Abstract
Two novel streptococcal superantigen genes (speLSe and speMSe) were identified from the Streptococcus equi genome database at the Sanger Center. Genotyping of 8 S. equi isolates and 40 Streptococcus pyogenes isolates resulted in the detection of the orthologous genes speL and speM in a restricted number of S. pyogenes isolates (15 and 5%, respectively). Surprisingly, the novel superantigen genes could not be found in any of the analyzed S. equi isolates. The results suggest that both genes are located on a mobile element that enables gene transfer between individual isolates and between streptococci from different Lancefield groups. S. equi pyrogenic exotoxin L (SPE-LSe)/streptococcal pyrogenic exotoxin L (SPE-L) and SPE-MSe/SPE-M are most closely related to SMEZ, SPE-C, SPE-G, and SPE-J, but build a separate branch within this group. Recombinant SPE-L (rSPE-L) and rSPE-M were highly mitogenic for human peripheral blood lymphocytes, with half-maximum responses at 1 and 10 pg/ml, respectively. The results from competitive binding experiments suggest that both proteins bind major histocompatibility complex class II at the β-chain, but not at the α-chain. The most common targets for both toxins were human Vβ1.1 expressing T cells. Seroconversion against SPE-L and SPE-M was observed in healthy blood donors, suggesting that the toxins are expressed in vivo. Interestingly, the speL gene is highly associated with S. pyogenes M89, a serotype that is linked to acute rheumatic fever in New Zealand.
Bacterial superantigens (SAgs) are small highly mitogenic proteins that are produced as monomeric precursor molecules with typical bacterial signal peptides (8). The mature secreted toxins simultaneously bind to major histocompatibility complex (MHC) class II antigens and T-cell-receptor (TcR) molecules, which leads to the stimulation of large numbers of T cells (16, 19, 27). Unlike conventional antigens, SAgs bind MHC class II outside the peptide binding groove and bind mainly to the CDR2 and HV4 regions on the TcR Vβ chain (12, 15, 17, 27, 38). Each SAg targets a specific set of TcR Vβ chains leaving a characteristic “fingerprint” in the stimulated T cells. The oligoclonal T-cell stimulation results in high systemic levels of the proinflammatory cytokines tumor necrosis factor alpha and interleukin-1β (IL-1β) and T-cell mediators, such as IL-2 and gamma interferon, that are released from antigen presenting cells and T cells (13, 27). This can cause hypotension, fever, and shock (9, 24, 37).
SAgs are produced mainly by the gram-positive bacteria Streptococcus pyogenes and Staphylococcus aureus (2, 27). In addition, some SAgs have also been found in other bacteria, e.g., the Mycoplasma arthitidis mitogen (10) and the Yersinia pseudotuberculosis mitogen (23).
S. pyogenes, a Lancefield group A streptococcus, is a human pathogen that causes a wide range of diseases, including acute tonsillitis, scarlet fever, necrotizing fasciitis, bacteremia, streptococcal toxic shock syndrome, and rheumatic fever (6, 11, 37). The streptococcal SAgs, which include streptococcal pyrogenic exotoxin A (SPE-A), -C, and -G to -J; SSA; and several allelic variants of streptococcal mitogenic exotoxin Z (SMEZ) are believed to play an important role as virulence factors in at least some of these diseases (7, 9, 24). Enterotoxins from S. aureus, which include staphylococcal enterotoxin A (SEA) through SEM and toxic shock syndrome toxin (TSST), cause food poisoning (except TSST) and toxic shock syndrome (13, 27, 23a).
Recently, two pyrogenic exotoxins from Streptococcus equi (SePE-H and SePE-I) were identified (4). These toxins are nearly identical to SPE-H and SPE-I, differing in just 3 amino acids (aa) and 1 aa, respectively. S. equi is a Lancefield group C streptococcus that causes strangles, a contagious inflammatory disease of the upper respiratory tract and associated lymph nodes of equids (18).
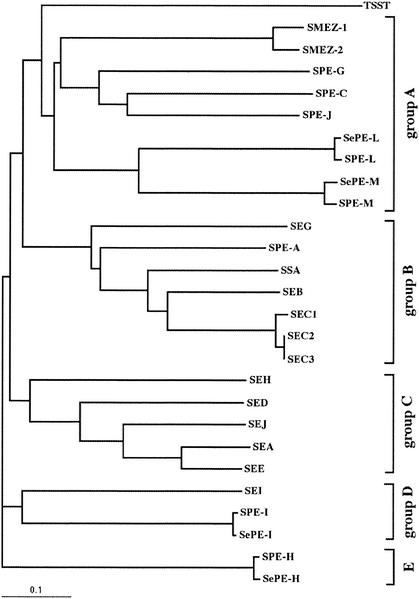
The structurally related staphylococcal and streptococcal SAgs share primary sequence identities from 20 to > 90% and have molecular masses of 24 to 28 kDa. They can be classified into four subfamilies (i) group A, which comprises SPE-C, SPE-G, SPE-J, and SMEZ; (ii) group B, which contains SEB, SEC1-3, SEG, SPE-A, and SSA; (iii) group C, with SEA, SED, SEE, SEH, and SEJ; (iv); group D, which contains SEI, SPE-I, and SePE-I; and group E, with SPE-H and SePE-H. TSST builds a separate branch within this family tree.
Several sag genes are located on mobile DNA elements, such as bacteriophage, integrated in the bacterial genome (14). Horizontal transfer of these mobile DNA elements is a proposed mechanism that might explain the close relation between SAgs from different bacterial species. This could also explain why individual bacterial isolates carry only certain combinations of sag genes. For example, speH and speI were found in S. pyogenes isolates at frequencies of only 24 and 16%, respectively, and both genes are located on prophage SF370.2 (14, 32). Thus far, no streptococcal or staphylococcal isolate has been found that carries a complete set of known sag genes.
Crystal structures of SEA, SEB, SEC2, SED, TSST, SPE-A, SPE-C, SPE-H, and SMEZ-2 show a conserved folding pattern comprising an NH2-terminal β-barrel globular domain and a COOH-terminal globular domain based on a β-grasp motif (3, 31).
Some SAgs, such as TSST and SEB, bind exclusively to the invariant MHC class II α-chain via a generic binding site located within the β-barrel domain (21, 36). Other SAgs, such as SPE-C, SPE-G, SPE-H, and SPE-J, contain a zinc binding motif within the COOH-terminal domain that is used to bind the polymorphic MHC class II β-chain via a tetrameric zinc coordination complex that involves the highly conserved His 81 residue on the HLA-DR1 β-chain (25, 26).
Recently, we identified four novel sag genes by mining the S. pyogenes M1 genomic database at the University of Oklahoma. The genes for speG, speH, speJ, and speI were cloned and expressed in Escherichia coli, and the purified recombinant proteins showed the typical SAg features (32, 33). The S. pyogenes genome project was completed in 2000, and only one more sag gene was found; it was named speK. However, speK is a pseudogene with an incomplete open reading frame (ORF) (14).
