Abstract
Background
Inuit infants have the highest reported rate of hospital admissions because of lower respiratory tract infections in the world. We evaluated the prevalence of reduced ventilation in houses in Nunavut, Canada, and whether this was associated with an increased risk of these infections among young Inuit children.
Methods
We measured ventilation in 49 homes of Inuit children less than 5 years of age in Qikiqtaaluk (Baffin) Region, Nunavut. We identified the occurrence of lower respiratory tract infections using a standardized questionnaire. Associations between ventilation measures and lower respiratory tract infection were evaluated using multiple logistic regression models.
Results
The mean number of occupants per house was 6.1 people. The mean ventilation rate per person was 5.6 L/s (standard deviation [SD] 3.7); 80% (37/46) of the houses had ventilation rates below the recommended rate of 7.5 L/s per person. The mean indoor carbon dioxide (CO2) concentration of 1358 (SD 531) ppm was higher than the recommended target level of 1000 ppm. Smokers were present in 46 homes (94%). Of the 49 children, 27 (55%) had a reported history of lower respiratory tract infection. Reported respiratory infection was significantly associated with mean CO2 levels (odds ratio [OR] 2.85 per 500-ppm increase in mean indoor CO2, 95% confidence interval [CI] 1.23–6.59) and occupancy (OR 1.81 for each additional occupant, 95% CI 1.14–2.86).
Interpretation
Reduced ventilation and crowding may contribute to the observed excess of lower respiratory tract infection among young Inuit children. The benefits of measures to reduce indoor smoking and occupancy rates and to increase ventilation should be studied.
Inuit infants in Qikiqtaaluk (Baffin) Region, Nunavut, Canada, have the highest reported rate of hospital admissions because of severe respiratory syncytial virus infection in the world, with annualized rates of up to 306 per 1000 infants.1 High rates of hospital admission because of lower respiratory tract infections have also been reported among Native infants in Alaska2 and Inuit infants in Greenland.3 Invasive Streptococcus pneumoniae infection, including pneumonia, is also relatively frequent.4 Respiratory syncytial virus infection is also unusually severe in this population: 12% of infants admitted to the Baffin Regional Hospital in Iqaluit (Qikiqtaaluk Region's regional hospital) required intubation and mechanical ventilation, necessitating costly and difficult air transport to tertiary care hospitals in southern Canada.1 Inuit and Alaska Native infants also have disproportionately high rates of permanent chronic lung disease after a lower respiratory tract infection.5 Alaska Native infants have been reported to have the highest prevalence of bronchiectasis recorded, nearly always preceded by recurrent severe lower respiratory tract infection.6–8 The reasons why young Inuit children have such severe respiratory infection remain unclear. Their immune function appears to be normal,6,9 and cystic fibrosis and primary ciliary dyskinesia are rare.6,7 Overcrowding and exposure to environmental tobacco smoke are believed to play important roles.1,10
Ventilation is the process by which fresh air is introduced and stale air removed from an occupied space.11 Adequacy of ventilation can be evaluated directly or indirectly: directly, by measuring air change rates and occupancy and then calculating ventilation per person; indirectly, or by monitoring the indoor concentration of carbon dioxide (CO2), which is a function of the number of occupants (the primary source of indoor CO2) and the amount of airflow available to clear CO2 from the building.12 In the winter of 2003, we completed a pilot study evaluating indoor air quality in the homes of 20 Inuit infants in Cape Dorset, Nunavut. These homes were single-storey dwellings, raised above ground, and had no basements because of permafrost.13 They were small relative to houses in southern Canada. Many of the houses were found to have inadequate ventilation, determined either directly or by evaluating indoor CO2. Exposure to environmental tobacco smoke was nearly universal.14 Our current study was designed to evaluate the hypothesis that inadequate ventilation is prevalent in the houses of young Inuit children in Nunavut and that it is associated with an increased risk of lower respiratory tract infection.15
Methods
Study design
The study was carried out in Inuit houses in 4 communities in Qikiqtaaluk Region, Nunavut: Cape Dorset, Igloolik, Clyde River and Pond Inlet. Each community has a population of 780–1200 people.16 Inuit housing is owned and maintained by the Nunavut Housing Corporation, Government of Nunavut, and all such housing is eligible for investigation of indoor air quality. The target sample size was 25 houses per community — about 15% of the housing in each hamlet. Indoor air quality was measured in a convenience sample of 95 houses selected by the Nunavut Housing Corporation and the local housing councils.17 Our report focuses on the subset of houses occupied by at least 1 Inuit child less than 5 years of age. When more than 1 child lived in a household, we included only the youngest in the study. Informed consent was obtained from each household.
