Abstract
Background and objectives: No studies have evaluated the relationship among spirituality, social support, and survival in patients with ESRD. This study assessed whether spirituality was an independent predictor of survival in dialysis patients with ESRD after controlling for age, diabetes, albumin, and social support.
Design, setting, participants, & measurements: A total of 166 patients who had ESRD and were treated with hemodialysis completed questionnaires on psychosocial variables, quality of life, and religious and spiritual beliefs. The religious variables were categorized into three scores on a 0 to 20 scale (low to high levels): Spirituality, religious involvement, and religion as coping. Social support was assessed using the Multidimensional Scale for Perceived Social Support. Analyses were also performed including and excluding patients with HIV infection. Religious variables were categorized on the basis of means, medians, and tertiles.
Results: In analyses that used religious variables, only the responses on the spirituality scale split at the mean were associated with survival. The association of other religious variables with survival did not reach significance. Social support correlated with spirituality, religion as coping, and religious involvement measures. Only social support and age were associated with survival when controlling for diabetes, albumin concentration, HIV infection, and spirituality.
Conclusions: These data suggest that the effects of spirituality may be mediated by social support. Larger, multicenter, prospective studies that use well-validated tools to measure religiosity and spirituality are needed to determine whether there is an independent association of spirituality variables with survival in patients with ESRD.
Relationships between spirituality and mortality have been investigated in medical populations but remain controversial (1–13). Variable associations have been found depending on definitions of spirituality and patient populations studied (1–11). Miller and Thoreson (12) explored nine different hypotheses regarding the relationship among religious beliefs, spirituality, and mortality. The only hypothesis that they found to be supported by persuasive evidence stated that “church/service attendance protects [only] healthy people against death.” Studies supporting a similar link in patients with chronic illnesses have also shown mixed results. Koenig et al. (14) evaluated approximately 4000 elderly patients to determine whether attendance at religious services during a 6-yr period was associated with survival. In adjusted analyses, there was a significantly lower mortality in patients who frequently attended church services.
Many researchers have suggested a publication bias, whereby only the studies that indicate a significant relationship are published (13). Most studies cited the need for more research on the relationship between spirituality and mortality before any firm conclusions can be reached. In addition, the health dimensions of lack of belief have not been well explored.
There also exists considerable debate on how to operationalize religiosity and spirituality. Whereas the first term often is associated with participation in social institutions and adherence to specific beliefs and practices, the latter is a broader term that typically pertains to life's vital qualities and an overall broad belief in the immaterial features of life (12). Spirituality relates to transcendent values and relationships and the way people find meaning, purpose, and hope in life and in the midst of suffering (15). A person may be spiritual and not religiously observant or observe rituals without a spiritual focus.
Few studies have specifically evaluated the potential association between spirituality and survival in patients with ESRD (16,17). We (18) previously showed that religious and spiritual beliefs are associated with decreased perception of burden of illness, decreased depressive affect, increased perception of social support, and higher satisfaction with life and perception of quality of life in an urban, predominantly black ESRD population. We also found that a “spiritual beliefs scale” correlated with several quality-of-life measures in patients with ESRD (19). Even though many of these psychosocial measures have been shown to be related to survival independently, no study to our knowledge has demonstrated a link between spirituality and survival in this population.
We determined whether three variables related to spirituality, religious beliefs, and practices and faith (spirituality, religious involvement, and religion as a coping measure) were independently associated with survival in hemodialysis patients with ESRD. We then assessed the relationship between social support and survival, regardless of whether the spiritual variables were included in analyses. We hypothesized that spiritual variables would be associated with survival in patients with ESRD.
Materials and Methods
Patient Population and Demographics
Patients were recruited from two dialysis units under the direction of George Washington University Medical Center full-time faculty nephrologists, located in Washington, DC. The population is composed of primarily black patients and has been described previously (18).
Recruitment
All patients who were enrolled in chronic hemodialysis programs at the two dialysis units were eligible to participate. The recruitment period ranged between October 3, 2001, and November 26, 2003. Each patient was initially approached by a trained research assistant who explained the study in detail and invited patients to complete a series of questionnaires regarding psychological status and quality of life. Questionnaires were administered by research assistants, who recorded verbal responses. At the time of data collection, patients gave consent to use the data in mortality analyses. Data collection was approved by the George Washington University Medical Center Committee on Human Research. Follow-up for vital status continued through July 2005.
