Abstract
The application method of adhesive systems affects both immediate and long-term bond strength. This systematic review analyzed in vitro studies comparing active versus passive application of adhesives on enamel and dentin, regardless of classification. A comprehensive search was conducted in PubMed/Medline, Embase, Scopus, Web of Science, Lilacs, and Grey Literature. Included studies assessed bond strength with active or passive application. Meta-analyses were stratified by substrate (enamel and dentin) and application mode (etch-and-rinse or self-etching), using a random-effects model and I² index for heterogeneity. The RobDEMAT tool assessed the risk of bias. Out of 3022 articles, 23 met the inclusion criteria. Meta-analysis showed that passive application of universal adhesives in etch-and-rinse mode resulted in higher bond strength to enamel. However, active application of etch-and-rinse or universal adhesives in etch-and-rinse mode improved bond strength on dentin. For self-etching or universal adhesives in self-etching mode, active application enhanced bond strength on both enamel and dentin. Few studies assessed longevity, but those that did reported positive outcomes for active application. One self-curing universal adhesive showed significantly different results. In conclusion, active application improves bond strength to dentin in two-step etch-and-rinse mode and to unconditioned enamel and dentin in self-etching mode.
Keywords: Dentin-bonding agents, Adhesion, Dental substrates, Application mode, Rubbing, Enamel
1. Introduction
Since the introduction of fourth-generation adhesive systems, which utilize the use of phosphoric acid for enamel and dentin treatment and employ a separate primer and bond in a etch-and-rinse three-step approach [1], the evolution of dental adhesives has focused on reducing operator dependency and advancing functional monomers that enhance chemical interaction while minimizing dentin demineralization [2], [3]. Furthermore, the advent of universal adhesives has revolutionized the field by offering a multi-mode application, compatible with both etch-and-rinse and self-etching techniques. Depending on the manufacturer’s guidelines, these adhesives can be applied to dry or moist demineralized dentin, thereby reducing technique sensitivity associated with the use of phosphoric acid [2], [4], [5].
The performance of adhesive systems, both immediately and over time, can be affected by various factors, some of which are independent of the operator’s skill. The application of phosphoric acid etching to dentin may lead to collagen fibril collapse, which can impair adhesive penetration depth and subsequently compromise hybrid layer formation [6]. This issue is further exacerbated by the challenge of maintaining optimal dentin moisture, which complicates the bonding process [7]. Additionally, water can become trapped at the adhesive interface during polymerization, weakening the hybrid layer and making it prone to hydrolytic degradation over time [8]. Other potential problems include incomplete monomer diffusion, leading to porosity within and beneath the hybrid layer [9], as well as the exposure of collagen fibrils [10]. These exposed fibrils are vulnerable to degradation by endogenous enzymes, such as matrix metalloproteinases (MMPs), cysteines, and cathepsins [11], [12], [13].
Similarly, factors such as contamination with saliva [14] or blood [15] during the restorative procedure, inadequate solvent evaporation [16], [17], [18], [19], or improper adhesive photoactivation [20], [21] can compromise bond strength and accelerate hydrolytic degradation, regardless of the adhesive classification. These issues often lead to an increased need for replacement restorations or restoration failures due to loss of retention. To mitigate these challenges, researchers have explored strategies such as the use of MMP inhibitors to enhance restoration longevity [22], the elimination of phosphoric acid on dentin and adhesion to dry dentin [4], and the recommendation of absolute isolation to prevent surface contamination. Additionally, clinical studies suggest that the active application of adhesives improves restoration retention and reduces marginal staining [23], [24].
Each adhesive system comes with specific application instructions provided by the manufacturer, detailing whether phosphoric acid is required, whether components need to be mixed or applied separately, and specifying application and photoactivation times. However, it is often unclear which components of the adhesive system should be actively applied and under what circumstances. Furthermore, the literature remains inconclusive regarding whether active application benefits all adhesive systems, irrespective of their classification. Therefore, this study aims to systematically review in vitro studies that compare the bond strength of adhesive systems applied actively versus passively on both enamel and dentin. The hypothesis tested is that there is no significant difference between active and passive application, regardless of the adhesive type or substrate evaluated.
2. Materials and methods
2.1. Protocol and registration
This systematic review followed the guidelines of the “Preferred Reporting Items for Systematic Reviews and Meta-Analyses” (PRISMA). As it involved in vitro studies, it was registered on the “Open Science Framework” platform (https://doi.org/10.17605/OSF.IO/RJMA4).
2.2. Sources of information and search strategies
The PICOT question (Population-Intervention-Comparison-Outcome-Study Design) was formulated as follows: (Population) Teeth with application of an adhesive system, (Intervention) Active application, (Comparison) Passive application, (Outcome) Bond strength, (Type of Study) In vitro studies. MeSH terms were defined using the Medline database, while synonyms and free terms were added based on the PICOT question, supported by sentinel articles and expertise in the field. All dental adhesives (self-etch, etch-and-rinse, and universal) were included in this study. Bond strength data were obtained from microtensile, microshear, and shear test results. Table 1 outlines the search strategy used for each database (PubMed/Medline, Embase, Scopus, Web of Science, and Lilacs). Additionally, a manual search was conducted in the gray literature (Open Gray and Google Scholar), but no additional documents were included. No restrictions were applied regarding the publication date, and no filters were used; however, studies in languages other than Portuguese, Spanish, or English were excluded.
Table 1.
Search strategy used in this study.
|
Pubmed/Medline | ||
|---|---|---|
| #1 | #2 | #3 |
| (“dental enamel” [MH] OR “dentin” [MH] OR “dental enamel” OR “enamel” OR “dentin” OR “tooth tissue” OR “dental tissue” OR “dental hard tissue” OR “tooth” OR “teeth”) | (“dentin-bonding agents” [MH] OR “dentin-bonding agents” OR “bond*” OR “dental adhesive” OR “adhesive*” OR “dentin bonding” OR “universal adhesive*” OR “etch-and-rinse” OR “self-etch” OR “resin bonding” OR “adhesion” OR “adhesive systems” OR “bonding agent*” OR “bonding system*” OR “dentin system*”) | (“application mode” OR “application method*” OR “active” OR “actively” OR “active application” OR “passive application” OR “rub*” OR “scrub*”) |
| #1 AND #2 AND #3 | ||
| Embase | ||
| #1 | #2 | #3 |
| 'enamel'/exp OR 'enamel' OR 'dentin'/exp OR 'dentin' OR 'tooth tissue'/exp OR 'tooth tissue' OR 'dental tissue' OR 'dental hard tissue' OR 'tooth' OR 'teeth' | 'dentin bonding agent'/exp OR 'dentin bonding agent' OR 'bond' OR 'dental adhesive'/exp OR 'dental adhesive' OR 'adhesive'/exp OR 'adhesive' OR 'dentin bonding' OR 'universal adhesive' OR 'etch-and-rinse' OR 'self-etch' OR 'resin bonding' OR 'adhesion'/exp OR 'adhesion' | 'application mode' OR 'application method* ' OR 'active' OR 'actively' OR 'active application' OR 'passive application' OR 'rub* ' OR 'scrub* ' |
