Abstract
Currently used vaccines protect mainly through the production of neutralizing antibodies. However, antibodies confer little or no protection for a majority of chronic viral infections that require active involvement of cytotoxic T lymphocytes (CTLs). Virus-like particles (VLPs) have been shown to be efficient inducers of cell-mediated immune responses, but administration of an adjuvant is generally required. We recently reported the generation of a novel VLP system exploiting the self-assembly property of the papaya mosaic virus (PapMV) coat protein. We show here that uptake of PapMV-like particles by murine splenic dendritic cells (DCs) in vivo leads to their maturation, suggesting that they possess intrinsic adjuvant-like properties. DCs pulsed with PapMV-like particles displaying the lymphocytic choriomeningitis virus (LCMV) p33 immunodominant CTL epitope (PapMV-p33) efficiently process and cross-present the viral epitope to p33-specific transgenic T cells. Importantly, the CTL epitope is also properly processed and presented in vivo, since immunization of p33-specific T-cell receptor transgenic mice with PapMV-p33 induces the activation of large numbers of specific CTLs. C57BL/6 mice immunized with PapMV-p33 VLPs in the absence of adjuvant develop p33-specific effector CTLs that rapidly expand following LCMV challenge and protect vaccinated mice against LCMV infection in a dose-dependent manner. These results demonstrate the efficiency of this novel plant virus-based vaccination platform in inducing DC maturation leading to protective CTL responses.
For the past 200 years, vaccines have been used widely to prevent infections. Since the development of the first vaccine against smallpox by Jenner, multiple vaccination strategies have been tested in animals and humans, with each of them showing variable levels of efficacy (13). However, the emergence of new infectious diseases and an incapacity to provide current vaccines to developing countries at low cost have prompted the development of novel vaccination strategies.
One of the major drawbacks of most currently available vaccines is their failure to induce cellular immunity against given antigens. Most vaccines promote the production of neutralizing antibodies that offer protection against acute viral infections (24, 47). In the context of chronic infections (e.g., hepatitis C virus and human immunodeficiency virus [HIV] infections), neutralizing antibodies are potent in controlling free viral particles but are usually inefficient at eliminating infected cells (4, 9, 19). Recognition and destruction of infected cells by specific cytotoxic T lymphocytes (CTLs) are essential for carrying out an effective battle against such viruses. Professional antigen-presenting cells (APCs) are key players in triggering adaptive immunity. In particular, dendritic cells (DCs) play a pivotal role in priming cellular immune responses (16, 36). To become strong inducers of immunity, DCs acquire a mature phenotype through diverse stimuli that induce a series of morphological and functional changes (20). These modifications include migration to lymphoid organs, production of cytokines and chemoattractant molecules, and enhanced expression of essential cosignaling molecules, such as CD86, CD80, and CD40, which allows the establishment of key interactions between DCs and T cells. In addition to the classical major histocompatibility complex class I (MHC-I) and MHC-II antigen presentation pathways, DCs were shown to be particularly potent in presenting exogenous antigens on MHC-I molecules through a process known as cross-presentation (10). To date, the in vivo importance of cross-presentation is still under debate, but recent studies have shown that this process probably plays a crucial role in driving T-cell responses to exogenous antigens and to pathogens that do not infect DCs (29). Therefore, due to the efficacy of DCs in inducing cellular immunity, new vaccination strategies should aim at targeting and activating these professional APCs to promote the development and maintenance of potent CTL responses.
Recently, virus-like particles (VLPs) have received much attention for their potential for vaccine development. VLPs mimic the structure of viral particles without containing infectious genetic material, making them safe alternatives to conventional live or attenuated vaccines (23). A number of different VLPs were shown to be highly immunogenic antigen carriers capable of inducing humoral immune responses. For example, VLPs expressing proteins from influenza virus, papillomavirus, and rotavirus all induce high titers of neutralizing or protective antibodies (25, 28, 35). Some VLPs were also shown to induce CTL responses. Recombinant parvovirus-like particles expressing an epitope from the nucleoprotein of lymphocytic choriomeningitis virus (LCMV) induce protective CTL responses (33). Hepatitis B virus surface antigen VLPs expressing both respiratory syncytial virus and human papillomavirus CTL epitopes elicit simultaneous responses to both pathogens (42). However, many VLPs require the coadministration of adjuvant-like molecules (i.e., CpGs or anti-CD40 antibodies) for the induction of strong CTL immunity (18, 27, 37, 44). In recent years, the use of plant virus-derived VLPs as novel systems for the expression of foreign epitopes and for the development of new vaccines has triggered much interest. By genetically modifying these viruses, immunogenic peptides can be fused efficiently to the coat protein (CP) and exposed on the surfaces of the assembled plant VLPs. To date, cowpea mosaic virus, tobacco mosaic virus, alfalfa mosaic virus, potato virus C, tomato bushy stunt virus, zucchini yellow mosaic virus, and plum pox virus are all examples of plant viruses that have been produced successfully and used for the presentation of murine and human epitopes (6, 7, 22).
We recently described the generation of a VLP system based on the papaya mosaic virus (PapMV) (39). PapMV, a member of the potexvirus family, displays a flexible rod-like structure composed of 1,400 subunits of the viral CP assembled around a positive-strand RNA (8, 34, 39, 46). PapMV VLPs, formed by the self-assembly of the CP after overexpression in Escherichia coli (39), can carry foreign epitopes and induce the production of specific antibodies in vaccinated mice (7). Moreover, we have recently shown that a human B-cell line can cross-present CTL epitopes displayed on PapMV VLPs to specific T cells in vitro in a proteasome-independent fashion (14). To determine whether such VLPs could also trigger the development of protective cellular immunity in vivo, PapMV VLPs carrying the H-2b-restricted dominant p33 CTL epitope from LCMV (PapMV-p33 VLPs) were engineered and evaluated for the capacity to induce CTL responses against LCMV. We show here that vaccination with PapMV-p33 VLPs induces DC maturation and cross-presentation of the p33 CTL epitope in vivo, resulting in the induction of protective cell-mediated antiviral immunity.
MATERIALS AND METHODS
Mice.
Female 6- to 10-week-old C57BL/6 mice were purchased from Charles River (Saint-Constant, Canada). P14 T-cell receptor (TCR) transgenic mice were obtained from P. Ohashi (Princess Margaret Hospital, Toronto, Canada). P14 mice express a transgenic Vα2 and Vβ8.1 TCR specific for the p33 CTL epitope from the LCMV surface glycoprotein. Seventy to 90% of their CD8+ T cells are p33 specific. All animal experiments were reviewed and approved by the INRS-IAF Animal Care and Use Committee.
Cells, virus, and peptides.
LCMV WE was obtained from R. M. Zinkernagel (Institute of Experimental Immunology, Zurich, Switzerland). The p33 synthetic peptide KAVYNFATM, corresponding to an H-2b-restricted CTL epitope from the LCMV surface glycoprotein, was synthesized by Sigma-Genosys (Oakville, Ontario). EL-4 thymoma cells (H-2b) were grown in minimum essential medium (MEM; Invitrogen Life Technologies, Burlington, Ontario) containing 10% heat-inactivated fetal bovine serum (FBS; Invitrogen). MC57G fibroblasts were cultured in MEM containing 5% heat-inactivated FBS.
