Abstract
Background
The transition of nursing master’s degree graduates to clinical practice involves complex challenges that can affect patient care and professional satisfaction. Empirical research on this transition in China is notably sparse, highlighting a significant research gap.
Objective
To explore the challenges faced by Chinese postgraduate nursing master’s students in their clinical work post-graduation using a qualitative approach informed by Meleis’ Transition Theory.
Methods
A qualitative descriptive design was adopted, utilizing phenomenological methods to investigate the clinical challenges faced by Chinese nursing master’s graduates. Fifteen graduates of the master’s degree in Nursing from four tertiary hospitals in Nantong, China, participated in in-depth semi-structured interviews conducted from June to August 2024. Thematic analysis was used to analyze the data.
Results
Six main themes were identified: (1) Professional Identity and Role Conflict, (2) Education and Practice Disconnection, (3) Dissatisfaction with Salary and Development Prospects, (4) Workload Overload and Sustainability Dilemmas, (5) Continuous education and professional title promotion pressure, and (6) Insufficient Research Resources and Support. These six themes are interconnected and mutually influence each other, collectively impacting the transition experience of nursing master’s graduates.
Conclusion
The findings highlight the multifaceted challenges faced by nursing master’s graduates in clinical practice. These insights have significant clinical implications for improving the transition experience and professional development of advanced nursing professionals, ultimately enhancing patient care quality. They also underscore the need for policy initiatives that align nursing education with clinical practice and provide robust support systems for new graduates, ensuring a smoother transition from academic to clinical settings.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12912-025-03790-7.
Keywords: Nursing master’s graduates, Clinical work, Qualitative research, Meleis’ transition theory, Phenomenological research
Introduction
Nursing education is a cornerstone of the healthcare system, playing a pivotal role in addressing the complex health demands of society [1, 2]. In China, the need for specialized nursing professionals has become increasingly critical as the healthcare system evolves and the population ages [3–5]. To meet this demand, the State Council of China approved the establishment of master’s degree programs in nursing in January 2010, recognizing the importance of advanced nursing education in enhancing patient care and health outcomes [6]. By the end of 2022, over 120 higher education institutions in China had initiated these programs, with 124 enrollment units admitting students pursuing a professional nursing master’s degree [7]. In this context, to meet the urgent need for high-level applied advanced practice nurse in both the economy and society as a whole, China began to implement the Program for the Development of Professional Degree Postgraduate Education (2020–2025) in 2020 to vigorously develop professional degree postgraduate education [8]. According to the China Health Yearbook [9], 8890 nurses had undergone postgraduate education, accounting for 0.2% of all nurses. The number of nursing master’s graduates has been steadily increasing, reflecting the growing emphasis on advanced nursing education [5]. This trend underscores the significant investment in nursing education and the growing recognition of the need for specialized nursing expertise in China [10]. Despite the growing number of nursing master’s graduates, the transition from academic settings to clinical practice remains a significant challenge [11, 12].
Recent studies indicate that newly graduated nursing master’s students often face difficulties in translating their academic knowledge into practical applications, adjusting to workplace cultures, and managing the heightened responsibilities of advanced roles [13, 14]. These challenges not only affect individual career satisfaction but also have broader implications for the healthcare system [15]. Specifically, the inability to effectively integrate advanced nursing education into clinical practice can lead to inefficiencies in patient care delivery and potential gaps in the continuity of care [16]. Additionally, the lack of structured support systems for new graduates can contribute to higher rates of burnout and turnover, further straining the healthcare workforce [17]. In South Korea, Minjeong An identified job and work environment satisfaction as critical factors affecting turnover intention for new graduate nurses [18]. In Bahrain, similar challenges have been documented, with studies highlighting the need for better alignment between nursing education and clinical practice [19–21]. This underscores the importance of addressing these challenges in many countries, such as China, Canada, Sweden, and South Korea.
While there is a growing body of research on the challenges faced by nursing master’s graduates in clinical practice, the majority of these studies have been conducted in Western contexts. In contrast to Western countries where structured mentorship and onboarding programs are more common, China’s nursing education and clinical practice systems often lack these supportive structures, exacerbating the challenges faced by new graduates. This contextual uniqueness underscores the need for targeted interventions specific to China’s healthcare environment [22]. In China, empirical research on the transition from academic to clinical settings for nursing master’s graduates is notably sparse. Existing studies often focus on quantitative data, which, while valuable, may fail to capture the nuanced and complex experiences of these graduates [23, 24]. Qualitative research, on the other hand, provides a deeper understanding of the personal experiences, perceptions, and emotions of nursing master’s graduates as they navigate the early stages of their careers [25]. This approach is particularly relevant given the unique cultural and systemic context of China’s nursing education and clinical practice environment. The use of a qualitative approach is well-supported by prior studies on nursing transitions, which highlight the importance of understanding the personal and contextual factors that influence the transition from academic to clinical settings. Qualitative methods allow for a more in-depth exploration of these factors, capturing the complexity and diversity of experiences among nursing master’s graduates [26]. This approach is essential for developing targeted interventions that address the specific needs of this cohort of nursing professionals in China.
Addressing the challenges faced by nursing master’s graduates is crucial for ensuring that the growing number of advanced nursing professionals can contribute effectively to the evolving healthcare needs of China’s aging population and complex healthcare environment. To better understand and address these challenges, we employed Meleis’ Transition Theory [27], which provides a comprehensive framework for understanding the process of transitioning from one role or state to another. This theory emphasizes the importance of mastering certain skills to manage a new state as an indicator of successful transition and highlights the role of support systems, mentorship, and structured onboarding programs in facilitating this transition. By applying Meleis’ Transition Theory, we aimed to identify the specific challenges faced by nursing master’s graduates and propose targeted interventions to support their professional development. The primary objective of this study is to conduct a qualitative exploration of the challenges faced by Chinese nursing master’s graduates in their clinical work. By understanding these challenges from the graduates’ perspectives, we aim to inform strategies that support their professional development and improve the transition from academic to clinical settings. We hope this study contributes to the body of knowledge on nursing education and practice in China and provides valuable insights for nursing educators, healthcare administrators, and policymakers. The following sections detail the study methods, results, discussion, and conclusions.
Methods
Aims
The aim of this study was to explore the challenges faced by Chinese nursing master’s graduates in their clinical work post-graduation.