Data Collection
Research assistants tracked the status of all patients by interviews with doctors and staff at both dialysis units, who verified information in the facilities’ computer databases. Data obtained was current status (alive or deceased), date of death, date of transplantation, and last day of treatment (when no follow-up data were available).
Measures
We used four items to assess spiritual belief, the importance of attending religious services, and the use of religion in coping with disease. Each question was scored on a scale from 0 to 10. We defined the religious variables as previously conceptualized (18). The “spirituality” score, the perception of the importance of faith and its helpfulness in coping with kidney failure, was the combination of questions 4 and 5 (Table 1). “Religious involvement,” or the perception of the importance of attending religious services and its helpfulness in coping with kidney failure, was defined as the combination of items 6 and 7. In addition, questions 5 and 7 were combined to form a “religion as a coping mechanism” score, a measure of religious feelings as coping mechanisms for dealing with the burden of kidney disease. Each question was scored on a scale from 0 to 10. The highest score attainable was 20 (10 points for each individual item) for each variable.
Table 1.
Questions regarding religious beliefsa
| I have felt physically terrible/well. |
| My life is worthless/worthwhile. |
| My life is meaningless/meaningful. |
| For me, faith or spiritual belief is not important/very important. |
| For me, in adjusting to my kidney disease, faith or belief is not helpful/very helpful. |
| For me, attending religious services is not worthwhile/very worthwhile. |
| For me, in adjusting to kidney failure, attending religious services is not worthwhile/very worthwhile. |
Single items were not assessed in this study. Answers scored on a scale from 0 to 10. Modified from reference (18).
Social support was assessed using the Multidimensional Scale of Perceived Social Support (MSP) (20,21). The scale, frequently used for patients with chronic kidney disease (22–26), includes 12 questions that measure perceived support from family, friends, and significant others. Patients’ scores were reported on a seven-point Likert scale with total scores ranging from 0 to 84, indicating low to high perceived social support. We (26) previously reported that higher social support scores of hemodialysis patients with ESRD were associated with improved survival.
Statistical Analysis
Statistical analyses were performed using SAS 8.2 (SAS Institute, Cary, NC). Data from patients who were alive at the end of the study were censored according to the number of days they survived. Twelve patients lacked survival time data. Data from 18 patients who were lost to follow-up were censored at their last day of treatment at their respective dialysis units. Data from 14 patients who had received transplants during the study period were censored depending on their known vital status. Data from transplant patients who were lost to follow-up were censored at date of transplantation.
Kaplan-Meier curves were constructed on the basis of spiritual parameters and MSP scores. Religious variables were categorized on the basis of medians, means, and tertiles. In survival analyses in which levels of the religious variables were categorized, the results of splits at the mean are presented.
Spearman correlation analyses were determined on the three spiritual variables and the social support scores. Proportional hazards regression was used to calculate the association of each religious variable with mortality. Analyses were then performed to assess the relationship of social support to survival with and without the spirituality variables. Covariates in all analyses included age, diabetes status, serum albumin concentration, presence of HIV infection, and level of social support in selected analyses. P = 0.05 was taken as the level of significance.
Results
Demographics and Patient Population
The sample was composed of 102 (61.4%) men and 64 (38.6%) women. A total of 89.2% of the study patients were African American, 7.8% were white, and 3.0% identified themselves as of other ethnicity. Ninety-five patients were recruited from one unit and 75 from the other. The study patients’ demographics are outlined in Table 2. The mean age of the population was 56.2 ± 13.8 yr. A total of 45.2% had diabetes, and 11.5% had HIV infection. The mean serum albumin concentration was 3.8 ± 0.4 g/dl. Patients’ mean Kt/V was 1.4 ± 0.24. The mean duration of treatment on dialysis at the time of administration of the original questionnaire was 41.2 ± 43.5 mo. By the conclusion of the study, mean duration of treatment was 68.0 ± 45.7 mo. The mean duration of follow-up for study participants was 19.4 ± 11.1 mo. There were no differences between the participants who were recruited at either unit in mean age, serum albumin concentration, vintage, Kt/V, or the proportion of patients with diabetes or HIV infection.
Table 2.