Cloning of recombinant PapMV-p33 construct.
The PapMV CP gene was cloned into the pET-3d-derived CPDN5 vector as previously described (39). The recombinant protein PapMV-p33 was derived from the PapMV CP construct fused to the p33 peptide (PapMV-p33) (Fig. 1A). To fuse the p33 peptide at the C terminus of CPΔN5, the oligonucleotides 5′-CTAGTGGTGGCGGTCTGTTGCTGAAAGCGGTGTATAACTTTGCGACCATGA-3′ and 5′-CGCGTCATGGTCGCAAAGTTATACACCGCTTTCAGCAACAGACCGCCACCA-3′ were annealed in 10 mM Tris, pH 8, and 50 mM NaCl and used directly for cloning into a plasmid containing the PapMV CP gene linearized with the SpeI-MluI restriction enzymes. The p33 peptide was flanked by three leucine and three glycine residues at its N terminus and by two threonine and one arginine residue at the C terminus. The insertion was positioned between the C terminus of PapMV CP and a six-His tag.
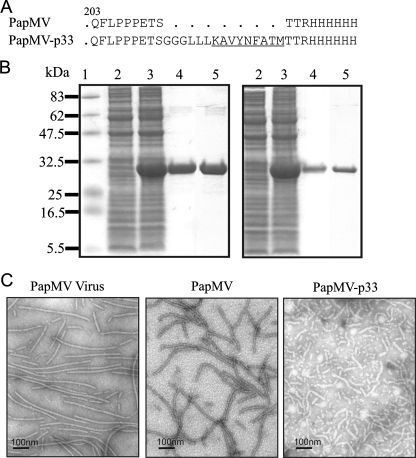
FIG. 1.
Expression and purification of PapMV-like particles. (A) The LCMV immunodominant p33 peptide (underlined) was fused between PapMV CP and a six-His tag located at the C terminus of the protein. (B) Purification of recombinant proteins. The size and purity of the recombinant proteins were confirmed by sodium dodecyl sulfate-polyacrylamide gel electrophoresis. Lanes: 1, molecular weight markers; 2, total bacterial lysates without plasmid; 3, total bacterial lysates expressing the recombinant protein; 4, proteins purified by nickel-affinity chromatography; 5, purified VLPs concentrated by ultracentrifugation. (C) Electron microscopy of PapMV native virions, PapMV VLPs, and PapMV-p33 VLPs. Bars, 100 nm.
Expression and purification of recombinant proteins from E. coli.
The E. coli expression strain BL21(DE3) RIL (Stratagene, La Jolla, CA) was transformed with the pET-3d plasmid containing the constructs of interest and maintained in 2× YT medium containing ampicillin (50 μg/ml). Recombinant proteins were purified by affinity chromatography on a nickel-Sepharose column as previously described (39). Two additional washing steps were done sequentially, using buffer A (10 mM Tris-HCl, 50 mM imidazole, 0.5% Triton X-100, pH 8) and then buffer B (10 mM Tris-HCl, 50 mM imidazole, 1% Zwittergent, pH 8) to remove endotoxin contamination. Protein purity was determined by sodium dodecyl sulfate-polyacrylamide gel electrophoresis and confirmed by immunoblot analysis using rabbit polyclonal antibodies specific to PapMV. Lipopolysaccharide (LPS) levels were determined by Limulus amebocyte lysate assay according to the manufacturer's instructions (Cambrex Bio Science, Walkersville, MD) and were always under 0.005 endotoxin unit/μg of protein.
Electron microscopy.
VLPs were diluted in 10 mM Tris-HCl, pH 8, and were allowed to adsorb for 3 min on a carbon-coated Formvar grid. The grid was then washed three times for 1 min each, using the same buffer, and stained with 0.1% uranyl acetate for 10 min at room temperature. The grids were then observed on a Jeol JEM220FS transmission electron microscope.
Antibodies and flow cytometry.
For cytometry analysis of mouse surface antigens, the following monoclonal antibodies (MAbs) were used: anti-CD4-fluorescein isothiocyanate (anti-CD4-FITC; clone H129.19), anti-CD8α-FITC or anti-CD8α-phycoerythrin (anti-CD8α-PE; clone 53-6.7), anti-CD11c-FITC (clone HL3), anti-CD40-PE (clone 3/23), anti-CD45R-FITC (clone RA3-6B2), anti-CD69-peridinin chlorophyll protein (PerCP)-Cy5.5 (clone H1.2F3), anti-CD80-PE (clone 16-10A1), and anti-CD86-PE (clone GL1). Isotype controls were used for the anti-CD40 and anti-CD86 MAbs (rat immunoglobulin G2a [IgG2a], κ chain) and for the anti-CD80 MAb (Armenian hamster IgG2, κ chain) (all from BD Biosciences, Mississauga, Ontario, Canada). The FITC-coupled F4/80 MAb (clone BM8) and anti-gamma interferon (anti-IFN-γ)-FITC (clone XMG1.2) were obtained from eBioscience (San Diego, CA). Staining was performed for 20 min at 4°C. PE-coupled p33-H-2b tetrameric complexes (Tet-gp33) were synthesized as previously described (1), and staining was performed for 20 min at 37°C. All cytometry analyses were performed on a FACSCalibur flow cytometer (BD Bioscience), and data were analyzed using WinMDI software.
Isolation of splenic DCs.
Spleens of C57BL/6 mice were treated with 400 U/ml collagenase type IV (Roche Diagnostics, Laval, Quebec, Canada) for 45 min at 37°C in 5% CO2. Spleen cells were isolated by passage through a 100-μm cell strainer and were incubated for 20 min at 4°C with CD11c-specific colloidal paramagnetic beads (Miltenyi Biotec, Auburn, CA) in prefiltered running buffer (0.5% bovine serum albumin in phosphate-buffered saline [PBS]). After being washed once with running buffer, CD11c+ spleen cells were positively selected using an autoMACS system (Miltenyi Biotec). The purity of the positive fraction was always above 95%. Where indicated, the negative fraction was kept for subsequent analysis. CD11c+ cells were cultured in 10% MEM and were analyzed by flow cytometry after being stained with FITC-coupled anti-mouse CD11c MAbs.
Capture assay of PapMV-like particles.
PapMV-like particles were labeled using an Alexa Fluor 647 protein labeling kit (Molecular Probes, Eugene, OR) according to the manufacturer's instructions. Labeling efficiencies were determined by spectrophotometry and were similar for both control and PapMV-p33 VLPs. For in vivo capture assay, C57BL/6 mice were injected intravenously (i.v.) with 100 μg of labeled VLPs, and CD11c+ cells were purified from spleens at 2 h postinjection. Samples from the negative fraction obtained after purification of splenic CD11c+ cells were stained with FITC-coupled anti-mouse CD45R, F4/80, CD8α, or CD4 MAb. For in vitro capture assay, purified CD11c+ spleen cells from C57BL/6 mice were pulsed for 2 h with various concentrations (0.5, 1, and 5 μg) of Alexa Fluor 647-labeled VLPs. All samples were analyzed as previously described.
