Abstract
Complications can arise from the application, wear, and removal of casts and splints. This text reviews common complications, risk factors, and prevention strategies while exploring the medical-legal implications of these complications. Being aware of common pitfalls can help reduce risk and promote optimal patient outcomes.
Key Concepts
-
(1)
Proper and judicious casting and splinting techniques are critical to prevent complications.
-
(2)
Thermal injuries can occur due to excessive curing heat and cast saw burns.
-
(3)
Poor cast molding can lead to skin sores and loss of fracture reduction.
-
(4)
Patients should be comfortable in their cast, and uncontrolled pain warrants investigation.
Keywords: Cast complications, Thermal injury, Pressure sore, Cast saw burn, Loss of reduction, Compartment syndrome
Introduction
Closed treatment with splints and/or casts for immobilization is the standard of care for many pediatric orthopaedic fractures. Casting and splinting are also often used for post-operative immobilization to protect surgical repairs. Given their frequent use, understanding the pitfalls of application and practice is critical to preventing complications that can lead to poor patient outcomes and medicolegal concerns.
High risk patients
While any patient can develop complications from casts or splints, specific subsets of the pediatric population are deemed higher risk due to their inability to effectively communicate, impaired sensation, or lack of pain perception. Very young children, those with developmental or speech delays, and those who are obtunded from head trauma or impaired from multi-limb trauma are at a high risk for missed or delayed complications. Additionally, patients with conditions that may impair sensation, such as peripheral neuropathy, spina bifida, spinal cord injury, and regional nerve blocks, are also considered high risk. In high-risk patient populations, careful monitoring, heightened suspicion, caregiver education, and preventative measures—such as additional cast padding or cast bivalving to accommodate swelling—should be considered (see Fig. 1).
Figure 1.
Severe dermatitis in an infant treated with a spica cast. Increased fussiness in a young child should be further evaluated with cast removal to evaluate for underlying skin complications. Image courtesy of Matthew Halanski, MD.
Common complications
Thermal injuries
The curing of plaster splints and casts produces an exothermic reaction, which generates variable amounts of heat. If excessive heat is retained near the skin, burns can result [1]. Temperatures >49 °C (120 °F) for 2–3 min can result in first-degree burns, and more prolonged exposures can result in second and third-degree burns (>8 min and >12 min, respectively) [2]. There are several risk factors associated with thermal injury. Water dip temperature >24 °C and plaster splint thickness >24 ply (such as edges where plaster is folded back) can increase the heat generated [3]. Placing a curing cast or splint on a pillow can limit heat dissipation and increase the risk of thermal injury [3]. These risk factors, when combined, can significantly compound the risk of complications. As one casting model demonstrated, the use of extra-fast setting plaster, applied with 20 layers and placed on a pillow during curing, resulted in a maintained temperature of over 50 °C (122 °F) for more than 20 min [4]. Additionally, pressure application, such as three-point molding for fracture reduction, can also increase localized temperatures, especially in cases where plaster is overwrapped with fiberglass [5].
Master's Method.
Dr. Matthew Halanski: Thermal injuries are rare, but folding over the ends of a plaster splint, rather than trimming the excess, or using extremely hot dip water (often done in the trauma setting when attempting to hurry) should be avoided. In these scenarios, the limb may be placed on pillows as other injuries are assessed, and commonly the patient may be sedated or have an altered mental status. All of these factors may create the perfect storm for a thermal injury (see Fig. 2).
Figure 2.
Volar (A) and dorsal (B) hand burns secondary to thermal injury from splint immobilization of a buckle fracture. Images courtesy of Jud Karlen, MD.
To minimize the risk of thermal injury, it is recommended that lukewarm water be used for dipping, casts be applied with thinner layers and trimmed at the edges to prevent back folding of materials, and adequate air circulation should be allowed. If patients become uncomfortable during the curing process and express concern for heat, removal of the cast and evaluating the skin is imperative.
Master's Method.
