Abstract
Objective
To compare the effectiveness of lipid lowering drugs in lowering serum cholesterol concentrations.
Design
Cross sectional study.
Setting
17 practices within 17 primary care groups in Trent region, United Kingdom.
Participants
Patients aged 35 years or over taking lipid lowering drugs and with at least two serum cholesterol concentrations recorded on computer.
Main outcome measures
Proportion of patients achieving serum cholesterol concentration of ⩽5 mmol/l and mean percentage reduction in serum cholesterol concentration.
Results
1353 of 2469 (54.8%) patients receiving lipid lowering treatment had a last recorded serum cholesterol concentration of ⩽5 mmol/l. Significantly more patients taking statins achieved the target value for serum cholesterol (5 mmol/l) than those taking fibrates (1307 (57%) v 46 (26%); P<0.0001). Atorvastatin and simvastatin were the most effective drugs in achieving the target. Significant differences were found between lipid lowering drugs for the pretreatment serum cholesterol concentration, the most recent cholesterol concentration, and the associated percentage reduction. Atorvastatin and simvastatin achieved the greatest percentage reduction in serum cholesterol concentrations (30.1%, 95% confidence interval 28.8% to 31.4%, and 28.0%, 26.7% to 29.3%, respectively). Although the mean serum cholesterol concentrations in this unselected population tended to be higher than those in clinical trials, the percentage reduction was consistent with the trials.
Conclusion
The ability of individual statins to lower serum cholesterol concentration varied, with atorvastatin and simvastatin being the most effective. The percentage reductions agreed with those of randomised controlled trials indicating likely benefits in unselected patients in primary care. As the initial serum cholesterol concentrations were higher than those in randomised controlled trials, target serum cholesterol values of ⩽5 mmol/l may be unrealistic even for patients taking the most efficacious drugs. Also, the higher initial levels could mean that the absolute reduction in cardiovascular risk in primary care patients is greater than thought.
What is already known on this topic
Statins in patients with coronary heart disease help reduce further cardiovascular events and improve survival
This seems to be a class effect of statins, although there may be important differences in effectiveness between them
Less than half of patients in the community who take lipid lowering drugs achieve target serum cholesterol values
What this study adds
Statins vary in their ability to lower serum cholesterol concentration, with atorvastatin and simvastatin achieving the best results
The percentage reductions agreed with those found in randomised controlled trials
Since the initial serum cholesterol concentrations were higher than in trials, absolute risk reductions in primary care patients may be greater than thought
Target values of ⩽5 mmol/l may be unrealistic even for patients on the most efficacious drugs, because the initial mean cholesterol values of primary care patients are higher than those of patients in trials
Introduction
Statins in patients with coronary heart disease help reduce further cardiovascular events and improve survival.1–4 The identification and treatment of hyperlipidaemia in patients with coronary heart disease is now a national priority, as reflected in the national service framework for coronary heart disease and national guidelines.5,6 However, a cross sectional survey of a nationally representative sample of 13 586 adults (aged 16 or over) found that of the 440 patients with coronary heart disease, only 114 (26%) were taking lipid lowering drugs. Only 50 (11%) patients had serum cholesterol levels within the target range of ⩽5 mmol/l recommended in guidelines.7 We have also reported a study in which a substantial proportion of patients had increased serum cholesterol levels despite taking lipid lowering drugs.8
We do not know why so many patients fail to achieve target lipid values while taking lipid lowering drugs, particularly as the results of clinical trials are so encouraging.1–4 The drugs may be less effective outside the setting of a clinical trial owing to poorer compliance or different population characteristics (body mass index, number of comorbidities, severity of hyperlipidaemia). Alternatively, lipid lowering drugs may be working as well as in the trials, hence patients should be getting the expected benefits, but the targets set in the guidelines may be unnecessary or unrealistic. Targets may be unrealistic if initial serum cholesterol levels in the unselected population at risk are substantially higher than those included in the trials. This is because a greater absolute reduction in serum cholesterol concentration would be required to reach the guideline targets. Alternatively, doctors may not be prescribing the most effective drugs owing to side effects or cost. We know relatively little about the comparative effectiveness of different lipid lowering drugs because studies that make direct comparisons of the drugs are uncommon. We have only been able to find one study comparing the effectiveness of statins.9 This randomised controlled trial compared five statins, at different doses, over an eight week period in 534 patients. It was published by the manufacturer whose statin was most effective. The study was limited to lower risk patients as obese patients or those with a history of myocardial infarction, recent coronary artery surgery, unstable angina, uncontrolled hypertension, or diabetes were excluded.9 Significantly greater reductions in serum cholesterol values were found with atorvastatin than with other statins.
