Abstract
Several prospective studies examining patients receiving physical therapy support the predictive validity of FABQ subscale scores. This has lead to the proposition that the FABQ would be a useful screening tool, permitting early identification of patients at risk for a poor outcome with an opportunity to modify the treatment accordingly. However, the predictive validity of the FABQ within physical therapy practice has yet to be examined. Predictive validity was analyzed between the FABQ-PA, FABQ-W using both disability and pain as the dependent variables using Pearson correlation coefficients and stepwise hierarchical linear regression modeling controlling for baseline variables. Separate analyses were run for patients with private health insurance and those receiving workers’ compensation. Further analysis of predictive validity was performed by dichotomizing the outcome of physical therapy. Patients were coded as having a poor outcome if they failed to achieve a minimum clinically important change in disability over the course of treatment. The accuracy of previously reported cut-off scales for both the FABQ-W and FABQ-PA were examined for both payor types. Results of the hierarchical linear regression analyses for patients with private insurance showed neither the FABQ-PA nor the FABQ-W score significantly improved the explained variance in change in pain or disability. For patients receiving workers’ compensation, only the FABQ-W subscale score significantly contributed to the model after controlling for the other baseline variables for both changes in disability and pain. Only the FABQ-W subscale was predictive of poor outcome and this was only identified in the worker’s compensation group. The results suggest that the work subscale of the FABQ might be an appropriate screening tool to identify patients with work-related LBP who are at risk for a poor outcome with routine physical therapy. Neither FABQ subscale was predictive of outcome for patients with private insurance, and the use of the FABQ, as a screening tool for patients with non-work-related LBP was not supported.
Keywords: Disability, Fear-avoidance beliefs, Low back pain, Outcome, Pain, Predictive validity
Introduction
A patient’s fear of pain may be more disabling than the pain itself [8]. Several investigators have proposed that patients with low back pain (LBP) who have heightened fear-avoidance beliefs exhibit avoidance behavior, altered movement patterns, and reduced physical activity, which in turn contributes to the persistence of pain and disability [8, 31, 33, 41, 45]. Several studies have found that the presence of elevated fear-avoidance beliefs is predictive of the development of chronic disability in patients with LBP [25, 31, 35]. This evidence has led to the suggestion that early identification of elevated fear-avoidance beliefs could lead to more appropriate early management strategies resulting in a decreased risk of chronicity [3, 5, 15].
The fear-avoidance beliefs questionnaire (FABQ) was developed to measure levels of fear and avoidance beliefs about work and physical activity in patients with LBP [44]. The instrument consists of two subscales, a four-item physical activity subscale (FABQ-PA), and a seven-item work subscale (FABQ-W). Each item is scored from 0 to 6 and summed to produce the subscale score. Possible scores range from 0–28 to 0–42 for the FABQ-PA and FABQ-W, respectively. The FABQ subscales have been shown to have high levels of internal consistency and test-retest reliability [19, 40]. Several cross-sectional studies have found a strong relationship between FABQ subscale scores and disability due to LBP [16, 27, 44]. Prospective studies performed in general practice settings confirm that FABQ subscale scores are predictive of future disability for patients with acute and chronic LBP [3, 6, 21, 24]. Prospective studies examining patients receiving physical therapy also support the predictive validity of FABQ subscale scores [1, 13, 15]. This has lead to the proposition that the FABQ would be a useful screening tool, permitting early identification of patients at risk for a poor outcome with an opportunity to modify the treatment accordingly [3, 14].
Belief that the FABQ may be useful screening tool to identify patients at risk of a poor outcome has led researchers to seek to identify cut-off scores that would define an “at-risk” patient. Fritz and George [10] studied patients with acute, work-related LBP and found an FABQ-W score > 29 was most predictive of return to work status after four weeks of physical therapy. No empirically derived cut-off scores for the FABQ-PA have been reported. Klaber-Moffett et al. [23] recommended a cut-off score > 13 based on a median split of baseline scores, and found that patients with chronic LBP scoring above this cut-off were more likely to benefit from an exercise program instead of usual care. Poiraudeau and colleagues [34] found that patients with sub-acute LBP scoring above this threshold had higher levels of disability and anxiety.
Further research is required to examine the predictive validity of the FABQ within Physical Therapy practice. Prior studies have been conducted in the context of controlled clinical studies with standardized inclusion criteria, treatment, and informed consent procedures. The validity of the FABQ subscale scores for predicting a poor outcome in routine physical therapy practice has not been reported. Previously reported cut-off scores also need to be examined in this setting. Although it has been shown that patients on workers compensation that exhibit high FABQ-W scores are less likely to return to work at a 4 week follow-up [12], no data exists to support this finding in patients who are not on workers compensation. The influence of payor type on the usefulness of the FABQ in physical therapy practice also has not been explored. The purpose of this study was to examine the predictive validity of the FABQ used in physical therapy clinics routinely administering the questionnaire at baseline to patients with LBP. Predictive validity was investigated by comparing baseline FABQ scores with clinical outcomes. We examined predictive validity separately for patients with private health insurance and those receiving workers’ compensation. A second purpose was to determine the predictive validity of previously reported cut-off scores for the FABQ-PA and FABQ-W in this sample of patients.
