Abstract
Background
Breast cancers (BC) in women carrying mutations in BRCA1 gene are more frequently estrogen receptor negative than the nonhereditary BC. Nevertheless, tamoxifen has been found to have a protective effect in preventing contralateral tumors in BRCA1 mutation carriers. The identification of the second human estrogen receptor, ERβ, raised a question of its role in hereditary breast cancer. The aim of this study was to assess the frequency of ERα, ERβ, PgR (progesterone receptor) and HER-2 expression in breast cancer patients with mutated BRCA1 gene and in the control group.
Methods
The study group consisted of 48 women with BRCA1 gene mutations confirmed by multiplex PCR assay. The patients were tested for three most common mutations of BRCA1 affecting the Polish population (5382insC, C61G, 4153delA). Immunostaining for ERα, ERβ and PgR (progesterone receptor) was performed using monoclonal antibodies against ERα, PgR (DakoCytomation), and polyclonal antibody against ERβ (Chemicon). The EnVision detection system was applied. The study population comprised a control group of 120 BC operated successively during the years 1998–99.
Results
The results of our investigation showed that BRCA1 mutation carriers were more likely to have ERα-negative breast cancer than those in the control group. Only 14.5% of BRCA1-related cancers were ERα-positive compared with 57.5% in the control group (P < 0.0001). On the contrary, the expression of ERβ protein was observed in 42% of BRCA1-related tumors and in 55% of the control group. An interesting finding was that most hereditary cancers (75% of the whole group) were triple-negative: ERα(-)/PgR(-)/HER-2(-) but almost half of this group (44.4%) showed the expression of ERβ.
Conclusion
In the case of BRCA1-associated tumors the expression of ERβ was significantly higher than the expression of ERα. This may explain the effectiveness of tamoxifen in preventing contralateral breast cancer development in BRCA1 mutation carriers.
Background
In 1990 Hall et al. discovered that familial breast cancer is associated with a defect in one of the genes located in the 17q21 chromosome [1]. This finding began a new era of research into hereditary breast cancer and consequently led to the identification of the BRCA1 and BRCA2 suppressor genes in 1994 and 1995, respectively. Although the structures and localization of the BRCA1 and BRCA2 genes differ, their functions seem to be similar because their transcripts are involved in the same processes [2-6]. These genes are responsible for maintaining the proper course of the cell cycle, for the repair of DNA damage, and are also instrumental in the process of cell differentiation. BRCA1 is also partially responsible for the activity of estrogen receptors (ER) and, when mutated, can inhibit the functions of these receptors [7].
BRCA1 and BRCA2 gene mutation carriers are at risk of developing breast cancer earlier than other patients. Breast cancer associated with this mutation has characteristic histopathological features: (i) the expression of estrogen and progesterone receptors is less frequently demonstrable, (ii) the grade of histopathological malignancy is higher and (iii) accumulation of p53 protein is observed more often than in sporadic cases of this malignancy [8,9]. Although these factors are usually associated with a poorer prognosis, their role in BRCA1 and BRCA2 mutation carriers is still controversial [10-15].
The role of tamoxifen in preventing the development of contralateral breast cancer in BRCA1 mutation carriers is not fully understood since it significantly reduces that risk despite low expression of ER [16]. The mechanism responsible for that has not been yet explained and estrogen receptor β may play a role here.
Estrogen receptor β (ERβ) was discovered in 1996 and was given its name in order to differentiate it from the previously known type of estrogen receptor (now named estrogen receptor α – ERα) [17,18]. The two estrogen receptors belong to a family of ligand-regulated transcription factors. They are transcripts of different genes sharing some structural similarities. When co-expressed, ERα and ERβ may form homo- or heterodimers upon binding specific ligands. As dimers, ERs are able to start transcription activity in two ways: through direct binding to specific regions of DNA, or through protein-protein interaction with other transcription factors. In the case of co-expression of both ERs, their roles may overlap. In certain situations, however, ERβ opposes the activity of ERα via the inhibition of ERα-mediated gene expression. These differences are also observed in the response to tamoxifen. This selective estrogen receptor modulator may work as a pure ER antagonist for ERβ, while it may have a partially agonistic effect for ERα [19]. In spite of increasing knowledge regarding the structure and in vitro activity of ERα and ERβ, their clinical role is still controversial and unclear [20].
For a better understanding of the functions of ERβ we explored its expression in BRCA1 mutation carriers and looked for coexistence patterns with other hormonal receptors (ERα, PgR) and HER-2 receptor.
Methods
The study group included 48 patients with mutations in the BRCA1 gene. The control group consisted of 120 subsequent breast cancer cases diagnosed over the period of 1998–1999. Patients from both groups underwent breast surgery from which specimens for histological and immunohistochemical testing were obtained. The study was approved by the local Bioethics Committee at the Medical University in Poznań.
