Abstract
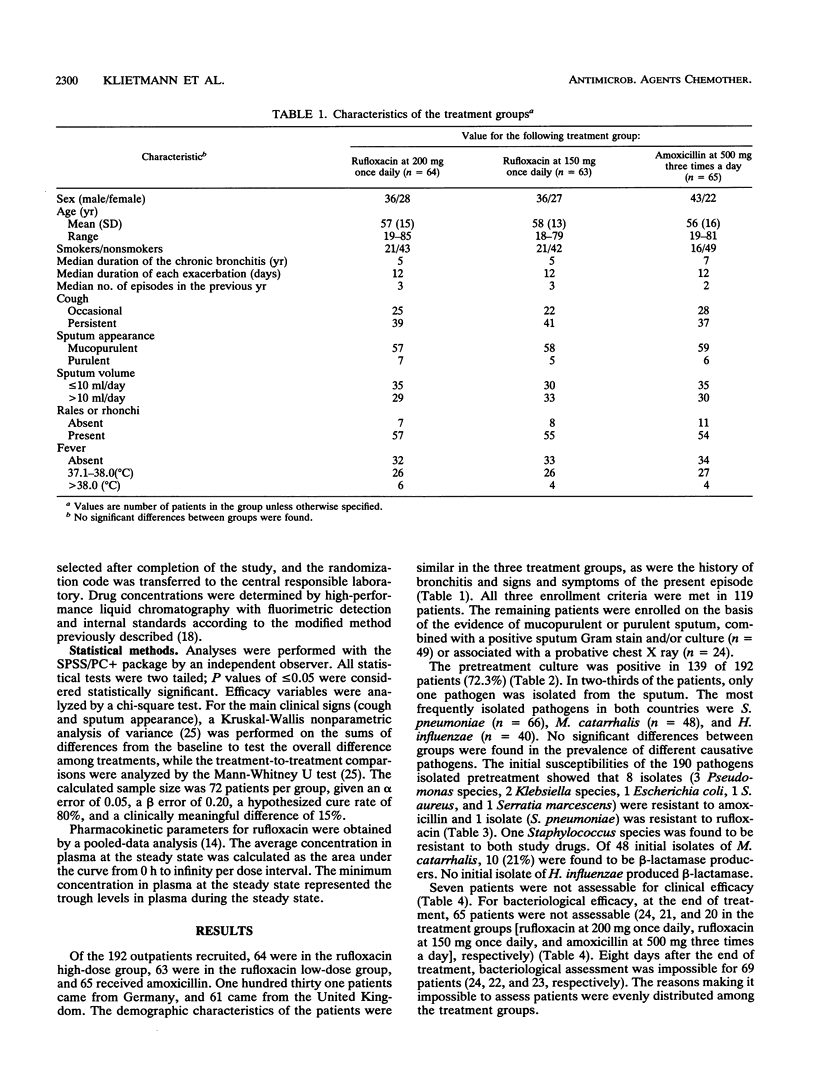
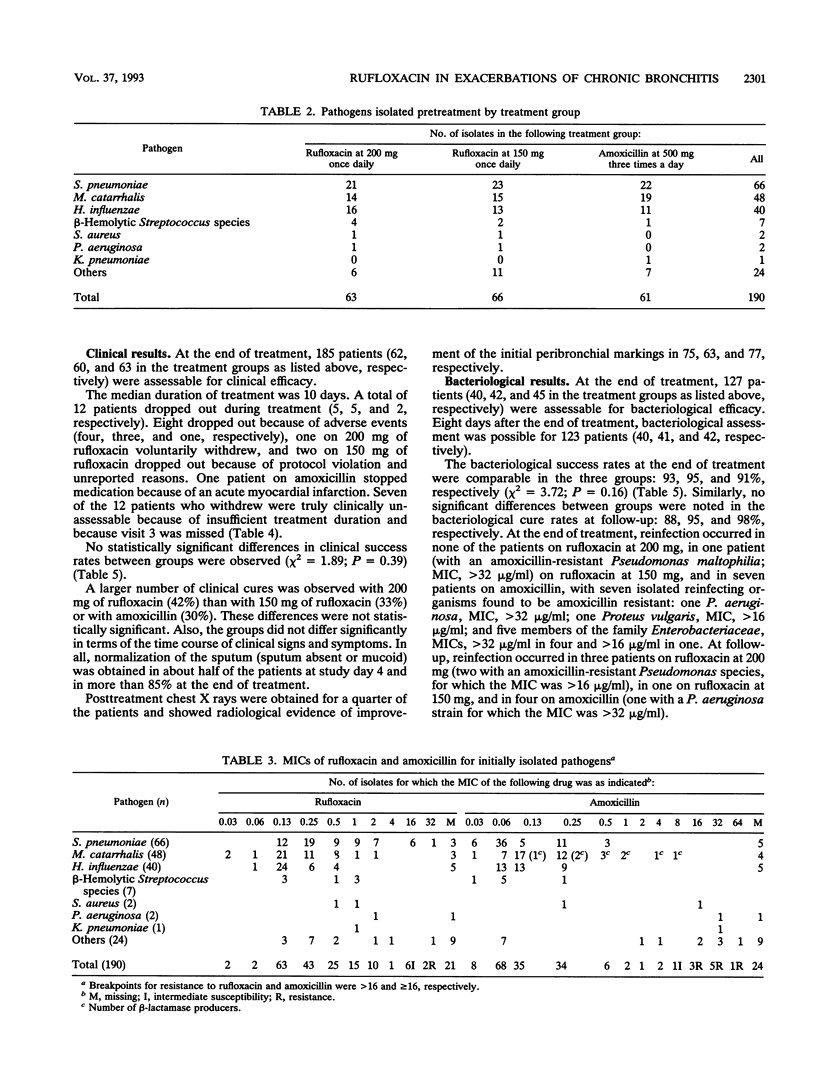
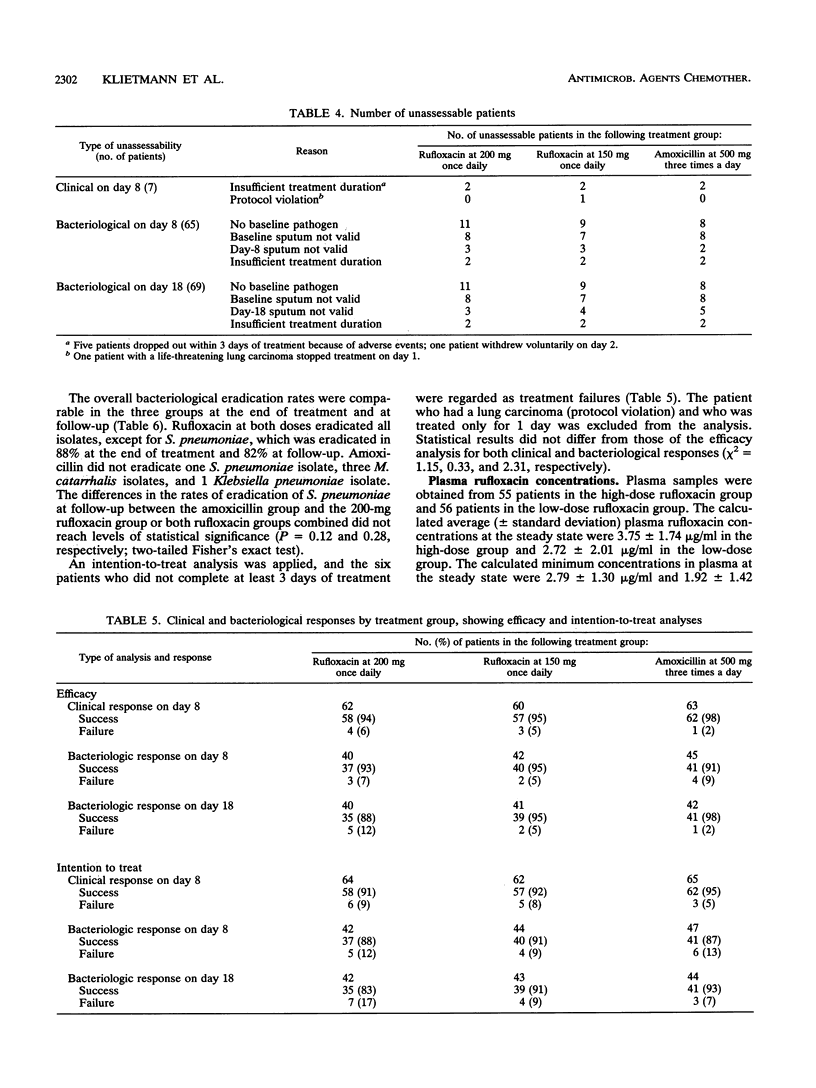
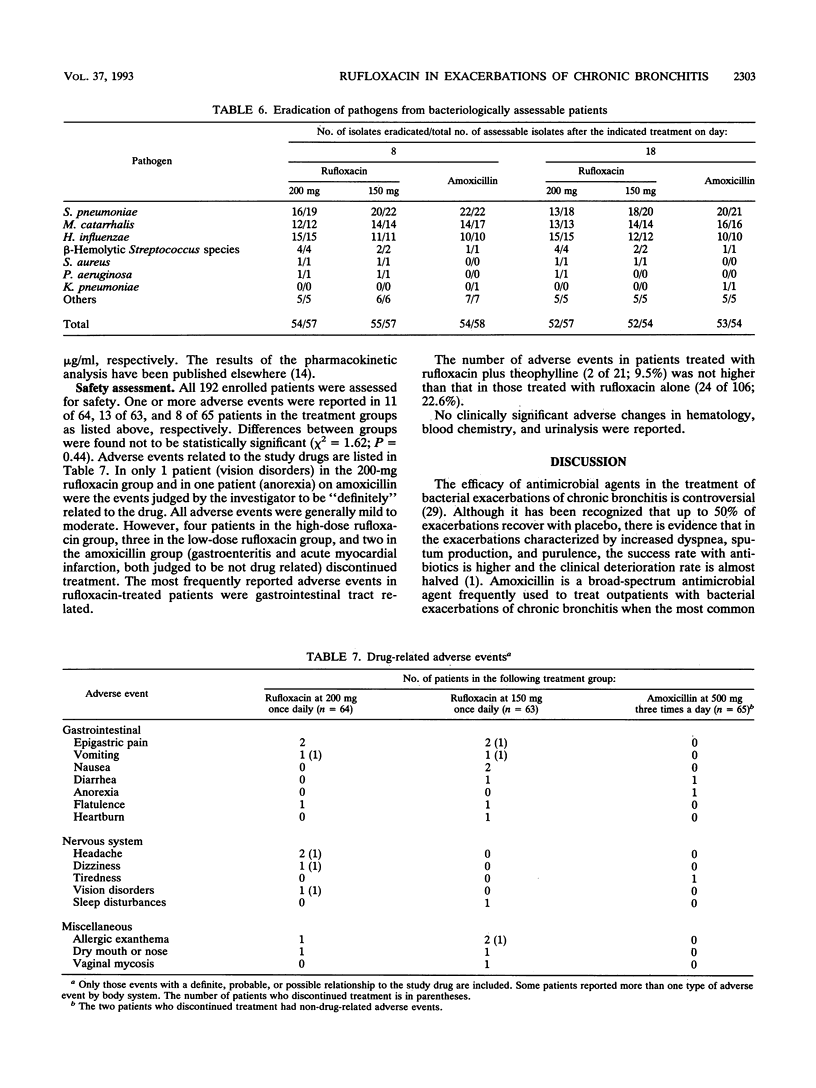
In a double-blind, randomized, multicenter study, the efficacy and safety of two dosage schedules of rufloxacin once daily were compared with those of amoxicillin three times a day in the treatment of 192 outpatients with exacerbations of chronic bronchitis. Rufloxacin was given as a single oral dose of 400 mg on day 1 and single daily doses of 200 mg on the subsequent 9 days (n = 64) or as 300 mg on day 1 and then 150 mg daily for 9 days (n = 63); amoxicillin was given as 500 mg orally three times a day for 10 days (n = 65). Clinical and bacteriological assessments were carried out before treatment, between study days 3 and 5, and at days 1 and 8 after treatment. Pretreatment cultures were positive for 139 patients, the most frequently isolated pathogens being Streptococcus pneumoniae, Moraxella catarrhalis, and Haemophilus influenzae. Clinical success rates were comparable in the three groups (94, 95, and 98%, respectively), as were bacteriological success rates at the end of treatment (93, 95, and 91%, respectively) and at follow-up (88, 95, and 98%, respectively). The power to detect a significant 15% difference in cure rates was 74.9%. Follow-up bacteriological failures from pneumococcal infection were 18% in both