Methods
A retrospective review of patients with LBP entered into an electronic database at five physical therapy clinics within Intermountain Healthcare (IHC) between first June 2003 and first September 2006 was performed. The clinics participating in the study represent outpatient orthopaedic clinics in the Salt Lake Valley (UT). The referral pattern to all involved sites is primary care or occupational Health clinics. This study qualified for exempt status from the Institutional Review Board at IHC. These clinics had instituted routine administration of the FABQ for patients with LBP along with other paperwork at the initial physical therapy session. Additionally, all clinicians were trained in a classification approach to the management of patients with LBP which involved treatment strategies including mobilization, stabilization and direction specific exercises [9]. However, we did not exert rigid control over the treatment delivered. Data from patients receiving physical therapy at these clinics are entered into an electronic database using Intranet Java Web Application. Data entered includes age, sex, duration of symptoms, number of physical therapy visits, third party payor type (private insurance, workers’ compensation, government-sponsored insurance (Medicare and Medicaid), length of stay and total cost of physical therapy treatments. Clinical outcome data (pain rating and a condition-specific disability score) are collected at each visit and entered into the database. For patients with LBP, an 11-point pain rating scale is used to indicate current pain intensity [22]. The modified Oswestry disability index (ODI) [11] is used to measure disability due to LBP. These questionnaires have high levels of test-retest reliability and responsiveness for patients with LBP [11, 19, 30].
All patients entered into the database from one of the included clinics during the study’s time period who completed the ODI as their condition-specific disability measure were screened for eligibility. To be eligible patients had to be between 18 and 65 years of age, exhibit an initial ODI score ≥10%, have received at least 3 physical therapy visits, and have a payor type of either private insurance or workers compensation (i.e., patients who were injured while at their place of employment). The charts of all patients who satisfied these criteria were manually reviewed. Only those patients with FABQ subscale scores from the initial examination in the chart were included in this study. For included patients we also examined the pain body diagram in the chart [46]. If the diagram did not indicate symptoms in the lumbar/buttock region the patient was excluded. Additionally, we classified included patients as having only LBP or LBP with leg symptoms if the diagram indicated symptoms extended distal to the buttock.
Data analysis
Baseline variables and scores on the outcome measures were compared between patients who were receiving workers compensation or private insurance using independent t-tests for continuous data and χ2 tests of independence for categorical data. The relationship between fear-avoidance beliefs and clinical outcomes of physical therapy was examined using Pearson correlation coefficients computed between the baseline FABQ subscale scores and pain rating and ODI scores from the initial and final physical therapy visits, and the change scores occurring with therapy for these measures. Coefficients were computed separately for each payor group.
Stepwise hierarchical linear regression analysis was used to examine the relationship between baseline FABQ subscale scores and changes in clinical outcome measures. Change in ODI scores served as the dependent variable. Age, duration of symptoms, sex, the presence of leg symptoms, and baseline pain and ODI scores were entered into the model in the first step. The baseline FABQ-PA score was entered in the second step. For each step, the adjusted R2 value was calculated, reflecting the goodness of fit of the linear model adjusted for the number of independent variables in the equation. The significance of the change in R2 at each step was tested. Standardized beta coefficients for each variable in the final model were calculated and the significance of each was tested under the null hypothesis that the coefficient was not different from zero. The analysis was repeated using the FABQ-W instead of the FABQ-PA in the second step. This hierarchical approach was used to determine if baseline FABQ subscale scores would further improve the fit of the regression model after controlling for age, sex, duration of symptoms, presence of leg symptoms, and baseline levels of pain and disability. Separate models were constructed for each payor group, and using change in pain rating as the dependent variable. We a prior set a p value of 0.05 to be considered statistically significant.
Further analysis of predictive validity was performed by dichotomizing the outcome of physical therapy. Patients were coded as having a poor outcome if they failed to achieve a minimum clinically important change for the ODI (six points) [11] over the course of treatment. Patients who achieved six or more points of change were coded as having a successful outcome. Receiver operator characteristic (ROC) curves were then constructed by plotting sensitivity values (true positive rate) on the y-axis and one-specificity values (false positive rate) on the x-axis for all possible cut-off scores for each FABQ subscale. The area under the curve (AUC) and 95% confidence interval [17] was obtained as a method for describing the ability of each FABQ subscale score to distinguish between patients who did or did not experience a poor outcome. AUC values describe the overall accuracy of a diagnostic test. An AUC value greater than 0.50 indicates that using the test improves the prediction of outcome over chance, while an AUC value of 1 represents perfect accuracy [29]. Separate ROC curves were constructed for the FABQ-PA and FABQ-W and for different payor types. Additionally, sensitivity, specificity and likelihood ratios were calculated for previously established cut-off scores of >13 for the FABQ-PA and >29 for the FABQ-W using a poor outcome as the reference standard. This was done to determine the accuracy of these cut-offs for identifying patients with a poor prognosis for improvement with physical therapy.
Results
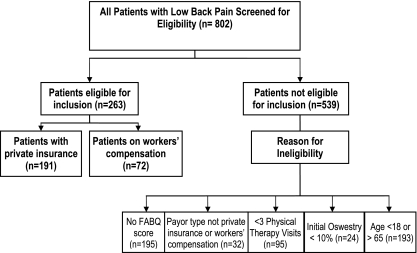
During the time period first January 2003 to first September 2006, 802 patients completed the ODI and were screened for eligibility, with 339 patients excluded on the basis of age, initial disability score, payor type, or number of physical therapy visits as identified through the database (Fig. 1). Of the 195 patients not eligible as a result of missing FABQ scores only 28 (14%) were on workers compensation. The charts of remaining patients were reviewed to assess the pain body diagram, and determine documentation of FABQ scores at the initial examination. An additional 189 patients were excluded, leaving 263 for inclusion in this study. Of the included patients, 191 were in the private insurance group and 72 were in the workers’ compensation group. During the study period 93.1% of patients receiving physical therapy in the included clinics were entered into the clinical outcomes database.
Fig. 1.
Flow diagram representing the identification of eligible patients
Those who were not eligible had a significantly lower baseline scores for the FABQ-W subscale (P = 0.003), initial ODI (P = 0.009) and the number of PT visits received (P = 0.001). Baseline variables for each payor type are presented in Table 1. Duration of symptoms data were missing for 59 patients (49 private insurance, 10 workers’ compensation). Significant differences were observed between payor types. The workers’ compensation group had a shorter symptom duration, higher initial ODI and FABQ-W scores, and a trend towards higher initial pain rating (P = 0.051) (Table 1).