| #1 AND #2 AND #3 | ||
| SCOPUS | ||
| #1 | #2 | #3 |
| TITLE-ABS-KEY (“dental enamel” [MH] OR “dentin” [MH] OR “dental enamel” OR “enamel” OR “dentin” OR “tooth tissue” OR “dental tissue” OR “dental hard tissue” OR “tooth” OR “teeth”) | TITLE-ABS-KEY (“dentin-bonding agents” [MH] OR “dentin-bonding agents” OR “bond*” OR “dental adhesive” OR “adhesive*” OR “dentin bonding” OR “universal adhesive*” OR “etch-and-rinse” OR “self-etch” OR “resin bonding” OR “adhesion” OR “adhesive systems” OR “bonding agent*” OR “bonding system*” OR “dentin system*”) | TITLE-ABS-KEY (“application mode” OR “application method*” OR “active” OR “actively” OR “active application” OR “passive application” OR “rub*” OR “scrub*”) |
| #1 AND #2 AND #3 | ||
| Web of Science | ||
| #1 | #2 | #3 |
| ALL= (“dental enamel” [MH] OR “dentin” [MH] OR “dental enamel” OR “enamel” OR “dentin” OR “tooth tissue” OR “dental tissue” OR “dental hard tissue” OR “tooth” OR “teeth”) | ALL= (“dentin-bonding agents” [MH] OR “dentin-bonding agents” OR “bond*” OR “dental adhesive” OR “adhesive*” OR “dentin bonding” OR “universal adhesive*” OR “etch-and-rinse” OR “self-etch” OR “resin bonding” OR “adhesion” OR “adhesive systems” OR “bonding agent*” OR “bonding system*” OR “dentin system*”) | ALL= (“application mode” OR “application method*” OR “active” OR “actively” OR “active application” OR “passive application” OR “rub*” OR “scrub*”) |
| LILACS | ||
| #1 | #2 | #3 |
| (MH: “dental enamel” OR MH: “dentin” OR “dental enamel” OR “enamel” OR “dentin” OR “tooth tissue” OR “dental tissue” OR “dental hard tissue” OR “tooth” OR “teeth”) | (MH: “dentin-bonding agents” OR “dentin-bonding agents” OR “bond*” OR “dental adhesive” OR “adhesive*” OR “dentin bonding” OR “universal adhesive*” OR “etch-and-rinse” OR “self-etch” OR “resin bonding” OR “adhesion” OR “adhesive systems” OR “bonding agent*” OR “bonding system*” OR “dentin system*”) | (“application mode” OR “application method*” OR “active” OR “actively” OR “active application” OR “passive application” OR “rub*” OR “scrub*”) |
| #1 AND #2 AND #3 | ||
2.3. Eligibility criteria, study selection and data extraction
In vitro studies evaluating the effect of active or passive application of dental adhesives on bond strength to dentin or enamel were included in this systematic review. The inclusion criteria were as follows: human or bovine teeth, analysis on dentin or enamel, use of dental adhesives (regardless of their classification), presence of a control group with passive application of the same adhesive, and evaluation of bond strength using microtensile, microshear, or shear tests. The exclusion criteria included: evaluation of root dentin, dry or rehydrated dentin after phosphoric acid etching, dentin substrates altered by irradiation or affected by caries, prior application of substances with different actions (such as antibacterial agents, metalloproteinase inhibitors, or disinfectants), active application using equipment like ultrasound or electric current, absence of a control group, and storage of teeth in solutions other than water, artificial saliva, thymol, chloramine T, or freezing (solutions not recommended: alcohol, glutaraldehyde, or any fixative substance).
After the searches, the references were transferred to the EndNote X9 software (Clarivate Analytics), and duplicates were removed. Two independent researchers (C.B.A. and G.L.M.C.) conducted the title and abstract screening in a blinded manner. In cases of disagreement, a third reviewer (P.M.M.) was consulted. The same researchers performed a full-text review of the selected articles to determine whether they met the predefined inclusion criteria. Only articles that fulfilled the inclusion criteria were selected for this study. Data extraction was carried out by two researchers (C.B.A. and T.Y.U.S.). In addition to microtensile data, notes were taken regarding publication characteristics (author, year, and journal) and study details (type of tooth, type of substrate, number of samples, test type, groups evaluated, evaluation time, classification of adhesives used, and brand names). When necessary, the WebPlotDigitizer 4.5 program (Ankit Rohatgi) was used to extract data from graphs.
2.4. Risk of bias
Two independent researchers (C.B.A. and M.D.S.L.) assessed the risk of bias for each selected article based on its level of evidence, using the RoBDEMAT tool [25]. To characterize the studies, nine items within four domains were evaluated: bias related to planning and allocation (D1), specimen preparation (D2), outcome assessment (D3) and data treatment and outcome reporting (D4). The evaluators adhered to the tool's guidelines to respond to signaling questions by selecting one of the following options “sufficiently reported/adequate,” “insufficiently reported,” or “not reported/not adequate.” Discrepancies or doubts were resolved through discussion between the two researchers. The synthesis of results for each item and document was performed using RevMan 5.3 software (Review Manager – The Cochrane Collaboration).
2.5. Meta-analysis and synthesis of results
Meta-analyses were conducted using RevMan 5.3 software. For this purpose, the means, standard deviations (in MPa), and sample sizes (in teeth) of each adhesive system from the selected studies were utilized. No subdivisions were made based on the type of test (tensile or shear) or the type of tooth (human or bovine). Where available, longevity data were also included. The meta-analysis employed a 95 % confidence interval, a random-effects model, and heterogeneity was assessed using the I² index. As the analysis was based on data from in vitro studies, the certainty of evidence was not evaluated using the GRADE approach.
3. Results
3.1. Selection of studies
The search strategy was conducted in April 2022. Initially, 3022 titles were identified, and after removing duplicates using the software, 2152 documents remained. Following the review of titles and abstracts, 33 articles were selected. Of these, four articles were excluded due to the unavailability of complete documents online. After a thorough and careful reading, an additional seven articles were excluded for the following reasons: absence of bond strength values for each group separating the factors [26], lack of standard deviation values [27], absence of a control group with passive application of the adhesive [28], use of extracted teeth stored in alcoholic solution [29] or formalin prior to use [30], [31], and bonding with etch-and-rinse adhesives on dry or rehydrated dentin after phosphoric acid etching [32]. No additional documents were identified in the gray literature. Subsequently, the search was updated in March 2024, and one additional study was included, resulting in a total of 23 articles selected for data extraction (Fig. 1).
Fig. 1.
Diagram of searches and selection of studies.
3.2. Characteristics of the studies
Table 2 provides a detailed description of each selected article. Regarding enamel applications, only one study evaluated universal in etch-and-rinse mode (testing four adhesives), while four studies examined self-etch (four adhesives) or universal adhesives used in self-etch mode (eight adhesives). For dentin applications, two studies evaluated etch-and-rinse adhesive (3 products), while two studies examined universal adhesives in etch-and-rinse mode (four products; 3 with post-thermocycling evaluation). Self-etch adhesives were assessed in twelve studies (13 adhesives; 5 with additional 3-month, 6-month, or 3-year evaluations), and universal adhesives in self-etch mode were investigated in seven studies (7 adhesives; 3 with thermocycling assessment). Among the 23 selected studies, 7 used bovine teeth, and 14 employed microtensile testing as a methodology to evaluate bond strength.
Table 2.
Characteristics of selected studies.