rufloxacin groups combined and 5% in the amoxicillin group. The 200-mg dose regimen achieved average steady-state concentrations in plasma higher than did the 150-mg dose regimen (3.75 versus 2.72 micrograms/ml). Adverse events occurred in 11 and 13 patients, respectively, on rufloxacin and 8 on amoxicillin. This study shows that rufloxacin once daily ay be a possible option for the treatment of acute exacerbations of chronic bronchitis. The 200-mg daily oral dose preceeded by a loading dose of 400 mg displays a better pharmacokinetic profile than the lower dose.
Full text
PDF





Selected References
These references are in PubMed. This may not be the complete list of references from this article.
- Anthonisen N. R., Manfreda J., Warren C. P., Hershfield E. S., Harding G. K., Nelson N. A. Antibiotic therapy in exacerbations of chronic obstructive pulmonary disease. Ann Intern Med. 1987 Feb;106(2):196–204. doi: 10.7326/0003-4819-106-2-196. [DOI] [PubMed] [Google Scholar]
- Brouwers J. R. Drug interactions with quinolone antibacterials. Drug Saf. 1992 Jul-Aug;7(4):268–281. doi: 10.2165/00002018-199207040-00003. [DOI] [PubMed] [Google Scholar]
- Cecchetti V., Fravolini A., Fringuelli R., Mascellani G., Pagella P., Palmioli M., Segre G., Terni P. Quinolonecarboxylic acids. 2. Synthesis and antibacterial evaluation of 7-oxo-2,3-dihydro-7H-pyrido[1,2,3-de][1,4]benzothiazine-6-carboxylic acids. J Med Chem. 1987 Mar;30(3):465–473. doi: 10.1021/jm00386a005. [DOI] [PubMed] [Google Scholar]