Table 1.
Demographic data for baseline variables for each payor type (values represent mean and standard deviations unless otherwise indicated)
| Variable | Private insurance (n = 191) | Workers compensation (n = 72) | Significance |
|---|---|---|---|
| Age | 41.8 (12.8) | 39.9 (13.3) | 0.29 |
| Sex (female %) | 55% | 42% | 0.16 |
| Symptom duration [median days (range)] | 42 days (0 days–6.6 years) (n = 142)a | 19.5 days (0 days–3 years) (n = 62)a | 0.004 |
| Symptoms distal to buttocks (yes %) | 41% | 50% | 0.16 |
| Initial Oswestry disability score | 37.3 (14.9) | 44.2 (15.6) | 0.001 |
| Initial pain rating | 5.4 (2.5) | 6.1 (2.1) | 0.051 |
| FABQ-PA | 14.6 (5.9) | 14.4 (6.6) | 0.77 |
| FABQ-W | 12.9 (10.1) | 23.3 (10.8) | <0.001 |
aData regarding symptom duration was missing for 49 patients in the private insurance group and 10 in the workers compensation group
Among patients with private insurance, significant correlations existed between the initial FABQ subscale scores and initial pain and disability (ODI) scores (Table 2). However, neither the FABQ-PA nor FABQ-W was correlated with the change in pain or disability over the course of treatment. For patients receiving workers’ compensation, neither FABQ subscale score correlated with initial pain or disability scores (Table 3). The FABQ-PA was significantly correlated with the change in disability (r = −0.32) and change in pain (r = −0.26). The FABQ-W had significant correlations with both the change in pain (r = −0.39) and disability (r = −0.50).
Table 2.
Pearson correlation coefficients examining the relationships between initial FABQ-PA and FABQ-W scores, initial and final ODI and pain rating, and change in ODI and pain rating for patients with private insurance
| FABQ-PA | FABQ-W | Initial ODI | Initial pain rating | Final ODI | Final pain rating | Change in ODI | Change in pain rating | |
|---|---|---|---|---|---|---|---|---|
| FABQ-PA | 0.20** | 0.35** | 0.30** | 0.17* | 0.11 | 0.14 | 0.18 | |
| FABQ-W | 0.29** | 0.23** | 0.26** | 0.17* | 0.017 | 0.060 | ||
| Initial ODI | 0.58** | 0.47** | 0.22* | 0.42** | 0.34** | |||
| Initial pain rating | 0.38** | 0.45** | 0.14 | 0.52** | ||||
| Final ODI | 0.75** | −0.59** | −0.35** | |||||
| Final pain rating | −0.58** | −0.53** | ||||||
| Change in ODI | 0.69** | |||||||
| Change in pain rating |
** Significant at P < 0.01, * significant at P < 0.05
Table 3.
Pearson correlational coefficients examining the relationships between initial FABQ-PA and FABQ-W scores, initial and final ODI and pain rating, and change in ODI and pain rating for the workers compensation group
| FABQ-PA | FABQ-W | Initial ODI | Initial pain rating | Final ODI | Final pain rating | Change in ODI | Change in pain rating | |
|---|---|---|---|---|---|---|---|---|
| FABQ-PA | 0.59** | −0.048 | −0.055 | 0.30** | 0.25* | −0.32* | −0.26* | |
| FABQ-W | −0.17 | −0.11 | 0.44** | 0.35** | −0.50** | −0.39** | ||
| Initial ODI | 0.66** | 0.44** | 0.29** | 0.33** | 0.19 | |||
| Initial pain rating | 0.21 | 0.12 | 0.33** | 0.50** | ||||
| Final ODI | 0.78** | −0.64** | −0.56** | |||||
| Final pain rating | −0.60** | −0.75** | ||||||
| Change in ODI | 0.76** | |||||||
| Change in pain rating |
** Significant at P < 0.01, * significant at P < 0.05
Results of the hierarchical linear regression analyses for patients with private insurance showed neither the FABQ-PA or FABQ-W score significantly improved the explained variance in change in pain or disability after controlling for age, duration of symptoms, sex, presence of leg symptoms, and baseline pain and disability (Tables 4, 5). For patients receiving workers’ compensation, only the FABQ-W subscale score significantly contributed to the model after controlling for the other baseline variables for both changes in disability (Table 6) and pain (Table 7) (adjusted R2 = 0.45, P = 0.001 and adjusted R2 = 0.37, P = 0.007, respectively).
Table 4.
Hierarchical linear regression analyses for patients with private insurance (n = 141) exploring the relationship between initial FABQ-PA and FABQ-W scores and change in disability, controlling for age, sex, symptom duration, the presence of symptoms distal to the buttocks, and initial pain and disability (ODI) scores
| Step | Variables | Adjusted R2 | Significance of R2 change | Standardized beta coefficient in the final model | Significance of beta coefficient |
|---|---|---|---|---|---|
| FABQ-PA | |||||
| Step 1 | Age | −0.061 | 0.44 | ||
| Days since onset | −0.070 | 0.38 | |||
| Sex | −0.074 | 0.35 | |||
| Initial pain rating | −0.20 | 0.049 | |||
| Initial ODI | 0.50 | <0.001 | |||
| Symptoms distal to buttock | −0.13 | 0.11 | |||
| 0.19 | <0.001 | ||||
| tep 2 | FABQ-PA | 0.18 | 0.78 | 0.02 | 0.78 |
| FABQ-W | |||||
| Step 1 | Age | −0.063 | 0.42 | ||
| Days since onset | −0.074 | 0.35 | |||
| Sex | −0.076 | 0.34 | |||
| Initial pain rating | −0.19 | 0.062 | |||
| Initial ODI | 0.51 | <0.001 | |||
| Symptoms distal to buttock | −0.13 | 0.11 | |||
| 0.19 | <0.001 | ||||
| Step 2 | FABQ-W | 0.18 | 0.57 | −0.046 | 0.57 |
Table 5.
