Abstract
Following infection of the host with a virus, the delicate balance between virus replication/spread and the immune response to the virus determines the outcome of infection, i.e., persistence versus elimination of the virus. It is unclear, however, what relative roles immunologic and virologic factors play during primary viral infection in determining the subsequent clinical outcome. By studying a cohort of subjects with primary HIV infection, it has been demonstrated that qualitative differences in the primary immune response to HIV, but not quantitative differences in the initial levels of viremia are associated with different clinical outcomes.
Keywords: primary infection, prognosis
Prospective studies on large cohorts of HIV-infected individuals have clearly indicated that the rates of progression of HIV disease may vary greatly among individuals (1). Several studies have attempted to determine the pathogenic mechanisms associated with progressive versus nonprogressive HIV disease. Preservation of immune function and low levels of virologic parameters are common findings in HIV-infected subjects with nonprogressive disease (1–9), whereas loss of immune function and high levels of virus are associated with rapid progression (1, 10). These observations have strongly suggested that the delicate balance between HIV replication and the immune response of the host may be critical for determining different rates of disease progression. Although retrospective analyses of the levels of viremia in plasma samples collected from 6 months to 2 years following seroconversion have clearly demonstrated that this parameter can be predictive of different rates of disease progression (11), these and other studies performed in subjects chronically infected with HIV have failed to identify any virologic or immunologic factors that clearly tilt the balance between the spread and containment of virus. However, the levels of viremia and the status of immune function that are observed during the stage of chronic HIV disease may have already been established by pathogenic events that had transpired at the time of the initial interaction between HIV and the immune system. Therefore, it is conceivable that analysis of virologic and immunologic parameters early during primary infection and during the transition from the acute to the chronic phase of infection, may provide important insights for the identification of those factors that influence the progression of HIV disease.
Both vigorous humoral and cellular immune responses have been detected during primary infection, and the temporal relationship between the appearance of an HIV-specific immune response, down-regulation of viremia, and resolution of the acute viral syndrome has been clearly established (12–18). These observations represent strong evidence of the fundamental role of the immune response in the control of the initial burst of virus replication in primary HIV infection. Standard immunologic parameters such as HIV-specific cytotoxic T lymphocyte (CTL) responses and antibodies against a variety of HIV proteins are common findings in subjects with primary HIV infection (12–18). Based on these analyses one may conclude that the primary immune response to HIV is similar among different individuals; nonetheless, these individuals may experience different rates of disease progression. Therefore, analysis of standard immunologic parameters may not be adequate to fully appreciate protective versus nonprotective immune responses. The molecular characterization of the cell-mediated immune response to HIV by analysis of the T cell receptor (TCR) repertoire is a more appropriate approach for determining the diversity and dynamics of the immune response among different individuals. The TCR is composed of an α and β chain, which are encoded by discontinuous, polymorphic gene segments (V, D, and J), and which mediate antigen recognition by T cells. The germ-line β chain V segment repertoire includes 47 functional members grouped into 24 families (19–20).
Previous studies have demonstrated that expansions of subsets of CD8+ cells of different Vβ families are a major component of the primary immune response to both HIV (21) and simian immunodeficiency virus infections (22). With regard to primary HIV infection, it has been shown that these Vβ expansions are oligo-monoclonal in nature, and that the expanded CD8+ Vβ T cell subsets contained HIV-specific CTLs (21). This was shown for the expanded Vβs 23 and 22 in patients 15 and 45, respectively (data not shown). This study analyzed the changes in the Vβ repertoire during primary HIV infection and during and following the transition to the chronic phase of infection, and has determined the relationship of these changes to the rate of disease progression.
MATERIALS AND METHODS
Patients.
Twenty-one subjects with well-documented historical, clinical, and laboratory parameters of primary HIV infection were studied serially at various times following infection. All patients included in this study experienced an acute, mononucleosis-like viral syndrome of variable severity. The clinical histories of patients 1–6 have been previously reported (12, 18). Patients 1, 2, 3, 4, 10, and 16 had a severe clinical syndrome, and the first five patients were hospitalized. Only patient 22 had mild symptoms (pharingitis and diarrhea) that did not require medical attention, whereas the remaining 14 patients had a clinical syndrome of moderate severity, which brought them to the attention of physicians. Only patients 15, 20, and 22 received mono-(zidovudine) or combination-(zidovudine plus didanosine) antiviral therapy during the first year of infection.
