Abstract
In the era of life-prolonging antiretroviral therapy, chronic fatigue is one of the most prevalent and disabling symptoms of people living with HIV/AIDS, yet its measurement remains challenging. No instruments have been developed specifically to describe HIV-related fatigue. We assessed the reliability and construct validity of the HIV-Related Fatigue Scale (HRFS), a 56-item self-report instrument developed through formative qualitative research and designed to measure the intensity and consequences of fatigue as well as the circumstances surrounding fatigue in people living with HIV. The HRFS has three main scales, which measure fatigue intensity, the responsiveness of fatigue to circumstances and fatigue-related impairment of functioning. The functioning scale can be further divided into subscales measuring impairment of activities of daily living, impairment of mental functioning and impairment of social functioning. Each scale demonstrated high internal consistency (Cronbach’s alpha=0.93, 0.91 and 0.97 for the intensity, responsiveness and functioning scales, respectively). The HRFS scales also demonstrated satisfactory convergent validity when compared to other fatigue measures. HIV-Related Fatigue Scales were moderately correlated with quality of nighttime sleep (rho = 0.46, 0.47 and 0.35) but showed only weak correlations with daytime sleepiness (rho = 0.20, 0.33 and 0.18). The scales were also moderately correlated with general mental and physical health as measured by the SF-36 Health Survey (rho ranged from 0.30 to 0.68 across the 8 SF-36 subscales with most >0.40). The HRFS is a promising tool to help facilitate research on the prevalence, etiology and consequences of fatigue in people living with HIV.
Keywords: fatigue, HIV, measurement, psychometric properties, validity
Introduction
In the era of life-prolonging antiretroviral therapy, chronic fatigue is one of the most prevalent and disabling symptoms of people living with HIV/AIDS (Duran et al., 2001; Henderson, Safa, Easterbrook, & Hotopf, 2005; Jenkin, Koch, & Kralik, 2006; Voss, 2005). Nevertheless, the precise definition, prevalence and etiology of HIV-related fatigue remain poorly described.
Multiple instruments have been developed to measure fatigue, although until recently there was no instrument that adequately measured fatigue in HIV-positive individuals (Barroso, 1999). Aaronson et al. (1999) highlighted the difficulty in measuring a construct as subjective as fatigue and noted that different measures tap into different aspects of fatigue. Some instruments simply measure the presence or absence of fatigue; others measure only one aspect of fatigue (e.g. physical fatigue or decreased muscle strength) (Hoover et al., 1993; Palenicek et al., 1993; Penkower et al., 1995; Perkins et al., 1995; Piedrola et al., 1996; Singh, Squier, Sivek, Wagener, & Yu, 1997; Vlahovet al., 1994; Whalen, Antani, Carey, & Landefeld, 1994). Some researchers have borrowed tools developed to measure concepts other than fatigue (e.g. performance or vitality) (O’Dell, Meighen, & Riggs, 1996; Reillo, 1993). Many of the instruments used to measure fatigue are very brief (four questions or less) and, although most of them have acceptable psychometric properties, they do not capture the full experience of HIV-related fatigue as encountered in our clinical experience (Barroso, 1999).
To fill this measurement need, our principal investigator (JB) developed a 56-item tool designed specifically to measure fatigue in people living with HIV (Barroso & Lynn, 2002). The HIV-Related Fatigue Scale (HRFS) was developed through formative qualitative research and designed to measure the intensity and consequences of fatigue as well as the circumstances surrounding fatigue in people living with HIV. In this paper we examined the reliability of the HRFS as well as its construct validity compared to other measures of fatigue and to measures of sleep quality and general health.
Methods
Instrument
The rationale for, and development of, the HRFS have been described in detail previously (Barroso & Lynn, 2002). In brief, through qualitative research with people living with HIV, a clinical investigator with 16 years of experience in HIV treatment (JB) identified conceptual distinctions between three primary dimensions of HIV-related fatigue: the intensity of the fatigue, the circumstances surrounding the fatigue and the consequences of fatigue (Barroso, 2001). Consequences of fatigue could be further categorized into impairment of performance of activities of daily living, impairment of social activities and impairment of mental functioning. A comprehensive literature review of the multiple instruments used to measure fatigue identified no instruments designed to adequately capture all three of the dimensions identified in the qualitative research and further identified no instruments that had been specifically developed for or validated in people living with HIV (Barroso, 1999; Barroso & Lynn, 2002). We therefore developed a new tool to measure HIV-related fatigue, informed by the existing literature and the prior qualitative research.
