Abstract
Background and Purpose
Obesity, a risk factor for obstructive sleep apnea (OSA), is usually estimated by body mass index (BMI). However, other adiposity-estimating equations may better capture variations in fat distribution. This study assessed the relationship between OSA severity and 15 adiposity-estimating equations, compared to BMI, with subgroup analyses by sex and age (<50 vs ≥50).
Patients and Methods
We conducted a cross-sectional cohort study using data from 5021 consecutive adults who underwent a Level 1 polysomnography (2015–2017) in a large academic sleep center in Ottawa, Canada. We assessed correlations between adiposity measures and the apnea–hypopnea index (AHI) and examined discriminative ability for moderate-to-severe (AHI ≥15/h) and severe OSA (AHI >30/h) using univariate logistic regressions.
Results
The mean age was 49.5 years, 46.6% were women; the mean BMI was 30.0 kg/m2 and 12.7% had severe OSA. All adiposity equations showed negligible (Pearson r 0.0 to ±0.3) to low (Pearson r ± 0.30 to 0.50) statistically significant correlations with AHI, with many of the equations having a marginally stronger correlation coefficient than BMI, in total and subgroup analysis. Discriminative ability for severe OSA was generally low, with c-indices ranging from 0.52 to 0.67 in the overall sample. However, in females under 50, several equations (eg, Gallagher 2000, Deurenberg 1991 and 1998, ECORE BF) reached excellent discriminative ability (c-indices 0.81), including BMI (c-index 0.80). This pattern was not observed in other subgroups.
Conclusion
In this clinical cohort, BMI was associated poorly with AHI; however, the other equations did not outperform BMI. Moreover, BMI demonstrated poor discriminative ability for moderate/severe and severe OSA, with none of the other equations performing better in this context. Notable subgroup differences—particularly among younger females—suggest that tailoring screening strategies by age and sex may improve risk stratification and support refining obesity-based screening approaches.
Keywords: obstructive sleep apnea, body mass index, adiposity, equations, apnea–hypopnea index, discriminative ability, sex and age stratification
Introduction
Recurring obstructive episodes of the upper airway characterised by apneas and hypopneas describe obstructive sleep apnea (OSA).1 The prevalence of OSA varies by age, sex, and country, with an estimated global prevalence for adults aged 30–69 at 936 million.2 Early screening and diagnosis are important, given the association of untreated OSA with various adverse health outcomes, including reduced executive function3 and increased motor vehicle accidents.4 Recent studies highlight the need for improved screening tools to enhance OSA early detection, especially in primary care settings.5,6
Among the various risk factors for OSA considered in screening tools, obesity is one of the most important.7 In 2016, the World Health Organization estimated that 650 million adults worldwide were obese.8 Adiposity status is incorporated in several clinical screening tools for OSA, including the STOP-BANG questionnaire,9 the Berlin questionnaire,10 the NoSAS11 and the BOAH scores,12 which use BMI to measure obesity, given its simplistic formula.8 However, all questionnaires rely on BMI, height, and weight, with no central obesity measures (eg, waist circumference) included.
Many studies estimate the relationship between obesity and OSA by utilizing BMI; some studies have found a positive correlation between BMI and AHI,13 while others have found no relationship.14 However, when compared to technologies including dual x-ray absorptiometry, a gold standard for body composition, BMI has been shown to misclassify adiposity status in a significant portion of individuals.15,16 While other technologies are valuable tools in measuring body fat,17 at a population level, they are not cost nor time effective options. Therefore, efforts have been made to develop novel equations using anthropometric data which are more strongly associated with true adiposity when compared to BMI.18 A study by Krachler et al explored the relationship between multiple anthropometric-derived equations and various cardiovascular risk factors.19 Two new equations, the Equation Córdoba for Estimation of Body Fat (ECORE-BF) and the Clínica Universidad de Navarra-Body Adiposity Estimator (CUN-BAE), have been developed to aid in estimating body fat.20–22
Little is known regarding these equations and their relationship with OSA prevalence and severity. Therefore, our research objective was to investigate correlations between different measures of obesity and markers of OSA presence and severity. We hypothesized stronger correlations between many of these novel adiposity equations and OSA presence/severity when compared to BMI. We also hypothesized that the relationship between different measures of obesity and OSA presence and severity varies by sex and age because of sex differences in fat distribution7 and age-related changes in body composition.23 In addition, postmenopausal changes and hormonal shifts in women may increase susceptibility to OSA. As such, stratified analysis by sex and age groups may improve prediction models and clinical risk stratification.
Materials and Methods
Study Design
We conducted a cross-sectional clinical cohort study using a database of consecutive adults (18 years and older) who underwent a diagnostic sleep study (Level 1 polysomnography [PSG]) between 2015 and 2017 in a large academic clinical center (Ottawa, Ontario, Canada). Ethics approval was completed through the Ottawa Health Science Network Research Ethics Board (OHSN-REB) (Protocol ID: 20210473-01H). Informed consent from the study participants for this specific study was not obtained. This study uses a database based on routinely collected de-identified clinical data registered and approved by the OHSN-REB. This study is a minimal-risk, meta-analysis, non-interventional, retrospective study that does not require enrollment or any sort of patient participation/contact and does not require any personally identifiable information. Patient confidentiality was upheld during the analysis and review of medical records, as only de-identified data was used in this study. The OHSN-REB abides by all applicable regulations and guidelines pertaining to human participant protection; these include, but are not limited to the Food and Drugs Act and applicable Regulations, the International Council on Harmonization Good Clinical Practice Guidelines, the Declaration of Helsinki: Ethical Principles for Medical Research Involving Human Subjects, the Tri-Council Policy Statement: Ethical Conduct for Research Involving Humans, and where applicable, US Federal Regulations (more details can be found at: https://www.ohri.ca/ohsn-reb/procedures.htm).
Data Source
The Ottawa Hospital Sleep database (NCT03834792) is a clinical database consisting of clinical and polysomnographic variables, including demographics, self-reported symptoms, medical history, and PSG indices. Each patient in the cohort underwent a full in-laboratory PSG recording that was scored by a sleep technologist and reviewed by a sleep physician. Height and weight were measured and recorded by a sleep technologist on the night of the sleep study. Details on the database are described elsewhere.24
PSG Indices Considered
Apnea index, apnea–hypopnea index (AHI), mean and minimum oxygen saturation in sleep, and percentage of sleep with an oxygen saturation of less than 88%. Where applicable, indices were quantified for position (ie, supine versus non-supine) and rapid eye movement (REM)/non-rapid eye movement (NREM) sleep. The sleep software used was Sandman 10.1, and event scoring was in accordance with the AASM (American Academy of Sleep Medicine) criteria 2012.25 The definition of hypopnea was as follows: ≥30% decrease in flow from baseline with an associated oxygen desaturation of ≥3% OR an associated arousal. AHI of 5–15, 15–30, and >30 were classified as mild, moderate, and severe OSA, respectively.
Adiposity-Estimating Equations
Fifteen equations, in addition to BMI, were selected based on data availability and a comprehensive literature review. The equations were as follows: the Rohrer index,26 University of Navarra Clinic-Body Fat Estimator (CUN-BAE) index,22 Equation Córdoba for Estimation of Body Fat (ECORE-BF),20 Body surface index (BSI), Normalized weight-adjusted index (NWAI),27 and equations by Larrson,28 Heo,29 Heitmann,30 Visser,31 Noppa,32 Gallagher (199633 and 200034) and Deurenberg (1989,35 1991,36 and 1998). 37 All equations are described in Table 1.
Table 1.
Adiposity Estimating Equations
| Name of Equation/Anthropometric Measurement | Equation/ Units |
|---|---|
| Body Mass Index (BMI) | Weight (kg)/ [height (m)]2 |
| Rohrer index | Weight (kg)/ [height (m)]3 |
| Equation by Larsson et al | Female: BF%= [−24.18 + 1.181 x (weight (kg) / height (m))] / weight (kg) x 100% |
| Male: BF%= [−30.84 + 1.120 x (weight (kg) /height (m))] / weight (kg) x 100% | |
| Equation by Gallagher et al (2000) | BF%= 64.5–848 x (1/BMI) + 0.079 x age (yrs) −16.4 x sex* + 0.05 x sex x age (yrs) + 39.0 x sex x (1/BMI) |
| Equation by Deurenberg et al (1991) | BF%= 1.2 x BMI + 0.23 x age (yrs) −10.8 x sex* − 5.4 |
| University of Navarra Clinic-Body Fat Estimator (CUN-BAE) index | BF%=−44.988+(0.503×age (yrs)) + (10.689×sex#)+(3.172×BMI) − (0.026×BMI2) + (0.181×BMI×sex) − (0.02×BMI×age (yrs)) − (0.005×BMI2×sex)+(0.00021×BMI2×age (yrs)) |
| Equation Córdoba for Estimation of Body Fat (ECORE-BF) | BF%=−97.102 + (0.123 x age (yrs)) + (11.900 x sex#) + (35.959 x (LnBMI)) |
| Body Surface Index (BSI) | BSI = Weight (kg) / √ BSA |
| BSA: weight (kg)0.425 x height (cm)0.725 x 0.007184 | |
| Normalized weight-adjusted index (NWAI) | [(weight (kg)/10) – (10 x height (m)) + 10] |
| Equation by Deurenberg et al (1998) | BF% = 1.294 x BMI + 0.20 x age (yrs) – 11.4 x sex* – 8.0 |
| Equation by Heo et al (2013) | Female: BF%= [−17.6 + 1.72 x (weight (kg)/height (m)2)]/ weight (kg) x 100% |
| Male: BF%= [−24.0 + 1.77 x (weight (kg)/height (m)2)]/ weight (kg) x 100% | |
| Equation by Heitmann et al (1990) | Female: BF% = [0.988 x BMI + 0.344 x weight (kg) + 0.094 x age (yrs) – 30.180]/weight (kg) x 100% |
| Male: BF% = [0.988 x BMI + 0.242 x weight (kg) + 0.094 x age (yrs) – 30.180]/weight (kg) x 100% | |
| Equation by Gallagher et al (1996) | BF% = 1.46 x BMI + 0.12 x age (yrs) – 11.61 x sex* – 10.02 |
| Equation by Visser et al (1994) (uses Siri’s equation for BF%) | BD = 0.0226 x sex* – 0.0022 x BMI + 1.0605 |
| BF% = (4.95/BD – 4.50) x 100% | |
| Equation by Noppa et al (1979) | BF% = [1.52 x BMI – 17.8]/weight (kg) x 100% |
| Equation by Deurenberg et al (1989) | Female: BF% = 0.672 x BMI + 26.6 |
| Male: BF% = 0.835 x BMI + 10.2 |
Notes: *Sex = 1 for males, 0 for females. #Sex = 0 for male, 1 for female.