We conducted this study to compare the effectiveness of individual lipid lowering drugs in lowering serum cholesterol concentration outside the setting of a clinical trial.
Methods
We conducted a cross sectional study, using one year follow up data collected during 2001 from 17 practices in Trent that had taken part in a study of the workload implications of the national service framework for coronary heart disease.10
The study population consisted of people aged 35 years or over receiving current lipid lowering treatment (defined as a prescription within the past three months) who also had at least two serum cholesterol values (at least 28 days apart) recorded on their general practice's computer. We excluded patients whose last prescription for lipid lowering drugs was over three months ago as they may have stopped treatment.
We used MIQUEST to extract the following data from the general practice computer systems: pseudo-anonymous unique identifying code; age; sex; dates and values of all recorded serum cholesterol concentrations; date, dose, and type of lipid lowering drugs; smoking status; body mass index; blood pressure; and comorbidity (stroke, diabetes, ischaemic heart disease).
For each patient we coded his or her drugs according to the most recent prescription issued. At the time of the study five statins were in general use (fluvastatin, cerivastatin, atorvastatin, simvastatin, and pravastatin); cerivastatin has since been withdrawn from the market. We grouped fibrates and other drugs together since the numbers were too few to make comparisons between individual preparations meaningful. We defined pretreatment serum cholesterol concentration as the earliest recorded serum cholesterol value, closest to the start of lipid lowering treatment.
Outcome measures
Our main outcome measure was the proportion of patients taking each lipid lowering drug who achieved a serum cholesterol concentration of ⩽5 mmol/l. This outcome was chosen in accordance with the type of binary outcome often stated in guidelines and used by general practitioners to monitor response to treatments. (The national service framework has a binary outcome and also an interval outcome—that is, a reduction of 30% or more. In practice, however, few general practitioners will work out the percentage.) Our secondary outcome was the percentage reduction in serum cholesterol concentrations with each lipid lowering drug. We included this measure as it tends to be consistent with the method for reporting results of the randomised controlled trials.
Analysis
We used SPSS (version 11.0) and STATA (version 7.0). We compared baseline characteristics of patients who met our inclusion criteria with those who had been excluded by using proportions (χ2 test), means (Student's t test), and medians (Mann-Whitney U test) as appropriate. We undertook a random effects unconditional logistic regression in STATA to determine unadjusted and adjusted odds ratios and 95% confidence intervals for the outcome of having a serum cholesterol concentration of ⩽5 mmol/l. We used simvastatin as the reference drug. Our main explanatory variable of interest was the type of drug (individual statins and fibrates as a group). We adjusted for the potential confounders of age, sex, obesity (body mass index <25, 25-30, >30, not recorded), smoking status (current, former smoker, non-smoker, not recorded), comorbidity (hypertension or not, ischaemic heart disease or not, diabetes or not, stroke or not), and pretreatment serum cholesterol concentrations (<6.0 mmol/l, 6.0-6.9 mmol/l, 7.0-7.9 mmol/l, 8.0-8.9 mmol/l, ⩾9 mmol, not recorded). We included registered general practice as a random effect.
We calculated the mean reduction in serum cholesterol values with 95% confidence intervals by one way analysis of variance, restricting the analysis to those patients with a pretreatment serum cholesterol value. We also undertook a random effects linear regression in STATA to determine the difference between the lipid lowering drugs (particularly atorvastatin) for the percentage reduction in serum cholesterol concentration achieved compared with simvastatin. We adjusted for age, sex, smoking status, comorbidity, obesity, and pretreatment serum cholesterol concentration. We included registered general practice as a random effect.