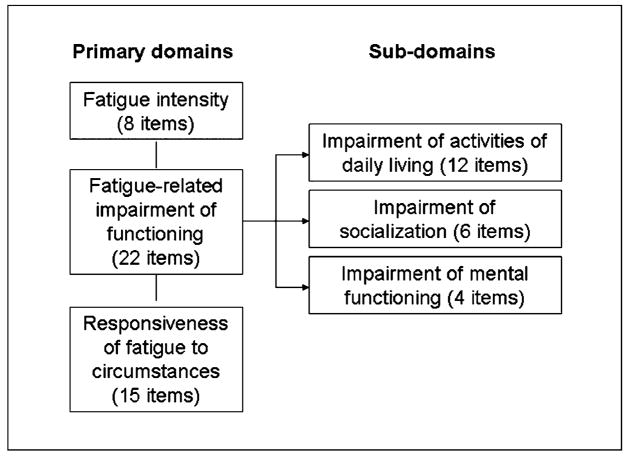
We developed the 56-item HRFS by adopting items from five existing fatigue instruments created for non-HIV populations (with authors’ permission) that matched the domains identified through the initial qualitative work and by creating additional items to address findings from the formative qualitative research that were not captured by any tool. Items were adopted from the Multidimensional Assessment of Fatigue (MAF: entirety – 16 items) (Belza, Henke, Yelin, Epstein, & Gilliss, 1993); the Fatigue Assessment Instrument (FAI: entirety – 29 items) (Schwartz, Jandorf, & Krupp, 1993); the General Fatigue Scale (2 of 7 items) (Meek & Nail, 1997); the Fatigue Impact Scale (4 of 40 items) (Fisk, Pontefract, Ritvo, Archibald, & Murray, 1994); and the Sleep and Infection Questionnaire (3 of 17 items) (Darko, McCutchan, Kripke, Gillin, & Golshan, 1992). Items were then divided into conceptually distinct groups corresponding to the domains identified in the formative qualitative research: fatigue intensity (8 items), fatigue-related impairment of functioning (22 items) and the responsiveness of the fatigue to circumstances (15 items). Remaining items are used individually to describe the respondent’s fatigue experience. The fatigue-related impairment items were further divided into three subscales: impairment of activities of daily living (12 items), impairment of socialization (6 items) and impairment of mental functioning (4 items) (Figure 1). All scales were coded to range from 1–10 with a higher value indicating more fatigue, impairment or responsiveness. Initial psychometric testing of the HRFS in 54 people living with HIV has been reported previously (Barroso & Lynn, 2002) and indicated strong content validity of the instrument and high internal consistency of each scale.
Figure 1.
The HIV-Related Fatigue Scale (HRFS): conceptual framework.
Sample
The present study reports estimates of reliability and convergent construct validity of the HRFS in 128 people living with HIV recruited for a longitudinal cohort study of the causes and consequences of fatigue in people living with HIV. Participants were recruited via flyers advertising the study at HIV/AIDS treatment centers and service organizations in a southern US state. Interested individuals were invited to participate if they met the following inclusion criteria: (1) HIV-positive, (2) ≥21 years old, (3) able to read and speak English competently and (4) mentally competent to provide reliable data. Both fatigued and non-fatigued individuals were eligible to enroll. Individuals were excluded if they had a co-morbid condition marked by fatigue such as renal disease, cancer or multiple sclerosis. Pregnant women and women less than 12 months postpartum were also excluded. In all, 128 individuals enrolled in the study and completed the baseline assessment. All study procedures were approved by the Duke University Institutional Review Board and all study participants provided written informed consent.
Data collection
Participants completed the HRFS during the inperson baseline assessment. Other instruments from the baseline assessment used in this analysis include the Pittsburgh Sleep Quality Index (PSQI) (Buysse, Reynolds, Monk, Berman, & Kupfer, 1989; Carpenter & Andrykowski, 1998), the Epworth Sleepiness Scale (ESS) (Johns, 2000, 2002) and the SF-36 Health Survey (Ware & Sherbourne, 1992; Ware et al., 1995) The PSQI yields a global scale of the respondent’s nighttime sleep quality, including overall quality, duration, efficacy, disturbed sleep, sleep-related dys-function and need for sleep medications; a higher score indicates poorer quality sleep (range 0–21). The ESS measures daytime sleepiness with questions addressing the respondent’s likelihood of dozing off or falling asleep during eight daytime activities such as reading, watching TV or riding in a car; a higher score indicates more daytime sleepiness (range: 0–24). The SF-36 measures eight domains of general health, including vitality, bodily pain and mental health; a higher score indicates better health (range: 0–100). The interviewer checked all instruments for completeness and clarified any skipped or missing items with the participant.
