Abstract
Background
While cardiac arrest during pregnancy is uncommon, its consequences can be severe and life-threatening. Existing literature suggests that providers have knowledge gaps regarding resuscitation in peripartum patients. Simulation has been used to train obstetrics nurses and other trainees in Advanced Cardiac Life Support (ACLS). However, training curricula designed for providers with little formal obstetric resuscitation experience is lacking.
Aims
To improve internal medicine residents’ knowledge and confidence related to the resuscitation of pregnant patients.
Methods
This was a one-group pre-test, immediate post-test, delayed post-test observational study. Prior to the simulation, residents completed a survey assessing their confidence managing pregnant patients as well as knowledge related to ACLS in pregnancy. Each team then participated in a 30-min simulation, received immediate feedback on their performance, and completed an immediate post-simulation knowledge assessment measure. Residents who agreed to participate in the study then completed a delayed post-simulation knowledge and confidence assessment survey three months following the training session.
Results
Eighty-six residents participated in the research study. Immediately after completing the simulation, participants exhibited significant improvements in knowledge related to uterine positioning (+34%), epinephrine dosing (+11%), and timing of perimortem delivery (+22%). Participants also reported increased confidence with managing cardiac arrest in pregnant patients and satisfaction with the simulation. Knowledge and confidence improvements were sustained at the three-month follow-up.
Conclusion
High fidelity simulation can be used to train internal medicine residents to manage cardiac arrest in pregnancy. Simulation training is associated with sustained improvements in medical knowledge and confidence related to peripartum resuscitation.
Keywords: Cardiac arrest, Pregnancy, Simulation, Internal medicine, Residency training
Introduction
Dynamic physiologic changes impact nearly every organ system of patients who are pregnant. Care of pregnant patients must account for this unique physiology as well as the demands of the fetus.1, 2, 3, 4 Although cardiopulmonary arrest in pregnancy is a rare event, over 30% of those who arrest in-hospital do not survive to hospital discharge.5
Providers’ lack of knowledge regarding resuscitation practices is one contributor to parturient mortality.6 In simulated scenarios, resuscitation teams have demonstrated significant deficiencies when evaluated according to the Advanced Cardiac Life Support (ACLS) algorithm for pregnant patients experiencing cardiopulmonary arrest.8, 9 Recognizing the unique physiologic changes and associated challenges of resuscitation during pregnancy, in 2020, the American Heart Association (AHA) published guidelines for managing in-hospital cardiac arrest in patients who are pregnant.7 These guidelines highlight the need for concurrent maternal and obstetric intervention to optimize outcomes.
Past efforts to address knowledge gaps and practical deficiencies in cardiopulmonary resuscitation of pregnant patients have included simulation-based training within obstetrics, anesthesia, midwifery students, and maternal fetal medicine (MFM) teams.10, 11, 12, 13, 14, 15 Notably, none of these simulations involved internal medicine physicians. Internal medicine providers care for obstetric patients as primary providers for patients who are pregnant and admitted to the hospital for non-obstetric causes, in intensive care settings, and as resuscitation team leaders.
To address previously identified provider knowledge gaps, we developed a simulation designed to improve internal medicine residents’ knowledge and confidence in providing resuscitation care to pregnant patients who experience cardiac arrest.
Methods
Study setting
This was a prospective, observational cohort trial at a tertiary care academic hospital. All internal medicine residents were scheduled to participate in this simulation. Prior to the simulation, a member of the research team informed the residents of the research aspect of the simulation and invited them to participate. All consenting residents completed pre- and immediately post-simulation confidence and knowledge assessments as well as repeat, post-simulation confidence and knowledge assessments three months after the simulation. Institutional review board (IRB) approval was obtained prior to initiation of the study (IRB 2021B0125).
Simulation
Participants completed the simulation in groups of four to six. Groups were assigned prior to the simulation to ensure varied post-graduate year representation. Each simulation took place in a high-fidelity simulation room facilitated by one of the authors and a simulation technician. Groups received basic patient information and current vitals prior to starting the simulation. Upon entering the simulation bay, each team member was encouraged to assume a required role within a typical resuscitation team (i.e. airway provider, monitor operator, medication administrator, team lead, code supervisor). Laboratory and other test results were provided at the request of the participants. Standard resuscitative medications and equipment including a defibrillator were available. Depending on the trainees’ actions/inactions the patient either responded appropriately to their interventions or decompensated. Throughout the simulation, the facilitator noted the teams’ performance on key critical actions including timely notification of the obstetrics team, displacement of the uterus to the left during CPR, administration of epinephrine, and timely (<2 min) defibrillation. The facilitator also took notes on the teams’ general code team performance and communication. At the conclusion of the simulation, a member from the research team debriefed the participants’ performance on the simulation using the gather-analyze-summarize (GAS) method. Primary learning objectives included demonstrating that pregnant patients require special considerations in addition to ACLS care and identifying additional interdisciplinary team members who are required during the decompensation of a pregnant patient. Secondary objectives included reviewing physiologic changes that occur in the peripartum patient and how these may affect resuscitation, identification and treatment of ventricular fibrillation (VF) arrest, and identifying common causes for hypoxia and cardiac arrest in pregnancy.