Hierarchical linear regression analyses for patients with private insurance (n = 141) exploring the relationship between initial FABQ-PA and FABQ-W scores and change in pain, controlling for age, sex, symptom duration, the presence of symptoms distal to the buttocks, and initial pain and disability (ODI) scores
| Step | Variables | Adjusted R2 | Significance of R2 change | Standardized beta coefficient in the final model | Significance of beta coefficient |
|---|---|---|---|---|---|
| FABQ-PA | |||||
| Step 1 | Age | −0.022 | 0.77 | ||
| Days since onset | −0.17 | 0.030 | |||
| Sex | −0.11 | 0.15 | |||
| Initial pain rating | 0.46 | <0.001 | |||
| Initial ODI | 0.005 | 0.96 | |||
| Symptoms distal to buttock | −0.065 | 0.38 | |||
| 0.26 | <0.001 | ||||
| Step 2 | FABQ-PA | 0.26 | 0.96 | −0.004 | 0.96 |
| FABQ-W | |||||
| Step 1 | Age | −0.022 | 0.77 | ||
| Days since onset | −0.17 | 0.028 | |||
| Sex | −0.11 | 0.15 | |||
| Initial pain rating | 0.46 | <0.001 | |||
| Initial ODI | 0.012 | 0.90 | |||
| Symptoms distal to buttock | −0.067 | 0.37 | |||
| 0.26 | <0.001 | ||||
| Step 2 | FABQ-W | 0.26 | 0.71 | −0.029 | 0.71 |
Table 6.
Hierarchical linear regression analyses for patients with workers’ compensation (n = 62) exploring the relationship between initial FABQ-PA and FABQ-W scores and change in disability (ODI), controlling for age, sex, symptom duration, the presence of symptoms distal to the buttocks, and initial pain and disability (ODI) scores
| Step | Variables | Adjusted R2 | Significance of R2 change | Standardized beta coefficient in the final model | Significance of beta coefficient |
|---|---|---|---|---|---|
| FABQ-PA | |||||
| Step 1 | Age | −0.31 | 0.006 | ||
| Days since onset | −0.24 | 0.036 | |||
| Sex | 0.23 | 0.059 | |||
| Initial pain rating | −0.009 | 0.95 | |||
| Initial ODI | 0.41 | 0.009 | |||
| Symptoms distal to buttock | 0.19 | 0.083 | |||
| 0.34 | <0.001 | ||||
| Step 2 | FABQ-PA | 0.35 | 0.19 | −0.15 | 0.19 |
| FABQ-W | |||||
| Step 1 | Age | −0.25 | 0.018 | ||
| Days since onset | −0.19 | 0.069 | |||
| Sex | 0.19 | 0.088 | |||
| Initial pain rating | 0.059 | 0.66 | |||
| Initial ODI | 0.29 | 0.048 | |||
| Symptoms distal to buttock | 0.13 | 0.21 | |||
| 0.34 | <0.001 | ||||
| Step 2 | FABQ-W | 0.45 | 0.001 | −0.37 | 0.001 |
Table 7.
Hierarchical linear regression analyses for patients with workers’ compensation (n = 62) exploring the relationship between initial FABQ-PA and FABQ-W scores and change in pain, controlling for age, sex, symptom duration, the presence of symptoms distal to the buttocks, and initial pain and disability (ODI) scores
| Step | Variables | Adjusted R2 | Significance of R2 change | Standardized beta coefficient in the final model | Significance of beta coefficient |
|---|---|---|---|---|---|
| FABQ-PA | |||||
| Step 1 | Age | −0.21 | 0.068 | ||
| Days since onset | −0.032 | 0.78 | |||
| Sex | 0.16 | 0.19 | |||
| Initial pain rating | 0.49 | 0.002 | |||
| Initial ODI | −0.087 | 0.58 | |||
| Symptoms distal to buttock | 0.17 | 0.13 | |||
| 0.29 | <0.001 | ||||
| Step 2 | FABQ-PA | 0.30 | 0.22 | −0.14 | 0.22 |
| FABQ-W | |||||
| Step 1 | Age | −0.16 | 0.16 | ||
| Days since onset | 0.008 | 0.95 | |||
| Sex | 0.13 | 0.27 | |||
| Initial pain rating | 0.55 | <0.001 | |||
| Initial ODI | −0.19 | 0.22 | |||
| Symptoms distal to buttock | 0.12 | 0.27 | |||
| 0.29 | <0.001 | ||||
| Step 2 | FABQ-W | 0.37 | 0.007 | −0.32 | 0.007 |
Overall 77 patients (29.3%) did not experience at least 6 points of change on the ODI and were considered to have a poor outcome. The percentage of patients with a poor outcome did not differ between patients with private insurance (29.8%) or receiving workers’ compensation (27.8%) (P = 0.74). For patients with private insurance, neither the FABQ-PA [AUC = 0.44 (95% CI: 0.35, 0.53)] nor the FABQ-W [AUC = 0.52 (95% CI: 0.44, 0.66)] subscale score was able to distinguish patients with or without a poor outcome better than chance. For patient’s receiving workers’ compensation both the FABQ-PA [AUC = 0.66 (95% CI: 0.51, 0.80)] and FABQ-W [AUC = 0.78 (95% CI: 0.66, 0.90)] were predictive of a poor outcome. For patients with private insurance the previously reported cut-off scores for the FABQ-PA and FABQ-W were not predictive of a poor outcome (confidence intervals for the positive and negative likelihood ratios include 1.0) (Table 8). Among patients receiving workers’ compensation, the FABQ-W cut-off (>29 points) was predictive of a poor outcome (positive likelihood ratio = 4.33 (95% CI: 2.27, 8.27); negative likelihood ratio = 0.30 (95% CI: 0.14, 0.65) (Table 8).