Statistical analysis
We measured reliability (the extent to which the items composing each scale are measuring a common latent construct) for each scale and subscale of the HRFS using Cronbach’s alpha. Generally, a Cronbach’s alpha of >0.70 is considered acceptable for a psychometric scale (Nunnally, 1978). We also calculated, for each item, the item-rest correlation (the correlation between that item and the scale formed from the remaining items) and Cronbach’s alpha of the scale formed from all items but the item in question. We computed correlation coefficients among the various HRFS scales.
We assessed convergent construct validity (the extent to which a scale correlates with other measures targeting the same latent construct) by correlating the HRFS with fatigue measures based on the MAF and the FAI (two shorter instruments embedded within the HRFS). We further examined correlation coefficients between the HRFS scales and the PSQI, the ESS and the SF-36 scales. We hypothesized that the HRFS scales would be moderately but not strongly correlated with nighttime sleep quality (PSQI) and that the HRFS would be only weakly correlated with daytime sleepiness (ESS). We further hypothesized that the HRFS would be moderately correlated with both mental and physical health as measured by the SF-36, and particularly with the SF-36 vitality scale. We refer to correlation coefficients >0.70 as strong, 0.40–0.70 as moderate and <0.40 as weak (Denton, Durning, & Hemmer, 2004) All reported p-values are from two-sided hypothesis tests.
Results
Sample characteristics
The sample has been described in detail elsewhere (Harmon, Barroso, Pence, Leserman, & Salahuddin, in press). The majority of the 128 participants were African American (66%) with the remainder primarily Caucasian (30%) (data not shown). Sixty-six percent of the subjects were male and most subjects were in their late thirties or forties (median age 44 years; interquartile range [IQR] 38–48). A majority of subjects were unemployed at baseline (n = 86; 67%). The sample predominantly comprised people who had lived with HIV infection for a long time, with a median time since diagnosis of 10 years (IQR 6–15 years). Most (82%) were on antiretroviral therapy at baseline. Many (65%) reported living with at least one other chronic illness (e.g. hypertension, depression, arthritis).
Reliability of HRFS
All scales and subscales of the HRFS demonstrated acceptable internal consistency, with values for Cronbach’s alpha of 0.93 (fatigue intensity), 0.97 (fatigue-related impairment of functioning) and 0.91 (responsiveness of fatigue to circumstances) for the primary scales, and 0.95 (impairment of ADL), 0.93 (impairment of socialization) and 0.92 (impairment of mental functioning) for the subscales of the fatiguerelated impairment scale (Table 1). All items demonstrated reasonable evidence of belonging to their assigned scale as supported by item-rest correlations and reliability coefficients calculated by eliminating individual items from each scale. The three primary scales of the HRFS were strongly correlated (range 0.71–0.86) (Table 2). The three subscales of fatiguerelated impairment of functioning were also strongly correlated (range 0.80–0.89).
Table 1.
Reliability of scales and subscales of the HIV-Related Fatigue Scale (HRFS) in 128 HIV-positive patients.
