Abstract
Healthy working-age adults are susceptible to illness or caregiving requirements resulting from annual seasonal influenza, leading to considerable societal and economic impacts. The objective of this targeted narrative review is to understand the societal burden of influenza in terms of absenteeism and productivity loss, based on the current literature. This review includes 48 studies on the impact of influenza and influenza-like illness (ILI) and reports on the effect of influenza vaccination, age, disease severity, caring for others, comorbidities, and antiviral prophylaxis on absenteeism and productivity loss due to influenza/ILI, focusing on publications originating from Canada, Europe, and the United States. Influenza/ILI results in substantial work time and productivity loss among working adults and students in Canada, Europe, and the United States, particularly those who are unvaccinated, are <65 years of age, or who have severe disease. Considerable work time and productivity loss is attributable to illness and caregiver burden related to influenza. Further research is required on the impact of influenza on absenteeism and productivity loss in adults with comorbidities to support the development of effective employer policies for working adults with underlying health conditions.
Keywords: absenteeism, caregivers, indirect cost, influenza, influenza-like illness, productivity loss
1. Introduction
Seasonal influenza epidemics affect a substantial proportion of the working-age population [1]. Annually, there are up to 50 million cases of influenza in Europe and 41 million cases in the United States [2,3]. Healthy adults are less susceptible to severe outcomes of influenza than older age groups, young children, and people with underlying health conditions [4,5]. However, they may still be affected by symptoms of influenza, including fever, cough, sore throat, runny nose, muscle and joint pain, and fatigue, resulting in absence from work [4,5]. Symptoms can last up to 1 week, although fatigue and cough may persist after other symptoms have resolved [4,5]. Healthy adults may also need to take time off work to care for family members with influenza infection [1]. Although people with influenza may be advised to stay at home while symptomatic to avoid transmission to others, employees may attend work while ill [6]. Presenteeism provides an opportunity to spread influenza and is associated with lost productivity from working at a reduced capacity due to the effects of illness [6,7].
Influenza virus infection is confirmed by laboratory testing. Clinical differentiation of influenza from other respiratory virus infections is difficult [4]. Thus, many studies on absenteeism and productivity loss assess influenza-like illness (ILI), either physician- or self-reported, based on the presence of a distinct set of symptoms. Although less precise than studies on confirmed influenza, data on ILI can also inform our understanding of the impact of influenza on working adults.
A recent systematic review highlighted a substantial productivity burden of influenza on the global workforce, noting that most employees still go to work with symptoms of influenza [8]. Furthermore, up to 75% of employees missed work due to influenza or ILI, and up to 75% of employed caregivers missed work to care for a household member with influenza or ILI. Therefore, the societal and economic impacts of absenteeism and productivity loss due to influenza illness and ILI are considerable [1].
The objective of this targeted narrative review is to understand the indirect burden of influenza in terms of absenteeism and productivity loss, based on the current literature, focusing on Canada, Europe, and the United States. The effects of influenza vaccination, age, disease severity, caring for others, comorbidities, and antiviral prophylaxis on absenteeism and productivity loss due to influenza/ILI were also evaluated.
2. Methods
Targeted Literature Search
A targeted literature search using PubMed was performed on 11 October 2023. Search terms were as follows: influenza, productivity, presentee*, absent*, loss, lost, school, work, indirect cost, and production. English language articles published since 1 January 2000, were included. Inclusion criteria were applied to the search results in a three-stage process (stage 1: review of titles; stage 2: review of abstracts; stage 3: review of full text). Articles were included if they contained data on seasonal influenza or ILI, data from Canada, Europe, or the United States, and data on at least one pre-defined outcome of interest. Pre-defined outcomes of interest were as follows: work time lost due to influenza/ILI, productivity loss due to influenza/ILI while at work, cost of work loss due to influenza/ILI, and work loss for the care of others. The review was limited to countries in North America and Europe due to similarities in income level, vaccination programs, and healthcare systems, in order to minimize bias. Editorials and opinion articles were excluded.
Inclusion criteria were applied and data were extracted by a single reviewer. Evidence was not graded for quality. Articles meeting the inclusion criteria were grouped by pre-defined outcomes of interest, as well as by the definition of influenza or ILI used, and the population studied (general adult working populations or specific populations, such as healthcare workers [HCWs]). Data on the impact of vaccination status, age, disease severity, comorbidities, and the use of antiviral prophylaxis on these outcomes were also extracted. No specific research hypothesis was defined, and no conceptual framework was used.
3. Results
The literature search returned 507 articles, of which 59 met the inclusion criteria. Of these, studies that contained data on absenteeism in school children alone (n = 19) were excluded (Figure 1). The remaining 40 articles included 39 original articles and one narrative review. A further eight articles were retrieved from the reference list of the narrative review article [1], leading to a total of 48 articles for inclusion in the final analysis.
Figure 1.
Literature search process.
3.1. Absenteeism Due to Influenza/ILI
3.1.1. General Adult Populations
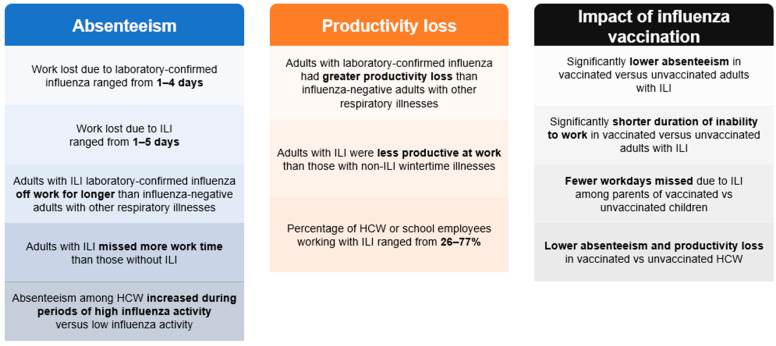
Studies assessing work loss due to influenza/ILI are shown in Table 1. Six studies assessed work loss due to laboratory-confirmed influenza [9,10,11,12,13,14]. Across these studies, the average days of work lost ranged from 1 to 4 (Figure 2) [11,12,13,14]. In studies that compared work time lost among people with laboratory-confirmed influenza and those who tested negative for influenza, people with confirmed influenza were off work for longer [9,11,13]. In England, among working adults (16–64 years of age), those with influenza A took more time off work or education than those who tested negative for influenza and had ILI or acute respiratory infection (ARI; 34% versus 30% and 12%). Time off work due to influenza B was close to that for influenza A and ILI (33%) [11]. In Italy, among parents of 962 children < 15 years of age, parents of children with confirmed influenza took more time off work than those with children with confirmed respiratory syncytial virus (RSV) infection (4 and 3 days of work lost by mothers and fathers of children with influenza, respectively, compared with 2 and 1 days for RSV; p < 0.05) [12].
Table 1.