The study was conducted in consultation with 2 local Inuit associations in Iqaluit: the Qikiqtani Inuit Association and Nunavut Tunngavik Inc. Ethics approval was obtained from the Research Ethics Board at the Children's Hospital of Eastern Ontario. A research licence was obtained from the Nunavut Research Institute (Iqaluit, Nunavut).
Investigation of indoor air quality
A trained inspector provided by the Nunavut Housing Corporation carried out a brief home inspection, and samplers were placed in the main living area. Indoor relative humidity, temperature and CO2 concentrations were measured simultaneously over 3–5 days with a portable monitor (YES 206LH monitor, YES Environment Technologies Inc., Delta, BC), which logged data every 15 minutes and detects CO2 with a nondispersive infrared technique.18 Natural air change rates were determined by means of the perfluorocarbon tracer gas technique.19 The study was carried out in 2005 between January and March, under extreme Arctic weather conditions: the mean outdoor temperature was –20°C (range –32°C to –4.5°C). Ventilation during this time of year, when doors and windows are normally kept shut, was expected to be poorest, and generally coincides with the peak rates of lower respiratory tract infection.
Study population
Households received the American Thoracic Society children's respiratory questionnaire (ATS-DLD-C), shortened and slightly modified for use in Nunavut. It was translated into Inuktitut when necessary and administered by a community liaison officer from the Qikiqtani Inuit Association.15,20 Data were collected about the child's age and sex, prior episodes of bronchiolitis or pneumonia, prior visits to the local nursing station, admissions to hospital, any prior history of prematurity or asthma, home occupancy and exposure to environmental tobacco smoke. These liaison officers had no background in health care or research, but they were trained by the senior investigator (T.K.) and an Inuktitut translator experienced in health care terminology provided by the Ottawa Health Sciences Network Inc. (Ottawa) in how to administer the health questionnaire. Interobserver reliability was not assessed.
Outcome measures
Our primary study outcome was whether children had ever experienced a lower respiratory tract infection. Since lower respiratory tract infection can be defined as infection of the intrathoracic airways or lung parenchyma, and because infection with respiratory syncytial virus involves contiguous spread of virus from the bronchioles to the alveoli, we considered a history of either bronchiolitis or pneumonia to constitute lower respiratory tract infection.21
Statistical analysis
Pearson correlation coefficients were used initially to measure correlations among quantitative variables. Associations between dichotomous health outcomes and characteristics of the infants and their homes were determined by odds ratios with 95% confidence intervals and univariate logistic regression. Multiple logistic regressions were performed with lower respiratory tract infection as the outcome variable. Because the sample was small and many of the variables for indoor air quality were highly and often causally related, we limited the multiple logistic regressions to minimally correlated variables. The first model used mean CO2 as the main exposure variable and was adjusted for age, sex of the infant and number of occupants in the home. Occupancy was the main exposure variable in the second model, this time adjusting for age, sex and ventilation rate. In this model, the ventilation rate (in litres per second) was used as the indicator of home ventilation, to separately evaluate the effects of occupancy and ventilation. For all analyses, p < 0.05 was considered to be statistically significant.
Results
Data on respiratory health and residential indoor air quality were collected for 49 children between 3 and 51 months of age (mean age 15.9 months). There were 3, 7, 15 and 24 children included from the 4 communities, respectively. Twenty-seven of the children (55%) were reported to have had a lower respiratory tract infection (defined as either bronchiolitis or pneumonia). Twenty-one of the children (43%) were reported to have been admitted to hospital in Nunavut and 11 (22%) to have required transfer to a tertiary care centre. Characteristics of the children are summarized in Table 1, and observations on indoor air quality in Table 2.22–24 Forty-six (94%) of the 49 homes had occupants who smoked, with a mean of 3 smokers (range 0–8) per household.