| Scale
|
Subscale
|
|||||
|---|---|---|---|---|---|---|
| Cronbach’s alpha | Iterm-rest correlation* | Cronbach’s alpha without this item** | Cronbach’s alpha | Iterm-rest correlation* | Cronbach’s alpha without this item** | |
| Fatigue intensity | 0.93 | |||||
| Level of fatigue today | 0.61 | 0.93 | ||||
| Level of fatigue most days | 0.79 | 0.92 | ||||
| To what degree has experienced fatigue | 0.79 | 0.92 | ||||
| Severity of fatigue | 0.81 | 0.92 | ||||
| Fatigue caused distress | 0.81 | 0.92 | ||||
| How often fatigued past week | 0.76 | 0.92 | ||||
| Easily fatigued | 0.78 | 0.92 | ||||
| Fatigue causes frequent problems | 0.74 | 0.92 | ||||
| Responsiveness of fatigue to circumstances | ||||||
| Fatigue is brought on by … | 0.91 | |||||
| HIV medications | 0.46 | 0.91 | ||||
| exercise | 0.62 | 0.91 | ||||
| heat | 0.69 | 0.90 | ||||
| long periods of inactivity | 0.65 | 0.91 | ||||
| stress | 0.69 | 0.90 | ||||
| depression | 0.64 | 0.91 | ||||
| work | 0.58 | 0.91 | ||||
| performance of activities of daily living | 0.64 | 0.91 | ||||
| prolonged fatigue after exercise | 0.64 | 0.91 | ||||
| Fatigue is alleviated by … | ||||||
| rest | 0.65 | 0.91 | ||||
| sleeping | 0.59 | 0.91 | ||||
| cool temperatures | 0.58 | 0.91 | ||||
| positive experiences | 0.63 | 0.91 | ||||
| Fatigue is … | ||||||
| worse in the afternoon | 0.64 | 0.91 | ||||
| worse in the morning | 0.45 | 0.91 | ||||
| Fatigue-related impairment of functioning | 0.97 | |||||
| Subscale: Impairment of activities of daily living | 0.95 | |||||
| Fatigue interferes with … | ||||||
| household chores | 0.82 | 0.97 | 0.82 | 0.95 | ||
| cooking | 0.76 | 0.97 | 0.73 | 0.95 | ||
| bathing/washing | 0.66 | 0.97 | 0.66 | 0.95 | ||
| dressing | 0.71 | 0.97 | 0.72 | 0.95 | ||
| working | 0.75 | 0.97 | 0.72 | 0.95 | ||
| shopping/errands | 0.88 | 0.97 | 0.86 | 0.95 | ||
| walking | 0.82 | 0.97 | 0.83 | 0.95 | ||
| exercise other than walking | 0.80 | 0.97 | 0.80 | 0.95 | ||
| planning activities | 0.80 | 0.97 | 0.75 | 0.95 | ||
| physical functioning | 0.78 | 0.97 | 0.79 | 0.95 | ||
| sustained physical functioning | 0.75 | 0.97 | 0.77 | 0.95 | ||
| carrying out duties/responsibilities | 0.78 | 0.97 | 0.80 | 0.95 | ||
| Subscale: Impairment of socialization | 0.93 | |||||
| Fatigue interferes with… | ||||||
| visiting/socializing | 0.79 | 0.97 | 0.85 | 0.90 | ||
| sexual activity | 0.73 | 0.97 | 0.77 | 0.91 | ||
| leisure/recreation | 0.83 | 0.97 | 0.85 | 0.90 | ||
| controlling temper | 0.72 | 0.97 | 0.66 | 0.93 | ||
| interactions with others outside home | 0.82 | 0.97 | 0.83 | 0.91 | ||
| work, family, social life | 0.84 | 0.97 | 0.76 | 0.92 | ||
| Subscale: Impairment of mental functioning | 0.92 | |||||
| Fatigue interferes with… | ||||||
| thinking clearly | 0.80 | 0.97 | 0.84 | 0.88 | ||
| thinking quickly | 0.85 | 0.97 | 0.92 | 0.86 | ||
| learning new things | 0.79 | 0.97 | 0.80 | 0.90 | ||
| concentration | 0.73 | 0.97 | 0.69 | 0.93 | ||
Correlation between the item and the scale formed from the remaining items.
Cronbach’s alpha of the scale formed from all items except this item.
Table 2.
Correlations between scales and subscales of the HIV-Related Fatigue Scale.
| Impairment subscales
|
||||||
|---|---|---|---|---|---|---|
| Fatigue intensity | Responsiveness to circumstances | Impairment of functioning (overall) | Impairment of ADL | Impairment of Socialization | Impairment of mental functioning | |
| Fatigue intensity | 1 | |||||
| Responsiveness to circumstances | 0.72 | 1 | ||||
| Impairment of functioning (overall) | 0.86 | 0.71 | 1 | |||
| Impairment of ADL | 0.86 | 0.70 | 0.98 | 1 | ||
| Impairment of socialization | 0.80 | 0.63 | 0.94 | 0.89 | 1 | |
| Impairment of mental functioning | 0.76 | 0.69 | 0.90 | 0.84 | 0.80 | 1 |
ADL: Activities of daily living.
