Abstract
Objectives
This study aimed to identify facilitators and barriers to parent-child communication in pediatric palliative care, providing insights for medical professionals developing targeted interventions to enhance parent-child communication and improve its effectiveness.
Methods
Whittemore and Knafl’s integrative review method was employed to guide a systematic search for literature in six databases (Medline, Embase, CINAHL Complete, PsycINFO, Web of Science, and Cochrane Library). Peer-reviewer articles published in the English language from inception to December 2023. All of the identified studies were screened, extracted, and analyzed independently by two researchers.
Results
Twenty-four articles were included. The findings of the relevant studies were analyzed using thematic analysis. Four themes were identified as facilitators: legacy-making, resilience training programs, guidance from the healthcare team, and positive communication. Seven themes were identified as barriers: denial, being unprepared and evasive, mutual protection, being overwhelmed by painful emotions and overloaded with information, incorrect views of medical professionals and parents, negative communication, and cultural context.
Conclusions
Parents and professionals should avoid myths about protecting the child and encourage open communication that respects the child’s wishes. The specialized pediatric palliative care team should carefully monitor parent-child communication, determine if any obstacles exist, and design more interventions to enhance it.
Keywords: Communication, Palliative care, Parent-child relationship, Pediatrics, Review
What is known?
-
•
Many misconceptions exist about how healthcare professionals communicate with parents or children in pediatric palliative care. Significant research has been devoted to developing educational strategies for effective provider communication with parents or children.
-
•
In pediatric palliative care, parent-child communication faces challenges that can impede emotional openness, information sharing, and treatment adherence.
What is new?
-
•
Open and positive parent-child communication based on mutual trust in pediatric palliative care allows for fluid communication so parties can address each other’s concerns and meet their needs and preferences.
-
•
Denial, the belief that children do not understand, and the protective approach to parent-child communication in pediatric palliative hinder sharing of information and emotions, maintaining close parent-child relationships, and implementing family-centered care.
-
•
This study provides information for developing parent-child communication strategies, enabling parents or professionals to avoid communication misconceptions.
1. Introduction
According to the WHO statistics, in 2022, the number of prevalent cancer cases (1-year) among children aged 0–19 was 197,653 [1]. An estimated 400,000 children worldwide develop cancer, and 100,000 die from it each year [2]. The National Pediatric Tumor Surveillance Annual Report (2022) showed that the average incidence rate of pediatric tumors in China in 2019–2020 was 125.72 per million [3]. Although the cure rate for cancer has generally improved, the mortality rate in children with cancer remains as high as 61% [4]. Pediatric palliative care provides physical, mental, and spiritual care through treatment and bereavement services for children diagnosed with life-threatening diseases and implements patient- and family-centered care [5]. The harmonious relationship between the team, parents, and the child is conducive to timely referral to pediatric palliative care, implementation of patient- and family-centered care, and improvement of the child’s and family’s quality of life [6,7].
Parent-child communication is when parents and children exchange information, thoughts, feelings, and attitudes to improve mutual understanding, trust, and cooperation [8]. It plays an instrumental role in understanding the thoughts and feelings of the children, alleviating their anxiety and depression, promoting harmonious family relationships, and strengthening family cohesion [[9], [10], [11], [12]]. Children with cancer experience a long course of illness, proper and effective communication can be used in decision-making and care planning in the best interests of the child [13]. While parent-child communication has many advantages and has been recommended by several guidelines [14,15], poor prognosis, difficulty in discussing death-related topics, mutual protection between parents and children, and negative consequences of communication may lead to unpromising parent-child communication [[16], [17], [18]].
Parent-child communication in pediatric palliative care has attracted much attention from the children’s perspective. Not only is it related to the needs of the parent and child, but parent-child communication also plays a pivotal role in the relationship between family members, patients, and health professionals [9,19].
Parents need to communicate with their children about their goals and preferences for treatment and symptom relief and to understand their emotional status when facing life-threatening illnesses [19]. Children also need to know from their parents the diagnosis of the disease, its progress, treatments, and professionals’ feedback [20]. Most parents want to maintain a “parental” role in front of their child by controlling the information the child knows. They believe some harmful elements should not be disclosed to the child to avoid unnecessary confusion and psychological burden [21,22]. A minority of parents held a different view, believing that the child should be informed at an appropriate time and open communication should be maintained to ensure mutual trust [23]. From the children’s perspective, they wanted to be informed about any medical details not screened by their parents and be able to communicate with healthcare professionals together with their parents [24].
Many studies have identified communication challenges between medical professionals and family members and relevant training for medical professionals [[25], [26], [27], [28], [29], [30], [31], [32], [33]]. Still, there have been few studies focusing on parent-child communication. Regarding parent-child communication in pediatric palliative care, current studies have focused on evaluating the status and influential factors of communication, the challenges encountered during communications, the experiences of children and their parents during communications, and interventions to enhance parent-child communications [18,22,[34], [35], [36]]. About 40% of parents still do not talk to their children about the prognosis of the disease and death, and understanding the reasons for this is necessary to promote unrestricted communication between parents and children [37]. A comprehensive and holistic understanding of barriers to and facilitators of communication between parents and their children within the pediatric palliative care context is lacking. This study aimed to integrate the facilitators and barriers of parent-child communication in palliative care using an integrative review approach.
2. Methods
2.1. Review design
This design was based on the methods developed by Whittemore and Knafl in 2005 [38], including problem identification, literature search, data evaluation, data analysis, and presentations. This review follows the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 guidelines [39].
2.2. Problem identification
What are the facilitators and barriers to parent-child communication in pediatric palliative care?
2.3. Literature search
Inclusion criteria included 1) related to facilitators of and barriers to communication between parents and their child (18 years or younger), 2) child with life-limiting diseases, 3) studies published in English, and 4) quantitative, qualitative, and mixed design. Exclusion criteria included 1) studies focused on parent-child communication interventions for children in palliative care designed or developed that have not yet been implemented in clinical settings, 2) protocols, editorial, review, case reports and abstracts, 3) without available full text, and 4) non-peer-reviewed literature.
The PICOS and PICoS framework were used as bases for the literature searching. PICOS: P (population): the child with life-limiting diseases and his/her parents; I (intervention): interventions aimed at improving parent-child communication within pediatric palliative care; C (comparison): interventions aimed at improving parent-child communication within pediatric palliative care not used; O (outcomes): parent-child communication; S (study design): quantitative (randomized controlled trials, non-randomized controlled trials, quasi-experimental studies, prospective and retrospective cohort studies, and cross-sectional studies). PICoS: P (population): the child with life-limiting diseases and his/her parents; I (interest of phenomena): facilitators of and barriers to communication between parents and their child (18 years or younger); Co (context): parent-child communication after diagnosis of a child’s life-limiting diseases; S (study design): qualitative (descriptive studies, phenomenological studies, grounded theory studies, case studies, and so forth), and mixed studies.