Analysis of Vβ Repertoire.
The Vβ repertoire in freshly unfractionated peripheral blood mononuclear cells (PBMC) collected at different time points from the onset of symptoms was analyzed by a semi-quantitative polymerase chain reaction (PCR). At least a doubling in the relative expression of Vβ families among sequential time points by PCR was required for the change to be considered significant. Briefly, 2 μg of total RNA, extracted by the RNAzol method (23), were reverse transcribed using random hexamers (20 μg ml−1; Promega), avian myeloblastosis virus reverse transcriptase (60 units; Life Science, Arlington Heights, IL) and dNTPs (Boehringer Mannheim). PCR analysis for the different Vβs used a 5′-specific Vβ primer and a common 3′ constant-domain Cβ primer. 5′ and 3′ Cα primers were included in each PCR reaction as internal controls. To monitor the migration of Vβ and Cα bands, 3′ Cβ and 3′ Cα primers were radiolabeled with [32P-γ]ATP (Amersham). Primer sequences of Vβ-specific oligonucleotides and of the control Cβ and Cα oligonucleotides have been reported (24). One aliquot of each PCR reaction was loaded and separated on 10% polyacrylamide gels containing 7 M urea. Gels were exposed overnight on Kodak storable phosphor screens, and the radioactive signal for each Vβ was quantified using a PhosphorImager (Molecular Dynamics).
Determination of Plasma Viremia.
Determination of viremia has been performed by competitive PCR in patients 1–6 (25–27), and branched-DNA has been used in the other patients included in this study (28). The same method has been used for the first and the last time points.
Statistical Analysis.
With regard to the slopes of CD4+ T cell decline, the results were graphed in a bivariate scattergram plot, and differences between the curves submitted to unpaired t test analysis. Similar statistical analysis was performed to determine the differences in the levels of viremia observed in the patients belonging to the three patterns of Vβ perturbations, either during primary infection or 1 year after primary infection.
RESULTS
Analysis of the Vβ Repertoire.
Analysis of the Vβ repertoire was performed in PBMC samples collected at different time points by using a semi-quantitative PCR assay (21, 24, 29). The first PBMC sample was generally collected within 1–8 weeks from the onset of symptoms, and longitudinal analysis was performed on at least three PBMC samples collected during the first 16–20 weeks from the onset of symptoms. Perturbations (i.e., increments and/or declines) of a Vβ family were considered to be significant only if there was at least a 2-fold change in the percentage of the Vβ family in question over several time points. However, 2-fold changes were not considered to be significant if they involved Vβ families that were expressed at very low levels (i.e., 1–2%). In fact, when the Vβ families are expressed at very low levels, the bands corresponding to these Vβs are generally very faint, and may be very difficult to measure accurately on the PhosphorImager. For these reasons, other authors (30) prefer to assign an arbitrary value of <1% to those families expressed at very low levels. The rationale for considering a 2-fold increase to be significant is based on the findings that: (i) changes of this magnitude have always been confirmed by cytofluorometric analysis when antibodies specific for the expanded Vβ families were available (21, 31), (ii) changes of this magnitude have always been found to be associated with the oligo-monoclonal nature of the expansions of the Vβ families in question (21, 31), and (iii) the TCR repertoire is very stable in the absence of antigenic stimulation. This latter point is supported by the observation that the TCR repertoire was consistently found to be identical in healthy HIV-negative homozygotic twins (29, 32, 33). It is obvious that these results would not be compatible with a high rate of spontaneous perturbations in the TCR repertoire.
Patterns of Vβ Perturbations.
Longitudinal analysis of the Vβ repertoire was performed on PBMC samples collected from 21 subjects during primary HIV infection and during and after the transition to the chronic phase. Three major patterns of Vβ perturbations were observed: (i) expansion of a single Vβ family (Type 1), (ii) expansion of two Vβ families (Type 2), and (iii) expansion of multiple Vβ families or no detectable expansions with polyclonal activation of multiple Vβ families (Type 3).
