Abstract
Background
Syrian children, among the most vulnerable groups, have faced profound physical and psychological consequences due to the protracted conflict. This review assesses the health and well-being of children living within Syria, with particular attention to internally displaced populations (IDPs).
Objectives
To synthesize research on child health in Syria from 2012 to 2024, identify key health challenges, assess study characteristics and geographical distribution, and highlight gaps to inform future policies and interventions.
Design
We conducted a scoping review in December 2024 using the PRISMA-ScR (Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews) methodology. We searched five academic databases (Medline Ovid, PubMed, Scopus, Web of Science, and Global Health) and selected studies published between January 2012 and December 2024. The search strategy followed the JBI Population–Concept–Context framework. Eligible studies included primary and secondary research, published in English or Arabic, that examined the health of children under 19 years old living within Syria in the context of the ongoing conflict. Grey literature was also retrieved from major organizational repositories (e.g., WHO, UNICEF, MSF, SAMS).
Results
A total of 1,189 records were retrieved, with 647 remaining after removing duplicates. After screening, 30 studies met the inclusion criteria. Most were observational, including cross-sectional (63.3%) and retrospective cohort (26.7%) designs. Surveys and medical records were the main data sources; oral examinations were common in dental studies, while anthropometry, blood tests, and interviews were less frequent. Data sources varied significantly by region (p < 0.001), with government-controlled areas relying on state institutions and non-government-controlled areas drawing on humanitarian data. Due to substantial heterogeneity, meta-analysis was not feasible. Notably, 80% of studies reported no external funding.
Conclusion
This review highlights major research gaps in child health within Syria, particularly among IDPs and in underserved regions. Most studies were observational, unfunded, and regionally concentrated, limiting broader applicability. Despite these constraints, this is the first comprehensive synthesis of health research focused on children within Syria, providing a foundation for future research, policy action, and targeted humanitarian interventions in conflict-affected settings.
Supplementary Information
The online version contains supplementary material available at 10.1186/s13031-025-00673-1.
Keywords: Child health, Syria, Conflict-Affected populations, Internally displaced persons (IDPs), Public health, Pediatric health, Health services
Introduction
The Syrian conflict, a profoundly complex and devastating crisis, began in 2011 with widespread demands for political freedom and reform. In December 2024, the Assad regime came to an end, with former opposition forces assuming power. Nevertheless, the future of Syria remains uncertain, characterized by a fragile balance of hope, fear, and ongoing demands for justice from the diverse components of Syrian society. Over the past 14 years, the country has experienced deep fragmentation, divided between the former government and various political factions. This protracted conflict has resulted in severe and far-reaching consequences, critically weakening Syria’s medical infrastructure and economic foundations, and posing enduring challenges to reconstruction, governance, and national reconciliation [1, 2]. The Syrian population can be broadly classified into three distinct groups: Syrian refugees residing in host countries, internally displaced persons (IDPs) within Syria, and those who remain in their homes but continue to endure extreme hardship due to the ongoing conflict. Each group faces distinct health challenges, yet comprehensive data on their specific conditions remains scarce, underscoring the urgent need for targeted research and intervention strategies to address their medical, nutritional, and psychological needs. In 2024, according to U.N. agencies, 16.7 million people, 7 million of them children are estimated in need of humanitarian aid in Syria [3]. While approximately 6.5 million Syrians are currently registered as refugees and asylum-seekers, primarily hosted in neighboring countries, an additional 6.8 million individuals remain internally displaced within Syria’s borders [3]. Notably, forced displacement peaked between December 2019 and March 2020, when nearly one million people were displaced due to escalating violence, of whom approximately 60% were children. According to recent reports, IDPs are facing more health challenges and higher mortality than refugees due to difficult access to health assistance [4–6]. Furthermore, more than half of the population in Syria, amounting to 12.1 million people, are currently experiencing acute food insecurity, including 2.6 million who are severely acutely food insecure. Additionally, 2.9 million people are at risk of sliding into hunger [7]. Children are particularly vulnerable during conflicts due to their physical, emotional, and developmental needs, often becoming the primary victims of the war cycle. Exposure to violence, loss of family members, displacement, and food insecurity severely impact their health and well-being, leading to long-term consequences. In conflict-affected regions, children face significant challenges such as malnutrition, inadequate healthcare, psychological trauma, and disrupted education, all of which hinder their development and future prospects [6]. According to UN data, in 2023, approximately 609,900 children under the age of five in Syria suffered from stunting due to prolonged undernutrition, resulting in irreversible physical and cognitive impairments that hinder their learning capacity, future productivity, and earning potential [8]. Despite numerous humanitarian efforts, evidence on the effectiveness of interventions addressing these challenges remains fragmented, and comprehensive assessments of the health and social outcomes for children affected by the Syrian conflict are limited [9].
The increase in health-related research following the conflict is evident; however, only 34% of the literature published between 2011 and 2019 specifically focused on the health of Syrians residing within Syria [9, 10]. Furthermore, a notable gap exists in research concerning child and maternal health during the post-conflict period [9]. This discrepancy underscores a critical shortfall in scholarly attention, revealing the insufficient focus on the unique health challenges faced by Syrian children and families, particularly those residing within Syria, amid the continuing conflict and instability. We anticipated that the existing literature on child health in post- conflict Syria would be highly heterogeneous in scope, methodology, and focus, while also being limited in both quantity and quality. Given these constraints, this scoping review aims to systematically map and assess the existing literature on the health and well-being of children living within Syria, including internally displaced populations, in order to highlight key health challenges, identify methodological and geographical gaps, and inform future research and targeted interventions to improve child health outcomes in conflict-affected settings.
Methods
Protocol
In December 2024, we conducted a scoping review of articles focused on the health of Syrian children living within Syria during the years of war. The review was carried out using the Preferred Reporting Items for Systematic Reviews and Meta-Analyses—Extension for Scoping Reviews (PRISMA-ScR) methodology [11] Registered on 16/01/2025 in PROSERO, number: CRD42025634285. (see online supplemental appendix 1 for the PRISMA-ScR checklist).
Search strategy and eligibility criteria
Our search strategy was constructed based on the population, concepts and context framework described by JBI [12], shown in Table 1. Academic literature searches were conducted using Medline Ovid, PubMed, Scopus, Web of Science and Globa Health. For each database, we employed a combination of MeSH terms and free-text keywords related to the health of Syrian children (full search strategy detailed in supplemental appendix S2). Inclusion criteria: (1) Articles were included if they investigated the health of Syrian children under 19 years old living within Syria specifically in relation to the recent conflict; and (2) were published between January 2012, and December 2024; (3) we included primary and secondary research, encompassing various study designs using qualitative, quantitative or mixed methods (Systematic reviews, observational studies, cross-sectional surveys, cohort studies, and qualitative studies). Exclusion criteria: (1) Articles were excluded if they did not focus on the health of Syrian children; or (2) were unrelated to the Syrian conflict; (3) articles concerning Syrian refugees not residing within Syria, (4) articles published before 2012, or (4) articles not written in English or Arabic. (5) Additionally, case reports, case series, editorials, letters to the editor, and conference proceedings were excluded.
Table 1.
Search strategy using population, concepts and context framework
| Population | Children and adolescents under 19 years old (internally displaced children and those residing in place). |
| Concept | Child health, encompassing physical and mental well-being, particularly as affected by conflict-related exposures. This includes both direct (e.g., injury, trauma) and indirect (e.g., displacement, infrastructure breakdown) consequences of the Syrian conflict. Geographic disparities (e.g., differences in health service availability across governorates). |
| Context |
Studies conducted within the Syrian context, with attention to geographic disparities such as differences in health service availability and access across governorates. Timeframe: Publications dated from 1st January 2012 to 31th December 2024. Language: †Syrian studies published in English or Arabic. |
†Studies will be defined as studies conducted on Syrian population living within Syria during the conflict
Moreover, relevant information was extracted from grey literature through systematic searches of publicly accessible databases and repositories maintained by key international organizations, including the International Rescue Committee (IRC), the International Committee of the Red Cross and Red Crescent (ICRC), the World Health Organization (WHO), the United Nations Children’s Fund (UNICEF), and several non-governmental organizations (NGOs) such as Save the Children, Médecins Sans Frontières (MSF), and the Syrian American Medical Society (SAMS). Although the search for grey literature followed a structured and targeted approach, it was inherently constrained by limitations in availability, accessibility, and inconsistencies in reporting standards across sources. The search strategy prioritized the identification of reports and publications directly relevant to the health of Syrian children in the context of the ongoing conflict, in accordance with the predefined inclusion criteria.
Guided by a predefined conceptual framework (Table 1), our analysis considered key conflict-related factors: including exposure to violence; displacement status; socioeconomic conditions; and geographic disparities, as central variables influencing child health outcomes. These factors were selected based on their recurrent significance in the existing literature and their theorized relationships with both physical and mental health consequences of conflict, such as trauma, malnutrition, and limited access to healthcare. This framework informed our inclusion criteria, data extraction process, and interpretation of findings.
Selection of sources of evidence and data extraction
Two researchers independently reviewed all titles, abstracts, and full-text articles, extracting relevant data. In cases of disagreement or uncertainty, they consulted a third researcher to review the content and make a final decision on contentious articles. The main review team, consisting of seven authors (SH, FA, IH, RK, SH, RA, and LZ), collaboratively discussed initial findings and resolved any disagreements between reviewers, ultimately agreeing on the publications for full-text review. A structured data charting form was collaboratively developed by two independent reviewers to extract key study characteristics, population details, health outcomes. The form underwent pilot testing with five studies to ensure completeness and was refined iteratively. Data charting was conducted independently and in duplicate to minimize bias. Discrepancies were resolved through discussion, with a third reviewer consulted if needed. The final form was implemented in Microsoft Excel (supplemental appendix 3). Missing or inconsistent data were addressed by contacting study authors or cross-referencing multiple sources. The process remained iterative, with revisions documented for transparency and reproducibility. Data extraction covered location, study design, study setting, intervention components, participant demographics, outcomes, key findings, financial statement, and affiliations. At least two reviewers conducted the data extraction for each publication, with discrepancies resolved through consensus and, when necessary, further discussion with additional reviewers. Included studies were collated and summarized based on the year of intervention and publication, first author name, first and last author affiliation, number, location, research topic, study type, intervention type, funding source, and outcomes specific to different populations.
In this study, we categorized research focusing on children residing within Syria during the conflict based on the location of data collection at the time each primary study was conducted, distinguishing between government-controlled (GC) and non-government-controlled areas (NGC). For consistency, government-controlled areas refer to territories under the control of the former Syrian regime during the respective study periods. In contrast, non-government-controlled areas encompass all regions outside of former Syrian regime authority, including territories governed by opposition forces, autonomous administrations (e.g., in northeast Syria), and other de facto authorities. We acknowledge that due to the dynamic nature of territorial control throughout the conflict, these classifications are inherently linked to specific timeframes and geopolitical contexts. To address this complexity, regional attributions were aligned with contemporaneous conflict mapping data (e.g., UN OCHA, ACAPS). Furthermore, significant demographic and humanitarian disparities exist across these areas. For example, in northwest Syria, comprising most of Idlib governorate and parts of Aleppo governorate, up to 70–80% of the population are IDPs, with children representing a substantial proportion. Similarly, northeast Syria operates under autonomous governance, facing distinct challenges such as political isolation and fluctuating humanitarian access.