Studies on work loss due to influenza/ILI.
| Publication | Location | Time Period | Study Design and Participants | Definition of Illness | Results |
|---|---|---|---|---|---|
| General adult populations: laboratory-confirmed influenza | |||||
| Petrie et al., 2016 [9] | United States | 2012–2013 | Prospective study of working adults (N = 1548) | Laboratory-confirmed influenza versus influenza-negative |
|
| Van Wormer et al., 2017 [10] | United States | 2012–2016 | Analysis of data from participants in vaccine effectiveness studies (N = 1278) | PCR-confirmed influenza-positive versus confirmed influenza-negative people with ARI |
|
| Fragaszy et al., 2018 [11] | England | 2006–2011 | Community cohort study (N = 2919) | PCR-confirmed influenza |
|
| Esposito et al., 2005 [12] | Italy | 2002–2003 | Prospective study of children attending emergency department (N = 1520) and their families | Laboratory-confirmed influenza |
|
| Principi et al., 2003 [13] | Italy | 2001–2002 | Study of children presenting to emergency department (N = 3771) and their household contacts | Laboratory-confirmed influenza |
|
| Carrat et al., 2002 [14] | France | 2000 | Household contact study | Laboratory-confirmed influenza |
|
| General adult populations: physician-diagnosed | |||||
| Karve et al., 2013 [15] | United States | 2000–2009 | Retrospective analysis of employee data from MarketScan databases | Influenza-related medical encounters with temporal co-occurrence of workplace absence |
|
| Karve et al., 2013 [16] | United States | 2005–2009 | Retrospective analysis of employee data from MarketScan databases | ≥1 medical claim with diagnosis of influenza |
|
| De Blasio et al., 2012 [17] | Norway | 2005–2010 | National registry data on GP-certified sick leave | ICPC-2 diagnosis of influenza (R80) |
|
| General adult populations: ILI | |||||
| Nettleman et al., 2001 [18] | United States | 1997–1998 | Survey of parents of schoolchildren (N = 954) | Respiratory illness, excluding asthma |
|
| Neuzil et al., 2002 [19] | United States | 2000–2001 influenza season | Survey of parents of school children (N = 216) | Fever, coryza, sore throat, cough, myalgia, earache, headache, nausea, vomiting, diarrhea |
|
| Akazawa et al., 2003 [20] | United States | January–July 1996 | Medical Expenditure Panel Survey Household component data (N = 7037) | ILI |
|
| Carrat et al., 2004 [21] | France | 1999–2000 influenza season | Observational household contact study (N = 701) | ILI |
|
| Nichol et al., 2005 [22] | United States | October 2002–April 2003 | Cohort study of college students (N = 4919) | ILI |
|
| Li et al., 2007 [23] | United States | 1996–2002 | Medical Expenditure Panel Survey (N = 12,850 households) | ILI |
|
| Palmer et al., 2010 [24] | United States | 2007–2008 influenza season | Observational cohort study of employees (N = 2013) | ILI (modified CDC definition) |
|
| De Perio et al., 2014 [25] | United States | 2013 | Survey of school employees (N = 412) | ILI, defined as being sick with fever and either sore throat or cough |
|
| Thorrington et al., 2017 [26] | England | 2012–2014 | Survey of parents/guardians (N = 161) | ILI, ECDC definition |
|
| Fragaszy et al., 2018 [11] | England | 2006–2011 | Community cohort study (N = 2919) | ILI, defined as fever ≥ 37.8 °C or feverish symptoms and either cough or sore throat, PCR-confirmed influenza |
|
| Tomonaga et al., 2021 [27] | Switzerland | 2016–2017 | Absenteeism data from Swiss Sentinel Surveillance Network of the Swiss Federal Office of Public Health (SFOPH) | ILI, defined as sudden onset of high fever >38 °C and cough or sore throat, as well as secondary illnesses after influenza |
|
| Millot et al., 2002 [28] | France | 1996–1997 | Survey of employees (N = 3663) | ILI, defined as association of fever with sudden systemic symptom and ≥1 respiratory sign (clinical or self-diagnosis) |
|
| Sessa et al., 2001 [29] | Italy | 1998–1999 | Cases of GP-diagnosed influenza followed up for outcome data (N = 6057) | Clinical influenza (GP diagnosis) |
|
| General adult populations: all-cause absenteeism and influenza/ILI surveillance trends | |||||
| De Blasio et al., 2012 [17] | Norway | 2005–2010 | Work absence data from Norwegian postal service | All-cause absenteeism (influenza attributable work loss estimated using Poisson regression based on ILI rates in the population) |
|
| Schanzer et al., 2011 [30] | Canada | 1995–2009 | Time series using data from Statistics Canada’s Labour Force Survey | All-cause absenteeism (influenza-attributable absenteeism modeled based on percentage of tests positive for influenza during each season and weekly/monthly trends in influenza activity) |
|
| Groenewold et al., 2019 [31] | United States | 2017–2018 | Workplace absenteeism surveillance (CDC Current Population Survey) | All-cause absenteeism among full-time workers during influenza epidemic |
|
| Specific populations: ILI | |||||
| Sartor et al., 2002 [32] | France | 1999 | Healthcare workers present during in-hospital influenza outbreak (N = 22) | ILI |
|
| Chiu et al., 2017 [33] | United States | 2014–2015 | Survey of healthcare workers (N = 1914) | ILI, defined as fever, sore throat, or cough |
|
| Jiang et al., 2019 [34] | Canada | 2010–2014 | Active surveillance of healthcare workers (N = 2093) | ARI (shortness of breath, cough, sore or scratchy throat, or coryza) |
|
| Hoang Johnson et al., 2021 [35] | United States | 2017–2018 | Healthcare worker survey (N = 2391) | ILI, defined as symptoms of fever, chills, cough, or sore throat |
|
| Szucs et al., 2001 [36] | Switzerland | 1999–2000 | Healthcare worker survey (N = 200) | ILI |
|
| Specific populations: all-cause absenteeism and influenza/ILI surveillance trends | |||||
| Van Buynder et al., 2015 [37] | Canada | 2012–2013 | Retrospective cohort study of healthcare workers | All-cause absenteeism pre- and during influenza seasons |
|
| Gianino et al., 2017 [38] | Italy | 2010–2013 | Hospital database analysis (N = 5291–5544 across years studied) | All-cause absenteeism during influenza epidemic and non-epidemic periods |
|
| Zaffina et al., 2019 [39] | Italy | 2016–2018 | Retrospective observational study of healthcare workers (N = 2090–2097 across time periods studied) | All-cause absenteeism during influenza epidemic and non-epidemic periods |
|
| Gianino et al., 2021 [40] | Italy | 2010–2013 2017–2018 | Healthcare worker absenteeism data from hospital database | Excess absenteeism in severe influenza season compared with non-epidemic period and with three moderate influenza seasons |
|
| Huiberts et al., 2022 [41] | The Netherlands | 2016–2019 | Data on registered schoolteacher sick leave, vaccine effectiveness and incidence of ILI in primary care | Total absenteeism and self-reported influenza sick leave extrapolated to total teacher population based on incidence of ILI |
|
Abbreviations: ARI, acute respiratory infection; CDC, US Centers for Disease Control and Prevention; CI, confidence interval; ECDC, European Centre for Disease Prevention and Control; GP, general practitioner; ICPC, International Classification of Primary Care; ILI, influenza-like illness; PCR, polymerase chain reaction; RSV, respiratory syncytial virus; SD, standard deviation; SFOPH, Swiss Federal Office of Public Health.
Figure 2.
Impact of influenza and ILI on absenteeism and productivity loss among adults. Abbreviations: HCW, healthcare worker; ILI, influenza-like illness.
Three studies used electronic health record data to assess absenteeism due to physician-diagnosed influenza [15,16,17]. Of these, two retrospective analyses of the MarketScan databases in the United States assessed absenteeism among those with influenza-related medical encounters or claims [15,16]. Across four influenza seasons, 30–37% of patients with influenza had ≥1 day of influenza-related workplace absence [16]. The mean duration of absence per person with influenza among those who took time off work ranged from 6.45 to 7.34 h across influenza seasons [16]. In an analysis of the data from the Norwegian Labour and Welfare service on sick leave classified as due to influenza according to International Classification of Primary Care (ICPC) codes, the rate of general practitioner-certified sick leave due to influenza was 1952 days per 100,000 employees (range 1595–2607) [17].
Thirteen studies assessed work loss due to ILI [11,18,19,20,21,22,23,24,25,26,27,28,29]. Definitions of ILI differed across studies. Nevertheless, individuals with ILI missed more work time than those without ILI [19,20,23,24] and those with other wintertime illnesses [11,22,24] across all studies that made these comparisons. Work time lost due to ILI ranged from 1 to 5 days (Figure 2) [11,20,21,22,24,25,26,27,29].