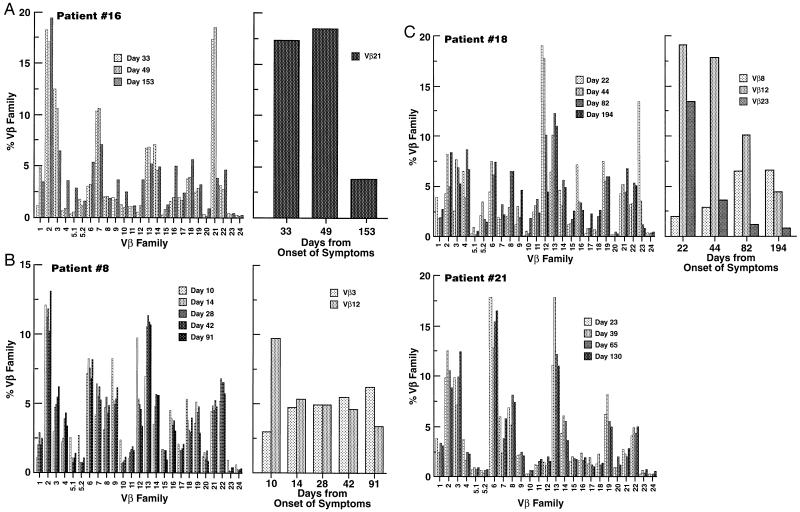
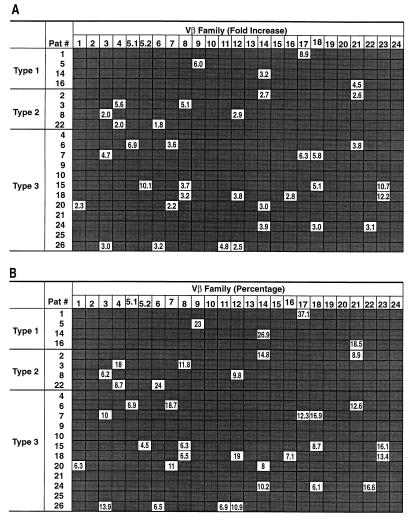
Representative examples of the above patterns are shown in Fig. 1. With regard to the distribution of the 21 patients into the 3 patterns of Vβ perturbations, 4 patients had a Type 1 pattern, 4 had a Type 2 pattern, whereas most patients (13 of 21) manifested a Type 3 pattern (Fig. 2). It is important to underscore that with regard to the criteria used for grouping the patients, the division was made strictly on the basis of the patterns of Vβ perturbations, which have been blindly analyzed, several months prior to the evaluation of the subsequent clinical outcome. The magnitude of the changes, i.e., fold increase or decline, in the relative percentage of the perturbed Vβ families observed over time were extremely variable among the different Vβs, and were not related to the type of Vβ perturbation observed (Fig. 2A). This was not surprising since there are substantial differences in the steady-state percentage of expression of the different Vβ families, and thus the number of fold increase or decline observed during an ongoing immune response can be, at least in part, dependent upon the initial steady-state level, and does not necessarily reflect the magnitude of the cell population that has been mobilized during the immune response. In addition, there were substantial differences in the percentage of the single Vβ families found perturbed in Type 1, Type 2, and Type 3 patterns (Fig. 2B). The percentage of the Vβ families found perturbed in the four patients with Type 1 pattern was higher (ranging between 18.5% and 37%) compared with that in Type 2 and Type 3 patterns (Fig. 2B). Despite the differences in the percentage of the different Vβ families among the three Types of Vβ perturbations (higher percentage of the perturbed Vβs in Type 1 versus Type 2 and Type 3), it is of note that if one totals the percentages of the different Vβs found perturbed in each patient, the overall percentage of the cell population potentially involved in the ongoing primary immune response to HIV infection generally ranged between 16% and 38% regardless of the type of Vβ perturbation observed (Fig. 2B). This is also the case in those patients (patients 4, 9, 10, 19, 21, and 25) in whom no significant Vβ perturbations were detected (Type 3); it has been consistently observed that, similar to those patients with significant Vβ perturbations, a large percentage (up to 50%) of CD8+ T cells expressed the HLA-DR activation marker (data not shown; refs. 21 and 31), which generally defines the activated cell population potentially involved in the ongoing immune response (34). In these patients, HLA-DR expression is distributed among different CD8+ Vβ cell subsets, whereas in patients with clear-cut Vβ expansions, HLA-DR antigen is preferentially expressed on the expanded Vβs (21, 31). Therefore, because multiple CD8+ Vβ cell subsets are activated even when Vβ perturbations were below 2-fold, patients showing these features were included in the Type 3 pattern.
