Abstract
Background
Breast cancer is the most prevalent cancer among women globally, including in Africa. Oncology is a relatively new discipline in many West African countries, particularly in Benin. There is currently a lack of data concerning the current state of cancer care infrastructure and oncology practices within these countries. The aim of the article is to describe the barriers and opportunities related to access to oncology care in Benin.
Methods
We employed a qualitative research design. Fifty-six semi-structured interviews were conducted with caregivers treating cancer (n=26), women with breast cancer (n=23), and representatives of associations (n=2). Additionally, 18 days of participant observation were conducted in a chemotherapy and palliative care departments in Cotonou, Benin. The data was analysed using Levesque et al.‘s theoretical framework on access to healthcare.
Results
Women encounter obstacles such as delayed diagnosis and unequal access to information, as well as socio-cultural beliefs that favour traditional medicine and discourage surgical interventions like mastectomy. The treatment pathway is often chaotic due to insufficient specialised caregivers and limited infrastructure, with services centralised in Cotonou forcing patients to travel long distances around the country. The current lack of radiotherapy requires patients in need to travel abroad for treatment. High costs of biomedical tests and treatments often lead to care abandonment, worsening health inequalities. However, positive changes should be highlighted, such as the establishment of the Inter-University Diploma in Gynaecological and Breast Oncology in 2013, the expansion of palliative care services in the country, and the planned opening of the Calavi International Hospital Centre in 2025. Challenges include continuing to train health professionals in oncology, further developing health financing and supporting civil society to raise awareness of breast cancer.
Conclusions
Benin is facing several challenges in relation to the provision of timely and high-quality care for women with breast cancer. However, there is a growing commitment to enhancing breast cancer care in Benin.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12885-025-14325-3.
Keywords: Cancer, Benin, Access to care, Barriers, Opportunities, Africa, Breast
Introduction
Breast cancer is the second most common cancer worldwide. In 2022, an estimated 2.31 million new cases were diagnosed, and almost 670,000 women died from this disease globally. The cancer burden is rising in sub-Saharan Africa (SSA), with geographical variations in the most prevalent types of cancer across the region [1]. The African continent accounts for 8.6% of global breast cancer cases and 13.6% of breast cancer-related deaths [2], although these figures are approximate. Indeed, most SSA countries have weak civil registration and mortality statistics systems [1]. Cancer registration remains underdeveloped in SSA; computer-based medical information systems are lacking, complicating the identification of new cases and the follow-up of cancer patients [1].
Breast cancer represents a significant global challenge in health, gender, socio-economic, and equity [3]. Access to quality care is influenced by cultural and individual factors, including geographical location. While significant disparities exist between high-income countries (HICs) and low- and middle-income countries (LMICs), inequalities also arise within countries along racial and socioeconomic lines [3]. A meta-analysis of women with breast cancer in SSA indicates estimated survival rates of 79% at 1 year, 56% at 3 years, and 40% at 5 years, with a higher survival rate observed in countries with a higher Human Development Index (HDI) [4]. A multinational African study, including women with breast cancer from Nigeria, Uganda, Zambia, and multiracial populations of Namibia and South Africa, showed that a more advanced stage at diagnosis was associated with being Black [5].
In 2022, the WHO launched a Global Breast Cancer Initiative (GBCI) [6]. The GBCI established a framework based on three pillars to achieve its primary objective: health promotion for early detection (pre-diagnostic interval), timely breast diagnostics (diagnostic interval), comprehensive breast-cancer management (treatment interval) [7]. A systematic review of studies in SSA examining factors impeding access to cancer care reveals that delays were attributed to multiple factors, including high costs of diagnostic and treatment services, lack of coordination among primary, secondary and tertiary healthcare sectors, inadequate staffing levels, and continued reliance on traditional healers and complementary medicines. Nevertheless, the authors identified a paucity of studies on this topic despite its significance, and inconsistencies in study design, which limits the broader impact of their findings [8]. The capacity to conduct robust research is steadily growing in SSA countries. Still considerable effort is needed to coordinate these resources to support a shared agenda based on national and regional priorities. Robust research to inform policies on barriers to early detection, timely diagnostics, and quality cancer care in SSA is lacking. The authors call for research into the complex interplay of these factors to build resilient and effective cancer control programs [8].
Benin is a French-speaking country in West Africa. The population was 13.35 million in 2022, with a fertility rate of 5.7 children per woman and a life expectancy of 61.2 years. In 2021-2022, the national poverty rate was 36.2 per cent. The country’s ranking on the United Nations Human Development Index (HDI) remains low, although it has improved over time. In 2020, Benin ranked 166 th out of 191 countries, with an HDI of 0.525 [9, 10]. In Benin, a cancer registry was set up in 2014 as part of the African Cancer Registry, showing that breast cancer is the most common cancer in terms of both incidence and mortality [11] and that women affected by this cancer have specific characteristics. Women with breast cancer in Benin are particularly young (median age of 49 years)) [12, 13], have more aggressive forms of the disease (31% of triple-negative cancers compared to 13% in France) [12, 14], and are diagnosed at advanced stage (stages III and IV) of the disease, which helps explain why they have a five-year survival rate of less than 50% (48.5%) [12]. However, little is known about the country’s concrete state of cancer care infrastructure and oncological practices. Thus, this article aims to describe the barriers and opportunities of access to oncology care in Benin to better inform policies on the barriers to quality cancer care.
Methodology
We used a qualitative research design that combined observations and in-depth interviews. We present our methodology following the Consolidated Criteria for Reporting Qualitative Research (COREQ) [15].
Research team and reflexivity
Personal characteristics and relationship with participants
Five people were involved in the data collection: a Beninese sociologist (MA) who is currently a PhD student (n=20 interviews), a French sociologist (CS) who has been conducting fieldwork and interviews with caregivers and women in Benin for 7 years (n=13 interviews), and three French students who were enrolled in a Master’s programme in France but did fieldwork in Benin during their research (MB, PP, LL) (19, 3 and 2 interviews respectively). The French sociologist also has a background as a midwife in France with some experience in West Africa.
The interviewers conducted 56 in-depth interviews using two interview grids (one for women, the other for caregivers). They systematically discussed their approaches at the different stages of data collection to ensure a common understanding of the questions. Some interviews were conducted by more than one interviewer to familiarise themselves with the interview grids.
Study design
Theoretical framework
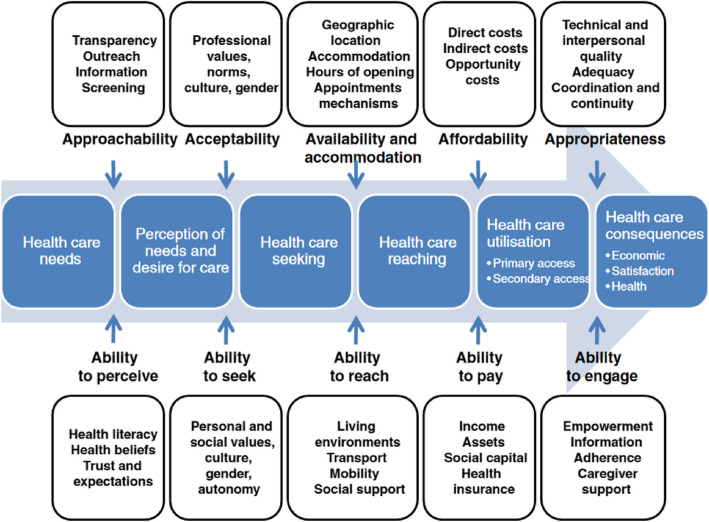
We used the theoretical framework developed by Levesque et al. [16] regarding access to healthcare (Fig. 1). We applied this framework a posteriori to organise and analyse collected data [17]. Access is considered as the possibility of identifying one’s healthcare needs, seeking healthcare services, reaching healthcare resources, obtaining or using healthcare services, and being offered services appropriate to one’s needs for care [16]. The results will therefore be presented according to the five dimensions of service accessibility : 1) approachability; 2) acceptability; 3) availability and accommodation; 4) affordability; 5) appropriateness, as well as according to the five corresponding abilities of individuals who interact with the dimensions of accessibility to generate access: 1) ability to perceive; 2) ability to seek; 3) ability to reach; 4) ability to pay; 5) and ability to engage.
Fig. 1.
Levesque et al.’s definition of access to healthcare [16]
Participant selection
The research took place in four cities in Benin (Abomey-Calavi, Bohicon, Cotonou, and Parakou) between December 2022 and April 2024. An interview with a Beninese caregiver was also conducted in Abidjan (Côte d’Ivoire) as a key informant on the issue of access to oncology care.
A purposeful sampling approach was employed to identify and select information-rich caregivers and women with specific expertise and experience in the field of cancer care in Benin [18]. Fifty-six semi-structured interviews were conducted with cancer caregivers in Benin (n=26), breast cancer women (n=23) and associations representatives (n=2). Among the twenty-six caregivers, five were interviewed twice, six months apart (Table 1).
Table 1.
