Abstract
Background
Interleukin (IL)-13 can modulate tumor immunosurveillance. The interplay between IL-13 and immunotherapy outcomes has not been well elucidated.
Methods
IL-13 expression was evaluated by tumor RNA sequencing (514 tumors; advanced/metastatic cancers). Transcripts were normalized to internal housekeeping genes and standardized relative to a reference population (735 tumors; 35 histologies) and ranked as percentile values: IL-13-high (75th–100th percentile) and non-high (0–74th percentile).
Results
Overall, 39.7% of 514 patients were men; median age, 61 years; 489 had clinical data annotation (217 immunotherapy treated; 272, immunotherapy naïve). Eighty-three of 514 patients (16.1%) showed high IL-13 expression, which was most common in sarcomas (29.2%) and independently correlated with high expression of IL-4 (odds ratio (OR)=4.20) and IL-2Rα (OR=4.63), non-high expression of TIM3 (OR=0.40), PD-L1 negativity (OR=0.40), and microsatellite instability (OR=4.03). In the immunotherapy-naïve analysis, patients with high versus non-high IL-13 levels had shorter overall survival (OS) from metastatic/advanced disease diagnosis (median, 24.5 versus 43.3 months) (HR 1.70, 95% CI 1.15–2.52, log-rank p=0.007). Interaction analysis between IL-13 levels and immunotherapy demonstrated that, among patients with non-high IL-13, those treated with immunotherapy had significantly shorter OS versus immunotherapy-naïve patients (p<0.001), whereas patients with high IL-13 levels had no significant difference in OS between immunotherapy treatment and naive groups.
Conclusion
High IL-13 RNA levels were associated with other important immunoregulatory biomarkers and were most common in sarcomas. High IL-13 expression correlated with poor OS in immunotherapy-naïve patients. The observation that immunotherapy was associated with decreased survival among patients with non-high IL-13 levels is intriguing. These findings are hypothesis-generating, require validation, and have potential implications for biomarker-driven patient stratification to enhance their translational relevance.
Keywords: cancer, IL-13, MSI, prognostic, RNA expression levels, sarcoma, STAT6, transcriptomics
Introduction
Interleukin (IL)-13 plays a role in both inflammatory diseases and cancer. A cytokine produced by basophils and T, B, mast, natural killer (NK), and dendritic cells,1 IL-13 binds to two different receptors: IL-13 receptor subunit alpha-1 (IL-13Rα1) and IL-13Rα2, a high-affinity membrane receptor.2 After binding to IL-13 or IL-4, the receptor heterodimers phosphorylate Janus tyrosine kinases (JAKs) or tyrosine kinase 2, resulting in the induction of various downstream signaling pathways, including STAT6, PI3K/AKT/mTOR, and ERK, which play critical roles in tumor development.3
In 2000, investigators described the critical function of IL-13 in the negative regulation of anti-tumor immunity. Using a mouse model, they demonstrated that IL-13, possibly produced by NK T cells, triggered the downregulation of immunosurveillance through the IL-4Rα–STAT6 pathway.4 Both IL-13 and IL-4 are known to activate the STAT6 signaling pathway by promoting transcription of STAT6-responsive genes.3,5 Furthermore, IL-13 appears to mediate invasion and metastasis through binding to IL-13Rα2.6 Several studies have shown that IL-13 promotes cancer cell proliferation in pancreatic,7 prostate,8 breast,9 and colorectal cancer,10 along with glioblastoma,11 and Hodgkin lymphoma.12 Investigators are exploring whether interactions between various proteins and the IL-13/IL-13Rα2/PTP1B axis promote tumor growth and invasion.11
IL-13Rα2 is an attractive therapeutic target owing to its overexpression in various cancers8 and rare expression in normal tissues13 (in contrast to IL-13Rα1, which is expressed in healthy cells.)13 Specifically, IL-13Rα2 is overexpressed in gliomas,13,14 squamous cell head and neck carcinomas,15 and AIDS-associated Kaposi’s sarcoma,16 where it plays an important role in cancer invasion,17 tumor progression,18 metastasis,19,20 and poor prognosis.21 Treatments targeting IL-13Rα2 in glioblastoma and other tumor types have shown promise.22,23 For example, intracranial infusions of chimeric antigen receptor (CAR)-engineered T cells targeting IL-13Rα2 were associated with intracranial and spinal tumor regression in a patient with recurrent multifocal glioblastoma.22 Similar to other immunoregulatory molecules,24 IL-13 may exhibit anti-tumor activity in addition to its pro-tumorigenic effects. Indeed, although IL-13 attenuates tumor immunosurveillance, there are also data indicating that local delivery of IL-13 to the tumor site can induce tumor regression or rejection.1,25 Notably, there is an unresolved distinction between prognostic and predictive immune biomarkers in immunotherapy and a relative paucity of data about IL-13 and its relationship to more established markers such as, programmed death ligand-1 (PD-L1), microsatellite 90 instability (MSI), and tumor mutational burden (TMB).
In this study, we measured IL-13 transcriptomic expression levels in 514 patients with diverse cancers and evaluated correlations with other immune markers. In addition, we investigated the complex prognostic and predictive role of IL-13 in patients treated with immune checkpoint inhibitors (ICIs) and in patients who were immunotherapy naïve. Our aim was to address the knowledge gap regarding IL-13 in the context of ICIs. Our hypothesis was that IL-13 levels have a prognostic and/or predictive association with outcomes in advanced cancer patients, including after ICI therapy.
Patients and Methods
Patients
IL-13 RNA expression levels were evaluated in tumor tissue samples from 514 patients with locally advanced or metastatic cancer treated at the University of California San Diego (UCSD) Moores Center for Personalized Cancer Therapy clinic. Among patients who were enrolled in the PREDICT study, those who had immunomic testing (at Omniseq) from July 2017 to November 2020 were included in this analysis. Patients had diverse tumor types and had received standard treatment or investigational agents within clinical trials. This study included any patient with advanced cancer for whom immunomic analysis was requested by the physician. Patient demographics, clinical characteristics, treatment, and outcome data, along with tumor pathological and molecular data, were recorded. The data cut-off date was June 24, 2022. The database has been previously reported.26–32 The study was conducted in compliance with UCSD Institutional Review Board guidelines (Study of Personalized Cancer Therapy to Determine Response and Toxicity, UCSD_PREDICT, NCT02478931). Written consent had been obtained from patients for any investigational intervention. The study complied with the Declaration of Helsinki.
Tissue Samples and Immune Gene Expression Profiling
Formalin-fixed, paraffin-embedded (FFPE) tissue samples were evaluated by RNA sequencing at a Clinical Laboratory Improvement Amendments–licensed and College of American Pathologists–accredited clinical laboratory, Labcorp, formerly OmniSeq (https://oncology.labcorp.com/os-welcome). If multiple samples were available for a patient, the first sample obtained was included in the analysis. RNA extraction was performed using the truXTRAC FFPE extraction kit (Covaris, Inc., Woburn, MA), with certain modifications made to the manufacturer’s instructions. Following purification, the RNA was dissolved in 50 μL of water, and its yield was determined using the Quant-iT RNA HS assay (Thermo Fisher Scientific, Waltham, MA). A predefined threshold of 10 ng RNA was employed as the acceptance criterion for suitable library preparation. The immuneResponseRNA plugin (v5.2.0.0) within Torrent Suite was utilized to obtain absolute readings of the RNA sequence. Transcripts were normalized to the selected internal housekeeping genes and were standardized relative to a reference population comprising 735 tumors of 35 different histologies.
