Summary
Background
Identifying inequalities is important for informing research, and policy efforts to reduce health disparities. This study measured the inequalities in hospitalisations for the costly and prevalent conditions in hospitalised children using association estimates.
Methods
Population-based cohort study using health administrative databases in Ontario, Canada between 2014 and 2019. The hospitalisation rate was determined for the costly and prevalent conditions in children. Hospitalisation inequalities by four equity stratifiers (material resources, rurality, sex, and immigrant status) were quantified using rate difference (RD), rate ratio (RR), and ratio of excess to total hospitalisation rate. Multivariable logistic regression analyses were also conducted.
Findings
In a population of 3·7 million children (median age 7·0 years, Interquartile range: 1·0–12·0), there were 612,597 hospitalisations. Large inequalities comparing children among least versus most resourced quintile was observed in low birth weight (RD: 1,823·3 hospitalisations per 100,000 children, 95% CI: 1,662·7, 1,983·9). Conditions with large inequalities comparing rural versus urban areas included low birth weight (RD: −1,833·2 hospitalisations per 100,000, 95% CI: −2,012·8, −1,653·6); and drug withdrawal syndrome in newborn (RR: 1·9, 95% CI: 1·7, 2·1; adjusted odds ratio (aOR): 1·4, 95% CI: 1·2, 1·5). Conditions with large inequalities comparing males versus females included low birth weight (RD: −888·3 hospitalisations per 100,000, 95% CI: −992·5, −784·02); and anorexia nervosa (RR: 0·08, 95% CI: 0·07, 0·10; aOR: 0·1, 95% CI: 0.1, 0.1). Conditions with large inequalities comparing non-refugee immigrants versus non-immigrants included major depressive disorder (RR: 2·8, 95% CI: 2·7, 2·9), and comparing refugees versus non-immigrants included drug withdrawal syndrome in newborn (RR: 0·09, 95% CI: 0·05, 0·15). Results from multivariable analyses were similar.
Interpretation
Newborn and mental health conditions had the largest inequalities in hospitalisations by the equity stratifiers. Findings from this study can be used to prioritise future health equity research to reduce health inequalities.
Funding
PSI Foundation.
Keywords: Paediatric, Hospitalisation, Health inequalities, Socioeconomic status, Rurality, Sex, Immigrant status
Research in context.
Evidence before this study
A literature search was conducted on MEDLINE-Ovid and EMBASE for articles published from database inception to January 31, 2024, to identify prioritisation studies in hospitalised children. This search was conducted by combining search terms and subject headings that were specific to the research database using AND/OR in the search statement. Search terms used included: “hospitaliz∗”, “hospital admission∗”, “hospital∗”, “pediatric∗”, “child∗”, “youth∗”, “adolescent∗”, “priorit∗”, “order”, and “rank∗”. There were 202,700 articles identified from the literature search, and after duplicates were removed and articles were screened, there were six prioritisation studies found that focused on hospitalised children. Most studies examined the burden of hospitalisations and identified the common and costly conditions in hospitalised children. However, none of these studies examined the health inequalities in hospital use for the common and costly conditions in children, or examined the hospital use by disadvantaged population groups, which can be used to identify priority areas for future research in hospitalised children.
Added value of this study
This population-based study leveraged large health administrative data focussing on children residing in Ontario, the most populous province in Canada. In a population of 3·7 million children and adolescents, there were 612,597 hospitalisations observed between 2014 and 2019. To our knowledge, this study is the first to measure inequalities in hospitalisations amongst the most costly and prevalent conditions in hospitalised children using association estimates. We found several newborn (e.g., low birth weight, drug withdrawal syndrome in newborn) and mental health conditions (e.g., adjustment disorders, major depressive disorder) with large inequalities in hospitalisations by material resources, rurality, child sex, and immigrant status. These inequalities were present using both relative (i.e., rate ratio, ratio of excess to total hospitalisation rate) and absolute measures (i.e., rate difference).
Implications of all the available evidence
Our study builds on previous prioritisation studies by using a health equity lens to identify where large disparities in hospitalisation exists, to direct future research efforts to these areas. These findings suggests that future health equity research and policy efforts should be directed towards newborn and mental health conditions to reduce the health inequalities in an effort towards attaining health equity in hospitalised children.
Introduction
Health inequalities, defined as measurable differences in health outcomes across population subgroups, e.g., by socioeconomic status, race, and geography, exist worldwide,1 and in many regions these inequalities are increasing over time.2,3 The mechanisms behind how sociodemographic and geographic factors interact with health are multi-factorial and complex, and include access to care, housing and neighbourhood ‘quality’, and affordability of health care services.3 Measuring inequalities requires categorising the population into subgroups based on specific characteristics, termed ‘equity stratifiers’.4 The PROGRESS-Plus framework—a guidance framework for equity-focused research5—summarises the most common population groups affected by health and health care inequalities including place of residence; gender/sex; and socioeconomic status.6 The ‘Plus’ portion includes other factors not listed in ‘PROGRESS’, but where disadvantage may exist, such as immigrant status.6,7
Previous studies have shown inequalities in hospital use by children based on socioeconomic status, geography, and sex.8,9 For instance, higher hospitalisation rates for asthma are associated with lower socioeconomic status and geographic location among Canadian children.8 In the United States, increased hospital admissions for diabetic ketoacidosis has been associated with female sex.9 Previous studies that examined associations between social, demographic, and geographic characteristics and hospitalisations focused on specific conditions. No study used a health-systems level approach to identify where inequalities in hospital use exists. Using a health equity lens to identify where disparities exist is necessary to determine strategies to alleviate gaps observed between the most and least disadvantaged groups, and to ultimately improve health equity.4,10
Therefore, the objective of this study was to measure inequalities in hospitalisation rates using association estimates for the most costly and prevalent conditions among children in Ontario, Canada's most populous province based on the following equity stratifiers: material resources (proxy measure of socioeconomic status), rurality, sex, and immigrant status.
Methods
Design, population, and data source
A cohort study of all children younger than 18 years of age living in Ontario, Canada between April 1, 2014 and March 31, 2019, and eligible for universal provincial health insurance (see Supplementary Figure S1 for exclusions) was conducted. Data were obtained from linked health administrative databases housed at ICES, and datasets were linked using unique encoded identifiers (see Supplementary Table S1 for details). This study was approved by the Research Ethics Board at the Hospital for Sick Children and is reported following the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guideline.11 Informed patient consent was waived as the study used deidentified administrative data only.
Outcome
The outcome was the condition-specific hospitalisation rate per 100,000 children for pooled years 2014/15–2018/2019 (referred to as 2014–2019). Hospital encounters were classified into clinical conditions using the Pediatric Clinical Classification System for use in Canada (PECCS-CA),12 based on the International Statistical Classification of Diseases and Related Health Problems, Tenth Revision, Canada (ICD-10-CA) most responsible diagnosis code for the encounter. Similarly indicated in a previous Ontario study,13 excluded were hospital encounters with missing or invalid birth, death, or discharge dates, with missing material resources or rurality data, with the most responsible diagnosis for normal newborn births, non-Ontario residents, and a discharge date after March 31, 2019. The hospitalisation rate was determined for 20 conditions which included the top 15 most costly and top 15 most prevalent conditions identified in the previous Ontario study.13
Equity stratifiers
Following the PROGRESS-Plus framework,6 four equity stratifiers - characteristics that group the population into subgroups to measure health inequalities - were selected: material resources, rurality, sex, and immigrant status. Data on race/ethnicity and gender were not available.