Convergent construct validity of HRFS
All HRFS scales were moderately to strongly correlated with the Multidimensional Assessment of Fatigue (MAF) (ρ ranged from 0.65–0.95) (Table 3). The HRFS intensity scale was strongly correlated with the Severity scale of the Fatigue Assessment Instrument (FAI) (ρ = 0.71) but not associated with the Situation-specific, Psychological Consequences or Responds to Rest/Sleep scales. The HRFS fatiguerelated impairment of functioning scale was moderately to strongly correlated with the FAI Severity (ρ = 0.81) and Psychological Consequences (ρ = 0.59) scales but showed little correlation with the other two FAI scales (ρ <0.30). The HRFS responsiveness of fatigue to circumstances scale was strongly correlated with the FAI Situation-Specific scale (ρ = 0.79) and moderately correlated with the other three FAI scales (ρ ranged from 0.48–0.60). Note that the MAF and FAI scales are embedded in the HRFS and were constructed from HRFS responses, which may partially explain the observed correlations. Specifically, the 8-item HRFS intensity scale contains 4 MAF and 2 FAI items, the 22-item HRFS fatigue-related impairment of functioning scale contains 11 MAF and 3 FAI items and the 15-item HRFS responsiveness of fatigue to circumstances scale contains 0 MAF and 9 FAI items.
Table 3.
Convergent construct validity of HRFS: correlation with other fatigue instruments.
| HRFS Scale
|
|||
|---|---|---|---|
| Fatigue intensity | Impairment of functioning | Responsiveness to circumstances | |
| MAF | 0.95 | 0.79 | 0.65 |
| FAI: Severity | 0.71 | 0.81 | 0.60 |
| FAI: Situation-specific | 0.23 | 0.29 | 0.79 |
| FAI: Psychological consequences | 0.35 | 0.59 | 0.48 |
| FAI: Responds to rest/sleep | −0.05 | −0.02 | 0.50 |
MAF: Multidimensional Assessment of Fatigue. FAI: Fatigue Assessment Instrument.
Poorer quality of nighttime sleep, as measured with the PSQI, was weakly to moderately associated with greater fatigue intensity, fatigue-related impairment and responsiveness of fatigue to circumstances (ρ = 0.46, 0.47 and 0.35, respectively) (Table 4). In examining individual components of the PSQI, most HRFS scales were moderately correlated with overall self-reported quality of sleep and sleep-related dys-function, i.e. having trouble staying awake during daytime activities (ρ ranged from 0.38–0.46) but showed weak correlation with average hours of sleep per night, sleep efficacy (i.e. percent of time in bed spent sleeping) and use of sleep medications (ρ ranged from 0.13–0.25) (data not shown). Greater daytime sleepiness, as measured by the ESS, demonstrated a weak correlation with all fatigue scales (ρ = 0.20, 0.33 and 0.18 for the intensity, impairment of functioning and responsiveness to circumstances scales, respectively).
Table 4.
Convergent construct validity of HRFS: correlation with measures of sleep and general health.
| HRFS Scale
|
|||
|---|---|---|---|
| Fatigue intensity | Impairment of functioning | Responsiveness to circumstances | |
| Pittsburgh Sleep Quality Index | 0.46 | 0.47 | 0.35 |
| Epworth Sleepiness Scale | 0.20 | 0.33 | 0.18 |
| SF-36 scales | |||
| Physical functioning | −0.55 | −0.63 | −0.48 |
| Role physical | −0.58 | −0.68 | −0.54 |
| Bodily pain | −0.45 | −0.55 | −0.37 |
| General health | −0.37 | −0.34 | −0.30 |
| Vitality | −0.58 | −0.60 | −0.50 |
| Social functioning | −0.60 | −0.68 | −0.46 |
| Role emotional | −0.55 | −0.63 | −0.43 |
| Mental health | −0.51 | −0.57 | −0.36 |
| Physical composite score | −0.51 | −0.59 | −0.47 |
| Mental composite score | −0.51 | −0.56 | −0.37 |
The HRFS scales were weakly to moderately correlated with all SF-36 health subscales and composite scores, with correlation coefficients ranging from 0.37–0.60 (fatigue intensity scale), 0.34–0.68 (fatigue-related impairment of functioning) and 0.36–0.54 (responsiveness of fatigue to circumstances). Of the eight SF-36 scales, the Social Functioning scale showed the highest correlation with the HRFS fatigue intensity and impairment of functioning scales, whereas the Role Physical scale showed the highest correlation with the HRFS responsiveness to circumstances scale. Of note, the SF-36 Vitality scale showed a moderate correlation with each of the three HRFS scales (ρ = 0.58, 0.60 and 0.50 for the intensity, impairment of functioning and responsiveness to circumstances scales, respectively), although several other SF-36 scales showed correlations of similar magnitude.
