Abstract
Purpose
The association between serum vitamin D level and cataract remains controversial. This study aims to evaluate the association between vitamin D level and cataract.
Methods
In this study, articles in the PubMed, Web of Science, and EMBASE databases were searched up to 30 August 2023 and 626 articles were screened. Four studies involving a total of 10,928 subjects with cataract and 10,117 control subjects met the inclusion criteria.
Results
Decreased serum vitamin D level was associated with higher incidence of cataract (P = 0.047; MD: -4.87; 95%CI: [-9.67, -0.07]). In the subgroup analysis by sex, a significant association was found between serum vitamin D level and cataract in both male (P = 0.01, MD: -2.15,95%CI: [-3.83, -0.46]) and female (P < 0.01; MD: -6.67,95%CI: [-8.20, -5.14]).In the subgroup analysis by the types of cataract, significant association was found between serum vitamin D level and nuclear (P < 0.01; MD: -10.48; 95%CI: [-12.72, -8.24]) and posterior subcapsular cataract (P = 0.02; MD: -6.05; 95%CI: [-11.30, -0.80]) but not in cortical cataract (P = 0.14; MD: -6.74; 95%CI: [-15.70, 2.22]).
Conclusion
This meta-analysis revealed potential association between serum vitamin D level and cataract, more significant in female, and the subtypes of nuclear and posterior subcapsular cataract.
Supplementary Information
The online version contains supplementary material available at 10.1007/s00417-024-06592-w.
Keywords: Cataract, Vitamin D, Serum vitamin D level, Types of cataract
Introduction
Cataract, opacification of the lens, is the main cause of blindness and visual impairment in middle-income and low-income countries [1, 2]. Studies have shown that of the 36 million people who are blind worldwide, about 1/3 of them are due to cataract and among the population of 216.6 million people with moderate or severe visual impairment, 52.6 million of them are attributed to cataract [3]. It is a complex multifactorial disease influenced by various genetic and environmental factors [4, 5]. Vitamin D plays various roles in preserving human health, encompassing the regulation of gene expression, anti-inflammatory, and anti-apoptotic properties [6]. A number of studies have shown that vitamin D deficiency may have an adverse impact on ocular and visual health, such as age-related macular degeneration, glaucoma and diabetic retinopathy [7–13].
Although clinical studies of vitamins and cataract have been the subject of frequent inquiry [14, 15], compared to other types of vitamins, there is still controversy about the association between vitamin D and cataract. Aidenloo reported that serum 25(OH) D level were inversely associated with cataract in women, and no such association has been found in men [16]. In contrast, Jee et, al concluded that serum vitamin D was associated with cataract in men and not in women [17]. There is also controversy regarding different types of cataract. Park suggested negative association between serum 25(OH) D level and the risk of nuclear cataract [18], while Rao's study found no significant association between the two [19].
However, so far, there is no systematic review on the association between vitamin D and cataract, and in order to advance knowledge based on the available evidence, we conducted a systematic review and meta-analysis with the aim of assessing the association between serum vitamin D level and cataract.
Methods
We conducted and reported this systematic review following the latest PRISMA guidelines [20]. The study protocol was registered on PROSPERO under the identification number CRD42023467576.
Search strategy
We searched three databases: PubMed, Embase, and Web of Science. These were published in English from the inception of each database to 30 August 2023. The search strategy consisted of two main elements connected by the AND operator: (1) cataract; and (2) vitamin D. For each of these core components, we identified controlled vocabulary (specifically, Medical Subject Headings [MeSH] terms) as well as relevant keywords. Complete information regarding all search terms can be found in the supplemental file.
Inclusion criteria and study selection
All studies had to meet the following inclusion criteria: (1) Two or more comparison groups (cataract and control groups) were included; (2) Studies with an outcome of a laboratory assessment of serum or plasma vitamin D level; (3) The study was published in English; (4) The full text of the article was accessible; and (5) The subjects were human. Animal studies, case reports, reviews, abstracts and editorials were excluded.
The articles were imported into a reference management software (Covidence; Veritas Health Innovation Ltd) for the purpose of study selection. Two reviewers (ZZJ and ZMX) independently assessed the titles and abstracts of the studies for eligibility. In cases of disagreement, a third reviewer (VLY) resolved the discrepancies. All studies identified as potentially eligible based on the title and abstract screening underwent a comprehensive full-text review by two independent reviewers (ZZJ and ODSC) using the same predetermined criteria. Any discrepancies in eligibility ratings were addressed through discussion or involvement of the third reviewer (VLY).
Data extraction and risk of bias assessment
From each article, the following data were collected and reviewed independently by two reviewers (ZZJ and ZMX): first author, publication year, country/region, age, sample size, male and female size, study design, type of cataract and considered vitamin D. The data extracted by the two reviewers were consistent. The risk of bias in case–control studies and cross-sectional study were assessed using the Newcastle–Ottawa Scale, with ratings categorized as high (≥ 8 stars), moderate (6–7 stars), or low (< 6 stars) [21].