Material resources, a dimension of the Ontario Marginalisation Index, is a comprehensive area-based measure of socioeconomic status and poverty at the neighbourhood level. The indicators used in the composite measure include income, employment, housing quality, educational attainment, and family structure characteristics.14 Material resources quintiles were created at the dissemination area level and assigned to individual records, with quintile 1 representing the most resourced (i.e., least deprived) and quintile 5 representing the least resourced (i.e., most deprived). Rurality - urban and rural place of residence - was measured using the Rurality Index for Ontario (RIO).15 Raw scores for the RIO range from 0 to 100, with urban defined as a score of <40 and rural defined as a score ≥40.15 The RIO measure was calculated based on population size and density, and travel time to the nearest basic and advanced referral centre (Supplementary Methods S1).15 Sex was categorised as male or female. Last, immigrant status was categorised as refugee immigrant (herein referred to as refugees), non-refugee immigrant, and non-immigrant.16 A child was classified as immigrant if the child or their mother had a record in the Immigration, Refugees and Citizenship Canada Permanent Resident Database. Their visa class in the record was used to determine if they were refugee or non-refugee. A child and child's mother without an immigration record was identified as non-immigrant.17
Statistical analysis
For each condition, the hospitalisation rate per 100,000 children was determined for children within a defined age group at risk of being hospitalised for that condition. The ‘at risk’ age group was determined based on the frequency distribution of hospitalisations for the condition to determine the age group with most encounters, and informed by the literature, e.g., for preterm newborn, age group was <1 years old (see Supplementary Table S2). The numerator for the condition-specific hospitalisation rate was the number of hospital encounters for the condition within the selected age group, pooled from 2014 to 2019, while the denominator was the annual Ontario population estimate of children within the selected age group,8 pooled from 2014 to 2019. Crude rates were computed to directly reflect the total burden of the outcome in the healthcare system. Next, hospital encounters for each condition were categorised into population subgroups by equity stratifiers8: material resources (quintiles 1–5), rurality (rural, urban), sex (male, female), and immigrant status (refugee, non-refugee immigrant, non-immigrant). Stratified condition-specific hospitalisation rates per 100,000 were calculated for the pooled years and for all population subgroups using population estimates as the denominator.8
Absolute and relative inequality measures were used to quantify the magnitude of inequalities in hospitalisation for each condition, to provide a more accurate depiction of inequalities, and to avoid skewed interpretation of the results.18 For each condition, the following inequality summary measures were calculated8,18: 1) rate difference (absolute measure); 2) rate ratio (relative measure); and 3) ratio of excess to total hospitalisation rate (relative measure).
The rate difference (RD) was calculated by subtracting the rate between the group with the highest expected condition-specific hospitalisation rate and the group with the lowest expected rate within the equity stratifier (i.e., reference group).8 Larger absolute values for RD indicate higher hospitalisation inequalities.19 The rate ratio (RR) was calculated by dividing the rate of the group with the highest expected hospitalisation rate by the rate of the group with the lowest expected rate within the equity stratifier (i.e., reference group).8,19 A RR further from one (in either direction) indicates higher hospitalisation inequalities.19 To calculate RD and RR, the groups hypothesised to have the highest expected rates were those in the least material resourced quintile, in rural areas, and males; the groups hypothesised to have the lowest expected rates were those in the most resourced quintile, in urban areas, and females (see Supplementary Methods S2). Corresponding 95% confidence intervals (CIs) were computed.
The ratio of excess to total hospitalisation rate was calculated by first summing the differences in the hospitalisation rates between each group in the equity stratifier and the group with the lowest expected condition-specific hospitalisation rate (reference group), and then dividing this figure by the total number of subgroups within the equity stratifier to determine total excess hospitalisation rate. Next, the ratio of the total excess hospitalisation rate to the overall hospitalisation rate in all groups within that equity stratifier was computed (Supplementary Methods S2).18 Higher ratios mean higher hospitalisation inequalities.19 This measure speaks to inequalities for equity stratifiers with more than two subgroups,19 and was computed for material resources only. For conditions where the subgroup that was expected to have the lowest hospitalisation rate had instead the higher rate (i.e., most resourced quintile), the ratio of excess to total hospitalisation was recalculated by flipping the reference group (i.e., would now be the least resourced quintile) in the formula to help with interpretation and understand where the proportion of excess hospitalisations from the total hospitalisation rate is coming from within the material resources subgroups.
Based on published work,7,16 for immigrant status, two RDs and RRs were calculated. One analysis compared the condition-specific hospitalisation rates between non-refugee immigrants and non-immigrants. A second analysis compared the hospitalisation rates between refugees and non-immigrants (Supplementary Methods S2).
For each condition, multivariable logistic regression analyses were conducted to examine if differences remained after adjusting for potential confounding variables. The outcome was recoded as a binary variable (hospitalised for the condition; yes/no). Covariates that might influence hospitalisation rate were identified a priori and included in the model8,9,20: age, sex, material resources, rurality, immigrant status, and complex chronic conditions (CCCs) [identified using the diagnostic and procedural codes from CIHI,21 and categorised as having CCCs present versus not]. CCCs were measured using hospital data from the past 2 years from baseline or from birth if the patient was younger than 2 years of age. The adjusted odds ratio (aOR) estimates for the association between each equity stratifier and hospitalisation for each condition were compared to the RR estimates. Since the prevalence of hospitalisation in the general child population is low (<10%), the OR yielded from logistic regression is a good approximation of RR, one of the relative inequality measures reported in our initial analysis.22
We also tested for interactions between material resources and immigrant status by including an interaction term between material resources and immigrant status to our fully adjusted logistic regression models, as prior literature reported both factors to have a combined effect on health services use.23,24 The interaction was considered statistically significant if the 95% CIs of the aORs comparing the least to most resourced quintile in the three immigrant status groups did not overlap; in this case, the results would support that the effect of material resources on hospitalisation for the condition differed between at least two of the immigrant status groups. Statistical analysis was conducted using the SAS Enterprise Guide software, version 8.3 (SAS Institute Inc.).
Role of the funding source
This study was funded by the Physicians' Services Incorporated (PSI) Foundation Grant Number: 21-01. The analyses, conclusions, opinions and statements expressed herein are solely those of the authors and do not reflect those of the funding source.
Results
Among 3·7 million children and adolescents in Ontario (51·3% male; median age 7·0 years, Interquartile range: 1·0–12·0; and 93·8% urban) (Table 1, Supplementary Figure S1), there were 612,597 hospital encounters between April 1, 2014 and March 31, 2019. The results for each equity stratifier are outlined below and summarised in Table 2, with additional details by each stratifier in Supplementary Tables S3–S8.
Table 1.
Characteristics of children in Ontario, Canada, 2014–2019.
| Characteristics | Children (n = 3,683,646 children) |
|---|---|
| Age range, n (%) | |
| <30 days | 666,913 (18·1) |
| ≥30 days–<1 year | 147,181 (4·0) |
| 1–4 years | 655,283 (17·8) |
| 5–12 years | 1,326,102 (36·0) |
| 13–17 years | 888,167 (24·1) |
| Age in years, median (IQR) | 7·0 (1·0–12·0) |
| Sex, n (%) | |
| Female | 1,792,763 (48·7) |
| Male | 1,890,883 (51·3) |
| Rurality of residence, n (%) | |
| Rural | 230,046 (6·2) |
| Urban | 3,453,600 (93·8) |
| Immigrant status, n (%) | |
| Refugee immigrant | 148,591 (4·0) |
| Non-refugee immigrant | 1,982,621 (53·8) |
| Non-immigrant | 1,552,434 (42·1) |
| No. of complex chronic conditions present,an (%) | |
| 0 | 3,611,220 (98·0) |
| 1 | 54,092 (1·5) |
| 2 | 10,981 (0·3) |
| ≥3 | 7,353 (0·2) |
| Material resources quintile, n (%) | |
| Q1 (most resourced) | 813,577 (22·1) |
| Q2 | 766,458 (20·8) |
| Q3 | 689,121 (18·7) |
| Q4 | 654,411 (17·8) |
| Q5 (least resourced) | 760,079 (20·6) |
Abbreviation: IQR, interquartile range.
Determined using child's hospital data for the previous 2 years, or until birth if child was younger than 2 years of age.
Table 2.
Comparison of initial results using rate ratio with univariable and multivariable logistic regression analysis for the association between factors and the hospitalisation for the 15 most costly and 15 most prevalent conditions (20 in total).