Figure 1.
Analysis of the TCR repertoire during primary infection. The Vβ repertoire in freshly isolated unfractionated PBMC collected at different time points from the onset of symptoms was analyzed by a semi-quantitative PCR assay (21, 24). A minimum of a doubling in the relative expression of Vβ families among sequential time points was considered to be significant. (A) Vβ repertoire in patient 16, who is representative of the Type 1 pattern of Vβ perturbations. (B) Patient 8 is representative of Type 2 pattern. (C) Patients 18 (perturbations of multiple Vβs) and 21 (no detectable expansions) are representative of Type 3 pattern.
Figure 2.
Analysis of the Vβ repertoire in 21 individuals with primary HIV infection. Patients are grouped on the basis of the three patterns (Type 1, Type 2, and Type 3) of Vβ perturbations. The results are shown only for those Vβs that were found significantly perturbed (>2-fold) during the longitudinal analysis; the numerical values shown corresponded to those detected at the time point in which the greatest change in fold increase was observed. The shaded box indicates that no significant changes were observed. (A) Results are expressed as fold increase and/or decline. (B) Percentages of the individual Vβs for which the changes in fold increase and/or decline have been shown in A. With regard to Vβ6 in patient 22, the percentage was very high (24%) at day 43, and progressively declined to 14% at day 106. Samples at later time points were not available; for this reason, the changes in Vβ6 were considered significant even if they were <2-fold. With regard to the changes of Vβ17 in patient 7, and Vβ8 in patients 15 and 18, the increments in the percentage of these Vβs were observed at later time points when the percentages of the other Vβs that were found to be perturbed had already declined. The Vβ repertoire was analyzed by a semi-quantitative PCR assay (21, 24, 29).
Relationship Between Levels of Viremia During Primary Infections and Different Patterns of Vβ Perturbations.
It was of interest to determine whether the levels of viremia detected in the first sample of plasma collected during primary infection were significantly different among the three groups of HIV-infected subjects experiencing different patterns of Vβ perturbations. In fact, there were no significant differences in the levels of viremia detected during primary infection among the three groups of patients with Vβ perturbations (Type 1 versus Type 2, P = 0.53; Type 1 versus Type 3, P = 0.29; and Type 2 versus Type 3, P = 0.77) (Table 1). Similarly, in a study including 72 patients with primary HIV infection, no relationship has been found between the levels of viremia detected during the first 6 months after infection and disease progression (T.S. and L.C., personal communication).
Table 1.
Levels of plasma viremia and CD4+ T cell counts in HIV-infected individuals with different patterns of Vβ expansions
| Vβ type | Patient | Plasma viremia first time point*
|
CD4+ T cells
|
Plasma viremia last time point
|
||
|---|---|---|---|---|---|---|
| HIV RNA copies, 10−3/ml | HIV RNA copies, 10−3/ml | Day | ||||
| Cell count/μl | Day | |||||
| Type 1 | 1 | 216 | 68 | 398 | 55 | 391 |
| 5 | 21,783 | 128 | 385 | 631 | 301 | |
| 14 | 457 | 76 | 359 | ND | ND | |
| 16 | 389 | 134 | 384 | 35 | 273 | |
| Type 2 | 2 | 2,217 | 390 | 578 | 5 | 553 |
| 3 | 1,350 | 393 | 556 | 89 | 556 | |
| 8 | 13 | 608 | 365 | 74 | 387 | |
| 22 | 210 | 433 | 358 | 70 | 489 | |
| Type 3 | 4 | 939 | 1045 | 483 | 13 | 435 |
| 6 | 228 | 622 | 343 | 144 | 343 | |
| 7 | 387 | 356 | 280 | 17 | 174 | |
| 9 | 91 | 419 | 368 | 18 | 466 | |
| 10 | <10 | 596 | 278 | <10 | 278 | |
| 15 | 21,000 | 665 | 339 | 21 | 339 | |
| 18 | 553 | 382 | 495 | 24 | 426 | |
| 19 | 437 | 575 | 330 | <10 | 423 | |
| 20 | 439 | 867 | 307 | 14 | 373 | |
| 21 | 90 | 1052 | 352 | 93 | 271 | |
| 24 | 15 | 750 | 113 | ND | ND | |
| 25 | ND | 504 | 209 | ND | ND | |
| 26 | 565 | 638 | 375 | 31 | 495 | |
Relationship Between Patterns of Vβ Perturbations and Progression of HIV Disease.