Table 8.
Accuracy statistics for predicting a poor outcome using previously reported cut-off scores for the FABQ-PA and FABQ-W
| Sensitivity (95% CI) | Specificity (95% CI) | Positive likelihood ratio (95% CI) | Negative likelihood ratio (95% CI) | |
|---|---|---|---|---|
| FABQ-PA: (cut-off > 13 points) | ||||
| Private insurance | 0.60 (0.47, 0.71) | 0.33 (0.26, 0.41) | 0.89 (0.70, 1.13) | 1.23 (0.83, 1.83) |
| Workers’ compensation | 0.70 (0.48, 0.86) | 0.48 (0.35, 0.61) | 1.46 (0.97, 2.18) | 0.58 (0.28, 1.19) |
| FABQ-W: (cut-off > 29 points) | ||||
| Private insurance | 0.070 (0.028, 0.17) | 0.92 (0.86, 0.95) | 0.86 (0.28, 2.57) | 1.01 (0.93, 1.11) |
| Workers’ compensation | 0.75 (0.53, 0.89) | 0.83 (0.70, 0.91) | 4.33 (2.27, 8.27) | 0.30 (0.14, 0.65) |
Discussion
This study sought to examine the usefulness of FABQ subscale scores used in typical physical therapy practice. An abundance of research has identified elevated fear-avoidance beliefs as a critical prognostic factor for many individuals with LBP, leading to recommendations that clinicians should routinely screen patients with LBP using tools such as the FABQ [3, 4, 14, 26]. Most of the research conducted to date has resulted from controlled clinical studies. A frequent concern raised about the application of research evidence into clinical practice is the lack of external validity and limited generalizability of controlled studies [28, 36]. It is therefore important to examine the usefulness of evidence-based recommendations when applied to everyday practice.
The results of this study suggest that the validity of the FABQ subscale scores for predicting which patients with LBP are likely to have a poor outcome with physical therapy depends on the payor type and the FABQ subscale used. Among patients receiving workers’ compensation, the initial FABQ-W score, although uncorrelated with concurrent measures of pain and disability, was highly correlated with the final pain and disability scores, and the changes in these scores over the course of treatment. Even after controlling for baseline variables with prognostic value, the FABQ-W explained a significant proportion of the variance in change in both pain and disability among patients receiving workers’ compensation. The predictive value of the FABQ-PA among patients receiving workers’ compensation was not as strong, and neither FABQ subscale score demonstrated predictive validity for patients with private insurance.
These findings suggest that only the FABQ-W subscale used with patients receiving workers’ compensation, which contributed 45% of the variance for the change in disability and 37% of the variance for change in pain, provided sufficient predictive validity to warrant consideration as a tool to guide clinical decision-making for the management of patients with LBP.
Among patients with private insurance, we found significant correlations between initial FABQ subscale scores and initial pain and disability scores, but the initial FABQ scores were not predictive of the outcome of physical therapy. The regression models constructed for patients with private insurance showed no additional prediction of changes in pain and disability once the baseline prognostic variables were controlled. This result is contrary to findings of previous research examining patients with primarily non-work-related LBP, which have found initial FABQ subscale scores to be predictive of outcome [1, 16, 24, 32]. Although the preponderance of the evidence supports the validity of initial FABQ subscale scores for predicting outcome among patients with non-work-related LBP, our results are in agreement with recent work by Sieben and colleagues [37, 38] that questions the predictive validity of the FABQ, at least among patients with acute LBP (<3 weeks duration). Our sample of patients with private insurance had mostly sub-acute or chronic symptoms (35% had symptoms <3 weeks duration), while those receiving workers’ compensation were more acute (54% had symptoms < 3 weeks duration), and we controlled for chronicity in our multi-variate prediction models. Our results suggest that payor-type may be more relevant than chronicity for establishing predictive validity of the FABQ for patients with LBP receiving physical therapy. This perhaps suggests that patients injured while at their place of employment who score high on the FABQ might have a poor prognosis with physical therapy intervention. Variations in methodology preclude strong conclusions; however, the results of this study and others do raise questions about the role of fear-avoidance beliefs and the potential usefulness of the FABQ for patients with LBP who do not have work-related LBP.
Belief in the prognostic consequence of elevated fear-avoidance beliefs has increased interest in identifying cut-off scores that would accurately detect a patient at risk for a poor outcome. We examined the accuracy of an FABQ-W cut-off score of >29 recommended in a previous study examining patients with work-related LBP [10]. This cut-off score was accurate in the present study for identifying patients receiving workers’ compensation at risk for a poor outcome. The original study reported a negative likelihood ratio of 0.08 and positive likelihood ratio of 2.28 for this cut-off score for predicting return to work after 4 weeks of physical therapy [10], compared with a negative likelihood ratio of 0.30 and positive likelihood ratio of 4.33 for predicting a poor outcome with physical therapy in the current study. For patients with private insurance this FABQ-W cut-off score was not useful for predicting a poor outcome (negative and positive likelihood ratio 0.86 and 1.01, respectively). According to Jaeschke et al. [20] accuracy can be considered moderate when the positive LR approaches 5.0 or the negative LR is less than 0.20.
The AUC value for the FABQ-W among patients with private insurance did not reveal accuracy greater than chance for detecting patients that would go on to have a poor outcome (AUC = 0.52). This result may not be surprising given that the FABQ-W is designed to detect fear-avoidance beliefs specifically about work, but it does indicate a need for caution in interpreting FABQ-W scores in patients with non-work-related LBP. Among patients with work-related LBP, however, a cut-off score of >29 may be useful for identifying patients with a poor prognosis at the initial encounter with the patient.