Statistical analysis
For each study included in the analysis, we calculated the mean difference (MD) in vitamin D level between the cataract and control groups, along with their corresponding 95% confidence interval (CI). To assess the heterogeneity among the pooled studies, we utilized both the χ2-based Q statistic and I2 metrics. In cases where heterogeneity was detected (p < 0.05 or I2 > 50%), a random-effects model was used; otherwise, a fixed-effects model was used. Meanwhile, we conducted subgroup analysis to assess the potential heterogeneity by gender and different types of cataract. For studies that only reported the means and standard deviations of individual subgroups, we followed the recommended approach by the Cochrane system to combine the mean and standard deviation of the two reported subgroups into a single group [22]. Furthermore, we conducted a sensitivity analysis using the leave-one-out strategy to examine the stability of the results. This involved systematically excluding individual studies from the analysis and assessing if their omission significantly affected the overall findings. For assessing publication bias in the included articles, we used the Egger's test. Statistical significance was defined as a p-value less than 0.05. All statistical analyses were performed using R (version 4.2.3).
Results
Search results and study characteristics
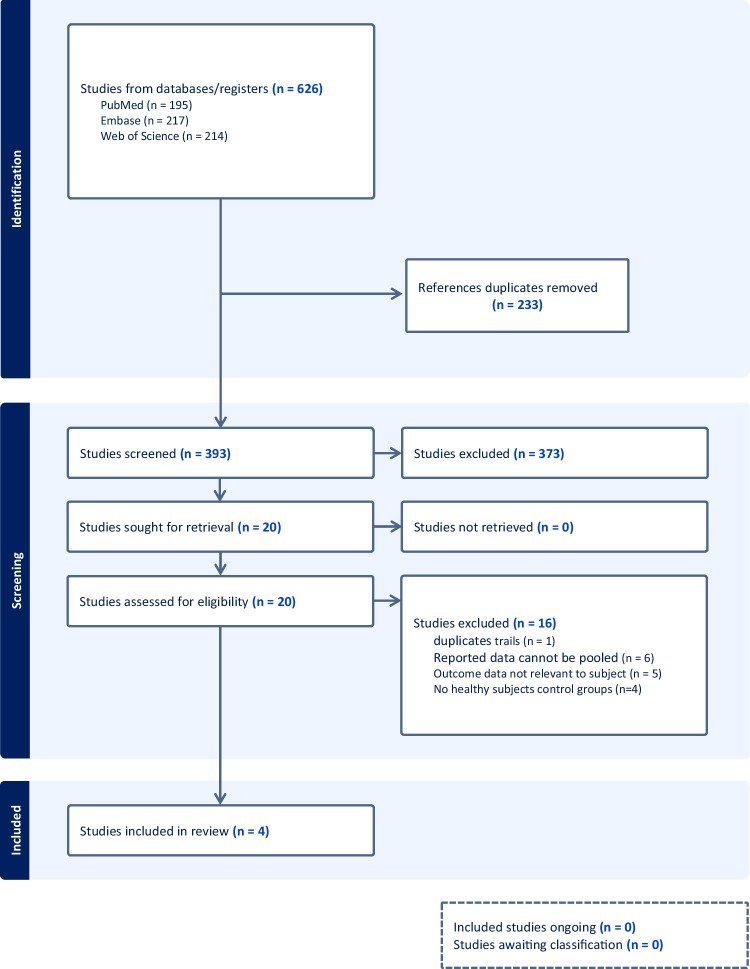
During the initial search of the three databases, a total of 626 studies were identified. After removing duplicate publications, 393 articles were screened for eligibility. Of the 20 studies eligible for full-text review, 4 met the inclusion criteria (Fig. 1 presented a flowchart that illustrated the process of conducting the article search in the study). Table 1 summarizes the study characteristics, designs, and findings. The final analysis included four studies, consisting of three case–control studies [16, 23, 24] and one cross-sectional studies [17]. Among them, two studies analyzed different types of cataract [16, 23], and three studies conducted analyses based on different genders [16, 17, 24]. The results of the quality assessment of the included studies are shown in Table 2. The quality score of these studies ranged from 6 to 7.
Fig. 1.
PRISMA Flow Diagram
Table 1.
