Abstract
Recently, mutations in the progranulin (PGRN) gene were found to cause familial and apparently sporadic frontotemporal lobe dementia (FTLD). Moreover, missense changes in PGRN were identified in patients with motor neuron degeneration, a condition that is related to FTLD. Most mutations identified in patients with FTLD until now have been null mutations. However, it remains unknown whether PGRN protein levels are reduced in the central nervous system from such patients. The effects of PGRN on neurons also remain to be established. We report that PGRN levels are reduced in the cerebrospinal fluid from FTLD patients carrying a PGRN mutation. We observe that PGRN and GRN E (one of the proteolytic fragments of PGRN) promote neuronal survival and enhance neurite outgrowth in cultured neurons. These results demonstrate that PGRN/GRN is a neurotrophic factor with activities that may be involved in the development of the nervous system and in neurodegeneration.
Introduction
Progranulin (PGRN) is a glycosylated protein released by a variety of cells. It contains a signal peptide and 7.5 tandem repeats of highly conserved granulin motifs each with 12 cysteine residues (Bateman et al., 1990; Shoyab et al., 1990; Bhandari et al., 1992; Plowman et al., 1992; He and Bateman, 2003). PGRN is widely expressed (Bhandari et al., 1993; Daniel et al., 2000) and has been implicated in many processes, such as development, tumor proliferation, wound healing, and inflammation (Bateman and Bennett, 1998; He and Bateman, 2003; Ahmed et al., 2007). In peripheral tissues, extracellular proteases, such as elastase, were shown to be able to cleave PGRN into several GRNs (GRN A–F and paragranulin), which probably have separate functions (Zhu et al., 2002; He and Bateman, 2003). In models of wound healing, secreted leukocyte protease inhibitor (SLPI) prevents PGRN processing through inhibition of elastase enzymatic activity and by binding PGRN and thus sequestering it from elastase (Zhu et al., 2002; He and Bateman, 2003).
Little is known about the role of PGRN in the central nervous system. PGRN is widely expressed during early neural development (Daniel et al., 2003) but later on its expression becomes restricted to defined neuronal populations, such as cortical and hippocampal pyramidal neurons and Purkinje cells (Daniel et al., 2000). It has been implicated in the sexual differentiation of the brain (Suzuki and Nishiahara, 2002). PGRN is up-regulated in activated microglial cells (Baker and Manuelidis, 2003; Baker et al., 2006; Mackenzie et al., 2006; Mukherjee et al., 2006) but not in astrocytes or oligodendrocytes.
Recently the interest in PGRN was raised because of the discovery of null mutations in the PGRN gene as a common cause of autosomal dominant tau-negative frontotemporal lobe dementia (FTLD; Baker et al., 2006; Cruts et al., 2006; Gass et al., 2006; Mukherjee et al., 2006; Pickering-Brown et al., 2006; Bronner et al., 2007; van der Zee et al., 2007). Furthermore, null mutations were also found in apparently sporadic patients (Le Ber et al., 2007). The majority of FTLD-causing mutations in PGRN are predicted to cause functional null alleles with premature termination of the coding sequence followed by nonsense-mediated decay of the mutant mRNA (Baker et al., 2006; Cruts et al., 2006). Therefore, haploinsufficiency with reduced PGRN-induced neuronal survival is thought to cause neurodegeneration. Missense mutations in PGRN have been identified as well. They were found in some patients with FTLD, with or without amyotrophic lateral sclerosis (ALS; Spina et al., 2007; van der Zee et al., 2007), and in rare ALS patients (Schymick et al., 2007; Sleegers et al., 2008). The pathogenetic nature of these missense mutations remains to be demonstrated. It was recently shown that several of these missense mutations reduce the release of PGRN and thus also give rise to insufficient availability of PGRN (Shankaran et al., 2008).
Whether PGRN levels are indeed reduced in the central nervous system of patients with null mutations requires confirmation and whether PGRN can directly affect neurons has not yet been shown. We therefore measured PGRN levels in the cerebrospinal fluid (CSF) from patients with PGRN mutations and controls and explored the potential neurotrophic effects of PGRN. The effects of exogenous PGRN and one of its proteolytic fragments (GRN E) were studied in cortical neurons and spinal motor neurons, the two types of neurons relevant for FTLD and ALS.