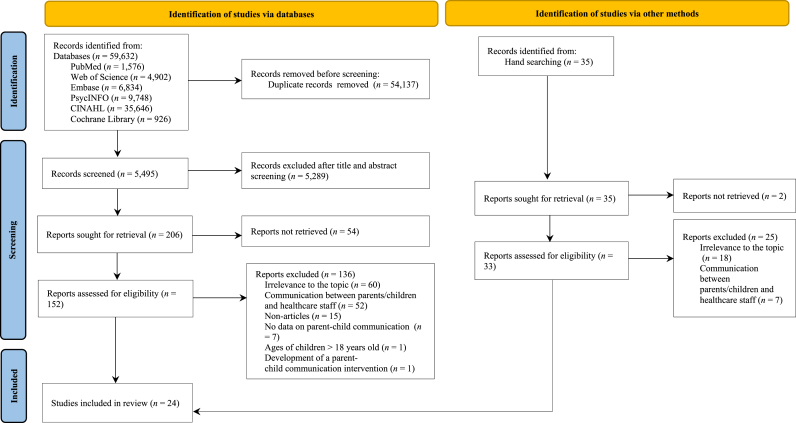
A updated comprehensive search for relevant papers in six electronic databases was conducted in June 2024. The six databases included Medline, Embase, CINAHL, PsycINFO, Web of Science, and Cochrane Library. A combination of MeSH terms, keywords, and synonyms for four search concepts, including “parent,” “child,” “palliative care,” and “communication,” were searched for papers published in English from inception until December 2023 (Appendix A). Manual searches of the reference lists of the identified relevant papers were also carried out. Two authors (M. Zhang, H. Li) independently screened the titles, abstracts, and full texts, where necessary, for eligibility against the inclusion/exclusion criteria. Discrepancies were resolved through group discussions and referrals by a third author (F. Li). The PRISMA flowchart (Fig. 1) represents the review process.
Fig. 1.
PRISMA 2020 flow diagram.
2.4. Quality appraisal
The Johns Hopkins Evidence-Based Practice model was used to assess the level of research evidence: true experimental (level I), quasi-experimental (level II), and non-experimental (level III) [40]. We used the Mixed Methods Approval Tool (MMAT) version 2018 to assess the methodological rigor [41]. This tool contains two screening questions and five methodological questions. Using this checklist, two authors (M. Zhang, H. Li) independently assessed the included studies and negotiated to resolve disagreements (Appendix B).
2.5. Data analysis
The following characteristics were extracted from the included studies: name of the first author, year of publication, location, participants, study design, methods of data collection, and findings. Data were synthesized using the constant comparison method described by Whittemore and Knafl in 2005, which applies to integrative reviews [38]. The following steps were performed: data reduction, data display, data comparison, and conclusion drawing and verification. There is limited research evidence on parent-child communication, and using an integrative research approach allows for a more comprehensive overview of facilitators and barriers by combining the results of multiple research designs. In quantitative studies, facilitators or barriers were determined based on the interventions or research findings. In contrast, in the qualitative study, a three-stage thematic analysis method, i.e., the coding of text “line-by-line,” the development of “descriptive themes,” and the generation of “analytical themes,” was conducted [42]. The research group discussed and agreed upon the extracted contents and analytical themes. 1)Step 1, data reduction. First, we classified the included studies according to their research methodology (quantitative or qualitative), and then we distinguished between specific research methods within the different study types. Next, we created a preliminary classification system (Appendix C), including the literature’s basic characteristics, such as authors, location, research method, study population, and outcomes. Finally, we created an Excel matrix (Appendix D) to identify facilitators and barriers to parent-children communication. The first and second authors extracted data from the original study according to Table 1 and Appendix B. 2) Step 2, data display. The relevant text from the original literature was entered into the classification system (Appendix C and Appendix B). This helps to clarify the relationship between the data and provides an opportunity to integrate data in the same category. The above two steps are used to ensure rigor in data extraction. 3) Step 3, data comparison. We first repeated reading primary sources and made line-by-line comparisons. The content was then coded, and codes with close or similar meanings were categorized hierarchically to form themes. 4) Step 4, conclusion and verification.
The extracted themes were categorized into facilitators and barriers, and the original data from the literature were verified for accuracy and confirmability. The above two steps ensure the rigor and trustworthiness of the data analyzed.
3. Results
3.1. Characteristics of the studies
A total of 59,632 records were retrieved from six electronic databases and manual searches. After deleting duplicates, 5,495 papers were screened based on the inclusion and exclusion criteria, and 5,289 papers were excluded. After reading the full texts of 185 papers, 24 papers were included [12,16,[24], [25], [26],36,[43], [44], [45], [46], [47], [48], [49], [50], [51], [52], [53], [54], [55], [56], [57], [58], [59], [60]]. These studies were conducted in United States (n = 11) [25,36,[43], [44], [45],[49], [50], [51], [52],56,59], three from the United Kingdom [16,24,54], one from China [12], one from Canada [48], one from Korea [47], two from Jordan [26,58], one from Slovakia [46], one from Ireland [57], one from Iran [53], one from Switzerland [55], and one from India [60]. Of the ten quantitative studies, two were randomized clinical trials [25,36], six were cross-sectional studies [44,[50], [51], [52],56,57], one longitudinal study [43], and one retrospective study [16]. Three of the 14 qualitative studies had a descriptive design [47,58,59]. One was a case study [26], seven were phenomenological studies [12,24,45,46,48,55,60], and three were grounded theory studies [49,53,54]. Considering the limited literature on parent-child communication in pediatric palliative care, studies that could not be appraised for quality were also included in the analysis. The basic characteristics and quality assessments of the included studies are presented in Appendix C and Appendix B, respectively.
3.2. Facilitators and barriers to parent-child communication in pediatric palliative care
Four themes were identified as facilitators: legacy-making, resilience training programs, guidance from the healthcare team, and positive communication. There were three subthemes of advice from the healthcare team: identifying poor communication crises promptly, providing guidance, and playing therapy. The barriers included seven themes: denial, being unprepared and evasive, incorrect views of medical professionals and parents, mutual protection, being overwhelmed by painful emotions and overloaded with information, negative communication, and cultural context. There were three subthemes of denial: unrealistic fantasies; fear; lack of time, opportunity, and trust. Facilitators and barriers to parent-child communication extracted from included studies are presented in Appendix D.
3.2.1. Facilitators
3.2.1.1. Legacy-making
Legacy-making is when children living with cancer do specific things to be remembered, such as making crafts for others, willing away belongings, writing letters to loved ones, and giving unique gifts [61]. Two studies used RCTs to identify the impact of legacy-making on parent-child communication [25,36]. Legacy-making could improve the quality of communication between fathers and children [25]. The group that used legacy-making performed better than the control group regarding emotional and school functioning, and digital storytelling provided parents with emotional comfort and facilitated parent-child communication [36].