| Condition | Factors | Initial results Rate ratio (95% CI) |
Unadjusted model Odds ratio (95% CI) |
Adjusted model Odds ratio (95% CI) |
|---|---|---|---|---|
| Drug withdrawal syndrome in newborn | Male Sex (ref: Female) | 1·1 (1·0, 1·2) | 1·1 (1·0, 1·2) | 1·1 (1·0, 1·2) |
| Rural (ref: Urban) | 1·9 (1·7, 2·1) | 1·9 (1·7, 2·2) | 1·4 (1·2, 1·5) | |
| Material resources quintile Q5 (ref: Q1) | 5·9 (5·1, 6·8) | 5·6 (4·9, 6·5) | Material resources quintile immigrant status interaction |
|
| Non-refugee immigrant (ref: Non-immigrant) | 0·1 (0·1, 0·2) | 0·1 (0·1, 0·1) | ||
| Refugees (ref: Non-immigrant) | 0·1 (0·1, 0·1) | 0·1 (0·1, 0·1) | ||
| Low birth weight | Male sex (ref: Female) | 0·9 (0·8, 0·9) | 0·8 (0·8, 0·9) | 0·8 (0·8, 0·9) |
| Rural (ref: Urban) | 0·7 (0·7, 0·7) | 0·7 (0·7, 0·7) | 0·7 (0·7, 0·7) | |
| Material resources quintile Q5 (ref: Q1) | 1·3 (1·3, 1·4) | 1·4 (1·3, 1·4) | 1·4 (1·3, 1·4) | |
| Non-refugee immigrant (ref: Non-immigrant) | 1·1 (1·0, 1·1) | 1·0 (1·0, 1·1) | 1·0 (1·0, 1·0) | |
| Refugees (ref: Non-immigrant) | 1·1 (1·1, 1·2) | 1·1 (1·0, 1·1) | 1·0 (1·0, 1·0) | |
| Neonatal hyperbilirubinemia | Male sex (ref: Female) | 1·1 (1·1, 1·2) | 1·1 (1·1, 1·2) | 1·1 (1·1, 1·2) |
| Rural (ref: Urban) | 1·01 (0·97, 1·06) | 1·0 (1·0, 1·1) | 1·0 (1·0, 1·1) | |
| Material resources quintile Q5 (ref: Q1) | 0·95 (0·92, 0·99) | 0·9 (0·9, 1·0) | 0·9 (0·9, 1·0) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·98 (0·96, 1·01) | 0·9 (0·9, 1·0) | 1·0 (0·9, 1·0) | |
| Refugees (ref: Non-immigrant) | 0·97 (0·92, 1·03) | 0·9 (0·9, 1·0) | 0·9 (0·9, 1·0) | |
| Neonatal hypoglycemia | Male sex (ref: Female) | 1·5 (1·4, 1·6) | 1·5 (1·4, 1·6) | 1·5 (1·4, 1·6) |
| Rural (ref: Urban) | 0·99 (0·90, 1·08) | 1·0 (0·9, 1·1) | 0·9 (0·8, 1·0) | |
| Material resources quintile Q5 (ref: Q1) | 1·1 (1·1, 1·2) | 1·1 (1·1, 1·2) | 1·2 (1·1, 1·3) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·8 (0·8, 0·9) | 0·8 (0·8, 0·9) | 0·8 (0·8, 0·8) | |
| Refugees (ref: Non-immigrant) | 0·9 (0·8, 1·0) | 0·9 (0·8, 1·0) | 0·9 (0·8, 1·0) | |
| Other perinatal conditionsa | Male sex (ref: Female) | 1·2 (1·2, 1·2) | 1·2 (1·2, 1·2) | 1·2 (1·2, 1·2) |
| Rural (ref: Urban) | 1·1 (1·0, 1·1) | 1·1 (1·1, 1·2) | 1·0 (1·0, 1·1) | |
| Material resources quintile Q5 (ref: Q1) | 1·2 (1·2, 1·3) | 1·2 (1·2, 1·2) | 1·2 (1·2, 1·3) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·7 (0·7, 0·7) | 0·7 (0·6, 0·7) | 0·7 (0·6, 0·7) | |
| Refugees (ref: Non-immigrant) | 1·01 (0·97, 1·06) | 1·0 (0·9, 1·0) | 0·9 (0·9, 1·0) | |
| Preterm newborn | Male sex (ref: Female) | 1·3 (1·3, 1·3) | 1·3 (1·3, 1·3) | 1·3 (1·3, 1·3) |
| Rural (ref: Urban) | 1·1 (1·0, 1·2) | 1·1 (1·1, 1·2) | 1·0 (1·0, 1·1) | |
| Material resources quintile Q5 (ref: Q1) | 1·1 (1·1, 1·2) | 1·1 (1·1, 1·2) | 1·1 (1·1, 1·2) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·7 (0·7, 0·7) | 0·7 (0·7, 0·7) | 0·7 (0·7, 0·7) | |
| Refugees (ref: Non-immigrant) | 0·9 (0·8, 1·0) | 0·9 (0·8, 0·9) | 0·9 (0·8, 0·9) | |
| Surfactant deficiency disorder | Male sex (ref: Female) | 1·6 (1·5, 1·7) | 1·6 (1·4, 1·7) | 1·6 (1·4, 1·7) |
| Rural (ref: Urban) | 1·1 (0·9, 1·3) | 1·1 (0·9, 1·3) | 1·0 (0·8, 1·1) | |
| Material resources quintile Q5 (ref: Q1) | 1·2 (1·1, 1·4) | 1·2 (1·0, 1·3) | 1·2 (1·1, 1·4) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·6 (0·6, 0·7) | 0·6 (0·6, 0·7) | 0·6 (0·6, 0·7) | |
| Refugees (ref: Non-immigrant) | 0·7 (0·6, 0·9) | 0·7 (0·6, 0·9) | 0·7 (0·6, 0·8) | |
| Transient tachypnoea of newborn | Male sex (ref: Female) | 1·5 (1·5, 1·6) | 1·5 (1·5, 1·6) | 1·5 (1·5, 1·6) |
| Rural (ref: Urban) | 1·1 (1·0, 1·2) | 1·1 (1·0, 1·2) | 1·0 (0·9, 1·1) | |
| Material resources quintile Q5 (ref: Q1) | 1·1 (1·0, 1·2) | 1·1 (1·0, 1·1) | 1·1 (1·0, 1·1) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·7 (0·7, 0·8) | 0·7 (0·7, 0·7) | 0·7 (0·7, 0·7) | |
| Refugees (ref: Non-immigrant) | 0·9 (0·8, 1·0) | 0·9 (0·8, 0·9) | 0·9 (0·8, 0·9) | |
| Bronchiolitis | Male sex (ref: Female) | 1·4 (1·4, 1·5) | 1·4 (1·4, 1·5) | 1·4 (1·4, 1·5) |
| Rural (ref: Urban) | 1·1 (1·0, 1·1) | 1·1 (1·0, 1·2) | 1·0 (0·9, 1·0) | |
| Material resources quintile Q5 (ref: Q1) | 1·5 (1·4, 1·5) | 1·4 (1·3, 1·5) | 1·4 (1·4, 1·5) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·7 (0·7, 0·7) | 0·6 (0·6, 0·7) | 0·7 (0·7, 0·7) | |
| Refugees (ref: Non-immigrant) | 0·9 (0·8, 1·0) | 0·9 (0·8, 0·9) | 0·8 (0·8, 0·9) | |
| Chemotherapy | Male sex (ref: Female) | 1·3 (1·2, 1·4) | 1·1 (1·1, 1·2) | 1·1 (1·1, 1·2) |
| Rural (ref: Urban) | 0·8 (0·8, 0·9) | 0·7 (0·6, 0·8) | 0·7 (0·6, 0·8) | |
| Material resources quintile Q5 (ref: Q1) | 1·1 (1·0, 1·2) | 1·2 (1·1, 1·3) | 1·1 (1·0, 1·3) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·7 (0·7, 0·7) | 0·5 (0·5, 0·6) | 1·0 (0·9, 1·1) | |
| Refugees (ref: Non-immigrant) | 0·9 (0·8, 1·0) | 0·9 (0·8, 1·1) | 1·1 (0·9, 1·3) | |
| Infectious, gastroenteritis | Male sex (ref: Female) | 1·1 (1·1, 1·2) | 1·1 (1·1, 1·1) | 1·1 (1·0, 1·1) |
| Rural (ref: Urban) | 0·8 (0·7, 0·8) | 0·8 (0·7, 0·9) | 0·7 (0·7, 0·8) | |
| Material resources quintile Q5 (ref: Q1) | 1·7 (1·6, 1·8) | 1·6 (1·6, 1·8) | 1·6 (1·5, 1·7) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·6 (0·6, 0·6) | 0·5 (0·5, 0·5) | 0·9 (0·9, 0·9) | |
| Refugees (ref: Non-immigrant) | 1·1 (1·0, 1·2) | 0·9 (0·8, 1·0) | 1·0 (0·9, 1·1) | |
| Pneumonia | Male sex (ref: Female) | 1·1 (1·1, 1·1) | 1·1 (1·1, 1·1) | 1·1 (1·0, 1·1) |
| Rural (ref: Urban) | 1·1 (1·0, 1·1) | 1·1 (1·0, 1·2) | 1·0 (1·0, 1·1) | |
| Material resources quintile Q5 (ref: Q1) | 1·5 (1·4, 1·5) | 1·4 (1·3, 1·5) | 1·4 (1·3, 1·4) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·5 (0·5, 0·5) | 0·4 (0·4, 0·5) | 0·9 (0·9, 0·9) | |
| Refugees (ref: Non-immigrant) | 0·9 (0·8, 1·0) | 0·8 (0·7, 0·8) | 1·0 (0·9, 1·0) | |
| Screening for suspected conditionsa | Male sex (ref: Female) | 1·00 (0·97, 1·04) | 1·0 (1·0, 1·0) | 1·0 (1·0, 1·0) |
| Rural (ref: Urban) | 0·3 (0·3, 0·4) | 0·3 (0·3, 0·4) | 0·4 (0·3, 0·4) | |