Dr. Matthew Halanski: Attempting to thicken a cast over the convexity of the heel or the elbow may also place excessive casting material in the concavity (anterior ankle/antecubital fossa). Embedding a posterior splint into the cast can place the material where it is needed, with less accumulation in the concavities.
Cast saw burns
Cast saw injuries can be a frequent casting complication, estimated to occur 1.3 to 7.2 times per 1000 casts [1]. Oscillating saw blades cause friction, which secondarily leads to abrasions and thermal burns. Many risk factors have been identified as predisposing to cast saw burns, including operator inexperience, patient sedation, poor cast saw blade condition, cutting over bony prominences or concavities, and prolonged blade contact near the skin [6,7]. Cutting a cast prior to curing of the cast material can also increase the risk for injury, with a previous study noting that allowing a plaster cast to set >12 min results in significantly fewer blade-to-skin touches [8] (see Fig. 3).
Master's Method.
Dr. Matthew Halanski: Two of the biggest studies looking at cast saw injuries (Ansari 1998 and Shore 2014) found that patients in the ED (especially at night) were most at risk for cast saw injuries.
Figure 3.
Example of a dull cast saw blade (left) and new cast saw blade (right). Note the stuck-on cast material and dull teeth, which contribute to poor blade condition and increase the risk of thermal injury. Image courtesy of Jessica McGraw-Heinrich, MD.
Preventative measures can be taken to reduce the risk of cast saw injury. Proper training of cast saw operators on casting models can familiarize users with safe use practices such as frequent checking of blade temperature, allowing time for cooling as needed, and use of an in-and-out technique to perforate the cast [1]. Use of a vacuum can reduce cast blade temperatures [9]. Frequent blade replacement, with some advocating changing blades a minimum of every 60 casts or 30 bivalves, can also reduce the risk of heat generation from use of a dull saw blade [9]. Additionally, the use of safety strips and cast cutting guides can reduce blade-to-skin contact, which in turn decreases patient anxiety and skin complications [10,11] (see Fig. 4).
Master's Method.
Dr. Matthew Halanski: Cast saw lacerations and burns can be minimized by limiting the blade to skin contact. The use of aids and proper technique, perforating (without excessive force) rather than sawing or dragging, can reduce the incidence of injury. The cast spreader can effectively “pop” any intervening material without risk of injury.
Figure 4.
A dorsal forearm cast-saw laceration secondary to cast bivalving. Image courtesy of Jessica McGraw-Heinrich, MD.
Cast/splint sores
Cast and splint sores are pressure-related injuries which can occur due to abnormal contact between the cast or splint and the patient's skin. These can arise from improper padding, wrinkling, or bunching of padding during application, excessive movement within the cast resulting in a change in positioning during wear, change in angle of joint immobilization while still curing, or wet or soiled casts resulting in skin breakdown [12,13]. Prevention of cast sores is imperative, and proper padding techniques and cast fit are essential (see Fig. 5).
Master's Method.
Dr. Matthew Halanski: The best prevention against cast sores is a well-fitting cast or splint. Migration of the limb in the cast due to decreased swelling, atrophy, and padding compression may all contribute to pressure injuries over time.
