Abstract
The HEALing (Helping to End Addiction Long-TermSM) Communities Study (HCS) tests the effectiveness of the Communities That HEAL intervention in decreasing opioid overdose deaths in 67 communities across four states. This intervention enlists a collaborative team of researchers, academic experts, and community coalitions to select and implement interventions from a menu of evidence-based practices, which include medications for opioid use disorder (MOUD). The New York team of the HCS developed an integrated network systems (INS) approach with a mapping tool for coaching coalitions in the selection of strategies for enhancing medication treatment. INS is a data and community-driven coaching tool where the coalitions develop a map of service delivery venues in their local community to better engage people with medication treatment wherever they may present. The map is structured around “core” services that can provide maintenance MOUD, and “satellites” which include the full range of settings where people with opioid use disorder are encountered and can be identified, possibly initiated on medication, and referred to core programs for ongoing MOUD care. This paper describes the rationale for the INS mapping tool with a discussion framed by the consolidated framework for implementation research and provides a case example of its application.
INTRODUCTION
Medications for opioid use disorder (MOUD) approved by the U.S. Food and Drug Administration (FDA) —methadone, buprenorphine, and extended-release naltrexone—have overwhelming evidence for their efficacy in reducing non-medical opioid use, improving health and psychosocial functioning, and for methadone and buprenorphine, reducing opioid overdose deaths (1–9). However, most individuals with opioid use disorder have never been treated with MOUD and those who do initiate MOUD often do not stay in treatment beyond the first few months (10–12). Despite the importance of improving MOUD access, linkage, engagement, and treatment retention in addressing the overdose crisis (13, 14), implementation initiatives are hindered by the varied and significant barriers to improving MOUD provision, which include negative attitudes toward MOUD and people with opioid use disorder, lack of prescribers, lack of funding for services, and restrictive state and federal regulations (15, 16).
The HEALing (Helping to End Addiction Long-TermSM) Communities Study (HCS) is a multi-site, parallel-group, cluster randomized, wait-list controlled trial engaging communities (n = 67) with a high burden of overdose deaths in Kentucky, Massachusetts, New York, and Ohio. In New York (NY), each “community” consists of a county or municipality that has among the highest burden of opioid overdoses outside of New York City. HCS is designed to test the Communities That HEAL intervention which aims to reduce opioid overdose deaths by at least 40% (17–19).
HCS aims to introduce or expand on three required categories of evidence-based practices that are specified through a “menu” in the opioid-overdose reduction continuum of care approach (20). The MOUD menu of practices is further divided into three MOUD submenus: 1) expanding treatment availability, 2) linkage to services, and 3) patient engagement and retention. In each selected community, a coalition consisting of a broad range of stakeholders, including MOUD and other service providers, local county government leadership, law enforcement, and people with lived/living experience (21), is tasked with selecting and implementing these evidence-based practices.
In NY, the study hires a locally recruited implementation team for each county consisting of a program manager for oversight, community engagement facilitator focused on partner collaboration, technical assistance coordinator to facilitate capacity building, and data coordinator to facilitate data-driven decisions. Community-driven approaches are supported through external facilitation or “coaching” to the community coalitions provided by an external academic team of researchers with expertise in implementation science and substance use disorder treatment (22, 23).
As the research team in NY began their external facilitation with the community coalitions and implementation teams, the integrated network systems (INS) approach was developed as a coaching strategy with a mapping tool to help coalitions select evidence-based strategies (24) for expanding MOUD provision and uptake. INS encourages communities to envision a comprehensive, community-wide network such that wherever people with opioid use disorder are encountered in the community there is capacity for identification, referral to treatment, and a network of clinicians to adequately provide MOUD. Herein, we describe INS and its development as a strategy to identify partners for referral and linkage to MOUD and other services across the eight NY communities participating in wave 1 of HCS. We also present a case example of applying this approach with one of those communities. We frame our discussion using the domains specified in the consolidated framework for implementation research, which combines a range of smaller implementation theories into a comprehensive framework to link implementation practices to outcomes and has been used in a variety of contexts to evaluate implementation approaches (25, 26).
METHODS
Overview of the HEALing Communities Study in New York
In HCS, funded by the National Institute on Drug Abuse as part of the National Institutes of Health HEAL InitiativeSM and described in detail elsewhere (17, 19), communities are randomized to the active two-year intervention beginning in year 1 (wave 1), or the wait-list control, which starts the intervention in year 3 (wave 2). Wave 1 has been completed and wave 2 began on July 1, 2022. This study protocol (Pro00038088) was approved by the HCS single site Institutional Review Board, Advarra Inc. (ClinicalTrial.gov Identifier: NCT04111939).
HCS uses community engagement, described in detail elsewhere (21), that proceeds through seven phases with goals ranging from the initial recruitment and training of a coalition of community stakeholders to oversee the intervention locally to the final phase which addresses the sustainability of strategies and core components implemented during the study (24). INS was developed in NY to assist with external facilitation in phase 4 (community action planning, when goals are set and strategies are selected) and phase 5 (implementation and monitoring) of HCS in response to challenges encountered when coaching the diverse NY counties on enhancing linkage to and delivery of MOUD.