Results
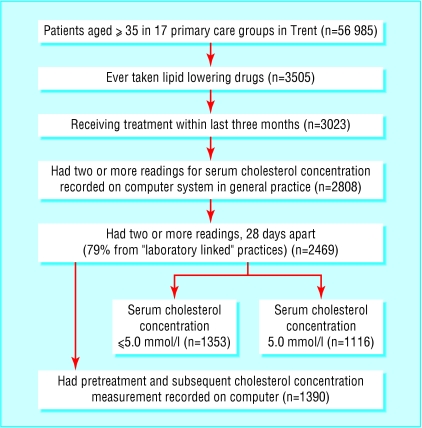
The figure shows the flow of patients in the study. Of the 2469 patients in our target population, 1612 (65.3%) had a diagnosis of ischaemic heart disease or had a current prescription for nitrates (table 1). Only 129 (8%) patients did not have at least one of the comorbidities of ischaemic heart disease, stroke, hypertension, or diabetes. Patients in the study group were of similar age, body mass index, and smoking status to patients who did not meet our inclusion criteria. Patients in our study group were significantly more likely to have one or more of the above comorbidities than patients who did not meet our inclusion criteria.
Table 1.
Characteristics of 2469 patients taking current lipid lowering drugs who have and have not achieved a target value for serum cholesterol concentration of ⩽5 mmol/l. Values are numbers (percentages) of patients unless stated otherwise
| Characteristic
|
No (%) of patients (n=2469)
|
Most recent serum cholesterol concentration
|
P value†
|
|
|---|---|---|---|---|
| ⩽5 mmol/l
|
5 mmol/l
|
|||
| Women | 939 (38.0) | 406 (43.2) | 533 (56.8) | <0.001 |
| Men | 1530 (62.0) | 947 (61.9) | 583 (38.1) | |
| Age group (years): | ||||
| 35-44 | 55 (2.2) | 22 (40.0) | 33 (60.0) | <0.001 |
| 45-54 | 311 (12.6) | 143 (46.0) | 168 (54.0) | |
| 55-64 | 745 (30.2) | 403 (54.1) | 342 (45.9) | |
| 65-74 | 1020 (41.3) | 598 (58.6) | 422 (41.4) | |
| ⩾75 | 338 (13.7) | 187 (55.3) | 151 (44.7) | |
| Body mass index: | ||||
| ⩽25 | 602 (24.4) | 332 (55.1) | 270 (44.9) | 0.001 |
| 25.1-30 | 958 (38.8) | 566 (59.1) | 395 (41.2) | |
| >30 | 672 (27.2) | 348 (51.8) | 326 (48.5) | |
| Not recorded | 232 (9.4) | 107 (46.1) | 125 (53.9) | |
| Smoking status: | ||||
| Non-smoker | 1382 (56.0) | 764 (55.3) | 618 (44.7) | 0.004 |
| Former smoker | 609 (24.7) | 356 (58.5) | 253 (41.5) | |
| Current smoker | 399 (16.2) | 201 (50.4) | 198 (49.6) | |
| Not recorded | 79 (3.2) | 32 (40.5) | 47 (59.5) | |
| Comorbidity*: | ||||
| Ischaemic heart disease | 1612 (65.3) | 1013 (62.8) | 599 (37.2) | <0.001 |
| Stroke | 287 (11.6) | 158 (55.1) | 129 (44.9) | 0.93 |
| Hypertension | 1187 (48.1) | 649 (54.7) | 538 (45.3) | 0.91 |
| Diabetes | 548 (22.2) | 302 (55.1) | 246 (44.9) | 0.87 |
| Total | 2469 (100) | 1353 (54.8) | 1116 (45.2) | |
Some patients had more than one comorbidity.
χ2 test.
Table 1 also compares the characteristics of the 1353 patients (54.8%) whose last recorded serum cholesterol concentration was within the target range with the 1116 patients (45.2%) whose last reading was high. Men were significantly more likely than women to have a last cholesterol reading within the target range. Patients with ischaemic heart disease were significantly more likely to have serum cholesterol values within the target range than patients without ischaemic heart disease.
Effectiveness of statins
Table 2 shows the number of patients in each group with a last recorded serum cholesterol of ⩽5 mmol/l. Overall, 951 patients (38.5%) took atorvastatin, 896 (36.3%) took simvastatin, 241 (9.8%) took cerivastatin, 136 (5.5%) took pravastatin, 65 (2.6%) took fluvastatin, and 180 (7.3%) took other drugs, including fibrates.
Table 2.