3.2.1.2. Resilience training programs
Resilience training programs enhance resilience through psychoeducation, positive thinking, cognitive skills, self-compassion skills, gratitude exercises, emotional regulation training, relaxation, and goal setting [62]. Parents who participated in resilience training were found to be better able to listen to and help their children express themselves, manage emotions, and deal with conflict [12].
3.2.1.3. Guidance from healthcare team
1) Identify poor communication crises promptly. Parents and children could access direct and specialized support from the palliative care team. The palliative care team should recognize the desire of the child and parents to express their feelings at an early stage of the diagnosis and provide guidance to the child and parent on communication knowledge, skills, common misconceptions, or any difficulties they may encounter in trying to convey their thoughts and information, to facilitate smooth and effective communication [25]. 2) Provide guidance. Nurses should encourage parents to communicate more therapeutically with their child during treatment so that the parents understand that communication can help in sharing concerns, problem-solving, and achieving desired outcomes [47]. Parents also want the doctor to communicate with the child in an age-appropriate manner. Because disclosing too much to younger children at once can increase the parent’s difficulty in communicating with the child [57]. Communication tools, including toys, books, audio, and video, are also basic materials to guide parents [57]. 3) Play therapy. Play is essential for a child’s physical, psychological, social, and cognitive development. Its role is critical for a child’s learning and communication abilities [63]. Play is also a way of sharing and expressing emotions. During play, children are more likely to understand the significance of the disease and help their parents convey its obscure and unexplainable aspects (e.g., hair loss, explaining the nature of the disease) and make difficult decisions [63]. It also allows the child and their parents to receive psychological support. Play therapy will enable parents and children to express themselves freely, increase mutual understanding, and enhance emotional communication and intimacy between parents [63]. Play therapy has been consistently shown to alleviate children’s emotional distress and abnormal behaviors [57,63]. Parents are the primary communicators with their children.
3.2.1.4. Positive communication
Positive communication should be characterized by proactive communication, warmth, child-centeredness, responsiveness, openness, honesty, hopefulness, naturalness, relaxation, helpfulness, and a positive response to the child’s emotional reactions [45,46,55]. Be sure to respond to the child’s questions directly, focus on and maintain the child’s topic, and positively guide the child in dealing with conflicts that arise in communication [51,52]. Parents and children are equal in their communication, and maintaining a partnership is conducive to communication. Parents should avoid playing the role of executives in communication to minimize parental control and management of their children [24,55].
3.2.2. Barriers
3.2.2.1. Denial
1) Unrealistic fantasies. Parents still hope that their child’s disease can be cured; such unrealistic hope makes them reluctant to tell their child the truth [45]. Parents believe that hope will sustain the child and themselves as the child continues receiving treatment. 2) Fear is a significant obstacle to the communication process [55]. Notably, parents feared addressing the life-threatening nature of the illness. Parents were worried that their child would give up treatment and start coping negatively or react aggressively (with anger, sadness, or frustration) once the child had been told about the truth. Parents were concerned that they could not handle their children’s emotions and reactions during the communication [45]. 3) Lack of time, opportunity, and trust. During the treatment, parents expressed uncertainty about the appropriate time to inform their children [16]. Parents wanted to tell their children but did not know how due to the lack of opportunities and time to share information [43,50]. Parents also reported that their child’s death was sudden and that treatment arrangements took too long before they had a chance to discuss it with their child [50].
3.2.2.2. Being unprepared and evasive
Parents refused to communicate with their children because they felt unprepared, were unsure of how to begin the communication, could not answer their child’s difficult questions and discuss sensitive end-of-life topics, and lacked illness-related information or communication skills [25,26,54,55]. Additionally, the children were not ready to discuss the content and could not discuss and accept lousy news and death-related topics [16]. Some parents were reluctant to share the entire content with their children, which they felt was unnecessary [48]. Parents screened the information provided by the doctor, selecting parts of the information that they thought were appropriate for the child and avoiding serious issues [24,53].
3.2.2.3. Mutual protection
Mutual protection between parents and children is a significant barrier to parent-child communication [26,46,47,49]. The practice of mutual protection tends to discourage the sharing of information and emotions [59]. Parents wanted to protect their children from emotional pain. Some parents prefer to suppress their feelings and protect their children and family members. Children prefer not to share their own doubts or psychological discomfort to avoid harming their parents and increasing their psychological burden.
3.2.2.4. Being overwhelmed by painful emotions and overloaded with information
Parents receive new information from various professionals, including test results, treatment options, disease progression, and prognosis. The amount of information is vast and sometimes contradictory [55]. When parents lack the resources to categorize this information, the considerable input in a short period leads to a lack of understanding of the professional vocabulary, preventing them from receiving effective messages and facing the dilemma of making decisions. Parents suffer complex and severe psychological stress under the pressures of recurring changes in the child’s condition, uncomfortable physical symptoms, and financial burdens [54,56]. In such a situation, parents are still in shock, not knowing what to tell their child, and are not in the mood to talk about these mind-numbing issues.
3.2.2.5. Incorrect views of medical professionals and parents
A common misconception is that parents and professionals underestimate children’s ability to understand illness and death and to cope with bad news, believing that children only need to know what is appropriate for their age and cognitive ability and that they do not need to know further [16]. Therefore, they chose not to inform the children or decided to disclose irrelevant information to protect them from bad news. Medical staff agreed with the parents’ incorrect view that as long as the child did not understand the disease, there was no need to let them know the truth about their disease and its prognosis to prevent possible harm to the child. The medical staff recognized the authority of the parents as caregivers in the caregiving process and believed that the parents should be informed first, not both the children and parents [26].
3.2.2.6. Negative communication
Negative communication encompasses failure to establish a communicative parent-children relationship, avoidance of open and honest communication, maintaining the child’s topic less frequently, and inappropriate reactions to conflicts [26,43,47,56]. It is characterized by hostility, neglect, and intrusiveness [49]. Children preferred to be informed by someone with whom they had a close, long-term relationship [24]. A lack of trust does not allow communication to begin. Inappropriate communication timing, failure of the child to meet parental expectations, disagreements, and arguments can leave a negative impression of communication and jeopardize the next one. Parents are eager to talk to their children. Nevertheless, they cry uncontrollably and feel pain during the discussion [57]. Adult children felt that communicating with their parents caused severe stress. The tense atmosphere of communication and inappropriate conflict resolution between the children and their parents during the communication process created harmful communication experiences [47].
3.2.2.7. Cultural context
Some Eastern cultures have unique sensitivities, repression, and death taboos. They are more accustomed to sharing good news and keeping unpleasant things unspoken, even if the bad news is known to all [53]. This norm is a constraint for everyone. In family conversations, parents refer to “this/that disease” as much as possible instead of using taboo words like “cancer” or “death” [53].
4. Discussion
Children with cancer usually have a strong sense of isolation, and they are eager to talk to those around them about their physical and psychological discomfort, as well as their confusion about the disease [10]. Parents are the closest, most reliable, and most trustworthy people to the child and accompany the child throughout treatment. Successful parent-child communication helps healthcare professionals obtain more information to adjust treatment strategies promptly, provides more up-to-date and accurate information to meet the needs of children and parents, and implements family-centered care. Parent-child communication patterns vary among children, and understanding the facilitators and barriers to parent-child communication can enable healthcare professionals to avoid the obstacles as early as possible, promote harmonious communication, and improve the quality of care.