| Reference | Substrate and number of teeth included per group (n) | Commercial Name (manufacturer) | Classification according to mode of action and clinical application protocol | Generation classification | Application method | Test used (evaluated time) |
|---|---|---|---|---|---|---|
| Ando et al., 2008 [33] | Bovine enamel (n = 10) |
I. Clearfil Tri-S Bond (Kuraray Noritake) II. G-Bond (GC Corp) |
Self-etch (one-step) | Seventh generation | No application of phosphoric acid Active: applied with light agitation. Passive: no rubbing. |
Shear (immediate) |
| Atalay & Meral, 2021 [34] | Bovine dentin (n = 12) |
I. Clearfil Universal Bond Quick (Kuraray Noritake) | Universal | Eighth generation | Etch-and-rinse: application of phosphoric acid 37 % and light drying. Self-etch: no application of phosphoric acid. Active: the bond was rubbed for 10 s, the solvent was volatilized until it stopped moving. Passive: the bond was not rubbed neither left acting for the same time, but the solvent was volatilized until it stopped moving. |
Microshear (immediate) |
| Botta et al., 2009 [35] | Human dentin (n = 8) |
I. Clearfil SE Bond (Kuraray Noritake) | Self-etch (two-step) | Sixth generation | Active: primer applied rubbing for 20 s. Passive: applied the primer and left acting for 20 s. |
Microtensile (immediate) |
| Bourgi R et al., 2023 [36] | Human dentin (n = 5) |
I. Prime Bond Universal (Dentsply) II. OptiBond Universal (Kerr Co) III. OptiBond FL (Kerr Co)* * IV. Clearfil SE Bond (Kuraray Noritake) |
Universal: I and II Etch-and-rinse (three-step): III Self-etch (two-step): IV |
Eighth generation (I and II) Fourth generation (III) Sixth generation (IV) |
Active: all adhesives were applied with active agitation for 20 s. Passive: applied for 20 s and left undisturbed. * *Previous application of phosphoric acid 37 % for 15 s and removal of excess moisture. |
Microtensile (Immediate) |
| Caneppele et al., 2012 [37] | Bovine enamel (n = 15) |
I. Futura Bond (Voco) II. Clearfil S3 Bond (Kuraray Noritake) III. Optibond All in One (Kerr Corp) |
Self-etch (one-step) | Seventh generation | No application of phosphoric acid. Active: applied rubbing for 20 s. Passive: left acting on surface for 20 s. |
Microtensile (immediate) |
| Carvalho et al., 2015 [38] | Bovine dentin (n = 5) |
I. One Step (BISCO) II. One Step Plus (BISCO) |
Etch-and-rinse (two-step)& | Fifth generation | Application of phosphoric acid 37 % for 15 s and removal of excess moisture. Active: vigorous rubbing. Passive: no rubbing. |
Microshear (immediate) |
| do Amaral et al., 2009 [39] | Human dentin (n = 5) |
I. Clearfil S3 Bond (Kuraray Noritake) II. Xeno III (Dentsply Sirona) III. Adper Prompt L-Pop (3 M) |
Self-etch (one-step) | Seventh generation | Active: applied rubbing the surface for 15–20 s. Passive: spread on the surface for 3–5 s and left acting for 15–20 s. |
Microtensile (immediate and 6 months) |
| do Amaral et al., 2010 [40] | Human dentin (n = 5) |
I. Clearfil S3 Bond (Kuraray Noritake) II. Xeno III (Dentsply Sirona) III. Adper Prompt L-Pop (3 M) |
Self-etch (one-step) | Seventh generation | Active: applied rubbing the surface for 15–20 s. Passive: spread on the surface for 3–5 s and left acting for 15–20 s. |
Microtensile (immediate) |
| Gokce et al., 2008 [41] | Human dentin (n = 10) |
I. Clearfil Protect Bond (Kuraray Noritake) | Self-etch (two-step) | Sixth generation | Active: applied actively for several times for 20 s. Passive: applied and left acting for 20 s. |
Shear (immediate) |
| Imai et al., 2017 [42] | Bovine enamel (n = 10) | I. Scotchbond Universal (3 M) II. All-Bond Universal (BISCO) III. Adhese Universal (Ivoclar Vivadent) IV. G-Premio Bond (GC Corp) |
Universal | Eighth generation | Etch-and-rinse: Application of 35 % phosphoric acid during15s and air drying. Self-etch: no phosphoric acid conditioning. Active: applied rubbing for the same time recommended by manufacturer. Passive: left acting on the surface for the same time. |
Shear (immediate) |
| Irmak et al., 2018 [43] | Human dentin (n = 6) |
I. Single Bond Universal (3 M) II. Clearfil Universal Bond (Kuraray Noritake) |
Universal | Eighth generation | Active: applied actively for 20 s with 40gf and 80gf. Passive: applied for 2 s and left acting for 18 s. |
Microtensile (immediate and 10.000 thermocycles) |
| Jang et al., 2019 [44] | Human dentin (n = 10) |
I. G-Premio Bond (GC Corp) | Universal | Eighth generation | Active: applied actively for 10 s. Passive: left acting on the surface for the same time. |
Microtensile (immediate and aged in sodium hypochlorite#) |
| Loguercio et al., 2011b [45] | Human dentin (n = 7) |
I. Clearfil S3 Bond (Kuraray Noritake) II. Xeno III (Dentsply Sirona) III. Adper Prompt L-Pop (3 M) |
Self-etch (one-step) | Seventh generation | Active: applied rubbing all the surface for 15–20 s. Passive: spread on the surface for 3–5 s and left acting for 15–20 s. |
Microtensile (immediate and 3 years) |
| Loguercio et al., 2015 [46] | Human enamel (n = 8) |
I. Adhese Universal (Ivoclar Vivadent) II. All Bond Universal (BISCO) III. Clearfil Universal (Kuraray Noritake) IV. Futura Bond U (Voco) V. G-Bond Plus (GC Corp) VI. Prime&Bond Elect (Dentsply Sirona) VII. ScotchBond Universal (3 M) |
Universal | Eighth generation | No application of phosphoric acid. Active: applied rubbing for the time recommended by manufacturer. Passive: left acting on the surface for the same time. |
Microshear (immediate) |
| Manhães et al., 2005 [47] | Human dentin (n = 2) |
I. Clearfil SE Bond (Kuraray Noritake) | Self-etch (two-step) | Sixth generation | Active: primer applied rubbing for 20 s. Passive: primer applied and left acting for 20 s. |
Microtensile (immediate) |
| Moritake et al., 2019 [48] | Human dentin (n = 10) |
I. All Bond Universal (BISCO) II. Adhese Universal (Ivoclar Vivadent) III. ScotchBond Universal (3 M) |
Universal | Eighth generation | Etch-and-rinse: application of phosphoric acid 35 % and drying. I and II: moisture dentin and III: dry* Self-etch: no application of phosphoric acid. Active: applied rubbing for the time recommended by manufacturer. Passive: left acting on surface for the same time. |
Microshear (immediate, 5000; 10,000; 30,000; and 50,000 thermocycles) |
| Pleffken et al., 2011 [49] |
Bovine dentin (n = 15) |
I. One Up Bond F Plus (Tokuyama Dental Corp) II. Clearfil SE Bond (Kuraray Noritake) III. Xeno III (Dentsply Sirona) IV. Futurabond NR (Voco) |
Self-etch (one-step (I, III and IV) and two-step (II)) | Seventh generation (I, II, and III) Sixth generation (II) |
Active: applied actively for the time recommended by manufacturer. Passive: left acting on the surface for the same time. |
Shear (immediate) |
| Prasansuttiporn et al., 2012 [50] | Human dentin (n = 3) |
I. Clearfil Protect Bond (Kuraray Noritake) II. Clearfil S3 Bond (Kuraray Noritake) III. Bond Force (Tokuyama Dental Corp) |
Self-etch (two-step (I) and one-step (II and III)) | Sixth generation (I) Seventh generation (II and III) |
Active: applied actively for the time recommended by manufacturer. Passive: left acting on the surface for the same time. |
Microtensile (Immediate) |
| Saikaew et al., 2021 [51] |
Human dentin (n = 6) |
I. Clearfil SE Bond (Kuraray Noritake) II. ScotchBond Universal (3 M) III. G-Premio Bond (GC Corp) |
Self-etch (two-step (I) and Universal (II and III)) | Sixth generation (I) Eighth generation (II and III) |
Active: applied rubbing for 5 – 10 s. Passive: left acting on the surface for the same time. |
Microtensile (Immediate) |
| Serin-Kalay et al., 2022 [52] |
Human dentin (n = 3) |
I. Clearfil Universal Bond Quick (Kuraray Noritake) II. G-Premio Bond (GC Corp) III. Tokuyama Universal Bond (Tokuyama Dental Corp) |
Universal | Eighth generation | Active: applied rubbing for 10 s. Passive: left acting on the surface for the same time. |
Microtensile (Immediate) |
| Thanatvarakorn et al., 2016 [53] | Human dentin (n = 5) |
I. Clearfil SE One (Kuraray Noritake) II. ScotchBond Universal (3 M) |
Self-etch (one-step (I) and Universal (II)) | Seventh generation (I) Eighth generation (II) |
Active: applied rubbing for 10 or 20 s. Passive: left acting on the surface for the same time. |
Microtensile (Immediate) |
| Torres et al., 2011 [54] | Bovine dentin (n = 15) |
I. Futura Bond (Voco) II. Clearfil S3 (Kuraray Noritake) III. Optibond All in One (Kerr Corp) |
Self-etch (one -step) | Seventh generation | Active: applied rubbing for 20 s. Passive: left acting on the surface for the same time. |
Microtensile (Immediate) |
| Zaki et al., 2016 [55] | Human dentin (n = 3) |
I. Adper Easy-One (3 M) II. Adper SE Plus (3 M) |
Self-etch (one-step (I) and two-step (II)) | Seventh generation (I) Sixth generation (II) |
Active: applied rubbing for 10–15 s or 15–20 s. Passive: left acting on the surface for the same time. |
Microshear (immediate and 3 months) |
Reported as “two-step universal” by manufacturer. Requires phosphoric acid conditioning.