Characteristics of included studies of vitamin D and cataract
| Author, Year |
Country | Study design | Different cataract type | Assay for vitamin D |
Cataract group | Control group | ||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| No | Male | Age | Vitamin D, ng/ml | No | Female | Age | Vitamin D, ng/ml | |||||
|
Abdellah 2019 [23] |
Egypt | Case–control study | Yes |
Serum,25(OH)D3; CMIA |
325 | 155 | 63.1 ± 6.3 | 7.6 ± 5.5 | 385 | 180 | 62.9 ± 6.7 | 18.5 ± 9.6 |
|
Aidenloo 2022 [16] |
Iran | Case–control study | Yes |
Serum,25(OH)D3; CMIA |
1241 | 636 | 64.7 ± 8.5 | 30.3 ± 9.9 | 200 | 100 | 62.6 ± 8.0 | 34.5 ± 8.5 |
|
Jee 2015 [17] |
Korea | Cross-sectional study | NO |
Serum,25(OH)D3; Radioimmunoassay |
9325 | Conflict | 63.6 ± 19.3 | 19.1 ± 9.7 | 9479 | Conflict | 49.5 ± 9.7 | 18.4 ± 9.7 |
|
Öktem 2021 [24] |
Turkey | Case–control study | NO |
Serum,25(OH)D3 CMIA |
37 | 18 | 48.1 ± 8.5 | 15.6 ± 8.4 | 53 | 27 | 49.3 ± 7.8 | 20.8 ± 7.1 |
CMIA: chemiluminescent microparticle immunoassay
Table 2.
Quality of included studies
| Author, Year |
Selection | comparability | Exposure | Overall score | Quality | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Case definition adequate | Representativeness of the cases | Selection of controls | Definition Of controls |
Comparability of cases and controls on the bias of the design or analysis | Ascertainment of exposure | Same method of ascertainment for cases and controls | Non-response rate | |||
| Abdellah 2019 [23] | 1 | 1 | 0 | 1 | 1 | 1 | 1 | 0 | 6 | Medium |
|
Aidenloo 2022 [16] |
1 | 1 | 1 | 1 | 1 | 1 | 1 | 0 | 7 | Medium |
|
Jee 2015 [17] |
1 | 1 | 1 | NA | 1 | 1 | 1 | 0 | 6 | Medium |
|
Öktem 2021 [24] |
1 | 1 | 0 | 1 | 1 | 1 | 1 | 0 | 6 | Medium |
NA: not applicable
Association between blood 25(OH)D concentration and cataract
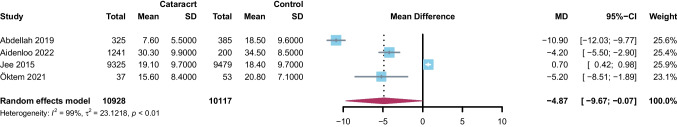
In all, the 4 studies had a total of 10,928 patients in the cataract group and 10,117 patients in the control group. The blood 25(OH)D level in the cataract group was lower than control group (P = 0.047, MD: -4.87,95%CI: [-9.67, -0.07]; Fig. 2), and there was significant heterogeneity among studies (I2 = 99%, p < 0.01).
Fig. 2.
Forest plot of the mean differences in the serum 25(OH)D level between cataract and control groups
Subgroup analysis
Sex
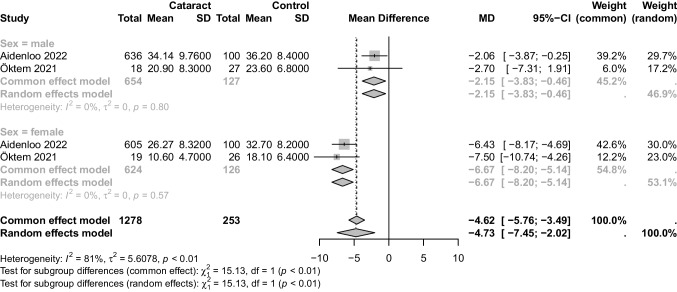
There were three studies that investigated the relationship between vitamin D and cataract in male and female subgroups. However, due to conflicting participant numbers of male and female in one of the studies, that particular study was excluded from the analysis [17]. As a result, a total of two studies were included in the analysis. Significant association between the serum 25(OH)D level and cataract was found in male (P = 0.01, MD: -2.15,95%CI: [-3.83, -0.46], I2 = 0; Fig. 3) and female(P < 0.01, MD: -6.67,95%CI: [-8.20, -5.14], I2 = 0; Fig. 3).
Fig. 3.
Forest plot of subgroup analysis of the associations between serum 25(OH)D level and cataract in different gender groups
Different types of cataract
Significant associations with serum 25(OH)D level were found in nuclear cataract (P < 0.01, MD: -10.48,95%CI: [-12.72, -8.24], I2 = 77%; Fig. 4) and posterior subcapsular cataract (P = 0.02, MD: -6.05,95%CI: [-11.30, -0.80], I2 = 94%; Fig. 4) but not in cortical cataract (P = 0.14, MD: -6.74,95%CI: [-15.70, 2.22], I2 = 98%; Fig. 4) and control group,
Fig. 4.