Assessments of TMB, PD-L1 positivity, and MSI status were performed as previously described.30 TMB was reported as eligible mutations per qualified panel size (mutations/megabase). PD-L1 immunohistochemical assessment was performed based on clinical practice, using three different assays (VENTANA PD-L1 SP142 assay [Ventana Medical Systems, Inc., Tucson, AZ], Dako PD-L1 22C3 pharmDx assay, and Dako PD-L1 28–8 pharmDx assay [Dako North America, Inc., Carpinteria, CA]). PD-L1 positivity was defined as a score of tumor-infiltrating immune cells ≥1% with SP142, a combined positive score ≥1% with 22C3, or a score of tumor cells ≥1% with 28–8. MSI status was categorized as unstable, stable, or inconclusive using an MSI-NGS assay.30
The Cancer Genome Atlas (TCGA) Cohort
The pan-cancer TCGA cohort was downloaded from the GDC data portal (https://portal.gdc.cancer.gov). The analysis focused on patients for whom both RNA-sequencing and clinical outcome data were available (N=10,111). Subsequently, patients with multiple RNA-sequencing data or with logical errors in survival data were excluded. The final cohort used in this study comprised 9,211 patients. Survival analysis was performed among patients with survival information (N=9,211). Transcripts per million (TPM) was used to stratify the IL-13 levels. The 75th percentile of TPM was used as a threshold to define a high level of IL-13 expression according to the IL-13 distribution. This cut-off was arbitrarily selected for consistency with previously published data.26–32
Outcome Endpoints and Statistical Analysis
The RNA expression profiles were stratified into high (75th–100th percentile), moderate (25th–74th percentile), or low (0–24th percentile) groups. Descriptive statistics (counts with percentages for categorical and median values with the corresponding ranges for continuous variables) were used to summarize patient characteristics and other variables of interest. Logistic regression was used to assess the association between IL-13 RNA expression and other clinical factors, as well as immune markers, including ICIs and interleukins. A parsimonious multivariate regression model was built using Akaike Information Criterion (AIC)-guided backward selection on the subset of patients with none of the considered covariates missing.
The association between IL-13 RNA expression and survival outcomes was evaluated by Kaplan-Meier analysis and examined using the Log rank test. Overall survival (OS) was defined as the time interval from the date of diagnosis of advanced disease to the date of death from any cause or last follow-up. Survival data were left-truncated at the sample collection date for the genomic test (or at the earliest availability of the test [January 1, 2017], when the collection date was unknown) to account for the immortal time before the time of the test, meaning that while survival time was counted from the date of diagnosis of advanced disease, patients were not considered at risk for death until the date of sample collection (and for patients with unknown date of sample collection we used January 1, 2017, as the earliest possible date they could have had the test).
An immunotherapy-naïve analysis dataset was constructed by including the entire follow-up of patients who never received immunotherapy, as well as the pre-immunotherapy period of patients who did receive immunotherapy, with censoring at the time of immunotherapy initiation. In patients who received immunotherapy, progression-free survival (PFS) was defined as the time interval from the start date of immunotherapy to the date of earliest documented disease progression, death from any cause, or last follow-up. No adjustment for the genomic test date was performed in the PFS analysis, as progression was possible before the genomic test. OS was measured from the starting date of immunotherapy until death from any cause or last follow-up, with left truncation as described above. Patients who were progression-free or alive at the time of the analysis (June 2022) were censored at the last follow-up. Cox regression models were applied to estimate the association between variables of interest and disease progression/mortality rates. The differential effect of IL-13 on OS with and without immunotherapy was evaluated by fitting a Cox regression model to the combination of the immunotherapy-naïve analysis set and the post-immunotherapy set, with immunotherapy as a time-varying grouping factor interacting with IL-13 status. A multivariable model was constructed using Cox regression models with AIC-guided backward selection on a subset of patients with none of the considered covariates missing. Wald test p-values are reported, with 95% partial likelihood confidence intervals for the estimates. All statistical analyses were performed using R, version 4.4.1 (R statistical computing, Vienna, Austria). Statistical significance was set at a two-sided p≤0.05.
Results
Patient Characteristics
Overall, 514 patients with diverse tumor types who were diagnosed with advanced disease from September 2004 to September 2020 were included in the study; 204 (39.7%) were men. The median age was 61 years (range, 24–93). The most common subtypes were colorectal (N=140 patients, 27.2%), pancreatic (N=55, 10.7%), breast (N=49, 9.5%), and ovarian (N=43, 8.4%) cancer. In total, 217 patients had received immunotherapy; 199 received a PD-1/PD-L1 inhibitor as monotherapy, 16 received a combination treatment of PD-1/PD-L1 and cytotoxic T-lymphocyte-associated protein 4 (CTLA-4) inhibitor; and two received a CTLA-4 inhibitor as monotherapy. The median number of immunotherapy treatment lines in the advanced setting was 2 (range 1–11). IL-13 transcript expression varied between and within tumor groups.
RNA sequencing was performed from July 2017 to November 2020. Of the 514 patients, 83 patients (16.1%) showed high expression of IL-13, while 431 patients (83.9%) had non-high expression. IL-13 transcript distribution is shown in Figure 1A. High IL-13 expression was more common among patients with sarcoma (29.2% [7/24]), neuroendocrine tumors (26.7% [4/15]), small intestine cancer (25.0% [3/12]), stomach cancer (24.0% [6/25]), and pancreatic cancer (21.8% [12/55]) compared to the overall pan-cancer average (16.1%, 83/514). Tumor types with ≥10 patients were included in this analysis (Figure 1B).
Figure 1.
(A) IL-13 RNA expression across all tumors. In total, 182 (35.4%) of 514 patients had no detectable IL-13 transcripts. Low indicates 0–24th percentile RNA rank, moderate indicates 25th-74th percentile RNA rank, and high indicates ≥75th percentile RNA rank. (B) IL-13 RNA expression per tumor type. A higher proportion of patients with sarcoma (29.2% [7/24]), neuroendocrine tumors (26.7% [4/15]), small intestine cancer (25.0% [3/12]), stomach cancer (24.0% [6/25]), pancreatic cancer (21.8% [12/55]), colorectal cancer (17.9% [25/140]), and uterine cancer (16.7% [4/24]) had high IL-13 expression compared to the overall pan-cancer average. Cancer types with ≥10 patients were included in this analysis.
High IL-13 RNA Levels Correlated with High MSI, High IL-4 and IL-2Rα, and a Diagnosis of Sarcoma
The association between expression levels of IL-13 and other immune markers was assessed. AIC was used to select variables included in the multivariable logistic regression analysis (Table 1). High IL-13 expression levels (≥75th percentile RNA rank score) independently correlated with high MSI (MSI-H; odds ratio [OR] 4.03, 95% confidence interval [CI] 1.10–13.8, p=0.03), high expression of other immune markers, including IL-4 (OR 4.20, 95% CI 1.80–9.58, p<0.001) and IL-2Rα (OR 4.63, 95% CI 2.30–9.39, p<0.001), non-high expression of TIM3 (OR 0.40, 95% CI 0.15–0.95, p=0.049), PD-L1 negativity by immunohistochemistry (OR 0.40, 95% CI 0.18–0.81, p=0.02), and diagnosis of sarcoma (OR 2.85, 95% CI 0.98–7.71, p = 0.04) (multivariate) (Figure 2).
Table 1.