Total number of people surveyed and interviews conducted in the study
| Number of respondents | Number of interviews | |
|---|---|---|
| Cancer caregivers | 26 | 31 |
| Breast cancer women | 23 | 23 |
| Associations representatives | 2 | 2 |
| Total | 51 | 56 |
The health professionals recruited play a key role in cancer care in Benin: gynaecologists and obstetricians (n=7), internists (n=3), radiotherapists (n=3), pathologists (n=3), oncologists (n=2), surgeons (n=2), nurses (n=4), pharmacists (n=1) and students specialising in gynaecology and obstetrics (n=1). Women with breast cancer were recruited through a surgeon working in Cotonou (n=20) and through observations in oncology wards (n=3). The association representatives (n=2) were from the leading breast cancer association in Benin and from the national palliative care association.
Settings
Interviews with healthcare professionals took place in healthcare facilities (n=27), at the Faculty of Health Sciences (n=1) or remotely via videoconference (n=3). Interviews with patients were conducted at home (n=20), at work (n=1) and in healthcare facilities (n=2). The two interviews with association representatives took place at one interviewer’s workplace and at the Faculty of Health Sciences of the other.
Data collection
The interview guides are common to the countries where the SENOVIE project is taking place (France, Benin, Cambodia, Mali). Interviews were conducted using interview grids for healthcare professionals (Appendix 1) and for women (Appendix 2). The following topics were covered with the healthcare professionals: the existence of professional training in oncology in Benin and their personal career paths (at the national and international levels); cancer care available in Benin (available human resources, infrastructure, key national and international actors, health policies, obstacles, and challenges); and the mobility of healthcare professionals and women (incoming and outgoing). During the interviews with women, the first part retraced their care pathway, including the first signs, the various recourses (formal and informal), contacts, information received, relations with healthcare professionals, difficulties, costs, and mobility. The second part was devoted to their relationship with their bodies and representations of ‘femininity’ (i.e. what it means to feel like a ‘woman’) in the context of the disease, including the effects of treatment on the body, the experience of amputation, self-image, sexuality, conjugality, perceived discrimination, the unveiling of the body, and relationships with other women (particularly possible co-wives). Across these two major themes, the issue of biographical ruptures was explored (marital, professional, and social ruptures). Lastly, interviews with association representatives reviewed the history of the association’s creation and then combined questions from the interview grids for health professionals and women; the selected questions addressed the provision of care, care pathways, and women’s life paths. All interviews were audio-recorded and transcribed.
The French sociologist (CS) and two of the master’s students (LL and PP) carried out participant observations in Cotonou at the beginning and end of the study period (October to November 2022, then February to April 2024). These observations aimed to familiarise themselves with patient care pathways and the organisation of medical services in Cotonou. In total, 18 days of observation were carried out in the chemotherapy unit of the Centre Hospitalier Universitaire de la Mère et de l’Enfant Lagune (CHU-MEL) (n=8) and in the internal medicine and palliative care departments of the Centre National Hospitalier Universitaire Hubert Koutougou Maga (CNHU-HKM, GHEZO camp area) during medical consultations, chemotherapy treatments and home visits with the palliative care team (n=10).
Analysis and findings
Data analysis
The data collected were organised and analysed according to the theoretical framework established by Levesque et al. [16] regarding access to healthcare (Fig. 1). This framework enabled a complex and in-depth understanding of the experiences of individuals navigating the healthcare system in Benin. Data analysis used a comprehensive approach to analyse experiences as they were lived and not necessarily as they objectively occurred [19]. CS and PP carried out the analysis without the use of software. The French sociologist (CS) and the master’s student (PP) presented two sets of results in Cotonou in December 2022 and April 2024, respectively, to sixty caregivers involved in breast cancer care at various health facilities in Benin. All participants agreed and contributed to improving the research results.
Reporting
We will include quotations from different participants in the results section to add transparency and trustworthiness to our findings and interpretations of the data.
Results
The healthcare professionals ranged in age from 26 to 62 years (median 41 years). Six were women, and twenty were men. All were born in Benin. The patients ranged in age from 33 to 71 (median age 53) and had a variety of occupations: they were nurses, shopkeepers, teachers, housewives, asset managers, secretaries, and pensioners. They were all women. They came from different parts of Benin, except one person born in Gabon. The two association representatives interviewed had women on their boards. One of them had suffered from breast cancer and the other was a caregiver. The median length of the interviews was 55 minutes for healthcare professionals, 49 minutes for patients and 77 minutes for associations. The observations and interviews highlighted various barriers and opportunities to access oncology care in Benin which are summarized in Table 2.
Table 2.
Barriers and opportunities to access oncology care in Benin for women with breast cancer
| Demand | Ability to perceive | Ability to seek | Ability to reach | Ability to pay | Ability to engage |
| Barriers |
-Persistent misunderstandings and lack of knowledge about breast cancer, its symptoms and treatment options -Socio-cultural misconception that breast cancer is contagious and inevitably fatal -Belief in mystical explanations for breast cancer that lead to traditional medicine |
-Frequent discontinuation of chemotherapy due to lack of understanding of side effects -Cultural rejection of surgery due to fear of witchcraft -Social representation of breasts as a symbol of femininity and maternity: immense work needed on the relationship with the body and family dynamics to accept mastectomy |
-Feelings of disorientation and wandering between care facilities, sometimes geographically distant |
-Systematic financial challenges -Personal debt and long-term family repercussions |
-Forced autonomy of patients within the care pathway, leading to missed opportunities |
| Opportunities | -Regular self-examination for some women | -Confidence in carers and in modern medicine as an essential driver for seeking care | -The importance of the social network for accessing appropriate medicines and care structures, particularly abroad | -Social capital as a major factor in patient care: mutual aid and financial donations from family and friends | -Support from family and friends, community networks and associations |
| Supply | Approachability | Acceptability | Availability and accommodation | Affordability | Appropriateness |
| Barriers |
-Limited and inequitable access to information -Lack of systematic screening |
-Lack of psychological care |
-Centralisation of care in Cotonou: induced intra-national mobility -Lack of specialised healthcare professionals: no training in the country, brain drain of young people trained abroad, and limited opening of specialised posts -Biomedical examinations face limited technical facilities and long waiting times -Stockouts and unavailability of ‘essential medicines’ as defined by the WHO -Unavailability of radiotherapy: the only solution is international mobility |
-Health insurance system highly fragmented and does not cover a large proportion of the population -Treatment varies according to patients’ financial means: breast cancer as a health inequality -Extremely high cost of diagnostic services and treatments, major financial inaccessibility of targeted therapy |
-Absence of a local Diplôme Universitaire (DU) in medical oncology -Absence of a local Diplôme d’Études Spécialisées (DES) in oncology |
| Opportunities |
-“Pink October” as an opportunity to raise awareness -Midwives play a role as entry points for breast cancer care |
-Caregiver-patient communication is a major factor in acceptance of the care pathway -Spiritual and religious beliefs as moral support -Civil society mobilisation in the face of the breast cancer taboo |
-Rebound in the specialty of pathology, leading to systematic improvements in diagnosis -Rare possibilities for surgical reconstruction following mastectomy |
-Surgery is a key stage in the treatment process due to its affordability -State funding for officials and the needy, subject to review by a commission -Financial support, although rare, from associations |
-Gradual structuring of breast cancer care, with increasing specialisation of healthcare professionals treating breast cancer -Introduction of the Diplôme Inter-Universitaire (DIU) in Gynaecological and Breast Oncology at the Faculty of Health Sciences (Cotonou) in 2013 -Growing medical cooperation and improving the circulation of knowledge: increasing number of congresses and forums, initiation of trans-hospital RCP -The rapid development of palliative care for breast cancer patients, thanks to the efforts of the Association Béninoise des Soins Palliatifs (ABSP, established in 2015) and the Programme National de Soins Palliatifs (PNSP, established in 2019) -Opening of the Centre Hospitalier International de Calavi (CHIC), scheduled for 2025, with an oncology department equipped with radiotherapy |
Approachability and ability to perceive
Knowledge and understanding of breast cancer in Benin
The discovery of the disease begins with the appearance of breast abnormalities perceived by women as a “pimple”, a “boo-boo”, a “blister”, or a “lump the size of a corn kernel”. In most cases, these initial painless symptoms do not worry them. This lack of concern delays doctor visits, thereby postponing diagnosis.
“When I got out of the shower, my left breast was itching a lot, so I stood in front of the mirror and noticed that, unlike my right breast, there was a line or a blue mark. That’s what made me examine myself, and when I felt it, I realised there was a lump. So, my first instinct was to take anti-inflammatories.” (Patient – Iyalola, 69, Abomey-Calavi, 2023).
In the wider community, breast cancer is often perceived as an infectious disease, and some fear that it can be transmitted to husbands through sexual contact. This “fear of contagion” is partly due to limited and unequal access to information.
Additionally, many individuals equate “cancer” with “death.” Women report this cultural perception and reveal that loved ones often use this belief to justify their lack of support.
“As soon as someone hears you have this disease, it’s as if you’re already counted among the dead.” (Patient – Philippine, 69, Cotonou, 2024).
According to healthcare professionals, this perception is partly rooted in the outcomes of past treatments when breast cancer was a little-understood disease, and treatment options within the country were inadequate.
