Abstract
Background
The relevance to coronary heart disease (CHD) of cytokines that govern inflammatory cascades, such as interleukin-6 (IL-6), may be underestimated because such mediators are short acting and prone to fluctuations. We evaluated associations of long-term circulating IL-6 levels with CHD risk (defined as nonfatal myocardial infarction [MI] or fatal CHD) in two population-based cohorts, involving serial measurements to enable correction for within-person variability. We updated a systematic review to put the new findings in context.
Methods and Findings
Measurements were made in samples obtained at baseline from 2,138 patients who had a first-ever nonfatal MI or died of CHD during follow-up, and from 4,267 controls in two cohorts comprising 24,230 participants. Correction for within-person variability was made using data from repeat measurements taken several years apart in several hundred participants. The year-to-year variability of IL-6 values within individuals was relatively high (regression dilution ratios of 0.41, 95% confidence interval [CI] 0.28–0.53, over 4 y, and 0.35, 95% CI 0.23–0.48, over 12 y). Ignoring this variability, we found an odds ratio for CHD, adjusted for several established risk factors, of 1.46 (95% CI 1.29–1.65) per 2 standard deviation (SD) increase of baseline IL-6 values, similar to that for baseline C-reactive protein. After correction for within-person variability, the odds ratio for CHD was 2.14 (95% CI 1.45–3.15) with long-term average (“usual”) IL-6, similar to those for some established risk factors. Increasing IL-6 levels were associated with progressively increasing CHD risk. An updated systematic review of electronic databases and other sources identified 15 relevant previous population-based prospective studies of IL-6 and clinical coronary outcomes (i.e., MI or coronary death). Including the two current studies, the 17 available prospective studies gave a combined odds ratio of 1.61 (95% CI 1.42–1.83) per 2 SD increase in baseline IL-6 (corresponding to an odds ratio of 3.34 [95% CI 2.45–4.56] per 2 SD increase in usual [long-term average] IL-6 levels).
Conclusions
Long-term IL-6 levels are associated with CHD risk about as strongly as are some major established risk factors, but causality remains uncertain. These findings highlight the potential relevance of IL-6–mediated pathways to CHD.
John Danesh and colleagues show that long-term IL-6 levels are associated with coronary heart disease risk, thus highlighting the potential relevance of IL-6−mediated pathways to coronary heart disease.
Editors' Summary
Background.
Coronary heart disease (CHD), the leading cause of death among adults in developed countries, kills one person in the US every minute. With age, “atherosclerotic plaques”—deposits of fats, calcium, and various cellular waste products—coat the walls of arteries, causing them to narrow and harden, interrupting blood flow through the body. When this occurs in the coronary arteries, which nourish the heart muscle, the end result is CHD. If a plaque breaks off the artery wall, it can get trapped in the arteries and completely stop the blood flow, causing death of the heart muscle. The technical term for this is “myocardial infarction” (MI), although it is more commonly known as a heart attack. Smoking, high blood pressure, high blood levels of cholesterol (a type of fat), being overweight, and being physically inactive all increase the risk of developing CHD, as do some inherited factors. Treatments for CHD include lifestyle changes (for example, losing weight and exercising regularly) and medications that lower blood pressure and blood cholesterol. In the worst cases, the narrowed artery can be widened using a device called a stent or surgically bypassed.
Why Was This Study Done?
Atherosclerosis might, at least partly, be an inflammatory condition. Inflammation—an immune response to injury characterized by swelling and redness—involves the production of proteins called “cytokines,” which attract cells of the immune system to the site of injury. In atherosclerosis, damage to the artery walls seems to trigger inflammation, which helps the atherosclerotic plaques grow. Because of the potential involvement of inflammation in atherosclerosis, increased levels of circulating cytokines might be associated with an increased risk of CHD. If they are, cytokines might provide a new therapeutic target for the treatment of CHD. In this study, the researchers have asked whether prolonged moderate increases in the cytokine interleukin-6 (IL-6) in the bloodstream are associated with CHD risk. IL-6, which is produced very early in inflammation, survives only briefly in the human body and its levels fluctuate within individuals. Consequently, its relevance to CHD has been unclear in previous studies.
What Did the Researchers Do and Find?
Between 1967 and 1991, nearly 25,000 healthy, mainly middle-aged people were enrolled into two studies—the Reykjavik Study and the British Regional Heart Study—and followed for about 20 years, during which time 2,138 people had a first-ever nonfatal heart attack or died of CHD. The researchers measured baseline IL-6 blood levels in these participants and in 4,267 similar participants who had not had a CHD event. They also measured IL-6 levels in 558 healthy participants several years into the study to determine a “regression dilution ratio” for IL-6. This ratio gives an idea of the year-to-year consistency of IL-6 levels. When the researchers used this ratio to estimate the impact of prolonged increases in IL-6 levels on CHD, they found that increased long-term IL-6 levels more than doubled the risk for CHD in their study populations. The researchers then combined these new results with those of 15 previous relevant studies. This combined analysis indicated very similar findings to those in the new data.
What Do These Findings Mean?
These findings indicate prolonged moderate increases in IL-6 levels are associated with risk of CHD as strongly as several major established risk factors, including blood pressure and blood cholesterol levels, but whether there is a cause-and-effect relationship remains unknown. More studies are needed to find out whether this result is generalisable to other populations, but the broad agreement between the Icelandic and British studies suggests that they should be. This study renews interest in IL-6–mediated inflammatory pathways and CHD.
Additional Information.
Please access these Web sites via the online version of this summary at http://dx.doi.org/10.1371/journal.pmed.0050078.
Read a related PLoS Medicine Perspective article
The MedlinePlus encyclopedia has pages on coronary heart disease and atherosclerosis (in English and Spanish)
Information is available from the US National Heart Lung and Blood Institute on coronary heart disease and atherosclerosis
Information for patients and caregivers is provided by the American Heart Association on all aspects of heart disease, including inflammation and heart disease
Information is available from the British Heart Foundation on heart disease and on keeping the heart healthy
Further details are available about the Reykjavik Study and the British Regional Heart Study
Wikipedia has pages on inflammation and on interleukin-6 (note that Wikipedia is a free online encyclopedia that anyone can edit; available in several languages)
Introduction
As atherosclerosis may be an inflammatory condition [1], there is interest in the relevance of various circulating inflammatory markers to cardiovascular diseases [2]. Inflammatory cascades are propagated by proximal mediators such as interleukin-6 (IL-6), a cytokine produced in various tissues. IL-6 exerts proinflammatory effects including stimulation of the liver to produce positive acute-phase proteins during tissue injury or infection [3–5]. Previous epidemiological studies of coronary heart disease (CHD) and inflammation have focused mainly on “downstream” acute phase reactants (e.g., fibrinogen [6] and C-reactive protein [7]) because they are comparatively stable within individuals over time. By contrast, investigation of IL-6 in CHD has been relatively limited because of its shorter half-life (<2 h) and greater within-person variability. Published prospective studies of IL-6 have yielded divergent odds ratios ranging from 1.0 to 3.0 [8–21]. However, as each report has typically comprised only a few hundred patients with CHD, the estimates involve wide, overlapping confidence intervals (CIs). A recent nonquantitative review [22] reported on published data from five prospective studies of IL-6 and CHD, but it comprised only about one-third of the currently published evidence, and it mixed results of studies involving different vascular outcomes and of different study designs. Even a more comprehensive and consistent review of published reports would not, however, have been able to assess appropriately IL-6–CHD associations, because no individual prospective study to our knowledge has yet made allowances for the cytokine's within-person variability. Owing to fluctuations in IL-6 values over time, comparisons using only baseline values may yield biased estimates of the true association, which can be corrected, for the most part, by using data from paired measurements [23–27] (see Methods).