Association Between High IL-13 Expression (N=83) and Other Clinical Factors Among All Patients (N=514) Using Logistic Regression
| Variable | Condition | Proportion of High IL-13 (≥75th Percentile RNA Rank) [83/514] | Univariable OR (95% CI) | Univariable P | Multivariable OR (95% CI) | Multivariable P |
|---|---|---|---|---|---|---|
| Age (years) | Continuous | – | 1.39 (0.87–2.24) | 0.176 | 1.94 (1.06–3.60) | 0.033; Older age is associated with high IL-13 |
| Sex | Male | 17% [34/204] | 1.07 (0.66–1.71) | 0.795 | ||
| Female | 16% [49/310] | – | ||||
| CTLA-4 * | ≥75th | 26% [23/87] | 2.20 (1.25–3.77) | 0.005 | ||
| <75th | 14% [60/427] | – | ||||
| LAG-3 * | ≥75th | 23% [27/116] | 1.85 (1.10–3.08) | 0.019 | 1.82 (0.89–3.68) | 0.10 |
| <75th | 14% [56/398] | – | ||||
| PD-L1 * | ≥75th | 22% [15/67] | 1.61 (0.83–2.96) | 0.139 | ||
| <75th | 15% [68/447] | – | ||||
| PD-L2 * | ≥75th | 22% [22/100] | 1.63 (0.93–2.78) | 0.078 | ||
| <75th | 15% [61/414] | – | ||||
| PD-1 * | ≥75th | 25% [23/93] | 1.98 (1.13–3.37) | 0.014 | ||
| <75th | 14% [60/421] | – | ||||
| CD4 * | ≥75th | 18% [19/107] | 1.16 (0.64–2.00) | 0.611 | ||
| <75th | 16% [64/407] | – | ||||
| VISTA * | ≥75th | 25% [41/166] | 2.39 (1.48–3.86) | <0.001 | ||
| <75th | 12% [42/348] | – | ||||
| TIM-3 * | ≥75th | 20% [18/90] | 1.38 (0.76–2.43) | 0.276 | 0.40 (0.15–0.95) | 0.049; High TIM-3 is negatively associated with high IL-13 |
| <75th | 15% [65/424] | – | ||||
| IL-4 * | ≥75th | 38% [18/47] | 3.84 (1.99–7.26) | <0.001 | 4.20 (1.80–9.58) | <0.001; High IL-4 is associated with high IL-13 |
| <75th | 14% [65/467] | – | ||||
| IL-2Rα * | ≥75th | 32% [36/111] | 3.64 (2.20–6.00) | <0.001 | 4.63 (2.30–9.39) | <0.001; High IL-2Rα is associated with high IL-13 |
| <75th | 12% [47/403] | – | ||||
| IL-2Rγ * | ≥75th | 18% [29/160] | 1.23 (0.74–2.01) | 0.413 | ||
| <75th | 15% [54/354] | – | ||||
| Sarcoma | Yes | 29% [7/24] | 2.24 (0.84–5.39) | 0.083 | 2.85 (0.98–7.71) | 0.044; Sarcoma is associated with high IL-13 |
| No | 16% [76/490] | – | ||||
| Other cancers | Yes | 8.7% [4/46] | 0.47 (0.14–1.20) | 0.16 | ||
| No | 17% [79/468] | – | ||||
| Neuroendocrine tumor | Yes | 27% [4/15] | 1.93 (0.53–5.81) | 0.269 | 2.89 (0.71–9.94) | 0.11 |
| No | 16% [79/499] | – | ||||
| Small intestine cancer | Yes | 25% [3/12] | 1.76 (0.38–6.04) | 0.405 | ||
| No | 16% [80/502] | – | ||||
| Breast cancer | Yes | 12% [6/49] | 0.70 (0.26–1.59) | 0.437 | ||
| No | 17% [77/465] | – | ||||
| Lung cancer | Yes | 10% [2/20] | 0.57 (0.09–2.01) | 0.452 | ||
| No | 16% [81/494] | – | ||||
| Pancreatic cancer | Yes | 22% [12/55] | 1.53 (0.74–2.95) | 0.229 | ||
| No | 15% [71/459] | – | ||||
| Ovarian cancer | Yes | 12% [5/43] | 0.66 (0.22–1.59) | 0.403 | ||
| No | 17% [78/471] | – | ||||
| Colorectal cancer | Yes | 18% [25/140] | 1.18 (0.70–1.96) | 0.520 | ||
| No | 16% [58/374] | – | ||||
| Uterine cancer | Yes | 17% [4/24] | 1.04 (0.30–2.84) | 0.944 | ||
| No | 16% [79/490] | – | ||||
| Stomach cancer | Yes | 24% [6/25] | 1.69 (0.60–4.14) | 0.279 | 2.87 (0.79–9.03) | 0.084 |
| No | 16% [77/489] | – | ||||
| Esophageal cancer | Yes | 5.9% [1/17] | 0.32 (0.02–1.58) | 0.27 | ||
| No | 17% [82/497] | – | ||||
| Head and neck cancer | Yes | 8.3% [1/12] | 0.47 (0.03–2.44) | 0.47 | ||
| No | 16% [82/502] | – | ||||
| Liver and bile duct cancer | Yes | 5.3% [1/19] | 0.28 (0.02–1.38) | 0.22 | ||
| No | 17% [82/495] | – | ||||
| Unknown primary cancer | Yes | 15% [2/13] | 0.94 (0.14–3.60) | 0.94 | ||
| No | 16% [81/501] | – | ||||
| TMB (muts/MB) | ≥10 | 18% [6/33] | 1.27 (0.46–3.02) | 0.610 | ||
| <10 | 15% [62/417] | – | ||||
| TMB (muts/MB) | ≥20 | 36% [4/11] | 3.35 (0.86–11.4) | 0.059 | ||
| <20 | 15% [64/439] | – | ||||
| PD-L1 IHC | Positive | 13% [21/156] | 0.74 (0.43–1.25) | 0.270 | 0.40 (0.18–0.81) | 0.015; Positive PD-L1 IHC is negatively associated with high IL-13 |
| Negative | 17% [62/357] | – | ||||
| MSI | High | 40% [6/15] | 3.58 (1.17–10.2) | 0.019 | 4.03 (1.10–13.8) | 0.028; MSI-H is associated with high IL-13 |
| Not high | 16% [73/465] | – |
Notes: Tabulation was performed with available patients in PD-L1 IHC (N=513), MSI (N=480), and TMB (N=450) due to missing data. Logistic regression analysis with AIC-based backward selection was performed to create a parsimonious set of predictors of IL-13 status. Model selection was performed on the subset of n=402 patients for whom none of the covariates of interest were missing. Fisher’s exact test was used for categorical variables, and Welch’s t-test was used for continuous variables. Bold text indicates statistically significant associations. *RNA percentile rank score is used for stratification.
Abbreviations: CI, confidence interval; IHC, immunohistochemistry; MB, megabase; MSI, microsatellite instability; muts, mutations; OR, odds ratio; TMB, tumor mutational burden.
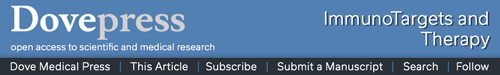
Figure 2.
Multivariable logistic regression analysis between IL-13 high levels [≥75th percentile RNA rank] and clinical and biologic factors (N=514). Both high TIM3 (≥75th percentile RNA rank) and high (≥1%) PD-L1 immunohistochemistry negatively and significantly correlated with high IL-13. Multivariable analysis was performed in N=423 patients due to missing data on PD-L1 IHC (available for N=513), MSI (available for N=480), and TMB (available for N=450). Confidence intervals were derived using profile likelihood. Bold text indicates statistically significant associations.
Clinical Outcomes
Immunotherapy-Naïve Patients with High Versus Non-High IL-13 RNA Levels Had Shorter OS
Of the 514 patients registered in this UCSD cohort, 489 patients (including 217 who received immunotherapy and 272 who were immunotherapy naïve) were eligible for survival analysis (the date of advanced/metastatic disease diagnosis was unavailable for 25 patients). The median follow-up was 24.4 months (interquartile range: 12.6–43.6). Of these 489 patients, 266 had died before the current analysis.
The UCSD patient cohort comprised 489 immunotherapy-naïve patients (272 patients who never received immunotherapy plus 217 patients who received immunotherapy but whose data were censored at the start of immunotherapy). Twenty-seven patients were excluded from this analysis: 25 patients underwent testing before ICI therapy; 1 patient underwent testing on the same day as ICI therapy; and 1 patient underwent testing on the date of last follow-up. Of the 462 evaluable patients, those with high IL-13 levels had shorter OS (median, 24.5 months) compared with patients with non-high IL-13 levels (median, 43.3 months) (HR 1.70, 95% CI 1.15–2.52, log-rank p = 0.007; Figure 3, Panel A). This observation (shorter OS for patients with high IL-13) was confirmed in the TCGA dataset (9211 patients, Figure 3, Panel D, p=0.04).
Figure 3.