Mystical beliefs and traditional medicine
However, many women interpret breast cancer in mystical terms. To them, it is a “spell,”, an “hex” or an “evil”. In Fongbé, a major language in Benin, there is no word for “cancer”. A woman with breast cancer might say “houanvou do anon tchemin” to describe her condition, which translates to “there is a worm in my breast”. The “worm” is seen as the manifestation of a curse “cast to kill women” (Healthcare professional – Carine, 46, 2022).
Healing is therefore viewed as something mystical or even religious. Traditional medicine is generally the preferred option for patients seeking treatment for breast cancer. Indeed, “you don’t go to the hospital for a curse. You first try to heal yourself with traditional remedies; you must find out who has wronged you.” (Healthcare professional – Willis, 2022).
Interviews highlight the influence of women’s families, who often encourage them to consult traditional healers, sometimes considered “charlatans” (Patient – Love, 42, Cotonou, 2024). While some patients follow family recommendations favoring traditional medicine, others marked by painful experiences, choose to break away from these practices. This is the case with Senami, whose testimony reveals this process of questioning :
"My older sister who I lived with - may she rest in peace - she died of it [breast cancer], so it was a shock to me. But when they told me that I had breast cancer, I had already made up my mind, because my elder sister, she didn’t go to the hospital. They told her it could be cured by traditional healers and she went there thinking they would cure it. When I told my younger sister about mine, they said the same thing. But I said no.” (Patient – Senami, 47, Cotonou 2023).
Doctors and representatives of associations note that most women come to the hospital for the first time when their symptoms become very concerning or even unbearable: a large mass in the breast, intense pain, growing sores, a foul smell, and necrosis.
Lack of systematic screening programs
As in many SSA countries, Benin currently lacks a systematic breast cancer screening program. In this study, breast cancer was generally discovered through self-examination by the women themselves or by primary healthcare professionals. Only two women detected their cancer during a screening exam, by ultrasound and mammography, which they deliberately sought out.
“They looked at me. ‘Who asked you to get a mammogram?’ – I said, ‘I did it myself.’ – ‘We’ve never seen someone come in on their own for a mammogram and actually find something. And yet there is something!’” (Patient – Ambre, 63, Abomey-Calavi, 2024).
One woman, a midwife by profession, highlights the need to implement an “annual subsidized gynecological check-up” in Benin, including appropriate screening exams.
“I told you; several midwives examined my left breast. They said, ‘Oh sister, you’re worrying for nothing. There’s nothing there.’ But I said, ‘Give me a voucher, I’ll get the tests done.’ And that’s what revealed the truth, you see. So, if she has 100 women to examine, she won’t have time to carefully palpate every quadrant, one by one. Do you understand? We need a screening and care center. You go there, they screen you.” (Patient – Philippine, 69, Cotonou, 2024).
Expanding awareness efforts
Awareness of breast cancer in Benin is increasing, albeit slowly, thanks to health professionals and awareness campaigns initiated by the government and civil society. Events like “Pink October” allow associations to train women in self-examination and inform them about treatment pathways. For doctors, a key goal is to reduce feelings of guilt in women diagnosed with breast cancer and to empower them to seek care.
“The first question people ask you is: ‘What did I do?’. And when there is this sense of guilt, it’s really dangerous, actually. But if we can help people understand that it’s not their fault and that it can be managed if diagnosed early, I think that will help us as healthcare workers.” (Healthcare professional – René, 2022).
Efforts focus particularly on educating women about the impact of early screening on survival rates, encouraging them to seek hospital care promptly.
“People don’t die in ignorance anymore; they come out to seek treatment. The positive thing about breast cancer in Benin is that people have really started moving out of ignorance. They know there’s care available for their illness. Before, if they had something in their breast, they’d turn to traditional treatments; they wouldn’t come to the hospital. It was all herbal teas and herbs. But really, we see there’s been a change.” (Healthcare professional – Chantal, 2022).
Midwives: a key link in accessing breast cancer care in Benin
Midwives emerge as the primary point of entry into breast cancer care for women in this study. Many women, upon discovering a lump, turn to midwives they know, while others first learn of a breast abnormality during a midwife’s exam, often in the context of pregnancy follow-up or family planning appointments. Midwives have consistently taken these initial signs seriously, referring women to hospital facilities that offer breast cancer care.
“At the ninth month, I went for a check-up there, and they also checked [the breasts], and they said there was something in my breast. And the midwife said what I have there could lead to breast cancer, and she referred us to a gynecologist in a private hospital.” (Patient – Cécile, 33, Cotonou, 2022).
Beyond their expertise in detecting lumps during consultations, midwives play a crucial role in breast cancer awareness and prevention.
“In fact, mom was watching TV one evening, May 5, Midwives’ Day or something like that. And the midwives’ association talked about breast self-exams. After the show, she just lay down and started examining herself. She said, ‘Hey, hey, girls, come here. I think I’ve something.’ So, I examined too and saw there was something. So, we went to see the gynecologist. He said, ‘Yes, there is something.’ They requested all the tests.” (Patient – Philippine, 69, Cotonou, 2024).
However, while pregnancy is a crucial moment for diagnosis, pregnant women diagnosed with breast cancer face a therapeutic impasse. For the women in this study who discovered breast cancer during pregnancy, treatment was delayed until after childbirth, and sometimes until after breastfeeding ended, which might have reduced their survival chances.
Acceptability and ability to seek
Interruptions in chemotherapy care
Chemotherapy is sometimes poorly accepted because the side effects are difficult to bear and understand. Patients feel that they are “adding a new disease” (Health professional - Carine, 2022) or turning into a “monster” (Association representative - Jeannette, 36, Cotonou, 2022), which frightens them and can lead to discontinuation of treatment.
“It [chemotherapy] is unpleasant, it’s unpleasant, and I even wonder if it doesn’t make me sicker than the illness itself.” (Patient – Kayanki, 52, Parakou, 2023).
Many women are lost to follow-up by healthcare professionals before completing their chemotherapy cycles, when the symptoms of breast cancer begin to subside with treatment.
“The fourth session, I refused. (…) Because I said, the illness is calm, but the treatment wants to kill me.” (Patient – Bernadette, 53, Cotonou, 2024).
Women’s decision to stop chemotherapy without their doctor’s approval reflects a misunderstanding of the disease and its treatment.
“We have patients, you start treatment with them, the mass disappears completely. This type of patient, she lets you know she’s not coming back; she’s finished. For her, she’s cured. No matter what you say, in her mind, the mass is gone.” (Healthcare professional – Willis, 2022).
Thus, healthcare providers play a crucial role in helping women accept the entire course of chemotherapy and its difficult side effects.
Cultural resistance to mastectomy: witchcraft beliefs and loss of femininity
One of the primary barriers to breast cancer treatment in Benin is the very common refusal of surgery, despite it being a critical step in the care pathway due to its financial and technical accessibility. The categorical opposition of women, or sometimes of their relatives, is a contributing factor to late diagnosis and delays in breast cancer treatment in this country: women avoid hospitals when they detect lumps, anticipating that they will not agree to surgery. Others seek treatment, wanting to start chemotherapy but rejecting the surgery that typically follows. Doctors then attempt to maintain contact with these women and to persuade them of the necessity of surgery.
“All our patients, when they come, they are clear and categorical: they will not have breast surgery. No matter what you say, no matter what you do, they won’t have breast surgery. Unless they come to a stage where it’s very severe, and for themselves, it’s unbearable. In that case, they ask you to operate for relief. When you are in a country like this, you take things with caution, you’re forced to find a way to make the patient accept. Sometimes we have to lie to the patient just to start the first treatment so that quickly things can reduce, so we don’t let it progress.” (Healthcare professional – Willis, 2022).
The refusal of surgery is partly culturally explained. People in Benin strongly believe that surgery is dangerous and that operating would worsen the disease.
“When the scalpel touches it, you die. It’s ideas that have been put into their heads.” (Healthcare professional – Carine, 2022).
According to the SOS Cancer association representative, patients view breast cancer as a “trapped papaya”, meaning, “if the doctor puts his tool in it, it will explode, and that’s it, only death awaits you” (Association representative – Jeannette, 36, Cotonou, 2022).
There is also a link between the belief in witchcraft, mentioned above, and the refusal of surgery. For the women interviewed, surgery is a moment anticipated by those who wish them harm.
“[Before the operation], I was a little scared. People talked a little. Since it’s Benin, in Africa, we shouldn’t talk about it. People take advantage to kill people, you know, mystical things! So I was a bit scared, I was stressed” (Patient – Alicia, 48, Cotonou, 2022).
Beyond mystical beliefs, mastectomy faces another significant cultural barrier: the deep-rooted perception of breasts as essential symbols of femininity and motherhood. For many women in Benin, breasts are not just physical organs but fundamental markers of womanhood, particularly through their nurturing role in breastfeeding. The prospect of mastectomy therefore represents more than a medical procedure – it threatens their very identity as women, with some patients expressing fear of becoming what they describe as “half-women” (Patient – Adjoké, 45, Cotonou, 2022). The journey to accept surgery can take years and involves significant work on their body image.
“It’s between losing my life and keeping my femininity. What will I choose? I have no choice. If that’s what it takes for me to live a little with my children, I have no qualms about it. The choice now is between life and femininity” (Patient – Prudo, 60, Cotonou, 2024).
