Abstract
Background: The article by Feachem et al, published in the BMJ in 2002, claimed to show that, compared with the United Kingdom (UK) National Health Service (NHS), the Kaiser Permanente healthcare system in the United States (US) has similar healthcare costs per capita, and performance that is considerably better in certain respects.
Aim: To assess the accuracy of Feachem et al's comparison and conclusions.
Method: Detailed re-examination of the data and methods used and consideration of the 82 letters responding to the article.
Results: Analyses revealed four main areas in which Feachem et al's methodology was flawed. Firstly, the populations of patients served by Kaiser Permanente and by the NHS are fundamentally different. Kaiser's patients are mainly employed, significantly younger, and significantly less socially deprived and so are healthier. Feachem et al fail to adjust adequately for these factors. Secondly, Feachem et al have wrongly inflated NHS costs by omitting substantial user charges payable by Kaiser members for care, excluding the costs of marketing and administration, and deducting the surplus from Kaiser's costs while underestimating the capital charge element of the NHS budget and other costs. They also used two methods of converting currency, the currency rate and a health purchasing power parity conversion. This is double counting. Feachem et al reported that NHS costs were 10% less per head than Kaiser. Correcting for the double currency conversion gives the NHS a 40% cost advantage such that per capita costs are $1161 and $1951 for the NHS and Kaiser, respectively. Thirdly, Feachem et al use non-standardised data for NHS bed days from the Organisation for Economic Cooperation and Development, rather than official Department of Health bed availability and activity statistics for England. Leaving aside the non-comparability of the population and lack of standardisation of the data, the result is to inflate NHS acute bed use and underestimate the efficiency of performance by at least 10%. Similar criticisms apply to their selective use of performance measures. Finally, Feachem et al claim that Kaiser is a more integrated system than the NHS. The NHS provides health care to around 60 million people free at the point of delivery, long-term and psychiatric care, and continuing care after 100 days whereas Kaiser provides care to 6 million people, mainly employed and privately insured. Important functions, such as health protection, education and training of healthcare professionals, and research and development are not included or properly costed in Feachem et al's integrated model.
Conclusion: We have re-examined the statements made by Feachem et al and show that the claims are unsupported by the evidence. The NHS is not similar to Kaiser in coverage, costs or performance.
Keywords: costs and cost analysis; health care quality; health services; national health service; personal health service; quality indicators, health care
Introduction
IN January 2002, the BMJ published an article that aimed to ‘compare the costs and performance of the [National Health Service] NHS with those of an integrated system for financing and delivery of health services (Kaiser Permanente) in California.’1 The article claimed to show that ‘Kaiser achieved better performance at roughly the same cost as the NHS’. Kaiser's members were said to experience ‘more comprehensive and convenient primary care services and much more rapid access to specialist services and hospital admissions.’ Furthermore, Kaiser's use of acute hospital beds was purported to be considerably lower than that of the NHS.
The article has become important in United Kingdom (UK) government policy making. The Treasury's review of NHS funding2 and the white paper for England, Delivering the NHS plan3 refer favourably to it, and to the Kaiser ‘model’ of care. Kaiser has also been invited to work with the NHS to help modernise services.4 In November 2003, the Secretary of State for Health in England, John Reid, addressed the National Association of Primary Care in the UK under the banner ‘Learning from Kaiser Permanente: how can the NHS make better use of its resources and improve patient care?’
Given the prominence of the Kaiser model in NHS policy, we now re-examine the methodology used to compare Kaiser with the NHS, and discuss the many biases that invalidate the conclusions drawn by Feachem et al.
Similar healthcare systems?
Feachem et al set the scene for the comparison by stating, ‘In many ways Kaiser Permanente is like the NHS’ on the basis of historical age and the fact that both organisations provide both primary and secondary services. However, they ignored major differences.
Kaiser
Kaiser is a health maintenance organisation (HMO), combining a system of private voluntary insurance and user charges with the delivery of health services. It provides care to a small proportion of the United States (US) population, in a country where approximately one person in six of the population has no healthcare insurance.
The value system is actuarial, in that healthcare benefits are provided to ‘members’ in return for premiums paid, on the basis of individual risk. Its patient population is highly selected, being employment based; that is, there is a ‘healthy worker’ effect.
Employees are offered a wide range of health plans that are linked to price. Furthermore, in some plans Kaiser does not provide care for chronic serious mental illness, care of the elderly is variable, and some care, such as that for a chronic illness, ceases altogether after 100 days.1,5
HOW THIS FITS IN
What do we know?