Forest plot of subgroup analysis of the association between serum 25(OH)D level and different types of cataract
Risk of bias
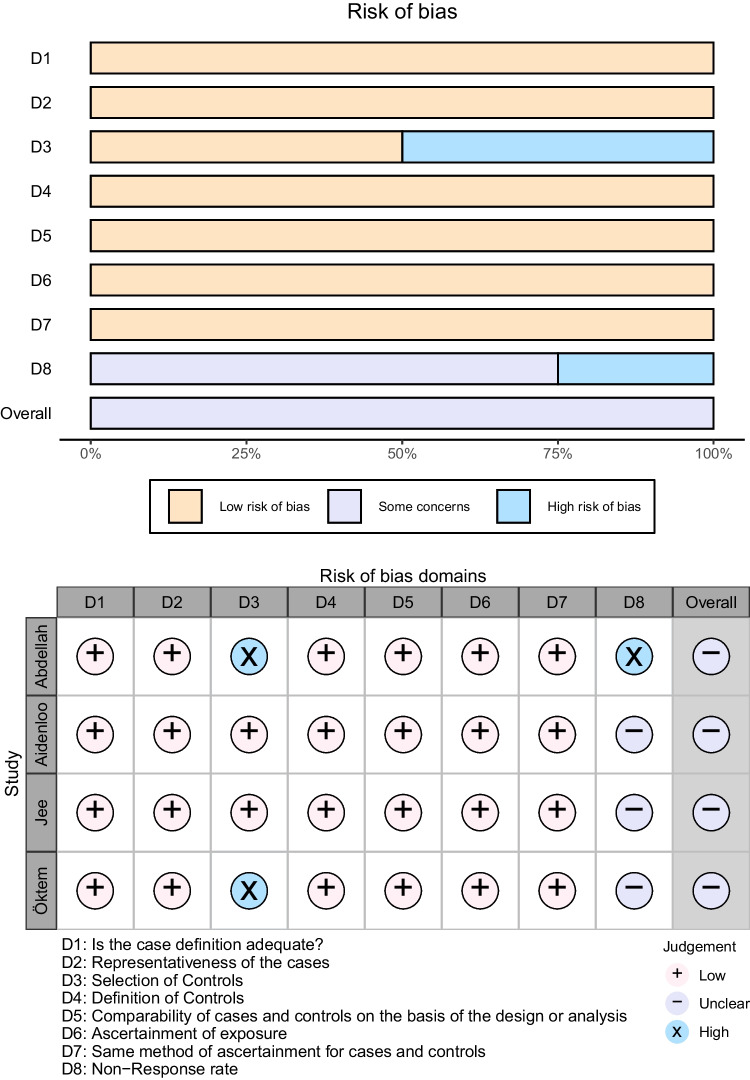
We assessed risk of bias by using the quality of the studies. All four articles were rated as having some concerns. Domain level and overall risk of bias for studies are presented in Fig. 5. There was no significant difference in publication bias (t = -1.66, P = 0.24). Moreover, we only included studies published in English, so there was a high risk of publication language bias.
Fig. 5.
Risk of bias of all included studies
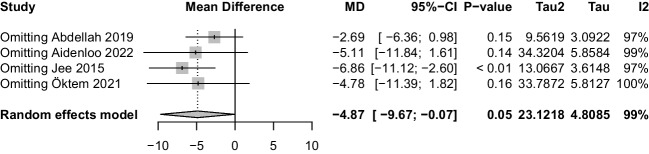
Sensitivity analysis
We conducted sensitivity analysis for these studies, the result showed that one study influenced the meta-analysis results. (Fig. 6).
Fig. 6.
Forest plot of sensitivity analysis
Heterogeneity
Statistical heterogeneity
Three of the included studies [16, 23, 24] reported serum vitamin D level using mean and standard deviation (SD), while one study [17] used mean and standard error (SE). Aidenloo [16] conducted analyses on the relationship between serum vitamin D level and cataract separately for different genders and different types of cataract, without analyzing the entire population as a whole. Therefore, there is a certain degree of heterogeneity statistically.
Clinical heterogeneity
The four included studies recruited patients from different age groups. Abdellah [23] and Aidenloo [16] included cataract patients with an average age of around 60 years. Jee [17] included participants from Korea National Health and Nutrition Examination Survey (KNHANES), with the cataract group having a mean age of 63.6 and the control group having a mean age of 49.5. Additionally, Öktem included a population of young adult cataract patients aged below 60 years. Furthermore, one study was conducted in Africa [23], while the remaining three studies were conducted in Asia [16, 17, 24].
