Abstract
Purpose
Treatment strategies for early and locally advanced rectal cancer are evolving, particularly with the increasing use of non-operative management and multidisciplinary decision-making.
The aim of this study is to establish an expert-based consensus on the preferred treatment strategies for early and locally advanced rectal cancer.
Methods
A 12-member steering committee was established to conduct a modified Delphi consensus process on rectal cancer management. The committee performed a systematic literature review (2014–2024) to inform survey development. A 49-question survey, including open-ended and multiple-choice items, was developed and refined. A panel of 44 colorectal surgery experts was selected based on academic contributions, and two Delphi rounds were conducted anonymously. Consensus was defined as ≥ 70% agreement. Based on panel responses, 29 consensus statements were formulated.
Results
The panel reached consensus on the importance of multidisciplinary evaluation and surgical expertise in total mesorectal excision. Structured MRI reporting was recommended. Total neoadjuvant therapy was preferred for high-risk tumors. Non-operative management was recommended in cases of clinical complete response, with defined surveillance strategies. The role of biopsy in near-complete responders was also addressed.
Conclusions
This international consensus provides structured guidance on the management of rectal cancer, emphasizing multidisciplinary planning, the role of total neoadjuvant therapy in organ preservation, and rigorous surveillance protocols in non-operative management. These recommendations aim to standardize care and support evidence-informed clinical decision-making.
Keywords: Rectal cancer, Non-operative management, Total neoadjuvant therapy, Multidisciplinary team, Clinical complete response, Consensus
Introduction
The Turkish Society of Colon and Rectal Surgery (TSCRS) is committed to advancing education and research in colorectal surgery, contributing to the establishment of patient care standards for colorectal diseases, shaping national health policies, and ensuring effective prevention and treatment strategies for colorectal diseases. Consistent with these objectives, TSCRS proactively develops benchmarks to standardize colorectal surgical practices.
The management of rectal cancer, particularly in its early and locally advanced stages, has undergone significant evolution over recent years. This evolution is largely driven by advancements in diagnostic imaging, surgical techniques, and the integration of multidisciplinary treatment approaches. Traditionally, the standard treatment model for rectal cancer has been radical surgery. However, this approach often results in high rates of permanent stomas and a broad spectrum of morbidities, significantly impacting patients’ quality of life [1, 2]. In response to these challenges, the management strategies have evolved to incorporate neoadjuvant chemoradiotherapy, shifting the focus towards organ-preservation strategies that offer both surgical and non-surgical options for the curative treatment of rectal cancer [1, 3].
While the introduction of local excision has provided an alternative management option for early rectal cancer, concerns about local and nodal recurrence persist [4, 5]. Local excision is deemed an appropriate curative-intent treatment for highly selected patients with cT1N0 rectal cancer who exhibit favorable clinical and histological features. For patients with more advanced cT disease who are medically unfit for radical surgery, transanal excision may be considered. Although local excision minimizes operative risks and functional sequelae, it does not sufficiently remove or pathologically stage the mesorectal lymph nodes, underscoring the importance of accurate preoperative staging and meticulous patient selection [6].
The role of multidisciplinary teams (MDTs) in rectal cancer management is increasingly crucial. MDT discussions can enhance preoperative clinical staging, modify and individualize multimodal treatment plans, address the technical aspects of surgery, and review pathologic staging. These teams have been shown to improve patient adherence to treatment protocols and contribute to enhanced survival outcomes [7]. Despite these benefits, further studies are needed to conclusively demonstrate the potential impact of MDT involvement on disease-free and overall survival [8–10].
Given the rapidly evolving landscape of rectal cancer management, there is a clear need for a comprehensive evaluation of current strategies. This Delphi study aims to establish consensus standards guided by current literature and expert opinion. By streamlining clinical practice and reducing variability in treatment strategies, this study not only provides guidance for clinical decision-making but also contributes to harmonizing therapeutic approaches in a field where practice remains heterogeneous.
Materials and methods
Establishment of steering committee
A steering committee of 12 colorectal surgeons was established to oversee the Delphi process. Responsibilities included the selection of expert panelists, a systematic literature review, survey development, data analysis, and drafting of consensus statements. To maintain neutrality, steering committee members did not participate in voting.
Literature review
A systematic PubMed search identified original articles, reviews, and meta-analyses on rectal cancer management published between January 2014 and January 2024. Search strategy and inclusion criteria are summarized in Table 1. Insights from this review informed the initial survey.
Table 1.
The search strategy summary
| Items | Specification |
|---|---|
| Date of search | 2024/03/01 |
| Databases and other sources searched | PubMed |
| Search terms used |
“Rectal cancer” [MeSH] AND “treatment” [MeSH] “Rectal cancer” [MeSH] AND “neoadjuvant” [MeSH] “Rectal cancer” [MeSH] AND “non-operative management” [MeSH] “Rectal cancer” [MeSH] AND “total neoadjuvant therapy (TNT),” [MeSH] “Rectal cancer” [MeSH] AND “consolidation” [MeSH] “Rectal cancer” [MeSH] AND “induction” [MeSH] “Rectal cancer” [MeSH] AND “non-operative management” [MeSH] “Rectal cancer” [MeSH] AND “clinical complete response (cCR)” [MeSH] “Rectal cancer” [MeSH] AND “pathologic complete response (pCR)” [MeSH] “Rectal cancer” [MeSH] AND “organ preservation” [MeSH] “Rectal cancer” [MeSH] AND “watch-and-wait” [MeSH] “Rectal cancer” [MeSH] AND “endoscopic biopsy” [MeSH] “Rectal cancer” [MeSH] AND “taTME” [MeSH] “Rectal cancer” [MeSH] AND “ctDNA” [MeSH] “Rectal cancer” [MeSH] AND “lateral pelvic lymph node dissection” [MeSH] “Rectal cancer” [MeSH] AND “immunotherapy” [MeSH] |
| Timeframe | 2014–2024 |
| Inclusion and exclusion criteria |
Focus was placed on original papers, reviews, and meta-analyses in English about management of rectal cancer The inclusion criteria encompassed full-text articles involving adults aged 18 years. Publications with relative low credibility and non-English publications were excluded |
| Selection process | It was conducted independently by the executive team members of the study; all members discussed the literature selection and obtained the consensus |
| Any additional considerations, if applicable | None |
Data extraction and survey development
Based on the insights gathered from the literature, a comprehensive survey consisting of 49 questions was developed. This survey included six open-ended questions, with the remaining questions formatted as multiple-choice or drop-down selections. The steering committee refined the survey through several meetings to ensure clarity, completeness, and relevance before distributing it to the expert panel.
Identification of experts and Delphi rounds
For participation in the Delphi panel, general surgeons with recognized expertise and significant academic contributions to the field of colorectal surgery were identified. Experts were selected based on their published research in relevant medical journals. Invitations were extended to 74 surgeons from diverse national and international regions to achieve comprehensive representation; of these, 44 experts agreed to participate. Turkish experts were selected among members of the Turkish Society of Colon and Rectal Surgery. The final panel consisted of experts from 12 countries, predominantly Turkey (n = 30), but also including the USA (n = 3), Switzerland (n = 2), and single participants from Malaysia, Spain, the UK, Russia, Lithuania, Brazil, Germany, Korea, and the Netherlands. While Turkey was the most represented country, the panel still reflected a range of international perspectives.
Consensus was developed through a structured Delphi methodology, utilizing open-ended and multiple-choice questions alongside a 3-point Likert scale (1: agree, 2: disagree, 3: undecided). The first Delphi round was conducted anonymously between August 23, 2024, and September 16, 2024. Responses and feedback from the experts were reviewed to revise the questions for the second round. Both the initial and revised questionnaires, along with their response rates, are provided in Table 2.
Table 2.
Questions and responses from round 1 and round 2
| Question | Round 1 | Round 2 |
|---|---|---|
| Q1. A multidisciplinary tumor board is essential for the management of rectal cancer | Agree: 97.5 | NA |
| Q2. Which disciplines should be included in the multidisciplinary tumor board for managing rectal cancer? (Select all that apply) |
Colorectal surgeon: 100% Medical oncologist: 98% Radiation oncologist: 98% Radiologist: 95% Pathologist: 98% |
NA |
| Q3. Which discipline do you believe should lead the multidisciplinary tumor board and ensure effective interdisciplinary communication? | E | NA |
| Q4. For lower complication rates and better oncological outcomes in rectal cancer treatment, the annual volume of procedures at the center should be as follows: | No consensus | Surgeons performing at least 20 rectal cancer cases per year and centers treating at least 40 rectal cancer cases per year: 70% |
| Q5. Which should be used in the staging of rectal cancer? (Select all that apply) | R |
Rectum specific MRI: 91% Abdomen CT: 70% Thorax CT: 98% |
| Q6. Which method do you use to define the level of the tumor in the rectum? | R: How can you determine the height of rectal cancers, excluding distal lesions that can be detected by digital rectal examination? | MRI: 70% |
| Q7. Which method do you prefer for bowel cleansing before elective rectal cancer surgery? | No consensus | No consensus |
| Q8. In the local staging of rectal cancer with MRI, select the essential information that must be included in the imaging technique and reporting |
• 3-plane high-resolution T2-weighted sequences are crucial: 78% • A routine protocol should include a diffusion-weighted sequence: 78% • Morphology of the tumour, its circumferential location within the rectal wall, and the height of the tumour measured from the anal verge should be reported: 93% • The mesorectal fascia (MRF), T stage, and suspected lymph node involvement should be reported: 100% • Presence of T2 hyperintense mucinous content should be specified: 73% • Relation of tumor with 3 key structures (internal sphincter, intersphincteric space, external sphincter) should be reported: 88% • EMVI should be reported: 90% |
NA |
| Q9. In which cases do you prefer partial mesorectal excision?(Select all that apply) | For upper rectum tumors: 81% | NA |
| Q10. In which patients who have undergone sphincter-preserving surgery do you prefer to apply a diverting ileostomy/colostomy? (Select all that apply) | No consensus | No consensus |
| Q11. Which method do you primarily prefer for the treatment of a clinical T1N0M0 rectal tumor located in the lower rectum? (Select all that apply) | R: Which method do you primarily prefer for the treatment of a cT1N0M0 rectal cancer located in the lower rectum? (Patient fit for surgery) |
Radical surgery: 4.5% Local excision: 95.5% -Conventional transanal local excision: 29.6% -TES (TEM/TEO/TAMIS): 52.3% -ESD: 13.6% |