Study design
This study employed a qualitative exploratory design with a phenomenological approach, informed by Meleis’ Transition Theory [27], to understand the experiences and challenges faced by nursing master’s graduates as they transition from academic to clinical settings. Meleis’ Transition Theory, which emphasizes the importance of support systems and mentorship in facilitating a successful transition, provided a theoretical framework for the study. Specifically, the theory guided the development of the interview questions by focusing on key areas such as professional identity, role conflict, and the integration of advanced education into clinical practice. During the coding process, the theory helped to identify and categorize themes related to these areas, ensuring that the analysis was grounded in the theoretical constructs of transition.
Participants and setting
We employed a mixed sampling strategy combining purposive and snowball sampling to recruit participants. Purposive sampling ensured representation across different demographics and clinical departments, while snowball sampling helped reach additional eligible participants through referrals. The criteria for “maximum variation” included selecting participants with diverse characteristics such as age, gender, and department, to capture a wide range of experiences and perspectives. The study was conducted in four tertiary hospitals in Nantong, China. These hospitals are large, comprehensive medical centers with diverse clinical specialties, including internal medicine, surgery, obstetrics and gynecology, pediatrics, and intensive care units. The hospitals vary in size, with bed capacities ranging from 800 to 1500. They serve a broad patient population and are recognized for their advanced medical services and research capabilities. Inclusion criteria: (1) Chinese nursing master’s graduates in clinical practice, (2) Possessing normal communication abilities. Exclusion criteria: (1) History of mental illness, (2) Participation in similar studies.
Data collection and analysis
Initially, we examined relevant literature on the challenges faced by nursing master’s graduates in clinical settings. This process helped us identify key themes and questions relevant to our research objectives. Based on this review, we developed a preliminary interview outline through intensive group deliberations among the research team. To further refine the interview guide, we conducted pilot interviews with three nursing master’s graduates who met our inclusion criteria. Feedback from these pilot interviews was invaluable in identifying areas for improvement and ensuring that the questions were clear, relevant, and effective in eliciting detailed responses. Additionally, we sought expert advice from professionals in the field of nursing psychology. Their input helped us enhance the interview guide by incorporating questions that captured the nuances of the participants’ experiences. Importantly, the final interview guide was developed exclusively for this study. The recruitment process began with initial contact through nursing managers and supervisors at the selected hospitals, who identified potential participants meeting the study criteria. Information sessions were then conducted to provide detailed study information and obtain informed consent from interested individuals. To expand the participant pool, snowball sampling was employed, where initial participants referred colleagues who might be eligible. Eligibility was confirmed through brief interviews, ensuring participants met the inclusion criteria and did not meet any exclusion criteria. In-depth interviews were subsequently conducted with eligible participants. From June to August 2024, the researchers conducted interviews with 15 individuals, with each session ranging from 30 to 45 min in length. The interviews were conducted in Mandarin Chinese, and the transcripts were translated into English by a professional translator to ensure accuracy and clarity. The interviews were conducted in quiet offices or clinics within the clinical settings of hospitals. Video recordings were used during the interviews to capture participants’ facial expressions and non-verbal behaviors, which provided richer contextual data and enhanced the depth of the qualitative analysis. This study set a sample size of 15 participants, based on the principle of data saturation in qualitative research. Data saturation was achieved after 12 interviews, with no new themes emerging. To confirm saturation, we conducted three additional interviews, which also yielded no new themes, thereby verifying that saturation had been reached [28]. This sample size aligns with the recommended range for phenomenological studies to capture diverse experiences [29]. No repeat interviews were conducted, and transcripts were returned to participants for verification. No significant non-participation was reported, and interviews were conducted in clinical settings with only participants and researchers present to ensure privacy during data collection.
Following data collection, thematic analysis was conducted systematically using NVivo 12.2 software. Interview transcripts were reviewed multiple times to identify recurring patterns and concepts, generating initial codes. Two researchers independently coded the transcripts to ensure consistency and rigor, with discrepancies resolved through discussion and reference to the original data. Initial codes were grouped into broader themes, which were refined and validated through iterative discussions among the research team and member checking with participants. Relevant participant quotes were selected to illustrate key themes and findings, ensuring they accurately reflect the participants’ experiences and perspectives. The final themes were cross-verified with the research objectives and literature to ensure relevance and validity. The findings are consistent with the data, clearly presenting the major themes identified. No minor themes were identified. For more information on the coding scheme used for thematic analysis.
Rigor
To ensure that the findings can be applied to different contexts, the research setting was thoroughly described. Several strategies have been used to guarantee reliability and validity: To assess the rigor of this research, we adhered to Lincoln and Guba’s criteria for enhancing credibility, transferability, reliability, and confirmability [30]. We maintained an audit trail for transparency and traceability throughout the research process. Reliability was ensured through various strategies. The interviewer is a female researcher with a master’s degree in nursing, specializing in qualitative research methods and studies within the nursing field. They had no prior relationship with the participants, ensuring objectivity and minimizing potential biases. The interviewer underwent training in qualitative research methods, including techniques for rapport-building, open-ended questioning, active listening, and maintaining a non-judgmental stance. This approach helped establish a professional rapport with participants, ensuring they felt comfortable sharing their experiences. Additionally, an external audit was conducted by two independent researchers with expertise in qualitative research methods. This audit evaluated the entire research process and findings, ensuring the rigor and validity of the study. The study was overseen by a senior coauthor holding a nursing master’s degree to maintain scientific rigor. The reliability of the results was confirmed through a thorough literature review and theoretical analysis, ensuring that the findings are well-grounded in existing knowledge and theory. In accordance with the Consolidated Criteria for Reporting Qualitative Research (COREQ), we rigorously evaluated the reliability and credibility of our study.
Ethical considerations
This study was approved by the Ethics Committee at Nantong’s Sixth People’s Hospital (approval code: NTLYLL2024028). We strictly followed ethical guidelines to ensure the protection of participants’ rights and well-being. All participants were provided with detailed information about the study, including its purpose, procedures, potential risks and benefits, and their rights to withdraw at any time without penalty. Written informed consent was obtained from each participant prior to their involvement in the study. This process ensured that participants were fully informed and voluntarily agreed to take part in the research. To protect the confidentiality and privacy of participants, several measures were implemented. All personal data were anonymized and stored securely. Participants were assured that their identities would not be disclosed in any reports or publications resulting from the study.
