Abstract
We recently reported that immature porcine Leydig cells express both somatostatin (SRIF) and SRIF receptor type-2 (sst-2) transcripts. The present study was therefore undertaken to assess whether SRIF might exert autocrine actions on these cells through sst2A receptor, one of the two sst2 isoforms known to exert important neuroendocrine and endocrine functions. Using a polyclonal antibody directed towards the C-terminal tail of the sst2A receptor subtype, receptor immunoreactivity was detected in a subpopulation of Leydig cells and spermatogonia. To address the physiological correlates of this expression we then studied the possible involvement of sst2 receptor in the regulation of testosterone secretion. Functional assays showed that the sst2 agonist octreotide inhibited both basal and hCG-stimulated testosterone secretion by testosterone pretreated Leydig cells. To assess whether sst2 receptor expression might be regulated by testosterone, we performed a semi-quantitative RT-PCR analysis of sst2 mRNA expression in Leydig cells cultured in the presence or in the absence of the androgen. A significant increase in sst2 receptor transcripts was observed in testosterone-treated cells. Taken together, these data suggest that SRIF can inhibit testosterone secretion through the sst2A receptor. The mechanism of the local inhibitory actions of SRIF is probably autocrine since immature porcine Leydig cells express SRIF itself and it might involve testosterone-induced increase of sst2 receptor expression in immature Leydig cells.
Background
Regulatory peptide somatostatin (SRIF) displays a broad tissue expression pattern. It modulates different cell functions such as endocrine and exocrine secretions and proliferation. These actions have been described in glands and in the gastrointestinal and immune systems. They are mediated via six receptors (sst1, sst2A, sst2B, sst3, sst4, sst5) encoded by five genes (sst1-5) located on distinct chromosomes. Few commonly available ligands (e.g. octreotide, MK 678 and RC 160) distinguish sst2/sst3/sst5- from sst1/sst4-receptors since they bind to sst2/sst3/sst5 subfamily with subnanomolar affinity and are 1000-fold less efficient on sst1/sst4 subfamily of receptors. Expression of different receptors is developmentally regulated in a time- and tissue-specific manner. It is also influenced by a variety of intra- and extra-cellular signals such as, for example, second messengers and steroid hormones (for, review, see [1]).
An accumulating body of evidence suggests that SRIF might play the role of a local regulatory factor in the testis. Indeed, SRIF has been identified in human [2], rat [3] and pig [4] testes. In particular, the analysis of SRIF-immunoreactivity at the cellular level has indicated its presence in spermatogonia and Leydig cells of immature pig testes [4]. Consistent with the hypothesis that the testis might be a potential SRIF target, sst receptor transcripts have been found in testes of different species. For example, the presence of sst3–sst5 transcripts has been reported in adult human testes [5,6]. In addition, SRIF receptor transcripts (sst1–sst3) have been visualized in adult rat testes where germ- and Sertoli cells contain all three transcripts while interstitial cells express only sst3 one [7]. In the immature pig testes, sst2 receptor mRNAs have been localized to Sertoli cells, spermatogonia and Leydig cells [4,8].
The role of the SRIF/SRIF receptor regulatory loop remains poorly understood in the mammalian testis. Recently published data point to the involvement of SRIF/sst2 receptor interaction in the control of proliferation of Sertoli cells [8] and spermatogonia [4]. Testosterone secretion by Leydig cells has been reported to be modulated in a complex manner after intra-testicular injection of SRIF in adult rats [9,10] thus strongly suggesting existence of functional SRIF receptors. However, the receptor subtypes involved in SRIF-mediated modulation of testosterone secretion have not been determined.
In this study, we searched for the presence of the sst2 receptor-protein in Leydig cells by a combined immunoblot / immunohistochemical approach and asked whether these receptors might be involved in the regulation of testosterone secretion. The functional relevance of sst2 receptors in immature porcine Leydig cells was analyzed by assessing their involvement in the control of basal and hCG-stimulated testosterone secretion. To approach a possible transcriptional regulation of sst2 receptor expression by testosterone, sst2 mRNAs were measured by semi-quantitative RT-PCR in the extracts obtained from cells cultured in the presence or in the absence of testosterone. On the whole, the results of these studies suggest that sst2 receptor might play a role in a "negative short loop feed-back" by which testosterone regulates its own secretion in Leydig cells.
Materials and Methods
Antibody preparation and Western blot analysis of sst2A immunoreactivity in the pig testis
The polyclonal R57 antibody was generated in New Zealand white rabbits against the peptide CERSDSKQDKSRLNETTETQRT after conjugation to keyhole limpet hemocyanin via the NH2-terminal cysteine using m-maleimidobenzoyl-N-hydroxysuccinimide. This sequence is located in the C-terminal region of the rat sst2A receptor and is conserved in the mouse, human [11] and pig [12] receptor isoforms.
Testes used in this study were obtained from 3-week-old pigs. At this perinatal age pigs are routinely castrated under local anesthesia on the farms. The castration is performed for the sake of body mass gain and meat taste improvement in the standard chain of production for human consumption.
Testicular fragments were homogeneized in ultrapure 9 M urea / 0.4% CHAPS (3-[3-chloramidopropyl]-dimethylammonio-1-propane-sulfonate)/ 5% mercaptoethanol (all from Sigma, L'Isle d'Abeau, France) at a concentration of 5 μg/5 μl, diluted 1:1 (vol / vol) in Laemmli-SDS sample buffer. The homogenates were electrophoresed on 10% SDS-polyacrylamide gels on a microscale [13]. After transfer onto nitrocellulose membranes (Schleicher & Schuell, PolyLabo, France), the membranes were blocked for 2 hours in 5% non-fat dry milk in phosphate buffered saline (PBS), incubated overnight with a polyclonal R57 primary antibody (1:2000 dilution) in non-fat dry 1% milk in PBS / 0.05% Tween 80. After repeated washings, the membranes were incubated with the alkaline phosphatase-coupled goat-anti-rabbit IgG in a 1:5000 dilution (Jackson, Intechim-Interbiotech, France) and developed in NBT / BCIP solution (5-bromo-4-chloro-o-indolyphosphate p-toluidin salt/ nitro blue tetrazolium).