Instruments
For the knowledge assessment component, we utilized four of 12 previously published questions regarding resuscitation of pregnant patients6 (Fig. 1). To evaluate confidence, participants indicated their confidence in caring for a pregnant patient who had suffered a cardiopulmonary arrest on a five-point Likert scale (1 = strongly disagree, 5 = strongly agree; see Appendix). This same assessment was administered before the simulation, immediately after the simulation and again 3-months later.
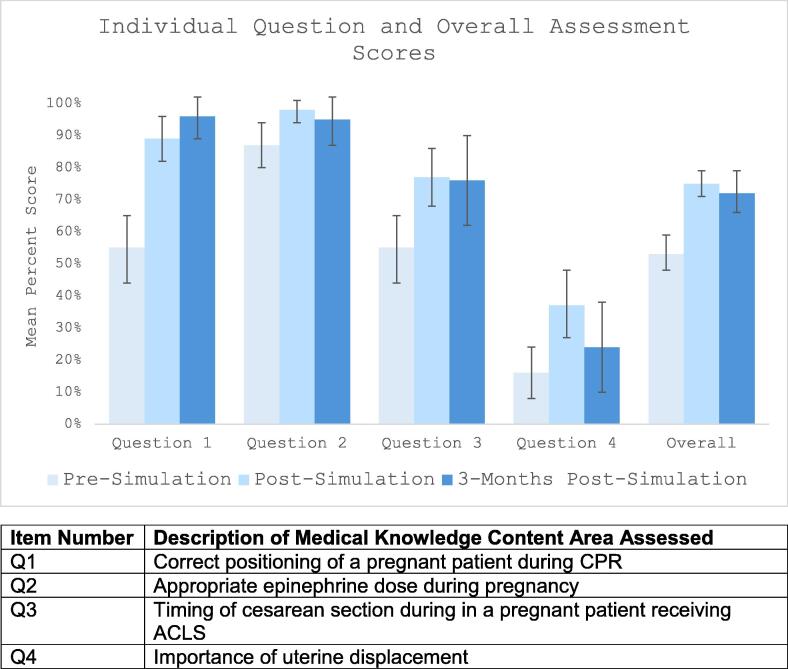
Fig. 1.
Resident performance by question on knowledge assessment measure pre-simulation, immediately post-simulation, and three months post-simulation.
Statistical analysis
Each knowledge-based item was coded dichotomously for a correct or incorrect response. We then computed the mean score for each item for the pre, immediate post, and 3-month follow-up surveys. We also computed an overall knowledge score using these four items. Participant identifiers were not collected and therefore inferential statistical testing was not completed.
Results
Pre-survey
A total of 125 residents were scheduled for the simulation; 86 consented to participate in the research study (69%). Thirty-nine residents were either absent on their scheduled simulation day or chose not to participate.
Participant demographics were collected during the initial pre-simulation survey. Notably, most participants had completed ACLS training within the past year (Table 1).
Table 1.
Demographic information as reported by the participants.
| Characteristic | No. of Respondents (%) |
|---|---|
| Gender | |
| Male | 43 (50) |
| Female | 39 (45) |
| No Response | 4 (5) |
| Training Year | |
| PGY-1 | 35 (41) |
| PGY-2 | 25 (29) |
| PGY-3 | 21 (24) |
| PGY-4 | 5 (6) |
| Completed ACLS Training (2021) | |
| Yes | 59 (72) |
| No | 23 (28) |
The pre-survey demonstrated baseline knowledge deficits related to the resuscitation of pregnant patients. Knowledge related to epinephrine administration and dosing was the highest of all the metrics with 87% of residents indicating the correct dose (Q2). Fifty-five percent of residents recognized the importance of leftward uterine displacement during chest compressions and 55% indicated the appropriate time interval for emergent cesarean section (Q1, Q3, respectively). When asked about the most appropriate “first steps” in resuscitative efforts of the parturient, only 16% of residents correctly identified displacement of the uterus (Q4). The mean score on this four-item pre-test was 53%.
