Abstract
Introduction
A previous article proposed an algorithm for defining somatization in children by classifying them into three categories: well, medically ill, and somatizer; the authors suggested further empirical validation of the algorithm (Postilnik et al., 2006). We use the Child Behavior Checklist (CBCL) to provide this empirical validation.
Method
Parents of children seen in pediatric clinics completed the CBCL (n=126). The physicians of these children completed specially-designed questionnaires. The sample comprised of 62 boys and 64 girls (age range 2 to 15 years). Classification categories included: well (n=53), medically ill (n=55), and somatizer (n=18). Analysis of variance (ANOVA) was used for statistical comparisons. Discriminant function analysis was conducted with the CBCL subscales.
Results
There were significant differences between the classification categories for the somatic complaints (p=<0.001), social problems (p=0.004), thought problems (p=0.01), attention problems (0.006), and internalizing (p=0.003) subscales and also total (p=0.001), and total-t (p=0.001) scales of the CBCL. Discriminant function analysis showed that 78% of somatizers and 66% of well were accurately classified, while only 35% of medically ill were accurately classified.
Conclusion
The somatization classification algorithm proposed by Postilnik et al. (2006) shows promise for classification of children and adolescents with somatic symptoms.
Keywords: somatoform disorders, pediatrics, child psychiatry, child psychology, algorithms, diagnostic techniques and procedures
Résumé
Introduction
Un article précédent proposait un algorithme destiné à définir la somatisation chez les enfants qui étaient classés dans trois catégories : enfants en bonne santé, enfants malades, et enfants qui somatisent. Les auteurs de cet article estimaient nécessaire de valider empiriquement l’algorithme (Postilnik et al., 2006) présenté. Nous avons utilisé la Child Behavior Checklist (CBCL) pour procéder à cette validation.
Méthodologie
Les parents des enfants vus en clinique pédiatrique ont rempli la CBCL (n=126), tandis que les médecins remplissaient un questionnaire spécial. L’échantillon consistait en 62 garçons et 64 filles âgés de 2 à 15 ans. Les sujets ont été classés en trois catégories : enfants bien portants (n=53), enfants malades (n=55), et enfants qui somatisent (n=18). L’analyse de variance (ANOVA) a été utilisée à des fins de comparaison statistique. L’analyse discriminante a porté sur les sous-échelles de la CBCL.
Résultats
On constate des écartssignificatifs entre les catégories des sous-échelles relatives aux plaintes de nature somatique (p=<0,001), problèmes de nature sociale (p=0,004), problèmes au niveau de la pensée (p=0,01), déficits d’attention (0,006), problèmes internalisés (p=0,003), et aussi des différences importantes par rapport au total (p=0,001), et au total T (p=0,001). L’analyse discriminante a permis de constater que 78 % des enfants qui somatisaient et 66 % des enfants bien portants étaient classés dans la bonne catégorie, contre 35 % seulement des enfants malades.
Conclusion
L’algorithme d’évaluation de la somatisation chez les enfants et les adolescents qui est proposé par Postilnik et al. (2006) a un avenir prometteur.
Keywords: troubles somatoformes, pédiatrie, psychiatrie de l’enfant, psychologie de l’enfant, algorithmes, techniques et méthodes diagnostiques
Introduction
The prevalence of somatic symptoms among children and adolescents ranges from 20% to 69% (Domenech-Llaberia et al., 2004; Knishkowy, Palti, Tima, Adler, & Gofin, 1995; Masi, Favilla, Millepiedi, & Mucci, 2000). If severe enough and if they cannot be fully explained as a purely medical condition, these symptoms can be diagnosed as somatoform disorders. According to the Diagnostic and Statistical Manual of Mental Disorders - 4th edition (DSM-IV; American Psychiatric Association, 1994), somatoform disorders include somatization disorder, undifferentiated somatoform disorder, conversion disorder, pain disorder, hypochondriasis, body dysmorphic disorder, and somatoform disorder not otherwise specified. One subtype of somatoform disorders is somatization disorder and includes repeated symptoms from four broad areas of pain, gastrointestinal, sexual, and pseudo-neurological domains (American Psychiatric Association, 1994). According to the DSM-IV (American Psychiatric Association, 1994), somatization disorder has a lifetime prevalence rate of 0.2% in men and 0.2% to 2% in women. DSM-IV does not specify somatization disorder prevalence data for children or adolescents. A recent chapter concluded that there is a lack of adequate data on somatization disorder prevalence in children and adolescents and that epidemiological research is necessary to study this topic (Essau, 2006).
