Abstract
Background:
The United States (US) is an extreme global outlier for drug-related death rates. However, data describing drug-related deaths are generally available only on an 8–13-month lag. Furthermore, granular details about substance-involvement are often not available, which particularly stymies efforts to track fatal polysubstance and novel psychoactive substance use. Detailed medical examiner records provide a powerful source of information for drug-related death surveillance, but have been underutilized.
Methods:
We pooled medical examiner data from five US states and 14 counties that together comprise 18% of the US population to examine demographic, geographic, and drug-specific trends in polysubstance drug-related deaths. We employed mixed effects logistic regression to identify demographic factors associated with polysubstance rather than single substance drug-related deaths. We assessed the correlations between drug classes and described geographic variation in the prevalence of specific drugs and the presence of novel and emerging psychoactive substances.
Results:
Our sample included 73,077 drug-related deaths from 2012 through early 2022. Nearly two-thirds of drug-related deaths were polysubstance-involved, with the number and percentage growing annually. High percentages of polysubstance drug-related deaths were observed in both urban and rural jurisdictions. After adjusting for year and jurisdiction, female, American Indian and Alaska Native, and White individuals had the most elevated odds of polysubstance drug-related deaths. Drug-related deaths involving benzodiazepines or opioids, whether pharmaceutical or illicit, and other pharmaceutical drugs were most likely to have polysubstance involvement, while methamphetamine-involved deaths were least likely to involve multiple substances. Strong correlations were observed between prescription opioids and prescription benzodiazepines, fentanyl and xylazine, and designer benzodiazepines and novel synthetic opioids.
Conclusions:
Analysis of detailed medical examiner records reveals the breadth and complexity of polysubstance drug-related deaths in the US. Future efforts to use this unique resource can improve population-based surveillance of drug-related deaths to better tailor interventions and solutions to this critical health crisis.
Keywords: Epidemiology, Polysubstance, Opioids, Stimulants, Benzodiazepines
Introduction
The United States (US) has entered the “fourth wave” of the overdose crisis, characterized by polysubstance drug-related deaths involving synthetic opioids (e.g., fentanyl) and stimulants (e.g., methamphetamine) (Ciccarone, 2021; Han et al., 2021). Polysubstance use poses unique risks for drug-related death and other health harms (e.g., infective endocarditis, cardiovascular disease) beyond those associated with the use of a single drug (Dai et al., 2022; Glick et al., 2021; Goodwin et al., 2022; Palis et al., 2022). Moreover, there is evidence that individuals engaged in polysubstance use are inadequately treated in the US healthcare system, which largely focuses on single substance use disorders. For example, a study of people with co-occurring opioid and methamphetamine use disorders found that while over 80% were treated for opioid use disorder, less than a quarter were treated for their methamphetamine use disorder (Yen Li et al., 2021).
Despite increased recognition of the importance of polysubstance use to the evolving overdose crisis, data characterizing polysubstance drug-related deaths are hampered by structural data system limitations. National statistics are based on International Classification of Diseases, tenth edition (ICD-10) codes which, at times, lump together dissimilar drugs. For instance, code T40.4 captures both fentanyl, a highly potent synthetic opioid implicated in over 70% of drug-related deaths in the most recently available data, and buprenorphine, a partial opioid agonist used in the treatment of opioid use disorder (National Center for Health Statistics, 2022). Here we employ detailed medical examiner records, which we argue can facilitate surveillance of emerging patterns that are obscured or delayed in national statistics (Centers for Disease Control and Prevention, 2022; Friedman et al., 2022a; Shiue et al., 2021; Shover et al., 2020; Shover et al., 2021; Trinidad et al., 2016). In this analysis, we leverage a novel dataset of detailed medical examiner records to characterize demographic, geographic, and specific drug aspects of polysubstance drug-related deaths.
Methods
Our research team systematically contacted medical examiner and coroner jurisdictions requesting detailed individual-level death records. Five states (Alaska, Connecticut, Minnesota, North Carolina, Wyoming) and 14 US counties voluntarily provided detailed death certificate data in spreadsheet files. Combined, these jurisdictions represent all four US Census regions and account for 18% of the US population (U.S. Census Bureau, 2021). The population density in these jurisdictions ranges from very rural (1.3 persons per square mile in Alaska) to very urban (5,583 persons per square mile in Cook County, IL) (U.S. Census Bureau, 2022). Not all jurisdictions could provide data for the entire 2012–2022 period. As such, jurisdictions contributed data covering varied periods of time between 2012 and early 2022. The number of records and years included are listed in Table 1.
Table 1.
Characteristics of single- and polysubstance drug-related deaths in select U.S. jurisdictions.