Discussion
In these analyses, the HRFS demonstrated satisfactory reliability as well as convergent and construct validity in describing the intensity, circumstances and consequences of fatigue in individuals living with HIV/AIDS. The three primary scales of the HRFS – fatigue intensity, fatigue-related impairment of functioning and responsiveness of fatigue to circumstances – each had acceptable reliability coefficients and each question showed evidence of belonging to its assigned scale. These results correspond well to an initial report from a smaller sample in which the reliability of the three HRFS scales were 0.84 (intensity), 0.95 (impairment of functioning) and 0.73 (responsiveness to circumstances) (Barroso & Lynn, 2002).
In assessing the instrument’s convergent construct validity, HRFS scales were strongly correlated with other fatigue instruments measuring similar constructs. It should be noted that we only compared the HRFS with fatigue instruments whose questions had been incorporated into the HRFS; further studies in which participants sequentially completed the HRFS and alternative fatigue instruments would provide additional valuable insights. Further, HRFS scales were moderately correlated with most SF-36 physical and mental health scores and with quality of nighttime sleep. Of note, the HRFS scales demonstrated a weak correlation with a measure of daytime sleepiness, underscoring the conceptual distinction between ‘sleepiness’ and chronic fatigue.
We chose to select items for inclusion in the HRFS and to group the items into scales based on the conceptual framework and dimensions identified through the formative qualitative research rather than employing a data-driven procedure such as exploratory factor analysis. The three HRFS scales did demonstrate strong correlations, ranging from 0.71–0.86, suggesting that the dimensions in the conceptual framework do overlap to a certain extent. Nevertheless, these separate subscales may be of use in describing the characteristics of HIV-related fatigue and in elucidating potential intervention opportunities.
This analysis was restricted to people living with HIV and did not include a sample of healthy controls. While the study was open to both fatigued and nonfatigued individuals, the large majority of participants reported being fatigued at baseline. Thus in the current analysis we were unable to assess the discriminant validity of the HRFS – the ability of the instrument to distinguish between those expected to be fatigued and non-fatigued. A future comparison of HRFS scores in this sample to scores in a sample of healthy controls would provide helpful further evidence on the utility of the HRFS.
The self-referral method of recruitment in this study may have introduced selection bias. Specifically, individuals experiencing fatigue may have been more likely to respond to study advertisements than those not fatigued; hence, this sample may have higher average fatigue scores than would be observed in a representative sample of people living with HIV. We note that the distributions of age, sex and race in this sample matched closely with the characteristics of prevalent HIV cases from the geographic area of recruitment.
The HRFS fills an important need for research seeking to describe and understand the etiology of HIV-related fatigue (Barroso, 1999; Barroso & Lynn, 2002). With potent antiretroviral therapy extending the lives of people living with HIV, HIV treatment plans must increasingly focus on the effective management of chronic symptoms and side-effects. Chronic fatigue is one of the most prevalent and debilitating symptoms of those living with HIV infection, yet the prevalence and etiology of HIVrelated fatigue have remained challenging to describe, due in part to limitations of existing measures of fatigue. Validation of tools such as the HRFS will facilitate more systematic research to describe the prevalence and characteristics of HIV-related fatigue and investigate its etiology as well as means to alleviate the fatigue of people living with HIV. Indeed, the HRFS has already been adopted by multiple domestic and international research projects. If further research indicates that the HRFS can identify changes in fatigue over time, it may further serve as a useful tool in evaluating the effectiveness of interventions seeking to ameliorate HIV-related fatigue.
Acknowledgments
This research was supported by the National Institute of Nursing Research, National Institutes of Health, 5R01NR008681 (Julie Barroso, PI) and Grant Number 1UL1RR024128-01 from the National Center for Research Resources (NCCR), a component of the National Institutes of Health (NIH) and NIH Roadmap for Medical Research. Its contents are solely the responsibility of the authors and do not necessarily represent the official view of NCRR or NIH.
Footnotes
Publisher's Disclaimer: Full terms and conditions of use: http://www.informaworld.com/terms-and-conditions-of-access.pdf
This article maybe used for research, teaching and private study purposes. Any substantial or systematic reproduction, re-distribution, re-selling, loan or sub-licensing, systematic supply or distribution in any form to anyone is expressly forbidden.
The publisher does not give any warranty express or implied or make any representation that the contents will be complete or accurate or up to date. The accuracy of any instructions, formulae and drug doses should be independently verified with primary sources. The publisher shall not be liable for any loss, actions, claims, proceedings, demand or costs or damages whatsoever or howsoever caused arising directly or indirectly in connection with or arising out of the use of this material.