Legacy-making allows parents and children to share memories of their shared life and eases a parent’s grief [25]. Leaving family members and friends with memories of significant moments that are meaningful and enjoyable is what patients usually think about when they know that they are facing imminent death. Parents can engage in legacy-making with their child three to four months before the child’s death [36]. Legacy-making encompasses a range of activities undertaken with the child, including creating crafts for others, willing away belongings, writing letters to loved ones, and giving unique gifts [61]. These activities can facilitate the child’s long-lasting memory among family and friends. Legacy-making helps parents and children accept reality and communicate openly [25].
Sufficient evidence exists to support play therapy, Internet-assisted play therapy, and role-playing for children’s physical, psychological, and behavioral improvement [63,64]. Play therapy is primarily appropriate for preschool and school-age children. The majority of studies are conducted by the therapist with the child. This can be achieved using a sand tray, painting, dress-up, big-energy, drawing, and playing with archetypes [65]. These activities are usually limited to approximately 30 mins [66].
Most studies and guidelines agree that parents should maintain sincere, unreserved communication with their children and choose an opportune time to tell them honest and accurate information about the disease [67,68]. Parent-child care (PC-CARE) is a behavioral intervention for children in which therapists (psychologists and clinical social workers) teach parents and children positive communication skills and how to use them [69]. Participation in the program has improved children’s adaptive skills, reduced parental stress, and increased parents’ positive communication skills [69]. Attachment and biobehavioral catch-up (ABC) can enhance parent-child communication by instructing parents to follow the child’s lead in answering questions [70].
A close relationship based on rapport and trust is the foundation of communication between parents and their children [71]. Children want the information they receive to be understandable and practical in order to prepare for what will happen [59]. In most cases, parents communicate with their child in a parental role, making the child perceive it not as a harmonious conversation but as a task to be done, which tends to create a sense of burden for the child. In addition, for children in pediatric palliative care, prolonged and repeated hospitalizations, pain from medical tests and treatments, and fear of death increase psychological distress [10]. This further contributes to the child’s inability to express their concerns, feelings adequately, wishes for treatment, and the effects of treatment.
Parents often do not know how to approach honest communication with their children and struggle to find a way to initiate discussions. When the disease is first diagnosed, it is an excellent time to communicate as the child experiences a change in condition or an unusual or altered behavior [68]. Healthcare professionals can start by learning the necessary parent-child communication skills using the COMFORT (C-communication, O-orientation and options, M-mindful communication, F-family, O-openings, R-relating, T-team) communication curriculum and communication toolkit [72]. In addition, doctors or nurses can explain the benefits of good communication to parents and children when examining the child, not just the examination results [73]. In collaboration with colleagues, the professional team can educate parents on effective communication strategies employed in various situations. These strategies include answering questions honestly, providing information in a gradual and structured manner, and allowing for periods of silence [73]. Informing the child of the truth at the time of diagnosis by asking questions such as, “Would you like to know what is going on in your body?” or “What would you like to know?” can build a relationship of trust and determine whether the child would like to communicate [68].
Almost 40% of the parents who had lost a child also said that they were unprepared to cope with their child’s emotional needs and would like to access support from their care team [74]. The professionals develop personalized care plans, manage the child’s condition, meet physical, emotional, and spiritual needs, manage symptoms, and improve the quality of life [5]. The multidisciplinary team is involved in the patient’s entire care and can listen to family members to discuss their concerns, provide feedback on the effectiveness of treatment, treatment wishes, and preferences, and become a mediator of communication [37]. Tools such as two-step interdisciplinary meetings and attachment theory-informed adaptations to communication styles have been developed to enhance doctor-patient communication, facilitate better communication outcomes, and manage difficult doctor-patient relationships [33,75]. Several guidelines recommend that a multidisciplinary team be involved in palliative care for children to provide family-centered care [37,76]. After a comprehensive and systematic assessment, the team offers essential physical, psychological, and spiritual support during the child’s treatment and develops a care plan for the child and family [77].
Health, illness, and social circumstances are inextricably linked. Hiding emotions, talking only about the good and not the bad, and avoiding conflicts about taboo topics have become customs in certain cultures [55]. Indeed, this habit is sometimes not helpful. Hernandez et al.’s study implemented culturally adapted programs to help children adjust to their mother’s cancer [78]. We must recognize that cultural context might be an obstacle that sometimes goes beyond a lack of communication knowledge and skills.
Parents are emotionally unstable and unable to communicate with their children as they go back and forth between hope and disappointment after the doctor has given them a plethora of new information [33]. Information overload tends to confuse parents, leading to a feeling of loss of control and intense anxiety and fear about the disease and treatment [55]. Active music engagement should be available for parents of children with traumatic stress symptoms following their child’s cancer diagnosis [79]. Preventing parental information overload by proactively eliciting their preferences for receiving details regarding the diagnosis and treatment [80]. Professionals can take a step-by-step approach to convey messages to parents, with several mobile programs to help parents better organize and understand them [58]. Parents may discuss emotional distress and seek financial, emotional, and spiritual support from family, friends, and informal groups at family games nights and parents’ afternoon tea/coffee breaks [81]. If parents require a temporary respite from their 24-h caregiving, respite care services are available [82]. Technology-based interventions (mobile device-based resilience training program, internet-based guided self-help program, and m-health supportive care intervention) can help parents obtain more information about the disease, participate in psychosocial program training, and relieve painful emotions [83]. Professionals can employ narrative therapy to facilitate the expression of feelings and sharing experiences by parents and children. This approach can assist parents in managing the emotional responses triggered by children [84].
There are several incorrect views about parent-child communication, especially on the topic of end-of-life discussions, where parents and healthcare providers believe that children are unable to understand the meaning of death or the medical information and that informing them about it will increase the burden, leading to negative emotions in children [68]. Medical professionals should reject the false notion that children cannot comprehend complex medical information. Instead, they should inquire about their patient’s understanding of their illness or impending death and then provide them with further information based on their comprehension. The therapist engages in a discussion with the child regarding the topic of death, allowing the child to express fears and fantasies about the rapid changes in the child's body in a developmentally appropriate manner [68].
Parental avoidance can make the child feel insecure and confused about their situation and alienate the parent-child relationship [47]. Avoidance or attempts to block them can lead to caregivers becoming detached from their child [26]. Most children want to be given accurate information about the disease, even at the same time as their parents [53]. Children say that they have the right to receive truthful information about the disease, no matter how old they are, and that doctors or parents should not selectively inform them of parts of the information, discussing only the good parts and hiding the bad news [67]. In reality, the child can determine what is happening by asking the doctor, talking to other children, or observing their physical condition [59]. To be a good parent in pediatric palliative care, one must make the child aware of reality and face it together, help the child make decisions, and make unselfish decisions in the child’s best interests [17].