Immunohistochemistry
Pig testes (n = 3) were fixed in 4% paraformaldehyde in PBS (pH 7.4) and embedded in paraffin. Sections (5 μm-thick) were mounted on positively charged glass slides and thereafter deparaffinized, hydrated and treated for 20 min at 95 C in citric buffer (pH 6). After washings (2 × 5 min) in PBS containing 0.1% Tween-20, the sections were preincubated 10 min at 37 C in peroxidase blocking reagent (Envision+ kit, Dako, Trappes, France), washed and incubated overnight at 4 C with R57 antibody in a 1:500 dilution. After two washings, the sections were incubated (30 min, 37 C) with goat-anti-rabbit IgG attached to a peroxidase-conjugated polymer backbone (Envision+ kit, Dako, Trappes, France). At the end of the incubation period, the non-bound secondary antibody was washed and sections were incubated 10 min at room temperature with 3-amino-9-ethylcarbazole to reveal a brown color at the site of peroxydase activity. After an extensive wash, the nuclei were counterstained with Mayer's hematoxylin.
Leydig cell preparation and culture
Leydig cells were prepared from immature porcine testes by collagenase (0.4 mg/ml, 90 min, 32 C) dispersion as previously described [14]. Collagenase was removed by centrifugation (200 × g for 10 min, 4 C). Resulting pellets were resuspended in the medium and allowed to sediment successively for 5 and 15 min. The crude interstitial cells were recovered from supernatants and Leydig cells were separated by Percoll gradient centrifugation. The content of Leydig cells in obtained preparations exceeded 90% as determined by histochemical 3β-hydroxy-steroid dehydrogenase staining (data not shown). Purified Leydig cells were plated in Petri dishes (60 × 15 mm, density of 5 × 106 cells/dish) for RNA extraction or in Falcon (Los Angeles, CA) 24-multiwell plates (0.5 × 106 cells/well) for testosterone assays. Cells were cultured at 32 C in a humidified atmosphere of 5% CO2, 95% air in DMEM/Ham's F-12 medium (1:1 vol/vol) containing sodium bicarbonate (1.2 mg/ml), 15 mM Hepes and gentamicin (20 μg/ml). The medium was further supplemented with insulin (2 μg/ml), transferrin (5 μg/ml) and α-tocopherol (10 μg/ml).
Testosterone pretreatment and secretion assays
Leydig cells were pretreated with testosterone over 48 h starting at day 4 after the beginning of the culture. The experimental conditions of testosterone pretreatment (150 ng/ml, 48 h) were chosen based on the previous studies from our laboratory targeting the androgen receptors of porcine Sertoli cells [15]. The assumption that a similar testosterone concentration may be used to target androgen receptors present on these two cell types was based on the previous findings demonstrating the presence of one single type of androgen receptor in the whole-testis preparations obtained from the immature pigs of the same perinatal age as those used in our study [16]. By consequence, androgen receptors expressed by any testicular cell type are obviously identical and can be efficiently targeted by the same testosterone concentration.
At the end of the pretreatment period, cells were washed and incubated in the fresh medium (1 h, 32 C) three times. Indeed, in the preliminary set of experiments we successively washed and then incubated cells (32 C, 1 h) to allow a dissociation of the residual testosterone possibly adsorbed on the cell surface. Testosterone concentration was monitored in the culture supernatants obtained at the end of the 1-hour incubation periods at 32 C. The number of washings was finally set at 3 since testosterone was undetectable in the supernatants of cultures obtained after 3 rounds of washings / incubations.
Secretion assays, in which the accumulation of secreted testosterone was measured in either basal or hCG-stimulated conditions, were performed at day 6 of culture. Indeed, immature porcine Leydig cells in primary culture retain their full steroidogenic capacity (i.e. they respond to hCG stimulation by high and stable testosterone secretion) between day 2 and 6 of culture [17]. A 3 h-period of stimulation by hCG (CR 127 13450 IU/mg obtained from Dr A.F. Parlow, NHPP, Torrance, CA) was chosen since, in this culture model, the accumulation of unconjugated steroids upon hCG addition is linear only during the first 4 h of treatment [18]. Testosterone levels were measured in the culture medium by using a previously reported specific RIA [19].
RT-PCR analysis of sst2 receptor expression
Cultured Leydig cells or testis fragments were washed with PBS solution and total RNAs were extracted with TRIzol reagent (Gibco BRL, Cergy Pontoise, France) according to the manufacturer's instructions.
For RT-PCR analysis, 3 μg of total RNA was reverse-transcribed in 10 μl of reaction mixture containing 200 μM dNTPs, 10 U/ml of Moloney Murine Leukemia Virus (MMLV) reverse transcriptase, 0.01 M dithiothreitol (DTT) and 5 μM random hexamer primers in 20 mM Tris-HCl buffer for 60 min at 37 C, followed by heating at 100 C for 5 min.
One-tenth (2 μl) of the first strand of cDNA synthesis reaction mixture was added to PCR buffer (100 mM Tris) containing 0.2 mM dNTP and 1.25 U Taq DNA polymerase in a total volume of 50 μl. GAPDH and sst2 primer sequences, concentrations and amplification conditions have been previously detailed elsewhere [8].
For semi-quantitative analysis of sst2 receptor expression, 2 μl of the RT reaction mixture from each sample were amplified with either sst2 [8] or β-actin [4] primers, [α33P]dATP (0.75 μCi), Taq polymerase (0.01 U/μl), dNTPs (100 μM), MgCl2 (1.5 mM) and buffer (50 mM Tris-HCl) according to the already reported conditions [4,8]. The PCR amplification was carried out using Trio-thermoblock (Biometra, Kontron Instruments, Champagne au Mont d'Or, France) for 5 min of initial denaturation at 94 C, followed by 20 cycles of amplification for β-actin (94 C for 30 s; 61 C for 60 s; 72 C for 60 s) or 25 cycles for sst2 (94 C for 30 s; 60 C for 60 s; 72 C for 60 s). Final elongation was achieved at 72 C for 5 min.
The number of PCR cycles was determined in preliminary experiments by performing from 20 to 35 and 15 to 30 amplification reactions for sst2 and β-actin, respectively. Amplification for sst2 and β-actin was linear up to 30 and 25 cycles, respectively (data not shown). In order to be sure that the amplification products to be analyzed were obtained during the linear phase of reaction, the number of PCR cycles was fixed to the last 5-cycle increment before saturation was reached (i.e. to 25 and 20 cycles for sst2 and β-actin, respectively). For negative controls, cDNA was replaced by water to confirm the absence of any reactive contamination.
