Abstract
Smart speakers have gained considerable consumer adoption and research interests. Despite their innovative interaction capabilities, a notable void exists in the literature, with no comprehensive scoping review that scrutinizes and consolidates the usage of smart speakers by providers and patients. This study performed a scoping review to explore the standalone use of smart speakers in health settings, focusing on their potential to support providers and empower patients to manage their health and well-being. Following Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines, a comprehensive search from January 2014-September 2023, using select keywords, was performed across PubMed, Web of Science, Medline, IEEE, ACM, JAMIA, Embase, CINHAL, EBSCO, and Cochrane. The literature search yielded 1546 articles, of which 59 met the inclusion criteria. The identified studies are categorized into helping patients (n=54) with themes of independent living, reducing loneliness and improving social life, aiding in patient self-care and self-management, promoting physical activity, rethinking health care and service delivery, remote patient monitoring and communication, health information queries and helping providers (n=24) with themes recording and accessing medical information, and reducing provider workload. These research studies, performed in a controlled environment with limited patients, have found smart speakers’ high feasibility, acceptability, and positive reception in patient care and support providers. Furthermore, the findings showcase opportunities to leverage and challenges to address for a future of integrating and using smart speakers seamlessly in health settings.
Article Highlights.
-
•
This systematic review identified 59 studies on using commercial smart speakers to support patients and providers. Studies primarily focused on the feasibility of the technology in health settings, with positive outcomes for acceptability and usability.
-
•
For patients, smart speakers found promise in areas, such as independent living, reducing loneliness, remote monitoring, and delivery of health care and services to promote self-reliance and improve efficiency, accessibility, and affordability.
-
•
For providers, smart speakers enable easy access to medical information, improve clinical efficiency, and reduce workload by handling trivial and nonclinical tasks.
-
•
Challenges remain around speech recognition, education on how to use smart speakers and formulate commands, integration and security issues with health care IT systems, and regulatory compliance.
Consumers increasingly use smart speakers, such as Amazon Echo and Google Home, in their daily tasks. Powered by artificial intelligence-based voice recognition, smart speakers allow consumers to interact with them using natural language and even have small conversations as humans do. The global smart speaker market is projected to grow to $24.8 billion by 2027.1 Across the available products, Amazon Echo and its variants dominate the market share, followed by Google, Apple, and others (Baidu, Alibaba, Huawei, etc.).2 The explosive growth and adoption of smart speakers can be attributed to ease of use (interaction without the need for traditional interfaces), interactive communication using natural language (intuitive and interactive communication style has made integration of smart speakers in daily lives seamless), accessibility (users can control various devices and access a wide range of services using voice), and affordability, to name a few. Furthermore, smart speaker providers provide software development kits (eg, Amazon Skills and Google Dialogflow) that allow developers to build applications, allowing businesses to connect with consumers through diverse channels. Presently, consumers use smart speakers to assist them in daily tasks (eg, reminders, alarms, etc.), information search (eg, weather, news, etc.), control devices, and entertainment (eg, listening to music, jokes, etc.).3,4 Researchers are studying the usage of smart speakers in education,5,6 marketing,7,8 privacy and confidentiality,9,10 consumer perception,9,11 and more.
Given the explosive growth and adoption of smart speakers in daily life and the existing knowledge gap regarding their use in health care, social care, and related areas, a comprehensive scoping review is warranted.12 This scoping review presents a comprehensive overview of the current usage of smart speakers in enhancing patient care and their overall well-being, improving health services, and supporting providers13 (refers to individuals, such as doctors, nurse practitioners, specialists, social workers, etc., who provide health care and services to patients in any setting). The review also identifies opportunities to seize and challenges to address for integrating smart speakers into health settings.
Methods
Protocol
The guidance for this scoping review is drawn from Arksey and O’Malley14 scoping framework, and Preferred Reporting Items for Systematic Reviews and Meta-Analyses for Scoping Reviews15 guided the scoping review reporting structure.
Search Strategy
The research study searched standard sources: PubMed, Web of Science, Medline, IEEE Explore, ACM Digital Health, JAMIA, Embase, CINHAL, EBSCO, and Cochrane, using the following query.
(“Amazon Echo” OR “Google Home” OR “Apple Homepod” OR “smart speaker” OR “conversational agent”) AND (“health” OR “clinical” OR “patient”)
The study used conversational agents to broaden the search and reduce the risk of missing published works relevant to the scoping review, as some authors referred to smart speakers as intelligent conversational agents. The search included all available fields, including title, abstract, full text, metadata, and other relevant information. The terms Amazon Echo, Google Home, and Apple HomePod are used as these commercial smart speakers dominate the market.2 Our search strategy was formulated incrementally, beginning with our initial search in August 2022. We subsequently performed a second search in December 2022, a third search in March 2023, and our final search in September 2023.
Eligibility Criteria
Table 1 summarizes the inclusion and exclusion criteria. Amazon Echo was the first smart speaker released in 2014, and Amazon Skills Kit, the software development kits for developing the applications, was released in 2018. Google Home was released in 2016, and Apple Homepod in 2018. Thus, we searched for published works from 2014 to September 2023. The search included only standalone use of smart speakers and excluded studies that use digital assistants (eg, Amazon Alexa, Google Home, Apple Siri, etc.) on smartphones, smart speakers built using custom hardware, and intelligent assistive technologies.
Table 1.
Inclusion and Exclusion Criteria
| Criterion | Inclusion | Exclusion |
|---|---|---|
| Types of published work | Journals and conferences published in peer-reviewed venues | Letter, editorial, abstract, workshop, clinical trial, white paper, and thesis |
| Timeline | From 2014 to September 2023 | Before 2014 and after September 2023 |
| Language | English | Other languages |
| Interest | Use of smart speakers by health care providers and patients to manage their health and overall well-being. | All other interests |
| Device | Commercially smart speakers | Intelligent voice agents16 and digital assistants used on smartphones and custom smart speakers |
Study Selection Methods
The authors searched the selected sources independently using the agreed search query and started screening the publications by reviewing titles and abstracts, independently assessing eligibility for full-paper review. In cases where there was a disagreement between the authors regarding the eligibility of a publication, it was marked for full-paper review to ensure a comprehensive assessment. Next, the authors independently reviewed the full text of the selected papers and finalized the inclusion or exclusion for the study. Any disagreements were resolved by discussion that required consensus from both authors.
Data Extraction and Variable Definitions
The following data points, as listed in Table 2, from the included articles: title, country, device used, audience, aim(s), study design, population, condition, and outcomes facilitated the narrative synthesis of the scoping review.
Table 2.