Results of genetic tests were obtained from the Prophylactics and Epidemiology Center in Poznań. In the search for mutations in the BRCA1 gene, tests were performed on DNA isolated from peripheral blood lymphocytes using a commercially available kit. They were carried out for three most common mutations of BRCA1 gene affecting the Polish population (5382insC, C61G, 4153delA). In Poland those three mutations in BRCA1 account for 86% of all BRCA1 and BRCA2 mutations. In the search for 5382insC and 4153delA mutations, the ASA-PCR method was used. For the detection of C61G mutation, the RELP-PCR method was applied.
Histological and immunohistochemical tests were completed in the Department of Tumor Pathology of the Medical University in Poznań. From formalin fixed and paraffin embedded specimens, 4 μm sections were cut and mounted onto positively charged glass microscope slides (Superfrost Plus, Menzel-Glaser, Germany). The sections were deparaffinized, rehydrated and subjected to antigen retrieval in citrate buffer in a microwave oven. The slides were then incubated in 3% hydrogen peroxide for 10 minutes to block endogenous peroxidase activity.
The primary antibodies used for immunostaining were as follows:
1. for ERα – a monoclonal mouse antibody clone 1D5 (Dako, Glostrup, Denmark; code No M 7047) was used at 1:50 dilution and slides were incubated at room temperature for 1 h;
2. for ERβ – a polyclonal rabbit antibody in which immunogen corresponds to NH2-terminus of the human ERβ, and, according to the manufacturer, the sequence used is conserved in all known isoforms (Chemicon International, Temecula, CA; catalog No AB1410). This antibody was used at a dilution of 1:500 and overnight in an incubation chamber at 4°C;
3. for PgR – a monoclonal mouse antibody clone PgR636, (Dako, Glostrup, Denmark; code M 3569) was used at a dilution of 1:100 and slides were incubated at room temperature for 1 h. This antibody (according to the manufacturer) has been demonstrated by Western blot to react with both forms of the progesterone receptor: the PR-A and PR-B.
The antibody reactions were revealed using Dako EnVision™+System-HRP. Subsequently the slides were incubated in DAB chromogen for 5 minutes at room temperature. The sections were counterstained with hematoxylin, and coverslipped.
Immunostained slides were evaluated by two independent observers in a "blinded" fashion, using light microscopy. Tumors were considered to be expressing receptors if a positive reaction (regardless of its intensity) was identified in at least 10% of the cancer cells' nuclei.
HER-2 protein was identified by means of the HecepTest™ kit (Dako). Tumors were classified as 0, 1+, 2+ or 3+ on the basis of the spread and intensity of membranous staining in invasive portions of the cancer. Tumors showing staining reactions in class 3+ were considered to be over-expressing HER-2. In the case of the 2+ results obtained, suggestive of over-expression of the HER-2 protein, amplification of the c-erbB2 gene was tested by the application of fluorescent in-situ hybridization (FISH). Cases with an immunohistochemistry result of 2+ but without amplification of the gene, as tested by FISH, were not considered to be over-expressing HER2.
To assess dependences Fisher' Exact Test (for 2 × 2 contingency tables) and the Fisher-Freeman-Halton (for larger contingency tables) test were applied. Significance was accepted at P < 0.05.
Results
The clinicopathological characteristics of breast cancer patients with mutated BRCA1 gene and those of the control group are shown in Table 1. BRCA1 gene mutations in the study group were identified as follows: 5382insC (77.5%), C61G (20.4%) and 4153delA (2%).
Table 1.
Clinicopathological characteristics of patient cohorts
| Parameter | BRCA1-associated breast cancers n = 48 | Control group n = 120 | P-value |
| Age | |||
| median (range) | 45 (29 – 68) | 57 (38 – 85) | <0.0001 |
| Age > 50 years | 16 (33%) | 82 (68%) | |
| Histological type | |||
| invasive ductal | 42 (87%) | 103 (85.8%) | 0.7993 |
| invasive lobular | 1 (2%) | 10 (8.3%) | 0.14 |
| medullary like | 5 (10%) | 0 | < 0.001 |
| other | 0 | 9 (7.5%) | < 0.001 |
| Tumor grade | |||
| I | 1 (2.0%) | 36 (29%) | <0.001 |
| II | 11 (22.9%) | 53 (44.1%) | 0.0122 |
| III | 27 (56.2%) | 26 (21.7%) | <0.0001 |
| unknown | 9 (18.7%) | 5 (4.2%) | 0.0017 |
| Tumor size | |||
| median | 2.2 | 3.0 | 0.14 |
| ≤ 2 cm | 28 (58.3%) | 53 (44.1%) | 0.102 |
| > 2 cm ≤ 5 cm | 16 (33.3%) | 50 (41.6%) | 0.282 |
| > 5 cm | 3 (6.2%) | 17 (14.1%) | 0.147 |
| unknown | 1 (2.0%) | 0 | |
| Lymph node | |||
| negative | 34 (70.8%) | 52 (43.3%) | 0.001 |
| positive ≤ 3 | 8 (16.6%) | 38 (31.6%) | 0.015 |
| positive >3 | 4 (8.3%) | 22 (18.0%) | 0.104 |
| unknown | 2 (4.1%) | 8 (6.6%) | |
| Bilateral breast cancer | 13 (27.1%) | 2 (1.7%) | <0.0001 |
| Mutation: | |||
| 5382insC | 37 (77.5%) | ||
| C61G | 10 (20.4%) | ||
| 4153delA | 1 (2%) |
The average age of patients with mutations in the BRCA1gene was 45 years, and 57 years in the control group.