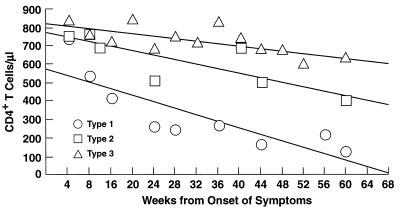
An important issue to investigate was the relationships among the three patterns of Vβ perturbations observed during primary infection and the rate of disease progression. In a preliminary analysis, CD4+ T cell counts determined approximately 1 year after primary infection were used as an indicator of the status of progression of HIV disease. The four HIV-infected subjects (patients 1, 5, 14, and 16) with a Type 1 pattern of Vβ perturbation had already progressed to AIDS 1 year after primary infection as indicated by CD4+ T cell counts below 200/μl (Table 1); the mean CD4+ T cell count in patients with Type 1 pattern was 101 ± 34 μl (Table 1). CD4+ T cell counts detected in patients with Type 2 pattern (patients 2, 3, 8, and 22) were significantly higher (456 ± 103 μl) than those found in patients with Type 1 pattern (Table 1). In 10 of 13 patients with Type 3 pattern, CD4+ T cell counts were above 500/μl, and the overall mean CD4+ T cell count in this group of patients was 651 ± 226 μl (Table 1). A more precise analysis of disease progression was performed by analyzing the slopes of decline of CD4+ T cells (Fig. 3). The values of CD4 T cell counts shown for each time point are the means of CD4 T cell counts detected in the patients (4 for type 1, 4 for type 2, and 13 for type 3) with different patterns of Vβ perturbations. The minimal estimates of CD4+ T cell loss per week obtained from this analysis were 8.76 cells for Type 1 pattern, 6.14 cells for Type 2, and 3.34 cells for Type 3. These slopes of decline of CD4+ T cells were significantly different among the three groups (Type 1 versus Type 2, P = 0.01; Type 1 versus Type 3, P = <0.0001; and Type 2 versus Type 3, P = 0.03) (Fig. 3). Therefore, these results indicate that the rate of disease progression was substantially different in HIV-infected individuals who had different patterns of Vβ perturbations during primary infection.
Figure 3.
Analyses of CD4+ T cell decline over time in patients with Type 1, Type 2, and Type 3 patterns of Vβ perturbations. Each slope was obtained from the best-fit line derived from linear regression. Each data point is generated by the mean of the CD4+ T cell counts detected during that time period in the different patients belonging to the three patterns of Vβ perturbations. From the slope, minimum estimates of CD4+ T cell loss per week were obtained.
Relationship Between Patterns of Vβ Perturbations and Levels of Viremia During Chronic Infection.
The patterns of Vβ perturbations were compared with the levels of viremia detected approximately 1 year after seroconversion. Levels of viremia at this time point were significantly higher in patients with Type 1 pattern compared with those with Type 3 pattern (Type 1 versus Type 3, P = 0.04); in addition, there was a trend toward a difference in levels of plasma viremia in Type 1 and 2 versus Type 3 that did not reach statistical significance (P = 0.09). These results were consistent with previous studies showing that the levels of viremia observed after 6 months following primary HIV infection and during chronic infection are a strong predictor of the rate of disease progression (11, 35) (T.S. and L.C., personal communication).
DISCUSSION
This study reveals that the primary immune response to HIV is qualitatively different among individuals. It is highly likely that both host and virologic factors contribute to the generation of this diversity. Among these factors, the HLA haplotype of the host and the T cell selection process during thymus ontogeny (36) likely contribute by regulating both the size and the fine specificity of the pool of virus-specific T cell clones that can be generated in response to infection. In addition, the intrinsic properties of certain regions of the viral genome allow them to code for immunodominant epitopes (37). Given the fact that these epitopes are the major targets of the immune response, it is likely that they play a major role in generating the specificity of the immune response.