Extracted Data Points and their Description
| Data Point | Description |
|---|---|
| Identifier | Identifier for the publication, such as Digital Object Identifier (DOI) or PubMed Identifier (PMID) |
| Title | Title of the publication |
| Country | Location of the study |
| Device | Smart speaker used for the study |
| Audience | Primary group using the device. Patient, Provider, and Caregiver |
| Aim | Goal of the research study |
| Study design | Methodology used to collect research data to support outcomes |
| Population | Demographic characteristics of the study participants |
| Population Condition | Health care condition(s) of the study patients |
| Outcomes | Outcome of the research study |
Results
Study Selection
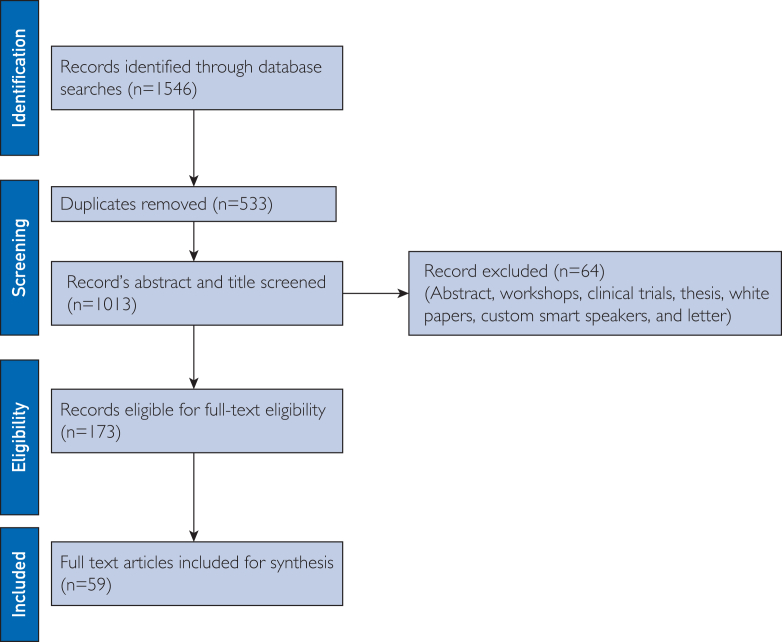
Figure 1 showcases the Preferred Reporting Items for Systematic Reviews and Meta-Analyses for Scoping Reviews workflow, illustrating the article selection process for this scoping review. The initial search resulted in 1546 publications and removed duplicates (n=533). Using the agreed inclusion and exclusion criteria (Table 1), the authors screened the publications (n=1013) abstract and title, identifying eligible publications (n=173) for a full-text review. After thoroughly examining the eligible publications, the scoping study comprised 59 publications, with the consensus reached by both authors.
Figure 1.
Illustration of PRIMSA workflow.
Characteristics of Included Studies
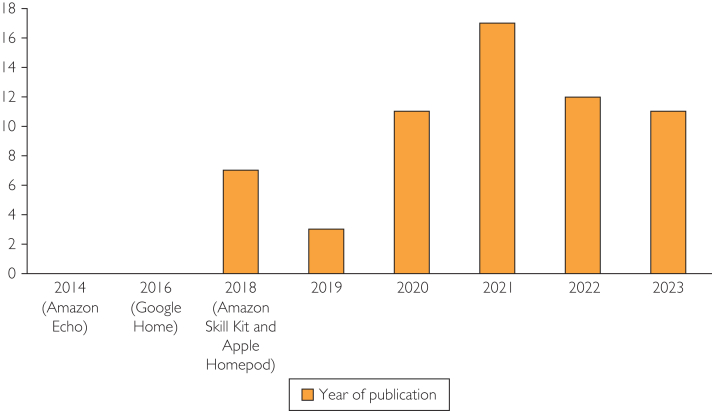
Supplemental document (Appendix 1, available online at https://www.mcpdigitalhealth.org/) enumerates the data points for included individual studies, and Table 317, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53, 54, 55, 56, 57, 58, 59, 60, 61, 62, 63, 64, 65, 66, 67, 68, 69, 70, 71, 72, 73, 74, 75, 76, 77 summarizes the data characteristics. Figure 2 reports the distribution of publications over time and the trend, signifying a growing interest among researchers in exploring the usage of smart speakers in health settings.
Table 3.
Scoping Review Study Characteristics
| Eligible Articles Characteristics |
|---|
| Research conducted |
| Australia (4)17, 18, 19, 20 |
| Canada (5)21, 22, 23, 24, 25 |
| Denmark (1)26 |
| India (1)27 |
| Ireland (1)28 |
| Italy (3)29, 30, 31 |
| Macedonia (1)32 |
| Netherlands (1)33 |
| South Korea (4)34, 35, 36, 37 |
| Switzerland (1)38 |
| United States (30)39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53, 54, 55, 56, 57, 58, 59, 60, 61, 62, 63, 64, 65, 66, 67, 68 |
| United Kingdom (7)69, 70, 71, 72, 73, 74, 75 |
| Patient primary condition |
| Autism (1)37 |
| Affective Disorders (1)26 |
| Breast Cancer (3)52,54,62 |
| Cardiovascular Disorder (1)61 |
| Cancer (2)50,51 |
| Chronic Conditions (3)17,18,70 |
| Cognitive Impairment (2)28,31 |
| COVID-19 (5)22,24,25,56,58 |
| Dementia (2)23,69 |
| Diabetes (3)44,46,70 |
| Intellectual Disability (5)19,20,33,72,73 |
| Heart Conditions (1)32 |
| Heart Failure (3)21,47,68 |
| Hypertension (1)46 |
| Visual impairments (1) |
| Device |
| Amazon Echo (14)29,39, 40, 41, 42,45,46,50,51,54,55,58,61,69,72, 73, 74, 75 |
| Amazon Echo Show (17)17,18,21,22,24,25,28,30,38,39,52,56,57,62,64,65,70 |
| Amazon Echo Dot (13)29,32,38,47,49,60,61,63,66,68,69,76,77 |
| Amazon Echo Spot (1)71 |
| Google Home Mini (4)23,29,48,53 |
| Google Nest Mini (2)26,38 |
| Google Home (12)19,20,27,28,31,33,42, 43, 44,67,72,73 |
| Apple Homepod Mini (2)29,38 |
| NUGU (3)34,35,37 |
| Aim/goal(s) |
| Support independent living (11)23,33,36,39,40,42,43,69, 70, 71, 72 |
| Reduce loneliness (6)33,39,41, 42, 43,71 |
| Self-care and self-management (6)21,37,44,47,62,68 |
| Medication adherence (1)45 |
| Remote patient monitoring (4)32,46,68,75 |
| Patient data collection and reporting (6)22,32,46,60,61,68 |
| Improve patient and provider communication (7)22,32,46,56, 57, 58,68 |
| Digital healthcare services (10)19,20,26,34,35,53, 54, 55,72,75 |
| Search medical information (3)29,38,67 |
| Promote and engage in physical activity (10)17,18,27,48, 49, 50, 51, 52,66,74 |
| Assist providers to retrieve and record medical information (2)60,61 |
| Reduce provider burden (16)19,20,22,24, 25, 26,34,35,54, 55, 56, 57, 58,64,65,73 |
| Reduce caregiver burden (6)23,28,30,31,69,70 |
Figure 2.
Represents the trend and distribution of publications over time.
Synthesis of Eligible Studies
Using natural language for interactions, smart speakers reduce the technological burden, making engagement with smart speakers natural and effortless. A plethora of research has been published and is ongoing to gain a deeper understanding of various facets of smart speakers.11,78,79 This scoping review summarized 59 studies eligible into 2 categories – Helping patients (n=54) and Helping providers (n=24) with multiple themes derived based on the research study’s primary aim(s) and conclusion(s) of the eligible studies. Smart speakers hold the potential to support patients (eg, independent living, enabling self-care and self-management, providing a voice, communication, etc.) and providers (eg, handling repetitive and trivial tasks, information on demand, etc.).
