Abstract
With improving neonatal survival for extremely premature babies, the challenge for neonatology is to improve outcome of surviving babies. This review concentrates on best evidence emerging in recent years on prevention of brain damage by early administration of drugs as well as avoidance of induced brain damage by hyperventilation and dexamethasone therapy given postnatally for chronic lung disease.
Studies in the modern era of neonatal intensive care (post‐1990) when antenatal steroids and postnatal surfactant became widely used have changed the outcome of very premature infants in two important ways. Firstly, it is well known to all that there has been a significant reduction in mortality in infants aged ⩽28 weeks. This has occurred in every developed country, and now results in the survival of over 50% of infants of 26 weeks' gestational age and 25% of infants of 24 weeks' gestational age.1 The fact that there is no evidence that the proportion of brain‐damaged babies has fallen over a similar period of time has been less well recognised and indeed a large study from some of the best centres in the United States showed no improvement in the outcome of babies born at <25 weeks' gestational age in 1996–9 compared with the same group born in 1993–6.2 These two statistics mean that more very premature babies than ever are surviving with disabilities.
We seem to be at or close to the limit of viability for severely preterm infants and further improvement in mortality cannot probably be made with current techniques. The challenge for neonatal intensive care is not to improve the numbers of babies surviving but to concentrate on producing a better quality of life for those who do survive. We must use research in our clinical practice to devise methods which will maximise cerebral function, and minimise harmful complications and side effects which result in the burden of disability. This paper is the result of my own understanding of recent research to answer the question—how can we protect the immature brain?
Drugs which may prevent early neonatal brain injury
Three drugs have been subjected to careful evaluation of their effect in preventing intraventricular haemorrhage (IVH) or periventricular leucomalacia (PVL) in premature infants.
Phenobarbitone
The first paper suggesting that phenobarbitone prevented IVH was published in 1981,3 but subsequent studies have not shown a similar effect. A Cochrane Library meta‐analysis4 concluded that the results of these studies when considered together show no effect of phenobarbitone in preventing IVH.
Etamsylate
Ethamsylate (now renamed etamsylate) was first shown in 1981 to reduce IVH in a group of premature babies,5 and recently a report on the outcome of survivors at the age of 3.5–4.2 years of a large multicentre trial6 has been published. There was no reduction in the rate of either cerebral palsy or intellectual impairment when the two groups were compared. There was a reduction in severe cognitive impairment in the etamsylate group, but more children in this group died and the improvement may have been due to fewer survivors. When death and significant impairment are used as a combined outcome measure, no differences are seen between the etamsylate and control groups.
Indomethacin
To date, 2872 infants have been enrolled in 19 randomised controlled trials (RCT) (including The Injury Prevention Program (TIPP),7 a single multicentre study enrolling over 1200 infants with very low birth weight). These studies have evaluated the role of indomethacin when given shortly after birth in preventing IVH and patent ductus arteriosus. A recent Cochrane Library meta‐analysis8 has shown that indomethacin significantly reduced the incidence of all grades of IVH (relative risk (RR) 0.88, confidence interval (CI) 0.80 to 0.98), the more severe grade 3 and 4 haemorrhage (RR 0.66, CI 0.53 to 0.82), and PVL or ischaemic changes (RR 0.44, CI 0.24 to 0.81). Although there were methodological problems with some studies, the very large TIPP study confirmed the protective effect of this drug on large haemorrhages.7
There are far fewer reports of neurodevelopmental outcome from these studies, but Schmidt et al9 described a follow‐up study of the surviving babies at 18 months from the TIPP cohort. They showed that early treatment with indomethacin does not improve the rate of babies surviving with disability at 18 months, despite the fact that there were considerably fewer babies who developed severe IVH or patent ductus arteriosis during the neonatal period. The meta‐analysis8 pooled outcome data from the TIPP trial and four others, and showed no reduction in the rate of adverse outcome in the indomethacin‐treated group.
These studies on drugs provide some interesting lessons for younger neonatologists. Firstly, the results from early intervention trials may be misleading and subsequent trials may not confirm early enthusiasm.
Secondly, markers of neurological disease such as large IVH may not predict which babies are at risk of disability later on, and there is no substitute for long‐term follow‐up studies of infants enrolled into randomised controlled trials.