Mutual protection is still common in the communication of children with cancer, and many doctors and parents believe that telling the child has no positive impact but rather makes the child feel anxious or panicky [26,58]. Medical personnel should promptly identify which families may be at risk of mutual protection. The disadvantages of mutual protection and the fact that mutual protection does not increase family stability can be delivered at the beginning of the diagnosis of the disease [8]. Demonstrating the benefits of positive parent-child communication to parents will not result in feelings of regret when their child has departed [26].
Pediatric palliative care is patient- and family-centered. Harmonious family relationships facilitate professionals meeting the needs and satisfying the child’s and the parents’ preferences. However, this study had several limitations. First, it only included literature in English and published, missing facilitators and barriers in other language contexts and grey literature. Second, some research on open communication suggests that it should be done in the child’s favor and does not apply to all contexts and all children. This study considered open communication a facilitator because most studies recommended open communication and stated that the benefits outweighed the disadvantages.
5. Conclusions
Facilitators and barriers in parent-child communication among children in palliative care can provide insights for professional care teams. Pediatric palliative care teams play an essential role in parent-child communication. They can design interventions to enhance the role of facilitators and mitigate the impact of barriers by promoting the implementation of legacy-making, creating a pleasant and favorable atmosphere for parent-child communication, providing accurate and precise information to parents, emphasizing the importance of open parent-child communication and its benefits to the child and family, and encouraging parent-child communication. The readiness of most physicians to conduct advance care discussions with parents is already high, but it remains limited to physician-parent communication and does not include the child in the communication. Steps should be taken to address how parents should approach parent-child communication, appropriate topics, and ways to respond to positive or negative reactions from the child. Parents should be available to their children to ensure they are listened to, understood, and supported. Parents should also establish a communicative relationship with the child, avoid an authoritarian attitude, and encourage them to express their thoughts and concerns freely. It should also be noted that older children need the support of their parents to face the pain and fear of the disease while pursuing independence. Parents should maintain appropriate distance from their older children. Modeling parent-child communication that adapts to the local cultural context is also necessary.
Data availability statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
CRediT authorship contribution statement
Miao Zhang: Conceptualization, Methodology, Validation, Formal analysis, Investigation, Data curation, Writing - original draft, Writing - review & editing, Project administration. Huanhuan Li: Conceptualization, Methodology, Validation, Formal analysis, Investigation, Resources, Data curation, Writing - review & editing, Supervision, Project administration. Fei Li: Conceptualization, Methodology, Validation, Formal analysis, Investigation, Resources, Data curation, Writing - review & editing. Yongai Zhang: Conceptualization, Methodology, Validation, Formal analysis, Writing - review & editing, Supervision, Project administration.
Declaration of competing interest
The authors declare that they have no competing interests.
Footnotes
Peer review under responsibility of Chinese Nursing Association.
Supplementary data to this article can be found online at https://doi.org/10.1016/j.ijnss.2024.08.001.
Appendices. Supplementary data
The following is/are the supplementary data to this article.
References
- 1.World Health Organization Data visualization tools for exploring the global cancer burden in 2022. https://gco.iarc.who.int/today/en/dataviz/pie?mode=population&types=2&sexes=0&cancers=39&show_table_pie=1&group_populations=0&age_end=3
- 2.World Health Organization WHO and St. Jude to dramatically increase global access to childhood cancer medicines. https://www.who.int/news/item/13-12-2021-who-and-st.-jude-to-dramatically-increase-global-access-to-childhood-cancer-medicines
- 3.National center for pediatric cancer surveillance . 2022. National pediatric tumor surveillance annual report.https://www.pcscn.org.cn/details?id=60248 [Google Scholar]
- 4.Siegel R.L., Miller K.D., Fuchs H.E., Jemal A. Cancer statistics, 2022. CA CANCER J CLIN. 2022;72(1):7–33. doi: 10.3322/caac.21708. [DOI] [PubMed] [Google Scholar]
- 5.Himelstein B.P., Hilden J.M., Boldt A.M. Weissman D pediatric palliative care. N Engl J Med. 2004;350(17):1752–1762. doi: 10.1056/NEJMra030334. [DOI] [PubMed] [Google Scholar]
- 6.Schröder J., Riiser K., Holmen H. The needs of healthcare personnel who provide home-based pediatric palliative care: a mixed method systematic review. BMC Health Serv Res. 2024;24(1):45. doi: 10.1186/s12913-023-10495-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Oberholzer A.E., Doolittle B.R. Flourishing, religion, and burnout among caregivers working in pediatric palliative care. Int J Psychiatry Med. 2024 doi: 10.1177/00912174241229926. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Gawinski L., Stiel S., Schneider N., Herbst F.A. Communication in dyads of adult children at the end of life with their parents and parents at the end of life with their adult children: findings from a mixed-methods study. Psycho Oncol. 2021;30(9):1535–1543. doi: 10.1002/pon.5728. [DOI] [PubMed] [Google Scholar]
- 9.Orm S., Haukeland Y.B., Vatne T., Fjermestad K. Measuring family communication in pediatric nursing: psychometric properties of the parent-child communication scale – child report (PCCS-cr) J Pediatr Nurs. 2022;62:78–83. doi: 10.1016/j.pedn.2021.10.022. [DOI] [PubMed] [Google Scholar]
- 10.Son H., Haase J., Docherty S.L. Parent-child communication in a childhood cancer context: a literature review. Pediatr Nurs. 2019;45(3):129–141. https://www.proquest.com/scholarly-journals/parent-child-communication-childhood-cancer/docview/2244069546/se-2 [Google Scholar]
- 11.Murphy L.K., Heathcote L.C., Prussien K.V., Rodriguez E.M., Hewitt J.A., Schwartz L.E., et al. Mother-child communication about possible cancer recurrence during childhood cancer survivorship. Psycho Oncol. 2021;30(4):536–545. doi: 10.1002/pon.5600. [DOI] [PubMed] [Google Scholar]