We report new data on IL-6 levels from two population-based prospective cohorts, the Reykjavik Study and the British Regional Heart Study (BRHS), which together comprise 24,230 predominantly middle-aged individuals with an average of almost 20 years of follow-up per participant. After exclusion of participants with any evidence of baseline coronary disease or stroke, 2,138 incident cases of CHD were available for the present analyses, more than four times as many CHD cases as in the largest previous study [13]. Paired measurements were made in random samples of participants in both studies in order to quantify (and correct for) long-term variation in IL-6 levels. We contextualised our new data by conducting an updated systematic review of all prospective studies of IL-6 and CHD based only in essentially general populations, comprising a further 3,592 CHD cases (defined as myocardial infarction [MI] or death attributed to CHD by World Health Organization [WHO] or similar criteria). Furthermore, we used new data from serial measurements made in our two prospective studies to correct for within-person variability in the studies included in the meta-analysis. The focus of the current report is on the magnitude of the association of IL-6 levels with CHD (rather than on the separate issue of risk prediction).
Methods
Study Population
The Reykjavik Study and the BRHS were initiated in 1967 and 1978, respectively, and have each been described in detail previously [28,29]. In the Reykjavik Study, men and women born between 1907 and 1935, resident in Reykjavik, Iceland, and its adjacent communities on December 1, 1966, were identified in the national population register and were invited to participate in the study during five stages of recruitment between 1967 and 1991. A total of 8,888 male and 9,681 female participants aged 33–86 y without a history of MI were recruited (72% response rate). Nurses administered questionnaires, made physical measurements, recorded an electrocardiogram (ECG), performed spirometry, and collected fasting venous blood samples to prepare serum that was stored at −20 °C for subsequent analysis. History of diabetes was self-reported. All participants have been monitored subsequently for cause-specific mortality (ascertained from central registers on the basis of a death certificate; ICD-9 codes 410–414 were used for CHD death) and for cardiovascular morbidity (diagnosis of MI was based on MONICA criteria), with a loss to follow-up of only about 0.6% to date. The BRHS enrolled 7,735 men aged 40–59 y (response rate 78%) randomly selected from general practice registers in each of 24 British towns during 1978–1980. Nurses administered questionnaires, made physical measurements, recorded an ECG, performed spirometry, and collected nonfasting venous blood samples from 5,661 men in 18 of the towns. Serum was obtained from the baseline blood samples and stored at −20 °C for subsequent analysis. Participants were monitored for all-cause mortality (ascertained through the National Health Service central registers, using ICD-9 codes 410–414 for CHD) and for cardiovascular morbidity (using general practitioners' reports and records, with diagnosis of MI based on WHO criteria), with a loss to follow-up of less than 1% to date. History of diabetes was, again, self-reported. Relevant institutional review boards approved each study, and participants provided informed consent.
Laboratory Measurements
IL-6 measurements were made in the Reykjavik Study and BRHS on available serum samples, using a sensitive enzyme-linked immunosorbent assay (ELISA; R & D Systems) in the Glasgow laboratory by the same technicians blinded to participants' disease status. The intra-assay coefficient of variability was 7%, and the inter-assay coefficient of variability was 8%. Measurements were made in pairs of samples from a randomly selected subset of baseline participants in each study, comprising 258 participants in the BRHS (samples collected at a median interval of about 4 y apart) and 300 participants in the Reykjavik Study (samples collected at a median interval of about 12 y apart). Because the temperature of storage of the initial BRHS samples was −20 °C, whereas it was −70 °C at the resurvey, there was scope in this study for slight overestimation of within-person variability in IL-6 levels, encouraging comparison of its findings with those from the Reykjavik Study in which conditions at the two surveys were identical. Lipid and other biochemical measurements involved standard assays, as previously described [28–30].
Statistical Analyses
In both the Reykjavik Study and BRHS, two or three control participants were randomly selected and frequency matched to incident CHD cases in 5-y age bands (and, in the Reykjavik Study, on calendar year of recruitment and sex; and in the all-male BRHS by town of residence), thereby obtaining the same joint frequency distributions of these factors among controls and cases. To limit any biases due to preexisting disease, prespecified principal analyses were restricted to the 2,138 individuals with CHD and 4,267 control participants who did not have baseline evidence of CHD or stroke (i.e., without baseline ECG abnormalities or self-reported prevalent MI, stroke, or angina) in a nested case–control comparison. Subsidiary analyses excluded patients who had CHD outcomes in the first 5 y of follow-up. Odds ratios for CHD per 2 standard deviations (SDs) increase in the natural logarithm (loge) of IL-6 were calculated using unconditional logistic regression (Stata, version 9). The odds ratios for a 2 SD change is similar to a comparison of extreme thirds of IL-6 values in a population. Analyses to investigate the shape of the IL-6–CHD association were conducted for groups defined by fifths of baseline IL-6 values in controls, with corresponding 95% CIs estimated from floating variances that reflect the amount of information underlying each group (including the reference group) [31–33]. To avoid overadjustment, adjustment for other inflammatory markers (e.g., C-reactive protein) was reserved for subsidiary analyses.
Correction for Regression Dilution
Data from paired measurements in the Reykjavik Study, which coincided with approximately the midpoint of this study's follow-up duration, were used to quantify and to correct for within-person variability in IL-6 and other risk factors, which are likely to be measured with error owing to both within-person biological variability and laboratory variability. Adjusted regression dilution ratios were calculated by Rosner's regression method [26] to quantify the extent to which single measurements of the markers reflect their long term average (i.e., “usual”) levels. Paired measurements from the BRHS were used solely for comparison. Statistical significance of the difference in the strength of CHD association with IL-6 compared to other markers was determined from differences in the loge odds ratios per 2 SD increase in 2,000 bootstrap samples of the data [34]. Uncertainties in the regression dilution ratios calculated from the 300 participants with repeats in the Reykjavik Study were incorporated into the CIs for CHD associations by adding to the observed regression dilution ratios an error term sampled from the regression dilution ratio distribution on each bootstrap sample. This correction was applied to odds ratios both in the Reykjavik Study and in the BRHS. Correction for multivariate within-person variability in both IL-6 and error-prone confounders was achieved using a multivariable linear regression model [27] from which conditional expectations of usual levels of IL-6 and the error-prone confounders were predicted and then substituted in place of the baseline levels in the logistic model to obtain the corrected odds ratios. Odds ratios for loge C-reactive protein, loge erythrocyte sedimentation rate, von Willebrand factor, systolic blood pressure, and total cholesterol were calculated using methods described for loge IL-6.