Table 1
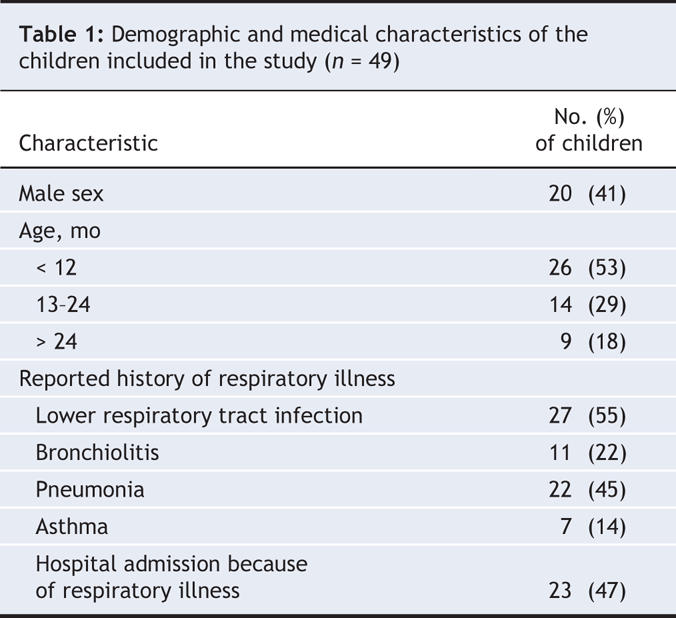
Table 2
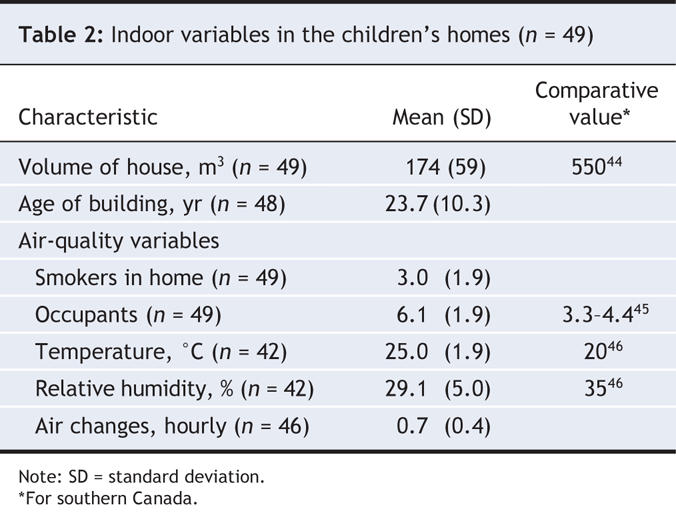
The 49 houses were small (Table 2), although newer houses tended to have larger indoor air volumes (r = 0.32, p = 0.027). The mean number of rooms (excluding bathrooms) per house was 2.8. Occupancy levels were high, with a mean of 6.1 (range 4–12) residents per house. Six houses (13% of 46) had ventilation below the recommended minimum of 0.35 changes of air per hour.25 Ventilation per person was low: the mean value per person was 5.6 L/s (standard deviation [SD] 3.7 L/s) and fell below the recommended limit (7.5 L/s per person) in 80% of these houses.26 Indoor mean CO2 levels were elevated, with a mean of 1358 (SD 531) ppm and a maximum of 2327 (SD 1068) ppm. The target recommended for Canadian residences (mean CO2 1000 ppm) and maximum recommended CO2 level of 3500 ppm were exceeded in 28 (67% of 42) and 5 (12% of 42) homes, respectively.27,28 The houses tended to be warm and dry. Relative humidity was positively associated with mean CO2 level (r = 0.75, p < 0.0001) and negatively associated with ventilation per person (r = –0.54, p < 0.001; Table 3).
Table 3
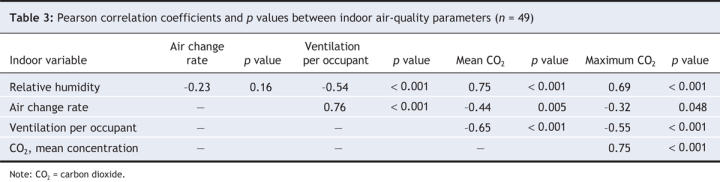
When the study houses were compared with 46 houses in these communities that were not occupied by young children, the differences in age of house, ventilation rate, temperature, relative humidity, and mean and maximum CO2 concentration were not statistically significant (data available from the corresponding author on request). The 46 houses not occupied by children were significantly larger (mean volume 223 m3 v. 174 m3, p = 0.002), with a lower calculated air change rate (0.53 v. 0.70 changes/h, p = 0.038). Because occupancy data were unavailable for the houses without children, we could not compare ventilation rates per person.