Helping Patients
Independent Living
Independent living is the ability of individuals to live independently in their own homes with minimal assistance while maintaining control over their lives. However, health issues, specifically related to cognitive decline and disabilities, and other health conditions, such as chronic conditions, hinder independent living and performing activities of daily living. Researchers are exploring smart speakers as an assistive technology, either standalone or combined with other digital technologies, to facilitate and support independent living. Dharan et al,23 Firth et al,69 and Balasubramanian et al70 research reports that smart speakers are feasible and efficient in assisting dementia patients to complete basic ADL or other activities without assistance. Van Wingerden et al,33 Smith et al,72 Corbett et al,40 McCloud et al,42 Wright,75 and O’Brien et al43 studies reported participants using smart speakers for communication, entertainment, information retrieval, keeping them engaged, and other self-reliance factors that support independent living. Edwards et al71 and Kadylak et al39 reported the benefits for the community housing residents, including enhanced engagement with home activities, enjoyment, calming effects, and skills acquisition. Using smart speakers, Kim36 reported the feasibility of promoting and improving positive health behavior among older adults. These findings collectively report that smart speakers support independent living.
Reduce Loneliness and Improving Social Life
Human beings are inherently social beings. Our community relations, engagements, and healthy social interactions drive our mental health and well-being. Researchers are leveraging smart speakers’ voice interaction model to reduce loneliness and improve social interactions. Jones et al41 developed a proof-of-concept smart speaker application that allows aging adults friendly greetings and polite interaction, considerably reducing loneliness. Van Wingerden et al,33 McCloud et al,42 Kadylak et al,39 Edwards et al,71 and O’Brien et al43 research studies found that smart speakers can serve as companions, a voice to talk to for adults living alone. These studies revealed that participants found value in having a voice to interact with and talk to daily, providing a sense of companionship and reducing feelings of isolation. Postresearch interviews and surveys revealed participants’ desire to continue using smart speakers for various daily tasks, reporting the potential of smart speakers to assist and engage older adults.33,41
Self-Care and Self-Management
There is a growing emphasis on encouraging patients to take an active role in their self-care and self-management, particularly among the increasing population dealing with chronic condition(s).80,81 Researchers are investigating whether smart speakers to support patients to effectively monitor symptoms, follow treatment plans, and embrace healthy lifestyle practices. Cheng et al44 developed an innovative Healthy Coping with Diabetes application, compliant with the American Association of Diabetic Educators guidelines, to assist patients with diabetes with self-management. The study participants found the application highly usable, with a user interface facilitating natural and seamless conversations. To better manage the symptoms of patients with metastatic breast cancer and to reduce the symptom burden, Gordon et al62 has translated Nurse Addressing Metastatic Individuals Everyday,82 a proven tablet-based digital tool, into a smart speaker application and reported the feasibility and acceptability of the technology in managing metastatic breast cancer symptoms. Corbett et al45 designed a medication adherence application and reported a decrease in missed medication doses compared with their baseline before using the smart speaker. The participants also expressed positive attitudes toward the usability and usefulness of the application, reporting its effectiveness in managing their medication schedules. Shara et al,68 Apergi et al,47 and Barbaric et al21 reported the feasibility of using smart speakers for sustainable delivery of self-care and self-management instructions. These studies concluded that voice technology would profoundly affect the quality of life for in-home, independent, and assisted-living patients. Cha et al37 found that smart speakers could be an engaging and empowering tool that supports adolescents with autism spectrum disorder in addressing their needs, promoting self-care, regulating negative emotions, and practicing conversational skills.
Encouraging, Engaging, and Supporting Physical Activity
Experts concur that physical activity has various health benefits for all age groups. However, the solution(s) to encourage and engage individuals in physical activity must be scalable, cost-effective, and customizable to the individual’s lifestyle. Carlin et al,74 Chin et al,48 Smolyak et al,66 Luo et al,49 Hassoon et al,50,51 Jansons et al,17,18 and Caru et al52 explored smart speakers to deliver physical activity programs. These studies examined the feasibility, usability, and effectiveness of using smart speakers as a remote delivery method for physical activity programs and compared their novel approach with other delivery mechanisms. Carlin et al74 delivered physical activity- and diet-related messages to families through smart speakers and reported high levels of engagement and acceptance of the technology from the participants. Chin et al,48 Smolyak et al,66 and Luo et al49 delivered exercise programs to older adults and reported the novel delivery model to be more engaging and motivating when compared with the other digital delivery models. Jansons et al18 provided pragmatic and tailored physical activity routines for older adults using smart speakers and subsequently delivered exercise-snacking interventions to older adults using the novel technology.17 Both studies found that the participants generally liked the flexibility and convenience offered by this novel approach. Vora et al27 developed a proof-of-concept using cloud computing, edge processing, and a smart speaker, showcasing the feasibility of delivering personalized exercise routines to individuals. Hassoon et al50,51 and Caru et al52 used smart speakers for personalized physical activity in a study group (many with breast cancer) and reported a significant increase in physical activity while using smart speakers compared with other digital interventions. These studies report that smart speakers can be the digital platform capable of delivering physical activity programs and interventions in a feasible, scalable, and accessible form to meet individual needs.
Rethinking the Delivery of Health Care and Services
The traditional health care model, centered around hospitals and clinics, has been the primary avenue for delivering health care services. As the demand grows, the resources within the traditional health care model face limitations, making it impractical to provide high-quality health care services consistently and effectively to everyone at scale, necessitating innovative health care and service delivery approaches. Wright75 reported that local authorities in London piloted small-scale initiatives to use smart speakers to offer telemedicine and related services to achieve sustainable care in response to the nation’s challenges in adult care. Patients with disabilities often face challenges in social interactions, which are crucial for managing daily tasks. However, social programs designed to support them are generally underfunded, and employing support staff to assist these patients can be costly. To this end, Smith et al73 and Greuter19,20 investigated using smart speakers to assist patients with disabilities in improving social skills. Smith et al73 delivered related health services to individuals with intellectual disabilities and reported that smart speakers can improve speech intelligibility among participants. Similarly, Greuter et al19 developed social games and interactive storytelling experiences to engage and enhance social interactions among patients with disability. The study reported that smart speakers are a feasible and cost-effective alternative to paid support. In another study, Greuter et al20 facilitates training and practice of social skills among adults with intellectual disabilities, allowing participants to explore the outcomes of various choices in diverse social situations. Compared with the conventional method of relying on a speech therapist, this novel approach presented immediate rewards, spaced practice, enhanced autonomy, intrinsic motivation, and reduced social barriers. Kim et al34 and Maharjan et al26 provided emotional and mental support to patients in need through smart speakers, traditionally provided by a specialist at a location. Kim et al34 provided emotional support to teenagers and reported the features of smart speakers, such as being good listeners, nonjudgmental, maintaining confidentiality, and offering suggestions or assistance, effectively helping teenagers manage stress. Maharjan et al26 smart speaker application, Sofia, allowed participants to self-report mental health by answering the WHO-5 questionnaire. The study reported high levels of engagement and acceptance, reporting the participant’s willingness to self-report mental health and well-being. Xu et al53 delivered dialogic reading experiences effectively for children through a smart speaker, yielding similar benefits to those achieved with a human specialist(s), and observed reduced irrelevant vocalizations and improved story comprehension. Kim et al35 confirmed the smart speaker efficiency and feasibility in delivering metamemory training, generally offered by experts at specialized centers. Similarly, Arem et al54 reported the feasibility, satisfaction, and acceptance of using smart speakers to provide cognitive behavioral therapy for insomnia to patients with breast cancer experiencing insomnia. Ismail et al55 studied the feasibility of an autonomously administered visual acuity examination using a smart speaker device in a clinical setting and reported that the differences in the reported data between the device and human values were statistically significant but were clinically insignificant.