Results and discussion
PGRN protein levels in the CSF from patients and controls
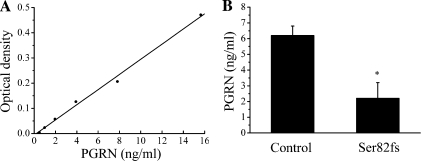
To measure PGRN protein levels, we developed an ELISA assay using a monoclonal PGRN antibody to coat 96-well plates, a polyclonal biotinylated PGRN antibody to detect the signal, and human recombinant PGRN as standard (Fig. 1 A). PGRN protein was detectable in CSF and was measured in the CSF from three patients carrying the Ser82fs mutation in PGRN and from 24 controls. The optical densities were 0.08 ± 0.04 and 0.23 ± 0.02 for patients and controls, respectively (P = 0.004). This corresponded to 2.2 ± 1.0 and 6.2 ± 0.6 ng/ml in patients and controls, respectively (P = 0.04; Fig. 1 B). The clearly reduced levels in patients with the Ser82fs mutation are in agreement with the predicted nonsense-mediated mRNA decay caused by the premature translation termination, resulting in reduced protein levels.
Figure 1.
Measurement of PGRN levels in the CSF by ELISA. (A) Example of standard curve of recombinant PGRN (R2 = 0.99). (B) Mean PGRN levels in controls (n = 24) and patients with a Ser82fs mutation (n = 3; *, P = 0.04). Error bars show mean ± SEM.
Effect of PGRN on neuronal survival
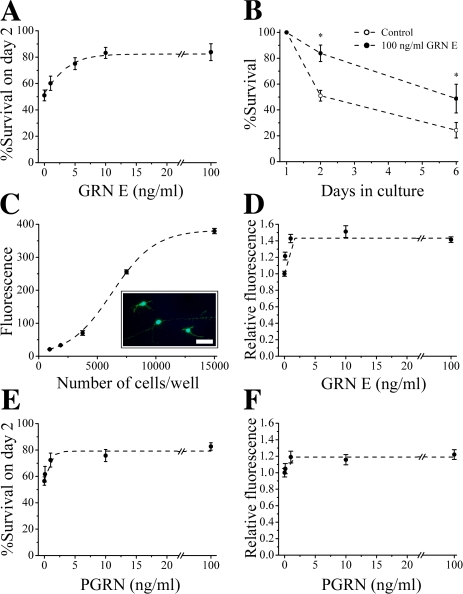
Although PGRN was shown to induce proliferation of PC-12 (rat adrenal gland pheochromocytoma) and SK-N-DZ (human brain neuroblastoma) cells (Daniel et al., 2000) and to inhibit apoptosis of tumor cells (He et al., 2002; Tangkeangsirisin et al., 2004), the effects of PGRN on neurons have not been established. To explore the neurotrophic potential of PGRN, we studied the effects of recombinant GRN E (aa 494–594 of PGRN, a functional proteolytic fragment of PGRN) and full-length PGRN (only lacking the first 18 aa, which code for the signal peptide) in monocultures of rat motor and cortical neurons. To reduce potential confounding effects from other growth factors, neurons were treated with GRN E or PGRN in serum-free medium with no other recombinant growth factors added. Motor neurons isolated from the ventral spinal cord were seeded at low density allowing reliable quantification of survival by counting experiments (Van Den Bosch et al., 2004; Van Damme et al., 2007). GRN E was added to these cultures on day 1 in culture and was found to support neuronal survival in a dose-dependent manner (Fig. 2 A). This neurotrophic effect was still visible after 1 wk, a time point at which only a limited number of neurons in these serum-free and neurotrophin-free cultures survive (Fig. 2 B). The maximal dose of GRN E increased neuronal survival by 64% on day 2 and by 101% on day 6.
Figure 2.
