Abstract
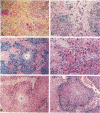
We compared hepatic morphology, hepatocellular siderosis, extrahepatic parenchymal siderosis, and (by chemical assay of liver and spleen) the amount of elemental iron and copper in 12 cases of perinatal hemochromatosis (PH) with 119 perinatal controls. Controls were subgrouped according to diagnoses based on clinical and autopsy findings; 37 had chronic liver disease, either hepatic fibrosis (17) or cirrhosis (20). Graded semiquantitatively, hepatocellular siderosis varied widely among controls, and some showed more than PH cases. By chemical assay, total hepatic iron in PH cases was not significantly greater than in any control group except the preterm. Therefore, our findings do not support an etiological role for iron in PH. Its distinctive hepatic morphology seems related to onset of liver disease during fetal life, when periportal hepatocytes normally contain hemosiderin (as in 71 of 82 controls without chronic liver disease). Environmental agents (such as hypoxia, virus, drug) that could damage a fetal liver would usually damage other fetal organs as well. They would be unlikely to recur in a subsequent pregnancy and thereby account for PH occurring in siblings. In initiating PH, therefore, putative environmental agents may need to interact with a factor or factors intrinsic to the developing fetal liver.
Full text
PDF













Images in this article
Selected References
These references are in PubMed. This may not be the complete list of references from this article.
- Bemmel L. A., Hack W. W., Seldenrijk C. A., Kneepkens C. M. Extensive hepatic necrosis in a premature infant. J Pediatr Gastroenterol Nutr. 1992 Feb;14(2):228–231. doi: 10.1097/00005176-199202000-00019. [DOI] [PubMed] [Google Scholar]
- Berger H. M., Lindeman J. H., van Zoeren-Grobben D., Houdkamp E., Schrijver J., Kanhai H. H. Iron overload, free radical damage, and rhesus haemolytic disease. Lancet. 1990 Apr 21;335(8695):933–936. doi: 10.1016/0140-6736(90)90997-j. [DOI] [PubMed] [Google Scholar]
- Bernstein J. Hepatic involvement in hereditary renal syndromes. Birth Defects Orig Artic Ser. 1987;23(1):115–130. [PubMed] [Google Scholar]
- Bove K. E., Wong R., Kagen H., Balistreri W., Tabor M. W. Exogenous iron overload in perinatal hemochromatosis: a case report. Pediatr Pathol. 1991 May-Jun;11(3):389–397. doi: 10.3109/15513819109064775. [DOI] [PubMed] [Google Scholar]
- Colletti R. B., Clemmons J. J. Familial neonatal hemochromatosis with survival. J Pediatr Gastroenterol Nutr. 1988 Jan-Feb;7(1):39–45. doi: 10.1097/00005176-198801000-00009. [DOI] [PubMed] [Google Scholar]
- Colombo C., Zuliani G., Ronchi M., Breidenstein J., Setchell K. D. Biliary bile acid composition of the human fetus in early gestation. Pediatr Res. 1987 Feb;21(2):197–200. doi: 10.1203/00006450-198702000-00017. [DOI] [PubMed] [Google Scholar]
- Esterly J. R., Slusser R. J., Ruebner B. H. Hepatic lesions in the congenital rubella syndrome. J Pediatr. 1967 Nov;71(5):676–685. doi: 10.1016/s0022-3476(67)80203-8. [DOI] [PubMed] [Google Scholar]
- Faa G., Liguori C., Columbano A., Diaz G. Uneven copper distribution in the human newborn liver. Hepatology. 1987 Sep-Oct;7(5):838–842. doi: 10.1002/hep.1840070508. [DOI] [PubMed] [Google Scholar]