Patient demographic and clinical characteristicsa
| Characteristic | Value |
|---|---|
| N | 166 |
| Race (%) | |
| black | 89.2 |
| white | 7.8 |
| other | 3.0 |
| Male (%) | 61.5 |
| Diabetes (%) | 45.2 |
| HIV infection (%) | 11.5 |
| Age (yr; mean ± SD) | 56.2 ± 13.8 |
| HD duration at study initiation (mo; mean ± SD) | 41.2 ± 43.5 |
| HD duration at study conclusion (mo; mean ± SD) | 68.0 ± 45.7 |
| duration of follow-up (mo; mean ± SD) | 19.4 ± 11.1 |
| serum albumin concentration (g/dl; mean ± SD) | 3.80 ± 0.40 |
| Kt/V (mean ± SD) | 1.40 ± 0.24 |
HD, hemodialysis.
The mean spirituality score was 17.5 ± 4.1, mean religious involvement score was 16.1 ± 6.0, and mean religion as coping mechanism score was 16.5 ± 4.9 (Table 3). The median spirituality score was 20, the highest score possible. The median scores for religious involvement and religion as a coping mechanism were slightly lower (19 and 18, respectively). For all three variables, the mode of the sample was 20. When the religious variables were analyzed excluding patients with HIV infection, the scores were similar. A total of 119 (67.6%) patients scored above the mean on the spirituality score. There were no differences between the participants who were recruited at either unit in mean spirituality, religious involvement, or religion as a coping mechanism score. There were no differences between the participants with spirituality or religion as coping mechanism score above and below the mean level in mean age, serum albumin concentration, vintage, Kt/V, or the proportion of patients with diabetes or HIV infection. There were no differences between the participants with religious involvement scores above and below the mean level in mean serum albumin concentration, vintage, Kt/V, or the proportion of patients with HIV infection, but there were differences between the two groups in age and the proportion of patients with diabetes. Patients with levels above the mean on any of the three spirituality scores had higher mean levels of perceived social support.
Table 3.
Patient spiritual, religious, and social support characteristics
| Characteristics | Mean | Median | Mode | Range |
|---|---|---|---|---|
| Spirituality | 17.5 ± 4.1 | 20 | 20 | 0 to 20 |
| Religious involvement | 16.1 ± 6.0 | 19 | 20 | 0 to 20 |
| Religion as coping | 16.5 ± 4.9 | 18 | 20 | 0 to 20 |
| Social support | 69.1 ± 13.2 | 72 | 84 | 22 to 84 |
The mean MSP score was 69.1 ± 13.2 for the entire sample, and the median score was 72. When patients with HIV infection were excluded, the mean MSP score was 69.6 ± 13.0, with a median of 72. There were no differences between the participants who were recruited at either unit in mean religion or social support scores.
Correlational Analyses
Social support scores correlated with spirituality scores (r = 0.33, P < 0.0001), religion as coping mechanism scores (r = 0.29, P = 0.0002), and religious involvement scores (r = 0.22, P = 0.005; Table 4). When patients with HIV infection were excluded from analyses, social support correlated with all of the religion variables (data not shown).
Table 4.
Correlation matrix of religious variables and social support (Spearman analyses)a
| Parameter | IREL | CREL | SPIR | MSP |
|---|---|---|---|---|
| IREL | r = 1.00 | r = 0.88 | r = 0.67 | r = 0.22 |
| P < 0.0001 | P < 0.0001 | P = 0.005 | ||
| CREL | r = 0.88 | r = 1.00 | r = 0.85 | r = 0.29 |
| P < 0.0001 | P < 0.0001 | P = 0.0002 | ||
| SPIR | r = 0.67 | r = 0.85 | r = 1.00 | r = 0.33 |
| P < 0.0001 | P < 0.0001 | P < 0.0001 | ||
| MSP | r = 0.22 | r = 0.29 | r = 0.33 | r = 1.00 |
| P = 0.0050 | P = 0.0002 | P < 0.0001 |
CREL, religion as coping mechanism score; IREL, religious involvement score; MSP, Multidimensional Scale of Perceived Social Support score; SPIR, spirituality score.
Survival
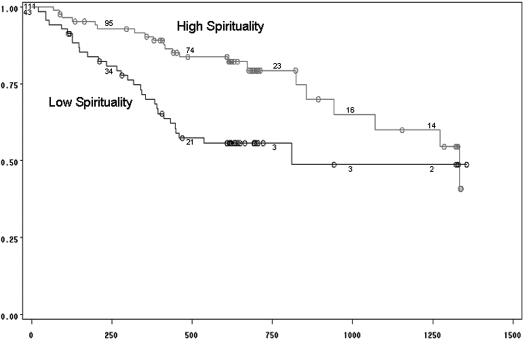
Ninety of 166 patients survived the study and observation periods. There was no difference in survival between patients in the study in either unit. When spirituality was divided into low and high groups on the basis of the mean, patients with higher spirituality scores had significantly increased survival (Figure 1). Social support was categorized by the mean. Patients with higher social support scores had improved survival (Figure 2). There was no difference between survival of patients with spirituality scores of 20 and those below the median value of 20 (data not shown).