| Q12. Which method do you primarily prefer for the treatment of a clinical T1N0M0 rectal tumor located in the mid rectum? (Select all that apply) | R: Which method do you primarily prefer for the treatment of a cT1N0M0 rectal cancer located in the mid rectum? (Patient fit for surgery) |
Radical surgery: 11.4% Local excision: 88.6% -Conventional transanal local excision: 0% -TES (TEM/TEO/TAMIS): 72.7% -ESD: 15.9% |
| Q13. Which method do you primarily prefer for the treatment of a clinical T1N0M0 rectal tumor located in the upper rectum? (Select all that apply) | R. Which method do you primarily prefer for the treatment of a cT1N0M0 rectal cancer located in the upper rectum? (Patient fit for surgery) |
Radical surgery: 34.9% Local excision: 65.1% -TES (TEM/TEO/TAMIS): 37.2% -ESD: 27.9% |
| Q14. If you plan to perform endoscopic local excision for cT1N0M0 rectal cancers, which method would you prefer? (Patient fit for surgery) |
TES (TEM/TEO/TAMIS): 85.4% ESD: 34.1% Options are revised for round 2 |
TEM-TEO: 16.7% TAMIS: 54.8% ESD: 23.8% I do not perform endoscopic local excision: 4.7% |
| Q15. Which tumors located in the rectum are suitable for curative local excision? (Select all that apply) |
No consensus Lesions occupying less than 1/3 of the lumen: 61% Lesions occupying less than 1/2 of the lumen: 22% Lesions occupying less than 2/3 of the lumen: 2.4% It doesn’t matter how much of the lumen is occupied: 19.5% Lesions smaller than 3 cm: 41.5% Lesions smaller than 5 cm: 17% The size of the lesion is not important: 22% Mobile lesions: 56.1% |
Less than 1/3 of the lumen: 59% < 3 cm: 52.3% Mobile lesions: 74.4% |
| Q16. Which histopathological features affect your decision for local excision in clinical T1N0 rectal tumors? (Select all that apply) |
Depth of submucosal invasion: 95% Tumor differentiation: 90% Perineural invasion: 81% Tumor budding: 81% Lymphovascular invasion: 93% |
NA |
| Q17. In clinical T1NOMO rectal tumors with positive surgical margins after endoscopic local excision/polypectomy or surgical margins closer than 1 mm but without other high-risk factors (High-risk factors: sm2-3 submucosal invasion depth, poor differentiation, perineural invasion, tumor budding, lymphovascular invasion), which approach do you follow? | R. For patients with pT1 cN0M0 rectal cancer and surgical margins closer than 1 mm after endoscopic local excision/polypectomy but without high-risk factors, which treatment approach do you prefer? (Assuming the patient is fit for surgery and sphincter-preserving surgery is possible) |
TME: 13.95% ESD (Scar excision): 13.95% TES or conventional full-thickness local re-excision: 39.5% Radiotherapy only: 7% Observation only: 25.6% |
| Q18. In clinical T1NOMO rectal tumors with positive surgical margins after endoscopic local excision/polypectomy or surgical margins closer than 1 mm but with other high-risk factors (High-risk factors: sm2-3 submucosal invasion depth, poor differentiation, perineural invasion, tumor budding, lymphovascular invasion), which approach do you follow? | R. For patients with pT1 cN0M0 rectal cancer and surgical margins closer than 1 mm after endoscopic local excision/polypectomy with high-risk factors, which treatment approach do you prefer? (Assuming the patient is fit for surgery and sphincter-preserving surgery is possible) |
TME: 61.4% ESD (scar excision): 0% TES or conventional full-thickness local re-excision: 22.8% Radiotherapy only: 15.9% Observation only: 0% |
| Q19. In clinical T1N0M0 rectal tumors with clear surgical margins after local excision but containing histopathological high-risk factors (High-risk factors: sm2-3 submucosal invasion depth, poor differentiation, perineural invasion, tumor budding, lymphovascular invasion), which approach do you follow? | R. For patients with pT1 cN0M0 rectal cancer and surgical margins closer than 1 mm after endoscopic local excision/polypectomy, but without high-risk factors, which treatment approach do you prefer? (Assuming the patient is fit for surgery and require APR if surgical treatment is to be preferred) |
APR:4.5% ESD (scar excision): 9.1% TES or conventional full-thickness local re-excision: 43.2% Radiotherapy only: 20.5% Observation only: 22.7% |
| Q20. In clinical T1N0M0 rectal tumors with clear surgical margins after local excision but not containing histopathological high-risk factors (High-risk factors: sm2-3 submucosal invasion depth, poor differentiation, perineural invasion, tumor budding, lymphovascular invasion), which approach do you follow? | R. For patients with pT1 cN0M0 rectal cancer and surgical margins closer than 1 mm after endoscopic local excision/polypectomy, with high-risk factors, which treatment approach do you prefer? (Assuming the patient is fit for surgery and require APR if surgical treatment is to be preferred) |
APR: 25% ESD (scar excision): 0% TES or conventional full-thickness local re-excision: 31.8% Radiotherapy only: 40.9% Observation only: 2.3% |
| Q21. How often do you think endoscopic assessment should be performed to evaluate the risk of recurrence after local excision of a T1 rectal tumor? | Open ended | |
| Q22. How long do you wait for surgery after standard neoadjuvant therapy? | R: In your opinion, how long should a patient typically wait for surgery after completing standard neoadjuvant therapy? (after completing radiotherapy) |
< 8 weeks: 2.3% 8–12 weeks: 47.7% > 12 weeks: 50% |
| Q23. What factors influence your decision to choose TNT? (Select all that apply) |
Pathological mesorectal lymph nodes in preoperative evaluation: 57% T4: 69% T3a/b: 19% T3c/d: 62% LARC located in the lower rectum: 81% LARC located in the mid rectum: 50% LARC located in the upper rectum: 12% CRM < 1 mm: 69% EMVI + : 67% Sphincter invasion: 74% Suspicion/invasion of levator muscle: 74% Enlarged lateral lymph nodes: 69% Presence of local symptoms (obstruction/bleeding): 12% ECOG performance scale: 24% |
Pathological mesorectal lymph nodes in preoperative evaluation: 59% T4: 84% T3a/b: 23% T3c/d: 66% LARC located in the mid rectum: 48% LARC located in the upper rectum:13.6% CRM < 1 mm: 81.8% EMVI + : 81.8% Enlarged lateral lymph nodes: 79.6% Presence of local symptoms (obstruction/bleeding): 9% ECOG performance scale: 18.2% |
| Q24. What sequence do you prefer for TNT? |
Long-term chemoradiotherapy + consolidation chemotherapy: 48.8% Short-term radiotherapy + consolidation chemotherapy: 4.9% Induction chemotherapy + long-term chemoradiotherapy: 9.8% Induction chemotherapy + short-term radiotherapy: 2.4% Induction chemotherapy + long-term chemoradiotherapy + chemotherapy: 31.7% Induction chemotherapy + short-term radiotherapy + chemotherapy: 2.4% Chemotherapy only: 0.00% |
Long-term chemoradiotherapy + consolidation chemotherapy: 81.8% Short-term radiotherapy + consolidation chemotherapy: 4.6% Induction chemotherapy + long-term chemoradiotherapy: 6.8% Induction chemotherapy + short-term radiotherapy: 0% Induction chemotherapy + long-term chemoradiotherapy + chemotherapy: 20.5% Induction chemotherapy + short-term radiotherapy + chemotherapy: 2.3% |
| Q25. In which cases should induction chemotherapy be preferred in TNT? (Select all that apply) | R. In which cases would you prefer induction chemotherapy followed by chemoradiotherapy in TNT? (Select all that apply) |
Pathological mesorectal lymph node in preoperative evaluation: 43.2% T4, large tumors: 36.4% T3a/b: 11.4% T3c/d: 22.7% LARC located in the lower rectum: 40.9% LARC located in the mid rectum: 22.7% LARC located in the upper rectum: 2.3% CRM < 1 mm: 34% EMVI + : 56.8% Sphincter invasion: 29.6% Suspicion/invasion of levator muscles: 31.8% Enlarged lateral lymph nodes: 50% Presence of local symptoms (obstruction/bleeding): 6.8% ECOG performance scale:4.6% None: 20.5% |
| Q26. In which cases should consolidation chemotherapy be preferred in TNT? (Select all that apply) | R. In which cases would you prefer chemoradiotherapy followed by consolidation chemotherapy in TNT? (Select all that apply) |
Pathological mesorectal lymph node in preoperative evaluation: 51.2% T4, large tumors: 79% T3a/b: 27.9% T3c/d: 58.1% LARC located in the lower rectum: 72% LARC located in the mid rectum: 53.5% LARC located in the upper rectum: 11.6% CRM < 1 mm: 74.4% EMVI + : 48.9% Sphincter invasion: 88.4% Suspicion/invasion of levator muscles: 83.7% Enlarged lateral lymph nodes: 46.5% Presence of local symptoms (obstruction/bleeding): 18.6% ECOG performance scale: 9.3% |
| Q27. Which criteria do you consider when deciding on a complete clinical response? |
Sao Paulo (Habr-Gama et al. Ann Surg 2019): 12.8% Amsterdam/Maastricht (Maas et al. JCO 2011): 2.6% MSKCC (Smith et al. JAMA Oncol 2019): 28.2% ESMO guidelines (Glynne-Jones et al. Ann Oncol 2017): 15% NCCN guidelines 2020: 41% |
E |
| Q28. When do you assess the treatment response (interim evaluation) after starting TNT? | R. Do you conduct interval evaluations during TNT? |
Yes: 83.7% No: 11.6% Undecided: 4.7% |
| Q29. Which of the following do you use to assess the response? (Select all that apply) |
Digital rectal examination: 88.4% Endoscopy: 93% MRI: 97.7% CT: 23.3% PET: 32.6% |
NA |
| Q30. How many weeks after completing TNT treatment should a complete clinical response assessment be performed? | R1. How many weeks after completing TNT should a complete clinical response assessment be performed for patients who started with induction chemotherapy? |
4–6 weeks: 25.6% 7–8 weeks: 18.6% 9–12 weeks: 32.6% > 12 weeks: 23.2% |
| R2. How many weeks after completing TNT should a complete clinical response assessment be performed for patients who started with chemoradio therapy? |
4–6 weeks: 31.8% 7–8 weeks: 31.8% 9–12 weeks: 11.4% > 12 weeks: 25% |
|
| Q31. What is your approach when a near-complete clinical response is obtained after neoadjuvant therapy? | R1. What is your approach when a near-complete clinical response is achieved after neoadjuvant therapy? |
Radical surgery (TME): 36.4% Additional chemotherapy: 4.6% Wait: 59.1% |
| R2. If you choose to wait, how long do you typically wait when a near-complete clinical response is achieved after neoadjuvant therapy? |
4 weeks: 37.1% 5–6 weeks: 11.4% 7–8 weeks: 22.9% 9–12 weeks: 17.2% > 12 weeks: 11.4% |
|
| Q32. Who should perform the endoscopy in the assessment of complete clinical response after TNT? (Select all that apply) |
General surgeon: 2.4% Colorectal surgeon: 95% Gastroenterologist: 19.1% |
E |
| Q33. If you think there is a near-complete clinical response endoscopically, would you take a biopsy? |
Yes: 44.2% No: 55.8% |
Yes: 29.5% No: 70.5% |
| Q34. Biopsy is necessary in the assessment of complete clinical response for NOM |
Agree: 18.6% Undecided: 7% Disagree: 74.4% |
NA |
| Q35. How long do you wait for surgery after completing TNT treatment? | R1. How many weeks after completing TNT should surgery be performed for patients who started with induction chemotherapy? |
< 8 weeks: 15.9% 8–12 weeks: 45.5% > 12 weeks: 38.6% |
| R2. How many weeks after completing TNT should surgery be performed for patients who started with chemoradiotherapy? |
< 8 weeks: 25% 8–12 weeks: 40.9% > 12 weeks: 34.1% |
|
| Q36. Which methods do you use in the follow-up of patients under non-operative management? (Select all that apply) |
CEA: 88.4% Digital rectal examination: 93% Endoscopy: 93% MRI: 97.7% CT: 48.8% PET/CT: 32.6% ctDNA: 7% Endorectal USG: 13.9% |
NA |
| Q37. If re-growth occurs in a patient being followed with NOM, what would be your choice? |
Local excision: 2.4% Radical surgery: 97.6% Administer chemotherapy: 0% |
NA |
| Q38. Do you use defined protocols in the follow-up of NOM patients? Do you have any additional suggestions? | Open ended | E |
| Q39. In your opinion, what are the potential short- and long-term risks associated with NOM? (Select all that apply) |
Local recurrence: 74.4% Distant metastasis: 81.4% Functional impairments secondary to radiotherapy: 58% Second primary malignancies secondary to radiotherapy: 41.9% Psychological impact: 41.9% Other (please specify): 16.3% |