Systematic Review
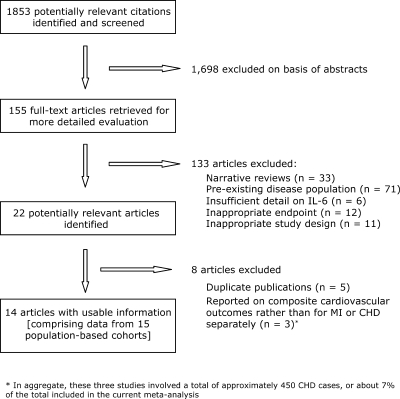
A systematic review of prospective, population-based studies of circulating IL-6 levels and CHD risk was conducted according to QUOROM (Quality of Reporting of Meta-analyses) guidelines (Texts S1 and S2). Studies published before May 2007 were sought using computer-based databases (MEDLINE, EMBASE, and Science Citation Index), and by scanning the reference lists of articles identified for all relevant studies and review articles (including meta-analyses). The computer-based searches combined free and MeSH search terms and combinations of key words related to IL-6 (e.g., “interleukin-6”, “IL-6”) and coronary disease (e.g., “coronary heart disease”, “myocardial ischemia”, “myocardial infarction”, “CHD”, “heart attack”, “MI”) without restricting language or publication date (flow chart in Figure 1). Data were extracted, where available, on study, geographic location, publication date, sample population, sampling methods (i.e., complete, random, etc.), sample source (plasma/serum), nature of sample (i.e., fresh or frozen, storage temperature), fasting status at time of blood sampling (duration of any fasting), blinding of lab worker to case versus control status, assay type, source and standard, analysis methods and units, case definition, any matching criteria, sample size (of total cohort and numbers with IL-6 measurements), numbers of cases (total, fatal CHD, nonfatal MI), numbers of controls, mean age, sex, time of baseline survey, duration of follow-up, mean or median IL-6 values, adjustment of confounders, and summary statistics. These details were extracted independently by two investigators using a prespecified data extraction form (Table S1). Discrepancies were resolved by discussion and by adjudication of a third reviewer.
Figure 1. QUOROM Flow Diagram Summarising the Search Strategy for Meta-analysis of IL-6 and CHD Outcomes in Generally Healthy Populations.
Prospective (cohort or “nested” case–control) studies based in essentially general populations (i.e., where participants were not selected on the basis of preexisting disease) with samples taken at baseline (i.e., prior to the occurrence of events) were eligible for inclusion in the current review. Analyses were restricted to studies with at least 1 y of follow-up and with outcomes defined as MI or coronary death. Three studies of IL-6 (comprising approximately 450 CHD cases or 7% of the total) [35–37] were excluded because they reported on composite cardiovascular outcomes rather than for MI or fatal CHD separately. To limit potential biases, analyses involved only within-study comparisons (i.e., cases and controls were directly compared only within each cohort). Results of the studies were combined using a random effects model. Associations of usual levels of IL-6 and CHD were estimated using correction factors derived from the Reykjavik Study and BRHS. Odds and hazard ratios were assumed to approximate the same measure of relative risk. Heterogeneity was quantified by the I2 statistic [38,39], and subsidiary subgroup analyses were conducted using metaregression [40] to investigate several study-level characteristics potentially explaining heterogeneity, including population sampling methods, duration of follow-up, source and type of IL-6 assay, blood storage temperature, geographical region, number of CHD cases, sex, degree of adjustment of other cardiovascular risk factors, and whether individuals with CHD at baseline were excluded from analysis. Test statistics from the metaregression based on the F-distribution were used to assess the statistical significance of these study-level characteristics in explaining heterogeneity.
Results
Baseline Correlates of IL-6 Levels
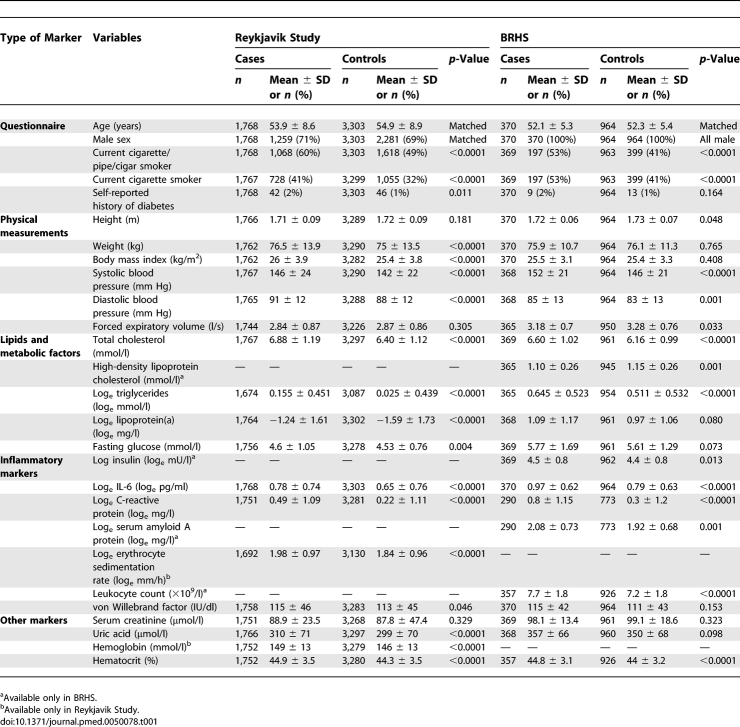
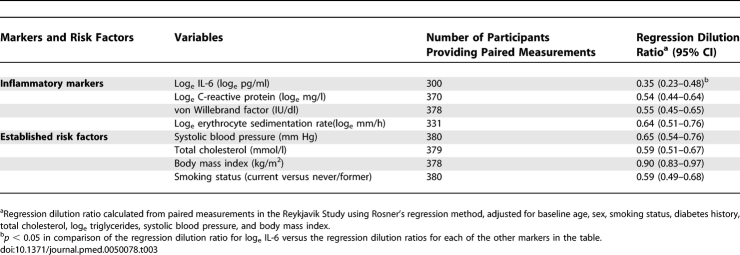
In the Reykjavik study, the median duration of follow-up of participants with CHD and control participants were 14 y and 23 y, respectively; in the BRHS, the corresponding durations were 9 y and 17 y, respectively. IL-6 levels were significantly higher in those with CHD than in control individuals in both the Reykjavik Study and in the BRHS, as were levels of several established cardiovascular risk factors (Table 1). Mean IL-6 levels were slightly higher in the male-only BRHS compared with the mixed-sex Reykjavik study. As shown in Table S2, baseline IL-6 levels were positively and highly significantly (p < 0.0001) associated with age, smoking, systolic blood pressure, and concentrations of triglycerides, fasting glucose, and several inflammatory markers (including C-reactive protein and the erythrocyte sedimentation rate), and somewhat less strongly with body mass index (p < 0.001). IL-6 levels were inversely associated with total cholesterol concentrations (p < 0.01). With the exception of correlations of IL-6 with smoking and measured inflammatory markers (for which the Pearson coefficient generally ranged between 0.20 and 0.43), even the highly significant correlations of IL-6 with other characteristics tended to be relatively small in magnitude.
Table 1.