Abbreviations: BD, body density; BF%, body fat percentage; BMI, body mass index; BSA, body surface area; BSI, body surface index.
Analyses: Descriptive statistics were used to characterize the cohort. We used Pearson correlations with 95% confidence intervals to assess the relationship between measures of OSA severity and adiposity estimating equations/anthropometric data listed above. A Pearson correlation coefficient of ±0.90 to 1.00 was interpreted as a very high correlation, ± 0.70 to 0.90 as a high correlation, ± 0.50 to 0.70 as a moderate correlation, ± 0.30 to 0.50 as low correlation and 0.0 to ±0.30 as a negligible correlation.38,39 Logistic regressions were used to assess the relationship and quantify the discriminative ability of various adiposity equations and the presence of moderate/severe (AHI>15) or severe OSA (AHI>30). The estimates, odds ratios (OR) and 95% confidence intervals (CIs), were standardized to report the effect per interquartile range (IQR)¸ comparing the 75th to 25th percentile. The discriminative ability was assessed using the c-statistic.40 The c-statistic value ranges from 0.5 to 1 with a value of 0.7–0.8, 0.8–0.9, and >0.9 interpreted as acceptable, excellent, and outstanding discrimination, respectively.41
Secondary analysis: To understand the effect of sex and age on the relationship between measures of OSA and obesity, given the importance of these variables on body composition,42 we repeated all analyses described above stratified by sex and age (<50 vs ≥50 as based on the median age distribution in the cohort). The age of 50 years is also often considered a clinically important cutoff due to several physiological (eg, close to the average age of menopause 43), epidemiological factors (eg, increased prevalence of moderate to severe OSA 44 and associated increased cardiovascular risk).45
The number of missing data for AHI, used to define OSA severity, ranged from 128 (2.5% for BMI) to 131 (2.6% for Heo and Heitmann equations). Since complete case analysis is considered reasonable and unlikely to introduce significant bias when missing data is below 5%,46 we proceeded with complete case analysis.
Results
Descriptive Data
The descriptive data in the total cohort and by subgroups are shown in Table 2 and Supplementary Table 1. Of 5021 adult individuals included in the current analysis, 2679 (53.4%) were male, and 2569 (51.2%) were 50 years and older. The mean age was 49.5 years (SD of 14.9), while the mean BMI and AHI were 30.0 kg/m2 (SD of 6.7) and 13.8/hr (SD of 15.79), respectively. The percentage of individuals with an AHI of <5, 5–15, 15–30, and >30 were 36.0% (1807), 31.5% (1581), 19.9% (997), and 12.7% (636), respectively.
Table 2.
Anthropometric and Polysomnographic Variables for the Study Population: Total and by Sex and Age Subgroups
| Variable | Total | Male | Female | Age <50 | Age > 50 | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| N | Mean | SD | N | Mean | SD | N | Mean | SD | N | Mean | SD | N | Mean | SD | ||||||
| Age (years) | 5021 | 49.5 | ± | 14.9 | 2679 | 49.5 | ± | 14.9 | 2341 | 49.5 | ± | 14.8 | 2452 | 37.0 | ± | 8.3 | 2569 | 61.4 | ± | 8.8 |
| Weight (kg) | 4892 | 87.4 | ± | 21.1 | 2612 | 92.5 | ± | 19.4 | 2279 | 81.6 | ± | 21.4 | 2403 | 89.3 | ± | 22.9 | 2489 | 85.7 | ± | 19.0 |
| Height (cm) | 4894 | 170.5 | ± | 10.1 | 2612 | 176.9 | ± | 7.6 | 2281 | 163.3 | ± | 7.4 | 2404 | 171.8 | ± | 10.0 | 2490 | 169.3 | ± | 10.1 |
| BMI (kg/m2) | 4893 | 30.0 | ± | 6.7 | 2612 | 29.5 | ± | 5.7 | 2280 | 30.6 | ± | 7.7 | 2403 | 30.2 | ± | 7.2 | 2490 | 29.9 | ± | 6.3 |
| ESS | 4983 | 8.4 | ± | 4.7 | 2659 | 8.2 | ± | 4.6 | 2323 | 8.7 | ± | 4.9 | 2435 | 8.9 | ± | 4.7 | 2548 | 7.9 | ± | 4.7 |
| PSG indices | ||||||||||||||||||||
| Apnea Index (events/hr) | 5021 | 3.1 | ± | 7.5 | 2679 | 4.1 | ± | 8.9 | 2341 | 2.0 | ± | 5.2 | 2452 | 2.3 | ± | 6.8 | 2569 | 3.9 | ± | 8.0 |
| AHI (events/hr) | 5021 | 13.8 | ± | 15.8 | 2679 | 16.5 | ± | 16.9 | 2341 | 10.8 | ± | 13.8 | 2452 | 10.9 | ± | 14.6 | 2569 | 16.7 | ± | 16.3 |
| Min. wake SaO2 (%) | 5018 | 75.7 | ± | 29.2 | 2677 | 75.3 | ± | 29.2 | 2340 | 76.2 | ± | 29.2 | 2452 | 77.7 | ± | 28.8 | 2566 | 73.9 | ± | 29.5 |
| Sleep with SaO2 < 88% (%) | 5021 | 1.5 | ± | 7.8 | 2679 | 1.5 | ± | 7.5 | 2341 | 1.5 | ± | 8.2 | 2452 | 0.9 | ± | 6.3 | 2569 | 2.2 | ± | 9.0 |
| Mean Sleep SaO2 (%) | 5020 | 94.8 | ± | 2.0 | 2678 | 94.7 | ± | 1.9 | 2341 | 95.0 | ± | 2.1 | 2451 | 95.5 | ± | 1.7 | 2569 | 94.1 | ± | 2.1 |
| Min Sleep SaO2 (%) | 5019 | 83.3 | ± | 17.6 | 2677 | 82.4 | ± | 18.2 | 2341 | 84.2 | ± | 16.8 | 2451 | 84.3 | ± | 18.6 | 2568 | 82.3 | ± | 16.4 |
| Adiposity-Estimating Equations | ||||||||||||||||||||
| Rohrer index | 4891 | 17.7 | ± | 4.3 | 2611 | 16.7 | ± | 3.3 | 2279 | 18.8 | ± | 4.9 | 2403 | 17.6 | ± | 4.5 | 2488 | 17.8 | ± | 4.1 |
| Larrson | 4890 | 34.4 | ± | 9.2 | 2611 | 28.7 | ± | 6.2 | 2279 | 40.9 | ± | 7.6 | 2403 | 34.3 | ± | 9.3 | 2487 | 34.6 | ± | 9.1 |
| Gallagher 2000 | 4892 | 32.2 | ± | 9.0 | 2612 | 26.1 | ± | 5.4 | 2280 | 39.0 | ± | 7.1 | 2403 | 30.7 | ± | 9.3 | 2489 | 33.6 | ± | 8.4 |
| Deurenberg 1991 | 4892 | 36.2 | ± | 10.6 | 2612 | 30.6 | ± | 7.5 | 2280 | 42.7 | ± | 9.8 | 2403 | 33.5 | ± | 10.8 | 2489 | 38.9 | ± | 9.6 |
| CUN BAE | 4892 | 35.9 | ± | 9.6 | 2612 | 30.2 | ± | 6.9 | 2280 | 42.4 | ± | 7.9 | 2403 | 34.5 | ± | 10.2 | 2489 | 37.2 | ± | 8.7 |
| ECORE BF | 4892 | 36.0 | ± | 10.1 | 2612 | 30.1 | ± | 6.8 | 2280 | 42.8 | ± | 8.9 | 2403 | 34.5 | ± | 10.4 | 2489 | 37.5 | ± | 9.6 |
| BSI | 4891 | 61.6 | ± | 11.1 | 2611 | 63.6 | ± | 10.0 | 2279 | 59.2 | ± | 11.9 | 2403 | 62.4 | ± | 12.1 | 2488 | 60.8 | ± | 10.1 |
| NWAI | 4891 | 1.7 | ± | 1.9 | 2611 | 1.6 | ± | 1.8 | 2279 | 1.8 | ± | 2.1 | 2403 | 1.7 | ± | 2.1 | 2488 | 1.6 | ± | 1.8 |
| Deurenberg 1998 | 4892 | 34.7 | ± | 11.1 | 2612 | 28.7 | ± | 7.8 | 2280 | 41.5 | ± | 10.4 | 2403 | 32.3 | ± | 11.5 | 2489 | 37.0 | ± | 10.3 |
| Heo | 4890 | 35.5 | ± | 8.8 | 2611 | 29.9 | ± | 5.7 | 2279 | 42.0 | ± | 7.1 | 2403 | 34.9 | ± | 8.6 | 2487 | 36.2 | ± | 8.9 |
| Heitmann | 4890 | 32.5 | ± | 8.9 | 2611 | 27.3 | ± | 5.5 | 2279 | 38.4 | ± | 8.3 | 2403 | 30.8 | ± | 9.1 | 2487 | 34.1 | ± | 8.4 |
| Gallagher 1996 | 4892 | 33.6 | ± | 11.9 | 2612 | 27.4 | ± | 8.4 | 2280 | 40.6 | ± | 11.4 | 2403 | 32.2 | ± | 12.5 | 2489 | 34.9 | ± | 11.2 |
| Visser | 4892 | 42.0 | ± | 9.6 | 2612 | 36.3 | ± | 6.1 | 2280 | 48.6 | ± | 8.7 | 2403 | 42.1 | ± | 10.0 | 2489 | 41.9 | ± | 9.2 |
| Noppa | 4891 | 31.3 | ± | 6.3 | 2611 | 28.8 | ± | 4.5 | 2279 | 34.2 | ± | 6.7 | 2403 | 30.8 | ± | 6.2 | 2488 | 31.8 | ± | 6.3 |
| Deurenberg 1989 | 4892 | 40.6 | ± | 7.9 | 2612 | 34.9 | ± | 4.8 | 2280 | 47.2 | ± | 5.2 | 2403 | 40.6 | ± | 8.1 | 2489 | 40.6 | ± | 7.7 |
Note: Data presented as means and standard deviations.
