Abstract
Background and significance
Congenital adrenal hyperplasia (CAH) is a genetic condition impairing adrenal steroid production, requiring lifelong steroid replacement, leading to decreased quality of life and a shortened lifespan. Preparing and supporting adolescents with CAH to develop health-related knowledge, skills, and decision-making during the pediatric-to-adult healthcare transition (HCT) is a priority. Many adolescents with CAH do not receive adequate HCT and do not attend follow-up care after transfer to an adult setting. The Comprehensive Adolescent Healthcare Transition (CAH-T) program was developed using CAH care guidelines and the Got Transition Six Core Elements of Healthcare Transition approach.
Purpose
This quality improvement (QI) initiative aimed to evaluate clinicians’ utilization and acceptance of the CAH-T program for addressing the HCT needs of adolescents with CAH in a southeastern United States pediatric endocrine clinic.
Intervention
Baseline demographics, the Health Care Transition Feedback Survey for Clinicians, and the Current Assessment of Healthcare Transition Activities were measured using surveys adopted from Got Transition. Clinicians were educated on the CAH-T program and patient education materials. Following implementation, clinicians documented all CAH-T program-recommended interventions provided in the clinic. Surveys were reassessed using repeated measures.
Evaluation
Twenty-nine clinicians participated. Eight separate patients received 53 total CAH-T program-recommended interventions during the three-month observation period. Paired assessment of the Current Assessment of Healthcare Transition Activities scores increased from 15.29 ± 8.32 to 24.00 ± 6.11 (p = 0.018; r = 0.63). The Health Care Transition Feedback Survey for Clinicians mean scores increased from 2.75 ± 0.26 to 3.30 ± 0.43 (p = 0.018; r = 0.59). These measures indicate increased utilization of HCT services and acceptance of HCT value. Clinicians suggested that time limitations, English-only transition education materials, and lack of electronic medical record integration were significant barriers to HCT support.
Implications for practice
A structured HCT program ensures clinicians provide adolescents with CAH support and guideline-based care. The CAH-T program offers an example of developing and implementing an HCT program for adolescents with CAH. Integration in the electronic medical record will ultimately increase program sustainability.
Keywords: Congenital adrenal hyperplasia, Healthcare transition, Quality improvement
1. Introduction
Congenital Adrenal Hyperplasia (CAH) is a group of autosomal recessive conditions impairing adrenal steroid synthesis, with a worldwide incidence of 1 in 9500 births.[1], [2], [3] The most common form of these conditions, 21-hydroxylase deficiency, leads to the underproduction of cortisol and aldosterone and the overproduction of adrenal androgens.4 Lifelong corticosteroid replacement with/without mineralocorticoid replacement is the mainstay of CAH management, and clinicians must balance the long-term consequences of supraphysiologic steroids and hyperandrogenism.2 Hormonal changes during puberty (i.e., insulin resistance, increased adrenal androgen production, and increased cortisol clearance) negatively impact CAH control during adolescence.[2], [5], [6] Diminished adherence to multiple-dose daily medications can further complicate disease management in this age group.[2], [5], [6] Therefore, adolescence presents an optimal time for increased health screening and engagement to prevent complications and improve quality of life.1
CAH increases the risks of health-related issues in adulthood, including obesity, hypertension, infertility, and osteopenia/osteoporosis.[1], [2], [7], [8], [9], [10] Many of these changes begin in adolescence, with health-related problems increasing in adulthood when not properly addressed.[1], [2], [5], [6], [9] Ultimately, these issues equate to higher healthcare costs and reduced quality of life. Fortunately, many of these complications can be diminished or eradicated through recommended health screening and patient engagement.[1], [6], [9], [11] Therefore, it is crucial to actively involve adolescents with CAH to increase health awareness, self-efficacy, and preventive care.[1], [2], [11], [12]
Effective pediatric-to-adult healthcare transition (HCT) remains an elusive concept with no universally accepted definition or measurement construct.13 White et al.14 define HCT as “the process of moving from a child/family-centered model of health care to an adult/patient-centered model of health care, with or without transferring to a new clinician.” This landmark paper also outlines key goals for HCT–enhancing adolescent and young adult health self-efficacy, fostering utilization of health services, and establishing cohesive pediatric and adult practices through HCT preparation, transfer, and adult-centered care integration.14
Clinical guidelines for CAH management support effective HCT and lifelong specialized care for the medical, sexual, and psychosocial needs of individuals with CAH.12 Supporting adolescents transitioning from pediatric to adult care services provides an opportunity to enforce health-promoting behaviors and build self-efficacy in condition management.[5], [15], [16] Adults with CAH who routinely attend adult care after HCT are shown to have significantly improved physical and psychological health, quality of life, and reduced healthcare costs compared to those lost to follow-up care.[15], [16], [17], [18] Conversely, when young adults with CAH are unprepared for adult-centered, health-related knowledge, self-efficacy, and autonomy–there is an increased risk of poor attendance in adult care settings, worsened health outcomes, increased health risks, increased costs, and increased mortality.[15], [16], [17], [18], [19], [20]
1.1. Problem description
This quality improvement (QI) initiative focuses on implementing an evidence-based HCT program (Comprehensive Adolescent Healthcare Transition [CAH-T]) for adolescents with CAH in a pediatric endocrinology clinic in the southeastern United States (US). While standardized HCT services are offered in this clinic for patients with diabetes, there was no standardized HCT approach for adolescents with CAH.