Figure 1.
Kaplan-Meier analysis of patients with ESRD and with high versus low spirituality. Gray line represents high spirituality (above the mean), and black line represents low spirituality.
Figure 2.
Kaplan-Meier analysis of patients with ESRD and with high versus low social support. Gray line represents high social support, and black line represents low (below the mean) social support.
In the entire sample, age, hypoalbuminemia, and HIV infection were also associated with increased risk for mortality (Table 5). Gender was not associated with survival in any of the analyses that we performed (data not shown). Because of the disproportionate number of black study participants, ethnicity was not used as a covariate. Higher spirituality scores evaluated by mean split in the entire sample were associated with longer survival (hazard ratio [HR] 0.49; 95% confidence interval [CI] 0.27 to 0.88; P = 0.02; Table 5). The relationship between spirituality and survival approached statistical significance in the smaller sample when patients with HIV infection were excluded from the analysis (HR 0.54; 95% CI 0.29 to 1.01; P = 0.052; data not shown). Higher religious involvement and religion as coping mechanism scores were not associated with survival, regardless of whether patients with HIV infection were included in analyses (data not shown). There was no significant association of spirituality scores and survival when evaluated by median split.
Table 5.
Relationship of spirituality and social support to survival in patients with ESRD: Individual analyses of role of spirituality and social supporta
| Parameter | HR | 95% CI | P |
|---|---|---|---|
| Analysis 1 | |||
| albumin | 0.31 | 0.13 to 0.75 | 0.001 |
| HIV infection | 3.53 | 1.32 to 9.48 | 0.010 |
| spirituality | 0.49 | 0.27 to 0.88 | 0.020 |
| Analysis 2 | |||
| albumin | 0.32 | 0.13 to 0.79 | 0.010 |
| HIV infection | 2.71 | 1.02 to 7.23 | <0.050 |
| social support | 0.48 | 0.27 to 0.84 | 0.010 |
All analyses controlled for age and diabetes. CI, confidence interval; HR, hazard ratio
Higher social support scores were also associated with longer survival in the entire sample (HR 0.48; 95% CI 0.27 to 0.84; P = 0.01; Table 5). This relationship persisted regardless of whether patients with HIV infection were included in analyses. MSP scores also predicted survival when analyses with religious involvement and religion as coping mechanism variables were entered as covariates in place of the spirituality measure (data not shown).
When spirituality and MSP scores were included in the analyses together with age, albumin, diabetes, and HIV status as covariates, social support was still associated with increased survival (HR 0.53; 95% CI 0.30 to 0.95; P = 0.03; Table 6). This relationship persisted regardless of whether patients with HIV infection were included in analyses (data not shown). MSP scores also predicted survival when analyses with religious involvement and religion as coping mechanism scores were entered as covariates in the place of spirituality (data not shown). The relationship between spirituality and survival approached statistical significance in this analysis (HR 0.57; 95% CI 0.31 to 1.04; P = 0.066; Table 6). There was no statistically significant interaction between the spirituality and social support variables in the Cox analyses outlined in Table 6 in the entire sample (data not shown).
Table 6.
Relationship of social support and spirituality to survival in patients with ESRD: Combined analyses of role of spirituality and social supporta
| Parameter | HR | 95% CI | P |
|---|---|---|---|
| Albumin | 0.30 | 0.12 to 0.73 | 0.008 |
| HIV infection | 3.03 | 1.12 to 8.19 | 0.030 |
| Spirituality | 0.57 | 0.31 to 1.04 | 0.066 |
| Social support | 0.53 | 0.30 to 0.95 | 0.030 |
All analyses controlled for age and diabetes.
Discussion
This study showed that increased spirituality, defined as importance of faith, as measured by a particular tool, was associated with improved survival in a hemodialysis population with ESRD at a single medical center. All three religion and spirituality measure scores in this study suggested ceiling effects, with most participants endorsing the maximum score. The associations between the spirituality variable and survival, however, were found even though the spirituality measures displayed ceiling effects. This relationship was previously shown in general medical populations (1–12). Religious experience was separated in this study into three variables to determine how each was associated with survival. Whereas increased “spirituality” was associated with survival, “religion as a coping mechanism” and “religious involvement” were not associated with decreased mortality in this relatively small study, suggesting that the instruments used may have been able to discriminate between an overall sense of “spirituality” and other factors that are associated with religious experience.