Thirdly, the effects of drugs on immature organisms may be contradictory and unpredictable. It is interesting to speculate on why indomethacin noticeably reduces lesions of the periventricular white matter (haemorrhagic or ischaemic), yet this is not associated with improved outcome later on. Indomethacin may possibly induce cerebral ischaemia as a result of its prostaglandin inhibition, and the obvious beneficial effects may be negated by adverse effects elsewhere.
Recent research has confirmed that to date there is no safe and effective drug in preventing IVH/PVL in preterm infants, but caution is recommended in this conclusion. The story on these drugs may not yet be finished because reanalysis of the outcome data of a group of babies enrolled in an indomethacin intervention study has suggested that surviving males given indomethacin have significantly higher verbal test scores than males not exposed to this drug.10 There may be subgroups of babies who may show different response according to sex or genetic susceptibility.
Hypocapnia
The association between brain damage and neonatal hypocapnia was first documented in 1987 independently by Greisen11 (cerebral palsy) and Calvert12 (PVL diagnosed by ultrasound). Since then, at least a further 13 papers have documented a similar response. The frequency of these reports on a positive association between hypocapnia and neonatal brain injury does not, however, mean that there is a direct causal link, but the hypothesis must be carefully examined. The observational nature of these reports does not lend them to careful comparison because each study has used a different gestational age group of premature infants, varying duration for investigating the postnatal age when hypocapnia occurs and, most importantly, different cut‐off levels for defining hypocapnia.
The scientific review of effect is based on a hierarchy of evidence, with large RCT most likely to prove the association to the clinicians' satisfaction. Hypocapnia is not recommended as a treatment of choice for neonatal lung or brain disease, and an RCT comparing babies exposed to hypocapnia, with controls exposed to normocarbia or hypercarbia cannot be justified. Any responsible ethics committee would not probably give approval for such a study. Nevertheless, the importance of preventing hypocapnia if an association with brain damage is proved means that these data must be subjected to careful analysis. The following questions need to be asked:
What is the biological plausibility of this hypothesis?
How strong are the clinical associations reported?
Are there animal data to support the neurotoxic effect of hypocapnia?
What is the biological plausibility of this hypothesis?
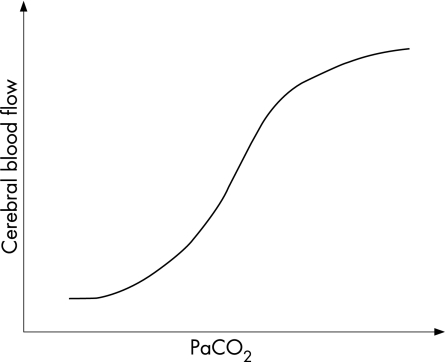
The normal PaCO2 (arterial carbon dioxide tension) level during the first week of life in premature babies is 4.4–4.8 kPa. It is well known that in the mature brain, changes in PaCO2 have a major effect on cerebral blood flow, with an S‐shaped relationship (fig 1). Hypocapnia causes severe vasoconstriction, thereby reducing cerebral blood flow, and this effect has also been shown in experimental neonatal animals and in human neonates. Can prolonged and intense vasoconstriction as the result of inadvertent hypocapnia lead to neonatal brain damage?
Figure 1 Graph showing the S‐shaped relationship between changes in arterial carbon dioxide tension (PaCO2) and cerebral blood flow.
How strong are the clinical associations reported?
Table 1 shows the 15 published reports on brain damage and hypocapnia. There is no consensus as to what is severe hypocapnia and this varies from PaCO2 <4.67 kPa to PaCO2 <2 kPa. Some studies have attempted to measure either the severity or the duration of hypocapnia by calculating an area under the curve value14,16 or by correcting hypocapnia for completed weeks of gestation and using a z score for comparison.15 In general, studies reporting abnormalities on cerebral ultrasound (“PVL”, a combination of severe IVH and PVL, periventricular echodensity, or cavitating “cystic” PVL) have described a lower threshold for PaCO2; in five of the seven studies the value was ⩽3.33 kPa on any occasion. One of these studies showed only the association between severe hypocapnia and PVL detected by imaging on the third day of life, and this association did not reach statistical significance on days 1 and 2.16
Table 1 Ultrasound abnormality of the white matter.