1.2. Available knowledge
Currently, eight published studies in France, the Netherlands, the United Kingdom, and Isreal have examined the HCT experiences of individuals with CAH.[15], [16], [17], [18], [19], [20], [21], [22] Although provided valuable insight, there is a lack of CAH-specific HCT research within the United States. Gradual progression to independent adult care, a structured process, psychological support, and information sharing are all central themes of transitional care.[14], [23], [24] Care specific to the transition of CAH patients incorporates tailored education regarding genetic testing, surgical history, medical disease management, stress dosing, emergency care, matters of sexuality and fertility, and preventable long-term comorbidities such as obesity, cardiovascular disease, and bone health.[15], [16], [17], [18], [19], [20], [21], [22]
Despite efforts to implement HCT processes, numerous obstacles can impede effective HCT for adolescents and young adults with CAH. A significant challenge within this population is care drop-out, with approximately 25% to 50% of individuals with CAH failing to engage in adult care.[15], [19], [20] Godbout et al.,18 Gleeson et al.,19 and Davidse et al.20 highlight how logistical failures, such as poor communication, appointment scheduling issues, and a lack of referral letters, accounted for 5–19% of young adult patients not attending care. Additionally, increasing nonattendance rates in the three years following transfer from pediatric services illustrate the challenges some young adults encounter post-transfer from pediatric services.19 Factors such as further distance from clinics and lower socioeconomic status correlate with a higher likelihood of nonattendance, underscoring the necessity for addressing barriers to care access during HCT and continuing support for young adults post-HCT.[15], [19]
Various models of provider transfer have been described within this literature. One proposed model is the shared or combined approach, where adolescents or young adults meet their adult care providers while still receiving care within the pediatric system.17 Another popular model is the transition clinic, where pediatric and adult providers share the clinical consultation of an individual for a transitional period. Evidence in CAH HCT is unclear on the effectiveness of this model.[17], [19] Where Gleeson et al.19 showed that the transition clinic model did not benefit adult clinical engagement, Twito et al.17 reported that participation in a transition clinic model significantly increased adherence to ongoing adult care. One of the more promising models suggests the role of a care coordinator to ensure successful HCT logistics.[16], [20] Additionally, a hub and spoke model (where specialty care providers work alongside local secondary care providers) has been suggested to engage more adults with CAH within the healthcare system.19 It is clear that no single transition model will be appropriate for every situation, and the proximity or availability of specialty care providers is often a limitation. Nevertheless, the literature supports that a systematic approach, with open communication and clinical collaboration between the pediatric and adult providers, including the primary care provider, will support patients and caregivers, increasing attendance to adult care visits and supporting the likelihood of continued care.[15], [16], [17], [18], [19]
1.3. Rationale
Three frameworks informed this initiative: 1) Theoretical Framework: The Promoting Action on Research Implementation in Health Services (PARIHS) Framework, derived from Rogers’ Diffusion of Innovations,25 2) QI Framework: Focus, Analyze, Develop, Execute, and Evaluate (FADE) Model, and 3) HCT Framework: Got Transition Six Core Elements of Health Care Transition. The PARIHS framework comprises three components: evidence, context, and facilitation.26 Evidence must align with professionals’ and patients’ needs, clinical experience, patient experience, and local data.26 Context considers the environment where research is implemented, including culture, leadership, and evaluation.26 Facilitation involves individuals who support changing practices.26 The FADE model guides clinicians through creating improvement in a system using a data-driven team approach.27 Got Transition is a national resource supporting clinicians in promoting effective HCT operated by the National Alliance to Advance Adolescent Health.28 The Six Core Elements of Transition include policy, tracking and monitoring, readiness assessment, transition planning, transfer of care, and completion.28
1.4. Specific aims
The Standards for Quality Improvement Reporting Excellence (SQUIRE) guidelines, which provide a structured framework for reporting on QI initiatives in healthcare settings, were used to develop this manuscript. This QI initiative aimed to assess the effectiveness of the CAH-T program in addressing the HCT needs of adolescents diagnosed with CAH within a pediatric endocrine clinic in the southeastern United States. This initiative evaluated clinicians’ utilization and acceptance of the CAH-T program.
2. Materials and methods
2.1. Context
The pediatric endocrine clinic is in an urban southeastern US setting within a free-standing pediatric teaching hospital. As a state newborn screening collaborative site, the clinic serves over 85% of the state’s pediatric CAH population, many of whom are rural-dwelling. The clinic serves an estimated 90 patients with CAH, with approximately 30 adolescents between 12 and 19 years old. Adolescents with CAH are routinely followed in a multidisciplinary team clinic, including social workers, registered dieticians, and licensed family counselors familiar with pediatric endocrine conditions and their related HCT needs. While all clinical staff were trained on the CAH-T program, the clinicians surveyed in this initiative included physicians (board-certified pediatric Endocrinologists, pediatric endocrine fellows, and residents), certified registered nurse practitioners, registered nurses, and licensed practical nurses. Pediatric urology, pediatric/adolescent gynecology, pediatric surgery, pediatric psychology, and genetic/genetic counseling services are available for in-house consultation or referral. Lab and radiology services are housed on-site.
The pediatric endocrinology division holds regular multidisciplinary HCT task force meetings overseeing the introduction of various HCT services. This HCT task force asked for external support from a local Doctor of Nursing Practice (DNP) QI team in developing and implementing an evidence-based HCT program for adolescents with CAH, ensuring appropriate age-based preventative screening, referrals, and a streamlined transfer of care to adult services.
Planning for this initiative began in January 2023, with stakeholder meetings with the DNP team and HCT task force to develop the CAH-T intervention. The QI team implemented the initiative in June 2023, and data collection continued for three months. This project impacted children with CAH, but due to a limited data collection timeline, the initial outcome measure focused on the clinicians' program acceptance and utilization.
2.1.1. FADE model
The FADE model was used as the QI Framework for this project. [Focus] Within the identified pediatric endocrinology clinic, no standard approach guided the HCT of adolescents with CAH where providers assisting in HCT did not implement all clinical care guidelines, lacked organized transfers of care, and had difficulty ensuring ample time for each adolescent during appointments. [Analyze] Literature supports that having a standardized approach to HCT preparation for adolescents with CAH can improve self-efficacy, health-related outcomes, and quality of life.[15], [16], [17], [18] Within the identified clinic, patients with CAH have multidisciplinary support, including clinicians, dedicated social workers, licensed family counselors and registered dieticians. [Develop] A structured HCT program was developed as a collaborative effort between the external QI team and the internal HCT task force (see Section 2.2). [Execute] Clinicians within the identified clinic were educated on the CAH-T program and patient education materials in June 2023. The QI team collected data between June and August 2023 to evaluate clinician acceptance and utilization of the CAH-T program.
2.2. Intervention
2.2.1. CAH-T program development and training
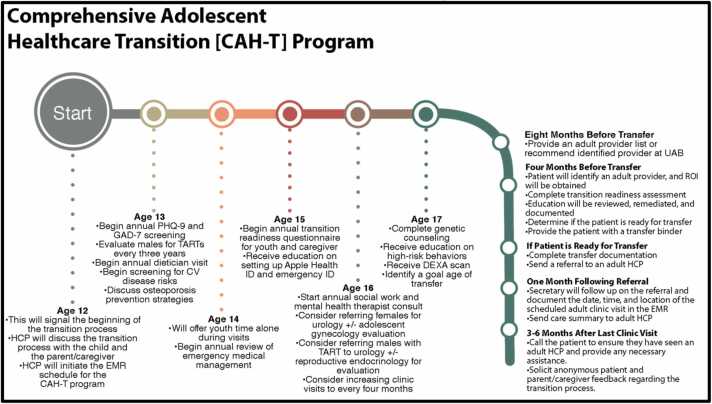
The CAH-T program was developed by a multidisciplinary QI team composed of three DNP nurses and a pediatric Endocrinologist using evidence-based CAH clinical care guidelines12 and CARES Foundation Comprehensive Care Center guidelines.11 The Got Transition Six Core Elements28 guided the CAH-T timing and process. Once the QI team established the interventions and timelines for the program, the pediatric endocrinology HCT task force and the primary local adult referral centers for individuals with CAH reviewed the program to ensure suitability and acceptability. After refining the program, the QI team developed a graphical display of CAH-T program interventions to guide clinicians in program adoption (Fig. 1). The CAH-T program comprehensively outlines approximately 50 interventions for individuals with CAH, beginning at 12 years of age and ending 3–6 months post-transfer to adult care (between the ages of 18 and 22). These interventions include preventative measures (i.e., testicular adrenal rest tumor screening, osteopenia prevention counseling, bone density evaluation), annual mental health screening, health counseling, transition readiness screening, referral to supportive services (pediatric urology, pediatric and adolescent gynecology, genetics), mental health counseling, social needs evaluation, emergency preparedness training, and care management streamlining the transfer between pediatric and adult services.