Confocal microscopy.
For the in vivo internalization assay, mice were injected i.v. with 100 μg of Alexa Fluor 647-labeled VLPs, and spleens were collected 2 h later. CD11c+ spleen cells were allowed to adhere to slides coated with poly-l-lysine (Sigma-Aldrich) by centrifugation at 650 rpm for 1 min. Cells were fixed with 10% formalin for 20 min and labeled for 45 min at room temperature with Alexa Fluor 488-conjugated wheat germ agglutinin (Molecular Probes) as a membrane marker. After three washes with PBS, slides were mounted using ProLong Gold antifade reagent (Molecular Probes) and analyzed using a Zeiss LSM 510 Meta scanning confocal microscope mounted on an Axiovert 100 oil immersion objective (Carl Zeiss, Jena, Germany). Images were processed using LSM 510 v3.2 software (Carl Zeiss). For the in vitro capture assay, purified CD11c+ spleen cells from naïve C57BL/6 mice were incubated for 2 h at 37°C with different quantities (0.5, 1, and 5 μg) of Alexa Fluor 647-labeled VLPs. Cells were then washed, stained, and analyzed as described above.
In vivo DC maturation assay.
C57BL/6 mice were immunized i.v. with 100 μg of control PapMV VLPs or PapMV-p33 VLPs or with 25 μg of LPS from E. coli serotype 5 (Sigma-Aldrich, Oakville, Ontario, Canada) as a positive control. At 2, 6, or 24 h postinjection, CD11c+ spleen cells were stained with FITC-coupled anti-mouse CD11c MAb in combination with PE-coupled anti-mouse CD40, CD80, or CD86 or isotype control MAbs. Samples were acquired and analyzed by flow cytometry as described above.
T-cell proliferation assay.
For in vitro assay, CD11c+ spleen cells were treated for 2 h with mitomycin C (Sigma-Aldrich). Following three washes in MEM with 5% FBS, 5 × 104 cells/well were added to 96-well round-bottomed plates and pulsed for 8 h with various concentrations (10, 100, 500, and 1,000 ng) of control PapMV or PapMV-p33 VLPs. LCMV p33 synthetic peptide-pulsed DCs served as positive controls. Magnetically isolated splenic p33-specific CD8 T lymphocytes from P14 transgenic mice were added (1 × 105/well) to pulsed DCs. After 24 h, 0.4 μCi of [3H]thymidine was added to each well, and cells were cultured for another 24 h. Cells were harvested with a Mach 2 model 96 harvester (TomTec, Hamden, CT), and proliferation of p33-specific CD8+ T lymphocytes was evaluated by measuring [3H]thymidine incorporation into cellular DNA with a Trillux 1450 MicroBeta counter (Perkin-Elmer, Woodbridge, Ontario, Canada). Surface expression of CD69 on proliferating p33-specific CD8+ T lymphocytes was also analyzed. Briefly, cells were stained with PE-coupled p33-H-2b tetrameric complex, FITC-coupled anti-mouse CD8α, and PerCP-coupled anti-mouse CD69 MAbs. Samples were acquired and analyzed by flow cytometry as described above. For in vivo assay, P14 transgenic mice were injected i.v. with 100 μg of control PapMV or PapMV-p33 VLPs. Spleens were collected at 24 h postimmunization, and the activation state of p33-specific CD8+ T lymphocytes was evaluated as described above.
Detection of p33-specific CD8+ T lymphocytes in immunized mice.
Spleens of immunized mice were collected 7 days following the last recall injection. Cells were stained with PE-coupled p33-H-2b tetrameric complexes and FITC-coupled anti-mouse CD8α MAb. 7-Amino-actinomycin D (7-AAD; BD Bioscience) was used for exclusion of dead cells. Samples (50,000 events in the lymphocyte gate) were acquired and analyzed by flow cytometry as described above. Statistical analysis was done by an unpaired t test, using GraphPad Prism 4.0 software.
Detection of IFN-γ-producing CD8+ T lymphocytes.
Five days following LCMV infection, spleen cells were restimulated for 5 h at 37°C, and production of IFN-γ by CD8+ cells was evaluated. Briefly, 1 × 106 spleen cells were incubated in 96-well round-bottomed plates in 5% RPMI supplemented with 100 units/ml mouse recombinant interleukin-2 (R&D Systems, Minneapolis, MN), 10 μg/ml brefeldin A (Sigma), and either PBS, 100 ng/ml phorbol myristate acetate (Sigma) and 1 μg/ml ionomycin (Sigma), or 10 μM p33 peptide (Sigma Genosys). Cells were then stained with PE-coupled anti-mouse CD8α MAb and 7-AAD (BD Bioscience). Cells were fixed, permeabilized, stained with an anti-IFN-γ-FITC MAb (eBioscience), and analyzed by flow cytometry as described above.
51Cr release assay.
Five days following LCMV infection of immunized mice, spleen cells were tested for cytotoxic activity in a standard 51Cr release assay as described previously (48).
LCMV focus-forming assay.
Immunized C57BL/6 mice were injected i.v. with 200 PFU of LCMV WE. At 5 days postinfection, spleens were collected and an LCMV focus-forming assay was performed as previously described (3).
RESULTS
DCs internalize PapMV VLPs and acquire a mature phenotype.
Overexpression of PapMV CP in E. coli produces VLPs that display a structure similar to that of the wild-type plant virus (39). We generated VLPs expressing the p33 immunodominant CTL epitope from the LCMV glycoprotein genetically fused to the CP through a triglycine, trileucine linker (Fig. 1A). Bacterial expression of control PapMV CP or PapMV-p33 yielded 29-kDa proteins (Fig. 1B, lanes 3) that were purified by nickel-affinity chromatography (Fig. 1B, lanes 4). Extensive washes were performed to remove all traces of LPS, and VLPs were isolated by high-speed ultracentrifugation (Fig. 1B, lanes 5). Electron microscopy analysis revealed that PapMV-p33 VLPs displayed a rod-like structure resembling that of native PapMV virions and control PapMV VLPs, but with a rougher appearance (Fig. 1C).