Methodological heterogeneity
The four included studies all measured serum 25-hydroxyvitamin D level. However, there were differences in the measurement methods and study designs among the studies. Abdellah, Aidenloo, and Öktem utilized chemiluminescent microparticle immunoassay, [16, 23, 24] while Jee used radioimmunoassay for measuring vitamin D level [17]. Furthermore, Abdellah, Aidenloo, and Öktem conducted case–control studies [16, 23, 24], while Jee conducted a population-based cross-sectional study [17].
Discussion
This is the first meta-analysis of the association between serum vitamin D level and cataract. In our study, a total of 4 studies were included, which included 10,928 participants in the cataract group and 10,117 participants in the control group. Our study suggested that a negative association between serum vitamin D level and cataract, supporting previous studies that reported similar results [23–25]. There may be various underlying mechanisms. Vitamin D has been shown to possess antioxidant properties, which may protect against oxidative stress and cellular damage in the lens of the eye [26, 27]. Additionally, due to its positive impact on the photooxidation of proteins, vitamin D potentially exhibits a preventive effect in the development of cataract [17, 28, 29]. Moreover, vitamin D is closely related to calcium, and the protective effect of calcium dobesilate against steroid-mediated cataract was reported in animal experiments by Velpandian and colleagues, probably due to its antioxidant and aldose reductase inhibitor properties [30]. Conversely, some studies reported that overloading of intracellular calcium concentrations may cause abnormal degradation of proteins and cell death, which in turn may lead to structural abnormalities in the lens [31, 32].
In the subgroup analysis of sex, we observed a significant association between serum vitamin D level and cataract in female and male. This result is different from Jee’s study, which vitamin D level is associated with cataract in men but not in women [17], possibly because when conducting the subgroup analysis, Jee’s study was not included due to inconsistent numbers of male and female between two tables in their study. Therefore, only two studies were included in our study for the subgroup analysis of sex [16, 24]. Also, Rao’s study reported that serum vitamin D level was protective against nuclear cataract in women younger than 70 years old only [19]. The reason for this discrepancy is unclear, and further studies are warranted.
There are three main types of aged-related cataract: nuclear, cortical, and posterior subcapsular [33]. When considering the different types of cataract, our findings suggest that the relationship between vitamin D level and cataract may vary depending on the types of cataract. Specifically, we observed that vitamin D level was negatively associated with the risk of nuclear cataract and posterior subcapsular cataract, whereas there was no significant association with cortical cataract. The associations between different types of cataract and vitamin D level remain uncertain with varying results across studies. Aidenloo reported that serum vitamin D level was inversely associated with nuclear and cortical cataract but not posterior subcapsular cataract in women [16], while inverse association between serum vitamin D and posterior subcapsular cataract was observed in Bozkurt and Atalay’s studies [34, 35]. Park’s results showed that there was negative association between serum vitamin D and nuclear cataract [18]. Contrarily, there was no significant association between serum vitamin D and nuclear cataract in Rao’s study [19]. These subtype-specific differences may be attributed to variations in the underlying pathophysiological processes involved in the development of different cataract subtypes.
Vitamin D supplement and cataract have been previously investigated. The Beaver Dam Eye Study indicated that there was a protective relationship between vitamin D intake and nuclear cataract [36]. However, other studies revealed that no significant association between vitamin D supplement and cataract [37, 38]. In a recent randomized controlled trial, participants were randomly assigned to receive regular high-dose vitamin D supplement (60,000 IU once per month) or placebo, and were followed up for a median duration of approximately 5 years. The results showed no significant difference in cataract surgery rates between the experimental group and the placebo group [39]. We found that high-level serum Vitamin D reduced the risk of cataract, indicating a potential role of vitamin D supplementation in ophthalmologic practice. Based on the current available evidence, the relationship between vitamin D supplement and cataract remains inconclusive. Further studies of vitamin D supplementation against cataract are warranted.
There are several limitations to this meta-analysis. Firstly, only four studies were included for analysis and the risk of bias in the four articles were rated as having some concerns based on the quality. Additionally, the heterogeneity is high, we conducted subgroup analysis only in sex and different types of cataract. The main cause of heterogeneity is sex. Meanwhile, we conducted the sensitivity analysis which revealed the Jee’s study influenced the meta-analysis results. The reason for this result could be that the study in question had a different study design and measurement method for vitamin D compared to the other three studies. Furthermore, this study included a much larger sample size than the other three studies and took a dominant role in our analysis. The details showed in Table 1. Additionally, various studies have indicated that Vitamin D plays a role in the pathogenesis and progression of diabetes [40]. Vitamin D deficiency increase the risk of developing type 2 diabetes. [41]Meanwhile, diabetes is the most common risk factor for cataract. [42]Among the four studies, two involve data on diabetes mellitus. In Jee’s study [17], the proportion of patients with diabetes was significantly higher in the cataract group compared to the non-cataract group. In the study by Aidenloo [16], the proportion of patients with diabetes were only significantly higher in the PSC group compared to the control group, and no significant differences in serum calcium levels were observed between the different cataract subgroups and the control group. However, since the vitamin D levels of the diabetic patients were not provided, we are unable to perform any further analysis and understanding of potential correlations.