| Totala | One substanceb | Polysubstanceb | chi2 | ||||
|---|---|---|---|---|---|---|---|
|
| |||||||
| Sex | p<0.001c | ||||||
| Male | 51,822 | 71% | 19,582 | 38% | 32,340 | 62% | |
| Female | 20,567 | 28% | 7,108 | 35% | 13,459 | 65% | |
| Unknown | 688 | 1% | 297 | 43% | 391 | 57% | |
| Race/Ethnicity | p<0.001d | ||||||
| American Indian or Alaska Native | 1,026 | 1% | 370 | 36% | 656 | 64% | |
| Asian | 1,007 | 1% | 538 | 53% | 469 | 47% | |
| Black or African American | 15,043 | 21% | 5,775 | 38% | 9,268 | 62% | |
| Hispanic or Latin American | 6,486 | 9% | 3,097 | 48% | 3,389 | 52% | |
| Native Hawaiian or Other Pacific Islander | 79 | 0.1% | 54 | 68% | 25 | 32% | |
| White | 45,756 | 63% | 15,880 | 35% | 29,876 | 65% | |
| Other | 345 | 0% | 122 | 35% | 223 | 65% | |
| More than one race | 1,517 | 2% | 480 | 32% | 1,037 | 68% | |
| Unknown | 1,818 | 2% | 671 | 37% | 1,147 | 63% | |
| Age group | p<0.001e | ||||||
| 0–13 years | 280 | 0.4% | 236 | 84% | 44 | 16% | |
| 14–18 years | 414 | 1% | 261 | 63% | 153 | 37% | |
| 19–24 years | 5,559 | 8% | 2,230 | 40% | 3,329 | 60% | |
| 25–29 years | 7,640 | 10% | 2,490 | 33% | 5,150 | 67% | |
| 30–39 years | 16,632 | 23% | 5,189 | 31% | 11,443 | 69% | |
| 40–49 years | 15,216 | 21% | 5,283 | 35% | 9,933 | 65% | |
| 50–59 years | 17,157 | 23% | 6,675 | 39% | 10,482 | 61% | |
| 60–69 years | 8,422 | 12% | 3,750 | 45% | 4,672 | 55% | |
| 70 years and older | 1,425 | 2% | 742 | 52% | 683 | 48% | |
| Unknown | 332 | 0% | 131 | 39% | 201 | 61% | |
| Source of drugs | |||||||
| Illicit drugs | 61,463 | 84% | 22,585 | 37% | 38,878 | 63% | p<0.001 |
| Pharmaceuticals | 25,475 | 35% | 3,843 | 15% | 21,632 | 85% | p<0.001 |
| Illicit drugs and pharmaceuticals | 14,779 | 20% | – | – | – | – | |
| Other | 14,409 | 20% | – | – | – | – | |
| Specific substances | |||||||
| Opioids | 52,109 | 71% | 11,881 | 23% | 40,228 | 77% | p<0.001 |
| Fentanyl and fentanyl analogs | 33,162 | 45% | 6,668 | 20% | 26,494 | 80% | p<0.001 |
| Heroin | 16,907 | 23% | 2,769 | 16% | 14,138 | 84% | p<0.001 |
| Prescription opioids | 14,598 | 20% | 2,421 | 17% | 12,177 | 83% | p<0.001 |
| Nitazenes, brorphine, U-47700 | 339 | 0.5% | 23 | 7% | 316 | 93% | p<0.001 |
| Opioids, unspecified | 814 | 1% | 0 | 0% | 814 | 100% | – |
| Stimulants | 37,881 | 52% | 12,988 | 34% | 24,893 | 66% | p<0.001 |
| Methamphetamine (w/ or w/out amphetamine) | 19,464 | 27% | 8,386 | 43% | 11,078 | 57% | p<0.001 |
| Amphetamine (w/out methamphetamine) | 1,156 | 2% | 186 | 16% | 970 | 84% | p<0.001 |
| Cocaine | 19,374 | 27% | 4,367 | 23% | 15,007 | 77% | p<0.001 |
| MDMA | 459 | 1% | 49 | 11% | 410 | 89% | p<0.001 |
| Benzodiazepines, thienodiazepines, and z-drugs | 12,483 | 17% | 216 | 2% | 12,267 | 98% | p<0.001 |
| Prescription benzodiazepines | 10,382 | 14% | 132 | 1% | 10,250 | 99% | p<0.001 |
| Designer benzodiazepines/thienodiazepines | 972 | 1% | 28 | 3% | 944 | 97% | p<0.001 |
| Z-drugs | 772 | 1% | 0 | 0% | 772 | 100% | p<0.001 |
| Benzodiazepines, unspecified | 1,326 | 2% | 61 | 5% | 1,265 | 95% | p<0.001 |
| Phencyclidine | 1,051 | 1% | 210 | 20% | 841 | 80% | p<0.001 |
| Xylazine | 918 | 1% | 1 | 0.1% | 917 | 100% | p<0.001 |
| Other illicit drugs | 913 | 1% | 107 | 12% | 806 | 88% | p<0.001 |
| Alcohol | 14,050 | 19% | – | – | – | – | |
| Antidepressants | 4,569 | 6% | 403 | 9% | 4,166 | 91% | |
| Gabapentinoids | 2,869 | 4% | 36 | 1% | 2,833 | 99% | |
| Other prescription medications | 4,020 | 6% | 228 | 6% | 3,792 | 94% | |
| Over the counter medications | 3,502 | 5% | 623 | 18% | 2,879 | 82% | |
| Inhalants | 411 | 1% | 312 | 76% | 99 | 24% | |
| Jurisdiction States | p<0.001 | ||||||
| Alaska | 730 | 1% | 195 | 27% | 535 | 73% | |
| Connecticut | 7,709 | 11% | 1,239 | 16% | 6,470 | 84% | |
| Minnesota | 5,530 | 8% | 2,322 | 42% | 3,208 | 58% | |
| North Carolina | 7,413 | 10% | 2,075 | 28% | 5,338 | 72% | |
| Wyoming | 923 | 1% | 418 | 45% | 505 | 55% | |
| Counties | |||||||
| Cobb, GA | 901 | 1% | 283 | 31% | 618 | 69% | |
| Cook, IL | 11,068 | 15% | 2,616 | 24% | 8,452 | 76% | |
| Harris, TX | 3,472 | 5% | 1,216 | 35% | 2,256 | 65% | |
| Jefferson, AL | 554 | 1% | 203 | 37% | 351 | 63% | |
| Los Angeles, CA | 13,596 | 19% | 7,012 | 52% | 6,584 | 48% | |
| Maricopa, AZ | 4,601 | 6% | 1,948 | 42% | 2,653 | 58% | |
| Milwaukee, WI | 2,497 | 3% | 710 | 28% | 1,787 | 72% | |
| Montgomery, PA | 1,058 | 1% | 275 | 26% | 783 | 74% | |
| Pinal, AZ | 415 | 1% | 231 | 56% | 184 | 44% | |
| Sacramento, CA | 1,721 | 2% | 1,137 | 66% | 584 | 34% | |
| San Diego, CA | 6,068 | 8% | 2,583 | 43% | 3,485 | 57% | |
| Summit, OH | 1,337 | 2% | 674 | 50% | 663 | 50% | |
| Tarrant, TX | 2,851 | 4% | 1,602 | 56% | 1,249 | 44% | |
| Travis, TX | 632 | 1% | 248 | 39% | 384 | 61% | |
| Total | 73,077 | 100% | 26,987 | 37% | 46,090 | 63% | |
. Column percentages.