The negative societal perception of a woman who has had breast surgery plays a major role in couple and family relationships.
“What’s even happening is that the in-laws are already telling the man to give up on his wife, that she’s no longer a woman, she’s a wreck. ‘How can you have a woman without a breast? What are you going to do with that?’ And they put such pressure on the husbands that they leave; they leave.” (Association representative – Jeannette, 36, Cotonou, 2022).
The importance of trust in healthcare providers
All the women who took part in the study were treated at a hospital. The interviews reveal the essential role of health literacy and education in the decision to seek medical care. Trust in modern medicine is a determining factor in women’s entry into the health system.
“At first, I was scared. I was scared because on my mother’s side, my mom died very young. She didn’t die of cancer, but three of her sisters did, and it’s not that they weren’t treated, because two were pharmacists and one was a pediatrician. And yet, they’re gone. It was always triple-negative. I said to myself: ‘Whatever happens, happens.’ But when I met the doctor, I don’t know where this conviction and trust came from, I don’t know, I can’t explain it, but when I met him, I said to myself: ‘I will be cured, and he’s the one who will cure me’. I believe that trust played a big role.” (Patient – Iyalola, 69, Abomey-Calavi, 2023).
Lack of psychological support but unwavering spiritual support
The people interviewed highlighted the “fundamental” importance of psychological support in cancer care, which is lacking in Benin. The patients share their traumas and difficulties in accepting the disease and treatment during the interviews.
“When the results came out, I didn’t accept the disease. And then the way I was told the diagnosis really traumatised me. I was completely lost. In another world, really. So the day before the operation I said: ‘Mum, let’s go home. She didn’t know what to tell me. She said: ‘You’re not going to do it anymore’. She said: ‘Then let’s go home early in the morning’. We went back with the first buses. So the hospital called me and said my bed was ready and all that. I said ‘I’m coming’, even though I was already on the bus” (Patient - Manon, 42, Cotonou, 2024).
Without this support, caregivers reluctantly and anxiously sometimes feel “forced to play the role of psychologist” (Healthcare professional – René, 2022).
“On a psychological level, a cancer patient, it’s really… I can tell you that for more than three months, I looked for a psychologist for my patients; I couldn’t find one. Even for the healthcare staff, we needed one” (Healthcare professional – François, 30, 2023).
Nevertheless, spiritual and religious support appears unshakable and provides immense moral support for patients.
“I was sure my Lord wouldn’t abandon me, I had this firm conviction, and that’s what gave me strength” (Patient – Géraldine, 71, Bohicon, 2023).
Spirituality even allows some to transcend the “shame” of having undergone a breast removal to raise awareness among other women about screening. Communicating about the treatments that saved them is, for them, like “talking about God”, sharing His word with the faithful “so that it doesn’t happen to them” (Patient – Nadia, 54, Cotonou, 2023).
Availability, accommodation and ability to reach
Centralisation of care in Cotonou: imposed intra-national mobility and therapeutic wandering
The management of breast cancer is largely centralised in Cotonou, the economic capital of Benin located in the far south of the country. Currently, two public hospitals are responsible for breast cancer care: historically at the Centre National Hospitalo-Universitaire (CNHU-HKM) in Cotonou, specifically in the visceral surgery department, and to a lesser extent at the University Clinic of Gynecology-Obstetrics; and more recently at the Centre Hospitalo-Universitaire de la Mère et de l’Enfant Lagune (CHU-MEL), where an oncology unit opened in 2019. Therefore, women must systematically travel to Cotonou if they wish to receive a diagnosis and subsequent treatment for their cancer, often traveling across the entire country. This regional mobility is made even more difficult because it is repeated multiple times during the care pathway. Patients report feelings of disorientation, wandering, and abandonment during this challenging journey, from which many drop out, with longer delays in care for patients who do not reside in Cotonou.
Lack of healthcare professionals specialising in breast cancer care
Benin faces a shortage of healthcare professionals specialising in breast cancer treatment. For pharmacists and nurses, this is particularly a “virgin territory” (Healthcare Professional – Carine, 2022). For doctors, this shortage is largely explained by the lack of training in medical oncology and radiotherapy locally, as well as deficiencies in technical resources that prevent the creation of specialised positions. The healthcare system also faces a “brain drain” (Healthcare Professional – Richard, 2022) of specialised Beninese doctors.
“When you come back, you return with just an A4 paper that is your diploma, but there is no structure capable of employing you properly. This is one of the realities of being a doctor in Benin. Benin does not systematically recruit its specialists. That’s what causes the brain drain. When a person comes and cannot find their place, they have to leave.” (Healthcare Professional – Richard, 2022).
Drained by countries where salary conditions are advantageous and technical resources are more efficient, this outward mobility of specialised doctors directly impacts breast cancer care in the country and greatly worries the remaining doctors in Benin, who are suffering from an increasingly heavy workload. This creates a “vicious circle” that demotivates new generations from practicing specialised medicine in their country.
“If you are not many doing the work, there will definitely be burnout. Because the number of patients is increasing” (Healthcare Professional – Habib, 2023).
Nevertheless, our study shows a “bounce back” in pathology (Healthcare professional – Romeo, 2023). The return of these specialist doctors to the country after their training has significantly advanced local care. They have improved breast cancer diagnosis and tumour characterisation, which is essential for establishing an appropriate treatment plan.
Diagnostic tests and staging assessments: conducted abroad, technical failures, significant delays
The management of breast cancer requires biomedical tests to specify the type of cancer, its stage of progression, the overall health status of the patient and any comorbidities, to establish the most relevant and appropriate treatment protocol. However, the technical resources in Benin remain limited regarding the available diagnostic tests and staging assessments. For instance, some equipment, such as PET scans and scintigraphy, are unavailable in the country. There is only one MRI machine in the public sector, which, like any machine, occasionally breaks down. Moreover, immunohistochemistry tests can rarely be conducted locally and are generally performed in laboratories in France. These various technical difficulties slow down and complicate care for Beninese patients, particularly financially.
“Here, the scanner was down, and I went to a private clinic, and I paid 180,000, whereas at the CNHU I would have paid 16,000.” (Patient – Géraldine, 71, Bohicon, 2023).
Stock breakdowns and unavailability of “essential medicines” according to the WHO
One of the significant challenges to accessing care for women with breast cancer in Benin lies in the availability of quality medicines. Indeed, the national supply system operates through a purchasing center, the Société béninoise pour l’approvisionnement en produits de santé (SoBAPS), which orders medications in bulk. These medications are then made available in hospital pharmacies or community pharmacies. However, due to the lack of standardisation in treatment protocols among prescribers and a lack of coordination during the ordering of medications, estimating demand becomes difficult. The consequences include recurring stockouts. When medications are unavailable, patients have several options, all of which lead to delays and additional expenses: they can order medications from SoBAPS by placing a deposit, turn to private wholesalers who set their prices, or procure them from another country by traveling there or sourcing them through their own networks. Thus, patients with limited financial and/or social capital face significant difficulties obtaining medications on time:
“He wrote the prescription, and I went to all the pharmacies; I couldn’t find any. Then I was told that the CNHU sold them, so I went there, and they told me they were out of stock and advised me to go to Lomé [Togo’s capital]. So, I went to Lomé, and there I found the product.” (Patient – Kayanki, 52, Parakou, 2023).
In addition, some key molecules in the treatment of certain breast cancers, such as trastuzumab (targeted therapy), which is listed by the WHO as an essential drug, are rarely available in Benin.
“There are patients who look for [medications] here and can’t find them; they prefer to find ways to obtain them from the sub-region, especially in Togo, Burkina Faso, Ivory Coast, Senegal, Ghana, and possibly in Morocco, Algeria, the Maghreb countries. And for those who are wealthy and have connections, there are some who take them directly from France themselves too. (…) Many patients sometimes visit two or three pharmacies, and as soon as they don’t find the product, they give up and may wait two or three weeks before resurfacing.” (Healthcare Professional – Yves, 2022).
Unavailability of radiotherapy: the only solution of extraterritorial mobility
Like some countries in SSA, radiotherapy is not available in Benin and this prevents breast conservative surgery and comprehensive therapeutic management of cancers locally. Although the government is now working to bring radiotherapy to the country, the current unavailability of radiotherapy in the country means that women who can afford it are forced to continue their treatment abroad.
“There is no radiotherapy center in Benin. We had a radiotherapist, but since there was no radiotherapy center, this radiotherapist now works in a foreign country. So currently, we have neither a radiotherapy center nor a radiotherapist. Therefore, all patients who need radiotherapy must leave the country.” (Healthcare Professional – Emmanuel, 2022).
The training and placement of the first Beninese specialist doctors directly impact the mobility for radiotherapy abroad. Indeed, between 2010 and 2016, most medical evacuations for radiotherapy were to France, where most of the hospital-university staff were trained. Mali then became, in 2016 and 2017, a key destination for breast cancer patients. Mali had a functional radiotherapy machine since 2012. Subsequently, the recruitment of this Beninese radiotherapist in Ivory Coast in 2018 attracted most of the radiotherapy mobilities to the private Centre National d’Oncologie Médicale et de Radiothérapie Alassane Ouattara (CNRAO) in Abidjan. Since the opening of the private International Cancer Center in Lomé (Togo) in November 2022, a new partnership has been established with this neighboring country of Benin.