The United Kingdom (UK) National Health Service (NHS) provides universal health care on the basis of need, without reference to ability to pay, to the entire population of around 60 million people. Kaiser Permanente (California) is a health maintenance organisation in the United States (US). It combines a funding system largely based on private voluntary insurance and user charges with the delivery of healthcare to a highly selected population of 6 million people in California, mainly employed and younger retired people. Comparison of healthcare systems requires that rigorous attention be paid to ensuring the comparability of the populations, standardisation and classification of data on bed utilisation, performance measures, and costs.
What does this paper add?
The article by Feachem et al, published in the BMJ in 2002 introduced serious errors and bias into the methodology. The claim of Feachem et al that the Kaiser Permanente healthcare system has similar healthcare costs per capita, and a performance that is considerably better in certain respects when compared with the UK NHS, is not supported by the evidence.
NHS
The NHS, by contrast, is a national system operating throughout the whole of the UK; that is, serving a population approximately ten times that covered by Kaiser in California. The value system of the UK NHS is that health care is a human right, guaranteed to every citizen by government.
Although the NHS is organised into separate primary care, community- and hospital-based services, the goal continues to be universal, comprehensive health care, provided regardless of the patient's ability to pay. NHS care extends to remote rural areas and islands and, in particular, the NHS covers the unemployed, the homeless, and other socially disadvantaged groups. It includes substantial services for patients with serious chronic mental illness. It makes no charges to patients for seeing any doctor, or for childbirth. It gives a lifelong guarantee of access to care to every single citizen, however long lasting or serious his or her medical condition.
Thus, the claim that ‘in many ways Kaiser is like the NHS’ in its healthcare system has not been, and cannot be, substantiated.
Similar populations?
The NHS provides health care to all 59.5 million residents of the UK. Kaiser insures and provides healthcare to its 8.1 million members in the US; that is, 2.8% of the total population of the US (288 million people).6 These are two very different populations.
Age, poverty, and low socioeconomic status are well recognised as being associated with poor health and greater health service use, both in the UK and the US.7-13 Feachem et al make some attempt to adjust for population differences in age, insurance, and socioeconomic status, but these are inadequate and it is of major academic concern that ‘like is not being compared with like’; that is, ‘apples are being compared with oranges’.14
Adjustments for age
The age–sex analysis reported by Feachem et al shows Kaiser's population to be significantly younger than that of the NHS (Figure 1). Kaiser's members include a lower proportion of people aged over 65 years (Kaiser 10.2% versus NHS 15.6%) and aged over 75 years (Kaiser 3.9% versus NHS 7.3%).1 Further evidence of Kaiser's selection bias is that death rates among Kaiser's population are only 6.7 per thousand compared with a death rate of 10.6 per thousand among the UK population in 1998.15
Figure 1.
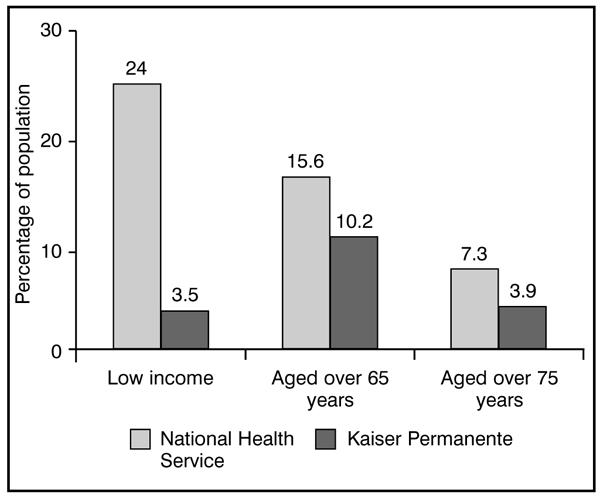
Comparison of National Health Service (UK) population and Kaiser Permanente's (California, US) membership: proportion of people on low incomes and older people aged over 65 and over 75 years.
To adjust for age differences, the authors used English figures for costs per adult in different age groups, but these data were inadequate to make an adjustment (Table 1). This is important because older people have more morbidity and are the highest users of Western healthcare systems; for example, people aged over 75 years in the UK consult with their general practitioner (GP) on average seven times a year.16 It is also well known that the final year of life attracts additional costs to any healthcare system.17
Table 1.
