCUS training on their subsequent utilization of POCUS exams within later clinical experiences during UME. Faculty perception of barriers to incorporating ultrasound into UME have been assessed, and found to include lack of trained faculty, lack of available time in the curriculum, lack of financial support, and lack of appropriate equipment [4, 5]. However, medical students’ perspective of barriers to their ability to utilize POCUS within UME after focused training has been less studied, and assessment of these student perceptions may provide valuable information to improving curriculum design and resource allocation. Thus, further study is needed regarding the effectiveness of training on increased POCUS utilization and assessment of barriers to utilization of POCUS by medical students in clinical settings.
The Extended Focused Assessment with Sonography (EFAST) is a type of POCUS exam used in the evaluation and treatment of trauma patients and other critically ill patients in the emergent setting [8]. The EFAST allows for rapid bedside assessment of multiple pathologies, including evaluation of intraperitoneal free fluid, pericardial effusion, hemothorax, and pneumothorax. Review of the literature shows that EFAST training is included in some UME curricula, and studies have shown that training in the EFAST results in increased confidence in performing and interpreting the examination’s results in various populations of health care workers [9, 10], including third and final year medical students [11, 12]. Additionally there is some evidence that focused training of health care workers in EFAST and other POCUS exams results in increased subsequent utilization [13, 14], but similar studies for medical students are lacking.
The primary aim of this study was to examine third year medical students’ perceptions of their confidence and readiness to conduct POCUS, specifically the EFAST exam, during clinical rotations, after completion of a two-week EFAST training program. The secondary aims were to: (1) assess students’ opportunity to observe or perform POCUS exams including EFAST, and (2) elicit students’ perceptions of barriers to student use of ultrasound exams during clinical rotations.
Methods
Study design and participants
This study used an observational mixed methods approach using an electronic survey for data collection. Study participants were Sam Houston State University College of Osteopathic Medicine (SHSU COM) third-year osteopathic medical students (OMS III students) who completed a 2-week introduction to EFAST curriculum at the beginning of their third-year as part of a required Clinical Clerkship Preparation (CCP) course in July 2022. Upon completion of the CCP course, the students began third-year core clerkships, which consisted of Emergency Medicine, Family Medicine, Inpatient/Adult Medicine, General Surgery, Pediatrics, Psychiatry, Rural & Underserved, and Women’s Health clerkships. Students were distributed amongst five SHSU COM sites during third-year clerkships, in Beaumont/Port Arthur, Conroe/Huntsville, Downtown Houston, Fort Bend, and Piney Woods (Nacogdoches/Lufkin), Texas. In July and August of 2023, after completion of their third-year clerkships, curriculum participants were anonymously surveyed regarding the EFAST curriculum they completed prior to the start of their third year, in August of 2022, and their utilization of POCUS during their third-year clerkships.
Development of the “Introduction to EFAST” curriculum using backward design
The first step in the design of the introduction to EFAST curriculum was the development of EFAST competencies for SHSU COM OMS III students upon completion of the CCP course (Table 1). These competencies were developed through review of professional society guidelines [15–17], followed by assessment of the educational needs of our particular institution. The developed competencies were mapped to SHSU COM Program Level Educational Elements, which are based on the seven American Association of Colleges of Osteopathic Medicine Osteopathic Core Competencies: Osteopathic Principles and Practice, Medical Knowledge, Patient Care, Interpersonal and Communication Skills, Professionalism, Practice-Based Learning and Improvement, and Systems-Based Practice. Once the competencies were established, they were then used to develop the EFAST curriculum using backward design [18]. In the four-step backward design process, the first step is to designate and characterize competencies that trainees must acquire, which was done as described above. Based on these competency statements, the second step was to establish specific learning objectives for the curriculum. Third, assessments were then designed to align with those objectives, and fourth, educational activities were then planned in accordance with the developed assessments.
Table 1.
EFAST competencies
| EFAST Competencies Developed for SHSU COM Clinical Clerkship Preparation OMS-III Students | |
|---|---|
|
• Describe indications, benefits, and limitations of EFAST in clinical care of patients (Patient Care) • Identify ultrasonographic findings of anatomic landmarks key to evaluating patients for free fluid in the abdomen, pleural space, and pericardium, and for pneumothorax (Application of Medical Knowledge) • Demonstrate the ability to communicate with patients about what the EFAST exam involves and demonstrate the ability to communicate the results of EFAST to the treatment team (Interpersonal and Communication Skills) • Demonstrate respectfulness of patients’ comfort and privacy during the ultrasound exam (Professionalism) • Perform self-assessment of EFAST exam performance and identify resources that will assist in performance improvement (Practice-Based Learning and Improvement) • Demonstrate the understanding that EFAST is a limited focused exam that together with history and physical exam aids in diagnosis, and that appropriate use of EFAST can expedite medical care (Systems-Based Practice) |
Assessment
Assessment consisted of a combination of an Observed Structured Clinical Exam (OSCE) and multiple choice questions (MCQs) included on the final exam of the CCP course. The OSCE consisted of student performance of the EFAST in a clinical scenario of a trauma patient simulated setting with standardized patients and one-on-one faculty observers. Both the standardized patients and faculty observers completed an assessment rubric. Standardized patients assessed the professionalism and communication skills of the students, and the faculty assessed the students’ ability to perform the EFAST exam and their ability to communicate regarding the indications for and findings of the exam in the standardized patient clinical context. The MCQs assessed the recognition of abnormal findings on ultrasound, diagnoses made through performing EFAST in context of clinical cases, and indications/limitations of EFAST.