Three studies assessed all-cause absenteeism modeled against seasonal trends in influenza activity to estimate influenza-related absenteeism [17,30,31]. Rates of influenza-related absenteeism varied by season, ranging from 3 to 12% [17,30,31]. In a study in Canada, seasonal influenza was estimated to account for 3% of all hours lost annually [30].
3.1.2. Specific Populations
Five studies assessed absenteeism due to ILI/ARI in HCWs [32,33,34,35,36]. The mean number of missed workdays was 0.47 among 1036 HCWs with ARI in a study in Canada [34]. The median number of missed workdays was 2 among 414 HCWs with ILI in a study in the United States [33] and was 4.3, on average, across 59 HCWs in a study in Switzerland [36]. Of 1180 HCWs with ILI in a second study in the United States, 71% reported an absence of >2 days [35]. All four studies that assessed all-cause absenteeism in HCWs during periods of high influenza versus low influenza activity showed that absenteeism increased during influenza seasons/epidemic periods [37,38,39,40].
One study assessed absenteeism during influenza epidemics among schoolteachers. Modeling predicted that 23–31% of the total teacher population of the Netherlands per year would be affected by influenza absenteeism [41].
3.2. Productivity Loss Due to Influenza/ILI
Studies assessing productivity loss with influenza/ILI (i.e., attending work while ill and working at a reduced capacity) are shown in Table 2. Two studies evaluating people with laboratory-confirmed influenza showed that individuals with influenza had greater self-assessed productivity loss than those without, or those with ARI, based on a 10-point rating scale [9,10]. In a study in France, 9% of 199 working adults with laboratory-confirmed influenza did not stop working, and the median time to return to usual work activity for those who did stop working was 7 days (95% confidence interval [CI], 7–9) [14].
Table 2.
Studies on productivity loss due to influenza/ILI.
| Publication | Location | Time Period | Study Design | Definition of Illness | Results |
|---|---|---|---|---|---|
| General adult populations: laboratory-confirmed influenza | |||||
| Petrie et al., 2016 [9] | United States | 2012–2013 | Prospective study of working adults (N = 1548) | Laboratory-confirmed influenza versus influenza negative |
|
| Van Wormer et al., 2017 [10] | United States | 2012–2016 | Analysis of data from participants in vaccine effectiveness studies (N = 1278) | PCR-confirmed influenza-positive versus confirmed influenza-negative people with ARI |
|
| Carrat et al., 2002 [14] | France | 2000 | Household contact study | Laboratory-confirmed influenza |
|
| General adult populations: ILI | |||||
| Carrat et al., 2004 [21] | France | 1999–2000 influenza season | Observational household contact study (N = 701) | ILI |
|
| Palmer et al., 2010 [24] | United States | 2007–2008 influenza season | Observational cohort study of employees (N = 2013) | ILI (modified CDC definition) |
|
| Specific populations: ILI | |||||
| De Perio et al., 2014 [25] | United States | 2012–2013 | Survey of school employees (N = 412) | ILI, defined as being sick with fever and either sore throat or cough |
|
| Chiu et al., 2017 [33] | United States | 2014–2015 | Survey of healthcare workers (N = 1914) | ILI, defined as fever, sore throat or cough |
|
| Cowman et al., 2019 [7] | United States | 2017–2018 | Staff survey at Medical Center (N = 220) | ILI, defined as CDC definition of fever and ≥1 of cough, sore throat, nasal congestion or body aches |
|
| Jiang et al., 2019 [34] | Canada | 2010–2014 | Active surveillance of healthcare workers (N = 2093) | ARI (shortness of breath, cough, sore or scratchy throat, or coryza) |
|
| Hoang Johnson et al., 2021 [35] | United States | 2017–2018 | Healthcare worker survey (N = 2391) | ILI, defined as symptoms of fever, chills, cough or sore throat |
|
Abbreviations: ARI, acute respiratory infection; CDC, US Centers for Disease Control and Prevention; CI, confidence interval; ILI, influenza-like illness; PCR, polymerase chain reaction; SD, standard deviation; SE, standard error.
Two studies evaluated productivity loss from ILI in general adult populations [21,24]. In a study in the United States, among 2013 employees, those with symptoms of ILI were significantly less productive, with a mean of 2.5 h (standard deviation [SD] 5.0) per day of reduced productivity compared with 1.1 h (SD 3.3) among those with other non-ILI wintertime illnesses (p < 0.001) [24]. In another study in France, median time taken to return to normal work activity among 701 people who visited a general practitioner for ILI was 7 days (range 6–8) [21].
Five studies evaluated productivity loss with ILI in specific populations (school employees or HCWs) [7,25,33,34,35]. The percentage of school employees or HCWs with ILI who worked while ill ranged from 26% to 77% (95% for ARI; Figure 2) [7,25,33,34,35].
3.3. Absenteeism and Productivity Loss by Subgroup
3.3.1. Vaccination Status
Studies assessing work loss or productivity loss due to influenza/ILI by influenza vaccination status are shown in Table 3.
Two studies in the United States assessed work hours missed or productivity loss due to laboratory-confirmed influenza in vaccinated and unvaccinated individuals [9,10]. Neither detected any significant impact of vaccination [9,10], although a potential benefit of vaccination was observed in one study for work hours missed (20 versus 24 h; difference −4.3%; 95% CI, from −10.9 to 2.8; p = 0.23) and productivity loss (5.9 versus 6.1 [10-point scale]; difference −0.1; 95% CI, from −0.5 to 0.3; p = 0.66) [9]. In a study in Italy, parents of vaccinated children with laboratory-confirmed influenza lost significantly fewer workdays versus parents with unvaccinated children with laboratory-confirmed influenza (n = 1098; 3.22 [SD 1.86] versus 4.78 [SD 2.34] maternal work days; 0.56 [SD 0.46] versus 0.98 [SD 2.24] paternal work days; both p = 0.001) [13]. In a study in the United States, more patients with influenza-related medical encounters in the MarketScan database had at least 1 day of work absence during vaccine-mismatched seasons versus matched seasons (26.0% versus 33.3%) [16].
Among studies assessing work loss due to ILI or all-cause absenteeism during influenza epidemics, several studies detected statistically significant differences between vaccinated and unvaccinated individuals [42,43,44]. However, in one study of 3663 workers in France, no statistically significant difference in the average number of days of sick leave among those absent for any medical cause was observed between vaccinated and unvaccinated employees [28]. In a Swiss study that assessed productivity loss in workers with ILI, vaccinated people had significantly shorter durations of inability to work than unvaccinated people (2.79 days [95% CI, 2.51–3.08] versus 3.22 days [95% CI, 3.16–3.28], p = 0.008) [27].
Two studies showed significant reductions in workdays missed due to ILI among household contacts of children from schools offering influenza vaccination versus those attending either of two control schools where vaccination was not offered (study 1: 1.3 versus 7.0 [school 1] and 5.7 [school 2] workdays lost, p = 0.0004; study 2: mean 0.292 versus 0.388 days, difference 0.07 [95% CI, 0–0.14], p = 0.04 [includes time taken off work to care for sick children]) [45,46]. Similarly, in another study of 23,014 working adults with household children, the prevalence of workdays lost in households with a vaccinated child was 0.92 times (95% CI, 0.80–1.06) that of households with an unvaccinated child. This difference was statistically significant when using a model that included paid sick leave (0.79 times; 95% CI, 0.67–0.93) [47].
Studies of HCWs noted potentially lower absenteeism rates and productivity loss in vaccinated versus unvaccinated workers [33,36,48]. Among a convenience sample of 341 HCWs, 3.4% of vaccinated HCWs were absent for more than 1 day due to ILI, compared with 13% of unvaccinated HCWs (p ≤ 0.006) [48]. Among a randomized sample of 200 university hospital employees, absenteeism rates due to ILI were 17% in vaccinated HCWs and 25% in unvaccinated HCWs (odds ratio 0.6; 95% CI, 0.2–1.7) [36]. In a survey of 1914 HCWs, 414 reported an ILI and 183 reported working with an ILI. Of these, 44.6% who reported working with an ILI had received an influenza vaccination, compared with 29.3% who were not vaccinated (p = 0.03) [33].