Local recurrence: 81.8% Functional impairments secondary to radiotherapy: 55% Second primary malignancies secondary to radiotherapy: 31.8% Psychological impact: 20.5% None of the above: 2.3% |
| Q40. What are your expectations for patients followed with NOM? (Select all that apply) |
Higher sphincter preservation rates: 81% Local recurrence comparable to surgery: 70.5% Survival comparable to surgery: 83.3% Satisfactory quality of life: 83.3% Other (please specify): 7.1% |
NA |
| Q41. What do you believe are the barriers and challenges to the successful implementation of NOM in patients being followed with this approach? (Select all that apply) |
Lack of standardized protocols: 67.4% Patient or doctor reluctance: 55.8% Patient adherence to treatment: 53.5% Patient adherence to follow-up: 76.7% Limited access to imaging methods: 55.8% Economic difficulties: 44.2% Medico-legal concerns: 53.5% Other (please specify): 13.9% |
Lack of standardized protocols: 79.6% Patient or doctor reluctance: 52.3% Patient adherence to treatment: 59% Limited access to imaging methods: 45.5% Economic difficulties: 34% Medico-legal concerns: 27.3% |
| Q42. For how many years should a patient who has achieved a complete clinical response after TNT and is being followed with a NOM protocol be monitored? | Open ended |
1–3 years: 4.5% 3–5 years: 25% 5–10 years: 50% Life-long: 20.5% |
| Q43. What do you do when a patient who has achieved a complete clinical response after TNT and is followed with a NOM protocol does not comply with the follow-up protocol? | Open ended | E |
| Q44. In light of the current literature, should TNT and NOM be recommended for all LARC patients? | Open ended |
Yes: 36.4% No: 54.6% Undecided: 9% |
| Q45. Can a patient who has received Standard CRT for LARC but has a complete response in preoperative response evaluation be switched to a NOM protocol? What should the recommended protocol be? | Open ended | E |
| Q46. Which findings on preoperative MRI should be considered metastatic in lateral pelvic lymph nodes? |
MRI assessment of lateral pelvic lymph node is limited in the setting of early T1/2 tumors as the likelihood of lateral nodal spread in T1/2 tumors is very low: 32.6% Tumors with lateral lymph node involved are considered locally advanced rectal cancers: 46.5% The presence or absence of lateral lymph nodes should always be reported, along with the long axis (in mm), and in which anatomical compartment the lateral lymph node is situated: 67.4% For internal iliac and obturator lymph nodes, a size of > 7 mm in the short axis is required for these nodes to be considered suspicious for metastastic: 76.7% Size criteria on preoperative MRI for lateral pelvic lymph nodes are applicable in the setting of T3/4 tumors located < 8 cm from the anal verge: 44.2% Unlike mesorectal nodal assessment, morphologic features are not typically used to determine lateral nodal involvement; rather, size criteria alone are assessed: 14% Local recurrence is more likely to occur in oval, long stretched nodes: 18.6% |
E |
| Q47. If pathological lateral pelvic lymph nodes regress after neoadjuvant therapy, do you perform dissection? |
Yes: 11.9% No: 88.1% |
NA |
| Q48. If pathological lateral pelvic lymph nodes persist after neoadjuvant therapy, do you perform dissection? |
No: 7.7% Yes: 92.3% |
NA |
| Q49. During lateral lymph node dissection, which of the following contributes to a safe and adequate dissection? (Select all that apply) |
Fluorescein angiography in indocyanine: 34.2% Infrared imaging: 0% Use of methylene blue: 0% Creation of pelvic modeling with a 3D printer: 0% Laparoscopic method: 51.2% Robotic method: 63.4% Open surgery: 43.9% Extraperitoneal approach: 12.2% None of above: 4.9% |
E |
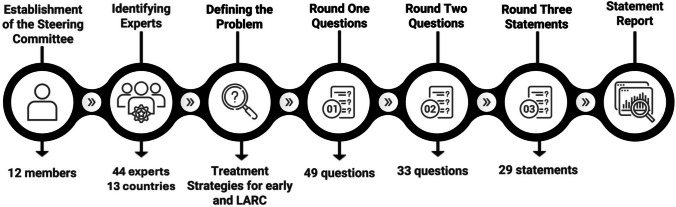
In the first round, a consensus was defined as achieving 70% or greater agreement among respondents. Expert comments and responses, particularly to open-ended questions, were analyzed individually to inform the development of the second round of questions. The second round took place between October 9, 2024, and October 24, 2024. Based on these responses, 29 consensus statements were developed, each receiving at least 70% agreement from panel members (Table 3). Following this second round, the Delphi process was completed (Fig. 1). These consensus thresholds align with previously published Delphi studies, where consensus is typically defined as exceeding 70% to 80% [11, 12].
Table 3.
Questions and responses from round 3
| Round 3 questionnaire | Agreement |
|---|---|
| Q1. For the effective treatment of rectal cancer, it is advised to engage in a collaborative approach involving a multidisciplinary team (MDT) for tumor board discussions. The MDT should include specialists in colorectal surgery, radiology, medical oncology, radiation oncology, and pathology |
Agree: 97.5% Disagree: 2.5% Undecided: 0% |
| Q2. The ideal annual volume of procedures at a center to ensure lower complication rates and better outcomes should involve surgeons performing at least 20 rectal cancer cases per year and centers treating at least 40 rectal cancer cases per year |
Agree: 94.9% Disagree: 0% Undecided: 5.1% |
| Q3. For clinical staging of rectal cancer, rectum-specific MRI and thoraco-abdominal CT scan should be performed |
Agree: 95.00% Disagree: 5% Undecided: 0% |
| Q4. MRI ± rigid rectoscopy should be used to assess the height of rectal cancers if the tumor is beyond the reach of a digital examination |
Agree: 92.5% Disagree: 5% Undecided: 2.5% |
| Q5. Mechanical bowel preparation and preoperative oral antibiotics may be preferred before elective rectal cancer surgery |
Agree: 87.5% Disagree: 7.5% Undecided: 5% |
| Q6. Structured MRI reporting increases diagnostic accuracy, optimizes treatment planning, provides inter-institutional standardization, and improves communication between multidisciplinary teams |
Agree: 100% Disagree: 0% Undecided: 0% |
| Q7. Partial mesorectal excision is recommended for surgical removal of tumors located only in the upper part of the rectum |
Agree: 87.5% Disagree: 12.5% Undecided: 0% |
| Q8. Local excision (endoscopic and conventional) should be preferred treatment for cT1N0M0 rectal cancers |
Agree: 82.5% Disagree: 12.5% Undecided: 5% |
| Q9. For a local excision of a rectal tumor mobility is essential, however tumor diameter and extention to the lumen are less critical |
Agree: 70% Disagree: 25% Undecided: 5% |
| Q10. After local excision with clear margins for pT1 cN0M0 rectal cancer, the following histopathological features (the depth of submucosal invasion, tumor differentiation, perineural invasion, tumor budding, and lymphovascular invasion) determine the need for additional treatment |
Agree: 92.5% Disagree: 5% Undecided: 2.5% |
| Q11. For patients with pT1 cN0M0 rectal cancer and surgical margins less than 1 mm after local excision or polypectomy, radical surgery (TME) is recommended, if high-risk factors are present and sphincter-sparing surgery is feasible. However, for patients without high-risk factors or those requiring APR for radical surgery, alternative treatment methods may be considered over radical surgery |
Agree: 85% Disagree: 7.5% Undecided: 7.5% |
| Q12. Patients receiving standard neoadjuvant therapy generally advised to wait at least 8 weeks after completing radiotherapy before proceeding with surgery |
Agree: 97.5% Disagree: 0% Undecided: 2.5% |
| Q13. TNT is recommended for rectal adenocarcinoma located in the lower rectum or in cases with high-risk factors, such as T4 tumors, a circumferential resection margin (CRM) of less than 1 mm, positive extramural vascular invasion (EMVI +), pathological lateral pelvic lymph nodes, sphincter involvement, or levator muscle invasion |
Agree: 97.5% Disagree: 2.5% Undecided: 0% |
| Q14. Long-course chemoradiotherapy followed by consolidation chemotherapy may be the preferred approach in TNT for the treatment of locally advanced rectal cancer |
Agree: 87.5% Disagree: 10% Undecided: 2.5% |
| Q15. Interval evaluations should be conducted during the course of TNT |
Agree: 89.7% Disagree: 7.7% Undecided: 2.6% |
| Q16. The response to TNT should be evaluated by using digital rectal examination, rectum-specific MRI, and endoscopy |
Agree: 100% Disagree: 0% Undecided: 0% |
| Q17. Clinical response assessment should be conducted 6–8 weeks after completing TNT |
Agree: 87.5% Disagree: 10% Undecided: 2.5% |
| Q18. If a near-complete clinical response is achieved after TNT, an additional wait for 4 to 8 weeks may be considered for the reassessment of the complete response |
Agree: 85% Disagree: 10% Undecided: 5% |
| Q19. Biopsy is not recommended for patients with a near-complete clinical response |
Agree: 82.5% Disagree: 7.5% Undecided: 10% |
| Q20. The interval between the completion of TNT and surgery should be at least 8 weeks |
Agree: 82.5% Disagree: 10% Undecided: 7.5% |
| Q21. For patients undergoing non-operative management the follow-up period should be more than 5 years |
Agree: 70% Disagree: 17.5% Undecided: 12.5% |
| Q22. For patients with tumor regrowth radical surgery should be preferred |
Agree: 92.5% Disagree: 7.5% Undecided: 0% |
| Q23. Nonoperative management should only be recommended for tumors located in the distal rectum |
Agree: 52.5% Disagree: 42.5% Undecided: 5% |
| Q24. Local regrowth and distant metastasis are main concerns for non-operative management |
Agree: 95% Disagree: 5% Undecided: 0% |
| Q25. To implement a safe nonoperative management program standardized treatment protocols should be established |
Agree: 97.5% Disagree: 2.5% Undecided: 0% |
| Q26. Nonoperative management prioritize achieving higher organ preservation rates, comparable local recurrence and survival rates, and better quality of life to patients undergoing resection |
Agree: 92.5% Disagree: 7.5% Undecided: 0% |
| Q27. If pathological lateral pelvic lymph nodes persist after neoadjuvant therapy, lateral pelvic lymph node dissection should be recommended |
Agree: 97.5% Disagree: 0% Undecided: 2.5% |
| Q28. If pathological lymph nodes regress after neoadjuvant therapy, lateral pelvic lymph node dissection may be considered unnecessary |
Agree: 82.5% Disagree: 15% Undecided: 2.5% |
| Q29. NOM after TNT is not universally recommended for all patients with locally advanced rectal cancer |
Agree: 80% Disagree: 12.5% Undecided: 7.5% |
Fig. 1.
Methodology of the study
Consensus statement recommendations
Role of MDT
In the management of rectal cancer, the multidisciplinary team plays a crucial role, involving collaboration among colorectal surgery, radiology, pathology, medical oncology, radiation oncology, and additional relevant specialties [6]. Several studies have reported that implementing an MDT approach can lead to improved patient adherence to treatment protocols and contribute to survival outcome rates [13]. Although it is generally assumed by clinicians that MDT decisions provide better accuracy and benefit to patients, there remains a need for further research to conclusively demonstrate the direct impact of MDTs on both short- and long-term patient outcomes [6–8, 13, 14].
The expert panel reached a consensus emphasizing that an MDT approach is essential for tumor board discussions. The MDT should include, at a minimum, colorectal surgeons, radiologists, medical and radiation oncologists, and pathologists.
Impact of surgical volume and experience
In the management of rectal cancer, there is no universally accepted annual case volume threshold for achieving better outcomes. Certain studies indicate that centers performing a minimum of 20–30 rectal cancer surgeries annually achieve superior outcomes. Conversely, other research suggests that an optimal annual case volume should be approximately 40–50 surgeries. Although high surgical volume may reduce perioperative complications, other factors are known to contribute to overall outcomes, including access to specialized services, timely multidisciplinary expertise, compliance with treatment recommendations, and socioeconomic factors [9, 15, 16].