Fig. 1.
Comprehensive Adolescent Healthcare Transition [CAH-T] Program Overview. This flow diagram displays the steps clinicians should follow when providing transitional care to adolescents and emerging young adults. The program starts at age 12 and ends between ages 18 and 21, with evaluations at one month and three to six months after the transfer to adult care.
Next, the QI team developed patient education materials and reviewed and approved by the HCT task force to guide clinicians in supporting patients/families throughout the program. Education materials were written with a 5th-grade reading level and directed toward an adolescent audience. CAH-T education materials included handouts outlining the clinic’s HCT policy, a CAH-T program overview, mental health screening, cardiovascular and bone health screening, adolescent health, transition readiness, safety, preparing for college with CAH, what to expect guides for referrals to pediatric urology, pediatric/adolescent gynecology, and genetic counseling, emergency management plans and action plans for stress and emergency steroid dosing. The supplementary files contain unbranded patient education materials.
Following ethics approval, baseline measures were obtained (see Section 3.2), and the QI team educated the multidisciplinary team on the CAH-T program, patient education materials, and documentation of program implementation. The QI team members (JD and LP) led the training sessions offered during routine staff meetings in person and via Zoom.29 Three training sessions were held, with an average session length of 45 min. Clinicians who could not attend a live session could view the Zoom29 session recording. The QI team was available to answer any of the clinic staff’s questions. LP was also available in the clinic weekly for any questions or concerns that staff encountered throughout the implementation process.
2.2.2. Six core elements
2.2.2.1. Policy
The QI team and HCT task force collaboratively developed a transitional care policy. The clinic then implemented this policy, making it readily available to all staff, adolescent patients with CAH, and caregivers.
2.2.2.2. Tracking and monitoring
The QI team made efforts to implement patient/data tracking using the clinic's electronic medical record (EMR). However, due to a recent change in the EMR system, implementation was delayed beyond the project's initiation. Therefore, the QI team created an Excel file and uploaded it to a shared drive within the clinic for clinicians to document their program utilization. A registry of patients was already in place and used for tracking and monitoring upcoming appointments.
2.2.2.3. Readiness assessment
The QI team supplied the clinic with one-page HCT readiness surveys (for youth and parents/caregivers) adapted from Got Transition resources.28 These surveys discussed concepts about patients’ health knowledge, skills, and healthcare utilization.
2.2.2.4. Transition planning
Clinicians were coached on transition planning resources, including scheduled teaching sessions for patients on medical knowledge related to CAH, stress dosing, and adulthood preparedness (sexual/reproductive health, college/career support, mental health). In the program, patients were to receive consultations with dieticians, social workers, and a psychologist before transition to aid in transition preparation.
2.2.2.5. Transfer of care
The QI team provided a form letter to the clinicians for communication with adult providers before care transfer. An established clinic point person (nurse practitioner or social worker) ensured that adult-care appointments were made before the last pediatric appointment and communicated this information with patients/families. Additionally, all patients received a medical discharge record outlining their diagnosis, genetic testing history, and treatment (including maintenance and stress dosing) at the time of transfer. All patients were to be transferred to adult care by 22 years of age.
2.2.2.6. Completion
The clinic designated an established clinic administrative staff member to contact the patient/family to ensure that an adult-care appointment had taken place and to solicit feedback from the patient/family regarding the transition process 3–6 months after the last pediatric appointment.
3. Theory/calculation
3.1. Study of the intervention
The QI team used assessments available through Got Transition for the clinical implementation of HCT programs to evaluate this initiative.28 Due to time limitations, pilot data was obtained on the clinicians' acceptance and utilization of the CAH-T program. Psychometric properties for the Got Transition assessments have yet to be established, as these tools are designed for use in various patient populations and healthcare systems. In this project, the QI team selected tools to measure process changes within the healthcare setting specific to implementing the Six Core Elements of Transition and the CAH-T tool. Internal consistency measures were evaluated on the data collected within this project.
3.2. Measures
The “Current Assessment of Healthcare Transition Activities” and the “Health Care Transition Feedback Survey” were collected via Qualtrics30 at baseline and three months post-implementation. Responses were anonymous; therefore, subject-generated identification codes were used to pair within-subject responses. Clinicians were also allowed to complete only a pre-implementation or post-implementation survey.
3.2.1. Demographics
Clinician demographics data included age, sex, clinician category (nurses, nurse practitioners, physicians), work experience, and education.
3.2.2. Program utilization
Clinicians were asked to document patient encounters meeting criteria for the CAH-T program within a secure Excel spreadsheet saved to a shared clinic drive. Staff recorded the date of the encounter, the patient's age, and any CAH-T interventions occurring during that encounter. Staff also documented when a recommended intervention did not occur and provided a reason for the delayed intervention.
3.2.3. Current assessment of healthcare transition activities
This tool was obtained from Got Transition resources28 to measure the progress of implementing the six core HCT elements into practice. Within this project, this assessment identified the utilization of HCT services via the CAH-T program. This assessment consists of eight questions, scored from 1 to 4, with 1 representing basic utilization of program elements and 4 representing comprehensive utilization of program elements. Scores were measured for individual questions and summed for an overall score out of 32 possible points.28
3.2.4. Health care transition feedback survey
This tool was also obtained from Got Transition resources28 to measure clinician perceptions on the HCT process—specifically, the acceptance of HCT practice changes introduced through the utilization of the CAH-T program. This assessment consists of 14 positively worded four-point Likert scale questions regarding the practice’s culture and HCT process and one open-ended question soliciting feedback on improving the implementation of HCT into the clinic process. The Likert scale questions are scored from (1) strongly disagree, (2) disagree, (3) agree, and (4) strongly agree. Additionally, there is an option to abstain from answering if unsure. Scores were measured for individual questions and averaged for a cumulative score out of 4 possible points, where 4 indicated the highest regard for HCT implementation.28
3.3. Analysis
All statistical analyses were performed with IBM SPSS Statistics 29.0 (IBM Corp. Released 2022. IBM SPSS Statistics for Windows, Version 29.0. Armonk, NY: IBM Corp). Clinician demographics were analyzed using descriptive statistics with measures of central tendency for continuous variables and proportion for categorical variables. Nonparametric statistics were used to calculate differences of means (Mann-Whitney-U for unpaired data and Wilcoxon Signed Ranks Test for paired responses). Significance was determined using a two-tailed p-value of ≤ 0.05. Effect sizes were calculated using the r = Z/√(n1 + n2) formula. Cronbach’s alpha was tested for internal consistency.