Errors made in the adjustment of costs for differences between the National Health Service (UK) and Kaiser Permanente (California).
| Adjustments made by Feachem et al | ||||
|---|---|---|---|---|
| NHS (UK) | KP (US) | Errors in adjustments | Effect on costs | |
| Gross expenditures/revenue | £58 500 m | $14 200 m | ||
| Adjustments for differences in | ||||
| Capital depreciation | −£1000 m | −$557 m | Cost of capital in the NHS underestimated by £2 billion.a | Increase NHS costs |
| Profits (more correctly surplus) | £0 | −$668 m | NHS equivalent of ‘profits’ is capital charges, consisting of depreciation and dividends payable on capital. The dividend element in NHS capital charges are not deducted from NHS costs. | Reduce KP costs |
| Adjustments for differences in benefits | ||||
| Dental care | −£1190 m | −$10 m | Deduction for NHS (UK) dental costs refers to England only. | Increase NHS costs |
| Long-term psychiatric care | −£3250 m | $0 | Costs for NHS long-term psychiatric care not found in reference cited. | Unknown |
| Other services | User charges for healthcare services not included in Kaiser's costs. No deduction from NHS costs for wider services not provided by Kaiser. | Reduce KP costs | ||
| Increase NHS costs | ||||
| Supplementary private health insurance | +£2630 m | $0 | No adjustment to Kaiser's costs for supplementary insurance taken out by their members (up to 12% of members insure for care outside the health plan).21 | Reduce KP costs |
| Adjustments for differences in special activities/circumstances | ||||
| Indirect service obligations | −£3587 m | −$497 m | Indirect costs integral to a health system should not have been deducted: indirect costs borne by US public health authorities should have been added to Kaiser's costs. | Reduce KP costs |
| Administrative costs | £0 | −$586 m | No deduction for NHS administrative costs. £1.9 billion should be deducted for England, with further deductions for Scotland, Wales and Northern Ireland.32 | Reduce KP costs |
| Increase NHS costs | ||||
| Net expenditure after adjustments | £52 103 m | $11 900 m | ||
| Per capita expenditure | £876 | $1951 | ||
| Adjustment for differences in medical cost environment: | ||||
| Conversion at rate of exchange | Multiply by 1.6 £876 to $1402 | $0 | Conversion of £ to $ should have been either in purchasing power parity at 1.52 or at market exchange rate of 1.6, but not both. | Increase NHS costs |
| Conversion at health sector | Multiply by 1.52 | Purchasing power parity health sector cost conversion of 1.52 not found in reference cited. | ||
| Purchasing power parity | $1402 to $2130 | $0 | ||
| Adjustment for differences in populations | ||||
| Age | −$260 | $0 | NHS age-specific per-capita costs used to reduce NHS costs by 12.2%. Age-specific per capita costs cited by the authors:18
|
Increase NHS costs |
| Socioeconomic group | −$106 | $0 | NHS per capita costs reduced by 5% using data from a study of the family expenditure survey:
|
Increase NHS costs |
The authors state that many American patients aged over 65 years, funded by the state Medicare system, choose Kaiser because it is a comprehensive package of care. They imply that they receive similar benefits to those received by older people through the NHS. This suggestion cannot be substantiated. Even when the proposed new Medicare benefits are introduced in 2006, older US patients will still have to pay 12 monthly premiums of $35; a total of $420 (approximately £280 per year) plus the first $250 of all drug costs, plus 25% of further drug costs up to $2250.18 In contrast, UK patients aged over 60 years (who use the majority of prescriptions) continue to receive all of their prescribed drugs for free. On the basis that the national average number of items prescribed for older UK patients was 26.5 per year in 1999–2000,19 and using an average cost of £11 per item, the NHS provides a cost advantage of at least £291 per patient per year for drugs alone, and far more under current arrangements. Feachem et al ignore this.
In the NHS, almost a quarter (23%) of all general practitioner contacts with patients aged over 75 years are in the patient's home;20 it is not clear whether Kaiser offers an equivalent service. There is also recent evidence from the US that organisations like Kaiser are finding ways to attract only ‘healthy’ elderly members who are less likely to need hospitalisation.21
Insured status
The UK has not considered insured and uninsured populations in relation to health care since 1948. Thus, most British citizens aged 56 years or under have no personal experience of not being insured for healthcare, and the extensive US literature on the subject has therefore not been of interest in the UK. However, it is central in a comparative study of the UK NHS and US Kaiser.
Feachem et al make it clear that Kaiser does have some dealings with some patients without health insurance, stating ‘Kaiser does however provide care to non-members; for example, 5% of all admissions to Kaiser community hospitals. Many of these are uninsured.’ However, they do not report exactly how many of the uninsured they treat, how extensive their care is, or how their care is costed and funded.
Feachem et al argue that, ‘the lower representation of poor and uninsured people among Kaiser's members does not give Kaiser a cost advantage’. This contradicts the large body of work in the US regarding the uninsured, which has been reviewed by the Institute of Medicine, an independent organisation providing scientific advice on health in the US. The Institute of Medicine has recently published evidence that the uninsured in the US are considerably less healthy than the insured; with as much as 25% higher standardised mortality rates.22 This places Kaiser, which covers an insured population rather than the unselected whole population of a nation, at a considerable cost advantage to the NHS.