Baseline Characteristics of Incident CHD Cases and Controls without Known Evidence of Coronary Disease at Baseline Nested within the Reykjavik Study and BRHS
Baseline IL-6 Levels and Incident CHD
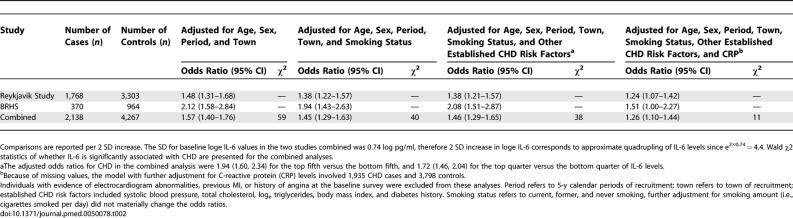
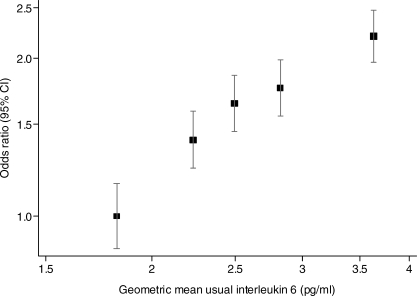
Table 2 provides odds ratios for CHD per 2 SD increase in baseline loge IL-6 levels. The minimally adjusted odds ratios (95% CI) for CHD per 2 SD increase were 1.48 (1.31–1.68) in the Reykjavik Study, 2.12 (1.58–2.84) in the BRHS, and 1.57 (1.40–1.76) in the combined dataset. After further adjustment for smoking status and several other established cardiovascular risk factors, the odds ratio per 2 SD increase fell to 1.38 (1.21–1.57) in the Reykjavik Study, 2.08 (1.51–2.87) in the BRHS, and 1.46 (1.29–1.65) in the combined dataset. Odds ratios did not change materially after exclusion of CHD outcomes recorded during the first 5 y of follow-up (odds ratio [95% CI] per 2 SD increase: 1.41 [1.24–1.60]) or in analyses including individuals with prevalent CHD at baseline (1.55 [1.38–1.73]). CHD risk increased continuously with increasing fifths of circulating IL-6 concentrations (Figure 2). Odds ratios did not vary substantially by levels of several established cardiovascular risk factors, except potentially by sex (p = 0.03) and cholesterol levels (p = 0.02), though the latter were only marginally significant findings in the context of multiple comparisons (Figure S1).
Table 2.
Relative Odds of CHD per 2 SD Increase in Baseline Loge IL-6 Levels in Participants without Known Coronary Disease at Baseline in the Reykjavik Study and the BRHS
Figure 2. Risk of CHD by Fifths of Baseline Circulating IL-6 Levels in a Pooled Analysis of Participants without Known CHD at Baseline in the Reykjavik Study and the BRHS.
Fifths were calculated on the basis of the distribution of controls in the combined dataset. CIs were calculated using floating variances. Sizes of data markers are proportional to the inverse of the variance of the odds ratios. Adjusted for cohort, age, sex, recruitment period, and town of recruitment.
Correction of Odds Ratios for Within-Person Variability
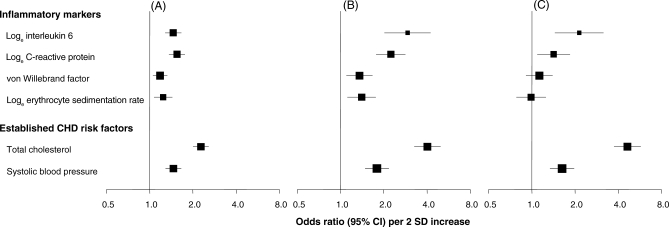
The regression dilution ratio for loge IL-6 was 0.41 (0.28–0.53) in 258 individuals who provided paired measurements on average 4 y apart in the BRHS, similar to the regression dilution ratio of 0.35 (0.23–0.48) in 300 individuals who provided paired measurements on average 12 y apart in the Reykjavik Study (mean loge IL-6 levels at baseline and at resurvey were 0.76 [SD 0.58] and 0.98 [SD 0.64] pg/ml, respectively, in BRHS and 0.63 [SD 0.70] and 0.88 [SD 0.68] pg/ml, respectively, in the Reykjavik Study). Similar point estimates for the regression dilution ratios of loge IL-6 levels over 4- and 12-y intervals may reflect that much of the variability in this marker is related to shorter-term rather than longer-term factors, although CIs around these estimates were relatively wide. As there were no signification associations between within-person differences in loge IL-6 levels and time intervals between measurements (p = 0.53), it is unlikely that increasing age of participants explains the generally higher mean loge IL-6 levels at resurvey. Table 3 indicates that the degree of within-person variability for IL-6 levels over 12 y was generally greater than those for other measured inflammatory markers and established cardiovascular risk factors (p < 0.05 for each comparison). Figure 3 (with numeric details shown in Table S3) shows three odds ratios for loge IL-6 and several other risk markers: (i) assessment 1 lists the odds ratio per 2 SD increase in baseline levels of the relevant risk marker adjusted for baseline levels of established risk factors (i.e., uncorrected for within-person variability in either exposure or confounder levels) (Figure 3A); (ii) assessment 2 lists the odds ratio per 2 SD increase in usual levels of the relevant risk marker adjusted for baseline levels of established risk factors (i.e., corrected for within-person variability only in levels of the exposure) (Figure 3B); and (iii) assessment 3 lists the odds ratio per 2 SD increase in usual levels of the relevant risk marker adjusted for usual levels of established risk factors (i.e., corrected for within-person variability in levels of both exposure and confounders) (Figure 3C). In assessment 1, the odds ratio for loge IL-6 is similar to those for loge C-reactive protein and systolic blood pressure, but lower than that for total cholesterol. In assessment 3, the odds ratio for loge IL-6 is comparable to those for some established risk factors. Figure 3 shows that the impact on odds ratios of correction for within-person variability in confounder levels varied in magnitude among risk markers, reflecting the markers' differing strength of associations with levels of confounders (and the differing degrees of within-person variability among such confounders [Table S3]). Sensitivity analyses allowing for uncertainty in the regression dilution ratios for the exposure variables (but not in the usual confounder levels, Table S3 legend) gave slightly wider CIs for the corrected associations.
Table 3.
Regression Dilution Ratios (95% CI) for IL-6, Other Measured Inflammatory Markers, and Some Established Cardiovascular Risk Factors, Based on Paired Measurements in Up to 380 Participants in the Reykjavik Study Who Provided Samples Approximately 12 Years Apart
Figure 3. Odds Ratios for CHD per 2 SD Increase in Several Inflammatory Markers and Established Cardiovascular Risk Factors Shown with Progressively Increasing Degrees of Correction for Within-person Variability in a Pooled Analysis of Participants without Known Coronary Disease at Baseline in the Reykjavik Study and the BRHS.
(A) Baseline exposure adjusted for baseline confounders.
(B) Usual exposure adjusted for baseline confounders.
(C) Usual exposure adjusted for usual confounders.