Abbreviations: AHI, apnea-hypopnea index; BMI, body mass index; ESS, Epworth Sleepiness Scale; PSG, polysomnography; SaO2, oxygen saturation.
Correlative Analysis
Table 3 shows Pearson correlations between adiposity estimating equations and indices derived from the PSG in the total cohort. All adiposity equations showed a statistically significant positive association with AHI ranging from 0.05 (Deurenberg 1989) to 0.31 (BSI). Most correlations were negligible (0.0 to ±0.3); however, BSI and NWAI were consistent with low correlations (± 0.30 to 0.50). Notably, BMI had a correlation coefficient of 0.29. Moreover, all equations were negatively associated with mean oxygen saturation in sleep. Correlation coefficients ranged from –0.11 (Deurenberg 1989) to –0.30 (Deurenberg 1991), thus negligible, but approaching low correlations. BMI had a correlation coefficient of −0.27. Similar findings, approaching low, but statistically significant, correlations were evident for other respiratory-related PSG variables (Table 3).
Table 3.
Pearson Correlations Between Sleep-Related Breathing Polysomnography Parameters and Adiposity Estimating Equations for the Total Cohort
| Variables | BMI | Rohrer index | Larrson | Gallagher 2000 |
| Apnea Index | 0.07 (0.04–0.10) | 0.05 (0.03–0.08) | −0.03 (−0.06–0.00) | −0.02 (−0.05–0.01) |
| AHI | 0.29 (0.26–0.31) | 0.25 (0.22–0.27) | 0.10 (0.07–0.13) | 0.11 (0.08–0.14) |
| Supine AHI | 0.22 (0.19–0.25) | 0.17 (0.14–0.20) | 0.03 (0.00–0.06) | 0.04 (0.01–0.07) |
| Non-Supine AHI | 0.33 (0.30–0.36) | 0.30 (0.27–0.32) | 0.16 (0.13–0.19) | 0.16 (0.13–0.19) |
| REM AHI | 0.39 (0.36–0.41) | 0.37 (0.35–0.40) | 0.26 (0.23–0.29) | 0.27 (0.24–0.30) |
| Non-REM AHI | 0.25 (0.23–0.28) | 0.21 (0.18–0.24) | 0.06 (0.04–0.09) | 0.07 (0.04–0.10) |
| Mean wake SaO2 | −0.15 (−0.18--0.13) | −0.14 (−0.17--0.11) | −0.07 (−0.10--0.04) | −0.10 (−0.13--0.07) |
| % sleep with SaO2 <88% | 0.08 (0.05–0.11) | 0.08 (0.06–0.11) | 0.06 (0.03–0.09) | 0.07 (0.04–0.10) |
| Mean sleep SaO2 | −0.27 (−0.30--0.25) | −0.25 (−0.28--0.23) | −0.16 (−0.19--0.14) | −0.20 (−0.23--0.17) |
| Mean REM SaO2 | −0.29 (−0.31--0.26) | −0.27 (−0.30--0.25) | −0.18 (−0.20--0.15) | −0.21 (−0.24--0.18) |
| Mean non-REM SaO2 | −0.26 (−0.29--0.24) | −0.24 (−0.27--0.22) | −0.15 (−0.18--0.13) | −0.19 (−0.22--0.16) |
| Min Sleep SaO2 | −0.09 (−0.12--0.06) | −0.08 (−0.11--0.05) | −0.04 (−0.07--0.01) | −0.04 (−0.07--0.01) |
| Variables | Deurenberg 1991 | CUN BAE | ECORE BF | BSI |
| Apnea Index | 0.03 (0.00–0.06) | 0.01 (−0.02–0.03) | 0.00 (−0.02–0.03) | 0.09 (0.06–0.12) |
| AHI | 0.20 (0.18–0.23) | 0.16 (0.13–0.18) | 0.16 (0.13–0.19) | 0.31 (0.28–0.33) |
| Supine AHI | 0.13 (0.10–0.16) | 0.09 (0.06–0.12) | 0.08 (0.05–0.11) | 0.27 (0.24–0.30) |
| Non-Supine AHI | 0.25 (0.23–0.28) | 0.21 (0.18–0.24) | 0.21 (0.19–0.24) | 0.33 (0.31–0.36) |
| REM AHI | 0.35 (0.33–0.38) | 0.31 (0.28–0.34) | 0.32 (0.29–0.34) | 0.36 (0.33–0.38) |
| Non-REM AHI | 0.16 (0.14–0.19) | 0.12 (0.09–0.15) | 0.12 (0.09–0.15) | 0.28 (0.26–0.31) |
| Mean wake SaO2 | −0.17 (−0.20--0.14) | −0.12 (−0.15--0.09) | −0.13 (−0.15--0.10) | −0.16 (−0.18--0.13) |
| % sleep with SaO2 <88% | 0.09 (0.07–0.12) | 0.07 (0.05–0.10) | 0.08 (0.05–0.11) | 0.06 (0.04–0.09) |
| Mean sleep SaO2 | −0.30 (−0.32--0.27) | −0.23 (−0.26--0.20) | −0.24 (−0.27--0.21) | −0.27 (−0.29--0.24) |
| Mean REM SaO2 | −0.31 (−0.34--0.28) | −0.24 (−0.27--0.21) | −0.25 (−0.28--0.22) | −0.27 (−0.29--0.24) |
| Mean non-REM SaO2 | −0.28 (−0.31--0.26) | −0.22 (−0.25--0.19) | −0.23 (−0.25--0.20) | −0.26 (−0.29--0.24) |
| Min Sleep SaO2 | −0.06 (−0.09--0.03) | −0.05 (−0.08--0.02) | −0.05 (−0.08--0.02) | −0.10 (−0.13--0.07) |