3.4. Ethical considerations
Internal review board exemption was obtained before implementing this QI initiative. No identifiable patient information was collected. Clinicians were not obligated to participate in this project, and all who participated did so voluntarily. Clinician data was collected anonymously to protect privacy.
4. Results
4.1. Demographic data
Twenty-nine of thirty-three (87%) clinicians participated in this QI initiative. All participating clinicians were female, with the majority being between 31 and 40 years of age and having 0 to 5 years of experience. Clinicians were 51.7% nurses, 27.6% physicians, and 20.7% nurse practitioners. Most clinicians received training on the CAH-T program in person. Further demographic details are highlighted in Table 1.
Table 1.
Demographic Data.
| Variable | n (%) |
|---|---|
| Age | |
| 21-30 | 6 (20.7%) |
| 31-40 | 16 (55.2%) |
| 41-50 | 5 (17.2%) |
| 51-60 | 1 (3.4%) |
| 61-70 | 1 (3.4%) |
| Gender | |
| Male | 0 (0%) |
| Female | 29 (100%) |
| Role | |
| Nurse | 15 (51.7%) |
| Nurse Practitioner | 6 (20.7%) |
| Physician | 8 (27.6%) |
| Years of experience in pediatric endocrinology | |
| 0-5 | 21 (72.4%) |
| 6-10 | 7 (24.1%) |
| 11-15 | 0 (0%) |
| 16-20 | 0 (0%) |
| 21 or more | 1 (3.4%) |
| Education | |
| Associate degree | 7 (24.1%) |
| Bachelor’s degree | 7 (24.1%) |
| Master’s degree | 6 (20.7%) |
| Doctoral Degree | 8 (27.6%) |
| Manner educated on CAH-T program | |
| In-Person | 22 (75.9%) |
| Live on Zoom | 5 (17.2%) |
| Recorded on Zoom | 2 (6.9%) |
4.2. Clinical data
This project impacted eight patients between June and August 2023. Three additional patients were scheduled but did not attend clinic appointments during observation. The impacted patients’ ages ranged from 12–21 years. Clinicians documented 53 CAH-T-recommended interventions among the eight patients. One patient was transferred to an adult provider during the three-month observation period. Clinicians deferred 14 interventions due to time, staffing, and logistical constraints. Raw intervention documentation data is available in the supplementary materials.
4.3. Current assessment of healthcare transition activities scores (Clinician Utilization)
Seven clinicians completed paired assessments, five completed an unpaired pre-test, and four completed an unpaired post-test. Table 2, Table 3 demonstrate the paired and unpaired assessment data, significance levels, and effect sizes for individual assessment components and cumulative assessment scores. Paired scores indicate a cumulative baseline score of 15.29 ± 8.32 and a cumulative post-test score of 24 ± 6.11 (p = 0.018, r = 0.63). Unpaired data demonstrate a cumulative baseline score of 13.6 ± 5.13 and a cumulative post-test score of 23 ± 9.29 (p = 0.063, r = 0.62). A visual display of all pre-and post-test raw data is available in the supplemental materials. The pre-test Cronbach’s alpha was calculated at 0.94 (95% CI 0.87–0.98), and the post-test Cronbach’s alpha was calculated at 0.94 (95% CI 0.87–0.98).
Table 2.
Paired Data for Current Assessment of Healthcare Transition Activities.
| Question | Pre-assessment | Post-assessment | Significance | Effect size (r) |
|---|---|---|---|---|
| Assessments Completed | n1 = 7 | n2 = 7 | ||
| Transition and Care Policy/Guide | 2.00 ± 1.41 | 3.57 ± 0.53 | p = 0.041 * | 0.55 |
| Tracking and Monitoring | 1.57 ± 1.13 | 4.00 ± 0.00 | p = 0.020 * | 0.62 |
| Transition Readiness | 1.57 ± 1.13 | 2.86 ± 1.21 | p = 0.066 | 0.49 |
| Transition Planning | 2.43 ± 0.79 | 3.43 ± 0.79 | p = 0.038 * | 0.55 |
| Transfer of Care | 2.00 ± 1.16 | 2.71 ± 1.38 | p = 0.129 | 0.41 |
| Transfer Completion | 2.00 ± 1.16 | 2.57 ± 1.13 | p = 0.046 * | 0.53 |
| Feedback | 1.86 ± 1.46 | 2.43 ± 1.13 | p = 0.046 * | 0.53 |
| Stakeholder Involvement | 1.86 ± 1.46 | 2.43 ± 1.13 | p = 0.046 * | 0.53 |
| Cumulative Score | 15.29 ± 8.32 | 24.00 ± 6.11 | p = 0.018 * | 0.63 |
Scale 1 (basic) to 4 (comprehensive); cumulative score out of 32 total possible points
*Statistically significant with p < 0.05
Calculated using Wilcoxon Signed Ranks Test; Effect size calculated: r = Z/√(n1 +n2)
Table 3.
Unpaired data for current assessment of healthcare transition activities.
| Question | Pre- assessment | Post- assessment | Significance | Effect size (r) |
|---|---|---|---|---|
| Assessments Completed | n1 = 5 | n2 = 4 | ||
| Transition and Care Policy/Guide | 2.00 ± 1.41 | 3.25 ± 0.96 | p = 0.161 | 0.47 |
| Tracking and Monitoring | 1.40 ± 0.55 | 3.00 ± 1.41 | p = 0.093 | 0.56 |
| Transition Readiness | 1.40 ± 0.90 | 3.00 ± 1.41 | p = 0.078 | 0.59 |
| Transition Planning | 2.00 ± 0.71 | 3.25 ± 0.96 | p = 0.071 | 0.60 |
| Transfer of Care | 1.80 ± 0.84 | 2.83 ± 1.19 | p = 0.058 | 0.63 |
| Transfer Completion | 2.00 ± 0.71 | 2.75 ± 1.26 | p = 0.252 | 0.38 |
| Feedback | 1.60 ± 0.89 | 2.75 ± 1.26 | p = 0.152 | 0.48 |
| Stakeholder Involvement | 1.40 ± 0.55 | 2.50 ± 1.29 | p = 0.125 | 0.48 |
| Cumulative Score | 13.6 ± 5.13 | 23.00 ± 9.29 | p = 0.063 | 0.62 |
Scale 1 (basic) to 4 (comprehensive); cumulative score out of 32 total possible points
*Statistically significant with p < 0.05
Calculated using Mann-Whitney-U; Effect size calculated: r = Z/√(n1 +n2)
4.4. Health care transition feedback survey for clinicians (Clinician Acceptance)
Eight clinicians completed paired assessments, five completed an unpaired pre-test, and four completed an unpaired post-test. Table 4, Table 5 demonstrate the paired and unpaired assessment data, significance levels, and effect sizes for individual assessment components and average total assessment scores. Paired scores indicate an average total baseline score of 2.75 ± 0.26 and an average total post-test score of 3.30 ± 0.43 (p = 0.018, r = 0.59). Unpaired data demonstrate an average total baseline score of 2.94 ± 0.26 and an average total post-test score of 3.48 ± 0.42 (p = 0.063, r = 0.64). Visual displays of all pre-and post-test raw data are available in the supplemental materials. The pre-test Cronbach’s alpha was calculated at 0.74 (95% CI 0.54–0.93), and the post-test Cronbach’s alpha was calculated at 0.91 (95% CI 0.82–0.97).