Unadjusted and adjusted odds ratios associated with having a serum cholesterol concentration of ⩽5 mmol/l for individual lipid lowering drugs compared with simvastatin
| Drug
|
Total
|
Last recorded serum cholesterol concentration ⩽5 mmol/l
|
Unadjusted odds ratio (95% CI)
|
P value
|
Adjusted odds ratio (95% CI)
|
P value
|
|---|---|---|---|---|---|---|
| Simvastatin | 896 | 530 (59.2) | 1.00 | 1.00 | ||
| Pravastatin | 136 | 62 (45.6) | 0.58 (0.40 to 0.83) | 0.003 | 0.60 (0.40 to 0.91) | 0.015 |
| Cerivastatin | 241 | 125 (51.9) | 0.74 (0.56 to 0.99) | 0.04 | 0.85 (0.60 to 1.21) | 0.38 |
| Fluvastatin | 65 | 23 (35.4) | 0.38 (0.22 to 0.64) | <0.0001 | 0.45 (0.25 to 0.81) | 0.008 |
| Atorvastatin | 951 | 567 (59.6) | 1.02 (0.85 to 1.23) | 0.84 | 1.15 (0.93 to 1.42) | 0.21 |
| Fibrates and others | 180 | 46 (25.6) | 0.24 (0.17 to 0.34) | <0.0001 | 0.24 (0.16 to 0.36) | <0.0001 |
Odds ratios adjusted for sex, age, obesity, smoking status, pretreatment serum cholesterol value, comorbidity (ischaemic heart disease, diabetes, hypertension, stroke), and registered general practice (as random effect).
Of the 2289 patients taking statins, 1307 (57.1%) reached the target range compared with 46 (25.6%) of those taking fibrates and other drugs (χ2=67.0, df=1, P<0.0001). Of the 951 patients taking atorvastatin, 567 (59.6%) reached the target range. A similar proportion of patients taking simvastatin (59.2%) achieved target values. However, only 23 (35.4%) of the 65 patients taking fluvastatin achieved target values.
Patients taking atorvastatin were no more likely than patients taking simvastatin to have serum cholesterol concentrations within the target range (adjusted odds ratio 1.15, 95% confidence interval 0.93 to 1.42) despite adjustment for age, sex, smoking status, obesity, comorbidity, pretreatment serum cholesterol levels, and registered general practice (table 2). Patients taking fluvastatin, pravastatin, or fibrates were significantly less likely to have a serum cholesterol concentration within the target range than patients taking simvastatin.
Table 3 shows the mean serum cholesterol concentrations before treatment and also the most recent values for each individual drug for the 1390 patients who had a pretreatment serum cholesterol concentration recorded. No significant difference was found between the individual statins for the proportion of patients with and without a pretreatment serum cholesterol concentration recorded. One way analysis of variance showed a significant difference between the drugs for pretreatment serum cholesterol concentrations (F=7.07, df=5; P<0.0001), most recent serum cholesterol concentrations (F=11.59, df=5; P<0.0001), and percentage reduction (F=9.68, df=5; P<0.0001). Atorvastatin and simvastatin achieved the greatest reduction in serum cholesterol concentration, with a mean percentage reduction of 30.1%, (28.8% to 31.4%) and 28.0% (26.7% to 29.3%), respectively. Simvastatin and atorvastatin achieved the lowest final serum cholesterol concentrations. The mean final cholesterol concentration for patients taking simvastatin was 5.05 (4.95 to 5.16) mmol/l and for patients taking atorvastatin it was 4.99 (4.90 to 5.09) mmol/l. The percentage reduction achieved in the randomised controlled clinical trials was similar to that in our study.
Table 3.