| Variables | NWAI | Deurenberg 1998 | Heo | Heitmann |
| Apnea Index | 0.08 (0.05–0.11) | 0.03 (0.00–0.05) | −0.02 (−0.05–0.00) | 0.00 (−0.02–0.03) |
| AHI | 0.30 (0.27–0.32) | 0.20 (0.17–0.22) | 0.08 (0.05–0.10) | 0.15 (0.12–0.18) |
| Supine AHI | 0.23 (0.20–0.26) | 0.12 (0.09–0.15) | 0.00 (−0.03–0.03) | 0.08 (0.05–0.11) |
| Non-Supine AHI | 0.34 (0.31–0.36) | 0.25 (0.22–0.27) | 0.13 (0.10–0.16) | 0.20 (0.17–0.23) |
| REM AHI | 0.39 (0.36–0.41) | 0.35 (0.32–0.37) | 0.23 (0.20–0.26) | 0.31 (0.28–0.34) |
| Non-REM AHI | 0.26 (0.24–0.29) | 0.16 (0.13–0.18) | 0.04 (0.01–0.07) | 0.11 (0.08–0.14) |
| Mean wake SaO2 | −0.15 (−0.18--0.13) | −0.15 (−0.18--0.13) | −0.06 (−0.09--0.04) | −0.13 (−0.16--0.11) |
| % sleep with SaO2 <88% | 0.08 (0.05–0.11) | 0.09 (0.06–0.12) | 0.06 (0.04–0.09) | 0.07 (0.05–0.10) |
| Mean sleep SaO2 | −0.27 (−0.30--0.25) | −0.28 (−0.30--0.25) | −0.14 (−0.17--0.11) | −0.24 (−0.27--0.22) |
| Mean REM SaO2 | −0.29 (−0.31--0.26) | −0.29 (−0.32--0.27) | −0.16 (−0.19--0.13) | −0.25 (−0.28--0.22) |
| Mean non-REM SaO2 | −0.26 (−0.29--0.24) | −0.27 (−0.29--0.24) | −0.13 (−0.16--0.10) | −0.23 (−0.26--0.21) |
| Min Sleep SaO2 | −0.09 (−0.12--0.06) | −0.06 (−0.09--0.03) | −0.02 (−0.05–0.00) | −0.05 (−0.08--0.02) |
| Variables | Gallagher 1996 | Visser | Noppa | Deurenberg 1989 |
| Apnea Index | 0.01 (−0.01–0.04) | −0.03 (−0.05–0.00) | 0.03 (0.00–0.05) | −0.05 (−0.08--0.03) |
| AHI | 0.18 (0.16–0.21) | 0.11 (0.09–0.14) | 0.17 (0.14–0.19) | 0.05 (0.02–0.08) |
| Supine AHI | 0.10 (0.07–0.13) | 0.03 (0.00–0.06) | 0.10 (0.07–0.13) | −0.03 (−0.06–0.00) |
| Non-Supine AHI | 0.24 (0.21–0.27) | 0.18 (0.15–0.21) | 0.21 (0.18–0.24) | 0.12 (0.09–0.15) |
| REM AHI | 0.34 (0.31–0.36) | 0.27 (0.25–0.30) | 0.30 (0.28–0.33) | 0.21 (0.18–0.24) |
| Non-REM AHI | 0.14 (0.12–0.17) | 0.08 (0.05–0.11) | 0.13 (0.10–0.16) | 0.02 (−0.01–0.05) |
| Mean wake SaO2 | −0.13 (−0.15--0.10) | −0.06 (−0.09--0.03) | −0.12 (−0.15--0.09) | −0.03 (−0.05–0.00) |
| % sleep with SaO2 <88% | 0.08 (0.05–0.11) | 0.06 (0.03–0.09) | 0.08 (0.05–0.10) | 0.05 (0.03–0.08) |
| Mean sleep SaO2 | −0.25 (−0.27--0.22) | −0.16 (−0.19--0.13) | −0.21 (−0.23--0.18) | −0.11 (−0.14--0.09) |
| Mean REM SaO2 | −0.26 (−0.29--0.24) | −0.19 (−0.21--0.16) | −0.22 (−0.25--0.19) | −0.14 (−0.17--0.11) |
| Mean non-REM SaO2 | −0.23 (−0.26--0.21) | −0.15 (−0.18--0.12) | −0.20 (−0.22--0.17) | −0.10 (−0.13--0.07) |
| Min Sleep SaO2 | −0.06 (−0.09--0.03) | −0.04 (−0.07--0.01) | −0.05 (−0.08--0.02) | −0.02 (−0.05–0.00) |
Notes: Estimates are presented as correlation coefficients (r) and 95% confidence intervals.
Abbreviations: AHI, apnea-hypopnea index; SaO2, oxygen saturation.
Logistic Regression and Receiver Operating Characteristic (ROC) Curves
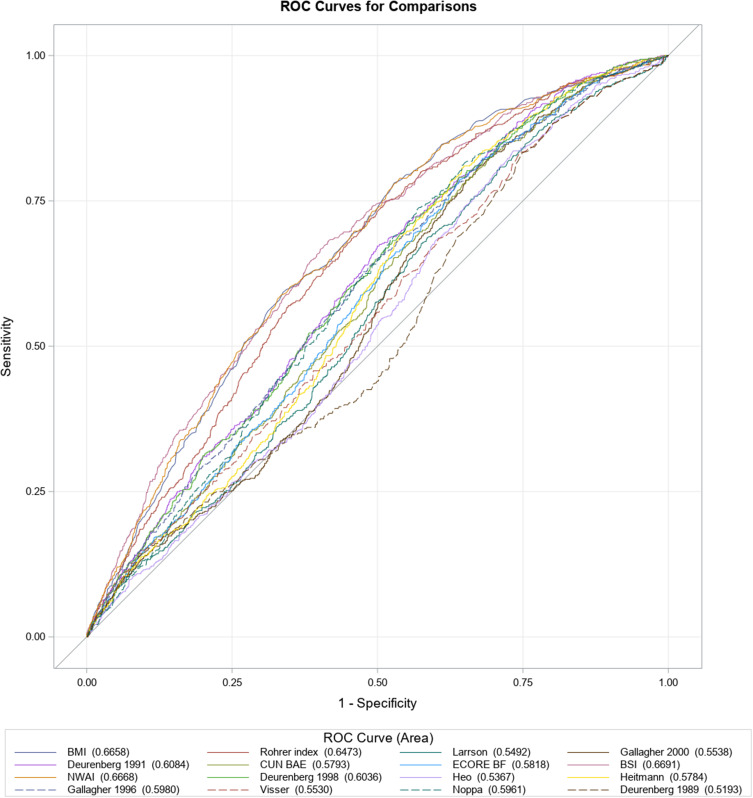
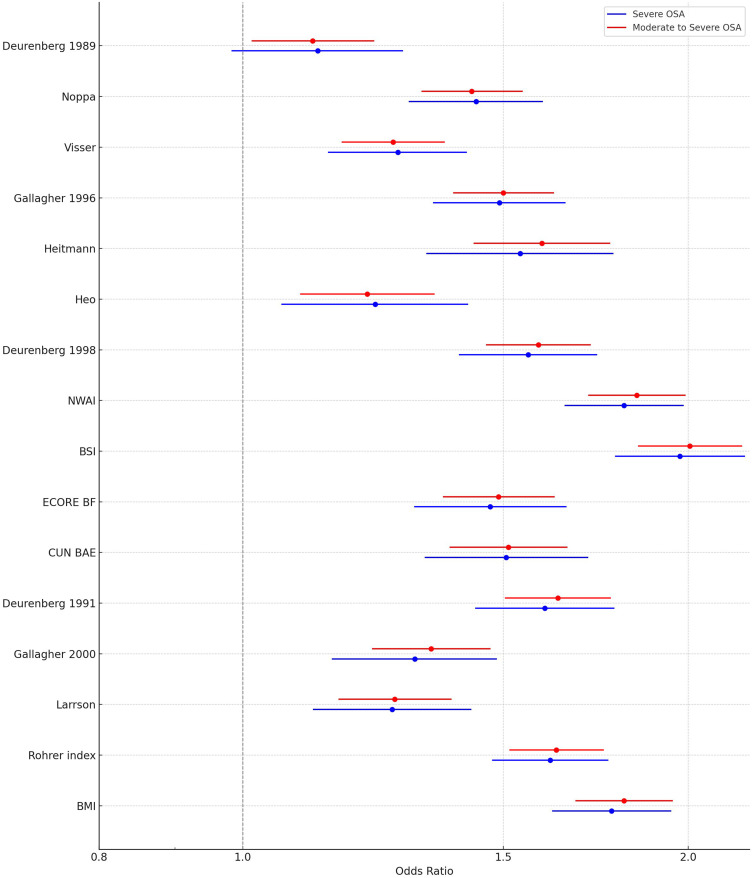
Figures 1–3 and Supplementary Table 2 present ROC curve analyses and ORs with 95% CIs and c-statistics from logistic regressions for the total cohort. The odds of being diagnosed with severe OSA associated with an IQR increase in obesity measures ranged from 1.12 to 1.97, with the highest odds associated with an increase in BSI (Figure 3 and Supplementary Table 2). The c-indices ranged from 0.52 to 0.67, demonstrating a less than acceptable discriminative ability, with BSI, NWAI, and BMI showing the greatest discriminative ability (Figure 1 and Supplementary Table 2). Similar trends were evident regarding moderate/severe OSA (Figure 2 and Supplementary Table 2).
Figure 1.
Receiver operating characteristic (ROC) curve analyses of BMI and 15 adiposity-estimating equations in discrimination of individuals with severe obstructive sleep apnea (OSA) versus not in the total study population.