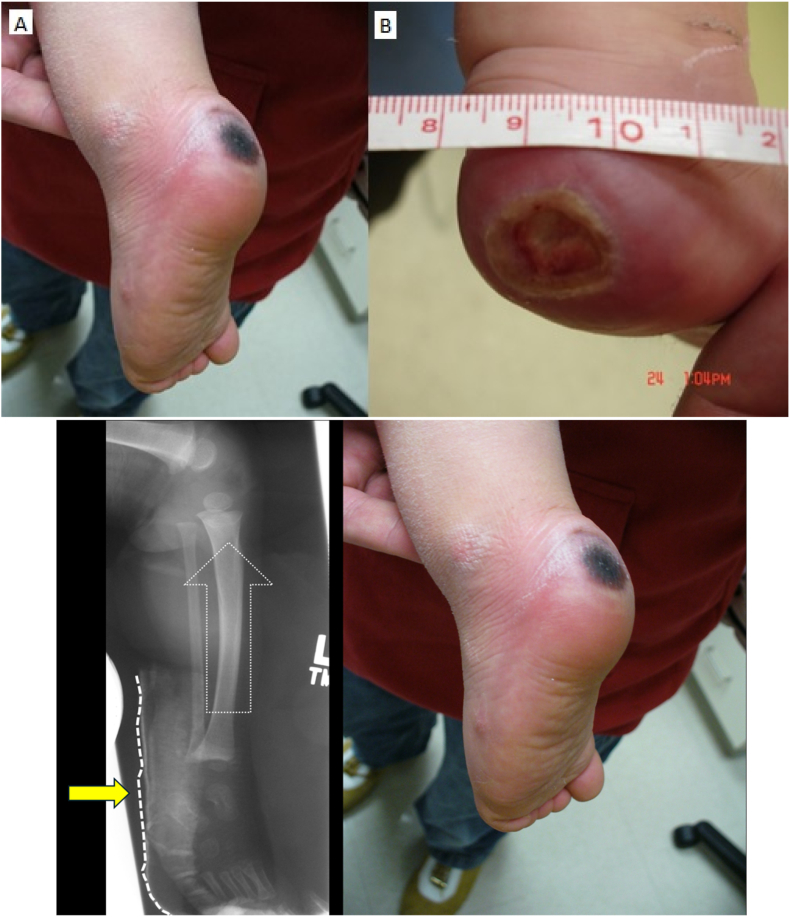
Figure 5.
Heel pressure sores in two different infants. Image A shows an unstageable pressure sore with eschar in place. Image B shows full-thickness skin loss with exposure of the underlying calcaneus. The first sore resulted from a poorly fitting splint that slipped down, leading to pressure on the heel. Images courtesy of Matthew Halanski, MD.
When rolling cast padding on the extremity, there should be 50% overlap at a minimum so that there are at least two layers of the cast padding between the skin and the cast, and bony prominences should have more than two layers. The use of long-arm and long-leg casts with the elbow and knee flexed to 90° in very young children (<2 years) will present slippage, and frequently changing the casts of high-risk patients can minimize cast slippage and resultant sores [13,14].
Master's Method.
Dr. Scott Mubarak: Sugar tong splints around the malleoli to the knee or from elbow to wrist are less likely to slide down or break posteriorly. These can be used in the acute setting to minimize slippage and resultant sores.
Use of foam padding can also be considered, as this may reduce the incidence of skin complications in high-risk patients [15]. When casting and splinting, the position of the extremity and spanned joints should be maintained during the completion of the curing process to prevent wrinkling, which can result in pressure sores. When pressure sores occur, offloading the affected areas and close monitoring via cast windows is necessary (see Fig. 6).
Master's Method.
Dr. Scott Mubarak: Late dorsiflexion of the ankle as the cast is setting up can lead to creasing of the soft roll or cast material at the anterior skin, which can cause a pressure sore. A similar problem can occur at the antecubital fossa with late elbow flexion when applying a long arm cast. No movement and good assistants are needed.
Figure 6.
Example of a posterior slab lower extremity splint that had loss of ankle dorsiflexion due to positioning not being maintained as the splint cured. This resulted in immobilization in equinus and wrinkling of splint material. Splint also had poor padding and the ends of splint were folded back, risking thermal injury. Image courtesy of Scott Rosenfeld, MD.
Cast sores can also occur from failure to remove objects such as jewelry from the extremity prior to immobilization, or from patients and/or family placing objects into the cast, which can create skin sores or skin breakdown. Families should be counseled on the importance of not placing anything into the cast. If there are any concerns for an object becoming stuck under the cast, the patient should be evaluated and the cast changed (see Figure 7, Figure 8).
Master's Method.
Dr. Matthew Halanski: In high-risk patients, especially those who are non-verbal or young, more frequent cast changes may minimize pressure sore injuries.
Figure 7.
Deep skin sore caused by placement of a cast over an elastic hairband left in place at the patient's ankle (A; image courtesy of Scott Rosenfeld, MD). Superficial skin sore caused by a bracelet that was not removed prior to immobilization (B; image courtesy of Matthew Halanski, MD).