Invasive ductal carcinoma (no special type) was found to occur at the same frequency in both the BRCA1-positive group as well as the control group (87% and 85.8%, respectively). Other tumor types were much less frequent, although it is noteworthy that all 5 patients with "medullary like" carcinoma came from the BRCA1 mutation carriers group (10%).
The assessment of histological malignancy was performed according to the Bloom-Richardson classification and showed that patients carrying BRCA1 mutations developed grade 3 tumors more often and had less frequent metastases to axillary lymph nodes.
In the BRCA1-positive group, the rate of patients who developed bilateral breast cancer accounted for 27.1% (13 cases). In the control group, bilateral breast cancer was found in 2 patients only (1.7%).
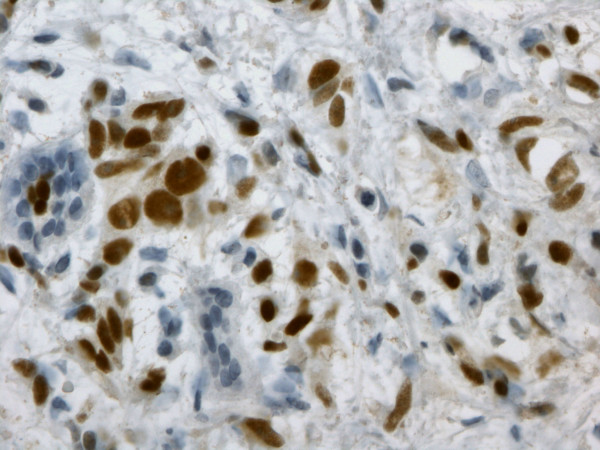
The presence of estrogen receptor α was detected in the tumors of 7 (14.5%) patients with BRCA1gene mutations and in 69 patients (57.5%) in the control group (Fig. 1).
Figure 1.
ERα immunostaining on paraffin-embedded invasive breast cancer using 1D5 Dako antibody (40× magnification).
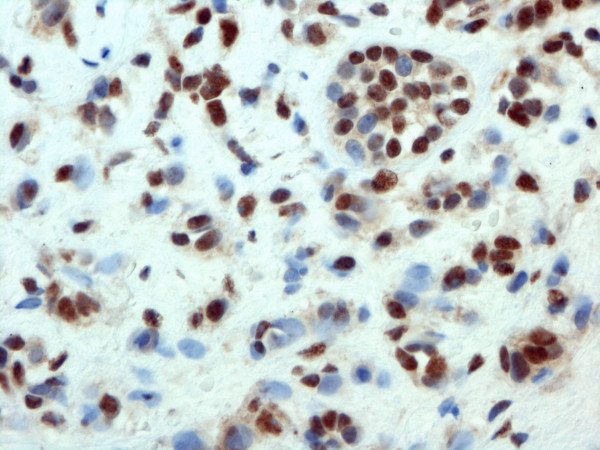
For progesterone receptors, the figures were 6 (12.5%) and 77 (64%), respectively. The expression of estrogen receptor β was detected in the tumors of 20 (42%) of the BRCA1-mutation patients and in 66 (55%) of the subjects in the control group (Table 2) (Fig. 2).
Table 2.
Receptor status in BRCA1-associated breast cancer and in cancer of the control group
| Expression of steroid receptors | BRCA1-associated breast cancers n = 48 | Control group n = 120 | P-value | ||
| n | (%) | n | (%) | ||
| ERα(+) | 7 | 14.5 | 69 | 57.5 | <0.0001 |
| ERβ(+) | 20 | 42 | 66 | 55 | 0.129 |
| PgR(+) | 6 | 12.5 | 77 | 64 | <0.0001 |
| HER2(+) | 3 | 6.2 | 20 | 16.7 | 0.064 |
Figure 2.
ERβ immunostaining on paraffin-embedded invasive breast cancer using antibody from Chemicon (40× magnification).
In the group with BRCA1 mutations, the most frequently found phenotype was ERα(-)/ERβ(-) observed in 52% of patients, followed by ERα(-)/ERβ(+) noticed in 33.3% cases. In the control group only 14.2% of the patients presented phenotype ERα(-)/ERβ(+). The most common phenotype observed in that group was ERα(+)/ERβ(+) – 40.8% (Table 3).
Table 3.