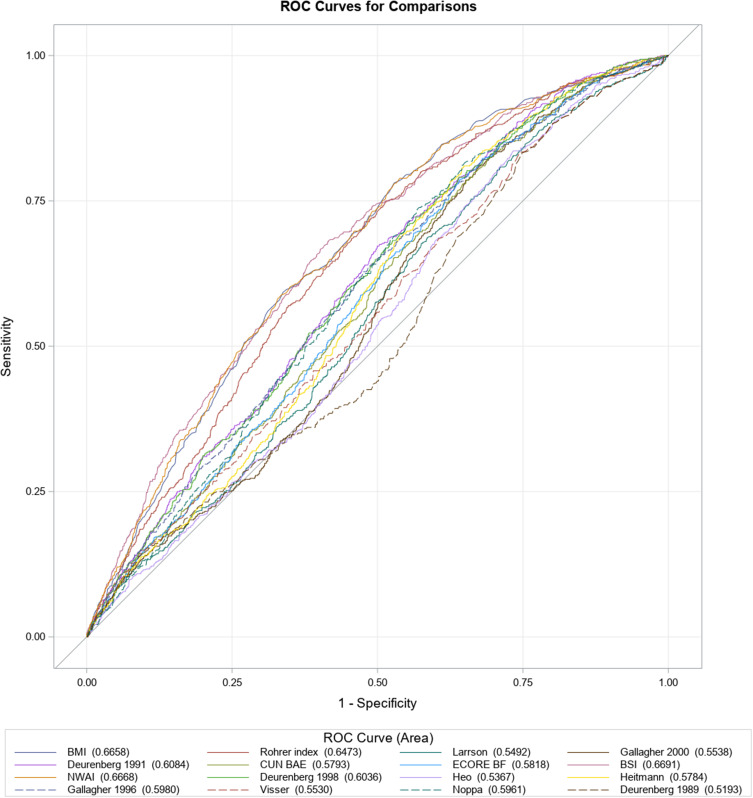
Figure 2.
Receiver operating characteristic (ROC) curve analyses of BMI and 15 adiposity-estimating equations in discrimination of individuals with moderate to severe obstructive sleep apnea (OSA) versus not in the total study population.
Figure 3.
Forest plot of odds ratio (OR) and 95% confidence interval (CI) of the association between BMI and 15 adiposity-estimating equations and severe or moderate to severe obstructive sleep apnea (OSA) for the total study population.
Correlative Analysis Stratified by Sex, Age, and Sex/Age Subgroups
When the cohort was stratified based on sex, age, and both age and sex, similar results were found (Supplementary Tables 3–10). While some adiposity equations had mildly stronger correlation coefficients than BMI, others had minimally weaker correlation coefficients with AHI. Regardless, all associations with AHI were generally negligible to low, with the highest correlation coefficient noted for REM AHI of 0.53 for Deurenberg 1991 and 1998 equation in female younger than 50 years old.
Logistic Regression and ROC Curves Stratified Based on Sex, Age, and Sex/Age Subgroups
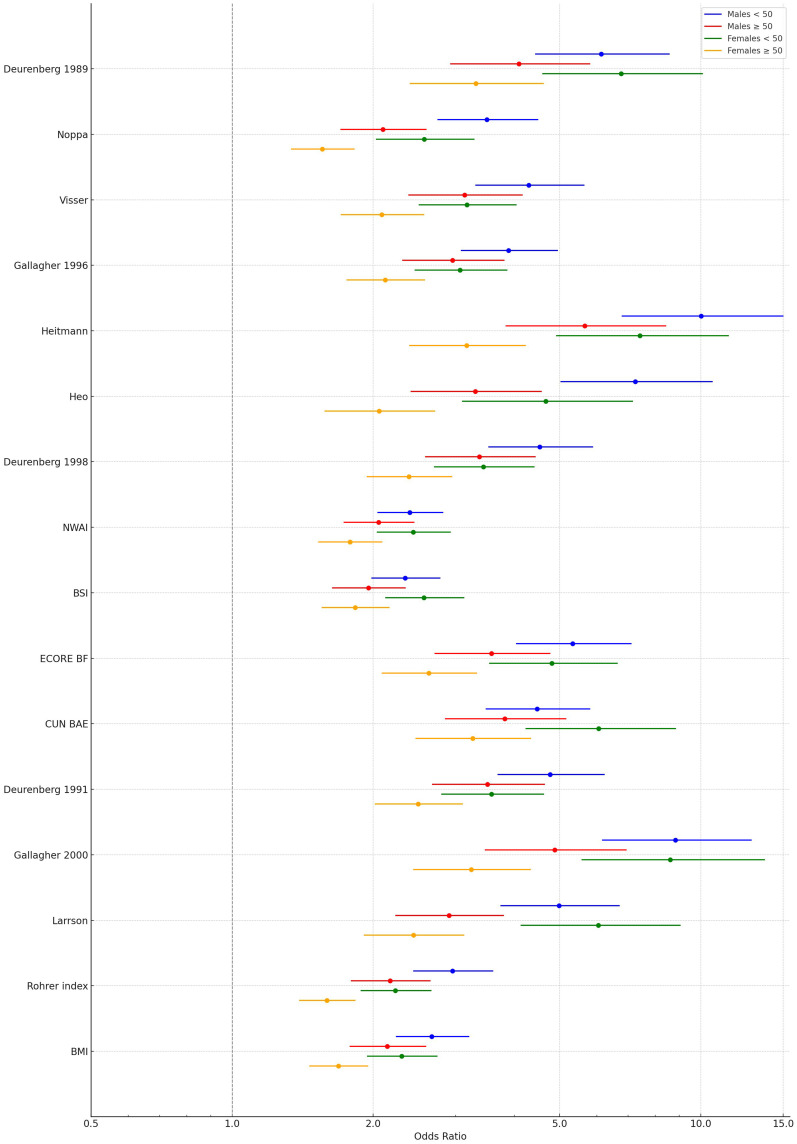
When the cohort was stratified based on sex, age, and both age and sex, similar results were found (Figure 4, Supplementary Tables 11 to 18 and Supplementary Figures 1–8). While some adiposity equations had mildly higher discriminatory ability for severe OSA compared to BMI, others had a minimally weaker discriminatory ability. Regardless, most equations’ discriminatory ability ranged from less than acceptable to acceptable. However, in females younger than 50, c-indices ranged from 0.73 to 0.81, demonstrating acceptable to excellent discriminative ability, with Gallagher 2000, Deurenberg 1991, ECORE BF, Deunrenberg 1998, Heitmann, and Gallagher 1996 all showing the greatest discriminative ability (c-indices of 0.81). However, other equations, including BMI, had c-indices of 0.80, also corresponding with excellent discriminative ability (Supplementary Table 17 and Supplementary Figure 7).
Figure 4.
Forest plot of odds ratio (OR) and 95% confidence interval (CI) of the association between BMI and 15 adiposity-estimating equations and moderate to severe obstructive sleep apnea (OSA) by sex and age subgroups.
Discussion
To our knowledge, this is the first study to comprehensively assess the relationship between the severity of OSA and a particular set of BMI, height, and weight-based adiposity-estimating equations, including the Rohrer index, CUN-BAE index, ECORE-BF, BSI, NWAI, and equations by Larrson, Heo, Heitmann, Visser, Noppa, Gallagher (1996 and 2000) and Deurenberg (1989, 1991, and 1998), compared with BMI. We did not demonstrate stronger correlations between novel adiposity equations and OSA presence/severity compared to BMI, as hypothesized, regardless of stratification. In the total study population, BMI was poorly correlated with AHI, and the other equations did not outperform BMI. Similarly, BMI demonstrates poor discriminative ability for moderate/severe and severe OSA; however, none of the other equations performed better in this context. This study further supports the argument that measures of obesity alone should not be used to discriminate between severe or moderate/severe OSA. Critically, no adiposity-estimating equations outperformed BMI.
In the literature, BMI has taken precedence for estimating obesity due to its ease of calculation. BMI is strongly associated with body fat,47 but can misclassify obesity in a proportion of individuals.15,16,48 Studies have demonstrated a relationship between increasing BMI and OSA13,49 and a similar correlation (r=0.38) between AHI and BMI,13 compared to the current study. Conversely, other studies found no relationship between AHI and BMI, but did note a negative relationship (r=−0.42) between minimum oxygen saturation and BMI,14 which was stronger than in the current study. Notably, for most of the used equations, cut-offs do not exist to qualify someone as underweight, normal weight, overweight, or obese as they do for BMI,8 and thus, estimates per IQR were used in the present study. Further studies are warranted to assess this complex relationship. Importantly, little data exists regarding OSA and obesity defined by the adiposity equations investigated in this study. At the time of the current manuscript preparation, only one study was available; this study showed an increased risk of self-reported sleep-disordered breathing with increasing Rohrer index in primary school students (OR of 1.82; 95% CI: 1.46–2.27; p<0.001).50 However, compared to our study, no objective measures of OSA were used, nor was a comparison to BMI made.