We have now extended our search for novel SAgs by mining other streptococcal genome databases. We here describe the identification of two novel sag genes from S. equi (speLSe and speMSe) and their respective orthologues in S. pyogenes (speL and speM). (Two genes in this gene family were designated sepe-h and sepe-i in a previous publication [4].) One intriguing feature of the speL gene is the strong association to the M89 serotype, which is linked to acute rheumatic fever in New Zealand.
MATERIALS AND METHODS
Bioinformatic tools.
The novel S. equi SAgs were identified by searching the microbial genome databases at the National Center for Biotechnology Information (http://www.ncbi.nlm.nih.gov/Microb_blast/unfinishedgenome.html) with highly conserved β5 and α4 regions of streptococcal and staphylococcal SAgs, using a TBLASTN search program.
The ORFs were defined by translating the DNA sequences around the matching regions and aligning the protein sequences to known SAgs using ClustalW at http://clustalw.genome.ad.jp (39) and ClustalX. The leader sequences were predicted using the SignalP V1.1 server at http://www.cbs.dtu.dk/services/SignalP. (29). The SAg family tree was generated using ClustalW and the TreeView Computer program (30).
Genotyping of S. equi and S. pyogenes isolates.
The New Zealand S. pyogenes isolates were obtained from the Institute of Environmental Sciences and Research in Porirua, New Zealand. Isolate 33117 was obtained from Pasteur Institute, Lille, France. The S. equi isolates were obtained from the Department of Microbiology, Otago University, Dunedin, New Zealand.
The streptococcal isolates were grown in brain heart infusion medium (Difco) at 37°C, and genomic DNA was prepared as described previously (34). Genotyping was carried out by PCR with 50 ng of purified streptococcal genomic DNA using the specific primer pairs sepe-l/spe-l (5′-GCGGATCCGATACGTACAATACAAATG-3′; 5′-GCGAATTCAATAGCATTCGACC-3′), sepe-m/spe-m (5′-GCGGATCCGAGGGGACTATTAATATTAAG-3′; 5′-GCGAATTCGGTTTCTTGATACTAAC-3′).
A primer pair specific to a DNA region encoding the 23S rRNA (33) was used as a positive control.
Generation of recombinant SPE-L (rSPE-L) and rSPE-M.
The spe-l and spe-m genes were amplified by PCR from 50 ng of genomic DNA of isolates 10846 and FP 4223, respectively, using the same primers as for genotyping. The PCR products encoding the mature proteins without the predicted leader sequences were enriched using the Wizard PCR DNA purification system (Promega) and cloned into T-tailed pBluescript SK II vectors (Stratagene), and this was followed by transformation into E. coli XL1 blue.
The cloned sag genes were analyzed by the dideoxy chain termination method using a Licor automated DNA sequencer (model 4200). Three subclones from every cloning experiment were analyzed to ensure that no Taq polymerase-related mutations were introduced. The DNA sequences have been annotated in the EMBL/GenBank/DDBJ databases.
The speL and speM genes were cloned from pBluescript into the BamHI-EcoRI cloning site of pET32-3c expression vector. This vector is a modified version of pET32a (Novagene) that expresses the highly specific protease 3C cleavage site (EVLFQ|GP [vertical bar indicates cleavage site]) from a picornavirus (40) just upstream of the inserted DNA. rSPE-L and rSPE-M were expressed in E. coli AD494(DE3) (Novagene) as thioredoxin (Trx) fusion proteins. Cultures were grown at 30°C and induced for 3 to 4 h after adding 0.2 mM isopropyl-β-d-thiogalactopyranoside (IPTG).
The Trx fusion proteins were purified on Ni2+ IDA Sepharose (Sigma), and the mature proteins were cleaved off from Trx on the column using protease 3C (provided by Keith Hudson, University of Oxford, Oxford, United Kingdom) overnight at room temperature. The eluates containing the recombinant toxins were collected and analyzed on sodium dodecyl sulfate-12.5% polyacrylamide gels according the procedure of Laemmli.
Toxin proliferation assay.
Human peripheral blood lymphocytes (PBLs) were purified from blood of a healthy donor by Histopaque Ficoll (Sigma) fractionation. The PBLs were incubated in 96-well round-bottom microtiter plates at 105 cells per well with RPMI-10 (RPMI with 10% fetal calf serum) containing various dilutions of recombinant toxins. The dilution series was performed in 1:5 steps from a starting toxin concentration of 10 ng/ml. After 3 days 0.1 μCi of [3H]thymidine was added to each well and cells were incubated for another 24 h. Cells were harvested, and the radiation in cells was counted on a scintillation counter.
TcR Vβ analysis.
Vβ enrichment analysis was performed by anchored multiprimer amplification. Human PBLs were incubated with recombinant toxin (20 pg/ml) at 106 cells/ml for 3 days. A twofold volume expansion of the culture followed, with medium containing IL-2 at 20 ng/ml. After another 24 h, stimulated and resting cells were harvested and RNA was prepared using Trizol reagent (Life Technologies). A 500-bp β-chain DNA probe was obtained by anchored multiprimer PCR as described previously (20), radiolabeled, and hybridized to individual Vβs and a Cβ DNA region dot blotted on a nylon membrane. The membrane was analyzed on a Molecular Dynamics Storm PhosphorImager using ImageQuant software. Individual Vβs were expressed as a percentage of all the Vβs determined by hybridization to the Cβ probe.
Radiolabeling and LG-2 binding experiments.
Recombinant toxin was radioiodinated by the chloramine T method as previously described (25). Labeled toxin was separated from free iodine by size exclusion chromatography using Sephadex G-25 (Pharmacia). LG2 cells were used for cell binding experiments, as previously described (25). Briefly, cells were harvested, resuspended in RPMI-10, and mixed at 106 cells/ml with 125I-tracer toxin (1 ng) and 0.0001 to 10 μg of unlabeled toxin and incubated at 37°C for 1 h. After washing with ice cold RPMI the pelleted cells were analyzed in a gamma counter.
For competitive binding studies, 1 ng of 125I-tracer toxin (rSPE-L or rSPE-M) was incubated with 0.0001 to 10 μg of unlabeled toxin (rSPE-L, rSPE-M, rSPE-C, rSEB, and rTSST) for 1 h.
Seroconversion experiments.
Five microliters of serum from human healthy donors were mixed with 10 μl of phosphate-buffered saline and 10 μl of 125I-labeled rSPE-L or rSPE-M and incubated for 1 h at 37°C. As controls, bovine serum albumin or rabbit antiserum against SPE-C or SMEZ was used instead of human sera. After adding 50 μl of protein A-staphylococcus cells (Toxin Technology) the samples were incubated for another 30 min at 4°C before the cells were spun down, washed in 1 ml of phosphate-buffered saline, and counted in a Cobra Gamma counter.
Nucleotide sequence accession numbers.
The accession numbers for the speL and speM genes are AF514282 and AF514283, respectively.