The distribution of ERα and ERβ in BRCA1-associated breast cancers and in cancers of the control group
| Receptors' status | BRCA1-associated breast cancers n = 48 | Control group n = 120 | P | ||
| N | (%) | N | (%) | ||
| ERα(+)/ERβ(+) | 4 | 8.3 | 49 | 40.8 | <0.0001 |
| ERα(+)/ERβ(-) | 3 | 6.2 | 20 | 16.7 | 0.086 |
| ERα(-)/ERβ(+) | 16 | 33.3 | 17 | 14.2 | 0.009 |
| ERα(-)/ERβ(-) | 25 | 52 | 34 | 28.3 | 0.004 |
The over-expression of the HER-2 receptor in patients with mutated BRCA1 genes was observed only in 3 cases (6.2%). In the control group over-expression of HER-2 was found in 20 cases (16.7%).
An interesting finding of this study is that most hereditary cancers have been found to be triple-negative: ERα(-)/PgR(-)/HER-2(-). Such a phenotype was found in 36 cases, which accounts for 75% of the whole group of patients with a mutated BRCA1 gene. 16 patients in that group expressed ERβ and presented the following phenotype: ERα(-)/PgR(-)/HER2(-)/ERβ(+). In the control group, the triple-negative phenotype was found in 24 patients (20%) of whom 5 had tumors expressing ERβ.
Discussion
In our study, patients with BRCA1 gene mutations were tested for the expression of steroid receptors (ERβ, ERα and PgR) and the HER-2 receptor in breast cancer tissue. In this group, ERβ was more common (42%), while ERα and PgR occurred less frequently (14.5% and 12.5% respectively). In the control group, the expression of ERα and PgR was 57.5 and 64%, respectively. In the case of ERα and PgR, the differences between the two groups were found to be statistically significant (p = 0.001). Those values are similar to those described by other authors [8,12,21,22]. In the case of ERβ, however, the differences of expression between those two groups were small.
Most of our control group patients were tested for the presence of BRCA1 mutations. Although those tests were not performed on all the controls, this cannot influence the overall findings of the study since in Poland BRCA1 mutations (unselected for age) occur only in about 3% of all breast cancer patients [23].
It has been pointed out in many studies that BRCA1 positive breast cancers rarely express ERα [8-12,20,21]. Further confirmation of that observation comes from recent studies made with the use of the cDNA microarray technique, showing that breast cancers may vary considerably in their molecular profile [24,25]. The largest group consists of tumors with a cellular profile matching that of the inner layers of the mammary glands, such as luminal cells (luminal types) and another group consists of tumors with basal cell profiles (basal types). These two groups differ in their expression of ERα. The luminal types express ERα, while the basal types usually do not. cDNA studies of breast cancers with underlying BRCA1 gene mutations show that the most common cancer type in this group is basal [26]. Moreover, basal type tumors show expression of receptors for epidermal growth factor (EGFR) more often. Generally, about half of the patients with BRCA1 gene mutations present the phenotype ER(-)/HER2(-)/EGFR(+) of the basal type of tumor, which is usually associated with poor prognosis [26-28]. On the other hand, there are data that suggest that the prognosis for BRCA1-positive patients is no worse than that for patients without mutations [10-14]. This discrepancy may suggest the influence of some incompletely explored prognostic and predictive factor(s).
Recent analyses suggest that ERβ may be an independent prognostic and predictive factor in the course of breast cancer [29-33]. However, its role has not yet been fully discovered. It is noteworthy that in our clinical material (in contrast to ERα) the expression of the ERβ in tumor tissues of patients with BRCA1 gene mutations is almost as frequent as in the non-hereditary breast cancer patients. It would be interesting to test whether frequent representation of ERβ in BRCA-positive tumors is actually responsible for the earlier reported activity of tamoxifen in the reduction of contralateral breast cancer risk.
Fan et al. showed that there is a link between estrogen receptors and the BRCA1 protein. In an in vitro study, BRCA1 protein proved to be one of the transcription regulators for active ERα. The transcription co-activator p300 plays an important role in this process, and its presence correlates with the ability of the BRCA1 protein to suppress the activation of ERα transcription [7].
Our study group displayed certain characteristics of hereditary breast cancer. One of these features was the young age of the patients. In this group, the average age of breast cancer diagnosis was 45 years, 12 years earlier than in the control group. The same average age at which the diagnosis was established, was reported for Spanish families and a similar age (43 years) in Markus's study of the population of Ashkenazi Jews [10]. Age is a well known factor influencing the expression of ERα. The fact that there was a 12-year difference in the average age between the BRCA1 gene mutations group and the control group must have some influence on the reported ERα expression in our study. Regarding ERβ expression, however, we believe that difference bears no material significance on the result. Our opinion is based on the fact that numerous studies have indicated that the expression of ERβ is not age-dependent.