With respect to their confidence, 88% (n = 76) of residents reported “somewhat disagreeing” (20%, n = 18) or “strongly disagreeing” (67%, n = 58) with the statement “I feel confident in my ability to manage maternal cardiac arrest.” The average for this confidence item was 1.52.
Simulation performance
Eighteen different resident groups completed the simulation over the course of three months. All 18 groups (100%) administered the correct dose of epinephrine. Thirteen groups (72%) defibrillated the patient appropriately. Twelve groups (67%) contacted the obstetric team for possible emergent c-section and eight groups (44%) displaced the uterus while completing CPR.
Post-survey
Eighty-three of the 86 residents who consented to participate in the study completed the post-simulation survey (97%). Knowledge related to epinephrine administration and dosing remained the highest of all the metrics with 98% of residents indicating the correct dose (Q2). Eighty-nine percent of residents recognized the importance of leftward uterine displacement during chest compressions at the conclusion of the simulation (Q1) and 77% indicated the appropriate time interval for emergent cesarean section (Q3). When responding to the appropriate “first steps” in the resuscitation of a pregnant patient, the number of correct responses improved to 37% from 16% during the pre-simulation assessment (Q4). Overall, participants scored 75% on the four-item post-test.
With respect to residents’ confidence in managing maternal cardiac arrest, following the simulation 66% (n = 55) of participants either somewhat agreed or strongly agreed that they were confident managing maternal cardiac arrest while 10% (n = 8) reported they either somewhat or strongly disagreed.
Immediately post-simulation, participants showed improvement in knowledge related to correct leftward uterine displacement positioning (+34%), epinephrine dosing (+11%), and timing of perimortem delivery (+22%). As for confidence, participants had a significant improvement for peripartum scenarios. The pre-simulation average was 1.52 which increased to 3.63 after completing the simulation (+139%). Immediately after the simulation, 77 individuals (90%) somewhat agreed or strongly agreed that the methods used to teach the simulation were effective. Seventy-eight individuals (91%) somewhat agreed or strongly agreed that the simulation was well-organized and professional.
Three month follow up
Forty-five residents completed at least some portion of the three-month follow-up survey and assessment (52%). Knowledge related to epinephrine administration remained high with 94% of residents answering this question (Q2); 96% of residents recognized the importance of leftward uterine displacement during chest compressions (Q1) and 76% indicated the appropriate time interval for emergent cesarean section (Q3); 24% identified the correct “first step” in resuscitation of the parturient (Q4; see Fig. 1). Residents’ mean performance on the four-item knowledge assessment was 72%.
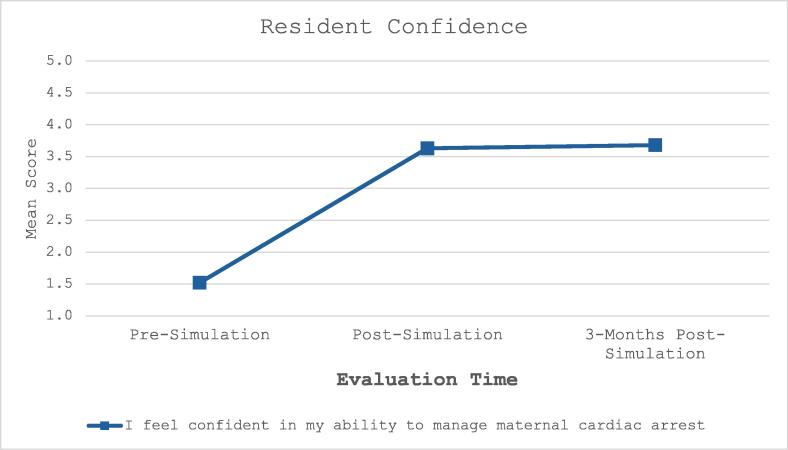
Of the participants who completed the three-month follow-up confidence assessment, 71% (n = 27) somewhat agreed or strongly agreed with the statement that they felt “confidence in my ability to manage maternal cardiac arrest.” Four individuals (11%) somewhat disagreed, and no one strongly disagreed (see Fig. 2). The average for this item slightly increased to 3.68 from the post-simulation assessment. In the three-month follow-up survey, thirty-six individuals (95%) somewhat or strongly agreed that the methods used to teach the simulation were effective and thirty-seven participants (97%) somewhat or strongly agreed that the simulation was well-organized and professional.
Fig. 2.