In the current study for females younger than 50, many obesity estimating equations, including BMI, showed an excellent discriminative ability for severe OSA. The differences observed when stratified by sex and age could be explained by variations in body fat percentages and distribution in males vs females,51,52 as women, on average, have more body fat than men53 and, as body fat can increase with age.54 However, equations incorporating sex-specific formulas may have performed poorly as they technically should not be used to assess discriminative ability in the total population, given different distributions for males and females. This assumption was confirmed by the fact that when stratified by age and sex, the discriminative ability for equations was very close (ie, smaller variation than in the total cohort). Furthermore, the relationship between BMI and AHI, as a predictor of OSA, varies between men and women. When assessing the impact of BMI on AHI, mediating factors—characteristics that help explain the relationship between two variables—have been shown to vary by sex. Upper airway mechanics have been additionally shown to be differentially controlled by sex, age, and BMI, and partly mediate the relationship between these risk factors and OSA.55 For example, Nokes et al in the study involved 2146 individuals (43% women), showing that BMI was significantly associated with AHI across both sexes and, at the same time, demonstrated the different AHI-BMI mediating factors between men and women.56 Specifically, while in men, the correlation between BMI and AHI was influenced by reductions in upper airway stiffness, circulatory delay, and an increased arousal threshold, in women, only upper airway stiffness and circulatory delay significantly mediate the BMI-AHI relationship.56 Taking together, these findings suggest the potential value of developing or adapting screening tools that account for sex- and age-related differences in obesity measures and OSA risk. For example, incorporating age- and sex-specific thresholds or weighting different anthropometric measures differently in prediction models could improve early identification of individuals at risk for OSA, particularly in underserved or underdiagnosed populations such as younger women. This approach may be especially relevant in specific settings, such as population-level screening, where access to full diagnostic testing is limited. However, given the exploratory nature of these stratified analyses and the potential for type I error due to multiple comparisons, these findings should be considered hypothesis-generating and require validation in external cohorts.
Regarding other metabolic conditions, Kracher et al showed BMI and adiposity estimated by averaging values obtained by Larsson, Gallagher, and Deurenberg (1991 and 1998), had higher discriminatory power when compared to DEXA for cardiometabolic risk markers (1.9% for BMI, 3.7% for adiposity-estimating equations p<0.01).19 Both the Deurenberg 1991 equation and CUN-BAE have also been shown to aid in identifying metabolic syndrome,57 which has been linked to OSA.58 For women, the Deurenberg 1991 equation and CUN-BAE had similar areas under the curve (AUC >0.90 and >0.89, respectively) for predicting metabolic syndrome (depending on the metabolic syndrome model).57 For men, both the Deurenberg and CUN-BAE had AUC values of >0.84 (depending on the metabolic syndrome model).57 In our current paper, it is unclear in the correlative analysis why the Deurenberg 1991 equation seemed to consistently have the highest r-value once the data was stratified; further investigations are required. Notably, the Deurenberg 1991 and other equations take into consideration age, sex, and BMI, which may aid in the performance.
Another obesity measure that could be considered while investigating the relationship between the severity of OSA and obesity is the Body Roundness Index (BRI). While newer, BRI specifically aims to augment the shortcomings of BMI by measuring visceral fat via waist circumference in addition to height and weight, as visceral fat is more closely linked to health risks when compared to overall body weight.59 Zhang et al explore further the relationship between BRI and all-cause mortality in their study of US adults using data from the National Health and Nutrition Examination Survey from 1999 to 2018 (N=32,995 and a median follow-up period of about 10 years).60 This study demonstrated an increasing trend of BRI during a nearly 20-year period, especially in women and elderly individuals, and a U-shaped association between BRI and all-cause mortality,60 suggesting that BRI as a noninvasive screening tool could be incorporated into public health practice, pending validation in future independent studies.
Our study is affected by several limitations. First, single-center cross-sectional study design and using clinical- (vs community) based data may affect the generalizability of our findings and may introduce selection bias. However, it is generalizable to the Canadian population given the current cohort’s median BMI of 28.9 kg/m2 was similar to the average BMI found in the Canadian Primary Care Sentinel Surveillance Network61 of 28.5 kg/m2 in January 2011 and 29.1 kg/m2 in December 2016. Regarding the percentage of severe OSA (12.7% in the current study), various Canadian studies differ regarding the percentage of individuals referred for a sleep study and ultimately diagnosed with severe OSA. For example, two studies, one from Saskatchewan and the other from British Columbia, reported severe OSA incidence of 5.2%62 and 26%,63 respectively. Notably, the Sleep Heart Health Study (5800 participants) had 21% of the population with moderate-severe sleep apnea.64 We also cannot exclude the possibility of measurement bias related to the BMI measurements (clinically routinely collected data) and variability in AHI due to night-to-night fluctuations. Thus, our results are needed to be externally validated, including on community-based cohorts. Another limitation was that only 15 obesity estimating equations were used in the analysis. Many more do exist in the literature,65 but we were limited by the variables accessible in the dataset – we did not have access to some variables required for other calculated equations, such as neck, waist, and hip circumference. Of note, both an increased waist circumference and waist-to-hip ratio have been associated with OSA severity and prevalence.66 Therefore, future studies should incorporate other adiposity estimating equations and imaging techniques,67 specifically focusing on fat distribution, to assess associations with OSA. To support the importance of fat distribution, the study that utilized abdominal magnetic resonance imaging before and after a weight loss intervention demonstrated that improved AHI with weight loss was primarily mediated by tongue fat reductions.68
Furthermore, while it was not in our study's focus, we could not exclude a modifiable effect of OSA endotypic traits on the relationship between adiposity estimating equations and OSA severity.69 For example, obese individuals often exhibit high upper airway collapsibility and poor upper airway compensation due to excess fat deposition around the airway and reduced lung volumes, while in non-obese individuals, OSA is more often driven by high loop gain, low arousal thresholds, or neuromuscular dysfunction rather than airway anatomy.1 OSA endotypic traits could also explain 30% of the relative sex differences in non-REM AHI.70 While exploring the intersection between age and sex, for men, age has been shown to correlate with increased collapsibility, increased loop gain, and decreased arousal threshold, whereas, in women, OSA endotypic traits were not associated with age, except for an increase in loop gain with advancing age.71
Overall, this is the first study to assess the relationship between measures of OSA severity and 15 BMI, height, and weight-based adiposity equations compared to BMI. While some equations had slightly stronger correlations with AHI, most had negligible or low correlations with AHI, regardless of stratification. While the discriminative ability for OSA for most equations was less than acceptable, in females younger than 50, many equations (including BMI) had excellent discriminative ability. These results further support the limitation of both the BMI, as one of the most commonly used measurements in clinics and research, and other evaluated BMI-based measures of adiposity in screening for OSA within clinical guidelines. However, if confirmed in future studies, in females under 50, BMI could serve as a simple screening tool for identifying those at risk for OSA. Future studies are required to both externally validate our findings and to further explore the relationship between other adiposity-estimating equations and OSA. Utilizing multi-parameter screening by combining BMI with measures of fat distribution, such as neck, waist, and hip circumference, demographic characteristics, relevant symptoms and the presence of relevant comorbidities, such as cardiovascular, may provide better discriminative value than using measures of adiposity alone. Advanced statistical methods, including machine learning,72 would also help to improve the discriminative power and personalized screening approach for OSA.
Acknowledgments
We acknowledge the Ottawa Methods Center at the Ottawa Hospital Research Institute for aiding with data analysis. The authors also wish to thank the research assistants at the Ottawa Hospital Research Institute, Moussa Meteb, Aseel Ahmad, and Randa Ahmad, for their role in databases preparation as well as Mouaz Saymeh for his role in the manuscript preparation.
Data Sharing Statement
The dataset from this study is available under REB approval upon reasonable request from the corresponding author.
Author Contributions
DW, GC, SDA, ZWG, JF, and TK were involved in the study conceptualization and methodology. MS, GC, SDA, ZWG, JF, ES, and BY were involved in validation, visualization, and writing (review and editing). DW and TK were also involved in investigation, formal analysis, validation, and writing (original draft). TK was additionally involved in project administration and supervision (of DW) and is a custodian of the TOH Sleep Database (data curation). ES was additionally involved in formal analysis. TK, ES, and DW had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. All co-authors (DW, MS, GC, SDA, ZWG, JF, ES, BY, TK) agreed on the journal to which the article will be submitted, reviewed, and agreed on all versions of the article before submission, during revision, the final version accepted for publication, and any significant changes introduced at the proofing stage, and take responsibility and be accountable for the contents of the article.
Disclosures/Disclosure of Interest
The TOH Sleep Database was created with the support from the Ottawa Hospital Sleep Walk and the University of Ottawa Department of Medicine (DOM) Developmental Research Grant (Ottawa, Ontario, Canada). The analyses, conclusions, opinions, and statements expressed herein are solely those of the authors and do not reflect those of the funding or data sources; no endorsement is intended or should be inferred.
The authors have no conflicts of interest to declare. TK was supported by the PSI Foundation when the project was conducted. Outside of the submitted work, TK projects are supported by the CIHR and CHEST foundations.
The abstract of this paper was presented at the 2022 American Thoracic Society International Conference as a poster presentation with interim findings. The poster’s abstract was published in the American Journal of Respiratory and Critical Care Medicine: https://doi.org/10.1164/ajrccm-conference.2022.205.1_MeetingAbstracts.A2709. Only the abstract was presented at the conference with preliminary results: correlation coefficients only for the total sample without stratifications. Since the abstract was presented, we have performed several additional analyses, including logistic regressions, presenting c-indices, visualizing the discriminative ability and subgroup analyses stratifying by age and sex; this is why additional co-investigators were involved in bringing expertise in the analytic approaches and interpretations of the obtained results.