These contextual factors critically influence health outcomes, service availability, and population vulnerabilities. Therefore, all comparative analyses presented in this study are interpreted within the framework of these regional, temporal, and socio-political dynamics, recognizing that direct comparisons must be approached with caution due to differing baseline conditions.
Moreover, Child health-related research was classified into conflict-related and non-conflict-related studies based on predefined criteria. Conflict-related studies were defined as those addressing health issues directly or indirectly attributable to the conflict, such as exposure to violence, displacement, and limited access to medical services or essential healthcare infrastructure. A comparative analysis was subsequently conducted to examine differences between conflict-related and non-conflict-related articles in terms of geographic distribution, data sources, bibliometric characteristics, and thematic focus. Furthermore, to facilitate a systematic analysis of the study findings, we categorized the included studies into six thematic domains: physical trauma and injuries, mental health, malnutrition, oral health, communicable diseases (CDs), and non-communicable diseases (NCDs), based on an inductive review of study objectives and health focus areas. We acknowledge that several studies addressed multiple health dimensions; therefore, studies were allowed to contribute to more than one thematic category where applicable.
Statistical analysis
Data management and analysis were conducted using SPSS Statistics for Windows, Version 23.0 (IBM Corporation, Armonk, NY, USA). Descriptive statistics were used to summarize the characteristics of the included studies. Frequencies and percentages were calculated for categorical variables, including bibliometric characteristics (e.g., study design, data source and type, funding status, and author affiliation), thematic focus, geographic distribution, and methodological approach. To assess temporal trends in child health research, the annual number of publications was analyzed and expressed as a percentage of the total included studies. Comparative analyses were conducted to examine differences between conflict-related and non-conflict-related studies. Bivariate associations between categorical variables were assessed using the Chi-square test. A p-value of < 0.05 was considered statistically significant.
Patient and public involvement Patients and/or the public were not involved in the design, or conduct, or reporting, or dissemination plans of this review as it’s a review of completed studies.
Results
Study characteristics
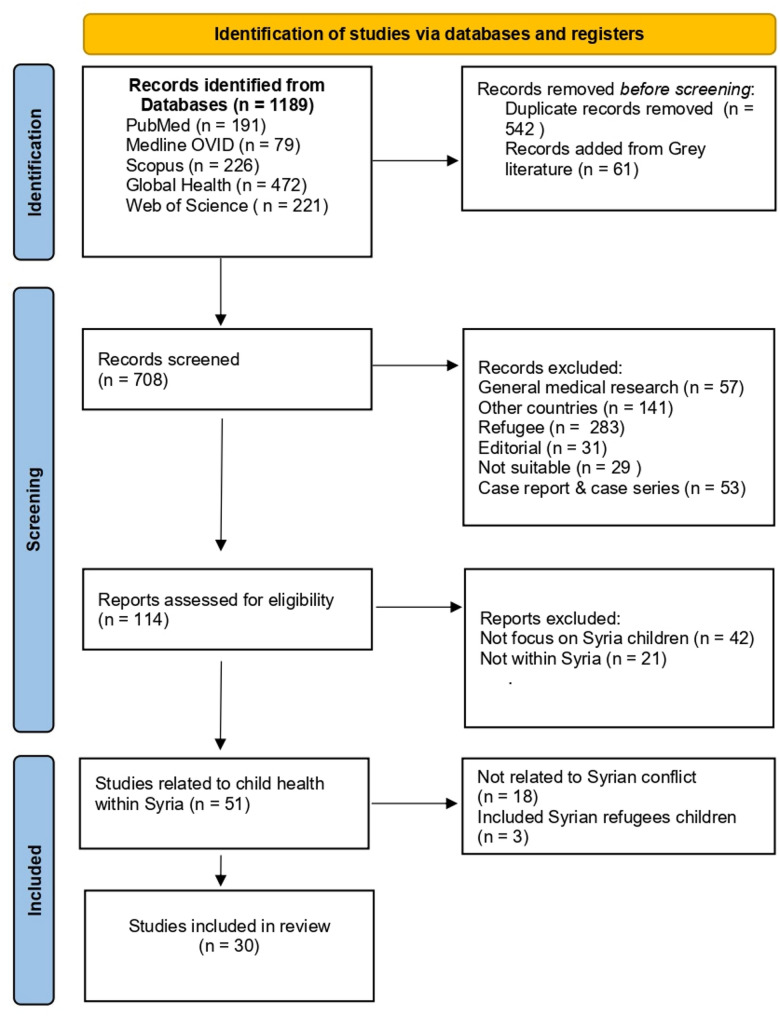
In total, 1,189 records were identified from academic databases. References were imported into the EndNote citation manager, and an initial screening was conducted. After removing duplicates, 647 records remained. An additional 61 records were identified through the grey literature review. During the initial screening, 541 records were excluded for not being relevant to the research topic (e.g., general medical research, unrelated to the Syrian population, not focused on health, or not addressing Syrian children living within Syria). A further 53 case reports and case series involving Syrian children were also excluded. Notably, all case reports and case series were unrelated to the ongoing Syrian conflict and affiliated with local institution. Of the 104 full-text articles reviewed, 51 focused on the health of children living within Syria, including 3 reviews. Of these, (64.7%, 33 articles) addressed issues related to the Syrian conflict, while 35.3%, 18 articles focused on non-conflict-related health issues. The results of a comparative analysis conducted between conflict-related and non-conflict-related articles revealed differences in geographic distribution, data sources, bibliometric characteristics, and thematic focus (see Table 2). All 3 reviews focused on conflict-related topics were addressing the health of Syrian children both within Syria and as refugees abroad. A total of 30 studies were included in this review, as determined by our inclusion criteria (see PRISMA flow diagram, Fig. 1).
Table 2.
Comparative analysis of Syrian child health research: Conflict-Related vs. Non-Conflict studies (n = 51)
| Non-conflict related n = 18 |
Conflict- related n = 33 |
p -value | Total n = 51 |
||
|---|---|---|---|---|---|
| Study location | |||||
| GC | 37.5% (18) | 39.6% (19) | 0.002 | 77.1% (37) | |
| NGC | - | 20.8% (10) | 20.8% (10) | ||
| GC & NGC | - | 2.1% (1) | 2.1% (1) | ||
|
The presence of at least one Syrian local affiliation | |||||
| Local | 35.3% (18) | 33.3% (17) | <0.001 | 68.6% (35) | |
| Non-local | - | 31.4% (16) | 31.4% (16) | ||
| Funding status | |||||
| Funded | 15.7% (8) | 11.8% (6) | 0.034 | 27.5% (14) | |
| Unfunded | 13.7% (7) | 49.0% (25) | 62.7% (32) | ||
| Not-reported | 5.9% (3) | 3.9% (2) | 9.8% (5) | ||
| Data type | |||||
| Primary data | 33.3% (17) | 47.1% (24) | 0.077 | 80.4% (41) | |
| Secondary data | 2.0% (1) | 17.6% (6) | 19.6% (10) | ||
| Source of data | |||||
| Schools & kindergartens | 10.4% (5) | 25% (12) | 0.037 | 35.4% (17) | |
| Local medical centers | 25% (12) | 18.8% (9) | 43.8% (21) | ||
| Non-Governmental Organizations | 2.1% (1) | 12.5% (6) | 14.6% (7) | ||
| Households or IDPs camps | - | 6.2% (3) | 6.2% (3) | ||
| Methodology | |||||
| Studies without intervention (descriptive observational) | 29.4% (15) | 56.9% (29) | 0.68 | 86.3% (44) | |
| Studies with intervention | 5.9% (3) | 7.8% (4) | 13.7% (7) | ||
| Theme of studies | |||||
| Mental Health | 3.9% (2) | 27.5% (14) | 0.028 | 31.4% (16) | |
| Oral Health | 21.6% (11) | 15.7% (8) | 0.015 | 37.3% (19) | |
| CDs | 2.0% (1) | 21.6% (11) | 0.037 | 23.5% (12) | |
| Malnutrition | 2.0% (1) | 17.6% (9) | 0.077 | 19.6% (10) | |
| Physical Injury | 0% (0) | 13.7% (7) | 0.042 | 13.7% (7) | |
| NCDs | 7.8% (4) | 9.8% (5) | 0.35 | 17.6% (9) | |
| Syrian Governorates* | n | n | % (n) | ||
| Damascus | 14 | 18 | 68.1% (32) | ||
| Aleppo | 2 | 7 | 19.1% (9) | ||
| Lattakia | 2 | 4 | 12.8% (6) | ||
| Idlib | - | 6 | 12.8% (6) | ||
| Homs | 2 | 2 | 8.5% (4) | ||
| Hama | - | 3 | 6.4% (3) | ||
| Raqqa | - | 2 | 4.3% (2) | ||
| Tatous | 1 | - | 2.1% (1) | ||
| As-Suwayda | 1 | 2.1% (1) | |||
| Deir-ez-Zor | 1 | 2.1% (1) | |||
| Rif Dimashq | - | - |
- - |
||
| Al-Hasakah | - | - | - | ||
| Quneitra | - | - | - | ||
| Daraa | - | - | - | ||
The Chi-Squared test was applied for bivariate analysis of categorical variables between Conflict- related and non-conflict related studies, p < 0.05. Categorical data are presented as % (n)
Abbreviations: GC (Government-controlled areas); NGC (Non-government-controlled area); IDPs (Internally Displaced Persons); CDs (Communicable Diseases); NCDs (Noncommunicable Diseases)
Note: Several studies spanned multiple governorates and addressed multiple health themes, contributing to more than one category in the analysis
Fig. 1.