We next evaluated the capacity of various murine splenic cells to interact with PapMV VLPs labeled with Alexa Fluor 647 in vivo. Fluorescent VLPs were administered to C57BL/6 mice by i.v. injection, and 2 h later, the number of VLPs associated with different cell types was determined by flow cytometry (Fig. 2A). All APCs (DCs, B cells, and macrophages) were able to interact with labeled PapMV-p33 VLPs to various extents, but DCs were the most efficient, with more than 40% of CD11c+ cells being associated with labeled PapMV-p33 VLPs. As expected, both CD4+ and CD8+ T cells did not significantly interact with the VLPs (data not shown). Interestingly, larger amounts of PapMV-p33 VLPs were associated with all APC types compared with control PapMV VLPs, suggesting that the presence of the CTL epitope influenced the interaction. To determine whether this was due to differences in VLP capture or dissemination in vivo, splenic DCs were purified and pulsed in vitro for 2 h with labeled VLPs, and the levels of VLPs associated with DCs were determined by flow cytometry (data not shown). Both VLPs associated with purified DCs with similar efficiencies, suggesting that differences observed in vivo were probably the result of different degradation or dissemination kinetics. Confocal microscopy analysis of sorted CD11c+ DCs from VLP-immunized mice confirmed that the fluorescently labeled material was localized in the cytoplasm (Fig. 2B). Fluorescently labeled PapMV-p33 VLPs were found mostly in large vesicular structures, in contrast to control PapMV particles, which appeared to be more evenly distributed in the cytoplasm. This suggests that insertion of the p33 epitope in PapMV VLPs possibly modified their structure, allowing them to be internalized by DCs in a more stable particulate form. This hypothesis is supported by the observation that PapMV VLPs fused to an irrelevant ovalbumin epitope showed a similar vesicular localization pattern to that of PapMV-p33 VLPs (data not shown).
FIG. 2.
Splenic DCs take up PapMV-like particles in vivo and acquire a mature phenotype. (A) C57BL/6 mice were injected i.v. with 100 μg of Alexa Fluor 647-labeled VLPs in PBS or with 100 μl of sterile PBS as a negative control. Spleens were collected at 2 h postimmunization, and total CD11c+ splenic DCs were isolated by magnetic bead separation and stained with FITC-labeled CD11c-specific MAbs. The negative fraction obtain after magnetic purification of CD11c+ cells was stained with FITC-coupled B220 or F4/80 specific MAb. Cells were analyzed by flow cytometry. Values shown in the upper right quadrants represent the percentages of given cell populations associated with labeled VLPs within the total population. (B) In vivo capture of VLPs was visualized by confocal microscopy analysis. Mice were injected with 100 μg of Alexa Fluor 647-labeled VLPs (red) in PBS or with 100 μl of sterile PBS as a negative control, and CD11c+ spleen cells were purified 2 h later. Purified CD11c+ spleen cells were allowed to adhere for 12 h to glass slides coated with poly-l-lysine and were fixed with 4% paraformaldehyde. Cells were labeled with wheat germ agglutinin conjugated to Alexa Fluor 488 (green) to visualize the plasma membrane. (C) C57BL/6 mice were injected i.v. with 100 μg VLPs in PBS. Spleens were collected at 6 h postimmunization, and CD11c+ cells were isolated by magnetic separation. Mice injected with 25 μg LPS served as positive controls. Purified CD11c+ DCs were stained with FITC-labeled CD11c-specific antibodies in combination with PE-labeled anti-CD40, -CD80, or -CD86 or isotypic control antibodies. Data are gated on the CD11c+ population. Data are shown for isotypic controls (dotted lines), PBS-injected mice (filled histograms), and VLP-injected mice (bold lines). These results are representative of three independent experiments.
Mature DCs are the most efficient APC type capable of priming naive T cells, and we therefore evaluated whether PapMV VLP uptake by splenic DCs could lead to their maturation. Six hours following i.v. immunization of C57BL/6 mice with PapMV VLPs, splenic CD11c+ DCs were isolated by magnetic cell sorting, and the upregulation of cosignaling molecules (CD40, CD80, and CD86) was determined by flow cytometry (Fig. 2C). Both control PapMV and PapMV-p33 VLPs similarly induced significant upregulation of CD40, CD80, and CD86, suggesting that the presence of the p33 epitope does not affect this process. Similar results were obtained at 24 h postinjection (data not shown). To ensure that maturation was not a result of traces of LPS contaminating the preparations, the endotoxin level in each purified VLP stock was quantified using the Limulus amebocyte lysate assay. The corresponding trace amounts of contaminating LPS were administered to C57BL/6 mice, and cytometric analysis of cosignaling molecule expression levels on DCs revealed that such minute amounts of LPS had no significant effect on DC maturation (data not shown). These results suggest that PapMV VLPs possess an intrinsic adjuvant-like property that induces DC maturation. Compared to other VLP-based systems, PapMV VLPs seem to be one of the more potent at inducing the upregulation of cosignaling molecules on DCs (15, 18, 40, 41).
DCs efficiently process and present the p33 CTL epitope displayed on PapMV VLPs.
To assess whether the LCMV p33 CTL epitope displayed on PapMV VLPs could be cleaved correctly, processed, and presented by DCs to specific T cells, purified splenic CD11c+ DCs were pulsed for 8 h with various concentrations of VLPs and cocultured with p33-specific naive CTLs isolated from TCR transgenic P14 mice. The proliferation of p33-specific CTLs was assessed by thymidine incorporation (Fig. 3A). PapMV-p33 was very efficiently processed and presented by DCs, as it induced high levels of CTL proliferation. As little as 100 ng of VLPs (equivalent to 2 ng of free peptide) induced significant T-cell proliferation, whereas up to 1 μg of control PapMV VLPs did not. The ability of pulsed DCs to activate p33-specific naive T cells was next analyzed by quantifying the upregulation of the T-cell activation marker CD69 by flow cytometry (Fig. 3B). p33-specific CTLs cocultured with PapMV-p33-pulsed DCs became fully activated, with more than 90% of cells upregulating CD69. To determine whether the efficient capture, processing, and presentation of heterologous epitopes presented on PapMV VLPs could also be observed in vivo, p33-specific P14 TCR transgenic mice were injected i.v. with 100 μg of PapMV VLPs, and the activation of splenic p33-specific CTLs was analyzed 24 h after injection by evaluating CD69 surface expression (Fig. 3C). More than 80% of splenic p33-specific T cells from PapMV-p33-injected P14 mice expressed CD69, compared to <4% for mice injected with control PapMV VLPs. Taken together, these results clearly demonstrate that DCs can efficiently process and cross-present the p33 CTL epitope displayed on PapMV VLPs.
FIG. 3.
In vitro and in vivo processing of the LCMV p33 CTL epitope displayed on PapMV-like particles by splenic DCs and cross-priming of naïve T cells. (A) Splenic DCs were purified by CD11c magnetic bead separation and pulsed for 8 h with the indicated concentrations of VLPs in 96-well culture plates. DCs pulsed with the p33 synthetic peptide served as a positive control. Splenic p33-specific CD8+ T lymphocytes purified from TCR transgenic P14 mice were then added to the pulsed DC cultures. Proliferation of p33-specific CD8+ T lymphocytes was assayed 48 h later by [3H]thymidine incorporation into cellular DNA. (B) Activation of p33-specific CD8+ T lymphocytes was analyzed by flow cytometry following 24 h of coculture between specific T cells and DCs pulsed for 8 h with 1 μg of VLPs. Cells were stained with FITC-labeled anti-CD8 antibodies, PerCP-labeled anti-CD69 antibodies, and PE-labeled p33-specific tetramers. (C) P14 mice were injected i.v. with 100 μg of VLPs in PBS, and 24 h later, total spleen cells were stained with FITC-labeled anti-CD8 antibodies, PerCP-labeled anti-CD69 antibodies, and PE-labeled p33-specific tetramers. Data are gated on the CD8+ T-cell population. Values shown in the upper right quadrants represent the percentages of activated p33-specific CD8+ T lymphocytes within the total spleen p33-specific CD8+ T-lymphocyte population. These results are representative of three independent experiments.