| Ref | Duration of HyC | Severity of HyC | Diagnosis |
|---|---|---|---|
| Calvert (1987)12 | ⩽3 days | <3.3 kPa | PVL |
| Fujimoto (1994)13 | ⩽28 days | <2.67 kPa | cPVL |
| Wiswell (1996)14 | ⩽3 days | <3.3 kPa (AUC) | PVE |
| Dammann (2001)15 | <24 h | z score (<4 kPa) | Echolucency |
| Okumura (2001)16 | ⩽3 days | <3.33 kPa (AUC) | |
| Erickson (2002)17 | ⩽48 h | <4 kPa | Large IVH and PVL |
| Giannokapalou (2004)18 | ⩽3 days | <3.33 kPa | cPVL |
| Resch (2004)19 | Any time | <4 kPa | cPVL and CP |
| Diagnosis of CP | |||
| Greisen (1987)11 | <24 h | <2 kPa | CP |
| Graziani (1992)20 | ⩽3 days | ⩽2.67 kPa | CP |
| Ikonen (1992)21 | ⩽3 days | ⩽4 kPa | “Handicap” |
| Salokorpi (1999)22 | <3 weeks | <3 kPa (two readings) Non‐significant trend to CP | |
| Collins (2001)23 | ⩽8 days | <4.67 kPa | CP |
| Neuropathology at autopsy | |||
| Hashimoto (1991)24 | <2.7 kPa | Ponto‐subicular necrosis | |
| Iida (1992)25 | Not specified | Multicystic encephalomalacia | |
AUC, area under the curve; CP, cerebral palsy; cPVL, cystic periventricular leucomalacia; HyC, hypocapnia; IVH, intraventricular haemorrhage; PVE, periventricular echolucency; PVL, periventricular leucomalacia.
Cases of hypocapnia published to April 2006.
Two neuropathological studies showed that babies with either multicystic encephalomalacia25 or pontosubicular necrosis24 had lower levels of PaCO2 in life than other dead infants without these ischaemic brain changes. In groups of surviving infants who developed subsequent cerebral palsy, there was a strong association with varying degrees of hypocapnia in all six studies.
Three studies performed multivariate analysis of a variety of perinatal factors strongly associated with perinatal brain damage. All showed a persistent effect on hypocapnia once other confounding factors had been considered, although in one study the effects of hypocapnia seemed to remain only when other causes for echolucency were not present.15 Another study found that coexistent hyperoxia could not be separated from the effects of hypocapnia,23 an observation also found in the only paper showing a significant relationship between hypocapnia and adverse outcome in full‐term infants after intrapartum asphyxia.26 The third study showed a link between hypocapnia and concurrent hyperbilirubinaemia.21 One study just examined twins (one of whom developed cystic periventricular leucomalacia and the other did not) in whom some risk factors might be better matched and found that the only risk factor for cystic periventricular leucomalacia was hypocapnia <4 kPa.19
In summary, the series of associations between hypocapnia and brain damage is compelling, but this association cannot be considered to be a causative one from these data alone. It is well recognised that relatively severe hypocapnia can occur in spontaneously breathing babies or those on continuous positive airway pressure. Okamura16 found that on day 3, spontaneously breathing babies with PVL had hypocapnia, with a higher respiratory rate than those who had not developed PVL. They suggest that perinatal brain damage leading to the diagnosis of PVL may cause hyperventilation in these babies, thereby maintaining a lower PaCO2 even after extubation.
Are there data on animals to support the neurotoxic effect of hypocapnia?
Research has shown that in neonatal piglets, mechanical ventilation in a group maintained hypocapnic (PaCO2 2.67 kPa) for only 1 h developed reduced brain energy levels and higher rate of cerebral cortex cellular disruption compared with a normocarbic group (PaCO2 5.3 kPa).27 A recent study on human neonates showed increased cerebral fractional oxygen extraction and a slower electroencephalogram signal on day 1 in relatively hypocapnic infants, and a higher serum lactate level which is consistent with a reduction of cerebral blood flow induced by lower values of PaCO2.28
Implications for clinical practice
Some babies are particularly sensitive to changing lung compliance and consequent hypocapnia. In particular, transfer from delivery suite to the neonatal unit has been shown to be associated with both hypocapnia and hyperoxia as a result of unpredictable lung performance in mechanically ventilated infants.28a In my own experience, hypocapnia may occur rapidly with changing lung compliance after artificial surfactant administration if blood gas measurements are not made frequently. Another risk group is babies with chronic lung disease with a high compensatory PaCO2 but whose PaCO2 drops rapidly when they require reventilation. As they have probably reset their cerebral arteriolar tone as a result of prolonged hypercapnia, a rapid fall in PaCO2 to normal levels may cause considerable cerebral underperfusion.