Sizes of data markers are proportional to the inverse of the variance of the odds ratios. Baseline (A) refers to measured values just at the initial examination. Usual (B and C) refers to an estimate of the long-term average values by employing data on repeat measurements from the Reykjavik Study (see Methods). Odds ratios are adjusted for cohort, age, sex, period and town of recruitment, smoking status, history of diabetes, total cholesterol, loge triglycerides, systolic blood pressure, and body mass index.
Updated Meta-analysis
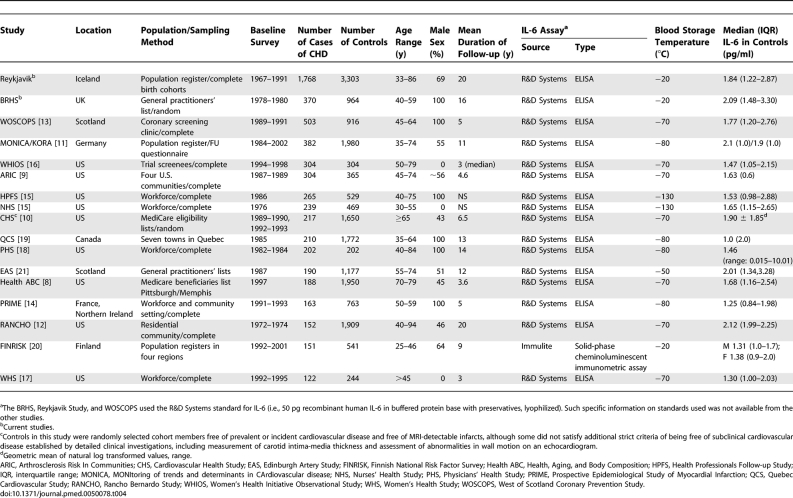
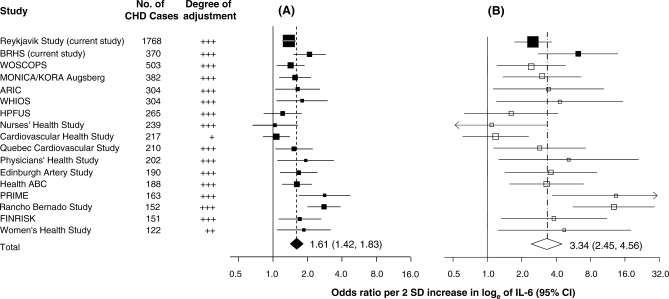
We identified 17 relevant studies [8–21] (including the two current studies, ten newly identified studies [8–13,17,19–21], and five studies [14–16,18] included in the previous published review [22]; flow chart in Figure 1). These studies comprised a total of 5,730 patients with MI or CHD death and 19,038 control individuals (weighted mean age at entry, 62 y; weighted mean follow-up, 6 y; Table 4). All studies, with one exception [20], used enzyme-linked immunosorbent assays produced by the same manufacturer, and all but two studies [10,17] adjusted for age, sex, and established cardiovascular risk factors. Using only within-study comparisons, the combined odds ratio (95% CI) was 1.61 (1.42–1.83) per 2 SD increase of baseline IL-6 levels and 3.34 (2.45–4.56) per 2 SD increase of usual IL-6 levels (Figure 4). Alternatively expressed, the odds ratios per 1 SD increase in baseline and usual IL-6 levels were 1.26 (1.19–1.35) and 1.83 (1.56–2.14), respectively. There was evidence of moderate heterogeneity among the 17 separate findings (I2 = 58%, 95% CI 28%–75%), but, as displayed in Figure S2, little of it was explained by differences in sample size (F1,15 = 0.91, p = 0.36), geographical location (F1,15 = 0.30, p = 0.59), population source (F2,14 = 0.76, p = 0.49), whether individuals with prevalent CHD at baseline were excluded from subsequent analyses (F1,15 = 2.08, p = 0.17), sex (F2,11 = 0.16, p = 0.85), reported duration of follow-up (F1,15 = 1.41, p = 0.25), or temperature of blood storage (F3,13 = 1.19, p = 0.35).
Table 4.
Characteristics of 17 Prospective Studies of Circulating IL-6 Concentrations and CHD Risk in Essentially General Populations
Figure 4. Summary of 17 Prospective Studies Reporting Adjusted Associations of CHD Risk per 2 SD Increase in Baseline IL-6 Levels and Usual IL-6 Levels, with Both Adjusted Only for Baseline Levels of Several Established Risk Factors.
(A) Baseline exposure adjusted for baseline confounders.
(B) Usual exposure adjusted for baseline confounders.
Baseline refers to measured values just at the initial examination. Usual refers to an estimate of the long-term average values. The correction for regression dilution (see Methods) in the two current studies (filled squares) was done using study-specific regression dilution ratios of 0.35 in Reykjavik study and 0.41 in the BRHS. A regression dilution ratio of 0.4 was assumed for other studies (empty squares) where such regression dilution ratio coefficients were unavailable. The odds ratio for a 1 SD increase in baseline and usual IL-6 levels are 1.26 (1.19–1.35) and 1.83 (1.56–2.14), respectively. Unshaded data markers were used in the second plot of this figure to indicate that correction for regression dilution involved use of coefficients from external studies, in contrast with the cohort-specific data on IL-6 variability available for the Reykjavik Study and BRHS. Sizes of data markers indicate the weight of each study in the analysis. Adjustment for within-person variability in levels of IL-6 and possible confounders requires access to individual participant data, currently available only in the Reykjavik Study and BRHS.
+, adjusted for age and sex; ++, adjusted for age, sex, and smoking status; +++, adjusted for age, sex, smoking status, and other established CHD risk factors; FINRISK, Finnish National Risk Factor Survey; HPFUS, Health Professionals' Follow-up Study; MONICA, MONItoring of trends and determinants in Cardiovascular disease; PRIME, Prospective Epidemiological Study of Myocardial Infarction; WHIOS, Women's Health Initiative Observational Study; WOSCOPS, West of Scotland Coronary Prevention Study.
Discussion
Previous reports on IL-6 levels and CHD have not been able to correct for within-person fluctuations in the levels of this short-acting cytokine, potentially yielding biased estimates. The present study, which made such correction on the basis of paired measurements of IL-6, indicates that long-term average (“usual”) IL-6 levels are about as strongly associated with CHD risk as are some major established risk factors. Increasing IL-6 levels are associated with progressively increasing odds ratios for CHD (i.e., there are continuous, approximately log-linear relationships). There are moderate associations of IL-6 levels with some established risk factors (notably smoking, diabetes, and dyslipidemia) and with several downstream inflammatory markers, consistent with the key role of IL-6 in mediating inflammatory cascades [3–5,41–44]. The current findings do not, of course, establish causality, but they may have implications for understanding disease mechanisms and for further research strategies.