Kaplan Meier survival analysis based on high (≥75th percentile RNA rank) versus non-high (<75th percentile RNA rank) IL-13 levels. (Panel (A) Overall survival among patients who did not receive immunotherapy from the date of metastatic/advanced disease to death plus immunotherapy-treated patients from the date of metastatic/advanced disease until immunotherapy initiation with censoring on that date for the latter group (left truncation) (N=462), (hazard ratio [HR] 1.70, 95% confidence interval [CI] 1.15–2.52, p=0.007) (patients with high IL-13 (≥75th percentile RNA rank) had shorter OS than those with non-high IL-13 (<75th percentile RNA rank). (Panel (B) Overall survival among patients treated with immunotherapy (N=217) from the start date of immunotherapy (HR 0.59, 95% CI 0.34–1.03, p=0.059). In contrast to the immunotherapy-naïve group shown in Panel A, patients with high IL-13 showed a trend toward longer OS compared to ICI-treated non-high IL-13 patients. (Panel (C) Progression-free survival among patients treated with immunotherapy (N=217) from the start date of immunotherapy (HR 0.73, 95% CI 0.48–1.11, p=0.14). (Panel (D) Overall survival stratified by IL-13 levels in a pan-cancer TCGA cohort with survival information (N=9,211). Transcripts per million (TMP) was used for stratifying the IL-13 levels. The threshold of the 75th percentile of TPM was used according to the IL-13 distribution (HR 1.10, 95% CI 1.00–1.19, p=0.04). Patients with high IL-13 had shorter OS than those with non-high IL-13 (similar to that found in the UCSD cohort in Panel A). Note that the censoring signs were omitted for readability in Panel D.
Interaction Analysis Showed That, in Patients with Non-High IL-13 (but Not in Patients with High IL-13), Those Treated with Immunotherapy Had Significantly Shorter OS Compared with Those Who Were Immunotherapy-Naïve
The results of univariate and multivariate analyses of OS with immunotherapy as a time-dependent group, adjusted for test timing (including Cox regression), are shown in Table 2. After univariable regression, variables chosen by AIC-guided backward selection were included in the multivariable analysis. The table shows that among patients with non-high IL-13, OS was shorter in patients treated with immunotherapy (OS measured after the start of ICI therapy) than in immunotherapy-naïve patients (p<0.001). Furthermore, there was an interaction between immunotherapy and IL-13 (high versus non-high). The increase in the hazard of death in ICI-treated versus immunotherapy-naïve patients was significantly lower in patients with high IL-13 compared to non-high IL-13 (p=0.039).
Table 2.
Univariate and Multivariate Analysis of Overall Survival with Immunotherapy as a Time-Dependent Group, Adjusted for Test Timing (Including Cox Regression)
| Characteristic | Patient Group | Univariable Models | Selected Multivariable Model | ||||||
|---|---|---|---|---|---|---|---|---|---|
| N | Event N | HR (95% CI) | p-value | N | Event N | HR (95% CI) | p-value | ||
| Immunotherapy | No ICI | 462 | 134 | – | 382 | 107 | – | ||
| After ICI | 217 | 132 | 2.65 (2.03–3.47) | <0.001 | 181 | 110 | 3.24 (2.40–4.38) | <0.001; Among patients with non-high IL-13, OS was shorter after the start of ICI compared to immunotherapy-naïve patients. | |
| IL-13 | Non-high (<75th) | 572 | 218 | – | 478 | 182 | – | ||
| High (≥75th) | 107 | 48 | 1.73 (1.17–2.56) | 0.006 | 85 | 35 | 1.50 (0.94–2.38) | 0.090 | |
| Immunotherapy x IL-13 group | All else | 649 | 252 | – | 540 | 208 | – | ||
| After ICI *High | 30 | 14 | 0.33 (0.17–0.66) | 0.002 | 23 | 9 | 0.42 (0.18–0.96) | 0.039; There was an interaction between immunotherapy and IL-13; high versus non-high. The increase in the hazard of death of ICI-treated versus immunotherapy-naïve patients was significantly lower in IL-13 high patients compared to IL-13 non-high patients. (See also Table 3) | |
| Age (years) | <61 | 331 | 124 | – | |||||
| ≥61 | 348 | 142 | 1.17 (0.92–1.48) | 0.21 | |||||
| Sex | Female | 401 | 158 | – | |||||
| Male | 278 | 108 | 1.03 (0.80–1.31) | 0.84 | |||||
| CTLA-4 | Non-high (<75th) | 566 | 232 | – | |||||
| High (≥75th) | 113 | 34 | 0.63 (0.44–0.90) | 0.012 | |||||
| LAG3 | Non-high (<75th) | 527 | 218 | – | |||||
| High (≥75th) | 152 | 48 | 0.64 (0.47–0.87) | 0.005 | |||||
| PD-L1 | Non-high (<75th) | 585 | 238 | – | |||||
| High (≥75th) | 94 | 28 | 0.85 (0.58–1.26) | 0.43 | |||||
| PD-L2 | Non-high (<75th) | 541 | 225 | – | |||||
| High (≥75th) | 138 | 41 | 0.67 (0.48–0.94) | 0.019 | |||||
| PD-1 | Non-high (<75th) | 556 | 231 | – | 472 | 194 | – | ||
| High (≥75th) | 123 | 35 | 0.57 (0.40–0.82) | 0.002 | 91 | 23 | 0.46 (0.28–0.73) | 0.001; High PD-1 correlated with longer OS | |
| CD4 | Non-high (<75th) | 538 | 216 | – | |||||
| High (≥75th) | 141 | 50 | 0.91 (0.67–1.24) | 0.55 | |||||
| VISTA | Non-high (<75th) | 468 | 182 | – | |||||
| High (≥75th) | 211 | 84 | 0.96 (0.74–1.25) | 0.77 | |||||
| TIM-3 | Non-high (<75th) | 557 | 226 | – | 474 | 193 | – | ||
| High (≥75th) | 122 | 40 | 0.67 (0.48–0.94) | 0.020 | 89 | 24 | 0.46 (0.29–0.74) | 0.001; High TIM-3 correlated with longer OS | |
| IL4 | Non-high (<75th) | 619 | 247 | – | |||||
| High (≥75th) | 60 | 19 | 0.66 (0.42–1.06) | 0.085 | |||||
| IL-2α | Non-high (<75th) | 539 | 218 | – | 452 | 179 | – | ||
| High (≥75th) | 140 | 48 | 0.84 (0.61–1.15) | 0.26 | 111 | 38 | 1.45 (0.95–2.20) | 0.084 | |
| IL-2Rγ | Non-high (<75th) | 472 | 180 | – | |||||
| High (≥75th) | 207 | 86 | 1.01 (0.78–1.31) | 0.94 | |||||
| TMB | <10 (muts/MB) | 549 | 216 | – | 513 | 201 | – | ||
| ≥10 (muts/MB) | 50 | 16 | 0.74 (0.44–1.22) | 0.24 | 50 | 16 | 0.60 (0.35–1.00) | 0.052 | |
| TMB | <20 (muts/MB) | 583 | 228 | – | |||||
| ≥20 (muts/MB) | 16 | 4 | 0.55 (0.20–1.48) | 0.23 | |||||
| PD-L1 IHC | Negative | 455 | 193 | – | |||||
| Positive | 223 | 73 | 1.06 (0.81–1.40) | 0.66 | |||||
| MSI | Not high | 613 | 244 | – | |||||
| High | 22 | 4 | 0.37 (0.14–0.98) | 0.046 | |||||
| Breast cancer | No | 624 | 247 | – | |||||
| Yes | 55 | 19 | 0.89 (0.55–1.42) | 0.62 | |||||
| Colorectal cancer | No | 497 | 189 | – | |||||
| Yes | 182 | 77 | 0.94 (0.72–1.22) | 0.63 | |||||
| Esophageal cancer | No | 653 | 256 | – | |||||
| Yes | 26 | 10 | 1.32 (0.70–2.50) | 0.39 | |||||
| Head and neck cancer | No | 664 | 258 | – | |||||
| Yes | 15 | 8 | 1.14 (0.56–2.32) | 0.71 | |||||
| Liver and bile duct cancer | No | 652 | 255 | – | |||||
| Yes | 27 | 11 | 1.38 (0.75–2.53) | 0.29 | |||||
| Lung cancer | No | 649 | 253 | – | |||||
| Yes | 30 | 13 | 1.32 (0.76–2.31) | 0.33 | |||||
| Neuroendocrine tumor | No | 660 | 261 | – | |||||
| Yes | 19 | 5 | 0.65 (0.27–1.57) | 0.34 | |||||
| Ovarian cancer | No | 620 | 243 | – | |||||
| Yes | 59 | 23 | 0.75 (0.48–1.15) | 0.19 | |||||
| Pancreatic cancer | No | 611 | 228 | – | 516 | 190 | – | ||
| Yes | 68 | 38 | 1.89 (1.34–2.68) | <0.001 | 47 | 27 | 2.49 (1.62–3.82) | <0.001; Pancreatic cancer correlated with shorter OS | |
| Sarcoma | No | 648 | 256 | – | |||||
| Yes | 31 | 10 | 0.59 (0.31–1.12) | 0.11 | |||||
| Small intestine cancer | No | 667 | 261 | – | |||||
| Yes | 12 | 5 | 1.44 (0.59–3.51) | 0.42 | |||||
| Stomach cancer | No | 645 | 252 | – | |||||
| Yes | 34 | 14 | 1.75 (1.02–3.01) | 0.042 | |||||
| Unknown primary cancer | No | 661 | 260 | – | |||||
| Yes | 18 | 6 | 1.15 (0.51–2.60) | 0.73 | |||||
| Uterine cancer | No | 645 | 255 | – | |||||
| Yes | 34 | 11 | 0.89 (0.49–1.63) | 0.71 | |||||
| Other cancer | No | 610 | 250 | – | |||||
| Yes | 69 | 16 | 0.56 (0.34–0.94) | 0.027 | |||||
Notes: After univariable regression, variables chosen by Akaike Information Criterion (AIC)-guided backward selection were included in the multivariable analysis. Bold text indicates statistically significant associations. * RNA percentile rank score is used for stratification.