References
- 1.Eckert DJ, Malhotra A. Pathophysiology of adult obstructive sleep apnea. Proc Am Thorac Soc. 2008;5(2):144–153. doi: 10.1513/pats.200707-114MG [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Benjafield AV, Ayas NT, Eastwood PR, et al. Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med. 2019;7(8):687–698. doi: 10.1016/S2213-2600(19)30198-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Olaithe M, Bucks RS. Executive dysfunction in OSA before and after treatment: a meta-analysis. Sleep. 2013;36(9):1297–1305. doi: 10.5665/sleep.2950 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.George CF. Sleep apnea, alertness, and motor vehicle crashes. Am J Respir Crit Care Med. 2007;176(10):954–956. doi: 10.1164/rccm.200605-629PP [DOI] [PubMed] [Google Scholar]
- 5.Li X, Zha L, Zhou L, et al. Diagnostic utility of obstructive sleep apnea screening questionnaires: a comprehensive meta-analysis. Sleep Breath. 2024;29(1):14. doi: 10.1007/s11325-024-03169-z [DOI] [PubMed] [Google Scholar]
- 6.Feltner C, Wallace IF, Aymes S, et al. Screening for obstructive sleep apnea in adults: updated evidence report and systematic review for the us preventive services task force. JAMA. 2022;328(19):1951–1971. doi: 10.1001/jama.2022.18357 [DOI] [PubMed] [Google Scholar]
- 7.Romero-Corral A, Caples SM, Lopez-Jimenez F, et al. Interactions between obesity and obstructive sleep apnea: implications for treatment. Chest. 2010;137(3):711–719. doi: 10.1378/chest.09-0360 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.WHO. Obesity and overweight. 2021; Available from: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight. Accessed May 7, 2025.
- 9.Mergen H, Altındağ B, Zeren Uçar Z, et al. The predictive performance of the STOP-bang questionnaire in obstructive sleep apnea screening of obese population at sleep clinical setting. Cureus. 2019;11(12):e6498. doi: 10.7759/cureus.6498 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Tan A, Yin JDC, Tan LWL, et al. Using the Berlin Questionnaire to predict obstructive sleep apnea in the general population. J Clin Sleep Med. 2017;13(3):427–432. doi: 10.5664/jcsm.6496 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Guichard K, Marti-Soler H, Micoulaud-Franchi J-A, et al. The NoSAS score: a new and simple screening tool for obstructive sleep apnea syndrome in depressive disorder. J Affect Disord. 2018;227:136–140. doi: 10.1016/j.jad.2017.10.015 [DOI] [PubMed] [Google Scholar]
- 12.da Silva Machado G, Araújo HGS, Corrêa PB, et al. The role of obstructive sleep apnea risk (BOAH Score) in predicting angina: evidence from NHANES 2017–2020. Sleep Science Practice. 2024;8(25). doi: 10.1186/s41606-024-00117-4. [DOI] [Google Scholar]
- 13.Lovin S, Bercea R, Cojocaru C, et al. Body composition in obstructive sleep apneahypopnea syndrome bio-impedance reflects the severity of sleep apnea. Multidiscip Respir Med. 2010;5(1):44–49. doi: 10.1186/2049-6958-5-1-44 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Ciavarella D, Tepedino M, Chimenti C, et al. Correlation between body mass index and obstructive sleep apnea severity indexes - A retrospective study. Am J Otolaryngol. 2018;39(4):388–391. doi: 10.1016/j.amjoto.2018.03.026 [DOI] [PubMed] [Google Scholar]
- 15.Kennedy AP, Shea JL, Sun G. Comparison of the classification of obesity by BMI vs. dual-energy X-ray absorptiometry in the Newfoundland population. Obesity. 2009;17(11):2094–2099. doi: 10.1038/oby.2009.101 [DOI] [PubMed] [Google Scholar]
- 16.Pinheiro A, Filho NS, França AKTDC, et al. Sensitivity and specificity of the body mass index in the diagnosis of obesity in patients with non-dialysis chronic kidney disease: a comparison between gold standard methods and the cut-off value purpose. Nutr Hosp. 2019;36(1):73–79. doi: 10.20960/nh.1880 [DOI] [PubMed] [Google Scholar]
- 17.Wang H, Chen YE, Eitzman DT. Imaging body fat: techniques and cardiometabolic implications. Arterioscler Thromb Vasc Biol. 2014;34(10):2217–2223. doi: 10.1161/ATVBAHA.114.303036 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Sun G, Cahill F, Gulliver W, et al. Concordance of BAI and BMI with DXA in the Newfoundland population. Obesity. 2013;21(3):499–503. doi: 10.1002/oby.20009 [DOI] [PubMed] [Google Scholar]
- 19.Krachler B, Völgyi E, Savonen K, et al. BMI and an anthropometry-based estimate of fat mass percentage are both valid discriminators of cardiometabolic risk: a comparison with DXA and bioimpedance. J Obes. 2013;2013:862514. doi: 10.1155/2013/862514 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Molina-Luque R, Romero-Saldaña M, Álvarez-Fernández C, et al. Equation cordoba: a simplified method for estimation of body fat (ECORE-BF). Int J Environ Res Public Health. 2019;16(22):4529. doi: 10.3390/ijerph16224529 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Molina-Luque R, Yañez AM, Bennasar-Veny M, et al. A comparison of equation cordoba for estimation of body fat (ECORE-BF) with other prediction equations. Int J Environ Res Public Health. 2020;17(21):7940. doi: 10.3390/ijerph17217940 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Ares Blanco J, Valdés Hernández S, Botas Cervero P, et al. Estimation of body fat mass using the CUN-BAE index and mortality risk by sex in the Asturias Study cohort. Endocrinol Diabetes Nutr (Engl. 2019;66(8):487–494. doi: 10.1016/j.endinu.2019.02.008 [DOI] [PubMed] [Google Scholar]
- 23.Malhotra A, Huang Y, Fogel R, et al. Aging influences on pharyngeal anatomy and physiology: the predisposition to pharyngeal collapse. Am J Med. 2006;119(1):72e9–14. doi: 10.1016/j.amjmed.2005.01.077 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Kendzerska T, Povitz M, Leung RS, et al. Obstructive sleep apnea and incident cancer: a large retrospective multicenter clinical cohort study. Cancer Epidemiol Biomarkers Prev. 2021;30(2):295–304. doi: 10.1158/1055-9965.EPI-20-0975 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Berry RB, Budhiraja R, Gottlieb DJ, et al. Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. Deliberations of the sleep apnea definitions task force of the American Academy of Sleep Medicine. J Clin Sleep Med. 2012;8(5):597–619. doi: 10.5664/jcsm.2172 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Mei Z, Grummer-Strawn LM, Pietrobelli A, et al. Validity of body mass index compared with other body-composition screening indexes for the assessment of body fatness in children and adolescents. Am J Clin Nutr. 2002;75(6):978–985. doi: 10.1093/ajcn/75.6.978 [DOI] [PubMed] [Google Scholar]
- 27.Domenech-Asensi G, Gómez-Gallego C, Ros-Berruezo G, et al. Critical overview of current anthropometric methods in comparison with a new index to make early detection of overweight in Spanish university students: the normalized weight-adjusted index. Nutr Hosp. 2018;35(2):359–367. doi: 10.20960/nh.1189 [DOI] [PubMed] [Google Scholar]
- 28.Larsson I, Henning B, Lindroos AK, et al. Optimized predictions of absolute and relative amounts of body fat from weight, height, other anthropometric predictors, and age 1. Am J Clin Nutr. 2006;83(2):252–259. doi: 10.1093/ajcn/83.2.252 [DOI] [PubMed] [Google Scholar]
- 29.Heo M, Kabat GC, Gallagher D, et al. Optimal scaling of weight and waist circumference to height for maximal association with DXA-measured total body fat mass by sex, age and race/ethnicity. Int J Obes. 2013;37(8):1154–1160. doi: 10.1038/ijo.2012.201 [DOI] [PubMed] [Google Scholar]
- 30.Heitmann BL. Evaluation of body fat estimated from body mass index, skinfolds and impedance. A comparative study. Eur J Clin Nutr. 1990;44(11):831–837. [PubMed] [Google Scholar]
- 31.Visser M, van den Heuvel E, Deurenberg P. Prediction equations for the estimation of body composition in the elderly using anthropometric data. Br J Nutr. 1994;71(6):823–833. doi: 10.1079/BJN19940189 [DOI] [PubMed] [Google Scholar]
- 32.Noppa H, Andersson M, Bengtsson C, et al. Body composition in middle-aged women with special reference to the correlation between body fat mass and anthropometric data. Am J Clin Nutr. 1979;32(7):1388–1395. doi: 10.1093/ajcn/32.7.1388 [DOI] [PubMed] [Google Scholar]
- 33.Gallagher D, Visser M, Sepulveda D, et al. How useful is body mass index for comparison of body fatness across age, sex, and ethnic groups? Am J Epidemiol. 1996;143(3):228–239. doi: 10.1093/oxfordjournals.aje.a008733 [DOI] [PubMed] [Google Scholar]
- 34.Gallagher D, Heymsfield SB, Heo M, et al. Healthy percentage body fat ranges: an approach for developing guidelines based on body mass index. Am J Clin Nutr. 2000;72(3):694–701. doi: 10.1093/ajcn/72.3.694 [DOI] [PubMed] [Google Scholar]
- 35.Deurenberg P, van der Kooy K, Hulshof T, et al. Body mass index as a measure of body fatness in the elderly. Eur J Clin Nutr. 1989;43(4):231–236. [PubMed] [Google Scholar]