Figure 8.
Examples of skin sores created by foreign bodies placed into casts. A and B are secondary to coins placed in arm casts. C is a severe pressure sore secondary to the placement of a Lincoln Log toy into the cast. Image D is secondary to a plastic toy placed into a leg cast. Images courtesy of Scott Rosenfeld, MD (A and C) and Matthew Halanski, MD (B and D).
Compartment syndrome/ischemia
Increased intra-compartmental pressures can lead to ischemia and muscle necrosis if not released in a timely fashion. In acute fractures and the early postoperative setting, swelling can be common, and restrictive or tight circumferential dressings, such as casts, can place an extremity at risk for compartment syndrome [12].
Casting technique can affect the fit of the cast and the tightness of the cast. Casts applied in which fiberglass is tightly wrapped without a stretch-relax technique of unrolled and gently wrapped, can result in a significantly tighter cast [12,16]. Techniques to split the cast, such as univalving or bivalving, can reduce compartment pressures beneath the cast. In one model, univalving plaster casts reduced pressures by 40–60%, and releasing the underlying cast padding reduced pressures an additional 10–20%. [12,16]. In another study, univalving fiberglass casts were noted to reduce cast pressures by 60%, and a 75% reduction in cast pressures was observed with cast bivalving. (Shaw) [17] Additionally, the use of a 10 mm cast spacer in a univalved cast was shown to reduce cast pressures similar to those of elastic wrapped bivalve casts [17]. In a biomechanical cast model study, univalving and bivalving were noted to decrease the bending stiffness and load to failure of fiberglass casts, with univalved casts having a higher load to failure than bivalve casts [18]. While cast valving can decrease pressures under the cast, it can also impact the pressure at three-point molding sites for fracture reduction. For standard molding of a dorsally displaced distal radius fracture, univalving a cast dorsally or volarly results in less pressure loss at the three point mold sites than radial or ulnar valving (Montgomery) [19] These techniques should be considered as preventative measures in high risk patients and patients with acute injuries or surgeries which might have associated swelling. Clinicians should be aware of the effects of cast valving techniques, both on reducing cast pressures and their effect on cast molding and strength, and take these into consideration when selecting a preferred method.
Master's Method.
Dr. Scott Mubarak: Bivalving a cast allows one to remove the dorsal or volar portion of the cast and allows examination of the worrisome compartments.
A notable series of lower leg ischemia after casting is that described by Mubarak et al. of 9 patients treated with 90/90 spica casting for femur fracture [20]. This series described ischemic injuries associated with the spica cast technique of first wrapping a below-the-knee cast and then pulling traction on that cast as the rest of the spica was applied. All patients in this series had pressure and ischemic problems, including deep muscle necrosis and full-thickness skin pressure sores. The mechanism of injury was described as pressure on the tissues of the calf by pulling traction and then fixing the leg in that position by connecting it to the rest of the cast. Additionally, leg elevation and hip/knee flexion can lead to hypoperfusion, further ischemia, and rebound swelling. Once the child awakens from anesthesia and muscles contract, there is even further pressure on the leg that is now in a fixed position from the cast.
Master's Method.
Dr. Scott Mubarak: Never use a cast as a traction device without a traversing pin. Even lifting the leg for the thigh and torso cast application allows the patient's leg to slide into the cast, causing the pressure points over the posterior calf and ankle dorsum.
Based on this series, the authors recommend traction on the bare calf and not through the cast as the spica is applied from abdomen to below the knee. Such principles can be applied to upper extremity casting, in which casting in extremes of flexion should be avoided to minimize risk for reduced venous outflow and a resultant forearm compartment syndrome (see Fig. 9).
Master's Method.
Dr. Matthew Halanski: A casted limb should be a more comfortable limb. If a child is more uncomfortable in a cast, the reason needs to be investigated.
Is the cast too tight? Bivalve it. Has a fracture, lost alignment/pressure sore developed? Radiographs may help – taking notice of the cast and the soft tissues, not just the bony alignment. Did the child put something down the cast? Radiograph and/or removal and re-application to check.