Educational activities
Educational activities consisted of didactic sessions and skills sessions with hands-on ultrasound practice. The didactic sessions consisted of two 50-min sessions, one on the basic physics of ultrasound in relation to appropriate ultrasound machine settings, probe selection, and commonly found artifacts, and the goals of a POCUS examination; and the other on EFAST, which focused on the clinical indications for EFAST and the normal and abnormal findings found on the EFAST ultrasound exam. The second session involved a live demonstration with a standardized patient and included how to communicate with, properly drape, and assess the comfort of patients during performance of an EFAST exam. The skills session consisted of one 2-h session of hands-on ultrasound practice with standardized patients. Students were also given access to handheld probes, which were available to check out to further practice ultrasound on their own time.
Faculty training
Faculty involved in the EFAST OSCE assessment were trained using videos made by an SHSU COM faculty member with 15 years of clinical experience in performing EFAST. One video provided an overview of the EFAST exam and how to perform it, and the other video described how to precept the OSCE assessment of the students participating in the EFAST curriculum. Faculty who participated in the assessment were also present at the skills practice sessions as session facilitators.
Data collection
Students who participated in the EFAST curriculum were anonymously surveyed via Qualtrics one year later upon completion of their third-year clinical clerkships. The survey was newly developed for this study, and the list of questions used in the survey is available in the supplementary material (Additional file 1). The development of this survey was informed by a general review of the literature and the identified aims of the study in conjunction with the design of the EFAST curriculum. The authors, R.G., K.S., A.R., and R.A., developed the survey. Survey questions were designed to assess the students’ perception of the quality and utility of the EFAST curriculum, with Likert scale (1-strongly disagree, 2-disagree, 3- neutral, 4-agree, 5-strongly agree) use to rate the responses. Survey questions were also designed to assess respondents’ opportunity for POCUS and EFAST utilization during their third-year clerkships in terms of ultrasound exam types, clinical settings, and clinical rotations where POCUS was used. The survey included open-ended questions, which assessed student perceptions of barriers to POCUS implementation during their clinical rotations. Demographic information regarding at which SHSU COM site respondents had been located for their clerkships was also collected.
Students were contacted via email with an initial invitation to complete the survey. The survey was open for two months for respondents to complete, and multiple reminders were sent via text-based messaging system during that time interval.
Data analysis
Quantitative analysis
For categorical variable data, frequencies and percentages were calculated. For continuous variable data, measures of central tendency, range, and variance were calculated.
Qualitative analysis
The narrative feedback provided by the respondents to the open-ended questions was analyzed using constant comparison analysis [19]. Two investigators (P.R. and R.A.) independently double coded the deidentified narrative feedback. P.R. and R.A. then reviewed the accuracy and relevance of the codes according to their interpretation of the students’ meaning. Discrepancies in coding were resolved by discussion between the two independent coders of rationale behind codes assigned until consensus was reached. Similar codes were merged and codes that were no longer relevant were removed. Axial coding was then completed by comparing text segments and codes to create categories made of similar codes, and to combine categories into broader themes.
Ethical considerations
Institutional Research Board (IRB) exemption for this project was granted by the IRB committee from SHSU. Informed consent was obtained from all participants.
Results
A total of 21 of 69 (30.4%) participants responded to the survey, with 17 (24.6%) participants completing the entire survey. Students from all 5 of the clinical sites responded to the survey, with 3 from Fort Bend, 4 from Conroe/Huntsville and Piney Woods, 5 from Beaumont/Port Arthur and 5 from Downtown Houston.
Quantitative analysis
All respondents rated the importance of training in ultrasound in medical school as moderately, very, or extremely important (Table 2).
Table 2.
Student perception of the importance of training in use of POCUS during medical school
| Number of Respondents | Percentage of Respondents | |
|---|---|---|
| Not at all important | 0 | 0 |
| Slightly important | 0 | 0 |
| Moderately important | 4 | 21.0 |
| Very important | 7 | 36.8 |
| Extremely important | 8 | 42.1 |
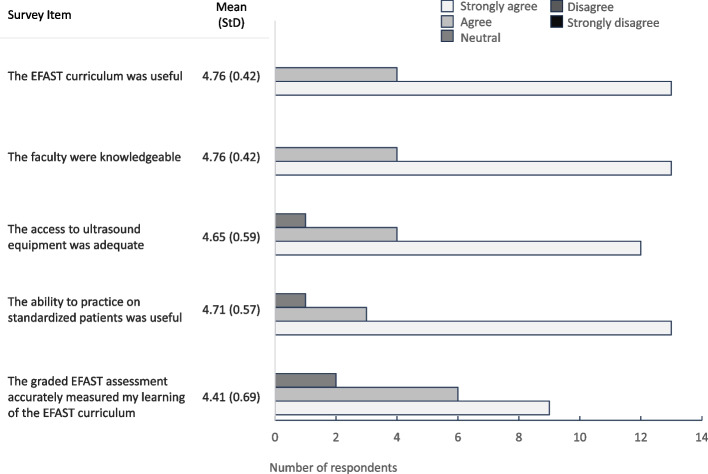
Respondents rated all items regarding the quality of the EFAST training highly with mean values of 4.41–4.76 on a 5 point Likert scale, stating that the EFAST curriculum was useful, faculty were knowledgeable, the access to ultrasound equipment was adequate, the ability to practice on Standardized Patients was useful, and the graded EFAST assessment accurately measured their learning of the EFAST curriculum (Fig. 1).