PCR products were resolved by 8% polyacrylamide gel electrophoresis. Products of amplification were visualized by using Kodak X-Omat S films (Eastman Kodak, Rochester, NY). The intensities of the autoradiographic bands were measured by densitometric scanning using the Intelligent quantifier (Bioimage, Omni Media scanner XRS). The results correspond to the optical densities (OD) of autoradiograms relative to three different RT-PCRs performed with RNAs extracted from Leydig cells from three independent cultures. The ODs corresponding to sst2 and β-actin mRNA expression in each individual sample were expressed in arbitrary units as a ratio of sst2 over β-actin densitometric intensities.
Data analysis
If not otherwise specified, data are presented as the mean ± SEM of triplicate determinations performed in at least three independent experiments carried out with different cell preparations or cell cultures. Statistical significance of the differences observed between experimental groups was determined by one-way ANOVA using InStat (Graph PAD Software) computer program. Post-hoc comparisons between treatment group means were made with the Bonferroni test for multiple comparisons. In sst2 receptor expression assays, the significance of the difference between the control- and testosterone treated groups was assessed by two-tailed t-test. Differences are considered as significant if p < 0.05.
Results
sst2A receptor expression in testicular homogenates and extracts from cultured Leydig cells
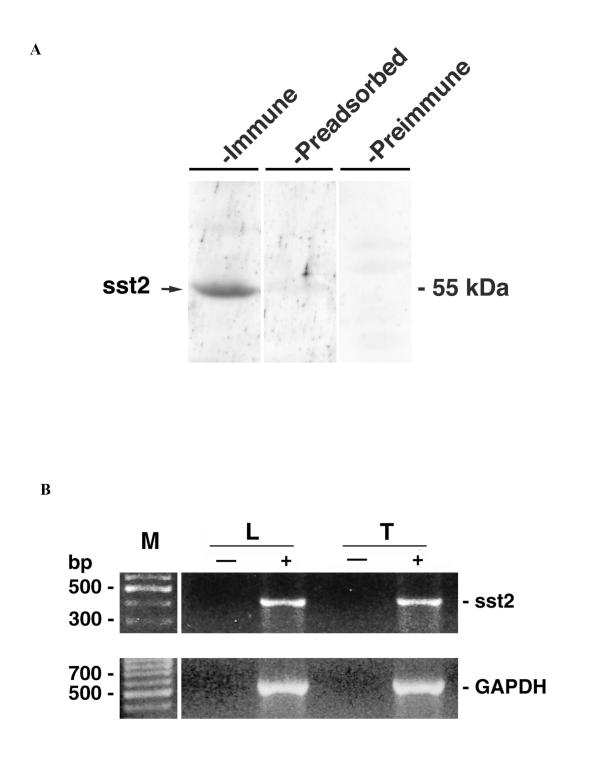
Western blot analysis was performed with R57 antibody on the whole soluble protein extracts obtained from testes of 3-week-old pigs. An R57-immunoreactive protein with an approximate molecular weight of 55 kDa (Fig. 1A, first lane) was identified. The staining of the immunoreactive protein was blocked by 1 μM antigenic peptide (Fig. 1A, second lane). No immunoreactive protein was detected with preimmune serum (Fig. 1A, third lane).
Figure 1.
The whole testicular extracts of immature porcine testes contain both sst2A receptor protein (A) and transcript (B). (A) Western blot analysis of sst2A receptor immunoreactivity in soluble protein extracts (100 μg) separated by 10 % SDS-PAGE. After the electrotransfer of proteins, the corresponding nitrocellulose membrane was divided into three parts. Two parts were immunoblotted with either R57 antibody alone (first lane: "immune") or in the presence of the antigenic peptide (second lane: "preadsorbed"). The third part was incubated in parallel with the preimmune serum (third lane: "preimmune"). Molecular mass (in kDa) is indicated by the arrow. (B) Amplification products obtained in PCR reaction with sst2-specific primers. Templates used in the reaction are: cDNA corresponding to the whole testicular tissue (lane "T+") and cultured Leydig cells (lane "L+") obtained in the RT reactions as described in Materials and Methods; mRNAs obtained from the whole testicular tissue (lane "T-") and cultured Leydig cells (lane "L-") and processed according to the same RT protocol as the former samples but without the addition of MMLV. The size (in bp) of DNA fragments is given by the lane "M". The lower panel shows the amplification of internal standard GAPDH-fragments in the corresponding samples.
Parallel RT-PCR analysis with sst2-specific primers showed that a fragment of an expected size (i.e. 415 bp) could be amplified when cDNAs obtained from total RNA extracts (prepared from the same testes as those used for protein extraction) were used as a template (Fig. 1B, lane "T+"). A product of an identical size was amplified from cDNAs corresponding to RNA extracts obtained from cultured Leydig cells (Fig. 1B, lane "L+"). The identities of the amplified fragments were checked by automated DNA sequencing using ABI Prism 310 Genetic Analyzer (Applied Biosystems, Courtaboeuf, France) (data not shown). The absence of any contamination was confirmed by the fact that no amplification products were obtained when cDNA template was replaced by water (data not shown). Similarly, no amplification occured in PCRs when they were performed after RT reactions in which RNAs has been processed without addition of MMLV (Fig. 1B, lanes "L-" and "T-").
sst2A receptor expression in Leydig cells in situ
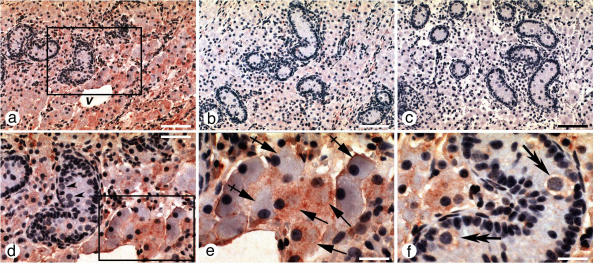
Expression of sst2 receptor protein was studied by immunohistochemistry on tissue sections from immature pigs. Positive immunostaining with R57 antibody was observed in both intratubular and interstitial compartments (Fig. 2a,2d,2e,2f). Detailed cytological analysis allowed us to attribute this immunoreactivity to spermatogonia and Leydig cells. However, both cell types immunostained heterogeneously, i.e. they showed varying (from low to strong) intensity of labeling (Fig. 2a,2d,2e,2f). The observed immunostaining was specific because it was abolished in the presence of 1 μM of exogenously added antigenic peptide (Fig. 2b). Testicular sections processed without incubation with R57 antibody displayed no immunoreactivity thus excluding any artifactual labeling (Fig. 2c).