“There is no such thing as a hypochondriac in a cast.” Charles T Price, MD.
Figure 9.
When placing a spica cast for treatment of femoral shaft fractures, traction should be applied through the bare calf and the spica applied from the abdomen proximally to below the knee distally. Images courtesy of Scott Mubarak, MD.
Loss of reduction
When used for fracture treatment, casts and splints can be molded to help maintain fracture alignment. Poor molding or inadequate immobilization can lead to fracture displacement during follow-up. Casts with excessive padding or asymmetry of padding application can result in a poor fit that predisposes to fracture displacement [21]. Sagittal-to-coronal cast index, a ratio of the inner cast diameter on lateral and anterior-posterior views, >0.7 has been shown to increase risk for fracture displacement in the treatment of forearm and distal radius fractures [21,22]. To minimize risk for fracture displacement, the applicator should ensure proper fit with three-point molding and a low cast index. Fractures should be monitored closely with serial radiographs, and if displacement occurs, re-manipulation or cast wedging can be considered (see Fig. 10).
Master's Method.
Dr. Matthew Halanski, MD: If a cast is well-fitting, cast wedging may be attempted. However, wedging is NOT a substitute or “fix” for a poorly fitting or poorly applied cast. Doing so will likely lead to additional problems with pressure. Furthermore, the clinician must carefully review post-wedging radiographs to ensure that the skin is not compromised by the procedure and that the neurovascular status of the limb is not affected.
Figure 10.
Example of a poorly molded “banana” shaped cast which can predispose to loss of fracture reduction. Image courtesy of Valerie Parrish, PA-C.
Medicolegal implications of cast complications
Cast-related complications have the potential to negatively impact patient care and can result in permanent disability. In a study of a large pediatric multispecialty care group, cast-related complications were found to be the leading cause of litigation [1]. The authors estimated that the average medical-legal cost of a single cast saw burn exceeded $15,000 [1]. Treatment of fractures and cast application are frequently among the most common claim categories in pediatric orthopaedic malpractice claims [22]. Compared to adult malpractice claims, pediatric claims are more likely to end in payment to the plaintiff, and settlement can favor the plaintiff in >50% of cases [23,24].
Though casting can be viewed as less invasive than surgical treatment, proper informed consent explaining potential complications should not be overlooked. The treating orthopaedist should discuss the diagnosis, describe the proposed casting procedure, including expected duration and outcomes, risks of casting such as those discussed above, alternative treatment options, and risks of no treatment [25]. Cast application technique and patient/parent warnings and return precautions should be appropriately documented. Routine follow-up is imperative to ensure early recognition of complications, and parent concerns should be addressed in a timely fashion to minimize delay of care when complications arise.
Summary
Proper cast and splint application is necessary to prevent common pitfalls and complications such as cast sores, cast saw burns, fracture displacement, and compartment syndrome. An understanding of patient and treatment risk factors and following the standards of care can minimize clinical and medicolegal risks.
To reduce the severity of complications, it is essential to educate and collaborate with patients and their caregivers. The general public frequently sees casts and splints and therefore assumes that these are risk-free. A knowledgeable provider will inform patients and families that casts and splints carry a 1% risk of complications, even in the most experienced hands. This awareness will not only highlight the possibility of cast-related issues but also help manage expectations. It is important to clarify where pain is expected (around the incisions or injured areas under the cast) and the anticipated duration of pain following surgery or fracture treatment. Inform the family that pain occurring days later, particularly if it is away from the injury or incision, is concerning. Encourage them to monitor for unusual pain patterns so they can seek assistance sooner rather than later.
Test your knowledge
Review questions and answers for the JPOSNA® Primer on Cast and Splint Application can be found through the links below.
Author contributions
Jessica A. McGraw-Heinrich: Conceptualization, Writing – original draft, Writing – review & editing. Jon C. Wall: Conceptualization, Writing – original draft, Writing – review & editing. Scott B. Rosenfeld: Conceptualization, Writing – original draft, Writing – review &editing.