Resident reported confidence with managing maternal cardiac arrest pre-simulation, immediate post-simulation, and three month post-simulation.
Discussion
Medical care of patients who are pregnant is complex and distinct from that of non-pregnant adults. Although rare, cardiopulmonary arrest during pregnancy is a catastrophic event. It is crucial that providers who respond to in-hospital cardiac arrest events are well-prepared to manage the unique physiologic needs of pregnancy to improve outcomes.
Internal medicine residents initially demonstrated lower pregnancy-specific resuscitation knowledge scores compared to previously published data involving anesthesia, emergency medicine, and obstetric providers.6 However, after participating in the simulation, residents demonstrated a significant improvement in their knowledge of maternal cardiac arrest management, which was sustained up to three months post-simulation.
While previous studies have shown improvement in maternal cardiac arrest knowledge and performance post-simulation,16 few have investigated whether cognitive and confidence improvements noted immediately post-simulation are sustained. One exception is a recent investigation of the effectiveness of obstetric life support education (OBLS) education immediately post-training and 6 and 12 months after education. In this randomized clinical trial, Shields and colleagues demonstrated improvements in confidence managing maternal cardiac arrest at 6 and 12 months post-simulation and sustained improvements in knowledge at 6 months post-simulation.17 However, participants included individuals in the pre-hospital and in-patient settings, and each group included at least one individual with five years of experience and one provider who had some experience managing pregnant patients. Though commendable, Shields and colleagues’ investigation required significant resource utilization to coordinate individuals from multiple different disciplines and secure the necessary space and time to provide the education. Here, we provide an example of how a maternal cardiac arrest simulation can be implemented with fewer resources while still achieving improvements in confidence and knowledge related to cardiac arrest in pregnancy. Additionally, our study was unique in that all simulation participants were internal medicine trainees who have very little formal experience caring for peripartum patients over the course of their residency. Prior studies typically involved individuals with some experiential knowledge when caring for patients who are pregnant (i.e. MFM and obstetric teams). One limitation of this study is its observational design. Additionally, there is a potential for selection bias as individuals who felt more comfortable with resuscitation practices may have been more likely to agree to participate in the research portion. Similarly, those who completed the three-month follow-up knowledge and confidence assessments may have differed from non-responders. Another limitation is the inability to attribute responses to specific individuals as participant responses were not matched and were instead analyzed in the aggregate. Lastly, this study was completed at a single large academic center which may limit generalizability of findings to other programs or institutions. Despite these limitations, this study shows that internal medicine residents exhibit increased knowledge following participation in a parturient cardiac arrest simulation. Future studies are needed to determine whether these improvements in knowledge are associated with improved performance and outcomes in the clinical environment.
Conclusions
After participating in a high-fidelity simulation, internal medicine residents showed a significant increase in both confidence and medical knowledge regarding cardiopulmonary resuscitation for patients who are pregnant. Increases in knowledge and confidence were sustained three months after completing this simulation, providing evidence of the effectiveness of this training activity.
CRediT authorship contribution statement
Carleen R. Spitzer: Writing – original draft, Visualization, Supervision, Methodology, Conceptualization. Philip P. Huang: Writing – review & editing, Visualization, Methodology, Conceptualization. Philip Y. Chang: Writing – review & editing, Resources, Investigation. Allison Rossetti: Writing – review & editing, Visualization, Conceptualization. Jeff Barbee: Writing – review & editing, Visualization, Methodology, Formal analysis.
Declaration of competing interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgments
The authors would like to thank the staff at the Clinical Skills Education and Assessment Center (CSEAC) at the Prior Health Sciences Library for their support and the use of simulation materials.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.resplu.2025.101038.
Contributor Information
Carleen R. Spitzer, Email: carleen.spitzer@osumc.edu.
Philip P. Huang, Email: philip.huang@osumc.edu.
Philip Y. Chang, Email: philip.chang@osumc.edu.
Allison Rossetti, Email: allison.rossetti@osumc.edu.
Jeff Barbee, Email: jeff.barbee@osumc.edu.