In both groups, the most frequent histological diagnosis was that of ductal carcinoma (87% and 85.8%, respectively). Another common histological type of breast cancer found in the mutation carriers group was "medullary like" carcinoma (10%). In the control group, however, not a single case of that type of cancer was identified. A higher rate of "medullary like" carcinoma is typical of BRCA1 mutation carriers and this diagnosis is associated with a relatively good prognosis [34,35]. Consequently, it was believed that this diagnosis positively affected the prognosis for BRCA1-positive patients. Unfortunately, a recent study failed to confirm that finding [36].
Patients with hereditary disease have been found to develop bilateral breast cancer more often. Our study has confirmed this observation as it has been found that bilateral breast cancer affected 13 patients of the study group (27.1%).
The above characteristics of hereditary breast cancer have been frequently described in the literature and are consistent with the previously published data. Little, however, has been said regarding the expression of ERβ. This appears to have been mentioned only once in a letter to the Editor of the Journal of Clinical Oncology which reported on estrogen receptor-beta expression in hereditary breast cancer where positive staining for ERβ was detectable in 94% (15 of 16) of BRCA1 associated breast cancers [37].
In our study, ERβ expression was present in 42% of BRCA1 mutation carriers. This seems to be important as it may explain the protective effect of tamoxifen in the prevention of contralateral tumor development in BRCA1 mutation carriers.
Out of the hereditary cancer patients in our study group, 75% were found to be triple-negative, lacking ERα, PgR and HER-2 over-expression. Unfortunately, at the current state of the art, neither hormonal therapy, nor immunotherapy (trastuzumab) in an adjuvant setting, can be offered to those patients.
Gruvberger-Saal et al [38] reported that the expression of ERβ is an independent marker for favourable prognosis after adjuvant tamoxifen treatment in ERα negative breast cancer patients. Bearing in mind that as many as 44% of the triple-negative patients in our study expressed ERβ, we propose that hormone therapy might be used in the treatment of BRCA1 mutation carriers expressing the ERα(-)/PgR(-/HER2(-)/ERβ(+) phenotype.
The results obtained in our study show that the expression of ERβ in BRCA1 gene mutation carriers is statistically higher than the expression of ERα. This may be why tamoxifen has proven to be effective in preventing the development of contralateral breast cancer in BRCA1 mutation carriers. Consequently, testing patients carrying BRCA1 mutations for the presence of ERβ might help to identify those who could benefit from endocrine therapy.
Conclusion
In the case of BRCA1-associated tumors the expression of ERβ was significantly higher than the expression of ERα. This may explain the effectiveness of tamoxifen in preventing contralateral breast cancer development in BRCA1 mutation carriers.
Abbreviations
ER – estrogen receptor
ERα – estrogen receptor alpha
ERβ – estrogen receptor beta
PgR – progesterone receptor
BRCA1 – breast cancer associated gene
BRCA2 – breast cancer associated gene
PCR – polymerase chain reaction
HER-2 – human epidermal growth factor receptor-2
SERM – selective estrogen receptor modulator
IHC – immunohistochemistry
ASA-PCR – amplicon sequence analysis – polymerase chain reaction
RFLP-PCR – restriction fragment length polymorphism – polymerase chain reaction
FISH – fluorescent hybridization in situ
EGFR – epidermal growth factor receptor
cDNA – complementary DNA
Competing interests
The author(s) declare that they have no competing interests.
Authors' contributions
ML conceived, designed and performed the study, coordinated the work and drafted the manuscript, KR participated in the draft of the manuscript, VF performed IHC tests, DG and MS carried out genetic tests, RK reviewed the manuscript and offered some comments, JB interpreted histopathological and IHC test results. All authors have read and approved the final manuscript.
Pre-publication history
The pre-publication history for this paper can be accessed here:
Contributor Information
Maria M Litwiniuk, Email: litwiniuk@skrzynka.pl.
Krzysztof Rożnowski, Email: krzysztof.roznowski@oncology.am.poznan.pl.
Violetta Filas, Email: vfilas@wp.pl.
Dariusz D Godlewski, Email: godlewski.open@wp.pl.
Małgorzata Stawicka, Email: gosiastawicka.open@wp.pl.
Remigiusz Kaleta, Email: remigiusz.kaleta@pharmacia.com.
Jan Bręborowicz, Email: janbreborowicz@wp.pl.