PRISMA flow diagram
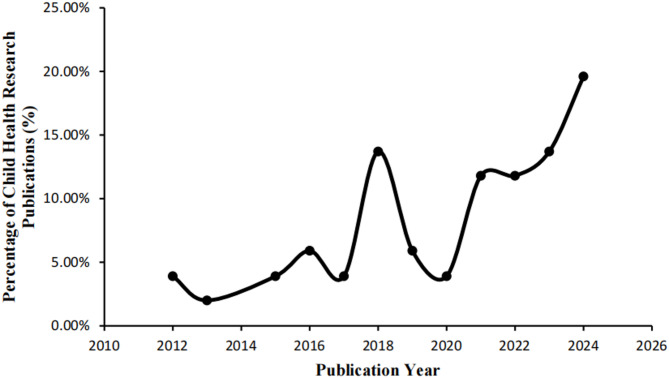
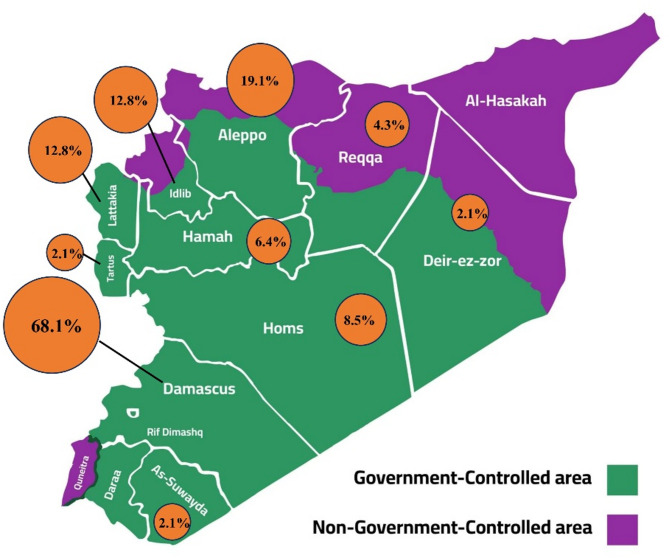
Child health research within Syria has shown a progressive increase over time, reaching its peak in 2024 (Fig. 2). As shown in Fig. 3, The majority of child health research was conducted in GC areas, comprising 77.1% of the included studies, with a notable concentration in Damascus (68.1%). Additional contributions came from Aleppo, Idlib, and Lattakia, though to a significantly lesser extent. However, there was a scarcity to an absence of studies in several other governorates, such as Deir-ez-Zor, Al-Hasakah and Daraa, highlighting significant geographical disparities in research coverage. The results indicate a significant disparity in the distribution of child health research between conflict-related and non-conflict-related studies (p = 0.002). Notably, all research conducted in NGC areas focused exclusively on conflict-related health issues. Additionally, all 16 studies affiliated exclusively with non-local institutions explicitly addressed conflict-related child health topics. Moreover, only 27.5% of child health research received funding, with a significantly higher proportion of non-conflict-related studies lacking financial support. Furthermore, our findings indicate significant differences in the focus of child health research between conflict-related and non-conflict-related contexts. Conflict-related research primarily focused on mental health, CDs, and childhood injuries, highlighting the acute and long-term health challenges associated with conflict. Conversely, non-conflict-related research emphasized children’s oral health, reflecting a greater focus on preventive and routine healthcare needs in stable settings. These differences in research priorities were statistically significant (P < 0.05 for all), underscoring the impact of contextual factors on shaping health research agendas. The majority of the studies, accounting for over 80%, were observational in nature, non-interventional, and predominantly utilized primary data collection methods coupled with quantitative analysis.
Fig. 2.
Annual Distribution of Child Health Research Publications in Syria (2012–2024)
Fig. 3.
Distribution of Child Health Research Across Syrian Governorates
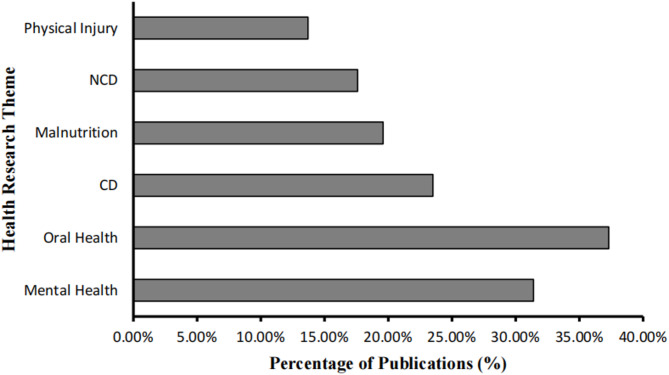
In terms of methodology, as shown in Fig. 4, Researchers frequently utilized surveys and medical records as primary sources for data extraction. In dental-related research, oral examinations were the most commonly employed method for data collection. In contrast, other methodologies such as anthropometric measurements, structured interviews, physical examinations, blood tests, and feces specimen were used less frequently. Moreover, a statistically significant association was found between study location and the type of data source used (p < 0.001). Studies conducted in government-controlled areas primarily relied on data obtained from official government institutions, including public hospitals and state-run schools. In contrast, studies carried out in non-government-controlled regions predominantly drew upon data provided by international and non-governmental organizations (NGOs), which play a key role in service delivery and health monitoring in those areas.
Fig. 4.
Distribution of Medical Research Themes in Child Health Studies by Percentage of Publications
Finally, we included 30 articles from the child health literature related to the Syrian conflict, selected based on the established inclusion criteria. This selection offers a comprehensive representation of the available research, enabling a focused analysis of child health issues within the context of the Syrian conflict. However, a meta-analysis could not be conducted due to the substantial heterogeneity of the studies, as their methodological diversity rendered statistical aggregation neither feasible nor meaningful. Characteristics of the 30 studies included in our review are presented in Table 3. The majority of the included studies were cross-sectional (63.3%) or retrospective cohort studies (26.7%), indicating a predominance of observational research designs. Only one study employed a randomized controlled trial (RCT) methodology. Additionally, two studies were prospective cohort studies, and two were case-control studies, providing a limited yet valuable comparative analysis of exposures and outcomes. Additionally, 80% of included studies received no funding at all.
Table 3.
Included studies characteristics
| First Author, Year, and Reference | Author Affiliations | Funding Status | Study Period | Geographic Location | Study Design | Population Characteristics | Key Findings |
|---|---|---|---|---|---|---|---|
| Vinay Kampalath, 2024 [13] |
First, Academic, USA. Last, Academic, UK. |
Unfunded | January 2018 to December 2022 | NGC (Idlib, Aleppo) | Retrospective Cohort |
< 18 yrs, N = 2,687,807, consultations, SAMS facilities |
Significant seasonal, displacement-related, age- and gender-specific consultation trends observed. Increased odds of injury, NCD, and mental disorder consultations with displacement and age > 12 years (p < 0.001); CD consultations decreased with displacement and peaked in winter (p < 0.001). |
| Hussein Hamdar, 2024 [14] | First & Last, Academic, Syria | Unfunded | January 2013 to January 2023 | GC (Damascus) | Retrospective Cohort |
< 13 yrs, N = 129, Public Hospital |
Challenges of diagnosing and managing tuberculosis (TB). Critical need for a multifaceted, context-specific, and pragmatic approach to TB management in conflict-affected settings. |
| Ilker Deniz Cingoz, 2022 [15] | First & Last, Academic, Turkey | Unfunded | December 2011 and May 2017 | NGC (Idlib, Aleppo) | Retrospective cohort |
< 18 yrs, years N = 62, Kilis State Hospital |
High prevalence of cranial gunshot injuries; 74.2% male patients with increased mortality in children under 9 years. |
| Seba Harphoush, 2023 [16] |
First, Academic, Syria. Last, Academic, China. |
Unfunded | February and December 2017 | GC (Homs) | Cross-Sectional |
6–9 yrs, N = 526, Schools |
Multiple forms of conflict-related malnutrition identified, including 13.8% stunting; public school students showed lower dietary intake and health knowledge scores compared to private schools during the COVID-19 pandemic. |
| Abdullah S. Terkawi, 2019 [17] |
First, Humanitarian, USA. Last, Academic, SAU. |
Unfunded | February to December 2017 | NGC (Idlib) | Prospective cohort |
< 19 yrs, N = 11,819, SEMA-affiliated medical center |
Urgent healthcare issues within this population, especially in IDPs camps, including severe malnutrition high rates of infectious diseases, and teenage pregnancy. |
| Lana Meiqari, 2017 [18] |
First & Last, Humanitarian (MSF), The Netherlands. |
Unfunded | 2013–2016 | NGC areas (Aleppo and Al Raqqa) | Retrospective Cohort |
< 5 yrs, N = 641 − 18,012 < 18 yrs, N = 1,823-2,849 Medical Centers (MSF’s activities in northern Syria.) |
High rates of infectious diseases and malnutrition, attributed to high mortality rate in children under 5 years old. Mortality rates were highest among children under 6 months. |
| Gerlant van Berlaer, 2017 [19] | First & Last, Academic, Belgium. | Unfunded | June 2015 | NGC (Idlib, Hamah, Lattakia) | Cross-sectional |
> 15 yrs, N = 1002, Households, shelters, & medical centers |
The study describes the deteriorating living conditions of children in northern Syria and the lack of healthcare, which contribute to a high prevalence of infections among children (64%) and an increase in epidemic incidence and morbidity. |
| Alan de Lima Pereira, 2018 [20] |
First, Humanitarian (MSF) Syria. Last, Humanitarian (MSF), The Netherlands |
Unfunded | 2015 | NGC (Aleppo) | Cross-sectional |
< 5 yrs, Pre- vaccination N = 212 Post- vaccination N = 280, Households |
The study demonstrates that the collapse of the formal public health system in Syria has led to a significant increase in the susceptibility of children to infectious diseases, with younger children being particularly vulnerable. |
| Abdallah Mohamed Elsafti, 2016 [21] |
First, Health, Qatar Last, Academic, Belgium. |
Unfunded | January to March 2023 | NGC (Aleppo, Idlib, Hamah, and Lattakia) | Cross-sectional |
< 15 yrs, N = 1001, Households & IDPs camps |
Children experienced displacement 20%, lack of education 51%, and insufficient health care provision 64%. These factors significantly elevate the risk of abuse, exploitation, malnutrition, and communicable diseases, leading to increased morbidity and mortality. |
| Chukwuma Mbaeyi, 2021 [22] |
First, Organization, USA. Last, Organization, Jordan. |
Funded, by the U.S. Centers for Disease Control and Prevention and the World Health Organization | January 2016 to December 2018 |
GC & NGC (Deir-ez-Zor, Raqqa, and Homs) |
Retrospective Cohort | 4–155 months, N = 74, medical centers | 96% of polio cases originated from Deir-ez-Zor; unvaccinated risk higher in outbreak zones (OR: 2.53; p < 0.0001). Three vaccination rounds achieved > 80% coverage, containing the outbreak within 120 days. |
| Bahaa Aldin Alhaffar, 2019 [23] | First & Last, Academic, Syria. | Unfunded | September 2016 to January 2017 | GC (Damascus) | Cross-Sectional |
9–14 yrs, N = 811, schools |
High levels of dental caries and elevated DMFT scores. Worsen oral health was associated with deteriorated socioeconomic status which linked to the Syrian conflict. |
| Muhammed Al-Huda Ballouk, 2019 [24] | First & Last, Academic, Syria. | Unfunded | September 2016 to January 2017. | GC (Damascus) | Cross-Sectional |
8–12 yrs, N = 1500, schools |
High prevalence of dental caries 79.1% and elevated DMFT and dmft indices. Relationship between localities and caries prevalence: p < 0.001. |
| Muhammed Al-Huda Ballouk, 2018 [25] | First & Last, Academic, Syria. | Unfunded | September- October 2017 | GC (Damascus) | Cross-Sectional |
8–12 yrs, N = 1500, schools |
High gingivitis prevalence (97.93%) linked to malnutrition, poor diet, lack of water fluoridation, limited healthcare access, and financial hardship; significant gender and locality differences (p < 0.001). |
| M. H. D. Bahaa Aldin Alhaffar, 2018 [26] | First & Last, Academic, Syria. | Unfunded | Not reported | GC (Damascus) | Cross-Sectional |
Mean = 12.5 yrs, N = 811, schools |
High prevalence of PTSD (91.5%) related to the Syrian conflict, which was associated with deteriorated oral health and a high dental caries rate of 86%, p = 0.045). |
| Sulaf H. Hamid, 2018 [27] | First & Last. Academic, Syria. |
Funded, by Damascus University |
Not-reported | GC (Damascus) | Case-Control | 9–14 yrs, N = 60, Public Hospital | Increased PTSD severity associated with deteriorated dental and gingival health; significant differences in Plaque and Gingival Index between PTSD and control groups (p < 0.0001). |
| Wail Habal, 2024 [28] |
First, Academic, GBR. Last, Academic, SAU. |
Unfunded | Not reported | GC (Damascus) | Cross-Sectional |
12–17 yrs, N = 99, Public Hospital |
PTSD (52.5%) and abnormal sleep (42.4%) were associated with poor oral health and adolescents smoking, linked to rural residence and lower parental education (p < 0.05). |
| Nada Raslan, 2021 [29] | First & Last, Academic, UK. | Unfunded | 2017 to 2019 |
NGC (Idlib) |
Retrospective Cohort & cross-Sectional |
4–14 yrs old, N = 376, Schools operated by Save the children organization |
