We describe a case of medically treated acute primary angle closure (APAC) resulting in severe visual loss owing to retinal haemorrhage. We are unaware of previous reports on this phenomenon in the world literature.
Case report
A 65‐year‐old woman visited her optometrist for a routine check. Her pupils were dilated and no pathology was found. Her vision progressively deteriorated that evening.
She attended the hospital and was noted to have unreactive mid‐dilated pupils bilaterally. Visual acuity was 20/60 OU (pinhole). Intraocular pressure (IOP) was 60 mm Hg OD and 66 mm Hg OS. Gonioscopy showed occluded angles. The patient had moderate hypermetropia but otherwise had no other ocular risk factors for angle closure.
A diagnosis of iatrogenic APAC was made and the patient was given intravenous acetazolamide, topical dexamethasone, iopidine 1% and pilocarpine 4%.
Ninety min later, IOPs was found to be 10 mm Hg OS. Acuity had improved to 20/30 OD and 20/20 OS.
Discharge was planned. After 2 h, the patient was still waiting for treatment when her vision deteriorated suddenly.
Visual acuity was hand motion OU. Pupils were small and IOP remained at 10 mm Hg OU. A clear fundal view was not possible because of miosis. B‐scan ultrasound was undertaken, which raised the suspicion of a “macular bleed”.
She was admitted and re‐examined the next morning. IOP remained controlled and corneas were clear. Visual acuity had improved marginally to counting fingers OD and 20/200 OS. She had bilateral YAG peripheral iridotomies and was subsequently dilated. Funduscopy showed extensive bilateral retinal and pre‐retinal haemorrhages (figs 1, 2). IOP remained normal 1 h after dilatation.
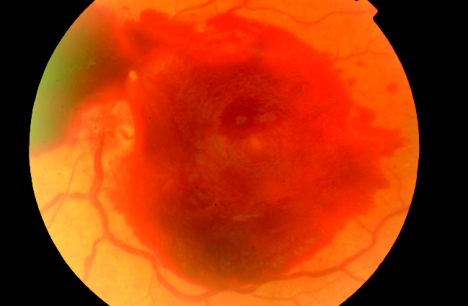
Figure 1 Colour fundus photograph showing severe pre‐retinal haemorrhages at the posterior poles of the right eye, which occurred 2 h after medical intraocular pressure reduction for acute primary angle closure.
Figure 2 Colour fundus photograph showing severe pre‐retinal haemorrhages at the posterior poles of the left eye, which occurred 2 h after medical intraocular pressure reduction for acute primary angle closure.
A diagnosis of bilateral decompression retinopathy secondary to rapid reduction in IOP was made. The patient was not taking aspirin, and had no evidence of bleeding diathesis, diabetes, vasculopathy or other systemic abnormalities that may have contributed to this complication.
Due to the severity of the visual loss it was elected to treat her surgically. She underwent bilateral vitrectomy within 1 month of onset and best corrected visual acuity improved to 20/20 in both eyes with normal IOP.
Comment
The case described is, to the best of our knowledge, unique in the literature. Decompression retinopathy is a rare complication that typically appears after glaucoma surgery. It usually manifests as transient scattered intraretinal haemorrhages at the posterior pole, which resolve within a few weeks, with visual acuity unaffected or slightly reduced.
Only three previous publications have described similar conditions.
Lai and colleagues1 describe two cases of self‐limiting retinal haemorrhages after argon laser peripheral iridoplasty for APAC. Both cases resolved conservatively and vision was restored. In other case reports following Waheeb and coworkers2 describe a case of unilateral retinal haemorrhage YAG peripheral iridotomies for APAC. Nah et al3 describe a patient with APAC treated by peripheral iridotomy. In the latter report scattered retinal haemorrhages developed 2 weeks after treatment. The haemorrhages resolved over time with no visual sequelae.
The exact aetiology of decompression retinopathy is still a matter of speculation. The effect of acute hypotony on the eye may result in mechanical changes in the scleral shell, resulting in shearing forces, or the pressure reduction may simply facilitate an increase in arterial inflow compromising retinal capillaries by hydrostatic mechanisms. Autoregulation of these capillaries may already be defective, particularly when they have been subjected to persistently raised IOP. Decompression retinopathy may be part of the spectrum of central retinal vein occlusion, where IOP reduction causes buckling of the lamina cribrosa with compression of the central retinal vein.
This patient shows a worrying complication of acute reduction in IOP. The development of retinal haemorrhages after solely medical treatment for APAC is exceedingly rare. The severity of the retinopathy despite the absence of major hypotony at any stage is clinically relevant. The prognosis seems to be excellent even when the condition is severe.
Footnotes
Competing interests: None.
References
- 1.Lai J S, Lee V Y, Leung D Y.et al Decompression retinopathy following laser peripheral iridoplasty for acute primary angle‐closure. Eye 2005191345–1347. [DOI] [PubMed] [Google Scholar]
- 2.Waheeb S A, Birt C M, Dixon W S. Decompression retinopathy following YAG laser iridotomy. Can J Ophthalmol 200136278–280. [DOI] [PubMed] [Google Scholar]
- 3.Nah G, Aung T, Yip C C. Ocular decompression retinopathy after resolution of acute primary angle closure glaucoma. Clin Exp Ophthalmol 200028319–320. [DOI] [PubMed] [Google Scholar]