Figure 2.
sst2A-like immunoreactivity on formalin-fixed, paraffin-embedded testis sections. Tissue sections were incubated with R57 anti-sst2A antibody (1:500 dilution) alone (a) or in the presence of exogenously added antigenic peptide (b). Negative control consisted in staining procedure in which anti-sst2A antibody was omitted (c). Magnified frame from the middle of (a) is shown in (d) with arrow-heads pointing to immuno-negative spermatogonia. Magnified field from the bottom right in (d) is shown in (e) with simple arrows pointing to the immuno-labeled Leydig cells; dashed arrows point to immuno-negative Leydig cells. (f) another section plane with double arrows pointing to immuno-labeled spermatogonia in the interior of seminiferous tubule. Note the staining heterogeneity of both Leydig cells and spermatogonia (d-f). Scale bars: A-C = 100 μM; D = 50 μM; E-F = 25 μM.
Functional involvement of sst2 receptor in the regulation of testosterone secretion
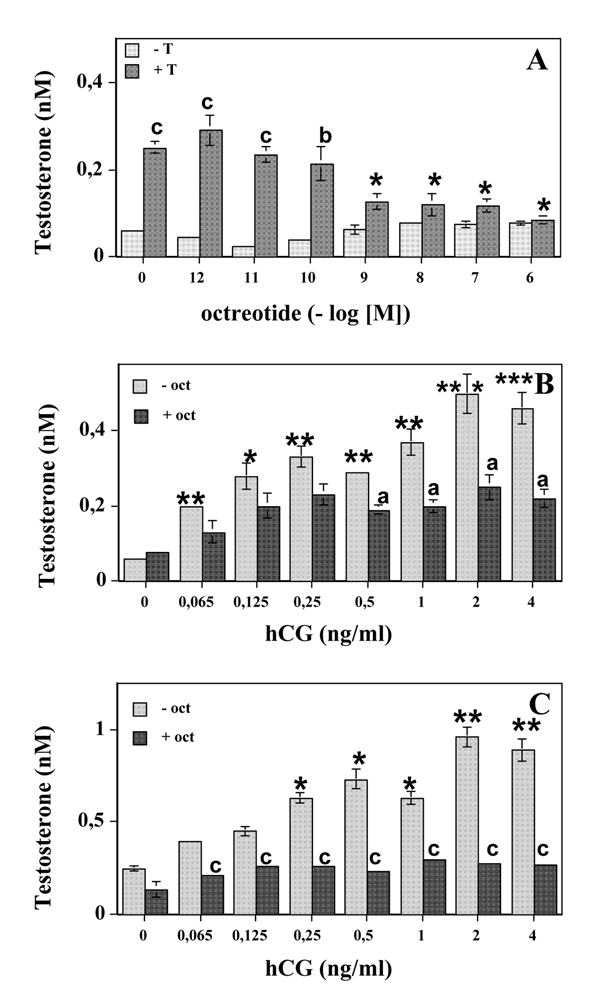
To approach the functional relevance of sst2 receptors of Leydig cells, we first assessed their possible involvement in the regulation of basal testosterone secretion. Addition of a relatively selective sst2 agonist octreotide (Novartis, Basel, Switzerland) had no significant effect on testosterone secretion (Fig. 3A).
Figure 3.
Functional involvement of sst2A receptor in the regulation of basal (A) and hCG-stimulated (B, C) testosterone secretion by immature porcine Leydig cells pretreated (A, C) or not (A, B) with testosterone. (A) Leydig cells were pretreated (48 h) in the absence of 150 ng/ml testosterone ("-T") or in its presence ("+T"). After 3 rounds of successive washings / incubations (1 h, 32 C), cells were incubated for the additional 3 h in the absence or in the presence of octreotide in the concentration range from 1 pM to 1 μM. At the end of the incubation period cell supernatans were collected for RIA determination of the secreted testosterone. *: p < 0.05 for testosterone secretion measured in the presence of the octreotide compared to that measured in its absence in testosterone pretreated group. b: p < 0.01; c: p < 0.001 for comparisons between testosterone-pretreated and testosterone-untreated cells at a given octreotide concentration. (B) Leydig cells were incubated (3 h) in the presence of the increasing concentrations of hCG (0.065–4 ng/ml range) and either in the absence ("-oct") or in the presence ("+oct") of 1 μM octreotide. Testosterone secretion was measured by RIA in the relevant supernatants. *: p < 0.05; **: p < 0.01 for hCG-stimulated testosterone secretion versus that measured in its absence. a: p < 0.05 for comparisons between octreotide-treated and untreated cells at a given octreotide concentration. (C) Leydig cells were pretreated with testosterone (150 ng / ml, 48 h), then washed as in (A) and incubated for additional 3 h in the presence of the increasing concentrations of hCG (0.065–4 ng/ml range) and either in the absence ("-oct") or in the presence ("+oct") of 1 μM octreotide. Testosterone secretion was measured by RIA in the relevant supernatants. *: p < 0.05; **: p < 0.01 for hCG-stimulated testosterone secretion versus that measured in its absence. c: p < 0.001 for comparisons between octreotide-treated and untreated cells at a given hCG concentration.
We next sought to determine whether the testosterone pretreatment (150 ng/ml, 48 h) could modify the octreotide actions on testosterone secretion by immature porcine Leydig cells. Interestingly, testosterone pretreatment by itself (i.e. in the absence of octreotide) greatly (4- to 5-fold) increased the capacity of immature Leydig cells to secrete testosterone (Fig. 3A: p < 0.001 for "-T" versus "+T" at octreotide concentration "0"). The observed increase in testosterone secretion by pretreated cells cannot be attributed to the assay contamination by exogenous testosterone added in order to perform culture pretreatment (see Testosterone pretreatment and secretion assays in Materials and Methods). However, a pretreatment of Leydig cells with testosterone revealed a capacity of octreotide to inhibit testosterone secretion in a dose-dependent manner (F = 17.73, p < 0.001 according to the global one-way ANOVA as compared to the testosterone pretreated cells incubated in the absence of octreotide). The maximal inhibitory effect was achieved at octreotide concentration range from 1 nM to 1 μM (Fig. 3A). In addition, a significant difference in testosterone secretion was seen between testosterone-treated and untreated Leydig cells for the cultures carried out in the presence of the low (p < 0.001 for 1–10 pM and p < 0.05 for 100 pM) octreotide concentrations (Fig. 3A).