Remote Patient Monitoring and Communication
Smart speakers can facilitate telehealth, as telehealth benefits patients and providers with outcomes equal to in-person care and reduces health costs. Rabbani et al46 used the voice interaction model, compared with textual input in other digital mHealth tools, to collect patient data and report it to the provider(s). The study reported a simplified data reporting approach that improved communication and information exchange between patient and provider(s). Dojchinovski et al32 proof-of-concept application monitors, reports, and retrieves patients’ medical information, allowing near real-time data communication between patient and provider(s). Apergi et al47 used smart speakers to collect responses to questions, focusing on compliance and heart failure symptoms, as a proactive measure to monitor heart failure patients and potentially reduce hospitalization. Dunn et al,56 Franco et al,57 and Ganni et al22 proved the feasibility of using smart speakers (with display) to monitor and communicate with patients diagnosed with coronavirus disease 2019 (COVID-19). Dhakal et al58 research reported their ability to help users self-assess COVID and monitor patients’ symptoms.
Accessing Health Information
As smart speakers continue to be used for information retrieval, Berube et al38 studied the reliability of the smart speaker responses to common questions on specific noncommunicable diseases. Napolitano et al29 evaluated smart speakers to assess their ability to recognize and respond to questions related to male sexual health. Owens et al67 performed a similar evaluation, but the focus was on the topic of prostate cancer. These studies reported the feasibility of delivering medical information and emphasized the necessity for enhanced collaboration between health care experts and smart speaker manufacturers to ensure consistent and reliable responses to health-related questions.
Helping Providers
Reporting Patient Medical Information
Although the implementation of electronic health record (EHR) has brought numerous benefits, it has also presented challenges for providers.83,84 Notably, the time spent by providers updating EHR could be spent directly interacting with patients and building rapport. Bhatt et al60 designed and developed a voice agent, DocPal, to reduce physician screen time and facilitate EHR interaction through voice commands. The initial testing of DocPal found promising results, reporting its success and feasibility in reducing screen time and improving workflow efficiency. Similarly, Jadczyk et al61 developed CardioCube, a smart speaker application that can verbally collect patients’ medical data, integrate it into the EHR, and auto-generate summarized medical reports. The goal is to assist medical professionals in streamlining the time-consuming paperwork involved in patient registration processes.
Reduce Provider Burden
An increased demand and workforce shortage in health settings has led to provider burnout. Researchers are leveraging smart speakers to deliver services traditionally provided by providers, directly or indirectly reducing their burden and burnout. Franco et al57 and Hain et al63 explored the use of smart speakers in attending to trivial patient needs, such as playing music, providing entertainment, and controlling nonmedical devices in the room. Offloading these nonmedical tasks allowed nurses to focus on the patient’s needs. Hain et al63 has also reported improved clinical and workflow efficiency. Liu et al65 extended the caring for caregivers online platform to smart speakers to provide guidance, self-care suggestions, and a voice to talk to for the well-being of caregivers, as caregivers tend to downplay their health needs and have difficulty accessing support. Health care services, such as metamemory training,35 cognitive behavioral therapy for insomnia,54 assessing visual acuity,55 helping patients with disabilities improve social skills,19,20,73 and supporting patient’s emotional health delivered to meet different patient26,34 needs through smart speakers, have reported to reduce provider workload and burden. Davitt et al,64 Sharma et al,24 Dhakal et al,58 Oulousian et al,25 Dunn et al,56 and Ganni et al22 developed voice agents that allowed patients to report their symptoms and get a diagnosis or recommendation during the COVID-19 pandemic, easing workload and protecting providers. Dharan et al,23 and Balasubramanian et al70 aided patients with dementia with ADL and other activities, reporting the possibility of reducing the caregiver burden by providing guidance, reminders, and prompts. Masina et al31 reported that smart speakers can assist individuals with disabilities in their daily tasks, reducing the workload on caregivers, particularly automatable tasks. However, their study established that patients require a certain level of cognitive and linguistic capabilities to fully use smart speakers. Alemi et al28 leveraged smart speakers to implement distributed caregiving, reducing primary caregiver burnout and burden. In addition, the smart speakers engaged patients and provided information to the caregivers on demand, enhancing the support for the elderly and easing the responsibilities of the primary caregiver. Similarly, Alloatti et al30 used smart speakers that assist caregivers by providing care instructions based on recipient conditions(s), accessing information on demand, setting reminders, etc. These studies highlight the potential of smart speakers to reduce the burden on health care professionals by delivering services and interventions to patients in a convenient and accessible manner.
Discussion
In this review, we explored the application of smart speakers—an innovative technology bringing potent audio speakers with natural language processing and advanced artificial intelligence—in health settings. Our analysis scrutinized 59 studies investigating addressing diverse issues, such as supporting patient care and well-being, enhancing delivery and accessibility to services, optimizing care efficiency and clinical workflows, reducing provider burden, and facilitating telehealth services. The usage of smart speakers in health care is still in its early stages, as evident by the focus of all the studies on understanding the feasibility, usability, and acceptance of this technology. Numerous studies also reported innovative ideas and approaches using smart speakers for delivering care. Although there is enthusiasm regarding the potential of smart speakers as a cost-effective means to enhance health care access and services, studies have also brought attention to practical challenges and barriers individuals or organizations face with the technology.
Comprehending the Feasibility, Acceptability, and Usability of the Technology
Novel digital technologies are disruptive, prompting researchers to conduct feasibility studies to understand their potential, features, and technology usage for specific problem(s). As these technologies become more feasible, acceptable, and mature, they are adapted to provide digital services in various fields, including health, which is the focus of this review. The primary goal(s) of all the research studies (n=59) is to explore the feasibility of using this new technology. The included studies assess the technology’s viability and serve as a guide for extensive randomized clinical trials with broader goals that considerably effect the community. In addition to feasibility, some research studies have also investigated the acceptability17,21,33,39,54,62,63,71,74,75,85 of this novel technology by patients and providers. Across all the studies, researchers report positive findings regarding feasibility, acceptability, and attitude toward use. These outcomes are attributed to the technology’s user-friendliness, ease of use, communication capabilities, and accessibility. However, it is essential to note that the outcomes reported have small participant pool and controlled environment, warranting further research with larger populations to assess the generalizability of smart speakers in health setting. Nonetheless, the initial evidence suggests that smart speakers show great promise in health care.