Information confirmed by corresponding author.
Aged values were not included in meta-analyses.
3.3. Risk of bias
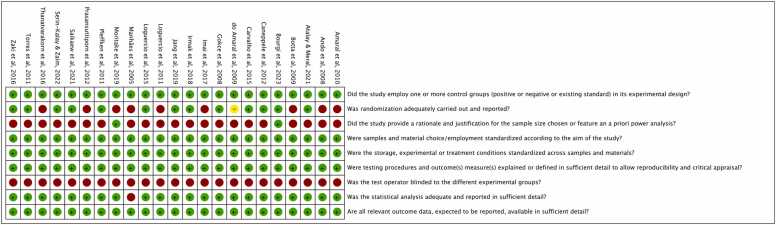
Fig. 2 displays the risk of bias assessment results for each evaluated study. The primary shortcomings identified include the absence of sample size calculations and inadequate randomization of specimens across groups. Additionally, one study [47] calculated bond strength using individual beam values rather than averaging results per tooth (the number of teeth per group was not specified), which compromises the analysis and statistical validity due to the limited number of adhesive repetitions per tooth. None of the studies reported whether the operator conducting the tests was blinded. Despite these issues, the majority of the studies were classified as having a low risk of bias, with the exception of one study [47], which was rated as having a medium risk of bias.
Fig. 2.
Risk of bias for each selected study.
3.4. Meta-analyses and synthesis of results
The bond strength data were categorized into enamel (Fig. 3, Fig. 4) and dentin (Fig. 5, Fig. 6). Furthermore, the results were organized based on the application method of the adhesive (etch-and-rinse (Fig. 3, Fig. 5) or self-etching (Fig. 4, Fig. 6)) and further subdivided by their classification (etch-and-rinse/self-etching or universal), number of steps (three-step, two-step, or one-step), and storage time. In instances where different active application strengths were tested [43], both results were included. Similarly, variations in dentin moisture, when etching was performed [37], [54], or differences in dentin preparation using sandpaper versus a diamond tip [35] were also considered. For studies evaluating the difference between one or two active or passive adhesive layers, only the results from one layer were included [49]. Results related to dentin prepared with a fine diamond tip [51], saliva contamination [34], application of phosphoric acid on dentin prior to using self-etching adhesives [41], Er:YAG laser application [35], [47], ultrasound application [44] or micro-vibration [36], or storage in sodium hypochlorite [44] were excluded. Regarding storage conditions, data for 3 months [55], 6 months [39], 3 years [45], and values after 50,000 thermocycles [48] were included. Additionally, the most recent application guidelines for each adhesive used in the selected studies were identified.
Fig. 3.
Forest plot showing the bond strength results of universal adhesives used in the etch-and-rinse mode in enamel. (I) Scotchbond Universal; (II) All-Bond Universal; (III) Adhese Universal e (IV) G-Premio Bond.
Fig. 4.
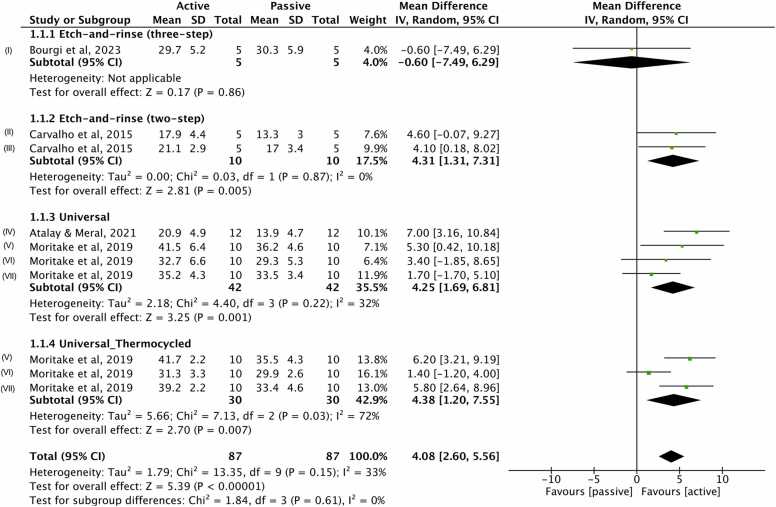
Forest plot showing the bond strength results of etch-and-rinse and universal adhesives used in the etch-and-rinse mode on dentin. (I) OptBond FL; (II) One-Step; (III) One-Step Plus; (IV) Clearfil Universal Bond Quick; (V) All Bond Universal; (VI) Adhese Universal e (VII) Scotchbond Universal.
Fig. 5.
Forest plot showing the bond strength results of self-etching and universal adhesives used in the self-etching mode on enamel. (I) Clearfil S3 Bond; (II) G-Bond; (III) Optibond All-in-One; (IV) Futurabond; (V) Scotchbond Universal; (VI) All-Bond Universal; (VII) Adhese Universal; (VIII) G-Premio Bond; (IX) Clearfil Universal; (X) Futurabond U; (XI) G-Bond Plus e (XII) Prime&Bond Elect.
Fig. 6.
Forest plot showing the bond strength results of self-etching and universal adhesives used in self-etching mode on dentin. (I) Adper Prompt L-Pop; (II) Xeno III; (III) Clearfil S3 Bond; (IV) One Up Bond F Plus; (V) Futurabond NR; (VI) Bond Force; (VII) Clearfil SE One; (VIII) Optibond All-in-One; (IX) Futurabond; (X) Adper Easy-One; (XI) Adper SE Plus; (XII) Clearfil SE Bond; (XIII) Clearfil Protect Bond; (XIV) Clearfil Universal Bond Quick; (XV) OptiBond Universal; (VXI) Prime&Bond Universal; (XVII) Scotchbond Universal; (XVIII) Clearfil Universal Bond; (XIX) G-Premio Bond; (XX) All Bond Universal; (XXI) Adhese Universal; and (XXII) Tokuyama Universal Bond.
3.4.1. Adhesives applied in etch-and-rinse mode
For the etch-and-rinse application of adhesives on enamel, only one study evaluated the use of a universal adhesive. Since this study assessed four different adhesives, a meta-analysis was conducted. The results favor for the passive application of these adhesives on enamel following acid etching (p < 0.001; Fig. 3). The mean total difference was 2.43 MPa, with low heterogeneity observed (I² = 47 %).
For dentin, two studies evaluated the use of etch-and-rinse adhesives for active or passive application. When a three-step etch-and-rinse adhesive was applied, no difference between active and passive application modes was observed (p = 0.86; Fig. 4 in section 1.1.1). In contrast, active application demonstrated superior bond strength for the two tested two-step adhesives (p = 0.005; Fig. 4 in section 1.1.2). Regarding universal adhesives, two articles were included, and the results similarly favored active application (p = 0.001; Fig. 4 in section 1.1.3). Additionally, after 50,000 thermocycles, active application of universal adhesives showed better bond strength outcomes (p = 0.007; Fig. 4 in section 1.1.4), as evaluated by a single study. When combining these three subgroups, active application consistently favored bond strength results for etch-and-rinse dentin adhesives (p < 0.001). The mean total difference was 4.08 MPa, with low heterogeneity observed (I² = 33 %).
3.4.2. Adhesives applied in self-etching mode
When actively applied to enamel, both self-etching adhesives (one-step) and universal adhesives in self-etching mode demonstrated superior bond strength results compared to passive application (p < 0.001; Fig. 5 in sections 1.1.1 and 1.1.2). Consequently, the overall analysis (across all subgroups) indicates that active application on enamel significantly outperforms passive application (p < 0.001; Fig. 5). The mean total difference was 2.83 MPa, with substantial heterogeneity observed (I² = 65 %).