73.7% of children faced mental health issues (anxiety, depression, PTSD) with poor socialization skills; adolescents were more prone to child labor, extreme poverty, aggressive behavior, and educational decline. |
| Aya Alsharif, 2024 [30] | First & Last, Academic, Syria. | Unfunded | Not reported | GC (Damascus) | Cross-Sectional |
2–17 yrs, N = 991, Public Hospital |
High prevalence of behavioral and emotional difficulties: 74.67% in children aged 2–4 years and 61.29% in those aged 5–17 years, linked to direct and indirect war-related factors (p < 0.05). |
| Mohammad Kalthom, 2024 [31] | First & Last, Academic, Iran. | Unfunded | Not reported | GC (Hamah) | RCT |
6–12 yrs, N = 92, Schools |
Self-Narrative Art Therapy significantly reduced PTSD symptoms across all dimensions (p < 0.01) among Syrian children affected by war. |
| Ameer Kakaje, 2020 [32] | First & Last, Academic, Syria. | Unfunded | 1 to 12 March 2020 | GC (Damascus) | Cross-Sectional |
< 18 yrs, N = 1369, Schools |
The study indicates 53% PTSD and problematic anger 62%, significantly associated with war exposure (p < 0.05), with social support playing a minimal role, The negative impact is more pronounced in females, and there is a high prevalence of smoking. |
| Jon Davis Perkins. 2021 [33] |
First, Academic, UK. Last, Academic, Qatar |
Funded Qatar National Library |
Not reported | GC (Damascus) | Cross-Sectional |
8–15 yrs, N = 250, Schools |
Supported cross-cultural use of self-report screening for depression and anxiety; females scored higher than males for anxiety (18.22 vs. 15.05, p = 0.003). |
| Jon Davis Perkins, 2018 [34] |
First, Academic, UK. Last, Academic, Syria. |
Unfunded | 2016 | GC (Damascus, Lattakia) | Cross-Sectional |
8–15 yrs, N = 492, Schools |
War-related traumatic stress significantly impacted psychological well-being; PTSD symptoms associated with warzone exposure (OR 1.84, 95% CI 1.02–3.30, p = 0.042) and displacement (OR 2.67, 95% CI 1.08–6.60, p = 0.034). |
| Mhd Obai Alchallah, 2023 [35] | First & Last, Academic, Syria. | Unfunded | Not-reported | GC (Damascus) | Cross-Sectional |
6–15 yrs, N = 1029, Schools |
High prevalence of OSAS (22.2%) linked to the Syrian conflict, with a positive correlation to daytime sleepiness, particularly among males.15.2% (p < 0.05). |
| Bahaa Aldin Alhaffar, 2022 [36] | First & Last, Academic, Syria. | Unfunded | February 2019 to April 2019. | GC (Damascus) | Cross-sectional study. |
3–14 years N = 40, Public Hospital |
Children undergoing chemotherapy showed higher DMFT and pain compared to healthy peers, linked to post-conflict healthcare shortages. |
| Issam N. Albaroudi, 2018 [37] | First & Last, Academic, Syria. |
Funded, by Damascus University |
November 2011 to November 2015 | GC (Damascus) | Cross-Sectional & prospective cohort | 4 months to 14 yrs, N = 1128, Public Hospital | Substantial prevalence of anemia (57%), iron deficiency (71.85%), and iron deficiency anemia (55.55%) during the Syrian conflict among a cohort of ostensibly healthy children in Damascus, Syria. |
| Aya Al Habbal, 2021 [38] | First & Last, Academic, Syria. | Unfunded | October 2019 to February 2020 | GC (Damascus) | Case-Control | > 18 yrs, N = 334, Medical center | Substantial burden of epilepsy identified after the conflict, with family history and central nervous system infections as major risk factors. |
| Yousser Mohammad, 2023 [39] |
First, Academic, Syria. Last, Academic, New Zealand. |
Funded, by The Medical Syndicate in Latakia and the Syrian Private University. |
2018–2019 | GC (Damascus, Lattakia) | Cross-Sectional |
13–14 yrs, N = 2315, Schools |
Non-communicable diseases The study shows increased asthma indicators among children, with wheeze prevalence at 19.8% and severe wheeze at 12.8%, linked to war-related pollution and stress. |
| Bassam Darwish, 2018 [40] | First & Last, Academic, Syria. | Unfunded | January 2005 to December 2016 | GC (Damascus) | Retrospective Study | > 18 yrs, N = 256, Public Hospital | Significant increase in the incidence of pediatric chest injuries in Syria post-conflict. The overall mortality rate was 7.8%. |
| Fatema Mohsen, 2021 [41] | First & Last, Academic, Syria. | Unfunded | January 2011 and June 2018. | GC (Damascus) | Retrospective Study |
> 13 years, N = 560, Public Hospitals |
High incidence of foreign body aspiration, peaking in the 1 to 3 years age group (67.2%), exacerbated by severe medical supply shortages post-conflict. |
| Pari Chowdhary, 2022 [42] |
First, Humanitarian, USA. Last, Humanitarian, Turkey. |
Funded, by the United Nations Population Fund (UNFPA) and USAID’s Bureau of Humanitarian Assistance. |
January to December 2020. |
NGC (Aleppo, Idlib) |
Cross-Sectional | 10–18 yrs, N = 104, Humanitarian Medical Center (AMAL Initiative activity) | 34% increase in child marriages post-conflict; health and social interventions improved self-esteem (+ 39%), community support for family planning (+ 27%), and advocacy for equal access to services (+ 35%). |
Abbreviations: GC (Government-controlled areas); NGC (Non-government-controlled area); PTSD (Post-Traumatic Stress Disorder); DMFT (Decayed, Missing, and Filled Teeth); IDPs (Internally Displaced Persons); RCT (Randomized Controlled Trial); OSAS (Obstructive Sleep Apnea Syndrome); CD (Communicable Diseases); NCD (Noncommunicable Diseases); SAMS (Syrian American Medical Society); SEMA (The Syrian Expatriates Medical Association); MSF (Médecins Sans Frontières)
Discussion
This scoping review identified 51 studies published after the onset of the Syrian conflict that focused on the health of children residing within Syria. Of these, 30 studies were directly or indirectly related to the impact of the conflict. The findings indicate a growing body of health research in Syria in the post-conflict period; however, substantial gaps persist in the literature, particularly concerning medical conditions associated with the Syrian conflict [43].
Burden of physical trauma and injuries
The protracted conflict in Syria has inflicted a severe toll on children’s physical health, particularly in war-affected regions such as Northern Syria. Although numerous children have sustained injuries as a direct result of the violence, only 13.7% of child health research conducted during the conflict has focused on physical trauma among children residing within Syria. This highlights a significant gap in the literature, particularly in capturing the realities faced by those living in active conflict zones [44]. Most available data come from hospitals in neighboring Turkey, especially facilities in border towns like Hatay and Kilis, which have served as key referral centers for injured Syrian children [45–48]. For instance, Çelikkaya et al. reported that over half of the children treated for war-related injuries at a major hospital in Hatay presented with severe trauma, and many died due to delayed intervention and injury severity [48]. Widespread shelling and aerial bombardments have been identified as the leading causes of pediatric mortality, accounting for over 70% of deaths in conflict zones [45, 49]. In 2016, child deaths from war-related injuries reached 23.3%, with the highest numbers reported in Aleppo, Idlib, and Daraa [50]. Moreover, forced displacement has significantly increased the risk of injury among children in Northern Syria. Adolescents aged 12–17 years were especially vulnerable, with markedly higher odds of trauma-related disorders compared to younger age groups [13]. Within Syria, particularly in GC regions, war-related injuries have also been reported; however, clinical response has been hampered by shortages of medical equipment, economic instability, and a lack of trained personnel [51–53]. A study from Al-Mouwasat Hospital found that one-third of burn patients died from their injuries, with children making up over half of the sample and showing the highest rates of leaving the hospital against medical advice [53]. Data collection within Syria remains limited due to security concerns and fear of government retaliation, particularly in underserved or besieged areas. These findings underscore the urgent need for improved documentation, coordinated trauma care, and child protection efforts within conflict settings.
Burden of mental disorders
The existing body of literature predominantly concentrates on the psychological well-being of Syrian children refugees residing in neighboring countries [54, 55]. In contrast, there is a notable paucity of research addressing the mental health of children remaining within Syria. However, indictors of higher prevalence of conflict-related mental disorders between Syrians living within Syria compared to Syrian refugees were reported [56]. Based on our results, mental health was number one on the list of discussed subjects on conflict related child health research. The toll of war on mental health has become increasingly acknowledged, with conditions such as: post-traumatic stress disorder (PTSD), depression, anxiety, obstructive sleep apnoea syndrome and increasing suicidal behaviors gaining recognition, which are largely attributed to worsening economic conditions and harsh living circumstances [34, 35, 54, 55]. Moreover, internal displacement, exposure to violence, and lack of basic resources in NGC areas have significantly contributed to the increased prevalence of mental disorders [13, 29, 49]. Adolescent boys, who were tragically drawn into armed conflicts and labor [29], and teenage girls, who were frequently subjected to early marriage [17, 42], are particularly affected. In GC areas, more than 50% of school-aged children demonstrated symptoms of PTSD as a result of prolonged exposure to armed conflict and internal displacement [32, 34]. Adolescent males, in particular, were subjected to forced labor, which was associated with deteriorating physical health, exacerbated anger issues, and a higher incidence of smoking [32]. These adverse psychosocial and physical factors have had a profound impact on students’ cognitive and emotional well-being, leading to a marked decline in academic performance across the affected student population. Furthermore, behavioral difficulties prevalence was notably high among children affected by the Syrian conflict, with 74.67% of children aged 2–4 years and 61.29% of children aged 5–17 years exhibiting such challenges. These behavioral issues were significantly associated with war-related factors, including the loss of family members, disruptions in school attendance, and ongoing economic hardships (p < 0.05) [30]. Although intervention studies were limited, supportive strategies demonstrated effectiveness [29]. For instance, art therapy significantly reduced PTSD symptoms among war-affected and internally displaced children (P < 0.01) [31]. Additionally, community-based social support programs for pregnant teenagers were found to enhance self-confidence and promote self-care behaviors [42]. Providing adequate mental health care faces notable challenges, including cultural barriers and a shortage of trained professionals [57, 58]. Expanding the psychiatric knowledge of medical staff and enhancing the availability of mental health services in public sectors, including medical centers and schools, are critical steps to alleviate the burden of conflict-related mental disorders [59].