RESULTS
Identification and sequence analysis of SAgs.
A number of complete and incomplete microbial genome projects are accessible at the National Center for Biotechnology Information Web page, which can be mined for DNA sequences of interest using standard BLAST search tools (http://www.ncbi.nlm.nih.gov/Microb_blast/unfinishedgenome.html). The genome databases of Streptococcus gordonii, Streptococcus pneumoniae, S. equi, and Streptococcus mutans were searched with a SAg peptide sequence corresponding to the highly conserved α4 region using the TBLASTN program.
Four significant matches and predicted ORFs with homology to streptococcal and staphylococcal SAgs were found by aligning translated DNA sequences with complete protein sequences of known SAgs. All ORFs were identified from the incomplete S. equi genome database at the Sanger Center, which contains a collection of more than 200 DNA sequence contiguous sequences derived from a shotgun plasmid library of the complete S. equi genome.
Two of these ORFs correlate with the previously described SePE-I and SePE-H (4). The third ORF identified showed 99% nucleotide identity to the hypothetical exotoxin gene speL found on the prophage ΦNIH1.1. sequence (NC003157) (22). This was labeled speLSe according to the S. equi nomenclature (S. equi pyrogenic exotoxin L). The fourth ORF showed no significant sequence homology to any known SAg, but contained the highly conserved SAg α4 peptide sequence and was named speMSe. The speLSe and speMSe genes are adjacent at the 5′ end of a 4,470-bp contiguous sequence separated by a 266-bp intergenic region.
Genotyping of S. equi and S. pyogenes isolates.
Genomic DNA from eight S. equi isolates were screened by PCR using specific primer pairs for the speLSe and speMSe genes. In addition, a primer pair specific to a streptococcal DNA region encoding the 23S rRNA was used as a positive control. Neither speLSe nor speMSe could be detected in any of the S. equi isolates, suggesting that they are located on mobile DNA elements and thus restricted in their distribution to certain S. equi isolates (data not shown).
Screening of S. pyogenes isolates (including 29 M-types and three MNT) identified the speLSe gene in 6 of 40 cases (15%) and the speMSe gene in 2 of 40 cases (5%) (Table 1) . The speLSe gene was restricted to only 5 M-types (M28, M41, M56, M59, and M89), and the speMSe gene was found in only 2 M-types (M80 and M92).
TABLE 1.
Genotyping of S. pyogenes isolates from New Zealanda
| S. pyogenes isolate | M/emm | Site | Disease or condition | PCR result with primer for:
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 23S | speA | speC | speGb | speHb | speI | speJ | ssa | speL | speM | smezb | ||||
| FP 1943 | M53 | TS | ST | + | − | + | + | − | − | + | − | − | − | + |
| FP 2658 | M59 | TS | ST | + | − | − | + | − | − | + | − | + | − | + |
| FP 4223 | M80 | TS | ST | + | − | − | + | − | − | + | − | − | + | + |
| FP 5417 | M41 | TS | ST | + | + | − | + | − | − | + | − | + | − | + |
| FP 5971 | M57 | TS | ST | + | + | + | + | + | − | + | − | − | − | + |
| 1/5045 | M4 | TS | ST | + | + | + | + | − | − | + | + | − | − | + |
| 82/20 | M4 | SK | Ulcer | + | − | − | + | − | − | + | + | − | − | + |
| 85/167 | M12 | TS | ST | + | − | − | + | + | + | + | − | − | − | + |
| 85/314 | M89 | WS | Wound | + | − | − | + | − | − | + | − | + | − | + |
| 85/437 | M81 | WS | Infections eczema | + | − | + | + | − | − | + | + | − | − | + |
| 85/723 | M22 | Ear | Otitis | + | − | + | + | − | − | + | + | − | − | + |
| 86/435 | M4 | TS | RF | + | − | + | + | − | − | + | + | − | − | + |
| 87/19 | M12 | TS | ST | + | + | + | + | + | + | + | − | − | − | + |
| 89/26 | M1 | TS | AGN | + | + | − | + | − | − | + | − | − | − | + |
| 90/424 | M4 | TS | ST | + | + | + | + | − | − | + | + | − | − | + |
| 94/229 | M49 | HVS | Endometritis | + | + | − | + | + | + | + | − | − | − | −c |
| 94/712 | M89 | WS | Cellulitis | + | − | + | + | − | − | + | − | − | − | + |
| 95/31(2) | M89 | WS | Abscess | + | − | − | + | − | − | + | − | − | − | + |
| 96/1 | M4 | HVS | Endometritis | + | − | + | + | − | − | + | + | − | − | + |
| 9779 | emm56 | TS | ST | + | − | − | + | − | − | + | − | + | − | + |
| 9893 | M82 | TS | ST | + | − | + | + | + | + | + | − | − | − | + |
| 10019 | emm44 | TS | ST | + | − | + | + | + | + | + | − | − | − | + |
| 10303 | emm59 | TS | ST | + | − | − | + | − | − | + | − | + | − | + |
| 10438 | ST3018 | TS | ST | + | + | − | + | − | − | + | − | − | − | + |
| 10463 | emm49 | TS | ST | + | + | − | + | − | − | + | + | − | − | + |
| 10649 | ST2267 | TS | ST | + | − | − | + | − | − | + | − | − | − | + |
| 10763 | M88 | TS | ST | + | − | + | + | − | − | + | + | − | − | + |
| 10791 | MNT | TS | ST | + | − | + | + | + | + | + | + | − | − | + |
| 10989 | M87 | TS | ST | + | − | − | + | − | − | + | − | − | − | + |
| 11070 | emm65 | TS | ST | + | − | − | + | + | − | + | − | − | − | −c |
| 11152 | M85 | TS | ST | + | − | − | + | + | − | + | − | − | − | −c |
| 11222 | M92 | TS | ST | + | + | + | + | + | − | + | − | − | + | + |
| 11227 | emm14 | TS | ST | + | − | − | + | − | − | + | − | − | − | + |
| 11276 | MNT | TS | ST | + | + | − | + | − | − | + | + | − | − | + |
| 11574 | ST809 | TS | ST | + | − | − | + | − | − | + | − | − | − | + |
| 11646 | ST4547 | TS | ST | + | − | − | + | − | − | + | + | − | − | + |
| 11686 | M91 | TS | ST | + | − | − | + | − | − | + | + | − | − | + |
| 11789 | MNT | TS | ST | + | + | + | + | − | − | + | − | − | − | + |
| ATCC | M1 | Wound | ND | + | − | + | + | + | + | + | − | − | − | + |
| 33117 | T28R28 | ND | STSS | + | − | − | + | − | − | + | − | + | − | + |
| % With positive PCR result | 100 | 31 | 42 | 100 | 26 | 16 | 100 | 32 | 15 | 5 | 92 | |||
| Strain M89 | ||||||||||||||
| 85/314 | M89 | WS | Wound | + | − | − | + | − | − | + | − | + | − | + |
| 95/361 | M89 | PS | Abscess | + | − | − | + | + | − | + | − | + | − | + |
| 82/675 | M89 | WS | Wound | + | − | + | + | − | − | + | − | + | − | + |
| 95/31 | M89 | WS | Abscess | + | − | − | + | − | − | + | − | − | − | + |
| 94/712 | M89 | WS | Cellulitis | + | − | + | + | − | − | + | − | + | − | + |
| 10846 | M89 | TS | ST | + | + | − | + | − | − | + | − | + | − | + |
| 89/54 | M89 | TS | ST | + | + | − | + | − | − | + | − | + | − | + |
| 94/11 | M89 | PS | Abscess | + | − | − | + | − | − | + | − | + | − | + |
| 95/127 | M89 | BC | Cellulitis | + | − | − | + | − | − | + | − | + | − | + |
| 84/781 | M89 | TS | ST | + | + | − | + | − | − | + | − | − | − | + |
| 96/364 | M89 | BC | Burns | + | − | − | + | − | − | + | − | − | − | + |
| % With positive PCR result | 100 | 27 | 18 | 100 | 9 | 0 | 100 | 0 | 73 | 0 | 100 | |||
Fifty-one S. pyogenes isolates (38 from New Zealand, 1 from France, 1 ATCC reference strain, and 11 S. pyogenes M89 isolates collected in New Zealand) were genotyped. The results are based on PCR analysis using purified genomic DNA and specific primers for each sag gene. The primers for speL and speM were designed using the DNA sequences of the orthologous speLSe and speMSe genes from S. equi. Site and disease abbreviations are as follows: TS, throat site; WS, wound site; SK, skin; PS, pus site; HVS, high vaginal site; BC, blood culture; ST, sore throat; RF, rheumatic fever; AGN, acute glumerulonephritis; STSS, streptococcal toxic shock; ND, not determined.