Vaccination with PapMV-p33 VLPs generates specific CTLs.
The ability of PapMV-p33 VLPs to induce the development of a specific CTL response in mice was then evaluated. Since we showed that PapMV VLPs possess adjuvant-like properties, C57BL/6 mice were injected i.v. with 100 μg of VLPs in PBS without adjuvant. Following the administration of three identical booster injections at 10-day intervals, total spleen cells were directly analyzed ex vivo by p33 tetramer staining (Fig. 4). Mice given PapMV-p33 VLPs developed significant numbers of p33-specific T cells (0.75% ± 0.05%) compared to mice injected with control PapMV VLPs (0.03% ± 0.008%) (P < 0.0001; n = 6). This shows that PapMV VLPs can efficiently prime peptide-specific T-cell responses in vivo without the need for an adjuvant.
FIG. 4.
Immunization with PapMV-p33 VLPs generates p33-specific CD8+ T lymphocytes. C57BL/6 mice were injected i.v. with 100 μg of VLPs in PBS, and identical recall injections were given 10, 20, and 30 days later. Total spleen cells were then double stained with FITC-labeled anti-CD8 antibodies and PE-labeled p33-specific tetramers. 7-AAD was used for dead cell exclusion. Data are gated on the total lymphocyte population. Values shown in the upper right quadrants represent the percentages of p33-specific CD8+ T lymphocytes within the total CD8+ T-lymphocyte population. These results are representative of four independent experiments.
Immunization with PapMV-p33 VLPs induces protective effector CTL responses against LCMV infection.
Acute LCMV infection is exclusively controlled by CTLs (5, 21, 49). To determine whether the CTL responses induced by PapMV VLP immunization could protect against viral infections, vaccinated mice were challenged with LCMV. Mice were primed with an i.v. injection of 100 μg of PapMV VLPs without adjuvant and received two or three identical booster injections at 10-day intervals. Mice were challenged with 200 PFU of LCMV 7 days after the last booster injection. To visualize CTL expansion, the number of p33-specific T cells was determined by tetramer staining 5 days following infection (Fig. 5A), at a time when p33-specific T cells generated by the primary response to LCMV are not yet detectable (data not shown). Mice who received two booster injections of PapMV-p33 VLPs showed p33-specific T-cell frequencies of ∼3.3% of CD8+ T cells (data not shown), whereas mice receiving three booster injections had even larger numbers of specific T cells (∼7.3%), suggesting that the frequency of specific T cells generated by vaccination increased through repeated injections. Importantly, mice vaccinated with either two (data not shown) or three booster injections of the control PapMV VLPs showed no detectable p33-specific CTLs (Fig. 5A). We next determined whether the p33-specific T cells generated through VLP vaccination displayed effector function by intracellular IFN-γ staining (Fig. 5B). Mice vaccinated with PapMV-p33 VLPs showed frequencies of IFN-γ production of ∼6.9% of CD8+ T cells, whereas no significant IFN-γ production was detected in the control PapMV-vaccinated group. It is noteworthy that the frequencies detected by tetramer staining and IFN-γ staining were very similar, suggesting that most p33-specific T cells detected by tetramer staining display effector function. We then evaluated whether these CTLs also displayed lytic effector function by using a standard 51Cr release assay (Fig. 5C). The PapMV-p33-vaccinated group showed high levels of cytolytic activity, whereas no cytotoxicity could be observed in the PapMV-vaccinated control group. To determine if such cytotoxic responses are protective against LCMV infection, splenic viral titers were determined 5 days following challenge (Fig. 6). Mice who received one or two booster injections of PapMV-p33 VLPs were partially protected from LCMV infection, whereas mice receiving three booster injections of the same VLP preparation were fully protected, as indicated by the absence of detectable virus in the spleen. In contrast, mice receiving three booster injections of control PapMV VLPs showed high LCMV titers in the spleen. Taken together, these results demonstrate that vaccination with PapMV-p33 VLPs induces the development of p33-specific effector T cells in a dose-dependent manner and that protection from LCMV infection correlates with the number of effector T cells generated.
FIG. 5.
Expansion of effector p33-specific CTLs following LCMV infection. C57BL/6 mice were injected i.v. with 100 μg of VLPs in PBS, followed by three recall injections at 10-day intervals. Seven days after the last recall injection, immunized mice were infected i.v. with 200 PFU of LCMV. (A) Expansion of p33-specific CD8+ T lymphocytes was assayed at 5 days postinfection by flow cytometry. Total spleen cells were double stained with FITC-labeled anti-CD8 antibodies and PE-labeled p33-specific tetramers. 7-AAD was used for dead cell exclusion. Data are gated on the total lymphocyte population. Values shown in the upper right quadrants represent percentages of p33-specific CD8+ T lymphocytes within the total CD8+ T-lymphocyte population. (B) Production of IFN-γ by CD8+ T lymphocytes was also assayed at 5 days postinfection by flow cytometry. Total spleen cells were restimulated with the p33 peptide for 5 h in vitro. Spleen cells were then surface stained with a PE-labeled anti-CD8 antibody. After fixation and permeabilization, cells were stained with an anti-IFN-γ-FITC MAb. 7-AAD was used to exclude dead cells. Data are gated on the total lymphocyte population. Values shown in the upper right quadrants represent percentages of CD8+ IFN-γ+ T lymphocytes within the total CD8+ T-lymphocyte population. (C) Spleen cells were tested for cytotoxic activity in a standard 5-h 51Cr release assay of unpulsed (open circles) and p33-pulsed (closed circles) EL-4 target cells. Results are representative of four independent experiments.
FIG. 6.
Immunization with PapMV-p33 VLPs induces protective immunity against LCMV infection. C57BL/6 mice were injected i.v. with 100 μg of VLPs in PBS, followed by identical recall injections 10, 20, and 30 days later. Seven days after the last recall injection, immunized mice were infected i.v. with 200 PFU of LCMV. Spleens from infected mice were removed 5 days after infection, and LCMV titers were determined by a standard focus-forming assay. Results are representative of three identical and independent experiments.