During phases 4 and 5 in NY, strategies for implementing or enhancing evidence-based practices were broadly outlined in action plans and then further detailed in implementation plan agreements (24, 27) between the county coalition and the local partner organizations (e.g., clinical services, peer organizations, law enforcement) that would implement these strategies. These agreements specify precise details such as roles of partners, measures to track progress, milestones, anticipated challenges with proposed responses, and focus populations. Strategies for each menu category are further refined in workgroups that consist of the local implementation team, local experts and service providers, and study team members. Further detail on the study-wide action planning and implementation process can be found in Young et al., 2022 (24).
In the NY site of HCS, community leadership is emphasized by hiring implementation team members into the local health or mental health department and having them report to their respective commissioners. Local champions (28) for each menu category have varied roles which include advocating for evidence-based practices, planning community events, and strengthening stakeholder relationships. Data and resources are exchanged from the study team to community stakeholders through regularly scheduled and ad hoc meetings, phased communication campaigns (29), technical assistance requests, and web-based data visualizations for communicating community metrics to the counties called “dashboards” (30).
The INS Approach for Community Implementation of MOUD
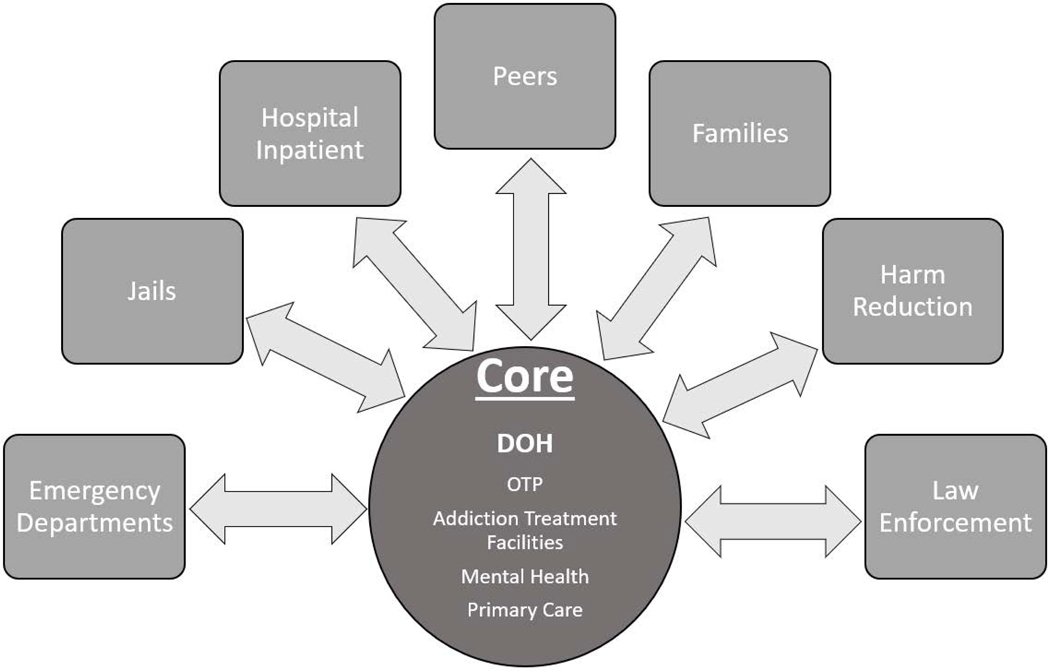
The INS mapping tool (figure 1), seeks to assist in coaching community coalitions to systemically enhance MOUD delivery by envisioning and documenting a network of relevant community resources and their relationships. The premise is that to achieve the increase in MOUD treatment needed to reduce overdose rates, communities require both sufficient treatment slots in programs providing MOUD appropriate to individuals’ needs (collectively, the “core”), as well as linkage to treatment from allied partners or programs (the “satellites”). It is intended to be a flexible coaching tool to assist communities in selecting evidence-based practices for MOUD expansion that can suit the uniquely available resources and needs of widely differing communities.
Figure 1 -.
Core services/facilities can provide long term medication treatment for opioid use disorder (MOUD), while the connected satellite services/facilities can identify individuals with opioid use disorder and refer to core MOUD providers, or identify, initiate MOUD, and refer to core providers for ongoing MOUD. Arrows represent the movement of individuals between these agencies. DOH: Department of Health; OTP: Opioid Treatment Program.
Within the INS structure, the core is intended to include clinical services that can deliver ongoing or maintenance MOUD. These could be traditional opioid treatment programs providing methadone maintenance or programs providing buprenorphine and/or extended-release naltrexone, including addiction treatment programs, mental health programs, or primary care clinics. The organization of the core permits programs providing at least one type of MOUD in any type of treatment setting to play a central role by collaborating with other referral sources or treatment programs, allowing for multiple core programs to form a network to ideally provide all MOUD treatment options in communities with sometimes limited treatment resources.
The role of the satellites is to identify people with opioid use disorder and either refer to the core for MOUD or initiate “bridging” (i.e., time-limited) MOUD, often “low-threshold” buprenorphine (31), with subsequent referral. Satellites include access points or resources, such as the criminal legal system (e.g., county jails, community supervision, opioid courts), harm reduction programs, mobile vans, emergency departments, and hospital inpatient units, as well as supportive services that enhance treatment participation such as housing or peer support services. During external facilitation meetings involving the research team and community implementation staff, the INS mapping tool is introduced as a scaffolding (figure 1). Coalitions create a visual map of the programs and services within their community already providing MOUD or linkage to MOUD while considering the current relationships between various organizations and sectors. Gaps and opportunities are identified where existing services need to be expanded or new services need to be built. Through the mapping process, INS encourages coalitions and implementation teams to envision a comprehensive, community-wide network that promotes identification and linkage to appropriate and relevant services from any location where people with opioid use disorder are encountered in the satellites.