No empirically derived cut-off score for the FABQ-PA has been reported in the literature, however, a cut-off of >13 has been used in several studies [23, 34]. This cut-off score did not result in a significant improvement in prediction of a poor outcome in either payor group (confidence intervals of all likelihood ratio values contain 1.0). This suggests that the FABQ-PA subscale has poor discriminative ability to identify patients at risk for a poor outcome with physical therapy. Perhaps physical activity subscales are more useful in identifying which patients with LBP are likely to benefit form a lumbar stabilization program rather than discriminating between those who will and will not have a successful outcome with therapy [18, 23].
It has been suggested that screening for high levels of fear-avoidance beliefs in patients with LBP might provide an opportunity to alter the patient management and attempt to reduce the likelihood of a poor outcome [3, 14, 15]. However, our findings recommend caution in using the FABQ subscale scores to identify patients with non-work-related LBP for whom an alternative management strategy is needed. Among patients with work-related LBP, the FABQ-W at a cut-off score of >29 may be useful for clinical decision-making; identifying those not likely to improve with traditional physical therapy who may warrant an alternative approach such as graded exercise or exposure, or other cognitive-behavioral strategies [2, 7, 39, 42, 43]. Further investigation is necessary to examine the effectiveness of alternative management strategies in this sub-group of patients.
There are several limitations of this study. Although we sought to examine the usefulness of initial FABQ scores recorded in clinics that routinely administer the questionnaire to all patients with LBP, we had to exclude 189 patients (23.6%) due to missing FABQ scores. While we have no indication of a systematic bias in the failure to obtain FABQ scores, it is possible that the missing scores may have influenced the results. Also, we noted a difference between those that were eligible for the analysis and those that were not for the FABQ-W subscale, initial ODI and the number of PT visits received. The results might have been different had all patients been eligible to participate. Additionally, we only investigated the ability of the FABQ to predict the outcome of physical therapy. The duration of physical therapy averaged about 30 days for these patients. This short-term follow-up does not allow us to make inferences regarding the usefulness of the FABQ for determining long-term prognosis. Finally, we examined FABQ scores in patients receiving routine physical therapy involving a variety of techniques and procedures. It is possible that the FABQ subscale scores might be best used to identify patients who are likely to respond to a more specific intervention protocol designed to address elevated fear-avoidance beliefs. Our results do suggest that the FABQ subscale scores are not useful in predicting the outcomes of physical therapy for patients with private insurance.
Conclusion:
The results of the current study suggest that the work subscale of the FABQ might be an appropriate screening tool to identify patients with work-related LBP who are at risk for a poor outcome with routine physical therapy. Neither FABQ subscale was predictive of outcome for patients with private insurance, and the use of the FABQ as a screening tool for patients with non-work-related LBP was not supported. Further research is needed to identify accurate screening tools to assist clinical decision-making by physical therapists.
Footnotes
The handling of data in this study was performed in compliance with the current laws of the United States of America inclusive of ethics approval.
References
- 1.Al-Obaidi SM, Beattie P, Al-Zoabi B, Al-Wekeel S. The relationship of anticipated pain and fear avoidance beliefs to outcome in patients with chronic low back pain who are not receiving workers’ compensation. Spine. 2005;30:1051–1057. doi: 10.1097/01.brs.0000160848.94706.83. [DOI] [PubMed] [Google Scholar]
- 2.Boersma K, Linton S, Overmeer T, Jansson M, Vlaeyen J, Jong J. Lowering fear-avoidance and enhancing function through exposure in vivo. A multiple baseline study across six patients with back pain. Pain. 2004;108:8–16. doi: 10.1016/j.pain.2003.03.001. [DOI] [PubMed] [Google Scholar]
- 3.Boersma K, Linton SJ. Screening to identify patients at risk: profiles of psychological risk factors for early intervention. Clin J Pain. 2005;21:38–43. doi: 10.1097/00002508-200501000-00005. [DOI] [PubMed] [Google Scholar]
- 4.Buer N, Linton SJ. Fear-avoidance beliefs and catastrophizing: occurrence and risk factor in back pain and ADL in the general population. Pain. 2002;99:485–491. doi: 10.1016/S0304-3959(02)00265-8. [DOI] [PubMed] [Google Scholar]
- 5.Burton AK, Waddell G, Tillotson KM, Summerton N. Information and advice to patients with back pain can have a positive effect. A randomized controlled trial of a novel educational booklet in primary care. Spine. 1999;24:2484–2491. doi: 10.1097/00007632-199912010-00010. [DOI] [PubMed] [Google Scholar]