Reported previously (34).
Positive by Southern blotting.
Interestingly, the M28 isolate was obtained from a patient suffering from streptococcal toxic shock syndrome, and M89 strains are strongly associated with acute rheumatic fever in New Zealand (28).
New Zealand S. pyogenes M89 isolates were genotyped for the spe-l gene, and 8 of 11 (73%) were positive, indicating a strong association between this M-type and the speL gene (Table 1).
Cloning and DNA analysis of speL and speM from S. pyogenes.
The speLSe gene was cloned from isolate 10846 (M89), and DNA sequence analysis revealed a strong sequence homology (99% nucleotide identity) to the S. equi speLSe. The gene was named speL according to the S. pyogenes nomenclature for the streptococcal pyrogenic exotoxin family. The speLSe and speL genes differ by only 7 bp, and the deduced protein sequences differ by 4 aa, of which two differences are conservative exchanges (Y225H and E229D) and two are moderate (I112S and N233D). Furthermore, the speL gene is 100% identical to the hypothetical exotoxin gene speL found on prophage ΦNIH1.1. sequence (NC003157).
The speMSe was cloned from isolate FP4223 (serotype M80), and DNA sequence comparison showed strong nucleotide homology to speMSe from S. equi (98.1% nucleotide identity) and was therefore labeled spe-m. The speMSe and speM genes differ by 13 bp, and the deduced protein sequences differ by 8 aa, of which 5 are conservative exchanges (V41I, I51M, H55Y, Y74H, and E137D). The three nonconservative exchanges are E37V, G175D, and N191K.
The calculated molecular masses are 27.4 kDa (SPE-LSe and SPE-L) and 26.2 kDa (SPE-MSe and SPE-M), and the calculated isoelectric points are 6.69 (SPE-LSe), 6.53 (SPE-L), 6.7 (SPE-MSe), and 7.1 (SPE-M). The minor differences between SPE-LSe and SPE-L and between SPE-MSe and SPE-M suggest that the proteins are orthologous with identical or very similar functions in the two streptococcal species.
A revised SAg family tree, based on primary amino acid sequence homology, shows that SPE-LSe and SPE-L as well as SPE-MSe and SPE-M belong to the same clade as SMEZ, SPE-C, SPE-G, and SPE-J (group A) but build a separate branch within that group (Fig. 1). SPE-LSe-SPE-L and SPE-MSe-SPE-M are most closely related to each other (42% amino acid identity and 51% similarity) followed by SPE-C (32% amino acid identity and 40% similarity).
FIG. 1.
Family tree of streptococcal and staphylococcal SAgs. The tree was created using ClustalW (39) and the TreeView computer program (30). The novel SAgs belong to group A, together with SPE-C, SPE-G, SPE-J, and SMEZ, but build a separate branch within this group.
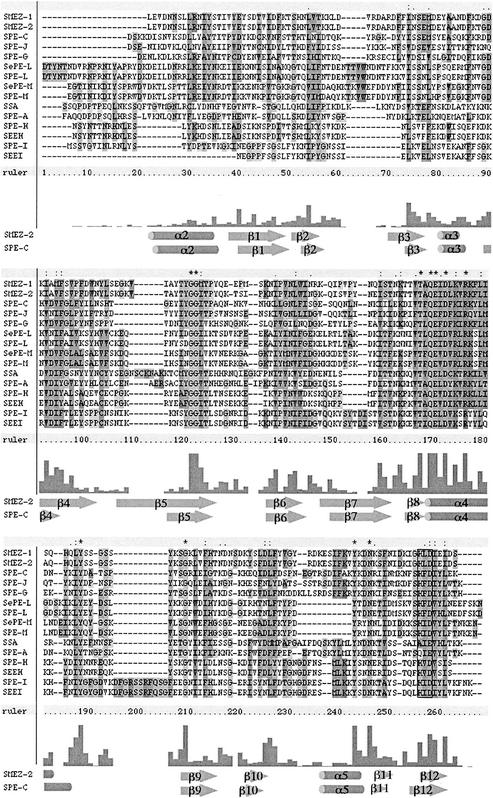
All novel SAgs contain a zinc binding motif near the C terminus that is common among most of the streptococcal SAgs, including all members of group A. Zinc is essential for binding to the polymorphic MHC class II β-chain via a divalent zinc ion (26, 35). In SPE-C, the zinc-binding residues are H167, H201, and D203, and in SMEZ-2 the zinc ion is bound by residues H162, H202, and D204 (3). The multiple protein sequence alignment (Fig. 2) shows that the most likely candidates for zinc binding are residues H191, H221, and D223 for SPE-LSe and SPE-L and H186, H217, and D218 for SPE-MSe and SPE-M.
FIG. 2.
Multiple alignment of streptococcal SAg protein sequences. The protein sequences of mature proteins were aligned using the ClustalX computer program. The clear box near the C terminus represents a primary zinc binding motif (H-X-D), a feature of all streptococcal toxins except SPE-A and SSA. Structural elements of SMEZ-2 and SPE-C, respectively, are shown below.