It is still not known for how long a baby remains hypocapnic before brain injury occurs, but from our understanding of the physiology it is likely to be a time‐related effect. The longer the duration of hypocapnia and the more marked its effect on vasoconstriction, the more ischaemic the brain will become. How long the brain can maintain cellular viability probably depends on many factors, most of which we do not yet understand.
We may not probably be able to prove to a scientific level of satisfaction whether hypocapnia causes brain damage, but the evidence from the 15 studies reviewed above does provoke anxiety, and the experimental results support the concept of a causative relationship with neonatal brain damage. In light of available evidence and the lack of any advantage being suggested for hypocapnia, my interpretation of the literature as it stands is to recommend strongly to avoid hypocapnia which arises as a result of inadequate monitoring of the effects of mechanical ventilation.
Postnatal dexamethasone
In 2001, an overview was published by Barrington29 reviewing the results of follow‐up studies in babies enrolled into RCT of corticosteroids to treat chronic lung disease. He showed that the risk of cerebral palsy among surviving followed‐up infants was doubled compared with control infants (RR 2.02, CI 1.51 to 2.71). He concluded that “the single most effective intervention which could currently be introduced for improving neuro‐developmental outcomes of extremely low birth weight infants would be to immediately abandon the use of postnatal steroids for chronic lung disease”. In the following year, the American Academy of Pediatrics and the Canadian Paediatric Society30 extended Barrington's meta‐analysis and identified three additional trials. This North American group made a number of recommendations including the following:
Postnatal use of systemic dexamethasone for the prevention or treatment of chronic lung disease (CLD) should be limited to carefully designed randomised double‐masked controlled trials.
Outside the context of a randomised, controlled trial, the use of corticosteroids should be limited to exceptional clinical circumstances (eg, an infant on maximal ventilatory and oxygen support).
A similar European guideline by Halliday31 recommended that “neonatal steroids should be avoided if at all possible”, although allowing that “steroids might be indicated for very ill ventilator‐dependent infants” and parental consent should be obtained before their use.
Although postnatal steroids are still used in Britain, these reports swung the pendulum towards extreme caution and, if the recommendations are accepted, to reserve the use of dexamethasone to a very few, very sick infants. Has research since 2001 caused the pendulum to move back towards more liberal use?
Over 35 blinded studies on postnatal steroids in the treatment of neonatal lung disease have been published since 1972 and have been subjected to a number of meta‐analyses. Unfortunately, interpretation of these studies is confused by three important confounders which have been well acknowledged by the authors of these reviews. They are:
Variation in postnatal timing of the exposure to the steroids
Contamination of studies by use of open‐label corticosteroid administered to babies in the studies for clinical indications
Variability in dosage and duration of treatment
Variation of timing
Halliday et al32,33,34 have published three Cochrane reviews on the effects of postnatal corticosteroids depending on the timing of exposure to the drug. In all, 21 studies32 were identified where babies were randomised within 96 h of birth. Although there were significant benefits as regards earlier extubation and decreased risk of chronic lung disease, there was also a statistically increased risk of cerebral palsy (RR 1.69, CI 1.20 to 2.38) and abnormal neurological examination (RR 1.81, CI 1.33 to 2.47) in the nine studies that reported follow‐up findings in the group of early treated infants.
Halliday et al33,34 performed a similar rigorous analysis of studies where corticosteroids were administered to babies at either 7–14 days or >3 weeks after birth. Clearly, the later the at‐risk group is identified, the fewer are the babies considered to require steroids for chronic lung disease (CLD). Seven studies enrolled 669 babies at 7–14 days and showed that the babies given corticosteroids had a reduced mortality at 28 days and less CLD at 28 days or at 36 post‐menstrual weeks.33 The nine trials of babies enrolled at >3 weeks showed no reduction in mortality, but there was a reduction in oxygen requirement at the post‐menstrual age of 36 weeks.34 There were limited follow‐up data from both age groups, but neither Cochrane review found a difference in the number of babies with cerebral palsy, neurodevelopmental disability or babies in the worst outcome group (death or cerebral palsy in survivors), when treatment was compared with controls.