Somatic symptoms and general function in children and adolescents have often been assessed using the Child Behavior Checklist (CBCL; Achenbach, 1992) for parental perceptions of child adjustment. The CBCL consists of eight subscales; withdrawn, somatic complaints, anxious/depressed, social problems, thought problems, attention problems, delinquent behavior, and aggressive behavior. The CBCL includes externalizing, internalizing, total, and total-t subscales. Subscales of the CBCL have been found to be highly correlated with the somatization subscale of the CBCL. A study of 54 girls (ages 6–12) found that those with precocious puberty had significantly higher scores than controls on the somatic complaints, withdrawn, social problems, and depression subscales of the CBCL (Xing-xing, Zhu-wen, Jian-jiang, Xiu-yin, & Xi-quiang, 2005). Another study of 4–18 year olds found that as compared to non suicidal children, those with suicidal ideation or suicidal attempts had significantly higher scores not only on the CBCL total, externalizing, internalizing, anxious/depressed, and aggressive subscales, but also on the somatic complaints subscale (Hukkanen, Sourander, & Bergroth, 2003).
Also, several studies among children show relationships among non-CBCL somatic measures and other measures related to the content measured by the eight subscales of the CBCL. Somatization is related to anxiety and depression among those with abdominal pain without an identifiable organic disease (Mulvaney, Lambert, Garber, & Walker, 2006). Somatic symptoms are higher among those with generalized anxiety disorder (Ginsburg, Riddle, & Davies, 2006). Explanatory thinking style for increased catastrophic thoughts related to pain and disability are higher among those with somatic complaints (Vervoort, Goubert, Eccleston, Bijttebier, & Crombez, 2006). Those with recurrent abdominal pain, a common somatic complaint, have higher scores on somatization, depression, anxiety, attention problems, and withdrawal (Robins, Schoff, Glutting, & Abelkop, 2003).
Among children and early adolescents the DSM-IV required sexual symptom criteria for somatization disorder may be difficult to determine. A previous article proposed an algorithm to categorize children into three classifications of well, medically ill, and somatizer (Postilnik, Eisman, Price, & Fogel, 2006). This algorithm incorporates objective medical information from physicians and child medical records along with subjective information provided by parents and/or the child. We empirically test this algorithm with a sample of children and adolescents to determine if it is able to differentiate between the three classifications of well, medically ill, and somatizer.
Method
Participants and Procedure
Participants were a convenience sample of 147 children and adolescents seen in the out-patient pediatric clinic of Coney Island Hospital (Brooklyn, NY) who were accompanied by a parent. The parent and/or child completed the research instruments described below. Informed consent was obtained from the parent and as appropriate for the child/adolescent. Only 126 participants completed information for the questionnaires. Reasons for the missing information from the 21 participants included refusal to complete the Child Behavior Checklist (CBCL) questionnaire (n = 5), and incomplete data from the Child’s Health Record Chart Review due to either loss of the Physician’s Questionnaire form after completion by not being placed in the child’s medical chart or non-legible/insufficient information from the child’s medical chart (n = 16), which resulted in an inability to classify the child. Of the 5 with missing CBCL scores, we were able to classify 3 individuals; 1 was medically ill and 2 were somatizers.
Instruments
Child Behavior Checklist
The Child Behavior Checklist, CBCL (Achenbach, 1992) was used to examine parental perceptions of child’s behavior. The scale used for this research (118 items) assesses a child’s behavior along eight dimensions, including the extent to which a parent perceives a child as withdrawn, having somatic complaints, anxious/depressed, having social problems, thought problems, attention problems, delinquent behavior, or aggressive behavior. For each item a parent was asked to rate the degree to which a particular behavior resembles the child’s current behavior (0=not true, 1=somewhat or sometimes true, 2=very often true). These raw scores were then converted to normative scores. A score at greater or equal to the 95th percentile on the normative scale was considered indicative of significant somatic complaints. The CBCL is widely used and has established reliability and validity (Achenbach, 1992).
Physician’s Questionnaire
The Physician’s Questionnaire (PQ; Postilnik et al., 2006) was completed by the child’s pediatrician at the time of the clinic visit. The PQ consists of four questions. The first question is, “Was the visit solely for a regular checkup?” where a yes/no response is provided. The other three questions are, “Do you think this child should be kept away from school or other daily activities?,” “Do you think this child’s health should be monitored closely in the immediate future?,” and “Do you recommend a follow-up visit?” These are all measured on a Likert scale ranging from 1=major restrictions and 7=no restrictions. For each item, a rating of either 1 or 2 is considered positive for a problem.