Burden of communicable diseases cds
CDs ranked second among medical concerns post- conflict, following mental disorders, in the context of children affected by the conflict. The majority of studies on CD in children have primarily focused on Northern Syria and IDP camps, reflecting the high prevalence of these conditions in regions severely affected by conflict and displacement [19, 60]. The deteriorating living conditions within IDP camps, coupled with widespread poverty and a severe lack of medical services, exacerbated the vulnerability of children to infections [17, 19, 20]. These risks peaked during the winter months, when overcrowded conditions and limited access to sanitation and healthcare facilities heightened the transmission of infectious diseases [13, 21]. Furthermore, vaccine-preventable infections emerged as a significant concern due to disruptions in routine immunization programs, which were compounded by the mass displacement and the associated breakdown in healthcare infrastructure [18, 20, 21]. Children under the age of five were particularly vulnerable to infections, a susceptibility often compounded by malnutrition, leading to elevated rates of morbidity and mortality [18, 21]. Syria was classified as one of the fragile countries in the face of the COVID-19 epidemic leading to destructive effects on women and child health [16, 61, 62]. More than two thirds of the children in Northern Syria suffer from infections, mainly of respiratory, neurological, digestive and dermatological origin [19, 63]. Children respiratory infection cases contributed to 73% of respiratory infection cases in Northern Syria prior to the COVID-19 epidemic [63]. Children and neonates’ mortality of infection has increased with the critical lack of medical services and hard access to medical points [64, 65]. Moreover, vaccine-preventable diseases such as tuberculosis (TB), measles, and polio were reported in both GC and NGC areas [14, 66, 67]. The implementation of vaccination program helped successfully supplant the vaccines related diseases [22]. The lack of appropriate maintenance and destroyed understructure contributed to insufficient clean water supplies and increase the chance of contamination which is the main cause of outbreaks like Cholera [68, 69]. Despite the lack of sufficient COVID pandemic related research in Syria, it’s very clear that COVID epidemic imposed a pressure on the Syrian socioeconomic situation and exacerbated the mental stress for the community which is already devasted by the war [70]. The negative impact of the COVID-19 pandemic on food insecurity and the nutritional status of children is also critical [16, 71]. Further detrimental impact was on the social, psychological, and economic well-being of children with health problems [72]. Furthermore, the COVID-19 crisis has escalated into a children’s crisis in IDP camps. The lack of child protection services, minimal preventive measures, and inadequate sanitation have left children, already suffering from weakened immune systems or underlying health conditions due to living in desperate conditions, particularly vulnerable to this vicious virus [65, 73].
Burden of oral diseases
Prior to the conflict, Syria has suffered from the burden of poor oral health between children and the heavy years of conflict had certainly worsen the children oral health in many aspects with limited studies in this field [74, 75]. Oral health is very important health indicator, which could be assessed easily and with affordable costs. In our search, 19 studies were detected examining the children oral health inside Syria after the conflict, 7 of them were included based on our criteria, with age ranged between 8 and 17 years old, the geographic distribution of these studies was in GC areas of Damascus governance, no studies related to oral health was detected in NGC areas. Notably, children with pre-existing medical conditions [76, 77], particularly those undergoing chemotherapy in Syria [36], exhibited a significantly higher incidence of poor oral health. The ongoing war has created numerous barriers to healthcare access and continuity of treatment, further exacerbating the oral health challenges faced by these children.
Additionally, a significant association between poor oral health and war-related mental health disorders was observed among school students in Damascus [26–28]. In addition to the high prevalence of smoking among adolescents, passive smoking among children also contributes to worsening oral health [78, 79]. The role of the conflict in the deteriorated oral health was expanding, with the collapse of families’ financial situation, decline the educational level and health awareness which contribute to the failure of the application of minimal health guidelines. In addition, high carbohydrates and sugar intake was related to early dental caries and linked to poor socioeconomic and knowledge background [74, 80].
Burden of malnutrition and non-communicable diseases NCDs
The nutritional status of children in Syria remains critically under-documented, particularly concerning micronutrient deficiencies such as iron deficiency anemia and vitamin D deficiency. This data gap limits the ability to implement targeted interventions. Nonetheless, existing evidence suggests severe levels of undernutrition among children, especially those living in IDP camps, due to widespread poverty, food insecurity, and inadequate healthcare access [81]. According to the WHO and Ministry of Health’s Nutrition Surveillance System (2018), the prevalence of Global Acute Malnutrition (GAM) among children under five was 12%, with 30% of those affected identified as stunted [82]. Recent studies further highlight a dual burden of malnutrition and obesity. In 2021, Syria recorded one of the highest global rates of concurrent stunting and overweight in children (12.3%) [83]. A national growth reference study found overweight and obesity rates of approximately 20% and 4% respectively, linked to increased consumption of low-cost, carbohydrate-rich diets amid economic decline [84]. Anemia remains widespread; for example, in Damascus, prevalence rates for anemia, iron deficiency, and iron deficiency anemia reached 57%, 71.85%, and 55.55%, respectively [37]. In NGC regions, malnutrition and severe acute malnutrition were notably higher among IDP children, particularly infants and toddlers [17, 18, 21]. One study reported nutritional deficiencies in 8% of the child population, with significantly higher rates of chronic anemia, malnutrition, and severe acute malnutrition observed among IDP children [17]. Additionally, girls had significantly higher odds of receiving nutrition consultation (AOR: 1.52, p < 0.001) [13].
Regarding non-communicable diseases, only nine studies addressed pediatric NCDs, five of which were conflict-related. These focused on conditions such as asthma, epilepsy, and cancer, primarily in GC areas [38, 39, 72, 85]. Post-conflict evidence points to increased asthma prevalence, likely linked to war-related stress and environmental exposure [39, 86, 87]. While data from non-government-controlled regions remain limited [17], findings suggest that displacement increases the likelihood of developing NCDs among children in northern Syria [13].
Challenges and gaps in child health research within Syria
During the past fourteen years, the IDP crisis in Syria has worsened both in quantity and quality, as IDPs often receive less recognition and protection and face greater barriers to accessing humanitarian interventions compared to refugee populations [6, 88, 89]. Despite the escalating needs and increased attention, funding remains critically insufficient, with a 62% shortfall reported in 2023 [90]. The socio-economic situation in Syria continues to deteriorate as sanctions persist and humanitarian funding decreases, resulting in a further breakdown in access to services and livelihoods [91]. This situation has been further exacerbated by the COVID-19 pandemic in 2020 and the earthquakes in 2023, which have intensified vulnerabilities, increased medical needs, displaced families once again, and heightened the suffering of children [92, 93].
Post-conflict health research has seen a notable increase in publication rates. However, research within Syria is subject to significant limitations [9, 10, 89]. Within Syria, researchers in GC areas encounter significant barriers, including inadequate funding, limited institutional support, and restricted access to essential tools and resources. Moreover, the ability to conduct conflict-related research in these regions is further constrained by political sensitivities, lack of data transparency, and concerns over researcher safety, all of which have impeded the production of independent and systematic studies in these areas despite the occurrence of significant conflict. Students at both government and non-government institutions face considerable challenges in securing financial support to pursue advanced research, compounded by the lack of reliable data due to the extensive damage and underdevelopment of the country’s infrastructure. The analysis revealed that only 27.5% of the total child health research conducted within Syria received funding, and 80% of conflict related research received no funds. This underscores a significant gap in financial support for critical research focused on the health of children in the region, highlighting the need for increased investment and resources to address the pressing health challenges faced by Syrian children. The lack of funding likely impacts both the reliability and comprehensiveness of the research, as limited financial resources constrain study design, sample size, data collection methods, and analytical rigor. Unfunded studies may also face challenges in ensuring adequate quality control, leading to increased risks of bias, incomplete data, and reduced generalizability of findings. In NGC areas, local institutions and international organizations are further restricted by difficult access and the dangers posed by ongoing conflict [9, 10, 81]. However, research in NGC regions has been more heavily supported by NGOs and funded by foreign organizations [18, 63, 81].
Furthermore, the ability of Syrian researchers to conduct high-quality studies is significantly constrained. This limitation is evidenced by our findings, which reveal that the majority of existing studies are observational in nature, lacking experimental interventions, and with a minimal presence of RCTs. This underscores the need for methodological advancements and greater research capacity within the Syrian scientific community [89]. The overall quality of included studies is moderate, with cross-sectional and retrospective cohort studies dominating the review. While they provide valuable epidemiological insights, their inability to establish causality, susceptibility to bias, and limited statistical control over confounders reduce their reliability. The inclusion of prospective cohort studies, case-control studies, and a single RCT adds depth but is insufficient to significantly strengthen causal inferences. This lack of methodological rigor directly limits the development of effective evidence-based policies and interventions, as policymakers are forced to rely on descriptive data without robust causal insights needed for targeted, efficient, and context-specific health strategies.
The findings underscore the imperative for an enhanced geographical diversity in research pertaining to IDP. Predominantly, studies on IDPs have been confined to north-western Syria, a trend also observed in another scoping review [49]. Additionally, consistent with findings from a previous review [10], our analysis highlights a significant geographic disparity in child health research within Syria. The majority of studies have been conducted in GC areas, particularly within the Damascus Governorate, often in affiliation with Damascus University. In contrast, research from other regions (such as Daraa, Al-Hasakah, Deir ez-Zor, and Raqqa) remains extremely limited or entirely absent. This underrepresentation is likely due to a combination of factors, including security concerns, restricted access for researchers, limited institutional capacity, and the collapse of healthcare and academic infrastructures in conflict-affected and opposition-held areas. Such research is exceedingly rare in other governorates, a gap further compounded by the absence of involvement from other local higher education institutions. This geographical concentration may lead to findings that do not accurately represent the broader spectrum of child health issues across Syria especially for IDP. Such geographic bias poses critical challenges to the generalizability of findings, as studies concentrated in relatively more stable, government-controlled areas may fail to capture the full extent of health burdens faced by children in underserved or severely affected regions, particularly among IDPs. This skewed evidence base risks informing policies and interventions that are not fully aligned with the needs of vulnerable populations across Syria.