Contamination by open‐label steroids
One meta‐analysis has considered the issue of contamination in studies on postnatal corticosteroids.35 In only two studies (randomising 154 infants) was there no contamination with open‐label steroids and in nine studies the contamination rate was <35%. On review of these studies, there was no significant reduction in mortality (relative difference (RD) −0.01, CI −0.08 to 0.06), but an increase in cerebral palsy (RD 0.09, CI 0.04 to 0.14) and combined death or cerebral palsy (RD 0.08, CI 0.01 to 0.16) was reported. A subgroup analysis of postnatal age at the time of exposure to steroids and low contamination rates was not possible owing to small numbers of infants randomised.
Variation in dosage
A review of 20 studies35 reported the range of cumulative dose in dexamethasone equivalent to be 0.4–8.0 mg/kg, a 20‐fold difference. Owing to the wide variation in dosage, no studies have attempted to assess the risk of disability with dosage equivalent. Recent studies have suggested that low‐dose dexamethasone has as beneficial an effect on weaning from the ventilator as placebo,36 although no follow‐up data are currently available.
Doyle et al35 explored the risk benefit of postnatal corticosteroid treatment on death or cerebral palsy dependent on the background risk of CLD, based on its incidence in the control group of babies. They showed that there was an increasingly favourable outcome as the background rate of CLD increased. The risk of death or cerebral palsy in infants treated with corticosteroids outweighed good outcome when the background risk of CLD was <50%. Thus, corticosteroids can be best justified in cases where the risk of CLD was highest.
In summary, early meta‐analyses seemed to be overly pessimistic in reporting the adverse long‐term effects of postnatal corticosteroids on the risk of cerebral palsy in surviving infants. More recent reviews support the increased risk of cerebral palsy when given early (⩽96 h), but not when given later. There is an association in reducing mortality when corticosteroids are given 7–14 days after birth, and a strong benefit in extubating babies when used after 2 weeks of age, without increasing the risk of death or disability. The greatest benefit seems to be when used in ventilator‐dependent babies who have a >50% background risk of CLD. In general, the lowest dose commensurate with benefit should be given for the shortest period of time.
Postnatal corticosteroid is a potentially neurotoxic drug when given in high dose or when used in the first 96 h of life. The mechanism by which it causes cerebral palsy is unknown, but may increase the risk of PVL. There is a strong association between CLD and adverse neurodevelopmental outcome. Corticosteroids given after birth reduce the incidence of CLD and therefore may improve the outcome. Early use exposes babies at lower risk of CLD to the potentially toxic effects of this group of drugs. Exposure in and after the second week of life does not seem to increase the risk of cerebral palsy or disability, but certainly has no protective effect on the brain. This group of drugs benefit lung function, allowing earlier extubation, and this may be an important indication for its use. In summary, postnatal corticosteroids may be indicated after 1 week of life in ventilator‐dependent babies in high oxygen concentration. Treatment of known risk factors such as infection, gastro‐oesophageal reflux and patent ductus arteriosis should precede steroid administration.
Summary
The dictum of primum non nocere is particularly relevant in neonatal medicine. There is little recent evidence that we can actively reduce brain damage to improve neurodevelopmental outcome in very immature babies, but the avoidance of risk factors such as hypocapnia and early exposure to postnatal corticosteroids is important in protecting the brain. After 1 week of life, corticosteroids do not seem to increase the risk of death or cerebral palsy and may be beneficial in reducing CLD‐associated neurodevelopmental abnormalities.
Abbreviations
CLD - chronic lung disease
IVH - intraventricular haemorrhage
PaCO2 - arterial carbon dioxide tension
PVL - periventricular leucomalacia
RCT - randomised controlled trial
TIPP - The Injury Prevention Program
Footnotes
Competing interests: None declared.