Qualitative differences in the primary immune response to HIV are reflected in the degree of diversity of the CD8+ Vβ repertoire that is mobilized. Stimulation of the Vβ repertoire may be limited predominantly to a single Vβ family, which is a clear indication of the induction of an immune response associated with mobilization of a very restricted TCR repertoire (Type 1 pattern), or to two (Type 2 pattern) or multiple Vβ families (Type 3 pattern), which reflects the mobilization of an increasingly broader TCR repertoire. Furthermore, it is important to underscore that there was no relationship between the mobilization of a restricted versus a broader TCR repertoire and HIV-specific CTL activity detected during primary infection. In previous studies (38), HIV-specific CTL activity was detected early during primary infection in patient 1 (Type 1), patients 2 and 3 (Type 2), and patients 4, 6, and 15 (Type 3), and the detection of virus-specific CTL activity was clearly independent of the patterns of Vβ perturbations.
Of particular importance was the finding that these qualitative differences in the cell-mediated immune response observed during the initial weeks of HIV infection were associated with different rates of disease progression (i.e., rapid progression and precipitous loss of CD4+ T cells versus a clinically stable course and CD4+ T cell counts above 500/μl). An obvious question relates to the association between the mobilization of a broader TCR repertoire and stable clinical course versus the association between mobilization of a restricted repertoire and rapid progression of HIV disease. In separate studies (G.P. and A.S.F., unpublished observations), we have demonstrated that the CD8+ Vβ families that are largely expanded during primary infection are rapidly deleted, thus indicating that the virus-specific immune response may be rapidly exhausted in those individuals with Type 1 (i.e., restricted) compared with those with Type 3 (i.e., broader) patterns of Vβ perturbations. Similarly, escape from the immune response by virus mutations (39) is much more likely in individuals who mobilize a restricted TCR repertoire compared with those who respond to HIV infection with a broader TCR repertoire. The possibility that mobilization of a broader TCR repertoire may be associated with protective immunity has been recently suggested in the simian immunodeficiency virus model (40).
The observation of a relationship between the diversity of the primary immune response and the rate of disease progression is particularly remarkable, since at the time of primary infection the levels of viremia were not significantly different in the three groups of patients with qualitatively different Vβ perturbations. One can fashion a unifying theme that combines the immunological findings in this study with the virologic observations of others (refs. 11 and 35, T.S. and L.C., personal communication). In this regard, effective down-regulation of the initial burst of viremia occurs both in individuals with oligoclonal and in those with polyclonal T cell responses. As a result, during or shortly after primary HIV infection, the levels of viremia do not predict the subsequent clinical outcome. However, in these individuals, the restricted immune response will ultimately be ineffective in controlling virus replication resulting in an increase in levels of viremia and diminution of CD4+ T cell counts over time. After 6 months to 1 year, levels of viremia then become predictive of clinical outcomes as previously reported (refs. 11 and 35; T.S. and L.C., personal communication). Therefore, qualitative differences in the primary immune response to HIV and not the initial levels of viremia during this stage of infection are predictive of the rate of disease progression.
Taken together, these results provide evidence that the initial interaction between the virus and the immune system of the host is an important determining factor in the subsequent clinical outcome, and that immunologic factors operative during primary infection, as much as or more than virologic factors, are critical determinants of the ultimate progression of HIV disease.
Footnotes
Abbreviations: CTL, cytotoxic T lymphocyte; TCR, T cell receptor; PBMC, peripheral blood mononuclear cell.