Table 4.
Paired data for healthcare transition feedback survey for clinicians.
| Question | n1 | Pre-Test Score | n2 | Post-Test Score | Significance | Effect Size (r) |
|---|---|---|---|---|---|---|
| Our practice takes time to consider ways to improve the HCT process. | 6 | 2.83 ± 0.75 | 7 | 3.71 ± 0.49 | p = 0.102 | 0.45 |
| Our practice encourages everyone (front office and clinical staff) to share ideas about their role in the HCT process. | 8 | 2.50 ± 0.76 | 8 | 3.13 ± 0.84 | p = 0.025 * | 0.56 |
| Our practice has successfully gained senior leadership buy-in for our HCT quality improvement effort. | 5 | 3.00 ± 0.00 | 5 | 3.60 ± 0.55 | p = 0.157 | 0.45 |
| Our practice leadership ensures we have the time and resources to plan for and implement changes to improve the HCT process. | 8 | 2.88 ± 0.64 | 7 | 3.29 ± 0.76 | p = 0.083 | 0.45 |
| Our practice has incorporated a structured HCT process into our workflow. | 7 | 2.57 ± 0.54 | 6 | 3.50 ± 0.55 | p = 0.059 | 0.52 |
| Front office and clinical staff operate as a team to implement the HCT process. | 8 | 2.38 ± 0.75 | 7 | 2.86 ± 0.70 | p = 0.083 | 0.45 |
| Youth/Young adults and parents/caregivers are valued partners in our HCT planning and quality improvement efforts. | 7 | 2.57 ± 0.54 | 8 | 3.25 ± 0.46 | p = 0.025 * | 0.58 |
| Having an HCT process in place in our practice improves safety and quality of care. | 8 | 3.38 ± 0.52 | 8 | 3.63 ± 0.52 | p = 0.317 | 0.25 |
| Having an HCT process in place in our practice improves youth/young adult and parent/caregiver experience. | 7 | 3.29 ± 0.49 | 7 | 3.71 ± 0.49 | p = 0.083 | 0.46 |
| Having an HCT process in place in our practice improves the clinician experience. | 8 | 3.25 ± 0.46 | 7 | 3.57 ± 0.53 | p = 0.157 | 0.36 |
| The HCT process we are currently using works for our practice. | 6 | 2.50 ± 0.55 | 7 | 3.14 ± 0.70 | p = 0.102 | 0.45 |
| Having an HCT process in place in our practice saves time for our clinicians. | 7 | 3.00 ± 0.58 | 5 | 3.80 ± 0.45 | p = 0.102 | 0.47 |
| Our practice has been successful in obtaining payment for HCT services. | 2 | 2.50 ± 0.71 | 4 | 3.50 ± 0.58 | * * | * * |
| Our practice has been successful in modifying our electronic medical records to incorporate HCT. | 6 | 2.33 ± 0.52 | 5 | 2.6 ± 0.55 | p = 0.317 | 0.30 |
| Cumulative Score | 8 | 2.75 ± 0.26 | 8 | 3.30 ± 0.43 | p = 0.018 * | 0.59 |
1 = strongly disagree; 2 = disagree; 3 = agree; 4 = strongly agree
*Statistically significant with p < 0.05; * *unable to calculate
Calculated using Wilcoxon Signed Ranks Test; Effect size calculated: r = Z/√(n1 +n2)
Table 5.
Unpaired data for healthcare transition feedback survey for clinicians.
| Question | n1 | Pre-Test Score | n2 | Post-Test Score | Significance | Effect Size (r) |
|---|---|---|---|---|---|---|
| Our practice takes time to consider ways to improve the HCT process. | 5 | 3.20 ± 0.45 | 4 | 3.64 ± 0.58 | p = 0.371 | 0.30 |
| Our practice encourages everyone (front office and clinical staff) to share ideas about their role in the HCT process. | 5 | 2.60 ± 0.55 | 4 | 3.50 ± 0.58 | p = 0.058 | 0.63 |
| Our practice has successfully gained senior leadership buy-in for our HCT quality improvement effort. | 5 | 3.40 ± 0.55 | 3 | 3.33 ± 0.58 | p = 0.860 | 0.06 |
| Our practice leadership ensures we have the time and resources to plan for and implement changes to improve the HCT process. | 3 | 3.00 ± 0.00 | 4 | 3.25 ± 0.50 | p = 0.386 | 0.33 |
| Our practice has incorporated a structured HCT process into our workflow. | 5 | 2.60 ± 0.55 | 4 | 3.25 ± 0.50 | p = 0.107 | 0.54 |
| Front office and clinical staff operate as a team to implement the HCT process. | 4 | 2.25 ± 0.96 | 4 | 3.00 ± 0.82 | p = 0.278 | 0.38 |
| Youth/Young adults and parents/caregivers are valued partners in our HCT planning and quality improvement efforts. | 5 | 3.00 ± 0.00 | 4 | 3.50 ± 0.58 | p = 0.091 | 0.56 |
| Having an HCT process in place in our practice improves safety and quality of care. | 5 | 3.20 ± 0.48 | 4 | 3.75 ± 0.50 | p = 0.120 | 0.52 |
| Having an HCT process in place in our practice improves youth/young adult and parent/caregiver experience. | 5 | 3.20 ± 0.45 | 4 | 3.75 ± 0.50 | p = 0.120 | 0.52 |
| Having an HCT process in place in our practice improves the clinician experience. | 5 | 3.00 ± 0.71 | 4 | 3.75 ± 0.50 | p = 0.107 | 0.54 |
| The HCT process we are currently using works for our practice. | 3 | 2.67 ± 0.58 | 4 | 3.50 ± 0.58 | p = 0.115 | 0.60 |
| Having an HCT process in place in our practice saves time for our clinicians. | 5 | 3.00 ± 0.71 | 3 | 3.67 ± 0.58 | p = 0.191 | 0.46 |
| Our practice has been successful in obtaining payment for HCT services. | 2 | 3.00 ± 0.00 | 2 | 4.00 ± 0.00 | p = 0.083 | 0.87 |
| Our practice has been successful in modifying our electronic medical records to incorporate HCT. | 2 | 3.00 ± 0.00 | 2 | 4.00 ± 0.00 | p = 0.083 | 0.87 |
| Cumulative Score | 5 | 2.94 ± 0.26 | 4 | 3.48 ± 0.42 | p = 0.063 | 0.64 |
1 = strongly disagree; 2 = disagree; 3 = agree; 4 = strongly agree
*Statistically significant with p < 0.05
Calculated using Mann-Whitney-U; Effect size calculated: r = Z/√(n1 +n2).