. Row percentages.
. Excludes unknown.
. Combines NHOPI and Other due to small sample sizes, excludes unknown.
. Combines 0–13 and 14–18 due to small sample sizes, excludes unknown.
For this analysis, we investigate “drug-related” deaths, as opposed to “overdose” deaths, in order to provide the most comparable assessment of trends between jurisdictions, given the information consistently provided on death certificates. Jurisdiction-level variation in US death certificate data have been well-documented in the literature; however, broad commonalities in their process facilitate comparison across jurisdictions (Warner et al., 2013). Generally, medical examiner or coroner offices are tasked with investigating all potential drug-related or overdose deaths (as well as all homicides, suicides, unattended deaths, and various other categories). These offices do not investigate all deaths that occur in a given jurisdiction, as some deaths are certified by other physicians (e.g. deaths that occur in the course of hospitalization or following a documented course of disease). Medical examiner and coroner death investigations may include post-mortem toxicological testing of blood, urine, or other specimens, autopsy, review of medical records, observation at scene of death, and interviews with family members or friends. The specific substances tested for in post-mortem toxicology varies both between and within jurisdiction, with some jurisdictions conducting all testing in an in-house lab, others using send-out testing to large private, national laboratories for all cases, and still others employing a combination of these approaches (e.g. testing for a standard list of drugs in-house and sending-out for more complex or ambiguous cases).
US death certificates can include up to four causes (A-D) as well as contributing causes. These do not typically include the term “overdose,” though the more commonly-employed terms “toxicity,” and “intoxication” can be understood to have a similar meaning. ICD-10 mortality codes are assigned for all deaths – including those not investigated by a medical examiner or coroner – separately from the death investigation, and are not typically available from a jurisdiction’s medical examiner or coroner’s office. ICD-10 mortality codes distinguish between “underlying” versus “multiple” cause of death, which does not map perfectly onto the A-D plus contributing causes schema. Overdose surveillance data in the US using ICD-10 mortality codes typically include the following underlying causes of death: Unintentional drug poisonings (X40-X44); Intentional drug poisonings (X60-X64); Homicide drug poisonings (X85); and undetermined drug poisonings (Y10-Y14).Only a few drugs and drug classes have their own three-digit ICD-10 code (e.g., heroin (T40.1), cocaine (T40.5), benzodiazepines (T42.4)) which can be listed as multiple but not underlying cause of death, whether the underlying cause is drug poisoning or something else. Many drugs and medications are grouped from longer ICD-10 codes into a three-digit category that contains multiple distinct drugs. ICD-10 mortality codes beyond three digits are generally not available. It is important to note that ICD-10 codes are assigned based on death certificate data, so the limitations of toxicological testing and determination of cause inherent in the fragmented death investigation system are carried forward into national surveillance data.
Substances identified through toxicological testing are only listed on the death certificate if the death investigator determines they contributed to causing death. For example, a death certificate for a decedent in a shooting homicide with a toxicological finding of a low level of cocaine would be unlikely to include the term “cocaine.” Conversely, the death certificate for an accidental drowning where the decedent had substantial levels of fentanyl detected upon toxicological testing would likely include the term “fentanyl” in the list of causes or contributing causes. Using the methods employed in the current analysis, only the second example would be classified as a drug-related death.
For this analysis, we assessed deaths that listed one or more of the following substances as a cause or contributing factor in the death certificate: fentanyl and fentanyl analogs, heroin, prescription opioids, novel synthetic opioids (e.g. nitazenes, brorphine, U-47700), methamphetamine (with or without other amphetamines), amphetamine (without methamphetamine), cocaine, 3,4-methylenedioxymethamphetamine (MDMA), benzodiazepines (prescription and designer), thienodiazepines, Z-drugs such as Zolpidem, phencyclidine, xylazine, other illicit drugs (ketamine, gamma hydroxybutyrate, synthetic cannabinoids, cannabinoids), antidepressants, gabapentinoids, other pharmaceutical drugs, over the counter medications, or inhalants (e.g. nitrous oxide, butane gas). Supplemental Table 1 contains a full list of over the counter and other prescription drugs included. We used a machine learning algorithm described elsewhere for initial classification (Goodman-Meza et al., 2022), followed by keyword-matching for less common substances. We excluded drug-related deaths where alcohol was the only substance listed, as these were often attributed to conditions arising from chronic alcohol use (e.g., cirrhosis, ketoacidosis) rather than acute intoxication. We further classified drugs by likely source: illicit (including “street drugs” and designer drugs not approved by the US Food and Drug Administration), pharmaceuticals (including prescription and over the counter drugs), and other (e.g., alcohol, inhalants). As the sample included locations with heterogeneous cannabis laws, we included both natural and synthetic cannabinoids in the illicit category, noting that there were no examples of natural cannabinoids other than tetrahydrocannabinol listed on death certificates. Various synthetic cannabinoids were listed as such or by specific compound name. Recognizing that overlap is possible in the illicit and pharmaceutical categories (e.g., fentanyl can be prescribed but in the US street drug supply it is overwhelmingly from illicitly manufactured sources), we use these categories as a proxy for both regulatory status and likely source of acquisition rather than a judgment of their medicinal value.
We classified a death as a polysubstance drug-related death if substances from two or more categories of drugs were listed on the death certificate. It is not possible to determine based on death certificate data (or ICD-10 mortality codes) whether co-occurrence of substances represents simultaneous use of multiple substances in one product (e.g., a speedball containing heroin and cocaine), simultaneous use of multiple products (e.g., taking multiple pills), or use of multiple substances in succession (e.g., taking a pill in the afternoon and smoking fentanyl in the evening). Therefore, our methods – like all large analyses of mortality data without detailed observation of scene or interviews with witnesses – capture polysubstance use in an approximate fashion.