- 12.Luo Y., Li H.C.W., Cheung A.T., Ho L.L.K., Xia W., Zhang J. Evaluating the experiences of parents of children with cancer engaging in a mobile device-based resilience training programme: a qualitative study. Support Care Cancer. 2022;30(7):6205–6214. doi: 10.1007/s00520-022-07066-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Akard T.F., Hendricks-Ferguson V.L., Gilmer M.J. Pediatric palliative care nursing. Ann Palliat Med. 2019;8(Suppl 1):39–48. doi: 10.21037/apm.2018.06.01. [DOI] [PubMed] [Google Scholar]
- 14.Feudtner C., Friebert S., Jewell J., Carter B., Friebert S., Feudtner C., et al. Pediatric palliative care and hospice care commitments, guidelines, and recommendations. Pediatrics. 2013;132(5):966–972. doi: 10.1542/peds.2013-2731. [DOI] [PubMed] [Google Scholar]
- 15.Lopez-Vargas P., Tong A., Crowe S., Alexander S.I., Caldwell P.H.Y., Campbell D.E., et al. Research priorities for childhood chronic conditions: a workshop report. Arch Dis Child. 2019;104(3):237–245. doi: 10.1136/archdischild-2018-315628. [DOI] [PubMed] [Google Scholar]
- 16.van der Geest I.M.M.M.D., van den Heuvel-Eibrink M.M.M.D.P., van Vliet L.M.P., Pluijm S.M.F.P., Streng I.C.M., Emcmdp Michiels, et al. Talking about death with children with incurable cancer: perspectives from parents. J Pediatr. 2015;167(6):1320–1326. doi: 10.1016/j.jpeds.2015.08.066. [DOI] [PubMed] [Google Scholar]
- 17.Gaab E.M., Owens R.G., MacLeod R.D. Primary caregivers' decisions around communicating about death with children involved in pediatric palliative care. J Hospice Palliat Nurs. 2013;15(6):322–329. doi: 10.1097/NJH.0b013e318293dc20. [DOI] [Google Scholar]
- 18.Jalmsell L., Kontio T., Stein M., Henter J.-I., Kreicbergs U. On the child's own initiative: parents communicate with their dying child about death. Death Stud. 2015;39(2):111–117. doi: 10.1080/07481187.2014.913086. [DOI] [PubMed] [Google Scholar]
- 19.Son H., Miller L.E. Family communication about cancer in Korea: a dyadic analysis of parent-adolescent conversation. Glob Qual Nurs Res. 2023;10 doi: 10.1177/23333936231199999. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Yamaji N., Suzuki D., Suto M., Sasayama K., Ota E. Communication tools used in cancer communication with children: a scoping review. Cancers. 2022;14(19):4624. doi: 10.3390/cancers14194624. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Cowfer B.A., Dietrich M.S., Akard T.F. Effect of time on quality of parent-child communication in pediatric cancer. Pediatr Blood Cancer. 2021;68(10) doi: 10.1002/pbc.29091. [DOI] [PubMed] [Google Scholar]
- 22.Barrett L., Fraser L., Noyes J., Taylor J., Hackett J. Understanding parent experiences of end-of-life care for children: a systematic review and qualitative evidence synthesis. Palliat Med. 2023;37(2):178–202. doi: 10.1177/02692163221144084. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Aldridge J., Shimmon K., Miller M., Fraser L.K., Wright B. ‘I can't tell my child they are dying’. Helping parents have conversations with their child. Arch Dis Child Educ Pract Ed. 2017;102(4):182–187. doi: 10.1136/archdischild-2016-311974. [DOI] [PubMed] [Google Scholar]
- 24.Young B., Dixon-Woods M., Windridge K.C., Heney D. Managing communication with young people who have a potentially life threatening chronic illness: qualitative study of patients and parents. BMJ. 2003;326(7384):305–308. doi: 10.1136/bmj.326.7384.305. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Akard T.F., Dietrich M.S., Friedman D.L., Gerhardt C.A., Given B., Hendricks-Ferguson V., et al. Improved parent-child communication following a RCT evaluating a legacy intervention for children with advanced cancer. Prog Palliat Care. 2021;29(3):130–139. doi: 10.1080/09699260.2020.1826778. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Atout M., Hemingway P., Seymour J. The practice of mutual protection in the care of children with palliative care needs: a multiple qualitative case study approach from Jordan. J Pediatr Nurs. 2019;45:e9–e18. doi: 10.1016/j.pedn.2018.12.004. [DOI] [PubMed] [Google Scholar]
- 27.Kaye E.C., Stall M., Woods C., Velrajan S., Gattas M., Lemmon M., et al. Prognostic communication between oncologists and parents of children with advanced cancer. Pediatrics. 2021;147(6):1. doi: 10.1542/peds.2020-044503. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Miller M.K., Blume E.D., Samsel C., Elia E., Brown D.W., Morell E. Parent-Provider communication in hospitalized children with advanced heart disease. Pediatr Cardiol. 2022;43(8):1761–1769. doi: 10.1007/s00246-022-02913-0. [DOI] [PubMed] [Google Scholar]
- 29.He L., Wu H., Li M., Deng X. A qualitative meta-synthesis of the caregiving experiences of adult children providing care for cancer patients in China: implications for multidisciplinary healthcare teams. Health Soc Care Community. 2022;30(6):e3829–e3842. doi: 10.1111/hsc.14073. [DOI] [PubMed] [Google Scholar]
- 30.Dean M., McClement S., Bond J.J.B., Daeninck P.J., Nelson F. Parental experiences of adult child death from cancer. J Palliat Med. 2005;8(4):751. doi: 10.1089/jpm.2005.8.751. [DOI] [PubMed] [Google Scholar]
- 31.Sisk B.A., Harvey K., Friedrich A.B., Antes A.L., Yaeger L.H., Mack J.W., et al. Multilevel barriers and facilitators of communication in pediatric oncology: a systematic review. Pediatr Blood Cancer. 2022;69(1) doi: 10.1002/pbc.29405. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Bartholdson C., Kreicbergs U., Sveen J., Lövgren M., Pohlkamp L. Communication about diagnosis and prognosis—a population-based survey among bereaved parents in pediatric oncology. Psycho Oncol. 2022;31(12):2149–2158. doi: 10.1002/pon.6058. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Archambault-Grenier M.A., Roy-Gagnon M.H., Gauvin F., Doucet H., Humbert N., Stojanovic S., et al. Survey highlights the need for specific interventions to reduce frequent conflicts between healthcare professionals providing paediatric end-of-life care. Acta Paediatr. 2018;107(2):262–269. doi: 10.1111/apa.14013. [DOI] [PubMed] [Google Scholar]
- 34.Goethals E.R., Soenens B., Wit M., Vansteenkiste M., Laffel L.M., Casteels K., et al. “Let's talk about it” the role of parental communication in adolescents' motivation to adhere to treatment recommendations for type 1 diabetes. Pediatr Diabetes. 2019;20(7):1025–1034. doi: 10.1111/pedi.12901. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Lykke C., Ekholm O., Schmiegelow K., Olsen M., Sjøgren P. End-of-life communication: a nationwide study of bereaved parents' perceptions. BMJ Support Palliat Care. 2022;12(e4):e616–e622. doi: 10.1136/bmjspcare-2018-001709. [DOI] [PubMed] [Google Scholar]