Results
Fifteen Chinese nursing master’s graduates (13 females and 2 males) participated in the study. The youngest participant was 26 years old, and the oldest was 43 years old. The participants in this study are nursing master’s graduates who are currently working in clinical settings across four tertiary hospitals in Nantong, China. While some are recent graduates, others have been in their roles for a few years. Despite their varying levels of experience, all participants face the common challenge of integrating advanced nursing education into clinical practice. Their work involves providing high-quality patient care, engaging in research activities, and managing administrative tasks, all within the environment of clinical nursing. The participants’ characteristics are presented in Table 1.
Table 1.
Characteristics of the participants (n = 15)
| Participants | Gender | Age | Education modes | Years of experience in nursing | Marital status |
|---|---|---|---|---|---|
| P1 | Female | 36 | Full-time | 9 | Married |
| P2 | Female | 43 | Part-time | 20 | Married |
| P3 | Female | 32 | Full-time | 6 | Married |
| P4 | Male | 37 | Full-time | 10 | Married |
| P5 | Male | 26 | Full-time | 1 | Unmarried |
| P6 | Female | 29 | Full-time | 4 | Unmarried |
| P7 | Female | 37 | Part-time | 10 | Married |
| P8 | Female | 30 | Full-time | 4 | Unmarried |
| P9 | Female | 27 | Full-time | 2 | Unmarried |
| P10 | Female | 35 | Full-time | 8 | Married |
| P11 | Female | 36 | Part-time | 9 | Married |
| P12 | Female | 34 | Full-time | 7 | Married |
| P13 | Female | 42 | Full-time | 17 | Married |
| P14 | Female | 29 | Full-time | 2 | Unmarried |
| P15 | Female | 34 | Part-time | 11 | Married |
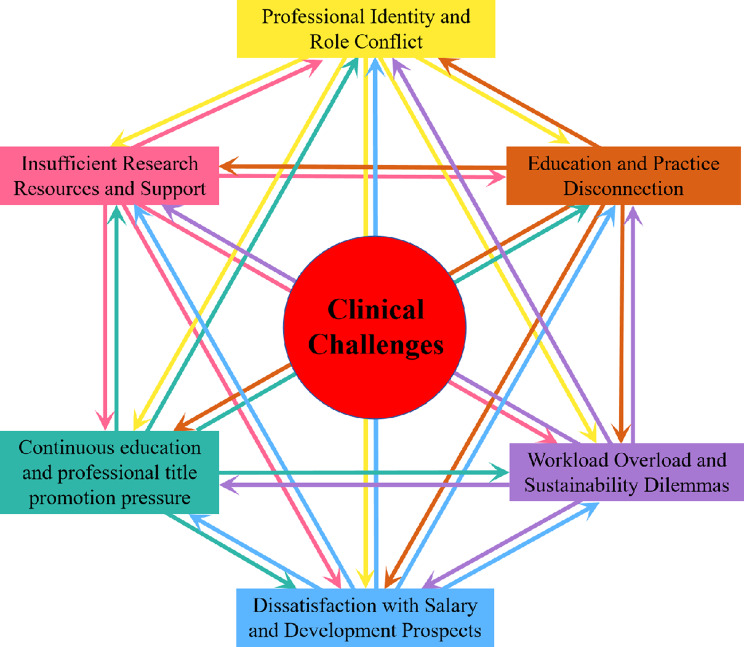
As shown in Fig. 1, the study identified six main themes that highlight the multifaceted challenges faced by Chinese nursing master’s graduates in their clinical work: Professional Identity and Role Conflict, Education and Practice Disconnection, Dissatisfaction with Salary and Development Prospects, Workload Overload and Sustainability Dilemmas, Continuous Education and Professional Title Promotion Pressure, and Insufficient Research Resources and Support. The key themes, definitions, and example quotes are presented in Table 2.
Fig. 1.
Six themes of challenges for Chinese nursing master’s graduates in clinical work
Table 2.
Results section with the summary
| Theme | Definition | Example Quote |
|---|---|---|
| 1.Professional Identity and Role Conflict | Discrepancy between advanced education and practical nursing roles | “Having earned my master’s degree, I anticipated assuming more specialized nursing roles, yet I have often found myself engaged in tasks akin to those of registered nurses.” (P5) |
| 2. Education and Practice Disconnection | Gap between theoretical knowledge and practical application | “I felt well prepared in terms of theoretical knowledge after my master’s, but the practical application of this knowledge in the hospital was a different story.” (P1) |
| 3. Dissatisfaction with Salary and Development Prospects | Unmet expectations regarding compensation and career advancement | “Despite earning a master’s degree, I feel that my salary does not reflect my level of education and expertise.” (P13) |
| 4. Workload Overload and Sustainability Dilemmas | Interconnected challenges of time constraints, role demands, and burnout | “I often find myself working long shifts with little downtime in between. The lack of work-life balance contributes to a sense of burnout.” (P4) |
| 5. Continuous Education and Professional Title Promotion Pressure | Expectation to pursue further education and career advancement | “The pressure to continuously educate myself and advance my professional title can be immense.” (P3) |
| 6. Insufficient Research Resources and Support | Lack of structured support for research activities | “Without defined pathways or mentorship, it’s difficult to know how to proceed with research projects and how to balance them with clinical duties.” (P9) |
Theme 1: Professional identity and role conflict
Nursing master’s graduates often experience a mismatch between their advanced education and the routine tasks they perform, leading to professional identity crises and role conflict. This theme highlights the challenge of reconciling their educational background with the practical demands of their work environment. Analysis revealed distinct patterns: some graduates reported role ambiguity due to underutilized skills, while others emphasized systemic constraints in hierarchical settings.
Having earned my master’s degree, I anticipated assuming more specialized nursing roles, yet I have often found myself engaged in tasks akin to those of registered nurses. This mismatch has sparked a conflict, as my advanced educational background is not reflected in my daily role. (P5).
The role expectations of the clinical setting do not always correspond with the advanced nursing practices I taught. The resulting gap can lead to frustration and role ambiguity. (P8).
The transition to finding our professional identity as nurses is complex. We’re pushed to adapt swiftly to the many demands of the nursing role, yet this rapid adaptation sometimes obscures our sense of identity, leading to feelings of confusion about where we truly fit within the nursing profession. (P12).
Theme 2: Education and practice disconnection
Nursing master’s graduates often face significant gaps between their advanced theoretical knowledge and the practical realities of clinical practice, which impedes the integration of evidence-based practices. This theme highlights the need for better alignment between academic training and clinical responsibilities. Two patterns emerged: (1) theory-practice chasm in routine care workflows, and (2) institutional resistance to innovation. University-affiliated hospitals demonstrated better education-practice alignment than non-teaching centers.