“I prefer to send them to Lomé because it’s closer, and it costs ten thousand francs at most for the trip. Whereas to Abidjan, you have to take a plane or a bus that takes days on the road. Most of the patients I have received have preferred to go to Lomé since it’s nearby.” (Healthcare Professional – Chantal, 2022).
However, most patients do not have the option to pursue this stage of treatment. Indeed, while radiotherapy treatment is extremely costly, the therapeutic mobility it entails comes with additional financial burdens and complex logistics. Yet, radiotherapy is fundamental to reducing the risk of recurrence.
“If a cancer requires radiotherapy and the patient is poor, it’s practically equivalent to a death sentence.” (Healthcare Professional – Emmanuel, 2022).
Thus, this is the main “knot” in cancer management in Benin, a “tragedy” that causes anxiety among patients.
“The woman you are treating and sending back into the world carries this sword of Damocles over her head in her daily life.” (Association Representative – Jeannette, 36, Cotonou, 2022).
Surgical reconstruction of the breast
Beninese women generally do not benefit from surgical breast reconstruction. Indeed, there are no plastic surgeons in Benin. However, plastic surgeons from Kuwait have made several missions to Benin to offer repair and reconstruction services. Nevertheless, all the women in our research who were offered reconstruction declined it. Women instead resort to external prostheses or tissue. Indeed, reconstruction represents a significant cost for a non-vital benefit, which demotivates women, even the wealthiest.
“The women who have had mastectomies; uh… I don’t know of any who have had breast reconstruction; just a few who are here, who came recently to get the [external] prosthesis, just two. Otherwise, they put cloth here to create harmony in their chest. Breast reconstruction is expensive. Already they struggle to undergo chemotherapy and complete the process. So, breast reconstruction is for affluent people! It’s for those… I don’t know any. Those who can do it just buy their external prosthesis.” (Healthcare Professional – Carine, 2022).
Additionally, women fear the surgery and particularly the impact of internal prostheses on their health.
“I thought about everything happening, we hear about the side effects, and I wonder if it’s worth it. I’m not yet 100% sure I will do it because of what they put inside… Will it not lead to other issues? I don’t know?” (Patient – Aure, 54, Cotonou, 2023).
Ultimately, many stated during interviews that they were unaware of the possibility of reconstruction.
Affordability and ability to pay
Major difficulty in following treatments
Benin’s current health insurance system is highly fragmented and does not cover a large proportion of the population. Several financial protection schemes coexist: contributory schemes covering civil servants, pensioners and formal sector employees; targeted fee exemptions; and voluntary community-based health insurance [20]. A previous report (2019) stated that only 8.4% of the population in Benin was covered by health insurance [21].
In 2019, the government launched a pilot project for Assurance pour le Renforcement du Capital Humain (ARCH). This project is part of the government’s efforts to provide a minimum package of basic social services to the most disadvantaged, with a view to achieving universal health coverage [22–24]. However, treatments for breast cancer are costly and inaccessible for the vast majority of patients. As a result, it is common for a patient to be unable to start treatment, and it is rare for a patient to complete her entire course of care.
“We realise that the leading cause of mortality here, whether from cancer or any other disease, is poverty and lack of access to care. We see everyday patients with curable diseases, cancers that we believe are curable, but we will lose them because the patients are too poor to access care or diagnosis.” (Healthcare Professional – Emmanuel, 2022).
Our observations and interviews with women and caregivers have allowed us to estimate the main direct costs of diagnosing and treating breast cancer in Cotonou (Table 3). These figures do not come from a quantitative or economic survey, but from a triangulation of our observations and interviews with caregivers and women. They may therefore vary over time and according to the place of care. They are given for illustrative purposes only.
Table 3.
Minimum direct costs of diagnosing and treating breast cancer in Cotonou, Benin
| FCFA | USD | |
| Ultrasound | 20,000 | 32 |
| Biopsy | 47,000 | 75 |
| CT scan | 163,000 | 261 |
| Chemotherapy (1) | 768,000 | 1,229 |
| Surgery (2) | 259,000 | 414 |
| Radiotherapy (3) | 2,725,000 | 4,360 |
| Hormonal therapy (one month) | 7,000 | 11 |
| Trastuzumab (per dose) | 1,250,000 | 2,000 |
| Details | ||
| (1) Chemotherapy | ||
| Pre-chemotherapy blood tests | 18,500 | 30 |
| Prescription chemotherapy products* | 32,000 | 51 |
| Chemotherapy consultation | 13,500 | 22 |
| Post chemotherapy prescription** | 32,000 | 51 |
| Total for a cycle of chemotherapy | 96,000 | 154 |
| Total if 8 cycles | 768,000 | 1,229 |
| (2) Surgery (mastectomy + curage) | ||
| Surgical procedure | 84,000 | 134 |
| Anaesthesia | 60,000 | 96 |
| Stay in intensive care*** | 15,000 | 24 |
| Hospitalization**** | 35,000 | 56 |
| Products (prescriptions) | 65,000 | 104 |
| Total surgery | 259,000 | 414 |
| (3) Radiotherapy | ||
| 25 sessions***** | 1,875,000 | 3,000 |
| Preparation | 300,000 | 480 |
| Airline tickets | 300,000 | 480 |
| Accommodation (1 month) | 250,000 | 400 |
| Total cost of conventionnally fractionated radiotherapy | 2,725,000 | 4,360 |
*if anthracycline-based chemotherapy
**to prevent side-effects
***if less than 24 hours and oxygen
****cheapest room at 7000/night; estimate 5 nights (= the minimum)
*****75,000 FCFA per session and 25 sessions required
For a woman with breast cancer, the minimum cost of standard treatment (surgery and chemotherapy) is 1,257,000 FCFA (2 011 USD) without radiotherapy and 3,982,000 FCFA (6 371 USD) with radiotherapy in Abidjan (Table 3). If the woman’s tumour has hormone receptors, she can then have hormone treatment to prevent the tumour coming back. Hormonal therapy, costing 7,000 FCFA per month, is more accessible but, unfortunately, not suitable for all patients. Treatment with trastuzumab is needed to improve survival in another type of breast cancer (HER2+) but one dose of trastuzumab, the basic molecule for targeted therapy, costs 1,250,000 FCFA. A patient needs 12 to 18 doses of trastuzumab. In comparison, the guaranteed minimum interprofessional wage (SMIG), which applies to a minority of Beninese, is 52,000 FCFA for 40 hours of work per week.
Individual care dictated by financial resources: breast cancer as a major health inequality
Health professionals are forced to adapt the treatment of each woman to her financial means, making breast cancer a major health inequality. Consequently, specific tests are sometimes omitted, which directly impacts care. For example, some women do not undergo histopathological and immunohistochemical tests, which are essential for determining the type of cancer and for selecting the appropriate therapeutic protocol. Most healthcare professionals surveyed in our study believe that health education influences patients’ individual choices regarding the financial sacrifices they are willing to make for the benefits of these diagnostic tests and evaluations.
“When we don’t explain to them the importance of the pathology test for further treatment, [the importance] of knowing the histological type or whatever, the patient quietly doesn’t bother to pay for the test!” (Healthcare Professional – Murielle, 2023).
Moreover, the differences in resources among patients are strongly felt in the timeliness of care and then in the consistency of long-term follow-up for this chronic disease.
“Due to a lack of funds to buy products, they are forced to miss appointments. It is only when they find the money that we can reschedule them to come back for treatment.” (Healthcare Professional – Justine, 29, 2022).
During fieldwork, we observed frequent interruptions in treatment, with some women having no financial capacity after the first two or three cycles of chemotherapy.
Indebtedness and long-term family impacts
Breast cancer is a disease that causes significant biographical ruptures. One of the primary consequences is the near-systematic loss of employment for patients.
“I was a secretary at a university. But when the illness began, I had to quit because of the treatments. They themselves told me: ‘Well madam, you know this is a private institution, so we can’t keep granting you permissions’. So, I had to stop.” (Patient – Janelle, 48, Cotonou, 2024).
To obtain treatment, many women have had to liquidate their savings, sell their land, take their children out of school, incur debt, or beg. They are forced to “destroy many things” to survive (Patient – Nadia, 54, Cotonou, 2023).
“I ask, I beg; I stay where there is the Camp Guezo pharmacy, I ask people, and they help me, and I go buy the medicines at the pharmacy ‘.” (Patient – Nadia, 54, Cotonou, 2023).
“No, I have already taken my daughter out of school because I can’t afford it anymore. So I told her to go into an apprenticeship. The eldest is also in an apprenticeship. So only the youngest goes to school” (Patient – Soma, 59, Abomey-Calavi, 2023).
“She bought a house, and they were living in it. And because of the illness, they sold the house to go for radiotherapy in Ghana. (…) At one point, they could no longer pay the rent. They became homeless.” (Healthcare Professional – Jean, 2022).
State financial support based on commission studies, association assistance, and the importance of social capital
As mentioned above, project for universal health coverage is underway in Benin. In the meantime, the Beninese government has implemented a support system for civil servants and for the very poor (ARCH), based on a commission study. This support applies to medical evacuations outside the country when treatments are not available in Benin.