- 36.Akard T.F., Dietrich M.S., Friedman D.L., Hinds P.S., Given B., Wray S., et al. Digital storytelling: an innovative legacy-making intervention for children with cancer. Pediatr Blood Cancer. 2015;62(4):658–665. doi: 10.1002/pbc.25337. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Snaman J., McCarthy S., Wiener L., Wolfe J. Pediatric palliative care in oncology. J Clin Oncol. 2020;38(9):954–962. doi: 10.1200/JCO.18.02331. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Whittemore R., Knafl K. The integrative review: updated methodology. J Adv Nurs. 2005;52(5):546–553. doi: 10.1111/j.1365-2648.2005.03621.x. [DOI] [PubMed] [Google Scholar]
- 39.Page M.J., McKenzie J.E., Bossuyt P.M., Boutron I., Hoffmann T.C., Mulrow C.D., et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. doi: 10.1136/bmj.n71. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Dang D., Dearholt S., Bissett K., Ascenzi J., Whalen M. fourth ed. Sigma Theta Tau International; Indianapolis: 2022. Johns hopkins evidence-based practice for nurses and healthcare professionals: model and guidelines. [Google Scholar]
- 41.Hong Q.N., Gonzalez-Reyes A., Pluye P. Improving the usefulness of a tool for appraising the quality of qualitative, quantitative and mixed methods studies, the Mixed Methods Appraisal Tool (MMAT) J Eval Clin Pract. 2018;24(3):459–467. doi: 10.1111/jep.12884. [DOI] [PubMed] [Google Scholar]
- 42.Thomas J., Harden A. Methods for the thematic synthesis of qualitative research in systematic reviews. BMC Med Res Methodol. 2008;8:45. doi: 10.1186/1471-2288-8-45. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Keim M.C., Lehmann V., Shultz E.L., Winning A.M., Rausch J.R., Barrera M., et al. Parent-child communication and adjustment among children with advanced and non-advanced cancer in the first year following diagnosis or relapse. J Pediatr Psychol. 2017;42(8):871–881. doi: 10.1093/jpepsy/jsx058. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Kassam A., Skiadaresis J., Alexander S., Wolfe J. Differences in end-of-life communication for children with advanced cancer who were referred to a palliative care team. Pediatr Blood Cancer. 2015;62(8):1409–1413. doi: 10.1002/pbc.25530. [DOI] [PubMed] [Google Scholar]
- 45.Smith L.E., Maybach A.M., Feldman A., Darling A., Akard T.F., Gilmer M.J. Parent and child preferences and styles of communication about cancer diagnoses and treatment. J Pediatr Oncol Nurs. 2019;36(6):390–401. doi: 10.1177/1043454219859235. [DOI] [PubMed] [Google Scholar]
- 46.Slaninka M., Krajmer P., Kolenova A. Main topics related to the disease, death, and dying in communication between parents and their adolescent children with incurable cancer. Bratisl Lek Listy. 2021;122(8):572–576. doi: 10.4149/bll_2021_091. [DOI] [PubMed] [Google Scholar]
- 47.Son H., Yang Y., Crego N., Docherty S.L. Communication Challenges in Korean families coping with adolescent cancer. Oncol Nurs Forum. 2020;47(6):E190–E198. doi: 10.1188/20.ONF.E190-E198. [DOI] [PubMed] [Google Scholar]
- 48.Zelcer S., Cataudella D., Cairney A.E.L., Bannister S.L. Palliative care of children with brain tumors: a parental perspective. Arch Pediatr Adolesc Med. 2010;164(3):225–230. doi: 10.1001/archpediatrics.2009.284. [DOI] [PubMed] [Google Scholar]
- 49.Nuss S.L. Redefining parenthood: surviving the death of a child. Cancer Nurs. 2014;37(1):E51–E60. doi: 10.1097/NCC.0b013e3182a0da1f. [DOI] [PubMed] [Google Scholar]
- 50.Kenney A.E., Bedoya S.Z., Gerhardt C.A., Young-Saleme T., Wiener L. End of life communication among caregivers of children with cancer: a qualitative approach to understanding support desired by families. Palliat Support Care. 2021;19(6):715–722. doi: 10.1017/S1478951521000067. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Rodriguez E.M., Murphy L., Vannatta K., Gerhardt C.A., Young-Saleme T., Saylor M., et al. Maternal coping and depressive symptoms as predictors of mother-child communication about a child's cancer. J Pediatr Psychol. 2016;41(3):329–339. doi: 10.1093/jpepsy/jsv106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Rodriguez E.M., Dunn M.J., Zuckerman T., Hughart L., Vannatta K., Gerhardt C.A., et al. Mother-Child communication and maternal depressive symptoms in families of children with cancer: integrating macro and micro levels of analysis. J Pediatr Psychol. 2013;38(7):732–743. doi: 10.1093/jpepsy/jst018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Bahrami M., Namnabati M., Mokarian F., Oujian P., Arbon P. Information-sharing challenges between adolescents with cancer, their parents and health care providers: a qualitative study. Support Care Cancer. 2017;25(5):1587–1596. doi: 10.1007/s00520-016-3561-z. [DOI] [PubMed] [Google Scholar]
- 54.Gibson F., Kumpunen S., Bryan G., Forbat L. Insights from parents of a child with leukaemia and healthcare professionals about sharing illness and treatment information: a qualitative research study. Int J Nurs Stud. 2018;83:91–102. doi: 10.1016/j.ijnurstu.2018.04.008. [DOI] [PubMed] [Google Scholar]
- 55.Badarau D.O., Wangmo T., Ruhe K.M., Miron I., Colita A., Dragomir M., et al. Parents' challenges and physicians' tasks in disclosing cancer to children. A qualitative interview study and reflections on professional duties in pediatric oncology. Pediatr Blood Cancer. 2015;62(12):2177–2182. doi: 10.1002/pbc.25680. [DOI] [PubMed] [Google Scholar]
- 56.Murphy L.K., Preacher K.J., Rights J.D., Rodriguez E.M., Bemis H., Desjardins L., et al. Maternal communication in childhood cancer: factor analysis and relation to maternal distress. J Pediatr Psychol. 2018;43(10):1114–1127. doi: 10.1093/jpepsy/jsy054. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Kenny M., Duffy K., Hilliard C., O'Rourke M., Fortune G., Smith O., et al. ‘It can be difficult to find the right words’: parents' needs when breaking news and communicating to children with cancer and their siblings. J Psychosoc Oncol. 2021;39(4):571–585. doi: 10.1080/07347332.2021.1890305. [DOI] [PubMed] [Google Scholar]
- 58.Alarjeh G., Boufkhed S., Alrjoub W., Guo P., Yurduşen S., Ahmed F., et al. Communication and information sharing with pediatric patients including refugees with advanced cancer, their caregivers, and health care professionals in Jordan: a qualitative study. Front Oncol. 2023;13 doi: 10.3389/fonc.2023.1118992. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Stanek C., Garcia D., Olsavsky A.L., Hill K.N., Himelhoch A.C., Kenney A.E., et al. Communication within families about advanced pediatric cancer: a qualitative study. Palliat Support Care. 2022:1–8. doi: 10.1017/S1478951522001705. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Salins N., Muckaden M.A., Ghoshal A., Jadhav S. Experiences of adolescents with cancer attending a tertiary care cancer centre: a thematic analysis. Indian J Palliat Care. 2022;28(4):428–433. doi: 10.25259/IJPC_24_2022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Foster T.L., Gilmer M.J., Davies B., Barrera M., Fairclough D., Vannatta K., et al. Bereaved parents' and siblings' reports of legacies created by children with cancer. J Pediatr Oncol Nurs. 2009;26(6):369–376. doi: 10.1177/1043454209340322. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Joyce S., Shand F., Tighe J., Laurent S.J., Bryant R.A., Harvey S.B. Road to resilience: a systematic review and meta-analysis of resilience training programmes and interventions. BMJ Open. 2018;8(6) doi: 10.1136/bmjopen-2017-017858. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Koukourikos K., Tzeha L., Pantelidou P., Tsaloglidou A. The importance of play during hospitalization of children. Mater Soc Med. 2015;27(6):438–441. doi: 10.5455/msm.2015.27.438-441. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Frasier K., Burker E., Chan D.V. Tablet therapy as an assistive technology-based treatment for anxiety in pediatric oncology. Assistive technology. 2022;34(5):533–542. doi: 10.1080/10400435.2021.1884919. [DOI] [PubMed] [Google Scholar]