References
- Hall JM, Lee MK, Newman B, Morrow JE, Anderson LA, Huey B, King MC. Linkage of early-onset familial breast cancer to chromosome 17q21. Science. 1990;250:1684–1689. doi: 10.1126/science.2270482. [DOI] [PubMed] [Google Scholar]
- Krainer M, Silvia-Arrieta S, Fitzgerald MG, Shimada A, Ishioka C, Kanamaru R, MacDonald DJ, Unsal H, Finkelstein DM, Bowcock A, Isselbacher KJ, Haber DA. Differential contributions of BRCA1 and BRCA2 to early-onset breast cancer. N Engl J Med. 1997;336:1416–1421. doi: 10.1056/NEJM199705153362003. [DOI] [PubMed] [Google Scholar]
- Struewing JP, Hartge P, Wacholder S, Baker SM, Berlin M, McAdams M, Timmerman MM, Brody LC, Tucker MA. The risk of cancer associated with specific mutations of BRCA1 and BRCA2 among Ashkenazi Jews. N Engl J Med. 1997;336:1401–1408. doi: 10.1056/NEJM199705153362001. [DOI] [PubMed] [Google Scholar]
- Miki Y, Swensen J, Shattuck-Eidens D, Futreal PA, Harshman K, Tavtigian S, Liu Q, Cochran C, Bennett LM, Ding W. A strong candidate for the breast and ovarian cancer susceptibility gene BRCA1. Science. 1994;266:66–71. doi: 10.1126/science.7545954. [DOI] [PubMed] [Google Scholar]
- Wooster R, Bignell G, Lancaster J, Swift S, Seal S, Mangion J, Collins N, Gregory S, Gumbs C, Micklem G, Berfoot R, Hamoudi R, Patel S, Rices C, Biggs P, Hashim J, Smith A, Connor F, Arason A, Gudmundsson J, Ficenec D, Kelsell D, Fordtonin DP, Bishop TD, Spurr NK, Ponder BAJ, Eeles R, Peto J, Devilee P, Cornelisse C, Lynch H, Narod S, Lenoir G, egilsson V, barkadottir RB, Easton DF, Bentley DR, Futreal A, Ashworth A, Stratton MR. Identification of the breast cancer susceptibility gene BRCA2. Nature. 1995;378:789–792. doi: 10.1038/378789a0. [DOI] [PubMed] [Google Scholar]
- Martin AM, Weber BL. Genetic and hormonal risk factor in breast cancer. J Natl Cancer Inst. 2000;92:1126–35. doi: 10.1093/jnci/92.14.1126. [DOI] [PubMed] [Google Scholar]
- Fan S, Ma YX, Wang C, Yuan R-Q, Meng Q, Wang L-A, Erdos M, Goldberg ID, Webb P, Kushner PJ, Pestell RG, Rosen EM. p300 Modulates the BRCA1 inhibition of estrogen receptor activity. Cancer Res. 2002;62:141–151. [PubMed] [Google Scholar]
- Lakhani SR, van de Vijver MJ, Jacquemier J, Thomas J, Anderson TJ, Osin PP, McGuffog L, Easton DF. The pathology of familial breast cancer: predictive value of immunohistochemical markers estrogen receptor, progesterone receptor, HER-2, and p53 in patients with mutations in BRCA1 and BRCA2. J Clin Oncol. 2002;20:2310–2318. doi: 10.1200/JCO.2002.09.023. [DOI] [PubMed] [Google Scholar]
- Honrado E, Benitez J, Palacios J. The pathology of hereditary breast cancer. Hereditary Cancer Clin Pract. 2004;2:131–138. doi: 10.1186/1897-4287-2-3-131. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Marcus JN, Watson P, Page DL, Narod SA, Lenoir GM, Tonin P, Linder-Stephenson L, Salerno G, Conway TA, Lynch HT. Hereditary breast cancer. Pathology, prognosis, and BRCA1 and BRCA2 gene linkage. Cancer. 1996;77:697–709. doi: 10.1002/(SICI)1097-0142(19960215)77:4<697::AID-CNCR16>3.0.CO;2-W. [DOI] [PubMed] [Google Scholar]
- Porter DE, Cohen BB, Wallace MR, Smyth E, Chetty U, Dixon JM, Steel CM, Carter DC. Breast cancer incidence, penetrance and survival in probable carriers of BRCA1 gene mutation in families linked to BRCA1 on chromosome 17q12-21. Br J Surg. 1994;10:1512–1515. doi: 10.1002/bjs.1800811038. [DOI] [PubMed] [Google Scholar]
- Verhoog LC, Brekelmans CT, Seynaeve C, van den Bosch LM, Dahmen G, van Geel AN, Bartels CC, Tilanus-Linthorst MM, Wagner A, Devilee P, Halley DJJ, van den Ouweland AM, Meijers-Heijboer EJ, Klijn JGM. Survival and tumor characteristics of breast-cancer patients with germline mutations of BRCA1. Lancet. 1998;351:316–321. doi: 10.1016/S0140-6736(97)07065-7. [DOI] [PubMed] [Google Scholar]