In the univariate analyses, reported lower respiratory tract infection was significantly associated with mean and maximum indoor CO2 levels, occupancy, relative humidity and age of house (Figure 1). Reported asthma was associated with increased maximum indoor CO2 concentrations (odds ratio [OR] 1.08, p = 0.048) but not with other measures of ventilation. The scarcity of nonsmoking households precluded any comparisons between smoking and nonsmoking households. Having more versus fewer smokers in the household was not associated with lower respiratory tract infection (Figure 1); although the number of cigarettes smoked would have more accurately represented exposure to environmental tobacco smoke, we did not collect this information. In a multiple logistic regression model, lower respiratory tract infection remained significantly associated with mean CO2 concentration (OR 3.34 per 500-ppm increase in mean CO2, 95% confidence interval [CI] 1.16–9.62) after adjusting for age, sex and occupancy. In a separate model, lower respiratory tract infection was also significantly associated with occupancy (OR 1.83 for each additional occupant, 95% CI 1.09–3.09) after adjusting for age, sex and ventilation rate.
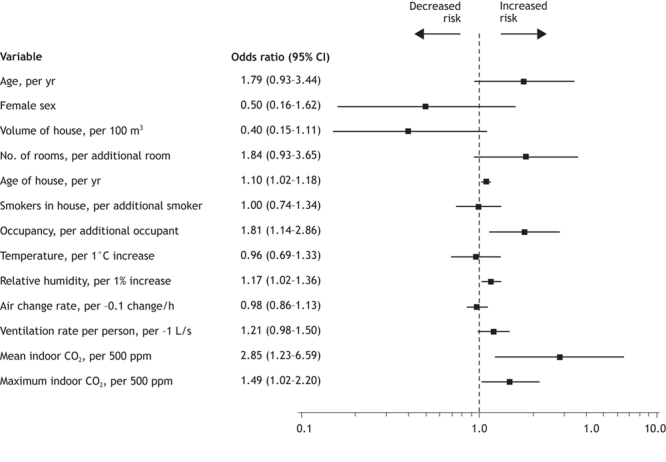
Figure 1: Forest plot (univariate logistic regression) indicating the association between demographic and housing variables and lower respiratory tract infection among 49 young Inuit children in Qikiqtaaluk (Baffin) Region, Nunavut.
Interpretation
Houses in Qikiqtaaluk Region were small and crowded relative to most Canadian homes, and they had reduced ventilation both in absolute terms and relative to the number of occupants. Ventilation was reduced in about 80% of the houses evaluated, with mean and peak CO2 levels commonly exceeding recommended values. In keeping with previous studies of young Inuit children,1–3 rates of reported lower respiratory tract infection were high compared with other populations.
Previous studies have suggested that the risk of lower respiratory tract infection in Inuit and Alaska Native infants is associated with overcrowded housing conditions. One such study1 noted that infants admitted to Baffin Regional Hospital because of lower respiratory tract infection generally lived in very crowded housing, with a mean of 6.4 occupants, including 3.0 children per house, very similar to the mean occupancy of 6.1 occupants per dwelling that we observed. Similarly, among Native children in Alaska, the risk of hospital admission because of respiratory syncytial virus infection was significantly associated with living with 7 or more additional people or with 4 or more children, even after controlling for socioeconomic status.29
We found a strong association between indoor CO2 levels and the risk of lower respiratory tract infection among the Inuit infants and young children in the study. An elevated CO2 level per se would not cause a respiratory infection, but it is a proxy for crowding and reduced ventilation, which may enhance the transmission of infection. Our findings suggest that inadequate home ventilation and overcrowding contributes to the high rate of lower respiratory tract infection observed among Inuit children. Reduced ventilation may increase the concentration of airborne virus. Crowding can increase viral transmission from person to person and increase the probability of an infected person living in the home. Similarly, in 3 office buildings in Boston, detection of indoor airborne rhinovirus was significantly associated with reduced ventilation; a 100-ppm increase in indoor CO2 concentration above background was associated with an increased risk of exposure to infectious droplets.30 Rudnick and Milton,31 in a mathematical model for predicting transmission of airborne rhinovirus in an indoor setting, suggested that an indoor CO2 concentration of 1000 ppm could be associated with increased airborne transmission of common respiratory infections.