- Finch C. A., Huebers H. Perspectives in iron metabolism. N Engl J Med. 1982 Jun 24;306(25):1520–1528. doi: 10.1056/NEJM198206243062504. [DOI] [PubMed] [Google Scholar]
- Gatter K. C., Brown G., Trowbridge I. S., Woolston R. E., Mason D. Y. Transferrin receptors in human tissues: their distribution and possible clinical relevance. J Clin Pathol. 1983 May;36(5):539–545. doi: 10.1136/jcp.36.5.539. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Glasgow A. M., Kapur S., Miller M. K., Brudno S. Neonatal hyperammonemia resulting from severe in utero hepatic necrosis. J Pediatr. 1986 Jan;108(1):136–138. doi: 10.1016/s0022-3476(86)80789-2. [DOI] [PubMed] [Google Scholar]
- Goldfischer S., Grotsky H. W., Chang C. H., Berman E. L., Richert R. R., Karmarkar S. D., Roskamp J. O., Morecki R. Idiopathic neonatal iron storage involving the liver, pancreas, heart, and endocrine and exocrine glands. Hepatology. 1981 Jan-Feb;1(1):58–64. doi: 10.1002/hep.1840010110. [DOI] [PubMed] [Google Scholar]
- Goldfischer S., Popper H., Sternlieb I. The significance of variations in the distribution of copper in liver disease. Am J Pathol. 1980 Jun;99(3):715–730. [PMC free article] [PubMed] [Google Scholar]
- Hayes A. M., Jaramillo D., Levy H. L., Knisely A. S. Neonatal hemochromatosis: diagnosis with MR imaging. AJR Am J Roentgenol. 1992 Sep;159(3):623–625. doi: 10.2214/ajr.159.3.1503038. [DOI] [PubMed] [Google Scholar]
- Hoogstraten J., de Sa D. J., Knisely A. S. Fetal liver disease may precede extrahepatic siderosis in neonatal hemochromatosis. Gastroenterology. 1990 Jun;98(6):1699–1701. doi: 10.1016/0016-5085(90)91110-r. [DOI] [PubMed] [Google Scholar]
- Iancu T. C. Biological and ultrastructural aspects of iron overload: an overview. Pediatr Pathol. 1990;10(1-2):281–296. doi: 10.3109/15513819009067114. [DOI] [PubMed] [Google Scholar]
- Jonas M. M., Kaweblum Y. A., Fojaco R. Neonatal hemochromatosis: failure of deferoxamine therapy. J Pediatr Gastroenterol Nutr. 1987 Nov-Dec;6(6):984–988. [PubMed] [Google Scholar]
- Kershisnik M. M., Knisely A. S., Sun C. C., Andrews J. M., Wittwer C. T. Cytomegalovirus infection, fetal liver disease, and neonatal hemochromatosis. Hum Pathol. 1992 Sep;23(9):1075–1080. doi: 10.1016/0046-8177(92)90272-5. [DOI] [PubMed] [Google Scholar]
- Knisely A. S., Harford J. B., Klausner R. D., Taylor S. R. Neonatal hemochromatosis. The regulation of transferrin-receptor and ferritin synthesis by iron in cultured fibroblastic-line cells. Am J Pathol. 1989 Feb;134(2):439–445. [PMC free article] [PubMed] [Google Scholar]
- Knisely A. S. Neonatal hemochromatosis. Adv Pediatr. 1992;39:383–403. [PubMed] [Google Scholar]
- Knisely A. S. Neonatal hemochromatosis. Am J Gastroenterol. 1988 Nov;83(11):1312–1313. [PubMed] [Google Scholar]
- Kurnetz R., Yang S. S., Holmes R., Harrison D. D. Neonatal jaundice and coagulopathy. J Pediatr. 1985 Dec;107(6):982–987. doi: 10.1016/s0022-3476(85)80209-2. [DOI] [PubMed] [Google Scholar]
- Metzman R., Anand A., DeGiulio P. A., Knisely A. S. Hepatic disease associated with intrauterine parvovirus B19 infection in a newborn premature infant. J Pediatr Gastroenterol Nutr. 1989 Jul;9(1):112–114. [PubMed] [Google Scholar]