- 36.Deurenberg P, Weststrate JA, Seidell JC. Body mass index as a measure of body fatness: age- and sex-specific prediction formulas. Br J Nutr. 1991;65(2):105–114. doi: 10.1079/BJN19910073 [DOI] [PubMed] [Google Scholar]
- 37.Deurenberg P, Yap M, van Staveren WA. Body mass index and percent body fat: a meta analysis among different ethnic groups. Int J Obes Relat Metab Disord. 1998;22(12):1164–1171. doi: 10.1038/sj.ijo.0800741 [DOI] [PubMed] [Google Scholar]
- 38.Hinkle DWW, Jurs S. Applied Statistics for the Behavioral Sciences. 5th ed. Boston: Houghton Mifflin; 2003. [Google Scholar]
- 39.Mukaka MM. Statistics corner: a guide to appropriate use of correlation coefficient in medical research. Malawi Med J. 2012;24(3):69–71. [PMC free article] [PubMed] [Google Scholar]
- 40.Pepe M. The Statistical Evaluation of Medical Tests for Classification and Prediction. Oxford, UK: Oxford University Press; 2003. [Google Scholar]
- 41.Hosmer DLS. Applied Logistic Regression. 2nd ed. New York, NY: John Wiley & Sons, Inc; 2000. [Google Scholar]
- 42.Huayi Z, Gang X, Laiyuan L, et al. Age- and sex-related trends in body composition among Beijing adults aged 20-60 years: a cross-sectional study. BMC Public Health. 2023;23(1):1519. doi: 10.1186/s12889-023-16459-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Santoro N. Perimenopause: from Research to Practice. J Womens Health. 2016;25(4):332–339. doi: 10.1089/jwh.2015.5556 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Peppard PE, Young T, Barnet JH, et al. Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol. 2013;177(9):1006–1014. doi: 10.1093/aje/kws342 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.D’Agostino RB, Vasan RS, Pencina MJ, et al. General cardiovascular risk profile for use in primary care: the Framingham Heart Study. Circulation. 2008;117(6):743–753. doi: 10.1161/CIRCULATIONAHA.107.699579 [DOI] [PubMed] [Google Scholar]
- 46.Bennett DA. How can I deal with missing data in my study? Aust N Z J Public Health. 2001;25(5):464–469. doi: 10.1111/j.1467-842X.2001.tb00294.x [DOI] [PubMed] [Google Scholar]
- 47.Ranasinghe C, Gamage P, Katulanda P, et al. Relationship between Body Mass Index (BMI) and body fat percentage, estimated by bioelectrical impedance, in a group of Sri Lankan adults: a cross sectional study. BMC Public Health. 2013;13(1):797. doi: 10.1186/1471-2458-13-797 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Rubino F, Cummings DE, Eckel RH, et al. Definition and diagnostic criteria of clinical obesity. Lancet Diabetes Endocrinol. 2025;13(3):221–262. doi: 10.1016/S2213-8587(24)00316-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Quintas-Neves M, Preto J, Drummond M. Assessment of bariatric surgery efficacy on obstructive sleep apnea (OSA). Rev Port Pneumol. 2016;22(6):331–336. doi: 10.1016/j.rppnen.2016.05.006 [DOI] [PubMed] [Google Scholar]
- 50.Sakamoto N, Gozal D, Smith DL, et al. Sleep duration, snoring prevalence, obesity, and behavioral problems in a large cohort of primary school students in Japan. Sleep. 2017;40(3). doi: 10.1093/sleep/zsw082. [DOI] [PubMed] [Google Scholar]
- 51.Blaak E. Gender differences in fat metabolism. Curr Opin Clin Nutr Metab Care. 2001;4(6):499–502. doi: 10.1097/00075197-200111000-00006 [DOI] [PubMed] [Google Scholar]
- 52.Davidson FE, Matsha TE, Erasmus RT, et al. Associations between body fat distribution and cardiometabolic risk factors in mixed-ancestry South African women and men. Cardiovasc J Afr. 2019;30(6):321–330. doi: 10.5830/CVJA-2019-028 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Bredella MA. Sex Differences in Body Composition. Adv Exp Med Biol. 2017;1043:9–27. [DOI] [PubMed] [Google Scholar]
- 54.Zamboni M, Rossi AP, Fantin F, et al. Adipose tissue, diet and aging. Mech Ageing Dev. 2014;136-137:129–137. doi: 10.1016/j.mad.2013.11.008 [DOI] [PubMed] [Google Scholar]
- 55.Kirkness JP, Schwartz AR, Schneider H, et al. Contribution of male sex, age, and obesity to mechanical instability of the upper airway during sleep. J Appl Physiol. 2008;104(6):1618–1624. doi: 10.1152/japplphysiol.00045.2008 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Nokes B, Orr JE, White S, et al. Effect of obesity on sleep apnea pathogenesis differs in women versus men: multiple mediation analyses in the retrospective SNOOzzzE cohort. J Appl Physiol. 2024;136(6):1516–1525. doi: 10.1152/japplphysiol.00925.2023 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Lopez-Gonzalez AA, Jover AM, Martínez CS, et al. The CUN-BAE, Deurenberg Fat Mass, and visceral adiposity index as confident anthropometric indices for early detection of metabolic syndrome components in adults. Sci Rep. 2022;12(1):15486. doi: 10.1038/s41598-022-19343-w [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Castaneda A, Jauregui-Maldonado E, Ratnani I, et al. Correlation between metabolic syndrome and sleep apnea. World J Diabetes. 2018;9(4):66–71. doi: 10.4239/wjd.v9.i4.66 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Shuster A, Patlas M, Pinthus JH, et al. The clinical importance of visceral adiposity: a critical review of methods for visceral adipose tissue analysis. Br J Radiol. 2012;85(1009):1–10. doi: 10.1259/bjr/38447238 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Zhang X, Ma N, Lin Q, et al. Body roundness index and all-cause mortality among US adults. JAMA Netw Open. 2024;7(6):e2415051. doi: 10.1001/jamanetworkopen.2024.15051 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Goodarzynejad H, Meaney C, Brauer P, et al. Recent trends in adult body mass index and prevalence of excess weight: data from the Canadian primary care sentinel surveillance network. Can Fam Physician. 2022;68(2):128–138. doi: 10.46747/cfp.6802128 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Dosman JA, Karunanayake CP, Fenton M, et al. Obesity, sex, snoring and severity of OSA in a first nation community in Saskatchewan, Canada. Clocks Sleep. 2022;4(1):100–113. doi: 10.3390/clockssleep4010011 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Allen AJ, Amram O, Tavakoli H, et al. Relationship between travel time from home to a regional sleep apnea clinic in British Columbia, Canada, and the severity of obstructive sleep. Ann Am Thorac Soc. 2016;13(5):719–723. doi: 10.1513/AnnalsATS.201509-613BC [DOI] [PubMed] [Google Scholar]
- 64.Mazzotti DR, Keenan BT, Lim DC, et al. Symptom subtypes of obstructive sleep apnea predict incidence of cardiovascular outcomes. Am J Respir Crit Care Med. 2019;200(4):493–506. doi: 10.1164/rccm.201808-1509OC [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Pineau JC, Ramirez Rozzi FV. Measuring body fat-How accurate is the extrapolation of predictive models in epidemiology? PLoS One. 2022;17(2):e0263590. doi: 10.1371/journal.pone.0263590 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Unal Y, Ozturk DA, Tosun K, et al. Association between obstructive sleep apnea syndrome and waist-to-height ratio. Sleep Breath. 2019;23(2):523–529. doi: 10.1007/s11325-018-1725-4 [DOI] [PubMed] [Google Scholar]
- 67.Glicksman A, Hadjiyannakis S, Barrowman N, et al. Body fat distribution ratios and obstructive sleep apnea severity in youth with obesity. J Clin Sleep Med. 2017;13(4):545–550. doi: 10.5664/jcsm.6538 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Wang SH, Keenan BT, Wiemken A, et al. Effect of weight loss on upper airway anatomy and the apnea-hypopnea index. The importance of tongue fat. Am J Respir Crit Care Med. 2020;201(6):718–727. doi: 10.1164/rccm.201903-0692OC [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Eckert DJ, White DP, Jordan AS, et al. Defining phenotypic causes of obstructive sleep apnea. Identification of novel therapeutic targets. Am J Respir Crit Care Med. 2013;188(8):996–1004. doi: 10.1164/rccm.201303-0448OC [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Won CHJ, Reid M, Sofer T, et al. Sex differences in obstructive sleep apnea phenotypes, the multi-ethnic study of atherosclerosis. Sleep. 2020;43. doi: 10.1093/sleep/zsz274 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Hang LW, Tsai Y-C, Finnsson E, et al. Sex-specific age-related worsening of pathological endotypic traits in patients with obstructive sleep apnea. Sleep. 2025;48(1). doi: 10.1093/sleep/zsae185. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Shi Y, Zhang Y, Cao Z, et al. Application and interpretation of machine learning models in predicting the risk of severe obstructive sleep apnea in adults. BMC Med Inform Decis Mak. 2023;23(1):230. doi: 10.1186/s12911-023-02331-z [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The dataset from this study is available under REB approval upon reasonable request from the corresponding author.