References
- 1.Haynes B F, Pantaleo G, Fauci A S. Science. 1996;271:324–328. doi: 10.1126/science.271.5247.324. [DOI] [PubMed] [Google Scholar]
- 2.Buchbinder S P, Katz M H, Hessol N A, O’Malley P M, Holmberg S D. AIDS. 1994;8:1123–1128. doi: 10.1097/00002030-199408000-00014. [DOI] [PubMed] [Google Scholar]
- 3.Cao Y, Quin L, Zhang L, Safrit J, Ho D D. N Engl J Med. 1995;332:201–208. doi: 10.1056/NEJM199501263320401. [DOI] [PubMed] [Google Scholar]
- 4.Easterbrook P J. AIDS. 1994;8:1179–1182. doi: 10.1097/00002030-199408000-00023. [DOI] [PubMed] [Google Scholar]
- 5.Kirchhoff F, Greenough T C, Brettler D B, Sullivan J L, Desrosiers R C. N Engl J Med. 1995;332:228–232. doi: 10.1056/NEJM199501263320405. [DOI] [PubMed] [Google Scholar]
- 6.Levy J A. AIDS. 1993;7:1401–1410. doi: 10.1097/00002030-199311000-00001. [DOI] [PubMed] [Google Scholar]
- 7.Lifson A R, Buchbinder S P, Sheppard H W. J Infect Dis. 1991;163:959–965. doi: 10.1093/infdis/163.5.959. [DOI] [PubMed] [Google Scholar]
- 8.Pantaleo G, Menzo S, Vaccarezza M, Graziosi C, Cohen O J, Demarest J F, Montefiori D, Orenstein J M, Fox C, Schrager L J, Margolick J B, Buchbinder S, Giorgi J V, Fauci A S. N Engl J Med. 1995;332:209–216. doi: 10.1056/NEJM199501263320402. [DOI] [PubMed] [Google Scholar]
- 9.Schrager L K, Young J M, Fowler M G, Mathieson B J, Vermund S H. AIDS. 1994;8:S95–S108. [Google Scholar]
- 10.Sheppard H W, Lang W, Asher M S, Vittinghoff E, Winkelstein W. AIDS. 1993;7:1159–1166. [PubMed] [Google Scholar]
- 11.Mellors J W, Kingsley L A, Rinaldo C R, Todd J A, Hoo B S, Kokka R P, Gupta P. Ann Intern Med. 1995;122:573–579. doi: 10.7326/0003-4819-122-8-199504150-00003. [DOI] [PubMed] [Google Scholar]
- 12.Clark S J, Saag M S, Decker W D, Campbell-Hill S, Roberson J L, Veldkamp P J, Kappes J C, Hahn B H, Shaw G M. N Engl J Med. 1991;324:954–960. doi: 10.1056/NEJM199104043241404. [DOI] [PubMed] [Google Scholar]
- 13.Daar E S, Moudgil T, Meyer R D, Ho D D. N Engl J Med. 1991;324:961–964. doi: 10.1056/NEJM199104043241405. [DOI] [PubMed] [Google Scholar]
- 14.Koup R A, Safrit J T, Cao Y, Andres C A, McLeod G, Borkowsky W, Farthing C, Ho D D. J Virol. 1994;68:4650–4655. doi: 10.1128/jvi.68.7.4650-4655.1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Moore J P, Cao Y, Ho D D, Koup R A. J Virol. 1994;68:5142–5155. doi: 10.1128/jvi.68.8.5142-5155.1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Reimann K A, Tenner-Racz K, Racz P. J Virol. 1994;68:2362–2370. doi: 10.1128/jvi.68.4.2362-2370.1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Tindall B, Cooper D A. AIDS. 1991;5:1–14. [PubMed] [Google Scholar]
- 18.Graziosi C, Pantaleo G, Butini L, Demarest J F, Saag M S, Shaw G M, Fauci A S. Proc Natl Acad Sci USA. 1993;90:6505–6509. doi: 10.1073/pnas.90.14.6405. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Arden B, Clatk S P, Kabelitz D, Mak T W. Immunogenetics. 1995;42:455–500. doi: 10.1007/BF00172176. [DOI] [PubMed] [Google Scholar]
- 20.Davis M M, Bjorkman P J. Nature (London) 1988;334:395–402. doi: 10.1038/334395a0. [DOI] [PubMed] [Google Scholar]
- 21.Pantaleo G, Demarest J F, Soudeyns H, Graziosi C, Denis F, Adelsberger J W, Borrow P, Saag M S, Shaw G M, Sekaly R P, Fauci A S. Nature (London) 1994;370:463–467. doi: 10.1038/370463a0. [DOI] [PubMed] [Google Scholar]