The INS mapping tool provides a visualization of the network of partners where organizational relationships and patient flow may be indicated similarly to how genograms or ecomaps are used to map social networks (32). INS extends the work of asset mapping (33) and builds on the HCS landscape analysis while emphasizing existing relationships, developing new relationships, and opportunities to participate as a component of the network.
Comparison to Other Community-Level Interventions for Opioid Use Disorder
The INS approach was devised to be an adaptable coaching strategy using a mapping tool that can complement existing implementation models, such as the community engagement work that is a key component of HCS. It draws from other MOUD implementation systems to create a flexible approach allowing for its components to be modified based on a community’s existing resources and needs.
Like the hub-and-spoke model, INS seeks to establish a strong center of treatment resources in each community. As originally applied in Vermont (34), “hubs” were designated as opioid treatment programs providing all forms of MOUD including methadone, and “spokes” were affiliated primary care programs in the surrounding community. Differing from the central single-agency hubs of the hub-and-spoke model, INS gathers different agencies to create each core that then work complementarily with support from the department of health and HCS. The satellites in INS may include not only medical practices, but also a range of other practices in clinical or non-clinical settings (e.g., hospital emergency departments, jails, harm reduction programs, peer organizations), building flexibility into resources available in the community for screening, time-limited MOUD treatment, and referral.
Similar to the office-based opioid treatment model (35), which draws from other collaborative care models for treating chronic diseases and relies on the hiring of nurse care managers, INS encourages care coordination across the core and satellites with liaisons between different agencies for opioid use disorder treatment tailored to each county. Instead of a focus on nurse care managers, who provide clinical guidance and liaise patients between different service providers, costs for peer and other linkage services must be embedded into the budgets of other treatment programs or supplied by grants.
INS may be used to complement rather than supplant existing implementation models. The aforementioned models benefited from substantial state funding or a favorable regulatory stance in their original applications (e.g. insurance reimbursement for nurse care managers that many states do not provide) and were effective in states where they were piloted, but demonstrated mixed results when implemented in other settings (36–38).
RESULTS
County Characteristics Mapped to the INS Approach
Table 1 summarizes the types of treatment programs, healthcare services, and other relevant services that could be potentially engaged in INS in the eight communities participating in wave 1 of HCS in NY. These data were obtained during coaching meetings as well as through a review of the implementation plan agreements. Also indicated are the services that provided MOUD at the start of the study and which had implementation plan agreements in place at the conclusion of wave 1.
Table 1.
Summary of availability of types of services/agencies within each New York wave 1 community.
| Addiction treatment | Opioid treatment program | Mental health | Primary care | Hospital | Emergency department | Peer program | Family program | Ham reduction program | Jail | Law enforcement | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Rural Communities | |||||||||||
| 1 | |||||||||||
| (A) Service | ✔* | ✔ | ✔* | ✔ | ✔* | ✔ | ✔ | ✔* | ✔ | ||
| (B) IPA | ✔ | ✔ | ✔ | ||||||||
| 2 | |||||||||||
| (A) Service | ✔* | ✔ | ✔* | ✔ | ✔* | ✔ | ✔ | ✔ | |||
| (B) IPA | ✔ | ✔ | ✔ | ||||||||
| 3 | |||||||||||
| (A) Service | ✔* | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | |||
| (C) IPA | ✔ | ✔ | ✔ | ✔ | ✔ | ||||||
| 4 | |||||||||||
| (A) Service | ✔* | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | |||
| (B) IPA | ✔ | ✔ | ✔ | ✔ | |||||||
| Urban Communities | |||||||||||
| 5 | |||||||||||
| (A) Service | ✔* | ✔* | ✔ | ✔* | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| (B) IPA | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | |||||
| 6 | |||||||||||
| (A) Service | ✔* | ✔* | ✔ | ✔* | ✔* | ✔* | ✔ | ✔ | ✔* | ✔* | ✔ |
| (B) IPA | ✔ | ✔ | ✔ | ✔ | |||||||
| 7 | |||||||||||
| (A) Service | ✔* | ✔* | ✔* | ✔* | ✔* | ✔* | ✔ | ✔* | ✔* | ✔ | |
| (B) IPA | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | |||
| 8 | |||||||||||
| (A) Service | ✔* | ✔* | ✔* | ✔* | ✔* | ✔* | ✔ | ✔ | ✔* | ✔* | ✔ |
| (B) IPA | ✔ | ✔ | |||||||||
Denotes programs providing MOUD (A) Categories of services/agencies with potential to provide or refer to medication for opioid use disorder (MOUD); (B) Services/agencies that supported an implementation plan agreement (IPA) at the end of wave 1. Some agencies were responsible for implementing several strategies and had multiple agreements in place.
Only half the counties, all urban, had at least one opioid treatment program providing methadone. All counties had one or more licensed addiction treatment program, which are required to provide access to MOUD by the NY Office of Addiction Services and Supports (39). However, the extent of MOUD availability varied and several programs noted low demand for MOUD and open treatment slots, which was inconsistent with the high estimated prevalence of opioid use disorder in their communities (40). This suggested the need for an improved system of identification and linkage and that available treatment options may not necessarily be acceptable or appropriate to the local population.