Several studies assessed all-cause absenteeism in vaccinated versus unvaccinated HCWs during influenza epidemic periods [37,38,39,40,49,50]. Significantly greater absenteeism rates were observed in unvaccinated HCWs across all studies [37,38,39,40,49,50].
Table 3.
Studies on absenteeism or productivity loss by vaccine status.
| Publication | Location | Time Period | Study Design and Participants | Definition of Illness | Results |
|---|---|---|---|---|---|
| General adult populations: laboratory-confirmed influenza | |||||
| Petrie et al., 2016 [9] | United States | 2012–2013 | Prospective study of working adults (N = 1548) | Laboratory-confirmed influenza versus influenza negative |
|
| Van Wormer et al., 2017 [10] | United States | 2012–2016 | Analysis of data from participants in vaccine effectiveness studies (N = 1278) | PCR-confirmed influenza-positive versus confirmed influenza-negative people with ARI |
|
| Principi et al., 2003 [13] | Italy | 2001–2002 | Study of children presenting to emergency department (N = 3771) and their household contacts | Laboratory-confirmed influenza |
|
| General adult populations: physician-diagnosed influenza/ILI | |||||
| Karve et al., 2013 [16] | United States | 2000–2009 | Retrospective analysis of employee data from MarketScan databases | Influenza-related medical encounters with temporal co-occurrence of workplace absence |
|
| General adult populations: ILI | |||||
| Nichol et al., 2008 [42] | United States | 2002–2003 | Survey of university students (N = 19,796) | ≥1 upper respiratory tract infection symptom (feverishness, chills, muscle aches, headache, sore throat, cough, runny nose or temperature of >38 °C) |
|
| Bridges et al., 2000 [43] | United States | 1997–1999 | Double-blind, placebo-controlled trial of inactivated influenza vaccine (N = 1184) | ILI, defined as feverishness or temperature of 37.7 °C plus cough or sore throat (CDC definition) |
|
| Millot et al., 2002 [28] | France | 1996–1997 | Survey of employees (N = 3663) | ILI, defined as association of fever with sudden systemic symptom and ≥1 respiratory sign |
|
| King et al., 2005 [45] | United States | 2003 | Controlled intervention study of schools with/without offer of influenza vaccination | Fever or respiratory illness |
|
| King et al., 2006 [46] | United States | 2004–2005 | Controlled intervention study of schools with/without offer of influenza vaccination | ILI, defined as fever or respiratory illness that included runny nose, nasal congestion, sinus problems, earache, ear infection, cough, sore throat, muscle aches, chills, or wheezing |
|
| Tomonaga et al., 2021 [27] | Switzerland | 2016–2017 | Absenteeism data from Swiss Sentinel Surveillance Network of the Swiss Federal Office of Public Health (SFOPH) | ILI, defined as sudden onset of high fever >38 °C and cough or sore throat, as well as secondary illnesses after influenza |
|
| General adult populations: all-cause absenteeism and influenza/ILI surveillance trends | |||||
| Bleser et al., 2019 [47] | United States | 2013–2015 | National Health Interview Surveys from working adults with children (N = 24,014) | All sick days (households with vaccinated versus unvaccinated children) |
|
| Ferro et al., 2020 [44] | Italy | 2017–2018 | Observational cohort study of employees of a manufacturing company (N = 408) | Comparison of absenteeism during influenza epidemic and non-epidemic periods |
|
| Specific populations: ILI | |||||
| Chiu et al., 2017 [33] | United States | 2014–2015 | Survey of HCWs (N = 1914) | ILI, defined as fever, sore throat, or cough |
|
| Speroni et al., 2005 [48] | United States | 2004–2005 | Convenience sample of HCWs (N = 341) | Specific symptoms (fever, headache, extreme tiredness, dry cough, sore throat, runny nose, stuffy nose, muscle aches) |
|
| Szucs et al., 2001 [36] | Switzerland | 1999–2000 | HCW survey (N = 200) | ILI |
|
| Specific populations: all-cause absenteeism and influenza/ILI surveillance trends | |||||
| Van Buynder et al., 2015 [37] | Canada | 2012–2013 | Retrospective cohort study of HCWs | All-cause sick hours |
|
| Gianino et al., 2021 [40] | Italy | 2010–2013 2017–2018 | HCWs absenteeism data from hospital database | Excess absenteeism in severe influenza season compared with non-epidemic period and with three moderate influenza seasons |
|
| Zaffina et al., 2019 [39] | Italy | 2016–2018 | Retrospective observational study of HCWs (N = 2090–2097 across time periods studied) | Comparison of absenteeism during influenza epidemic and non-epidemic periods |
|
| Antinolfi et al., 2020 [49] | Italy | 2017–2018 | Retrospective study of HCWs (N = 4382) | Comparison of absenteeism during influenza epidemic and non-epidemic periods |
|
| Gianino et al., 2017 [38] | Italy | 2010–2013 | Hospital database analysis (N = 5291–5544 across years studied) | Comparison of absenteeism during influenza epidemic and non-epidemic periods |
|
| Costantino et al., 2020 [51] | Italy | 2007–2019 | Hospital data on absenteeism among HCWs | Acute sickness during influenza seasons, pre-, and post-interventions to increase vaccine coverage |
|
| Murti et al., 2019 [50] | Canada | 2012–2017 | HCW payroll/absenteeism data (N = 107,258) | All sick time |
|
| Huiberts et al., 2022 [41] | The Netherlands | 2016–2019 | Data on registered schoolteacher sick leave, vaccine effectiveness. and incidence of ILI in primary care | Self-reported influenza sick leave |
|
Abbreviations: ARI, acute respiratory infection; CDC, US Centers for Disease Control and Prevention; CI, confidence interval; HCW, healthcare worker; ILI, influenza-like illness; OR, odds ratio; PCR, polymerase chain reaction; RR, risk ratio; SD, standard deviation; SFOPH, Swiss Federal Office of Public Health; VE, vaccine effectiveness.
3.3.2. Age Group
Nine studies evaluated work loss due to influenza/ILI by age group [10,11,16,27,30,33,34,52,53]. Generally, in studies of general adult populations, less work time was lost, and productivity was reduced to a lesser extent, in older versus younger adults. In a survey of working Canadian adults with diagnosed influenza or self-reported ILI, those who were 50–64 years of age were more likely than those ≥65 years of age to be absent from work (p = 0.009 in 2019/2020) or to be present but working at low capacity (p = 0.02 in 2018/2019) [52]. In a community cohort study of 2919 adults in England, a smaller percentage of adults ≥65 years of age than 16–64 years of age took time off for work/education due to ILI (9% versus 26%), influenza A (13% versus 31%), and influenza B (0% versus 20%); however, no statistical comparisons were made [11]. In Switzerland, among 3971 cases of ILI, the mean number of workdays lost per case was similar across age classes <65 years of age and was lower than average in those ≥65 years of age [27]. Younger age groups had a higher rate of cases of inability to work than older age groups. In a retrospective analysis of the MarketScan databases, individuals 45–64 years of age had higher influenza-related workplace absence hours than those 25–44 years of age (range 7.6–9.7 versus 5.2–6.6). Similarly, individuals 45–64 years of age had the highest influenza-related productivity loss costs, followed by those in the 25–44 years of age group, for all four influenza seasons studied [16]. A study from the Canadian Labour Force Survey found that the level of influenza activity was associated with hours lost in younger age groups (18–44 years of age) only, while the proportion of hours lost due to any illness or disability increased significantly with age [30].