4.5. Qualitative feedback
The post-intervention Health Care Transition Feedback Survey for Clinicians included two optional open-ended questions: 1) What are the barriers to successfully implementing HCT for patients with CAH? and 2) Do you have any ideas to better implement HCT into the clinic process? Nine clinicians (75%) responded to question one, and seven (58%) responded to question two. Four respondents (44%) reported that time limitations were the most significant barrier to implementing the CAH-T. Other reported barriers to implementation included having English-only materials available (n = 1, 11%), the need for EMR integration to track HCT progress (n = 2, 22%), and patient nonattendance in clinic (n = 2, 22%). Reported facilitators to implementation of the CAH-T included having a coordinated plan (n = 2, 28.5%), transition tools, and patient education materials (n = 2, 28.5%). Clinicians reported that having a policy and protocol for HCT increased awareness and enabled the implementation of workflow changes (n = 2, 28.5%).
5. Discussion
5.1. Summary
This QI initiative demonstrates the feasibility of implementing an evidence-based HCT program for AYAs with CAH. Though clinical indicators of patient outcomes will not be evident for some time, this project exhibited favorable clinician acceptance and utilization. Clinician engagement was greatest among nursing staff, though physician and advanced practice provider support was also evident. HCT requires interdisciplinary collaboration, with nurses providing many HCT services in specialty-care settings.31 Nurses often provide education, advocacy, and support for adolescents and young adults as they navigate HCT. However, most pediatric nurses providing this care need specialized training in HCT services.31 Including interdisciplinary input and providing education on HCT services to various clinicians is critical to the overall success of the implementation of HCT programs.
5.2. Interpretation
Many participating clinicians had less than five years of experience in endocrine practice, and several reported an increased desire for clear guidelines, HCT policies, transition tools, and patient education materials. These findings represent the needs of early-career clinicians and specialty-practice nurses. Research also advocates for enhanced HCT training, guidelines, and tools for interdisciplinary clinicians in pediatric and adult settings.[14], [32], [33] Future studies exploring the relationships between the barriers and facilitators of HCT program implementation and clinician role and experience level are needed, as these factors likely influence the uptake of practice changes.
Clinical data from this initiative substantiates the complexity of HCT preparation among adolescents and young adults with CAH, with 53 interventions implemented among eight patients. Additionally, clinicians documented the need to delay eleven interventions until future appointments, citing a lack of time for health counseling/transition education within clinical encounters. Time constraints were the most frequently cited barrier to program implementation among participating clinicians. This concern highlights the need for HCT to be an ongoing process with clearly outlined goals for each progressing age. Furthermore, securing reimbursement for HCT services would afford clinicians the additional time necessary to provide adequate support for adolescents, young adults, and their parents/caregivers throughout the HCT process.34 These findings are consistent with previously reported barriers to HCT program implementation14 and underscore the need for improved reimbursement models for HCT services.34
The “Current Assessment of Healthcare Transition Activities” assessment quantified the utilization of the Got Transition Six Core Elements of Transition. Data revealed that the implementation of the CAH-T program and education on HCT for this patient population promoted uptake of the Got Transition Six Core Elements, with many individual aspects of this assessment (policy/guide, tracking and monitoring, transition planning, transfer completion, feedback, and stakeholder involvement) reaching a clinically meaningful rate of change within paired and unpaired responses.
The “Healthcare Transition Feedback Survey for Clinicians” quantified the participating clinicians' beliefs and values (acceptance) regarding HCT services. The response rates for individual questions varied among participants. This observation may indicate that clinicians could not discern the intended meaning of the item, did not feel they had enough experience to respond to an item, or could not respond to the item with the given categories of responses.35 Missing data likely also contributed to the lower internal consistency of the pre-test; however, this phenomenon was not noted in post-test scores, which may be due to test-retest bias.36
Items with the highest nonresponse rates elicited information regarding payment for HCT services and implementation within the EMR. Within this QI project, EMR implementation of the CAH-T program was not feasible due to the recent implementation of a new EMR system within the hospital. Plans are in place for the CAH-T program to be implemented within the EMR for patient tracking and documentation of HCT services. Payment for HCT services demonstrates an area for increased clinician education. Resources for HCT reimbursement are available through the Got Transition website to educate clinic staff on billing codes for HCT services.37
Participating clinicians experienced increased acceptance of HCT as a valuable aspect of pediatric endocrine care for AYAs with CAH. Responses indicated clinically relevant increases in individual elements of the assessment (involving all staff in the HCT process and partnering with adolescents, young adults, and their families in HCT efforts). These findings underscore the effectiveness of developing an HCT plan using clinical guidelines and Got Transition resources in increasing clinician awareness and utilization of HCT services and support.
5.3. Limitations
This initiative faced several limitations. One major limitation was the project timeline, which was constrained to three months of intervention observation. Given the infrequency of CAH patient encounters (often two-three visits per year in adolescence), three months limited the opportunity for patient-program interactions. Ideally, an extended period would be allocated for increased clinician experience and patient-program interactions. However, as with any QI initiative, this small test of change offers the opportunity to reflect on the positive and negative aspects of the program to improve the process going forward. Results at this stage show a clear benefit and positive change; therefore, clinic staff will continue to monitor patient-program interactions to determine the long-term implications as the program continues.
Furthermore, due to the restricted timeline of this initiative, input was limited to clinicians, which limited the sample size. This data reduction necessitates using nonparametric analysis, which provides less robust data. Expanding on this work, feedback from adolescents and young adults with CAH, parents/caregivers, and clinicians would give a more expansive understanding of the program’s benefit within the population and health system. The findings from this work support continued observation of program outcomes due to clinically relevant results despite the small sample size. However, findings from this pilot initiative should not be generalized beyond the study sample.