“The Beninese government will assist two types of patients: those who are employees of the Beninese state, for whom the government will systematically try to provide help. Then there are the indigent patients; the Beninese state will also try to help them, but it is more difficult given the budget constraints…” (Healthcare Professional – Emmanuel, 2022).
However, the President of the Republic of Benin, Patrice Talon, publicly stated in 2018, during a meeting with the Islamic Union of Benin, that these medical evacuations would be prohibited in the coming years to invest in the country’s healthcare infrastructure [25]. In fact, these medical evacuations primarily benefit a very small elite while placing a heavy burden on the Beninese taxpayer [26]. The goal is to gradually stop these evacuations by making all oncology care possible within Benin.
For patients who do not have access to state support, their care relies on their social capital, meaning it depends on their husbands, family, friends, colleagues, and neighbors. No patient in our study was able to finance their treatments alone. Moreover, associations such as Rotary and SOS Cancer attempt to support some women financially. Unfortunately, most of very poor patients do not receive assistance due to the lack of budgets from these associations.
Appropriateness and ability to engage
An imposed autonomy of patients accompanied by a loss of opportunity
The lack of a structured care pathway for women with breast cancer in Benin puts them in difficult situations and forces them to fend for themselves, often relying on the support of family and women from their community who have faced similar battles. For example, women must transport their samples to testing centers themselves or obtain chemotherapy drugs.
“My husband and I brought the sample home in my fridge! So, every day I open the fridge, see my sample and talk to it, saying ‘Listen, don’t disappoint me.” (Patient – Jeannette, 36, Cotonou, 2022).
Healthcare professional Romeo explains that the risk for a patient who must bring their own biopsy sample to the pathologist is that “they may keep the specimen with them or throw it away or do something else. In any case, they do not take the specimen to the lab.” (2023).
“In June 2016, I agreed to do it, and they removed the lumps; there were just two or three small lumps. Then they put them in a small vial and asked me to have it analysed. Out of ignorance and naivety, I left it and said, ‘Well, I have nothing’. I abandoned the vial. A few months later, seven, eight, or nine months later, the nodules had grown back stronger. So, when I recontacted him [the doctor], he said: ‘If you don’t do the analysis, don’t come see me’.” (Patient – Manon, 42, Cotonou, 2024).
The gradual structuring of training in breast cancer care
For about a decade, breast cancer care has been gradually structured around increasingly experienced healthcare professionals trained in gynecological oncology. Indeed, whereas organ specialists (visceral surgeons, obstetric gynecologists) handled cancers in the past, today, more and more medical professionals specialise in oncology.
“We are among the first properly trained oncologists returning to Benin. Previously, oncology was more practiced with organ specialists.” (Healthcare Professional – Richard, 2022).
Although specialised training in oncology or radiotherapy is still not fully available in Benin. Physicians are going abroad for training or can supplement their specialty training with additional courses in oncology. A Joint University Diploma in gynecological and breast oncology was established in 2019 at the Faculty of Health Sciences in Cotonou, aimed at training gynecologists, surgeons, and palliative care professionals in the medical management of gynecological and breast cancers. The establishment of a University Diploma in anticancer chemotherapy and a Specialist Diploma (Diplôme d’Études Spécialisées, DES) in oncology is also anticipated.
Additionally, growing medical collaborations, particularly through the organisation of conferences and forums, are contributing to the improvement of care, knowledge sharing, and the formalisation of therapeutic consensus. Multidisciplinary team meetings (RCP) have been initiated in Benin to enhance breast cancer management, allowing healthcare professionals to collaborate and pool resources on a national scale.
“In Cotonou, you can imagine that we have a few oncologists, but in the north of the country, there is a problem. They have a university hospital, but they don’t have specialists. And in areas without a university hospital, it’s even worse. Benin has 6,000 cancer cases each year. If all 6,000 cases have to come to CNHU in the small service you saw, we cannot manage. A digestive surgeon with 30 years of service in the north knows very well how to perform a digestive organ resection, but maybe he needs a little help knowing when to operate, when to use chemotherapy, what techniques to apply. We can offer that through discussions in RCP.” (Healthcare Professional – Lionel, 2023).
Medical cooperation in Benin through RCPs, but more broadly in the SSA region, aims to disseminate harmonised guidelines from the National Comprehensive Cancer Network (NCCN) for SSA. These guidelines enable healthcare professionals in these countries to implement the treatment plans most suited to their specific contexts.
“In multidisciplinary meetings, with medical oncologists, radiotherapists, and everyone present, the appropriate protocol is often indicated, but we adjust it based on what we have.” (Healthcare Professional – Marius, 2023).
Finally, the emergence of a new generation of oncology specialists enables the establishment of dedicated oncology services, such as recently at the CHU-MEL. Furthermore, a new hospital—the International Hospital Center of Calavi (CHIC)—will open in 2025 with an oncology service equipped with radiotherapy facilities.
Palliative care that supports women with cancer
As we have seen, women with breast cancer face multiple barriers to accessing care, with sometimes inadequate or incomplete treatments, which explains the rapid recourse to palliative care in Benin.
“It’s when it’s completely incurable and everything that they approach doctors who, at that moment, sometimes refuse to operate on them, so we place them under palliative care.” (Association Representative – Jeannette, 36, Cotonou, 2022).
Palliative care is a priority area in Benin. In September 2018, the Beninese government adopted the Five-Year Plan for Palliative Care (PQSP) and subsequently created the National Palliative Care Program (PNSP) in 2019. With this government initiative, Benin became the first country in French-speaking Africa to implement a palliative care program and national plan integrated into the country’s health system, following the WHO recommendation WHA67-19 issued at the 67 th World Health Assembly (2014).
This program, part of the Beninese government’s reform of medical evacuations abroad, aims to improve the quality of life of people suffering from cancer and other potentially fatal diseases [27]. Nearly 90% of palliative care patients in Benin are cancer patients [28]. Thus, palliative care currently represents the most accessible form of breast cancer management in Benin, particularly in the absence of a funded and effective National Cancer Plan.
Moreover, in 2015, the Beninese Association for Palliative Care (ABSP) was established, offering a holistic approach that addresses the physical, emotional, spiritual, and social needs of patients, and at a low cost. The association is gradually spreading its model by providing support for the opening and operation of palliative care units established by the PNSP throughout the country, particularly through mobile home visit teams. It also participates in the establishment of training programs in palliative care, notably with the creation of a master’s program in Palliative Care at the National Medical and Health Institute of the University of Abomey-Calavi in 2021.
Discussion
This study reveals interconnected and persistent barriers to access to cancer care in Benin, linked to socio-cultural and structural challenges. Oncology care in Benin is characterised by late detection of breast cancer, reluctance of women to undergo mastectomy, lack of specialised personnel, limited technical facilities and high costs of treatment, which make access to care unaffordable for the majority of patients. Most of these factors are not specific to Benin but are common to many SSA countries. Indeed, a systematic review of the literature examined the health system factors that influence the time between diagnosis and start of treatment in women with breast cancer in SSA [29]. Among the barriers identified, misdiagnosis, misinterpretation and mismanagement were the most common, followed by provider attitudes (inappropriate attitudes, strikes and corruption) and the high cost of medical investigations and treatment. Geographical inaccessibility to healthcare and lack of diagnostic centres and oncology-qualified staff were among the infrastructure problems. The systematic review [29] concluded that policymakers in SSA need to address the issue of affordability of breast cancer care through appropriate universal health coverage policies and strengthen the clinical skills of health professionals to ensure timely diagnosis and appropriate care for women with breast cancer in this region. In this regard, there is a need to develop knowledge transfer activities in Africa to inform policymakers and stakeholders through evidence-based data [30].
Our research did, however, reveal certain specific features of Benin or the region.
Oncology healthcare professionals, including midwives, must continue to be trained
Our study revealed a shortage of healthcare professionals with oncology training at all levels, including pharmacists, nurses, and doctors but indicated that midwives can play a pivotal role in the early diagnosis of breast cancer as primary care health professionals. The particularly young age of women with breast cancer in Benin and women’s high fertility [9] means that they are often close to pregnancy, childbirth or breastfeeding at the first sign of the disease and are often attended by midwives who can refer them first. This is not specific to Benin - the same was found in Mali [31] - but it is very specific to the region. The government must be aware of the potential of midwives in the fight against breast cancer in Benin and involve them in health policies.
Migrating to seek treatment
The need to migrate within and outside the country to access care was very present in the interviews for this research. International mobility for cancer treatment is extremely common in SSA. A survey of health professionals found that over 90% knew cancer patients who had travelled abroad for treatment, and 75% had referred patients abroad themselves. It should be noted that most respondents were in East Africa, and that the most commonly cited destination for ‘medical tourism’ was India. The most common reason cited was the perception of a higher quality of care in foreign health facilities. This was closely followed by mistrust of the local health system and the social prestige or affluence associated with international treatment [32].