References
- 1.Levene M. Is intensive care for very immature babies justified? Acta Paediatr 200493149–152. [DOI] [PubMed] [Google Scholar]
- 2.Hintz S R, Kendrick D E, Vohr B R.et al Changes in neurodevelopmental outcomes at 18 to 22 months' corrected age among infants of less than 25 weeks' gestational age born in 1993–1999. Pediatrics 20051151645–1651. [DOI] [PubMed] [Google Scholar]
- 3.Donn S M, Roloff D W, Goldstein G W. Prevention of intraventricular haemorrhage in preterm infants by phenobarbitone: a controlled trial. Lancet 1981ii215–217. [DOI] [PubMed] [Google Scholar]
- 4.Whitelaw A. Postnatal phenobarbitone for the prevention of intraventricular haemorrhage in preterm infants [review]. Cochrane Library, Issue 1. Oxford: Update Software, 2006 [DOI] [PubMed]
- 5.Morgan M E I, Benson J W T, Cooke R W I. Ethamsylate reduces the incidence of periventricular haemorrhage in very low birth weight babies. Lancet 1981ii830–831. [DOI] [PubMed] [Google Scholar]
- 6.Schulte J, Osborne J, Benson J W T. Developmental outcome of the use of etamsylate for prevention of periventricular haemorrhage in a randomised controlled trial. Arch Dis Child Fetal Neonatal Ed 200590F31–F35. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Schmidt B, Davis P, Moddemann D.et al Long‐term effects of indomethacin prophylaxis in extremely‐low‐birth‐weight infants. New Engl J Med 20013441966–1972. [DOI] [PubMed] [Google Scholar]
- 8.Fowlie P W, Davis P G. Prophylactic intravenous indomethacin for preventing mortality and morbidity in preterm infants. Cochrane Library, Issue 1. Oxford: Update Software, 2006
- 9.Schmidt B, Davis P, Moddemann D. Long‐term effects of indomethacin prophylaxis in extremely‐low‐birth‐weight infants. N Engl J Med 20013441966–1972. [DOI] [PubMed] [Google Scholar]
- 10.Ment L R, Vohr B R, Makuch R W.et al Prevention of intraventricular hemorrhage by indomethacin in male preterm infants. J Pediatr 2004145832–834. [DOI] [PubMed] [Google Scholar]
- 11.Greisen G, Munck H, Lou H. Severe hypocarbia in preterm infants and neurodevelopmental deficit. Acta Paediatr Scand 198776401–404. [DOI] [PubMed] [Google Scholar]
- 12.Calvert S A, Hoskins E M, Fong K W.et al Etiological factors associated with the development of periventricular leukomalacia. Acta Paediatr Scand 198776254–259. [DOI] [PubMed] [Google Scholar]
- 13.Fujimoto S, Togari H, Yamaguchi N.et al Hypocarbia and cystic periventricular leukomalacia in premature infants. Arch Dis Child Fetal Neonatal Ed 199471F107–F110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Wiswell T, Graziani L J, Kornhauser M S.et al Effects of hypocarbia on the development of cystic periventricular leukomalacia in premature infants treated with high‐frequency jet ventilation. Pediatrics 199698918–924. [PubMed] [Google Scholar]
- 15.Dammann O, Allred E, Kuban K.et al Hypocarbia during the first 24 postnatal hours and white matter echolucencies in newborns ⩽28 weeks gestation. Pediatr Res 200149388–393. [DOI] [PubMed] [Google Scholar]
- 16.Okumura A, Hayakawa F, Kato T.et al Hypocarbia in preterm infants with periventricular leukomalacia: the relation between hypocarbia and mechanical ventilation. Pediatrics 2001107469–475. [DOI] [PubMed] [Google Scholar]
- 17.Erickson S J, Grauaug A, Gurrin L.et al Hypocarbia in the ventilated preterm infant and its effect on intraventricular haemorrhage and bronchopulmonary dysplasia. J Paediatr Child Health 200238560–562. [DOI] [PubMed] [Google Scholar]
- 18.Giannakopoulou C, Korakaki E, Manoura A.et al Significance of hypocarbia in the development of periventricular leukomalacia in preterm infants. Pediatr Int 200446268–273. [DOI] [PubMed] [Google Scholar]