By showing that pathways mediated by long-term IL-6 levels are associated with CHD risk about as strongly as are some major established risk factors, the current data reinforce interest in the connection between inflammatory pathways and cardiovascular diseases. The data also underscore the need for investigations of proximal inflammatory mediators that can quantify and correct for within-person variability. Serious underestimation is likely without such correction because, as demonstrated in the current study, the variability in IL-6 levels is substantially higher than for downstream inflammatory markers and several established CHD risk factors. Hence, given the central role of IL-6 levels in inflammatory pathways and its continuous association with CHD risk, it warrants further investigation as a plausible potential therapeutic target. There are initial reports of reductions in circulating IL-6 concentrations in randomised trials of statins, although these agents have other effects, notably lowering low-density lipoprotein cholesterol [45–47]. Future investigations should involve complementary strategies to help judge causality, such as large-scale studies of specific genetic markers as proxies for circulating IL-6 levels [48] (although it is now uncertain whether the −174 G/C IL-6 polymorphism is materially correlated with IL-6 levels [49]) and, possibly, use of selective IL-6 antagonists in early randomized trials [50], although the pleiotropic actions of IL-6 could complicate such an approach.
The strengths and potential limitations of the present report merit careful consideration. The current study reports new data from two population-based prospective cohorts comprising more than four times as many patients with first-ever CHD than in the previous largest report. Both the Reykjavik Study and BRHS identified participants in population registers, involved high response and follow-up rates, and involved robust ascertainment of incident MI and coronary death. Their broadly similar results support the generalisability of the current findings. Assay methods used in the current study were similar to those in earlier reports, yielding similar median IL-6 levels (Table 4). Although the current studies involved more prolonged blood storage than previous studies, they produced associations with CHD risk at least as strong as in earlier studies, arguing against underestimation due to sample degradation. Paired IL-6 (and other) measurements enabled approximate correction for within-person variability in a way that implies that long-term average IL-6 values are relevant to CHD risk, consistent with prevailing hypotheses of sustained low-grade inflammation, but it is not clear why mean loge IL-6 levels were generally higher at resurvey examinations.
In comparison with a previous nonquantitative review [22], the current meta-analysis involved almost five times as many incident CHD cases from population-based prospective studies (thereby enhancing statistical power), strictly defined CHD as MI or fatal CHD (thereby enhancing accuracy of disease classification), excluded (where possible) people with prevalent cardiovascular disease (thereby limiting potential biases), and explored in detail potential sources of heterogeneity (thereby probing possible causes of study diversity). This updated review suggests that the apparently divergent estimates reported in earlier studies were probably chiefly due to random error. Further studies are needed to test whether associations of IL-6 with CHD are importantly modified by lipid concentrations, as suggested by exploratory analyses in the current report. Studies are also needed with serial measurements in larger numbers of participants over different intervals in order to assess IL-6 variability in greater detail (e.g., assessment of any changes in mean levels and variability over time). This information will enable study-specific and time-dependent correction for regression dilution [23,51,52], whereas in the current meta-analysis the correction factor was derived from repeat measurements in only the Reykjavik Study. Adjustment for within-person variability in both exposure and confounder levels across all available studies will require access to individual participant data, as demonstrated by such adjustment in the current analyses of the Reykjavik Study and BRHS.
Conclusion
Long-term IL-6 levels are associated with CHD risk about as strongly as are some major established risk factors, but causality remains uncertain. These findings highlight the potential relevance of IL-6–mediated pathways to CHD.
Supporting Information
(60 KB PPT)
(8 KB PPT)
(49 KB DOC)
(103 KB DOC)
(41 KB DOC)
(33 KB PDF)
(48 KB DOC)
Acknowledgments
Mark B. Pepys, Kausik Ray, and Emanuele Di Angelantonio commented helpfully; J. Wheeler provided statistical support; E. Poorhang and P. Welsh conducted IL-6 assays.
Abbreviations
- BRHS
British Regional Heart Study
- CHD
coronary heart disease
- CI
confidence interval
- ECG
electrocardiogram
- IL-6
interleukin-6
- MI
myocardial infarction
- SD
standard deviation
Footnotes
Author contributions. JD, PHW, and VG conceived and designed the current work. SK and FW analysed the data. JD and SK drafted the paper. JD, SK, NS, AW, SBA, FW, JPTH, GE, AR, PHW, GDOL, and VG contributed to the writing of the paper. SK, AGM, NS, FW, and JPTH conducted the systematic review. LL collected the follow-up data in the BRHS. AR and GDOL supervised IL-6 assays.
Funding: This study was supported by programme and project grants from the British Heart Foundation (to JD, PHW, GDOL, and VG) and by the Raymond and Beverly Sackler Research Award in the Medical Sciences (to JD). SA is supported by a National Institutes of Health-Cambridge fellowship and her doctoral studies are cosupervised by T. Harris at the National Institute on Aging. Aspects of the study were supported by an unrestricted educational grant from GlaxoSmithKline (to JD). The funding bodies had no role in study design, data collection and analysis, decision to publish or preparation of the manuscript.
Competing Interests: The authors have declared that no competing interests exist.
References
- Hansson GK. Inflammation, atherosclerosis, and coronary artery disease. N Engl J Med. 2005;352:1685–1695. doi: 10.1056/NEJMra043430. [DOI] [PubMed] [Google Scholar]
- Pearson TA, Mensah GA, Alexander RW, Anderson JL, Cannon RO, III, et al. Markers of inflammation and cardiovascular disease: application to clinical and public health practice: a statement for healthcare professionals from the Centers for Disease Control and Prevention and the American Heart Association. Circulation. 2003;107:499–511. doi: 10.1161/01.cir.0000052939.59093.45. [DOI] [PubMed] [Google Scholar]