- 22.Chen Z W, Kou Z C, Lekutis C, Zhou D, Halloran M, Li J, Sodroski J, Lee-Parritz D, Letvin N L. J Exp Med. 1995;182:21–31. doi: 10.1084/jem.182.1.21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Chomczynski P, Sacchi N. Anal Biochem. 1987;162:156–159. doi: 10.1006/abio.1987.9999. [DOI] [PubMed] [Google Scholar]
- 24.Labrecque N, McGrath H, Subramanyam M, Huber B T, Sekaly R P. J Exp Med. 1993;177:1735–1743. doi: 10.1084/jem.177.6.1735. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Piatak M, Saag M S, Yang L C, Clark S J, Kappes J C, Luk K C, Hahn B H, Shaw G M, Lifson J D. Science. 1993;259:1749–1754. doi: 10.1126/science.8096089. [DOI] [PubMed] [Google Scholar]
- 26.Bagnarelli P, Menzo S, Valenza A, Manzin A, Giacca M, Anearani F, Scalise G, Varaldo P E, Clementi M. J Virol. 1992;66:7328–7335. doi: 10.1128/jvi.66.12.7328-7335.1992. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Holodniy M, Katrenstein D, Israelski D, Merrigan T. J Clin Invest. 1991;88:1755–1759. doi: 10.1172/JCI115494. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Dewar R, Highbarger H, Sarmiento M, Todd J, Vasudevachari M, Davey R J, Kovacs J A, Salzman N P, Lane H C, Urdea M S. J Infect Dis. 1994;170:1172–1179. doi: 10.1093/infdis/170.5.1172. [DOI] [PubMed] [Google Scholar]
- 29.Rebai N, Pantaleo G, Demarest J F, Ciurli C, Soudeyns H, Adelsberger J W, Vaccarezza M, Walker R E, Sékaly R P, Fauci A S. Proc Natl Acad Sci USA. 1994;91:1529–1533. doi: 10.1073/pnas.91.4.1529. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Choi Y W, Kotzin B, Herron L, Callahan J, Marrack P, Kappler J. Proc Natl Acad Sci USA. 1989;86:8941–8945. doi: 10.1073/pnas.86.22.8941. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Pantaleo G, Fauci A S. Annu Rev Immunol. 1995;13:487–512. doi: 10.1146/annurev.iy.13.040195.002415. [DOI] [PubMed] [Google Scholar]
- 32.Gulwani-Akolkar B, Posnett D N, Janson C H, Grunewald J, Wigzell H, Akolkar P, Gregersen P K, Silver J. J Exp Med. 1991;174:1139–1146. doi: 10.1084/jem.174.5.1139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Hawes G E, Struyk L, van den Elsen P J. J Immunol. 1993;150:2033–2045. [PubMed] [Google Scholar]
- 34.Moretta A, Pantaleo G, Moretta L, Cerottini J C, Mingari M C. J Exp Med. 1983;157:743–754. doi: 10.1084/jem.157.2.743. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Mellors J W, Rinaldo C R, Gupta P, White R M, Todd J A, Kingsley L A. Science. 1996;272:1167–1170. doi: 10.1126/science.272.5265.1167. [DOI] [PubMed] [Google Scholar]
- 36.Von Boehmer H. Annu Rev Immunol. 1988;6:309–326. doi: 10.1146/annurev.iy.06.040188.001521. [DOI] [PubMed] [Google Scholar]
- 37.McMichael A J, Walker B D. AIDS. 1994;8:S155–S173. [Google Scholar]
- 38.Borrow P, Lewicki H, Hahn B H, Shaw G M, Oldstone M B. J Virol. 1994;68:6103–6110. doi: 10.1128/jvi.68.9.6103-6110.1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Phillips R E, Rowland-Jones S, Nixon D F, Gotch F M, Edwards J P, Ogunlesi A O, Elvin J G, Rothbard J A, Bangham C R M, Rizza C R, McMichael A J. Nature (London) 1991;354:453–459. doi: 10.1038/354453a0. [DOI] [PubMed] [Google Scholar]
- 40.Chen Z W, Shen L, Regan J D, Kou Z, Chim S H, Letvin N L. J Immunol. 1996;156:1469–1475. [PubMed] [Google Scholar]