PGRN/GRN improves neuronal survival. (A) Effect of GRN E on survival of motor neurons on day 2 in culture normalized to survival on day 1 (n = 5–11; R2 = 0.99). (B) Effect of GRN E on the survival of motor neurons at different time points in culture (n = 5–11; *, P < 0.03). (C) Fluorescence (fluorescein counts/1,000) emitted by cortical neurons seeded in different densities after loading with calcein-AM on day 2 in culture (n = 5; R2 = 0.99; inset shows neurons loaded with calcein; Bar, 50 μm). (D) Effect of GRN E on fluorescence of cortical neurons on day 2 in culture normalized to untreated control (n = 8–15; R2 = 0.98). (E) Effect of PGRN on survival of motor neurons (n = 6–10; R2 = 0.95). (F) Effect of PGRN on survival of cortical neurons (n = 9; R2 = 0.95). Error bars show mean ± SEM.
Similar results were obtained in cortical neurons. To quantify survival of cortical cultures, a calcein-acetyoxymethyl (AM) assay was used (Bozyczko-Coyne et al., 1993; Lin et al., 2001). This assay proved to reliably reflect the number of living cells in culture, as shown in Fig. 2 C. To assure that the signal obtained was in the linear part of the assay, 10,000 cells per well were seeded for survival experiments. GRN E improved survival of cortical neurons by 41.4% (Fig. 2 D), confirming that the GRN E proteolytic fragment of PGRN has neurotrophic properties.
The full-length precursor, PGRN, exerted similar neurotrophic properties, both in motor and cortical neurons (Fig. 2, E and F). The maximal effect observed was a 38.5 and 22.0% increase in neuronal survival for motor and cortical neurons, respectively.
The effects of GRN E and PGRN on motor and cortical neurons were dose-dependent and the ED50 (0.1–3 ng/ml) approximated the ED50 of the proliferative effects on cell lines reported previously (Zhou et al., 1993).
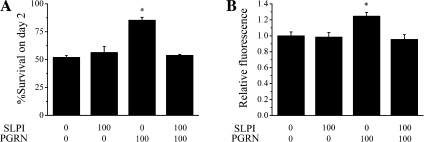
In wound healing, SLPI was shown to block PGRN processing both by inhibiting the proteolytic activity of elastase and by direct binding to PGRN (Zhu et al., 2002). We therefore investigated the effect of SLPI on the effects of PGRN in neuronal cultures and found that coadministration of SLPI abolished the neurotrophic effects of PGRN on both motor neurons and cortical neurons (Fig. 3, A and B). This suggests that proteolysis of PGRN is needed for it to have neurotrophic effects. Alternatively, because of its dual actions, SLPI may scavenge PGRN and thus keep PGRN from exerting its neurotrophic effect.
Figure 3.
Inhibition of PGRN by SLPI abolishes its neurotrophic properties. (A and B) Effect of SLPI (ng/ml) on the neurotrophic properties of PGRN (ng/ml) in motor neurons (A; n = 3–4; *, P < 0.001) and cortical neurons (B; n = 6; *, P < 0.01). Error bars show mean ± SEM.
Effect of PGRN on neurite outgrowth
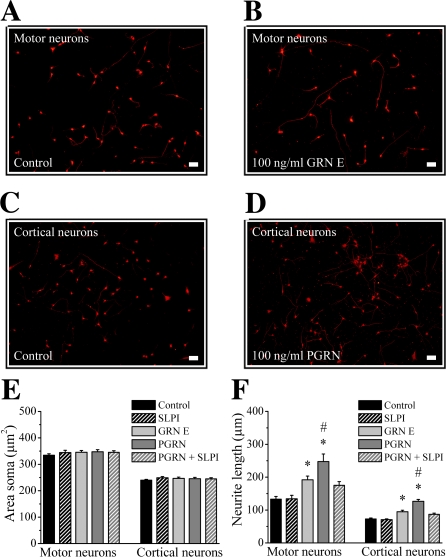
To study the effect of PGRN/GRN on neurite outgrowth, motor and cortical neuronal cultures were treated with GRN E or PGRN on day 0 and cells were stained for neurofilament heavy chain (NF-H) after 24 h. This allowed us to quantify the size of the soma and the length of neurites present (Fig. 4, A–D). GRN E and PGRN had no effect on the size of the cell soma. Both molecules increased the maximal neurite length, an effect that was especially apparent after the treatment of cells with full-length PGRN (Fig. 4, E and F). Again, the neurite outgrowth–stimulating effect of PGRN was inhibited by SLPI (Fig. 4 F).