Notable is the lack of MOUD availability in many county jails prior to HCS and limited engagement via implementation plan agreements during HCS, especially since this setting presents an opportunity to engage high-risk individuals with MOUD (41). Some agencies, which included jails, were included in the actions plans and initially had agreements that were subsequently withdrawn or never came to fruition due to an inability to meet milestones or lack of desired continued participation by the agency. Other agencies, such as emergency departments already prescribing MOUD, had their own opioid treatment initiatives and chose not to formally engage in these agreements. Several counties had success in developing implementation plan agreements to introduce MOUD in mental health programs where co-occurring substance use disorders are common. In all sites, buprenorphine, followed by naltrexone and methadone, was the most common medication selected for an implementation strategy (27).
Case Example Applying the INS Approach to a Rural County
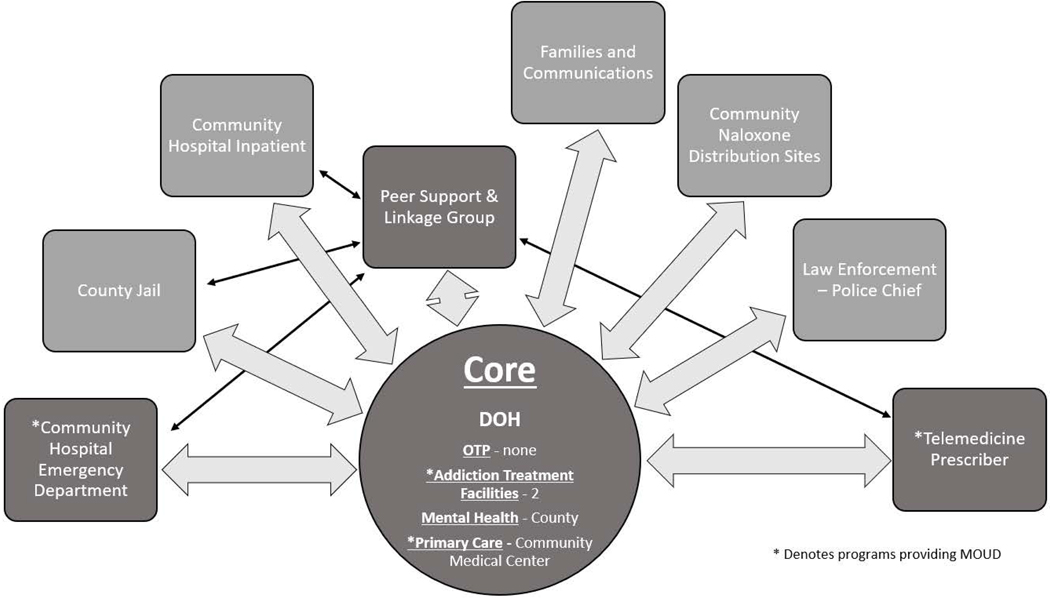
An example of INS mapping applied to a NY county is shown in figure 2. This rural county did not have an opioid treatment program to anchor its delivery of MOUD in the core. However, they were able to develop an INS network to facilitate MOUD delivery by creating a core consisting of a mental health clinic that had increased its substance use treatment and prescribing of MOUD alongside a primary care clinic and state-funded addiction treatment programs. Patients requiring methadone travelled to an opioid treatment program in a neighboring county (not included in figure 2).
Figure 2 -.
Services in dark grey had implementation plan agreements in place while services in light grey did not. Abbreviations: DOH: Department of Health; OTP: Opioid Treatment Program.
There was initially a shortage of buprenorphine prescribers in the county, so the coalition opted to temporarily contract with an out-of-county prescriber for telemedicine buprenorphine initiation services as they scaled up other components of their core. The mental health center subsequently hired a nurse practitioner to prescribe buprenorphine and was able to enhance its role within the community’s MOUD core. Satellites that were successfully engaged included a peer support and referral program which was essential to providing linkage to and maintaining engagement in treatment in this small community. It thus had a more central role in INS, represented visually in figure 2 by its proximity to the core and connections to several other satellites. These examples illustrate the flexibility of the INS for each community to customize its approach to expanding MOUD based on available services and gaps to be filled.
Also shown in figure 2 are the satellites which were involved in the study but did not have active implementation plan agreements in place. Agreements with the county jail and community hospital could not be agreed upon within the implementation period, although these were originally included in action plans to develop or expand services.
DISCUSSION
The INS approach was developed to assist in coaching communities toward the critical goal of improving effective delivery of MOUD. INS encourages county coalitions to visually map community-based clinical services and programs into a network (figure 1) with core agencies providing MOUD and satellite agencies identifying individuals with opioid use disorder and linking to the core. In the consolidated framework for implementation research, implementation constructs are groups into five major domains: intervention characteristics, inner and outer settings, characteristics of the individuals involved, and the process of implementation (25). We discuss the experiences and challenges encountered within these domains below.
Our findings are limited by being based partly on the unstructured observations of the research teams providing coaching to the communities, as well as the implementation plan agreements for MOUD set forth by each county. The overall effectiveness (i.e., increases in prescribing of MOUD and reductions in overdose rates) will be evaluated by the primary outcome analyses of HCS.