One important difference between the novel SAgs and other streptococcal SAgs is a gap in amino acid sequence between residues 207 and 208 (in SPE-LSe and SPE-L) and residues 202 and 203 (in SPE-MSe and SPE-M) (Fig. 2). In the protein structures of SPE-C, SPE-H, and SMEZ-2, the amino acids in this region form part of the β10-α5 loop and the structure determining the α5 helix (3, 35). Structure-determining regions, unlike surface loops, are generally strongly conserved in SAgs, suggesting that there is potential for a major difference in the SPE-L/SPE-M protein structure in this region compared to other SAgs.
Expression of rSPE-L and rSPE-M.
To produce recombinant proteins of SPE-L and SPE-M, the individual subcloned genes (coding for the mature toxins without leader sequence) were transferred to expression vector pET32-3c and transformed into E. coli AD494(DE3). Fusion proteins of Trx-SPE-L and Trx-SPE-M were completely soluble and gave yields of approximately 20 mg per liter. The recombinant toxins were cleaved off from the Trx using protease 3C, while still bound on the affinity column. The recombinant proteins differ from their native counterparts by four additional N-terminal residues (GPGS) introduced by the BamHI restriction site and the protease 3C recognition site. However, a potential influence on the function of the recombinant proteins seems rather unlikely, as the crystal structures of the closely related proteins SMEZ-2, SPE-C, and SPE-H show that the N terminus is facing away from both the TcR and the MHC class II binding site (3, 35).
Eluates containing the purified toxins were collected and analyzed for purity on a sodium dodecyl sulfate-12% polyacrylamide gel.
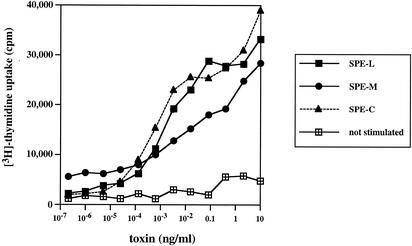
To ensure the native conformation of the purified recombinant toxins, a standard [3H]thymidine incorporation assay was performed to test for their potency to stimulate PBLs. Both toxins were active on human T cells (Fig. 3). rSPE-C was included as a reference protein.
FIG. 3.
Stimulation of human T cells with recombinant toxins. PBLs were isolated from human blood samples and incubated with various concentrations of recombinant toxin (in duplicates). After 3 days, 0.1 μCi of [3H]thymidine was added, and cells were incubated for another 24 h before being harvested and counted on a scintillation counter.
The half-maximal responses for rSPE-L and rSPE-M were 1 and 10 pg/ml, respectively. No activity was detected at less than 0.1 pg/ml. SPE-L was as potent as rSPE-C that also had a half-maximal value of 1 pg/ml. rSPE-M was less active than rSPE-C but still more potent than the previously described SPE-H (50 pg/ml) (33).
Significant seroconversion against SPE-L and SPE-M was detected in sera from healthy human blood donors. Out of twenty subjects, seven were identified with seroconversion against SPE-L, and six serum samples had significant antibody titers against SPE-M (data not shown). These results suggest that both toxins are actually expressed by the bacteria.
Vβ specificity of recombinant toxins.
The human TcR Vβ specificity of the recombinant toxins was determined by multiprimer anchored PCR and dot blot analysis using a panel of 21 human Vβ DNA regions. The Vβ enrichment after stimulation with toxin was compared to the Vβ profile of PBLs stimulated with the unspecific T-cell mitogen concanavalin A (ConA).
Both toxins showed very similar results, with Vβ1.1 TcR being the primary target. T cells carrying the Vβ1.1 TcR were stimulated >80 times and nearly 70 times more with rSPE-L or rSPE-M, respectively, than with ConA (Table 2).
TABLE 2.
Vβ specificity of recombinant toxins on human PBLsa
| Vβ cDNA | % of Vβ enrichment after stimulation with:
|
||
|---|---|---|---|
| ConA | SPE-L | SPE-M | |
| 1.1 | 0.1 | 8.44 | 6.75 |
| 2.1 | 3.94 | 4.46 | 4.2 |
| 3.1 | 19.57 | 6.53 | 9.83 |
| 4.1 | 0.12 | 0.98 | 1.41 |
| 5.1 | 1.82 | 2.78 | 3.69 |
| 5.3 | 12.06 | 10.2 | 13.96 |
| 5.8 | 3.31 | 4.49 | 4.43 |
| 6.3 | 1.03 | 1.57 | 2.15 |
| 6.4 | 0.63 | 1.41 | 1.47 |
| 6.9 | 5.96 | 4.85 | 4.92 |
| 7.3 | 0.84 | 0.94 | 1.1 |
| 7.4 | 2.31 | 1.71 | 1.47 |
| 8.1 | 0.3 | 0.68 | 0.79 |
| 9.1 | 1.34 | 1.78 | 2.05 |
| 12.3 | 15.36 | 7.76 | 8.93 |
| 12.5 | 1.17 | 1.38 | 1.94 |
| 14.1 | 0.3 | 0.79 | 0.95 |
| 15.1 | 2.26 | 3.92 | 4.25 |
| 17.1 | −0.07 | 1.05 | 1.12 |
| 18.1 | 1.51 | 2.54 | 3.13 |
| 22a | 1.1 | 2.09 | 2.27 |
| 23.1 | 0.45 | 1.39 | 1.41 |
| Total | 71.6 | 78 | 82.2 |
Human PBLs were incubated with recombinant toxin (20 pg/ml) for 4 days. Relative enrichment of Vβ cDNAs was analyzed from RNA of toxin-stimulated and ConA-stimulated PBLs by anchored-primer PCR and reverse dot blot to a panel of 22 different Vβ cDNAs. The figures represent the percentage of each Vβ with respect to total Cβ. Significant responses are underlined.
Interestingly, the total of the Vβs stimulated with rSPE-L or rSPE-M was only 78 and 82%, respectively, suggesting that one or more additional Vβs were stimulated which are not represented in the panel. To further investigate this possibility, the Vβ cDNAs from rSPE-L- and rSPE-M-stimulated T cells were cloned into a pBluescript vector and the DNA sequences of 10 randomly selected clones were analyzed. Five out of five cDNAs from rSPE-L-stimulated T cells and four of five cDNAs from rSPE-M stimulated T cells were identified as Vβ1.1. One rSPE-M-expanded cDNA was identified as Vβ5.8. However, Vβ 5.8 was not significantly enriched by either toxin (around 4.5%) compared to ConA-stimulated cells (3.3%) (Table 2).
MHC class II binding.
As previously mentioned, the protein sequences of SPE-L and SPE-M contain the conserved zinc binding motif that is required for binding to the polymorphic MHC class II β-chain.