We also found that increased perception of social support was associated with survival. This relationship was shown in previous studies of patients with a variety of chronic medical illnesses (25–31); however, there has been limited information regarding the relationship between social support and survival in patients with ESRD (26,31–34). In adjusted analyses, we found that dialysis patients with higher MSP scores survived longer than those with lower perceived social support levels. Previously, we showed that a 1-SD increase in perceived social support among hemodialysis patients was associated with a 20% decrease in mortality (26,31,35).
Social support may improve patient outcomes through at least five mechanisms in patients with chronic disease, including increased access to health care, increased compliance with physician prescriptions, improvements in nutritional status and overall sense of quality of life, modulation of the immune system, and a decrease in depressive affect (26,31). The correlation coefficient between the religious variables and the social support scores was associated with statistical significance but indicates a modest relationship among these variables. This may be the result of a true weak relationship among these factors, suggesting an independent association of the two factors with survival, or, alternatively, may be related to the specific tools that we used. Such issues need to be addressed in well-designed follow-up studies, with validated measures.
There is also a relationship between religion and increased perception of social support (36). People who identify themselves as spiritual or religious are often involved in religious communities and typically report higher social support scores compared with individuals who are not identified as religious.
In a multicenter study that included this patient population, we previously showed that quality-of-life assessments but not demographic or medical characteristics correlated with a spiritual beliefs scale (19). In a previous report on the baseline characteristics of this study population, we showed that all three spiritual scales correlated with increased perception of satisfaction with life and decreased indices of depressive affect and assessments of illness burden (18). Both depression and perception of illness burden have been associated with increased mortality in patients with ESRD in our studies (26,37), as well as others (38–40). Koenig (41) recently delineated the salient interconnections between spiritual values and coping, associated with lower levels of depression. These findings suggest that spiritual beliefs are indeed associated with psychosocial factors, which have been linked to enhanced survival in several different chronic illnesses (42).
Although spiritual factors may have an independent association with survival in the chronically ill and in patients with ESRD, the mechanisms underlying any such links remain unclear. Recently, we summarized studies that linked psychosocial factors to stressors (31,42), which may activate immune and inflammatory responses that are associated with enhancing the susceptibility to infection or the development of atherosclerosis (42,43). Unfortunately, we do not have information regarding these mediators or the causes of death in the patients in this relatively small pilot study.
In analyses in which spirituality and social support were assessed simultaneously, the link between spirituality and survival in this population was attenuated. This suggests that higher social support may mediate the effect of increased spirituality on survival. One reason that spirituality might not have significantly predicted survival above and beyond social support, in addition to the limited sample size, is that the ceiling effects on the spirituality measure may have limited the ability to detect effects of spirituality. With a modal score of 20 and a mean score of 17.5, it seems that the scores fell in a fairly restricted range in this relatively religious population. With a more sensitive measure allowing a much wider range of scores in the high spirituality category, it is possible that we might have been able to detect significant variance above and beyond that contributed by social support. Such considerations may have determined the lack of significance in our analyses of spirituality using median splits. A median split in this case reflects a comparison between the extremely spiritually oriented and those who scored just slightly lower, perhaps diminishing the ability to demonstrate differences; however, it is also possible that other, unaccounted variables contribute to the relationship of spirituality with survival and between religious variables and social support. In addition, it would be desirable to study a population with more diverse spiritual and religious characteristics, including atheists and nonobservant participants, including a wide range of denominational affiliations.