- Cesana M., Broccali G., Imbimbo B. P., Crema A. Effect of single doses of rufloxacin on the disposition of theophylline and caffeine after single administration. Int J Clin Pharmacol Ther Toxicol. 1991 Apr;29(4):133–138. [PubMed] [Google Scholar]
- Chodosh S. Acute bacterial exacerbations in bronchitis and asthma. Am J Med. 1987 Apr 27;82(4A):154–163. [PubMed] [Google Scholar]
- Cogo R., Rimoldi R., Mattina R., Imbimbo B. P. Steady-state pharmacokinetics of rufloxacin in elderly patients with lower respiratory tract infections. Ther Drug Monit. 1992 Feb;14(1):36–41. doi: 10.1097/00007691-199202000-00006. [DOI] [PubMed] [Google Scholar]
- Davies B. I., Maesen F. P. Treatment of Branhamella catarrhalis infections. J Antimicrob Chemother. 1990 Jan;25(1):1–4. doi: 10.1093/jac/25.1.1. [DOI] [PubMed] [Google Scholar]
- Dirksen M., Focht J., Boerema J. Rufloxacin once daily in acute exacerbations of chronic bronchitis. Infection. 1991 Jul-Aug;19(4):297–300. doi: 10.1007/BF01644971. [DOI] [PubMed] [Google Scholar]
- Imbimbo B. P., Broccali G., Cesana M., Crema F., Attardo-Parrinello G. Inter- and intrasubject variabilities in the pharmacokinetics of rufloxacin after single oral administration to healthy volunteers. Antimicrob Agents Chemother. 1991 Feb;35(2):390–393. doi: 10.1128/aac.35.2.390. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jacoby G. A., Archer G. L. New mechanisms of bacterial resistance to antimicrobial agents. N Engl J Med. 1991 Feb 28;324(9):601–612. doi: 10.1056/NEJM199102283240906. [DOI] [PubMed] [Google Scholar]
- Kayser F. H., Morenzoni G., Santanam P. The Second European Collaborative Study on the frequency of antimicrobial resistance in Haemophilus influenzae. Eur J Clin Microbiol Infect Dis. 1990 Nov;9(11):810–817. doi: 10.1007/BF01967379. [DOI] [PubMed] [Google Scholar]
- Kisicki J. C., Griess R. S., Ott C. L., Cohen G. M., McCormack R. J., Troetel W. M., Imbimbo B. P. Multiple-dose pharmacokinetics and safety of rufloxacin in normal volunteers. Antimicrob Agents Chemother. 1992 Jun;36(6):1296–1301. doi: 10.1128/aac.36.6.1296. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Klietmann W., Focht J., Nösner K. Comparative in vitro activity of ciprofloxacin against aerobic and anaerobic bacteria from clinical isolates. Arzneimittelforschung. 1987 Jun;37(6):661–666. [PubMed] [Google Scholar]
- Klugman K. P. Pneumococcal resistance to antibiotics. Clin Microbiol Rev. 1990 Apr;3(2):171–196. doi: 10.1128/cmr.3.2.171. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lindsay G., Scorer H. J., Carnegie C. M. Safety and efficacy of temafloxacin versus ciprofloxacin in lower respiratory tract infections: a randomized, double-blind trial. J Antimicrob Chemother. 1992 Jul;30(1):89–100. doi: 10.1093/jac/30.1.89. [DOI] [PubMed] [Google Scholar]