The expert panel reached a consensus that surgeons should perform at least 20 rectal cancer surgeries per year in centers that manage a minimum of 40 cases annually to reduce complications and improve patient outcomes.
Staging and imaging
Determining tumor location and initial assessment
Accurate assessment of tumor location relative to the anal verge is essential in rectal cancer management. Physical examination and endoscopy are the primary methods. For non-palpable tumors, MRI and rigid rectoscopy are complementary tools to assess tumor height and proximal extent [17–20].
MRI and structured reporting
High-resolution, rectum-specific MRI is central to local staging. It provides critical information regarding tumor size, mesorectal fascia involvement, and lymph node status. To optimize diagnostic utility, MRI should be performed using standardized protocols and interpreted by experienced radiologists using structured reporting.
The expert panel reached a consensus recommending structured MRI reporting as essential for improving diagnostic accuracy, enhancing multidisciplinary communication, enabling institutional standardization, and avoiding overtreatment. Combined use of MRI and endorectal ultrasound may further improve staging accuracy, particularly for early-stage tumors (T1–T2) (21–27). This approach may help select patients for organ preservation and avoid unnecessary neoadjuvant therapy.
Thoracoabdominal imaging
For distant staging, contrast-enhanced thoraco-abdominal CT is recommended to detect pulmonary and hepatic metastases. MRI or PET-CT may be used selectively for further characterization of indeterminate lesions, but routine PET-CT is not supported by current evidence [28–31].
The expert panel reached a consensus that rectal MRI and thoraco-abdominal CT are the preferred imaging modalities for clinical staging. For tumors extending above the reach of digital examination, either MRI or rigid rectoscopy is suggested.
Preoperative bowel preparation
The use of mechanical bowel preparation (MBP) combined with oral antibiotics before colorectal surgery significantly reduces surgical site infections (SSI), shortens hospital stay, and lowers readmission rates. The addition of oral antibiotics enhances the effect of MBP by reducing the colonic bacterial load [32–35].
The expert panel reached a strong consensus recommending routine administration of MBP with oral antibiotics prior to elective rectal cancer surgery. In round 1, 59% of experts selected mechanical bowel preparation with preoperative oral antibiotics, and in round 2 this proportion increased to 61%. As is typical in Delphi processes, participants reviewed prior round results and gradually converged toward this option, which subsequently reached consensus in round 3.
Surgical techniques
Mesorectal excision
Tumor location within the rectum dictates the extent of mesorectal excision. For upper rectal cancers, partial mesorectal excision (PME) should extend at least 5 cm below the distal tumor margin to address potential tumor spread. For mid and lower rectal cancers, total mesorectal excision (TME) with a minimum 2 cm distal margin is recommended to reduce the risk of local recurrence [36, 37]. However, in selected low rectal cancers treated with intersphincteric resection, a 1-cm clear margin may be sufficient according to current evidence.
The expert panel reached a consensus recommending PME for upper rectal tumors and TME for tumors in the mid and lower rectum.
Local excision
Local excision is an option for selected patients with clinical T1N0 rectal cancers located in the low or mid rectum. However, the risk of occult lymph node metastasis ranges from 6 to 11%, and recurrence rates may exceed 20% in the presence of high-risk histopathological features. These include poor differentiation, lymphovascular invasion, perineural invasion, tumor budding (grades 1–3, with higher grades associated with worse prognosis), deep submucosal invasion (SM3), or positive resection margins. In patients with such features, radical resection or adjuvant chemoradiotherapy with close surveillance should be considered [38–44].
Common criteria for selecting patients for local excision include lesion size < 3 cm, tumor involvement < 30% of the rectal circumference, good or moderate differentiation, and absence of lymphovascular invasion, perineural invasion, high-grade tumor budding (grade 2–3), and lymph node involvement [40].
The panel reached the following consensus statements regarding local excision:
• Local excision (endoscopic or conventional) is the preferred approach for cT1N0M0 tumors located in the low or mid rectum.
• Tumor mobility is a more critical selection criterion than size or circumferential involvement.
• After local excision with clear margins, high-risk pathological features should guide further treatment decisions.
• For patients with pT1 cN0M0 tumors and a surgical margin < 1 mm, no consensus was reached regarding the benefit of additional surgery; however, radical resection may be considered when high-risk factors are present and sphincter preservation is feasible. In patients requiring APR or lacking high-risk features, non-operative approaches may be appropriate alternatives.
Total neoadjuvant therapy (TNT)
TNT has emerged as a strategy to overcome the limitations of conventional treatment for locally advanced rectal cancer. Traditionally, treatment includes neoadjuvant chemoradiotherapy (CRT), surgery, and adjuvant chemotherapy. However, completion rates for adjuvant therapy remain suboptimal (32–82%) due to postoperative complications and chemotherapy-related toxicity [6, 45–49].
TNT integrates systemic chemotherapy and radiotherapy before surgery, improving compliance and enabling earlier systemic disease control. Studies have shown higher chemotherapy completion rates and increased pathological complete response (pCR) and clinical complete response (cCR) rates with TNT compared to standard CRT followed by adjuvant therapy [50–56]. pCR rates with TNT exceed 30%, versus 15–20% with conventional CRT [57].
TNT also facilitates organ preservation in patients achieving cCR through a “watch-and-wait” approach, reducing the need for total mesorectal excision (TME) and permanent stomas [58, 59]. Accordingly, current NCCN guidelines endorse TNT as a preferred option for stage II–III rectal cancer [60]. Nonetheless, ongoing research is refining its optimal use through extended follow-up data.
TNT strategies
TNT regimens are generally categorized into two approaches:
• Induction chemotherapy, in which systemic chemotherapy is administered before CRT, is followed by surgery.
• Consolidation chemotherapy, in which CRT precedes systemic chemotherapy and surgery.
Radiotherapy may be delivered as either short-course (25 Gy in 5 fractions) or long-course (45–54 Gy in 25–30 fractions). The optimal regimen and sequence remain under investigation, with several trials comparing outcomes.
Key clinical trials
• CAO/ARO/AIO-12 compared induction vs. consolidation chemotherapy. Consolidation achieved a higher pCR rate (25% vs. 17%), though not statistically significant. Long-term outcomes, including DFS and recurrence, were similar [61, 62].
• PRODIGE-23 utilized induction FOLFIRINOX followed by CRT. The TNT arm showed significantly higher pCR (27.5% vs. 11.7%), along with improved 5-year DFS (+7.6%) and OS (+6.9%) compared to standard CRT [53, 63].
• OPRA focused on organ preservation in patients achieving cCR. While 3-year DFS was similar between induction and consolidation arms (76%), the consolidation group had higher proctectomy-free survival (53% vs. 41%) [64–66].
• Polish II evaluated short-course RT followed by FOLFOX4. pCR and R0 resection rates were comparable to long-course CRT, with TNT demonstrating lower acute toxicity [67].
• RAPIDO targeted high-risk rectal cancer. TNT improved pCR (28.4% vs. 14.3%) and reduced disease-related treatment failure. However, a higher local recurrence rate was observed in the TNT group during long-term follow-up [21, 68].
• STELLAR compared short-course RT + CAPOX versus long-course CRT. TNT improved overall survival (86.5% vs. 75.1%) but did not significantly affect metastasis-free or locoregional recurrence rates [69].
The panel recommended TNT for patients with low rectal tumors and those with high-risk features, including:
• T4 tumors
• Circumferential resection margin (CRM) < 1 mm
• Extramural vascular invasion (EMVI+)
• Pathological lateral pelvic lymph nodes
• Sphincter or levator involvement
Among TNT approaches, long-course CRT followed by consolidation chemotherapy was favored. This strategy was associated with improved compliance, greater tumor regression, and higher rates of cCR and pCR. Induction regimens, although effective, were noted to have higher toxicity and reduced RT completion in some patients.
Although long-term oncologic outcomes of induction and consolidation appear broadly comparable, the panel favored consolidation primarily due to higher treatment compliance, greater tumor regression, and improved organ preservation observed in practice and supported by OPRA trial data. This preference may reflect expert practice patterns rather than definitive evidence of superiority, and both strategies remain acceptable according to current guidelines.
Assessing the efficacy of TNT for rectal cancer
Interval evaluations
A major concern with TNT is the potential delay in definitive surgery, which may lead to tumor progression in nonresponders. While most patients experience regression, approximately 20% show minimal or no response to TNT [53, 70]. In such cases, extending the interval between radiation and surgery or adding further chemotherapy is unlikely to improve outcomes.
The RAPIDO trial reported a higher rate of ypT4 tumors in the TNT group (9% vs. 6%), suggesting increased progression risk among nonresponders [52]. Similarly, a retrospective study of 102 patients found that poor responders had significantly worse progression-free survival compared to responders [71].
These findings highlight the importance of timely interim evaluations during TNT. Early identification of nonresponders (potentially through MRI or other imaging) can facilitate prompt surgical intervention and avoid disease progression.
The expert panel reached a consensus that interval evaluations are essential during TNT to guide timely treatment decisions.
Response assessment to TNT
cCR after TNT should be evaluated using a multimodal approach, including digital rectal examination (DRE), flexible sigmoidoscopy, and pelvic MRI using a dedicated rectal cancer protocol.
MRI is the cornerstone of response assessment due to its ability to distinguish fibrosis from residual tumor. A dark T2-weighted (T2w) signal without intermediate intensity and the absence of suspicious lymph nodes suggests cCR. Adding diffusion-weighted imaging (DWI) improves sensitivity to 84%, compared to 50% with T2w alone [72–74]. MRI can also differentiate near-complete clinical response (ncCR) from incomplete response [71].
However, limitations exist. In a study by De la Pinta et al., MRI correctly staged only 23% of tumors, highlighting issues with both over- and understaging [75]. Thus, advanced imaging protocols and interpretation expertise remain essential.
Endoscopic evaluation complements MRI in assessing mucosal healing. Flat white scars with or without telangiectasia suggest cCR, while nodularity or ulceration may indicate ncCR [76, 77]. Routine biopsy is discouraged due to high false-negative rates and poor correlation with final pathology [76].
Digital rectal examination (DRE) remains useful, particularly for distal tumors. A smooth, flat scar is typical of cCR, while nodules or irregularities may indicate ncCR or residual disease. When combined with MRI, DRE enhances diagnostic specificity up to 98% [76, 78].
Despite improvements in imaging and clinical assessment, up to 30% of true cCR cases may be missed, underscoring the need for ongoing refinement in evaluation strategies.
The expert panel reached a consensus that response assessment after TNT should include DRE, rectal MRI, and endoscopy.
Timing of clinical response assessment
The optimal timing for assessing cCR after TNT varies based on treatment protocol and remains an area of active investigation.
For standard CRT or short-course radiotherapy (SCRT), cCR is typically evaluated at around 12 weeks from treatment initiation [79]. In TNT protocols with induction or consolidation chemotherapy—such as RAPIDO and PRODIGE-23—assessment is often done at 24 weeks, while extended TNT regimens like those in OPRA may require evaluation as late as 34–38 weeks [53, 64–66, 68, 80].
Tumor regression can continue for several weeks after treatment, and delayed evaluation may increase organ preservation rates. However, not all patients benefit from prolonged observation. PET/CT studies show that many tumors stop regressing beyond 12 weeks and may show renewed activity [81]. Therefore, delaying surgery in nonresponders may lead to worse outcomes.
A sequential evaluation approach is recommended. Early assessment (6–8 weeks post-treatment) helps identify nonresponders who may need prompt surgery, while responders can be observed longer to maximize the chance of non-operative management.
The expert panel reached a consensus recommending that cCR assessment should ideally occur between 6 and 8 weeks after completion of TNT.
Near-complete clinical response
Managing patients with a ncCR after TNT requires a balance between preserving organ function and ensuring oncologic safety. Options include extended observation, local excision, further chemotherapy, or proceeding to TME.