A similar outcome was observed when adhesives were actively applied to dentin, with both self-etching adhesives (one-step and two-step) and universal adhesives in self-etching mode demonstrating superior bond strength results (p < 0.01; Fig. 6 in sections 1.1.1, 1.1.2, and 1.1.3). The most significant exception was the Tokuyama Universal Bond adhesive, which showed an opposing result (-3.80) and was evaluated by only one study (Fig. 6 in section 1.1.3). After storage periods of 3 months (p = 0.09), 6 months (p < 0.001), 3 years (p < 0.001), and 50,000 thermocycles (p = 0.006), active application continued to yield better bond strength outcomes in dentin (Fig. 6 in sections 1.1.4, 1.1.5, 1.1.6, and 1.1.7). Notably, only the thermocycling results pertained to universal adhesives. It is important to note that each storage condition was assessed by only one study. Overall, regardless of subgroups, active application on dentin significantly enhanced bond strength when using self-etching or universal adhesives (p < 0.001; Fig. 6). The mean total difference was 6.03 MPa, with considerable heterogeneity observed (I² = 87 %).
3.4.3. Manufacturer’s recommendation and composition of included adhesives
Table 3 outlines the composition and manufacturer-recommended application methods for each adhesive used in the selected studies. For etch-and-rinse adhesives, active application is generally indicated, though light agitation is advised. Notably, seven self-etching adhesives and three universal adhesives do not specify whether active application is recommended in their instructions for use.
Table 3.
Commercial name, composition, and indication of the manufacturer of the adhesives.
| Commercial brand | Composition | Indicates active application |
|---|---|---|
| Etch-and-rinse adhesives | ||
| One Step | Bis-GMA, BPDM, HEMA, initiator e acetone | Yes –slightly |
| One Step Plus | Bis-GMA, BPDM, HEMA, glass particle (8,5 %) and acetone | Yes –slightly |
| OptiBond FL | Etchant: 37.5 % H3PO4 Primer: HEMA, GPDM, MMEP, water, ethanol, CQ, and BHT Adhesive: Bis-GMA, HEMA, GDMA, CQ, and filler (fumed SiO2, barium aluminoborosilicat, Na2SiF6), coupling factor A174 |
Yes –slightly |
| Self-etch adhesives | ||
| Adper Easy-One | BIS-GMA, HEMA, dimethacrylates, ethanol, water, a novel photoinitator sys-tem, polyitaconic acids and a methacrylate functional acrylic | No |
| Adper Prompt L-Pop | Liquid 1(red blister): methacrylated phosphoricesters, Bis-GMA, initiators based oncamphorquinone and stabilizers Liquid 2(yellow blister): water, HEMA,polyalkenoic acid and stabilizers | Yes |
| Adper SE Plus | Liquid A: water, surfactant, HEMA and pink colorant Liquid B: UDMA, TEGDMA, TMPTMA, HEMA phosphates, MHP, bonded zirconia nano-fillers. |
Yes |
| Bond Force | Methacryloyloxyalkyl acid phosphate, TEG-DMA, bis-GMA, HEMA, glass fillers, isopropyl alcohol, CQ, water | Yes |
| Clearfil Protect Bond | Primer: 10-MDP, MDPB, HEMA, hydrophillic aliphatic dimethacrylate, N, N-dieth-anol-p-toluidine, CQ, water Bond: bis-GMA, HEMA, hydrophobic dimethacrylate, 10-MDP, MDPB, toluidine, silanated silica, CQ, sodium fluoride | No |
| Clearfil SE Bond | Primer: 10-MDP, HEMA, hydrophilicaliphatic dimethacrylate, dl-CQ, water Bond: 10-MDP, HEMA, hydrophilicaliphatic dimethacrylate, dl-CQ, water |
No |
| Clearfil SE One | MDP, bis-GMA, HEMA, hydrophilic aliphatic dimethacrylate, hydrophobic aliphatic methacrylate, ethanol, initiator, filler, accelerators, distilled water, NaF, CQ | No |
| Clearfil Tri-S Bond (or Clearfil S3 Bond) | MDP, Bis-GMA, HEMA, dimetacrilato hidrofóbico, dl-canforquinona, sílica coloidal silanada, álcool etílico e água | No |
| Futura Bond NR | Bis-GMA, dimethacrylates, hydroxyethyl methacrylate, BHT, ethanol, organic acids, fluorides, silicate fillerLiquid A: methacryloyloxyalkyl acid phosphate (phosphoric acid monomer) | Yes |
| G-Bond | 4-MET, UDMA, acetone, water, silanated colloidal silica, initiator | No |
| One Up Bond F Plus | Agent A: MAC−10 (malonic acid 10-methacryl oxide camethylene); meth-acryloxyalkyl acid phosphate, bis-GMA, TEG-DMA, photoinitiators Agent B: HEMA, water, aluminum glass powder silica; photoinitiators | Yes |
| Optibond All in One | GPDM, methacrylate453080 Premise446158 (SDS Kerr) monomer, water,ethanol, acetone,initiator, filler,sodiumhexafluorosilicate | Yes |
| Xeno III | Liquid A (green cap): HEMA, purified water,ethanolurethane, dimethacrylate resin, BHT,highly dispersed silicon dioxide Liquid B(black cap): phosphoric acidmodified polymethacrylate | No |
| Universal adhesives | ||
| Adhese Universal | HEMA, MDP, Bis-GMA, MCAP, D3MA, ethanol, water,highly dispersed silicon dioxideand camphorquinone | Yes |
| All-Bond Universal | MDP, Bis-GMA, HEMA,ethanol, water, initiators | Yes |
| Clearfil Universal | MDP, Bis-GMA, HEMA,camphorquinone, hydrophilicaliphatic dimethacrylate, silanecoupling agent, colloidal silica andaccelerators | Yes |
| Clearfil Universal Bond Quick | 10- MDP, bis-GMA, 2-HEMA, hydrophilic amide monomers, colloidal silica,silane coupling agent, sodium fluoride, dl-camphorquinone, ethanol, water | Yes |
| Futurabond U | EMA, Bis-GMA, HEDMA, acidic adhesive monomer,UDMA, catalyst | Yes |
| G-Bond Plus (ou G-aenial Bond) | Acetone,dimethacrylate, 4methacryloxyethyltrimellitateanhydride, phosphoric acid estermonomer, silicon dioxide, photoinitiator, distilled water. | No |
| G-Premio Bond | MDP, 4-MET, MEPS, BHT (butylated hydroxytoluene), acetone, dimethacrylate resins, photoinitiator, aluminium oxide, water, phosphoric acid ester monomer | No |
| Prime&Bond Elect | Mono-, di- andtrimethacrylate resins; PENTADiketone; Organic phosphineoxide; Stabilizers; Cetylaminehydrofluoride; Acetone; Water | Yes |
| Prime Bond Universal | 10-MDP, PENTA, isopropanol, water, photoinitiator, bi- and multifunctional acrylate | Yes |
| OptiBond Universal | Acetone, HEMA, GDMA, ethanol, GPDM | Yes |
| Scotchbond Universal (or Single Bond Universal) | 10-MDP, HEMA, silane,dimethacrylate resins, Vitrebond copolymer, filler,ethanol, water,initiators | Yes |
| Tokuyama Universal Bond | Liquid A: phosphoric acid monomer (3D-SR monomer), Bis-GMA, TEGDMA, HEMA, MTU−6Liquid B: acetone, isopropyl alcohol., water, borate catalyst, c-MPTES, peroxide | No |
4. Discussion
Overall, in this study, active application improved bond strength to dentin when etch-and-rinse, self-etching, and universal adhesives were used. For enamel, active application enhanced bond strength only for self-etching and universal adhesives in self-etching mode without selective acid conditioning, leading to the rejection of the tested hypothesis. A clinical trial comparing the use of two single-step self-etching adhesives applied actively or passively in class V restorations found that active application improved retention and reduced marginal pigmentation in enamel after one year [56]. According to the authors, active application appears to accelerate solvent evaporation while promoting better monomer diffusion through the dentinal smear layer, resulting in more effective demineralization [47], [56] and enhanced interaction between the smear layer and underlying dentin [40], [56]. Similarly, improved solvent evaporation and better resin infiltration into etched enamel reduce marginal pigmentation after active application of these adhesives [24], [57]. Thus, the meta-analysis results evaluating self-etching adhesives on both enamel and dentin align with the findings of the clinical trial. However, this study does not compare active versus passive application of self-etching adhesives with selective phosphoric acid etching of enamel.