Funding
No funding was received.
Ethics approval and consent
The author(s) declare that no patient consent was necessary as no images or identifying information are included in the article.
Declaration of competing interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgments
We thank our consultant cast masters Scott Mubarak, MD, and Matthew A. Halanski, MD.
Footnotes
This article is part of a special issue entitled: POSNA Primer on Cast and Splint Application published in Journal of the Pediatric Orthopaedic Society of North America.
Supplementary material to this article can be found online at https://doi.org/10.1016/j.jposna.2025.100244.
Appendix A. Supplementary material
The following is/are the supplementary data to this article.
References
- 1.Larson J.E., Nicolay R.W. Cast saw burn prevention: an evidence-based review. J Am Acad Orthop Surg. 2021;29(9):380–385. doi: 10.5435/JAAOS-D-20-00723. [DOI] [PubMed] [Google Scholar]
- 2.Williamson C., Scholtz J.R. Time-temperature relationships in thermal blister formation. J Invest Dermatol. 1949;12(1):41–47. doi: 10.1038/jid.1949.7. [DOI] [PubMed] [Google Scholar]
- 3.Halanski M.A., Halanski A.D., Oza A., Vanderby R., Munoz A., Noonan K.J. Thermal injury with contemporary cast-application techniques and methods to circumvent morbidity. J Bone Joint Surg Am. 2007;89(11):2369–2377. doi: 10.2106/JBJS.F.01208. [DOI] [PubMed] [Google Scholar]
- 4.Hutchinson M.J., Hutchinson M.R. Factors contributing to the temperature beneath plaster or fiberglass cast material. J Orthop Surg Res. 2008;3:10. doi: 10.1186/1749-799X-3-10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Deignan B.J., Iaquinto J.M., Eskildsen S.M., Woodcock C.A., Owen J.R., Wayne J.S., Kuester V.G. Effect of pressure applied during casting on temperatures beneath casts. J Pediatr Orthop. 2011;31(7):791–797. doi: 10.1097/BPO.0b013e31822d3897. [DOI] [PubMed] [Google Scholar]
- 6.Shore B.J., Hutchinson S., Harris M. Epidemiology and prevention of cast saw injuries: results of a quality improvement program at a single institution. J Bone Joint Surg Am. 2014;96(4):e31. doi: 10.2106/JBJS.L.01372. [DOI] [PubMed] [Google Scholar]
- 7.Halanski M.A. How to avoid cast saw complications. J Pediatr Orthop. 2016;36(Suppl 1):S1–S5. doi: 10.1097/BPO.0000000000000756. [DOI] [PubMed] [Google Scholar]
- 8.Steiner S.R.H., Gendi K., Halanski M.A., Noonan K.J. Efficiency and safety: the best time to valve a plaster cast. J Bone Joint Surg Am. 2018;100(8) doi: 10.2106/JBJS.17.00389. [DOI] [PubMed] [Google Scholar]
- 9.McNeil D.S., Trenholm J.A.I. Establishing safety parameters for orthopaedic cast saw blade usage. J Pediatr Orthop. 2021;41(10):e884–e888. doi: 10.1097/BPO.0000000000001928. [DOI] [PubMed] [Google Scholar]
- 10.Stork N.C., Lenhart R.L., Nemeth B.A., Noonan K.J., Halanski M.A. To cast, to saw, and not to injure: can safety strips decrease cast saw injuries? Clin Orthop Relat Res. 2016;474(7):1543–1552. doi: 10.1007/s11999-016-4723-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Sevencan A. Current complications of cast removal with oscillating saws and a novel method for reducing such complications: a comparative clinical study. J Bone Joint Surg Am. 2023;105(1):35–41. doi: 10.2106/JBJS.21.01556. [DOI] [PubMed] [Google Scholar]