Recommendations for rebuilding child health and Well-being in Post-Conflict Syria
The rehabilitation of public infrastructure following the Syrian conflict is a national imperative, particularly in the health sector. Rebuilding the healthcare system requires coordinated efforts among all stakeholders, including the implementation of supportive legislation, strategic planning, and the integration of modern technologies to overcome structural and operational challenges.
To inform effective interventions, future research must gradually adopt more rigorous yet context-appropriate methodologies, such as prospective cohort studies, nested case-control designs, and implementation science approaches. Our review underscores the urgent need to invest in research capacity-building, particularly among local institutions and community organizations, to foster context-specific, community-driven research. Expanding methodological diversity and addressing geographic gaps will be critical to generating reliable, locally relevant evidence and ensuring that health policies are equitable, inclusive, and responsive to regional disparities.
Comprehensive and ongoing monitoring of children’s health is vital to understanding both the immediate and long-term consequences of conflict exposure. Reliable data collection will allow for the tailoring of health interventions to specific needs and vulnerabilities. In particular, systematic investigations into communicable diseases (CDs) and non-communicable diseases (NCDs) among children across all Syrian governorates should be prioritized. Such research should evaluate not only disease burden but also the capacity, resilience, and readiness of medical facilities. It must also identify systemic barriers, resource constraints, and infrastructural deficits that hinder effective healthcare delivery. These findings are critical for evidence-based policy formulation and resource allocation aimed at improving child health at both regional and national levels.
Mental health services must be urgently rehabilitated to address the psychological toll of protracted conflict, particularly among children. Expanding the psychiatric training of healthcare professionals and increasing the availability of mental health services—especially within public institutions such as schools and health centers—is essential to reduce the burden of post-traumatic stress, anxiety, and related disorders.
Emerging evidence suggests that psychological distress from conflict exposure is also linked to poor oral health in children. Consequently, oral health research should be broadened to encompass diverse age groups and regions. Schools, given their accessibility and trust within communities, are well-positioned to serve as research sites and platforms for implementing health promotion and preventive interventions.
In the broader context of child protection and development, schools play a vital role beyond education. They serve as safe spaces that shield children from exploitation and child labor while facilitating access to psychological, nutritional, and healthcare services. Strengthening the education sector, through targeted financing, teacher training, and psychosocial support, is thus an urgent priority. The interdependence of the health and education sectors in post-conflict Syria underscores the need for collaborative planning and implementation of child-focused interventions.
Finally, while the debate over international sanctions on Syria remains politically complex, their humanitarian consequences cannot be overlooked. Easing or lifting sanctions could facilitate the delivery of essential medical supplies and aid, support economic recovery, and improve the broader social determinants of child health. Enhanced economic stability could reduce psychosocial stressors among children and provide a foundation for long-term improvements in well-being and opportunity.
Actionable next steps for rebuilding child health and well-being in post-conflict Syria
Short-term (Within 12 Months)
Advocate for Humanitarian Adjustment or Lifting of Sanctions.
Engage international stakeholders to ease or lift sanctions that restrict the importation of essential medical supplies, equipment, and humanitarian aid.
Prioritize exemptions for child health services, medications, and food security programs to immediately improve health outcomes and reduce psychosocial stressors among children.
-
2.
Conduct a National Rapid Assessment.
Map the availability and gaps in pediatric health services, mental health infrastructure, school-based health programs, and the implementation of nutrition support and child protection programs across all governorates.
Use findings to prioritize high-need areas and guide the allocation of resources and programmatic support.
-
3.
Establish a Conflict-Aware Health Surveillance System.
Launch sentinel surveillance in schools and clinics to monitor key child health indicators such as malnutrition, trauma symptoms, communicable and non-communicable diseases, and the treatment of war-related injuries.
Ensure data collection systems are sensitive to conflict exposure and capable of informing targeted health interventions in high-risk areas.
-
4.
Initiate Capacity-Building Programs.
Organize workshops and online training for local professionals on child-focused research, basic mental health care, and data collection.
-
5.
Support Local Research Networks.
Provide micro-grants and technical support to local universities and NGOs to conduct small-scale, regionally focused health studies.
Medium-term (1–3 Years)
-
6.
Expand Rigorous Epidemiological Studies.
Implement multicenter prospective cohort studies and RCTs focusing on nutrition, NCDs, CDs, mental health, and oral health.
-
7.
Integrate School-Based Health Services.
Pilot comprehensive school health programs offering screening, counseling, and preventive care in partnership with local health departments.
-
8.
Develop and Implement a National Oral Health Strategy.
Launch region-specific oral health campaigns targeting schoolchildren, particularly in areas affected by conflict and displacement.
-
9.
Rehabilitate Mental Health Infrastructure.
Rebuild mental health services in public health facilities and schools, and train general practitioners in basic psychological care.
-
10.
Formalize Health-Education Collaboration.
Establish inter-ministerial working groups to design joint policies and shared funding mechanisms for health and education interventions.
Long-term (3–5 Years)
-
11.
Institutionalize Data-Driven Policy Development.
Create a National Child Health Observatory to coordinate data collection, analysis, and policy translation at national and subnational levels.
-
12.
Rebuild Health Infrastructure with Modern Technologies.
Integrate telemedicine, mobile health tools, and e-health platforms into post-conflict reconstruction to expand care delivery in hard-to-reach areas.
-
13.
Sustain Local Ownership and International Collaboration.
Strengthen long-term partnerships between Syrian institutions and international research centers to promote sustainable, evidence-informed child health strategies.
Limitations
This study acknowledges several important limitations that should be considered when interpreting the findings:
Due to significant geographic constraints and the moderate quality of available evidence within the child health literature in Syria, detailed analysis of specific child health parameters was not feasible. Additionally, regional classifications used in this study reflect territorial control and demographic conditions at the time of data collection, which have been highly dynamic throughout the Syrian conflict. Therefore, these classifications may not represent static or uniform entities over time.
The study reflects the inherent difficulties associated with research in conflict zones, including:
Methodological challenges, such as reliance on observational studies and limited access to comprehensive data.
Financial constraints, due to scarce funding opportunities for in-country research.
Logistical barriers, including security concerns, displacement, and restricted access to certain regions.
While much of the existing health research has focused on Syrian refugees in neighboring countries, there is a noticeable gap in studies addressing the health and well-being of IDPs and children residing within Syria. This imbalance limits comprehensive understanding of child health realities for those remaining inside conflict-affected areas.
The fluid nature of territorial control, ongoing displacement, and demographic shifts throughout the conflict present additional challenges in ensuring that findings remain representative over time.
Despite these limitations, this study offers a valuable contribution to the literature on child health and child rights violations in conflict settings. To our knowledge, it represents the first review explicitly focusing on the post- conflict health realities of children within Syria, highlighting critical gaps and informing future research priorities.
Conclusion
Given the geographic constraints, heterogeneity, and moderate quality of available evidence, a precise analysis of specific child health parameters in Syria remains challenging. However, this review makes a valuable contribution to the literature on child health and rights violations in conflict settings. The findings highlight methodological, financial, and logistical barriers to research in conflict zones, along with significant gaps in medical research, particularly concerning children within Syria, conflict-affected areas, and IDPs. Despite these limitations, this is the first review to explicitly examine the post- conflict health realities of children in Syria. As Syria transitions into a post-conflict era, there is an urgent need to rebuild not only the physical infrastructure but also the institutional frameworks that support research, healthcare delivery, and sustainable development.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Author contributions
SH Led the conceptualization, design, and methodology of the study, and was responsible for drafting and writing the manuscript. SH, FA, IH independently reviewed all titles, abstracts, and full-text articles, extracting relevant data. In cases of disagreement or uncertainty, they consulted a third researcher (RK or RA), LZ supervised and assisted in structuring the manuscript, reviewing drafts, and ensuring consistency in reporting. All authors provided critical revisions, contributed to the interpretation of findings, and approved the final version of the manuscript for submission.
Funding
The authors confirm the independence of this research completely from any governmental or non-governmental authorities or local /international organizations, and the research is self-funded by the authors.
Data availability
Data is provided within the manuscript or supplementary information files.
Declarations
Ethics approval and consent to participate
Not applicable.
Competing interests
The authors declare no competing interests.
Footnotes
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Seba Harphoush, Email: sebaharphoush6@gmail.com.
Zhong Li, Email: lz-ny@njmu.edu.cn.
References
- 1.Sahloul MZ, Monla-Hassan J, Sankari A, Kherallah M, Atassi B, Badr S, Abbara A, Sparrow A. War is the enemy of health. Pulmonary, critical care, and sleep medicine in War-Torn Syria. Ann Am Thorac Soc. 2016;13(2):147–55. [DOI] [PubMed] [Google Scholar]
- 2.Alhaffar MHDBA, Janos S. Public health consequences after ten years of the Syrian crisis: a literature review. Globalization Health 2021;17(1):111. [DOI] [PMC free article] [PubMed]
- 3.Syrian refugee crisis. facts, FAQs, and how to help [https://www.worldvision.org/refugees-news-stories/syrian-refugee-crisis-facts]
- 4.Cantor D, Swartz J, Roberts B, Abbara A, Ager A, Bhutta ZA, Blanchet K, Madoro Bunte D, Chukwuorji JC, Daoud N, et al. Understanding the health needs of internally displaced persons: A scoping review. J Migr Health. 2021;4:100071. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Abbara A, Rayes D, Ekzayez A, Jabbour S, Marzouk M, Alnahhas H, Basha S, Katurji Z, Sullivan R, Fouad FM. The health of internally displaced people in Syria: are current systems fit for purpose? J Migr Health. 2022;6:100126. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Aburas R, Najeeb A, Baageel L, Mackey TK. The Syrian conflict: a case study of the challenges and acute need for medical humanitarian operations for women and children internally displaced persons. BMC Med 2018;16(1):65. [DOI] [PMC free article] [PubMed]
- 7.Syrian Arab Republic| Project profile. Building local resilience in the Syrian Arab Republic [https://openknowledge.fao.org/items/a87064c8-c985-463d-9334-0755dd57fa96]
- 8.UNICEF. UNICEF warns of looming child nutrition crisis in Syria amid 12 years of conflict and deadly earthquakes. https://www.unicef.org. (2023 ).Accessed 24 May 2025. https://www.unicef.org/press-releases/unicef-warns-looming-child-nutrition-crisis-syria-amid-12-years-conflict-and-deadly
- 9.Abdul-Khalek RA, Kayyal W, Akkawi AR, Almalla M, Arif K, Bou-Karroum L, El-Harakeh A, Elzalabany MK, Fadlallah R, Ghaddar F, et al. Health-related articles on Syria before and after the start of armed conflict: a scoping review for the Lancet-American university of Beirut commission on Syria. Confl Health. 2020;14(1):73. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Abouzeid M, Elzalabany MK, Nuwayhid I, Jabbour S. Conflict-related health research in Syria, 2011–2019: a scoping review for the Lancet-AUB commission on Syria. Confl Health. 2021;15:1–34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, Moher D, Peters MD, Horsley T, Weeks L. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169(7):467–73. [DOI] [PubMed] [Google Scholar]
- 12.Pollock D, Peters MD, Khalil H, McInerney P, Alexander L, Tricco AC, Evans C, de Moraes ÉB, Godfrey CM, Pieper D. Recommendations for the extraction, analysis, and presentation of results in scoping reviews. JBI Evid Synth. 2023;21(3):520–32. [DOI] [PubMed] [Google Scholar]
- 13.Kampalath V, Tarnas M, Patel V, Hamze M, Albik A, Kassas MA, Loutfi R, Abbara A. 6535 The impact of armed conflict on paediatric healthcare consultations in Northwest Syria. In.: BMJ Publishing Group Ltd; 2024.