Statistical methods
We employed chi-square tests to compare differences in polysubstance involvement by demographic, geographic, and specific substances. For each specific drug or drug class of interest, we calculated the inter-drug correlations across the entire dataset. To identify demographic correlates of polysubstance drug-related deaths, we fit a mixed effects logistic regression model with polysubstance involvement as the outcome, sex, age, and race/ethnicity as independent variables, and year and jurisdiction as random effects to control for any potential compositional bias. In the adjusted model, we selected as reference groups for categorical variables the group with the lowest percentage of polysubstance involvement (e.g., for race/ethnicity, we used Asian as the reference group to facilitate easier comparison between odds ratios over 1). Finally, we calculated the three most commonly involved drugs in drug-related deaths in each jurisdiction with full-year data for 2021, and determined the set of drugs that were not reported in each jurisdiction that year.
Ethics
This research was determined by the UCLA Institutional Review Board to be exempt from Institutional Review Board oversight as it involved only data from deceased persons and was therefore not human subjects research.
Results
We assess a final sample size of 73,077 drug-related deaths, with records spanning from 2012 through early 2022 (Table 1). The majority (63%, n=46,090) involved two or more substances, with 29% (n=21,455) involving three or more substances. Most (84%) drug-related deaths involved illicit drugs, about a third (35%) involved pharmaceuticals, and 20% simultaneously involved drugs likely to be illicit and drugs likely to be pharmaceutical in origin. Of drug-related deaths involving pharmaceuticals, 85% were polysubstance-involved, compared to 63% of deaths involving illicit drugs.
In bivariate comparisons, polysubstance involvement was most common among women (p<0.001), people aged 25–49 years (p<0.001), and the following racial and ethnic groups: American Indian or Alaska Native, Black or African American, more than one race, and White (p<0.001). There was considerable heterogeneity in polysubstance involvement by jurisdiction, with Alaska; Connecticut; North Carolina; Cook County, IL; Milwaukee County, WI; Montgomery County, PA all having more than 70% polysubstance involvement. Polysubstance involvement was least common in Sacramento County, CA, where two-thirds of drug-related deaths involved only one substance.
In the multivariate model, each additional year of age was associated with slightly lower odds of polysubstance involvement, about one percent lower odds for each year of age (Table 2, and see a detailed age pattern in Table 1). Female decedents had significantly higher odds of polysubstance involvement (aOR = 1.21, 95% CI, 1.17, 1.25). Asian decedents had the lowest odds of polysubstance involvement. Comparatively, American Indian and Alaska Native individuals (aOR 1.86, 95% CI 1.54, 2.23) and White individuals (aOR 1.68, 95% CI 1.47, 1.91) had the highest odds of polysubstance involvement.
Table 2.
Mixed effects logistic regression of demographic correlates of polysubstance involvement in drug-related deaths with jurisdiction as random effects (n=70,917).
| Crude OR | 95% CI | Adjusted OR | 95% CI | |
|---|---|---|---|---|
|
| ||||
| Sex | ||||
| Female | 1.18 | (1.14, 1.23) | 1.21 | (1.17, 1.25) |
| Male (ref) | – | – | – | – |
| Age (per year) | 0.99 | (0.99, 0.99) | 0.99 | (0.99, 0.99) |
| Race/ethnicity* | ||||
| American Indian or Alaska Native | 1.88 | (1.56, 2.26) | 1.86 | (1.54, 2.23) |
| Asian (ref) | – | – | – | – |
| Black or African American | 1.20 | (1.05, 1.37) | 1.27 | (1.11, 1.46) |
| Hispanic or Latin American | 1.50 | (1.31, 1.72) | 1.48 | (1.29, 1.70) |
| More than one race | 1.35 | (1.13, 1.61) | 1.31 | (1.10, 1.56) |
| Other | 1.50 | (1.18, 1.90) | 1.50 | (1.18, 1.91) |
| White | 1.59 | (1.39, 1.81) | 1.68 | (1.47, 1.91) |
| Year | 1.1 | (1.09, 1.11) | 1.1 | (1.1, 1.1) |
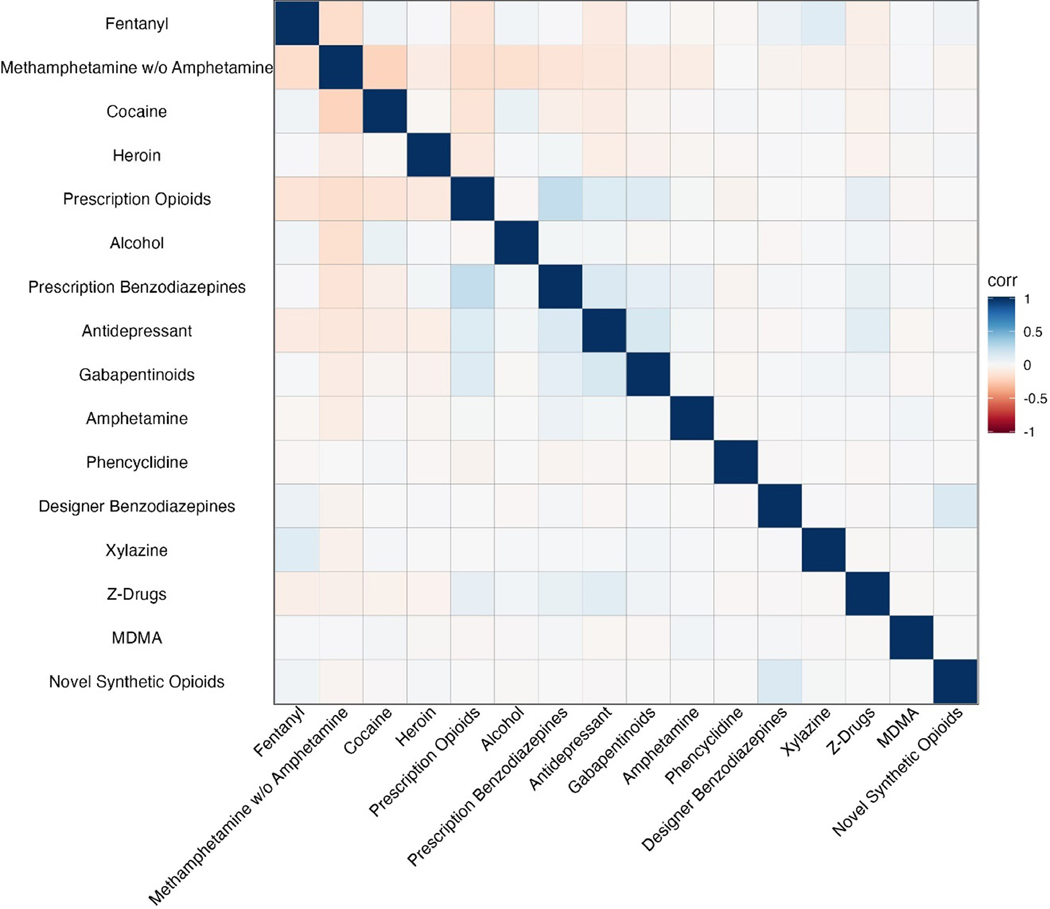
Of the drug classes examined, drug-related deaths related to methamphetamine or inhalants were least likely to be polysubstance-involved. In contrast, over 90% of drug-related deaths related to benzodiazepines, thienodiazepines, and z-drugs—regardless of whether they were pharmaceuticals or designer drugs—were polysubstance-involved, as did over 90% of deaths involving novel synthetic opioids, and all non-opioid prescription drugs (antidepressants, gabapentinoids, or other prescription drugs). Fig. 1 displays correlations between drug classes. The most substantial overlap occurred between prescription opioids with prescription benzodiazepines, and designer benzodiazepines with novel synthetic opioids. There was also appreciable overlap between all classes of prescription drugs, and between fentanyl and xylazine. All but one of 918 xylazine-involved deaths were polysubstance-involved. Though drug-related deaths involving both pharmaceuticals and illicit drugs were relatively common, accounting for one third of all polysubstance drug-related deaths, the correlations were lowest between illicit stimulants (i.e., methamphetamine and cocaine) and prescription drugs of all classes.