Fig. 1.
Respondents’ rating of the quality of the EFAST curriculum. Respondents rated perceptions regarding the following aspects of the EFAST curriculum: usefulness, faculty knowledge, access to ultrasound equipment and standardized patients and appropriateness of the EFAST assessment
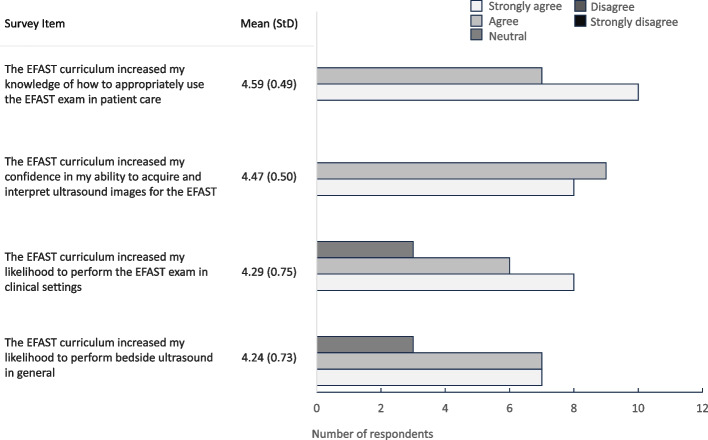
Respondents also highly rated various outcomes of the EFAST curriculum, with mean values from 4.24–4.59, including that it increased their knowledge of how to appropriately use EFAST exam in patient care, increased their confidence in their ability to acquire and interpret ultrasound images for the EFAST, increased their likelihood to perform the EFAST exam in clinical settings, and increased their likelihood to perform bedside ultrasound in general (Fig. 2).
Fig. 2.
Respondents’ perceptions of outcomes of the EFAST curriculum. Respondents rated perceptions regarding the following outcomes of the EFAST curriculum: increase in knowledge and appropriate use of the EFAST exam, confidence and ability to acquire and interpret EFAST images, likelihood to perform EFAST, and likelihood to perform bedside ultrasound in general
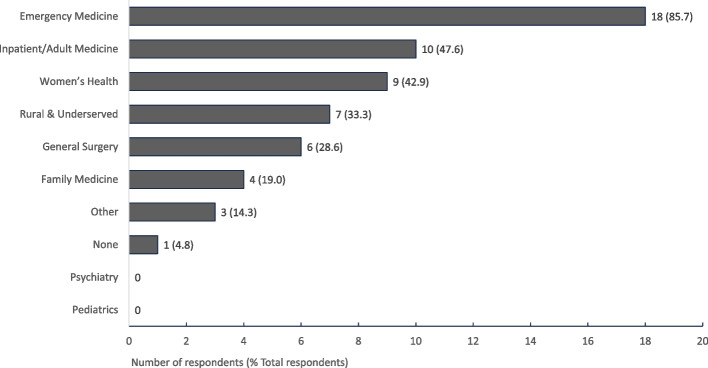
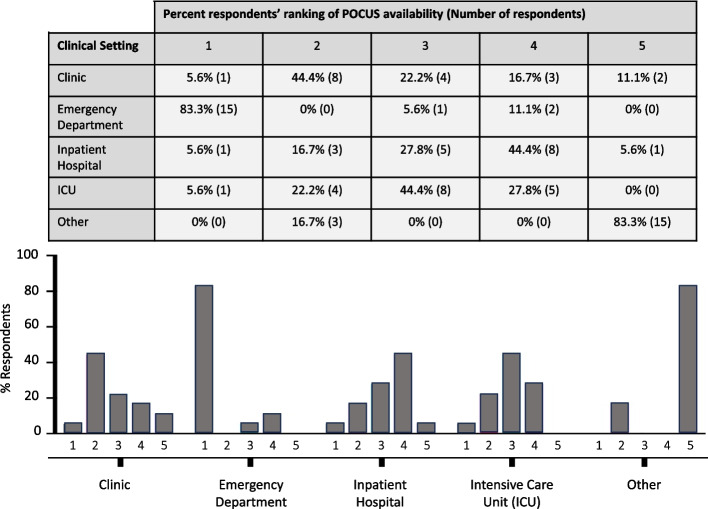
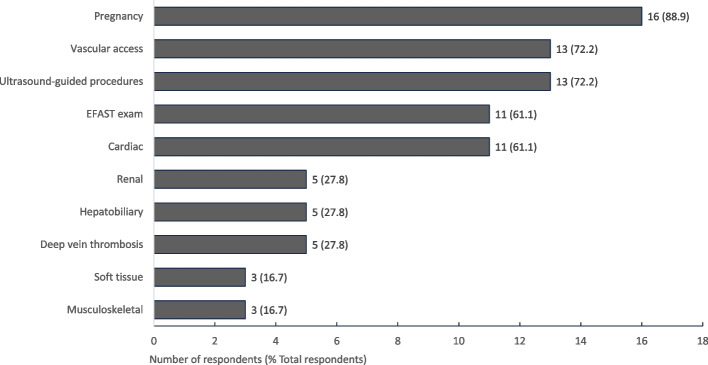
Respondents reported access to ultrasound machines most commonly on Emergency Medicine clerkships, followed by Inpatient/Adult Medicine and Women’s Health clerkships (Fig. 3). Lack of machine availability was reported by all respondents on Pediatrics and Psychiatry clerkships, and one respondent reported not having machine availability on any clerkship. When asked to rank the clinical settings in which POCUS was most commonly available, the majority of respondents (83.3%) ranked the Emergency Department as the setting in which POCUS was most often available to them (Fig. 4). The POCUS exams students most commonly reported as either performing themselves or observing clinicians on their clerkships perform were pregnancy-related, ultrasound guided procedures, vascular access, EFAST, and cardiac exams (Fig. 5).
Fig. 3.
POCUS machine availability on clerkships. POCUS availability on each clerkship rotation as reported by survey respondents. n = 21 respondents
Fig. 4.
Respondents ranking of clinical setting in which POCUS was most available. Respondents ranked POCUS availability in the following clinical settings: clinic, emergency department, inpatient hospital and ICU (1 = most available, 5 = least available). n = 18 respondents
Fig. 5.
Types of POCUS exams respondents participated in. POCUS exams performed during clerkship rotations, by respondents or supervising clinicians, as reported by respondents across all clerkships. n = 18 respondents