Extended observation is supported by evidence showing that tumor regression may continue for 6–12 weeks beyond the standard assessment window. The ReSARCh trial, for example, reported higher complete response rates when local excision was delayed to 12 weeks post-CRT [85]. Importantly, meta-analyses indicate that delaying surgery does not significantly increase metastasis risk, provided there is rigorous surveillance [83, 84].
However, TME remains the standard for oncologic control and is often used when the response is uncertain. Still, many patients who undergo TME after ncCR are later found to have pCR, raising concerns of overtreatment [86].
The expert panel reached a consensus that for patients with ncCR after TNT, an additional observation period of 4 to 8 weeks may be considered to allow for further tumor regression before reassessment.
The role of biopsy in patients with near-complete clinical response
Endoscopic biopsy is not recommended for routine use in assessing residual disease after neoadjuvant therapy in rectal cancer due to its low diagnostic accuracy.
Although biopsy may appear intuitive in the setting of mucosal abnormalities, its negative predictive value is poor. Studies show that many patients with negative biopsy results still harbor residual disease at final pathology [87, 88]. This inaccuracy largely stems from the inability of superficial biopsies to capture residual tumor cells located deeper within the rectal wall or extending laterally beyond visible mucosal changes [88, 89].
Misleading biopsy results may falsely suggest a complete response, potentially delaying curative surgery or leading to inappropriate non-operative management decisions.
The expert panel reached a consensus advising against routine biopsy in patients with near-complete clinical response due to its potential to misguide clinical decisions.
The interval between the completion of TNT and surgery
Unlike conventional neoadjuvant protocols, which typically involve surgery within 6–12 weeks of completing radiation, TNT generally requires longer intervals before surgical intervention. While these prolonged intervals may raise concerns regarding increased surgical complexity or risk, evidence from major clinical trials such as PRODIGE-23 and RAPIDO suggests otherwise. In PRODIGE-23, the R0 resection rate was 95% in the TNT group, compared to 94% in the conventional arm. In RAPIDO, both groups achieved a 90% R0 resection rate. TME specimen quality and postoperative complication rates were also similar between groups [53, 68]. These findings support the safety and oncologic adequacy of extended surgical intervals following TNT. Prolonged intervals may enhance tumor regression, thereby increasing pCR rates, which is an important prognostic marker. However, excessive delays may lead to fibrosis and technical challenges during surgery, potentially increasing intraoperative risk.
The expert panel reached a consensus recommending that surgery be performed at least 8 weeks after completing TNT to optimize oncological outcomes while maintaining surgical safety and feasibility.
Non-operative management
Applicability in distal rectal cancer
NOM following TNT has been traditionally favored for distal rectal tumors, due to their anatomical accessibility and ease of surveillance. These tumors are more amenable to evaluation via DRE and flexible endoscopy, making the assessment of cCR more reliable. Moreover, NOM in this setting offers a significant quality-of-life advantage by avoiding APR and the need for a permanent colostomy. Studies report local regrowth in ~30% of patients managed with NOM within the first 3 years. Over 90% of these recurrences are endoluminal, underscoring the importance of DRE and endoscopic surveillance for early detection and successful salvage surgery [81, 90, 91]. On the other hand, an open-ended round 1 item briefly explored whether patients with LARC who achieve a clinical complete response after standard CRT should transition to NOM and, if so, what protocol to follow. Responses were highly heterogeneous and did not permit a structured statement; therefore, the steering committee did not carry this item forward to subsequent rounds.
Extending NOM beyond distal tumors
Emerging data challenge the notion that NOM should be limited to distal rectal cancers. Several recent studies suggest that mid-rectal tumors may achieve similar cCR rates, demonstrate comparable local regrowth patterns, and maintain high success rates for salvage surgery, akin to distal lesions [78, 92].
This evolving evidence, combined with improvements in MRI and diffusion-weighted imaging, enhances the ability to monitor for mesorectal and pelvic recurrences, potentially broadening eligibility for NOM beyond distal locations.
The expert panel did not reach a consensus on whether NOM should be limited to specific tumor locations within the rectum. In round 3 of the Delphi process, only 52% of panelists agreed with the statement: “Non-operative management should only be recommended for tumors located in the distal rectum.”
Follow-up period for non-operative management
Patients managed with NOM after achieving cCR require a strict surveillance protocol to detect local regrowth and distant metastasis. Local regrowth occurs in 20–30% of cases, usually within the first 3 years [65, 93]. Intensive monitoring during this early period is critical to promptly identify regrowth, enabling successful salvage surgery with R0 resection rates and survival outcomes comparable to those undergoing immediate TME [65]. Surveillance typically involves clinical examinations, endoscopy, and radiological assessments every 8–12 weeks during the first 3 years, with intervals extending thereafter.
After the third year, when the regrowth risk drops below 5%, follow-up intervals may be extended to every 6 months until year 5 [95]. Annual follow-up is advised beyond 5 years as long as the rectum is preserved [65, 66, 94, 95].
Normalization of carcinoembryonic antigen (CEA) levels (typically < 5 ng/mL) after neoadjuvant therapy correlates with tumor regression, providing a valuable marker of therapeutic response, particularly in patients with elevated baseline CEA levels. Rising CEA levels during surveillance may signal local or distant recurrence, thus warranting further investigation (98).
Emerging techniques such as circulating tumor DNA (ctDNA) analysis (liquid biopsy) are under investigation for their potential in surveillance. Current evidence regarding ctDNA is inconclusive; while some studies suggest elevated ctDNA levels may predict recurrence risk, others fail to demonstrate an association with pathological complete response (pCR). Thus, ctDNA remains investigational and is not yet recommended for routine NOM follow-up [97].
The expert panel reached a consensus recommending that patients undergoing NOM require a surveillance period extending beyond 5 years.
Local regrowth and distant metastasis during non-operative management
Local regrowth refers to tumor recurrence within the rectal wall, mesorectum, or pelvic compartment after an initial cCR, and is distinct from recurrence following TME [98]. It typically occurs within the first 3 years of NOM, with reported rates ranging from 15 to 34%. Data from the International Watch & Wait Database indicate a 25% rate of local regrowth within 2 years, predominantly endoluminal and detectable via DRE and endoscopy in over 90% of cases [90, 91, 93, 99].
The most significant predictor of local regrowth is baseline clinical T stage, with risk increasing approximately 10% per stage: ~20% for cT2, ~30% for cT3, and ~40% for cT4 tumors [100]. Other contributing factors include deep tumor invasion and bulky nodal involvement, although baseline N stage alone is not independently associated with regrowth risk [95]. Achieving and sustaining cCR beyond 3 years is associated with a markedly reduced risk of subsequent regrowth, underscoring the importance of initial treatment response.
Salvage surgery remains the cornerstone for managing local regrowth and offers curative potential. Approximately 90% of regrowth cases can be treated with R0 resection, ensuring excellent local control [101–103]. While salvage TME is the standard approach, local excision may be appropriate for carefully selected patients with small, superficial regrowths. However, salvage TME often requires more extensive procedures, including APR in distal tumors involving the levator ani muscles. As a result, APR rates are higher in the salvage setting compared to upfront TME [104]. Although local excision may preserve function and reduce morbidity, it carries a greater risk of subsequent recurrence and should be reserved for highly selected cases [51, 105].
Patients undergoing salvage TME generally achieve excellent local control, with recurrence rates under 5%. However, overall survival may vary based on the characteristics of the regrowth and the timing of intervention. Notably, salvage APR is associated with higher morbidity and reduced quality of life. Comparative studies have shown similar survival outcomes between patients undergoing salvage surgery after regrowth and those treated with immediate TME for incomplete response. However, patients who underwent immediate TME after a favorable response demonstrated better outcomes than those who required delayed salvage surgery and had ypT3–4 disease at resection [103, 106].
While patients with sustained cCR have a low risk (5–10%) of distant metastases, the development of local regrowth increases this risk to approximately 24%. This suggests that regrowth may reflect aggressive tumor biology, acting independently as a driver of metastatic progression [107, 108]. Although the metastatic risk declines after 5 years of disease-free survival, patients with a history of regrowth remain at elevated risk for several years, emphasizing the need for prolonged surveillance [109].
The expert panel reached a consensus that radical surgery remains the preferred treatment option for patients who develop local regrowth during NOM follow-up.
Lateral pelvic lymph nodes
In the era of neoadjuvant chemoradiotherapy, selective lateral pelvic lymph node dissection (LPLND) has emerged as a focused strategy for managing LPLNs in patients with locally advanced rectal cancer. Although TNT has significantly improved both systemic and local control, it does not consistently eliminate enlarged LPLNs particularly when lymph nodes remain radiologically suspicious after neoadjuvant treatment. Historically, Eastern centers have routinely performed LPLND for rectal cancer, even before the introduction of TNT, reflecting different approaches to managing lymphatic spread and recurrence patterns. In contrast, Western practice has traditionally relied on TNT and TME alone, reserving LPLND due to concerns regarding added morbidity and uncertain oncological benefit [110, 111].
However, emerging data from both Eastern and Western institutions increasingly support a selective approach to LPLND based on post-treatment MRI characteristics. Persistently enlarged nodes—especially those with a short-axis diameter >5–7 mm—have been associated with a significantly increased risk of harboring residual disease and subsequent lateral pelvic recurrence [112, 113].
Retrospective studies, including those from MD Anderson Cancer Center, suggest that MRI-guided selective LPLND-targeting nodes with persistent enlargement, irregular borders, or heterogeneous signals, can significantly reduce recurrence rates without the higher complication risks seen in more extensive dissections [110]. For example, Peacock et al. reported that 34.1% of patients with persistently enlarged LPLNs following TNT had residual nodal metastases on pathology, suggesting TNT alone may be insufficient in this subgroup [114].
Similarly, international multicenter data show that, in patients with LPLNs ≥ 7 mm post-treatment, the addition of LPLND to TNT and TME reduced local recurrence rates from 25.6% to 5.7% [111]. This targeted approach achieves oncological control while minimizing unnecessary dissections and associated complications such as urinary or sexual dysfunction.
While a short-axis diameter ≥ 5 mm on MRI is generally accepted as a threshold for considering LPLND, further studies are needed to refine imaging criteria and validate long-term oncologic and functional outcomes of this approach [113].
The expert panel reached consensus on the following statements regarding the management of lateral pelvic lymph nodes in rectal cancer:
If pathological lateral pelvic lymph nodes persist after completion of neoadjuvant therapy, LPLND is recommended on the ipsilateral side.
If radiologically suspicious lymph nodes regress following neoadjuvant therapy, LPLND may not be necessary.
Limitations
The expert panel was presented with a series of structured questions concerning various aspects of rectal cancer management, each accompanied by multiple-choice response options. Given the potential for diverse subcategories within these questions, the panel’s responses may not facilitate a broad generalization regarding the treatment of rectal cancer. The inherent variability in clinical presentations, coupled with the nuanced decision-making required in tailoring treatment to individual patients, underscores the challenges in establishing one-size-fits-all recommendations. The consensus provides expert guidance but must be applied within individualized multidisciplinary care contexts. One limitation of our study is the absence of radiologists, gastroenterologists, and oncologists in the Delphi panel. Although these specialties play a central role in staging, treatment planning, and multidisciplinary decision-making, their participation could not be secured due to recruitment constraints. This limits the breadth of multidisciplinary input and highlights the need for broader specialty involvement in future consensus efforts. Furthermore, our expert panel was primarily composed of specialists from the same country, which may limit the international generalizability of our findings.
Conclusion
This Delphi consensus provides practical guidance for the management of early and locally advanced rectal cancer, emphasizing multidisciplinary collaboration, standardized MRI reporting, the adoption of TNT for high-risk tumors, and structured protocols for NOM (Table 4).
Table 4.