Child’s Health Record Chart Review
The Child’s Health Record Chart Review (CHRCR; Postilnik et al., 2006) is a protocol used to examine a child’s medical charts. The CHRCR examines the following aspects of the physician’s record of the physical exam: diagnosis, medication, general health indicators, and frequency of service utilization. Each child participant’s medical chart was examined by two trained graduate student research assistants and inter-rater reliability was calculated with these two separate raters. Perfect kappa scores were obtained (Kappa=1, p=<0.001).
Somatization Classification Algorithm
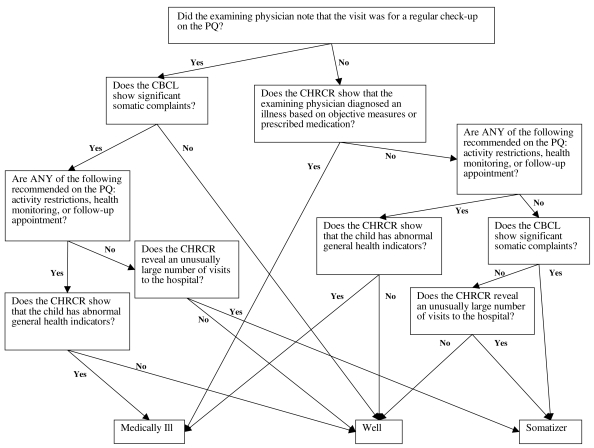
The child classification status was determined by a combination of the following instruments: (1) the somatic symptoms scale of the CBCL, (2) the PQ, and (3) the CHRCR. Children were classified into three different groups: well (i.e., those with no history of recurrent somatic complaints), medically ill (i.e., those with identifiable medical illness or physical abnormality), and somatizer (i.e., those with a history of recurrent somatic complaints). Detailed flowcharts demonstrating this algorithm have been previously published (Postilnik et al., 2006). The Figure shows one of the flowcharts for this classification approach from the original article. As this was published in an open access journal, this article can be freely retrieved from the journal website for those interested in more details of the classification approach.
Statistical Analysis
Analysis of variance (ANOVA), the Pearson chi-square test, or the Fisher’s exact test, were used to compare demographic characteristics as appropriate. As the eight CBCL subscales were not normally distributed, they were transformed with a logarithmic transformation. This included adding the value of one to each sub-scale, as some individuals had values of zero, precluding logarithmic transformation. A multivariate analysis of variance (MANOVA) was conducted with the eight CBCL subscales: (1) withdrawn, (2) somatic complaints, (3) anxious/depressed, (4) social problems, (5) thought problems, (6) attention problems, (7) delinquent behavior, and (8) aggressive behavior. Following a significant Wilks’ Lambda, separate ANOVA analyses were conducted for each of the CBCL subscales. Post-hoc comparisons were performed using Least Significant Difference (LSD) comparisons. Due to the possibility of unequal sample sizes between the groups, Welch ANOVA was also conducted. Also, ANOVA comparisons were performed for the CBCL internalizing, externalizing, total, and total-t scores, along with LSD post-hoc comparisons. Welch ANOVA was also conducted. Discriminant function analysis was conducted with the logarithmic transformed eight CBCL subscales. ANOVA and LSD post-hoc comparisons were performed for the obtained discriminant functions. Discriminant function classifications were performed to predict membership in the three classified groups of well, medically ill, and somatizer. SPSS Version 11.5 (SPSS, 2002) was used for all analyses, except for the Fisher’s exact test, where Stata/SE Version 9.2 (Stata, 2006) was used.
Results
With regard to those that we were not able to classify, there were no statistical differences in age (p = 0.99), sex (p = 0.78), or race/ethnicity (p = 0.80) between those whom we were able to completely classify and those whom we did not have sufficient information to classify. Table 1 shows the demographic characteristics of the sample. The average age was approximately seven years (range 2 to 15 years) and did not differ between the groups. Sex was approximately equally distributed and did not differ between the groups. Race/ethnicity included a high percentage of minority groups, including African Americans, Asian Americans, and Hispanic Americans, while Caucasians made up only a small percentage of the sample. There were no significant race/ethnicity differences between the groups.