Figure 4.
Effect of PGRN/GRN on soma size and neurite outgrowth. (A–D) NF-H staining of motor neuron (A and B) and cortical culture (C and D) treated with GRN E (B), PGRN (D), or control (A and C; Bar, 50 μm). (E and F) Effect of 100 ng/ml GRN E or PGRN (in the absence and presence of 100 ng/ml SLPI) on soma size (E) and maximal neurite length (F; n = 109–476; *, significantly different from control [P < 0.001]; #, significantly different from GRN E [P < 0.03]). Error bars show mean ± SEM.
From these experiments, it is clear that neurite length is mainly affected by PGRN and, to a lesser extent, by GRN E, whereas the opposite was true for the effect on neuronal survival. This differential effect of GRN E and PGRN on neuronal survival and axonal outgrowth, respectively, supports the hypothesis that different GRNs and their precursors may have distinct biological functions (Zhu et al., 2002).
Recently, PGRN-deficient mice have been generated (Kayasuga et al., 2007). These mice develop normally and do not show behavioral or motor abnormalities until 11 wk of age. However, it remains to be seen whether these animals develop axonal loss or neurodegeneration as they age.
Our results demonstrate that PGRN/GRN is a neurotrophic factor that enhances neuronal survival and axonal outgrowth. It supports the hypothesis that a relative lack of PGRN in patients with PGRN mutations may alter the integrity of neurites and lead to neurodegeneration. Mechanisms other than the lack of neurotrophic effect resulting from PGRN shortage may play a role in PGRN-associated neurodegeneration as well. In a recent study, PGRN knockdown was found to induce caspase-dependent cleavage of TDP-43 with accumulation of TDP-43 fragments (Zhang et al., 2007), similar to what is seen in FTLD and ALS (Neumann et al., 2006).
Although insufficient trophic support for neurons has been an appealing hypothesis for the pathogenesis of neurodegenerative disorders and the premise for many therapeutic strategies (Vande Velde and Cleveland, 2005), PGRN is the only neurotrophic factor identified to cause human disease through null mutations and haploinsufficiency. Therefore, it is warranted to investigate the therapeutic potential of PGRN for neurodegenerative disorders.
Materials and methods
PGRN ELISA
CSF samples from three FTLD patients caused by null mutations in PGRN and 24 controls were obtained after informed consent and approval by the local ethical committee. The PGRN levels were measured by ELISA. To do so, 96-well plates were coated with monoclonal anti-PGRN antibody (R&D Systems) blocked with 1% BSA before samples and standard (recombinant human PGRN; R&D Systems) were loaded. Afterward, bound PGRN was detected using biotinylated polyclonal anti-PGRN antibody (R&D Systems), avidin–biotin–peroxidase complex, and ortho-phenylenediamine. Absorbance was measured at 490 nm. Western blots stained with the antibodies used in this assay showed that only recombinant PGRN was recognized, not recombinant GRN E or PGRN cleavage products obtained by elastase treatment (1 U/ml for 30 min at 25°C; Athens Research & Technology).
Neuronal cultures
Monocultures of cortical and motor neurons were prepared from 14-d-old Wistar rat embryos as previously described (Van Damme et al., 2003, 2007; Van Den Bosch et al., 2004) and plated in culture dishes (40,000 cells per dish for spinal cultures) or 96-well plates (10,000 cells per well) coated with poly-l-ornithine and laminin. Ventral spinal cords were dissected from rat embryos and dissociated enzymatically and mechanically. A motor neuron–enriched neuronal population was obtained by centrifugation on a 6.5% Optiprep cushion. For cortical cultures, the cortex was dissociated by trypsinization and trituration but the density centrifugation was omitted. The culture medium consisted of L15 supplemented with 0.2% sodium bicarbonate, 3.6 mg/ml glucose, 20 nM progesterone, 5 μg/ml insulin, 0.1 mM putrescine, 0.1 mg/ml conalbumin, 30 nM sodium selenite, 100 U/ml penicillin, 100 μg/ml streptomycin, 5% chick embryo extract, 2% and horse serum. No horse serum was added in the serum-free medium, which still contained chick embryo extract. Cultures were kept in a 7% CO2 humidified incubator at 37°C. Most cells in culture stained positive for NF-H and neuron-specific nuclear protein (NeuN) on day 1 after seeding. Few cells stained positive for the astroglial marker glial fibrillary acidic protein (GFAP) or the oligodendroglial marker O4.