Among HCWs, work loss and productivity work loss generally did not differ by age. In an online survey of 220 employees/trainees at a medical center in the United States, the percentage of workers who reported presenting to work with ILI was not significantly associated with age group [7]. Among 2093 HCWs in Canada, a multivariable analysis showed no difference in the number working with ARI across age groups [34]. Among 1914 HCWs in the United States, the percentage who reported working with ILI did not significantly differ by age group (18–34 years, 42.3%; 35–49 years, 45.6% [p = 0.68 versus 18–34 years]; ≥50 years, 34.7% [p = 0.33 versus 18–34 years]) [33]. In a study involving 5401 HCWs in Italy, there was a significant increase in sick leave during seasonal influenza epidemics for all age ranges [53].
3.3.3. Disease Severity
Four studies evaluated the impact of disease severity on work time lost or productivity loss due to influenza/ILI; all suggested a link between increased severity and more work time lost [14,27,34,40]. In a study of the Swiss workforce, patients reporting a high fever (>38 °C) had a significantly longer duration of inability to work (3.37 days [95% CI, 3.19–3.56] versus 3.05 days [95% CI, 2.79–3.30] for people without a high fever; p = 0.014) [27]. In a survey of household contacts in France, the number of lost workdays was correlated with the symptom score on the first day of illness (r = 0.45, p < 0.001) [14]. Among 5287 HCWs in Italy, a significantly greater excess of absenteeism was observed during a severe influenza season compared with a moderate influenza season (+0.75 days/person, p = 0.03) [40]. One study in 2093 Canadian HCWs demonstrated that productivity loss with ARI increased with increasing symptom severity score [34].
3.3.4. Caring for Others
Caring for others with influenza/ILI contributed to work time loss. Among households with medical insurance coverage and school-age children in the United States, households with ILI missed 0.89 (95% CI, 0.48–1.30) more workdays while caring for ill household members versus households without ILI [23]. In a survey of 161 parents or guardians in England, mean work absence to care for children with ILI (n = 34) was 3.7 days (95% CI, 2.7–4.8) [26]. In a survey of school children in the United States, for every 100 children, influenza accounted for an estimated 20 days of work missed by parents [19]. Another survey of 954 parents of school children reported that an adult missed work to care for an ill child in 53% of families [18].
Across studies, the percentage of cases of work loss attributed to caring for others ranged from 1% to 9% [11,17,27]. In the community cohort study of 2919 adults in England, the percentage of illnesses during which a working adult took time off from work or education to care for an ill working adult was 13% for influenza A and 0% for influenza B [11]. In a study of the Swiss workforce, 90% of cases of inability to work due to influenza/ILI were due to a person’s own illness, 1–2% of cases were due to caregiving, and 8–9% of cases were a combination of both [27]. In Norway, approximately 4–5% of work absences were attributed to care for sick children with influenza [17].
3.3.5. Comorbidities
Data on the impact of comorbidities on work loss due to influenza/ILI are limited. In one retrospective study of the MarketScan databases, among influenza cases with comorbid asthma, more than 36% had at least 1 day of influenza-related workplace absence for each of the four influenza seasons [16]. In a survey of 412 employees in the United States, those with a weakened immune system caused by cancer, chronic illness, or medications were less likely to report working while ill than those without (20.0% versus 78.7%; p = 0.01); diabetes and asthma were not associated with working while ill [25]. In employees in Switzerland, increased risk of complications and medication had no significant impact on the duration of their inability to work [27].
3.3.6. Prophylaxis
One study assessed the impact of prophylaxis on work time lost due to influenza/ILI [54]. In this study of 800 HCWs in the United States, offering oseltamivir prophylaxis to exposed HCWs had no apparent impact on overall absenteeism rates or duration of sick leave compared with the previous influenza season, during which only exposed, unvaccinated HCWs were offered prophylaxis [54].
3.4. Cost of Work Loss Due to Influenza/ILI
Studies evaluating the cost of work time lost due to influenza/ILI are shown in Table 4. In the United States, the cost of productivity loss was higher among people with influenza-related medical encounters in the MarketScan database during vaccine-mismatched seasons compared with matched seasons (USD 51,483 versus USD 31,454 per 100,000 members) [15]. Consistent with this, three studies noted higher costs of absenteeism among unvaccinated compared with vaccinated employees or HCWs [39,43,44]. Other factors associated with increased cost due to work time lost included younger age [27,53], the presence of comorbidities [16], and caring for family members with ILI [23].
Table 4.
Studies on cost of work loss due to influenza/ILI.
| Publication | Location | Time Period | Study Design | Definition of Illness | Results |
|---|---|---|---|---|---|
| General adult populations: physician-diagnosed influenza | |||||
| Karve et al., 2013 [16] | United States | 2005–2009 | Retrospective analysis of employee data from MarketScan databases | ≥1 medical claim with diagnosis of influenza |
|
| Karve et al., 2013 [15] | United States | 2000–2009 | Retrospective analysis of employee data from MarketScan databases | Influenza-related medical encounters with temporal co-occurrence of workplace absence |
|
| General adult populations: ILI | |||||
| Nettleman et al., 2001 [18] | United States | 1998 | Survey of parents of schoolchildren (N = 954) | Respiratory illness, excluding asthma |
|
| Akazawa et al., 2003 [20] | United States | January–July 1996 | Household survey (N = 7037) | ILI |
|
| Li et al., 2007 [23] | United States | 1996–2002 | Medical Expenditure Panel Survey (N = 12,850 households) | ILI |
|
| Tomonaga et al., 2021 [27] | Switzerland | 2016–2017 | Absenteeism data from Swiss Sentinel Surveillance Network of the Swiss Federal Office of Public Health (SFOPH) | ILI, defined as sudden onset of high fever >38 °C and cough or sore throat, as well as secondary illnesses after influenza |
|
| Ferro et al., 2020 [44] | Italy | 2017–2018 | Observational cohort study of employees of a manufacturing company (N = 408) | Comparison of absenteeism during influenza epidemic and non-epidemic periods |
|
| Bridges et al., 2000 [43] | United States | 1997–1999 | Double-blind, placebo-controlled trial of inactivated influenza vaccine (N = 1184) | ILI, defined as feverishness or temperature of 37.7 °C plus cough or sore throat (CDC definition) |
|
| Healthcare workers: ILI | |||||
| Szucs et al., 2001 [36] | Switzerland | 1999–2000 | Healthcare worker survey (N = 200) | ILI |
|
| Healthcare workers: influenza surveillance trends | |||||
| Zaffina et al., 2019 [39] | Italy | 2016–2018 | Retrospective observational study of healthcare workers (N = 2090–2097 across time periods studied) | Comparison of absenteeism during influenza epidemic and non-epidemic periods |
|
| Gianino et al., 2019 [53] | Italy | 2010–2013 | Hospital data on absenteeism (N = 5401) | Sporadic absences (any cause) during influenza epidemic periods |
|
Abbreviations: CDC, Centers for Disease Control and Prevention; ILI, influenza-like illness; SFOPH, Swiss Federal Office of Public Health.
4. Discussion
This targeted review suggests an association between influenza/ILI and work/productivity loss. Work time lost and productivity loss due to laboratory-confirmed influenza were consistently higher than work loss because of other respiratory diseases and wintertime illnesses compared to people without influenza [9,10,11,12,13,27]. The majority of studies assessed work time lost due to ILI and demonstrated that individuals with ILI missed more work time and were less productive than those without ILI or with other wintertime illnesses [20,22,23,24]. Among specific populations (HCWs and school employees), ILI was associated with considerable work time and productivity loss [25,32,33,34,35], and absenteeism was higher during periods of high influenza versus low influenza activity [37,38,39,40]. These findings suggest that ILI is an appropriate surrogate for laboratory-confirmed influenza when assessing absenteeism and productivity loss.
