Abstract
Marcus Gunn Jaw Winking Synkinesis (MGJWS) is a rare congenital condition characterized by unilateral ptosis that improves with ipsilateral jaw movement. It frequently presents alongside other ocular abnormalities, including strabismus and anisometropia, which significantly increase the risk of amblyopia. Monocular elevation deficiency (MED), a type of strabismus marked by impaired elevation of the eye in all gaze positions, is most commonly associated with MGJWS. We report the case of a 14-year-old male with a history of refractive amblyopia who presented with both MGJWS and MED. This case supports emerging evidence that MGJWS and MED may represent phenotypic variations of the same neurodevelopmental disorder, with the severity of ptosis possibly potentiating the co-occurrence of MED. It also underscores the importance of early and comprehensive ophthalmologic evaluation in patients with MGJWS for the detection of coexisting ocular abnormalities that increase the risk of amblyopia.
Keywords: amblyopia, double levator palsy, marcus-gunn jaw winking synkinesis, monocular elevation deficiency, strabismus
Introduction
First described by Scottish ophthalmologist Robert Marcus Gunn in 1883, Marcus Gunn Jaw Winking Synkinesis (MGJWS) is a rare congenital condition characterized by unilateral ptosis that improves with stimulation of the ipsilateral pterygoid muscles. It occurs in 2% to 13% of patients with congenital ptosis and presents as elevation of the ptotic eyelid during movements such as chewing or mouth opening [1]. The mechanism behind MGJWS results from misrouted signals from the trigeminal nerve, whereby motor impulses intended for the external pterygoid muscle are misrouted to the levator palpebrae superioris muscle, leading to involuntary eyelid elevation during jaw movement [2]. Although MGJWS may present as an isolated finding, it more often presents alongside other ocular abnormalities like strabismus or anisometropia, many of which are associated with an increased risk for the development of amblyopia [3].
The risk of the development of unilateral amblyopia, defined as decreased visual acuity in one eye caused by abnormal binocular interactions during the early stages of visual development, is compounded by the presence of strabismus or other refractive errors. In one study, strabismus was associated with a 2.7 to 18 times greater odds of amblyopia development when present [4,5]. One type of strabismus, monocular elevation deficiency (MED), is characterized by the inability to elevate one eye in abduction, adduction, and primary gaze [6,7]. The pattern of gaze limitations seen in isolated MED is theorized to occur through either thickening of the inferior rectus muscle or through disruptions to the unilateral center for upgaze, with the oculomotor nerve being functionally intact for most patients [6]. Though the underlying pathophysiology is not fully understood, MED frequently co-occurs with MGJWS and represents the most common type of strabismus observed, with studies reporting a prevalence of 25% to 48% among patients with the condition [3,8].
Given the extensive overlap between MGJWS, MED, and other ocular abnormalities that increase the risk of amblyopia development, the presentation of MGJWS in a patient should prompt further investigation into other possible irregularities for amblyopia risk stratification. Thus, to further shed light on the association between MGJWS and accompanying ocular abnormalities, we present the case of a 14-year-old male with a history of refractive amblyopia who presented to the ophthalmology clinic with MGJWS and MED.
Case presentation
A 14-year-old male with a history of refractive amblyopia was referred to the ophthalmology clinic for evaluation of left upper eyelid ptosis, which has been present since birth. Slit-lamp examination revealed a palpebral fissure height of 8 mm in the right eye and 3 mm in the left, with marginal reflex distance (MRD) measurements of +3 mm in the right eye and -2 mm in the left. Notably, the patient’s ptosis improved significantly when he opened his mouth, as illustrated in Figure 1. Upward gaze in the left eye was also restricted in all gaze positions, as shown in Figure 2. No evidence of esotropia or epiblepharon was observed on examination. Given the patient’s restricted upward gaze and ptosis that improved with jaw movement, these findings were suggestive of MGJWS with accompanying MED.
Figure 1. Preoperative evaluation of MGJWS.
Image A was taken at rest. Image B was taken during active jaw movement.