Abbreviations: CI, confidence interval; HR, hazard ratio; IHC, immunohistochemistry; MB, megabase; MSI, microsatellite instability; muts, mutations; TMB, tumor mutational burden.
In contrast to the observation in immunotherapy-naïve patients, in the immunotherapy treatment UCSD dataset (N=217), patients with high IL-13 levels had a trend towards longer OS after immunotherapy compared with patients with non-high IL-13 levels (Figure 3, Panel B, p=0.059) (in contrast to the observation in immunotherapy-naive patients, who had shorter OS if they had high IL-13) (Figure 3 panel A). There was no difference in PFS between immunotherapy-treated patients with high IL-13 and those with non-high IL-13 (Figure 3, Panel C, p=0.14). Notably, when we focus on the interactions between IL-13 levels and immunotherapy in the UCSD dataset, among patients with non-high IL-13, those treated with immunotherapy had significantly shorter OS compared with those who were immunotherapy-naïve (Table 3, p<0.001). In contrast, in patients with high IL-13, there was no significant survival difference between those who were and those who were not treated with immunotherapy (Table 3, p=0.43). Multivariate Cox analysis for OS is depicted in Figure 4 and further demonstrates that non-high IL-13 interacts with immunotherapy, resulting in a worse outcome; such an interaction was not significant for patients with high IL-13.
Table 3.
Analysis of the Interaction Between IL-13 Level, Immunotherapy versus No Immunotherapy Treatment, and Overall Survival
| Subgroup | Comparison for OS | HR (95% CI) | P | Comment |
|---|---|---|---|---|
| Immunotherapy-naïve patient analysis* | IL-13 high (≥75th percentile RNA rank) vs. IL-13 non-high (<75th) | 1.50 (0.94–2.38) | 0.09 | There was a trend for immunotherapy-naïve patients with high versus non-high IL-13 to have shorter OS from diagnosis of advanced/metastatic disease. |
| ICI treated (N=217 patients)^ | IL-13 high (≥75th percentile RNA rank) vs. IL-13 non-high (<75th) | 0.63 (0.31–1.26) | 0.19 | There was a trend for ICI-treated patients with high versus non-high IL-13 to have longer OS from the start time of the first ICI. |
| Non-high IL-13 (<75th percentile RNA rank) | ICI vs. no ICI | 3.24 (2.40–4.38) | <0.001 | Among patients with non-high IL-13 levels, those who received ICI had significantly shorter OS compared to those who were immunotherapy-naïve. |
| High IL-13 (≥75th percentile RNA rank) | ICI vs. No ICI | 1.36 (0.63–2.97) | 0.43 | Among patients with high IL-13 levels, there was no difference in OS in those who received ICI vs. those who were immunotherapy-naïve. |
Notes: *The immunotherapy-naïve group was analyzed for OS from the time of diagnosis of metastatic/advanced disease; this group included OS analysis from the time of diagnosis of metastatic/advanced disease to death (or if the patient was still alive at data cut-off or date of last visit, whichever was earlier, censoring on that date) for 272 patients never treated with an ICI. It also included the time period from diagnosis of metastatic/advanced disease to the start of the first ICI in 217 patients who received an ICI; OS in this group was censored at the start time of ICI. Bold text indicates statistically significant associations. ^ICI-treated patients were analyzed for OS from the time of receipt of first ICI to death (or if the patient was still alive at data cut-off or date of last visit, whichever was earlier, censoring on that date) in 217 patients treated with an ICI.
Abbreviations: CI, confidence interval; HR, hazard ratio; ICI, immune checkpoint inhibitor; OS, overall survival.
Figure 4.
Interaction between high IL-13 transcripts and outcome. Forest plot of multivariable Cox analysis for overall survival. High pertains to ≥75th RNA percentile; non-high is <75th RNA percentile rank. The figure shows that non-high IL-13 interacts with immunotherapy, resulting in a worse outcome; such an interaction was not significant for patients with high IL-13 (see also Figure 3).
A synthesis of the above data indicates that the association between high IL-13 and OS by ICI treatment or no treatment did not change; instead, patients with non-high IL-13 had significantly shorter OS when treated with ICI as compared to when not treated with ICI, therefore making the ICI-treated high IL-13 patients appear to have longer OS compared with the non-high IL-13 patients.
Discussion
ICIs hold promise for selected patients with diverse tumor types, but despite remarkable advances in treatment with immunotherapy, patients still develop primary resistance to ICIs or have disease progression after initial benefit. In addition to well-studied predictive biomarkers such as MSI-H, TMB, and PD-L1, further investigation may identify immune-related biomarkers that can be prognostic independent of immunotherapy administration, predictive of response to immunotherapy, or even serve as therapeutic targets for innovative approaches.
In our study, 16.1% of patients with diverse advanced cancers showed high tumor expression of IL-13 RNA (>75th percentile), while 431 patients 83.9% had non-high IL-13 expression. IL-13 levels varied between and within tumor types, but sarcomas had the greatest percentage of tumor samples with high IL-13 expression. The role of IL-13 and its receptor subunits, IL-13Rα1 and IL-13Rα2, in tumor growth5 and OS33 in patients with sarcomas has been previously explored, but data are limited and the association between IL-13 expression levels and prognosis in patients with sarcoma is unclear.
We found that high IL-13 expression levels independently and significantly correlated with other immune-relevant markers, including MSI-H, high IL-4 and IL-2Rα levels, non-high expression of TIM3 (<75th percentile RNA rank), and PD-L1 negativity. Both cytokines—IL-13 and IL-4—share a common receptor, a heterodimer comprising IL-13Rα1 and IL-4 receptor α.2 Binding of either IL-13 or IL-4 to its receptor leads to Jak/STAT signaling pathway activation, with subsequent transcription of genes involved in T-cell function, antigen presentation by B cells, and immunoglobulin class switching to immunoglobulin E.34 There is little data on the association between IL-13 expression levels and MSI-H. Investigators have previously evaluated the expression of 48 cytokines in MSI-H and MSI-low colorectal tumors using Bio-Plex multiplex cytokine assays.35 Some cytokines were differentially expressed between the two subgroups; however, IL-13 was barely detectable at best, and no association could be established between it and MSI status or other cytokines.35 TIM-3 expression has been extensively studied in cancer as a prognostic factor and as a potential target for monoclonal and bispecific antibodies.29,36 However, the interaction between TIM-3 expression levels and other immune-related molecules, including cytokines and ICIs, remains to be further elucidated.37–39
Notably, we demonstrated that high IL-13 RNA expression levels were a significant prognostic factor for poorer OS in UCSD patients who had not received immunotherapy. TCGA analysis provided similar data, demonstrating worse OS in patients with high IL-13 RNA levels. Few other investigators have reported on the prognostic role of IL-13;40 Saigusa et al indicated that low serum IL-13 levels were associated with poor prognosis in patients with colorectal cancer, which appears to contradict our observations.40 However, it should be kept in mind that there were also different methodologies used. For instance, our UCSD and TCGA results reflect RNA expression, whereas the aforementioned study examined serum cytokine levels; moreover, we analyzed pan-cancer cohorts, while the study by Saigusa et al focused on colorectal cancer. Interestingly, while patients with high IL-13 levels showed shorter survival than patients with non-high IL-13 in the absence of ICI therapy, this trend was reversed in the presence of ICI therapy. Further analysis (Table 3) showed that the correlation between high IL-13 and OS did not actually change in the presence or absence of ICI therapy; rather, patients with non-high IL-13 had significantly worse OS when treated with ICI, as compared to when not treated with ICI, which made the ICI-treated patients with high IL-13 appear to do better than the ICI-treated patients with non-high IL-13. This analysis suggests that in patients with non-high IL-13, those treated with ICIs had a shorter OS compared to those not treated with ICIs.