Pretreatment and most recent serum cholesterol concentration (mmol/l), and percentage reduction by individual lipid lowering drugs. Values are means (95% confidence intervals) unless stated otherwise
| Drug
|
No of patients
|
Pretreatment serum cholesterol concentration
|
Last recorded serum cholesterol concentration
|
% reduction
|
|---|---|---|---|---|
| Fluvastatin | 45 | 7.41 (7.14 to 7.69) | 5.64 (5.34 to 5.94) | 23.66 (20.33 to 26.99) |
| Pravastatin | 78 | 7.14 (6.89 to 7.39) | 5.31 (5.09 to 5.53) | 24.85 (22.03 to 27.67) |
| Cerivastatin | 124 | 6.99 (6.73 to 7.24) | 5.44 (5.22 to 5.66) | 21.17 (18.69 to 23.65) |
| Simvastatin | 480 | 7.12 (7.00 to 7.25) | 5.05 (4.95 to 5.16) | 28.02 (26.71 to 29.34) |
| Atorvastatin | 554 | 7.26 (7.15 to 7.36) | 4.99 (4.90 to 5.09) | 30.11 (28.84 to 31.38) |
| Fibrates and others | 109 | 7.94 (7.52 to 8.35) | 5.71 (5.46 to 5.96) | 25.14 (21.84 to 28.44) |
| Total | 1390 | 7.24 (7.16 to 7.31) | 5.15 (5.09 to 5.21) | 27.70 (26.91 to 28.49) |
Pretreatment serum cholesterol values, ranges, and associated percentage reduction in three randomised controlled trials: the 4S study of simvastatin included participants with serum cholesterol concentration of 5.5 to 8.0 mmol/l (mean 6.7 mmol/l) and achieved a 25% reduction; the LIPID study of pravastatin included participants with serum cholesterol concentrations of 4.0 to 7.0 mmol/l (mean 5.6 mmol/l) and achieved a 20% reduction; the CARE study of pravastatin included participants with serum cholesterol concentrations of <6.2 mmol/l (mean 5.4 mmol/l) and achieved an 18% reduction.
We compared the adjusted mean percentage reduction achieved by atorvastatin with that achieved by simvastatin and found no significant difference (mean difference 1.61%, −0.09 to 3.31). This was despite adjustments for sex, age, obesity, smoking status, pretreatment serum cholesterol concentrations, comorbidity, and registered general practice.
Discussion
The statins vary significantly in their ability to lower serum cholesterol concentrations, with atorvastatin and simvastatin achieving the best results. We found that statins can achieve similar percentage reductions in serum cholesterol concentrations in a primary care setting as in randomised double blind placebo controlled clinical trials.
Initial serum cholesterol concentrations in our study population were higher than those for patients in the clinical trials, which may partly explain the high proportion of patients who fail to achieve the target values set in guidelines, because a greater absolute reduction is needed to achieve the target value of ⩽5 mmol/l. This is important not only for determining whether patients are receiving adequate treatment, but also for doctors whose performance may be monitored by using such targets in funding formulas. We also found that statins were being used in patients with established cardiovascular disease or in those who were likely to be at high risk because of comorbidity such as stroke, diabetes, or hypertension. This is compatible with the approach required in the national service framework for coronary heart disease. Our data, however, show that there is still room for improvement in the overall management of hyperlipidaemia in primary care and, given the expected benefits, there is a strong case for further directing resources to this end.
Traditional studies of drug effectiveness are randomised placebo controlled trials or comparison trials. Such studies may exclude elderly patients or those with comorbidity, reducing potential biases but reducing the generalisability of the findings to the real world of clinical therapeutics. Such studies may also be conducted over a short period of time.
Limitations of study
Cross sectional analysis of drug effectiveness in patients using routine clinical data has limitations as a research methodology. The patients are not randomised and biases may arise in the selection of a treatment for particular patient characteristics. For example, one statin might be preferred when cholesterol concentrations are highest or when a patient is non-responsive to another statin. We used multivariate analysis to adjust for differences in several baseline characteristics, including pretreatment serum cholesterol concentrations, to minimise any bias. The data may be incomplete or inaccurate and there may be recording biases—only increased cholesterol concentration being recorded, for example. As almost 80% of patients were in practices where test results are posted automatically into the patients' records from the laboratory, we do not expect this to have substantially biased our results. Just over half of our population had pretreatment serum cholesterol concentrations recorded on computer, but we found no difference between each drug for the proportion of patients with such values recorded.
Although practices may be atypical in their behaviour, we have no reason to believe that any of the 17 practices in our study were unusual in their interest in or clinical behaviour towards hyperlipidaemia; we have evidence that the patients from such practices are representative of the population of Trent, and Trent is similar to the rest of the United Kingdom.11 Certainly these patients represented a “real life” casemix: 92% had at least one of the four major comorbidities (ischaemic heart disease, stroke, hypertension, or diabetes), and 55% were aged over 65. Despite these limitations, descriptive studies, interpreted with suitable caution, can offer some useful insight to complement the data from studies using randomisation.