- 6.Carragee EJ, Alamin TF, Miller JL, Carragee JM. Discographic, MRI and psychosocial determinants of low back pain disability and remission: a prospective study in subjects with benign persistent back pain. Spine J. 2005;5:24–35. doi: 10.1016/j.spinee.2004.05.250. [DOI] [PubMed] [Google Scholar]
- 7.Crombez G, Vervaet L, Lysens R, Baeyens F, Eelen P. Avoidance and confrontation of painful, back-straining movements in chronic back pain patients. Behav Modif. 1998;22:62–77. doi: 10.1177/01454455980221004. [DOI] [PubMed] [Google Scholar]
- 8.Crombez G, Vlaeyen JW, Heuts PH, Lysens R. Pain-related fear is more disabling than pain itself: evidence on the role of pain-related fear in chronic back pain disability. Pain. 1999;80:329–339. doi: 10.1016/S0304-3959(98)00229-2. [DOI] [PubMed] [Google Scholar]
- 9.Delitto A, Erhard RE, Bowling RW. A treatment-based classification approach to low back syndrome: identifying and staging patients for conservative treatment. Phys Ther. 1995;75:470–485. doi: 10.1093/ptj/75.6.470. [DOI] [PubMed] [Google Scholar]
- 10.Fritz JM, George SZ. Identifying psychosocial variables in patients with acute work-related low back pain: the importance of fear avoidance beliefs. Phys Ther. 2002;82:973–983. [PubMed] [Google Scholar]
- 11.Fritz JM, Irrang JJ. A comparison of a modified Oswestry low back disability questionnaire and the Quebec back pain disability scale. Phys Ther. 2001;81:776–788. doi: 10.1093/ptj/81.2.776. [DOI] [PubMed] [Google Scholar]
- 12.Fritz JM, Delitto A, Erhard RE. Comparison of classification-based physical therapy with therapy based on clinical practice guidelines for patients with acute low back pain: a randomized clinical trial. Spine. 2003;28:1363–1371. doi: 10.1097/00007632-200307010-00003. [DOI] [PubMed] [Google Scholar]
- 13.Fritz JM, George SZ, Delitto A. The role of fear-avoidance beliefs in acute low back pain: relationships with current and future disability and work status. Pain. 2001;94:7–15. doi: 10.1016/S0304-3959(01)00333-5. [DOI] [PubMed] [Google Scholar]
- 14.George SZ. Fear: a factor to consider in musculoskeletal rehabilitation. J Orthop Sports Phys Ther. 2006;36:264–266. doi: 10.2519/jospt.2006.0106. [DOI] [PubMed] [Google Scholar]
- 15.George SZ, Fritz JM, Bialosky JE, Donald DA. The effect of a fear-avoidance-based physical therapy intervention for patients with acute low back pain: results of a randomized clinical trial. Spine. 2003;28:2551–2560. doi: 10.1097/01.BRS.0000096677.84605.A2. [DOI] [PubMed] [Google Scholar]
- 16.George SZ, Fritz JM, McNeil DW. Fear-avoidance beliefs as measured by the fear-avoidance beliefs questionnaire: change in fear-avoidance beliefs questionnaire is predictive of change in self-report of disability and pain intensity for patients with acute low back pain. Clin J Pain. 2006;22:197–203. doi: 10.1097/01.ajp.0000148627.92498.54. [DOI] [PubMed] [Google Scholar]
- 17.Hanley J, McNeil B. The meaning and use of the area under receiver operating characteristic (ROC) curve. Radiology. 1982;143:29–36. doi: 10.1148/radiology.143.1.7063747. [DOI] [PubMed] [Google Scholar]
- 18.Hicks GE, Fritz JM, Delitto A, McGill SM. Preliminary development of a clinical prediction rule for determining which patients with low back pain will respond to a stabilization exercise program. Arch Phys Med Rehabil. 2005;86:1753–1762. doi: 10.1016/j.apmr.2005.03.033. [DOI] [PubMed] [Google Scholar]
- 19.Jacob T, Baras M, Zeev A, Epstein L. Low back pain: reliability of a set of pain measurement tools. Arch Phys Med Rehabil. 2001;82:735–742. doi: 10.1053/apmr.2001.22623. [DOI] [PubMed] [Google Scholar]
- 20.Jaeschke R, Guyatt GH, Sackett DL. Users’ guides to the medical literature. III. How to use an article about a diagnostic test. B. What are the results and will they help me in caring for my patients? The evidence-based Medicine Working Group. JAMA. 1994;271:703–707. doi: 10.1001/jama.271.9.703. [DOI] [PubMed] [Google Scholar]
- 21.Jellema P, Horst HE, Vlaeyen JW, Stalman WA, Bouter LM, Windt DA. Predictors of outcome in patients with (sub)acute low back pain differ across treatment groups. Spine. 2006;31:1699–1705. doi: 10.1097/01.brs.0000224179.04964.aa. [DOI] [PubMed] [Google Scholar]
- 22.Jensen MP, Turner JA, Romano JM. What is the maximum number of levels needed in pain intensity measurement? Pain. 1994;58:387–392. doi: 10.1016/0304-3959(94)90133-3. [DOI] [PubMed] [Google Scholar]
- 23.Klaber Moffett JA, Carr J, Howarth E. High fear-avoiders of physical activity benefit from an exercise program for patients with back pain. Spine. 2004;29:1167–1172. doi: 10.1097/00007632-200406010-00002. [DOI] [PubMed] [Google Scholar]
- 24.Klenerman L, Slade PD, Stanley IM, Pennie B, Reilly JP, Atchison LE, Troup JD, Rose MJ. The prediction of chronicity in patients with an acute attack of low back pain in a general practice setting. Spine. 1995;20:478–484. doi: 10.1097/00007632-199502001-00012. [DOI] [PubMed] [Google Scholar]
- 25.Linton SJ. A review of psychological risk factors in back and neck pain. Spine. 2000;25:1148–1156. doi: 10.1097/00007632-200005010-00017. [DOI] [PubMed] [Google Scholar]