DISCUSSION
There is an urgent need for the development of vaccines capable of inducing cellular responses against chronic viral infections and cancers. We describe here a novel plant virus-based vaccination platform that induces protective cellular immune responses. PapMV-like particles displaying the immunodominant p33 CTL epitope from LCMV are internalized by DCs and cross-presented to specific CTLs. We recently reported that this is achieved through a proteasome-independent pathway (14), as shown for another VLP-based system (30). Importantly, and in contrast to many VLPs described so far, PapMV-like particles directly prime protective CTL responses in vivo without an adjuvant (i.e., CpGs or anti-CD40). This ability probably resides in their intrinsic capacity to induce DC maturation. The critical importance of activating APCs for priming CTL responses to VLPs was demonstrated in a study by Storni et al. (37). Hepatitis B virus VLPs fused to the p33 CTL epitope induced effective protection against LCMV infection only when they were coadministered with anti-CD40 antibodies or CpG oligonucleotides, suggesting that these particular VLPs do not directly induce DC maturation. Similarly, another VLP system based on bacteriophage Qβ could induce large numbers of peptide-specific T cells in a prime-boost regimen, but again, CpG oligonucleotides were required (32). CpGs have been shown to be potentially harmful by destroying splenic architecture and inducing immunosuppression following repetitive treatment and by altering fetal development at high doses (11, 26). Thus, the ability of PapMV VLPs to induce DC maturation without the need of coinjecting CpGs offers a significant advantage compared to other systems that are more dependent on adjuvant administration. Our results suggest that PapMV particles possess pathogen-associated molecular patterns (PAMPs) recognized by a pattern recognition receptor on DCs which, upon binding, leads to their maturation. We previously showed that assembly of PapMV VLPs into rod-like structures requires RNA (39). Thus, one possible PAMP candidate associated with PapMV VLPs could be bacterial RNA. Pattern recognition receptors, such as Toll-like receptors, have been implicated in the activation of DCs by VLPs, as illustrated by the failure of human papillomavirus VLPs to upregulate interleukin-12 and IFN-α and -γ in DCs lacking MyD88, a key adaptor protein involved in the signaling pathway of many Toll-like receptors (43). Recently, McCormick et al. reported that tobacco mosaic virus (TMV)-like particles also induce DC maturation, demonstrating that recognition of plant virus PAMPs by DCs is not restricted to PapMV but is probably a more general phenomenon (18). However, in this system, the ability of TMV VLPs to induce DC maturation was not sufficient to allow avoidance of the use of adjuvant, since administration of CpG DNA was needed to confer partial protection against tumor challenge (18).
We showed that larger amounts of PapMV-p33 VLPs than control PapMV VLPs were associated with splenic APCs at 2 h postimmunization. This was not due to different binding and uptake efficiencies, since both VLPs were internalized similarly by purified DCs in vitro. This suggests that PapMV-p33 VLPs have different dissemination or degradation kinetics in vivo from that of control PapMV-VLPs, indirectly influencing uptake by splenic APCs. Supporting evidence for this comes from confocal microscopy analysis showing that PapMV-p33 VLPs are found mostly in intracytoplasmic vesicles as large aggregates, in contrast to control PapMV VLPs, which appear to be more evenly distributed in the cytoplasm. A similar observation was made using a control VLP expressing the SIINFEKL CTL epitope of ovalbumin (data not shown). Slight modifications in the overall VLP structure induced by the insertion of the foreign epitopes might render the VLPs more stable in vivo. Additional experiments will be required to pinpoint the exact mechanism involved and the precise intracellular localization of the internalized VLPs.
In this study, we show that vaccination of naive C57BL/6 mice with PapMV VLPs without adjuvant induces p33-specific CTLs. Relatively high p33-specific CTL frequencies were generated by VLP vaccination, as shown by their direct ex vivo detection by tetramer staining. Most other VLP systems displaying the p33 epitope have been shown to require the use of adjuvant to generate significant CTL responses (32, 37, 38). Moreover, compared to vaccination with peptide-loaded DCs or peptide in adjuvant, PapMV-p33 VLPs induce either larger or similar numbers of p33-specific T cells (17, 37, 45). In addition, the p33-specific CTLs induced by PapMV-p33 VLP vaccination rapidly expand following LCMV infection, and their frequency is augmented with the number of injections given. Moreover, induced CTLs produce IFN-γ and show strong cytolytic activity against p33-pulsed target cells. Importantly, protection from LCMV infection correlates with the frequency of specific T cells generated and the number of VLP doses given. This situation is reminiscent of prime-boost protocols used to trigger highly effective T-cell responses. It is well recognized that the heterologous prime-boost approach is a highly effective way of generating specific CTLs (2, 12, 31). However, the efficiency of a homologous prime-boost regimen is less well documented. Nevertheless, a study by Schwarz et al. showed that vaccines based on VLPs are equally effective at inducing antiviral CTL responses if they are administered in a homologous or heterologous prime-boost setting (32). In addition, they showed that repeated injections of VLPs were required to maintain high frequencies of specific CTLs. Our results support these data and suggest that repeated homologous recall injections of a CTL epitope displayed on PapMV VLPs also induce a highly efficient T-cell response that can protect against a rapidly spreading viral infection.
In conclusion, our data demonstrate that PapMV-based VLPs can directly interact with DCs, inducing their maturation, leading to the efficient processing and cross-presentation of an LCMV CTL epitope, and triggering a protective antiviral T-cell response. We believe that the future use of plant virus-based vaccines should provide a safe, stable, and economical prophylactic tool for the fight against chronic viral infections and cancer.
Acknowledgments
This work was supported by grants 53355 from the Canadian Institutes of Health Research and 262607 from the Natural Sciences and Engineering Research Council of Canada. A. Lamarre is a Canadian Institutes of Health Research New Investigator Award recipient and holds the Jeanne et J.-Louis Lévesque Chair in Immunovirology from the J.-Louis Lévesque Foundation. P. Lacasse thanks the Armand-Frappier Foundation for studentship support.
We thank Pamela Ohashi for providing P14 mice and Marcel Desrosiers for assistance with flow cytometry analysis. We also thank Tanya Girard, Veronika von Messling, and Emmanuel Moreau for critically reviewing the manuscript.
Footnotes
Published ahead of print on 7 November 2007.