Further experiments were designed to assess the capacity of SRIF agonist to inhibit hCG-stimulated testosterone secretion. To do that, Leydig cell cultures were simultaneously incubated with octreotide, added at the concentration eliciting a maximal inhibitory effect in basal conditions (1 μM), and increasing concentrations of hCG (0.065–4 ng/ml). The results obtained in these experiments showed that in the presence of octreotide, hCG could still elicit a slight increase in testosterone secretion although, for all hCG concentrations tested, this increase was not significantly different from the controls incubated without hCG addition (Fig. 3B). By contrast, in the absence of octreotide, hCG triggered a significant increase of testosterone secretion even at the lowest (0.065 ng/ml) concentration tested (Fig. 3B). Besides, the analysis of the inhibitory actions of octreotide on hCG-mediated induction of testosterone secretion point to a statistically significant difference between octreotide treated and untreated cells at hCG concentrations greater than 0.5 ng/ml (Fig. 3B).
The effects of testosterone pretreatment (150 ng/ml, 48 h) on octreotide-mediated inhibition of testosterone secretion were also studied in hCG-stimulated conditions. Similarly as in cell cultures pretreated with testosterone and assayed in basal conditions, testosterone pretreatment per se increased its own secretion by hCG-stimulated Leydig cells. Moreover, such an increase was additive to hCG stimulation (Table 1). Thus, hCG-stimulated testosterone secretion in testosterone-pretreated cells was about twice that measured in untreated cells at all (0.065–4 ng/ml) hCG concentrations tested (Table 1). In these experimental conditions, octreotide added at 1 μM concentration, was able to significantly (p < 0.001 at all hCG concentrations tested for comparisons between "-oct" and "+oct") inhibit the hCG-triggered increase of testosterone secretion by testosterone-pretreated Leydig cells (Fig. 3C). Moreover, after testosterone pretreatment, the octreotide could completely prevent hCG-induced increase in testosterone secretion at all hCG concentrations tested (Fig. 3C).
Table 1.
Stimulation of testosterone secretion by hCG in control and testosterone-pretreated Leydig cellsa.
| Secreted tesosterone (nM) | ||
| hCG (ng/ml) | control | pretreated |
| 0 | 0.060 ± 0.0001b | 0.250 ± 0.013* |
| 0.065 | 0.200 ± 0.003d | 0.400 ± 0.004* |
| 0.125 | 0.280 ± 0.034c | 0.450 ± 0.024* |
| 0.250 | 0.330 ± 0.028d | 0.630 ± 0.026c,* |
| 0.500 | 0.290 ± 0.030d | 0.730 ± 0.052c,* |
| 1 | 0.370 ± 0.035d | 0.630 ± 0.034c,* |
| 2 | 0.500 ± 0.052e | 0.960 ± 0.052d,* |
| 4 | 0.460 ± 0.043e | 0.890 ± 0.061d,* |
a pretreatment conditions are given in "Materials and Methods". bdata are expressed as mean ± SEM. c,d,etestosterone secretion significantly (c:p < 0.05; d:p < 0.01; e:p < 0.001) higher in the presence of hCG than in its absence in either control- or testosterone-pretreated cells *testosterone secretion significantly (p < 0.01) higher for the same hCG concentration in testosterone-pretreated than control cells.
Modulation of sst2 receptor expression by testosterone
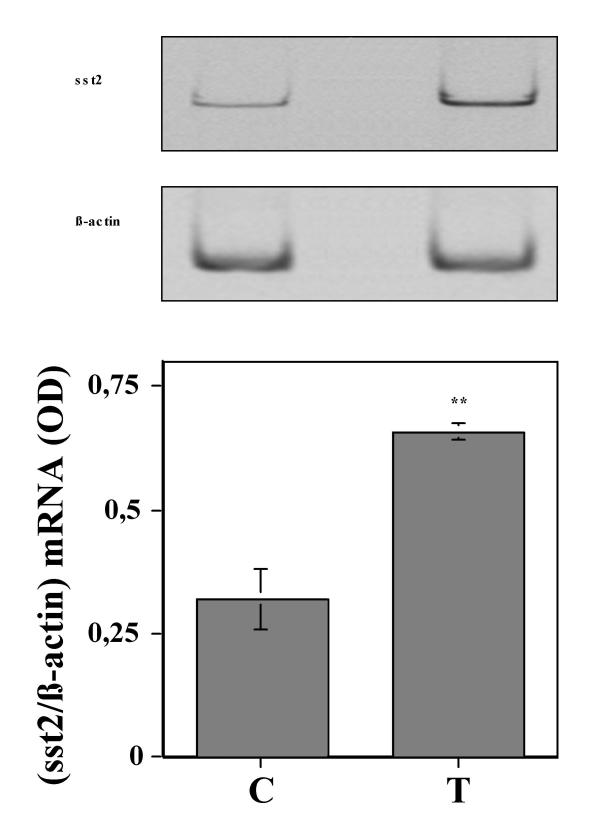
In order to address the mechanism of the observed inhibitory actions of octreotide that were revealed by testosterone pretreatment, we analyzed the expression of sst2 receptor transcripts in control and testosterone-pretreated Leydig cells. Testosterone treatment of these cells in the identical conditions as those used in functional assays (i.e. 150 ng/ml over 48 h) showed that the quantity of sst2 transcripts double in pretreated cells (Fig. 4).
Figure 4.
Testosterone pretreatment (150 ng/ml, 48 h) triggers an increase in sst2A receptor mRNA expression. At the upper panel are shown the representative autoradiograms from one experiment. At the lower panel are depicted the histograms representing the mean ± SEM of optical densities (ODs) measured on corresponding autoradiograms for each determination performed in three independent experiments (see "Materials and Methods"). C = control; T = testosterone-pretreated (150 ng/ml; 48 h); **: p < 0.01 versus "C".