Other investigators have evaluated the role of IL-13 in cancer tumorigenesis, cell proliferation, and patient prognosis in different malignancies. For instance, in patients with localized clear-cell renal cell carcinoma who underwent nephrectomy, high tumor expression of IL-13 and IL-4 was independently associated with increased recurrence and poor overall survival.41 In another study, IL-13 was shown to be present in the angiosarcoma microenvironment, with strong expression noted in atypical tumor cells.42 Additionally, IL-13 promoted cell proliferation via the IL-13/IL-13Rα2 pathway. Finally, in diffuse intrinsic pontine glioma, transcriptomic analysis demonstrated significant IL-13 pathway activation and overexpression of IL-13 receptors, further supporting this pathway as a potential immunotherapeutic target.43 Collectively, these findings suggest that high IL-13 expression levels may increase tumor progression through immune modulation, proliferative signals, and oncogenic pathway activation, while also representing a potential therapeutic target in diverse tumor types. However, no studies have evaluated the role of IL-13 expression levels as a predictive biomarker for immunotherapy.
The complex interplay between IL-13 expression levels and the benefit, or lack thereof, from immunotherapy is incompletely understood. However, preliminary data suggest a potential correlation between IL-13 expression levels and the anti-tumor effects of immunotherapeutic approaches. In one study, a targeted cytotoxin comprised IL-13 and an exotoxin was shown to induce apoptosis in IL-13Rα2+ tumor cells.44 The cytotoxin combined with an IL-13Rα2 DNA cancer vaccine demonstrated synergistic anti-tumor effects, decreasing tumor growth and metastatic potential in murine tumor models that naturally express IL-13Rα2. On the other hand, although IL-13 is considered to be a cytokine that downregulates tumor immunosurveillance, data also indicate that local delivery of IL-13 at the tumor site can induce tumor regression or rejection mediated by granulocytes and macrophages.1,25 These conflicting roles of the IL-13 signaling pathway in cancer may be due to the complexity of cytokine networks, the diverse cell types involved (both immune and non-immune), and the variety of downstream signaling pathways, including the NFκB, STAT, and MAPK signaling pathways.45,46 This complexity is further amplified by the ability of these components to interact cooperatively in feedback loops.46
Other factors that may have influenced the associations noted in our analyses include immune exhaustion, tumor microenvironment composition, and treatment selection bias. The results also suggest both prognostic (outcomes-related) and predictive (treatment-related) implications for IL-13 levels. Indeed, immunotherapy-naïve patients with high IL-13 RNA levels had shorter OS than those with non-high IL-13 levels, suggesting a prognostic relationship. However, the interaction analysis showed that in patients with non-high IL-13 (but not in patients with high IL-13), those treated with immunotherapy had significantly shorter OS compared with those who were immunotherapy-naïve, suggesting a predictive relationship.
Our study has several limitations. First, the pan-cancer analysis limited the assessment of individual tumor types, though it may also suggest the generalizability of our results. Second, immunomic analysis was requested at the discretion of the treating physicians, potentially leading to a selection bias. Third, regarding the analysis of TCGA data, there were limitations associated with the lack of treatment information. Forth, measuring bulk RNA does not provide single-cell information; this aspect should be addressed in future analyses. Fifth, the choice of the 75th percentile cut-off for defining high IL-13 expression, while consistent with prior work, remains somewhat arbitrary. Sixth, reliance on AIC-guided selection and heterogeneity in PD-L1 assays and treatment indications raises the possibility of residual confounding and selection bias. Seventh, retrospective treatment allocation, heterogeneity across tumor types, and unmeasured factors (eg., performance status, disease burden, line of therapy) may influence the observed associations. Finally, the observational and physician-directed nature of immunotherapy exposure introduces potential confounding.
In conclusion, our data suggest that IL-13 RNA expression levels differ between and within diverse tumor types. High IL-13 levels were associated with MSI-H, high IL-4, high IL-2Rα, and non-high TIM3 expression levels, as well as negative PD-L1 immunohistochemistry, and were more common in sarcomas. High IL-13 expression was associated with poorer OS in immunotherapy-naïve patients. Importantly, among patients with non-high IL-13 levels, those who received immunotherapy had significantly shorter survival than those who remained immunotherapy naïve, but this difference in survival was not seen in patients with high IL-13. These findings are hypothesis-generating, require validation, and have potential implications for biomarker-driven patient stratification to enhance their translational relevance. Further prospective studies evaluating the predictive, prognostic and biologic role of IL-13 in both immunotherapy-naïve and immunotherapy-treated cancer patients are warranted.
Acknowledgments
This work was supported in part by Labcorp/OmniSeq and by the National Cancer Institute at the National Institutes of Health (grant P30 CA023100 to SK).
Funding Statement
RK is funded in part by 5U01CA180888-08 and 5UG1CA233198-05. AMT is supported by Mr. and Mrs. Steven Mckenzie’s Endowment, Katherine Russell Dixie’s Distinguished Professorship Endowment, and donor funds from Jamie’s Hope and Mrs. and Mr. James Ritter for Dr. Tsimberidou’s Personalized Medicine Program and by the National Institutes of Health/National Cancer Institute award number P30 CA016672 (University of Texas MD Anderson Cancer Center).
Abbreviations
CTLA-4, cytotoxic T-lymphocyte–associated protein 4; IL, interleukin; IL-13Rα1, IL-13 receptor subunit alpha-1; JAK, Janus tyrosine kinase; MSI, microsatellite instability; OS, overall survival; PD-L1, programmed death ligand-1; PFS, progression-free survival; TCGA, The Cancer Genome Atlas; TMB, tumor mutational burden; TPM, transcripts per million; UCSD, University of California San Diego.
Data Sharing Statement
The raw data presented in this study is available on request from Dr. Razelle Kurzrock.
Ethics Approval and Patient Consent
This study was conducted in accordance with the guidelines of the UCSD Institutional Review Board (Study of Personalized Cancer Therapy to Determine Response and Toxicity, UCSD_PREDICT, NCT02478931) and any investigational interventions/therapies for which all patients gave written informed consent. Protocols were approved by the UCSD Internal Review Board (UCSD IRB number 130794).
Consent for Publication
Patients gave informed consent for all investigational interventions.
Author Contributions
All authors made a significant contribution to the work reported, whether in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising, or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
EF declares advisory role of Amgen; travel grants from Pfizer, AstraZeneca, Genesis; speaker fees from Lilly, GSK, AstraZeneca; and stock ownership from Genprex Inc., Deciphera Pharmaceuticals, Inc.
RK has received research funding from Boehringer Ingelheim, Debiopharm, Foundation Medicine, Genentech, Grifols, Guardant, Incyte, Konica Minolta, MedImmune, Merck Serono, Omniseq, Pfizer, Sequenom,;Takeda, and TopAlliance and from the NCI; has received consultant and/or speaker fees and/or advisory board/consultant for Actuate Therapeutics, AstraZeneca, Bicara Therapeutics, Inc., Biological Dynamics, Caris, Datar Cancer Genetics, Daiichi, EISAI, EOM Pharmaceuticals, Iylon, LabCorp, Lanuaria, Merck, NeoGenomics, Neomed, Pfizer, Precirix, Prosperdtx, Regeneron, Roche, TD2/Volastra, Turning Point Therapeutics, X-Biotech; has an equity interest in CureMatch Inc.; serves on the Board of CureMatch and CureMetrix, and is a co-founder of CureMatch.