Intervention and Process
INS was developed to complement and assist with the key phases of HCS aimed at expansion of MOUD and strengthening of delivery systems. By visually mapping the elements of MOUD treatment and opioid use disorder identification in a community and how they could interact, INS intends to provide a broad structure to identify current strengths and gaps and assist in developing effective strategies within a community treatment network. Importantly, the core-satellite structure allows organizations with limited resources to play a central role in the provision of opioid use disorder treatment and provides the opportunity for the implementation team to engage in conversations about expanding MOUD. This adaptability makes the INS mapping tool particularly well-suited for small to medium-sized communities, where organizations may not have ability to provide all forms of MOUD and agencies are easily tracked and engaged.
The flexibility of INS also has potential drawbacks. The emphasis on community autonomy made it difficult to advocate for goals that were not a high priority or had significant barriers in some community stakeholders or component programs. This was seen in the change toward initiating MOUD in jails. Though initiating buprenorphine in jails has been shown to decrease recidivism (42–44), it also requires a substantial hiring of support staff and care coordination that we were not able to provide during the study’s limited intervention period. Although we are yet to know the impacts on implementation from this intervention period, parallel efforts by other organizations in the state (i.e., in the Outer Setting) are being synchronized. NY state legislature recently passed a bill requiring jails to provide all three FDA approved forms of MOUD for those with opioid use disorder (45). Expansion of Medicaid coverage through the Affordable Care Act and the allowance for individuals to have federal Medicaid funds pay for services while incarcerated though the Reentry Act of 2023 (46) should also increase the receipt of MOUD as it has in current Medicaid expansion states (47–48). Addressing racial inequities in opioid-related health outcomes and overdoses also proved challenging and dedicated antiracist efforts are likely needed to overcome structural racism in all communities (49).
The flexibility of INS has similarities to community-engagement focused iterations of the hub- and-spoke model that widen the scope beyond the medical model. For example, ones with a social work or peer-based recovery focus also incorporate interventions such as prevention and harm reduction as well as recovery support (37, 50). As in other rurally implemented experiences of the hub-and-spoke model, we also encountered challenges recruiting supporting programs (i.e., satellites) due to factors such as lack of or waning interest, financial vulnerabilities, and preference for informal relationships over a more demanding formal research relationship (51). Though expanding methadone access through new programs, more efficient enrollment, sustainability planning, or transportation initiatives were discussed during workgroup and coalition meetings, the steps and funding for a full-service opioid treatment program license and facility required an extended intervention period and additional financial resources.
INS may also be viewed analogously to the visualization dashboards and system dynamics modeling which the NY HCS also utilizes (30, 52, 53). These approaches show data and build quantitative models predicting the key outcome of opioid overdose deaths as a function of more proximal outcomes such as naloxone distribution numbers and patients initiated on MOUD, producing diagrams of these factors and their interactions. INS is a more qualitative approach for envisioning the system of MOUD treatment resources in a community for the purposes of planning and implementation. Future work might seek to embed INS within larger system dynamics models for a community.
Inner Setting
A major goal of the INS approach is to help communities modify their inner setting by improving communication between service providers to improve the ability of patients to move within this network and access appropriate resources. Cataloguing programs and services across the eight NY wave 1 communities according to the INS rubric (table 1) identified common gaps and opportunities, including the absence of methadone maintenance in rural communities and a relative lack of MOUD within mental health or criminal legal systems. The case example of the process of applying INS in a rural NY community (figure 2) showed success in building a modest core of MOUD treatment across addiction, mental health, and primary care services and some satellite referral capacity facilitated by a peer organization.
Barriers encountered included limited services overall in small rural counties, and stigma and misinformation around MOUD that stymied MOUD initiation in the criminal legal system and local hospitals where a small number of physicians or administrators were responsible for decisions. Some programs cited discomfort with treating individuals with opioid use disorder and lack of adequate staffing and infrastructure to support addiction services. Analogous barriers have been identified in previous MOUD integration efforts, such as insufficient funding, lack of expert consultation, and lack of clinical backup and allied behavioral counseling (38). The INS approach has the potential to address some of these barriers by providing a community-wide referral network to support MOUD and allied providers.
Outer Setting
HCS provided some limited discretionary financing, but communities had to develop third party reimbursement or seek grants to fund expanded services. Reimbursement for clinical services in many communities is mostly funded by public funds such as Medicaid or block grants (54). Our study team provided billing reimbursement training to agencies who requested this technical assistance. Additionally, the team provided technical assistance on costing for MOUD in jails (55) as communities prepared for the legislation requiring carceral settings to provide all FDA approved medications for opioid use disorder. Self-financing is a major challenge in the short-term but may ultimately be more sustainable than grant funding. However, many ancillary services such as peer support and care coordination continue to have low reimbursement rates, and this was difficult to address within the study timeframe. As mentioned when discussing the intervention process, larger parallel state or federal efforts may be needed to adequately address these issues. Additionally, the COVID-19 pandemic disrupted study progress (56, 57) and diverted substantial county resources and attention of community health systems away from treating opioid use disorder towards contact tracing and other pandemic priorities.
Characteristics of Individuals
There was sometimes competition for study funding between clinical programs, who struggled with how to fund MOUD-related services given limited third-party reimbursement. The medications themselves were also broadly misunderstood, highlighting the need for education at all levels (patients, providers, program managers, other community stakeholders) and technical assistance to providers. Bias against MOUD was common, countered with advocacy by the HCS research team and local champions as well as public communications campaigns that were part of HCS and customized to each county. Observing successful cases of patients treated with MOUD can also be powerful in overcoming stigma and misunderstanding.