Of respondents reporting access to POCUS machines, 94.4% reported observing a clinician perform POCUS at least once on their clinical rotations, with 33.3% reporting observing a clinician perform POCUS greater than 15 times (Table 3). Of respondents reporting access to POCUS machines, 88.9% reported performing POCUS at least once during clinical rotations, with the majority (55.6%) reporting performing POCUS 1–5 times. Regarding performance of EFAST specifically, 72.2% of respondents reported performing EFAST at least once, with 2 students reporting performing it more than 15 times (Table 3).
Table 3.
POCUS utilization on clinical rotations
| Number of Times Exam Utilized | Number Respondents Reporting Personal EFAST Performance (% Total) | Number Respondents Reporting Personal POCUS Performance (% Total) | Number Respondents Reporting Observing Clinician POCUS Performance (% Total) |
|---|---|---|---|
| Never | 4 (23.5%) | 2 (11.1%) | 1 (5.6%) |
| 1–5 times | 10 (58.8%) | 10 (55.6%) | 2 (11.1%) |
| 5–10 times | 1 (5.9%) | 4 (22.2%) | 7 (38.9%) |
| 10–15 times | 0 (0%) | 1 (5.6%) | 2 (11.1%) |
| > 15 times | 2 (11.8%) | 1 (5.6%) | 6 (33.3%) |
In addition, no students reported turning down the opportunity to perform ultrasound when it was offered to them.
Qualitative analysis
The survey contained four open-ended questions regarding the EFAST curriculum and barriers to using EFAST during clinical rotations. Constant comparison analysis revealed several dominant codes for each question.
For the survey question “What was most useful about the EFAST curriculum sessions?”, codes included safe simulated learning environment and learning the EFAST indications.
Student #01 commented “They were a nice, simulated environment that offered time for correction and growth.” Several students noted the benefits of hands-on practice with ultrasound resulting in an increase in their comfort level with POCUS in general. Student #03: “Hands on time with ultrasound. Even though I did not perform EFAST scans during 3rd year, my comfort level with handling probes and interpreting images was extrapolated to other targeted examinations that I was able to perform.” Students also commented on the benefits of being able to practice on standardized patients during the EFAST sessions.
Students also found learning the indications for EFAST to be a useful part of the curriculum. Student #20 valued: “Learning the indications which were tested on exams.”
In response to the question “What could have been done to improve the EFAST curriculum sessions?”, dominant codes were more ultrasound practice sessions and addition of pathology.
Students frequently commented that more practice sessions with ultrasound would have improved the EFAST curriculum. Student #01 recommended: “More practice and exposure of using ultrasound in several sessions.”
Several students commented that including pathology in the EFAST curriculum could improve the sessions. Student #11: “Focus on indications for eFAST, identification of pathology on eFAST, next steps when pathology is identified “. Student #10 similarly recommended to “Show common pathologic findings”.