- Gaffney DK, Brohet RM, Lewis CM, Holden JA, Buys SS, Neuhausen SL, Steele L, Avizonis V, Stewart JR, Cannon-Albright LA. Response to radiation therapy and prognosis in breast cancer patients with BRCA1 and BRCA2 mutations. Radiother Oncol. 1998;47:129–136. doi: 10.1016/S0167-8140(98)00023-1. [DOI] [PubMed] [Google Scholar]
- Stoppa-Lyonnet D, Ansquer Y, Dreyfus H, Gautier C, Gauthier-Villars M, Bourstyn E, Clough KB, Magdelénat H, Pouillart P, Vincent-Salomon A, Fourquet A, Asselain B. Familial Invasive breast cancer: worse outcome related to BRCA1 mutations. J Clin Oncol. 2000;18:4053–4059. doi: 10.1200/JCO.2000.18.24.4053. [DOI] [PubMed] [Google Scholar]
- Robson ME, Chappuis PO, Satagopan J, Wong N, Boyd J, Goffin JR, Hudis C, Roberge D, Norton L, Bégin LR, Offit K, Foulkes WD. A combined analysis of outcome following breast cancer: Differences in survival based on BRCA1 /BRCA2 mutation status and administration of adjuvant treatment. Breast Cancer Res. 2004;6:R8–R17. doi: 10.1186/bcr658. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Narod SA, Brunet JS, Ghadirian P, Robson M, Heimdal K, Neuhausen SL, Stoppa-Lyonnet D, Lerman C, Pasini B, de los Rios P, Weber B, Lynch H. Tamoxifen and risk of contralateral breast cancer in BRCA1 and BRCA2 mutation carriers: a case-control study. Lancet. 2000;356:1876–1881. doi: 10.1016/S0140-6736(00)03258-X. [DOI] [PubMed] [Google Scholar]
- Kuiper GG, Enmark E, Pelto-Huikko M, Nilsson S, Gustaffson JA. Cloning of a novel receptor expressed in rat prostate and ovary. Proc Natl Acad Sci USA. 1996;93:5925–5930. doi: 10.1073/pnas.93.12.5925. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mosselman S, Polman J, Dijkema R. ER-β: identification and characterisation of a novel human estrogen receptor. FEBS Lett. 1996;392:49v53. doi: 10.1016/0014-5793(96)00782-X. [DOI] [PubMed] [Google Scholar]
- Barkhem T, Carlsson B, Nilsson Y, Enmark E, Gustafsson J-Å, Nilsson S. Differential response of estrogen receptor alpha and estrogen receptor β to partial estrogen agonists/antagonists. Mol Pharmacol. 1998;54:105–112. doi: 10.1124/mol.54.1.105. [DOI] [PubMed] [Google Scholar]
- Speirs V. Oestrogen receptor β in breast cancer: good, bad or still too early to tell? J Pathol. 2002;197:143–147. doi: 10.1002/path.1072. [DOI] [PubMed] [Google Scholar]
- Eisinger F, Jacquemier J, Nogues C, Birnbaum D, Sobol H. Steroid receptors in hereditary breast carcinomas associated with BRC1 or BRCA2 mutations or unknown susceptibility genes. Cancer. 1999;85:2291–2295. doi: 10.1002/(SICI)1097-0142(19990515)85:10<2291::AID-CNCR26>3.0.CO;2-9. [DOI] [PubMed] [Google Scholar]
- Lynch BJ, Holden JA, Buys SS, Neuhausen SL, Gaffney DK. Pathobiologic characteristics of hereditary breast cancer. Hum Pathol. 1998;29:1140–1144. doi: 10.1016/S0046-8177(98)90427-0. [DOI] [PubMed] [Google Scholar]
- Górski B, Cybulski C, Huzarski T, Byrski T, Gronwald J, Jakubowska A, Stawicka M, Grodecka-Gazdecka S, Szwiec M, Urbański K, Mituś J, Marczyk E, Dziuba J, Wandzel P, Surdyka D, Haus O, Janiszewska H, Dębniak T, Tołoczko-Grabarek A, Medrek K, Masojć B, Mierzejewski M, Kowalska E, Narod SA, Lubiński J. Breast cancer predisposing alleles in Poland. Breast Cancer Res Treat. 2005;92:19–24. doi: 10.1007/s10549-005-1409-1. [DOI] [PubMed] [Google Scholar]
- Sørlie T, Perou CHM, Tibshirani R, Aas T, Geisler S, Johnsen H, Hastie T, Eisen MB, van de Rijn M, Jeffrey SS, Thorsen T, Quist H, Matese JC, Brown PO, Botstein D, Eystein Lønning P, Børresen-Dale AL. Gene expression patterns of breast carcinomas distinguish tumor subclasses with clinical implications. PNAS. 2001;98:10869–10874. doi: 10.1073/pnas.191367098. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sørlie T, Tibishirani R, Parker J, Hastie T, Marron JS, Nobel A, Deng S, Johnsen H, Pesich R, Geisler S, Demeter J, Perou CM, Lonning PE, Brown PO, Borresen-Dale A-L, Botstein D. Repeated observation of breast tumor subtypes in independent gene expression data sets. PNAS. 2003;100:8418–8423. doi: 10.1073/pnas.0932692100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Foulkes WD, Stefansson IM, Chappuis PO, Bégin LR, Goffin JR, Wong N, Trudel M, Akslen LA. Germline BRCA1 mutations and a basal epithelial phenotype in breast cancer. J Natl Cancer Inst. 2003;95:1482–1485. doi: 10.1093/jnci/djg050. [DOI] [PubMed] [Google Scholar]