Discussion
The data presented in this study show that SRIF inhibits both basal- and hGC-stimulated testosterone secretions by immature porcine Leydig cells. However, testosterone pretreatment was necessary to reveal this inhibition in basal conditions whereas in hCG-stimulated conditions, the inhibitory effects of SRIF on testosterone secretion were detectable in the absence of testosterone pretreatment but were more pronounced in testosterone pretreated Leydig cells. Induction of sst2 receptor expression by testosterone might be one of the underlying molecular mechanisms responsible for the inhibition of testosterone secretion by SRIF. These findings, combined with the results we have previously reported on SRIF-mediated inhibition of spermatogonia- and Sertoli cell-proliferation [4,8], bring new arguments for the inhibitory role of SRIF in the control of testicular cell functions. Moreover, this work provides further insights on the importance of SRIF in testicular cell-cell interactions and on its mode of actions. Thus, given the previously documented SRIF-immunoreactivity of immature porcine Leydig cells [4], the presence of the functional sst2 receptors on Leydig cells shown here point to the autocrine actions of SRIF on Leydig cells. These intra-testicular actions are additional to the already suggested paracrine actions of SRIF on Sertoli cells and its autocrine actions on spermatogonia [4].
The culture conditions used here were validated by the observed low basal testosterone secretion [20] and induction of testosterone secretion by hCG in the same range of magnitude as that reported previously for the similar culture conditions [17,21]. The maximal inhibition of testosterone secretion by octreotide is achieved at nanomolar concentration, in agreement with subnanomolar affinity of octreotide on sst2 receptor subtype [1]. Western blot assays allowed us to identify an sst2A-immunoreactive protein with an apparent mass of approximately 55 kDa, in agreement with the range of 60 to 110 kDa reported for the molecular mass of previously identified sst2 receptors, depending on the cell and tissue types studied [22-27]. Similarly, the size of the fragments obtained in our RT-PCR from Leydig cell RNA extracts with the same sst2A-specific primers is identical to those previously reported in different cell types of immature porcine testes [4,8] and in human tissues [28].
Our data show that SRIF inhibits both basal and stimulated testosterone secretion by Leydig cells. However, such inhibition can be evidenced only when the level of testosterone secretion was elevated either by testosterone pretreatment alone or in combination with hCG stimulation. Besides, the mechanism of the testosterone-induced testosterone secretion in immature pig testes was beyond the scope of our study and remains unknown. However, it seems clear that testosterone has different actions on Leydig cells depending on the developmental stage: it increases its own secretion in immature Leydig cells [[29,30], present study] whereas in adult cells it has rather inhibitory actions via a "short-loop negative feed-back" mechanism [31].
The fact that SRIF-mediated inhibition of testosterone secretion could be revealed only in the context of the elevated testosterone secretion is probably related to the low level of testosterone secretion by immature Leydig cells in the absence of hCG [20] or testosterone pretreatment. Such a low basal rate of testosterone secretion might explain why the inhibitory actions of SRIF, expected to further lower the already low basal secretion, were not detectable. Indeed, during the initial phase of this work we took advantage of the immature porcine Leydig cells model since, based on the in vivo data [9,10], SRIF actions on testosterone secretion were expected to be rather stimulatory. Consequently, the possible SRIF-mediated alterations of testosterone secretion would be more accurately measured in the presence of the low basal level of testosterone secretion. The obtained results are, however, in contrast with that hypothesis. The differences between SRIF actions observed between previous [9,10] and present studies might be related to different species (rat versus pig) since in all three studies immature animals were used. Nevertheless, the inhibitory actions of SRIF on the testosterone secretion observed in the present study are in agreement with the data relative to SRIF-induced inhibition of the majority of hormonal secretion studied so far (for review, see [1]).
Our findings on testosterone-mediated sst2 receptor mRNA induction represent a contribution to the understanding of the molecular mechanisms by which SRIF receptor expression is regulated. Indeed, transcriptional regulation of SRIF receptors by various hormones has been previously documented. For example, thyroid hormone triggers a specific induction of mRNA for sst1 and sst5 in murine thyrotropic tumors [32]. Steroid hormones also modulate SRIF receptor expression. For example, estradiol up-regulates mRNA for sst2 receptor in human breast cancer cells [33] and in rat pituitary cells [34]. In addition, in the latter cells estradiol increases sst3 mRNA expression and inhibits sst1, sst4 and sst5 expression [34]. Both positive and negative regulations of sst1 and sst2 receptors by glucocorticoids have been reported [35]. All these hormones (including testosterone) have in common the transduction via nuclear receptors that directly influence the expression of the target genes. Consistently, relevant response elements for some of these hormones have been identified in promoters of sst receptor genes (for review, see [1]). Further experiments are now needed in order to assess the presence of the consensus androgen-binding element (ARE) in the promoter of sst2 receptor gene. Interestingly, testosterone-induced up-regulation of sst1 receptor mRNAs has been reported in the rat anterior pituitary [36].
There is general agreement that many local factors such as cytokines and growth factors are implicated in negative regulation of testosterone secretion (for review, see [37]). However, the molecular mechanisms by which high testosterone levels are linked to the induction of these factors are not completely characterized. The findings presented here extend the list of local factors capable of inhibiting testosterone secretion. They also offer a possible molecular basis for the local, SRIF-mediated relay of high testosterone levels by which this androgen might inhibit its own secretion through a "short loop negative feed-back" inhibition of testosterone secretion [31]. Previously reported testosterone capacity to increase SRIF expression (for review, see [1]) is consistent with the latter hypothesis and the model of immature porcine Leydig cells in culture allows now to test it directly. Demonstration of such an intra-testicular regulation would be reminiscent of the reported intra-hypothalamic "short loop negative feed-back" inhibition of GH secretion through GH-induced increase of sst1 receptor mRNA [38].
Acknowledgments
Acknowledgments
We are indebted to Drs Stolz (Novartis, Basel, Switzerland) and Parlow (NHPP, Torrance, CA) for the generous gift of octreotide and hCG, respectively.
We should like to thank Dr A. Gougeon and Dr S. Bauer for their precious help on immunohistochemistry, Christelle El Ghamrawy for help during the setting-up of semi-quantitative RT-PCR assays, Mrs G. Thoiron for the English translation and the farmer, Mr. P. Bouteille, for providing us with porcine testes at castration.
Contributor Information
Joanna Fombonne, Email: fombonne.j@jean-roche.univ-mrs.fr.
Zsolt Csaba, Email: csaba@broca.inserm.fr.
Ysander von Boxberg, Email: boxberg@iaf.cnrs-gif.fr.
Amandine Valayer, Email: amandine.valayer@wanadoo.fr.