Fig. 1.
Correlations between specific substances involved in drug-related deaths, select US jurisdictions, 2012–2021.
In 2021, there were geographic patterns in the specific drug combinations involved in drug-related deaths. Of the five states and eight counties with data corresponding to the full year 2021, fentanyl was part of the most common polysubstance combination in all but one jurisdiction (Table 3). In all jurisdictions in the Western Census Region, the most common combination included fentanyl and methamphetamine, though Alaska’s most common combination also included heroin. Most jurisdictions in the other three Census Regions had fentanyl and cocaine as the most common polysubstance combination, with the exception of Minnesota (fentanyl and methamphetamine), Summit County, OH (fentanyl and methamphetamine), and Travis County, TX (methamphetamine and cocaine).
Table 3.
Most common polysubstance combinations involved in drug-related deaths, 2021.
| Jurisdiction | Population per square mile, 2020 US Census | n | Most Common | Second Most Common | Third Most Common |
|---|---|---|---|---|---|
|
| |||||
| States | |||||
| Alaska | 1.3 | 228 | Methamphetamine, Fentanyl, Heroin (N=23) | Methamphetamine, Fentanyl (N=20) | Rx Opioids, Methamphetamine, Fentanyl (N=18) |
| Connecticut | 744.7 | 1,519 | Fentanyl, Cocaine (N=149) | Fentanyl, Alcohol (N=92) | Fentanyl, Cocaine, Alcohol (N=91) |
| North Carolina | 71.7 | 1,383 | Fentanyl, Cocaine (N=347) | Methamphetamine, Fentanyl (N=219) | Fentanyl, Cocaine, Alcohol (N=132) |
| Minnesota | 214.7 | 2,589 | Methamphetamine, Fentanyl (N=154) | Fentanyl, Alcohol (N=53) | Fentanyl, Cocaine (N=49) |
| Wyoming | 5.9 | 188 | Methamphetamine, Fentanyl (N=12) | Fentanyl, Heroin (N=10) | Methamphetamine, Alcohol (N=10) |
| Counties | |||||
| Cobb, GA | 2,254.8 | 168 | Fentanyl, Cocaine (N=13) | Methamphetamine, Fentanyl (N=11) | Fentanyl, Alcohol (N=8) |
| Cook, IL | 5,583.0 | 2,126 | Fentanyl, Cocaine (N=230) | Fentanyl, Heroin (N=146) | Fentanyl, Alcohol (N=110) |
| Los Angeles, CA | 2,466.9 | 2,766 | Methamphetamine, Fentanyl (N=511) | Fentanyl, Cocaine (N=123) | Fentanyl, Alcohol (N=81) |
| Pinal, AZ | 79.3 | 145 | Methamphetamine, Fentanyl (N=20) | Rx Opioids, Fentanyl (N=5) | Fentanyl, Cocaine (N=5) |
| Sacramento, CA | 1,642.1 | 397 | Methamphetamine, Fentanyl (N=29) | Fentanyl, Alcohol (N=11) | Rx Opioids, Methamphetamine (N=10) |
| Summit, OH | 1,309.2 | 218 | Methamphetamine, Fentanyl (N=50) | Fentanyl, Cocaine (N=20) | Fentanyl, Alcohol (N=13) |
| Tarrant, TX | 2,439.2 | 493 | Fentanyl, Cocaine (N=30) | Methamphetamine, Fentanyl (N=19) | Fentanyl, Alcohol (N=14) |
| Travis, TX | 1,297.9 | 214 | Methamphetamine, Cocaine (N=7) | Fentanyl, Rx Benzos (N=6) | Cocaine, Alcohol (N=6) |
Discussion
Drawing on a novel dataset comprised of medical examiner records representing all four US Census Regions and a wide range of rural and urban environments, we identified key trends in polysubstance drug-related deaths. We find that the proportion of drug-related deaths that were polysubstance-involved was high and increasing each year. Women, American Indian and Alaska Native, and White individuals faced the highest burden of polysubstance drug-related deaths during the study period. Polysubstance involvement was more common among younger people, with the highest percentages among individuals aged 25–49. There was substantial geographic variation in both polysubstance involvement and in specific drugs implicated. Polysubstance involvement was more common in both the most rural (Alaska) and most urban (Cook County, IL) jurisdictions included in the sample, as well as several eastern and midwestern jurisdictions with population densities in between these extremes, suggesting that demographic factors may be more important than population density. . Generally, novel psychoactive substances (e.g., xylazine, novel synthetic opioids, designer benzodiazepines) were more present in eastern and midwestern jurisdictions, which may reflect well-documented geographic patterns of temporal drug trends (Friedman et al., 2022b; Shover et al., 2020; Warner et al., 2013).