In response to the survey question “What barriers have there been to you using the EFAST exam during clinical rotations?” dominant codes included lack of patients with indication for EFAST, time constraints, attending comfort level with ultrasound, availability of ultrasound machines and physician/resident preference to perform.
Several students commented that the lack of patients that needed an EFAST exam was a barrier to use of the exam. Student #04 stated: “Have not had a patient with a possible need for it yet”. Student #18 found acuity level and clinical setting to be a barrier by stating “usually low acuity in rural area bc only level 3 trauma ER”.
Other barriers identified by respondents included time constraints. Student #07 commented that “docs want to go faster than i am going”. Students also identified lack of ultrasound machine availability and the comfort level of the physician with ultrasound as barriers to using the EFAST exam during clinical rotations. Student #02: “Lack of availability of the U/S or a provider that was not comfortable with using it”. Student #19 commented: “Many physicians are not confident in their ability to use ultrasound.”
Additionally, some students found that physicians preferring to perform the EFAST themselves was a barrier to student use of EFAST. Student #11: “Resident/physician will perform the exam due to greater competency”.
In response to the survey question regarding teaching done by clerkship preceptors (‘If your preceptor did provide guidance/education points to you regarding POCUS, what specific learning topic was provided?’), several students noted vascular access and fetal monitoring as learning topics provided by their clerkship preceptors.
Discussion
As POCUS has been increasingly utilized in the practice of medicine, the design and implementation of ultrasound-related curriculum that prepares medical students for the appropriate use of ultrasound in medicine is a rapidly transforming aspect of UME. This study describes the development and implementation of a brief focused introduction to EFAST curriculum delivered to preclerkship students, and assesses their perception of the quality and utility of this curriculum one year later after clinical experience in third-year clerkships. While prior studies have indicated medical students can demonstrate appropriate performance of EFAST and report increased confidence in performing the EFAST immediately following focused training sessions [11, 12], fewer studies have examined medical students’ perception of the impact of POCUS training in subsequent clinical settings within UME. When surveyed one year after participation in the EFAST curriculum, respondents in our study highly rated the quality of the EFAST curriculum, reporting that participation resulted in perception of increased knowledge of the appropriate clinical use of EFAST and increased ability to perform the exam. Survey respondents also indicated their perception that participating in the curriculum increased their likelihood of performing the EFAST exam and POCUS in general during their clerkships. Some studies have indicated that focused EFAST training results in increased utilization among health care workers, with trauma providers who underwent EFAST training having increased EFAST use on chart review, and Emergency Medicine registrars who received training in EFAST reporting higher levels of use of EFAST after receiving increased training during residency [13, 20]. Our study builds on these previous studies by indicating that survey respondents, representing a subset of this cohort of medical students who participated in this introduction to EFAST curriculum early in their medical education, report that EFAST training increased their confidence and perception of readiness to perform the EFAST exam and bedside ultrasound in general in the year subsequent to the EFAST training.
Qualitative analysis of respondents’ narrative feedback indicates that students valued the simulated environment to learn and practice the EFAST exam, particularly valuing the hands-on nature of the skills lab and the opportunity to practice on standardized patients. Survey respondents connected experiences gained through participating in the simulated environment to being more comfortable with performing ultrasound on real patients in clinical settings, and respondents reported increased likelihood of performing POCUS exams as a result of participating in the curriculum. Prior studies indicate that the more often learners perform ultrasound exams during training, the more likely they are to perform those exams later in clinical settings [13]. This is important as POCUS has been identified as a hands-on skill that requires continued utilization in order to achieve and maintain proficiency [21].
Students in our survey indicated several barriers to utilization of EFAST on clinical rotations, including time constraints, lack of patients with indications for EFAST, lack of ultrasound machine availability, and clinician comfort level with EFAST. These student perceptions of barriers to utilization of EFAST are similar to barriers reported by faculty in previous studies regarding the incorporation of POCUS in UME, which included lack of trained faculty, lack of available time in the curriculum, lack of financial support, and lack of appropriate equipment [2–5]. The similarity of responses across students and faculty draws attention to the importance of addressing these barriers during development of ultrasound curriculum by institutions.
Students in our survey also recommended potential improvements to the introduction to EFAST curriculum that could assist in addressing these barriers, including incorporation of pathological findings into the curriculum. Pathology was introduced to students in the curriculum through still images and videos during the didactic sessions and was assessed via the MCQ portion of the assessment. However, students did not gain experience performing ultrasound on patients with pathology in this pre-clerkship curricula involving a standardized patient-based EFAST assessment model. Integration of ultrasound images of pathological findings or simulated pathology within the OSCE assessment portion of the curriculum may have provided additional value to the students and assisted with students developing clinical decision-making skills regarding the management of patients with pathology identified on EFAST exams.