- 12.Halanski M., Noonan K.J. Cast and splint immobilization: complications. J Am Acad Orthop Surg. 2008;16(1):30–40. doi: 10.5435/00124635-200801000-00005. [DOI] [PubMed] [Google Scholar]
- 13.Drake D.F., Ritzman T.F. Cast-related complications. Orthop Clin N Am. 2021;52(3):231–240. doi: 10.1016/j.ocl.2021.03.005. [DOI] [PubMed] [Google Scholar]
- 14.Ravi M., Fernandez Faith E., Whitaker A., Kaffenberger J. Dermatologic complications of orthopedic casts in pediatric patients. Pediatr Dermatol. 2022;39(1):5–11. doi: 10.1111/pde.14884. [DOI] [PubMed] [Google Scholar]
- 15.Murgai R.R., Compton E., Patel A.R., Ryan D., Kay R.M. Foam padding in postoperative lower extremity casting: an inexpensive way to protect patients. J Pediatr Orthop. 2018;38(8):e470–e474. doi: 10.1097/BPO.0000000000001212. [DOI] [PubMed] [Google Scholar]
- 16.Davids J.R., Frick S.L., Skewes E., Blackhurst D.W. Skin surface pressure beneath an above-the-knee cast: plaster casts compared with fiberglass casts. J Bone Joint Surg Am. 1997;79:565–569. doi: 10.2106/00004623-199704000-00013. [DOI] [PubMed] [Google Scholar]
- 17.Shaw K.A., Moreland C., Boomsma S.E., Hire J.M., Topolski R., Cameron C.D. Volumetric considerations for valving long-arm casts: the utility of the cast spacer. Am J Orthoped. 2018;47(7) doi: 10.12788/ajo.2018.0061. [DOI] [PubMed] [Google Scholar]
- 18.Crickard C.V., Riccio A.I., Carney J.R., Anderson T.D. Analysis and comparison of the biomechanical properties of univalved and bivalved cast models. J Pediatr Orthop. 2011;31(1):39–43. doi: 10.1097/BPO.0b013e318202c446. [DOI] [PubMed] [Google Scholar]
- 19.Montgomery B.K., Perrone K.H., Yang S., Segovia N.A., Rinsky L., Pugh C.M., Frick S.L. Does the location of short-arm cast univalve effect pressure of the three-point mould? J Child Orthop. 2020;14(3):236–240. doi: 10.1302/1863-2548.14.200034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Mubarak S.J., Frick S., Sink E., Rathjen K., Noonan K.J. Volkmann contracture and compartment syndromes after femur fractures in children treated with 90/90 spica casts. J Pediatr Orthop. 2006;26(5):567–572. doi: 10.1097/01.bpo.0000230329.06460.f7. [DOI] [PubMed] [Google Scholar]
- 21.Webb G.R., Galpin R.D., Armstrong D.G. Comparison of short and long arm plaster casts for displaced fractures in the distal third of the forearm in children. J Bone Joint Surg Am. 2006;88(1):9–17. doi: 10.2106/JBJS.E.00131. [DOI] [PubMed] [Google Scholar]
- 22.Chess D.G., Hyndman J.C., Leahey J.L., Brown D.C., Sinclair A.M. Short arm plaster cast for distal pediatric forearm fractures. J Pediatr Orthop. 1994;14(2):211–213. doi: 10.1097/01241398-199403000-00015. [DOI] [PubMed] [Google Scholar]
- 23.Oetgen M.E., Parikh P.D. Characteristics of orthopaedic malpractice claims of pediatric and adult patients in private practice. J Pediatr Orthop. 2016;36(2):213–217. doi: 10.1097/BPO.0000000000000412. [DOI] [PubMed] [Google Scholar]
- 24.Galey S.A., Margalit A., Ain M.C., Brooks J.T. Medical malpractice in pediatric orthopaedics: a systematic review of US case law. J Pediatr Orthop. 2019;39(6):e482–e486. doi: 10.1097/BPO.0000000000001348. [DOI] [PubMed] [Google Scholar]
- 25.Suk M., Udale A.M., Helfet D.L. Orthopaedics and the law. J Am Acad Orthop Surg. 2005;13(6):397–406. doi: 10.5435/00124635-200510000-00004. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.