Table 1.
Demographic Characteristics of 126 Children and Adolescents
| Variable | Well M (SD)or % (#) | Medically Ill M (SD)or % (#) | Somatizer M (SD)or % (#) | p-value |
|---|---|---|---|---|
| Age (years) | 7.44 (3.37) | 7.34 (3.58) | 7.86 (3.72) | 0.84 |
| Sex | 0.83 | |||
| Boy | 47.2% (25) | 49.1% (27) | 55.6% (10) | |
| Girl | 52.8% (28) | 50.9% (28) | 44.4% (8) | |
| Race/Ethnicity | 0.52 | |||
| African American | 25.0% (12) | 22.0% (11) | 33.3% (6) | |
| Asian American | 43.8% (21) | 30.0% (15) | 33.3% (6) | |
| Caucasian | 10.4% (5) | 18.0% (9) | 11.1% (2) | |
| Hispanic American | 16.7% (8) | 30.0% (15) | 22.2% (4) | |
| Other | 4.2% (2) | 0.0% (0) | 0.0% (0) |
Note: M = mean, SD = standard deviation.
Table 2 shows ANOVA comparisons for the eight CBCL subscales. Before these ANOVA comparisons were conducted, a MANOVA was performed with a significant Wilks’ Lambda (p=0.001) indicating that the eight subscales were independent. An overall pattern existed for all eight subscales where “well” had the lowest means, “medically ill” the next highest, and “somatizer” the greatest means. Of the eight subscales, four had statistically significant differences between the groups, with a fifth approaching significance. Repeating these analyses with Welch ANOVA showed similar significant and non-significant results. The somatic complaints subscale was significantly different between the groups. Post-hoc LSD comparisons showed that “well” differed from “somatizer” (p=<0.001), and from “medically ill” (p=0.007), and “somatizer” differed from “medically ill” (p=<0.001). The anxious/depressed subscale only approached significance. However, a post-hoc LSD comparison showed that “well” differed from “somatizer” (p=0.02) and “somatizer” from “medically ill” approached significance (p=0.08). The social problems subscale was significantly different between the groups. Post-hoc LSD comparisons showed that “well” differed from “somatizer” (p=0.001), and “somatizer” differed from “medically ill” (p=0.01). The thought problems subscale was significantly different between the groups. Post-hoc LSD comparisons showed that “well” differed from “somatizer” (p=0.04), and “well” differed from “medically ill” (p=0.005). The attention problems subscale was significantly different between the groups. Post-hoc LSD comparisons showed that “well” differed from “somatizer” (p=0.001) and “somatizer” differed from “medically ill” (p=0.03).
Table 2.
Child Behavior Checklist Subscale Comparisons for the Categories of Well, Medically Ill, and Somatizer
| Variable | Well M (SD) (n = 53) | Medically Ill M (SD) (n = 55) | Somatizer M (SD) (n = 18) | F Statistic | p-value | Post-hoc |
|---|---|---|---|---|---|---|
| Withdrawn | 1.75 (1.77) | 2.25 (2.49) | 2.83 (3.35) | 1.09 | 0.34 | — |
| Somatic Complaints | 0.60 (1.17) | 1.60 (2.50) | 3.67 (3.01) | 17.18 | <0.001 | a, b, c |
| Anxious/Depressed | 2.64 (2.82) | 2.89 (2.77) | 4.83 (4.36) | 2.85 | 0.06 | A |
| Social Problems | 1.85 (1.90) | 2.25 (1.92) | 3.50 (1.95) | 5.81 | 0.004 | a, c |
| Thought Problems | 0.57 (1.05) | 1.20 (1.38) | 1.39 (1.88) | 4.81 | 0.01 | a, b |
| Attention Problems | 2.11 (1.92) | 3.00 (3.09) | 4.72 (3.54) | 5.34 | 0.006 | a, c |
| Delinquent Behavior | 1.06 (1.01) | 1.27 (1.35) | 2.06 (2.31) | 1.14 | 0.32 | — |
| Aggressive Behavior | 5.38 (4.93) | 5.95 (4.90) | 7.89 (5.47) | 1.22 | 0.30 | — |
Note: M = mean, SD = standard deviation. Mean and standard deviation values are original values. F statistic and p-values are for the logarithmic transformed values. Post-hoc code for comparisons consists of: a = well differ from somatizer, b = well differ from medically ill, c = somatizer differ from medically ill
Table 3 shows a similar mean pattern as for the CBCL subscales where for all the variables, “well” had the lowest means, “medically ill” the next highest, and “somatizer” the greatest means. In these analyses there were significant differences between the groups for the CBCL internalizing, CBCL total, and CBCL total-t sub-scales, but no significant differences for the CBCL externalizing subscale. Repeating these analyses with Welch ANOVA showed similar significant and non-significant results. Post-hoc LSD comparisons for the CBCL internalizing sub-scale showed that “well” differed from “somatizer” (p=0.001) and “somatizer” differed from “medically ill” (p=0.02). Post-hoc LSD comparisons for the CBCL total subscale showed that “well” differed from “somatizer” (p=<0.001), “well” differed from “medically ill” (p=0.05), and “somatizer” differed from “medically ill” (p=0.01). Post-hoc LSD comparisons for the CBCL total-t subscale showed that “well” differed from “somatizer” (p=0.001), “well” differed from “medically ill” (p=0.02), and “somatizer” differed from “medically ill” (p=0.05).
