Pigmented purpuric dermatoses (PPDs) are clinical conditions presenting as red-brown maculopapular eruptions due to the extravasation of red blood cells (RBCs) with subsequent deposition of hemosiderin in the skin. PPD usually affects the adult population, but rarely, it may be seen in the pediatric age group as well.[1] Here, we report a case of Schamberg disease (one of the commonest PPDs) in a 16-year-old child since the age of 10 years.
A 16-year-old female child presented to our outpatient department (OPD) with a history of recurrent reddish-brown rashes over both legs for the last six years. The individual episodes were acute in onset and progressed to involve the legs bilaterally up to the knees within a few days. The rash was preceded by prolonged standing and exertion and was associated with mild pruritus, myalgia, and heaviness in the legs. Initially, it was less frequent, but with time the frequency of the rash increased to 1 to 2 episodes every month. There were no complaints of joint pain, abdominal pain, recurrent oral ulcers, photosensitivity or any clinical feature suggestive of a connective tissue disorder. There was no history of any oral or topical medication preceding the eruption.
On examination, multiple reddish-brown discrete to confluent, non-palpable and non-blanchable macular rashes were present over bilateral legs [Figure 1]. The oral, genital, and ocular mucosae and hair and nails examination revealed no abnormality. Based on the clinical presentation, differential diagnoses of leukocytoclastic vasculitis and childhood PPD (Schamberg disease) were considered. Routine workups, including blood counts (CBCs), liver and kidney function tests (LFTs and KFTs), viral serologies (HBsAg, HCV, HIV-1 and 2), ANA and coagulation profiles were within normal limits. The venous Doppler study of both legs was normal. A skin biopsy for pathological examination revealed perivascular and peri-adnexal infiltrations of lymphocytes, plasma cells with extravasation of erythrocytes, and hemosiderin deposition in the dermis and subcutaneous layer [Figure 2a and b]. Perl’s Prussian blue (PPB) stain revealed deposition of hemosiderin [Figure 3]. Direct immunofluorescence (DIF) study for immunoglobulin G (IgG), IgA, IgM and C3 was negative.
Figure 1.

Multiple reddish-brown discrete to confluent, non-palpable and non-blanch-able macular rashes present over both legs
Figure 2.

Mild spongiosis of epidermis with perivascular and peri adnexal lymphocytic infiltration and hemosiderin deposition in dermis [H and E × 10] (a); Extravasation of RBCs at few places (blue oval), hemosiderin deposition in the dermis (red arrow) [H and E × 40] (b)
Figure 3.