Opportunity to Push the Boundaries of Telehealth
Smart speakers have proven to be an efficient mHealth tool to deliver remote health care and services, effectively bridging geographic gaps between patients and providers and improving accessibility. Studies have reported smart speakers’ ability to monitor patient health remotely—which supports proactive health management, specifically chronic conditions,32,46,68,75 delivering interventions44,50,51,62,74 and custom physical activity programs, communicating efficiently,22,32,46,56,57 and removing the constraints of physical proximity for care and services.26,34 As technology advances, the synergy between telehealth and mHealth holds great promise for developing a more patient-centric, accessible, and efficient health care and services ecosystem.
Opportunity to Improve Efficiency and Experience of Health Care and Services
Rising health care costs and the traditional model of providing health services at specific, physical locations have raised concern, driving experts to seek cost-effective, innovative approaches to assist the growing population. Studies have found individual/patient(s) to have positive and pleasant experiences while using smart speakers during hospital stays,56,57,63 which extends to individual/patient(s) living in senior living communities. Smart speakers also positively affect provider efficiency57,60,61,63 and assist individual/patient(s) in diagnosis.24,25,58,68 Furthermore, smart speaker-delivered health care and services.19,20,26,34,35,53, 54, 55,72,73can be more efficient in some scenarios compared with traditional health care service model(s) that necessitate individuals to visit a clinic or specialized providers. Compared with commonly used mHealth devices, such as smartphones and wearables, smart speakers offer a more affordable hardware option. The smart speaker, as a powerful mHealth tool that can interact using natural language and pilot studies reporting positive experience and improved efficiency, makes the device a promising tool for providing personalized care, services, and interventions to a wide range of individuals.
Challenges Interacting with the Technology in Natural Language
The included studies have identified challenges associated with smart speakers in health care. Although users use natural language with these devices, they must follow a specific structured format with designated trigger words, posing a problem for older adults who require training to use smart speakers effectively.71 Researchers have observed instances in which participants grew frustrated when their commands were not structured as expected and smart speakers failed to respond appropriately.31,37,42,85 Participants faced difficulties in understanding and giving commands,30,33,45 maintaining extended conversations,65 using trigger words,19,20 understanding responses,49 lack of feedback and acknowledgment from the device,39 and the speed of response narration,33,44 collectively contributed to their frustration. Moreover, participants’ long pauses26,31 caused interruptions, as the smart speaker mistakenly interpreted the pause as the end of the command or conversation, leading to overlapping conversations, confusion, and further frustration. These findings underscore the importance of providing sufficient training and guidance to individuals, especially older adults, to overcome these challenges and ensure smart speakers are efficient digital health tools. Improving user understanding of trigger words, command structure, and expected responses can enhance the user experience and reduce frustration.
Challenges Integrating the Novel Technology with Existing Health Technology and Infrastructure
Smart speakers’ untapped potential holds immense promise in digital health care, proven by studies showcasing feasibility, acceptability, and future possibilities. Nevertheless, these studies have also identified barriers to overcome and fully use their potential in health care. Currently, smart speakers are primarily designed for individual consumer use and cannot be effectively deployed across enterprise health care organizations.56,63,64,71,75,76 For instance, they may not comply with federal and state health laws and lack tools for remote management, configuration, and monitoring capabilities.64,71,76 Compared with mature software systems with well-established tools and processes for remote management and monitoring, the software powering smart speakers offers a different level of control, leading to security, privacy, and reliability challenges within health care organizations’ software and information ecosystems. Addressing these challenges will require collaboration between smart speaker manufacturers, health care organizations, and regulatory bodies. It will be necessary to develop standards and guidelines specific to the health care context, establish robust security and privacy measures, and design smart speakers with the needs and requirements of health care organizations in mind.
Strengths and Limitations
Our review has several notable strengths. First, we followed a rigorous process for searching, screening, and selecting pertinent literature, ensuring the validity and reliability of the included studies.14,15 Second, our search had recent papers up to September 2023, used diverse data sources, and employed broad search terms to enhance the comprehensiveness of our scoping review. This inclusive perspective allows for a more nuanced and insightful analysis of the subject matter, bolstering the overall strength of our scoping review. Although it is essential to acknowledge that our study did not critically appraise the literature or conduct a meta-analysis, our methods align with the aims and purpose of a scoping review.12 Nonetheless, it is essential to recognize that by limiting our search to well-known databases and studies written in English, our scoping review may have overlooked valuable papers written in other languages, studies with varying terminology, unpublished and in-progress studies, and published in alternative sources. In addition, the authors reviewed the studies' acknowledgment and conflict of interest to report the studies directly funded or supported by smart speaker vendors. However, studies indirectly supported by the vendors, studies with adverse outcomes and not published, or those failing to report funding sources could introduce bias in the review. Considering these limitations and biases is important when interpreting our review’s findings and potential implications.
Conclusion
This study presents a scoping review of the literature on smart speakers in health care, examining their use by patients to manage their health and assist health care providers. The review identified various health conditions and issues that were targeted, and the research study goals, outcomes, and challenges associated with using smart speakers in health care. The findings indicated that the current studies primarily focused on assessing the feasibility and usability of smart speakers in health care, often with limited participants, a logical step for understanding the technology itself. However, the review also identified several strengths across these studies, including the ability to deliver health care services with high feasibility and acceptability. Smart speakers are perceived as an affordable and engaging digital tool that offers artificial intelligence capabilities and a novel interaction modality, which could help overcome the limitations of the current health care delivery model. This work serves as a valuable reference for researchers seeking to comprehensively understand smart speaker use in health settings. This work provides a strong foundation for future research on smart speakers in health care, such as further research and validation by independent informaticists and stakeholders to enhance the validity and value.
Potential Competing Interests
The authors report no competing interests.
Acknowledgments
We would like to thank Andrew William for his help in the data curation of this work.
Footnotes
Supplemental material can be found online at https://www.mcpdigitalhealth.org/. Supplemental material attached to journal articles has not been edited, and the authors take responsibility for the accuracy of all data.