I felt well prepared in terms of theoretical knowledge after my master’s, but the practical application of this knowledge in the hospital was a different story. There was a lack of integration between the latest research and everyday nursing practices. (P1).
My master’s education emphasized the importance of critical thinking and innovation in nursing, but the clinical environment often favored tradition and routine over new ideas. This made it challenging to apply the forward-thinking approaches I had learned. (P14).
Theme 3: Dissatisfaction with salary and development prospects
Nursing master’s graduates often express dissatisfaction with their salaries and limited career advancement opportunities, feeling that their advanced skills are not adequately recognized. This theme highlights the need for better compensation and career development pathways. Dissatisfaction manifested differently: early-career nurses prioritized salary inadequacy, while mid-career nurses focused on opaque promotion pathways.
I hope for more opportunities to participate in decision-making and leadership positions, but currently, I feel that my potential is not being fully utilized. This stagnation in my career development is very frustrating. (P6).
I expected my advanced knowledge and skills to be recognized and reflected in higher pay and better career development opportunities. However, I feel that my efforts are not being adequately rewarded. (P9).
I expect more career advancement opportunities after completing my master’s degree, but the reality is that there are limited chances for promotion, which makes me uncertain about my future career path. (P13).
Theme 4: Workload overload and sustainability dilemmas
Nursing master’s graduates often struggle with balancing high standards of clinical care, research demands, and administrative tasks, leading to significant workload overload and burnout. This theme highlights the need for better time management and support systems to maintain professional efficacy and personal well-being. Specifically, patterns included severe time poverty and emotional exhaustion.
I often find myself working long shifts with little downtime in between. The lack of work‒life balance contributes to a sense of burnout, making it hard to recharge and maintain my passion for nursing. (P4).
The dual demands of providing high-standard clinical care and producing research outputs are often at odds. There’s an expectation to contribute significantly to both areas, which can lead to an overwhelming sense of pressure and burnout. (P10).
The immediate demands of patient care often overshadow research tasks, yet the expectation to contribute to the scientific community through publishing remains. This constant struggle to meet both expectations, along with administrative duties, leaves me feeling overwhelmed and burnt out. Time management becomes a significant issue, as there are never enough hours in the day to fulfill all my responsibilities effectively. It’s a constant battle to maintain a sustainable pace and deliver quality care without neglecting other professional obligations. (P11).
Time management is a significant challenge in my role. Among staff meetings, patient care, and the pursuit of professional development, there is seldom downtime. This makes it hard to find space for reflection and relaxation, which are crucial for maintaining my well-being and preventing burnout. (P15).
Theme 5: Continuous education and professional title promotion pressure
Nursing master’s graduates often face significant pressure to continuously pursue higher education and professional advancement. This theme highlights the need for structured support and resources to facilitate ongoing professional development. Specifically, patterns included intense educational competition pressure and anxiety over professional title promotion, with female nurses perceiving higher levels of stress.
There’s an unspoken expectation that as a master’s graduate, I should be at the forefront of my field. This means I need to continuously seek out new educational opportunities, which can be both motivating and overwhelming. (P2).
The pressure to continuously educate myself and advance my professional title can be immense. It is a constant reminder that in nursing, the learning never stops, and there’s always more I need to know and do. (P3).
The pursuit of continuous education and professional title promotion, including the consideration of applying for a Ph.D., adds a new dimension to job stress. There’s always a sense of urgency to keep learning and advancing, which can be overwhelming in the face of other work and life commitments. (P13).
Theme 6: Insufficient research resources and support
Nursing master’s graduates often lack structured frameworks or mentorship to guide their research endeavors, complicating the balance between clinical and scholarly responsibilities. This theme highlights the need for better research support and mentorship programs. Specifically, patterns included the absence of mentors versus insufficient resources.
Having completed my master’s degree, I find myself at a crossroads, grappling with uncertainty about my career trajectory. The absence of a clear cultivation plan for nursing graduate students from hospital leadership leaves us in a state of confusion. We’re expected to evolve professionally, yet we’re navigating this journey without the necessary guidance and resources. This lack of a structured approach to our career development can lead to frustration and a sense of being underutilized, as we strive to understand our roles and how to effectively advance within the nursing profession. (P7).
One of the main challenges I have faced is the lack of a clear structure for postgraduate research. Without defined pathways or mentorship, it’s difficult to know how to proceed with research projects and how to balance them with clinical duties. (P9).
As a nursing master’s graduate, I anticipated having access to resources and support that would facilitate my professional growth. However, the reality is that we often find ourselves navigating our career development independently, lacking a comprehensive cultivation plan from hospital leadership. This can lead to feelings of frustration and being underutilized. (P15).
The identified themes are interconnected, highlighting the multifaceted nature of the challenges faced by nursing master’s graduates. The disconnection between education and practice (Theme 2) exacerbates professional identity conflicts (Theme 1), while workload overload (Theme 4) and the pressure for continuous education (Theme 5) contribute to burnout and dissatisfaction with career prospects (Theme 3). These findings underscore the need for comprehensive interventions that address multiple aspects of the transition from academic to clinical settings. One surprising finding was the high prevalence of workload overload and burnout (Theme 4), with 80% of participants reporting significant challenges in balancing clinical, research, and administrative tasks. This proportion was determined based on the number of participants who mentioned workload overload during their interviews, relative to the total number of participants.
Discussion
This qualitative study explores the clinical work challenges faced by Chinese nursing master’s graduates during their transition to clinical practice. The study identified six main themes that capture the challenges faced by Chinese nursing master’s graduates in their transition to clinical practice. These challenges align with Meleis’ Transition Theory [27], which emphasizes the importance of mastering certain skills to manage a new state as an indicator of successful transition. Specifically, themes such as “Professional Identity and Role Conflict” and “Education and Practice Disconnection” reflect the initial transition conditions that nursing master’s graduates face as they move from academic to clinical settings. Ongoing struggles like “Workload Overload and Sustainability Dilemmas” and “Continuous Education and Professional Title Promotion Pressure” serve as process indicators, highlighting the dynamic nature of the transition and the continuous efforts required to navigate the clinical environment. Long-term impacts such as “Dissatisfaction with Salary and Development Prospects” and “Insufficient Research Resources and Support” are outcome indicators that reflect the broader consequences of these transition challenges. These challenges form a self-reinforcing cycle, starting with an education-practice disconnect and leading to systemic attrition. The findings underscore the need for targeted interventions to support their professional development within clinical settings and through broader systemic changes.