Table 3.
Child Behavior Checklist Externalizing, Internalizing, Total, and Total-t Subscale Comparisons for the Categories of Well, Medically Ill, and Somatizer
| Variable | Well M (SD) (n = 53) | Medically Ill M (SD) (n = 55) | Somatizer M (SD) (n = 18) | F Statistic | p-value | Post-hoc |
|---|---|---|---|---|---|---|
| Externalizing | 46.51 (8.76) | 48.05 (8.69) | 50.94 (11.17) | 1.63 | 0.20 | —- |
| Internalizing | 48.15 (9.26) | 51.22 (9.68) | 57.39 (11.74) | 6.03 | 0.003 | a, c |
| Total | 19.00 (12.96) | 25.16 (15.38) | 36.44 (26.43) | 7.71 | 0.001 | a, b, c |
| Total-t | 46.96 (9.17) | 51.24 (9.28) | 56.39 (12.25) | 6.94 | 0.001 | a, b, c |
Note: M = mean, SD = standard deviation. Post-hoc code for comparisons consists of: a = well differ from somatizer, b = well differ from medically ill, c = somatizer differ from medically ill
Table 4 shows comparisons for the two discriminant functions obtained from the discriminant function analysis. Discriminant function 1 consisted of CBCL somatic complaints, anxious/depressed, social problems, attention problems, delinquent behavior, and aggressive behavior subscales. Discriminant function 2 consisted of CBCL withdrawn and thought problems subscales. In the ANOVA comparisons for discriminant function 1, the three groups of well, medically ill, and somatizer significantly differed from each other. Post-hoc LSD comparisons showed that “well” differed from “somatizer” (p=<0.001), “well” differed from “medically ill” (p=0.002), and “somatizer” differed from “medically ill” (p=<0.001). In the ANOVA comparisons for discriminant function 2, the three groups of well, medically ill, and somatizer significantly differed from each other. Post-hoc LSD comparisons showed that “well” differed from “medically ill” (p=0.03) and “somatizer” from “medically ill” approached significance (p=0.06).
Table 4.
Comparisons of Discriminant Functions for the Child Behavior Checklist Subscales
| Variable | Well M (SD) (n = 18) | Medically Ill M (SD) (n = 55) | Somatizer M (SD) (n = 53) | F Statistic | p-value | Post-hoc |
|---|---|---|---|---|---|---|
| Discriminant Function 1 | −0.52 (0.84) | 0.10 (1.13) | 1.21 (1.02) | 20.52 | <0.001 | a, b, c |
| Discriminant Function 2 | −0.17 (0.94) | 0.25 (1.06) | −0.28 (0.99) | 3.13 | 0.047 | b |
Note: M = mean, SD = standard deviation. Mean and standard deviation values are logarithmic transformed values. Post-hoc code for comparisons consists of: a = well differ from somatizer, b = well differ from medically ill, c = somatizer differ from medically ill
Table 5 shows the predicted discriminant function classifications for the three groups: well, medically ill, and somatizer. For those classified as “well,” 66.0% were correctly classified, with 17.0% each incorrectly classified as either “medically ill” or “somatizer.” For those classified as “medically ill,” only 34.5% were correctly classified, with 43.6% incorrectly classified as “well” and 21.8% incorrectly classified as “somatizer.” For those classified as “somatizer,” 77.8% were correctly classified, with 16.7% incorrectly classified as “well” and 5.6% as “medically ill.”