MGJWS: Marcus-Gunn jaw winking synkinesis
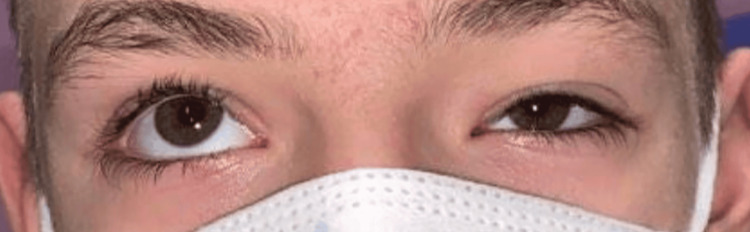
Figure 2. Preoperative evaluation of MED in primary gaze.
MED: Monocular elevation deficiency
Due to a good levator function of 12 to 13 mm in the left eye and a negative Hering’s law response, the patient initially underwent levator advancement surgery. At the one-week postoperative visit, the MRD improved to +2 mm. However, due to persistent ptosis, a frontalis sling procedure was subsequently performed. One week following the second surgery, the patient exhibited minimal evidence of MGJWS, which was only apparent with effort. Residual ptosis persisted, with an MRD of 0 mm at rest and +2 mm during brow activation, though the accuracy of the examination was limited by expected postoperative edema. Unfortunately, further assessments could not be performed, as the patient was lost to follow-up.
Discussion
Although the association between MGJWS and MED is well-documented, the underlying mechanism connecting them remains unclear. Shahabinia et al. suggest that this relationship may be explained within the broader framework of congenital cranial dysinnervation disorders (CCDDs), a spectrum of congenital, non-progressive conditions with a common underlying etiology [9]. According to their hypothesis, a developmental failure in the proper innervation of the levator palpebrae superioris and the superior rectus muscle, both normally innervated by the superior branch of the oculomotor nerve, results in congenital ptosis and MED, respectively. Concurrently, this disruption may also lead to MGJWS by inducing aberrant synaptic connections between the oculomotor and trigeminal nuclei due to their anatomical proximity during early neurodevelopment. This mechanism elegantly explains the simultaneous manifestation of MGJWS and MED, reinforcing the hypothesis that they represent varying manifestations of a single neurodevelopmental disorder.
Furthermore, a pattern emerging from recent case reports suggests that the severity of ptosis may predict the presence of MED in patients with MGJWS. Shah et al. described an 18-year-old male with bilateral MGJWS, in whom the eye with more pronounced ptosis also exhibited MED [10]. Another report by Shahabinia et al. described a 13-year-old girl with severe congenital ptosis who had both MGJWS and MED, whereas her aunt, who had milder ptosis, exhibited MGJWS without MED [9]. Our case aligns with this trend because the patient’s severely ptotic eye, evident by MRD -2, was affected by both MGJWS and MED. This observed correlation strengthens the hypothesis that MGJWS and MED may not be distinct conditions but rather varying phenotypic expressions of a single neurodevelopmental disorder. The dual manifestation likely reflects the degree of dysinnervation, whereby more severe disruptions of oculomotor nerve development increase the chance of forming aberrant oculomotor-trigeminal synapses, leading to the dual presentation of MGJWS and MED.
This report aims to highlight the frequent association between MGJWS and co-existing conditions such as strabismus, particularly MED, and anisometropia, both of which are strongly linked to the development of amblyopia [3]. In fact, the incidence of amblyopia has been reported in 35% to 59% of patients with MGJWS, underscoring the need for early detection and management [8,11]. Given this strong association, clinicians should maintain a high index of suspicion for these abnormalities when evaluating patients with MGJWS to prevent amblyopia and its long-term consequences. Effective management requires a comprehensive ophthalmologic assessment with careful consideration of the severity of ptosis and the extent of jaw-winking [9]. Patients should also be counseled on the potential need for multiple surgeries to achieve satisfactory cosmetic outcomes, as demonstrated in this case.
In addition, this report explores the current literature on the possible pathophysiological link between MGJWS and MED. Although data remain limited, emerging evidence suggests that both conditions may represent varying phenotypic expressions of the same neurodevelopmental disorder belonging to a group of conditions referred to as CCDDs [9,12]. Further studies are needed to verify these hypotheses with the goal of improving our understanding of these conditions and optimizing treatment strategies to minimize the cosmetic, visual, and surgical burden on affected patients.
Conclusions
This report reinforces the well-documented association between MGJWS and MED. It also supports the hypothesis that these conditions likely represent different manifestations of the same neurodevelopmental disorder. Early and comprehensive ophthalmologic evaluation is critical in patients with MGJWS to detect and address coexisting conditions, such as strabismus and anisometropia, before the onset of amblyopia. Further research is needed to elucidate the underlying pathophysiological mechanisms linking MGJWS and MED to enhance our understanding of these conditions and develop optimized management strategies that improve patient outcomes.