Employment and socioeconomic status
The authors do not adjust for employment status, despite this having considerable implications for an individual's health status and their access to health care.23 People who have serious physical or mental disabilities, learning difficulties, personality disorders, alcoholism, or who are homeless, asylum seekers, travellers, those who are living chaotic lives, or who have a criminal record are less likely to be in regular employment, and so are less likely to be included on Kaiser's list of members. But these vulnerable patient groups with poorer health provide considerable challenges to healthcare organisations and professionals who provide care for them. Hence, Kaiser has a selected population of patients; largely excluding the most deprived proportion of the population, and is biased towards more stable, healthier, and easier to care for people.
Feachem et al's adjustment for differences in socioeconomic status is fundamental to ensuring the comparability of the study. They reduce NHS costs by 5% on the basis of a figure published by the Office for National Statistics, derived from the UK family expenditure survey.24 However, this survey neither collects data on NHS costs nor examines expenditure in relation to socioeconomic status.
Thus the claim that, ‘Kaiser is like the NHS’ does not hold with respect to the populations served.
Similar services?
Feachem et al overlook key service differences and, in doing so, introduce a number of methodological errors that all work in favour of Kaiser (Table 1).
Consultation charges paid by patients
Feachem et al rightly took into account the charges payable by patients for obtaining prescriptions. However, they ignored other, higher charges to Kaiser members; up to $50 (£28) every time patients see their primary care practitioner or attend hospital outpatient clinics, approximately $85 (£56) every time they attend the emergency centre, and up to $500 (£285) when they are admitted for childbirth.5 Some Kaiser members (12%) take extra private health insurance to cover for these additional costs and elements of care that are not covered by the health plan.25
These ‘hidden costs’, called ‘cost sharing’ or ‘co-payments’ in the US, are borne by Kaiser's members, in order to enable Kaiser to keep its own costs down. Those using the NHS pay none of these charges. The authors chose not to adjust for them in the comparison, but did include the costs of private insurance taken out by ‘members’ of the NHS. The effect was to over-inflate the relative costs of the NHS.
Integrated systems
Feachem et al emphasise the word ‘integrated’ in relation to the Kaiser system. They conclude by describing Kaiser's ‘integration throughout the system’, as one of the reasons for its purported superior performance. However, they do not define what they mean by the term ‘integration’. The authors appear to approach integration from the perspective of specialist clinical services. However, they do not properly consider the main strengths of the NHS.
The Shorter Oxford English Dictionary defines integration as ‘combined into a whole, united, undivided.’26 Although the newly formed NHS of 1948 continued the separation of primary care services from community- and hospital-based services, the aim of the NHS continues to be universal, comprehensive health care, provided regardless of the patient's ability to pay, and available across the UK. In contrast, Kaiser provides care to a highly selected group of patients, largely on the basis of ability to pay.
The authors' approach to the term integration, in failing to recognise the key principles of universal comprehensive care, introduced biases to the cost comparison. From the outset, the NHS was planned so that clinical care would not be delivered in isolation from education, training, research and development, and the work of statutory and regulatory bodies concerned with health care and the prevention and control of disease. In the NHS, these costs are integral to its functioning and amount to approximately £7 billion.27
The authors did not take proper account of the integrated nature of these services when it made its cost comparisons. Kaiser does educate and train healthcare professionals but the cost is borne by the Federal and State governments in the US and not from Kaiser's own budget. In our view, these services are integral and an estimate of these additional services should have been made and included in the costs. In contrast, the authors chose to remove Kaiser's considerable expenditure on sales, marketing, malpractice insurance, and risk-adjusted pricing despite these being integral to Kaiser's system. These should also have been included in the comparison.
A recent analysis by Leatherman et al also shows how the NHS system is more efficient than the multiple US systems.28 The NHS encourages investments for health gain, for both individual patients and society. In contrast, some quality of care programmes, including health promotion and disease prevention, may not represent ‘good investments’ in the US market system of privately run healthcare organisations, since the benefits (financial rewards) often fall to the insurer (Medicare, for example), rather than the provider; that is, perverse incentives operate.