In West Africa, cancer treatment facilities and patient international flows are evolving very rapidly. For many years, Mali was a place of inward therapeutic mobility thanks to the presence of a radiotherapy unit in Bamako, but the closure of the radiotherapy unit for more than two years (August 2022 - October 2024) due to maintenance problems and restructuring of the premises has redirected the flow of patients [31, 33]. We have also seen in this article that, for many years, Benin sent its patients for radiotherapy to France, then to Côte d’Ivoire and Togo, and that the imminent opening of a high-tech hospital is very likely to reduce this outflow and even attract new inflows to the country.
However, our research also highlights the constraints within the country itself with care concentrated in the capital. In Burkina Faso, a study of children with cancer shows the same difficulties in accessing care for families [34]. The number of stages in the care process increases with distance from the capital. Travelling within the country for treatment is a source of suffering for patients and their families. There is an urgent need to decentralise oncological care in Benin.
Beninese government invests heavily in infrastructure
The construction of a new international hospital 20 km from Cotonou, scheduled to open in 2025, demonstrates the government’s commitment to improving healthcare standards. The CHIC hospital will be equipped with the necessary technical resources to treat cancer patients. A key concern for the local community is to identify the intended population for the hospital and to ensure that it is accessible to all, particularly the most vulnerable. It has been found that the current and long-term costs of new facilities have been underestimated in LMICs. This is particularly the case in relation to maintenance, human and material resources, and training, which are required to guarantee safe and affordable services [35]. There is a great deal of optimism among the public with regard to this hospital and the prospect of comprehensive cancer treatment in Benin. However, this also highlights the hospital-centred approach to health in Benin and may mask other factors necessary to combat breast cancer.
The need to get back to basics: strengthening civil society and raising awareness among women
Our SENOVIE research in several LMICs (Mali, Benin, Cambodia) has shown that women arrive at a very advanced stage of the disease with little knowledge about breast cancer and its treatment (www.senovie.org). At this stage of our findings, we believe it is necessary to go back to the grassroots of public health by strengthening civil society [36] and testing different community interventions to increase women’s knowledge and ability to act in the face of this problem.
Despite the high visibility of Pink October in Cotonou, Benin, with numerous awareness-raising events, civil society remains under-mobilised on this issue and lacks the necessary resources and financial and moral support. Breast cancer is a topic that is often avoided in Benin, and there is no direct translation for the term in the country’s majority language, Fongbé. Communication between healthcare professionals and the population can be challenging in African countries where there is a lack of alignment between biomedical terminology and popular representations [37]. In the field of cancer, African languages sometimes use terminologies that may contribute to fear, health disparities, and barriers to care, which in turn pose communication difficulties for health professionals [38]. Cancer associations can play a significant role in combating treatment-related stigma by destigmatising breast cancer and providing women with comprehensive information and support throughout their treatment journey [39].
A survivors’ association, SOS Cancer, was founded in 2016 and leads awareness campaigns on female cancers (cervical and breast) in Benin. The association’s primary goal is to create a “support forum” where women can share helpful information about their care and openly discuss the “taboo” of breast cancer, as they see it, in their country. The survivors of SOS Cancer provide support, moral encouragement, and hope to those fighting the disease. The association engages in several activities: when possible, they organise awareness campaigns, provide training on self-examination, and donate prostheses. It should be noted, however, that this association is not very active at present, particularly following the successive deaths of its last two presidents.
A systematic review highlights that in LMICs, community health workers (CHWs) have also a role to play in raising awareness and providing education, taking histories and performing clinical breast examinations, making referrals and helping people access specialist services, and providing follow-up care in the community. However, there is a need to provide details of CHWs training programmes for breast cancer detection, as well as the financial implications of such an approach [40]. While we have previously documented the beneficial role of a highly active patient association in Mali, which successfully mobilised policy makers and raised awareness among women [31, 39], our research in Benin underlines the urgent need to strengthen civil society around breast cancer in Benin and to develop a community-based approach.
Limitations and strengths
The qualitative design allows us to gain a comprehensive and detailed understanding of the topic. The conceptual framework proposed by Levesque et al. [16] proved invaluable in analysing and ordering our results. The a posteriori use of the framework was instrumental in elucidating the discrepancy between the supply and demand of access to care, with the former being more heavily represented in the results. The costs we have given for breast cancer treatment are indicative and are not based on a quantitative sample but are the result of a triangulation between our observations in the departments and our interviews with women and carers.
One of the strengths of the study is that the results of this research have been presented to healthcare professionals in Cotonou. Our collective understanding of the challenges that need to be addressed in terms of access to oncology care serves to reinforce these findings.
Conclusion
This article demonstrates the existence of interconnected and persistent barriers to access to cancer care in Benin, which are linked to structural, socio-cultural and financial challenges. Late detection of breast cancer, due to a lack of systematic screening and unequal access to information, contributes to the low survival rate in the country. In addition, deeply rooted socio-cultural beliefs, such as a mystical view of breast cancer and the perception of mastectomy as an attack on femininity, steer many patients towards traditional medicine and hinder acceptance of medical treatment. Structurally, the treatment pathway is marked by a shortage of specialised professionals, limited technical facilities and the centralisation of care in Cotonou, forcing many patients to travel long distances to access services. The unavailability of certain essential medicines, which are frequently out of stock, exacerbates the situation by making it difficult to continue treatment. In addition, the high cost of treatment makes access to care unaffordable for most patients, leading to frequent dropouts and loss to follow-up. However, the Beninese government has recently demonstrated its commitment to tackling cancer but should not forget to work hand in hand with civil society to raise awareness in communities.
Supplementary Information
Acknowledgements
We thank the SENOVIE research group which associates Clémence Schantz (scientific leader), Moufalilou Aboubakar, Myriam Baron, Gaëtan Des Guetz, Anne Gosselin, Hamidou Niangaly, Valéry Ridde, Luis Teixeira, Bakary Abou Traoré (coscientific leaders), Emmanuel Bonnet, Fanny Chabrol, Abdourahmane Coulibaly, Justin Lewis Denakpo, Annabel Desgrées du Loû, Kadiatou Faye, Freddy Gnangnon, Pascale Hancart Petitet, Joseph Larmarange, Dolorès Pourette, Léa Prost, Beauta Rath, Julie Robin, Hélène Sacca Robin, Priscille Sauvegrain, Angéline Tonato Bagnan and Alassane Traoré.
Authors’ contributions
CS initiated this research and has obtained funding. FG, MAb, AKA, ATA recruited the respondents and made the observations possible. GF, MAb, AKA, JLD, ATB and HRS coordinated the fieldwork. CS, MAg, LL, MB, LT and PP collected the data. CS and PP analysed the data. CS, GF, MAb, AKA, JLD, ATB, LT and PP were involved in interpreting the results through two workshops. LT and VR were involved every step of the way. CS and PP wrote the first version of the article, which all coauthors amended and improved. All authors validated the final version of the article.
Funding
This work benefitted from financial support from the Institut National du Cancer (INCa) (DA N°2022-135 SCHANTZ); the French Collaborative Institute on Migration, coordinated by the CNRS under the reference ANR-17- CONV-0001; the Institut de Recherche pour le Développement (IRD); the Ceped UMR 196; and the Cité du Genre, IdEx University of Paris, ANR-18-IDEX-0001. The GIS Institut du Genre and the MSH Paris Nord also provided financial support for this research.
Data availability
The datasets generated and analysed in the current study are not publicly available due to their sensitive nature and the fact that the interviews are pseudonymised but not fully anonymised. However, they are available from the corresponding author upon reasonable request.
Declarations
Ethics approval and consent to participate
The study was conducted in accordance with the Declaration of Helsinki. Ethical approval for the study was obtained from the Comité d’Éthique de la Recherche en Sciences de la Santé (CER-SS) on 14 December 2022—Decision N°010/2022/CER-SS. To guarantee the anonymity of participants, pseudonyms were assigned to the patients interviewed. Given the ease of identification in this restricted professional environment, we used the term “healthcare professional” without specifying gender or age for caregivers. Informed consent to participate was obtained from all of the participants in the study.
Consent for publication
Not applicable.
Competing interests
One of the co-authors, Luis Teixeira, has been employed as Medical Director at the Centre Hospitalier International de Calavi since September 2024.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Clémence Schantz, Email: Clemence.schantz@ird.fr.
the SENOVIE group:
Clémence Schantz, Freddy Houéhanou Rodrigue Gnangnon, Moufalilou Aboubakar, Justin Lewis Denakpo, Angéline Tonato Bagnan, Hélène Robin Sacca, Luis Teixeira, Valéry Ridde, Myriam Baron, Gaëtan Des Guetz, Anne Gosselin, Hamidou Niangaly, Bakary Abou Traoré, Emmanuel Bonnet, Fanny Chabrol, Abdourahmane Coulibaly, Annabel Desgrées du Loû, Kadiatou Faye, Pascale Hancart Petitet, Joseph Larmarange, Dolorès Pourette, Léa Prost, Beauta Rath, Julie Robin, Priscille Sauvegrain, and Alassane Traoré
References
- 1.Bray F, Parkin DM, Gnangnon F, Tshisimogo G, Peko JF, Adoubi I, et al. Cancer in sub-Saharan Africa in 2020: a review of current estimates of the national burden, data gaps, and future needs. Lancet Oncol. 2022;23(6):719–28. [DOI] [PubMed] [Google Scholar]
- 2.Global Cancer Observatory. Breast. IARC/OMS; 2022. https://gco.iarc.fr/today/en/fact-sheets-cancers.