Another noteworthy limitation of this study was the need for EMR integration. Due to institutional and technology support challenges, the QI team and HCT task force were unsuccessful at implementing this in a seamless documenting center, necessitating clinicians to use an external file to document patient encounters/interventions. Although this made the program possible in the clinic, this decision increased the clinician documentation burden and was reported as a barrier to program implementation. In the future, the program will be implemented into their EMR, easing clinician burden.
Additionally, the lack of validation associated with the assessments provided by Got Transition was a limitation. While these tools are designed to be customizable to meet the specific needs within a given practice or system, their psychometric properties have not been internally or externally validated.28 The assessments used for this initiative are intended to evaluate clinicians’ current HCT beliefs and practices within a healthcare system. These assessments can be used to identify areas within the Six Core Elements of HCT that are proving difficult to implement and areas of successful implementation; however, their use should be interpreted with caution, recognizing that these measurement tools do not predict or ensure successful transition outcomes.
Research is needed to support the transition needs of AYAs with CAH, their parents/caregivers, and the pediatric and adult clinicians caring for this population. Several clinical guidelines for supporting HCT in CAH populations have yet to be adequately researched, with many based on clinical observation.12 Understanding what interventions are needed in the pediatric setting to better support adult outcomes with CAH is critical to reducing long-term morbidity and mortality in this condition.
6. Conclusion
This QI initiative is the first to implement an evidence-based program, framed with Got Transition’s Six Core Elements of HCT, for a population of adolescents and young adults with CAH in the US. Though clinical guidelines for CAH advocate for comprehensive multidisciplinary support, research on HCT for individuals with CAH remains limited, and this remains a problematic area of care delivery for many institutions. By offering an example program that is both feasible and acceptable to clinicians and supported by the free resources available through Got Transition, we hope that more centers can implement similar processes to improve adolescent and young adult support for individuals with CAH.
Funding
This work was supported by funding from the University of Alabama at Birmingham’s Graduate Blazer Fellowship and the Alabama League for Nursing’s Doctoral Nursing Scholarship, supporting project dissemination.
Ethical statement
Internal review board exemption was obtained before implementing this QI project. No patient information was collected as part of this initiative. Clinicians were not obligated to participate in this project, and all who participated did so voluntarily. Clinician data was collected anonymously to protect privacy.
CRediT authorship contribution statement
Lauren Mays: Writing – review & editing, Validation, Project administration, Methodology, Conceptualization. Leen Matalka: Writing – review & editing, Validation, Supervision, Project administration. Leslie Pitts: Writing – review & editing, Writing – original draft, Project administration, Methodology, Investigation, Funding acquisition, Formal analysis, Data curation, Conceptualization. Jocelyn Dennis: Writing – review & editing, Writing – original draft, Methodology, Investigation, Funding acquisition, Formal analysis, Data curation, Conceptualization.
Declaration of Competing Interest
The authors declare the following financial interests/personal relationships which may be considered as potential competing interests: Jocelyn Dennis, Leslie Pitts, Leen Matalka, and Lauren Mays reports financial support was provided by Alabama League of Nursing. Leslie Pitts reports a relationship with Eton Pharmaceuticals Inc that includes: consulting or advisory, speaking and lecture fees, and travel reimbursement. Leslie Pitts, previously employed by Children’s of Alabama Pediatric Endocrinology Clinic. Leen Matalka is currently employed as an attending physician at Children’s of Alabama Pediatric Endocrinology Clinic.
Footnotes
Supplementary data associated with this article can be found in the online version at doi:10.1016/j.hctj.2024.100057.
Appendix A. Supplementary material
Supplementary material
.
Data availability
Data will be made available on request.
References
- 1.Bachelot A. Transition of care from childhood to adulthood: congenital adrenal hyperplasia. Endocr Dev. 2018;33:17–33. doi: 10.1159/000487523. [DOI] [PubMed] [Google Scholar]
- 2.Claahsen-van der Grinten H.L., Speiser P.W., Ahmed S.F., et al. Congenital adrenal hyperplasia-Current insights in pathophysiology, diagnostics, and management. Endocr Rev. 2022;43(1):91–159. doi: 10.1210/endrev/bnab016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Witchel S.F. Congenital adrenal hyperplasia. J Pedia Adolesc Gynecol. 2017;30(5):520–534. doi: 10.1016/j.jpag.2017.04.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Navarro-Zambrana A.N., Sheets L.R. Ethnic and national differences in congenital adrenal hyperplasia incidence: a systematic review and meta-analysis. Horm Res Paediatr. 2022 doi: 10.1159/000526401. [DOI] [PubMed] [Google Scholar]
- 5.Chawla R., Rutter M., Green J., Weidler E.M. Care of the adolescent patient with congenital adrenal hyperplasia: special considerations, shared decision making, and transition. Semin Pedia Surg. 2019;28(5) doi: 10.1016/j.sempedsurg.2019.150845. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Choi J.-H., Yoo H.-W. Management issues of congenital adrenal hyperplasia during the transition from pediatric to adult care. Korean J Pedia. 2017;60(2):31–37. doi: 10.3345/kjp.2017.60.2.31. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Arlt W., Willis D.S., Wild S.H., et al. United Kingdom Congenital Adrenal Hyperplasia Adult Study Executive (CaHASE) Health status of adults with congenital adrenal hyperplasia: a cohort study of 203 patients. J Clin Endocrinol Metab. 2010;95(11):5110–5121. doi: 10.1210/jc.2010-0917. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Fleming L., Van Riper M., Knafl K. Management of childhood congenital adrenal hyperplasia-an integrative review of the literature. J Pedia Health Care. 2017;31(5):560–577. doi: 10.1016/j.pedhc.2017.02.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Jenkins-Jones S., Parviainen L., Porter J., et al. Poor compliance and increased mortality, depression and healthcare costs in patients with congenital adrenal hyperplasia. Eur J Endocrinol. 2018;178(4):309–320. doi: 10.1530/EJE-17-0895. [DOI] [PubMed] [Google Scholar]