Comparison of statins
Three quarters of the patients in our study were taking atorvastatin or simvastatin, and these were the statins associated with the greatest percentage reduction in serum cholesterol concentrations and the highest proportions of patients achieving target levels. Our multivariate analysis showed that atorvastatin and simvastatin yielded the best results, whether the outcome was the target value for serum cholesterol concentration or mean percentage reduction in cholesterol concentration. Pravastatin, fluvastatin, and fibrates were less effective in lowering serum cholesterol concentration. Our ranking of the effectiveness of the lipid lowering drugs was similar to that found in the single previous randomised controlled trial comparing five statins.9
On the basis of effectiveness of lipid lowering alone, atorvastatin or simvastatin should probably be the statins of first choice in primary care. These drugs are associated with a greater reduction in cholesterol concentration and a greater chance of achieving target cholesterol levels despite adjustment for cofounders. We are aware that there have been no direct comparisons of the clinical outcomes in patients taking different statins and, realistically, such studies are unlikely. Furthermore, some of the benefits derived from these drugs may be due to other mechanisms apart form lipid lowering, such as antithrombotic activity, antioxidant effects, or anti-inflammatory effects.12 Initial serum cholesterol concentrations were higher than in the randomised controlled trials, therefore the absolute risk reductions in primary care patients (and hence the overall population benefits) may be greater than thought. Achieving target cholesterol values of 5mmol/l or less may, however, be unrealistic.
Figure.
Flow of patients through study
Acknowledgments
We thank the participating general practices; Andy Meal, Vicky Hammersley, and Lynne Wright for advice on MIQUEST queries; and Lindsay Groom and Janet Yates for their comments on a late draft.
Footnotes
Funding: Trent NHS Executive.
Competing interests: None declared.
Ethical approval: Trent multicentre research ethics committee.
References
- 1.Scandinavian Simvastatin Survival Group. Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian Simvastatin Survival Study (4S) Lancet. 1994;344:1383–1389. [PubMed] [Google Scholar]
- 2.Long-term Intervention with Pravastatin in Ischaemic Heart Disease (LIPID) Study Group. Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. N Engl J Med. 1998;339:1349–1357. doi: 10.1056/NEJM199811053391902. [DOI] [PubMed] [Google Scholar]
- 3.Sacks FM, Pfeffer MA, Moye LA. The effects of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels. The CARE study. N Engl J Med. 1996;335:1001–1009. doi: 10.1056/NEJM199610033351401. [DOI] [PubMed] [Google Scholar]
- 4.Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in 20,536 high risk individuals: a randomised placebo-controlled trial. Lancet. 2002;360:7–22. [Google Scholar]
- 5.Department of Health. National service framework for coronary artery disease: modern standards and service models. London: Stationery Office; 2000. [Google Scholar]
- 6.British Cardiac Society, British Hyperlipidaemia Association, British Hypertension Society, Association. Joint British recommendations on prevention of coronary heart disease in clinical practice: summary. BMJ. 2000;320:705–708. doi: 10.1136/bmj.320.7236.705. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Primatesta P, Poulter N. Lipid concentrations and the use of lipid lowering drugs: evidence from a national cross sectional survey. BMJ. 2000;321:1322–1325. doi: 10.1136/bmj.321.7272.1322. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Hippisley-Cox J, Pringle M, Crown N, Meal A, Wynn A. Sex inequalities in ischaemic heart disease in general practice: cross sectional survey. BMJ. 2001;322:832. doi: 10.1136/bmj.322.7290.832. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Jones P, Kafonek S, Laurora I, Hunninghake D. Comparative dose efficacy study of atorvastatin versus simvastatin, pravastatin, lovastatin, and fluvastatin in patients with hypercholesterolaemia. Am J Cardiol. 1998;81:582–587. doi: 10.1016/s0002-9149(97)00965-x. [DOI] [PubMed] [Google Scholar]
- 10.Hippisley-Cox J, Pringle M. General practice workload implications of the national service framework for coronary heart disease. BMJ. 2001;323:269–270. doi: 10.1136/bmj.323.7307.269. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Hammersley V, Hippisley-Cox J, Wilson A, Pringle M. A comparison of research general practices and their patients with other practices—cross sectional survey in Trent. Br J Gen Pract. 2002;52:463–468. [PMC free article] [PubMed] [Google Scholar]
- 12.Chong P, Seeger J, Franklin C. Clinically relevant differences between the statins. Am J Med. 2000;11:390–400. doi: 10.1016/s0002-9343(01)00870-1. [DOI] [PubMed] [Google Scholar]