This study has several limitations. The spirituality scales that we used, devised in collaboration with the Robert Wood Johnson Foundation Promoting Excellence in End-of-Life Care End-Stage Renal Disease Work Group (44), have not been fully validated or subjected to test–retest reliability determinations; therefore, confirmatory studies stemming from our exploratory findings will need to be performed using these measures after validation or other validated parameters. In addition, because the determination of “spirituality” and “religiosity” in clinical studies has not been uniform or endorsed by consensus, it should be noted that the measures used in this study cannot reliably distinguish between these characteristics. The skewed responses to the questionnaires suggest that broader populations will have to be studied and/or that the measures may need to be rescaled. The questionnaires were administered by research assistants. As noted previously, this presents an issue of potential experimental demand (18), but such data collection methods are necessary in populations that have high levels of illiteracy and have the advantage of maintaining uniform administration. As outlined previously, surveys that sample a dialysis unit population over a period of time do not take into account stage of the life cycle of the patient with ESRD (42,45), which may contribute to the heterogeneity of findings. Further studies should be performed in defined populations, such as incident patients, or using longitudinal follow-up to address this limitation. The relatively small sample size of this study and the number of events preclude the use of a large number of standard covariates in Cox regression analyses (46). We do not have data on hospitalizations, cause of death, or religious denomination in this pilot study, which limits the conclusions that can be drawn from our findings. The patient population was primarily composed of urban black patients with ESRD, which may further limit study generalizability. Tanyi et al. (17) specifically showed that black individuals have high spirituality scores, at baseline, compared with a white cohort. In addition, our sample was composed primarily of prevalent patients, raising the possibility of survival bias.
Interactions between patients’ underlying medical illness and their environment influence psychological adjustment and play a unique role in the pathogenesis and progression of disease. This complexity makes it difficult to establish causality in a cohort study. Another inherent limitation of an observational study is the potential for recall and selection biases. The more compliant and “healthier” patients may have been more likely to participate in surveys. It is also possible that experimental demand (18) and social desirability may have influenced the patients’ answers to interviewers’ questions with respect to quality of life and spirituality.
Conclusions
An association between spirituality and survival may be partially explained by increased perception of social support in hemodialysis patients who participate in religious activities. Larger, multicenter, prospective cohort studies, including longitudinal observations and assessments of cardiovascular risk factors and inflammatory mediators, as well as broader consideration of other psychosocial factors such as socioeconomic factors and perception of discrimination (42) are needed for further evaluation of any fine-grained relationships between spirituality and survival in patients with ESRD, with broader participation of different ethnic groups from different parts of the country and the world.
Disclosures
None.
Acknowledgments
S.D.C. was supported by a research fellowship award from the National Kidney Foundation. J.S. and B.C. were supported by Gill Fellowships at the George Washington University School of Medicine.
Published online ahead of print. Publication date available at www.cjasn.org.
References
- 1.Levin JS: How religion influences morbidity and health: Reflections on natural history, salutogenesis, and host resistance. Soc Sci Med 43: 849–864, 1996 [DOI] [PubMed] [Google Scholar]
- 2.Koenig HG: Is Religion Good for your Health? New York, Haworth Press, 1997
- 3.Ellison CG: Religious involvement and subjective well-being. J Health Soc Behav 32: 80–99, 1991 [PubMed] [Google Scholar]
- 4.Martin WT: Religiosity and United States suicide rates, 1972–1978. J Clin Psychol 40: 1166–1169, 1984 [DOI] [PubMed] [Google Scholar]