References
- Aaronson LS, Teel CS, Cassmeyer V, Neuberger GB, Pallikkathayil L, Pierce J, et al. Defining and measuring fatigue. Image–the Journal of Nursing Scholarship. 1999;31:45–50. doi: 10.1111/j.1547-5069.1999.tb00420.x. [DOI] [PubMed] [Google Scholar]
- Barroso J. A review of fatigue in people with HIV infection. Journal of the Association of Nurses in AIDS Care. 1999;10:42–49. doi: 10.1016/S1055-3290(06)60342-7. [DOI] [PubMed] [Google Scholar]
- Barroso J. “Just worn out.” A qualitative study of HIV-related fatigue. In: Funk SG, Tornquist EM, Leeman J, Milers MS, Harrell JS, editors. Key aspects of preventing and managing chronic illness. New York: Springer; 2001. pp. 183–194. [Google Scholar]
- Barroso J, Lynn MR. Psychometric properties of the HIV-Related Fatigue Scale. Journal of the Association of Nurses in AIDS Care. 2002;13:66–75. doi: 10.1016/S1055-3290(06)60242-2. [DOI] [PubMed] [Google Scholar]
- Belza BL, Henke CJ, Yelin EH, Epstein WV, Gilliss CL. Correlates of fatigue in older adults with rheumatoid arthritis. Nursing Research. 1993;42:93–99. [PubMed] [Google Scholar]
- Buysse DJ, Reynolds CF, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Research. 1989;28:193–213. doi: 10.1016/0165-1781(89)90047-4. [DOI] [PubMed] [Google Scholar]
- Carpenter JS, Andrykowski MA. Psychometric evaluation of the Pittsburgh Sleep Quality Index. Journal of Psychosomatic Research. 1998;45:5–13. doi: 10.1016/s0022-3999(97)00298-5. [DOI] [PubMed] [Google Scholar]
- Darko DF, McCutchan JA, Kripke DF, Gillin JC, Golshan S. Fatigue, sleep disturbance, disability and indices of progression of HIV infection. American Journal of Psychiatry. 1992;149:514–520. doi: 10.1176/ajp.149.4.514. [DOI] [PubMed] [Google Scholar]
- Denton GD, Durning SJ, Hemmer PA. A call for use of confidence intervals with correlation coefficients. Teaching and Learning in Medicine. 2004;16:111–112. doi: 10.1207/s15328015tlm1601_20. [DOI] [PubMed] [Google Scholar]
- Duran S, Spire B, Raf F, Walter V, Bouhour D, Journot V, et al. Self-reported symptoms after initiation of a protease inhibitor in HIV-infected patients and their impact on adherence to HAART. HIV Clinical Trials. 2001;2:38–45. doi: 10.1310/R8M7-EQ0M-CNPW-39FC. [DOI] [PubMed] [Google Scholar]
- Fisk JD, Pontefract A, Ritvo PG, Archibald CJ, Murray TJ. The impact of fatigue on patients with multiple sclerosis. Canadian Journal of Neurological Science (Le Journal Canadien des Sciences Neurologiques) 1994;21:9–14. [PubMed] [Google Scholar]
- Harmon J, Barroso J, Pence BW, Leserman J, Salahuddin N. Demographic and illness-related variables associated with HIV-related fatigue. Journal of the Association of Nurses in AIDS Care. doi: 10.1016/j.jana.2007.08.005. in press. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Henderson M, Safa F, Easterbrook P, Hotopf M. Fatigue among HIV-infected patients in the era of highly active antiretroviral therapy. HIV Medicine. 2005;6:347–352. doi: 10.1111/j.1468-1293.2005.00319.x. [DOI] [PubMed] [Google Scholar]
- Hoover DR, Saah AJ, Bacellar H, Murphy R, Visscher B, Anderson R, et al. Signs and symptoms of ‘asymptomatic’ HIV-1 infection in homosexual men. Multicenter AIDS Cohort Study. Journal of Acquired Immune Deficiency Syndromes. 1993;6:66–71. [PubMed] [Google Scholar]
- Jenkin P, Koch T, Kralik D. The experience of fatigue for adults living with HIV. Journal of Clinical Nursing. 2006;15:1123–1131. doi: 10.1111/j.1365-2702.2006.01343.x. [DOI] [PubMed] [Google Scholar]
- Johns MW. Sensitivity and specificity of the Multiple Sleep Latency Test (MSLT), the Maintenance of Wakefulness Test and the Epworth Sleepiness Scale: Failure of the MSLT as a gold standard. Journal of SleepResearch. 2000;9:5–11. doi: 10.1046/j.1365-2869.2000.00177.x. [DOI] [PubMed] [Google Scholar]