- 14.Hamdar H, Nahle AA, Ataya J, Jawad A, Salame H, Jaber R, Kassir M, Wannous H. Comparative analysis of pediatric pulmonary and extrapulmonary tuberculosis: A single-center retrospective cohort study in Syria. Heliyon 2024;10(17):e36779. [DOI] [PMC free article] [PubMed]
- 15.Cingoz ID, Kaya I, Sahin MC, Vural M. Pediatric cranial injuries: the Syrian civil war. Childs Nerv Syst. 2022;38(9):1743–49. [DOI] [PubMed] [Google Scholar]
- 16.Harphoush S, Shahood B, Harphoush I, Awudi DA, Ahmad S, Zaitoun M, Weeto MM, Li Z. The impact of crisis and COVID-19 on Syrian children growth, health awareness and nutritional practices. A cross-sectional study. BMC Pediatr. 2023;23(1):295. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Terkawi AS, Bakri B, Alsadek AS, Al-Hasan AH, Alrahhal MS, Alsaleh FM, Alsatouf FA, Arab MI, Jnaid H, Hadid AA. Child and adolescent health in Northwestern Syria: findings from healthy-Syria 2017 study. Avicenna J Med. 2019;9(02):61–74. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Meiqari L, Hoetjes M, Baxter L, Lenglet A. Impact of war on child health in Northern Syria: the experience of médecins Sans frontières. Eur J Pediatr. 2018;177(3):371–80. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.van Berlaer G, Elsafti AM, Al Safadi M, Souhil Saeed S, Buyl R, Debacker M, Redwan A, Hubloue I. Diagnoses, infections and injuries in Northern Syrian children during the civil war: A cross-sectional study. PLoS ONE. 2017;12(9):e0182770. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.de Lima Pereira A, Southgate R, Ahmed H, O’Connor P, Cramond V, Lenglet A. Infectious disease risk and vaccination in Northern Syria after 5 years of civil war: the MSF experience. PLoS Curr 2018;(10 ):1371. [DOI] [PMC free article] [PubMed]
- 21.Elsafti AM, van Berlaer G, Al Safadi M, Debacker M, Buyl R, Redwan A, Hubloue I. Children in the Syrian civil war: the Familial, educational, and public health impact of ongoing violence. Disaster Med Public Health Prep. 2016;10(6):874–82. [DOI] [PubMed] [Google Scholar]
- 22.Mbaeyi C, Moran T, Wadood Z, Ather F, Sykes E, Nikulin J, Al Safadi M, Stehling-Ariza T, Zomahoun L, Ismaili A, et al. Stopping a polio outbreak in the midst of war: lessons from Syria. Vaccine. 2021;39(28):3717–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Alhaffar BA, Alawabdi R, Barakat L, Kouchaji C. Oral health and socio-economic status among children during Syrian crisis: a cross-sectional study. BMC Oral Health. 2019;19(1):165. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Ballouk MA-H, Dashash M. Caries prevalence and dental health of 8–12 year-old children in Damascus City in Syria during the Syrian crisis; a cross-sectional epidemiological oral health survey. BMC Oral Health. 2019;19:1–6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Ballouk MA-H, Dashash M. The gingival health status of 8–12 year-old children in Damascus City in Syria during the Syrian crisis: a cross-sectional epidemiological oral health survey. BMC Res Notes. 2018;11(1):1–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Alhaffar MBA, Mustafa K, Sabbagh S, Yabrode K, Shebib G, Kouchaji C. Seven years of war in Syria: the relation between oral health and PTSD among children. Indian J Oral Health Res. 2018;4(1):10. [Google Scholar]
- 27.Hamid SH, Dashash MAD. The impact of post-traumatic stress disorder on dental and gingival status of children during Syrian crisis: A preliminary study. J Investig Clin Dent. 2019;10(1):e12372–12372. [DOI] [PubMed] [Google Scholar]
- 28.Habal W, Alkattan R, Hajeer MY, Alkhouli M, Al-Nerabieah Z, Habal T, Awawdeh M. Impact of Syrian conflict on the oral health of adolescents: A Cross-Sectional study. Cureus. 2024;16(2):e54613–54613. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Raslan N, Hamlet A, Kumari V. Mental health and psychosocial support in conflict: children’s protection concerns and intervention outcomes in Syria. Confl Health 2021, 15(1):19. [DOI] [PMC free article] [PubMed]
- 30.Alsharif A, Al Habbal O, Gabadian A, El Maamoun R, Al Faraj A, Kamr Aldin T, Haitham Aldammad O, Alkayakhi A, Al Habbal A. Behavioral difficulties and associated factors among the ‘lost generation’ of Syrian children and adolescents. Sci Rep. 2024;14(1):9286–9286. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Kalthom M, Nazeri A, Faramarzi S. The effectiveness of Self-Narrative Art therapy in reducing (PTSD) symptoms among War-Affected Syrian children. J Child Adolesc Trauma 2024;(1):209–16. [DOI] [PMC free article] [PubMed]
- 32.Kakaje A, Al Zohbi R, Alyousbashi A, Abdelwahed RNK, Aldeen OH, Alhalabi MM, Ghareeb A, Latifeh Y. Post-traumatic stress disorder (PTSD), anger and mental health of school students in Syria after nine years of conflict: a large-scale school-based study. Psychol Med. 2022;52(10):1923–33. [DOI] [PubMed] [Google Scholar]
- 33.Perkins JD, Alós J. Rapid mental health screening in conflict zones: a translation and cross-cultural adaptation into Arabic of the shortened revised child anxiety and depression scale (RCADS-25). Confl Health. 2021;15(1):1–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Perkins JD, Ajeeb M, Fadel L, Saleh G. Mental health in Syrian children with a focus on post-traumatic stress: a cross-sectional study from Syrian schools. Soc Psychiatry Psychiatr Epidemiol. 2018;53(11):1231–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Alchallah MO, Safiah MH, Kajjoun MMB, Al Ashabi KK, Ataya S, Mohsen F, Bakdounes D, ElHomsi MO, Alolabi H, Alistwani D. Prevalence of childhood obstructive sleep Apnoea syndrome and its role in daytime sleepiness in Syria: a large-scale school-based cross-sectional study. Ann Med Surg. 2023;85(6):2579. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Alhaffar MBA, Mustafa K, Alsabbagh S, Alhaffar O, Kakaje A. Oral Health Among Children With Haematological Malignancies In Syria. 2022.
- 37.Albaroudi IN, Khodder M, Al Saadi T, Turk T, Youssef LA. Prevalence, diagnosis, and management of iron deficiency and iron deficiency anemia among Syrian children in a major outpatient center in Damascus, Syria. Avicenna J Med. 2018;8(3):92–103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Al Habbal A, AlSharif A, Almubark A, Fattouh H, Hamzeh G, Kakaje A. Risk factors associated with epilepsy in children and adolescents: A case-control study from Syria. Epilepsy Behav. 2021;114(Pt A):107596. [DOI] [PubMed] [Google Scholar]
- 39.Mohammad Y, Rafea S, Latifeh Y, Haydar T, Jamal H, Alkhayer G, Dib G, Al-Massalmeh MS, Al-Lahham A, Fawaz Y, et al. Global asthma network phase I Syria asthma surveillance and the impact of the war. J Thorac Dis. 2023;15(5):2873–81. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Darwish B, Mahfouz MZ, Al-Nosairat S, Izzat MB. Changing pattern and outcome of pediatric chest injuries in urban Syria. Asian Cardiovasc Thorac Ann. 2018;26(5):367–70. [DOI] [PubMed] [Google Scholar]
- 41.Mohsen F, Bakkar B, Melhem S, Altom R, Sawaf B, Alkhija I, Nahas LD. Foreign body aspiration in a tertiary Syrian centre: A 7-year retrospective study. Heliyon. 2021;7(3):e06537. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Chowdhary P, Kalyanpur A, Mekuria FT, Altinci I. Elevating married adolescents’ voices for responsive reproductive healthcare in Syria. Front Reprod Health. 2022;4:780952. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Coutts A, Fouad FM, Abbara A, Sibai AM, Sahloul Z, Blanchet K. Responding to the Syrian health crisis: the need for data and research. Lancet Respiratory Med. 2015;3(3):e8–9. [DOI] [PubMed] [Google Scholar]
- 44.McIntyre J. Syrian civil war: a systematic review of trauma casualty epidemiology. BMJ Mil Health. 2020;166:261–5. [DOI] [PubMed] [Google Scholar]
- 45.Kahraman A, Özkan M, Durmus M. Child injuries in the Syrian civil war. Turkish J Plast Surg. 2019;27(3):123–6. [Google Scholar]
- 46.Çelikel A, Karbeyaz K, Kararslan B, Arslan MM, Zeren C. Childhood casualties during civil war: Syrian experience. J Forensic Leg Med. 2015;34:1–4. [DOI] [PubMed] [Google Scholar]
- 47.Er E, Çorbacıoğlu ŞK, Güler S, Aslan Ş, Seviner M, Aksel G, Bekgöz B. Analyses of demographical and injury characteristics of adult and pediatric patients injured in Syrian civil war. Am J Emerg Med. 2017;35(1):82–6. [DOI] [PubMed] [Google Scholar]
- 48.Çelikkaya ME, Atıcı A, Çigdem E, Akçora B. Innocent children in the Syrian civil war. Eur J Pediatr Surg. 2020;30(02):215–9. [DOI] [PubMed] [Google Scholar]
- 49.Kampalath V, Tarakji A, Hamze M, Loutfi R, Cohn K, Abbara A. The impacts of the Syrian conflict on child and adolescent health: a scoping review. J Public Health. 2023;45(3):621–30. [DOI] [PubMed] [Google Scholar]
- 50.Guha-Sapir D, Schluter B, Rodriguez-Llanes JM, Lillywhite L, Hicks MH-R. Patterns of civilian and child deaths due to war-related violence in Syria: a comparative analysis from the violation Documentation center dataset, 2011-16. Lancet Global Health. 2018;6(1):E103–10. [DOI] [PubMed] [Google Scholar]
- 51.Hanafi I, Munder E, Ahmad S, Arabhamo I, Alziab S, Badin N, Omarain A, Jawish MK, Saleh M, Nickl V, et al. War-related traumatic brain injuries during the Syrian armed conflict in Damascus 2014–2017: a cohort study and a literature review. BMC Emerg Med. 2023;23(1):35. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Arafat S, Alsabek MB, Ahmad M, Hamo I, Munder E. Penetrating abdominal injuries during the Syrian war: patterns and factors affecting mortality rates. Injury. 2017;48(5):1054–7. [DOI] [PubMed] [Google Scholar]