Additionally, gaining experience in the ultrasound of pathological conditions would likely be useful in addressing the student survey respondents’ identified barriers to EFAST utilization of lack of patients with indications for EFAST and the time constraints of often fast-paced clinical settings of their third-year clerkships. Survey respondents valued the hands-on practice of using ultrasound during the training curriculum, and additional practice sessions or self-directed ultrasound practice time could likewise address these barriers. The EFAST training curriculum implemented in this study required resources of handheld portable ultrasound machines, standardized patients, and knowledgeable faculty to design and teach the sessions. Implementation of programs without these resources may require increased reliance on online learning materials and simulation of cases. Incorporation of technology to simulate pathological findings and to assist students in the development of ultrasound manual skills in the simulated preclinical environment has been identified as a future direction to explore in the development of ultrasound-related curriculum [22, 23].
Students in our survey indicated access to POCUS machines and opportunities to perform POCUS most commonly during their Emergency Medicine clerkship and in the Emergency Department, but also reported access in multiple other clerkships and clinical settings, reflecting the rise of POCUS in multiple medical specialties and venues of clinical care [24]. Survey respondents also identified POCUS exams they most often encountered during third-year clerkships, including pregnancy-related ultrasound and ultrasound-guided procedures, such as vascular access. These findings can guide the prioritization of additional module development within our curriculum. Identification of clinical settings, types of rotations, and specific ultrasound applications where students most often encounter access to POCUS during third-year clerkships may be used to inform further targeted modification of ultrasound curriculum.
Design and delivery of ultrasound curriculum in UME is a developing field, with professional societies and experts calling for increased incorporation of ultrasound in UME curriculum [24, 25]. This study involved the development of an introduction to EFAST curriculum using backward design by first determining the desired competencies of OMS III students through review of professional society guidelines and the needs of our particular institution. The curriculum assessments were then designed to assess student demonstration of those competencies, with educational activities’ format and content subsequently developed to maximize student success on the assessment. This may serve as a model for other institutions to develop EFAST and other POCUS curriculum at their institutions.
A limitation of this study is the low survey response rate. While the quality and impact of the EFAST curriculum was highly rated by respondents, this feedback represents a subset of students who participated in the EFAST training curriculum rather than the entire cohort, which may have introduced bias in the results. While there were respondents from each of the clinical sites, the number of respondents from each site was low (between 3–5 respondents at each site). This low response rate across clinical sites hindered our ability to compare a demographic variable within out study population of differing clinical rotation sites at which students were located for their third-year clerkship sites. These SHSU COM clerkship sites included rural, semi-urban, and urban community settings. While POCUS is often widely available in urban academic centers, some studies indicate less access to POCUS in rural areas [26, 27], despite research suggesting the benefit of POCUS may be greater in rural, under-resourced areas [28]. Thus, with improved survey response rates, this study could have provided an opportunity to investigate differences in EFAST and POCUS availability and use between these different settings.
Our study was limited to student perception of the impact of the curriculum and barriers to EFAST and POCUS utilization, which, while deliberate in the design of this study, is an inherently limited perspective. Additional measures of training effectiveness, such as preceptor evaluations or direct observation of clinical performance by preceptors, would strengthen the assessment of the EFAST training curriculum’s effectiveness. Additionally, the study design relied on students’ self-reported use of EFAST and POCUS over the preceding year, which requires recall of clinical experiences over an extended period of time, and thus may have included under-reporting or over-reporting of frequency of EFAST and POCUS utilization. Future studies will evaluate third-year clerkship preceptors’ perceptions regarding student readiness to perform EFAST, as well as preceptor-identified barriers to EFAST and POCUS performance by students, with comparisons made to the student perceptions as assessed in this study. Additionally, further longitudinal data would provide insight into the impact of the EFAST training on clinical proficiency, and future studies involving follow-up at the end of medical school or during residency will add valuable data regarding skill retention and application of EFAST and POCUS training in various specialties.
Conclusions
Our study demonstrates the impact of including a POCUS curriculum in pre-clerkship UME curriculum, with student participants clearly identifying the EFAST curriculum as effective in increasing knowledge of the appropriate use and performance of EFAST in clinical settings, as well as increased student perception of confidence in performing EFAST specifically, and POCUS exams in general. This study describes the implementation of a competency-based POCUS curriculum developed through deliberate backward design based on professional guidelines and core competencies, and then modified by anticipated needs of the institution and the community it serves. Furthermore, our study suggests that student perception of POCUS curriculum effectiveness may provide a valuable contribution to continual curriculum improvement informed by institutional and community needs.
Supplementary Information
Additional file 1. Survey used in the study. List of questions used to survey the students in this study.
Abbreviations
- POCUS
Point-of-Care Ultrasound
- UME
Undergraduate medical education
- EFAST
Extended Focuses Assessment with Sonography
- OMS III
Third-year osteopathic medical students
- SHSU COM
Sam Houston State University College of Osteopathic Medicine
- CCP
Clinical Clerkship Preparation
- OSCE
Observed Structured Clinical Exam
- MCQs
Multiple Choice Questions
- IRB
Institutional Review Board
Authors’ contributions
R.A., R.G., K.S., and A.R. designed the study, collected the data, and contributed to the quantitative analysis of the data. R.G. and K.S. conducted the literature review. R.A. and P.R. conducted the qualitative data analysis and were major contributors to writing of the manuscript. P.R. also contributed to the quantitative data analysis. All contributed to the editing of the manuscript. All authors read and approved the final manuscript.