The rapid expansion of nursing education in China has not been matched by corresponding advances in clinical practice environment. The mismatch between educational preparation and clinical expectations can be attributed to several factors. First, the curriculum in Chinese nursing programs may not fully prepare graduates for the realities of clinical practice, leading to role ambiguity and identity crises [31]. Second, the hierarchical structure of Chinese healthcare institutions often places new graduates in roles that are more aligned with those of registered nurses, rather than leveraging their advanced skills and knowledge. Compared to Western countries where structured mentorship and onboarding programs are more common [32, 33], Chinese nursing graduates often enter clinical settings with limited support and guidance. Additionally, the hierarchical nature of Chinese healthcare institutions often limits the autonomy and decision-making power of new graduates, complicating their transition to clinical practice. In contrast, Western nursing programs often emphasize critical thinking and leadership skills, which are more readily applicable in clinical settings [34]. Addressing these challenges requires a multifaceted approach: (1) Incorporating practical training in nursing education programs to bridge academic-clinical gaps. Establishing mentorship opportunities within academic curricula to enhance professional guidance [35, 36], (2) Implementing structured onboarding programs in healthcare institutions to support new graduates. Designing clear career pathways in clinical settings to promote long-term professional development [37].
Our findings underscore the significant gap between the theoretical knowledge acquired during nursing master’s programs and the practical realities of clinical practice [38], a challenge that is particularly pronounced in China [7]. This gap is exacerbated by the traditional focus on theoretical knowledge in nursing education, which may not be readily applicable in clinical settings [39]. Additionally, the clinical environment in China often prioritizes routine practices over innovative approaches, making it difficult for new graduates to implement their advanced learning [40]. Compared to Australia, where nursing education often includes more practical training and mentorship opportunities, Chinese nursing programs may not fully prepare graduates for the complexities of clinical practice [41]. Similar to China, Japan also faces challenges in nursing education. While Japan’s nursing education system is more established, it still emphasizes the need for practical training and mentorship to better prepare graduates for clinical settings [42]. This discrepancy highlights the need for nursing education programs in China to emphasize evidence-based practice and critical thinking skills. Clinical settings should also foster environments that encourage the application of new knowledge and support the professional growth of new graduates. These strategies are essential for bridging the education-practice gap and enhancing the effectiveness of nursing master’s graduates in clinical practice.
Our study highlights the particular challenges faced by Chinese nursing master’s graduates, who often feel that their advanced qualifications are not adequately recognized or rewarded. This dissatisfaction is exacerbated by the lack of clear career pathways and limited promotional opportunities, which are particularly pronounced in China due to the hierarchical structure of the healthcare system [43]. Compared to America, where nursing professionals often benefit from more transparent career progression frameworks and better compensation policies [44], Chinese nursing graduates face significant barriers to professional advancement. This disparity underscores the need for policymakers in China to implement fair compensation policies and develop clear career progression frameworks to address these issues. Additionally, nursing education programs should provide career counseling and mentorship to support graduates’ professional aspirations, helping them navigate the complexities of the healthcare system and achieve their career goals [45].
The demanding nature of clinical practice, combined with the expectation to contribute to research and administrative tasks, leads to significant workload overload. This is exacerbated by the limited availability of support systems and resources. Compared to Canada, where healthcare institutions often provide more robust support systems and resources for stress management [46], Chinese nursing graduates face a more pronounced challenge due to the hierarchical structure of healthcare institutions and the limited emphasis on work-life balance [47]. Addressing workload overload requires the development of workload standards and the provision of adequate support systems. Healthcare institutions should also promote work-life balance and provide resources for stress management and burnout prevention [48].
Our study highlights the unique challenges faced by Chinese nursing master’s graduates, who often feel overwhelmed by the expectation to pursue higher education and professional titles while managing immediate clinical duties. Compared to countries like the United States and Australia [44, 49], where structured mentorship programs and career development resources are more prevalent, Chinese nursing graduates face greater challenges due to limited support systems [50]. To address these issues, nursing education programs in China should incorporate structured mentorship and career counseling, while healthcare institutions should provide resources for stress management and professional growth [51].
Internationally, nursing professionals often struggle with limited research frameworks and mentorship opportunities, particularly in resource-limited settings. In China, these challenges are exacerbated by the rapid expansion of nursing education, which has outpaced the development of supportive clinical environments [52]. Additionally, the hierarchical structure of healthcare institutions in China further limits opportunities for professional development and advancement among new graduates. Developed countries [53, 54] have more established frameworks for nurse education and mentorship, emphasizing lifelong learning and structured support systems. In Japan, Shinya Ohno et al. highlighted the significant burden faced by caregivers of cancer patients within the Japanese healthcare system, emphasizing the importance of structured support in facilitating transitions [55]. Similarly, See et al. [56] conducted a qualitative systematic review that identified significant challenges in the role transition of newly graduated nurses, including the need for mentorship and structured onboarding programs. Addressing these disparities requires global collaboration and the implementation of evidence-based strategies to bridge the gap between education and clinical practice [54].