- 19.Resch B, Jammernegg A, Vollaard E.et al Preterm twin gestation and cystic periventricular leucomalacia. Arch Dis Child Fetal Neonatal Ed 200489F315–F320. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Graziani L J, Spitzer A R, Mitchell D G.et al Mechanical ventilation in preterm infants: neurosonographic and developmental studies. Pediatrics 199290515–522. [PubMed] [Google Scholar]
- 21.Ikonen R S, Janas M O, Koivikko M J.et al Hyperbilirubinemia, hypocarbia and periventricular leukomalacia in preterm infants: relationship to cerebral palsy. Acta Paediatr 199281802–807. [DOI] [PubMed] [Google Scholar]
- 22.Salokorpi T, Rajantie I, Viitala J.et al Does perinatal hypocarbia play a role in the pathogenesis of cerebral palsy? Acta Paediatr 199988571–575. [DOI] [PubMed] [Google Scholar]
- 23.Collins M P, Lorenz J M, Jetton J R.et al Hypocapnia and other ventilation‐related risk factors of cerebral palsy in low birth weight infants. Pediatr Res 200150712–719. [DOI] [PubMed] [Google Scholar]
- 24.Hashimoto K, Takeuchi Y, Takashima S. Hypocarbia as a pathogenic factor in pontosubicular necrosis. Brain Dev 199113155–157. [DOI] [PubMed] [Google Scholar]
- 25.Iida K, Takashima S, Takeuchi Y. Etiologies and distribution of neonatal leukomalacia. Pediatr Neurol 19928205–209. [DOI] [PubMed] [Google Scholar]
- 26.Klinger G, Beyene J, Shah P.et al Do hyperoxaemia and hypocapnia add to the risk of brain injury after intrapartum asphyxia? Arch Dis Child Fetal Neonatal Ed 200590F49–F52. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Fritz K I, Ashraf Q M, Mishra O P.et al Effect of moderate hypocapnic ventilation on nuclear DNA fragmentation and energy metabolism in the cerebral cortex of newborn piglets. Pediatr Res 200150586–589. [DOI] [PubMed] [Google Scholar]
- 28.Victor S, Appleton R E, Beirne M.et al Effect of carbon dioxide on background cerebral electrical activity and fractional oxygen extraction in very low birth weight infants just after birth. Pediatr Res 200558579–585. [DOI] [PubMed] [Google Scholar]
- 28a.Tracy M, Downe L, Holberton J. How safe is intermittent positive pressure ventilation in preterm babies ventilated from delivery to newborn intensive care unit? Arch Dis Child Fetal Neonatal Ed 200489F84–F87. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Barrington K J. The adverse neuro‐developmental effects of postnatal steroids in the preterm infant: a systematic review of RCTs. BMC Pediatr 200111. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.American Academy of Pediatrics, Canadian Paediatric Society, Fetus and Newborn committee Postnatal corticosteroids to treat or prevent chronic lung disease in preterm infants. Pediatrics 2002109330–338. [DOI] [PubMed] [Google Scholar]
- 31.Halliday H L. Guidelines on neonatal steroids. Prenatal Neonatal Med 20016371–373. [Google Scholar]
- 32.Halliday H L, Ehrenkranz R A, Doyle L W. Early postnatal (<96 hours) for preventing chronic lung disease in preterm infants [review]. Cochrane Library, Issue 1. Oxford: Update Software, 2006
- 33.Halliday H L, Ehrenkranz R A, Doyle L W. Moderately early (7–14 days) postnatal corticosteroids for preventing chronic lung disease in preterm infants [review]. Cochrane Library, Issue 1. Oxford: Update Software, 2006
- 34.Halliday H L, Ehrenkranz R A, Doyle L W. Delayed (>3 weeks) postnatal corticosteroids for chronic lung disease in preterm infants [review]. Cochrane Library, Issue 1. Oxford: Update Software, 2006
- 35.Doyle L W, Halliday H L, Ehrenkranz R A. Impact of postnatal systemic corticosteroids on mortality and cerebral palsy in preterm infants: effect modification by risk for chronic lung disease. Pediatrics 2005115655–661. [DOI] [PubMed] [Google Scholar]
- 36.Doyle L W, Davis P G, Morley C J.et al Low dose dexamethasone facilitates extubation among chronically ventilator‐dependent infants: a multicenter, international, randomised, controlled trial. Pediatrics 200611775–83. [DOI] [PubMed] [Google Scholar]