Consensus summary
| Topic | Consensus statements | Agreement(%) |
|---|---|---|
| 1. Role of MDT in decision-making |
MDT discussion is essential for optimal treatment decisions High-volume centers (≥ 40 rectal cancer cases per year) improve outcomes |
97 94 |
| 2. Staging and imaging |
Standardized high-resolution MRI should be used for accurate local staging and treatment planning Thoraco-abdominal CT is recommended for metastasis evaluation |
95 |
| 3. Preoperative bowel preparation | Mechanical bowel preparation with oral antibiotics may reduce surgical site infections | 87 |
| 4. Surgical techniques |
Partial mesorectal excision is recommended for upper rectal tumors Local excision may be used for cT1N0 tumors, provided no high-risk features exist |
87 82 |
| 5. Total neoadjuvant therapy |
Recommended for tumors with high-risk factors Consolidation may improve organ preservation rates Interval evaluations should be conducted during TNT |
97 87 89 |
| 6. Non-operative management and clinical response |
NOM is primarily recommended for distal rectal cancers Assessment of cCR: MRI, endoscopy, and digital rectal exam should be used Timing: Clinical response should be assessed 6–8 weeks post-TNT ncCR: Additional 4–8 weeks of observation may improve cCR rates Biopsy for ncCR: Not recommended due to poor predictive value |
52 100 87 85 82 |
| 7. Interval between TNT completion and surgery | Surgery should be performed at least 8 weeks post-TNT for optimal regression | 97 |
| 8. Non-operative management follow-up |
1–3 years: MRI, DRE, endoscopy every 3 months 3–5 years: MRI, DRE, endoscopy every 6 months > 5 years: Annual follow-up |
100 |
| 9. LPLN dissection | Recommended for persistent pathological LPLNs after neoadjuvant therapy | 97 |
The integration of TNT and NOM in appropriately selected cases marks a paradigm shift in clinical practice. Importantly, these strategies must be balanced with patient-centered decision making, recognizing that treatment choices affect not only oncologic outcomes but also long-term function and quality of life. Organ preservation strategies may reduce morbidity, whereas radiation and chemotherapy can result in late toxicities such as pelvic bone complications, impaired sexual function, secondary malignancies, and chemotherapy-induced neurotoxicity. Individualized discussions between patients and multidisciplinary teams are therefore essential to align treatment plans with patient values and expectations.
Future prospective studies are needed to validate these recommendations, refine surveillance protocols, and incorporate emerging technologies. Continued collaboration between international colorectal surgery and oncology societies will be key to achieving global standardization and improved outcomes.
Acknowledgements
The authors sincerely thank the leadership and members of TSCRS, as well as all expert panel participants who contributed their valuable insights and expertise to this Delphi study.
Author contribution
C.T., T.B., A.E.C., F.K., E.G., I.E.B.: Study conception design C.T., T.B., A.E.C., A.C.Y., E.C., I.E.C., I.H.O., M.A.K., O.A., O.B., R.K., Y.S., I.E.B.: Data Acquisition C.T., T.B., A.E.C., F.K., E.G., I.E.B.: Data analysis and interpretation C.T., T.B.: Drafting the article C.T., T.B., A.E.C., F.K., E.G., A.C.Y., E.C., I.E.C., I.H.O., M.A.K., O.A., O.B., R.K., Y.S., I.E.B.: Critical revision for intellectual content All authors approved the final version of the manuscript All authors agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved
Data availability
The data generated and analyzed in this Delphi consensus study consist of anonymized expert panel responses. Due to the nature of the Delphi methodology and the requirement to preserve participant confidentiality, the raw datasets cannot be made publicly available. De-identified, aggregate data supporting the findings of this study may be available from the corresponding author upon reasonable request, subject to approval by the study investigators and in compliance with confidentiality agreements.
Declarations
Competing interests
The authors declare no competing interests.
Footnotes
Cihad Tatar and Tayfun Bisgin are the first authors.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Azevedo JM, Vailati BB, Julião GPS et al (2019) Current surgical strategies in the management of rectal cancer. Curr Colorectal Cancer Rep 15:18–27 [Google Scholar]
- 2.Stornes T, Wibe A, Nesbakken A et al (2016) National early rectal cancer treatment revisited. Dis Colon Rectum 59:623–629 [DOI] [PubMed] [Google Scholar]
- 3.Rouleau-Fournier F, Brown CJ (2019) Can less be more? Organ preservation strategies in the management of rectal cancer. Curr Oncol 26:S16–S23 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Althumairi AA, Gearhart SL (2015) Local excision for early rectal cancer: transanal endoscopic microsurgery and beyond. J Gastrointest Oncol 6:296–306 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Halverson AL, Morris AM, Cleary RK, et al (2019) For patients with early rectal cancer, does local excision have an impact on recurrence, survival, and quality of life relative to radical resection? Ann Surg Oncol. 2019;26:2497–2506. [DOI] [PubMed]
- 6.You YN, Hardiman KM, Bafford A (2020) The American Society of Colon and Rectal Surgeons clinical practice guidelines for the management of rectal cancer. Dis Colon Rectum 63(9):1191–1222 [DOI] [PubMed] [Google Scholar]
- 7.Karagkounis G, Stocchi L, Lavery IC et al (2018) Multidisciplinary conference and clinical management of rectal cancer. J Am Coll Surg 226(5):874–880 [DOI] [PubMed] [Google Scholar]
- 8.Ioannidis A, Konstantinidis M, Apostolakis S et al (2018) Impact of multidisciplinary tumor boards on patients with rectal cancer. Mol Clin Oncol 9:135–137 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Richardson B, Preskitt J, Lichliter W et al (2016) The effect of multidisciplinary teams for rectal cancer on delivery of care and patient outcome. Am J Surg 211:46–52 [DOI] [PubMed] [Google Scholar]
- 10.van de Velde CJ, Boelens PG, Borras JM et al (2014) EURECCA colorectal: multidisciplinary management: European consensus conference colon & rectum. Eur J Cancer 50(Suppl 1):e1–e34 [DOI] [PubMed] [Google Scholar]
- 11.Naughton B, Roberts L, Dopson S et al (2017) Medicine authentication technology as a counterfeit medicine-detection tool: a Delphi method study. BMJ Open 7:e013838 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Gurland BH, Olson CH, McCarthy MS (2024) Core descriptor sets for rectal prolapse outcomes research using a modified delphi consensus. Dis Colon Rectum 67(6):841–849 [DOI] [PubMed] [Google Scholar]
- 13.MacDermid E, Hooton G, MacDonald M (2009) Improving patient survival with the colorectal cancer multi-disciplinary team. Colorectal Dis 11:291–295. 10.1111/j.1463-1318.2008.01580.x [DOI] [PubMed] [Google Scholar]
- 14.Aquina CT, Probst CP, Kelly KN et al (2015) High volume improves outcomes: the argument for centralization of rectal cancer surgery. Surgery 157(4):632–642. 10.1016/j.surg.2014.11.013 [DOI] [PubMed] [Google Scholar]
- 15.Schrag D, Panageas KS, Riedel E et al (2002) Hospital and surgeon procedure volume as predictors of outcome following rectal cancer resection. Ann Surg 236(5):583–592. 10.1097/00000658-200211000-00003 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Billingsley KG, Morris AM, Green P (2008) Does surgeon case volume influence nonfatal adverse outcomes after rectal cancer resection? J Am Coll Surg. 10.1016/j.jamcollsurg.2007.12.042 [DOI] [PMC free article] [PubMed]
- 17.Acuna SA, Elmi M, Shah PS (2017) Preoperative localization of colorectal cancer: a systematic review and meta-analysis. Surg Endosc 31:2366–2379 [DOI] [PubMed] [Google Scholar]
- 18.Kirchoff DD, Hang JH, Cekic V et al (2014) Endoscopic tattooing to mark distal margin for low anterior rectal and select sigmoid resections. Surg Innov 21:376–380 [DOI] [PubMed] [Google Scholar]
- 19.Cipe G, Cengiz MB, Idiz UO et al (2016) The effects of preoperative endoscopic tattooing on distal surgical margin and ileostomy rates in laparoscopic rectal cancer surgery: a prospective randomized study. Surg Laparosc Endosc Percutan Tech 26:301–303 [DOI] [PubMed] [Google Scholar]
- 20.Okada K, Sadahiro S, Ogimi T et al (2018) Tattooing improves the detection of small lymph nodes and increases the number of retrieved lymph nodes in patients with rectal cancer who receive preoperative chemoradiotherapy: a randomized controlled clinical trial. Am J Surg 215:563–569 [DOI] [PubMed] [Google Scholar]
- 21.Faletti R, Gatti M, Arezzo A (2018) Preoperative staging of rectal cancer using magnetic resonance imaging: comparison with pathological staging. Minerva Chir 73:13–19 [DOI] [PubMed] [Google Scholar]
- 22.Klessen C, Rogalla P, Taupitz M (2007) Local staging of rectal cancer: the current role of MRI. Eur Radiol 17:379–389 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Lahaye MJ, Engelen SM, Nelemans PJ et al (2005) Imaging for predicting the risk factors–the circumferential resection margin and nodal disease–of local recurrence in rectal cancer: a meta-analysis. Semin Ultrasound CT MR 26:259–268 [DOI] [PubMed] [Google Scholar]
- 24.Xie H, Zhou X, Zhuo Z et al (2014) Effectiveness of MRI for the assessment of mesorectal fascia involvement in patients with rectal cancer: a systematic review and meta-analysis. Dig Surg 31(2):123–134 [DOI] [PubMed] [Google Scholar]
- 25.Lambregts DM, Boellaard TN, Lahaye MJ et al (2011) Rectal cancer: improved survival with high diagnostic performance for the mesorectal fascia. Eur Radiol 21(1):129–137 [Google Scholar]
- 26.Taylor FG, Quirke P, Heald RJ et al (2011) Preoperative high-resolution magnetic resonance imaging can identify good prognosis stage I, II, and III rectal cancer best managed by surgery alone: a prospective, multicenter European study. Ann Surg 253(4):711–719 [DOI] [PubMed] [Google Scholar]
- 27.Wlodarczyk J, Taitano G, Serniak N et al (2021) Does a standardized distance cut-off accurately predict the length of the rectum? Using MRI to analyze the height of the peritoneal reflection. Turk J Colorectal Dis 31(4):291–299 [Google Scholar]
- 28.Fowler KJ, Kaur H, Cash BD et al (2017) ACR appropriateness criteria® pretreatment staging of colorectal cancer. J Am Coll Radiol 14:S234–S244 [DOI] [PubMed] [Google Scholar]
- 29.Kaur H, Hindman NM, Al-Refaie WB (2017) ACR appropriateness criteria® suspected liver metastases. J Am Coll Radiol 14:S314–S325 [DOI] [PubMed] [Google Scholar]
- 30.Adam R, de Gramont A, Figueras J (2015) Managing synchronous liver metastases from colorectal cancer: a multidisciplinary international consensus. Cancer Treat Rev 41:729–741 [DOI] [PubMed] [Google Scholar]
- 31.Vera R, González-Flores E, Rubio C (2020) Multidisciplinary management of liver metastases in patients with colorectal cancer: a consensus of SEOM, AEC, SEOR, SERVEI, and SEMNIM. Clin Transl Oncol 22:647–662 [DOI] [PubMed] [Google Scholar]
- 32.Morris MS, Graham LA, Chu DI (2015) Oral antibiotic bowel preparation significantly reduces surgical site infection rates and readmission rates in elective colorectal surgery. Ann Surg 261:1034–1040 [DOI] [PubMed] [Google Scholar]
- 33.Bellows CF, Mills KT, Kelly TN et al (2011) Combination of oral non-absorbable and intravenous antibiotics versus intravenous antibiotics alone in the prevention of surgical site infections after colorectal surgery: a meta-analysis of randomized controlled trials. Tech Coloproctol 15:385–395 [DOI] [PubMed] [Google Scholar]
- 34.Cannon JA, Altom LK, Deierhoi RJ et al (2012) Preoperative oral antibiotics reduce surgical site infection following elective colorectal resections. Dis Colon Rectum 55:1160–1166 [DOI] [PubMed] [Google Scholar]
- 35.Mayir B, Ensari CÖ, Çakır T et al (2015) Approach of Turkish general surgeons about mechanical bowel preparation before elective colorectal surgery. Turk J Colorectal Dis 25(1):1–6 [Google Scholar]
- 36.Hida J, Yasutomi M, Maruyama T et al (1997) Lymph node metastases detected in the mesorectum distal to carcinoma of the rectum by the clearing method: justification of total mesorectal excision. J Am Coll Surg 184:584–588 [PubMed] [Google Scholar]
- 37.Scott N, Jackson P, al-Jaberi T et al (1995) Total mesorectal excision and local recurrence: a study of tumour spread in the mesorectum distal to rectal cancer. Br J Surg 82:1031–1033 [DOI] [PubMed] [Google Scholar]
- 38.Brunner W, Widmann B, Marti L et al (2016) Predictors for regional lymph node metastasis in T1 rectal cancer: a population-based SEER analysis. Surg Endosc 30:4405–4415 [DOI] [PubMed] [Google Scholar]
- 39.Nascimbeni R, Burgart LJ, Nivatvongs S (2002) Risk of lymph node metastasis in T1 carcinoma of the colon and rectum. Dis Colon Rectum 45:200–206 [DOI] [PubMed] [Google Scholar]
- 40. Benson AB, Venook AP, Al-Hawary MM, et al (2019) Rectal cancer, Version 3.2019, NCCN Clinical Practice Guidelines in Oncology. Available at: www nccn.org. Accessed September 1, 2019.