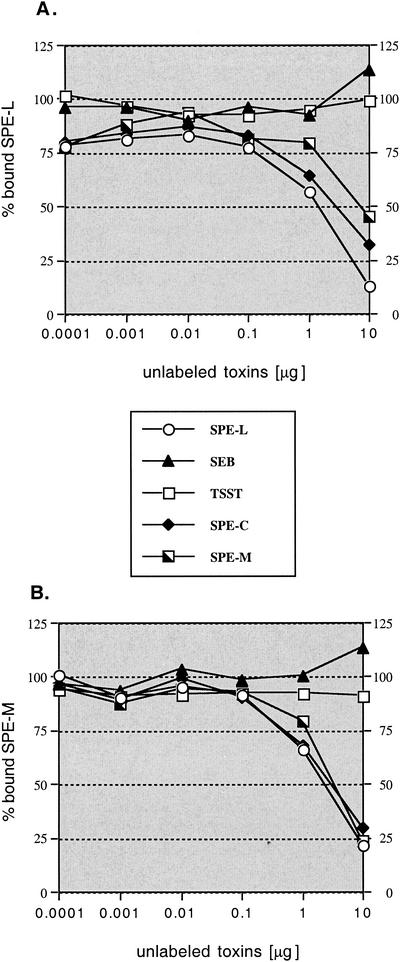
In an attempt to determine the orientation of the toxins on MHC class II, competition binding experiments were performed. The recombinant toxins were radiolabeled and tested with excess of unlabeled toxin for binding to LG-2 cells. rSEB, rTSST, and rSPE-C were used as reference proteins. SPE-C binds exclusively to the MHC class II β-chain using the zinc binding motif (25, 26), while SEB and TSST both exclusively bind to the MHC class II α-chain in a different, zinc-independent binding mode (1, 21, 36). The results are shown in Fig. 4. Binding of radiolabeled rSPE-L or rSPE-M was inhibited with excess amounts of unlabeled rSPE-C, rSPE-L, and rSPE-M. In contrast, excess amounts of unlabeled rSEB or rTSST did not influence binding of radiolabeled rSPE-L and rSPE-M. These results suggest that both, SPE-L and SPE-M, bind MHC class II exclusively to the β-chain in a zinc-dependent binding mode. This is a consistent feature among all group A members of the SAg family.
FIG. 4.
Competition binding studies with rSPE-L and rSPE-M. LG-2 cells were incubated in duplicate with 1 ng of 125I-labeled recombinant toxin and increasing amounts of unlabeled toxins. After 1 h cells were washed and counted. (A) Competition assay with labeled rSPE-L; (B) competition assay with labeled rSPE-M.
DISCUSSION
Two novel sag genes, speLSe and speMSe, have been identified from the S. equi genome database at the Sanger Center. Subsequently, the orthologue genes speL and speM genes were identified from S. pyogenes.
The increasing number of genome sequencing projects and the availability of the raw sequencing data on the Internet facilitates the rapid identification of novel genes by sequence similarity. We have recently increased the number of known streptococcal SAgs after searching the S. pyogenes M1 genome database at Oklahoma University (32, 33). Interestingly, only three sag genes (speG, speJ, and smez) were found on all analyzed S. pyogenes isolates, whereas all other streptococcal SAg genes occur with different frequencies due to their location on mobile genetic elements. Horizontal gene transfer appears to be the likely mechanism for the distribution of sag genes, not only between different S. pyogenes isolates, but also between different streptococcal species. The speJ and speI genes occur with frequencies of 26 and 16%, respectively, within S. pyogenes isolates, and orthologues of these genes (sepe-h and sepe-i) have recently been found in S. equi (4). This suggests that many more SAgs are likely to exist in other streptococcal isolates. Genotyping of 40 S. pyogenes isolates showed that speL and speM occur with low frequencies (15 and 5%, respectively) and are therefore likely to be on mobile DNA element(s). The S. equi orthologues speLSe and speMSe could not be detected in any of the analyzed S. equi isolates, suggesting that they are rare in this species. The speL gene is identical to a hypothetical SAg gene that has recently been identified on the streptococcal prophage ΦNIH1.1. Ikebe et al. showed that all of 18 M3/T3 isolates recovered from Japan during or after 1992 have the speL gene, while none of 10 T3 isolates recovered before 1973 have this gene (22). This suggests a very recent horizontal transfer of speL between different S. pyogenes isolates and between S. pyogenes and S. equi. The fact that this prophage does not carry the speM gene and the fact that none of our analyzed S. pyogenes isolates carry both sag genes suggest that speM is located on a different prophage. However, the speI gene also could not be detected in all speH-positive isolates (Table 1), despite the fact that both genes are located on the SF370.2 prophage on the S. pyogenes M1 SF370 genome (14). A possible reason for the separation from speL is that speM might have been lost in some S. pyogenes isolates during integration of the prophage into the streptococcal genome.
One of the most interesting outcomes of this study is the finding that the speL gene is linked to S. pyogenes M89, a serotype that is strongly associated with acute rheumatic fever in New Zealand (28). SAgs have been implicated in acute rheumatic fever, but their role in the pathology of the disease remains elusive (6). Screening of a much larger panel of clinical isolates is currently under way to determine the strength of this linkage between spe-l and strains causing acute rheumatic fever.
The novel toxins are closely related to the streptococcal and staphylococcal SAgs. Recombinant forms of SPE-L and SPE-M are extremely potent stimulators of human PBLs at nanomolar concentrations, confirming their role as SAgs. Seroconversion against SPE-L and SPE-M was observed in several blood samples from healthy donors, suggesting in vivo expression of both toxins. Despite their highly conserved core structure, individual SAgs differ remarkably in their surface-exposed regions. This explains why immune responses against SAgs are highly specific, e.g., polyclonal serum raised against a certain SAg does not cross-react with any other SAg (data not shown). Therefore, seroconversion against a particular SAg is a strong indicator for the actual production of this SAg by the bacteria and also suggests a potential role as a virulence factor.
The data presented here suggest that SPE-L and SPE-M bind MHC class II exclusively at the β-chain via a zinc binding complex. This assumption is supported by the fact that both toxins contain the characteristic zinc binding motif (H-X-D) close to the C terminus and by the results from the competitive binding assays. Excess concentrations of rSPE-C, a toxin that exclusively binds to the MHC class II β-chain (26) clearly inhibited SPE-L and SPE-M from binding to LG-2 cells. In contrast, the typical MHC class II α-chain binding toxins SEB and TSST showed no inhibition effect. This MHC class II binding mode appears to be conserved among all group A members of the SAg family (Fig. 1). SSA and SPE-A are the only streptococcal SAgs known thus far that lack the zinc binding motif and are unable to bind to the MHC class II α-chain. Both toxins belong to the group B clade in the SAg family tree and are more closely related to the staphylococcal enterotoxins than to any other streptococcal toxin.
Interestingly, SPE-L and SPE-M both stimulate mainly Vβ 1.1-expressing T cells. Usually, SAgs can be distinguished by their characteristic combination of Vβ targets. This finding might explain why none of the analyzed streptococcal isolates carried both genes, speL and speM, as the need to activate a single Vβ can met by a single toxin and two toxins with the same function would be unlikely to offer a significant selective advantage.