Environmental tobacco smoke may be another risk factor for lower respiratory tract infection in Inuit children. In a meta-analysis,32 environmental tobacco smoke significantly increased the risk of hospital admission because of lower respiratory tract infection during infancy and early childhood. Presence of smokers in the home was associated with a significantly increased risk of lower respiratory tract infection in Sisimiut, Greenland,10 and in Alaska.29 Jenkins and colleagues33 reported that 94% of Inuit infants in Iqaluit were exposed to environmental tobacco smoke in the home, like the rate of 94% we observed, and much higher than the frequency of about 25% found in southern Canada.34 Although some studies have found some evidence of a dose–response effect of environmental tobacco smoke,35,36 no “safe” level has been identified. Improving ventilation without reducing exposure is unlikely to diminish the effects of environmental tobacco smoke on this population. The Nunavut Department of Health and Social Services has introduced a program to reduce smoking indoors.37
Other contaminants of indoor air may be associated with an increased risk of lower respiratory tract infection among children. Although earlier studies suggested that indoor nitrogen dioxide concentration was associated with lower respiratory tract infection in infants,38 this has not been supported by recent investigations.39,40 In our Cape Dorset pilot study,14 we did not find elevated indoor nitrogen dioxide concentrations. Lower respiratory tract infection in children has been associated with reported mould and indoor fungal exposure.41 Houses in Nunavut have a very low relative humidity, and indoor mould levels measured in the Cape Dorset pilot study tended to be low except in infants' mattresses, which could increase the risk of lower respiratory tract infection.14 The reported effects of humidity on viral infection of the lower respiratory tract have been contradictory and may depend on the viruses examined. Low relative humidity improves the survival of rhinovirus and influenza virus and reduces aerosol particle size, increasing suspended time. However, high relative humidity increases the survival of other important respiratory viruses, such as adenovirus.8,42 This may explain in part our observed association between lower respiratory tract infection and relative humidity.
Our study has several limitations. First, the cross-sectional study design precludes the demonstration of causality. Second, the study was limited by its small sample, which reduced the precision of our odds ratio estimates. However, given the small size of the hamlets in Qikiqtaaluk Region, a major increase in our sample size would have required either the consent of nearly every suitable household in each community surveyed or the inclusion of nearly twice as many isolated communities, which would have been prohibitively complex and expensive.43 Third, indoor air quality was measured during a relatively short interval, and many variables such as indoor CO2 concentration often fluctuate. Myatt and coworkers,30 however, found a significant relationship between recovery of airborne viruses and indoor CO2 concentration averaged over a 47-hour sampling period, similar to our observations. Fourth, because exposure to environmental tobacco smoke was nearly universal in our study, we cannot conclude whether an association between ventilation and lower respiratory tract infection exists in nonsmoking households. Fifth, we did not evaluate the effects of socioeconomic status indicators such as income. Income levels in Nunavut are generally low, and we believe income was relatively uniform among occupants of these government-funded housing units.44,45
Houses included in the study were not selected randomly; we cannot exclude the possibility that the elders on the local housing councils deliberately selected the most crowded or poorest-quality housing. Although this could have skewed our prevalence estimates for the findings of indoor air quality, this would not have affected associations between indoor air quality and health outcomes. Also, the selected houses were similar to those studied previously by our research team in these communities and in Cape Dorset that did not contain young children, apart from being somewhat smaller and therefore having a somewhat higher calculated air change rate.17
Other limitations of our study include potential diagnostic misclassification and recall bias. Respiratory health outcomes, including hospital admission, were determined retrospectively via occupant survey. However, the questionnaire used was well standardized, and self-report is a technique often used for research into indoor air quality.20,38,46 The liaison officers were not health care professionals, and some terms (e.g., “wheezing”) cannot be translated precisely into Inuktitut. This may have reduced the specificity of survey responses. To mitigate this, we focused on well-defined health outcomes such as lower respiratory tract infection and hospital admission rather than on respiratory symptoms. Unfortunately, we could not verify hospital admissions directly from health records or medical evacuation data, in part because names can be spelled in many ways in Inuktitut, and we did not record subjects' health card information. However, the reported rate of bronchiolitis we obtained (22%) is consistent with the published hospital admission rates of 19.7 per 100 children less than 1 year of age.47
Our study suggests that reduced ventilation rates relative to house volume and crowding are prevalent in Nunavut and may increase the risk of lower respiratory tract infection among young Inuit children. Efforts to improve ventilation relative to occupancy — by developing simple and effective methods of improving home ventilation under the extreme Arctic winter conditions or by increasing the number of houses, or both — are recommended. Further measures to reduce exposure to environmental tobacco smoke in Nunavut houses are also required. We are planning a study to examine whether the installation of a ventilation system with an air supply and exhaust can reduce the frequency of lower respiratory tract infection in this population. Additional research will be needed to examine the relation between reduced ventilation and risk of respiratory infection in homes, schools and offices, particularly as buildings become more tightly sealed to improve energy efficiency.25
@ See related article page 167
Acknowledgments
This study was made possible with the support of the following individuals and organizations: Bob Thompson, Joy Thompson and Chris d'Arcy (Nunavut Housing Corporation) coordinated and funded the home inspectors and assisted with the selection of the study houses; John MacDougall (Qikiqtani Inuit Association, Iqaluit, Nunavut) coordinated the Community Liaison Officers; and Dr. Jim Robar (Canada Mortgage and Housing Corporation) assisted with funding. We thank the Qikiqtani Inuit Association Community Liaison Officers who carried out the health surveys, helped develop local community project awareness and approval, and provided advice on culturally appropriate adjustment of the study design: Rebecca Hutchings (Cape Dorset), Lizzie Palituq (Clyde River), Nathan Tulugarjuk (Igloolik) and David Qamaniq (Pond Inlet). Matthew Jaw, Mayor of Cape Dorset, Nunavut, provided local community approval for the research. The local elders and members of the housing councils of Cape Dorset, Igloolik, Clyde River and Pond Inlet, Nunavut, assisted with the selection of study houses and provided local community approval for the research. Mrs. Annett Filler performed the data entry. We also thank Dr. Paul Villeneuve (Health Canada) for reviewing the manuscript.