Conclusion
In this meta-analysis, we reported that there was a possible association between serum vitamin D level and cataract, and indicated that the association between serum vitamin D level and cataract varied across sex and different types of cataract. However, drawing conclusions at this stage seems premature due to the limited number of studies available so far. Therefore, prospective, multicenter, and larger-scale studies are needed in the future.
Supplementary Information
Below is the link to the electronic supplementary material.
Funding
No funding was received for this research.
Declarations
Ethical approval
Regarding this systematic review and meta-analysis, no approval was required from an authorized Medical Ethics Committee since this is a review of priorly published studies with no patient identifying information.
Informed consent
All authors also ascertain that informed consent was confirmed to had been obtained from all individual participants involved in the included studies.
Conflict of Interest
All authors declare no conflict of interests.
Footnotes
Zhenzhen Jue and Ziming Xu Contributed equally as co-first authors.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Liu YC, Wilkins M, Kim T, Malyugin B, Mehta JS (2017) Cataracts. Lancet (London, England) 390(10094):600–612. 10.1016/s0140-6736(17)30544-5 [DOI] [PubMed] [Google Scholar]
- 2.Asbell PA, Dualan I, Mindel J, Brocks D, Ahmad M, Epstein S (2005) Age-related cataract. Lancet (London, England). 365(9459):599–609. 10.1016/s0140-6736(05)17911-2 [DOI] [PubMed] [Google Scholar]
- 3.Flaxman SR, Bourne RRA, Resnikoff S, Ackland P, Braithwaite T, Cicinelli MV, Das A, Jonas JB, Keeffe J, Kempen JH, Leasher J, Limburg H, Naidoo K, Pesudovs K, Silvester A, Stevens GA, Tahhan N, Wong TY, Taylor HR (2017) Global causes of blindness and distance vision impairment 1990–2020: a systematic review and meta-analysis. Lancet Global Health 5(12):e1221–e1234. 10.1016/s2214-109x(17)30393-5 [DOI] [PubMed] [Google Scholar]
- 4.Choquet H, Melles RB, Anand D, Yin J, Cuellar-Partida G, Wang W, Hoffmann TJ, Nair KS, Hysi PG, Lachke SA, Jorgenson E (2021) A large multiethnic GWAS meta-analysis of cataract identifies new risk loci and sex-specific effects. Nature Commun 12(1):3595. 10.1038/s41467-021-23873-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Wang Y, Li F, Zhang G, Kang L, Guan H (2016) Ultraviolet-B induces ERCC6 repression in lens epithelium cells of age-related nuclear cataract through coordinated DNA hypermethylation and histone deacetylation. Clinical Epigenetics 8:62. 10.1186/s13148-016-0229-y [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Zmijewski MA (2019) Vitamin D and Human Health. International journal of molecular sciences. 20(1). 10.3390/ijms20010145 [DOI] [PMC free article] [PubMed]
- 7.Tideman JW, Polling JR, Voortman T, Jaddoe VW, Uitterlinden AG, Hofman A, Vingerling JR, Franco OH, Klaver CC (2016) Low serum vitamin D is associated with axial length and risk of myopia in young children. Eur J Epidemiol 31(5):491–499. 10.1007/s10654-016-0128-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Layana AG, Minnella AM, Garhöfer G, Aslam T, Holz FG, Leys A, Silva R, Delcourt C, Souied E, Seddon JM (2017) Vitamin D and Age-Related Macular Degeneration. Nutrients 9(10). 10.3390/nu9101120 [DOI] [PMC free article] [PubMed]
- 9.Ayyagari R, Chen YI, Zangwill LM, Holman M, Dirkes K, Hai Y, Arzumanyan Z, Slight R, Hammel N, Girkin CA, Liebmann JM, Feldman R, Dubiner H, Taylor KD, Rotter JI, Guo X, Weinreb RN (2019) Association of severity of primary open-angle glaucoma with serum vitamin D levels in patients of African descent. Mol Vis 25:438–445 [PMC free article] [PubMed] [Google Scholar]
- 10.Yuan J, Zhou JB, Zhao W, Zhang RH, Cai YH, Shu LP, Qi L, Yang JK (2019) Could Vitamin D be Associated with Proliferative Diabetic Retinopathy? Evidence from Pooling Studies. Horm Metab Res Hormon- und Stoffwechselforschung Horms et metabolisme 51(11):729–734. 10.1055/a-1010-6449 [DOI] [PubMed] [Google Scholar]