- 10.Merke D.P., Poppas D.P. Management of adolescents with congenital adrenal hyperplasia. Lancet Diabetes Endocrinol. 2013;1(4):341–352. doi: 10.1016/S2213-8587(13)70138-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Auchus R.J., Witchel S.F., Leight K.R., et al. Guidelines for the development of comprehensive care centers for congenital adrenal hyperplasia: guidance from the CARES Foundation initiative. Int J Pedia Endocrinol. 2010;2010 doi: 10.1155/2010/275213. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Speiser P.W., Arlt W., Auchus R.J., et al. Congenital adrenal hyperplasia due to steroid 21-hydroxylase deficiency: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2018;103(11):4043–4088. doi: 10.1210/jc.2018-01865. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Parsons H.M., Abdi H.I., Nelson V.A., et al. Agency for Healthcare Research and Quality (US); 2022. Transitions of care from pediatric to adult services for children with special healthcare needs. [DOI] [PubMed] [Google Scholar]
- 14.White P.H., Cooley W.C. Transitions Clinical Report Authoring Group, American Academy Of Pediatrics, American Academy Of Family Physicians, American College Of Physicians. Supporting the health care transition from adolescence to adulthood in the medical home. Pediatrics. 2018;142(5) doi: 10.1542/peds.2018-2587. [DOI] [PubMed] [Google Scholar]
- 15.Bachelot A., Vialon M., Baptiste A., et al. Impact of transition on quality of life in patients with congenital adrenal hyperplasia diagnosed during childhood. Endocr Connect. 2017;6(7):422–429. doi: 10.1530/EC-17-0094. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Le Roux E., Menesguen F., Tejedor I., et al. Transition of young adults with endocrine and metabolic diseases: The “TRANSEND” cohort. Endocr Connect. 2021;10(1):21–28. doi: 10.1530/EC-20-0520. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Twito O., Shatzman-Steuerman R., Dror N., et al. The “combined team” transition clinic model in endocrinology results in high adherence rates and patient satisfaction. J Pedia Endocrinol Metab. 2019;32(5):505–511. doi: 10.1515/jpem-2019-0056. [DOI] [PubMed] [Google Scholar]
- 18.Godbout A., Tejedor I., Malivoir S., et al. Transition from pediatric to adult healthcare: assessment of specific needs of patients with chronic endocrine conditions. Horm Res Paediatr. 2012;78(4):247–255. doi: 10.1159/000343818. [DOI] [PubMed] [Google Scholar]
- 19.Gleeson H., Davis J., Jones J., et al. The challenge of delivering endocrine care and successful transition to adult services in adolescents with congenital adrenal hyperplasia: Experience in a single centre over 18 years. Clin Endocrinol. 2013;78(1):23–28. doi: 10.1111/cen.12053. [DOI] [PubMed] [Google Scholar]
- 20.Davidse K., van Staa A., Geilvoet W., et al. We mind your step: understanding and preventing drop-out in the transfer from paediatric to adult tertiary endocrine healthcare. Endocr Connect. 2022;11(5) doi: 10.1530/EC-22-0025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Downing J., Gleeson H., Clayton P.E., et al. Communication with young people in paediatric and adult endocrine consultations: an intervention development and feasibility study. BMC Endocr Disord. 2017;17(1):33. doi: 10.1186/s12902-017-0182-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Ekbom K., Lajic S., Falhammar H., Nordenström A. Transition readiness in adolescents and young adults living with congenital adrenal hyperplasia. Endocr Pr. 2023;29(4):266–271. doi: 10.1016/j.eprac.2023.01.010. [DOI] [PubMed] [Google Scholar]
- 23.Cooley W.C., Sagerman P.J., American Academy of Pediatrics, American Academy of Family Physicians, American College of Physicians, Transitions Clinical Report Authoring Group Supporting the health care transition from adolescence to adulthood in the medical home. Pediatrics. 2011;128(1):182–200. doi: 10.1542/peds.2011-0969. [DOI] [PubMed] [Google Scholar]
- 24.Schwartz L.A., Tuchman L.K., Hobbie W.L., Ginsberg J.P. A social-ecological model of readiness for transition to adult-oriented care for adolescents and young adults with chronic health conditions. Child Care Health Dev. 2011;37(6):883–895. doi: 10.1111/j.1365-2214.2011.01282.x. [DOI] [PubMed] [Google Scholar]
- 25.Bergström A., Ehrenberg A., Eldh A.C., et al. The use of the PARIHS framework in implementation research and practice-A citation analysis of the literature. Implement Sci. 2020;15(1):68. doi: 10.1186/s13012-020-01003-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Rycroft-Malone J. The PARIHS framework--a framework for guiding the implementation of evidence-based practice. J Nurs Care Qual. 2004;19(4):297–304. doi: 10.1097/00001786-200410000-00002. [DOI] [PubMed] [Google Scholar]
- 27.Wiseman B., Kaprielian V.S., Josie King Foundation. What is quality improvement?. Accessed March 21, 2023. 〈https://josieking.org/patientsafety/module_a/methods/fade.htm〉.
- 28.White P., Schmidt A., Ilango S., et al Six core elements of health care transition 3.0: An implementation guide. Got Transition, The National Alliance to Advance Adolescent Health. Published July 2020. Accessed October 31, 2022. 〈https://gottransition.org/6ce/?leaving-ImplGuide-full〉.
- 29.Zoom Video Communications, Inc. Zoom. Published 2024. Accessed February 27, 2024. 〈https://www.zoom.us/〉.
- 30.Qualtrics. Qualtrics XM. Published 2024. Accessed February 26, 2024. 〈https://www.qualtrics.com/〉.
- 31.Disabato J.A., Mannino J.E., Betz C.L. Pediatric nurses’ role in health care transition planning: National survey findings and practice implications. J Pedia Nurs. 2019;49:60–66. doi: 10.1016/j.pedn.2019.08.003. [DOI] [PubMed] [Google Scholar]
- 32.Okumura M.J., Kuo D.Z., Ware A.N., et al. Improving health care transitions for children and youth with special health care needs. Acad Pedia. 2022;22(2S):S7–S13. doi: 10.1016/j.acap.2021.03.014. [DOI] [PubMed] [Google Scholar]
- 33.Betz C.L. Health care transition for adolescents with special healthcare needs: where is nursing? Nurs Outlook. 2013;61(5):258–265. doi: 10.1016/j.outlook.2012.08.009. [DOI] [PubMed] [Google Scholar]
- 34.Calabrese S., Lee S., Mollica M.A., et al. Navigating pediatric to adult healthcare transition: a national institutes of health workshop. J Pedia. 2022;244:234–240.e1. doi: 10.1016/j.jpeds.2022.01.052. [DOI] [PubMed] [Google Scholar]
- 35.de Leeuw E.D., Hox J., Huisman M. Prevention and treatment of item nonresponse. J Stat. 2003;19(2):153–176. [Google Scholar]
- 36.Rettig T., Blom A.G. In: Measurement Error in Longitudinal Data. Oxford University Press; 2021. Memory effects as a source of bias in repeated survey measurement; pp. 3–18. [DOI] [Google Scholar]
- 37.Schmidt A., McManus M., White P. The National Alliance to Advance Adolescent Health. Am Acad Pediatr 2023 Coding Paym Tip Sheet Transit Pediatr adult Health care. 2023 〈https://www.gottransition.org/resource/?2023-coding-tip-sheet〉 Published August 2023. Accessed September 15. [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplementary material
Data Availability Statement
Data will be made available on request.