AMT declares receipt of Clinical Trial Research Funding (received through the institution): OBI Pharma, Agenus, Vividion, Macrogenics, AbbVie, IMMATICS, Novocure, Tachyon, Parker Institute for Cancer Immunotherapy, Tempus, and Tvardi; fees for consulting or advisory roles for Avstera Therapeutics, Bioeclipse, BrYet, Diaccurate, Macrogenics, NEX-I, and VinceRx.
T.J.J. is an employee of Labcorp and owns stock in Labcorp.
SP was an employee of Labcorp at the time of this study.
The authors report no other conflicts of interest in this work.
References
- 1.Terabe M, Park JM, Berzofsky JA. Role of IL-13 in regulation of anti-tumor immunity and tumor growth. Cancer Immunol Immunother. 2004;53(2):79–20. doi: 10.1007/s00262-003-0445-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.LaPorte SL, Juo ZS, Vaclavikova J, et al. Molecular and Structural Basis of Cytokine Receptor Pleiotropy in the Interleukin-4/13 System. Cell. 2008;132(2):259–272. doi: 10.1016/j.cell.2007.12.030 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Gordon S, Martinez FO. Alternative Activation of Macrophages: mechanism and Functions. Immunity. 2010;32(5):593–604. doi: 10.1016/j.immuni.2010.05.007 [DOI] [PubMed] [Google Scholar]
- 4.Terabe M, Matsui S, Noben-Trauth N, et al. NKT cell–mediated repression of tumor immunosurveillance by IL-13 and the IL-4R–STAT6 pathway. Nat Immunol. 2000;1(6):515–520. doi: 10.1038/82771 [DOI] [PubMed] [Google Scholar]
- 5.Hosoyama T, Aslam MI, Abraham J, et al. IL-4R Drives Dedifferentiation, Mitogenesis, and Metastasis in Rhabdomyosarcoma. Clin Cancer Res. 2011;17(9):2757–2766. doi: 10.1158/1078-0432.CCR-10-3445 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Little AC, Pathanjeli P, Wu Z, et al. IL-4/IL-13 Stimulated Macrophages Enhance Breast Cancer Invasion Via Rho-GTPase Regulation of Synergistic VEGF/CCL-18 Signaling. Front Oncol. 2019;9. doi: 10.3389/fonc.2019.00456 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Formentini A, Prokopchuk O, Sträter J, et al. Interleukin-13 exerts autocrine growth-promoting effects on human pancreatic cancer, and its expression correlates with a propensity for lymph node metastases. Int J Colorectal Dis. 2009;24(1):57–67. doi: 10.1007/s00384-008-0550-9 [DOI] [PubMed] [Google Scholar]
- 8.Maini A, Hillman G, Haas GP, et al. Interleukin-13 Receptors on Human Prostate Carcinoma Cell Lines Represent a Novel Target for a Chimeric Protein Composed of IL-13 and a Mutated Form of Pseudomonas Exotoxin. J Urol;1997. 948–953. doi: 10.1097/00005392-199709000-00077 [DOI] [PubMed] [Google Scholar]
- 9.Srabovic N, Mujagic Z, Mujanovic-Mustedanagic J, et al. Interleukin 13 expression in the primary breast cancer tumor tissue. Biochem Med;2011. 131–138. doi: 10.11613/BM.2011.021 [DOI] [PubMed] [Google Scholar]
- 10.Wright K, Kolios G, Westwick J, et al. Cytokine-induced Apoptosis in Epithelial HT-29 Cells Is Independent of Nitric Oxide Formation. J Biol Chem. 1999;274(24):17193–17201. doi: 10.1074/jbc.274.24.17193 [DOI] [PubMed] [Google Scholar]
- 11.Bartolomé RA, Martín-Regalado Á, Pintado-Berninches L, et al. Schnurri-3 drives tumor growth and invasion in cancer cells expressing interleukin-13 receptor alpha 2. Cell Death Dis. 2023;14(11):742. doi: 10.1038/s41419-023-06255-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Skinnider BF, Kapp U, Mak TW. Interleukin 13: a Growth Factor in Hodgkin Lymphoma. Int Arch Allergy Immunol. 2001;126(4):267–276. doi: 10.1159/000049523 [DOI] [PubMed] [Google Scholar]
- 13.Kawakami M, Leland P, Kawakami K, et al. Mutation and Functional Analysis of IL-13 Receptors in Human Malignant Glioma Cells. Oncol Res Featuring Preclinical Clin Cancer Ther. 2001;12(11):459–467. doi: 10.3727/096504001108747468 [DOI] [PubMed] [Google Scholar]
- 14.Newman JP, Wang GY, Arima K, et al. Interleukin-13 receptor alpha 2 cooperates with EGFRvIII signaling to promote glioblastoma multiforme. Nat Commun. 2017;8(1):1913. doi: 10.1038/s41467-017-01392-9 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Kawakami M, Kawakami K, Kasperbauer JL, et al. Interleukin-13 receptor alpha2 chain in human head and neck cancer serves as a unique diagnostic marker. Clin Cancer Res. 2003;9(17):6381–6388. [PubMed] [Google Scholar]
- 16.Husain SR, Puri RK. Interleukin-13 fusion cytotoxin as a potent targeted agent for AIDS-Kaposi’s sarcoma xenograft. Blood. 2000;95(11):3506–3513. doi: 10.1182/blood.V95.11.3506 [DOI] [PubMed] [Google Scholar]
- 17.Fujisawa T, Joshi B, Nakajima A, et al. A Novel Role of Interleukin-13 Receptor α2 in Pancreatic Cancer Invasion and Metastasis. Cancer Res. 2009;69(22):8678–8685. doi: 10.1158/0008-5472.CAN-09-2100 [DOI] [PubMed] [Google Scholar]
- 18.Kang M-A, Lee J, Lee CM, et al. IL13Rα2 Is Involved in the Progress of Renal Cell Carcinoma through the JAK2/FOXO3 Pathway. J Pers Med. 2021;11(4):284. doi: 10.3390/jpm11040284 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Bartolomé RA, García-Palmero I, Torres S, et al. IL13 Receptor α2 Signaling Requires a Scaffold Protein, FAM120A, to Activate the FAK and PI3K Pathways in Colon Cancer Metastasis. Cancer Res. 2015;75(12):2434–2444. doi: 10.1158/0008-5472.CAN-14-3650 [DOI] [PubMed] [Google Scholar]
- 20.Márquez-Ortiz RA, Contreras-Zárate MJ, Tesic V, et al. IL13Rα2 Promotes Proliferation and Outgrowth of Breast Cancer Brain Metastases. Clin Cancer Res. 2021;27(22):6209–6221. doi: 10.1158/1078-0432.CCR-21-0361 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Barderas R, Bartolomé RA, Fernandez-Aceñero MJ, et al. High Expression of IL-13 Receptor α2 in Colorectal Cancer Is Associated with Invasion, Liver Metastasis, and Poor Prognosis. Cancer Res. 2012;72(11):2780–2790. doi: 10.1158/0008-5472.CAN-11-4090 [DOI] [PubMed] [Google Scholar]
- 22.Brown CE, Alizadeh D, Starr R, et al. Regression of Glioblastoma after Chimeric Antigen Receptor T-Cell Therapy. N Engl J Med. 2016;375(26):2561–2569. doi: 10.1056/NEJMoa1610497 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Jaén M, Martín-Regalado Á, Bartolomé RA, et al. Interleukin 13 receptor alpha 2 (IL13Rα2): expression, signaling pathways and therapeutic applications in cancer. Biochim Biophys Acta Rev Cancer. 2022;1877(5):188802. doi: 10.1016/j.bbcan.2022.188802 [DOI] [PubMed] [Google Scholar]
- 24.Hsieh ML, Nishizaki D, Adashek JJ, et al. Toll-like receptor 3: a double-edged sword. Biomark Res. 2025;13(1):32. doi: 10.1186/s40364-025-00739-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Lebel-Binay S, Laguerre B, Quintin-Colonna F, et al. Experimental gene therapy of cancer using tumor cells engineered to secrete interleukin-13. Eur J Immunol. 1995;25(8):2340–2348. doi: 10.1002/eji.1830250833 [DOI] [PubMed] [Google Scholar]