Neuronal survival
The survival of monocultures of motor neurons was quantified by direct counting of unfixed cells under phase contrast, as previously described (Van Den Bosch et al., 2004). Neurons in a marked area of 1 cm2 were counted before (on day 1 after seeding) application of PGRN/GRN or control. After counting on day 1, the medium was replaced by serum-free medium. Because partial recombinant human PGRN (coding for GRN E) was dissolved in buffer containing reduced glutathione, this was added to the corresponding controls as well. The relative survival was calculated as the number of cells on day 2 or 6 in culture divided by the number of cells on day 1.
Survival of cortical neurons was quantified using a calcein assay (Bozyczko-Coyne et al., 1993; Lin et al., 2001). On day 1 in culture, neuronal cultures seeded in 96-well plates were treated with PGRN/GRN or control buffer. Neuronal survival was quantified 24 h later. On day 2 in culture, cells were loaded with 2 μM calcein-AM in the culture medium for 1 h at 37°C. After replacement of the medium with PBS, fluorescence was measured on a microplate reader (excitation, 480 nm; emission, 535 nm). After subtraction of background signal from wells without cells, the values obtained were normalized to untreated control wells. For every condition, the mean of at least five wells was taken (considered as n = 1).
Immunocytochemistry
Immunostainings were performed as previously described (Van Damme et al., 2007). Cells were fixed for 20 min using 4% PFA. Cultures were incubated with NF-H antibody (1:400; rabbit polyclonal), NeuN antibody (1:1,000; mouse monoclonal), GFAP antibody (1:1,000; mouse monoclonal), and O4 (1:500; mouse monoclonal) overnight. The appropriate Alexa555- and Alexa488-labeled antibodies (1:500) were used to develop the stain.
Quantification of neurite length
Motor and cortical neuronal cultures were exposed to recombinant PGRN/GRN in serum-free medium immediately after seeding for 24 h and stained for NF-H on day 1 in culture. Photographs of representative areas of the culture were taken on an upright microscope (DMRB; Leica) at a magnification of 10 (0.3 NA; PL Fluotar; Leica) at room temperature using a camera (DXM 1200; Nikon). The size of the cell soma and the longest neurite of more than 100 neurons per experimental condition were measured on the obtained digital pictures using Lucia imaging software (version 4.60; Laboratory Imaging).
Materials and statistics
Media and additives were obtained from Invitrogen. All other chemicals were obtained from Sigma-Aldrich. Partial recombinant human PGRN (aa 494–594, coding for GRN E and flanking regions) was obtained from Abnova Corporation. Full-length recombinant human PGRN (aa 18–593) was obtained from R&D Systems. NF-H and GFAP antibodies were obtained from Sigma-Aldrich. NeuN antibody was obtained from Millipore and anti-oligodendrocyte marker 04 was obtained from R&D Systems. Alexa-labeled secondary antibodies were obtained from Invitrogen.
Mean data are shown as mean ± SEM and Student's t tests were used to calculate significance. When more than two groups were compared, a one-way analysis of variance with Tukey-Kramer multiple comparisons was used.
Acknowledgments
We thank W. Scheveneels and N. Hersmus for their excellent technical assistance.
This work was supported by grants from the Fund for Scientific Research Flanders, the University of Leuven, the Belgian government (Interuniversity Attraction Poles, program P6/43 of the Belgian Federal Science Policy Office), the Stem Cell Institute Leuven, and the ALS Association. E. Bogaert, P. Van Damme, and D. Lambrechts are supported by the Fund for Scientific Research Flanders. W. Robberecht is supported through the E. von Behring Chair for Neuromuscular and Neurodegenerative Disorders.
Abbreviations used in this paper: ALS, amyotrophic lateral sclerosis; AM, acetyoxymethyl; CSF, cerebrospinal fluid; FTLD, frontotemporal lobe dementia; GFAP, glial fibrillary acidic protein; GRN, granulin; NF-H, neurofilament heavy chain; PGRN, progranulin; SLPI, secreted leucocyte protease inhibitor.