Footnotes
Une version française de ce résumé est disponible à l'adresse www.cmaj.ca/cgi/content/full/177/2/155/DC1
This article has been peer reviewed.
Contributors: Thomas Kovesi, Nicolas Gilbert, Don Fugler, Robert Dales and J. David Miller provided substantial contributions to the conception and design of the study. Corrine Stocco provided substantial contributions to the design of the study. Thomas Kovesi, Nicolas Gilbert, Corrine Stocco and Don Fugler contributed to the acquisition, analysis and interpretation of data. Mireille Guay contributed to the analysis and interpretation of data. Thomas Kovesi drafted the article and all other authors revised the article critically for important intellectual content. All authors gave final approval of the version to be published.
This study was supported by Health Canada, the Canada Mortgage and Housing Corporation and the Program of Energy Research and Development, Natural Resources Canada (grant no. PERD-089), Ottawa, Ont.
Competing interests: None declared.
Correspondence to: Dr. Thomas Kovesi, Pediatric Respirologist, Children's Hospital of Eastern Ontario, 401 Smyth Rd., Ottawa ON K1H 8L1; fax 613 738-4886; kovesi@cheo.on.ca
REFERENCES
- 1.Banerji A, Bell A, Mills EL, et al. Lower respiratory tract infections in Inuit infants on Baffin Island. CMAJ 2001;164:1847-50. [PMC free article] [PubMed]
- 2.Karron RA, Singleton RJ, Bulkow L, et al. Severe respiratory syncytial virus disease in Alaska native children. RSV Alaska Study Group. J Infect Dis 1999;180:41-9. [DOI] [PubMed]
- 3.Koch A, Sorensen P, Homoe P, et al. Population-based study of acute respiratory infections in children, Greenland. Emerg Infect Dis 2002;8:586-93. [DOI] [PMC free article] [PubMed]
- 4.Davidson M, Parkinson AJ, Bulkow LR, et al. The epidemiology of invasive pneumococcal disease in Alaska, 1986-1990–ethnic differences and opportunities for prevention. J Infect Dis 1994;170:368-76. [DOI] [PubMed]
- 5.Hemmelgarn B, Ernst P. Airway function among Inuit primary school children in far northern Quebec. Am J Respir Crit Care Med 1997;156:1870-5. [DOI] [PubMed]
- 6.Fleshman JK, Wilson JF, Cohen JJ. Bronchiectasis in Alaska Native children. Arch Environ Health 1968;17:517-23. [DOI] [PubMed]
- 7.Singleton R, Morris A, Redding G, et al. Bronchiectasis in Alaska Native children: causes and clinical courses. Pediatr Pulmonol 2000;29:182-7. [DOI] [PubMed]
- 8.Herbert FA, Wilkinson D, Burchak E, et al. Adenovirus type 3 pneumonia causing lung damage in childhood. Can Med Assoc J 1977;116:274-6. [PMC free article] [PubMed]
- 9.Culman KN, Ward BJ, Pekeles GS, et al. Differences in costimulatory molecules on peripheral blood mononuclear cells in Inuit and non-Inuit Canadian infants [abstract]. Interscience Conference on Antimicrobial Agents and Chemotherapy; 1999 Sept 26–29; San Francisco.