Catherine Rey, Email: rey@lsgrisn.univ-lyon1.fr.
Mohamed Benahmed, Email: benahmed@lsgrisn.univ-lyon1.fr.
Pascal Dournaud, Email: dournaud@broca.inserm.fr.
Slavica Krantic, Email: krantic.s@jean-roche.univ-mrs.fr.
References
- Patel YC. Somatostatin and its receptor family. Frontiers in Neuroendocrinology. 1999;20:157–198. doi: 10.1006/frne.1999.0183. [DOI] [PubMed] [Google Scholar]
- Sasaki A, Yoshinaga K. Immunoreactive somatostatin in male reproductive system in humans. J Clin Endocrinol Metab. 1989;68:996–999. doi: 10.1210/jcem-68-5-996. [DOI] [PubMed] [Google Scholar]
- Pekary AE, Yamada T, Sharp B, Bhasin S, Swerdlof RS, Hershman JM. Somatostatin-14 and -28 in the rat male reproductive system. Life Sci. 1984;34:939–945. doi: 10.1016/0024-3205(84)90298-4. [DOI] [PubMed] [Google Scholar]
- Goddard I, Bauer S, Gougeon A, Lopez F, Giannetti N, Susini C, Benahmed M, Krantic S. Somatostatin inhibits Stem Cell Factor Messenger RNA expression by Sertoli cells and Stem Cell Factor-Induced DNA synthesis in isolated seminiferous tubules. Biol Reprod. 2001;65:1732–1742. doi: 10.1095/biolreprod65.6.1732. [DOI] [PubMed] [Google Scholar]
- Baou N, Bouras M, Droz JP, Benahmed M, Krantic S. Evidence for a selective loss of somatostatin receptor subtype expression in male germ cell tumors of seminoma type. Carcinogenesis. 2000;21:805–810. doi: 10.1093/carcin/21.4.805. [DOI] [PubMed] [Google Scholar]
- Baou N, Bouras M, Droz JP, Dutrieux-Berger N, Bouvier R, Benahmed M, Krantic S. Somatostatin receptor expression profile as a potential criterion for discrimination between seminoma and non-seminoma testiculatr tumors. Cancer Detection and Prevention. 2001;25:446–453. [PubMed] [Google Scholar]
- Zhu LJ, Krempels K, Bardin CW, O'Carroll AM, Mezey E. The localization of messenger ribonucleic acids for somatostatin receptors 1, 2, and 3 in rat testis. Endocrinology. 1998;139:350–357. doi: 10.1210/endo.139.1.5661. [DOI] [PubMed] [Google Scholar]
- Krantic S, Benahmed M. Somatostatin inhibits FSH-induced adenylyl cyclase activity and proliferation in immature porcine Sertoli cell via sst2 receptor. Biol Reprod. 2000;62:1835–1843. doi: 10.1095/biolreprod62.6.1835. [DOI] [PubMed] [Google Scholar]
- Gerendai I, Csaba Z, Csernus V. Effect of intratesticular administration of somatostatin on testicular function in immature and adult rats. Life Sciences. 1996;59:859–866. doi: 10.1016/0024-3205(96)00376-1. [DOI] [PubMed] [Google Scholar]
- Gerendai I. Fine-tuning control of testicular function. Neurobiology. 1997;5:347–359. [PubMed] [Google Scholar]
- Kluxen F, Bruns C, Lubbert H. Expression cloning of a rat brain somatostatin receptor cDNA. Proc Natl Acad Sci. 1992;89:4618–4622. doi: 10.1073/pnas.89.10.4618. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Matsumoto K, Yokogoshi Y, Fujinaka Y, Zhang C, Saito S. Molecular cloning and sequencing of porcine somatostatin receptor 2. Biochem Biophys Res Commun. 1994;199:298–305. doi: 10.1006/bbrc.1994.1228. [DOI] [PubMed] [Google Scholar]
- van Boxberg Y. Protein analysis on two-dimensional polyacrylamide gels in the femtogram range: use of a new sulfur-labeling reagent. Anal Biochem. 1988;169:372–375. doi: 10.1016/0003-2697(88)90298-9. [DOI] [PubMed] [Google Scholar]
- Benahmed M, Chauvin MA, Morera AM, DePeretti E. Somatomedin C/insulin-like growth factor 1 is a possible intratesticular regulator of Leydig cell activity. Mol Cell Endocrinol. 1987;50:69–77. doi: 10.1016/0303-7207(87)90078-5. [DOI] [PubMed] [Google Scholar]
- Benbrahim-Tallaa L, Tabone E, Tosser-Klopp G, Hatey F, Benahmed M. Glutathione S-transferase alpha expressed in porcine Sertoli cells is under the control of follicle-stimulating hormone and testosterone. Biol Reprod. 2002;66:1734–1742. doi: 10.1095/biolreprod66.6.1734. [DOI] [PubMed] [Google Scholar]
- Tripepi S, Carelli A, Perrotta E, Brunelli E, Tavolaro R, Facciolo RM, Canonaco M. Morphological and functional variations of Leydig cells in testis of the domestic pig during the different biological stages of development. J Exp Zool. 2000;287:167–175. doi: 10.1002/1097-010X(20000701)287:2<167::AID-JEZ7>3.0.CO;2-3. [DOI] [PubMed] [Google Scholar]
- Mauduit C, Goddard I, Besset V, Tabone E, Rey C, Gasnier F, Dacheux F, Benahmed M. Leukemia inhibitory factor antagonizes gonadotropin induced testosterone synthesis in cultured porcine Leydig cells: sites of actions. Endocrinology. 2001;142:2509–2520. doi: 10.1210/endo.142.6.8177. [DOI] [PubMed] [Google Scholar]
- Orava M, Haour F, Leinonen P, Ruokonen A, Vihko R. Relationships between unconjugated and sulphated steroids in porcine primary Leydig cell culture. J Steroid Biochem. 1985;22:507–512. doi: 10.1016/0022-4731(85)90170-0. [DOI] [PubMed] [Google Scholar]
- Forest M, Cathiard A, Bertrand J. Total and unbound testosterone levels in the newborns and normal hypogonadal children: use of sensitive radio-immunoassay for testosterone. J Clin Endocrinol Metab. 1973;36:1132–1142. doi: 10.1210/jcem-36-6-1132. [DOI] [PubMed] [Google Scholar]