Supplemental Online Material
References
- 1.Smart home speakers Global Industry Analysts. https://www.marketresearch.com/Global-Industry-Analysts-v1039/Smart-Home-Speakers-32479167/
- 2.Laricchia F. 2022. Market share of global smart speaker shipments from 3rd quarter 2016 to 1st quarter 2022, by Vendor.https://www.statista.com/statistics/792604 [Google Scholar]
- 3.Smart speakers research with the public. Community Research. https://www.ofcom.org.uk/__data/assets/pdf_file/0022/249142/Smart-speakers-research.pdf
- 4.Laricchia F. Smart speaker use case frequency in the United States as of January 2020. https://www.statista.com/statistics/994696/united-states-smart-speaker-use-case-frequency/
- 5.Ioana-Alexandra T., Camelia Ş., Laura D. Towards accessibility in education through smart speakers. An ontology based approach. Procedia Comput Sci. 2021;192:883–892. doi: 10.1016/j.procs.2021.08.091. [DOI] [Google Scholar]
- 6.Terzopoulos G., Satratzemi M. Voice assistants and smart speakers in everyday life and in education. Inform Educ. 2020;19:473–490. doi: 10.15388/infedu.2020.21. [DOI] [Google Scholar]
- 7.Lee H., Cho C.H. Uses and gratifications of smart speakers: modelling the effectiveness of smart speaker advertising. Int J Advert. 2020;39(7):1150–1171. doi: 10.1080/02650487.2020.1765657. [DOI] [Google Scholar]
- 8.Smith K.T. Marketing via smart speakers: what should Alexa say? J Strateg Mark. 2020;28(4):350–365. doi: 10.1080/0965254X.2018.1541924. [DOI] [Google Scholar]
- 9.Lau J., Zimmerman B., Schaub F. Alexa, Are you listening? privacy perceptions, concerns and privacy-seeking behaviors with smart speakers. Proc ACM Hum-Comput Interact. 2018;2(CSCW):1–31. doi: 10.1145/3274371. [DOI] [Google Scholar]
- 10.Lutz C., Newlands G. Privacy and smart speakers: A multi-dimensional approach. Inf Soc. 2021;37(3):147–162. doi: 10.1080/01972243.2021.1897914. [DOI] [Google Scholar]
- 11.Ashfaq M., Yun J., Yu S. My smart speaker is cool! perceived coolness, perceived values, and users’ attitude toward smart speakers. Int J Hum Comput Interact. 2021;37(6):560–573. doi: 10.1080/10447318.2020.1841404. [DOI] [Google Scholar]
- 12.Munn Z., Peters M.D.J., Stern C., Tufanaru C., McArthur A., Aromataris E. Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Med Res Methodol. 2018;18(1):143. doi: 10.1186/s12874-018-0611-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Scarff J.R. What’s in a name? The problematic term “provider.”. Fed Pract. 2021;38(10):446–448. doi: 10.12788/fp.0188. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Arksey H., O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32. doi: 10.1080/1364557032000119616. [DOI] [Google Scholar]
- 15.Tricco A.C., Lillie E., Zarin W., et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169(7):467–473. doi: 10.7326/M18-0850. [DOI] [PubMed] [Google Scholar]
- 16.Wienrich C., Carolus A. Development of an instrument to measure conceptualizations and competencies about conversational agents on the example of smart speakers. Front Comput Sci. 2021;3 doi: 10.3389/fcomp.2021.685277. [DOI] [Google Scholar]
- 17.Jansons P., Fyfe J.J., Dalla Via J., Daly R.M., Scott D. Barriers and enablers associated with participation in a home-based pragmatic exercise snacking program in older adults delivered and monitored by Amazon Alexa: a qualitative study. Aging Clin Exp Res. 2023;35(3):561–569. doi: 10.1007/s40520-022-02327-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Jansons P., Fyfe J., Via J.D., Daly R.M., Gvozdenko E., Scott D. Barriers and enablers for older adults participating in a home-based pragmatic exercise program delivered and monitored by Amazon Alexa: a qualitative study. BMC Geriatr. 2022;22(1):248. doi: 10.1186/s12877-022-02963-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Greuter S., Balandin S., Watson J. Social games are fun: exploring social interactions on smart speaker platforms for people with disabilities. Acad Med. 2019:429–435. doi: 10.1145/3341215.3356308. [DOI] [Google Scholar]
- 20.Greuter S., Watson J., Balandin S. Social adventure: designing interactive smart speaker social skills games for people with intellectual disabilities. Int J Gaming Comput-Mediat Simul. 2022;14(1):1–21. doi: 10.4018/IJGCMS.303107. [DOI] [Google Scholar]
- 21.Barbaric A., Munteanu C., Ross H., Cafazzo J.A. Design of a patient voice app experience for heart failure management: usability study. JMIR Form Res. 2022;6(12) doi: 10.2196/41628. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Ganni E., Razaghizad A., Oulousian E., et al. Attitudes about artificially intelligent interactive voice response systems using amazon Alexa in cardiovascular clinics: insights from the VOICE-COVID-19 study. J Cardiovasc Transl Res. 2023;16(3):541–545. doi: 10.1007/s12265-022-10289-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Dharan N.M., Alam M.R., Mihailidis A. Speech-based prompting system to assist with activities of daily living: a feasibility study. Gerontechnology. 2021;20(2):1–12. doi: 10.4017/gt.2021.20.2.436.06. [DOI] [Google Scholar]
- 24.Sharma A., Oulousian E., Ni J., et al. Voice-based screening for SARS-CoV-2 exposure in cardiovascular clinics. Eur Heart J Digit Health. 2021;2(3):521–527. doi: 10.1093/ehjdh/ztab055. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Oulousian E., Chung S.H., Ganni E., et al. Voice-based screening for SARS-CoV-2 exposure in cardiovascular clinics (VOICE-COVID-19-II): protocol for a randomized controlled trial. JMIR Res Protoc. 2023;12 doi: 10.2196/41209. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Maharjan R., Doherty K., Rohani D.A., Bækgaard P., Bardram J.E. Experiences of a speech-enabled conversational agent for the self-report of well-being among people living with affective disorders: an in-the-wild study. ACM Trans Interact Intell Syst. 2022;12(2):1–29. doi: 10.1145/3484508. [DOI] [Google Scholar]
- 27.Vora J., Tanwar S., Tyagi S., Kumar N., Rodrigues J.J.P.C. 2017 IEEE 19th International Conference on E-Health Networking, Applications and Services (Healthcom) IEEE; 2017. Home-based exercise system for patients using IoT enabled smart speaker; pp. 1–6. [DOI] [Google Scholar]
- 28.Alemi Y., Loughman B., Uriyo M. Distributed caregiving for cognitively impaired individuals: a case report. Cureus. 2023;15(2) doi: 10.7759/cureus.34677. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Napolitano L., Barone B., Spirito L., et al. Voice assistants as consultants for male patients with sexual dysfunction: a reliable option? Int J Environ Res Public Health. 2023;20(3):2612. doi: 10.3390/ijerph20032612. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Alloatti F., Tasso R., Bolioli A., et al. 2021 IEEE Symposium on Computers and Communications (ISCC) IEEE; 2021. “Can You Help Me Measure My Blood Sugar?” Co-design of a Voice Interface to Assist Patients and Caregivers at Home; pp. 1–4. [DOI] [Google Scholar]
- 31.Masina F., Orso V., Pluchino P., et al. Investigating the accessibility of voice assistants with impaired users: mixed methods study. J Med Internet Res. 2020;22(9) doi: 10.2196/18431. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Dojchinovski D., Ilievski A., Gusev M. 2019 42nd International Convention on Information and Communication Technology, Electronics and Microelectronics (MIPRO) IEEE; 2019. Interactive home healthcare system with integrated voice assistant; pp. 284–288. [DOI] [Google Scholar]