| Material resources quintile Q5 (ref: Q1) | 1·2 (1·1, 1·2) | 1·1 (1·0, 1·1) | 1·0 (0·9, 1·0) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·7 (0·7, 0·7) | 0·6 (0·6, 0·6) | 1·3 (1·3, 1·4) | |
| Refugees (ref: Non-immigrant) | 1·2 (1·1, 1·3) | 1·0 (0·9, 1·1) | 1·4 (1·2, 1·5) | |
| Acute appendicitis without peritonitisb | Male sex (ref: Female) | 1·3 (1·2, 1·3) | 1·3 (1·2, 1·3) | 1·3 (1·2, 1·3) |
| Rural (ref: Urban) | 0·96 (0·88, 1·04) | 1·0 (0·9, 1·1) | 0·9 (0·9, 1·0) | |
| Material resources quintile Q5 (ref: Q1) | 0·9 (0·8, 0·9) | 0·9 (0·8, 0·9) | 0·9 (0·9, 1·0) | |
| Non-refugee immigrant (ref: Non-immigrant) | 1·3 (1·2, 1·3) | 1·1 (1·1, 1·2) | 0·6 (0·6, 0·7) | |
| Refugees (ref: Non-immigrant) | 1·3 (1·2, 1·4) | 1·1 (1·0, 1·2) | 0·8 (0·7, 0·9) | |
| Asthma | Male sex (ref: Female) | 1·5 (1·5, 1·6) | 1·6 (1·5, 1·7) | 1·6 (1·5, 1·6) |
| Rural (ref: Urban) | 0·8 (0·8, 0·9) | 0·9 (0·8, 1·0) | 0·8 (0·7, 0·9) | |
| Material resources quintile Q5 (ref: Q1) | 1·8 (1·7, 1·9) | 1·6 (1·5, 1·7) | 1·7 (1·6, 1·8) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·5 (0·5, 0·5) | 0·4 (0·4, 0·4) | 0·8 (0·7, 0·8) | |
| Refugees (ref: Non-immigrant) | 0·8 (0·8, 0·9) | 0·6 (0·6, 0·7) | 0·7 (0·7, 0·8) | |
| Hypertrophy of tonsils and adenoids | Male sex (ref: Female) | 1·2 (1·2, 1·3) | 1·2 (1·2, 1·3) | 1·2 (1·2, 1·3) |
| Rural (ref: Urban) | 1·4 (1·3, 1·6) | 1·5 (1·4, 1·6) | 1·3 (1·2, 1·4) | |
| Material resources quintile Q5 (ref: Q1) | 1·4 (1·3, 1·5) | 1·4 (1·3, 1·5) | 1·4 (1·3, 1·5) | |
| Non-refugee immigrant (ref: Non-immigrant) | 0·4 (0·4, 0·5) | 0·4 (0·4, 0·4) | 0·7 (0·6, 0·7) | |
| Refugees (ref: Non-immigrant) | 0·8 (0·7, 0·9) | 0·7 (0·6, 0·8) | 0·8 (0·8, 0·9) | |
| Adjustment disordersc | Male sex (ref: Female) | 0·4 (0·4, 0·4) | 0·4 (0·4, 0·4) | 0·4 (0·4, 0·4) |
| Rural (ref: Urban) | 1·4 (1·3, 1·5) | 1·4 (1·3, 1·6) | 1·2 (1·1, 1·4) | |
| Material resources quintile Q5 (ref: Q1) | 2·1 (2·0, 2·3) | 2·1 (1·9, 2·3) | Material resources quintile immigrant status interaction |
|
| Non-refugee immigrant (ref: Non-immigrant) | 2·0 (1·9, 2·1) | 1·8 (1·7, 1·9) | ||
| Refugees (ref: Non-immigrant) | 0·7 (0·6, 0·9) | 0·7 (0·6, 0·8) | ||
| Anorexia nervosa | Male sex (ref: Female) | 0·1 (0·1, 0·1) | 0·1 (0·1, 0·1) | 0·1 (0·1, 0·1) |
| Rural (ref: Urban) | 0·8 (0·6, 1·0) | 0·9 (0·7, 1·2) | 0·9 (0·7, 1·2) | |
| Material resources quintile Q5 (ref: Q1) | 0·5 (0·4, 0·6) | 0·4 (0·4, 0·5) | 0·5 (0·4, 0·6) | |
| Non-refugee immigrant (ref: Non-immigrant) | 1·8 (1·6, 2·0) | 1·5 (1·3, 1·7) | 0·6 (0·5, 0·7) | |
| Refugees (ref: Non-immigrant) | 0·7 (0·5, 1·0) | 0·5 (0·3, 0·8) | 0·3 (0·2, 0·6) | |
| Anxiety disorders | Male sex (ref: Female) | 0·3 (0·3, 0·3) | 0·4 (0·3, 0·4) | 0·4 (0·3, 0·4) |
| Rural (ref: Urban) | 1·4 (1·3, 1·6) | 1·5 (1·4, 1·7) | 1·4 (1·2, 1·5) | |
| Material resources quintile Q5 (ref: Q1) | 1·4 (1·3, 1·6) | 1·4 (1·2, 1·5) | Material resources quintile immigrant status interaction |
|
| Non-refugee immigrant (ref: Non-immigrant) | 1·9 (1·8, 2·0) | 1·7 (1·6, 1·8) | ||
| Refugees (ref: Non-immigrant) | 0·5 (0·4, 0·7) | 0·4 (0·3, 0·6) | ||
| Major depressive disorder | Male sex (ref: Female) | 0·3 (0·3, 0·3) | 0·3 (0·3, 0·3) | 0·3 (0·3, 0·3) |
| Rural (ref: Urban) | 1·3 (1·2, 1·3) | 1·4 (1·3, 1·5) | 1·3 (1·2, 1·4) | |
| Material resources quintile Q5 (ref: Q1) | 1·4 (1·3, 1·5) | 1·3 (1·2, 1·4) | Material resources quintile immigrant status interaction |
|
| Non-refugee immigrant (ref: Non-immigrant) | 2·8 (2·7, 2·9) | 2·5 (2·3, 2·6) | ||
| Refugees (ref: Non-immigrant) | 0·7 (0·6, 0·8) | 0·5 (0·4, 0·6) |
Abbreviation: 95% CI, 95% confidence interval.
Note: If the interaction between material resources and immigrant status was statistically significant, it was noted in the table as the following in the adjusted model: Material resources quintile ∗ immigrant status interaction.
Details on the top most responsible ICD-10-CA diagnosis codes that led to hospital encounters for the non-specific paediatric condition in children are listed in Supplementary Table S9.
For rurality, only 99·7% of the data were used for univariate logistic regression since there was a warning that ridging had failed to improve the log likelihood if 100% of the data were used for the univariate analysis.
Adjustment disorders are emotional or behavioural symptoms in response to a critical life event or an external life stressor.25
Inequalities in hospitalisations by material resources
Several conditions within the <1 year old age group had high hospitalisation rates in all material resources quintiles, with low birth weight having the highest rate (6,094·8 per 100,000 children, 95% CI: 6,038·2–6,151·5 per 100,000) (Supplementary Table S3). The most responsible diagnosis codes that led to hospital encounters for the non-specific paediatric conditions included in this study are presented in Supplementary Table S9. For majority of the conditions (17 of 20), the hospitalisation rates were greater in children in the least versus most resourced quintile. Newborn conditions such as low birth weight, and drug withdrawal syndrome in newborn had the highest absolute inequalities in hospitalisation when comparing children in the least versus most resourced quintile (Supplementary Table S4). The highest relative inequalities in hospitalisation by material resources were observed in drug withdrawal syndrome in newborn (RR: 5·9, 95% CI: 5·1–6·8; Ratio of excess to total: 0·63), and adjustment disorders (see Supplementary Table S2 footnote for definition) (RR: 2·1, 95% CI: 2·0–2·3; Ratio of excess to total: 0·37).
Neonatal hyperbilirubinemia, acute appendicitis without peritonitis, and anorexia nervosa had higher hospitalisation rates in the most versus least resourced group, therefore the ratio of excess to total hospitalisation summary measure was recalculated (Supplementary Table S4). Large relative inequalities in hospitalisation were observed for anorexia nervosa (RR: 0·5, 95% CI: 0·4–0·6; Ratio of excess to total: 0·28).