Appendix A. Supplementary material
The following are the Supplementary data to this article:
References
- 1.Soskin P.N., Yu J. Resuscitation of the pregnant patient. Emerg Med Clin N Am. 2019;37:351–363. doi: 10.1016/j.emc.2019.01.011. [DOI] [PubMed] [Google Scholar]
- 2.Enomoto N., Yamashita T., Furuta M., et al. Effect of maternal positioning during cardiopulmonary resuscitation: a systematic review and meta-analysis. BMC Pregnancy Childbirth. 2022;22(159) doi: 10.1186/s12884-021-04334-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Helviz Y., Einav S. Maternal cardiac arrest. Curr Opin Anaesthesiol. 2019;32(3):298–306. doi: 10.1097/ACO.0000000000000719. [DOI] [PubMed] [Google Scholar]
- 4.Fischer C., Bonnet M.P., Girault A., Le Ray C. Update: focus in-hospital maternal cardiac arrest. J Gynecol Obstet Hum Reprod. 2019;48(5):309–314. doi: 10.1016/j.jogoh.2019.02.007. [DOI] [PubMed] [Google Scholar]
- 5.Hoyert D. Center for Disease Control and Prevention: National Center for Health Statistics; 2024. Maternal Mortality Rates in the Unites States, 2022. [DOI] [PubMed] [Google Scholar]
- 6.Cohen S.E., Andes L.C., Carvalho B. Assessment of knowledge regarding cardiopulmonary resuscitation of pregnant women. Int J Obstet Anesth. 2008;17(1):20–25. doi: 10.1016/j.ijoa.2007.10.002. [DOI] [PubMed] [Google Scholar]
- 7.Maslovitz S., Barkai G., Lessing J., ZIv A., Many A. Recurrent obstetric management mistakes identified by simulation. Obstet Gynecol. 2007;109:1295–1300. doi: 10.1097/01.AOG.0000265208.16659.c9. [DOI] [PubMed] [Google Scholar]
- 8.Lipman S.S., Daniels K.I., Carvalho B., et al. Deficits in the provision of cardiopulmonary resuscitation during simulated obstetric crises. Am J Obstet Gynecol. 2010;203(2):179.e1–179.e5. doi: 10.1016/j.ajog.2010.02.022. [DOI] [PubMed] [Google Scholar]
- 9.Jeejeebhoy F., Zelop C.M., Lipman S., et al. Cardiac arrest in pregnancy. Circulation. 2015;132(18):1747–1773. doi: 10.1161/CIR.0000000000000300. [DOI] [PubMed] [Google Scholar]
- 10.Adams J., Cepeda Brito J.R., Baker L., et al. Management of maternal cardiac arrest in the third trimester of pregnancy: a simulation-based pilot study. Crit Care Res Pract. 2016;2016 doi: 10.1155/2016/5283765. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Hards A., Davies S., Salman A., Erik-Soussi M., Balki M. Management of simulated maternal cardiac arrest by residents: didactic teaching versus electronic learning. Can J Anaesth. 2012;59(9):852–860. doi: 10.1007/s12630-012-9752-2. [DOI] [PubMed] [Google Scholar]
- 12.Vogel K., Bernloehr A., Willmeroh T., Blattgerste J., Hellmers C., Bauer N.H. Augmented reality simulation-based training for midwifery students and its impact on perceived knowledge, confidence and skills for managing critical incidents. Midwifery. 2024;136 doi: 10.1016/j.midw.2024.104064. [DOI] [PubMed] [Google Scholar]
- 13.Lee A, Sheen JJ, Richards S. Intrapartum Maternal Cardiac Arrest: A Simulation Case for Multidisciplinary Providers | MedEdPORTAL. https://www.mededportal.org/doi/full/10.15766/mep_2374-8265.10768. Accessed 13 December 2022. [DOI] [PMC free article] [PubMed]
- 14.Buttle R.A., Detlefs S., Crump C., Goffman D., Foley M.R., Deering S. Cardiac arrest management in pregnancy: review of team performance in high-fidelity simulations [A337] Obstet Gynecol. 2022;139:97S. doi: 10.1016/j.ajogmf.2022.100626. [DOI] [PubMed] [Google Scholar]
- 15.Fisher N., Eisen L.A., Bayya J.V., et al. Improved performance of maternal-fetal medicine staff after maternal cardiac arrest simulation-based training. Am J Obstet Gynecol. 2011;205(3):239.e1–239.e5. doi: 10.1016/j.ajog.2011.06.012. [DOI] [PubMed] [Google Scholar]
- 16.Shields A.D., Vidosh J., Thomson B.A., et al. Validation of a simulation-based resuscitation curriculum for maternal cardiac arrest. Obstet Gynecol. 2023;142(5):1189–1198. doi: 10.1097/AOG.0000000000005349. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Shields A.D., Vidosh J., Minard C., et al. Obstetric life support education for maternal cardiac arrest: a randomized clinical trial. JAMA Netw Open. 2024;7(11) doi: 10.1001/jamanetworkopen.2024.45295. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.