- 11.Shetty R, Sethu S, Deshmukh R, Deshpande K, Ghosh A, Agrawal A, Shroff R (2016) Corneal Dendritic Cell Density Is Associated with Subbasal Nerve Plexus Features, Ocular Surface Disease Index, and Serum Vitamin D in Evaporative Dry Eye Disease. BioMed research international. 4369750. 10.1155/2016/4369750 [DOI] [PMC free article] [PubMed]
- 12.Sadaka A, Nguyen K, Malik A, Brito R, Berry S, Lee AG (2019) Vitamin D and Selenium in a Thyroid Eye Disease Population in Texas. Neuro-Ophthalmology (Aeolus Press) 43(5):291–294. 10.1080/01658107.2019.1566382 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Sobrin L, Stanwyck LK, Pan W, Hubbard RA, Kempen JH, VanderBeek BL (2018) Association of Hypovitaminosis D With Increased Risk of Uveitis in a Large Health Care Claims Database. JAMA Ophthalmology 136(5):548–552. 10.1001/jamaophthalmol.2018.0642 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Tanito M (2021) Reported evidence of vitamin E protection against cataract and glaucoma. Free Radical Biology Med 177:100–119. 10.1016/j.freeradbiomed.2021.10.027 [DOI] [PubMed] [Google Scholar]
- 15.Jiang H, Yin Y, Wu CR, Liu Y, Guo F, Li M, Ma L (2019) Dietary vitamin and carotenoid intake and risk of age-related cataract. Am J Clin Nutr 109(1):43–54. 10.1093/ajcn/nqy270 [DOI] [PubMed] [Google Scholar]
- 16.Aidenloo NS, Motarjemizadeh Q, Nahriq SM (2022) Serum concentrations of 25-hydroxyvitamin D and different subtypes of age-related cataract; a case-control study. Immunopathologia Persa. 8(1). 10.34172/ipp.2022.16
- 17.Jee D, Kim EC (2015) Association between serum 25-hydroxyvitamin D levels and age-related cataracts. J Cataract Refract Surg 41(8):1705–1715. 10.1016/j.jcrs.2014.12.052 [DOI] [PubMed] [Google Scholar]
- 18.Park S, Choi NK (2017) Serum 25-hydroxyvitamin D and Age-Related Cataract. Ophthalmic Epidemiology 24(5):281–286. 10.1080/09286586.2017.1281427 [DOI] [PubMed] [Google Scholar]
- 19.Rao P, Millen AE, Meyers KJ, Liu Z, Voland R, Sondel S, Tinker L, Wallace RB, Blodi BA, Binkley N, Sarto G, Robinson J, LeBlanc E, Mares JA (2015) The Relationship Between Serum 25-Hydroxyvitamin D Levels and Nuclear Cataract in the Carotenoid Age-Related Eye Study (CAREDS), an Ancillary Study of the Women’s Health Initiative. Investigative Ophthalmology Visual Sci 56(8):4221–4230. 10.1167/iovs.15-16835 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ (Clinical research ed). 372:n71. 10.1136/bmj.n71 [DOI] [PMC free article] [PubMed]
- 21.Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. 2000
- 22.JPT H, T L, JJ D. Chapter 6: Choosing effect measures and computing estimates of effect: Cochrane Handbook for Systematic Reviews of Interventions version 6.0 2019 [updated (updated July 2019). Available from: https://training.cochrane.org/handbook/current/chapter-06#section-6-5-2 (table 6.5.2a)
- 23.Abdellah MM, Mostafa EM, Salama EH, Mohamed ER (2019) Association of Serum 25-Hydroxyl Vitamin D Deficiency and Age-Related Cataract: A Case-Control Study. J Ophthalmol. 2019. 10.1155/2019/9312929. [DOI] [PMC free article] [PubMed]
- 24.Öktem Ç, Aslan F (2021) Vitamin D Levels in Young Adult Cataract Patients: A Case-Control Study. Ophthalmic Res 64(1):116–120. 10.1159/000509602 [DOI] [PubMed] [Google Scholar]
- 25.Liu H, Shen X, Yu T, Wang Y, Cai S, Jiang X, Cai X (2022) A putative causality of vitamin D in common diseases: A mendelian randomization study. Frontiers Nutr 9:938356. 10.3389/fnut.2022.938356 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Alvarez JA, Chowdhury R, Jones DP, Martin GS, Brigham KL, Binongo JN, Ziegler TR, Tangpricha V (2014) Vitamin D status is independently associated with plasma glutathione and cysteine thiol/disulphide redox status in adults. Clin Endocrinol 81(3):458–466. 10.1111/cen.12449 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Uberti F, Lattuada D, Morsanuto V, Nava U, Bolis G, Vacca G, Squarzanti DF, Cisari C, Molinari C (2014) Vitamin D protects human endothelial cells from oxidative stress through the autophagic and survival pathways. J Clin Endocrinol Metabol 99(4):1367–1374. 10.1210/jc.2013-2103 [DOI] [PubMed] [Google Scholar]