References
- Ahmed, Z., I.R. Mackenzie, M.L. Hutton, and D.W. Dickson. 2007. Progranulin in frontotemporal lobar degeneration and neuroinflammation. J. Neuroinflammation. 4:7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Baker, C.A., and L. Manuelidis. 2003. Unique inflammatory RNA profiles of microglia in Creutzfeldt-Jakob disease. Proc. Natl. Acad. Sci. USA. 100:675–679. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Baker, M., I.R. Mackenzie, S.M. Pickering-Brown, J. Gass, R. Rademakers, C. Lindholm, J. Snowden, J. Adamson, A.D. Sadovnick, S. Rollinson, et al. 2006. Mutations in progranulin cause tau-negative frontotemporal dementia linked to chromosome 17. Nature. 442:916–919. [DOI] [PubMed] [Google Scholar]
- Bateman, A., and H.P. Bennett. 1998. Granulins: the structure and function of an emerging family of growth factors. J. Endocrinol. 158:145–151. [DOI] [PubMed] [Google Scholar]
- Bateman, A., D. Belcourt, H. Bennett, C. Lazure, and S. Solomon. 1990. Granulins, a novel class of peptide from leukocytes. Biochem. Biophys. Res. Commun. 173:1161–1168. [DOI] [PubMed] [Google Scholar]
- Bhandari, V., R.G. Palfree, and A. Bateman. 1992. Isolation and sequence of the granulin precursor cDNA from human bone marrow reveals tandem cysteine-rich granulin domains. Proc. Natl. Acad. Sci. USA. 89:1715–1719. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bhandari, V., A. Giaid, and A. Bateman. 1993. The complementary deoxyribonucleic acid sequence, tissue distribution, and cellular localization of the rat granulin precursor. Endocrinology. 133:2682–2689. [DOI] [PubMed] [Google Scholar]
- Bozyczko-Coyne, D., B.W. McKenna, T.J. Connors, and N.T. Neff. 1993. A rapid fluorometric assay to measure neuronal survival in vitro. J. Neurosci. Methods. 50:205–216. [DOI] [PubMed] [Google Scholar]
- Bronner, I.F., P. Rizzu, H. Seelaar, S.E. van Mil, B. Anar, A. Azmani, L.D. Kaat, S. Rosso, P. Heutink, and J.C. van Swieten. 2007. Progranulin mutations in Dutch familial frontotemporal lobar degeneration. Eur. J. Hum. Genet. 15:369–374. [DOI] [PubMed] [Google Scholar]
- Cruts, M., I. Gijselinck, J. van der Zee, S. Engelborghs, H. Wils, D. Pirici, R. Rademakers, R. Vandenberghe, B. Dermaut, J.J. Martin, et al. 2006. Null mutations in progranulin cause ubiquitin-positive frontotemporal dementia linked to chromosome 17q21. Nature. 442:920–924. [DOI] [PubMed] [Google Scholar]
- Daniel, R., Z. He, K.P. Carmichael, J. Halper, and A. Bateman. 2000. Cellular localization of gene expression for progranulin. J. Histochem. Cytochem. 48:999–1009. [DOI] [PubMed] [Google Scholar]
- Daniel, R., E. Daniels, Z. He, and A. Bateman. 2003. Progranulin (acrogranin/PC cell-derived growth factor/granulin-epithelin precursor) is expressed in the placenta, epidermis, microvasculature, and brain during murine development. Dev. Dyn. 227:593–599. [DOI] [PubMed] [Google Scholar]
- Gass, J., A. Cannon, I.R. Mackenzie, B. Boeve, M. Baker, J. Adamson, R. Crook, S. Melquist, K. Kuntz, R. Petersen, et al. 2006. Mutations in progranulin are a major cause of ubiquitin-positive frontotemporal lobar degeneration. Hum. Mol. Genet. 15:2988–3001. [DOI] [PubMed] [Google Scholar]
- He, Z., and A. Bateman. 2003. Progranulin (granulin-epithelin precursor, PC-cell-derived growth factor, acrogranin) mediates tissue repair and tumorigenesis. J. Mol. Med. 81:600–612. [DOI] [PubMed] [Google Scholar]