Accounting errors and double counting
Kaiser's financial surplus
The authors describe Kaiser as a ‘not-for-profit’ organisation,29 however, this is not strictly the case. Kaiser can pass on profits directly to its doctor-shareholders through Permanente Medical Groups, a separate arm providing medical care. Furthermore, profits may be passed indirectly to ‘for-profit’ providers, subcontracted by Kaiser Health Plan to provide certain services. Hence, Kaiser's financial surplus (the authors term this ‘profit’) can be reinvested in its operations and/or returned to its doctor-shareholders as financial incentives. In addition to issues relating to possible conflicts of interest, this annual surplus is part of Kaiser's operating costs. It was, therefore, an accounting error to remove Kaiser's $668 million surplus from their overall costs (as the authors did in their Table 1). The surplus is derived from the money paid by Kaiser members in subscriptions and charges. Correcting this error alone increases Kaiser's costs by about $100 per person.30
NHS capital charges and the costs of capital
Alternatively, the NHS equivalent of surplus could have been deducted from NHS costs, namely the surplus it has to make and pay to the UK Treasury annually in the form of capital charges. A further £1.6 billion would need to be deducted from the NHS costs (see footnote to Table 1). Feachem et al accounted for the ‘costs of capital’ by deducting £1000 million for NHS capital depreciation and £348 million ($557 million) for Kaiser. It is not clear why these were excluded from the analysis when capital costs (‘greater investment in information technology’) were one of the reasons given for Kaiser's purported superior performance.
Other major elements of the true ‘cost of capital’ were not considered within either system; for example, the authors did not take into account the costs to the NHS for expenditure on GP premises schemes and private finance initiative schemes, which account for almost £400 million a year (Table 1).
The currency conversion
Kaiser's costs were obtained in US dollars and UK NHS costs in pounds sterling. Obviously, there has to be a process of conversion.
There are three different methods of doing this: using a currency conversion rate, the purchasing power parity rate, or the healthcare sector purchasing power parity rate. We do not need to detail the theoretical case to determine which method is optimum, and are tolerant of using any one of these methods. But Feachem et al report first converting the currency at the then published value and then, in addition, they apply the healthcare sector purchasing parity factor of 152%.
Dr Clive Smee, the then Chief Economist of the Department of Health, describes it as ‘simply wrong to adjust for healthcare prices over and above adjusting for general difference in prices’. We agree with Dr Smee that this is a form of arithmetical double counting that biases the figures in Kaiser's favour. The impact of this second financial conversion is dramatic. Feachem et al report that NHS costs are 10% less per head. Correcting for the improper use of the double currency conversion gives the NHS a 40% cost advantage of $1161 per person for the NHS compared with Kaiser's per person costs of $1951. Thus, although the remaining cost adjustments still operate to the disadvantage of the NHS, it still costs significantly less than Kaiser.
Misunderstanding NHS data
Counting hospital beds
Feachem et al rely on Organisation for Economic Cooperation and Development (OECD) data for counting hospital beds in the NHS, rather than the standard official bed statistics for England. There are considerable discrepancies between derivative OECD data and official NHS bed availability and activity statistics for England.
As Nigel Edwards, the Director of Policy for the NHS Confederation, points out, Feachem et al's figures of 1000 NHS bed days per 1000 population per year must be an overestimate of NHS bed use. As he points out, ‘If every [NHS] bed was full on every day of the year with no gap … of more than 1 day the maximum number of bed days … would be 897… even allowing for the use of corridors, 1000 [NHS] bed days … appears to be a fiction’. Edwards fears that important lessons about bed use may be lost using weak and inaccurate statistics.33 Feachem et al's claim that differences in bed use is one of the main reasons that Kaiser is more efficient and integrated than the NHS cannot be supported by the data. A recent analysis that purports to show that Kaiser uses fewer hospital bed days than the NHS, again fails to take proper account of the non-comparability of the populations.34
Quality markers
The assessment of quality of care in health systems has attracted worldwide interest, with conferences, books, and journals now regularly appearing exclusively on this subject. There are hundreds of indicators available. In studies of this kind, the appropriate methodology is to use a widely accepted framework for measuring quality, or for a neutral external authority to choose quality markers that assess a broad range of quality measures.35-37 According to the Royal Statistical Society Working Party, ‘performance monitoring done well is broadly productive for those concerned. Done badly, it can be very costly and not merely ineffective, but harmful and indeed destructive’.38
In their study, Feachem et al arbitrarily selected nine indicators out of the many hundreds available, without providing a reason for their choice. Furthermore, as noted by Professor Andrew Bindman in his BMJ USA editorial, ‘the methods for collecting information on quality were neither standardised nor audited across the health systems, nor were the results adjusted for the large measured differences in the patient populations’.39
Feachem et al's choice of indicators operate generally to Kaiser's advantage (Table 2). They need to be considered in relation to the core NHS principles of universal access and services provided free at the point of delivery. In the US, millions of people experience the fear of losing healthcare insurance cover, owing to low-paid employment or chronic long-term illness, the anxiety of choosing different healthcare plans at different stages of life, the non-transferability of medical records, difficulty in accessing and affording medical services on low incomes, limited range or reducing healthcare benefits after 100 days, and a cap on medication available. Feachem et al did not use these principles, or indeed mention them, in deriving a quality framework against which to evaluate the systems.