Our data suggest an accelerating rate of polysubstance use of opioids and stimulants—warranting particular concern given that concurrent use of both drug classes has been associated with heightened drug-related death compared to the use of either drug classes alone (Palis et al., 2022). Though men substantially outnumber women in drug-related death rates, and may report greater rates of polysubstance use (Goodwin et al., 2022), we found that a greater proportion of drug-related deaths among women were polysubstance-involved. This may be partially explained by previous epidemiological work showing that drug-related deaths among women were more likely to involve pharmaceuticals (Skurtveit et al., 2022; Wightman et al., 2021), which we find to be more closely associated with polysubstance drug-related deaths compared to illicit drugs.
Our findings on racial and ethnic disparities in polysubstance drug-related deaths should be considered in light of evidence of growing racial disparities in drug-related deaths in recent years (Friedman and Hansen, 2022c; Han et al., 2022; Humphreys et al., 2022), as well as previous epidemiological findings that American Indian and Alaska Natives have had elevated rates of polysubstance drug-related deaths involving opioids (Qeadan et al., 2022). In the early 2000s opioid-related death rates grew the fastest among American Indian and Alaska Native and White individuals (Humphreys et al., 2022), which were the racial groups with the highest burden of polysubstance drug-related deaths in the current analysis. However, substantial work has shown that opioid-related deaths among Black and African Americans has surpassed that of White individuals in more recent years, and drug-related mortality among Hispanic and Latin Americans has grown more quickly than other groups (Friedman and Hansen, 2022c; Romero et al., 2023). It is therefore important to note that the share of drug-related deaths in these racial and ethnic groups attributable to polysubstance is also substantially elevated. Future work developing and expanding strategies to provide culturally competent overdose prevention and other harm reduction services targeted to people who use multiple substances is critical to reduce these disparities (Anastario et al., 2022; Febres-Cordero et al., 2023).
Limitations
Although the jurisdictions represented cover a large proportion of the US population, they may not provide findings that are fully generalizable to other parts of the US. Because data were provided voluntarily, this should be considered to be a convenience sample, and it is possible that jurisdictions that did not provide these data differ systematically from those that did. Previous work has shown how jurisdictions differ in how they certify drug-related deaths and identify specific drugs (Warner et al., 2013), including which substances are part of standard toxicological screening, autopsy rate, how deaths are classified, as well as differences between medical examiner versus coroner systems (Denham et al., 2022). The keyword matching techniques used to identify specific substances likely missed less-common drugs and medications. There may be limited instance of drug name misspellings, which would lead to misclassification and underestimation of the importance of each drug class. Our analysis was not able to identify when a death involved more than one drug from the same drug class; thus, the true amount of polysubstance involvement may be even higher when considering deaths that involve, for example, two prescription opioids or multiple fentanyl analogues. As with any research relying on medical examiner data, identification of specific substances is only possible so far as medical examiner offices test for these substances. Budget constraints, technology, and varying awareness of emerging drug trends may result in under-testing for less common or newer drugs (Ropero-Miller et al., 2020). Using contributory cause of death, as we did, may mitigate some of these concerns (Boslett et al., 2020). Jurisdictions may have differential rates of prescribing medications, which could influence which substances are implicated in drug-related deaths.
Public health implications
Our analysis identifies important facets of polysubstance drug-related deaths that would be impossible to determine using standard national datasets. The substantial overlap between illicit and pharmaceutical substances highlights the need for service providers to consider that an individual presenting for one kind of treatment or harm reduction service may be knowingly or unknowingly using substances in multiple drug classes. Community-based drug checking interventions can shed light on this and provide a better understanding of the illicit drug supply (Maghsoudi et al., 2022), as well as informing the degree to which polysubstance drug-related deaths arise from intentional polysubstance use versus unintentional use, contamination, or misrepresented products. Drug seizure data can also provide key information, but these sources are often made public only after considerable delay, if at all. Broad spectrum naloxone training and provision is necessary to reverse opioid related overdoses (Febres-Cordero et al., 2023), but it may not be a sufficient intervention in the setting of increasing deaths due to polysubstance use (Messinger et al., 2023). Interventions in the management of stimulant and benzodiazepine overdoses are increasingly necessary. In the absence of direct antagonists to stimulants to reverse overdoses, safe environments (e.g., overdose prevention sites) and safe supply of substances for people with stimulant use disorder are potential interventions to reduce the number of polysubstance use deaths(Chalfin et al., 2023; Fleming et al., 2020; Harding et al., 2022; Lambdin et al., 2022; Mansoor et al., 2022). Analysis of detailed medical examiner records reveals the breadth and complexity of polysubstance drug-related deaths in the US. Future efforts to use this unique resource can improve population-based surveillance of drug-related deaths to better tailor interventions and solutions to this critical health crisis.
Supplementary Material
Supplementary material associated with this article can be found, in the online version, at doi:10.1016/j.drugpo.2024.104397.
Acknowledgments
The authors wish to thank the medical examiners and coroners who generously supplied detailed death certificate data used for this analysis.
Funding
CLS was supported by a grant from the National Institutes of Health and National Institute on Drug Abuse (K01-DA050771). JRF received support from the UCLA Medical Scientist Training Program (National Institute of General Medical Sciences training grant (GM008042). DGM was supported by a grant from the National Institute of Health and National Institute on Drug Abuse (K08-DA048163–03). CLS and DGM were supported by supported by a grant from the National Institute of Health and National Institute on Drug Abuse (R01-DA57630). The funders had no role in the design, conduct, or decision to publish this manuscript.