Many coalitions especially encountered bias against methadone and buprenorphine in the criminal legal system. While some jails had the capability and stated willingness to provide MOUD, we found treatment rates to be exceedingly low and sometimes absent. As in the general community, this was also attributed to lack of demand or lack of clinical appropriateness and was inconsistent with the high estimated prevalence of opioid use disorder in jails. The burden of research documentation also discouraged some individuals and agencies from formally participating in HCS, though not specifically INS.
County coalitions were generally receptive to the visual mapping process of INS focused on MOUD that built on a baseline landscape analysis and community profile development. In counties where the study team felt that medication linkage, engagement, or treatment retention needed improvement, it was helpful in further emphasizing the gaps in care, and to what part of the care continuum would be most effective to focus more resources, as well as which areas were particularly strong.
CONCLUSIONS
INS was developed as a coaching tool to help communities plan where MOUD treatment or opioid use disorder identification capacity is present or needed and how to connect services across a community into a well-defined network. The core-satellite structure was specifically designed to be a flexible approach that can accommodate communities with varied or limited resources. It may be used best when combined with other implementation models, such as community-engagement, as well as larger state or federal initiatives. It provides a particularly helpful framework for smaller, underserved communities with fewer MOUD treatment resources.
Highlights:
The integrated network systems (INS) approach uses a coaching mapping tool to enhance delivery of medications for opioid use disorder (MOUD). It is a flexible, community-led approach where communities aided by expert consultation map out available community resources and services.
INS mapping focuses on developing a “core” of services that can provide ongoing MOUD, along with a set of “catellite” programs to support and funnel patients with opioid use disorder into core services.
INS allows for the flexibility to develop a map and organization of services that is adaptable to the available resources in any community.
Disclosures and Acknowledgments:
Dr. Nunes has served as an Investigator on NIH funded studies to which in-kind medication or digital therapeutics were donated by Alkermes, Braeburn, Indivior, Pear Therapeutics, and CHESS Health, and has served as a consultant without compensation to Alkermes, Indivior, Pear Therapeutics, and Camurus. Dr. Blevins has served as a paid consultant to Pear Therapeutics. Dr. Levin receives grant support from US World Meds, research support from Aelis Pharmaceuticals, medication from Indivior for research, and royalties from APA publishing. In addition, Dr. Levin served as a nonpaid member of a Scientific Advisory Board for Alkermes, Indivior, Novartis, Teva, and US WorldMeds and is a consultant to Major League Baseball.
This research was supported by the National Institutes of Health and the Substance Abuse and Mental Health Services Administration through the NIH HEAL (Helping to End Addiction Long-termSM) Initiative under award number UM1DA049415 (ClinicalTrials.gov Identifier: NCT04111939) and by the National Institute on Alcohol Abuse and Alcoholism (award K23AA028295). We wish to acknowledge the participation of the HEALing Communities Study communities, community coalitions, and Community Advisory Boards and state government officials who partnered with us on this study. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health, the Substance Abuse and Mental Health Services Administration or the NIH HEAL InitiativeSM.
Footnotes
Previous Presentation: None
REFERENCES
- 1.Wakeman SE, Larochelle MR, Ameli O, et al. : Comparative Effectiveness of Different Treatment Pathways for Opioid Use Disorder. JAMA Netw Open 2020; 3:e1920622–e1920622 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Mattick RP, Breen C, Kimber J, et al. Buprenorphine maintenance versus placebo or methadone maintenance for opioid dependence. Cochrane Database Syst Rev. 2014. Feb 6;(2):CD002207 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Weiss RD, Potter JS, Fiellin DA, et al. : Adjunctive counseling during brief and extended buprenorphine-naloxone treatment for prescription opioid dependence: a 2-phase randomized controlled trial. Arch Gen Psychiatry 2011; 68:1238–1246 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Hser Y-I, Evans E, Huang D, et al. : Long-term outcomes after randomization to buprenorphine/naloxone versus methadone in a multi-site trial. Addiction 2016; 111: 695–705 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Lee JD, Friedmann PD, Kinlock TW, et al. : Extended-Release Naltrexone to Prevent Opioid Relapse in Criminal Justice Offenders. N Engl J Med 2016; 374:1232–1242 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Lee JD, Nunes EV, Novo P, et al. : Comparative effectiveness of extended-release naltrexone versus buprenorphine-naloxone for opioid relapse prevention (X:BOT): a multicentre, open-label, randomised controlled trial. Lancet 2018; 391:309–318 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Lofwall MR, Walsh SL, Nunes EV, et al. : Weekly and Monthly Subcutaneous Buprenorphine Depot Formulations vs Daily Sublingual Buprenorphine With Naloxone for Treatment of Opioid Use Disorder: A Randomized Clinical Trial. JAMA Intern Med 2018; 178:764–773 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Haight B, Learned S, Laffont C, et al. : Efficacy and safety of a monthly buprenorphine depot injection for opioid use disorder: a multicentre, randomised, double-blind, placebo-controlled, phase 3. Lancet 2019, 393: 778–790 [DOI] [PubMed] [Google Scholar]