Table 2.
Errors made in the comparison of performance between the National Health Service (UK) and Kaiser Permanente (California).
| Performance measures compared | Errors in comparisons | Effect on conclusions |
|---|---|---|
| Inputs | ||
| Specialists per 100 000 people | No comparison made of primary and community care:
|
No evidence to support claim that ‘Kaiser's members experience more comprehensive and convenient primary care services’ |
| Primary care facilities | Geographic access not examined | |
| Use of inpatient beds | UK bed data based on spurious OECD source | Increase apparent NHS bed use by at least 10% |
| Kaiser's data unpublished | ||
| No adjustment for age, socioeconomic status, or health status | ||
| Bed classification systems not comparable | ||
| Access and responsiveness | ||
| Primary care | Equity of access not examined | Core objective of NHS (equity) not examined |
| Time spent with primary care doctor not adjusted for different working practices (US specialists in primary care versus NHS GPs) | Reduce NHS performance | |
| For NHS based on 1992/1993 survey | ||
| Specialist referral | Waiting time data:
|
|
| Patient convenience | Differences in prescribing practices not adjusted for | Reduce NHS performance |
| Quality | ||
| Vaccination, cancer screening, diabetic care, cardiovascular care, transplantations per 100 000 | Outcomes of care not examined | Only limited aspects of quality compared |
| Comparison unadjusted for socioeconomic status | Data lacks validity | |
| Vaccination and screening rates presented for Kaiser's members in US not California | Reduce NHS performance | |
| Data for NHS diabetic care not found in cited reference | ||
| Data for NHS (UK) cardiovascular care cited as 1998, but refer to deprived inner London borough between 1988 and 1997 | ||
OECD = Organisation for Economic Cooperation and Development; NHS = National Health Service.
Feachem et al make a series of claims that the Kaiser system is superior to the NHS system. They imply that Kaiser is successful and generally superior to the other US systems. The article makes no reference to difficulties, let alone failures, of Kaiser in the US. For example, Gitterman et al, writing about Kaiser's financial losses and failures in expansion, say, ‘Kaiser is concentrated in urban areas in California … It is likely that certain markets, such as most rural or commuter areas, may not have the geographic conditions to sustain a profitable private sector prepaid group plans’ [authors' italics].40
Furthermore, in 2003 the California Institute for Health Systems Performance published a consumer guide ranking the quality of care in 181 hospitals across California. The score was based on the recent hospital experiences of 35 000 patients, and included a survey of patients' experiences with respect to patient preferences, coordination of care, information and education, physical comfort, emotional support, involvement of family and friends, and transition to home. Kaiser accounted for 27 hospitals out of the 181 surveyed, and 11 of them were rated below average for quality of care, whereas the remainder were only rated average.41
Conclusion
Feachem et al's article appeared in January 2002, and has attracted an unusual amount of attention and citations (with 82 rapid responses in the BMJ alone42). The NHS has funded teams from primary care trusts in England to travel to California to study the Kaiser system. More recently, John Reid has stated ‘there are five lessons we can learn from Kaiser — keeping patients out of hospital, active management of patients, self care and shared care, and the use of information, but most notably how to increase integration’.43
Benchmarking is a useful way of identifying issues of importance and facilitating analysis. We agree that some of the features of the Kaiser system are desirable for patients and represent higher quality care than is available from the NHS; for example, providing 20 minutes for primary care consultations and a higher ratio of doctors to patients. Nevertheless, Feachem et al make a number of other claims that our analysis shows cannot be substantiated.
Comparing how different healthcare systems work can generate new ideas in providing care, but this work is complex and easily subject to bias and error.
We have re-examined the striking statements made by Feachem et al and show that they are unsupported by the evidence.
Conflict of interest
D Pereira Gray holds a consultancy with the St Leonard's Research Practice and is an honorary elected Foreign Associate Member of the Institute of Medicine, Washington, DC, US.
Acknowledgments
We would like to thank Dr Jean Shaoul, Dr James Lancaster, Professor Colin Leys, Professor Azeem Majeed, Professor Alison Macfarlane and Professor Alan Maynard in the UK; Professor Andy Bindman, Dr Kevin Grumbach, Professor Charlene Harrington and Dr Freddy Chen, our US colleagues; and David Rowland, Sylvia Godden, and David Price in the Public Health Policy Unit. The library and information service of the RCGP provided helpful information.