- 5.Cornstock GW, Partridge KB: Church attendance and health. J Chronic Dis 24: 665–672, 1972 [DOI] [PubMed] [Google Scholar]
- 6.Zuckerman DM, Kasl SV, Ostfeld AM: Psychosocial predictors of mortality among the elderly poor: The role of religion, well-being, and social contacts. Am J Epidemiol 119: 410–423, 1984 [DOI] [PubMed] [Google Scholar]
- 7.Oxman TE, Freeman DH, Manheimer ED: Lack of social participation or religious strength and comfort as risk factors for death after cardiac surgery in the elderly. Psychosom Med 57: 5–15, 1995 [DOI] [PubMed] [Google Scholar]
- 8.Strawbridge WJ, Cohen RD, Shema SJ, Kaplan GA: Frequent attendance at religious services and mortality over 28 years. Am J Public Health 87: 957–961, 1997 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Koenig HG, George LK, Cohen HJ, Hays JC, Larson DB, Blazer DG: The relationship between religious activities and cigarette smoking in older adults. J Gerontol A Biol Sci Med Sci 53: M426–M434, 1998 [DOI] [PubMed] [Google Scholar]
- 10.Koenig HG, Cohen HJ, George LK, Hays JC, Larson DB, Blazer DG: Attendance at religious services, interleukin-6, and other biological indicators of immune function in older adults. Int J Psychiatry Med 27: 233–250, 1997 [DOI] [PubMed] [Google Scholar]
- 11.Koenig HG, George LK, Cohen HJ, Larson DB, Cohen HJ, Blazer DG: The relationship between religious activities and blood pressure in older adults. Int J Psychiatry Med 28: 189–213, 1998 [DOI] [PubMed] [Google Scholar]
- 12.Miller WR, Thoresen CE: Spirituality, religion and health: An emerging research field. Am Psychol 58: 24–35, 2003 [DOI] [PubMed] [Google Scholar]
- 13.Matthews DA, McCullough ME, Larson DB, Koenig HG, Swyers JP, Milano MG: Religious commitment and health status: A review of the research and implications for family medicine. Arch Fam Med 7: 118–124, 1998 [DOI] [PubMed] [Google Scholar]
- 14.Koenig HG, Hays JC, Larson DB, George LK, Cohen HJ, McCullough ME, Meador KG, Blazer DG: Does religious attendance prolong survival? A six-year follow-up study of 3968 older adults. J Gerontol A Biol Sci Med Sci 54: M370–M376, 1999 [DOI] [PubMed] [Google Scholar]
- 15.Report III-Contemporary Issues in Medicine: Communication in Medicine, Medical School Objectives Project. Association of American Medical Colleges, 1999. Available at: https://services.aamc.org/Publications/index.cfm?fuseaction=Product.displayForm&prd_id=200&prv_id=241. Accessed January 25, 2008 [PubMed]
- 16.Matthews WJ, Conti J, Sireci SG: The effects of intercessory prayer, positive visualization, and expectancy on the well-being of kidney dialysis patients. Altern Ther Health Med 7: 42–52, 2001 [PubMed] [Google Scholar]
- 17.Tanyi RA, Werner JS: Spirituality in African American and Caucasian women with end-stage renal disease on hemodialysis treatment. Health Care Women Int 28: 141–154, 2007 [DOI] [PubMed] [Google Scholar]
- 18.Patel SS, Shah VS, Peterson RA, Kimmel PL: Psychosocial variables, quality of life, and religious beliefs in ESRD patients treated with hemodialysis. Am J Kidney Dis 40: 1013–1022, 2002 [DOI] [PubMed] [Google Scholar]
- 19.Kimmel PL, Emont SL, Newmann JM, Danko H, Moss AH: ESRD patient quality of life: Symptoms, spiritual beliefs, psychosocial factors, and ethnicity. Am J Kidney Dis 42: 713–721, 2003 [DOI] [PubMed] [Google Scholar]
- 20.Zimet GD, Dahlem NW, Zimet SG: The multidimensional scale of perceived social support. J Pers Assess 52: 30–41, 1988 [Google Scholar]
- 21.Dahlem NW, Zimet G, Walker R: The multidimensional scale of perceived social support: A confirmation study. J Clin Psychol 47: 756–761, 1991 [DOI] [PubMed] [Google Scholar]
- 22.Shidler NR, Peterson RA, Kimmel PL: Quality of life and psychosocial relationships in patients with chronic renal insufficiency. Am J Kidney Dis 32: 557–566, 1998 [DOI] [PubMed] [Google Scholar]
- 23.Weisbord SD, Fried F, Arnold RM, Fine MJ, Levenson DJ, Peterson RA, Switzer GE: Prevalence, severity and importance of physical symptoms in chronic hemodialysis patients. J Am Soc Nephrol 16: 2487–2494, 2005 [DOI] [PubMed] [Google Scholar]
- 24.Sacks CR, Peterson RA, Kimmel PL: Perception of illness and depression in chronic renal disease. Am J Kidney Dis 15: 31–39, 1990 [DOI] [PubMed] [Google Scholar]
- 25.Kimmel PL: Psychosocial factors in dialysis patients. Kidney Int 59: 1599–1613, 2001 [DOI] [PubMed] [Google Scholar]