- 41.Doornebosch PG, Tollenaar RA, De Graaf EJ (2009) Is the increasing role of transanal endoscopic microsurgery in curation for T1 rectal cancer justified? A systematic review. Acta Oncol 48:343–353 [DOI] [PubMed] [Google Scholar]
- 42.Kidane B, Chadi SA, Kanters S, Colquhoun PH, Ott MC (2015) Local resection compared with radical resection in the treatment of T1N0M0 rectal adenocarcinoma: a systematic review and meta-analysis. Dis Colon Rectum 58:122–140 [DOI] [PubMed] [Google Scholar]
- 43.You YN, Baxter NN, Stewart A, Nelson H (2007) Is the increasing rate of local excision for stage I rectal cancer in the United States justified?: a nationwide cohort study from the National Cancer Database. Ann Surg 245:726–733 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Russo S, Anker CJ, Abdel-Wahab M (2019) Executive summary of the American Radium Society appropriate use criteria for local excision in rectal cancer. Int J Radiat Oncol Biol Phys 105:977–993 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Ma B, Ren Y, Chen Y et al (2019) Is adjuvant chemotherapy necessary for locally advanced rectal cancer patients with pathological complete response after neoadjuvant chemoradiotherapy and radical surgery? A systematic review and meta-analysis. Int J Colorectal Dis 34:113–121 [DOI] [PubMed] [Google Scholar]
- 46.Denost Q, Fleming CA, Burghgraef T (2023) An international multicenter prospective study evaluating the long-term oncological impact of adjuvant chemotherapy in ypN+ rectal cancer. Ann Surg 277:299–304 [DOI] [PubMed] [Google Scholar]
- 47.Breugom AJ, Swets M, Bosset JF et al (2015) Adjuvant chemotherapy after preoperative (chemo)radiotherapy and surgery for patients with rectal cancer: a systematic review and meta-analysis of individual patient data. Lancet Oncol 16:200–207 [DOI] [PubMed] [Google Scholar]
- 48.Fleshman J, Branda ME, Sargent DJ et al (2019) Disease-free survival and local recurrence for laparoscopic resection compared with open resection of stage II to III rectal cancer: follow-up results of the ACOSOG Z6051 randomized controlled trial. Ann Surg 269:589–595 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Morris MC, Winer LK, Lee TC, Shah SA, Rafferty JF, Paquette IM (2021) Omission of adjuvant chemotherapy in rectal cancer patients with pathologic complete response: a national analysis. J Gastrointest Surg 25:1857–1865 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Zaborowski A, Stakelum A, Winter DC (2019) Systematic review of outcomes after total neoadjuvant therapy for locally advanced rectal cancer. Br J Surg 106:979–987 [DOI] [PubMed] [Google Scholar]
- 51.Garcia-Aguilar J, Chow OS, Smith DD et al (2015) Effect of adding mFOLFOX6 after neoadjuvant chemoradiation in locally advanced rectal cancer: a multicentre, phase 2 trial. Lancet Oncol 16:957–966 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Bahadoer RR, Dijkstra EA, van Etten B et al (2021) Short-course radiotherapy followed by chemotherapy before total mesorectal excision (TME) versus preoperative chemoradiotherapy, TME, and optional adjuvant chemotherapy in locally advanced rectal cancer (RAPIDO): a randomised, open-label, phase 3 trial. Lancet Oncol 22:29–42 [DOI] [PubMed] [Google Scholar]
- 53.Conroy T, Bosset JF, Etienne PL et al (2021) Neoadjuvant chemotherapy with FOLFIRINOX and preoperative chemoradiotherapy for patients with locally advanced rectal cancer (UNICANCER-PRODIGE 23): a multicentre, randomised, open-label, phase 3 trial. Lancet Oncol 22:702–715 [DOI] [PubMed] [Google Scholar]
- 54.Kasi A, Abbasi S, Handa S et al (2020) Total neoadjuvant therapy vs standard therapy in locally advanced rectal cancer: a systematic review and meta-analysis. JAMA Netw Open 3:e2030097 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55. Riesco-Martinez MC, Fernandez-Martos C, Gravalos-Castro C, et al (2020) Impact of total neoadjuvant therapy vs. standard chemoradiotherapy in locally advanced rectal cancer: a systematic review and meta-analysis of randomized trials Cancers (Basel). 2020;12:3655. [DOI] [PMC free article] [PubMed]
- 56.Kong JC, Soucisse M, Michael M et al (2021) Total neoadjuvant therapy in locally advanced rectal cancer: a systematic review and meta-analysis of oncological and operative outcomes. Ann Surg Oncol 28:7476–7486 [DOI] [PubMed] [Google Scholar]
- 57.Cercek A, Roxburgh CSD, Strombom P et al (2018) Adoption of total neoadjuvant therapy for locally advanced rectal cancer. JAMA Oncol 4:e180071 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Fujita S, Mizusawa J, Kanemitsu Y (2017) Mesorectal excision with or without lateral lymph node dissection for clinical stage II/III lower rectal cancer (JCOG0212): a multicenter, randomized controlled, noninferiority trial. Ann Surg 266:201–207 [DOI] [PubMed] [Google Scholar]
- 59.Habr-Gama A, Perez RO, Nadalin W et al (2004) Operative versus nonoperative treatment for stage 0 distal rectal cancer following chemoradiation therapy: long-term results. Ann Surg 240:711–717 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Benson AB, Venook AP, Al-Hawary MM et al (2022) Rectal cancer, version 2.2022, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw 20:1139–1167 [DOI] [PubMed] [Google Scholar]
- 61.Fokas E, Allgauer M, Polat B et al (2019) Randomized phase II trial of chemoradiotherapy plus induction or consolidation chemotherapy as total neoadjuvant therapy for locally advanced rectal cancer: CAO/ARO/AIO-12. J Clin Oncol 37:3212–3222 [DOI] [PubMed] [Google Scholar]
- 62.Fokas E, Schlenska-Lange A, Polat B (2022) Chemoradiotherapy plus induction or consolidation chemotherapy as total neoadjuvant therapy for patients with locally advanced rectal cancer: long-term results of the CAO/ARO/AIO-12 randomized clinical trial. JAMA Oncol 8:e215445 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63. Etienne PL, Rio E, Evesque L, et al (2023) Total neoadjuvant therapy with mFOLFIRINOX versus preoperative chemoradiation in patients with locally advanced rectal cancer: 7-year results of PRODIGE 23 phase III trial, a UNICANCER GI trial. J Clin Oncol 41:LBA3504. [DOI] [PubMed]
- 64.Smith JJ, Chow OS, Gollub MJ et al (2015) Organ preservation in rectal adenocarcinoma: a phase II randomized controlled trial evaluating 3-year disease-free survival in patients with locally advanced rectal cancer treated with chemoradiation plus induction or consolidation chemotherapy, and total mesorectal excision or nonoperative management. BMC Cancer 15:767 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Garcia-Aguilar J, Patil S, Gollub MJ et al (2022) Organ preservation in patients with rectal adenocarcinoma treated with total neoadjuvant therapy. J Clin Oncol 40:2546–2556 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Verheij FS, Omer DM, Williams H et al (2024) Long-term results of organ preservation in patients with rectal adenocarcinoma treated with total neoadjuvant therapy: the randomized phase II OPRA trial. J Clin Oncol 42:500–506 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Cisel B, Pietrzak L, Michalski W et al (2019) Long-course preoperative chemoradiation versus 5 × 5 Gy and consolidation chemotherapy for clinical T4 and fixed clinical T3 rectal cancer: long-term results of the randomized Polish II study. Ann Oncol 30:1298–1308 [DOI] [PubMed] [Google Scholar]
- 68.Dijkstra EA, Nilsson PJ, Hospers GAP et al (2023) Locoregional failure during and after short-course radiotherapy followed by chemotherapy and surgery compared to long-course chemoradiotherapy and surgery—five-year follow-up of the RAPIDO trial. Ann Surg 278:e766–e772 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Jin J, Tang Y, Hu C et al (2022) Multicenter, randomized, phase III trial of short-term radiotherapy plus chemotherapy versus long-term chemoradiotherapy in locally advanced rectal cancer (STELLAR). J Clin Oncol 40:1681–1692 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Zhang H, Li G, Cao K, Zhai Z, Wei G, Qu H et al (2022) Impact of total neoadjuvant therapy consisting of consolidation chemotherapy on locally advanced rectal cancer survival. Int J Colorectal Dis 37:1657–1668. 10.1007/s00384-022-04179-7 [DOI] [PubMed] [Google Scholar]
- 71.Chapman BC, Lai S, Friedrich T, Lieu CH, Moskalenko M, Olsen J et al (2022) Rectal cancer: clinical and molecular predictors of a complete response to total neoadjuvant therapy. Dis Colon Rectum. 10.1097/DCR.0000000000002245 [DOI] [PubMed] [Google Scholar]
- 72. Beets-Tan RGH, Lambregts DMJ, Maas M, Bipat S, Barbaro B, Curvo-Semedo L, et al (2016) Magnetic resonance imaging for clinical management of rectal cancer: updated recommendations from the 2016 European Society of Gastrointestinal and Abdominal Radiology (ESGAR) consensus meeting. Eur Radiol 2018;28:1465–75. [DOI] [PMC free article] [PubMed]
- 73.Awiwi MO, Kaur H, Ernst R, Rauch GM, Morani AC, Stanietzky N et al (2023) Restaging MRI of rectal adenocarcinoma after neoadjuvant chemoradiotherapy: imaging findings and potential pitfalls. Radiographics 43:e220135 [DOI] [PubMed] [Google Scholar]
- 74.Van Der Paardt MP, Zagers MB, Beets-Tan RG, Stoker J, Bipat S (2013) Patients who undergo preoperative chemoradiotherapy for locally advanced rectal cancer restaged by using diagnostic MR imaging: a systematic review and meta-analysis. Radiology 269:101–112 [DOI] [PubMed] [Google Scholar]
- 75.Pinta CDL, Martín M, Sempere C et al (2019) MRI value to predict pathologic staging in locally advanced rectal cancer after neoadjuvant chemoradiation. Turk J Colorectal Dis 29(1):39–45 [Google Scholar]
- 76.Habr-Gama A, Sao Juliao GP, Vailati BB, Sabbaga J, Aguilar PB, Fernandez LM et al (2019) Organ preservation in cT2N0 rectal cancer after neoadjuvant chemoradiation therapy: the impact of radiation therapy dose-escalation and consolidation chemotherapy. Ann Surg 269:102–107 [DOI] [PubMed] [Google Scholar]
- 77.Van Der Sande ME, Maas M, Melenhorst J, Breukink SO, Van Leerdam ME, Beets GL (2021) Predictive value of endoscopic features for a complete response after chemoradiotherapy for rectal cancer. Ann Surg 274:e541–7 [DOI] [PubMed] [Google Scholar]