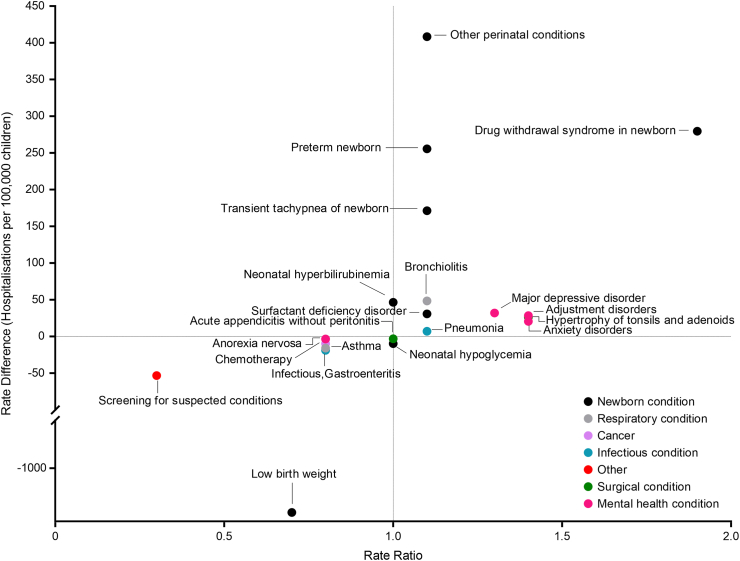
Fig. 1 illustrates the rate difference versus rate ratio for the 20 conditions. Drug withdrawal syndrome in newborn had a high rate difference and high rate ratio. Results from the multivariable logistic regression analyses were similar (Table 2, Supplementary Tables S10–S29).
Fig. 1.
Inequalities in the hospitalisation rate by material resources for the 15 most costly and 15 most prevalent conditions. The figure presents the inequalities in hospitalisation rate by material resources using rate difference and rate ratio. A rate difference greater than 0 indicates that the hospitalisation rate for the condition was greater in the least resourced quintile than the most resourced quintile, and a rate difference lesser than 0 indicates that the hospitalisation rate was lower in the least resourced quintile than the most resourced quintile. A rate ratio greater than 1 indicates that the hospitalisation rate for the condition was greater in the least resourced quintile than the most resourced quintile, while a rate ratio lesser than 1 indicates that the rate was lower in least resourced quintile than the most resourced quintile. Conditions with the largest inequalities (i.e., have high rate difference and rate ratio) will be those in the top-right and bottom-left areas of the panels.
Inequalities in hospitalisations by rurality
Hospitalisation rate for 12 of the 20 conditions was higher in children residing in rural compared to urban areas (Supplementary Table S5). Newborn conditions such as drug withdrawal syndrome in newborn, and preterm newborn had the highest absolute inequalities in hospitalisation when comparing rural to urban areas. Drug withdrawal syndrome in newborn (RR: 1·9, 95% CI: 1·7–2·1) had also the highest relative inequalities in hospitalisation. Low birth weight (RD: −1,833·2 hospitalisations per 100,000, 95% CI: −2,012·8 to −1,653·6 per 100,000), and screening for suspected conditions (RR: 0·3, 95% CI: 0·3–0·4) had high absolute and relative hospitalisation disparities respectively, but with a higher rate in urban versus rural areas. Fig. 2 outlines the rate difference versus rate ratio for the conditions. Again, newborn conditions (e.g., drug withdrawal syndrome in newborn, low birth weight) had a large rate difference and large rate ratio when comparing rural to urban areas.
Fig. 2.
Inequalities in the hospitalisation rate by rurality for the 15 most costly and 15 most prevalent conditions. The figure presents the inequalities in hospitalisation rate by rurality using rate difference and rate ratio. A rate difference greater than 0 indicates that the hospitalisation rate for the condition was greater in children residing in rural compared to urban areas, and a rate difference lesser than 0 indicates that the hospitalisation rate was lower in rural compared to urban areas. A rate ratio greater than 1 indicates that the hospitalisation rate for the condition was greater in children residing in rural versus urban areas, while a rate ratio lesser than 1 indicates that the rate was lower in rural compared to urban areas. Conditions with the largest inequalities (i.e., have high rate difference and rate ratio) will be those in the top-right and bottom-left areas of the panels.
In multivariable analyses, results were similar compared to the initial RR, but 7 of 12 conditions that had slightly higher hospitalisation rates for children residing in rural compared to urban areas, no longer had a statistically significant difference in the odds of hospitalisation by rurality (Table 2, Supplementary Tables S10–S29). From the 12 conditions, the five that remained with a higher odds of hospitalisation in rural compared to urban areas even after adjustment were: drug withdrawal syndrome in newborn, hypertrophy of tonsils and adenoids, adjustment disorders, anxiety disorders, and major depressive disorder.
Inequalities in hospitalisations by sex
The hospitalisation rates were higher in males for 14 conditions, while higher in females for 5 conditions, including all four mental health conditions (Supplementary Table S6). The largest inequalities in hospitalisation by sex (males greater than females) were observed in newborn conditions such as transient tachypnoea of newborn, preterm newborn, and other perinatal conditions. Surfactant deficiency disorder (RR: 1·6, 95% CI: 1·5–1·7) had the highest relative inequalities in hospitalisation.
Low birth weight (RD: −888·3 hospitalisations per 100,000, 95% CI: −992·5 to −784·02 hospitalisations per 100,000), and mental health conditions including anorexia nervosa (RR: 0·08, 95% CI: 0·07–0·10), anxiety disorders (RR: 0·33, 95% CI: 0·31–0·35), major depressive disorder (RR: 0·28, 95% CI: 0·26–0·29), and adjustment disorders (RR: 0·37, 95% CI: 0·35–0·39) also had high hospitalisation disparities by sex, but with the rates higher in females versus males (Supplementary Table S6). Fig. 3 illustrates the rate difference versus rate ratio; newborn conditions (e.g., transient tachypnoea of newborn) had a large rate ratio and large rate difference when comparing males to females. Results from the multivariable analyses were similar to the initial RR results (Table 2, Supplementary Tables S10–S29).
Fig. 3.
Inequalities in the hospitalisation rate by sex for the 15 most costly and 15 most prevalent conditions. The figure presents the inequalities in hospitalisation rate by sex using rate difference and rate ratio. A rate difference greater than 0 indicates that the hospitalisation rate for the condition was greater in males than females, and a rate difference lesser than 0 indicates that the hospitalisation rate was lower in males than females. A rate ratio greater than 1 indicates that the hospitalisation rate for the condition was greater in males than females, while a rate ratio lesser than 1 indicates that the rate was lower in males than females. Conditions with the largest inequalities (i.e., have high rate difference and rate ratio) will be those in the top-right and bottom-left areas of the panels.
Inequalities in hospitalisations by immigrant status
For 11 conditions, the hospitalisation rates were highest in non-immigrant children (Supplementary Table S7). When comparing non-refugee immigrants to non-immigrants, with rates greater in non-refugee immigrants, the highest absolute inequalities in hospitalisation was observed in low birth weight (Supplementary Table S8). The highest relative inequalities were observed in mental health conditions such as major depressive disorder (RR: 2·8, 95% CI: 2·7–2·9), and adjustment disorders (RR: 2·01, 95% CI: 1·91–2·12). Newborn conditions such as other perinatal conditions (RD: −1,621·6 hospitalisations per 100,000, 95% CI: −1,715·7 to −1,527·6 hospitalisation per 100,000), preterm newborn (RD: −859·8 hospitalisations per 100,000, 95% CI: −930·9 to −788·8 hospitalisation per 100,000), and drug withdrawal syndrome in newborn (RR: 0·13, 95% CI: 0·11–0·16), also had high hospitalisation disparities along with hypertrophy of tonsils adenoids (RR: 0·44, 95% CI: 0·42–0·46), but with the rates higher in non-immigrants versus non-refugee immigrants.
When comparing refugees to non-immigrants, with rates greater in refugees, the highest absolute inequalities in hospitalisation was observed in low birth weight, and highest relative inequalities in hospitalisation was observed in acute appendicitis without peritonitis (RR: 1·3, 95% CI: 1·2–1·4) (Supplementary Table S8). Drug withdrawal syndrome in newborn (RR: 0·09, 95% CI: 0·05–0·15), preterm newborn (RD: −311·5 hospitalisations per 100,000, 95% CI: −487·5 to −135·5 hospitalisations per 100,000), and anxiety disorders (RR: 0·5, 95% CI: 0·4–0·7) were also observed to have high hospitalisation disparities, but with rates greater in non-immigrants versus refugees.