SPE-L and SPE-M differ from their S. equi orthologues by only 4 and 8 aa, respectively, and most of the exchanges are conservative. All of the nonconservative exchanges are at amino acid positions that are not well conserved among the SSAs. This suggests that SPE-LSe and SPE-MSe are likely to function in an identical fashion to their S. pyogenes orthologues SPE-L and SPE-M. It is not known yet what role SAgs play in S. equi. Artiushin and coworkers recently reported that SePE-I and SePE-H were highly mitogenic on horse PBLs and pyrogenic for rabbits. Furthermore, horses that had recovered from strangles or been immunized with SePE-I were resistant to the pyrogenic effect of SePE-I (4). Interestingly, an epidemic outbreak of nephritis in Nova Serrana, Brazil, has recently been reported, and throat cultures indicated that nephritis was associated with group C S. equi (5).
Two novel SAgs were found in streptococcal strains belonging to two different Lancefield groups, group A and group C. The sag genes are most likely located on a mobile DNA element that allows horizontal transfer of these genes between different streptococcal species, such as S. equi and S. pyogenes. The significant association of speL to S. pyogenes strain M89, which causes acute rheumatic fever, suggests a potential involvement of SPE-L in this disease. However, this has to be reevaluated after screening a larger panel of S. pyogenes isolates. It remains to be seen whether sag genes will also be found in other non-group A streptococci.
Acknowledgments
We gratefully acknowledge the S. equi Sequencing Group at the Sanger Institute for making their DNA sequences available on the Internet. We thank Diana Martin, Institute of Environmental Sciences and Research, Porirua, New Zealand, for the New Zealand S. pyogenes isolates; John Tagg, Otago University, Dunedin, New Zealand, for the S. equi isolates; and Heide Mueller-Alouf, Pasteur Institute, Lille, France, for the S. pyogenes 33117 isolate.
This study was supported by the Health Research Council of New Zealand and by an Early Career Excellence Grant from the University of Auckland.
Editor: V. J. DiRita
REFERENCES
- 1.Acharya, K. R., E. F. Passalacqua, E. Y. Jones, K. Harlos, D. I. Stuart, R. D. Brehm, and H. S. Tranter. 1994. Structural basis of superantigen action inferred from crystal structure of toxic-shock syndrome toxin-1. Nature 367:94-97. [DOI] [PubMed] [Google Scholar]
- 2.Alouf, J. E., H. Mueller-Alouf, and W. Koehler. 1999. Superantigenic Streptococcus pyogenes erythrogenic/pyrogenic exotoxins, p. 567-588. In J. E. Alouf and J. H. Freer (ed.), Sourcebook of bacterial protein toxins. Academic Press, San Diego, Calif.
- 3.Arcus, V. L., T. Proft, J. A. Sigrell, H. M. Baker, J. D. Fraser, and E. N. Baker. 2000. Conservation and variation in superantigen structure and activity highlighted by the three-dimensional structures of two new superantigens from Streptococcus pyogenes. J. Mol. Biol. 299:157-168. [DOI] [PubMed] [Google Scholar]
- 4.Artiushin, S. C., J. F. Timoney, A. S. Sheoran, and S. K. Muthupalani. 2002. Characterization and immunogenicity of pyrogenic mitogens SePE-H and SePE-I of Streptococcus equi. Microb. Pathog. 32:71-85. [DOI] [PubMed] [Google Scholar]
- 5.Balter, S., A. Benin, S. W. Pinto, L. M. Teixeira, G. G. Alvim, E. Luna, D. Jackson, L. LaClaire, J. Elliott, R. Facklam, and A. Schuchat. 2000. Epidemic nephritis in Nova Serrana, Brazil. Lancet 355:1776-1780. [DOI] [PubMed] [Google Scholar]
- 6.Bathnagar, A., A. Grover, and N. K. Ganguly. 1999. Superantigen-induced T cell responses in acute rheumatic fever and chronic rheumatic heart disease patients. Clin. Exp. Immunol. 116:100-106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Bernal, A., T. Proft, J. D. Fraser, and D. N. Posnett. 1999. Superantigens in human disease. J. Clin. Immunol. 19:149-157. [DOI] [PubMed] [Google Scholar]
- 8.Betley, M. J., D. W. Borst, and L. B. Regassa. 1992. Staphylococcal enterotoxins, toxic shock syndrome toxin and streptococcal exotoxins: a comparative study of their molecular biology. Chem. Immunol. 55:1-35. [PubMed] [Google Scholar]
- 9.Bohach, G. A., D. J. Fast, R. D. Nelson, and P. M. Schlievert. 1990. Staphylococcal and streptococcal pyrogenic toxins involved in toxic shock syndrome and related illnesses. Crit. Rev. Microbiol. 17:251-272. [DOI] [PubMed] [Google Scholar]
- 10.Cole, B. C., and C. L. Atkin. 1991. The Mycoplasma arthritidis T-cell mitogen, MAM: a model superantigen. Immunol. Today 12:271-276. [DOI] [PubMed] [Google Scholar]
- 11.Cone, L. A., P. M. Woodard, P. M. Schlievert, and G. S. Tomory. 1987. Clinical and bacteriologic observations of a toxic shock-like syndrome due to Streptococcus pyogenes. N. Engl. J. Med. 317:146-149. [DOI] [PubMed] [Google Scholar]
- 12.Dellabona, P., J. Peccoud, J. Kappler, P. Marrack, C. Benoist, and D. Mathis. 1990. Superantigens interact with MHC class II molecules outside of the antigen groove. Cell 62:1115-1121. [DOI] [PubMed] [Google Scholar]
- 13.Fast, D. J., P. M. Schlievert, and R. D. Nelson. 1989. Toxic shock syndrome-associated staphylococcal and streptococcal pyrogenic toxins are potent inducers of tumor necrosis factor production. Infect. Immun. 57:291-294. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Ferretti, J. J., W. M. McShan, D. Ajdic, D. J. Savic, G. Savic, K. Lyon, C. Primeaux, S. Sezate, A. N. Suvorov, S. Kenton, H. S. Lai, S. P. Lin, Y. Qian, H. G. Jia, F. Z. Najar, Q. Ren, H. Zhu, L. Song, J. White, X. Yuan, S. W. Clifton, B. A. Roe, and R. McLaughlin. 2001. Complete genome sequence of an M1 strain of Streptococcus pyogenes. Proc. Natl. Acad. Sci. USA 98:4658-4663. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Fleischer, B., and H. Schrezenmeier. 1988. T cell stimulation by staphylococcal enterotoxins. Clonally variable response and requirement for major histocompatibility complex class II molecules on accessory or target cells. J. Exp. Med. 167:1697-1707. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Fraser, J., V. Arcus, P. Kong, E. Baker, and T. Proft. 2000. Superantigens—powerful modifiers of the immune system. Mol. Med. Today 6:125-132. [DOI] [PubMed] [Google Scholar]