REFERENCES
- 1.Altman, J. D., P. A. Moss, P. J. Goulder, D. H. Barouch, M. G. McHeyzer-Williams, J. I. Bell, A. J. McMichael, and M. M. Davis. 1996. Phenotypic analysis of antigen-specific T lymphocytes. Science 27494-96. [DOI] [PubMed] [Google Scholar]
- 2.Amara, R. R., F. Villinger, J. D. Altman, S. L. Lydy, S. P. O'Neil, S. I. Staprans, D. C. Montefiori, Y. Xu, J. G. Herndon, L. S. Wyatt, M. A. Candido, N. L. Kozyr, P. L. Earl, J. M. Smith, H. L. Ma, B. D. Grimm, M. L. Hulsey, J. Miller, H. M. McClure, J. M. McNicholl, B. Moss, and H. L. Robinson. 2001. Control of a mucosal challenge and prevention of AIDS by a multiprotein DNA/MVA vaccine. Science 29269-74. [DOI] [PubMed] [Google Scholar]
- 3.Battegay, M., S. Cooper, A. Althage, J. Banziger, H. Hengartner, and R. M. Zinkernagel. 1991. Quantification of lymphocytic choriomeningitis virus with an immunological focus assay in 24- or 96-well plates. J. Virol. Methods 33191-198. [DOI] [PubMed] [Google Scholar]
- 4.Bramwell, V. W., and Y. Perrie. 2005. The rational design of vaccines. Drug Discov. Today 101527-1534. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Byrne, J. A., and M. B. Oldstone. 1984. Biology of cloned cytotoxic T lymphocytes specific for lymphocytic choriomeningitis virus: clearance of virus in vivo. J. Virol. 51682-686. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Canizares, M. C., L. Nicholson, and G. P. Lomonossoff. 2005. Use of viral vectors for vaccine production in plants. Immunol. Cell Biol. 83263-270. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Denis, J., N. Majeau, E. Acosta-Ramirez, C. Savard, M. C. Bedard, S. Simard, K. Lecours, M. Bolduc, C. Pare, B. Willems, N. Shoukry, P. Tessier, P. Lacasse, A. Lamarre, R. Lapointe, C. Lopez Macias, and D. Leclerc. 2007. Immunogenicity of papaya mosaic virus-like particles fused to a hepatitis C virus epitope: evidence for the critical function of multimerization. Virology 36359-68. [DOI] [PubMed] [Google Scholar]
- 8.Erickson, J. W., J. B. Bancroft, and R. W. Horne. 1976. The assembly of papaya mosaic virus protein. Virology 72514-517. [DOI] [PubMed] [Google Scholar]
- 9.Freeman, A. J., G. Marinos, R. A. French, and A. R. Lloyd. 2001. Immunopathogenesis of hepatitis C virus infection. Immunol. Cell Biol. 79515-536. [DOI] [PubMed] [Google Scholar]
- 10.Heath, W. R., G. T. Belz, G. M. Behrens, C. M. Smith, S. P. Forehan, I. A. Parish, G. M. Davey, N. S. Wilson, F. R. Carbone, and J. A. Villadangos. 2004. Cross-presentation, dendritic cell subsets, and the generation of immunity to cellular antigens. Immunol. Rev. 1999-26. [DOI] [PubMed] [Google Scholar]
- 11.Heikenwalder, M., M. Polymenidou, T. Junt, C. Sigurdson, H. Wagner, S. Akira, R. Zinkernagel, and A. Aguzzi. 2004. Lymphoid follicle destruction and immunosuppression after repeated CpG oligodeoxynucleotide administration. Nat. Med. 10187-192. [DOI] [PubMed] [Google Scholar]
- 12.Kent, S. J., A. Zhao, S. J. Best, J. D. Chandler, D. B. Boyle, and I. A. Ramshaw. 1998. Enhanced T-cell immunogenicity and protective efficacy of a human immunodeficiency virus type 1 vaccine regimen consisting of consecutive priming with DNA and boosting with recombinant fowlpox virus. J. Virol. 7210180-10188. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Leclerc, C. 2003. New approaches in vaccine development. Comp. Immunol. Microbiol. Infect. Dis. 26329-341. [DOI] [PubMed] [Google Scholar]
- 14.Leclerc, D., D. Beauseigle, J. Denis, H. Morin, C. Pare, A. Lamarre, and R. Lapointe. 2007. Proteasome-independent major histocompatibility complex class I cross-presentation mediated by papaya mosaic virus-like particles leads to expansion of specific human T cells. J. Virol. 811319-1326. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Lenz, P., P. M. Day, Y. Y. Pang, S. A. Frye, P. N. Jensen, D. R. Lowy, and J. T. Schiller. 2001. Papillomavirus-like particles induce acute activation of dendritic cells. J. Immunol. 1665346-5355. [DOI] [PubMed] [Google Scholar]
- 16.Levin, D., S. Constant, T. Pasqualini, R. Flavell, and K. Bottomly. 1993. Role of dendritic cells in the priming of CD4+ T lymphocytes to peptide antigen in vivo. J. Immunol. 1516742-6750. [PubMed] [Google Scholar]
- 17.Ludewig, B., S. Ehl, U. Karrer, B. Odermatt, H. Hengartner, and R. M. Zinkernagel. 1998. Dendritic cells efficiently induce protective antiviral immunity. J. Virol. 723812-3818. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.McCormick, A. A., T. A. Corbo, S. Wykoff-Clary, L. V. Nguyen, M. L. Smith, K. E. Palmer, and G. P. Pogue. 2006. TMV-peptide fusion vaccines induce cell-mediated immune responses and tumor protection in two murine models. Vaccine 246414-6423. [DOI] [PubMed] [Google Scholar]
- 19.McMichael, A. J. 2006. HIV vaccines. Annu. Rev. Immunol. 24227-255. [DOI] [PubMed] [Google Scholar]
- 20.Mellman, I., and R. M. Steinman. 2001. Dendritic cells: specialized and regulated antigen processing machines. Cell 106255-258. [DOI] [PubMed] [Google Scholar]
- 21.Moskophidis, D., S. P. Cobbold, H. Waldmann, and F. Lehmann-Grube. 1987. Mechanism of recovery from acute virus infection: treatment of lymphocytic choriomeningitis virus-infected mice with monoclonal antibodies reveals that Lyt-2+ T lymphocytes mediate clearance of virus and regulate the antiviral antibody response. J. Virol. 611867-1874. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Natilla, A., G. Piazzolla, M. Nuzzaci, P. Saldarelli, C. Tortorella, S. Antonaci, and P. Piazzolla. 2004. Cucumber mosaic virus as carrier of a hepatitis C virus-derived epitope. Arch. Virol. 149137-154. [DOI] [PubMed] [Google Scholar]
- 23.Noad, R., and P. Roy. 2003. Virus-like particles as immunogens. Trends Microbiol. 11438-444. [DOI] [PubMed] [Google Scholar]
- 24.Pantaleo, G., and R. A. Koup. 2004. Correlates of immune protection in HIV-1 infection: what we know, what we don't know, what we should know. Nat. Med. 10806-810. [DOI] [PubMed] [Google Scholar]
- 25.Parez, N., C. Fourgeux, A. Mohamed, C. Dubuquoy, M. Pillot, A. Dehee, A. Charpilienne, D. Poncet, I. Schwartz-Cornil, and A. Garbarg-Chenon. 2006. Rectal immunization with rotavirus virus-like particles induces systemic and mucosal humoral immune responses and protects mice against rotavirus infection. J. Virol. 801752-1761. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Prater, M. R., V. J. Johnson, D. R. Germolec, M. I. Luster, and S. D. Holladay. 2006. Maternal treatment with a high dose of CpG ODN during gestation alters fetal craniofacial and distal limb development in C57BL/6 mice. Vaccine 24263-271. [DOI] [PubMed] [Google Scholar]