- 26.Linton SJ, Hallden K. Can we screen for problematic back pain? A screening questionnaire for predicting outcome in acute and subacute back pain. Clin J Pain. 1998;14:209–215. doi: 10.1097/00002508-199809000-00007. [DOI] [PubMed] [Google Scholar]
- 27.Mannion AF, Junge A, Taimela S, Muntener M, Lorenzo K, Dvorak J. Active therapy for chronic low back pain: part 3. Factors influencing self-rated disability and its change following therapy. Spine. 2001;26:920–929. doi: 10.1097/00007632-200104150-00015. [DOI] [PubMed] [Google Scholar]
- 28.Naylor CD. Grey zones of clinical practice: some limits to evidence-based medicine. Lancet. 1995;345:840–842. doi: 10.1016/S0140-6736(95)92969-X. [DOI] [PubMed] [Google Scholar]
- 29.Obuchowski NA. Receiver operating characteristic curves and their use in radiology. Radiology. 2003;229:3–8. doi: 10.1148/radiol.2291010898. [DOI] [PubMed] [Google Scholar]
- 30.Pengel HM, Refshauge K, Maher C. Responsiveness of pain, disability, and physical impairment outcomes in patients with low back pain. Spine. 2004;29:879–883. doi: 10.1097/00007632-200404150-00011. [DOI] [PubMed] [Google Scholar]
- 31.Phillips HC. Avoidance behaviour and its role in sustaining chronic pain. Behav Res Ther. 1987;25:279. doi: 10.1016/0005-7967(87)90005-2. [DOI] [PubMed] [Google Scholar]
- 32.Picavet HS, Vlaeyen JW, Schouten JS. Pain catastrophizing and kinesiophobia: predictors of chronic low back pain. Am J Epidemiol. 2002;156:1028–1034. doi: 10.1093/aje/kwf136. [DOI] [PubMed] [Google Scholar]
- 33.Pincus T, Vlaeyen JW, Kendall NA, Korff MR, Kalauokalani DA, Reis S. Cognitive-behavioral therapy and psychosocial factors in low back pain: directions for the future. Spine. 2002;27:E133–E138. doi: 10.1097/00007632-200203010-00020. [DOI] [PubMed] [Google Scholar]
- 34.Poiraudeau S, Rannou F, Baron G, Le HA, Coudeyre E, Rozenberg S, Huas D, Martineau C, Jolivet-Landreau I, Garcia-Mace J, Revel M, Ravaud P. Fear-avoidance beliefs about back pain in patients with subacute low back pain. Pain. 2006;124:305–311. doi: 10.1016/j.pain.2006.04.019. [DOI] [PubMed] [Google Scholar]
- 35.Potter RG, Jones JM. The evolution of chronic pain among patients with musculoskeletal problems: a pilot study in primary care. Br J Gen Pract. 1992;42:462–464. [PMC free article] [PubMed] [Google Scholar]
- 36.Rothwell PM. External validity of randomised controlled trials: “to whom do the results of this trial apply?”. Lancet. 2005;365:82–93. doi: 10.1016/S0140-6736(04)17670-8. [DOI] [PubMed] [Google Scholar]
- 37.Sieben JM, Portegijs PJ, Vlaeyen JW, Knottnerus JA. Pain-related fear at the start of a new low back pain episode. Eur J Pain. 2005;9:635–641. doi: 10.1016/j.ejpain.2004.12.007. [DOI] [PubMed] [Google Scholar]
- 38.Sieben JM, Vlaeyen JW, Portegijs PJ, Verbunt JA, Riet-Rutgers S, Kester AD, Korff M, Arntz A, Knottnerus JA. A longitudinal study on the predictive validity of the fear-avoidance model in low back pain. Pain. 2005;117:162–170. doi: 10.1016/j.pain.2005.06.002. [DOI] [PubMed] [Google Scholar]
- 39.Staal JB, Hlobil H, Twisk JW, Smid T, Koke AJ, Mechelen W. Graded activity for low back pain in occupational health care: a randomized, controlled trial. Ann Intern Med. 2004;140:77–84. doi: 10.7326/0003-4819-140-2-200401200-00007. [DOI] [PubMed] [Google Scholar]
- 40.Swinkels-Meewisse EJ, Swinkels RA, Verbeek AL, Vlaeyen JW, Oostendorp RA. Psychometric properties of the Tampa Scale for kinesiophobia and the fear-avoidance beliefs questionnaire in acute low back pain. Man Ther. 2003;8:29–36. doi: 10.1054/math.2002.0484. [DOI] [PubMed] [Google Scholar]
- 41.Vlaeyen JW, Jong J, Geilen M, Heuts PH, Breukelen G. The treatment of fear of movement/(re)injury in chronic low back pain: further evidence on the effectiveness of exposure in vivo. Clin J Pain. 2002;18:251–261. doi: 10.1097/00002508-200207000-00006. [DOI] [PubMed] [Google Scholar]
- 42.Vlaeyen JW, Jong JR, Onghena P, Kerckhoffs-Hanssen M, Kole-Snijders AM. Can pain-related fear be reduced? The application of cognitive-behavioural exposure in vivo. Pain Res Manag. 2002;7:144–153. doi: 10.1155/2002/493463. [DOI] [PubMed] [Google Scholar]
- 43.Vlaeyen JW, Jong J, Geilen M, Heuts PH, Breukelen G. Graded exposure in vivo in the treatment of pain-related fear: a replicated single-case experimental design in four patients with chronic low back pain. Behav Res Ther. 2001;39:151–166. doi: 10.1016/S0005-7967(99)00174-6. [DOI] [PubMed] [Google Scholar]
- 44.Waddell G, Newton M, Henderson I, Somerville D, Main CJ. Fear-avoidance beliefs questionnaire and the role of fear-avoidance beliefs in chronic low back pain and disability. Pain. 1993;52:157–168. doi: 10.1016/0304-3959(93)90127-B. [DOI] [PubMed] [Google Scholar]
- 45.Watson PJ, Booker CK, Main CJ. Evidence for the role of psychological factors in abnormal paraspinal activity in patients with chronic low back pain. J Musculoskeletal Pain. 1997;4:41–56. doi: 10.1300/J094v05n04_05. [DOI] [Google Scholar]
- 46.Werneke M, Hart DL, Cook D. A descriptive study of the centralization phenomenon. A prospective analysis. Spine. 1999;24:676–683. doi: 10.1097/00007632-199904010-00012. [DOI] [PubMed] [Google Scholar]