Most studies that assessed the impact of vaccination on absenteeism demonstrated less work time and productivity loss, as well as lower costs, among vaccinated versus unvaccinated individuals [9,13,27,42,43,44], members of households with vaccinated children versus those with unvaccinated children [45,46,47], or during vaccine-mismatched seasons [16]. As influenza vaccination has been shown to reduce the rate of infection and severity of disease [4], the impact of vaccination on absenteeism and productivity loss is not unexpected. Several studies document that greater disease severity was associated with increased work time lost or productivity loss [14,27,34,40].
Work time and productivity losses were generally higher in adults younger than 60–65 years of age than in older adults [10,11,27,52]. This may have been due to a smaller proportion of older adults being in work; however, the same trend was observed in a study that included working adults only [52]. Younger age groups are likely to have higher exposure to influenza, resulting from the presence of children in the household acting as a natural reservoir, as well as greater time spent working or out of the household at events and gatherings than older adults. Caring for others with influenza/ILI also contributed to work time lost by the caregiver [11,17,18,19,23,26,27], which may disproportionately affect younger adults. Furthermore, older adults may have been more likely to have been vaccinated against influenza, as, in many countries, vaccination is only recommended for adults >65 years of age and for those with risk conditions or high exposure to infection [4].
Data on the impact of comorbidities on work time and productivity loss due to influenza/ILI were limited. People with certain underlying health conditions, including asthma, chronic lung, heart, or kidney disease, diabetes, and immunocompromising conditions or medications are known to be at high risk of developing serious complications of influenza infection [4,55]. Further research is warranted to determine whether specific comorbidities may be particularly associated with increased absenteeism or productivity loss.
The findings of this review are generally consistent with other reviews that have included articles from outside of Canada, Europe, and the United States. Overall, the average days of work lost across studies assessing laboratory-confirmed influenza ranged from 1 to 4 [11,12,13,14]. This is comparable to values seen worldwide in the narrative literature review by Keech et al., which estimated 1.5–4.9 working days lost due to laboratory-confirmed influenza [1]. Similarly, in a recent systematic literature review, mean work time lost due to influenza/ILI ranged from <1 to >10 days, but was often reported to be approximately 2–3 days [8].
Limitations of this review include the small number of articles on each pre-defined outcome of interest. Certain countries were overrepresented (e.g., the United States, Italy, France, Switzerland, and Canada), while no relevant studies from Spain or Germany were identified. Overall, the literature search identified only 48 articles for inclusion, highlighting a need for further research on this topic, No meta-analyses were performed, and no quality assessment was carried out. As the majority of the studies included were small observational studies, the quality of the methodology may have been low, representing a risk of bias. In addition, while influenza was consistently defined, the definitions of ILI and ARI differed by study in terms of the symptoms included, and some did not state the definition used. As differences were minimal and the countries included were similar in terms of income level and vaccination programs, combining conclusions from these studies was warranted. However, care should be taken when making direct comparisons across studies, given the differences in study designs.
5. Conclusions
Influenza/ILI has been shown to result in significant work time and productivity losses among working adults in Canada, Europe, and the United States, particularly those who are unvaccinated, are <65 or <60 years of age, or who have severe disease. Further research is required on the impact of influenza on absenteeism and productivity loss in adults with comorbidities to support the development of effective employer policies for working adults with underlying health conditions. Research into the impact of vaccination on absenteeism and productivity loss could support the economic and health benefits of vaccination and facilitate our understanding of the potential benefits of extending vaccination programs to wider adult populations.
Acknowledgments
Medical writing support, including assisting authors with the development of the outline and initial draft and incorporation of comments, was provided by Helene Wellington and Rachel Wright, and editorial support was provided by Ian Norton, all from Scion (a division of Prime, London, UK), supported by CSL Seqirus according to Good Publication Practice guidelines (Link).
Author Contributions
D.F., M.P., M.J.L. and J.M.-Q. made substantial contributions to the design, conception, analysis, and interpretation of literature review findings; critically reviewed draft manuscripts for important intellectual content and provided input into draft manuscripts; and provided final approval of the version to be published. All authors have read and agreed to the published version of the manuscript.
Data Availability Statement
Data included in this review article are those provided in published papers.
Conflicts of Interest
David Fisman has received honoraria for participating in advisory boards with Merck, Sanofi-Pasteur, CSL Seqirus, Pfizer, and AstraZeneca related to influenza, SARS-CoV-2, and pneumococcal vaccines. Myron J. Levin received honoraria from CSL Seqirus, GSK, Pfizer, Moderna, Curevo, AstraZeneca, and Dynavax for taking part in advisory boards. He has also received institution funding for investigator-led studies from GSK. Maarten Postma has received honoraria from CSL Seqirus for taking part in advisory boards. Joaquin Mould-Quevedo is an employee of CSL Seqirus.
Funding Statement
Medical writing support was funded by CSL Seqirus.
Footnotes
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content.
References
- 1.Keech M., Beardsworth P. The impact of influenza on working days lost: A review of the literature. Pharmacoeconomics. 2008;26:911–924. doi: 10.2165/00019053-200826110-00004. [DOI] [PubMed] [Google Scholar]
- 2.European Centre for Disease Prevention and Control . Factsheet About Seasonal Influenza. European Centre for Disease Prevention and Control; Stockholm, Sweden: 2022. [Google Scholar]
- 3.Centers for Disease Control and Prevention . Disease Burden of Flu. Centers for Disease Control and Prevention; Atlanta, GA, USA: 2023. [Google Scholar]
- 4.World Health Organization (WHO) Influenza (Seasonal) [(accessed on 1 October 2023)]. Available online: https://www.who.int/news-room/fact-sheets/detail/influenza-(seasonal)
- 5.Krammer F., Smith G.J.D., Fouchier R.A.M., Peiris M., Kedzierska K., Doherty P.C., Palese P., Shaw M.L., Treanor J., Webster R.G., et al. Influenza. Nat. Rev. Dis. Primers. 2018;4:3. doi: 10.1038/s41572-018-0002-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Edwards C.H., Tomba G.S., de Blasio B.F. Influenza in workplaces: Transmission, workers’ adherence to sick leave advice and European sick leave recommendations. Eur. J. Public Health. 2016;26:478–485. doi: 10.1093/eurpub/ckw031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Cowman K., Mittal J., Weston G., Harris E., Shapiro L., Schlair S., Park S., Nori P. Understanding drivers of influenza-like illness presenteeism within training programs: A survey of trainees and their program directors. Am. J. Infect. Control. 2019;47:895–901. doi: 10.1016/j.ajic.2019.02.004. [DOI] [PubMed] [Google Scholar]