Footnotes
CRediT authorship contribution statement
Chelsea L. Shover: Conceptualization, Formal analysis, Methodology, Writing – original draft. Joseph R. Friedman: Conceptualization, Formal analysis, Methodology, Writing – review & editing. Ruby Romero: Data curation, Project administration, Writing – review & editing. Sergio Jimenez: Data curation, Writing – review & editing. Jacqueline Beltran: Data curation, Writing – review & editing. Candelaria Garcia: Data curation, Writing – review & editing. David Goodman-Meza: Writing – review & editing, Formal analysis, Visualization.
Declaration of competing interest
The authors have no conflicts of interest to declare.
Ethics
This research was determined by the UCLA Institutional Review Board to be exempt from Institutional Review Board oversight as it involved only data from deceased persons and was therefore not human subjects research.
References
- Anastario M, Firemoon P, Rodriguez AM, Wade C, Prokosch C, Rink E, & Wagner E (2022). A pilot study of polysubstance use sequences across the lifespan among Assiniboine and Sioux people who use injection drugs. International Journal of Environmental Research and Public Health, (1), 20. 10.3390/ijerph20010543 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Boslett AJ, Denham A, & Hill EL (2020). Using contributing causes of death improves prediction of opioid involvement in unclassified drug overdoses in US death records. Addiction, 115(7), 1308–1317. 10.1111/add.14943 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Centers for Disease Control and Prevention. (2022). State unintentional drug overdose reporting system (SUDORS). Retrieved June 17 from https://www.cdc.gov/drugoverdose/fatal/dashboard/index.html.
- Chalfin A, del Pozo B, & Mitre-Becerril D (2023). Overdose prevention centers, crime, and disorder in New York City. JAMA Network Open, 6(11), Article e2342228. 10.1001/jamanetworkopen.2023.42228. e2342228-. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ciccarone D (2021). The rise of illicit fentanyls, stimulants and the fourth wave of the opioid overdose crisis. Current Opinion in Psychiatry, 34(4), 344–350. 10.1097/yco.0000000000000717 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dai Z, Smith GS, Hendricks B, & Bhandari R (2022). Brief report: Cause of death among people discharged from infective endocarditis related hospitalization-West Virginia, 2016–2019. Clinical Cardiology, 45(5), 536–539. 10.1002/clc.23812 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Denham A, Vasu T, Avendano P, Boslett A, Mendoza M, & Hill EL (2022). Coroner county systems are associated with a higher likelihood of unclassified drug overdoses compared to medical examiner county systems. The American Journal of Drug and Alcohol Abuse, 48(5), 606–617. 10.1080/00952990.2022.2072223 [DOI] [PubMed] [Google Scholar]
- Febres-Cordero S, Smith DJ, Wulkan AZ, Béliveau AJ, Gish A, Zine S, Fugitt L, & Giordano NA. (2023). It’s what the community demands: Results of community-based emergency opioid overdose trainings. Public Health Nursing, 40(1), 44–53. 10.1111/phn.13151 [DOI] [PubMed] [Google Scholar]
- Fleming T, Barker A, Ivsins A, Vakharia S, & McNeil R (2020). Stimulant safe supply: A potential opportunity to respond to the overdose epidemic. Harm Reduction Journal, 17(1), 6. 10.1186/s12954-019-0351-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Friedman J, Bourgois P, Godvin M, Chavez A, Pacheco L, Segovia LA, … Arredondo J (2022a). The introduction of fentanyl on the US-Mexico border: An ethnographic account triangulated with drug checking data from Tijuana. International Journal of Drug Policy, 104, Article 103678. 10.1016/j.drugpo.2022.103678 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Friedman J, Montero F, Bourgois P, Wahbi R, Dye D, Goodman-Meza D, & Shover C (2022b). Xylazine spreads across the US: A growing component of the increasingly synthetic and polysubstance overdose crisis. Drug and Alcohol Dependence, 233, Article 109380. 10.1016/j.drugalcdep.2022.109380 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Friedman JR, & Hansen H (2022c). Evaluation of increases in drug overdose mortality rates in the US by race and ethnicity before and during the COVID-19 pandemic. JAMA Psychiatry, 79(4), 379–381. 10.1001/jamapsychiatry.2022.0004 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Glick SN, Klein KS, Tinsley J, & Golden MR (2021). Increasing heroin-methamphetamine (Goofball) use and related morbidity among Seattle area people who inject drugs. The American Journal on Addictions, 30(2), 183–191. 10.1111/ajad.13115 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Goodman-Meza D, Shover CL, Medina JA, Tang AB, Shoptaw S, & Bui AAT (2022). Development and validation of machine models using natural language processing to classify substances involved in overdose deaths. JAMA Network Open, 5 (8), Article e2225593. 10.1001/jamanetworkopen.2022.25593. e2225593-. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Goodwin SR, Moskal D, Marks RM, Clark AE, Squeglia LM, & Roche DJO (2022). A scoping review of gender, sex and sexuality differences in polysubstance use in adolescents and adults. Alcohol and Alcoholism, 57(3), 292–321. 10.1093/alcalc/agac006 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Han B, Compton WM, Jones CM, Einstein EB, & Volkow ND (2021). Methamphetamine use, methamphetamine use disorder, and associated overdose deaths among US adults. JAMA Psychiatry, 78(12), 1329–1342. 10.1001/jamapsychiatry.2021.2588 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Han B, Einstein EB, Jones CM, Cotto J, Compton WM, & Volkow ND (2022). Racial and ethnic disparities in drug overdose deaths in the US during the COVID-19 pandemic. JAMA Network Open, 5(9), Article e2232314. 10.1001/jamanetworkopen.2022.32314. e2232314-. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Harding RW, Wagner KT, Fiuty P, Smith KP, Page K, & Wagner KD (2022). It’s called overamping”: Experiences of overdose among people who use methamphetamine. Harm Reduction Journal, 19(1), 4. 10.1186/s12954-022-00588-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Humphreys K, Shover CL, Andrews CM, Bohnert ASB, Brandeau ML, Caulkins JP, Chen JH, Cuéllar M-F, Hurd YL, Juurlink DN, Koh HK, Krebs EE, Lembke A, Mackey SC, Larrimore Ouellette L, Suffoletto B, & Timko C. (2022). Responding to the opioid crisis in North America and beyond: Recommendations of the Stanford-Lancet Commission. The Lancet. 10.1016/S0140-6736(21)02252-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lambdin BH, Davidson PJ, Browne EN, Suen LW, Wenger LD, & Kral AH (2022). Reduced emergency department visits and hospitalisation with use of an unsanctioned safe consumption site for injection drug use in the United States. Journal of General Internal Medicine, 37(15), 3853–3860. 10.1007/s11606-021-07312-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Maghsoudi N, Tanguay J, Scarfone K, Rammohan I, Ziegler C, Werb D, & Scheim AI (2022). Drug checking services for people who use drugs: A systematic review. Addiction, 117(3), 532–544. 10.1111/add.15734 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mansoor M, McNeil R, Fleming T, Barker A, Vakharia S, Sue K, & Ivsins A (2022). Characterizing stimulant overdose: A qualitative study on perceptions and experiences of “overamping”. International Journal of Drug Policy, 102, Article 103592. 10.1016/j.drugpo.2022.103592 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Messinger JC, Beletsky L, Kesselheim AS, & Barenie RE (2023). Moving naloxone over the counter is necessary but not sufficient. Annals of Internal Medicine, 176(8), 1109–1112. 10.7326/m23-0852 [DOI] [PubMed] [Google Scholar]
- National Center for Health Statistics. (2022). Wide-ranging online database for epidemiologic research https://wonder.cdc.gov/wonder/help/main.html#What/20is/20WONDER.