- Kerr R, Stirling D, Ludlam CA. Interleukin 6 and haemostasis. Br J Haematol. 2001;115:3–12. doi: 10.1046/j.1365-2141.2001.03061.x. [DOI] [PubMed] [Google Scholar]
- Le JM, Vilcek J. Interleukin 6: a multifunctional cytokine regulating immune reactions and the acute phase protein response. Lab Invest. 1989;61:588–602. [PubMed] [Google Scholar]
- Woodward M, Rumley A, Tunstall-Pedoe H, Lowe GD. Associations of blood rheology and interleukin-6 with cardiovascular risk factors and prevalent cardiovascular disease. Br J Haematol. 1999;104:246–257. doi: 10.1046/j.1365-2141.1999.01158.x. [DOI] [PubMed] [Google Scholar]
- Meade TW, Ruddock V, Stirling Y, Chakrabarti R, Miller GJ. Fibrinolytic activity, clotting factors, and long-term incidence of ischaemic heart disease in the Northwick Park Heart Study. Lancet. 1993;342:1076–1079. doi: 10.1016/0140-6736(93)92062-x. [DOI] [PubMed] [Google Scholar]
- Kuller LH, Tracy RP, Shaten J, Meilahn EN. Relation of C-reactive protein and coronary heart disease in the MRFIT nested case-control study. Multiple Risk Factor Intervention Trial. Am J Epidemiol. 1996;144:537–547. doi: 10.1093/oxfordjournals.aje.a008963. [DOI] [PubMed] [Google Scholar]
- Cesari M, Penninx BW, Newman AB, Kritchevsky SB, Nicklas BJ, et al. Inflammatory markers and onset of cardiovascular events: results from the Health ABC study. Circulation. 2003;108:2317–2322. doi: 10.1161/01.CIR.0000097109.90783.FC. [DOI] [PubMed] [Google Scholar]
- Folsom AR, Chambless LE, Ballantyne CM, Coresh J, Heiss G, et al. An assessment of incremental coronary risk prediction using C-reactive protein and other novel risk markers: the atherosclerosis risk in communities study. Arch Intern Med. 2006;166:1368–1373. doi: 10.1001/archinte.166.13.1368. [DOI] [PubMed] [Google Scholar]
- Jenny NS, Tracy RP, Ogg MS, Luong LA, Kuller LH, et al. In the elderly, interleukin-6 plasma levels and the −174G>C polymorphism are associated with the development of cardiovascular disease. Arterioscler Thromb Vasc Biol. 2002;22:2066–2071. doi: 10.1161/01.atv.0000040224.49362.60. [DOI] [PubMed] [Google Scholar]
- Koenig W, Khuseyinova N, Baumert J, Thorand B, Loewel H, et al. Increased concentrations of C-reactive protein and IL-6 but not IL-18 are independently associated with incident coronary events in middle-aged men and women: results from the MONICA/KORA Augsburg case-cohort study, 1984–2002. Arterioscler Thromb Vasc Biol. 2006;26:2745–2751. doi: 10.1161/01.ATV.0000248096.62495.73. [DOI] [PubMed] [Google Scholar]
- Langenberg C, Bergstrom J, Scheidt-Nave C, Pfeilschifter J, Barrett-Connor E. Cardiovascular death and the metabolic syndrome: role of adiposity-signaling hormones and inflammatory markers. Diabetes Care. 2006;29:1363–1369. doi: 10.2337/dc05-2385. [DOI] [PubMed] [Google Scholar]
- Lowe GD, Rumley A, McMahon AD, Ford I, O'Reilly DS, et al. Interleukin-6, fibrin D-dimer, and coagulation factors VII and XIIa in prediction of coronary heart disease. Arterioscler Thromb Vasc Biol. 2004;24:1529–1534. doi: 10.1161/01.ATV.0000135995.39488.6c. [DOI] [PubMed] [Google Scholar]
- Luc G, Bard JM, Juhan-Vague I, Ferrieres J, Evans A, et al. C-reactive protein, interleukin-6, and fibrinogen as predictors of coronary heart disease: the PRIME Study. Arterioscler Thromb Vasc Biol. 2003;23:1255–1261. doi: 10.1161/01.ATV.0000079512.66448.1D. [DOI] [PubMed] [Google Scholar]
- Pai JK, Pischon T, Ma J, Manson JE, Hankinson SE, et al. Inflammatory markers and the risk of coronary heart disease in men and women. N Engl J Med. 2004;351:2599–2610. doi: 10.1056/NEJMoa040967. [DOI] [PubMed] [Google Scholar]
- Pradhan AD, Manson JE, Rossouw JE, Siscovick DS, Mouton CP, et al. Inflammatory biomarkers, hormone replacement therapy, and incident coronary heart disease: prospective analysis from the Women's Health Initiative observational study. JAMA. 2002;288:980–987. doi: 10.1001/jama.288.8.980. [DOI] [PubMed] [Google Scholar]
- Ridker PM, Hennekens CH, Buring JE, Rifai N. C-reactive protein and other markers of inflammation in the prediction of cardiovascular disease in women. N Engl J Med. 2000;342:836–843. doi: 10.1056/NEJM200003233421202. [DOI] [PubMed] [Google Scholar]
- Ridker PM, Rifai N, Stampfer MJ, Hennekens CH. Plasma concentration of interleukin-6 and the risk of future myocardial infarction among apparently healthy men. Circulation. 2000;101:1767–1772. doi: 10.1161/01.cir.101.15.1767. [DOI] [PubMed] [Google Scholar]
- St-Pierre AC, Cantin B, Bergeron J, Pirro M, Dagenais GR, et al. Inflammatory markers and long-term risk of ischemic heart disease in men A 13-year follow-up of the Quebec Cardiovascular Study. Atherosclerosis. 2005;182:315–321. doi: 10.1016/j.atherosclerosis.2005.02.009. [DOI] [PubMed] [Google Scholar]
- Tuomisto K, Jousilahti P, Sundvall J, Pajunen P, Salomaa V. C-reactive protein, interleukin-6 and tumor necrosis factor alpha as predictors of incident coronary and cardiovascular events and total mortality. A population-based, prospective study. Thromb Haemost. 2006;95:511–518. doi: 10.1160/TH05-08-0571. [DOI] [PubMed] [Google Scholar]
- Tzoulaki I, Murray GD, Lee AJ, Rumley A, Lowe GD, et al. Relative value of inflammatory, hemostatic, and rheological factors for incident myocardial infarction and stroke: the Edinburgh Artery Study. Circulation. 2007;115:2119–2127. doi: 10.1161/CIRCULATIONAHA.106.635029. [DOI] [PubMed] [Google Scholar]
- Lobbes MB, Lutgens E, Heeneman S, Cleutjens KB, Kooi ME, et al. Is there more than C-reactive protein and fibrinogen? The prognostic value of soluble CD40 ligand, interleukin-6 and oxidized low-density lipoprotein with respect to coronary and cerebral vascular disease. Atherosclerosis. 2006;187:18–25. doi: 10.1016/j.atherosclerosis.2005.11.005. [DOI] [PubMed] [Google Scholar]
- Clarke R, Shipley M, Lewington S, Youngman L, Collins R, et al. Underestimation of risk associations due to regression dilution in long-term follow-up of prospective studies. Am J Epidemiol. 1999;150:341–353. doi: 10.1093/oxfordjournals.aje.a010013. [DOI] [PubMed] [Google Scholar]
- Fibrinogen Studies Collaboration. Wood AM, White I, Thompson SG, Lewington S, et al. Regression dilution methods for meta-analysis: assessing long-term variability in plasma fibrinogen among 27,247 adults in 15 prospective studies. Int J Epidemiol. 2006;35:1570–1578. doi: 10.1093/ije/dyl233. [DOI] [PubMed] [Google Scholar]
- Knuiman MW, Divitini ML, Buzas JS, Fitzgerald PE. Adjustment for regression dilution in epidemiological regression analyses. Ann Epidemiol. 1998;8:56–63. doi: 10.1016/s1047-2797(97)00107-5. [DOI] [PubMed] [Google Scholar]