Fig. 4 illustrates the rate difference versus rate ratio comparing non-refugee immigrants to non-immigrants, and Fig. 5 comparing refugees to non-immigrants. Fig. 4 outlines newborn conditions (e.g., drug withdrawal syndrome in newborn) and major depressive disorder to have a large rate difference and rate ratio. In Fig. 5, drug withdrawal syndrome in newborn was observed to have a large rate difference and rate ratio.
Fig. 4.
Inequalities in the hospitalisation rate comparing non-refugee immigrants to non-immigrants for the 15 most costly and 15 most prevalent conditions. The figure presents the inequalities in hospitalisation rate by immigrant status using rate difference and rate ratio. A rate difference greater than 0 indicates that the hospitalisation rate for the condition was greater in non-refugee immigrants compared to non-immigrants, and a rate difference lesser than 0 indicates that the hospitalisation rate was lower in non-refugee immigrants compared to non-immigrants. A rate ratio greater than 1 indicates that the hospitalisation rate for the condition was greater in non-refugee immigrants versus non-immigrants, while a rate ratio lesser than 1 indicates that the rate was lower in non-refugee immigrants versus non-immigrants. Conditions with the largest inequalities (i.e., have high rate difference and rate ratio) will be those in the top-right and bottom-left areas of the panels.
Fig. 5.
Inequalities in the hospitalisation rate comparing refugees to non-immigrants for the 15 most costly and 15 most prevalent conditions. The picture presents the inequalities in hospitalisation rate by immigrant status using rate difference and rate ratio. A rate difference greater than 0 indicates that the hospitalisation rate for the condition was greater in refugees compared to non-immigrants, and a rate difference lesser than 0 indicates that the hospitalisation rate was lower in refugees compared to non-immigrants. A rate ratio greater than 1 indicates that the hospitalisation rate for the condition was greater in refugees versus non-immigrants, while a rate ratio lesser than 1 indicates that the rate was lower in refugees versus non-immigrants. Conditions with the largest inequalities (i.e., have high rate difference and rate ratio) will be those in the top-right and bottom-left areas of the panels.
Results from the multivariable analyses identified some differences compared to the initial RRs (Table 2, Supplementary Tables S10–S29). When comparing non-refugee immigrants to non-immigrants, the observed effect size for mental health conditions changed. For example, in anorexia nervosa, the association reversed from higher hospitalisation rates in non-refugee immigrants versus non-immigrants (RR: 1·8, 95% CI: 1·6–2·0) to higher hospitalisation rates in non-immigrants than non-refugee immigrants (aOR: 0·6, 95% CI: 0·5–0·7). For the comparison between refugees to non-immigrants, the effect size for acute appendicitis without peritonitis changed direction in the multivariable model suggesting a higher hospitalisation in non-immigrants versus refugees (aOR: 0·8, 95% CI: 0·7–0·9), while for anorexia nervosa the change in the magnitude of effect from the initial RR versus the multivariable model revealed it to have higher relative hospitalisation disparities than initially estimated (RR: 0·7, 95% CI: 0·5–1·0; aOR: 0·3, 95% CI: 0·2–0·6).
Interaction effect between material resources and immigrant status on hospitalisation
Hospitalisation for four conditions (i.e., Drug withdrawal syndrome in newborn, adjustment disorders, anxiety disorders, and major depressive disorder) were identified with a statistically significant interaction between material resources and immigrant status (Supplementary Tables S10, S26, S28 and S29). Furthermore, the effect of material resources (comparing the least to most resourced quintile) on hospitalisation significantly differed for non-immigrants compared to the other two groups, with the highest odds for hospitalisation among non-immigrants.
Discussion
Measuring health inequalities across population subgroups can identify where avoidable and unjust differences in health and health care exists, to act on them, and to measure progress towards attaining health equity.4,10 We used population-based health administrative data to determine stratified hospitalisation rates across population groups by four important equity stratifiers for the most costly and prevalent conditions in hospitalised children. Newborn and mental health conditions—low birth weight, drug withdrawal syndrome in newborn, adjustment disorders (emotional or behavioural symptoms in response to a critical life event or an external life stressor25), and anxiety disorders—had large inequalities by material resources, rurality, sex, and immigrant status. Findings remained mostly consistent once adjusted for potential confounding factors, however, for some conditions, there were differences in the magnitude and/or direction of the effect between immigrant status and hospitalisation. Moreover, for three mental health conditions and one newborn condition, there was a statistically significant interaction between material resources and immigrant status with hospitalisation as the outcome. Our findings suggest where future health equity research and policy efforts should focus to address and reduce the inequalities observed across the population. This study is the first step in building a health equity research agenda, as it identifies areas that should be prioritised for future research of interventions to narrow the health inequalities gap.
Newborn conditions (e.g., low birth weight, drug withdrawal syndrome in newborn) had large differences in both absolute and relative inequality measures, with children in the least resourced group having a higher hospitalisation rate. A UK systematic review similarly reported that area deprivation was strongly associated with infants having low birth weight, with odds of 1·81 (95% CI: 1·71–1·92) for low birth weight when comparing those in the highest to the lowest deprivation quintile.26 Prior work that examined mother-infant dyads has also reported a strong association between infants with drug withdrawal syndrome in newborn and low socioeconomic status based on maternal residential neighbourhood.27 Mothers in poor socioeconomic environments often experience economic constraints and exposure to long-standing psychological stress, resulting in unhealthy lifestyles and poor pregnancy outcomes.28 It is essential that optimal healthcare is provided during the prenatal, childbirth and postpartum periods to reduce harm and prevent further adverse outcomes in the infants.27
Hospitalisation rates for 12 of the 20 conditions were higher in children living in rural versus urban areas, however, after adjusting for confounders, higher rates remained for only five conditions including drug withdrawal syndrome in newborn. Rural residents often have difficulties accessing appropriate obstetric and neonatal care, and have higher rates of poverty, which increases the risk of severe maternal and perinatal morbidity.29 Prior studies observed similar hospitalisation inequalities by rurality for drug withdrawal syndrome in newborn.30 Therefore, it is important that policy efforts address the rural-urban differences in social determinants of health, including providing timely prenatal and postnatal care in rural areas to reduce the risk of adverse outcomes.29 Large hospitalisation inequalities by rurality were also observed for low birth weight but with higher hospitalisation rates in urban versus rural areas. This finding aligns with the existing evidence of infants residing in rural areas being less likely to be small for gestational age compared to in urban areas.29
Hospitalisation rates for 14 of the 20 conditions were higher in males compared to females. Prior studies have noted higher hospitalisations in males for conditions such as the ambulatory care sensitive conditions,31 with variation based on age in children.8 The sex-related differences observed may be due to the hormonal differences between the sexes and their effect on the immune system,32 or sex-based differences in seeking care, in perception of symptoms, and knowledge of disease self-management.8 Hospitalisation disparities by sex were also the largest for newborn conditions. Our findings corroborate existing literature that newborn conditions such as surfactant deficiency disorder is more prevalent in males than females in newborn infants.33 We also observed large hospitalisation inequalities for mental health conditions by sex, with high rates in females, consistent with previous research among children.34 This sex-difference observed may be due to females having a higher prevalence of mental health disorders such as mood disorders compared to males, as observed in an adult-study.35 Although higher hospital use was observed in females, it is important to note that suicide death rates were observed to be far higher in males among children and adolescents,36 indicating the need of mental health support for both sex.
Over half of the conditions had the highest hospitalisation rate in non-immigrant children. Similar findings of higher hospitalisation rates in non-immigrants versus immigrants have been reported in a previous Canadian study with an adult population,20 due to the healthy immigrant effect. Yet the magnitude of this effect decreased as the immigrants' time in Canada extends, reflecting the loss of the immigrants' health advantage.20 Interestingly, large hospitalisation inequalities were observed for mental health conditions (e.g., major depressive disorder, anorexia nervosa), with larger hospitalisation rates in non-refugee immigrants compared to non-immigrants. However, after adjusting for potential confounding, the hospitalisation for these conditions were greater in non-immigrants. The higher mental health hospitalisations in non-immigrants compared to immigrants may be due to the healthy immigrant effect, and factors including self-selection and screening prior to arrival.37 Previous studies have also reported lower hospital admissions for mental health conditions in immigrants compared to non-immigrants,23,38,39 however, from immigrants who have been hospitalised, a high proportion of them were involuntary admitted.23 Involuntary admissions for immigrant youths may be due to barriers in accessing mental health services, inadequate knowledge of mental health services, differences in the culture, and language proficiency observed in immigrants.40 Interventions to improve access to, and quality of, outpatient mental health care in both immigrant and non-immigrant children should be implemented.16
For three mental health conditions, we observed an interaction effect between material resources and immigrant status on hospitalisations, with children in the least versus most resourced quintile having a higher odds of hospitalisations, and this increased risk being more pronounced in non-immigrant children compared to immigrant children. Similar findings of this relationship have been reported in previous studies.23,24 It has also been reported that for mental health services use such as community-based mental health service use or emergency department use, rates of service use were lower in immigrants compared to non-immigrants.23 The lower use in hospital services for mental health in immigrants may be due to cultural barriers (i.e., norms, or stigma), language barriers, and structural barriers (i.e., transportation, costs) that makes it difficult for them to access hospital care.41 One study reported that although there were lower hospital admissions among immigrants, a greater proportion of involuntary hospital admissions were found among immigrants compared to non-immigrants, implying that immigrants lacks preventable mental health services.23 Policy makers can focus on determining ways to improve access to mental health services to immigrants and improve the socioeconomic disparity in hospital use for mental health in non-immigrants.