- 10.Koch A, Molbak K, Homoe P, et al. Risk factors for acute respiratory tract infections in young Greenlandic children. Am J Epidemiol 2003;158:374-84. [DOI] [PubMed]
- 11.Hui S. Lecture: Air movement and natural ventilation. Available: www.arch.hku.hk/teaching/lectures/airvent (accessed 2007 May 17).
- 12.Jankovic JT, Ihle R, Vick D. Occupant generated carbon dioxide as a measure of dilution ventilation efficiency. Am Ind Hyg Assoc J 1996;57:756-9. [DOI] [PubMed]
- 13.Kovesi T, Gilbert NL, Creery D, et al. Indoor air quality risk factors for severe lower respiratory tract infections in Inuit infants in Baffin Region, Nunavut, Canada: a pilot study [abstract]. Am J Respir Crit Care Med 2004;2:A696. [DOI] [PubMed]
- 14.Kovesi T, Creery D, Gilbert NL, et al. Indoor air quality risk factors for severe lower respiratory tract infections in Inuit infants in Baffin Region, Nunavut: a pilot study. Indoor Air 2006;16:266-75. [DOI] [PubMed]
- 15.Kovesi T, Stocco C, Dales RE, et al. A multi-community survey of indoor air quality risk factors for severe lower respiratory tract infections (LRTI) in Inuit infants in Baffin region, Nunavut, Canada [abstract]. Proc Am Thorac Soc 2006;3:A397. [DOI] [PubMed]
- 16.Statistics Canada. Births and deaths statistics for Cape Dorset, NT. Available: www12.statcan.ca/english/profil/Details/details1hlth.cfm?SEARCH=BEGINS&PSGC=61&SGC=6104007&A=A&LANG=E&Province=61&PlaceName=Cape%20Dorset&CSDNAME=Cape%20Dorset&CMA=0&SEARCH=BEGINS&DataType=1&TypeNameE=Hamlet&ID=14163 (accessed 2007 May 17).
- 17.Fugler D. Nunavut housing ventilation research 2003–2005. Ottawa: Canada Mortgage and Housing Corporation; 2005. Report no 05-116.
- 18.YES-206LH series, indoor air quality monitor — logger, operation manual [pamphlet]. Rev C. Delta (BC): YES Environment Technologies Inc; 2003.
- 19.Nathanson T. Health Canada. Indoor air quality in office buildings: a technical guide. Ottawa: Minister of Supply and Services Canada; 1995. Cat no H46-2/93-16 Erev. Available: www.hc-sc.gc.ca/ewh-semt/alt_formats/hecs-sesc/pdf/pubs/air/office_building-immeubles_bureaux/93ehd-dhm166_e.pdf (accessed 2007 May 17).
- 20.Ferris BG. Epidemiology Standardization Project (American Thoracic Society). Am Rev Respir Dis 1978;118:1-120. [PubMed]
- 21.McIntosh K. Infections due to respiratory syncytial virus. In: Behrman RE, Vaughan VC, Nelson WE, editors. Nelson textbook of pediatrics. 13th ed. Philadelphia: Saunders; 1987. p. 680-2.
- 22.Office of Energy Efficiency; National Energy Use Database. 1997 Survey of household energy use — summary report. Ottawa, Natural Resources Canada; 2000. Available: http://oee.nrcan.gc.ca/publications/infosource/pub/energy_use/sheu_e/index.cfm (accessed 2007 May 17).
- 23.Lawton MD, Dales RE, White J. The influence of house characteristics in a Canadian community on microbiological contamination. Indoor Air 1998;8:2-11.
- 24.Dumont R. Ventilation control in medium air tightness houses. Ottawa: Canada Mortgage and Housing Corporation; 1995.
- 25.Shaw CY. Canadian building digest. CBD-245. Mechanical ventilation and air pressure in houses. Available: http://irc.nrc-cnrc.gc.ca/pubs/cbd/cbd245_e.html (accessed 2007 May 17).
- 26.American Society of Heating Refrigerating and Air Conditioning Engineers Inc. ASHRAE handbook fundamentals,1997. Atlanta: American Society of Heating, Refrigerating and Air-Conditioning Engineers Inc; 1997. p. 25.5.
- 27.American Society of Heating Refrigerating and Air-Conditioning Engineers Inc. ASHRAE standard 62.1-2004: ventilation for acceptable indoor air quality. Appendix E, Table E-2. Atlanta: The Society; 2004. p. 38.