- Bernier M, Gibb W, Haour F, Collu R, Saez J, Ducharme J. Studies with purified immature porcine Leydig cells in culture. Biol Reprod. 1178;29:1172–1983. doi: 10.1095/biolreprod29.5.1172. [DOI] [PubMed] [Google Scholar]
- Mauduit C, Gasnier F, Rey C, Chauvin MA, Stocco DM, Louisot P, Benahmed M. Tumor necrosis factor-α inhibits Leydig cell steroidogenesis through a decrease in steroidogenic acute regulatory protein expression. Endocrinology. 1998;139:2863–2868. doi: 10.1210/endo.139.6.6077. [DOI] [PubMed] [Google Scholar]
- Helboe L, Moller M, Norregaard L, Schiodt M, Stidsen C. Development of selective antibodies against the human somatostatin receptor subtypes sst1–sst5. Brain Res Mol Brain Res. 1997;49:82–8. doi: 10.1016/S0169-328X(97)00127-7. [DOI] [PubMed] [Google Scholar]
- Hunyady B, Hipkin RW, Shonbrunn A, Mezey E. Immunohistochemical localization of somatostatin receptor sst2A in the rat pancreas. Endocrinology. 1997;138:2632–2635. [PubMed] [Google Scholar]
- Mezey E, Hunyady B, Mitra S, Hayes E, Liu Q, Schaeffer J, Schonbrunn A. Cell specific expression of the sst2A and sst5 somatostatin receptors in the rat anterior pituitary. Endocrinology. 1998;139:414–419. doi: 10.1210/endo.139.1.5807. [DOI] [PubMed] [Google Scholar]
- Lopez F, Esteve JP, Buscail L, Delesque N, Saint-Laurent N, Theveniau M, Nahmias C, Vaysse N, Susini C. The tyrosine phosphatase SHP-1 associates with the sst2 somatostatin receptor and is an essential component of sst2-mediated inhibitory growth signaling. J Biol Chem. 1997;272:24448–24454. doi: 10.1074/jbc.272.39.24448. [DOI] [PubMed] [Google Scholar]
- Hofland LJ, Liu Q, Van Koetsveld PM, Zuijderwijk J, Van Der Ham F, Krijger RR, Schonbrunn A, Lamberts SWJ. Immunohistochemical detection of somatostatin receptor subtypes sst1 and sst2A in human somatostatin receptor positive tumors. J Clin Endocrinol Metab. 1999;84:775–780. doi: 10.1210/jcem.84.2.5497. [DOI] [PubMed] [Google Scholar]
- Reubi JC, Laissue JA, Waser B, Steffen DL, Hipkin RW, Schonbrunn A. Immunohistochemical detection of somatostatin sst2A receptors in the lymphatic, smooth muscular and peripheral nervous systems of the human gastrointestinal tract: facts and artifacts. J Clin Endocrinol Metab. 1999;84:2942–2950. doi: 10.1210/jcem.84.8.5878. [DOI] [PubMed] [Google Scholar]
- Kubota A, Yamada Y, Kagimoto S, Shimatsu A, Imamura M, Tsuda K, Imura H, Seino S, Seino Y. Identification of somatostatin receptor subtypes and an implication for the efficacity of somatostatin analogue SMS 201-995 in treatment of human endocrine tumors. J Clin Invest. 1994;93:1321–1325. doi: 10.1172/JCI117090. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hardy MP, Kelce WR, Klinefelter GR, Ewing LL. Differenciation of Leydig cell precursor in vitro: a role for androgen. Endocrinology. 1990;127:488–490. doi: 10.1210/endo-127-1-488. [DOI] [PubMed] [Google Scholar]
- Purvis K, Calandra R, Naess O, Attramadal A, Torjesen PA, Hansson V. Do androgens increase Leydig cell sensitivity to luteinizing hormone? Nature. pp. 169–170. [DOI] [PubMed]
- Darney KJ, Ewing L. Autoregulation of testosterone secretion in perfused rat testes. Endocrinology. 1981;109:993–995. doi: 10.1210/endo-109-3-993. [DOI] [PubMed] [Google Scholar]
- James R, Sarapura V, Bruns C, Raulf F, Dowding J, Gordon D, Wood W, Ridgway E. Thyroid hormone-induced expression of specific somatostatin receptor subtypes correlates with involution of the TtT-97 murine thyrotrope tumor. Endocrinology. 1997;138:719–724. doi: 10.1210/endo.138.2.4951. [DOI] [PubMed] [Google Scholar]
- Xu Y, Song J, Berelowitz M, Bruno J. Estrogen regulates somatostatin receptor subtype 2 messengeer ribonucleic acid expression in human breast cancer cells. Endocrinology. 1996;137:5634–5640. doi: 10.1210/endo.137.12.8940394. [DOI] [PubMed] [Google Scholar]
- Djordjijevic D, Zhang J, Priam M, Viollet C, Gourdji D, Kordon C, Epelbaum J. Effects of 17-beta estradiol on somatostatin receptor expression and inhibitory effects on growth hormone and prolactin release in rat pituitary cell cultures. Endocrinology. 1998;139:2272–2277. doi: 10.1210/endo.139.5.5990. [DOI] [PubMed] [Google Scholar]
- Xu Y, Berelowitz M, Bruno J. Dexamethasone regulates somatostatin receptor subtype messenger ribonucleic acid expression in rat pituitary GH4C1 cells. Endocrinology. 1995;136:5070–5075. doi: 10.1210/endo.136.11.7588243. [DOI] [PubMed] [Google Scholar]
- Senaris R, Lago F, Dieguez C. Gonadal regulation of somatostatin receptor 1, 2 and 3 mRNA levels in thee rat anterior pituitary. Mol Brain Res. 1996;38:171–175. doi: 10.1016/0169-328X(96)00042-3. [DOI] [PubMed] [Google Scholar]
- Benahmed M. Growth factors and cytokines in the testis. In: Comhaire FH, editor. Male infertility. London, Chapman & Hall Medical; 1996. pp. 55–95. [Google Scholar]
- Guo F, Beaudet A, Shaffer-Tannenbaum G. The effect of hypophysectomy and growth hormone replacement on sst1 and sst2 somatostatin receptor subtype messenger ribonucleic acids in the arcuate nucleus. Endocrinology. 1996;137:3928–3935. doi: 10.1210/endo.137.9.8756568. [DOI] [PubMed] [Google Scholar]