This study provides the qualitative exploration of the challenges faced by Chinese nursing master’s graduates, identifying key themes such as professional identity struggles, education-practice gaps, dissatisfaction with salary and career prospects, workload overload, continuous education pressures, and insufficient research support. While these findings illuminate China’s unique transition dynamics, their implications resonate globally. These challenges can significantly impact career trajectories over time. Persistent professional identity conflicts and education-practice gaps may lead to ongoing job dissatisfaction and reduced career advancement opportunities. Chronic workload overload and burnout can negatively affect long-term job performance and personal well-being, potentially leading to higher turnover rates. Additionally, continuous education pressures and insufficient research support may limit professional growth and innovation. Addressing these challenges is crucial for the long-term professional development and well-being of nursing master’s graduates. We recommend the following strategic actions for academic institutions, hospital administrators, and policymakers: (1) Curriculum Reform and Clinical Integration: nursing curricula should be revised to incorporate more experiential learning, clinical simulations, and interdisciplinary training that mirror the real-world expectations of advanced clinical roles. Collaboration between academic institutions and clinical partners must be strengthened to close the education-practice gap. (2) Structured Mentorship and Onboarding Programs: establishing formal mentorship systems and structured transition programs within healthcare facilities can help graduates build confidence, reduce role ambiguity, and foster long-term professional identity development. (3) Transparent Career Pathways and Fair Compensation: institutions must develop transparent promotion criteria and equitable salary structures that reflect the qualifications and contributions of nursing master’s graduates. This will enhance job satisfaction, retention, and leadership development. (4) Research Support and Protected Time: hospitals should invest in research infrastructure, mentorship, and designated time for scholarly activities to support nurses in fulfilling their dual roles as clinicians and researchers. (5) Workload Management and Wellness Programs: implementing workload standards, shift limitations, and wellness programs will mitigate burnout, promote sustainability, and enhance overall care quality. (6) Policy Alignment with National and Global Nursing Strategies: efforts must align with national goals and WHO’s Global Strategic Directions for Nursing and Midwifery (2021–2025), ensuring that nursing graduates are not only clinically competent but also adequately supported to fulfill their potential [57]. This underscores the urgent need for better time management and support systems to prevent burnout and enhance professional satisfaction. Short-term feasibility suggestions include implementing structured mentorship programs and providing immediate support systems to help nursing master’s graduates manage their workload and professional identity conflicts. Medium-to-long-term policy suggestions involve developing comprehensive career development frameworks, aligning nursing education with clinical practice through curriculum reform, and advocating for fair compensation and better research support structures. These interventions are crucial for improving job satisfaction, reducing burnout, and enhancing the overall quality of patient care. Our study uniquely identifies the specific context of China’s healthcare system, where the rapid expansion of nursing education has outpaced the development of supportive structures for new graduates. The study’s limitations include a small sample size (n = 15) and the restriction to hospitals in Nantong, which may limit the generalizability of the findings. The voluntary nature of participation could introduce selection bias, while the reliance on retrospective accounts may lead to recall bias. The findings are context-specific and may not be applicable to other regions or countries. Future research should address these limitations by employing larger, more diverse samples, using stratified random sampling, and incorporating multiple data sources and methodological approaches. The interviewer’s background and the translation process from Chinese to English may have influenced participant responses and nuanced meanings. Future research should address these limitations by employing multiple interviewers with diverse backgrounds and utilizing bilingual research teams to ensure accurate and nuanced translations. Additionally, using larger and more diverse samples will enhance the representativeness and generalizability of the findings, thereby minimizing potential biases. Despite these limitations, the study’s contributions-particularly its actionable recommendations and theoretical extensions—outweigh its constraints. While our study is limited to a specific region, the identified challenges, such as the education-practice gap and workload overload, are likely to be relevant in other areas experiencing similar educational transitions, suggesting that our findings may offer insights for broader application. Addressing these recommendations holistically will improve the transition experience of nursing master’s graduates, optimize their clinical contributions, and ultimately enhance patient care outcomes. Future research should explore regional and longitudinal variations in transition experiences to inform scalable, context-sensitive reforms in nursing education and practice.
Conclusion
This study provides a qualitative exploration of the clinical work challenges faced by Chinese nursing master’s graduates. Key themes identified include professional identity struggles, education-practice gaps, dissatisfaction with salary and career prospects, workload overload, continuous education pressures, and insufficient research support. These findings highlight the multifaceted challenges that nursing master’s graduates encounter during their transition from education to clinical practice. To address these challenges and enhance the professional satisfaction and effectiveness of nursing master’s graduates, we recommend implementing curriculum reforms to align nursing education more closely with clinical demands through increased practical training and mentorship opportunities. Salaries should be adjusted to reflect advanced qualifications and responsibilities, thereby improving job satisfaction. Workload standards should be established to promote work-life balance and mitigate burnout. Structured onboarding programs, including mentorship and support systems, should be provided for new graduates to facilitate a smoother transition to clinical practice. Clear career progression frameworks should be developed to enhance professional development and opportunities for advancement. Additionally, research support should be strengthened through the establishment of mentorship programs and the allocation of resources to help graduates balance clinical and scholarly responsibilities effectively. These measures are crucial for enhancing the professional satisfaction and effectiveness of nursing master’s graduates in clinical practice. Policymakers and hospital administrators should consider these findings when developing strategies to improve nursing education and practice, ultimately contributing to the improvement of patient care outcomes.
Supplementary Information
Below is the link to the electronic supplementary material.
Acknowledgements
The authors thank all the participants who volunteered to participate in this study.
Author contributions
Y.W. was responsible for writing the manuscript and collecting data. W.H. and X.X. played key roles in data processing. J.G. and Q.X. put forward important revision suggestions and made corresponding modifications for this article. All authors contributed to the article and approved the submitted version.
Funding
This work was supported by Major Research Project of Jiangsu Provincial Association for Degrees and Graduate Education (JSSYXHZD2023-1) and Subproject of Jiangsu Provincial Association for Degrees and Graduate Education (JSYXHXM2023-ZYB21). The funding sources had no role to play in the study design, the collection and interpretation of the data, writing of the report, or decision to submit this paper for publication.
Data availability
The de-identified transcripts used for this study are available upon reasonable request to the corresponding author.
Declarations
Ethics approval and consent to participate
The study was reviewed and approved by the Ethics Committee of the Sixth People’s Hospital of Nantong (Ethics approval number: NTLYLL2024028). All methods were performed in accordance with the relevant guidelines and regulations (Declaration of Helsinki). All the participants provided informed consent to participate in the study voluntarily.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Footnotes
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Yanchi Wang and Wei Huang contributed equally to this work.
Contributor Information
Qing Xia, Email: xq.well@163.com.
Jian Gu, Email: gujianntu@163.com.