- 26.Moussa P. Transcriptomic analysis of GITR and GITR ligand reveals cancer immune heterogeneity with implications for GITR targeting. Am J Cancer Res. 2024;14(4):1634–1648. doi: 10.62347/ECED5481 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Shreenivas A, Nishizaki D, Lee S, et al. Clinical and Biologic Correlates of ADORA2A Transcriptomic Expression in Cancer. Int J Mol Sci. 2024;25(9):4742. doi: 10.3390/ijms25094742 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Miyashita H. The transcriptomic expression pattern of immune checkpoints shows heterogeneity between and within cancer types. Am J Cancer Res. 2024;14(5):2240–2252. doi: 10.62347/JRJP7877 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Ahmed J, Nishizaki D, Miyashita H, et al. TIM-3 transcriptomic landscape with clinical and immunomic correlates in cancer. Am J Cancer Res. 2024;14(5):2493–2506. doi: 10.62347/MQFF6404 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Nishizaki D, Kurzrock R, Miyashita H, et al. Viewing the immune checkpoint Vista: landscape and outcomes across cancers. ESMO Open. 2024;9(4):102942. doi: 10.1016/j.esmoop.2024.102942 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Adashek JJ. LAG-3 transcriptomic expression correlates linearly with other checkpoints, but not with clinical outcomes. Am J Cancer Res. 2024;14(1):368–377. doi: 10.62347/MVDH5025 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Krishnamurthy N, Nishizaki D, Lippman SM, et al. High CTLA-4 transcriptomic expression correlates with high expression of other checkpoints and with immunotherapy outcome. Ther Adv Med Oncol. 2024;16. doi: 10.1177/17588359231220510 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Kim KM, Hussein UK, Park S-H, et al. Expression of IL4Rα and IL13Rα1 are associated with poor prognosis of soft-tissue sarcoma of the extremities, superficial trunk, and retroperitoneum. Diagn Pathol. 2021;16(1):2. doi: 10.1186/s13000-020-01066-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Goenka S, Kaplan MH. Transcriptional regulation by STAT6. Immunol Res. 2011;50(1):87–96. doi: 10.1007/s12026-011-8205-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Boissière-Michot F, Lazennec G, Frugier H, et al. Characterization of an adaptive immune response in microsatellite-instable colorectal cancer. Oncoimmunology. 2014;3(6):e29256. doi: 10.4161/onci.29256 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Sauer N, Janicka N, Szlasa W, et al. TIM-3 as a promising target for cancer immunotherapy in a wide range of tumors. Cancer Immunol Immunother. 2023;72(11):3405–3425. doi: 10.1007/s00262-023-03516-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Ocaña-Guzman R, Ramon-Luing LA, Vazquez-Bolaños LA, et al. Tim-3 Is Differentially Expressed during Cell Activation and Interacts with the LSP-1 Protein in Human Macrophages. J Immunol Res. 2023;2023:1–11. doi: 10.1155/2023/3577334 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Nakae S, Iikura M, Suto H, et al. TIM-1 and TIM-3 enhancement of Th2 cytokine production by mast cells. Blood. 2007;110(7):2565–2568. doi: 10.1182/blood-2006-11-058800 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Su EW, Lin JY, Kane LP. TIM-1 and TIM-3 proteins in immune regulation. Cytokine. 2008;44(1):9–13. doi: 10.1016/j.cyto.2008.06.013 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Saigusa S, Tanaka K, Inoue Y, et al. Low Serum Interleukin-13 Levels Correlate with Poorer Prognoses for Colorectal Cancer Patients. Int Surg. 2014;99(3):223–229. doi: 10.9738/INTSURG-D-13-00259.1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Chang Y, Xu L, An H, et al. Expression of IL-4 and IL-13 predicts recurrence and survival in localized clear-cell renal cell carcinoma. Int J Clin Exp Pathol. 2015;8(2):1594–1603. [PMC free article] [PubMed] [Google Scholar]
- 42.Saito H, Chan JY, Omori I, et al. IL-13/IL-13Rα2 axis promotes proliferation of angiosarcoma cells. Sci Rep. 2025;15(1):31236. doi: 10.1038/s41598-025-15933-6 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Berlow NE, Svalina MN, Quist MJ, et al. IL-13 receptors as possible therapeutic targets in diffuse intrinsic pontine glioma. PLoS One. 2018;13(4):e0193565. doi: 10.1371/journal.pone.0193565 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Nakashima H, Terabe M, Berzofsky JA, et al. A Novel Combination Immunotherapy for Cancer by IL-13Rα2–Targeted DNA Vaccine and Immunotoxin in Murine Tumor Models. J Immunol. 2011;187(10):4935–4946. doi: 10.4049/jimmunol.1102095 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Bernstein ZJ, Shenoy A, Chen A, et al. Engineering the IL-4/IL-13 axis for targeted immune modulation. Immunol Rev. 2023;320(1):29–57. doi: 10.1111/imr.13230 [DOI] [PubMed] [Google Scholar]
- 46.Manzano S, Caffarel MM. Cytokine-centered strategies to boost cancer immunotherapy. Mol Oncol. 2025;19(3):579–583. doi: 10.1002/1878-0261.13818 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The raw data presented in this study is available on request from Dr. Razelle Kurzrock.



![A forest plot showing odds ratios for factors associated with high interleukin 13 expression. Multivariable logistic regression analysis between IL-13 high levels [≥75th percentile RNA rank] and clinical and biologic factors (N=514). A forest plot with a table and horizontal confidence-interval lines. Columns are Variable, N, Odds ratio and p. The x-axis label is Odds ratio (unitless), with tick labels 0.2, 0.5, 1, 2, 5, 10. A vertical dashed reference line is at 1. Rows (all N equals 423) list point estimates (square markers) with confidence intervals and p values: Age ≥61 (years), odds ratio 1.94 with confidence interval 1.06 to 3.60, p 0.03. High LAG3, odds ratio 1.82 with confidence interval 0.89 to 3.68, p 0.10. High TIM3, odds ratio 0.40 with confidence interval 0.15 to 0.95, p 0.049. High IL-4, odds ratio 4.20 with confidence interval 1.80 to 9.58, p less than 0.001. High IL-2Rα, odds ratio 4.63 with confidence interval 2.30 to 9.39, p less than 0.001. PD-L1 IHC positive, odds ratio 0.40 with confidence interval 0.18 to 0.81, p 0.02. MSI high, odds ratio 4.03 with confidence interval 1.10 to 13.81, p 0.03. Neuroendocrine Tumors, odds ratio 2.89 with confidence interval 0.71 to 9.94, p 0.11. Sarcoma, odds ratio 2.85 with confidence interval 0.98 to 7.71, p 0.04. Stomach Cancer, odds ratio 2.87 with confidence interval 0.79 to 9.03, p 0.08. The detailed data points are as follows: - For Age greater than or equal to 61 (years), N is 423, the odds ratio (95% CI) is 1.94 (1.06, 3.60) and p is 0.03. - For High LAG3, N is 423, the odds ratio (95% CI) is 1.82 (0.89, 3.68) and p is 0.10. - For High TIM3, N is 423, the odds ratio (95% CI) is 0.40 (0.15, 0.95) and p is 0.049. - For High IL-4, N is 423, the odds ratio (95% CI) is 4.20 (1.80, 9.58) and p is less than 0.001. - For High IL-2Ralpha, N is 423, the odds ratio (95% CI) is 4.63 (2.30, 9.39) and p is less than 0.001. - For PD-L1 IHC positive, N is 423, the odds ratio (95% CI) is 0.40 (0.18, 0.81) and p is 0.02. - For MSI high, N is 423, the odds ratio (95% CI) is 4.03 (1.10, 13.81) and p is 0.03. - For Neuroendocrine Tumors, N is 423, the odds ratio (95% CI) is 2.89 (0.71, 9.94) and p is 0.11. - For Sarcoma, N is 423, the odds ratio (95% CI) is 2.85 (0.98, 7.71) and p is 0.04. - For Stomach Cancer, N is 423, the odds ratio (95% CI) is 2.87 (0.79, 9.03) and p is 0.08.](https://cdn.ncbi.nlm.nih.gov/pmc/blobs/6c2e/13155402/33b6f0cbd546/ITT-15-578703-g0002.jpg)