- 3.Coles CE, Anderson BO, Cameron D, Cardoso F, Horton R, Knaul FM, et al. The Lancet Breast Cancer Commission: tackling a global health, gender, and equity challenge. Lancet. 2022;399(10330):1101–3. [DOI] [PubMed] [Google Scholar]
- 4.Limenih MA, Mekonnen EG, Birhanu F, Jima BR, Sisay BG, Kassahun EA, et al. Survival patterns among patients with breast cancer in sub-Saharan Africa: a systematic review and meta-analysis. JAMA Netw Open. 2024;7(5):e2410260. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.McKenzie F, Zietsman A, Galukande M, Anele A, Adisa C, Parham G, et al. Drivers of advanced stage at breast cancer diagnosis in the multicountry African breast cancer - disparities in outcomes (ABC-DO) study. Int J Cancer. 2018;142(8):1568–79. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.WHO. The Global Breast Cancer Initiatives - Empowering women, building capacity, providing care for all. Geneva, Switzerland; 2022. p. 3. https://www.who.int/initiatives/global-breast-cancer-initiative.
- 7.WHO. The Global Breast Cancer Initiative Implementation Framework - Assessing, strengthening and scaling up services for the early detection and management of breast cancer. Geneva: WHO; 2023 p. 118. Disponible sur: https://www.who.int/initiatives/global-breast-cancer-initiative. Cité 5 août 2024.
- 8.Lombe DC, Mwamba M, Msadabwe S, Bond V, Simwinga M, Ssemata AS, et al. Delays in seeking, reaching and access to quality cancer care in sub-Saharan Africa: a systematic review. BMJ Open. 2023;13(4):e067715. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Institut National de la Statistique et de l’Analyse Économique (INSAE), ICF. Enquête Démographique et de Santé au Bénin, 2017-2018. Cotonou, Bénin et Rockville, Maryland, USA : INSAE et ICF.; 2019. p. 675. Disponible sur: https://dhsprogram.com/publications/publication-FR350-DHS-Final-Reports.cfm. Cité 23 avr 2019.
- 10.World Bank. World Bank. 2024. Bénin - Vue d’ensemble. Disponible sur: https://www.banquemondiale.org/fr/country/benin/overview. Cité 5 août 2024.
- 11.Global Cancer Observatory. Benin. IARC/OMS; 2022. https://gco.iarc.fr/today/en/fact-sheets-populations#countries.
- 12.Gnangnon FHR, Parenté A, Aboubakar M, Kiki-migan Y, Totah T, Gbessi DG, et al. Prognostic factors and overall survival of breast cancer in Benin: a hospital-based study. BMC Womens Health. 2024;24(1):295. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Giaquinto AN, Sung H, Miller KD, Kramer JL, Newman LA, Minihan A, et al. Breast cancer statistics, 2022. CA Cancer J Clin. 2022;72(6):524–41. [DOI] [PubMed] [Google Scholar]
- 14.Deluche E, Antoine A, Bachelot T, Lardy-Cleaud A, Dieras V, Brain E, et al. Contemporary outcomes of metastatic breast cancer among 22,000 women from the multicentre ESME cohort 2008–2016. Eur J Cancer Oxf Engl. 1990;2020(129):60–70. [DOI] [PubMed] [Google Scholar]
- 15.Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care J Int Soc Qual Health Care. 2007;19(6):349–57. [DOI] [PubMed] [Google Scholar]
- 16.Levesque JF, Harris MF, Russell G. Patient-centred access to health care: conceptualising access at the interface of health systems and populations. Int J Equity Health. 2013;12(1):18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Cu A, Meister S, Lefebvre B, Ridde V. Assessing healthcare access using the Levesque’s conceptual framework- a scoping review. Int J Equity Health. 2021;20(1):116. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Palinkas LA, Horwitz SM, Green CA, Wisdom JP, Duan N, Hoagwood K. Purposeful sampling for qualitative data collection and analysis in mixed method implementation research. Adm Policy Ment Health Ment Health Serv Res. 2015;42(5):533–44. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Weber M. Economie et Société 1. Les catégories de la sociologie. Pocket: Paris; 1995. p. 416. [Google Scholar]
- 20.Paul E, Sambiéni NE, Wangbe JP, Fecher F, Bourgeois M. Budgeting challenges on the path towards universal health coverage: the case of Benin. Health Econ Rev. 2020;10(1):28. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Présidence de la République du Bénin. Assurance pour le Renforcement du Capital Humain (ARCH). Bénin; 2019. p. 17.
- 22.République du Bénin. Assurance pour le Renforcement du Capital Humain (ARCH). 2017. p. 45.
- 23.République du Bénin. Décret portant sur les modalités de mise en oeuvre de l’assurance maladie obligatoire en République du Bénin. 327 du 21 juin 2023. https://sgg.gouv.bj/doc/decret-2023-327/.
- 24.Gnammou J, Sambieni NE, Bourgeois M. L’Assurance maladie du programme ARCH au Bénin : conception, gouvernance et défis de pérennisation. Afr Contemp. 2025;1(279):39–57. [Google Scholar]
- 25.Face à la communauté musulmane, Patrice Talon parle des évacuations sanitaires. 2018. Disponible sur: https://www.youtube.com/watch?v=5K8h87n7wAo. Cité 27 janv 2022.
- 26.Amoussou-Guenou KM, Fachinan OH, Gbénou S, Komongui DG, Houndétoungan GD. Place de la scintigraphie et de la radiothérapie dans les évacuations sanitaires hors du Bénin de 2006 à 2010. Médecine Nucl. 2013;37(10–11):507–10. [Google Scholar]
- 27.Ministère de la santé République du Bénin. Plan quinquennal soins palliatifs au Bénin 2022-2026. 2022. p. 79.
- 28.Agbodande KA, Prudencio RDTK, Gnintoungbe S, Sowanou AKV. Sociodemographic characteristics and identified needs among patients followed in palliative care units in the Republic of Benin. Hosp Palliat Med Int J. 2019;3(2):32–5. [Google Scholar]
- 29.Gbenonsi G, Boucham M, Belrhiti Z, Nejjari C, Huybrechts I, Khalis M. Health system factors that influence diagnostic and treatment intervals in women with breast cancer in sub-Saharan Africa: a systematic review. BMC Public Health. 2021;21(1):1325. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Robin J, Schantz C, Ly M, Traoré BA, Faye K, Dancoisne A, et al. Knowledge transfer interventions on cancer in Africa and Asia: a scoping review. BMC Cancer. 2025;25(704):1–15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Schantz C, Coulibaly A, Traoré A, Traoré BA, Faye K, Robin J, et al. Access to oncology care in Mali: a qualitative study on breast cancer. BMC Cancer. 2024;24(1):81. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Rubagumya F, Carson L, Afolayan D, Rugengamanzi E, Nnko GA, Abdihamid O, et al. Medical tourism for cancer treatment: trends, trajectories, and perspectives from African countries. JCO Glob Oncol. 2024;10:e2400131. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Schantz C, Diarra I, Traoré A, Traoré BA, Chabrol F, Sogoba S. Radiothérapie et lutte contre les cancers : défis de maintenance de l’unique accélérateur linéaire à l’Hôpital du Mali. Santé Publique. 2022;34(3):425–8. [DOI] [PubMed] [Google Scholar]
- 34.Arcens Somé MT, Nikiema A. Explorer les parcours thérapeutiques des enfants atteints de cancer au Burkina Faso. EchoGéo. 2024;(70). Disponible sur: https://journals.openedition.org/echogeo/28182. Cité 20 janv 2025.
- 35.Chabrol F, Albert L, Ridde V. 40 years after Alma-Ata, is building new hospitals in low-income and lower-middle-income countries beneficial? BMJ Glob Health. 2019;3(Suppl 3):e001293. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.WHO. Voice, agency, empowerment - handbook on social participation for universal health coverage. Geneva: World Health Organization; 2021. p. 252. [Google Scholar]
- 37.Jaffré Y, de Sardan JPO. La Construction sociale des maladies, les entités nosologiques populaires en Afrique de l’Ouest. Paris: Presses Universitaires de France - PUF; 1999. p. 376. [Google Scholar]
- 38.Simba H, Mutebi M, Galukande M, Mahamat-Saleh Y, Aglago E, Addissie A, et al. Cancer care terminology in African languages. JAMA Netw Open. 2024;7(8):e2431128. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Schantz C, Coulibaly A, Faye K, Traoré D. Amazons in Mali? Women’s experiences of breast cancer and gender (re)negotiation. Soc Sci Med. 2024;348:116874. [DOI] [PubMed] [Google Scholar]
- 40.O’Donovan J, Newcomb A, MacRae MC, Vieira D, Onyilofor C, Ginsburg O. Community health workers and early detection of breast cancer in low-income and middle-income countries: a systematic scoping review of the literature. BMJ Glob Health. 2020;5(5):e002466. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The datasets generated and analysed in the current study are not publicly available due to their sensitive nature and the fact that the interviews are pseudonymised but not fully anonymised. However, they are available from the corresponding author upon reasonable request.