- 53.Torbey A, Shibani M, Alzabibi MA, Eddin AS, Mdawr E, Mouhanna W, Sawaf B, Alakhrass D, Asaad SA, Alhouri AN, et al. The epidemiology of in-hospital burn patients in a tertiary hospital in Damascus, Syria. A retrospective cohort study. Injury. 2023;54(2):435–41. [DOI] [PubMed] [Google Scholar]
- 54.Murray JS. Toxic stress and child refugees. J Spec Pediatr Nurs. 2018;23(1):e12200. [DOI] [PubMed] [Google Scholar]
- 55.Dangmann C, Dybdahl R, Solberg Ø. Mental health in refugee children. Curr Opin Psychol. 2022;48:101460. [DOI] [PubMed] [Google Scholar]
- 56.Kakaje A, Al Zohbi R, Hosam Aldeen O, Makki L, Alyousbashi A, Alhaffar MBA. Mental disorder and PTSD in Syria during wartime: a nationwide crisis. BMC Psychiatry. 2021;21(1):2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Hamza MK, Hicks MH-R. Implementation of mental health services in conflict and post-conflict zones: lessons from Syria. Avicenna J Med. 2021;11(1):8–14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Colucci E, Jaroudy S, Rossmann M. Piloting of a suicide first aid gatekeeper training (online) for children and young people in conflict affected areas in Syria. Int Rev Psychiatry. 2022;34(6):640–8. [DOI] [PubMed] [Google Scholar]
- 59.Latifeh Y, Hanafi I, Alhoulaiby S, Alandab F. Crisis-based psychiatry curriculum update: A cross-sectional study and an expert reflection from Syria. Asian J Psychiatr 2021;61:102681. [DOI] [PubMed]
- 60.Alsaied T, Mawas A, Al Sayah F, Kental A, Saqqur M. A new primary health-care system in the Syrian opposition territories: good effort but Far from being perfect. Avicenna J Med. 2017;7(4):189–92. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Rodo M, Singh L, Russell N, Singh NS. A mixed methods study to assess the impact of COVID-19 on maternal, newborn, child health and nutrition in fragile and conflict-affected settings. Confl Health. 2022;16(1):1–17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Abu-Ras W, Ashraf AbuLaban A, Talat AlQaisi S, AlQaisi MT, Decker E. Orphans in Syria and Iraq Juggling Balls: Wars, COVID-19, and the NGO’s financial crisis. Int J Qual Stud Health Well-being 2023, 18(1):2170010. [DOI] [PMC free article] [PubMed]
- 63.Basha L, Socarras A, Akhter MW, Hamze M, Albaik A, Hussein I, Tarakji A, Hamadeh M, Loutfi R, Kewara M. Impact of the Syrian conflict and forced displacement on respiratory health: an analysis of primary data from a humanitarian organisation. BMJ Open Respir Res. 2023;10(1):e001636. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Cetin BS, Orman A. Burkholderia cepacia complex infections in urgently referred neonates from Syrian border regions to a hospital in Turkey: A Cross-Border cluster. Child (Basel) 2022;9(10):1566. [DOI] [PMC free article] [PubMed]
- 65.Basha L, Hamze M, Socarras A, Akhtar M, Albaik A, Hussien I, Tarakji A, Hamadeh M, Loutfi R, Kewara M. Respiratory health and the Syrian conflict: a scoping literature review. Med Confl Surviv. 2024;40(2):111–52. [DOI] [PubMed] [Google Scholar]
- 66.Ismail SA, Abbara A, Collin SM, Orcutt M, Coutts AP, Maziak W, Sahloul Z, Dar O, Corrah T, Fouad FM. Communicable disease surveillance and control in the context of conflict and mass displacement in Syria. Int J Infect Dis. 2016;47:15–22. [DOI] [PubMed] [Google Scholar]
- 67.Mehtar S, AlMhawish N, Shobak K, Reingold A, Guha-Sapir D, Haar RJ. Measles in conflict-affected Northern Syria: results from an ongoing outbreak surveillance program. Confl Health. 2021;15:1–14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Eneh SC, Admad S, Nazir A, Onukansi FO, Oluwatobi A, Innocent DC, Ojo TO. Cholera outbreak in Syria amid humanitarian crisis: the epidemic threat, future health implications, and response strategy–a review. Front Public Health. 2023;11:1161936. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Sparrow A, Almilaji K, Tajaldin B, Teodoro N, Langton P. Cholera in the time of war: implications of weak surveillance in Syria for the who’s preparedness—a comparison of two monitoring systems. BMJ Global Health. 2016;1(3):e000029. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Alhaffar M, Mkhallalati H, Alrashid Alhiraki O, Marzouk M, Khanshour A, Douedari Y, Howard N. They cannot afford to feed their children and the advice is to stay home. How‥? A qualitative study of community experiences of COVID-19 response efforts across Syria. PLoS ONE. 2022;17(11):e0277215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Zemrani B, Gehri M, Masserey E, Knob C, Pellaton R. A hidden side of the COVID-19 pandemic in children: the double burden of undernutrition and overnutrition. Int J Equity Health. 2021;20(1):1–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Khalil D, Alyoussef R, Al Hosni H, Idriss S, Ahmad A, Al Rooh S, Ghanem KM. The psychosocial impact of the COVID-19 pandemic on families of children with Cancer in the Low-income setting. J Pediatr Hematol Oncol. 2023;45(7):e857–60. [DOI] [PubMed] [Google Scholar]
- 73.Minogue O, Yamin. Amjad: A Children’s Crisis: Update on Al Hol camp and COVID-19 concerns. In.; 2020.
- 74.Joury E. Syria profile of the epidemiology and management of early childhood caries before and during the time of crisis. Front Public Health. 2019;7:271. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Kazwini R, Kasem T, Alhuda NEA, Albarshah M, Subeh D, Alhaffar M. Oral health assessment in a sample of displaced people as a result of the war in Syria in Damascus City: results of non-profit initiative. BMC Oral Health. 2021;21(1):532. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Ghannam AN, Dashash M, Darjazini Nahhas L. Assessment of oral health status and quality of life in hearing-impaired children from Syria. BDJ Open. 2024;10(1):57. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Bsesa SS, Srour S, Dashash M. Oral health-related quality of life and oral manifestations of Syrian children with congenital heart disease: a case-control study. BMC Oral Health. 2023;23(1):316. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Misrabi G, Karkoutly M, Bshara N. The effect of secondhand smoke exposure on dental caries and gingival health among schoolchildren in Damascus, Syria: a cross-sectional study. BMC Oral Health. 2023;23(1):745. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Habal W, Alkattan R, Hajeer MY, Alkhouli M, Al-Nerabieah Z, Habal T, Awawdeh M. Impact of Syrian conflict on the oral health of adolescents: A Cross-Sectional study. Cureus. 2024;16(2):e54613. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Joury E, Khairallah M, Sabbah W, Elias K, Bedi R. Inequalities in the frequency of free sugars intake among Syrian 1-year-old infants: a cross-sectional study. BMC Oral Health. 2016;16:1–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Akik C, Semaan A, Shaker-Berbari L, Jamaluddine Z, Saad GE, Lopes K, Constantin J, Ekzayez A, Singh NS, Blanchet K et al. Responding to health needs of women, children and adolescents within Syria during conflict: intervention coverage, challenges and adaptations. Confl HEALTH 2020;14:37. [DOI] [PMC free article] [PubMed]
- 82.Bozo M, Khudari H, Mohammad M. Scale-up of malnutrition screening by the world health organization in Syria. Field Exch. 2019;61:57. [Google Scholar]
- 83.Khaliq A, Wraith D, Nambiar S, Miller Y. A review of the prevalence, trends, and determinants of coexisting forms of malnutrition in neonates, infants, and children. BMC Public Health. 2022;22(1):879. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Zamlout A, Alwannous K, Kahila A, Yaseen M, Albadish R, Aleid M, Hamzah K, Monther M, Akkari O, Hasan A, et al. Syrian National growth references for children and adolescents aged 2–20 years. BMC Pediatr. 2022;22(1):282. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Hawari I, Eskandar MB, Alzeer S. The role of lead, manganese, and zinc in autism spectrum disorders (ASDS) and attention-deficient hyperactivity disorder (ADHD): a case-control study on Syrian children affected by the Syrian crisis. Biol Trace Elem Res. 2020;197(1):107–14. [DOI] [PubMed] [Google Scholar]
- 86.Mohammad Y, Rafea S, Latifeh Y, Khaddam A, Sawaf B, Zakaria MI, Al Masalmeh MS, Fawaz Y, Allaham A, Almani I, et al. Erratum to uncontrolled and under-diagnosed asthma in a Damascus shelter during the Syrian crisis. J Thorac Dis. 2018;10(5):E409. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Kakaje A, Alhalabi MM, Alyousbashi A, Hamid A, Hosam Aldeen O. Allergic Rhinitis and Its Epidemiological Distribution in Syria: A High Prevalence and Additional Risks in War Time. BioMed Res Int 2020, 2020. [DOI] [PMC free article] [PubMed]
- 88.Akbarzada S, Mackey TK. The Syrian public health and humanitarian crisis: a ‘displacement’in global governance? Glob Public Health. 2018;13(7):914–30. [DOI] [PubMed] [Google Scholar]
- 89.DeJong J, Ghattas H, Bashour H, Mourtada R, Akik C, Reese-Masterson A. Reproductive, maternal, neonatal and child health in conflict: a case study on Syria using countdown indicators. BMJ Global Health. 2017;2(3):e000302. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Committee IR. Syria Multi-Sector Needs Assessment - March 2024. In.; 2024.
- 91.Sen K. Starvation of children in Syria–sanctions and the politics of revenge. Indian J Med Ethics. 2014;11(1):63. [DOI] [PubMed] [Google Scholar]
- 92.Al-Mandhari A. Earthquakes as triggers for public health disasters: WHO and health systems’ response. East Mediterr Health J. 2023;29(3):165–7. [DOI] [PubMed] [Google Scholar]
- 93.Patwary MM, Ashraf S, Swed S, Shoib S. The impact of the devastating Turkey-Syria earthquake on the fragile health care system in war-torn Syria. Prehosp Disaster Med. 2023;38(4):537–8. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
Data is provided within the manuscript or supplementary information files.