Similarly, a clinical trial evaluated the active or passive application of a etch-and-rinse two-step adhesive in non-carious cervical lesions and concluded that vigorous active application improved the retention of these restorations after one year compared to passive application or light active application [23]. The authors suggest that vigorous active application of the adhesive generates mechanical pressure, compressing the collagen network (exposed by phosphoric acid etching) like a sponge [23]. As the collagen network re-expands, the adhesive infiltrates more effectively through this collapsed structure [23], [58]. Similar to single-step self-etching adhesives, active application of etch-and-rinse two-step adhesives also enhances solvent evaporation and monomer diffusion. More efficient solvent evaporation improves the polymerization reaction and the degree of conversion of the adhesives, enhancing the material's mechanical properties and, consequently, bond strength, while also reducing sorption and water solubility [16], [17], [18], [19]. Taken together, active application, for both self-etch and etch-and-rinse adhesives can also increase the moieties’ kinetics of dentin promoting deeper monomer penetration while simultaneously facilitating solvent evaporation [23], [56]. For these same reasons, a reduction in marginal pigmentation of the restorations was observed [23]. In the present study, two studies evaluated the active application of etch-and-rinse adhesives to dentin, and the overall results align with the findings of the clinical trial, except when OptiBond FL (a three-step adhesive) was used, which showed no difference between active and passive application.
In contrast, the active application of universal adhesives in etch-and-rinse mode on enamel reduced bond strength for most of the adhesives tested in the only study included in this systematic review [42]. According to the authors, manual pressure applied to enamel previously etched with phosphoric acid may have caused the collapse of enamel prisms [42], which are more fragile than collagen fibrils, resulting in a smaller area for mechanical interlocking and, consequently, lower bond strength. The mechanical action of micro-brush application potentially disrupts the characteristic etched enamel morphology (spicular etching pattern), leading to inferior bond performance [42]. Among the four adhesives evaluated, only one showed no statistical difference between active and passive application. However, this adhesive was applied for only 10 seconds (compared to 20 seconds for the others), which may have minimized the deleterious effect on the conditioned enamel [42]. Additionally, this adhesive has a more acidic pH (1.5) and contains acetone as its solvent (it's volatile and hygroscopic nature could improve monomer diffusion). The authors suggest that the formation of hydrogen ions (H⁺) may have enhanced demineralization and facilitated more effective chemical bonding between the functional monomers and calcium in hydroxyapatite. This study further demonstrated that phosphoric acid pre-treatment significantly increased enamel's total surface free energy in baseline measurements. Interestingly, when adhesives were applied in total-etch mode, active application demonstrated reduced total free energy compared to passive application across all tested materials. Both total free-energy and hydrogen-bonding components were notably diminished with active application, likely due to accelerated formation of hydrophobic calcium salts during active agitation [42]. It is important to note that enamel shear bond strength values were consistently higher for all tested materials when adhesives were applied in total-etch mode rather than in self-etch mode [42].
Still on universal adhesives, active application improved bond strength to dentin in both etch-and-rinse and self-etching modes, as well as to enamel when applied in self-etching mode. This improvement can be attributed to the factors previously discussed, such as better solvent evaporation, enhanced resin infiltration in both enamel and dentin, and more effective conditioning when applied without prior phosphoric acid etching [23], [56]. Among the universal adhesives included in the meta-analysis, only one—Tokuyama Universal Bond—showed a discrepant result when applied to dentin in self-etching mode [52]. According to the authors, this adhesive relies on a chemical curing mechanism (self-curing—borate catalyst system), and active application may negatively affect this reaction, compromising bond strength outcomes [52]. Notably, the manufacturer of this adhesive does not recommend active application.
Longer storage times and thermocycling (50,000 cycles) have demonstrated the effectiveness of universal adhesives applied actively in both etch-and-rinse and self-etching modes on dentin [48]. Additionally, self-etching adhesives have shown consistent performance even after 3 years of storage [45]. According to Moritake et al. [48], the active application of universal adhesives enhances the durability of the dentin bond. This improvement is attributed to the adhesive's ability to promote dental demineralization, achieve deeper penetration, and establish chemical bonding with the substrate, regardless of the application method. Furthermore, active application has been associated with higher bond strength values compared to passive application. In line with these findings, Loguercio et al. [45] observed reduced silver nitrate infiltration in vitro after 3 years of storage for self-etching adhesives applied to dentin, contrasting with the immediate results reported by do Amaral et al. [40].
Although the bond strength results were not categorized by test type (microtensile or shear/microshear), tooth type (human or bovine), or adhesive brand, no significant discrepancies were observed among the studies regarding the preference for active or passive application, with the exception of self-curing adhesives. This review adhered to the same methodological parameters as a previously published systematic review on bond strength [22]. However, the results should be interpreted cautiously due to several factors: the overall mean bond strength values showed only minor variations (4.08 MPa for etch-and-rinse mode on dentin; 2.83 MPa for self-etching mode on enamel; 6.03 MPa for self-etching on dentin), the limited number of studies included for etch-and-rinse and universal adhesives in etch-and-rinse mode, and the substantial heterogeneity observed in two meta-analyses. Notably, these meta-analyses included a larger number of studies, which may explain the high heterogeneity. Potential sources of variability include differences in tooth type, testing methods, light-curing units, equipment, and cell load parameters used across the studies.
In general, manufacturers should provide clear instructions on whether adhesives (for each step) should be applied actively or passively, considering factors such as the etching mode (etch-and-rinse or self-etching), the use of phosphoric acid, their mode of cure, or the type of substrate applied, as these variables may influence the optimal application method.
5. Conclusion
The active application of light-curing adhesive systems in two-step etch-and-rinse mode enhances bond strength to dentin, while in self-etching mode (one- and two-step), it improves bond strength to unconditioned enamel and dentin. However, active application is not recommended following the use of phosphoric acid on enamel or for dual-cure/self-cured adhesives. These findings highlight the importance of selecting the appropriate application technique based on the substrate and adhesive mode to optimize bonding efficacy.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