- 28.Jee D, Kang S, Yuan C, Cho E, Arroyo JG (2016) Serum 25-Hydroxyvitamin D Levels and Dry Eye Syndrome: Differential Effects of Vitamin D on Ocular Diseases. PloS One 11(2):e0149294. 10.1371/journal.pone.0149294 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Sella R, Afshari NA (2019) Nutritional effect on age-related cataract formation and progression. Curr Opin Ophthalmol 30(1):63–69. 10.1097/icu.0000000000000537 [DOI] [PubMed] [Google Scholar]
- 30.Velpandian T, Nirmal J, Gupta P, Vijayakumar AR, Ghose S (2010) Evaluation of calcium dobesilate for its anti-cataract potential in experimental animal models. Methods Find Exp Clin Pharmacol 32(3):171–179. 10.1358/mf.2010.32.3.1423888 [DOI] [PubMed] [Google Scholar]
- 31.Gupta PD, Johar K, Vasavada A (2004) Causative and preventive action of calcium in cataracto-genesis. Acta Pharmacologica Sinica 25(10):1250–1256 [PubMed] [Google Scholar]
- 32.Duncan G, Wormstone IM (1999) Calcium cell signalling and cataract: role of the endoplasmic reticulum. Eye (London England) 13(Pt 3b):480–483. 10.1038/eye.1999.125 [DOI] [PubMed] [Google Scholar]
- 33.Poudel KC, Jimba M, Poudel-Tandukar K, Wakai S (2005) Lack of occupational health research in Nepal. American J Pub Health 95(4):550–551. 10.2105/ajph.2004.059543 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Atalay K, Gezer Savur F, Kirgiz A, Erdogan Kaldirim H, Zengi O (2020) Serum vitamin d levels in different morphologic forms of age related cataract. Acta endocrinologica (Bucharest Romania : 2005) 16(2):178–182. 10.4183/aeb.2020.178. [DOI] [PMC free article] [PubMed]
- 35.Brown CJ, Akaichi F (2015) Vitamin D deficiency and posterior subcapsular cataract. Clin Ophthalmol (Auckland NZ) 9:1093–1098. 10.2147/opth.S84790 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Mares-Perlman JA, Brady WE, Klein BE, Klein R, Haus GJ, Palta M, Ritter LL, Shoff SM (1995) Diet and nuclear lens opacities. Am J Epidemiol 141(4):322–334. 10.1093/aje/141.4.322 [DOI] [PubMed] [Google Scholar]
- 37.Tavani A, Negri E, La Vecchia C (1996) Food and nutrient intake and risk of cataract. Ann Epidemiol 6(1):41–46. 10.1016/1047-2797(95)00099-2 [DOI] [PubMed] [Google Scholar]
- 38.Appleby PN, Allen NE, Key TJ (2011) Diet, vegetarianism, and cataract risk. Am J Clin Nutr 93(5):1128–1135. 10.3945/ajcn.110.004028 [DOI] [PubMed] [Google Scholar]
- 39.Rahman ST, Waterhouse M, Romero BD, Baxter C, English D, Mackey DA, Ebeling PR, Armstrong BK, McLeod DSA, Hartel G, O’Connell RL, van der Pols JC, Venn AJ, Webb PM, Whiteman DC, Neale RE (2023) Vitamin D Supplementation and the Incidence of Cataract Surgery in Older Australian Adults. Ophthalmology 130(3):313–323. 10.1016/j.ophtha.2022.09.015 [DOI] [PubMed] [Google Scholar]
- 40.Grammatiki M, Rapti E, Karras S, Ajjan RA, Kotsa K (2017) Vitamin D and diabetes mellitus: Causal or casual association? Rev Endocr Metab Disord 18(2):227–241. 10.1007/s11154-016-9403-y [DOI] [PubMed] [Google Scholar]
- 41.Pittas AG, Kawahara T, Jorde R, Dawson-Hughes B, Vickery EM, Angellotti E, Nelson J, Trikalinos TA, Balk EM (2023) Vitamin D and Risk for Type 2 Diabetes in People With Prediabetes : A Systematic Review and Meta-analysis of Individual Participant Data From 3 Randomized Clinical Trials. Ann Intern Med 176(3):355–363. 10.7326/m22-3018 [DOI] [PubMed] [Google Scholar]
- 42.Klein R, Klein BEK. Epidemiology of Ocular Functions and Diseases in Persons With Diabetes. In: Cowie CC, Casagrande SS, Menke A, Cissell MA, Eberhardt MS, Meigs JB, et al., editors. Diabetes in America. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases (US); 2018. [PubMed]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.