- 33.Van Wingerden E., Vacaru S.V., Holstege L., Sterkenburg P.S. Hey Google! Intelligent personal assistants and well-being in the context of disability during COVID-19. J Intellect Disabil Res. 2023;67(10):973–985. doi: 10.1111/jir.13064. [DOI] [PubMed] [Google Scholar]
- 34.Kim J., Kim Y., Kim B., Yun S., Kim M., Lee J. Extended Abstracts of the 2018 CHI Conference on Human Factors in Computing Systems. Association for Computing Machinery; 2018. Can a machine tend to teenagers’ Emotional Needs? a study with conversational agents; pp. 1–6. (CHI EA ’18). [DOI] [Google Scholar]
- 35.Kim J., Shin E., Han K., et al. Efficacy of smart speaker–based metamemory training in older adults: case-control cohort study. J Med Internet Res. 2021;23(2) doi: 10.2196/20177. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Kim D. Can healthcare apps and smart speakers improve the health behavior and depression of older adults? A quasi-experimental study. Front Digit Health. 2023;5 doi: 10.3389/fdgth.2023.1117280. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Cha I., Kim S.I., Hong H., Yoo H., Lim Y kyung. Proceedings of the 2021 CHI Conference on Human Factors in Computing Systems. Acad Med; 2021. Exploring the Use of a Voice-based Conversational Agent to Empower Adolescents with Autism Spectrum Disorder; pp. 1–15. [DOI] [Google Scholar]
- 38.Bérubé C., Kovacs Z.F., Fleisch E., Kowatsch T. Reliability of commercial voice assistants’ responses to health-related questions in noncommunicable disease management: factorial experiment assessing response rate and source of information. J Med Internet Res. 2021;23(12) doi: 10.2196/32161. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Kadylak T., Blocker K.A., Kovac C.E., Rogers W.A. Understanding the potential of digital home assistant devices for older adults through their initial perceptions and attitudes. Gerontechnology. 2022;21(1):1–10. doi: 10.4017/GT.2022.21.1.486.06. [DOI] [Google Scholar]
- 40.Corbett C.F., Bowers D.C., Combs E.M., et al. Using virtual home assistants to address vulnerable adults’ complex care needs: an exploratory feasibility study. J Gerontol Nurs. 2023;49(6):33–40. doi: 10.3928/00989134-20230512-05. [DOI] [PubMed] [Google Scholar]
- 41.Jones V.K., Hanus M., Yan C., Shade M.Y., Blaskewicz Boron J., Maschieri Bicudo R. Reducing loneliness among aging adults: the roles of personal voice assistants and anthropomorphic interactions. Front Public Health. 2021;9 doi: 10.3389/fpubh.2021.750736. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.McCloud R., Perez C., Bekalu M.A., Viswanath K. Using smart speaker technology for health and well-being in an older adult population: pre-post feasibility study. JMIR Aging. 2022;5(2) doi: 10.2196/33498. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.O'Brien K., Light S.W., Bradley S., Lindquist L. Optimizing voice-controlled intelligent personal assistants for use by home-bound older adults. J Am Geriatr Soc. 2022;70(5):1504–1509. doi: 10.1111/jgs.17625. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Cheng A., Raghavaraju V., Kanugo J., Handrianto Y.P., Shang Y. 2018 15th IEEE Annual Consumer Communications & Networking Conference (CCNC) IEEE; 2018. Development and evaluation of a healthy coping voice interface application using the Google home for elderly patients with type 2 diabetes; pp. 1–5. [DOI] [Google Scholar]
- 45.Corbett C.F., Combs E.M., Chandarana P.S., et al. Medication adherence reminder system for virtual home assistants: mixed methods evaluation study. JMIR Form Res. 2021;5(7) doi: 10.2196/27327. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Rabbani M., Tian S., Anik A.A., et al. 2022 IEEE 46th Annual Computers, Software, and Applications Conference (COMPSAC) IEEE; 2022. Towards developing a voice-activated self-monitoring application (VoiS) for adults with diabetes and hypertension; pp. 512–519. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Apergi L.A., Bjarnadottir M.V., Baras J.S., et al. Voice interface technology adoption by patients with heart failure: pilot comparison study. JMIR MHealth UHealth. 2021;9(4) doi: 10.2196/24646. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Chin J., Quinn K., Muramatsu N., Marquez D. A user study on the feasibility and acceptance of delivering physical activity programs to older adults through conversational agents. Proc Hum Factors Ergon Soc Annu Meet. 2020;64(1):33–37. doi: 10.1177/1071181320641010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Luo Y., Lee B., Choe E.K. Proceedings of the 2020 CHI Conference on Human Factors in Computing Systems. Acad Med; 2020. TandemTrack: shaping consistent exercise experience by complementing a mobile app with a smart speaker; pp. 1–13. [DOI] [Google Scholar]
- 50.Hassoon A., Schrack J., Naiman D., et al. Increasing physical activity amongst overweight and obese cancer survivors using an Alexa-based intelligent agent for patient coaching: protocol for the Physical Activity by Technology Help (PATH) Trial. JMIR Res Protoc. 2018;7(2) doi: 10.2196/resprot.9096. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Hassoon A., Baig Y., Naiman D.Q., et al. Randomized trial of two artificial intelligence coaching interventions to increase physical activity in cancer survivors. Npj Digit Med. 2021;4(1):168. doi: 10.1038/s41746-021-00539-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Caru M., Abdullah S., Qiu L., et al. Women with metastatic breast cancer don’t just follow step-count trends, they exceed them: an exploratory study. Breast Cancer Res Treat. 2023;200(2):265–270. doi: 10.1007/s10549-023-06980-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Xu Y., Aubele J., Vigil V., Bustamante A.S., Kim Y.S., Warschauer M. Dialogue with a conversational agent promotes children’s story comprehension via enhancing engagement. Child Dev. 2022;93(2):e149–e167. doi: 10.1111/cdev.13708. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Arem H., Scott R., Greenberg D., Kaltman R., Lieberman D., Lewin D. Assessing breast cancer survivors’ perceptions of using voice-activated technology to address insomnia: feasibility study featuring focus groups and in-depth interviews. JMIR Cancer. 2020;6(1) doi: 10.2196/15859. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Ismail H.O., Moses A.R., Tadrus M., Mohamed E.A., Jones L.S. Feasibility of use of a smart speaker to administer snellen visual acuity examinations in a clinical setting. JAMA Netw Open. 2020;3(8) doi: 10.1001/jamanetworkopen.2020.13908. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Dunn M., Landman A., Cartright J., et al. Notes from the field: a voice-activated video communication system for nurses to communicate with inpatients with COVID-19. JMIR Form Res. 2022;6(3) doi: 10.2196/31342. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Franco J., Solad Y., Venkatesh A.K., et al. Exploratory descriptive analysis of smart speaker utilization in the emergency department during the COVID-19 pandemic. J Emerg Med. 2023;64(4):506–512. doi: 10.1016/j.jemermed.2023.01.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Dhakal P., Damacharla P., Javaid A.Y., Vege H.K., Devabhaktuni V.K. 2020 International Conference on Artificial Intelligence & Modern Assistive Technology (ICAIMAT) IEEE; 2020. IVACS: I ntelligent V oice A ssistant for C oronavirus Disease (COVID-19) S elf-Assessment; pp. 1–6. [DOI] [Google Scholar]