References
- 1.Milia E., Cumbo E., Cardoso R.J., Gallina G. Current dental adhesives systems. A narrative review. Curr Pharm Des. 2012;18:5542–5552. doi: 10.2174/138161212803307491. [DOI] [PubMed] [Google Scholar]
- 2.Chen C., Niu L.N., Xie H., Zhang Z.Y., Zhou L.Q., Jiao K., et al. Bonding of universal adhesives to dentine—Old wine in new bottles? J Dent. 2015;43:525–536. doi: 10.1016/j.jdent.2015.03.004. [DOI] [PubMed] [Google Scholar]
- 3.Van Meerbeek B., Yoshihara K., Yoshida Y., Mine A., De Munck J., Van Landuyt K.L. State of the art of self-etch adhesives. Dent Mater. 2011;27:17–28. doi: 10.1016/j.dental.2010.10.023. [DOI] [PubMed] [Google Scholar]
- 4.Kumagai R.Y., Hirata R., Pereira P.N.R., Reis A.F. Moist vs over-dried etched dentin: FE-SEM/TEM and bond strength evaluation of resin-dentin interfaces produced by universal adhesives. J Esthet Restor Dent. 2020;32:325–332. doi: 10.1111/jerd.12537. [DOI] [PubMed] [Google Scholar]
- 5.Sebold M., André C.B., Sahadi B.O., Breschi L., Giannini M. Chronological history and current advancements of dental adhesive systems development: a narrative review. J Adhes Sci Technol. 2020;35:1941–1967. doi: 10.1080/01694243.2020.1865611. [DOI] [Google Scholar]
- 6.Manso A.P., Marquezini L., Jr, Silva S.M., Pashley D.H., Tay F.R., Carvalho R.M. Stability of wet versus dry bonding with different solvent-based adhesives. Dent Mater. 2008;24:476–482. doi: 10.1016/j.dental.2007.04.009. [DOI] [PubMed] [Google Scholar]
- 7.Lopes L.S., Calazans F.S., Hidalgo R., Buitrago L.L., Gutierrez F., Reis A., Loguercio A.D., Barceleiro M.O. Six-month follow-up of cervical composite restorations placed with a new universal adhesive system: a randomized clinical trial. Oper Dent. 2016;41:465–480. doi: 10.2341/15-309-C. [DOI] [PubMed] [Google Scholar]
- 8.Boushell L.W. MMPs. J Esthet Restor Dent. 2013;25:217–218. doi: 10.1111/jerd.12044. [DOI] [PubMed] [Google Scholar]
- 9.Tay F.R., King N.M., Chan K.M., Pashley D.H. How can nanoleakage occur in self-etching adhesive systems that demineralize and infiltrate simultaneously? J Adhes Dent. 2002;4:255–269. [PubMed] [Google Scholar]
- 10.Breschi L., Mazzoni A., Ruggeri A., Cadenaro M., Di Lenarda R., De Stefano Dorigo E. Dental adhesion review: aging and stability of the bonded interface. Dent Mater. 2008;24:90–101. doi: 10.1016/j.dental.2007.02.009. [DOI] [PubMed] [Google Scholar]
- 11.Breschi L., Maravic T., Cunha S.R., Comba A., Cadenaro M., Tjäderhane L., et al. Dentin bonding systems: from dentin collagen structure to bond preservation and clinical applications. Dent Mater. 2018;34:78–96. doi: 10.1016/j.dental.2017.11.005. [DOI] [PubMed] [Google Scholar]
- 12.Sebold M., Giannini M., André C.B., Sahadi B.O., Maravic T., Josic U., et al. Bonding interface and dentin enzymatic activity of two universal adhesives applied following different etching approaches. Dent Mater. 2022;38:907–923. doi: 10.1016/j.dental.2022.03.001. [DOI] [PubMed] [Google Scholar]
- 13.Tjäderhane L., Nascimento F.D., Breschi L., Mazzoni A., Tersariol I.L., Geraldeli S., et al. Optimizing dentin bond durability: control of collagen degradation by matrix metalloproteinases and cysteine cathepsins. Dent Mater. 2013;29:116–135. doi: 10.1016/j.dental.2012.08.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Chaudhari R.R., Srivastava H.R., Raisingani D., Prasad A.B., Chinchalkar R.P., Gattani S., et al. Effect of saliva contamination on shear bond strength of self-etch adhesive system to dentin: an in vitro study. Int J Clin Pedia Dent. 2021;14:443–446. doi: 10.5005/jp-journals-10005-1981. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Taneja S., Kumari M., Bansal S. Effect of saliva and blood contamination on the shear bond strength of fifth-, seventh-, and eighth-generation bonding agents: An in vitro study. J Conserv Dent. 2017;20:157–160. doi: 10.4103/0972-0707.218310. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Bail M., Malacarne-Zanon J., Silva S.M., Anauate-Netto A., Nascimento F.D., Amore R., et al. Effect of air-drying on the solvent evaporation, degree of conversion and water sorption/solubility of dental adhesive models. J Mater Sci Mater Med. 2012;23:629–638. doi: 10.1007/s10856-011-4541-y. [DOI] [PubMed] [Google Scholar]
- 17.Furuse A.Y., Peutzfeldt A., Asmussen E. Effect of evaporation of solvents from one-step, self-etching adhesives. J Adhes Dent. 2008;10:35–39. [PubMed] [Google Scholar]
- 18.Loguercio A.D., Loeblein F., Cherobin T., Ogliari F., Piva E., Reis A. Effect of solvent removal on adhesive properties of simplified etch-and-rinse systems and on bond strengths to dry and wet dentin. J Adhes Dent. 2009;11:213–219. [PubMed] [Google Scholar]
- 19.Takahashi A., Sato Y., Uno S., Pereira P.N., Sano H. Effects of mechanical properties of adhesive resins on bond strength to dentin. Dent Mater. 2002;18:263–268. doi: 10.1016/s0109-5641(01)00046-x. [DOI] [PubMed] [Google Scholar]
- 20.André C.B., Nima G., Sebold M., Giannini M., Price R.B. Stability of the light output, oral cavity tip accessibility in posterior region and emission spectrum of light-curing units. Oper Dent. 2018;43:398–407. doi: 10.2341/17-033-L. [DOI] [PubMed] [Google Scholar]
- 21.Price R.B., Felix C.M., Whalen J.M. Factors affecting the energy delivered to simulated class I and class V preparations. J Can Dent Assoc. 2010;76 [PubMed] [Google Scholar]
- 22.Montagner A.F., Sarkis-Onofre R., Pereira-Cenci T., Cenci M.S. MMP inhibitors on dentin stability: a systematic review and meta-analysis. J Dent Res. 2014;93:733–743. doi: 10.1177/0022034514538046. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Loguercio A.D., Raffo J., Bassani F., Balestrini H., Santo D., do Amaral R.C., et al. 24-month clinical evaluation in non-carious cervical lesions of a two-step etch-and-rinse adhesive applied using a rubbing motion. Clin Oral Invest. 2011;15:589–596. doi: 10.1007/s00784-010-0408-8. [DOI] [PubMed] [Google Scholar]
- 24.Zander-Grande C., Ferreira S.Q., da Costa T.R., Loguercio A.D., Reis A. Application of etch-and-rinse adhesives on dry and rewet dentin under rubbing action: a 24-month clinical evaluation. J Am Dent Assoc. 2011;142:828–835. doi: 10.14219/jada.archive.2011.0272. [DOI] [PubMed] [Google Scholar]
- 25.Delgado A.H., Sauro S., Lima A.F., Loguercio A.D., Della Bona A., Mazzoni A., et al. RoBDEMAT: A risk of bias tool and guideline to support reporting of pre-clinical dental materials research and assessment of systematic reviews. J Dent. 2022;127 doi: 10.1016/j.jdent.2022.104350. [DOI] [PubMed] [Google Scholar]
- 26.Araújo C.T.P., Prieto L.T., Costa D.C., Bosso M.A., Coppini E.K., Dias C.T.S., et al. Active application of primer acid on acid-treated enamel: Influence on the bond effectiveness of self-etch adhesives systems. Microsc Res Tech. 2017;80:943–949. doi: 10.1002/jemt.22887. [DOI] [PubMed] [Google Scholar]
- 27.Torres C.R., Barcellos D.C., Pucci C.R., Lima Gde M., Rodrigues C.M., Siviero M. Influence of methods of application of self-etching adhesive systems on adhesive bond strength to enamel. J Adhes Dent. 2009;11:279–286. [PubMed] [Google Scholar]
- 28.Hardan L., Orsini G., Bourgi R., Cuevas-Suárez C.E., Nicastro M., Lazarescu F., et al. Effect of active bonding application after selective dentin etching on the immediate and long-term bond strength of two universal adhesives to dentin. Polymers (Basel) 2022;14:1129. doi: 10.3390/polym14061129. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Kharouf N., Rapp G., Mancino D., Hemmerlé J., Haikel Y., Reitzer F. Effect of etching the coronal dentin with the rubbing technique on the microtensile bond strength of a universal adhesive system. Dent Med Probl. 2019;56:343–348. doi: 10.17219/dmp/111697. [DOI] [PubMed] [Google Scholar]