- He, Z., A. Ismail, L. Kriazhev, G. Sadvakassova, and A. Bateman. 2002. Progranulin (PC-cell-derived growth factor/acrogranin) regulates invasion and cell survival. Cancer Res. 62:5590–5596. [PubMed] [Google Scholar]
- Kayasuga, Y., S. Chiba, M. Suzuki, T. Kikusui, T. Matsuwaki, K. Yamanouchi, H. Kotaki, R. Horai, Y. Iwakura, and M. Nishihara. 2007. Alteration of behavioural phenotype in mice by targeted disruption of the progranulin gene. Behav. Brain Res. 185:110–118. [DOI] [PubMed] [Google Scholar]
- Le Ber, I., J. van der Zee, D. Hannequin, I. Gijselinck, D. Campion, M. Puel, A. Laquerriere, T. De Pooter, A. Camuzat, M. Van den Broeck, et al. 2007. Progranulin null mutations in both sporadic and familial frontotemporal dementia. Hum. Mutat. 28:846–855. [DOI] [PubMed] [Google Scholar]
- Lin, H., R. Bhatia, and R. Lal. 2001. Amyloid beta protein forms ion channels: implications for Alzheimer's disease pathophysiology. FASEB J. 15:2433–2444. [DOI] [PubMed] [Google Scholar]
- Mackenzie, I.R., M. Baker, S. Pickering-Brown, G.Y. Hsiung, C. Lindholm, E. Dwosh, J. Gass, A. Cannon, R. Rademakers, M. Hutton, and H.H. Feldman. 2006. The neuropathology of frontotemporal lobar degeneration caused by mutations in the progranulin gene. Brain. 129:3081–3090. [DOI] [PubMed] [Google Scholar]
- Mukherjee, O., P. Pastor, N.J. Cairns, S. Chakraverty, J.S. Kauwe, S. Shears, M.I. Behrens, J. Budde, A.L. Hinrichs, J. Norton, et al. 2006. HDDD2 is a familial frontotemporal lobar degeneration with ubiquitin-positive, tau-negative inclusions caused by a missense mutation in the signal peptide of progranulin. Ann. Neurol. 60:314–322. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Neumann, M., D.M. Sampathu, L.K. Kwong, A.C. Truax, M.C. Micsenyi, T.T. Chou, J. Bruce, T. Schuck, M. Grossman, C.M. Clark, et al. 2006. Ubiquitinated TDP-43 in frontotemporal lobar degeneration and amyotrophic lateral sclerosis. Science. 314:130–133. [DOI] [PubMed] [Google Scholar]
- Pickering-Brown, S.M., M. Baker, J. Gass, B.F. Boeve, C.T. Loy, W.S. Brooks, I.R. Mackenzie, R.N. Martins, J.B. Kwok, G.M. Halliday, et al. 2006. Mutations in progranulin explain atypical phenotypes with variants in MAPT. Brain. 129:3124–3126. [DOI] [PubMed] [Google Scholar]
- Plowman, G.D., J.M. Green, M.G. Neubauer, S.D. Buckley, V.L. McDonald, G.J. Todaro, and M. Shoyab. 1992. The epithelin precursor encodes two proteins with opposing activities on epithelial cell growth. J. Biol. Chem. 267:13073–13078. [PubMed] [Google Scholar]
- Schymick, J.C., Y. Yang, P.M. Andersen, J.P. Vonsattel, M. Greenway, P. Momeni, J. Elder, A. Chio, G. Restagno, W. Robberecht, et al. 2007. Progranulin mutations and amyotrophic lateral sclerosis or amyotrophic lateral sclerosis-frontotemporal dementia phenotypes. J. Neurol. Neurosurg. Psychiatry. 78:754–756. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shankaran, S.S., A. Capell, A.T. Hruscha, K. Fellerer, M. Neumann, B. Schmid, and C. Haass. 2008. Missense mutations in the progranulin gene linked to frontotemporal lobar degeneration with ubiquitin-immunoreactive inclusions reduce progranulin production and secretion. J. Biol. Chem. 283:1744–1753. [DOI] [PubMed] [Google Scholar]