- 9.Nunes EV, Gordon M, Friedmann PD, et al. : Relapse to opioid use disorder after inpatient treatment: Protective effect of injection naltrexone. J Subst Abuse Treat 2018; 85:49–55 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Williams AR, Nunes EV, Bisaga A, et al. : Development of a Cascade of Care for Responding to the Opioid Epidemic. Am J Drug Alcohol Abuse 2019; 45:1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Morgan JR, Schackman BR, Leff JA, et al. : Injectable naltrexone, oral naltrexone, and buprenorphine utilization and discontinuation among individuals treated for opioid use disorder in a United States commercially insured population. J Subst Abuse Treat 2018; 85:90–96 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Jones CM, Han B, Baldwin GT, et al. : Use of Medication for Opioid Use Disorder Among Adults With Past-Year Opioid Use Disorder in the US, 2021. JAMA Netw Open 2023; 6:e2327488–e2327488 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.D’Onofrio G, O’Connor PG, Pantalon MV, et al. : Emergency Department–Initiated Buprenorphine/Naloxone Treatment for Opioid Dependence: A Randomized Clinical Trial. JAMA 2015; 313:1636. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Walley AY, Lodi S, Li Y, et al. : Association between mortality rates and medication and residential treatment after in‐patient medically managed opioid withdrawal: a cohort analysis. Wiley Online Libr 2020; 115:1496–1508 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Molfenter T, Fitzgerald M, Jacobson N, et al. : Barriers to Buprenorphine Expansion in Ohio: A Time-Elapsed Qualitative Study. J Psychoactive Drugs 2019; 51:272–279 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Grimm CA: Geographic Disparities Affect Access to Buprenorphine Services for Opioid Use Disorder. Pub no OEI-12–17-00240. U.S Department of Health and Human Services, Office of Inspector General, 2020. oig.hhs.gov/oei/reports/oei-12-17-00240.pdf [Google Scholar]
- 17.HEALing Communities Study Consortium: The HEALing (Helping to End Addiction Long-term SM) Communities Study: Protocol for a cluster randomized trial at the community level to reduce opioid overdose deaths through implementation of an integrated set of evidence-based practices. Drug Alcohol Depend 2020; 217:108335 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.El-Bassel N, Jackson RD, Samet J, et al. : Introduction to the special issue on the HEALing Communities Study. Drug Alcohol Depend 2020; 217: 108327 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Chandler RK, Villani J, Clarke T, et al. : Addressing opioid overdose deaths: The vision for the HEALing communities study. Drug Alcohol Depend 2020; 217: 108329 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Winhusen T, Walley A, Fanucchi LC, et al. : The Opioid-overdose Reduction Continuum of Care Approach (ORCCA): Evidence-based practices in the HEALing Communities Study. Drug Alcohol Depend 2020; 217: 108325 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Sprague Martinez L, Rapkin BD, Young A, et al. : Community engagement to implement evidence-based practices in the HEALing communities study. Drug Alcohol Depend 2020; 217:108326 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Walunas TL, Ye J, Bannon J, et al. : Does coaching matter? Examining the impact of specific practice facilitation strategies on implementation of quality improvement interventions in the Healthy Hearts in the Heartland study. Implement Sci 2021; 16:1–12 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Gustavson AM, Kenny ME, Wisdom JP, et al. : Fluctuations in barriers to medication treatment for opioid use disorder prescribing over the course of a one-year external facilitation intervention. Addict Sci Clin Pract 2021; 16: 1–7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Young AM, Brown JL, Hunt T, et al. : Protocol for community-driven selection of strategies to implement evidence-based practices to reduce opioid overdoses in the HEALing Communities Study: a trial to evaluate a community-engaged intervention in Kentucky, Massachusetts, New York and Ohio. BMJ Open 2022; 12:e059328 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Damschroder LJ, Aron DC, Keith RE, et al. : Fostering implementation of health services research findings into practice: A consolidated framework for advancing implementation science. Implement Sci 2009; 4:1–15 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Kirk MA, Kelley C, Yankey N, et al. : A systematic review of the use of the Consolidated Framework for Implementation Research. Implement Sci 2016; 11:1–13 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Chandler R, Nunes EV, Tan S, et al. : Community selected strategies to reduce opioid-related overdose deaths in the HEALing (Helping to End Addiction Long-term SM) communities study. Drug Alcohol Depend 2023; 245:109804 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Miech EJ, Rattray NA, Flanagan ME, et al. : Inside help: An integrative review of champions in healthcare-related implementation. SAGE open Med 2018; 6:205031211877326 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Lefebvre RC, Chandler RK, Helme DW, et al. : Health communication campaigns to drive demand for evidence-based practices and reduce stigma in the HEALing communities study. Drug Alcohol Depend 2020; 217:108338 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Wu E, Villani J, Davis A, et al. : Community dashboards to support data-informed decision-making in the HEALing communities study. Drug Alcohol Depend 2020; 217: 108331 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Jakubowski A, Fox A: Defining Low-threshold Buprenorphine Treatment. J Addict Med 2020; 14(2):95. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Rempel GR, Neufeld A, Kushner KE: Interactive use of genograms and ecomaps in family caregiving research. J Fam Nurs 2007; 13:403–419 [DOI] [PubMed] [Google Scholar]