- 17.Fraser, J. D. 1989. High-affinity binding of staphylococcal enterotoxins A and B to HLA-DR. Nature 339:221-223. [DOI] [PubMed] [Google Scholar]
- 18.Harrington, D. J., I. C. Sutcliffe, and N. Chanter. 2002. The molecular basis of Streptococcus equi infection and disease. Microb. Infect. 4:501-510. [DOI] [PubMed] [Google Scholar]
- 19.Herman, A., J. W. Kappler, P. Marrack, and A. M. Pullen. 1991. Superantigens: mechanism of T-cell stimulation and role in immune responses. Annu. Rev. Immunol. 9:745-772. [DOI] [PubMed] [Google Scholar]
- 20.Hudson, K. R., H. Robinson, and J. D. Fraser. 1993. Two adjacent residues in Staphylococcal enterotoxins A an E determine T cell receptor Vβ specificity. J. Exp. Med. 177:175-185. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Hurley, J. M., R. Shimonkevitz, A. Hanagan, K. Enney, E. Boen, S. Malmstrom, B. L. Kotzin, and M. Matsumura. 1995. Identification of class II major histocompatibility complex and T cell receptor binding sites in the superantigen toxic shock syndrome toxin 1. J. Exp. Med. 181:2229-2235. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Ikebe, T., A. Wada, Y. Inagaki, K. Sugama, R. Suzuki, D. Tanaka, A. Tamari, Y. Fujinaga, Y. Abe, Y. Shimuzu, and H. Watanabe. 2002. Dissemination of the phage-associated novel superantigen gene speL in recent invasive and noninvasive Streptococcus pyogenes M3/T3 isolates in Japan. Infect. Immun. 70:3227-3233. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Ito, Y., J. Abe, K. Yoshino, T. Takeda, and T. Kohsaka. 1995. Sequence analysis of the gene for a novel superantigen produced by Yersinia pseudotuberculosis and expression of the recombinant protein. J. Immunol. 154:5896-5906. [PubMed] [Google Scholar]
- 23a.Jarraud, S., M. A. Peyrat, A. Lim, A. Tristan, M. Bes, C. Mougel, J. Etienne, et al. 2001. egc, a highly prevalent operon of enterotoxin gene, forms a putative nursery of superantigens in Staphylococcus aureus. J. Immunol. 166:669-677. [DOI] [PubMed] [Google Scholar]
- 24.Kotzin, B. L., D. Y. Leung, J. Kappler, and P. Marrack. 1993. Superantigens and their potential role in human disease. Adv. Immunol. 54:99-166. [DOI] [PubMed] [Google Scholar]
- 25.Li, P. L., R. E. Tiedemann, S. L. Moffat, and J. D. Fraser. 1997. The superantigen streptococcal pyrogenic exotoxin C (SPE-C) exhibits a novel mode of action. J. Exp. Med. 186:375-383. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Li, Y., H. Li, N. Dimasi, J. K. McCormick, R. Martin, P. Schnuck, P. M. Schlievert, and R. A. Mariuzza. 2001. Crystal structure of a superantigen bound to the high-affinity, zinc-dependent site on MHC class II. Immunity 14:93-104. [DOI] [PubMed] [Google Scholar]
- 27.Marrack, P., and J. Kappler. 1990. The staphylococcal enterotoxins and their relatives. Science 248:705-711. [DOI] [PubMed] [Google Scholar]
- 28.Martin, D. R., L. M. Voss, S. J. Walker, and D. Lennon. 1994. Acute rheumatic fever in Auckland, New Zealand: spectrum of associated group A streptococci different from expected. Pediatr. Infect. Dis. J. 13:264-269. [DOI] [PubMed] [Google Scholar]
- 29.Nielsen, H., J. Engelbrecht, S. Brunak, and G. von Heijne. 1997. Identification of prokaryotic and eukaryotic signal peptides and prediction of their cleavage sites. Protein Eng. 10:1-6. [DOI] [PubMed] [Google Scholar]
- 30.Page, R. D. M. 1996. TREEVIEW: an application to display phylogenetic trees on personal computers. Comput. Appl. Biosci. 12:357-358. [DOI] [PubMed] [Google Scholar]
- 31.Papageorgiou, A. C., and K. R. Acharya. 2000. Microbial superantigens: from structure to function. Trends Microbiol. 8:369-375. [DOI] [PubMed] [Google Scholar]
- 32.Proft, T., V. L. Arcus, V. Handley, E. N. Baker, and J. D. Fraser. 2001. Immunological and biochemical characterization of streptococcal pyrogenic exotoxins I and J (SPE-I and SPE-J) from Streptococcus pyogenes. J. Immunol. 166:6711-6719. [DOI] [PubMed] [Google Scholar]
- 33.Proft, T., S. L. Moffatt, C. J. Berkahn, and J. D. Fraser. 1999. Identification and characterization of novel superantigens from Streptococcus pyogenes. J. Exp. Med. 189:89-101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Proft, T., S. L. Moffatt, K. D. Weller, A. Paterson, D. Martin, and J. D. Fraser. 2000. The streptococcal superantigen SMEZ exhibits wide allelic variation, mosaic structure, and significant antigenic variation. J. Exp. Med. 191:1765-1776. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Roussel, A., B. F. Anderson, H. M. Baker, J. D. Fraser, and E. N. Baker. 1997. Crystal structure of the streptococcal superantigen SPE-C: dimerization and zinc binding suggest a novel mode of interaction with MHC class II molecules. Nat. Struct. Biol. 4:635-643. [DOI] [PubMed] [Google Scholar]
- 36.Seth, A., L. J. Stern, T. H. Ottenhoff, I. Engel, M. J. Owen, J. R. Lamb, R. D. Klausner, and D. C. Wiley. 1994. Binary and ternary complexes between T-cell receptor, class II MHC and superantigen in vitro. Nature 369:324-327. [DOI] [PubMed] [Google Scholar]
- 37.Stevens, D. L. 2000. Streptococcal toxic shock syndrome associated with necrotizing fasciitis. Annu. Rev. Med. 51:271-288. [DOI] [PubMed] [Google Scholar]
- 38.Sundberg, E. J., H. Li, A. S. Llera, J. K. McCormick, J. Tormo, P. M. Schlievert, K. Karjalainen, and R. A. Mariuzza. 2002. Structures of two streptococcal superantigens bound to TCRβ chains reveal diversity in the architecture of T cell signaling complexes. Structure 10:687-699. [DOI] [PubMed] [Google Scholar]
- 39.Thompson, J. D., D. G. Higgins, and T. J. Gibson. 1994. CLUSTAL W: improving the sensitivity of progressive multiple sequence alignment. Nucleic Acids Res. 22:4673-4680. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Walker, P. A., L. E. Leong, P. W. Ng, S. H. Tan, S. Waller, D. Murphy, and A. G. Porter. 1994. Efficient and rapid affinity purification of proteins using recombinant fusion proteases. Bio/Technology 12:601-605. [DOI] [PubMed] [Google Scholar]