References
- 1.Feachem RGA, Sekhri NK, White KL. Getting more for their dollar: a comparison of the NHS with California's Kaiser Permanente. BMJ. 2002;324:135–143. doi: 10.1136/bmj.324.7330.135. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.HM Treasury Health Trends Review Team. Securing our future health: taking a long-term view. Final report. London: HMSO; 2002. http://www.hm-treasury.gov.uk/wanless/ (accessed 30 Apr 2004) [Google Scholar]
- 3.Department of Health. Delivering the NHS plan. Next steps on investment, next steps on reform. London: The Stationery Office; 2002. [Google Scholar]
- 4.US groups to work with PCTs on pilot project. Health Serv J. 2002;112:5. Anonymous. [Google Scholar]
- 5.Kaiser Permanente. California health plans. http://pubappl2.kp.org/smallbusiness/smallbusiness/literature/sbTraditionalPlan2004.pdf (accessed 12 May 2004)
- 6.US Census Bureau. Population estimates. 2001. Jul 1, http://eire.census.gov/popest/data/states/tables/NST-EST2003-01.php (accessed 11 May 2004)
- 7.Black D, Morris J, Smith C, Townsend P. Inequalities in health: a report of a research working group. London: Department of Health and Social Security; 1980. [Google Scholar]
- 8.Acheson D. Independent inquiry into inequalities in health report. London: The Stationery Office; 1998. http://www.archive.official-documents.co.uk/document/doh/ih/ih.htm (accessed 30 Apr 2004) [Google Scholar]
- 9.Department of Health. Saving lives: our healthier nation. London: The Stationery Office; 1999. http://www.archive.official-documents.co.uk/document/cm43/4386/4386.htm (accessed 30 Apr 2004) [Google Scholar]
- 10.Pappas G, Queen S, Hadden W, Fisher G. The increasing disparity in mortality between socioeconomic groups in the United States, 1960 and 1986. N Engl J Med. 1993;329:103–109. doi: 10.1056/NEJM199307083290207. [DOI] [PubMed] [Google Scholar]
- 11.Kaplan G, Pamuk E, Lynch J, et al. Inequality in income and mortality in the United States; analysis of mortality and potential pathways. BMJ. 1996;312:999–1003. doi: 10.1136/bmj.312.7037.999. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Backlund E, Sorlie PD, Johnson NJ. The shape of the relationship between income and mortality in the United States. Evidence from the National Longitudinal Mortality Study. Ann Epidemiol. 1996;6:12–20. doi: 10.1016/1047-2797(95)00090-9. [DOI] [PubMed] [Google Scholar]
- 13.Majeed A, Bardsley M, Morgan D, et al. Cross sectional study of primary care groups in London: association of measures of socioeconomic and health status with hospital admission rates. BMJ. 2000;321:1057–1060. doi: 10.1136/bmj.321.7268.1057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Anilkulmar AC. Apples and Oranges [Rapid response] BMJ. 2002 Jan. http://bmj.bmjjournals.com/cgi/eletters/324/7330/135#18848 (accessed 30 Apr 2004) [Google Scholar]
- 15.Hughes T. If it seems too good to be true, maybe it isn't [Rapid response] BMJ. 2002 Jan. http://bmj.bmjjournals.com/cgi/eletters/324/7330/135#19074 (accessed 30 Apr 2004) [Google Scholar]
- 16.Office for National Statistics Social Survey Division. Living in Britain: results from the General Household Survey 1998. London: The Stationery Office; 2000. http://www.statistics.gov.uk/lib2000/resources/fileattachments/ghs98.pdf (accessed 30 Apr 2004) [Google Scholar]
- 17.Lubitz JG, Riley GF. Trends in Medicare payments in the last year of life. N Engl J Med. 1993;328:1092–1096. doi: 10.1056/NEJM199304153281506. [DOI] [PubMed] [Google Scholar]
- 18.Reid T. Bush set for victory with Medicare bill. The Times. 2003;25 Nov:14. [Google Scholar]
- 19.Department of Health. Prescriptions dispensed in the community. Statistics for 1990-2000. London: Department of Health; 2001. [Google Scholar]
- 20.National Statistics. Living in Britain: results from the 2000 General Household Survey. London: The Stationery Office; 2001. http://www.statistics.gov.uk/lib2000/resources/fileattachments/ghs2000.pdf (accessed 30 Apr 2004) [Google Scholar]
- 21.Morgan RO, Virnig BA, DeVito CA, Persily NA. The Medicare-HMO revolving door — the healthy go in and the sick go out. N Engl J Med. 1997;337:169–175. doi: 10.1056/NEJM199707173370306. [DOI] [PubMed] [Google Scholar]