- 28.Enmet Canada Ltd. Notes on CO2 (indoor air quality). Available: www.enmetgasdetection.com/articles/notes_on_co2.htm (accessed 2007 May 17).
- 29.Bulkow LR, Singleton RJ, Karron RA, et al. Risk factors for severe respiratory syncytial virus infection among Alaska native children. Pediatrics 2002;109:210-6. [DOI] [PubMed]
- 30.Myatt TA, Johnston SL, Zuo Z, et al. Detection of airborne rhinovirus and its relation to outdoor air supply in office environments. Am J Respir Crit Care Med 2004;169:1187-90. [DOI] [PubMed]
- 31.Rudnick SN, Milton DK. Risk of indoor airborne infection transmission estimated from carbon dioxide concentration. Indoor Air 2003;13:237-45. [DOI] [PubMed]
- 32.Li JS, Peat JK, Xuan W, et al. Meta-analysis on the association between environmental tobacco smoke (ETS) exposure and the prevalence of lower respiratory tract infection in early childhood. Pediatr Pulmonol 1999;27:5-13. [DOI] [PubMed]
- 33.Jenkins AL, Gyorkos TW, Joseph L, et al. Risk factors for hospitalization and infection in Canadian Inuit infants over the first year of life — a pilot study. Int J Circumpolar Health 2004;63:61-70. [DOI] [PubMed]
- 34.Canadian Institute for Health Information. Canadian Lung Association, Health Canada, et al. Respiratory disease in Canada. Ottawa: Editorial Board Respiratory Disease in Canada, Health Canada; 2001. Available: www.phac-aspc.gc.ca/publicat/rdc-mrc01/pdf/rdc0901e.pdf (accessed 2007 May 17).
- 35.Jedrychowski W, Flak E. Maternal smoking during pregnancy and postnatal exposure to environmental tobacco smoke as predisposition factors to acute respiratory infections. Environ Health Perspect 1997;105:302-6. [DOI] [PMC free article] [PubMed]
- 36.Ugnat AM, Mao Y, Miller AB, et al. Effects of residential exposure to environmental tobacco smoke on Canadian children. Can J Public Health 1990;81:345-9. [PubMed]
- 37.Department of Health and Social Services; Government of Nunavut. Health promotion programs. Available: www.gov.nu.ca/hsssite/promo.shtml (accessed 2007 May 17).
- 38.Triche EW, Belanger K, Beckett W, et al. Infant respiratory symptoms associated with indoor heating sources. Am J Respir Crit Care Med 2002;166:1105-11. [DOI] [PubMed]
- 39.Sunyer J, Puig C, Torrent M, et al. Nitrogen dioxide is not associated with respiratory infection during the first year of life. Int J Epidemiol 2004;33:116-20. [DOI] [PubMed]
- 40.Chauhan AJ, Inskip HM, Linaker CH, et al. Personal exposure to nitrogen dioxide (NO2) and the severity of virus-induced asthma in children. Lancet 2003;361:1939-44. [DOI] [PMC free article] [PubMed]
- 41.Stark PC, Burge HA, Ryan LM, et al. Fungal levels in the home and lower respiratory tract illnesses in the first year of life. Am J Respir Crit Care Med 2003;168:232-7. [DOI] [PubMed]
- 42.Arundel AV, Sterling EM, Biggin JH, et al. Indirect health effects of relative humidity in indoor environments. Environ Health Perspect 1986;65:351-61. [DOI] [PMC free article] [PubMed]
- 43.Nunavut Bureau of Statistics. Nunavut: community population estimates. Available: www.gov.nu.ca/popestimates.pdf (accessed 2007 May 17).
- 44.Clark M, Riben P, Nowgesic E. The association of housing density, isolation and tuberculosis in Canadian First Nations communities. Int J Epidemiol 2002;31:940-5. [DOI] [PubMed]
- 45.Young TK, Mollins CJ. The impact of housing on health: an ecologic study from the Canadian Arctic. Arctic Med Res 1996;55:52-61. [PubMed]
- 46.Dales RE, Zwanenburg H, Burnett R, et al. Respiratory health effects of home dampness and molds among Canadian children. Am J Epidemiol 1991;134:196-203. [DOI] [PubMed]
- 47.Creery D, Lyer P, Samson L, et al. Costs associated with infant bronchiolitis in the Baffin region of Nunavut. Int J Circumpolar Health 2005;64:38-45. [DOI] [PubMed]