- 26.Kimmel PL, Peterson RA, Weihs KL, Simmens SJ, Alleyne S, Cruz I, Veis JH: Psychosocial factors, behavioral compliance and survival in urban hemodialysis patients. Kidney Int 54: 245–254, 1998 [DOI] [PubMed] [Google Scholar]
- 27.Kroenke CH, Kubzansky LD, Schernhammer ES, Holmes MD, Kawachi I: Social networks, social support, and survival after breast cancer diagnosis. J Clin Oncol 24: 1105–1111, 2006 [DOI] [PubMed] [Google Scholar]
- 28.Waxler-Morrison N, Hislop TG, Mears B, Kan L: Effects of social relationships on survival for women with breast cancer: A prospective study. Soc Sci Med 33: 177–183, 1991 [DOI] [PubMed] [Google Scholar]
- 29.Brummett BH, Mark DB, Siegler IC, Williams RB, Babyak MA, Clapp-Channing NE, Barefoot JC: Perceived social support as a predictor of mortality in coronary patients: Effects of smoking, sedentary behavior, and depressive symptoms. Psychosom Med 67: 40–45, 2005 [DOI] [PubMed] [Google Scholar]
- 30.Luttik ML, Jaarsma T, Moser D, Sanderman R, van Veldhuisen DJ: The importance and impact of social support on outcomes in patients with heart failure: An overview of the literature. J Cardiovasc Nurs 20: 162–169, 2005 [DOI] [PubMed] [Google Scholar]
- 31.Cohen SD, Sharma T, Acquaviva K, Peterson RA, Patel SS, Kimmel PL: Social support and chronic kidney disease: An update. Adv Chronic Kidney Dis 14: 335–344, 2007 [DOI] [PubMed] [Google Scholar]
- 32.Thong MS, Kaptein AA, Krediet T, Boeschoten EW, Dekker FW: Social support predicts survival in dialysis patients. Nephrol Dial Transplant 22: 845–850, 2007 [DOI] [PubMed] [Google Scholar]
- 33.McClellan WM, Stanwyck DJ, Anson CA: Social support and subsequent mortality among patients with end-stage renal disease. J Am Soc Nephrol 4: 1028–1034, 1993 [DOI] [PubMed] [Google Scholar]
- 34.Friend R, Singletary Y, Mendell NR, Nurse H: Group participation and survival among patients with end-stage renal disease. Am J Public Health 76: 670–672, 1986 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Kimmel PL, Patel SS: Quality of life in patients with chronic kidney disease: Focus on end-stage renal disease treated with hemodialysis. Semin Nephrol 26: 68–79, 2006 [DOI] [PubMed] [Google Scholar]
- 36.George LK, Larson DB, Koenig HG, McCullough ME: Spirituality and health: What we know and what we need to know. Soc Clin Psychol 19: 102–116, 2000 [Google Scholar]
- 37.Kimmel PL, Peterson RA, Weihs KL, Simmens SJ, Alleyne S, Cruz I, Veis JH: Multiple measurements of depression predict mortality in a longitudinal study of chronic hemodialysis patients. Kidney Int 57: 2093–2098, 2000 [DOI] [PubMed] [Google Scholar]
- 38.Boulware LE, Liu Y, Fink NE, Coresh J, Ford DE, Klag MJ, Powe NR: The temporal relation between depression symptoms, cardiovascular disease events and mortality in ESRD: Contribution of reverse causality. Clin J Am Soc Nephrol 1: 496–504, 2006 [DOI] [PubMed] [Google Scholar]
- 39.Lopes AA, Albert JM, Young EW, Satayathum S, Pisoni RL, Andreucci VE, Mapes DL, Mason NA, Fukuhara S, Wikström B, Saito A, Port FK: Screening for depression in hemodialysis patients: Associations with diagnosis, treatment, and outcomes in the DOPPS [erratum appears in Kidney Int 66: 2486, 2004]. Kidney Int 66: 2047–2053, 2004 [DOI] [PubMed] [Google Scholar]
- 40.DeOreo PB: Hemodialysis patient-assessed functional health status predicts continued survival, hospitalization, and dialysis-attendance compliance. Am J Kidney Dis 30: 204–212, 1997 [DOI] [PubMed] [Google Scholar]
- 41.Koenig HG: Spirituality and depression: A look at the evidence. South Med J 100: 737–739, 2007 [DOI] [PubMed] [Google Scholar]
- 42.Cukor D, Cohen SD, Peterson RA, Kimmel PL: Psychosocial aspects of chronic disease: ESRD as a paradigmatic illness. J Am Soc Nephrol 18: 3042–3055, 2007 [DOI] [PubMed] [Google Scholar]
- 43.McEwen BS: Protective and damaging effects of stress mediators. N Engl J Med 338: 171–179, 1998 [DOI] [PubMed] [Google Scholar]
- 44.End-Stage Renal Disease Workgroup: Full Report: Recommendations to the Field, Princeton, NJ, Robert Wood Johnson Foundation, 2000
- 45.Kimmel PL: Towards a developmental view of end-stage renal disease. Am J Kidney Dis 15: 191–193, 1990 [DOI] [PubMed] [Google Scholar]
- 46.Vittinghoff E, McCulloch CE: Relaxing the rule of ten events per variable in logistic and Cox regression. Am J Epidemiol 165: 710–718, 2007 [DOI] [PubMed] [Google Scholar]