- Mattina R., Bonfiglio G., Cocuzza C. E., Gulisano G., Cesana M., Imbimbo B. P. Pharmacokinetics of rufloxacin in healthy volunteers after repeated oral doses. Chemotherapy. 1991;37(6):389–397. doi: 10.1159/000238885. [DOI] [PubMed] [Google Scholar]
- Murray P. R., Washington J. A. Microscopic and baceriologic analysis of expectorated sputum. Mayo Clin Proc. 1975 Jun;50(6):339–344. [PubMed] [Google Scholar]
- Norrby S. R. Side-effects of quinolones: comparisons between quinolones and other antibiotics. Eur J Clin Microbiol Infect Dis. 1991 Apr;10(4):378–383. doi: 10.1007/BF01967014. [DOI] [PubMed] [Google Scholar]
- Powell M. Chemotherapy for infections caused by Haemophilus influenzae: current problems and future prospects. J Antimicrob Chemother. 1991 Jan;27(1):3–7. doi: 10.1093/jac/27.1.3. [DOI] [PubMed] [Google Scholar]
- Thys J. P., Jacobs F., Byl B. Role of quinolones in the treatment of bronchopulmonary infections, particularly pneumococcal and community-acquired pneumonia. Eur J Clin Microbiol Infect Dis. 1991 Apr;10(4):304–315. doi: 10.1007/BF01967004. [DOI] [PubMed] [Google Scholar]
- Wise R., Andrews J. M., Matthews R., Wolstenholme M. The in-vitro activity of two new quinolones: rufloxacin and MF 961. J Antimicrob Chemother. 1992 Jun;29(6):649–660. doi: 10.1093/jac/29.6.649. [DOI] [PubMed] [Google Scholar]