Strengths of this study include: using a novel approach to identify research priorities in hospitalised children (i.e., uses a health equity lens); using population-based comprehensive health administrative data of children eligible for universal provincial health insurance to examine study objectives; using a multivariable model approach to confirm if the associations between the equity stratifiers and hospitalisation were still present after adjustment; and examining the inequalities in paediatric hospitalisations using multiple important equity stratifiers following the PROGRESS-Plus framework. Nevertheless, there were some study limitations. First, the study uses data from health administrative databases which may have coding errors of the discharge diagnosis codes of the hospital encounters. This can result in misclassification of some encounters. Second, other important equity stratifiers such as race, ethnicity, disability, and Indigenous identity, were not examined due to the lack of available data, nor were specific indicators of the child's parents or family, such as parental level of education. Sex but not gender was examined; gender and sex are social stratifying factors as both biological and gender-based differences between girls and boys result in differences in health outcomes. Third, an area-level measure of socioeconomic status was used instead of an individual-level measure. Studies have reported that area-level socioeconomic status measures have limitations as proxies for individual-level socioeconomic status measures.42 Fourth, there are limitations using the Ontario Marginalisation Index including incomplete census enumeration of certain populations (e.g., Indigenous individuals that live on reserves). Fifth, the data used in this study were collected before the COVID-19 pandemic and may not represent current inequalities.
Conclusion
This population-based cohort study measured the inequalities in hospitalisations for the most costly and prevalent conditions in hospitalised children using association estimates, and identified several newborn and mental health conditions with the largest inequalities by material resources, rurality, sex, and immigrant status. In addition, for three mental health conditions and one newborn condition, the effect of material resources on hospitalisation significantly differed in non-immigrants compared with refugees and non-refugee immigrants. The findings from this study are the first step in identifying where to direct future health equity research efforts, and also where future drill downs should be conducted - focussing on newborn (e.g., drug withdrawal syndrome in newborn) and mental health conditions - to determine opportunities to reduce health inequalities, and monitor progress towards attaining health equity in hospitalised children.
Contributors
All authors of this study participated in the concept, study design, and interpretation of data. Dr. Gill, Ms. Thavam, Ms. Zhu, Dr. Parkin, Dr. To, and Dr. Mahant contributed to the acquisition and/or analysis of the data. Dr. Gill, Dr. To, and Ms. Zhu had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. The manuscript was drafted by Dr. Gill, Ms. Thavam, and Dr. Mahant, and then was critically revised for important intellectual content by all authors of this study. The analyses, conclusions, opinions and statements expressed herein are solely those of the authors and do not reflect those of the funding source. We have not been paid to write this article by a pharmaceutical company or other agency. All authors accept responsibility to submit for publication. Dr. Gill had the final responsibility for the decision to submit for publication.
Data sharing statement
The dataset for this study is held securely in coded form at ICES. While legal data sharing agreements between ICES and data providers (e.g., healthcare organisations and government) prohibit ICES from making the dataset publicly available, access may be granted to those who meet pre-specified criteria for confidential access, available at www.ices.on.ca/DAS (email: das@ices.on.ca). Details on submitting a request form to access the data is found in the following hyperlink (https://www.ices.on.ca/DAS/Submitting-your-request). ICES has presented a publicly available data dictionary for the databases used in this study and can be found using the following hyperlink (https://datadictionary.ices.on.ca/Applications/DataDictionary/Default.aspx). The full dataset creation plan is available from the authors upon request.
Declaration of interests
Dr. Gill has received grants from the Canadian Institute of Health Research (CIHR), the PSI Foundation, and The Hospital for Sick Children. Dr. Cohen is a member of the Committee to Evaluate Drugs which provides advice to Ontario's Ministry of Health on Public Drug Policy. All other authors declare no conflict of interest.
Acknowledgements
We thank the non-financial support provided by Michelle Quinlan (Team Lead- Knowledge Mobilization, National Newcomer Navigation Network, Children's Hospital of Eastern Ontario).
This study was funded by the Physicians' Services Incorporated (PSI) Foundation Grant Number: 21-01. This study was also supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health (MOH) and the Ministry of Long-Term Care (MLTC). ICES is an independent, non-profit research institute whose legal status under Ontario's health information privacy law allows it to collect and analyze health care and demographic data, without consent, for health system evaluation and improvement. Parts or whole of this material are based on data and/or information compiled and provided by the Canadian Institute for Health Information (CIHI) and by Immigration, Refugees and Citizenship Canada (IRCC) current to [September 30, 2020]. The analyses, conclusions, opinions and statements expressed herein are solely those of the authors and do not reflect those of the funding or data sources; no endorsement by ICES or the Ontario MOH is intended or should be inferred.
Footnotes
Supplementary data related to this article can be found at https://doi.org/10.1016/j.lana.2025.101056.
Contributor Information
Peter J. Gill, Email: peter.gill@sickkids.ca.
Ontario Pediatric Hospital Care Study Group (OPHCSG):
Peter J. Gill, Sanjay Mahant, Francine Buchanan, Wenjia Chen, Ronald Cohn, Mairead Green, Matt Hall, Kate Langrish, Colin Macarthur Macarthur, and Myla Moretti
Canadian Paediatric Inpatient Research Network (PIRN):
Peter J. Gill, Sanjay Mahant, Patricia C. Parkin, Ann Bayliss, Ronik Kanani, Sean Murray, Catherine Pound, Mahmoud Sakran, Anupam Sehgal, Sepi Taheri, and Gita Wahi
Appendix ASupplementary data
References
- 1.World Health Organization . World Health Organization; Geneva: 2013. Handbook on Health Inequality Monitoring: With a Special Focus on Low- and Middle-income Countries. [Google Scholar]
- 2.National Center for Health Statistics (US) National Center for Health Statistics; Hyattsville (MD): 2016. Health, United States, 2015: with special feature on racial and ethnic health disparities.https://www.ncbi.nlm.nih.gov/books/NBK367640/ [Google Scholar]
- 3.National Academies of Sciences, Engineering, and Medicine; Health and Medicine Division; Board on Population Health and Public Health Practice; Committee on Community-Based Solutions to Promote Health Equity in the United States . National Academies Press (US); Washington, DC: 2017. Communities in Action: Pathways to Health Equity. [DOI] [Google Scholar]
- 4.World Health Organization . World Health Organization; Geneva: 2017. National Health Inequality Monitoring: A Step-by-step Manual. Licence: CC BY-NC-SA 3.0 IGO. [Google Scholar]
- 5.Welch V., Petticrew M., Tugwell P., et al. PRISMA-Equity 2012 extension: reporting guidelines for systematic reviews with a focus on health equity. PLoS Med. 2012;9 doi: 10.1371/journal.pmed.1001333. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.O'Neill J., Tabish H., Welch V., et al. Applying an equity lens to interventions: using PROGRESS ensures consideration of socially stratifying factors to illuminate inequities in health. J Clin Epidemiol. 2014;67:56–64. doi: 10.1016/j.jclinepi.2013.08.005. [DOI] [PubMed] [Google Scholar]
- 7.Public Health Agency of Canada Key health inequalities in Canada: a national portrait – executive summary. 2018. https://www.canada.ca/en/public-health/services/publications/science-research-data/key-health-inequalities-canada-national-portrait-executive-summary.html
- 8.Canadian Institute for Health Information . CIHI; Ottawa, ON: 2018. Asthma Hospitalizations Among Children and Youth in Canada: Trends and Inequalities. [Google Scholar]