- 33.Dorfman D: Identify Assets and Resources Available. Rural Health Information Hub, 1998. www.ruralhealthinfo.org/toolkits/rural-toolkit/1/asset-identification#:~:text=Identify%20Assets%2FResources%20Available&text=Asset%20mapping%20is%20a%20systematic,elements%20of%20the%20local%20economy. [Google Scholar]
- 34.Brooklyn JR, Sigmon SC: Vermont Hub-and-Spoke Model of Care for Opioid Use Disorder: Development, Implementation, and Impact. J Addict Med 2017; 11:286–292 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.LaBelle CT, Han SC, Bergeron A, et al. : Office-Based Opioid Treatment with Buprenorphine (OBOT-B): Statewide Implementation of the Massachusetts Collaborative Care Model in Community Health Centers. J Subst Abuse Treat 2016; 60:6–13 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Snell-Rood C, Willging C, Showalter D, et al. : System-level factors shaping the implementation of “hub and spoke” systems to expand MOUD in rural areas. Subst Abus 2021; 42:716–725 [DOI] [PubMed] [Google Scholar]
- 37.Best D, Higham D, Pickersgill G, et al. : Building Recovery Capital through Community Engagement: A Hub and Spoke Model for Peer-based Recovery Support Services in England. Alcohol Treat Q 2021; 39:1, 3–15 [Google Scholar]
- 38.Quest TL, Merrill JO, Roll J, et al. : Buprenorphine therapy for opioid addiction in rural Washington: the experience of the early adopters. J Opioid Manag 2012; 8:29–38 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.General Service Standards for Substance Use Disorder Outpatient Programs. Part 882.OASAS, 2022. oasas.ny.gov/system/files/documents/2022/09/822.pdf [Google Scholar]
- 40.New York State - Opioid Annual Report. New York State Department of Health, 2017. https://www.health.ny.gov/statistics/opioid/data/pdf/nys_opioid_annual_report_2017.pdf
- 41.Brinkley-Rubinstein L, Zaller N, Martino S, et al. : Criminal justice continuum for opioid users at risk of overdose. Addict Behav 2018; 86:104–110 [DOI] [PubMed] [Google Scholar]
- 42.Matsumoto A, Santelices C, Evans EA, et al. : Jail-based reentry programming to support continued treatment with medications for opioid use disorder: Qualitative perspectives and experiences among jail staff in Massachusetts. Int J Drug Policy 2022; 109:103823 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Stopka TJ, Rottapel RE, Ferguson WJ, et al. : Medication for opioid use disorder treatment continuity post-release from jail: A qualitative study with community-based treatment providers. Int J Drug Policy 2022; 110:103803 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Evans EA, Wilson D, Friedmann PD: Recidivism and mortality after in-jail buprenorphine treatment for opioid use disorder. Drug Alcohol Depend 2022; 231:109254 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.The New York State Senate. Assembly Bill A533. The New York State Senate, 2021–2022 Legislative Session. www.nysenate.gov/legislation/bills/2021/A533
- 46.HS Releases New Guidance to Encourage States to Apply for New Medicaid Reentry Section 1115 Demonstration Opportunity to Increase Health Care for People Leaving Carceral Facilities. U.S. Department of Health and Human Services, 2023. https://www.hhs.gov/about/news/2023/04/17/hhs-releases-guidance-to-encourage-states-to-apply-for-medicaid-reentry-section-1115-demonstration-opportunity-to-increase-health-care.html
- 47.Khatri UG, Howell BA, Winkelman TNA: Medicaid Expansion Increased Medications For Opioid Use Disorder Among Adults Referred By Criminal Justice Agencies. Health Aff 2021; 40(4), 562–570 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Burns ME, Cook S, Brown LM, et al. : Association Between Assistance With Medicaid Enrollment and Use of Health Care After Incarceration Among Adults With a History of Substance Use. JAMA Netw Open 2022; 5:e2142688–e2142688 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Chatterjee A, Glasgow LS, Bullard M, et al. : Placing Racial Equity at the Center of Substance Use Research: Lessons From the HEALing Communities Study. Am J Public Health 2022; 112:204–208 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.McCormick KA, Holleran Steiker LK: A social work perspective on the opioid solution: a community-based expansion of the hub-and-spoke ecosystem. J Soc Work Pract 2021; 21(3), 308–315 [Google Scholar]
- 51.Green B, Rhubart DC, Filteau MR: Barriers for Implementing the Hub and Spoke Model to Expand Medication for Opioid Use Disorder: A Case Study of Montana. Subst Abuse 2021; 15, 11782218211039781 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Carey G, Malbon E, Carey N, et al. : Systems science and systems thinking for public health: a systematic review of the field. BMJ Open 2015; 5(12), e009002 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.El-Bassel N, Gilbert L, Hunt T, et al. : Using community engagement to implement evidence-based practices for opioid use disorder: A data-driven paradigm & systems science approach. Drug Alcohol Depend 2021; 222: 108675/ [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Federal Regulation of Methadone Treatment. Methadone Treatment. The National Academies Press, Institute of Medicine, 1995. nap.nationalacademies.org/read/4899/chapter/8 [PubMed] [Google Scholar]
- 55.Ryan DA, Montoya ID, Koutoujian PJ, et al. : Budget impact tool for the incorporation of medications for opioid use disorder into jail/prison facilities. J Subst Use Addict Treat 2023; 146:208943 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Root ED, Slavova S, LaRochelle M, et al. : The impact of the national stay-at-home order on emergency department visits for suspected opioid overdose during the first wave of the COVID-19 pandemic. Drug Alcohol Depend 2021; 228:108977 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Walters ST, Chandler RK, Clarke T, et al. : Modifications to the HEALing Communities Study in response to COVID-19 related disruptions. Drug Alcohol Depend 2021; 222: 108669 [DOI] [PMC free article] [PubMed] [Google Scholar]