- 65.van Breemen C. Using play therapy in paediatric palliative care: listening to the story and caring for the body. Int J Palliat Nurs. 2009;15(10):510–514. doi: 10.12968/ijpn.2009.15.10.44888. [DOI] [PubMed] [Google Scholar]
- 66.Li R., Shen X., Zhang L., Chan Y., Yao W., Zhang G., et al. Effects of Child Life intervention on the symptom cluster of pain-anxiety-fatigue-sleep disturbance in children with acute leukemia undergoing chemotherapy. Asia Pac J Oncol Nurs. 2023;10(7) doi: 10.1016/j.apjon.2023.100243. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Jalmsell L., Lövgren M., Kreicbergs U., Henter J.-I., Frost B.-M. Children with cancer share their views: tell the truth but leave room for hope. Acta Paediatr. 2016;105(9):1094–1099. doi: 10.1111/apa.13496. [DOI] [PubMed] [Google Scholar]
- 68.Beale E.A., Baile W.F., Aaron J. Silence is not golden: communicating with children dying from cancer. J Clin Oncol. 2005;23(15):3629–3631. doi: 10.1200/JCO.2005.11.015. [DOI] [PubMed] [Google Scholar]
- 69.Hawk B.N., Timmer S.G., Armendariz L.A.F., Boys D.K., Urquiza A.J., Fernandez Y.G.E. Improving children's behavior in seven sessions: a randomized controlled trial of parent-child care (PC-CARE) for children aged 2-10 years. Child Psychiatry Hum Dev. 2024;55(2):336–349. doi: 10.1007/s10578-022-01406-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Zajac L., Raby K.L., Dozier M. Sustained effects on attachment security in middle childhood: results from a randomized clinical trial of the attachment and biobehavioral catch-up (ABC) intervention. J Child Psychol Psychiatry. 2020;61(4):417–424. doi: 10.1111/jcpp.13146. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Huang L., Wu W., Yang F. Parenting style and subjective well-being in children and youth: a meta-analysis. Psychol Rep. 2024 doi: 10.1177/00332941241256883. 332941241256883. [DOI] [PubMed] [Google Scholar]
- 72.Wittenberg E., Reb A., Kanter E. Communicating with patients and families around difficult topics in cancer care using the COMFORT communication curriculum. Semin Oncol Nurs. 2018;34(3):264–273. doi: 10.1016/j.soncn.2018.06.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Schuetze D., Ploeger C., Hach M., Seipp H., Kuss K., Bosner S., et al. Care practices of specialized outpatient pediatric palliative care teams in collaboration with parents: results of participatory observations. Palliat Med. 2022;36(2):386–394. doi: 10.1177/02692163211065294. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Feraco A.M., Dussel V., Orellana L., Kang T.I., Geyer J.R.M.D., Rosenberg A.R., et al. Tumor talk and child well-being: perceptions of “good” and “bad” news among parents of children with advanced cancer. J Pain Symptom Manage. 2017;53(5):833–841. doi: 10.1016/j.jpainsymman.2016.11.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Swanepoel A. Fifteen-minute consultation: attachment as a model to understand and manage difficult doctor–parent relationships. Arch Dis Child Educ Pract Ed. 2019;104(4):178–182. doi: 10.1136/archdischild-2018-315570. [DOI] [PubMed] [Google Scholar]
- 76.Carter K., Raybin J., Ambroggio L., Frydenlund M., Thomas J., Squiers K., et al. Inpatient pediatric palliative care consult requests and recommendations. J Pediatr Health Care. 2022;36(3):248–255. doi: 10.1016/j.pedhc.2021.10.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Zahedi F., Kadivar M., Khanali Mojen L., Asadabadi M., Tajalli S., Ilkhani M., et al. The ethical challenges of palliative care from the perspectives of pediatricians: a qualitative study in Iran. Front Pediatr. 2022;10 doi: 10.3389/fped.2022.928476. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Hernandez A., Reyes C.L., Garcia I., Palacios R.L. “I Felt Defeated. I Felt Helpless”: social determinants of health influencing the cancer survivorship of a young latina mother. J Cancer Ther. 2022;13(7):440–449. doi: 10.4236/jct.2022.137039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Robb S.L., Stegenga K., Perkins S.M., Stump T.E., Moody K.M., Henley A.K., et al. Mediators and moderators of active music engagement to reduce traumatic stress symptoms and improve well-being in parents of young children with cancer. Integr Cancer Ther. 2023;22 doi: 10.1177/15347354231218266. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Hendricks-Ferguson V.L., Haase J.E. Parent perspectives of receiving early information about palliative and end-of-life care options from their child's pediatric providers. Cancer Nurs. 2019;42(4):E22–E30. doi: 10.1097/NCC.0000000000000589. [DOI] [PubMed] [Google Scholar]
- 81.Gunter M.D., Duke G. Social support to reduce uncertainty in childhood cancer in south Texas: a case study. J Pediatr Oncol Nurs. 2019;36(3):207–218. doi: 10.1177/1043454219835450. [DOI] [PubMed] [Google Scholar]
- 82.Hizanu Dumitrache M., Boeriu E., Tanasescu S., Balan A., Oprisoni L.A., Popa M.V., et al. Benefits of respite services on the psycho-emotional state of families of children admitted to hospice palliative care unit: preliminary study on parents' perceptions. Healthcare (Basel) 2024;12(7):748. doi: 10.3390/healthcare12070748. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Luo Y., Xia W., Cheung A.T., Ho L.L.K., Zhang J., Xie J., et al. Effectiveness of a mobile device-based resilience training program in reducing depressive symptoms and enhancing resilience and quality of life in parents of children with cancer: randomized controlled trial. J Med Internet Res. 2021;23(11) doi: 10.2196/27639. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Jackson A.C., Liang R.P., Frydenberg E., Higgins R.O., Murphy B.M. Parent education programmes for special health care needs children: a systematic review. J Clin Nurs. 2016;25(11–12):1528–1547. doi: 10.1111/jocn.13178. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.