- 8.Blanchet Zumofen M.H., Frimpter J., Hansen S.A. Impact of Influenza and Influenza-Like Illness on Work Productivity Outcomes: A Systematic Literature Review. Pharmacoeconomics. 2023;41:253–273. doi: 10.1007/s40273-022-01224-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Petrie J.G., Cheng C., Malosh R.E., VanWormer J.J., Flannery B., Zimmerman R.K., Gaglani M., Jackson M.L., King J.P., Nowalk M.P., et al. Illness Severity and Work Productivity Loss Among Working Adults With Medically Attended Acute Respiratory Illnesses: US Influenza Vaccine Effectiveness Network 2012–2013. Clin. Infect. Dis. 2016;62:448–455. doi: 10.1093/cid/civ952. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Van Wormer J.J., King J.P., Gajewski A., McLean H.Q., Belongia E.A. Influenza and Workplace Productivity Loss in Working Adults. J. Occup. Environ. Med. 2017;59:1135–1139. doi: 10.1097/JOM.0000000000001120. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Fragaszy E.B., Warren-Gash C., White P.J., Zambon M., Edmunds W.J., Nguyen-Van-Tam J.S., Hayward A.C., Flu Watch Group Effects of seasonal and pandemic influenza on health-related quality of life, work and school absence in England: Results from the Flu Watch cohort study. Influenza Other Respir. Viruses. 2018;12:171–182. doi: 10.1111/irv.12506. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Esposito S., Gasparini R., Bosis S., Marchisio P., Tagliabue C., Tosi S., Bianchi C., Crovari P., Principi N. Clinical and socio-economic impact of influenza and respiratory syncytial virus infection on healthy children and their households. Clin. Microbiol. Infect. 2005;11:933–936. doi: 10.1111/j.1469-0691.2005.01270.x. [DOI] [PubMed] [Google Scholar]
- 13.Principi N., Esposito S., Marchisio P., Gasparini R., Crovari P. Socioeconomic impact of influenza on healthy children and their families. Pediatr. Infect. Dis. J. 2003;22:S207–S210. doi: 10.1097/01.inf.0000092188.48726.e4. [DOI] [PubMed] [Google Scholar]
- 14.Carrat F., Sahler C., Rogez S., Leruez-Ville M., Freymuth F., Le Gales C., Bungener M., Housset B., Nicolas M., Rouzioux C. Influenza burden of illness: Estimates from a national prospective survey of household contacts in France. Arch. Intern. Med. 2002;162:1842–1848. doi: 10.1001/archinte.162.16.1842. [DOI] [PubMed] [Google Scholar]
- 15.Karve S., Meier G., Davis K.L., Misurski D.A., Wang C.C. Influenza-related health care utilization and productivity losses during seasons with and without a match between the seasonal and vaccine virus B lineage. Vaccine. 2013;31:3370–3388. doi: 10.1016/j.vaccine.2013.04.081. [DOI] [PubMed] [Google Scholar]
- 16.Karve S., Misurski D.A., Meier G., Davis K.L. Employer-incurred health care costs and productivity losses associated with influenza. Hum. Vaccin. Immunother. 2013;9:841–857. doi: 10.4161/hv.23413. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.De Blasio B.F., Xue Y., Iversen B., Gran J.M. Estimating influenza-related sick leave in Norway: Was work absenteeism higher during the 2009 A(H1N1) pandemic compared to seasonal epidemics? Eurosurveillance. 2012;17:20246. doi: 10.2807/ese.17.33.20246-en. [DOI] [PubMed] [Google Scholar]
- 18.Nettleman M.D., White T., Lavoie S., Chafin C. School absenteeism, parental work loss, and acceptance of childhood influenza vaccination. Am. J. Med. Sci. 2001;321:178–180. doi: 10.1097/00000441-200103000-00004. [DOI] [PubMed] [Google Scholar]
- 19.Neuzil K.M., Hohlbein C., Zhu Y. Illness among schoolchildren during influenza season: Effect on school absenteeism, parental absenteeism from work, and secondary illness in families. Arch. Pediatr. Adolesc. Med. 2002;156:986–991. doi: 10.1001/archpedi.156.10.986. [DOI] [PubMed] [Google Scholar]
- 20.Akazawa M., Sindelar J.L., Paltiel A.D. Economic costs of influenza-related work absenteeism. Value Health. 2003;6:107–115. doi: 10.1046/j.1524-4733.2003.00209.x. [DOI] [PubMed] [Google Scholar]
- 21.Carrat F., Schwarzinger M., Housset B., Valleron A.J. Antibiotic treatment for influenza does not affect resolution of illness, secondary visits or lost workdays. Eur. J. Epidemiol. 2004;19:703–705. doi: 10.1023/B:EJEP.0000036807.40105.97. [DOI] [PubMed] [Google Scholar]
- 22.Nichol K.L., D’Heilly S., Ehlinger E. Colds and influenza-like illnesses in university students: Impact on health, academic and work performance, and health care use. Clin. Infect. Dis. 2005;40:1263–1270. doi: 10.1086/429237. [DOI] [PubMed] [Google Scholar]
- 23.Li S., Leader S. Economic burden and absenteeism from influenza-like illness in healthy households with children (5–17 years) in the US. Respir. Med. 2007;101:1244–1250. doi: 10.1016/j.rmed.2006.10.022. [DOI] [PubMed] [Google Scholar]
- 24.Palmer L.A., Rousculp M.D., Johnston S.S., Mahadevia P.J., Nichol K.L. Effect of influenza-like illness and other wintertime respiratory illnesses on worker productivity: The child and household influenza-illness and employee function (CHIEF) study. Vaccine. 2010;28:5049–5056. doi: 10.1016/j.vaccine.2010.05.011. [DOI] [PubMed] [Google Scholar]
- 25.De Perio M.A., Wiegand D.M., Brueck S.E. Influenza-like illness and presenteeism among school employees. Am. J. Infect. Control. 2014;42:450–452. doi: 10.1016/j.ajic.2013.11.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Thorrington D., Balasegaram S., Cleary P., Hay C., Eames K. Social and Economic Impacts of School Influenza Outbreaks in England: Survey of Caregivers. J. Sch. Health. 2017;87:209–216. doi: 10.1111/josh.12484. [DOI] [PubMed] [Google Scholar]
- 27.Tomonaga Y., Zens K.D., Lang P., Born R., Schwenkglenks M., Swiss Sentinel Surveillance Network Productivity losses due to influenza and influenza-like illness in Switzerland: Results of the Swiss Sentinel Surveillance Network in a non-pandemic era. Swiss Med. Wkly. 2021;151:w30022. doi: 10.4414/SMW.2021.w30022. [DOI] [PubMed] [Google Scholar]
- 28.Millot J.L., Aymard M., Bardol A. Reduced efficiency of influenza vaccine in prevention of influenza-like illness in working adults: A 7 month prospective survey in EDF Gaz de France employees, in Rhone-Alpes, 1996–1997. Occup. Med. 2002;52:281–292. doi: 10.1093/occmed/52.5.281. [DOI] [PubMed] [Google Scholar]
- 29.Sessa A., Costa B., Bamfi F., Bettoncelli G., D’Ambrosio G. The incidence, natural history and associated outcomes of influenza-like illness and clinical influenza in Italy. Fam. Pract. 2001;18:629–634. doi: 10.1093/fampra/18.6.629. [DOI] [PubMed] [Google Scholar]
- 30.Schanzer D.L., Zheng H., Gilmore J. Statistical estimates of absenteeism attributable to seasonal and pandemic influenza from the Canadian Labour Force Survey. BMC Infect. Dis. 2011;11:90. doi: 10.1186/1471-2334-11-90. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Groenewold M.R., Burrer S.L., Ahmed F., Uzicanin A., Luckhaupt S.E. Health-Related Workplace Absenteeism Among Full-Time Workers—United States, 2017-2018 Influenza Season. MMWR. Morb. Mortal. Wkly. Rep. 2019;68:577–582. doi: 10.15585/mmwr.mm6826a1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Sartor C., Zandotti C., Romain F., Jacomo V., Simon S., Atlan-Gepner C., Sambuc R., Vialettes B., Drancourt M. Disruption of services in an internal medicine unit due to a nosocomial influenza outbreak. Infect. Control Hosp. Epidemiol. 2002;23:615–619. doi: 10.1086/501981. [DOI] [PubMed] [Google Scholar]