- 59.Yang S., Lee J., Sezgin E., Bridge J., Lin S. Clinical advice by voice assistants on postpartum depression: cross-sectional investigation using Apple Siri, Amazon Alexa, Google Assistant, and Microsoft Cortana. JMIR mHealth uhealth. 2021;9(1) doi: 10.2196/24045. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Bhatt V., Li J., Maharjan B. 2020 IEEE International Conference on E-Health Networking, Application & Services (HEALTHCOM) IEEE; 2021. DocPal: A Voice-based EHR assistant for health practitioners; pp. 1–6. [DOI] [Google Scholar]
- 61.Jadczyk T., Kiwic O., Khandwalla R.M., et al. Feasibility of a voice-enabled automated platform for medical data collection: CardioCube. Int J Med Inform. 2019;129:388–393. doi: 10.1016/j.ijmedinf.2019.07.001. [DOI] [PubMed] [Google Scholar]
- 62.Gordon B.R., Qiu L., Doerksen S.E., et al. Addressing metastatic individuals everyday: rationale and design of the nurse AMIE for Amazon Echo Show trial among metastatic breast cancer patients. Contemp Clin Trials Commun. 2023;32 doi: 10.1016/j.conctc.2023.101058. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Hain P “Peachy,” Cancio P, Morales G, et al. Improving nurse and patient experiences with voice-controlled intelligent personal assistants. Nurse Lead. 2023;21(2):252-258. doi:10.1016/j.mnl.2022.06.009
- 64.Davitt J.K., Brown J. Using voice and touchscreen controlled smart speakers to protect vulnerable clients in long-term care facilities. HB Degenholtz., editor. Innov Aging. 2022;6(4):igac024. doi: 10.1093/geroni/igac024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Liu Y., Wang L., Kearns W R., et al. Extended Abstracts of the 2021 CHI Conference on Human Factors in Computing Systems. Acad Med; 2021. Integrating a voice user interface into a virtual therapy platform; pp. 1–6. [DOI] [Google Scholar]
- 66.Smolyak D., Lee B., Choe E.K. Extended Abstracts of the 2018 CHI Conference on Human Factors in Computing Systems. Acad Med; 2018. TandemTrack: promoting consistent exercise leveraging multimodal training and tracking; pp. 1–6. [DOI] [Google Scholar]
- 67.Owens O.L., Leonard M., Singh A. Efficacy of Alexa, Google Assistant, and Siri for supporting informed prostate cancer screening decisions for African-American Men. J Cancer Educ. 2023;38(5):1752–1759. doi: 10.1007/s13187-023-02330-8. [DOI] [PubMed] [Google Scholar]
- 68.Shara N., Mohammed S., Bjarnadottir M., Apergi L.A., Anderson K.M. Personalized activated technology with heart failure disease specific functionality. J Card Fail. 2020;26(10) doi: 10.1016/j.cardfail.2020.09.266. [DOI] [Google Scholar]
- 69.Firth N.C., Harding E., Sullivan M.P., Crutch S.J., Alexander D.C. P4-148: Echoes around the home: can the amazon Echo be used in the home to help those living with dementia? Alzheimers Dement. 2018;14(7S_Part_28):4–148. doi: 10.1016/j.jalz.2018.06.2552. [DOI] [Google Scholar]
- 70.Balasubramanian G.V., Beaney P., Chambers R. Digital personal assistants are smart ways for assistive technology to aid the health and wellbeing of patients and carers. BMC Geriatr. 2021;21(1):643. doi: 10.1186/s12877-021-02436-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Edwards K.J., Jones R.B., Shenton D., et al. The use of smart speakers in care home residents: implementation study. J Med Internet Res. 2021;23(12) doi: 10.2196/26767. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Smith E., Sumner P., Hedge C., Powell G. Smart-speaker technology and intellectual disabilities: agency and wellbeing. Disabil Rehabil Assist Technol. 2023;18(4):432–442. doi: 10.1080/17483107.2020.1864670. [DOI] [PubMed] [Google Scholar]
- 73.Smith E., Sumner P., Hedge C., Powell G. Smart speaker devices can improve speech intelligibility in adults with intellectual disability. Int J Lang Commun Disord. 2021;56(3):583–593. doi: 10.1111/1460-6984.12615. [DOI] [PubMed] [Google Scholar]
- 74.Carlin A., Logue C., Flynn J., Murphy M.H., Gallagher A.M. Development and feasibility of a family-based health behavior intervention using intelligent personal assistants: randomized controlled trial. JMIR Form Res. 2021;5(1) doi: 10.2196/17501. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Wright J. The Alexafication of adult social care: virtual assistants and the changing role of local government in England. Int J Environ Res Public Health. 2021;18(2):812. doi: 10.3390/ijerph18020812. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Choi Y.K., Thompson H.J., Demiris G. Use of an internet-of-things smart home system for healthy aging in older adults in residential settings: pilot feasibility study. JMIR Aging. 2020;3(2) doi: 10.2196/21964. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Chung J., Winship J., Parsons P., Falls K., Bleich M. Stakeholder perspectives on implementation of smart speakers for aging in place in low-income senior housing: a qualitative study. J Gerontol Nurs. 2022;48(10):33–39. doi: 10.3928/00989134-20220908-05. [DOI] [PubMed] [Google Scholar]
- 78.Ling H.C., Chen H.R., Ho K.K.W., Hsiao K.L. Exploring the factors affecting customers’ intention to purchase a smart speaker. J Retail Consum Serv. 2021;59 doi: 10.1016/j.jretconser.2020.102331. [DOI] [Google Scholar]
- 79.Schönherr L., Golla M., Eisenhofer T., et al. Unacceptable, where is my privacy? Exploring accidental triggers of smart speakers. Preprint. 2008 doi: 10.48550/ARXIV.2008.00508. Published online 2020. arXiv. [DOI] [Google Scholar]
- 80.Lawless M.T., Tieu M., Feo R., Kitson A.L. Theories of self-care and self-management of long-term conditions by community-dwelling older adults: a systematic review and meta-ethnography. Soc Sci Med. 2021;287 doi: 10.1016/j.socscimed.2021.114393. [DOI] [PubMed] [Google Scholar]
- 81.Martínez N., Connelly C.D., Pérez A., Calero P. Self-care: a concept analysis. Int J Nurs Sci. 2021;8(4):418–425. doi: 10.1016/j.ijnss.2021.08.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Schmitz K.H., Zhang X., Winkels R., et al. Developing “Nurse AMIE”: a tablet-based supportive care intervention for women with metastatic breast cancer. Psycho-Oncology. 2020;29(1):232–236. doi: 10.1002/pon.5301. [DOI] [PubMed] [Google Scholar]
- 83.Hingle S. Electronic health records: an unfulfilled promise and a call to action. Ann Intern Med. 2016;165(11):818–819. doi: 10.7326/M16-1757. [DOI] [PubMed] [Google Scholar]
- 84.Khairat S., Coleman C., Ottmar P., Jayachander D.I., Bice T., Carson S.S. Association of electronic health record use with physician fatigue and efficiency. JAMA Netw Open. 2020;3(6) doi: 10.1001/jamanetworkopen.2020.7385. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Kim S. Exploring how older adults use a smart speaker–based voice assistant in their first interactions: qualitative study. JMIR MHealth UHealth. 2021;9(1) doi: 10.2196/20427. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.