- van der Groep P, Bouter A, van der Zanden R, Menko FH, Buerger H, Verheijen RHM, van der Wall E, van Diest PJ. RE: Germline BRCA1 mutations and a basal epithelial phenotype in breast cancer. J Natl Cancer Inst. 2004;96:712. doi: 10.1093/jnci/djh114. [DOI] [PubMed] [Google Scholar]
- Faulkes WD, Brunet JS, Stefansson IM, Straume O, Chappuis PO, Bégin LR, Hamel N, Goffin JR, Wong N, Trudel M, Kapusta L, Porter P, Akslen LA. The prognostic implication of basal-like (cycline E high/p27 low/p53+ glomeruloid-microvascular-proliferation +) phenotype of BRCA1-related breast cancer. Cancer Res. 2004;64:830–835. doi: 10.1158/0008-5472.CAN-03-2970. [DOI] [PubMed] [Google Scholar]
- Omoto Y, Inoue S, Ogawa S, Toyama T, Yamashita H, Muramatsu M, Kobayashi S, Iwase H. Clinical value of the wild-type estrogen receptor beta expression in breast cancer. Cancer Lett. 2001;163:207–212. doi: 10.1016/S0304-3835(00)00680-7. [DOI] [PubMed] [Google Scholar]
- Hopp T, Weiss H, Parra I, Cui Y, Osborne , Fuqua S. Low levels of estrogen receptor beta protein predict resistance to tamoxifen therapy in breast cancer. Clin Cancer Res. 2004;10:7490–7499. doi: 10.1158/1078-0432.CCR-04-1114. [DOI] [PubMed] [Google Scholar]
- Esslimani-Sahla M, Simony-Lafontaine J, Kramar A, Lavaill R, Mollevi C, Warner M, Gustafsson J-A, Rochefort H. Estrogen receptor beta (ERbeta) level but not its ERbetacx variant helps to predict tamoxifen resistance in breast cancer. Clin Cancer Res. 2004;10:5769–5776. doi: 10.1158/1078-0432.CCR-04-0389. [DOI] [PubMed] [Google Scholar]
- O'Neill P, Davies M, Shaaban A, Innes H, Torevell A, Sibson D, Foster C. Wild-type oestrogen receptor beta (ERbeta1) mRNA and protein expression in Tamoxifen-treated post-menopausal breast cancers. Br J Cancer. 2004;91:1694–1702. doi: 10.1038/sj.bjc.6602183. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Murphy LC, Watson PH. Is oestrogen receptor-β predictor of endocrine therapy responsiveness in human breast cancer. Endocr Relat Cancer. 2006;13:327–334. doi: 10.1677/erc.1.01141. [DOI] [PubMed] [Google Scholar]
- de la Hoya M, Osario A, Godino J, Sullerio S, Tosar A, Perez-Segura P, Fernandez C, Rodríguez R, Díaz-Rubio E, Benítez J, Devilee P, Caldés T. Association between BRCA1 and BRCA2 mutations and cancer phenotype in Spanish breast/ovarian cancer families: implication for genetic testing. Int J Cancer. 2002;97:466–471. doi: 10.1002/ijc.1627. [DOI] [PubMed] [Google Scholar]
- Adem C, Reynolds C, Soderberg CL, Slezak JM, McDonnell SK, Sebo TJ, Schaid DJ, Myers JL, Sellers TA, Hartmann LC, Jenkins RB. Pathologic characteristics of breast parenchyma in patients with hereditary breast carcinoma, including BRCA1 and BRCA2 mutation carriers. Cancer. 2003;97:1–11. doi: 10.1002/cncr.11048. [DOI] [PubMed] [Google Scholar]
- Rosen EM, Fan S, Isaacs C. BRCA1 in hormonal carcinogenesis: basic and clinical research. Endocr Relat Cancer. 2005;12:533–548. doi: 10.1677/erc.1.00972. [DOI] [PubMed] [Google Scholar]
- Daidone MG, Veneroni S, Capelletti V, Radice P, Pierotti MA, Younes M. Estrogen receptor-beta expression in hereditary breast cancer. J Clin Oncol. 2002;20:3752–3753. doi: 10.1200/JCO.2002.99.116. [DOI] [PubMed] [Google Scholar]
- Gruvberger-Saal SK, Bendahl PO, Saal LH, Laakso M, Hegardt C, Eden P, Peterson C, Malmstro P, Isola J, Borg A, Ferno M. Estrogen receptor β expression is associated with tamoxifen response in ERα-negative breast carcinoma. Clin Cancer Res. 2007;13:1987–1994. doi: 10.1158/1078-0432.CCR-06-1823. [DOI] [PubMed] [Google Scholar]