- Rosner B, Willett WC, Spiegelman D. Correction of logistic regression relative risk estimates and confidence intervals for systematic within-person measurement error. Stat Med. 1989;8:1051–1069. doi: 10.1002/sim.4780080905. [DOI] [PubMed] [Google Scholar]
- Rosner B, Spiegelman D, Willett WC. Correction of logistic regression relative risk estimates and confidence intervals for measurement error: the case of multiple covariates measured with error. Am J Epidemiol. 1990;132:734–745. doi: 10.1093/oxfordjournals.aje.a115715. [DOI] [PubMed] [Google Scholar]
- Jonsdottir LS, Sigfusson N, Gudnason V, Sigvaldason H, Thorgeirsson G. Do lipids, blood pressure, diabetes, and smoking confer equal risk of myocardial infarction in women as in men? The Reykjavik Study. J Cardiovasc Risk. 2002;9:67–76. [PubMed] [Google Scholar]
- Walker M, Whincup PH, Shaper AG. The British Regional Heart Study 1975–2004. Int J Epidemiol. 2004;33:1185–1192. doi: 10.1093/ije/dyh295. [DOI] [PubMed] [Google Scholar]
- Danesh J, Wheeler JG, Hirschfield GM, Eda S, Eiriksdottir G, et al. C-reactive protein and other circulating markers of inflammation in the prediction of coronary heart disease. N Engl J Med. 2004;350:1387–1397. doi: 10.1056/NEJMoa032804. [DOI] [PubMed] [Google Scholar]
- Easton DF, Peto J, Babiker AG. Floating absolute risk: an alternative to relative risk in survival and case-control analysis avoiding an arbitrary reference group. Stat Med. 1991;10:1025–1035. doi: 10.1002/sim.4780100703. [DOI] [PubMed] [Google Scholar]
- Greenland S, Michels KB, Robins JM, Poole C, Willett WC. Presenting statistical uncertainty in trends and dose-response relations. Am J Epidemiol. 1999;149:1077–1086. doi: 10.1093/oxfordjournals.aje.a009761. [DOI] [PubMed] [Google Scholar]
- Plummer M. Improved estimates of floating absolute risk. Stat Med. 2004;23:93–104. doi: 10.1002/sim.1485. [DOI] [PubMed] [Google Scholar]
- Carpenter J, Bithell J. Bootstrap confidence intervals: when, which, what? A practical guide for medical statisticians. Stat Med. 2000;19:1141–1164. doi: 10.1002/(sici)1097-0258(20000515)19:9<1141::aid-sim479>3.0.co;2-f. [DOI] [PubMed] [Google Scholar]
- Harris TB, Ferrucci L, Tracy RP, Corti MC, Wacholder S, et al. Associations of elevated interleukin-6 and C-reactive protein levels with mortality in the elderly. Am J Med. 1999;106:506–512. doi: 10.1016/s0002-9343(99)00066-2. [DOI] [PubMed] [Google Scholar]
- Kip KE, Marroquin OC, Shaw LJ, Arant CB, Wessel TR, et al. Global inflammation predicts cardiovascular risk in women: a report from the Women's Ischemia Syndrome Evaluation (WISE) study. Am Heart J. 2005;150:900–906. doi: 10.1016/j.ahj.2005.02.002. [DOI] [PubMed] [Google Scholar]
- Volpato S, Guralnik JM, Ferrucci L, Balfour J, Chaves P, et al. Cardiovascular disease, interleukin-6, and risk of mortality in older women: the women's health and aging study. Circulation. 2001;103:947–953. doi: 10.1161/01.cir.103.7.947. [DOI] [PubMed] [Google Scholar]
- Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21:1539–1558. doi: 10.1002/sim.1186. [DOI] [PubMed] [Google Scholar]
- Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–560. doi: 10.1136/bmj.327.7414.557. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thompson SG, Sharp SJ. Explaining heterogeneity in meta-analysis: a comparison of methods. Stat Med. 1999;18:2693–2708. doi: 10.1002/(sici)1097-0258(19991030)18:20<2693::aid-sim235>3.0.co;2-v. [DOI] [PubMed] [Google Scholar]
- Pickup JC. Inflammation and activated innate immunity in the pathogenesis of type 2 diabetes. Diabetes Care. 2004;27:813–823. doi: 10.2337/diacare.27.3.813. [DOI] [PubMed] [Google Scholar]
- Ritchie SA, Connell JM. The link between abdominal obesity, metabolic syndrome and cardiovascular disease. Nutr Metab Cardiovasc Dis. 2007;17:319–326. doi: 10.1016/j.numecd.2006.07.005. [DOI] [PubMed] [Google Scholar]
- Szekanecz Z, Kerekes G, Der H, Sandor Z, Szabo Z, et al. Accelerated atherosclerosis in rheumatoid arthritis. Ann N Y Acad Sci. 2007;1108:349–358. doi: 10.1196/annals.1422.036. [DOI] [PubMed] [Google Scholar]
- Yanbaeva DG, Dentener MA, Creutzberg EC, Wesseling G, Wouters EF. Systemic effects of smoking. Chest. 2007;131:1557–1566. doi: 10.1378/chest.06-2179. [DOI] [PubMed] [Google Scholar]
- McCarey DW, McInnes IB, Madhok R, Hampson R, Scherbakov O, et al. Trial of Atorvastatin in Rheumatoid Arthritis (TARA): double-blind, randomised placebo-controlled trial. Lancet. 2004;19:2015–2021. doi: 10.1016/S0140-6736(04)16449-0. [DOI] [PubMed] [Google Scholar]
- Ray KK, Cannon CP. The potential relevance of the multiple lipid-independent (pleiotropic) effects of statins in the management of acute coronary syndromes. J Am Coll Cardiol. 2005;46:1425–1433. doi: 10.1016/j.jacc.2005.05.086. [DOI] [PubMed] [Google Scholar]
- Rezaie-Majd A, Maca T, Bucek RA, Valent P, Muller MR, et al. Simvastatin reduces expression of cytokines interleukin-6, interleukin-8, and monocyte chemoattractant protein-1 in circulating monocytes from hypercholesterolemic patients. Arterioscler Thromb Vasc Biol. 2002;22:1194–1199. doi: 10.1161/01.atv.0000022694.16328.cc. [DOI] [PubMed] [Google Scholar]
- Smith GD, Ebrahim S. Mendelian randomization: prospects, potentials, and limitations. Int J Epidemiol. 2004;33:30–42. doi: 10.1093/ije/dyh132. [DOI] [PubMed] [Google Scholar]
- Sie MP, Sayed-Tabatabaei FA, Oei HH, Uitterlinden AG, Pols HA, et al. Interleukin 6 −174 g/c promoter polymorphism and risk of coronary heart disease: results from the rotterdam study and a meta-analysis. Arterioscler Thromb Vasc Biol. 2006;26:212–217. doi: 10.1161/01.ATV.0000194099.65024.17. [DOI] [PubMed] [Google Scholar]
- Maini RN, Taylor PC, Szechinski J, Pavelka K, Broll J, et al. Double-blind randomized controlled clinical trial of the interleukin-6 receptor antagonist, tocilizumab, in European patients with rheumatoid arthritis who had an incomplete response to methotrexate. Arthritis Rheum. 2006;54:2817–2829. doi: 10.1002/art.22033. [DOI] [PubMed] [Google Scholar]
- Frost C, White IR. The effect of measurement error in risk factors that change over time in cohort studies: do simple methods overcorrect for ‘regression dilution'. Int J Epidemiol. 2005;34:1359–1368. doi: 10.1093/ije/dyi148. [DOI] [PubMed] [Google Scholar]
- Boshuizen HC, Lanti M, Menotti A, Moschandreas J, Tolonen H, et al. Effects of past and recent blood pressure and cholesterol level on coronary heart disease and stroke mortality, accounting for measurement error. Am J Epidemiol. 2007;165:398–409. doi: 10.1093/aje/kwk021. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
(60 KB PPT)
(8 KB PPT)
(49 KB DOC)
(103 KB DOC)
(41 KB DOC)
(33 KB PDF)
(48 KB DOC)