References
- 1.Persolja M. General nurses’ and nursing technicians’ complexity of activities: cross-sectional study. J Nurs Manag. 2021;29(7):2175–82. [DOI] [PubMed] [Google Scholar]
- 2.Fu X, You L, Liu X, Zheng J, Gubrud-Howe P, Liu J, Li M, Wan L. Developing trends of initial nursing education in China from 2006 to 2017: a descriptive analysis based on national-level data. Nurse Educ Today. 2022;110:105271. [DOI] [PubMed] [Google Scholar]
- 3.Zhang H, Luo D, Lu Y, Zhu H, Zhang G, Li M. Growth and challenges of china’s nursing workforce from 1998 to 2018: A retrospective data analysis. Int J Nurs Stud. 2021;124:104084. [DOI] [PubMed] [Google Scholar]
- 4.Xie C, Li L, Li Y. Wheels stuck in the mud: a qualitative study of experiences of academic burnout in graduate nursing students. Nurse Educ Today. 2024;140:106287. [DOI] [PubMed] [Google Scholar]
- 5.Jiang H, Zhang T, Zhang S, Ma H, Luo Y. Nursing postgraduates learning experience of professional curriculum in china: a qualitative study. Nurs Open. 2024;11(7):e2244. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Ghosh M, Nosaka K, Saunders R, Gallagher O, Towell-Barnard A, Ghosh D, Gent L, Coventry L. Patient perception of involvement in nursing bedside handover: a cross-sectional study. J Adv Nurs. 2025. [DOI] [PMC free article] [PubMed]
- 7.Zhang C, Xu C, Wang R, Han X, Yang G, Liu Y. The learning experiences and career development expectations of Chinese nursing master’s degree students: a qualitative investigation. Nurse Educ Pract. 2024;77:103996. [DOI] [PubMed] [Google Scholar]
- 8.Sutharson PB, Maaskant JM, Eskes AM. The dutch-translated cultural competence assessment scale for nurses: cross-cultural adaptation and validation. Int J Nurs Stud Adv. 2025;8:100303. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Momenyan S, Mousavi SM, Dadkhahtehrani T, Sarvi F, Heidarifar R, Kabiri F, Mohebi E, Koohbor M. Predictive validity and inter-rater reliability of the persian version of full outline of unresponsiveness among unconscious patients with traumatic brain injury in an intensive care unit. Neurocrit Care. 2017;27(2):229–36. [DOI] [PubMed] [Google Scholar]
- 10.Song C, Yao L, Song Y, Liu L. The hotspots and trends of nursing master’s education in china: a bibliometric analysis from 2000 to 2022. BMC Med Educ. 2024;24(1):1082. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Wu X, Hayter M, Lee AJ, Yuan Y, Li S, Bi Y, Zhang L, Cao C, Gong W, Zhang Y. Positive spiritual climate supports transformational leadership as means to reduce nursing burnout and intent to leave. J Nurs Manag. 2020;28(4):804–13. [DOI] [PubMed] [Google Scholar]
- 12.Nour V, Williams AM. Theory becoming alive: the learning transition process of newly graduated nurses in Canada. Can J Nurs Res. 2019;51(1):6–13. [DOI] [PubMed] [Google Scholar]
- 13.Benner P. Educating nurses: a call for radical transformation-how far have we come? J Nurs Educ. 2012;51(4):183–4. [DOI] [PubMed] [Google Scholar]
- 14.Ghorbani A, Mohammadi N, Rooddehghan Z, Bakhshi F, Nasrabadi AN. Transformational leadership in development of transformative education in nursing: a qualitative study. BMC Nurs. 2023;22(1):17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Lan X, Zheng S, Li C, Xu L, Lou Y. Transferring knowledge and skills from an international collaborative nursing educational program to clinical practice: A qualitative study. Nurse Educ Today. 2024;143:106365. [DOI] [PubMed] [Google Scholar]
- 16.Chau JPC, Lo SHS, Lam SKY, Saran R, Thompson DR. Critical elements in nursing graduates’ transition to advanced practice roles and their perceived impact on patient care: an exploratory, descriptive study of graduates’ and their managers’ perceptions. BMC Nurs. 2022;21(1):122. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Garcia D, Kazemitabar M, Bjork E, Daniele T, Mihailovic M, Cloninger KM, Frota MA, Cloninger CR. Nursing students’ personality (Temperament and Character), burnout symptoms, and health and well-being. Int J Nurs Stud Adv. 2024;6:100206. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.An M, Heo S, Hwang YY, Kim J, Lee Y. Factors affecting turnover intention among new graduate nurses: focusing on job stress and sleep disturbance. Healthc (Basel) 2022;10(6). [DOI] [PMC free article] [PubMed]
- 19.Kim SO, Choi YJ. Nursing competency and educational needs for clinical practice of Korean nurses. Nurse Educ Pract. 2019;34:43–7. [DOI] [PubMed] [Google Scholar]
- 20.Afaneh T, Villamor MY, Opinion F, Hassan N, Mihdawi M. Exploring the gap between school of nursing theoretical foundations and clinical practice. J Prof Nurs. 2023;49:158–64. [DOI] [PubMed] [Google Scholar]
- 21.Lee JE, Sim IO. Gap between college education and clinical practice: experience of newly graduated nurses. Nurs Open. 2020;7(1):449–56. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Magi L, Uibu E, Moi AL, Mortensen M, Naustdal K, Polluste K, Lember M, Kangasniemi M. Collaborative learning linking nursing practice and education - interview study with master’s students and teachers. Nurse Educ Today. 2024;139:106261. [DOI] [PubMed] [Google Scholar]
- 23.Xu H, Dong C, Yang Y, Sun H. Developing a professional competence framework for the master of nursing specialist degree program in china: a modified delphi study. Nurse Educ Today. 2022;118:105524. [DOI] [PubMed] [Google Scholar]
- 24.Li S, Wei Z, Shang S, Hou S. Status and development suggestions for the training of master of nursing professional degree graduate students. Chin Nurs Educ. 2024;21(8):962–8. [Google Scholar]
- 25.Li Y, Wang C, Tan W, Jiang Y. The transition to advanced practice nursing: a systematic review of qualitative studies. Int J Nurs Stud. 2023;144:104525. [DOI] [PubMed] [Google Scholar]
- 26.Shoghi M, Sajadi M, Oskuie F, Dehnad A, Borimnejad L. Strategies for bridging the theory-practice gap from the perspective of nursing experts. Heliyon. 2019;5(9):e02503. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Bilgic FS, Bozkurt G. Effect of online infant care training and postpartum counseling based on meleis’ transition theory on mothers’ readiness for care and breastfeeding: a randomized controlled trial. Clin Exp Pediatr. 2024;67(10):521–30. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Hennink MM, Kaiser BN, Marconi VC. Code saturation versus meaning saturation: how many interviews are enough? Qual Health Res. 2017;27(4):591–608. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Moser A, Korstjens I. Series: practical guidance to qualitative research. Part 3: sampling, data collection and analysis. Eur J Gen Pract. 2018;24(1):9–18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Mirzakhani K, Yas A, Khadivzadeh T. Explaining the perception and experiences of breastfeeding in mothers who have a high risk pregnancy: a protocol study. Reprod Health. 2024;21(1):74. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Linder S, Wiggins M. The effects of practice on graduate nursing students’ objective structured clinical examination scores. J Nurs Educ 2025:1–3. [DOI] [PubMed]