- 78.Maas M, Lambregts DM, Nelemans PJ, Heijnen LA, Martens MH, Leijtens JW et al (2015) Assessment of clinical complete response after chemoradiation for rectal cancer with digital rectal examination, endoscopy, and MRI: selection for organ-saving treatment. Ann Surg Oncol 22:3873–3880 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79. Glynne-Jones R, Wyrwicz L, Tiret E, Brown G, Rödel C, Cervantes A, et al (2017) Rectal cancer: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 28:iv22–40. [DOI] [PubMed]
- 80.Battersby NJ et al (2017) A rectal cancer feasibility study with an embedded phase III trial design assessing magnetic resonance tumour regression grade (mrTRG) as a novel biomarker to stratify management by good and poor response to chemoradiotherapy (TRIGGER): study protocol for a randomised controlled trial. Trials 18:394 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81. Perez RO, Habr-Gama A, Sao Juliao GP, Gama-Rodrigues J, Sousa AH, Campos FG, et al (2012) Optimal timing for assessment of tumor response to neoadjuvant chemoradiation in patients with rectal cancer: do all patients benefit from waiting longer than 6 weeks? Int J Radiat Oncol Biol Phys. 2012;84(5):1159–65. [DOI] [PubMed]
- 82. Habr-Gama A, Sao Juliao GP, Fernandez LM, et al (2019) Achieving a complete clinical response after neoadjuvant chemoradiation that does not require surgical resection: it may take longer than you think! Dis Colon Rectum. 2019;62:802–8. [DOI] [PubMed]
- 83.Martens MH, Maas M, Heijnen LA, Lambregts DM, Leijtens JW, Stassen LP et al (2016) Long-term outcome of an organ preservation program after neoadjuvant treatment for rectal cancer. JNCI J Natl Cancer Inst 108(12):djw171 [DOI] [PubMed] [Google Scholar]
- 84. Hupkens BJ, Maas M, Martens MH, Van Der Sande ME, Lambregts DM, Breukink SO, et al (2018) Organ preservation in rectal cancer after chemoradiation: should we extend the observation period in patients with a clinical near-complete response? Ann Surg Oncol. 2018;25:197–203. [DOI] [PubMed]
- 85.Marchegiani F, Palatucci V, Capelli G et al (2022) Rectal sparing approach after neoadjuvant therapy in patients with rectal cancer: the preliminary results of the resarch trial. Ann Surg Oncol 29(3):1880–1889 [DOI] [PubMed] [Google Scholar]
- 86.Lynn PB, Strombom P, Garcia-Aguilar J (2017) Organ-preserving strategies for the management of near-complete responses in rectal cancer after neoadjuvant chemoradiation. Clin Colon Rectal Surg 30(5):395–403 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87. Perez RO, Habr-Gama A, Pereira GV, et al (2012) Role of biopsies in patients with residual rectal cancer following neoadjuvant chemoradiation after downsizing: can they rule out persisting cancer? Colorectal Dis. 2012;14(6):714–20. [DOI] [PubMed]
- 88.Duldulao MP, Lee W, Streja L (2013) Distribution of residual cancer cells in the bowel wall after neoadjuvant chemoradiation in patients with rectal cancer. Dis Colon Rectum 56(2):142–149 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.Smith FM, Wiland H, Mace A, Pai RK, Kalady MF (2014) Depth and lateral spread of microscopic residual rectal cancer after neoadjuvant chemoradiation: implications for treatment decisions. Colorectal Dis 16(8):610–615 [DOI] [PubMed] [Google Scholar]
- 90.López-Campos F, Martín-Martín M, Fornell-Pérez R, García-Pérez JC, Die-Trill J, Fuentes-Mateos R et al (2020) Watch and wait approach in rectal cancer: current controversies and future directions. World J Gastroenterol 26:4218–4239 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Van Der Valk MJM, Hilling DE, Bastiaannet E, Kranenbarg EMK, Beets GL, Figueiredo NL et al (2018) Long-term outcomes of clinical complete responders after neoadjuvant treatment for rectal cancer in the International watch & wait database (IWWD): an international multicentre registry study. Lancet 391:2537–2545 [DOI] [PubMed] [Google Scholar]
- 92.Georgiou P, Tan E, Gouvas N et al (2009) Extended lymphadenectomy versus conventional surgery for rectal cancer: a meta-analysis. Lancet Oncol 10:1053–1062 [DOI] [PubMed] [Google Scholar]
- 93.Dattani M, Heald RJ, Goussous G et al (2018) Oncological and survival outcomes in watch and wait patients with a clinical complete response after neoadjuvant chemoradiotherapy for rectal cancer: a systematic review and pooled analysis. Ann Surg 268:955–967 [DOI] [PubMed] [Google Scholar]
- 94.Cerdan-Santacruz C, Vailati B, Juliao GS, Habr-Gama A, Perez RO (2022) Watch and wait: why, to whom and how. Surg Oncol 43:101774 [DOI] [PubMed] [Google Scholar]
- 95.Fernandez LM, Sao Juliao GP, Figueiredo NL, Beets GL, Van Der Valk MJ, Bahadoer RR et al (2021) Conditional recurrence-free survival of clinical complete responders managed by watch and wait after neoadjuvant chemoradiotherapy for rectal cancer in the International Watch & Wait Database: a retrospective, international, multicentre registry study. Lancet Oncol 22(1):43–50 [DOI] [PubMed] [Google Scholar]
- 96.Probst CP, Becerra AZ, Aquina CT, Tejani MA, Hensley BJ, González MG et al (2016) Watch and wait? –Elevated pretreatment CEA is associated with decreased pathological complete response in rectal cancer. J Gastrointest Surg 20:43–52 [DOI] [PubMed] [Google Scholar]
- 97.Morais M, Pinto DM, Machado JC, Carneiro S (2022) CtDNA on liquid biopsy for predicting response and prognosis in locally advanced rectal cancer: a systematic review. Eur J Surg Oncol 48:218–227 [DOI] [PubMed] [Google Scholar]
- 98.Heald R, Beets G, Carvalho C (2014) Report from a consensus meeting: Response to chemoradiotherapy in rectal cancer—predictor of cure and a crucial new choice for the patient: on behalf of the Champalimaud 2014 Faculty for ‘Rectal cancer: When NOT to operate. Colorectal Dis 16:334–337 [DOI] [PubMed] [Google Scholar]
- 99.Juliao GS, Karagkounis G, Fernandez L, Habr-Gama A, Vailati B, Dattani M et al (2020) Conditional survival in patients with rectal cancer and complete clinical response managed by watch and wait after chemoradiation: recurrence risk over time. Ann Surg 272:138–144 [DOI] [PubMed] [Google Scholar]
- 100.Chadi S, Malcomson L, Ensor J, Riley RD, Vaccaro CA, Rossi GL et al (2018) Factors affecting local regrowth after watch and wait for patients with a clinical complete response following chemoradiotherapy in rectal cancer (InterCoRe consortium): an individual participant data meta-analysis. Lancet Gastroenterol Hepatol 3:825–836 [DOI] [PubMed] [Google Scholar]
- 101. Fernandez LMM, Figueiredo NLM, Habr-Gama AM, et al (2020) Salvage surgery with organ preservation for patients with local regrowth after watch and wait: is it still possible? Dis Colon Rectum. 2020;63:1053–1062. [DOI] [PubMed]
- 102.Habr-Gama A, Gama-Rodrigues J, Juliao GS et al (2014) Local recurrence after complete clinical response and watch and wait in rectal cancer after neoadjuvant chemoradiation: impact of salvage therapy on local disease control. Int J Radiat Oncol Biol Phys 88:822–828 [DOI] [PubMed] [Google Scholar]
- 103. Nasir I, Fernandez L, Vieira P, et al (2019) Salvage surgery for local regrowths in watch & wait – are we harming our patients by deferring the surgery? Eur J Surg Oncol. 2019;45:1559–1566. [DOI] [PubMed]
- 104. Smith FM, Ahad A, Perez RO, et al (2017) Local excision techniques for rectal cancer after neoadjuvant chemoradiotherapy: what are we doing? Dis Colon Rectum. 2017;60:228–239. [DOI] [PubMed]
- 105.Lefevre JH, Mineur L, Kotti S et al (2016) Effect of interval (7 or 11 weeks) between neoadjuvant radiochemotherapy and surgery on complete pathologic response in rectal cancer: a multicenter, randomized, controlled trial (GRECCAR-6). J Clin Oncol 34:3773–3780 [DOI] [PubMed] [Google Scholar]
- 106.Kong JC, Guerra GR, Warrier SK et al (2017) Outcome and salvage surgery following “watch and wait” for rectal cancer after neoadjuvant therapy: a systematic review. Dis Colon Rectum 60:335–345 [DOI] [PubMed] [Google Scholar]
- 107.Socha J, Kępka L, Michalski W (2020) The risk of distant metastases in rectal cancer managed by a watch-and-wait strategy – a systematic review and meta-analysis. Radiother Oncol 144:1–6 [DOI] [PubMed] [Google Scholar]
- 108.Fernandez LM, Juliao GPS, Renehan AG et al (2023) The risk of distant metastases in patients with clinical complete response managed by watch and wait after neoadjuvant therapy for rectal cancer: the influence of local regrowth in the international watch and wait database. Dis Colon Rectum 66:41–49 [DOI] [PubMed] [Google Scholar]
- 109.Cerdan-Santacruz C, São Julião GP, Vailati BB et al (2023) Watch and wait approach for rectal cancer. J Clin Med 12(8):2873 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110. Malakorn S, Yang Y, Bednarski BK, et al (2019) Who should get lateral pelvic lymph node dissection after neoadjuvant chemoradiation? Dis Colon Rectum. 2019;62:1158–1166. [DOI] [PubMed]
- 111.Ogura A, Konishi T, Cunningham C et al (2019) Neoadjuvant (chemo)radiotherapy with total mesorectal excision only is not sufficient to prevent lateral local recurrence in enlarged nodes: results of the multicenter lateral node study of patients with low cT3/4 rectal cancer. J Clin Oncol 37:33–43 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 112. Kim MJ, Kim TH, Kim DY, et al (2015) Can chemoradiation allow for omission of lateral pelvic node dissection for locally advanced rectal cancer? J Surg Oncol. 2015;111:459–464. [DOI] [PubMed]
- 113. Kim MJ, Park SC, Kim TH, et al (2016) Is lateral pelvic node dissection necessary after preoperative chemoradiotherapy for rectal cancer patients with initially suspected lateral pelvic node? Surgery. 2016;160:366–376. [DOI] [PubMed]
- 114.Peacock O, Manisundaram N, Dibrito SR et al (2022) MRI directed surgical decision making for lateral pelvic lymph node dissection in rectal cancer after total neoadjuvant therapy (TNT). Ann Surg 276:654–664 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The data generated and analyzed in this Delphi consensus study consist of anonymized expert panel responses. Due to the nature of the Delphi methodology and the requirement to preserve participant confidentiality, the raw datasets cannot be made publicly available. De-identified, aggregate data supporting the findings of this study may be available from the corresponding author upon reasonable request, subject to approval by the study investigators and in compliance with confidentiality agreements.