- Johns MW. Sleep propensity varies with behaviour and the situation in which it is measured: The concept of somnificity. Journal of SleepResearch. 2002;11:61–67. doi: 10.1046/j.1365-2869.2002.00274.x. [DOI] [PubMed] [Google Scholar]
- Meek P, Nail LM. Internal consistency, reliability and construct validity of a new measure of cancer treatment related fatigue: The General Fatigue Scale (GFS). Oncology Nursing Society Annual Congress; New Orleans, LA. 1997. [Google Scholar]
- Nunnally JC. Psychometric theory. 2. New York: McGraw-Hill; 1978. [Google Scholar]
- O’Dell MW, Meighen M, Riggs RV. Correlates of fatigue in HIV infection prior to AIDS: A pilot study. Disability & Rehabilitation. 1996;18:249–254. doi: 10.3109/09638289609166309. [DOI] [PubMed] [Google Scholar]
- Palenicek J, Nelson KE, Vlahov D, Galai N, Cohn S, Saah AJ. Comparison of clinical symptoms of human immunodeficiency virus disease between intravenous drug users and homosexual men. Archives of Internal Medicine. 1993;153:1806–1812. [PubMed] [Google Scholar]
- Penkower L, Dew MA, Kingsley L, Zhou SY, Lyketsos CG, Wesch J, et al. Alcohol consumption as a cofactor in the progression of HIV infection and AIDS. Alcohol. 1995;12:547–552. doi: 10.1016/0741-8329(95)00042-9. [DOI] [PubMed] [Google Scholar]
- Perkins DO, Leserman J, Stern RA, Baum SF, Liao D, Golden RN, et al. Somatic symptoms and HIV infection: Relationship to depressive symptoms and indicators of HIV disease. American Journal of Psychiatry. 1995;152:1776–1781. doi: 10.1176/ajp.152.12.1776. [DOI] [PubMed] [Google Scholar]
- Piedrola G, Casado JL, Lopez E, Moreno A, Perez-Elias MJ, Garcia-Robles R. Clinical features of adrenal insufficiency in patients with acquired immunodeficiency syndrome. Clinical Endocrinology (Oxf) 1996;45:97–101. doi: 10.1111/j.1365-2265.1996.tb02066.x. [DOI] [PubMed] [Google Scholar]
- Reillo MR. Hyperbaric oxygen therapy for the treatment of debilitating fatigue associated with HIV/AIDS. Journal of the Association of Nurses in AIDS Care. 1993;4:33–38. [PubMed] [Google Scholar]
- Schwartz JE, Jandorf L, Krupp LB. The measurement of fatigue: A new instrument. Journal of Psychosomitic Research. 1993;37:753–762. doi: 10.1016/0022-3999(93)90104-n. [DOI] [PubMed] [Google Scholar]
- Singh N, Squier C, Sivek C, Wagener MM, Yu VL. Psychological stress and depression in older patients with intravenous drug use and human immunodeficiency virus infection: Implications for intervention. International Journal of STD & AIDS. 1997;8:251–255. doi: 10.1258/0956462971920000. [DOI] [PubMed] [Google Scholar]
- Vlahov D, Munoz A, Solomon L, Astemborski J, Lindsay A, Anderson J, et al. Comparison of clinical manifestations of HIV infection between male and female injecting drug users. Aids. 1994;8:819–823. doi: 10.1097/00002030-199406000-00015. [DOI] [PubMed] [Google Scholar]
- Voss J. Predictors and correlates of fatigue in HIV/AIDS. Journal of Pain and Symptom Management. 2005;29:173–184. doi: 10.1016/j.jpainsymman.2004.05.006. [DOI] [PubMed] [Google Scholar]
- Ware JE, Jr, Kosinski M, Bayliss MS, McHorney CA, Rogers WH, Raczek A. Comparison of methods for the scoring and statistical analysis of SF-36 health profile and summary measures: Summary of results from the Medical Outcomes Study. Medical Care. 1995;33(Suppl 4):AS264–AS279. [PubMed] [Google Scholar]
- Ware JE, Jr, Sherbourne CD. The MOS 36-item short-form health survey (SF-36) I. Conceptual framework and item selection. Medical Care. 1992;30:473–483. [PubMed] [Google Scholar]
- Whalen CC, Antani M, Carey J, Landefeld CS. An index of symptoms for infection with human immunodeficiency virus: Reliability and validity. Journal of Clinical Epidemiology. 1994;47:537–546. doi: 10.1016/0895-4356(94)90300-x. [DOI] [PubMed] [Google Scholar]