- Shoyab, M., V.L. McDonald, C. Byles, G.J. Todaro, and G.D. Plowman. 1990. Epithelins 1 and 2: isolation and characterization of two cysteine-rich growth-modulating proteins. Proc. Natl. Acad. Sci. USA. 87:7912–7916. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sleegers, K., N. Brouwers, S. Maurer-Stroh, M.A. van Es, P. Van Damme, P.W. van Vught, J. van der Zee, S. Serneels, T. De Pooter, M. Van den Broeck, et al. 2008. Progranulin genetic variability contributes to amyotrophic lateral sclerosis. Neurology. 10.1212/01.wnl.0000289191.54852.75. [DOI] [PubMed]
- Spina, S., J.R. Murrell, E.D. Huey, E.M. Wassermann, P. Pietrini, M.A. Baraibar, A.G. Barbeito, J.C. Troncoso, R. Vidal, B. Ghetti, and J. Grafman. 2007. Clinicopathologic features of frontotemporal dementia with progranulin sequence variation. Neurology. 68:820–827. [DOI] [PubMed] [Google Scholar]
- Suzuki, M., and M. Nishiahara. 2002. Granulin precursor gene: a sex steroid-inducible gene involved in sexual differentiation of the rat brain. Mol. Genet. Metab. 75:31–37. [DOI] [PubMed] [Google Scholar]
- Tangkeangsirisin, W., J. Hayashi, and G. Serrero. 2004. PC cell-derived growth factor mediates tamoxifen resistance and promotes tumor growth of human breast cancer cells. Cancer Res. 64:1737–1743. [DOI] [PubMed] [Google Scholar]
- Van Damme, P., G. Callewaert, J. Eggermont, W. Robberecht, and L. Van Den Bosch. 2003. Chloride influx aggravates Ca2+-dependent AMPA receptor-mediated motoneuron death. J. Neurosci. 23:4942–4950. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Van Damme, P., E. Bogaert, M. Dewil, N. Hersmus, D. Kiraly, W. Scheveneels, I. Bockx, D. Braeken, N. Verpoorten, K. Verhoeven, et al. 2007. Astrocytes regulate GluR2 expression in motor neurons and their vulnerability to excitotoxicity. Proc. Natl. Acad. Sci. USA. 104:14825–14830. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Van Den Bosch, L., E. Storkebaum, V. Vleminckx, L. Moons, L. Vanopdenbosch, W. Scheveneels, P. Carmeliet, and W. Robberecht. 2004. Effects of vascular endothelial growth factor (VEGF) on motor neuron degeneration. Neurobiol. Dis. 17:21–28. [DOI] [PubMed] [Google Scholar]
- van der Zee, J., I. Le Ber, S. Maurer-Stroh, S. Engelborghs, I. Gijselinck, A. Camuzat, N. Brouwers, R. Vandenberghe, K. Sleegers, D. Hannequin, et al. 2007. Mutations other than null mutations producing a pathogenic loss of progranulin in frontotemporal dementia. Hum. Mutat. 28:416. [DOI] [PubMed] [Google Scholar]
- Vande Velde, C., and D.W. Cleveland. 2005. VEGF: multitasking in ALS. Nat. Neurosci. 8:5–7. [DOI] [PubMed] [Google Scholar]
- Zhang, Y.J., Y.F. Xu, C.A. Dickey, E. Buratti, F. Baralle, R. Bailey, S. Pickering-Brown, D. Dickson, and L. Petrucelli. 2007. Progranulin mediates caspase-dependent cleavage of TAR DNA binding protein-43. J. Neurosci. 27:10530–10534. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhou, J., G. Gao, J.W. Crabb, and G. Serrero. 1993. Purification of an autocrine growth factor homologous with mouse epithelin precursor from a highly tumorigenic cell line. J. Biol. Chem. 268:10863–10869. [PubMed] [Google Scholar]
- Zhu, J., C. Nathan, W. Jin, D. Sim, G.S. Ashcroft, S.M. Wahl, L. Lacomis, H. Erdjument-Bromage, P. Tempst, C.D. Wright, and A. Ding. 2002. Conversion of proepithelin to epithelins: roles of SLPI and elastase in host defense and wound repair. Cell. 111:867–878. [DOI] [PubMed] [Google Scholar]