Table 5.
Classification of Somatization Algorithm Categories with Discriminant Function Analysis
| Predicted Group
| |||||
|---|---|---|---|---|---|
| Variable | Well % (#) | Medically Ill % (#) | Somatizer % (#) | Total | |
| Original Group | Well % (#) | 66.0% (35) | 17.0 (9) | 17.0 (9) | 53 |
| Medically Ill % (#) | 43.6% (24) | 34.5% (19) | 21.8% (12) | 55 | |
| Somatizer % (#) | 16.7% (3) | 5.6% (1) | 77.8% (14) | 18 | |
Discussion
The classification system based upon the algorithm was able to successfully differentiate between the three groups of “well,” “medically ill,” and “somatizer” using the somatic complaints, social problems, thought problems, and attention problems subscales of the CBCL and also approached significance for the CBCL anxious/depressed subscale.
Our findings are consistent with other research on the CBCL. The finding that thought problems are correlated with somatic complaints was supported (Vervoort et al., 2006). Additionally, several researchers found somatization to be correlated with social problems and attention problems (Robins et al., 2003; Xing-xing et al., 2005).
Several researchers also found anxiety (Ginsburg et al., 2006; Robins et al., 2003) and depression (Mulvaney et al., 2006; Robins et al., 2003; Xing-xing et al., 2005) to be correlated with somatization. However, in our analyses the CBCL anxious/depressed sub-scale only approached significance. Also, we report that the classification system did not differentiate for the withdrawn CBCL subscale. This is different from studies reporting a relationship of somatization with the CBCL withdrawn subscale (Robins et al., 2003; Xing-xing et al., 2005).
Our discriminant function analysis showed that 78% of somatizers were accurately classified by using this algorithm, with the majority of the misclassifications for the well group. This is quite a good result as clearly clinicians can easily discern if someone is well or not well (i.e., whether not well as either medically ill or as a somatizer). Also, these percentages are similar to others reported for discriminant function analysis. For example, discriminant function analysis showed that 76% of children with recurrent abdominal pain (RAP) were accurately classified as somatizers (Robins et al., 2003). Also, the discriminant function analysis results were also promising for the well group, in which 66% of the sample was classified correctly. However, the discriminant function analysis results for the medically ill group were not as promising, as only 35% of our sample was classified correctly. However, as the majority of mis-classifications were among those now incorrectly classified as well, a competent clinician would clearly be able to discriminate between “medically ill” and “well,” and not be misled by a false classification result. Therefore, this classification approach has promise in discriminating somatizers from those that are medically ill, as the somatizers are not likely to be misclassified as medically ill.
As discussed in the original theoretical article proposing the algorithm (Postilnik et al., 2006), clinical implications for this research include that it can help identify children whose suffering may not be adequately acknowledged by their primary care physicians. These primary care physicians may now refer these children for appropriate mental health treatment by mental health care professionals. Also, it may allow pediatricians to reduce medical care costs and patient burden by reducing the numerous and often unnecessary medical testing.
One strength of this study is that the participants represented diverse ethnicity, a population not typically studied. However, others may interpret this as a limitation in that it may not be generalizable to the population in general. Other limitations of this study include the absence of structured diagnostic interviews, or clinician assigned diagnoses for somatization disorder using DSM-IV criteria. Therefore, since there was no formal gold standard, we were unable to calculate sensitivity and specificity values for this algorithm. Also, although the CBCL is often considered as the standard for self-report assessment of children, it is only a self-report and also it is only one particular self-report measure. Although the PQ is only a few items, there have been no reliability or validity studies with it. Also, physician responses to the PQ may not only be a function of the physician’s direct observations, but also may be influenced by the parent’s expressed opinion to the physician about a child’s health condition. Lastly, the discriminant analyses suggest some need for fine tuning the algorithm to be more accurate for classifying those medically ill.
In conclusion, these results offer promise for the future of classifying children with somatization. The somatization algorithm used clearly was able to classify somatizers. This approach may offer a way of differentiating between children who are medically ill and those who are somatizers. Future research should include formal psychiatric diagnostic interviews to allow for calculation of sensitivity, specificity, positive predictive value, and negative predictive value.
Figure 1.
Flowchart detailing an algorithm for classifying children as medically ill, somatizers, or well.