- 33.Chiu S., Black C.L., Yue X., Greby S.M., Laney A.S., Campbell A.P., de Perio M.A. Working with influenza-like illness: Presenteeism among US health care personnel during the 2014-2015 influenza season. Am. J. Infect. Control. 2017;45:1254–1258. doi: 10.1016/j.ajic.2017.04.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Jiang L., McGeer A., McNeil S., Katz K., Loeb M., Muller M.P., Simor A., Powis J., Kohler P., Di Bella J.M., et al. Which healthcare workers work with acute respiratory illness? Evidence from Canadian acute-care hospitals during 4 influenza seasons: 2010–2011 to 2013–2014. Infect. Control Hosp. Epidemiol. 2019;40:889–896. doi: 10.1017/ice.2019.141. [DOI] [PubMed] [Google Scholar]
- 35.Hoang Johnson D., Osman F., Bean J., Stevens L., Shirley D., Keating J.A., Johnson S., Safdar N. Barriers and facilitators to influenza-like illness absenteeism among healthcare workers in a tertiary-care healthcare system, 2017-2018 influenza season. Infect. Control Hosp. Epidemiol. 2021;42:1198–1205. doi: 10.1017/ice.2020.1396. [DOI] [PubMed] [Google Scholar]
- 36.Szucs T.D., Ruef C., Muller D., Sokolovic E., Beeler I., Ostermayer W. The economic impact of influenza in a university hospital setting. Infect. Control Hosp. Epidemiol. 2001;22:472–474. doi: 10.1086/503405. [DOI] [PubMed] [Google Scholar]
- 37.Van Buynder P.G., Konrad S., Kersteins F., Preston E., Brown P.D., Keen D., Murray N.J. Healthcare worker influenza immunization vaccinate or mask policy: Strategies for cost effective implementation and subsequent reductions in staff absenteeism due to illness. Vaccine. 2015;33:1625–1628. doi: 10.1016/j.vaccine.2015.01.048. [DOI] [PubMed] [Google Scholar]
- 38.Gianino M.M., Politano G., Scarmozzino A., Charrier L., Testa M., Giacomelli S., Benso A., Zotti C.M. Estimation of sickness absenteeism among Italian healthcare workers during seasonal influenza epidemics. PLoS ONE. 2017;12:e0182510. doi: 10.1371/journal.pone.0182510. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Zaffina S., Gilardi F., Rizzo C., Sannino S., Brugaletta R., Santoro A., Castelli Gattinara G., Ciofi Degli Atti M.L., Raponi M., Vinci M.R. Seasonal influenza vaccination and absenteeism in health-care workers in two subsequent influenza seasons (2016/17 and 2017/18) in an Italian pediatric hospital. Expert Rev. Vaccines. 2019;18:411–418. doi: 10.1080/14760584.2019.1586541. [DOI] [PubMed] [Google Scholar]
- 40.Gianino M.M., Kakaa O., Politano G., Scarmozzino A., Benso A., Zotti C.M. Severe and moderate seasonal influenza epidemics among Italian healthcare workers: A comparison of the excess of absenteeism. Influenza Other Respir. Viruses. 2021;15:81–90. doi: 10.1111/irv.12777. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Huiberts A., van Cleef B., Tjon A.T.A., Dijkstra F., Schreuder I., Fanoy E., van Gageldonk A., van der Hoek W., van Asten L. Influenza vaccination of school teachers: A scoping review and an impact estimation. PLoS ONE. 2022;17:e0272332. doi: 10.1371/journal.pone.0272332. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Nichol K.L., D’Heilly S., Ehlinger E.P. Influenza vaccination among college and university students: Impact on influenzalike illness, health care use, and impaired school performance. Arch. Pediatr. Adolesc. Med. 2008;162:1113–1118. doi: 10.1001/archpedi.162.12.1113. [DOI] [PubMed] [Google Scholar]
- 43.Bridges C.B., Thompson W.W., Meltzer M.I., Reeve G.R., Talamonti W.J., Cox N.J., Lilac H.A., Hall H., Klimov A., Fukuda K. Effectiveness and cost-benefit of influenza vaccination of healthy working adults: A randomized controlled trial. JAMA. 2000;284:1655–1663. doi: 10.1001/jama.284.13.1655. [DOI] [PubMed] [Google Scholar]
- 44.Ferro A., Bordin P., Benacchio L., Fornasiero F., Bressan V., Tralli V., Moretti F., Majori S. Influenza vaccination and absenteeism among healthy working adults: A cost-benefit analysis. Ann. Ig. 2020;32:234–244. doi: 10.7416/ai.2020.2346. [DOI] [PubMed] [Google Scholar]
- 45.King J.C., Jr., Cummings G.E., Stoddard J., Readmond B.X., Magder L.S., Stong M., Hoffmaster M., Rubin J., Tsai T., Ruff E., et al. A pilot study of the effectiveness of a school-based influenza vaccination program. Pediatrics. 2005;116:e868–e873. doi: 10.1542/peds.2005-1301. [DOI] [PubMed] [Google Scholar]
- 46.King J.C., Jr., Stoddard J.J., Gaglani M.J., Moore K.A., Magder L., McClure E., Rubin J.D., Englund J.A., Neuzil K. Effectiveness of school-based influenza vaccination. N. Engl. J. Med. 2006;355:2523–2532. doi: 10.1056/NEJMoa055414. [DOI] [PubMed] [Google Scholar]
- 47.Bleser W.K., Miranda P.Y., Salmon D.A. Child Influenza Vaccination and Adult Work Loss: Reduced Sick Leave Use Only in Adults With Paid Sick Leave. Am. J. Prev. Med. 2019;56:251–261. doi: 10.1016/j.amepre.2018.09.013. [DOI] [PubMed] [Google Scholar]
- 48.Speroni K.G., Dawson E., Atherton M., Corriher J. Influenza vaccination: Incidence of symptoms and resulting absenteeism in hospital employees. AAOHN J. 2005;53:477–483. doi: 10.1177/216507990505301103. [DOI] [PubMed] [Google Scholar]
- 49.Antinolfi F., Battistella C., Brunelli L., Malacarne F., Bucci F.G., Celotto D., Cocconi R., Brusaferro S. Absences from work among healthcare workers: Are they related to influenza shot adherence? BMC Health Serv. Res. 2020;20:763. doi: 10.1186/s12913-020-05585-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Murti M., Otterstatter M., Orth A., Balshaw R., Halani K., Brown P.D., Hejazi S., Thompson D., Allison S., Bharmal A., et al. Measuring the impact of influenza vaccination on healthcare worker absenteeism in the context of a province-wide mandatory vaccinate-or-mask policy. Vaccine. 2019;37:4001–4007. doi: 10.1016/j.vaccine.2019.06.014. [DOI] [PubMed] [Google Scholar]
- 51.Costantino C., Casuccio A., Caracci F., Bono S., Calamusa G., Ventura G., Maida C.M., Vitale F., Restivo V. Impact of Communicative and Informative Strategies on Influenza Vaccination Adherence and Absenteeism from Work of Health Care Professionals Working at the University Hospital of Palermo, Italy: A Quasi-Experimental Field Trial on Twelve Influenza Seasons. Vaccines. 2019;8:5. doi: 10.3390/vaccines8010005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Waite N.M., Pereira J.A., Houle S.K.D., Gilca V., Andrew M.K. The impact of influenza on the ability to work, volunteer and provide care: Results from an online survey of Canadian adults 50 years and older. BMC Public Health. 2022;22:2119. doi: 10.1186/s12889-022-14581-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Gianino M.M., Politano G., Scarmozzino A., Stillo M., Amprino V., Di Carlo S., Benso A., Zotti C.M. Cost of Sickness Absenteeism during Seasonal Influenza Outbreaks of Medium Intensity among Health Care Workers. Int. J. Environ. Res. Public Health. 2019;16:747. doi: 10.3390/ijerph16050747. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Puig-Asensio M., Douglas M., Holley S., Kukla M.E., Abosi O., Mascardo L., Carmody B., Gent C., Diekema D.J., Hartley P., et al. Impact of expanded influenza post-exposure prophylaxis on healthcare worker absenteeism at a tertiary care center during the 2017-2018 season. Infect. Control Hosp. Epidemiol. 2019;40:260–261. doi: 10.1017/ice.2018.317. [DOI] [PubMed] [Google Scholar]
- 55.Centers for Disease Control and Prevention . People at Higher Risk of Flu Complications. Centers for Disease Control and Prevention; Atlanta, GA, USA: 2023. [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
Data included in this review article are those provided in published papers.