- Moerman P., Pauwels P., Vandenberghe K., Devlieger H., Fryns J. P., Verresen H., Jaeken J., Lauweryns J., Eggermont E. Neonatal haemochromatosis. Histopathology. 1990 Oct;17(4):345–351. doi: 10.1111/j.1365-2559.1990.tb00739.x. [DOI] [PubMed] [Google Scholar]
- Mostoufizadeh M., Lack E. E., Gang D. L., Perez-Atayde A. R., Driscoll S. G. Postmortem manifestations of echovirus 11 sepsis in five newborn infants. Hum Pathol. 1983 Sep;14(9):818–823. doi: 10.1016/s0046-8177(83)80304-9. [DOI] [PubMed] [Google Scholar]
- RUEBNER B. H., MIYAI K. THE PATHOLOGY OF NEONATAL HEPATITIS AND BILIARY ATRESIA WITH PARTICULAR REFERENCE TO HEMOPOIESIS AND HEMOSIDERIN DEPOSITION. Ann N Y Acad Sci. 1963 Dec 30;111:375–391. doi: 10.1111/j.1749-6632.1963.tb36978.x. [DOI] [PubMed] [Google Scholar]
- Raju U. B., Ezhuthachan S., Ma C. K. Perinatal idiopathic hemochromatosis. Henry Ford Hosp Med J. 1988;36(4):187–190. [PubMed] [Google Scholar]
- Risdon R. A., Barry M., Flynn D. M. Transfusional iron overload: the relationship between tissue iron concentration and hepatic fibrosis in thalassaemia. J Pathol. 1975 Jun;116(2):83–95. doi: 10.1002/path.1711160204. [DOI] [PubMed] [Google Scholar]
- Robbins C., Holzman I. R. Diffuse hepatic infarction with complete recovery in a neonate. J Pediatr. 1992 May;120(5):786–788. doi: 10.1016/s0022-3476(05)80249-5. [DOI] [PubMed] [Google Scholar]
- Ruebner B. H., Bhagavan B. S., Greenfield A. J., Campbell P., Danks D. M. Neonatal hepatic necrosis. Pediatrics. 1969 Jun;43(6):963–970. [PubMed] [Google Scholar]
- Rushton D. I. Fetal and neonatal liver disease. Diagn Histopathol. 1981 Jan-Mar;4(1):17–48. [PubMed] [Google Scholar]
- SCHULZ D. M., GIORDANO D. A., SCHULZ D. H. Weights of organs of fetuses and infants. Arch Pathol. 1962 Sep;74:244–250. [PubMed] [Google Scholar]
- Silver M. M., Beverley D. W., Valberg L. S., Cutz E., Phillips M. J., Shaheed W. A. Perinatal hemochromatosis. Clinical, morphologic, and quantitative iron studies. Am J Pathol. 1987 Sep;128(3):538–554. [PMC free article] [PubMed] [Google Scholar]
- Silver M. M., Cave C. T., Kirpalani H. Case 6. Perinatal hemochromatosis. Pediatr Pathol. 1989;9(2):203–210. doi: 10.3109/15513818909022351. [DOI] [PubMed] [Google Scholar]
- Singh S., Sills J. H., Waffarn F. Interesting case presentation: neonatal hemochromatosis as a cause of ascites. J Perinatol. 1990 Jun;10(2):214–216. [PubMed] [Google Scholar]
- Sullivan J. L., Newton R. B. Serum antioxidant activity in neonates. Arch Dis Child. 1988 Jul;63(7 Spec No):748–750. doi: 10.1136/adc.63.7_spec_no.748. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Witzleben C. L., Uri A. Perinatal hemochromatosis: entity or end result? Hum Pathol. 1989 Apr;20(4):335–340. doi: 10.1016/0046-8177(89)90042-7. [DOI] [PubMed] [Google Scholar]
- Zuppan C. W., Bui H. D., Grill B. G. Diffuse hepatic fibrosis in congenital cytomegalovirus infection. J Pediatr Gastroenterol Nutr. 1986 May-Jun;5(3):489–491. doi: 10.1097/00005176-198605000-00029. [DOI] [PubMed] [Google Scholar]
- van Deursen C., de Metz M., Koudstaal J., Brombacher P. Measurement of liver iron content in paraffin-embedded biopsies. J Clin Chem Clin Biochem. 1988 Nov;26(11):689–691. doi: 10.1515/cclm.1988.26.11.689. [DOI] [PubMed] [Google Scholar]