Funding
Not applicable.
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Declarations
Ethics approval and consent to participate
Institutional Research Board (IRB) exemption for this project was granted by the IRB committee from SHSU. Informed consent was obtained from all participants.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Moore CL, Copel JA. Point-of-care ultrasonography. N Engl J Med. 2011;364(8):749–57. [DOI] [PubMed] [Google Scholar]
- 2.Bahner DP, Goldman E, Way D, Royall NA, Liu YT. The state of ultrasound education in U.S. medical schools: results of a national survey. Acad Med. 2014;89(12):1681–6. 10.1097/ACM.0000000000000414. PMID: 25099238. [DOI] [PubMed] [Google Scholar]
- 3.Dinh VA, Fu JY, Lu S, Chiem A, Fox JC, Blaivas M. Integration of ultrasound in medical education at United States medical schools: a national survey of directors’ experiences. J Ultrasound Med. 2016;35(2):413–9. 10.7863/ultra.15.05073. Epub 2016 Jan 18 PMID: 26782166. [DOI] [PubMed] [Google Scholar]
- 4.Russell FM, Zakeri B, Herbert A, Ferre RM, Leiser A, Wallach PM. The state of point-of-care ultrasound training in undergraduate medical education: findings from a national survey. Acad Med. 2022;97(5):723–7. 10.1097/ACM.0000000000004512. Epub 2022 Apr 27 PMID: 34789665. [DOI] [PubMed] [Google Scholar]
- 5.Tarique U, Tang B, Singh M, Kulasegaram KM, Ailon J. Ultrasound curricula in undergraduate medical education: a scoping review. J Ultrasound Med. 2018;37(1):69–82. [DOI] [PubMed] [Google Scholar]
- 6.Glass C, Sarwal A, Zavitz J, Nitsche J, Joyner J, Johnson LL, Garcia-Vargas J, O’Brien MC. Scoping review of implementing a longitudinal curriculum in undergraduate medical education: the wake forest experience. Ultrasound J. 2021;13(1):23. 10.1186/s13089-021-00206-w. PMID:33871741;PMCID:PMC8055803. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Nelson BP, Hojsak J, Dei Rossi E, Karani R, Narula J. Seeing is believing: evaluating a point-of-care ultrasound curriculum for 1st-year medical students. Teach Learn Med. 2017;29(1):85–92. 10.1080/10401334.2016.1172012. Epub 2016 May 18. PMID: 27191830. [DOI] [PubMed] [Google Scholar]
- 8.Netherton S, Milenkovic V, Taylor M, Davis PJ. Diagnostic accuracy of eFAST in the trauma patient: a systematic review and meta-analysis. CJEM. 2019;21(6):727–38. 10.1017/cem.2019.381. PMID: 31317856. [DOI] [PubMed] [Google Scholar]
- 9.Monti JD, Perreault MD. Impact of a 4-hour introductory eFAST training intervention among ultrasound-naïve U.S. military medics. Mil Med. 2020;185(5–6):e601–8. 10.1093/milmed/usaa014. PMID: 32060506. [DOI] [PubMed] [Google Scholar]
- 10.O’Connor L, Beth-Urhoy M, Allegra S, Dowd A, Nordberg A, Boardman T, Gleeson T, Lindsay R. A novel point-of-care ultrasound curriculum for air critical care personnel. West J Emerg Med. 2023;24(1):30–7. 10.5811/westjem.2022.12.57599. PMID:36735009;PMCID:PMC9897250. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Cevik AA, Noureldin A, El Zubeir M, Abu-Zidan FM. Assessment of EFAST training for final year medical students in emergency medicine clerkship. Turk J Emerg Med. 2018;18(3):100–4. 10.1016/j.tjem.2018.05.004. PMID:30191188;PMCID:PMC6107923. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Krause C, Krause R, Krause R, Gomez N, Jafry Z, Dinh VA. Effectiveness of a 1-hour extended focused assessment with sonography in trauma session in the medical student surgery clerkship. J Surg Educ. 2017;74(6):968–74. 10.1016/j.jsurg.2017.03.007. Epub 2017 May 4. PMID: 28479071. [DOI] [PubMed] [Google Scholar]
- 13.Pencil K. eFAST simulation training for trauma providers. J Trauma Nurs. 2017;24(6):376–80. 10.1097/JTN.0000000000000329. PMID: 29117056. [DOI] [PubMed] [Google Scholar]
- 14.Steinwandel U, Coventry LL, Kheirkhah H. Evaluation of a Point-of-care ultrasound (POCUS) workshop for peripheral intravenous cannulation. BMC Med Educ. 2023;23(1):451. 10.1186/s12909-023-04428-5. PMID: 37337172; PMCID: PMC10280877. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.American Academy of Family Physicians. AAFP recommended curriculum guidelines for family medicine residents point of care ultrasound. Reprint No. 290D. https://www.aafp.org/dam/AAFP/documents/medical_education_residency/program_directors/Reprint290D_POCUS.pdf. Accessed 10 March 2022.