Note: CBCL = Child Behavior Checklist, CHRCR = Child’s Health Record Chart Review, PQ = Physician’s Questionnaire. Original figure reprinted from Postilnik et al., 2006 with permission. It also can be viewed in the original article freely available at http://www.cacap-acpea.org/onottaca/doc.nsf/files/4D9AC1A899B10618872571A800797BF6/$file/2006MayAlgorithmforDefiningSomatization.pdf
References
- Achenbach TM. Manual for the child behavior checklist/14–18 and 1991 profile. Burlington, VT: University of Vermont Department of Psychiatry; 1991. [Google Scholar]
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4. Washington, DC: Author; 1994. [Google Scholar]
- Domenech-Llaberia E, Jane C, Canals J, Ballespi S, Esparo G, Garralda E. Parental reports of somatic symptoms in preschool children: Prevalence and associations in a Spanish sample. Journal of the American Academy of Child and Adolescent Psychiatry. 2004;43(5):598–604. doi: 10.1097/00004583-200405000-00013. [DOI] [PubMed] [Google Scholar]
- Essau CA. Somatoform disorders. In: Essau CA, editor. Child and Adolescent Psychopathology: Theoretical and Clinical Implications. New York: Routledge; 2006. pp. 221–245. [Google Scholar]
- Ginsburg GS, Riddle MA, Davies M. Somatic symptoms in children and adolescents with anxiety disorders. Journal of the American Academy of Child and Adolescent Psychiatry. 2006;45(10):1179–1187. doi: 10.1097/01.chi.0000231974.43966.6e. [DOI] [PubMed] [Google Scholar]
- Hukkanen R, Sourander A, Bergroth L. Suicidal ideation and behavior in children’s homes. Nordic Journal of Psychiatry. 2003;57(2):131–137. doi: 10.1080/08039480310000969. [DOI] [PubMed] [Google Scholar]
- Knishkowy B, Palti H, Tima C, Adler B, Gofin R. Symptom clusters among young adolescents. Adolescence. 1995;30(118):351–362. [PubMed] [Google Scholar]
- Lieb R, Mastaler M, Wittchen H. Do somatoform disorders affect adolescents and young adults? First epidemiological findings based on a representative population sample. Verhaltenstherapie. 1998;8(2):81–93. [Google Scholar]
- Masi G, Favilla L, Millepiedi S, Mucci M. Somatic symptoms in children and adolescents referred for emotional and behavioral disorders. Psychiatry: Interpersonal and Biological Processes. 2000;63(2):140–149. doi: 10.1080/00332747.2000.11024905. [DOI] [PubMed] [Google Scholar]
- Mulvaney S, Lambert EW, Garber J, Walker LS. Trajectories of symptoms and impairment for pediatric patients with functional abdominal pain: A 5-year longitudinal study. Journal of the American Academy of Child and Adolescent Psychiatry. 2006;45(6):737–744. doi: 10.1097/10.chi.0000214192.57993.06. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Postilnik I, Eisman HD, Price R, Fogel J. An algorithm for defining somatization in children. Journal of the Canadian Academy of Child and Adolescent Psychiatry. 2006;15(2):64–74. Accessed May 15, 2007. Available at URL: http://www.cacap-acpea.org/onottaca/doc.nsf/files/4D9AC1A899B10618872571A800797BF6/$file/2006MayAlgorithmforDefiningSomatization.pdf. [PMC free article] [PubMed]
- Robins PM, Schoff KM, Glutting JJ, Abelkop AS. Discriminative validity of the behavioral assessment system for children-parent rating scales in children with recurrent abdominal pain and matched controls. Psychology in the Schools. 2003;40(2):145–154. [Google Scholar]
- SPSS. Version 11.5. Chicago: Author; 2002. [Google Scholar]
- Stata/SE. Version 9.2. College Station, TX: StataCorp LE; 2006. [Google Scholar]
- Vervoot T, Goubert L, Eccleston C, Bijttebier P, Crombez G. Catastrophic thinking about pain is independently associated with pain severity, disability, and somatic complaints in school children and children with chronic pain. Journal of Pediatric Psychology. 2006;31(7):674–683. doi: 10.1093/jpepsy/jsj059. [DOI] [PubMed] [Google Scholar]
- Xing-xing Z, Zhu-wen Y, Jian-jiang Z, Xiu-yin W, Xi-qiang D. A preliminary study on mental health in children with precocious puberty and their parents. Chinese Journal of Clinical Psychology. 2005;13(3):348–349. [Google Scholar]