- 27.Qian, J., Y. Dong, Y. Y. Pang, R. Ibrahim, J. A. Berzofsky, J. T. Schiller, and S. N. Khleif. 2006. Combined prophylactic and therapeutic cancer vaccine: enhancing CTL responses to HPV16 E2 using a chimeric VLP in HLA-A2 mice. Int. J. Cancer 1183022-3029. [DOI] [PubMed] [Google Scholar]
- 28.Quan, F. S., C. Huang, R. W. Compans, and S. M. Kang. 2007. Virus-like particle vaccine induces protective immunity against homologous and heterologous strains of influenza virus. J. Virol. 813514-3524. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Rock, K. L., and L. Shen. 2005. Cross-presentation: underlying mechanisms and role in immune surveillance. Immunol. Rev. 207166-183. [DOI] [PubMed] [Google Scholar]
- 30.Ruedl, C., T. Storni, F. Lechner, T. Bachi, and M. F. Bachmann. 2002. Cross-presentation of virus-like particles by skin-derived CD8(−) dendritic cells: a dispensable role for TAP. Eur. J. Immunol. 32818-825. [DOI] [PubMed] [Google Scholar]
- 31.Schneider, J., S. C. Gilbert, T. J. Blanchard, T. Hanke, K. J. Robson, C. M. Hannan, M. Becker, R. Sinden, G. L. Smith, and A. V. Hill. 1998. Enhanced immunogenicity for CD8+ T cell induction and complete protective efficacy of malaria DNA vaccination by boosting with modified vaccinia virus Ankara. Nat. Med. 4397-402. [DOI] [PubMed] [Google Scholar]
- 32.Schwarz, K., E. Meijerink, D. E. Speiser, A. C. Tissot, I. Cielens, R. Renhof, A. Dishlers, P. Pumpens, and M. F. Bachmann. 2005. Efficient homologous prime-boost strategies for T cell vaccination based on virus-like particles. Eur. J. Immunol. 35816-821. [DOI] [PubMed] [Google Scholar]
- 33.Sedlik, C., M. Saron, J. Sarraseca, I. Casal, and C. Leclerc. 1997. Recombinant parvovirus-like particles as an antigen carrier: a novel nonreplicative exogenous antigen to elicit protective antiviral cytotoxic T cells. Proc. Natl. Acad. Sci. USA 947503-7508. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Sit, T. L., M. G. Abouhaidar, and S. Holy. 1989. Nucleotide sequence of papaya mosaic virus RNA. J. Gen. Virol. 702325-2331. [DOI] [PubMed] [Google Scholar]
- 35.Slupetzky, K., R. Gambhira, T. D. Culp, S. Shafti-Keramat, C. Schellenbacher, N. D. Christensen, R. B. Roden, and R. Kirnbauer. 2007. A papillomavirus-like particle (VLP) vaccine displaying HPV16 L2 epitopes induces cross-neutralizing antibodies to HPV11. Vaccine 252001-2010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Steinman, R. M., and M. Pope. 2002. Exploiting dendritic cells to improve vaccine efficacy. J. Clin. Investig. 1091519-1526. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Storni, T., F. Lechner, I. Erdmann, T. Bachi, A. Jegerlehner, T. Dumrese, T. M. Kundig, C. Ruedl, and M. F. Bachmann. 2002. Critical role for activation of antigen-presenting cells in priming of cytotoxic T cell responses after vaccination with virus-like particles. J. Immunol. 1682880-2886. [DOI] [PubMed] [Google Scholar]
- 38.Storni, T., C. Ruedl, K. Schwarz, R. A. Schwendener, W. A. Renner, and M. F. Bachmann. 2004. Nonmethylated CG motifs packaged into virus-like particles induce protective cytotoxic T cell responses in the absence of systemic side effects. J. Immunol. 1721777-1785. [DOI] [PubMed] [Google Scholar]
- 39.Tremblay, M. H., N. Majeau, M. E. Gagne, K. Lecours, H. Morin, J. B. Duvignaud, M. Bolduc, N. Chouinard, C. Pare, S. Gagne, and D. Leclerc. 2006. Effect of mutations K97A and E128A on RNA binding and self assembly of papaya mosaic potexvirus coat protein. FEBS J. 27314-25. [DOI] [PubMed] [Google Scholar]
- 40.Tsunetsugu-Yokota, Y., Y. Morikawa, M. Isogai, A. Kawana-Tachikawa, T. Odawara, T. Nakamura, F. Grassi, B. Autran, and A. Iwamoto. 2003. Yeast-derived human immunodeficiency virus type 1 p55(Gag) virus-like particles activate dendritic cells (DCs) and induce perforin expression in Gag-specific CD8(+) T cells by cross-presentation of DCs. J. Virol. 7710250-10259. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Warrino, D. E., W. C. Olson, M. I. Scarrow, L. J. D'Ambrosio-Brennan, R. S. Guido, D. M. Da Silva, W. M. Kast, and W. J. Storkus. 2005. Human papillomavirus L1L2-E7 virus-like particles partially mature human dendritic cells and elicit E7-specific T-helper responses from patients with cervical intraepithelial neoplasia or cervical cancer in vitro. Hum. Immunol. 66762-772. [DOI] [PubMed] [Google Scholar]
- 42.Woo, W. P., T. Doan, K. A. Herd, H. J. Netter, and R. W. Tindle. 2006. Hepatitis B surface antigen vector delivers protective cytotoxic T-lymphocyte responses to disease-relevant foreign epitopes. J. Virol. 803975-3984. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Yang, R., F. M. Murillo, H. Cui, R. Blosser, S. Uematsu, K. Takeda, S. Akira, R. P. Viscidi, and R. B. Roden. 2004. Papillomavirus-like particles stimulate murine bone marrow-derived dendritic cells to produce alpha interferon and Th1 immune responses via MyD88. J. Virol. 7811152-11160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Young, S. L., M. Wilson, S. Wilson, K. W. Beagley, V. Ward, and M. A. Baird. 2006. Transcutaneous vaccination with virus-like particles. Vaccine 245406-5412. [DOI] [PubMed] [Google Scholar]
- 45.Zarei, S., S. Abraham, J. F. Arrighi, O. Haller, T. Calzascia, P. R. Walker, T. M. Kundig, C. Hauser, and V. Piguet. 2004. Lentiviral transduction of dendritic cells confers protective antiviral immunity in vivo. J. Virol. 787843-7845. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Zhang, H., E. Todderud, and G. Stubbs. 1993. Crystallization and preliminary X-ray analysis of papaya mosaic virus coat protein. J. Mol. Biol. 234885-887. [DOI] [PubMed] [Google Scholar]
- 47.Zinkernagel, R. M., A. Lamarre, A. Ciurea, L. Hunziker, A. F. Ochsenbein, K. D. McCoy, T. Fehr, M. F. Bachmann, U. Kalinke, and H. Hengartner. 2001. Neutralizing antiviral antibody responses. Adv. Immunol. 791-53. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Zinkernagel, R. M., T. Leist, H. Hengartner, and A. Althage. 1985. Susceptibility to lymphocytic choriomeningitis virus isolates correlates directly with early and high cytotoxic T cell activity, as well as with footpad swelling reaction, and all three are regulated by H-2D. J. Exp. Med. 1622125-2141. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Zinkernagel, R. M., and R. M. Welsh. 1976. H-2 compatibility requirement for virus-specific T cell-mediated effector functions in vivo. I. Specificity of T cells conferring antiviral protection against lymphocytic choriomeningitis virus is associated with H-2K and H-2D. J. Immunol. 1171495-1502. [PubMed] [Google Scholar]