- 9.Malik F.S., Hall M., Mangione-Smith R., et al. Patient characteristics associated with differences in admission frequency for diabetic ketoacidosis in United States children's hospitals. J Pediatr. 2016;171:104–110. doi: 10.1016/j.jpeds.2015.12.015. [DOI] [PubMed] [Google Scholar]
- 10.Canadian Institute for Health Information . CIHI; Ottawa, ON: 2018. In Pursuit of Health Equity: Defining Stratifiers for Measuring Health Inequality — A Focus on Age, Sex, Gender, Income, Education and Geographic Location. [Google Scholar]
- 11.von Elm E., Altman D.G., Egger M., Pocock S.J., Gøtzsche P.C., Vandenbroucke J.P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007;370:1453–1457. doi: 10.1016/S0140-6736(07)61602-X. [DOI] [PubMed] [Google Scholar]
- 12.Gill P.J., Thavam T., Anwar M.R., et al. Pediatric clinical classification system for use in Canadian inpatient settings. PLoS One. 2022;17 doi: 10.1371/journal.pone.0273580. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Gill P.J., Thavam T., Anwar M.R., et al. Prevalence, cost, and variation in cost of pediatric hospitalizations in Ontario, Canada. JAMA Netw Open. 2022;5 doi: 10.1001/jamanetworkopen.2021.47447. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Matheson F.I., Moloney G., van Ingen T. St. Michael's Hospital; Toronto, ON: 2018. 2016 Ontario Marginalization Index: User Guide.https://www.publichealthontario.ca/-/media/documents/O/2017/on-marg-userguide.pdf [Google Scholar]
- 15.Kralj B. Ontario Medical Association Economics Department; Toronto, ON: 2009. Measuring Rurality—RIO2008 BASIC: Methodology and Results. [Google Scholar]
- 16.Saunders N.R., Gill P.J., Holder L., et al. Use of the emergency department as a first point of contact for mental health care by immigrant youth in Canada: a population-based study. CMAJ. 2018;190:E1183–E1191. doi: 10.1503/cmaj.180277. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Saunders N.R., Macpherson A., Guan J., Sheng L., Guttmann A. Unintentional injuries in children and youth from immigrant families in Ontario, Canada: a population-based cross-sectional study. CMAJ Open. 2017;5:E90–E96. doi: 10.9778/cmajo.20160099. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Canadian Institute for Health Information . CIHI; Ottawa, ON: 2010. Hospitalization Disparities by Socio-economic Status for Males and Females.https://secure.cihi.ca/free_products/disparities_in_hospitalization_by_sex2010_e.pdf [Google Scholar]
- 19.Schlotheuber A., Hosseinpoor A.R. Summary measures of health inequality: a review of existing measures and their application. Int J Environ Res Public Health. 2022;19 doi: 10.3390/IJERPH19063697. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Laberge M., Leclerc M. Immigration factors and potentially avoidable hospitalizations in Canada. SSM Popul Health. 2018 Dec 8;7 doi: 10.1016/j.ssmph.2018.100336. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Canadian Institute for Health Information . CIHI; Ottawa, ON: 2020. Children and Youth With Medical Complexity in Canada — methodology Notes.https://www.cihi.ca/sites/default/files/document/children-youth-with-medical-complexity-meth-notes-en.pdf [Google Scholar]
- 22.Tripepi G., Jager K.J., Dekker F.W., Wanner C., Zoccali C. Measures of effect: relative risks, odds ratios, risk difference, and ‘number needed to treat’. Kidney Int. 2007;72:789–791. doi: 10.1038/sj.ki.5002432. [DOI] [PubMed] [Google Scholar]
- 23.Kaoser R., Thakore P., Peterson S., et al. The relationship between neighbourhood income and youth mental health service use differs by immigration experience: analysis of population-based data in British Columbia, Canada. Int J Equity Health. 2024;23:1–12. doi: 10.1186/s12939-024-02352-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Durbin A., Moineddin R., Lin E., Steele L.S., Glazier R.H. Examining the relationship between neighbourhood deprivation and mental health service use of immigrants in Ontario, Canada: a cross-sectional study. BMJ Open. 2015;5 doi: 10.1136/bmjopen-2014-006690. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Lorenz L., Perkonigg A., Maercker A. A socio-interpersonal approach to adjustment disorder: the example of involuntary job loss. Eur J Psychotraumatol. 2018;9 doi: 10.1080/20008198.2018.1425576. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Weightman A.L., Morgan H.E., Shepherd M.A., Kitcher H., Roberts C., Dunstan F.D. Social inequality and infant health in the UK: systematic review and meta-analyses. BMJ Open. 2012;2 doi: 10.1136/bmjopen-2012-000964. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Lisonkova S., Richter L.L., Ting J., et al. Neonatal abstinence syndrome and associated neonatal and maternal mortality and morbidity. Pediatrics. 2019;144 doi: 10.1542/peds.2018-3664. [DOI] [PubMed] [Google Scholar]
- 28.Ohlsson A., Shah P. Institute of Health Economics; Edmonton, Canada: 2008. Determinants and Prevention of Low Birth Weight: A Synopsis of the Evidence. [Google Scholar]
- 29.Lisonkova S., Haslam M.D., Dahlgren L., Chen I., Synnes A.R., Lim K.I. Maternal morbidity and perinatal outcomes among women in rural versus urban areas. CMAJ. 2016;188:E456–E465. doi: 10.1503/cmaj.151382. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Villapiano N.L.G., Winkelman T.N.A., Kozhimannil K.B., Davis M.M., Patrick S.W. Rural and urban differences in neonatal abstinence syndrome and maternal opioid use, 2004 to 2013. JAMA Pediatr. 2017;171:194–196. doi: 10.1001/jamapediatrics.2016.3750. [DOI] [PubMed] [Google Scholar]
- 31.Lu S., Kuo D.Z. Hospital charges of potentially preventable pediatric hospitalizations. Acad Pediatr. 2012;12:436. doi: 10.1016/j.acap.2012.06.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Bouman A., Heineman M.J., Faas M.M. Sex hormones and the immune response in humans. Hum Reprod Update. 2005;11:411–423. doi: 10.1093/humupd/dmi008. [DOI] [PubMed] [Google Scholar]
- 33.Dani C., Reali M.F., Bertini G., et al. Risk factors for the development of respiratory distress syndrome and transient tachypnoea in newborn infants. Italian Group of Neonatal Pneumology. Eur Respir J. 1999;14:155–159. doi: 10.1034/j.1399-3003.1999.14a26.x. [DOI] [PubMed] [Google Scholar]
- 34.Arakelyan M., Freyleue S., Avula D., et al. Pediatric mental health hospitalizations at acute care hospitals in the US, 2009-2019. JAMA. 2023;329:1000–1011. doi: 10.1001/jama.2023.1992. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Seedat S., Scott K.M., Angermeyer M.C., et al. Cross-national associations between gender and mental disorders in the world health organization world mental health surveys. Arch Gen Psychiatry. 2009;66:785–795. doi: 10.1001/archgenpsychiatry.2009.36. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Bitsko R.H., Claussen A.H., Lichstein J., et al. Mental health surveillance among children — United States, 2013–2019. MMWR Suppl. 2022;71:1–42. doi: 10.15585/mmwr.su7102a1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Durbin A., Moineddin R., Lin E., Steele L.S., Glazier R.H. Mental health service use by recent immigrants from different world regions and by non-immigrants in Ontario, Canada: a cross-sectional study. BMC Health Serv Res. 2015;15:336. doi: 10.1186/s12913-015-0995-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Durbin A., Lin E., Moineddin R., Steele L.S., Glazier R.H. Use of mental health care for nonpsychotic conditions by immigrants in different admission classes and by refugees in Ontario, Canada. Open Med. 2014;8:e136. [PMC free article] [PubMed] [Google Scholar]
- 39.Grundy A., Ng E., Rank C., et al. Mental health and neurocognitive disorder–related hospitalization rates in immigrants and Canadian-born population: a linkage study. Can J Public Health. 2023;114:692–704. doi: 10.17269/s41997-023-00740-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Salami B., Mason A., Salma J., et al. Access to healthcare for immigrant children in Canada. Int J Environ Res Public Health. 2020;17:3320. doi: 10.3390/ijerph17093320. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Derr A.S. Mental health service use among immigrants in the United States: a systematic review. Psychiatr Serv. 2015;67:265. doi: 10.1176/appi.ps.201500004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Moss J.L., Johnson N.J., Yu M., Altekruse S.F., Cronin K.A. Comparisons of individual- and area-level socioeconomic status as proxies for individual-level measures: evidence from the Mortality Disparities in American Communities study. Popul Health Metr. 2021;19:1–10. doi: 10.1186/s12963-020-00244-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.