- Palis H, Xavier C, Dobrer S, Desai R, Sedgemore KO, Scow M, Lock K, Gan W, & Slaunwhite A (2022). Concurrent use of opioids and stimulants and risk of fatal overdose: A cohort study. BMC Public Health, 22(1), 2084. 10.1186/s12889-022-14506-w [DOI] [PMC free article] [PubMed] [Google Scholar]
- Qeadan F, Madden EF, Mensah NA, Tingey B, Herron J, Hernandez-Vallant A, Venner KL, English K, & Dixit A (2022). Epidemiological trends in opioid-only and opioid/polysubstance-related death rates among American Indian/Alaska Native populations from 1999 to 2019: A retrospective longitudinal ecological study. BMJ Open, 12(5), Article e053686. 10.1136/bmjopen-2021-053686 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Romero R, Friedman JR, Goodman-Meza D, & Shover CL (2023). US drug overdose mortality rose faster among hispanics than non-hispanics from 2010 to 2021. Drug and Alcohol Dependence, 246, Article 109859. 10.1016/j.drugalcdep.2023.109859 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ropero-Miller JD, Smiley-McDonald HM, Zimmer SA, & Bollinger KM (2020). A census of medicolegal death investigation in the United States: A need to determine the state of our nation’s toxicology laboratories and their preparedness for the current drug overdose epidemic. Journal of Forensic Sciences, 65(2), 544–549. 10.1111/1556-4029.14277 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shiue KY, Austin AE, Proescholdbell S, Cox ME, Aurelius M, & Naumann RB (2021). Literal text analysis of poly-class and polydrug overdose deaths in North Carolina, 2015–2019. Drug and Alcohol Dependence, 228, Article 109048. 10.1016/j.drugalcdep.2021.109048 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shover CL, Falasinnu TO, Dwyer CL, Santos NB, Cunningham NJ, Freedman RB, Vest NA, & Humphreys K (2020). Steep increases in fentanyl-related mortality west of the Mississippi River: Recent evidence from county and state surveillance. Drug and Alcohol Dependence, 216, Article 108314. 10.1016/j.drugalcdep.2020.108314 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shover CL, Falasinnu TO, Freedman RB, & Humphreys K (2021). Emerging characteristics of isotonitazene-involved overdose deaths: A case-control study. Journal of Addiction Medicine, 15(5), 429–431. 10.1097/adm.0000000000000775 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Skurtveit S, Odsbu I, Gjersing L, Handal M, Lid TG, Clausen T, & Hamina A (2022). Individuals dying of overdoses related to pharmaceutical opioids differ from individuals dying of overdoses related to other substances: A population-based register study. European Addiction Research, 28(6), 419–424. 10.1159/000526145 [DOI] [PubMed] [Google Scholar]
- Trinidad JP, Warner M, Bastian BA, Minino AM, & Hedegaard H (2016). Using literal text from the death certificate to enhance mortality statistics: Characterizing drug involvement in deaths. National Vital Statistics Reports: From the Centers for Disease Control and Prevention, National Center for Health Statistics, National Vital Statistics System, 65(9), 1–15. [PubMed] [Google Scholar]
- U.S. Census Bureau. (2021). Geographic levels. https://www.census.gov/programs-surveys/economic-census/guidance-geographies/levels.html.
- U.S. Census Bureau. (2022). U.S. Census QuickFacts. Retrieved January 10 from https://www.census.gov/quickfacts/fact/table/US/PST045221.
- Warner M, Paulozzi LJ, Nolte KB, Davis GG, & Nelson LS (2013). State variation in certifying manner of death and drugs involved in drug intoxication deaths. Academic Forensic Pathology, 3(2), 231–237. 10.23907/2013.029 [DOI] [Google Scholar]
- Wightman RS, Perrone J, Scagos R, Hallowell BD, Krieger M, Li Y, McGregor AJ, Nelson LS, & Marshall BDL (2021). Toxicological and pharmacologic sex differences in unintentional or undetermined opioid overdose death. Drug and Alcohol Dependence, 227, Article 108994. 10.1016/j.drugalcdep.2021.108994 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Yen Li M, Alba GA, Mitton J, & Bearnot B (2021). Care-engaged individuals with polysubstance use in Northeastern US are undertreated for methamphetamine use disorder: A retrospective cohort study. Addiction Science & Clinical Practice, 16(1), 57. 10.1186/s13722-021-00267-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.