- 22.Institute of Medicine. Hidden costs, value lost: uninsurance in America. Washington: National Academies Press; 2003. Committee on the Consequences of Uninsurance; p. 106. [PubMed] [Google Scholar]
- 23.Smith P, Sheldon TA, Carr Hill RA, et al. Allocating resources to health authorities: results and policy implications of small area analysis of use of inpatient services. BMJ. 1994;309:1050–1054. doi: 10.1136/bmj.309.6961.1050. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Lakin C. The effects of taxes and benefits on household income, 1999–2000. London: Office for National Statistics; 2001. [Google Scholar]
- 25.Himmelstein D, Woolhandler S. War is peace. Freedom is slavery. US HMOs are more efficient than the NHS [Rapid response] BMJ. 2002 Feb. http://bmj.bmjjournals.com/cgi/eletters/324/7330/135#19418 (accessed 30 Apr 2004) [Google Scholar]
- 26.Little W, Trumble W, Brown L, editors. Shorter Oxford English Dictionary. Oxford: Oxford University Press; 2002. [Google Scholar]
- 27.Department of Health. The Government's expenditure plans. Departmental report 2003. London: The Stationery Office; 2003. http://www.dh.gov.uk/assetRoot/04/07/24/08/04072408.pdf (accessed 30 Apr 2004) [Google Scholar]
- 28.Leathermann S, Berwick D, Iles D, et al. The business case for quality: case studies and an analysis. Health Aff (Millwood) 2003;22:16–30. doi: 10.1377/hlthaff.22.2.17. [DOI] [PubMed] [Google Scholar]
- 29.Maltby P. Promoting the public interest. Interim report on public interest companies. London: Institute for Public Policy Research; 2002. pp. 9–15. [Google Scholar]
- 30.Wilding TC. Article should not be published in its present form. [Rapid response] BMJ. 2003 Jan 23; http://bmj.bmjjournals.com/cgi/eletters/324/7330/135#18950 (accessed 30 Apr 2004) [Google Scholar]
- 31.House of Commons Health Committee. Public expenditure on health and personal social services 2001. London: The Stationery Office; 2001. [Google Scholar]
- 32.Smee C. What have we really learned from the NHS Kaiser comparison? [Rapid response] BMJ. 2002 Feb. http://bmj.bmjjournals.com/cgi/eletters/324/7330/135#19161 (accessed 30 Apr 2004) [Google Scholar]
- 33.Edwards N. Major errors in the bed day calculation [Rapid response] BMJ. 2002 Feb. http://bmj.bmjjournals.com/cgi/eletters/324/7330/135#19366 (accessed 30 Apr 2004) [Google Scholar]
- 34.Ham C, York N, Sutch S, Shaw R. Hospital bed utilisation in the NHS, Kaiser Permanente, and the US Medicare programme: analysis of routine data. BMJ. 2003;327:1257–1260. doi: 10.1136/bmj.327.7426.1257. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Donabedian A. The quality of care: how can it be assessed? JAMA. 1988;260:1743–1748. doi: 10.1001/jama.260.12.1743. [DOI] [PubMed] [Google Scholar]
- 36.Maxwell R. Dimensions of quality revisited: from thought to action. Qual in Health Care. 1992;1:171–177. doi: 10.1136/qshc.1.3.171. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.McColl A, Roderick P, Gabbay J, et al. Performance indicators for primary care groups: an evidence-based approach. BMJ. 1998;317:1354–1360. doi: 10.1136/bmj.317.7169.1354. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Royal Statistical Society Working Party on Performance Monitoring in the Public Services. Performance indicators: good, bad and ugly. London: Royal Statistical Society; 2003. [Google Scholar]
- 39.Bindman A. Whose health care is more efficient — fuzzy math obscures comparison of US and UK. BMJ. 2003;327:E96–E98. [Google Scholar]
- 40.Gitterman DP, Weiner BJ, Domino ME, et al. The rise and fall of a Kaiser Permanente expansion region. The Millbank Quarterly. 2003;81:567–601. doi: 10.1046/j.0887-378X.2003.00295.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.California Institute for Health Systems Performance. What patients think of California hospitals. Oakland: California Healthcare Foundation; 2003. [Google Scholar]
- 42.BMJ. Rapid responses to: Feachem RGA, Sekhri NK, White KL. Getting more for their dollar: a comparison of the NHS with California's Kaiser Permanente. BMJ. 2002;324:135–143. doi: 10.1136/bmj.324.7330.135. http://bmj.bmjjournals.com/cgi/eletters/324/7330/135 (accessed 4 May 2004) [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Reid J. London: Department of Health; 2003. Nov 4, Learning from the market — not copying it [Speech] [Google Scholar]