- 16.American College of Emergency Physicians. Ultrasound guidelines: emergency, point-of-care, and clinical ultrasound guidelines in medicine. Ann Emerg Med. 2017;69(5):e27–54 https://www.annemergmed.com/article/S0196-0644(16)30935-0/pdf. [DOI] [PubMed] [Google Scholar]
- 17.American College of Emergency Physicians. Emergency ultrasound standard reporting guidelines. 2018. https://www.acep.org/siteassets/uploads/uploaded-files/acep/clinical-and-practice-management/policy-statements/information-papers/emergency-ultrasound-standard-reporting-guidelines---2018.pdf.
- 18.Wiggins G, McTighe J. What is backward design. Understand Design. 1998;1:7–19. [Google Scholar]
- 19.Glaser BG. The constant comparative method of qualitative analysis. Soc Probl. 1965;12(4):436–45. 10.2307/798843. [Google Scholar]
- 20.Sweetman G, Fear M, Hird K. Experience of a tutor centric model for sonography training of emergency department registrars in an Australian urban emergency department 2009–2012. Australas J Ultrasound Med. 2015;18(3):112–7. 10.1002/j.2205-0140.2015.tb00210.x. Epub 2015 Dec 31. PMID: 28191252; PMCID: PMC5024959. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Kimura BJ, Sliman SM, Waalen J, Amundson SA, Shaw DJ. Retention of ultrasound skills and training in “Point-of-Care” cardiac ultrasound. J Am Soc Echocardiogr. 2016;29(10):992–7. 10.1016/j.echo.2016.05.013. Epub 2016 Jun 29 PMID: 27372559. [DOI] [PubMed] [Google Scholar]
- 22.Narang A, Bae R, Hong H, Thomas Y, Surette S, Cadieu C, Chaudhry A, Martin RP, McCarthy PM, Rubenson DS, Goldstein S, Little SH, Lang RM, Weissman NJ, Thomas JD. Utility of a deep-learning algorithm to guide novices to acquire echocardiograms for limited diagnostic use. JAMA Cardiol. 2021;6(6):624–32. 10.1001/jamacardio.2021.0185. PMID:33599681;PMCID:PMC8204203. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Sjogren AR, Leo MM, Feldman J, Gwin JT. Image segmentation and machine learning for detection of abdominal free fluid in focused assessment with sonography for trauma examinations: a pilot study. J Ultrasound Med. 2016;35(11):2501–9. 10.7863/ultra.15.11017. Epub 2016 Oct 13. PMID: 27738293; PMCID: PMC7929643. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Díaz-Gómez JL, Mayo PH, Koenig SJ. Point-of-care ultrasonography. N Engl J Med. 2021;385(17):1593–602. 10.1056/NEJMra1916062. PMID: 34670045. [DOI] [PubMed] [Google Scholar]
- 25.Hoppmann RA, Mladenovic J, Melniker L, Badea R, Blaivas M, Montorfano M, Abuhamad A, Noble V, Hussain A, Prosen G, Villen T, Via G, Nogue R, Goodmurphy C, Bastos M, Nace GS, Volpicelli G, Wakefield RJ, Wilson S, Bhagra A, Kim J, Bahner D, Fox C, Riley R, Steinmetz P, Nelson BP, Pellerito J, Nazarian LN, Wilson LB, Ma IWY, Amponsah D, Barron KR, Dversdal RK, Wagner M, Dean AJ, Tierney D, Tsung JW, Nocera P, Pazeli J, Liu R, Price S, Neri L, Piccirillo B, Osman A, Lee V, Naqvi N, Petrovic T, Bornemann P, Valois M, Lanctot JF, Haddad R, Govil D, Hurtado LA, Dinh VA, DePhilip RM, Hoffmann B, Lewiss RE, Parange NA, Nishisaki A, Doniger SJ, Dallas P, Bergman K, Barahona JO, Wortsman X, Smith RS, Sisson CA, Palma J, Mallin M, Ahmed L, Mustafa H. International consensus conference recommendations on ultrasound education for undergraduate medical students. Ultrasound J. 2022;14(1):31. 10.1186/s13089-022-00279-1. PMID:35895165;PMCID:PMC9329507. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Talley BE, Ginde AA, Raja AS, Sullivan AF, Espinola JA, Camargo CA Jr. Variable access to immediate bedside ultrasound in the emergency department. West J Emerg Med. 2011;12(1):96–9 PMID: 21691479; PMCID: PMC3088382. [PMC free article] [PubMed] [Google Scholar]
- 27.Mengarelli M, Nepusz A, Kondrashova T. A comparison of point-of-care ultrasonography use in rural versus urban emergency departments throughout Missouri. Mo Med. 2018;115(1):56–60 PMID: 30228684; PMCID: PMC6139795. [PMC free article] [PubMed] [Google Scholar]
- 28.Lyon M, Blaivas M, Brannam L. Use of emergency ultrasound in a rural ED with limited radiology services. Am J Emerg Med. 2005;23(2):212–4. 10.1016/j.ajem.2004.05.007. PMID: 15765351. [DOI] [PubMed]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Additional file 1. Survey used in the study. List of questions used to survey the students in this study.
Data Availability Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.