- 32.Gautam S, Poudel A, Paudyal K, Prajapati MM. Transition to professional practice: perspectives of new nursing graduates of Nepal. BMC Nurs. 2023;22(1):273. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.John McKitterick D, Peters MDJ, Corsini N, Chiarella M, Eckert M. International nursing students’ and international nursing graduates’ experiences of transition to the nursing workforce: a systematic review of qualitative evidence. Nurse Educ Pract. 2021;55:103147. [DOI] [PubMed] [Google Scholar]
- 34.Douglass B, Stager SL, Shaw K, Hite A, Solecki S, Stanik-Hutt J, Tufts G. Professional identity in nursing: why it is important in graduate education. J Prof Nurs. 2024;52:50–5. [DOI] [PubMed] [Google Scholar]
- 35.Relster M, Nielsen SH, Thrysoe L, Dieperink KB, Nielsen DS, Tolstrup LK. Transition from masters of nursing to clinical practice. Nurse Educ Today. 2023;128:105882. [DOI] [PubMed] [Google Scholar]
- 36.Schwendimann R, Fierz K, Spichiger E, Marcus B, De Geest S. A master of nursing science curriculum revision for the 21st century - a progress report. BMC Med Educ. 2019;19(1):135. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Lonn BB, Hornsten A, Styrke J, Hajdarevic S. Transitioning to the clinical research nurse role - A qualitative descriptive study. J Adv Nurs. 2022;78(11):3817–29. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Cantlay A, Salamanca J, Golaw C, Wolf D, Maas C, Nicholson P. Self-perception of readiness for clinical practice: a survey of accelerated masters program graduate registered nurses. Nurse Educ Pract. 2017;24:34–42. [DOI] [PubMed] [Google Scholar]
- 39.Xiao H, Li S, Su Q, Huang H, Wu L. Construction and practice of the one student with multiple mentors guidance model for master of nursing professional degree graduate students. Nurs Res. 2025;39(3):396–400. [Google Scholar]
- 40.Meng N, Wu P, Lin X, Xia H, Moheds S, Cai W, Du X, You S. Mixed research on the ways to improve the practical innovation ability of master of nursing professional degree graduate students. J Nurs Manag. 2024;24(8):651–6. [Google Scholar]
- 41.Chen J, Zhou Y, Cheng L, Ma Y. Current situation and enlightenment of master of nursing professional degree talent training in Australia. J Nurs. 2024;39(5):70–4. [Google Scholar]
- 42.Mikkonen K, Utsumi M, Tuomikoski AM, Tomietto M, Kaucic BM, Riklikiene O, Vizcaya-Moreno F, Nakaoka A, Yamakawa M, Inoue M, et al. Mentoring of nursing students-A comparative study of Japan and five European countries. Jpn J Nurs Sci. 2022;19(2):e12461. [DOI] [PubMed] [Google Scholar]
- 43.Spiller K, Ossenberg C, Takashima M, Henderson A. Comparable achievement of workplace performance of student and graduate nurses: a quantitative cohort evaluation. Nurse Educ Pract. 2025;82:104205. [DOI] [PubMed] [Google Scholar]
- 44.Scales K. Transforming direct care jobs, reimagining long-term services and supports. J Am Med Dir Assoc. 2022;23(2):207–13. [DOI] [PubMed] [Google Scholar]
- 45.Liu M, Dong Q, Chen D. Current status and influencing factors of occupational success of nursing graduate students in tertiary First-class hospitals. Mil Nurs. 2024;41(10):44–7. [Google Scholar]
- 46.Ganann R, Weeres A, Lam A, Chung H, Valaitis R. Optimization of home care nurses in canada: a scoping review. Health Soc Care Community. 2019;27(5):e604–21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Jin T, Zhou Y, Zhang L. Job stressors and burnout among clinical nurses: a moderated mediation model of need for recovery and career calling. BMC Nurs. 2023;22(1):388. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Talebiazar N, Anzali BC, Abbasi M, Azizi N, Goli R, Faraji N, Bagheri M, Amiri N, Kazemi S. Does mindfulness-based stress reduction training have an impact on the occupational burnout and stress experienced by nurses? A randomized controlled trial. Int Arch Occup Environ Health. 2025;98(1):1–11. [DOI] [PubMed] [Google Scholar]
- 49.Ocampo FA, McIntyre BG, Massey D, Saunders R. Nursing student reflections on a research internship: a reflective discussion following the gibbs’ reflective cycle. Nurse Educ Today. 2025;145:106481. [DOI] [PubMed] [Google Scholar]
- 50.Mo Y, Li H, Tian L, Sui W, Meng H, Li C, Jing X. Establishment and practice of an advanced nursing practice workshop. Chin J Nurs. 2020;55(6):911–5. [Google Scholar]
- 51.Mijares AH, Radovich P. Structured mentorship and the nursing clinical ladder. Clin Nurse Spec. 2020;34(6):276–81. [DOI] [PubMed] [Google Scholar]
- 52.Xiang D, Ge S, Zhang Z, Twumwaah Budu J, Mei Y. Relationship among clinical practice environment, creative self-efficacy, achievement motivation, and innovative behavior in nursing students: A cross-sectional study. Nurse Educ Today. 2023;120:105656. [DOI] [PubMed] [Google Scholar]
- 53.Pool IA, van Zundert H, Ten Cate O. Facilitating flexibility in postgraduate nursing education through entrustable professional activities to address nursing shortages and career prospects. Int Nurs Rev. 2024;71(3):419–23. [DOI] [PubMed] [Google Scholar]
- 54.Farsi Z, Nasiri M, Sajadi SA, Khavasi M. Comparison of iran’s nursing education with developed and developing countries: a review on descriptive-comparative studies. BMC Nurs. 2022;21(1):105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Ohno S, Chen Y, Sakamaki H, Matsumaru N, Tsukamoto K. Humanistic and economic burden among caregivers of patients with cancer in Japan. J Med Econ. 2020;23(1):17–27. [DOI] [PubMed] [Google Scholar]
- 56.See ECW, Koh SSL, Baladram S, Shorey S. Role transition of newly graduated nurses from nursing students to registered nurses: a qualitative systematic review. Nurse Educ Today. 2023;121:105702. [DOI] [PubMed] [Google Scholar]
- 57.Nkowane AM, Ferguson SL. The world health organization launches the 2016–2020 global strategic directions for strengthening nursing and midwifery. Nurs Econ. 2016;34(4):206–7. [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The de-identified transcripts used for this study are available upon reasonable request to the corresponding author.