Perl’s Prussian blue (PPB) stain showing deposition of hemosiderin [×40]
Therefore, based on clinicopathologic features, a final diagnosis of pediatric Schamberg disease (childhood PPD) was made. The patient was started on tab. Vitamin C 500 mg once daily orally with oral antihistamine and mild topical corticosteroid (Fluticasone). At the two-months follow-up, there was no further episode with symptomatic improvement in pruritus. Antihistamine and topical corticosteroid cream were stopped, and the patient maintained on vitamin C 500 mg daily. The patient is on follow-up with no further episodes.
Pigmented purpuric dermatoses (PPDs) clinically manifest as erythematous to purplish-brown macules, patches and petechiae due to the extravasation of RBCs with hemosiderin deposition in the skin. This condition usually affects the adult population. As seen in our index case, the presentation of a PPD in the pediatric age group is very uncommon. Schamberg disease and lichen aureus were earlier described as subtypes in the pediatric age group.[1] In literature, Schamberg disease is the only subtype significantly associated with generalised presentations.[2] The probable pathomechanism of PPDs is thought to be due to capillary fragility, endothelial dysfunction, altered cell-mediated immunity (CMI) and extracellular matrix abnormalities. Certain extrinsic factors, such as medications, infections, contact allergens, etc., and intrinsic factors, including increased chronic veinous insufficiency, veinous hypertension, and autoimmune diseases, also influence the occurrence of PPDs [Figure 4].[1,3] Childhood PPDs should be distinguished from other causes of pigmented purpura, Other D/Ds of pediatric Schamberg’s disease are lichen aureus, leukocytoclastic vasculitis, pigmented purpuric dermatosis of Gougerot and Blum, eczematoid such as purpura of Doucas and Kapetanakis, purpura annularis telangiectodes of Majocchi, and scurvy (discussed in Table 1).[3,4] Several cases of recurrent PPDs have been reported preceding cutaneous T cell lymphoma (CTCL). It suggests that PPDs could be a potential warning sign of CTCL.[5,6] Therefore, pathologic examination and DIF are essential to confirm the diagnosis and rule out the other etiologies of purpuric lesions.
Figure 4.
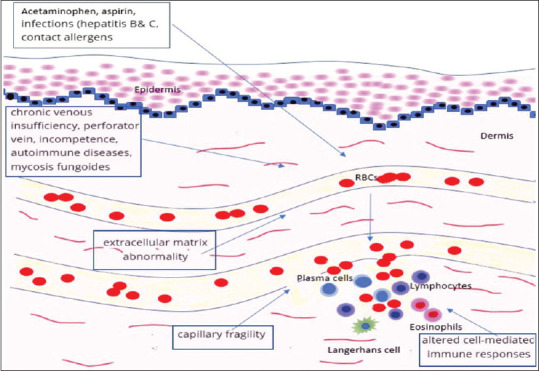
The pathomechanism of pigmented purpuric dermatoses
Table 1.
Differential diagnosis of pediatric Schamberg’s disease
| DDs | Differentiating feature |
|---|---|
| Lichen aureus | Clinically distinctive golden colour |
| Leukocytoclastic vasculitis | Palpable nature of the lesions |
| Pigmented purpuric dermatosis of Gougerot and Blum | Red-brown lichenoid papules that tend to fuse and form plaques |
| Eczematoid purpura of Doucas and Kapetanakis | Intensely itchy, with characteristic eczematous features; Mild lichenification present |
| Purpura annularis telangiectodes (Majocci disease) | Annular, purpuric lesions with central clearing and slight atrophy |
| Scurvy | Purpuric lesions with other features (perifollicular purpura, coiled hairs, bleeding gums, and dietary history of reduced vitamin C intake) |
To conclude, we hereby describe a rare case of pediatric Schamberg disease with an emphasis on excluding other systemic causes of purpuric lesions in children.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Conflicts of interest
There are no conflicts of interest.
Funding Statement
Nil.
References
- 1.Spigariolo CB, Giacalone S, Nazzaro G. Pigmented purpuric dermatoses: A complete narrative review. J Clin Med. 2021;10:2283. doi: 10.3390/jcm10112283. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Ollech A, Paller AS, Kruse L, Kenner-Bell B, Chamlin S, Wagner A, et al. Pigmented purpuric dermatosis in children: A retrospective cohort with emphasis on treatment and outcomes. J Eur Acad Dermatol Venereol. 2020;34:2402–8. doi: 10.1111/jdv.16397. [DOI] [PubMed] [Google Scholar]
- 3.Park J-H, Kang HY. Generalized schamberg disease in a child. Ann Dermatol. 2013;25:524–5. doi: 10.5021/ad.2013.25.4.524. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Zaldivar Fujigaki JL, Anjum F. StatPearls. Treasure Island (FL): StatPearls Publishing; 2024. Schamberg disease. [PubMed] [Google Scholar]
- 5.Nasimi M, Bonabiyan M, Lajevardi V, Azizpour A, Nejat A, Dasdar S, et al. Pigmented purpuric dermatoses versus purpuric mycosis fungoides: Clinicopathologic similarities and new insights into dermoscopic features. Australas J Dermatol. 2022;63:81–5. doi: 10.1111/ajd.13759. [DOI] [PubMed] [Google Scholar]
- 6.Çaytemel C, Baykut B, Ağırgöl Ş, Caf N, Demir FT, Türkoğlu Z, et al. Pigmented purpuric dermatosis: Ten years of experience in a tertiary hospital and awareness of mycosis fungoides in differential diagnosis. J Cutan Pathol. 2021;48:611–6. doi: 10.1111/cup.13949. [DOI] [PubMed] [Google Scholar]