- 30.Miyazaki M., Platt J.A., Onose H., Moore B.K. Influence of dentin primer application methods on dentin bond strength. Oper Dent. 1996;21:167–172. [PubMed] [Google Scholar]
- 31.Vinagre A., Ramos J., Messias A., Marques F., Caramelo F., Mata A. Microtensile Bond Strength and Micromorphology of Bur-cut Enamel Using Five Adhesive Systems. J Adhes Dent. 2015;17:107–116. doi: 10.3290/j.jad.a34060. [DOI] [PubMed] [Google Scholar]
- 32.Dal-Bianco K., Pellizzaro A., Patzlaft R., de Oliveira Bauer J.R., Loguercio A.D., Reis A. Effects of moisture degree and rubbing action on the immediate resin-dentin bond strength. Dent Mater. 2006;22:1150–1156. doi: 10.1016/j.dental.2005.10.010. [DOI] [PubMed] [Google Scholar]
- 33.Ando S., Watanabe T., Tsubota K., Yoshida T., Irokawa A., Takamizawa T., et al. Effect of adhesive application methods on bond strength to bovine enamel. J Oral Sci. 2008;50:181–186. doi: 10.2334/josnusd.50.181. [DOI] [PubMed] [Google Scholar]
- 34.Atalay C., Meral E. Does rubbing of universal adhesive reduce the negative effect of saliva on adhesion? J Adhes Dent. 2021;23:57–65. doi: 10.3290/j.jad.b916859. [DOI] [PubMed] [Google Scholar]
- 35.Botta S.B., Vieira S.N., Cordon R., Marques M.M., Matos A.B. Can the method of primer application influence adhesion to Er:YAG-laser irradiated dentin? J Conte Dent Pr. 2009;10:49–57. [PubMed] [Google Scholar]
- 36.Bourgi R., Hardan L., Cuevas-Suárez C.E., Devoto W., Kassis C., Kharma K., et al. Effectiveness of different application modalities on the bond performance of four polymeric adhesive systems to dentin. Polymers (Basel) 2023;15:3924. doi: 10.3390/polym15193924. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Caneppele T.M., Torres C.R., Sassaki A., Valdetaro F., Fernandes R.S., Prieto de Freitas C., et al. Effects of surface hydration state and application method on the bond strength of self-etching adhesives to cut enamel. J Adhes Dent. 2012;14:25–30. doi: 10.3290/j.jad.a22091. [DOI] [PubMed] [Google Scholar]
- 38.Carvalho C.N., Francci C.E., Costa J.F., Bauer J. Effect of filler and application mode on micro-shear bond strength of etch-and-rinse adhesive systems. Rev Port Estomatol Med Dent Cir Maxilofac. 2015;56:89–94. doi: 10.1016/j.rpemd.2015.05.002. [DOI] [Google Scholar]
- 39.do Amaral R.C., Stanislawczuk R., Zander-Grande C., Michel M.D., Reis A., Loguercio A.D. Active application improves the bonding performance of self-etch adhesives to dentin. J Dent. 2009;37:82–90. doi: 10.1016/j.jdent.2008.09.010. [DOI] [PubMed] [Google Scholar]
- 40.do Amaral R.C., Stanislawczuk R., Zander-Grande C., Gagler D., Reis A., Loguercio A.D. Bond strength and quality of the hybrid layer of one-step self-etch adhesives applied with agitation on dentin. Oper Dent. 2010;35:211–219. doi: 10.2341/09-198-L. [DOI] [PubMed] [Google Scholar]
- 41.Gokce K., Aykor A., Ersoy M., Ozel E., Soyman M. Effect of phosphoric acid etching and self-etching primer application methods on dentinal shear bond strength. J Adhes Dent. 2008;10:345–349. [PubMed] [Google Scholar]
- 42.Imai A., Takamizawa T., Sai K., Tsujimoto A., Nojiri K., Endo H., et al. Influence of application method on surface free-energy and bond strength of universal adhesive systems to enamel. Eur J Oral Sci. 2017;125:385–395. doi: 10.1111/eos.12361. [DOI] [PubMed] [Google Scholar]
- 43.Irmak Ö., Yaman B.C., Orhan E.O., Ozer F., Blatz M.B. Effect of rubbing force magnitude on bond strength of universal adhesives applied in self-etch mode. Dent Mater J. 2018;37:139–145. doi: 10.4012/dmj.2017-018. [DOI] [PubMed] [Google Scholar]
- 44.Jang J.H., Jeon B.K., Mo S.Y., Park M., Choi D., Choi K.K., et al. Effect of various agitation methods on adhesive layer formation of HEMA-free universal dentin adhesive. Dent Mater J. 2019;38:101–106. doi: 10.4012/dmj.2018-031. [DOI] [PubMed] [Google Scholar]
- 45.Loguercio A.D., Stanislawczuk R., Mena-Serrano A., Reis A. Effect of 3-year water storage on the performance of one-step self-etch adhesives applied actively on dentine. J Dent. 2011;39:578–587. doi: 10.1016/j.jdent.2011.06.005. [DOI] [PubMed] [Google Scholar]
- 46.Loguercio A.D., Muñoz M.A., Luque-Martinez I., Hass V., Reis A., Perdigão J. Does active application of universal adhesives to enamel in self-etch mode improve their performance? J Dent. 2015;43:1060–1070. doi: 10.1016/j.jdent.2015.04.005. [DOI] [PubMed] [Google Scholar]
- 47.Manhães L., Oliveira D.C., Marques M.M., Matos A.B. Influence of Er:YAG laser surface treatment and primer application methods on microtensile bond strength self-etching systems. Photo Laser Surg. 2005;23:304–312. doi: 10.1089/pho.2005.23.304. [DOI] [PubMed] [Google Scholar]
- 48.Moritake N., Takamizawa T., Ishii R., Tsujimoto A., Barkmeier W.W., Latta M.A., et al. Effect of active application on bond durability of universal adhesives. Oper Dent. 2019;44:188–199. doi: 10.2341/17-384-L. [DOI] [PubMed] [Google Scholar]
- 49.Pleffken P.R., de Almeida Lourenço A.P., Torres C.R., Bühler Borges A. Influence of application methods of self-etching adhesive systems on adhesive bond strength to dentin. J Adhes Dent. 2011;13:517–525. doi: 10.3290/j.jad.a21417. [DOI] [PubMed] [Google Scholar]
- 50.Prasansuttiporn T., Nakajima M., Foxton R.M., Tagami J. Scrubbing effect of self-etching adhesives on bond strength to NaOCl-treated dentin. J Adhes Dent. 2012;14:121–127. doi: 10.3290/j.jad.a22340. [DOI] [PubMed] [Google Scholar]
- 51.Saikaew P., Chowdhury A., Sattabanasuk V., Srimaneekarn N., Teanchai C., Carvalho R.M., et al. Bonding performance of self-etching adhesives to bur-cut dentin with active application mode. J Adhes Dent. 2021;23:357–365. doi: 10.3290/j.jad.b1645379. [DOI] [PubMed] [Google Scholar]
- 52.Serin-Kalay T., Zaim B. Effect of alternative self-etch applications on dentin bond strength of “No Wait Concept” universal adhesives. Odovtos. 2022;24:58–66. doi: 10.15517/ijds.2021.45844. [DOI] [Google Scholar]
- 53.Thanatvarakorn O., Prasansuttiporn T., Takahashi M., Thittaweerat S., Foxton R.M., Ichinose S., et al. Effect of scrubbing technique with mild self-etching adhesives on dentin bond strengths and nanoleakage expression. J Adhes Dent. 2016;18:197–204. doi: 10.3290/j.jad.a36033. [DOI] [PubMed] [Google Scholar]
- 54.Torres C.R.G., Caneppele T.M.F., Borges A.B., Shoji A.V., Nunes T.M., Batista G.R. Effects of surface hydration and application method on the bond strength of self-etching adhesives to dentin. J Adhes. 2011;87:1099–1111. doi: 10.1080/00218464.2011.609452. [DOI] [Google Scholar]
- 55.Zaki Z.M., Nagi S.M., Mohamed A.A., Zaazou M.H., El-Din I.M. Effect of different application techniques on microshear bond strength of self-etch adhesives to dentin. J Adhes Sci Technol. 2016;30:2044–2059. doi: 10.1080/01694243.2016.1175253. [DOI] [Google Scholar]
- 56.Zander-Grande C., Amaral R.C., Loguercio A.D., Barroso L.P., Reis A. Clinical performance of one-step self-etch adhesives applied actively in cervical lesions: 24-month clinical trial. Oper Dent. 2014;39(3):228–238. doi: 10.2341/12-286-C. [DOI] [PubMed] [Google Scholar]
- 57.Cehreli S.B., Eminkahyagil N. Effect of active pretreatment of self-etching primers on the ultramorphology of intact primary and permanent tooth enamel. J Dent Child. 2006;73:86–90. [PubMed] [Google Scholar]
- 58.Kubo S., Yokota H., Yokota H., Hayashi Y. Two-year clinical evaluation of one-step self-etch systems in non-carious cervical lesions. J Dent. 2009;37:149–155. doi: 10.1016/j.jdent.2008.10.008. [DOI] [PubMed] [Google Scholar]