Disclosures
Human subjects: Informed consent for treatment and open access publication was obtained or waived by all participants in this study.
Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following:
Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work.
Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work.
Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Author Contributions
Concept and design: Omar Moussa Pasha, Gabriela Espinoza, Rocio Bentivegna
Acquisition, analysis, or interpretation of data: Omar Moussa Pasha, Gabriela Espinoza, Rocio Bentivegna
Drafting of the manuscript: Omar Moussa Pasha, Gabriela Espinoza, Rocio Bentivegna
Critical review of the manuscript for important intellectual content: Omar Moussa Pasha, Gabriela Espinoza, Rocio Bentivegna
Supervision: Gabriela Espinoza, Rocio Bentivegna
References
- 1.Marcus Gunn jaw-winking synkinesis: clinical features and management. Demirci H, Frueh BR, Nelson CC. Ophthalmology. 2010;117:1447–1452. doi: 10.1016/j.ophtha.2009.11.014. [DOI] [PubMed] [Google Scholar]
- 2.Paradoxical synkinetic levator inhibition and excitation. An electromyographic study of unilateral oculopalpebral and bilateral mandibulopalpebral (Marcus Gunn) synkineses in a 74-year-old man. Hepler RS, Hoyt WF, Loeffler JD. Arch Neurol. 1968;18:416–424. doi: 10.1001/archneur.1968.00470340102009. [DOI] [PubMed] [Google Scholar]
- 3.Clinical features associated with the jaw winking syndrome. Digout LG, Awad AH. Am Orthopt J. 2001;51:125–131. doi: 10.3368/aoj.51.1.125. [DOI] [PubMed] [Google Scholar]
- 4.Amblyopia preferred practice pattern. Cruz OA, Repka MX, Hercinovic A, et al. Ophthalmology. 2023;130:0. doi: 10.1016/j.ophtha.2022.11.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Amblyopia: types, diagnosis, treatment, and new perspectives. Zagui RMB. https://www.aao.org/education/disease-review/amblyopia-types-diagnosis-treatment-new-perspectiv Am Acad Ophthalmol. 2019 [Google Scholar]
- 6.Congenital monocular elevation deficiency. Kim JH, Hwang JM. Ophthalmology. 2009;116:580–584. doi: 10.1016/j.ophtha.2008.10.023. [DOI] [PubMed] [Google Scholar]
- 7.The progress of clinical research and treatment of monocular elevation deficiency. Tang K, Lu XZ, Bi HS. https://pubmed.ncbi.nlm.nih.gov/37670662/ Zhonghua Yan Ke Za Zhi. 2023;59:764–769. doi: 10.3760/cma.j.cn112142-20221102-00558. [DOI] [PubMed] [Google Scholar]
- 8.The Marcus Gunn phenomenon. A review of 71 cases. Pratt SG, Beyer CK, Johnson CC. Ophthalmology. 1984;91:27–30. doi: 10.1016/s0161-6420(84)34331-7. [DOI] [PubMed] [Google Scholar]
- 9.The possibility of Marcus Gunn jaw-winking and monocular elevation deficiency being the same disease. Shahabinia S, Jafari R, Maskopaii SR. J Pediatr Rev. 2020;8:23–28. [Google Scholar]
- 10.Bilateral Marcus Gunn jaw winking synkinesis with monocular elevation deficiency: a case report and literature review. Shah AD, Kumar AB, Kothari K. Int Ophthalmol. 2012;32:199–201. doi: 10.1007/s10792-012-9538-0. [DOI] [PubMed] [Google Scholar]
- 11.The quantification, natural course, and surgical results in 57 eyes with Marcus Gunn (jaw-winking) syndrome. Doucet TW, Crawford JS. Am J Ophthalmol. 1981;92:702–707. doi: 10.1016/s0002-9394(14)74665-3. [DOI] [PubMed] [Google Scholar]
- 12.Ptosis associated with monocular elevation deficiency. Zafar SN, Khan A, Azad N, Ali M, Naseer S, Iqbal S. https://pubmed.ncbi.nlm.nih.gov/19757696/ J Pak Med Assoc. 2009;59:522–524. [PubMed] [Google Scholar]